Abstract
Charcot–Marie–Tooth disease (CMT) subsumes many different inherited neuropathies. CMT and related neuropathies are among the most common inherited neurological disorders, affecting ~1 in 2,500 people globally and including both sexes. Mutations in genes that cause demyelinating forms of CMT often affect the proteins of the myelin sheath, the unfolded protein response, endosomal signalling and recycling, or key transcription factors. Mutations in genes that cause axonal forms often affect mitochondrial biology, aminoacyl-tRNA synthetases, molecular chaperones or the axonal cytoskeleton. All forms of CMT result in length-dependent, progressive axonal loss that correlates with clinical impairments such as distal upper and lower limb weakness, musculoskeletal deformity, absent deep tendon reflexes and distal sensory deficits. Compared with the general population, children and adults with CMT have reduced quality of life across physical, emotional and social domains, with the physical domain being the most disabling. Disease-modifying therapies are not yet available for any form of CMT. Management includes rehabilitative approaches such as muscle strength training and orthotic devices, surgical interventions, symptom relief and anticipatory monitoring of associated complications. The investigation of genetically authentic cellular, organoid and animal models will enable the development of rational therapies. Natural history studies and biomarkers will enable potential therapies to be critically evaluated.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 1 digital issues and online access to articles
$119.00 per year
only $119.00 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Tooth, H. H. The peroneal type of progressive muscular atrophy. Thesis, Univ. Cambridge (H. K. Lewis, 1886).
Charcot, J. & Marie, P. Sur une forme particulière d’atrophie musculaire progressive: souvent familial, débutante par les pieds et les jambes et atteignant plus tard les mains [French]. Rev. Med. 6, 97–138 (1886).
Deenen, J. C. W., Verbeek, A. L. M., Verschuuren, J. J. G. M., van Engelen, B. G. M. & Voermans, N. C. Prevalence and incidence rates of 17 neuromuscular disorders: an updated review of the literature. J. Neuromuscul. Dis. https://doi.org/10.1177/22143602241313118 (2025).
Skre, H. Genetic and clinical aspects of Charcot-Marie-Tooth disease. Clin. Genet. 6, 98–118 (1974).
Johnson, N. E. et al. Patient identification of the symptomatic impact of Charcot-Marie-Tooth disease type 1A. J. Clin. Neuromuscul. Dis. 15, 19–23 (2013).
Burns, J., Ramchandren, S., Ryan, M. M., Shy, M. & Ouvrier, R. A. Determinants of reduced health-related quality of life in pediatric inherited neuropathies. Neurology 75, 726–731 (2010).
Fridman, V. et al. CMT subtypes and disease burden in patients enrolled in the Inherited Neuropathies Consortium natural history study: a cross-sectional analysis. J. Neurol. Neurosurg. Psychiatry 86, 873–878 (2015). This is a very large cohort study analysing data from 1,652 patients evaluated at 13 specialist centres and determining the distribution of CMT subtypes and disease burden.
Record, C. J. et al. Whole genome sequencing increases the diagnostic rate in Charcot-Marie-Tooth disease. Brain 147, 3144–3156 (2024). This study analyses the diagnostic rate of a large cohort of patients in a single specialist inherited neuropathy centre.
Yiu, E. M. et al. Clinical practice guideline for the management of paediatric Charcot-Marie-Tooth disease. J. Neurol. Neurosurg. Psychiatry 93, 530–538 (2022). These international clinical practice guidelines provide evidence-based and consensus-based management recommendations for children with CMT, promote optimal and standardized care, and can be used to advocate for and improve access to multidisciplinary services.
Sivera Mascaro, R. et al. Clinical practice guidelines for the diagnosis and management of Charcot-Marie-Tooth disease. Neurologia 40, 290–305 (2024).
Marttila, M. et al. Molecular epidemiology of Charcot-Marie-Tooth disease in Northern Ostrobothnia, Finland: a population-based study. Neuroepidemiology 49, 34–39 (2017).
Carey, I. M. et al. Prevalence and incidence of neuromuscular conditions in the UK between 2000 and 2019: a retrospective study using primary care data. PLoS ONE 16, e0261983 (2021).
Müller, K. I., Ghelue, M. V., Lund, I., Jonsrud, C. & Arntzen, K. A. The prevalence of hereditary neuromuscular disorders in Northern Norway. Brain Behav. https://doi.org/10.1002/brb3.1948 (2021).
Ma, M. et al. A meta-analysis on the prevalence of Charcot-Marie-Tooth disease and related inherited peripheral neuropathies. J. Neurol. 270, 2468–2482 (2023).
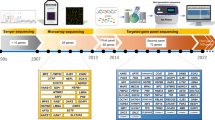
Pipis, M., Rossor, A. M., Laura, M. & Reilly, M. M. Next-generation sequencing in Charcot–Marie–Tooth disease: opportunities and challenges. Nat. Rev. Neurol. 15, 644–656 (2019).
Park, H. J., Choi, Y. C., Oh, J. W. & Yi, S. W. Prevalence, mortality, and cause of death in Charcot-Marie-Tooth disease in Korea: a nationwide, population-based study. Neuroepidemiology 54, 313–319 (2020).
Braathen, G. J. Genetic epidemiology of Charcot-Marie-Tooth disease. Acta Neurol. Scand. https://doi.org/10.1111/ane.12013 (2012).
Khedr, E. M. et al. Prevalence of neuromuscular disorders in Qena governorate/Egypt: population-based survey. Neurological Res. 38, 1056–1063 (2016).
Yalcouyé, A., Esoh, K., Guida, L. & Wonkam, A. Current profile of Charcot-Marie-Tooth disease in Africa: a systematic review. J. Peripher. Nerv. Syst. 27, 100–112 (2022).
Theadom, A. et al. Prevalence of Charcot-Marie-Tooth disease across the lifespan: a population-based epidemiological study. BMJ Open https://doi.org/10.1136/bmjopen-2019-029240 (2019).
Barreto, L. C. et al. Epidemiologic study of Charcot-Marie-Tooth Disease: a systematic review. Neuroepidemiology 46, 157–165 (2016).
Pisciotta, C. et al. Clinical spectrum and frequency of Charcot–Marie–Tooth disease in Italy: data from the national CMT registry. Eur. J. Neurol. 30, 2461–2470 (2023).
Cornett, K. M. D. et al. Phenotypic variability of childhood Charcot-Marie-Tooth disease. JAMA Neurol. 73, 645–651 (2016).
Roggenbuck, J. et al. Diagnostic and clinical utility of comprehensive multigene panel testing for patients with neuropathy. J. Peripher. Nerv. Syst. 29, 363–367 (2024).
Ma, Y., Duan, X., Liu, X. & Fan, D. Clinical and mutational spectrum of paediatric Charcot-Marie-Tooth disease in a large cohort of Chinese patients. Front. Genet. https://doi.org/10.3389/fgene.2023.1188361 (2023).
Sivera, R. et al. Charcot-Marie-Tooth disease: genetic and clinical spectrum in a Spanish clinical series. Neurology 81, 1617–1625 (2013).
Abe, A. et al. Molecular diagnosis and clinical onset of Charcot-Marie-Tooth disease in Japan. J. Hum. Genet. 56, 364–368 (2011).
Hayashi, M. et al. Molecular analysis of the genes causing recessive demyelinating Charcot-Marie-Tooth disease in Japan. J. Hum. Genet. 58, 273–278 (2013).
Candayan, A., Parman, Y. & Battaloğlu, E. Clinical and genetic survey for Charcot-Marie-Tooth neuropathy based on the findings in Turkey, a country with a high rate of consanguineous marriages. Balk. Med. J. 39, 3–11 (2022).
Sevilla, T. et al. Genetics of the Charcot-Marie-Tooth disease in the Spanish Gypsy population: the hereditary motor and sensory neuropathy-Russe in depth. Clin. Genet. 83, 565–570 (2013).
Gooding, R. et al. A novel Gypsy founder mutation, p.Arg1109X in the CMT4C gene, causes variable peripheral neuropathy phenotypes. J. Med. Genet. 42, e69 (2005).
Aboussouan, L. S., Lewis, R. A. & Shy, M. E. Disorders of pulmonary function, sleep, and the upper airway in Charcot-Marie-Tooth disease. Lung 185, 1–7 (2007).
Boerkoel, C. F., Takashima, H., Bacino, C. A., Daentl, D. & Lupski, J. R. EGR2 mutation R359W causes a spectrum of Dejerine-Sottas neuropathy. Neurogenetics 3, 153–157 (2001).
Gabreëls-Festen, A. Dejerine-Sottas syndrome grown to maturity: overview of genetic and morphological heterogeneity and follow-up of 25 patients. J. Anat. 200, 341–356 (2002).
Kosmanopoulos, G. P. et al. TRPV4 neuromuscular disease registry highlights bulbar, skeletal and proximal limb manifestations. Brain 148, 238–251 (2025).
Vaeth, S., Vaeth, M., Andersen, H., Christensen, R. & Jensen, U. B. Charcot-Marie-Tooth disease in Denmark: a nationwide register-based study of mortality, prevalence and incidence. BMJ Open https://doi.org/10.1136/bmjopen-2017-018048 (2017).
Schorling, E. et al. Cost of illness in Charcot-Marie-Tooth neuropathy: results from Germany. Neurology 92, E2027–E2037 (2019).
Sullivan, J. M. et al. Gain-of-function mutations of TRPV4 acting in endothelial cells drive blood-CNS barrier breakdown and motor neuron degeneration in mice. Sci. Transl. Med. 16, eadk1358 (2024).
Abrams, C. K. & Scherer, S. S. Gap junctions in inherited human disorders of the central nervous system. Biochim. Biophys. Acta 1818, 2030–2047 (2012).
Pashkova, N. et al. Disrupting the transmembrane domain interface between PMP22 and MPZ causes peripheral neuropathy. iScience 27, 110989 (2024).
Prior, R. et al. PMP22 duplication dysregulates lipid homeostasis and plasma membrane organization in developing human Schwann cells. Brain 147, 3113–3130 (2024). This study takes advantage of a CMT1A mouse model and patient-derived induced pluripotent stem cells differentiated into Schwann cell precursors to show how the PMP22 duplication leads to plasma membrane disruptions by altered intracellular lipid homeostasis and the potential therapeutic target of this disease mechanism in CMT1A.
Kister, A. & Kister, I. Overview of myelin, major myelin lipids, and myelin-associated proteins. Front. Chem. 10, 1041961 (2022).
Hetz, C., Zhang, K. & Kaufman, R. J. Mechanisms, regulation and functions of the unfolded protein response. Nat. Rev. Mol. Cell Biol. 21, 421–438 (2020).
Fridman, V. & Saporta, M. A. Mechanisms and treatments in demyelinating CMT. Neurotherapeutics 18, 2236–2268 (2021).
Wrabetz, L. et al. Different intracellular pathomechanisms produce diverse myelin protein zero neuropathies in transgenic mice. J. Neurosci. 26, 2358–2368 (2006).
Fratta, P. et al. A nonsense mutation in myelin protein zero causes congenital hypomyelination neuropathy through altered P0 membrane targeting and gain of abnormal function. Hum. Mol. Genet. 28, 124–132 (2019).
Veneri, F. A. et al. A novel mouse model of CMT1B identifies hyperglycosylation as a new pathogenetic mechanism. Hum. Mol. Genet. 31, 4255–4274 (2022).
Shackleford, G. et al. A new mouse model of Charcot-Marie-Tooth 2 J neuropathy replicates human axonopathy and suggest alteration in axo-glia communication. PLoS Genet. 18, e1010477 (2022).
Stendel, C. et al. SH3TC2, a protein mutant in Charcot-Marie-Tooth neuropathy, links peripheral nerve myelination to endosomal recycling. Brain 133, 2462–2474 (2010).
Roberts, R. C. et al. Mistargeting of SH3TC2 away from the recycling endosome causes Charcot-Marie-Tooth disease type 4C. Hum. Mol. Genet. 19, 1009–1018 (2010).
Edgar, J. R. et al. A dysfunctional endolysosomal pathway common to two sub-types of demyelinating Charcot-Marie-Tooth disease. Acta Neuropathol. Commun. 8, 165 (2020).
Williams, A. C. & Brophy, P. J. The function of the Periaxin gene during nerve repair in a model of CMT4F. J. Anat. 200, 323–330 (2002).
Sivera, R. et al. Expanding the clinical spectrum of DRP2-associated Charcot-Marie-Tooth disease. Neurology 102, e209174 (2024).
Brennan, K. M. et al. Absence of dystrophin related protein-2 disrupts Cajal bands in a patient with Charcot-Marie-Tooth disease. Neuromuscul. Disord. 25, 786–793 (2015).
Marchesi, C. et al. Four novel cases of periaxin-related neuropathy and review of the literature. Neurology 75, 1830–1838 (2010).
Sherman, D. L., Wu, L. M., Grove, M., Gillespie, C. S. & Brophy, P. J. Drp2 and periaxin form cajal bands with dystroglycan but have distinct roles in Schwann cell growth. J. Neurosci. 32, 9419–9428 (2012).
Burgess, R. W. & Storkebaum, E. tRNA dysregulation in neurodevelopmental and neurodegenerative diseases. Annu. Rev. Cell Dev. Biol. 39, 223–252 (2023).
Tennakoon, R. & Cui, H. Aminoacyl-tRNA synthetases. Curr. Biol. 34, R884–R888 (2024).
Mora, N. et al. Glycyl-tRNA sequestration is a unifying mechanism underlying GARS1-associated peripheral neuropathy. Nucleic Acids Res. https://doi.org/10.1093/nar/gkaf201 (2025).
Ermanoska, B. et al. Tyrosyl-tRNA synthetase has a noncanonical function in actin bundling. Nat. Commun. 14, 999 (2023). This study shows how mutations in YARS1 , one of the tRNA synthetases, result in CMT through a non-canonical function involving actin bundling and thereby highlight the need to consider non-canonical protein functions when investigating primary disease mechanisms in CMT.
Jones, E. A. et al. Regulation of the PMP22 gene through an intronic enhancer. J. Neurosci. 31, 4242–4250 (2011).
Jones, E. A. et al. Interactions of Sox10 and Egr2 in myelin gene regulation. Neuron Glia Biol. 3, 377–387 (2007).
Mathis, S. et al. Neuropathologic characterization of INF2-related Charcot-Marie-Tooth disease: evidence for a Schwann cell actinopathy. J. Neuropathol. Exp. Neurol. 73, 223–233 (2014).
Gatti, P., Schiavon, C., Cicero, J., Manor, U. & Germain, M. Mitochondria- and ER-associated actin are required for mitochondrial fusion. Nat. Commun. 16, 451 (2025).
Labat-de-Hoz, L., Jiménez, M., Correas, I. & Alonso, M. A. Regulation of formin INF2 and its alteration in INF2-linked inherited disorders. Cell Mol. Life Sci. 81, 463 (2024).
McCray, B. A. et al. Neuropathy-causing TRPV4 mutations disrupt TRPV4-RhoA interactions and impair neurite extension. Nat. Commun. 12, 1444 (2021).
Kotaich, F., Caillol, D. & Bomont, P. Neurofilaments in health and Charcot-Marie-Tooth disease. Front. Cell Dev. Biol. 11, 1275155 (2023).
Lancaster, E. et al. Myelinated axons fail to develop properly in a genetically authentic mouse model of Charcot-Marie-Tooth disease type 2E. Exp. Neurol. 308, 13–25 (2018).
Van de Vondel, L., De Winter, J., Timmerman, V. & Baets, J. Overarching pathomechanisms in inherited peripheral neuropathies, spastic paraplegias, and cerebellar ataxias. Trends Neurosci. 47, 227–238 (2024).
Markworth, R., Bähr, M. & Burk, K. Held up in traffic-defects in the trafficking machinery in Charcot-Marie-Tooth Disease. Front. Mol. Neurosci. 14, 695294 (2021).
Benoy, V. et al. Development of improved HDAC6 inhibitors as pharmacological therapy for axonal Charcot-Marie-Tooth Disease. Neurotherapeutics 14, 417–428 (2017).
Beijer, D., Sisto, A., Van Lent, J., Baets, J. & Timmerman, V. Defects in axonal transport in inherited neuropathies. J. Neuromuscul. Dis. 6, 401–419 (2019).
Sisto, A. et al. Autophagy induction by piplartine ameliorates axonal degeneration caused by mutant HSPB1 and HSPB8 in Charcot-Marie-Tooth type 2 neuropathies. Autophagy 21, 1116–1143 (2025).
Vendredy, L., Adriaenssens, E. & Timmerman, V. Small heat shock proteins in neurodegenerative diseases. Cell Stress Chaperones 25, 679–699 (2020).
Palaima, P., Berciano, J., Peeters, K. & Jordanova, A. LRSAM1 and the RING domain: Charcot-Marie-Tooth disease and beyond. Orphanet J. Rare Dis. 16, 74 (2021).
Lu, J. Q. & Tarnopolsky, M. A. Mitochondrial neuropathy and neurogenic features in mitochondrial myopathy. Mitochondrion 56, 52–61 (2021).
Ferreira, T. et al. Variants in mitochondrial disease genes are common causes of inherited peripheral neuropathies. J. Neurol. 271, 3546–3553 (2024).
Chen, W., Zhao, H. & Li, Y. Mitochondrial dynamics in health and disease: mechanisms and potential targets. Signal. Transduct. Target. Ther. 8, 333 (2023).
Niemann, A. et al. The Gdap1 knockout mouse mechanistically links redox control to Charcot-Marie-Tooth disease. Brain 137, 668–682 (2014).
Wolf, C. et al. GDAP1 loss of function inhibits the mitochondrial pyruvate dehydrogenase complex by altering the actin cytoskeleton. Commun. Biol. 5, 541 (2022).
Rebelo, A. P. et al. SORD-deficient rats develop a motor-predominant peripheral neuropathy unveiling novel pathophysiological insights. Brain 147, 3131–3143 (2024).
Cortese, A. et al. Biallelic mutations in SORD cause a common and potentially treatable hereditary neuropathy with implications for diabetes. Nat. Genet. 52, 473–481 (2020).
Penno, A. et al. Hereditary sensory neuropathy type 1 is caused by the accumulation of two neurotoxic sphingolipids. J. Biol. Chem. 285, 11178–11187 (2010).
Garofalo, E. et al. Oral L-serine supplementation in mice and humans with hereditary sensory autonomic neuropathy type 1. J. Clin. Invest. 121, 4735–4745 (2011).
Beijer, D. et al. A recurrent missense variant in ITPR3 causes demyelinating Charcot-Marie-Tooth with variable severity. Brain 148, 227–237 (2025).
Van Lent, J. et al. Advances and challenges in modeling inherited peripheral neuropathies using iPSCs. Exp. Mol. Med. 56, 1348–1364 (2024).
Pareyson, D. & Marchesi, C. Natural history and treatment of peripheral inherited neuropathies. Adv. Exp. Med. Biol. 652, 207–224 (2009).
Figley, M. D. & DiAntonio, A. The SARM1 axon degeneration pathway: control of the NAD+ metabolome regulates axon survival in health and disease. Curr. Opin. Neurobiol. 63, 59–66 (2020).
Moss, K. R., Bopp, T. S., Johnson, A. E. & Höke, A. New evidence for secondary axonal degeneration in demyelinating neuropathies. Neurosci. Lett. 744, 135595 (2021).
Sato-Yamada, Y. et al. A SARM1-mitochondrial feedback loop drives neuropathogenesis in a Charcot-Marie-Tooth disease type 2A rat model. J. Clin. Invest. https://doi.org/10.1172/JCI161566 (2022). This study reveals that mitochondrial defects in CMT2A activate SARM1, which amplifies axonal degeneration through a damaging feedback loop, and that SARM1 deletion breaks this cycle to restore neuronal integrity.
Rossaert, E. & Van Den Bosch, L. HDAC6 inhibitors: translating genetic and molecular insights into a therapy for axonal CMT. Brain Res. 1733, 146692 (2020).
Le Pichon, C. E. et al. Loss of dual leucine zipper kinase signaling is protective in animal models of neurodegenerative disease. Sci. Transl. Med. https://doi.org/10.1126/scitranslmed.aag0394 (2017).
Klein, D. & Martini, R. Myelin and macrophages in the PNS: an intimate relationship in trauma and disease. Brain Res. 1641, 130–138 (2016).
Bosco, L., Falzone, Y. M. & Previtali, S. C. Animal models as a tool to design therapeutical strategies for CMT-like hereditary neuropathies. Brain Sci. https://doi.org/10.3390/brainsci11091237 (2021).
Juneja, M., Burns, J., Saporta, M. A. & Timmerman, V. Challenges in modelling the Charcot-Marie-Tooth neuropathies for therapy development. J. Neurol. Neurosurg. Psychiatry 90, 58–67 (2019).
Bouhy, D. & Timmerman, V. Animal models and therapeutic prospects for Charcot-Marie-Tooth disease. Ann. Neurol. 74, 391–396 (2013).
Fledrich, R., Stassart, R. M. & Sereda, M. W. Murine therapeutic models for Charcot-Marie-Tooth (CMT) disease. Br. Med. Bull. 102, 89–113 (2012).
Gautier, B. et al. AAV2/9-mediated silencing of PMP22 prevents the development of pathological features in a rat model of Charcot-Marie-Tooth disease 1A. Nat. Commun. 12, 2356 (2021).
Stavrou, M. et al. A translatable RNAi-driven gene therapy silences PMP22/Pmp22 genes and improves neuropathy in CMT1A mice. J. Clin. Invest. https://doi.org/10.1172/jci159814 (2022). This study provides compelling preclinical evidence that AAV9-delivered RNA interference silencing of PMP22 can durably improve myelination and motor function in CMT1A, supporting its potential as a translatable gene therapy.
Zhao, H. T. et al. PMP22 antisense oligonucleotides reverse Charcot-Marie-Tooth disease type 1A features in rodent models. J. Clin. Invest. 128, 359–368 (2018).
Boutary, S. et al. Squalenoyl siRNA PMP22 nanoparticles are effective in treating mouse models of Charcot-Marie-Tooth disease type 1A. Commun. Biol. 4, 317 (2021).
Das, I. et al. Preventing proteostasis diseases by selective inhibition of a phosphatase regulatory subunit. Science 348, 239–242 (2015). This work demonstrates that selective inhibition of PPP1R15A by Sephin1 prolongs the adaptive UPR, restores proteostasis and prevents neuropathy in a CMT1B mouse model, highlighting UPR modulation as a therapeutic strategy.
D’Antonio, M. et al. Resetting translational homeostasis restores myelination in Charcot-Marie-Tooth disease type 1B mice. J. Exp. Med. 210, 821–838 (2013).
Bai, Y. et al. Treatment with IFB-088 improves neuropathy in CMT1A and CMT1B mice Mol. Neurobiol. 59, 4159–4178 (2022).
Panosyan, F. B. et al. Cross-sectional analysis of a large cohort with X-linked Charcot-Marie-Tooth disease (CMTX1). Neurology 89, 927–935 (2017).
Shy, M. E. et al. CMT1X phenotypes represent loss of GJB1 gene function. Neurology 68, 849–855 (2007).
Kagiava, A. et al. AAV9-mediated Schwann cell-targeted gene therapy rescues a model of demyelinating neuropathy. Gene Ther. 28, 659–675 (2021).
Kagiava, A. et al. Gene replacement therapy in two Golgi-retained CMT1X mutants before and after the onset of demyelinating neuropathy. Mol. Ther. Methods Clin. Dev. 30, 377–393 (2023).
Georgiou, E. et al. AAV9-mediated SH3TC2 gene replacement therapy targeted to Schwann cells for the treatment of CMT4C. Mol. Ther. 31, 3290–3307 (2023).
De Jonghe, P., Timmerman, V., Nelis, E., Martin, J. J. & Van Broeckhoven, C. Charcot-Marie-Tooth disease and related peripheral neuropathies. J. Peripher. Nerv. Syst. 2, 370–387 (1997).
Krajewski, K. M. et al. Neurological dysfunction and axonal degeneration in Charcot-Marie-Tooth disease type 1A. Brain 123, 1516–1527 (2000).
Lewis, R. A., Li, J., Fuerst, D. R., Shy, M. E. & Krajewski, K. Motor unit number estimate of distal and proximal muscles in Charcot-Marie-Tooth disease. Muscle Nerve 28, 161–167 (2003).
Shy, M. E. et al. Reliability and validity of the CMT neuropathy score as a measure of disability. Neurology 64, 1209–1214 (2005).
Wojciechowski, E. et al. Gait patterns of children and adolescents with Charcot-Marie-Tooth disease. Gait Posture 56, 89–94 (2017).
Prada, V. et al. Charcot-Marie-Tooth neuropathy score and ambulation index are both predictors of orthotic need for patients with CMT. Neurol. Sci. 43, 2759–2764 (2022).
Laurá, M. et al. Prevalence and orthopedic management of foot and ankle deformities in Charcot-Marie-Tooth disease. Muscle Nerve 57, 255–259 (2018).
Pareyson, D., Scaioli, V. & Laurà, M. Clinical and electrophysiological aspects of Charcot-Marie-Tooth disease. Neuromol. Med. 8, 3–22 (2006).
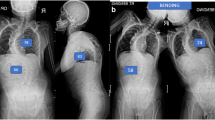
Dwan, L. N. et al. Reliability and sensitivity of radiographic measures of hip dysplasia in childhood Charcot-Marie-Tooth disease. Hip Int. 33, 323–331 (2023).
Karol, L. A. & Elerson, E. Scoliosis in patients with Charcot-Marie-Tooth disease. J. Bone Jt Surg. Am. 89, 1504–1510 (2007).
Leone, E. et al. Incidence and risk factors for patellofemoral dislocation in adults with Charcot-Marie-Tooth disease: an observational study. Physiother. Res. Int. 28, e1996 (2023).
Laurá, M., Pipis, M., Rossor, A. M. & Reilly, M. M. Charcot-Marie-Tooth disease and related disorders: an evolving landscape. Curr. Opin. Neurol. 32, 641–650 (2019).
Eggermann, K. et al. Hereditary neuropathies. Dtsch. Arztebl Int. 115, 91–97 (2018).
Pipis, M. et al. Natural history of Charcot-Marie-Tooth disease type 2A: a large international multicentre study. Brain 143, 3589–3602 (2020).
Sanmaneechai, O. et al. Genotype–phenotype characteristics and baseline natural history of heritable neuropathies caused by mutations in the MPZ gene. Brain 138, 3180–3192 (2015).
Pipis, M. et al. Charcot-Marie-Tooth disease type 2CC due to NEFH variants causes a progressive, non-length-dependent, motor-predominant phenotype. J. Neurol. Neurosurg. Psychiatry 93, 48–56 (2022).
Record, C. J. et al. Genetic analysis and natural history of Charcot-Marie-Tooth disease CMTX1 due to GJB1 variants. Brain 146, 4336–4349 (2023).
Bertini, A. et al. Disease progression in Charcot-Marie-Tooth disease type 4B (CMT4B) associated with mutations in myotubularin-related proteins 2 and 13. Eur. J. Neurol. 32, e70084 (2025).
Cortese, A. et al. Genotype and phenotype spectrum of Charcot-Marie-Tooth disease due to mutations in SORD. Brain https://doi.org/10.1093/brain/awaf021 (2025). This cross-sectional, multicentre study evaluated the genotype and phenotype spectrum of 144 patients with SORD deficiency, a relatively newly identified CMT subtype that causes axonal, motor-predominant CMT.
Attarian, S., Fatehi, F., Rajabally, Y. A. & Pareyson, D. Hereditary neuropathy with liability to pressure palsies. J. Neurol. 267, 2198–2206 (2020).
Li, J., Krajewski, K., Shy, M. E. & Lewis, R. A. Hereditary neuropathy with liability to pressure palsy. Neurology 58, 1769–1773 (2002).
Dubourg, O., Mouton, P., Brice, A., LeGuern, E. & Bouche, P. Guidelines for diagnosis of hereditary neuropathy with liability to pressure palsies. Neuromuscul. Disord. 10, 206–208 (2000).
Rossor, A. M., Haddad, S. & Reilly, M. M. The evolving spectrum of complex inherited neuropathies. Curr. Opin. Neurol. 37, 427–444 (2024).
Yiu, E. M. & Ryan, M. M. Genetic axonal neuropathies and neuronopathies of pre-natal and infantile onset. J. Peripher. Nerv. Syst. 17, 285–300 (2012).
Yiu, E. M. & Ryan, M. M. Demyelinating prenatal and infantile developmental neuropathies. J. Peripher. Nerv. Syst. 17, 32–52 (2012).
Lischka, A. et al. Genetic pain loss disorders. Nat. Rev. Dis. Primers 8, 41 (2022).
England, J. D. et al. Practice parameter: evaluation of distal symmetric polyneuropathy: role of laboratory and genetic testing (an evidence-based review). Neurology 72, 185–192 (2009).
Bontrager, J. E. et al. Urine sorbitol and xylitol for the diagnosis of sorbitol dehydrogenase deficiency-related neuropathy. Neurology 105, e214425 (2025).
Nicholson, G. & Nash, J. Intermediate nerve conduction velocities define X-linked Charcot-Marie-Tooth neuropathy families. Neurology 43, 2558–2564 (1993).
Rouger, H. et al. Charcot-Marie-Tooth disease with intermediate motor nerve conduction velocities: characterization of 14 Cx32 mutations in 35 families. Hum. Mutat. 10, 443–452 (1997).
De Jonghe, P., Timmerman, V. & Van Broeckhoven, C. 2nd Workshop of the European CMT consortium: 53rd ENMC international workshop on classification and diagnostic guidelines for Charcot-Marie-Tooth Type 2 (CMT2-HMSN II) and distal hereditary motor neuropathy (distal HMN-spinal CMT) 26-28 September 1997, Naarden, The Netherlands. Neuromuscul. Disord. 8, 426–431 (1998).
Kaku, D. A., Parry, G. J., Malamut, R., Lupski, J. R. & Garcia, C. A. Uniform slowing of conduction velocities in Charcot-Marie-Tooth polyneuropathy type 1. Neurology 43, 2664–2667 (1993).
Lewis, R. A. & Sumner, A. J. The electrodiagnostic distinctions between chronic familial and acquired demyelinative neuropathies. Neurology 32, 592–596 (1982).
Record, C. J. et al. Recessive variants in PIGG cause a motor neuropathy with variable conduction block, childhood tremor, and febrile seizures: expanding the phenotype. Ann. Neurol. 97, 388–396 (2025).
Record, C. J. et al. Unusual upper limb features in SORD neuropathy. J. Peripher. Nerv. Syst. 27, 175–177 (2022).
Villar-Quiles, R. N. et al. Leukoencephalopathy and conduction blocks in PLEKHG5-associated intermediate CMT disease. Neuromuscul. Disord. 31, 756–764 (2021).
Frezatti, R. S. S. et al. Conduction block and temporal dispersion in a SIGMAR1-related neuropathy. J. Peripher. Nerv. Syst. 27, 316–319 (2022).
Parmar, J. M., Laing, N. G., Kennerson, M. L. & Ravenscroft, G. Genetics of inherited peripheral neuropathies and the next frontier: looking backwards to progress forwards. J. Neurology, Neurosurg. Psychiatry 95, 992–1001 (2024).
Cortese, A. et al. Biallelic expansion of an intronic repeat in RFC1 is a common cause of late-onset ataxia. Nat. Genet. 51, 649–658 (2019).
Grosz, B. R. et al. Long read sequencing overcomes challenges in the diagnosis of SORD neuropathy. J. Peripher. Nerv. Syst. 27, 120–126 (2022).
Ando, M. et al. Clinical phenotypic diversity of NOTCH2NLC-related disease in the largest case series of inherited peripheral neuropathy in Japan. J. Neurol. Neurosurg. Psychiatry 94, 622–630 (2023).
Hobara, T. et al. Linking LRP12 CGG repeat expansion to inherited peripheral neuropathy. J. Neurol. Neurosurg. Psychiatry 96, 140–149 (2025).
Liao, Y. C. et al. GGC repeat expansion of NOTCH2NLC in Taiwanese patients with inherited neuropathies. Neurology 98, e199–e206 (2022).
Wang, H. et al. GGC repeat expansion in the NOTCH2NLC gene is associated with a phenotype of predominant motor-sensory and autonomic neuropathy. Front. Genet. 12, 694790 (2021).
Yu, J. et al. GGC repeat expansions in NOTCH2NLC causing a phenotype of distal motor neuropathy and myopathy. Ann. Clin. Transl. Neurol. 8, 1330–1342 (2021).
Groza, C. et al. Pangenome graphs improve the analysis of structural variants in rare genetic diseases. Nat. Commun. 15, 657 (2024).
Castaldi, P. J., Abood, A., Farber, C. R. & Sheynkman, G. M. Bridging the splicing gap in human genetics with long-read RNA sequencing: finding the protein isoform drivers of disease. Hum. Mol. Genet. 31, R123–R136 (2022).
Bis-Brewer, D. M., Fazal, S. & Züchner, S. Genetic modifiers and non-Mendelian aspects of CMT. Brain Res. 1726, 146459 (2020).
Tao, F. et al. Variation in SIPA1L2 is correlated with phenotype modification in Charcot-Marie-Tooth disease type 1A. Ann. Neurol. 85, 316–330 (2019).
Richards, S. et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet. Med. 17, 405–424 (2015).
Joynt, A. C. M., Axford, M. M., Chad, L. & Costain, G. Understanding genetic variants of uncertain significance. Paediatrics Child. Health 27, 10–11 (2022).
Hoffman-Andrews, L. The known unknown: the challenges of genetic variants of uncertain significance in clinical practice. J. Law Biosci. 4, 648–657 (2017).
Chen, E. et al. Rates and classification of variants of uncertain significance in hereditary disease genetic testing. JAMA Netw. Open. 6, e2339571 (2023).
Bailey, E. et al. INSPIRE CMT-SORD clinical trial: month 18 and month 24 results and designing the next randomized study [abstract O 597]. J. Peripher. Nerv. Syst. 30, S262 (2025).
Gazulla, J., Almárcegui, C. & Berciano, J. Reversible inflammatory neuropathy superimposed on Charcot-Marie-Tooth type 1A disease. Neurol. Sci. 39, 793–794 (2018).
Hoffman, E. M. et al. Impairments and comorbidities of polyneuropathy revealed by population-based analyses. Neurology 84, 1644–1651 (2015).
Kapoor, M. et al. Plasma neurofilament light chain concentration is increased and correlates with the severity of neuropathy in hereditary transthyretin amyloidosis. J. Peripher. Nerv. Syst. https://doi.org/10.1111/jns.12350 (2019).
Evans, M. R. B. et al. Twelve-month change in quantitative MRI calf muscle fat fraction in CMT1A predicts clinical change over 4 years. Ann. Clin. Transl. Neurol. https://doi.org/10.1002/acn3.52314 (2025). This study in patients with CMT1A demonstrates that a 12-month change in calf muscle fat fraction on MRI correlates with clinical progression over 4 years, as measured by the CMT examination score.
Morrow, J. M. et al. MRI biomarker assessment of neuromuscular disease progression: a prospective observational cohort study. Lancet Neurol. https://doi.org/10.1016/S1474-4422(15)00242-2 (2015).
Svaren, J. et al. Schwann cell transcript biomarkers for hereditary neuropathy skin biopsies. Ann. Neurol. 85, 887–898 (2019).
Wang, H. et al. Transmembrane protease serine 5: a novel Schwann cell plasma marker for CMT1A. Ann. Clin. Transl. Neurol. 7, 69–82 (2020).
Fridman, V. et al. Randomized trial of l-serine in patients with hereditary sensory and autonomic neuropathy type 1. Neurology https://doi.org/10.1212/wnl.0000000000006811 (2019).
Burns, J. et al. Validation of the Charcot-Marie-Tooth disease pediatric scale as an outcome measure of disability. Ann. Neurol. 71, 642–652 (2012).
Mandarakas, M. R. et al. Development and validation of the Charcot-Marie-Tooth disease infant scale. Brain 141, 3319–3330 (2018).
Mandarakas, M. R. et al. Multicenter validation of the Charcot-Marie-Tooth functional outcome measure. Neurology 102, e207963 (2024).
McKay, M. J. et al. Reference values for developing responsive functional outcome measures across the lifespan. Neurology 88, 1512–1519 (2017).
McKay, M. J. et al. Normative reference values for strength and flexibility of 1,000 children and adults. Neurology 88, 36–43 (2017).
Cornett, K. M. D. et al. Designing and implementing a web-based platform for accurate and reliable clinical outcome measures and global certification for evaluating Charcot-Marie-Tooth disease. J. Peripher. Nerv. Syst. 30, e70062 (2025).
Sadjadi, R. et al. Psychometrics evaluation of Charcot-Marie-Tooth Neuropathy Score (CMTNSv2) second version, using Rasch analysis. J. Peripher. Nerv. Syst. 19, 192–196 (2014).
Ramchandren, S. et al. Development and validation of the pediatric Charcot-Marie-Tooth disease quality of life outcome measure. Ann. Neurol. 89, 369–379 (2021).
Wu, T. T. et al. Validation of the parent-proxy pediatric Charcot-Marie-Tooth disease quality of life outcome measure. J. Peripher. Nerv. Syst. 28, 237–251 (2023).
Wu, T. T. et al. Validation of the parent-proxy version of the pediatric Charcot-Marie-Tooth disease quality of life instrument for children aged 0-7 years. J. Peripher. Nerv. Syst. 28, 382–389 (2023).
Food and Drug Administration. Digital Health Technologies for Remote Data Acquisition in Clinical Investigations: Guidance for Industry, Investigators, and Other Stakeholders https://www.fda.gov/regulatory-information/search-fda-guidance-documents/digital-health-technologies-remote-data-acquisition-clinical-investigations (FDA, 2023).
Cornett, K. et al. Evaluating physical activity, gait and balance using wearable sensors in pediatric CMT [abstract O 537]. J. Peripher. Nerv. Syst. 30, S233 (2025).
Padua, L. et al. Novel outcome measures for Charcot-Marie-Tooth disease: validation and reliability of the 6-min walk test and stepwatch activity monitor and identification of the walking features related to higher quality of life. Eur. J. Neurol. 23, 1343–1350 (2016).
Siskind, C. E. et al. A review of genetic counseling for Charcot Marie Tooth disease (CMT). J. Genet. Couns. 22, 422–436 (2013).
Conde, R. M., Senem, I., Dos Santos, M., de Lima Osorio, F. & Marques Junior, W. Effectiveness of exercise therapy for individuals diagnosed with Charcot-Marie-Tooth disease: a systematic review of randomized clinical trials. J. Peripher. Nerv. Syst. 28, 169–178 (2023).
Burns, J. et al. Safety and efficacy of progressive resistance exercise for Charcot-Marie-Tooth disease in children: a randomised, double-blind, sham-controlled trial. Lancet Child. Adolesc. Health 1, 106–113 (2017). This paper provides evidence from a randomized, controlled trial of the effectiveness and safety of progressive resistance exercise on ankle dorsiflexion strength.
Ramdharry, G. M. et al. A pilot study of proximal strength training in Charcot-Marie-Tooth disease. J. Peripher. Nerv. Syst. 19, 328–332 (2014).
Lindeman, E. et al. Strength training in patients with myotonic dystrophy and hereditary motor and sensory neuropathy: a randomized clinical trial. Arch. Phys. Med. Rehabil. 76, 612–620 (1995).
Wallace, A. et al. Community exercise is feasible for neuromuscular diseases and can improve aerobic capacity. Neurology 92, e1773–e1785 (2019).
Ferraro, F. et al. Effects of intensive rehabilitation on functioning in patients with mild and moderate Charcot-Marie-Tooth disease: a real-practice retrospective study. Neurol. Sci. 45, 289–297 (2024).
Mori, L. et al. Treadmill training in patients affected by Charcot-Marie-Tooth neuropathy: results of a multicenter, prospective, randomized, single-blind, controlled study. Eur. J. Neurol. 27, 280–287 (2020).
Dudziec, M. M. et al. Home-based multi-sensory and proximal strengthening program to improve balance in Charcot-Marie-Tooth disease type 1A: a proof of concept study. Muscle Nerve 69, 354–361 (2024).
Prada, V. et al. Hand rehabilitation treatment for Charcot-Marie-Tooth disease: an open label pilot study. J. Neurol. Neurophysiol. 9, 465 (2018).
Rose, K. J., Raymond, J., Refshauge, K., North, K. N. & Burns, J. Serial night casting increases ankle dorsiflexion range in children and young adults with Charcot-Marie-Tooth disease: a randomised trial. J. Physiother. 56, 113–119 (2010).
Refshauge, K. M., Raymond, J., Nicholson, G. & van den Dolder, P. A. Night splinting does not increase ankle range of motion in people with Charcot-Marie-Tooth disease: a randomised, cross-over trial. Aust. J. Physiother. 52, 193–199 (2006).
Ramdharry, G. M., Pollard, A. J., Marsden, J. F. & Reilly, M. M. Comparing gait performance of people with Charcot-Marie-Tooth disease who do and do not wear ankle foot orthoses. Physiother. Res. Int. 17, 191–199 (2012).
Guillebastre, B., Calmels, P. & Rougier, P. R. Assessment of appropriate ankle-foot orthoses models for patients with Charcot-Marie-Tooth disease. Am. J. Phys. Med. Rehabil. 90, 619–627 (2011).
Phillips, M. F., Robertson, Z., Killen, B. & White, B. A pilot study of a crossover trial with randomized use of ankle-foot orthoses for people with Charcot-Marie-Tooth disease. Clin. Rehabil. 26, 534–544 (2012).
Ounpuu, S., Garibay, E., Acsadi, G., Brimacombe, M. & Pierz, K. The impact of orthoses on gait in children with Charcot-Marie-Tooth disease. Gait Posture 85, 198–204 (2021).
Kim, A., Frecklington, M., Philps, A. & Stewart, S. The effect of ankle-foot orthoses on gait characteristics in people with Charcot-Marie-Tooth disease: a systematic review and meta-analysis. J. Foot Ankle Res. 17, e70003 (2024).
Burns, J., Crosbie, J., Ouvrier, R. & Hunt, A. Effective orthotic therapy for the painful cavus foot: a randomized controlled trial. J. Am. Podiatr. Med. Assoc. 96, 205–211 (2006).
Vinci, P. & Gargiulo, P. Poor compliance with ankle-foot-orthoses in Charcot-Marie-Tooth disease. Eur. J. Phys. Rehabil. Med. 44, 27–31 (2008).
Zuccarino, R., Anderson, K. M., Shy, M. E. & Wilken, J. M. Satisfaction with ankle foot orthoses in individuals with Charcot-Marie-Tooth disease. Muscle Nerve 63, 40–45 (2021).
Scheffers, G., Hiller, C., Refshauge, K. & Burns, J. Prescription of foot and ankle orthoses for children with Charcot–Marie–Tooth disease: a review of the evidence. Phys. Ther. Rev. 17, 79–90 (2012).
Laura, M., Barnett, J., Benfield, J., Ramdharry, G. M. & Welck, M. J. Foot surgery for adults with Charcot-Marie-Tooth disease. Practical Neurol. 24, 275–284 (2024).
Videler, A., Eijffinger, E., Nollet, F. & Beelen, A. A thumb opposition splint to improve manual dexterity and upper-limb functioning in Charcot-Marie-Tooth disease. J. Rehabil. Med. 44, 249–253 (2012).
Reilly, M. M. et al. 221st ENMC International Workshop: Foot Surgery in Charcot-Marie-Tooth disease. 10-12 June 2016, Naarden, The Netherlands. Neuromuscul. Disord. 27, 1138–1142 (2017).
Pfeffer, G. B. et al. A Consensus Statement on the Surgical Treatment of Charcot-Marie-Tooth Disease. Foot Ankle Int. 41, 870–880 (2020).
Ramdharry, G. et al. A prospective study on surgical management of foot deformities in Charcot Marie Tooth disease. J. Peripher. Nerv. Syst. 26, 187–192 (2021).
Faldini, C. et al. Surgical treatment of cavus foot in Charcot-Marie-Tooth disease: a review of twenty-four cases: AAOS exhibit selection. J. Bone Jt Surg. Am. 97, e30 (2015).
Lin, T. et al. Surgical outcomes of cavovarus foot deformity in children with Charcot-Marie-Tooth disease. Neuromuscul. Disord. 29, 427–436 (2019).
Estilow, T., Kozin, S. H., Glanzman, A. M., Burns, J. & Finkel, R. S. Flexor digitorum superficialis opposition tendon transfer improves hand function in children with Charcot-Marie-Tooth disease: case series. Neuromuscul. Disord. 22, 1090–1095 (2012).
Wood, V. E., Huene, D. & Nguyen, J. Treatment of the upper limb in Charcot-Marie-Tooth disease. J. Hand Surg. Br. 20, 511–518 (1995).
Langensiepen, S. et al. Measuring procedures to determine the Cobb angle in idiopathic scoliosis: a systematic review. Eur. Spine J. 22, 2360–2371 (2013).
Tan, K. A. et al. Hip dysplasia in Charcot-Marie-Tooth disease: insights from a large cohort of children and adolescents. J. Peripher. Nerv. Syst. 30, e70002 (2025).
Katzberg, H. D., Khan, A. H. & So, Y. T. Assessment: symptomatic treatment for muscle cramps (an evidence-based review): report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 74, 691–696 (2010).
Blyton, F., Ryan, M. M., Ouvrier, R. A. & Burns, J. Muscle cramp in pediatric Charcot-Marie-Tooth disease type 1A: prevalence and predictors. Neurology 77, 2115–2118 (2011).
Johnson, N. E. et al. Prospective study of muscle cramps in Charcot-Marie-Tooth disease. Muscle Nerve 51, 485–488 (2015).
Bellofatto, M. et al. Frequency, entity and determinants of fatigue in Charcot-Marie-Tooth disease. Eur. J. Neurol. 30, 710–718 (2023).
Bellofatto, M. et al. Daytime sleepiness and sleep quality in Charcot-Marie-Tooth disease. J. Neurol. 270, 5561–5568 (2023).
Jagersma, E., Jeukens-Visser, M., van Paassen, B. W., Meester-Delver, A. & Nollet, F. Severe fatigue and reduced quality of life in children with hereditary motor and sensory neuropathy 1A. J. Child. Neurol. 28, 429–434 (2013).
Boentert, M. et al. Fatigue, reduced sleep quality and restless legs syndrome in Charcot-Marie-Tooth disease: a web-based survey. J. Neurol. 257, 646–652 (2010).
Boentert, M. et al. Sleep disorders in Charcot-Marie-Tooth disease type 1. J. Neurol. Neurosurg. Psychiatry 85, 319–325 (2014).
Price, R. et al. Oral and topical treatment of painful diabetic polyneuropathy: practice guideline update summary: report of the AAN guideline subcommittee. Neurology 98, 31–43 (2022).
Bates, D. et al. A comprehensive algorithm for management of neuropathic pain. Pain Med. 20, S2–S12 (2019).
Donlevy, G. A. et al. Association of body mass index with disease progression in children with Charcot-Marie-Tooth disease. Neurology 101, e717–e727 (2023).
Cavaletti, G., Forsey, K. & Alberti, P. Toxic medications in Charcot-Marie-Tooth patients: a systematic review. J. Peripher. Nerv. Syst. 28, 295–307 (2023).
Sheth, S. et al. Diabetes mellitus exacerbates motor and sensory impairment in CMT1A. J. Peripher. Nerv. Syst. 13, 299–304 (2008).
Radkowski, P. et al. A review of muscle relaxants in anesthesia in patients with neuromuscular disorders including Guillain-Barré syndrome, myasthenia gravis, Duchenne muscular dystrophy, Charcot-Marie-Tooth disease, and inflammatory myopathies. Med. Sci. Monit. 30, e945675 (2024).
De Grado, A., Serio, M., Saveri, P., Pisciotta, C. & Pareyson, D. Charcot-Marie-Tooth disease: a review of clinical developments and its management — what’s new in 2025? Expert Rev. Neurother. 25, 427–442 (2025).
Isbister, G. K., Burns, J., Prior, F. & Ouvrier, R. A. Safety of nitrous oxide administration in patients with Charcot-Marie-Tooth disease. J. Neurol. Sci. 268, 160–162 (2008).
Skorupinska, M., Ramdharry, G., Byrne, B., Laura, M. & Reilly, M. M. Pregnancy and delivery in patients with Charcot-Marie-Tooth disease and related disorders. Obstet. Med. 16, 83–87 (2023).
Rudnik-Schoneborn, S., Rohrig, D., Nicholson, G. & Zerres, K. Pregnancy and delivery in Charcot-Marie-Tooth disease type 1. Neurology 43, 2011–2016 (1993).
Pisciotta, C. et al. Pregnancy in Charcot-Marie-Tooth disease: data from the Italian CMT National Registry. Neurology 95, e3180–e3189 (2020).
Rudnik-Schoneborn, S. et al. Pregnancy outcome in Charcot-Marie-Tooth disease: results of the CMT-NET cohort study in Germany. Eur. J. Neurol. 27, 1390–1396 (2020).
Burns, J., Ryan, M. M. & Ouvrier, R. A. Quality of life in children with Charcot-Marie-Tooth disease. J. Child. Neurol. 25, 343–347 (2010).
Vinci, P. et al. Quality of life in patients with Charcot-Marie-Tooth disease. Neurology 65, 922–924 (2005).
Schorling, E. et al. Health-related quality of life and satisfaction with German health care services in patients with Charcot-Marie-Tooth neuropathy. J. Neuromuscul. Dis. 9, 211–220 (2022).
Padua, L. et al. Variables influencing quality of life and disability in Charcot Marie Tooth (CMT) patients: Italian multicentre study. Neurol. Sci. 27, 417–423 (2006).
Redmond, A. C., Burns, J. & Ouvrier, R. A. Factors that influence health-related quality of life in Australian adults with Charcot-Marie-Tooth disease. Neuromuscul. Disord. 18, 619–625 (2008).
Calvert, M. et al. Health-related quality of life and supportive care in patients with rare long-term neurological conditions. Qual. Life Res. 22, 1231–1238 (2013).
Pfeiffer, G., Wicklein, E. M., Ratusinski, T., Schmitt, L. & Kunze, K. Disability and quality of life in Charcot-Marie-Tooth disease type 1. J. Neurol. Neurosurg. Psychiatry 70, 548–550 (2001).
Dai, S. et al. A cross-sectional survey on the health status of patients with Charcot-Marie-Tooth disease in a Chinese national patient group. J. Neurol. 272, 322 (2025).
Johnson, N. E. et al. Quality-of-life in Charcot Marie Tooth disease: the patient’s perspective. Neuromuscul. Disord. 24, 1018–1023 (2014).
Rehbein, T. et al. Patient-reported disease burden in the accelerate clinical trials in Charcot-Marie-Tooth disease study. J. Peripher. Nerv. Syst. 29, 487–493 (2024).
Thomas, F. P. et al. Patient-reported symptom burden of Charcot-Marie-Tooth disease type 1A: findings from an observational digital lifestyle study. J. Clin. Neuromuscul. Dis. 24, 7–17 (2022).
Johnson, N. E. et al. The Charcot-Marie-Tooth health index: evaluation of a patient-reported outcome. Ann. Neurol. 84, 225–233 (2018).
Bellofatto, M. et al. Anxiety and depression in Charcot-Marie-Tooth disease: data from the Italian CMT National Registry. J. Neurol. 270, 394–401 (2023).
Ivanovic, V. et al. Physical and mental aspects of quality of life in patients with Charcot-Marie-Tooth disease type 1A. Front. Neurol. 13, 852150 (2022).
Bjelica, B. et al. Employment status of patients with Charcot-Marie-Tooth type 1A. Acta Neurol. Belg. 122, 641–646 (2022).
Rule, P. D. & Hill, P. L. Psychosocial factors and well-being among adults with Charcot-Marie-Tooth disease: a cross-sectional study. Rehabil. Psychol. 68, 431–442 (2023).
Reilly, M. M. et al. Trials for slowly progressive neurogenetic diseases need surrogate endpoints. Ann. Neurol. 93, 906–910 (2023).
Cornett, K. M. et al. Natural history of Charcot-Marie-Tooth disease during childhood. Ann. Neurol. 82, 353–359 (2017). This study enumerates the 2-year rate of disease progression in children with CMT assessed by the CMT Pediatric Scale (CMTPedS), a reliable Rasch-built linearly weighted disability scale evaluating fine and gross motor function, strength, sensation and balance.
Anens, E., Emtner, M. & Hellstrom, K. Exploratory study of physical activity in persons with Charcot-Marie-Tooth disease. Arch. Phys. Med. Rehabil. 96, 260–268 (2015).
Radhakrishnan, K., El-Mangoush, M. A. & Gerryo, S. E. Descriptive epidemiology of selected neuromuscular disorders in Benghazi, Libya. Acta Neurol. Scand. 75, 95–100 (1987).
Mladenovic, J. et al. Epidemiology of Charcot-Marie-Tooth disease in the population of Belgrade, Serbia. Neuroepidemiology 36, 177–182 (2011).
Lousa, M. et al. Genetic epidemiology, demographic, and clinical characteristics of Charcot-Marie-Tooth disease in the island of Gran Canaria (Spain). J. Peripher. Nerv. Syst. 24, 131–138 (2019).
Combarros, O., Calleja, J., Polo, J. M. & Berciano, J. Prevalence of hereditary motor and sensory neuropathy in Cantabria. Acta Neurol. Scand. 75, 9–12 (1987).
Holmberg, B. H. Charcot-Marie-Tooth disease in northern Sweden: an epidemiological and clinical study. Acta Neurol. Scand. 87, 416–422 (1993).
Morocutti, C. et al. Charcot-Marie-Tooth disease in Molise, a central-southern region of Italy: an epidemiological study. Neuroepidemiology 21, 241–245 (2002).
Nicolaou, P. et al. Charcot-Marie-Tooth disease in Cyprus: epidemiological, clinical and genetic characteristics. Neuroepidemiology 35, 171–177 (2010).
Gumundsson, B., Ólafsson, E., Jakobsson, F. & Lúvígsson, P. Prevalence of symptomatic Charcot-Marie-Tooth disease in Iceland: a study of a well-defined population. Neuroepidemiology 34, 13–17 (2010).
Lefter, S., Hardiman, O. & Ryan, A. M. A population-based epidemiologic study of adult neuromuscular disease in the Republic of Ireland. Neurology 88, 304–313 (2017).
Kurihara, S. et al. An epidemiological genetic study of Charcot-Marie-Tooth disease in Western Japan. Neuroepidemiology 21, 246–250 (2002).
Libberecht, K. et al. The influence of lysosomal stress on dental pulp stem cell-derived Schwann cells. Biomolecules https://doi.org/10.3390/biom14040405 (2024).
Pisciotta, A. et al. Neural crest derived stem cells from dental pulp and tooth-associated stem cells for peripheral nerve regeneration. Neural Regen. Res. 15, 373–381 (2020).
Dobner, J., Diecke, S., Krutmann, J., Prigione, A. & Rossi, A. Reassessment of marker genes in human induced pluripotent stem cells for enhanced quality control. Nat. Commun. 15, 8547 (2024).
Sullivan, S. et al. Quality control guidelines for clinical-grade human induced pluripotent stem cell lines. Regen. Med. 13, 859–866 (2018).
Ehrhardt, M. J. et al. Improving quality and quantity of life for childhood cancer survivors globally in the twenty-first century. Nat. Rev. Clin. Oncol. 20, 678–696 (2023).
Acknowledgements
V.T. discloses support for the research for this work from the European Union via the EU4Health Programme (EUCMTSC, no. 101232916). Views and opinions expressed are, however, those of the author(s) only and do not necessarily reflect those of the European Union or HADEA. Neither the European Union nor the granting authority can be held responsible for them. J.B. discloses support for the research for this work from The Charcot-Marie-Tooth Association (Inherited Neuropathy Consortium, SR-202601) and Muscular Dystrophy Association (CERTIFYCMT, 1060929).
Author information
Authors and Affiliations
Contributions
Introduction (S.S.S. and J.B.); Epidemiology (B.M.-C., V.T. and S.S.S.); Mechanisms/pathophysiology (V.T., M.D’A., J.D.W. and S.S.S.); Diagnosis, screening and prevention (B.M.-C., J.D.W., M.L. and S.S.S.); Management (E.M.Y. and M.L.); Quality of life (E.M.Y. and M.L.); Outlook (J.B. and S.S.S.); overview of Primer (J.B.).
Corresponding author
Ethics declarations
Competing interests
J.B., V.T., M.L., E.M.Y., M.D’A., B.M.-C., J.D.W. and S.S.S. are principal and/or co-investigators for clinical studies of CMT and related neuropathies. J.B., B.M.-C. and S.S.S. have consulted for Applied Therapeutics. J.B. has consulted for Alesta Therapeutics and NMD Pharma. V.T. provides occasional service to the pharmaceutical industry and CROs to validate therapeutic compounds in iPSC-derived 2D and 3D cell model systems. M.D’A. has consulted for InFlectis Bioscience. S.S.S. has consulted for DTx Therapeutics, Novartis, Passage Bio, Pfizer and Toray Industries.
Peer review
Peer review information
Nature Reviews Disease Primers thanks A. Schenone, T. Sevilla, H. Takashima and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Burns, J., Timmerman, V., Laurá, M. et al. Charcot–Marie–Tooth disease and related neuropathies. Nat Rev Dis Primers 12, 3 (2026). https://doi.org/10.1038/s41572-025-00679-2
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41572-025-00679-2