Abstract
The lymphatic vasculature is recognized for its roles in immunity, lipid transport and fluid homeostasis, but has been ignored, until recently, for its involvement in adipose tissue metabolism, obesity and associated comorbidities. States of overnutrition, such as in obesity, are associated with impairment of lymphatic function, leading to localized lymphoedema, adipogenesis and insulin resistance. Conversely, compromised lymphatic vasculature integrity can induce adiposity and accelerate insulin resistance. Through the use of advanced ‘omics’ and bioinformatic technologies coupled with functional experiments in cells, mice and humans, we now know that the lymphatic system is more than just a transport conduit and is intimately involved in tissue and organ homeostasis, including in adipose tissue. In this Review, we summarize the interconnected causes of obesity and lymphatic dysfunction with a particular focus on delineating the underappreciated yet fundamental crosstalk between the lymphatic network and white and brown adipose tissues. We also synthesize information on lymph-directed therapeutic strategies that have the potential to transform outcomes in obesity.
Key points
-
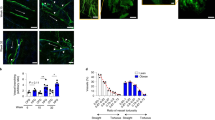
The extent of lymphatic vascularization is different between brown and white adipose tissue and depots.
-
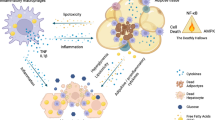
Obesity-remodelled adipose tissue secretes factors that induce lymphatic dysfunction.
-
Lymphatic dysfunction initiates and accelerates adiposity, inflammation and systemic insulin resistance.
-
Restoring lymphatic function supports the resolution of obesity and its associated comorbidities.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Liu, J. et al. Impact of abdominal visceral and subcutaneous adipose tissue on cardiometabolic risk factors: the Jackson Heart Study. J. Clin. Endocrinol. Metab. 95, 5419–5426 (2010).
Trevaskis, N. L., Kaminskas, L. M. & Porter, C. J. From sewer to saviour — targeting the lymphatic system to promote drug exposure and activity. Nat. Rev. Drug. Discov. 14, 781–803 (2015).
Miller, N. E. et al. Secretion of adipokines by human adipose tissue in vivo: partitioning between capillary and lymphatic transport. Am. J. Physiol. Endocrinol. Metab. 301, E659–E667 (2011).
Escobedo, N. et al. Restoration of lymphatic function rescues obesity in Prox1-haploinsufficient mice. JCI Insight 1, e85096 (2016).
Cao, E. et al. Mesenteric lymphatic dysfunction promotes insulin resistance and represents a potential treatment target in obesity. Nat. Metab. 3, 1175–1188 (2021).
Bénézech, C. et al. Inflammation-induced formation of fat-associated lymphoid clusters. Nat. Immunol. 16, 819–828 (2015).
Baluk, P. et al. Functionally specialized junctions between endothelial cells of lymphatic vessels. J. Exp. Med. 204, 2349–2362 (2007).
Schoofs, H. et al. Dynamic cytoskeletal regulation of cell shape supports resilience of lymphatic endothelium. Nature 641, 465–475 (2025).
Triacca, V., Güç, E., Kilarski, W. W., Pisano, M. & Swartz, M. A. Transcellular pathways in lymphatic endothelial cells regulate changes in solute transport by fluid stress. Circ. Res. 120, 1440–1452 (2017).
Lim, H. Y. et al. Lymphatic vessels are essential for the removal of cholesterol from peripheral tissues by SR-BI-mediated transport of HDL. Cell Metab. 17, 671–684 (2013).
Leak, L. V. & Burke, J. F. Ultrastructural studies on the lymphatic anchoring filaments. J. Cell Biol. 36, 129–149 (1968).
Engeset, A., Olszewski, W., Jaeger, P. M., Sokolowski, J. & Theodorsen, L. Twenty-four hour variation in flow and composition of leg lymph in normal men. Acta Physiol. Scand. 99, 140–148 (1977).
Zawieja, S. D. et al. Cellular characterization of the mouse collecting lymphatic vessels reveals that lymphatic muscle cells are the innate pacemaker cells. eLife 12, RP90679 (2025).
Pond, C. M. & Mattacks, C. A. Interactions between adipose tissue around lymph nodes and lymphoid cells in vitro. J. Lipid Res. 36, 2219–2231 (1996).
Pond, C. M. & Mattacks, C. A. In vivo evidence for the involvement of the adipose tissue surrounding lymph nodes in immune responses. Immunol. Lett. 63, 159–167 (1998).
Pond, C. M. & Mattacks, C. A. The source of fatty acids incorporated into proliferating lymphoid cells in immune-stimulated lymph nodes. Br. J. Nutr. 89, 375–383 (2003).
Durot, S. et al. Multi-omics analysis reveals metabolic diversity underlying endothelial cell functions. Life Sci. Alliance 9, e202503526 (2026).
Wong, B. W. et al. The role of fatty acid β-oxidation in lymphangiogenesis. Nature 542, 49–54 (2017).
Meçe, O. et al. Lipid droplet degradation by autophagy connects mitochondria metabolism to Prox1-driven expression of lymphatic genes and lymphangiogenesis. Nat. Commun. 13, 2760 (2022).
García-Caballero, M. et al. Role and therapeutic potential of dietary ketone bodies in lymph vessel growth. Nat. Metab. 1, 666–675 (2019).
Hawighorst, T. et al. Thrombospondin-1 selectively inhibits early-stage carcinogenesis and angiogenesis but not tumor lymphangiogenesis and lymphatic metastasis in transgenic mice. Oncogene 21, 7945–7956 (2002).
Cifarelli, V. et al. Visceral obesity and insulin resistance associate with CD36 deletion in lymphatic endothelial cells. Nat. Commun. 12, 3350 (2021).
Massier, L. et al. An integrated single cell and spatial transcriptomic map of human white adipose tissue. Nat. Commun. 14, 1438 (2023).
Emont, M. P. et al. A single-cell atlas of human and mouse white adipose tissue. Nature 603, 926–933 (2022).
Hildreth, A. D. et al. Single-cell sequencing of human white adipose tissue identifies new cell states in health and obesity. Nat. Immunol. 22, 639–653 (2021).
Westcott, G. P. et al. Single-nuclear transcriptomics of lymphedema-associated adipose reveals a pro-lymphangiogenic stromal cell population. Prepint at bioRxiv https://doi.org/10.1101/2025.02.18.638907 (2025).
Miranda, A. M. A. et al. Selective remodelling of the adipose niche in obesity and weight loss. Nature 644, 769–779 (2025).
Lee, M. J., Wu, Y. & Fried, S. K. Adipose tissue heterogeneity: implication of depot differences in adipose tissue for obesity complications. Mol. Asp. Med. 34, 1–11 (2013).
Steinberg, G. R., Valvano, C. M., De Nardo, W. & Watt, M. J. Integrative metabolism in MASLD and MASH: pathophysiology and emerging mechanisms. J. Hepatol. 83, 584–595 (2025).
Bondareva, O. et al. Single-cell profiling of vascular endothelial cells reveals progressive organ-specific vulnerabilities during obesity. Nat. Metab. 4, 1591–1610 (2022).
Redondo, P. A. G. et al. Lymphatic vessels in human adipose tissue. Cell Tissue Res. 379, 511–520 (2020).
Loft, A. et al. Towards a consensus atlas of human and mouse adipose tissue at single-cell resolution. Nat. Metab. 7, 875–894 (2025).
Vijay, J. et al. Single-cell analysis of human adipose tissue identifies depot- and disease-specific cell types. Nat. Metab. 2, 97–109 (2020).
Arngrim, N., Simonsen, L., Holst, J. J. & Bülow, J. Reduced adipose tissue lymphatic drainage of macromolecules in obese subjects: a possible link between obesity and local tissue inflammation? Int. J. Obes. 37, 748–750 (2013).
Savetsky, I. L. et al. Lymphatic function regulates contact hypersensitivity dermatitis in obesity. J. Invest. Dermatol. 135, 2742–2752 (2015).
Weitman, E. S. et al. Obesity impairs lymphatic fluid transport and dendritic cell migration to lymph nodes. PLoS ONE 8, e70703 (2013).
García Nores, G. D. et al. Obesity but not high-fat diet impairs lymphatic function. Int. J. Obes. 40, 1582–1590 (2016).
Hespe, G. E. et al. Exercise training improves obesity-related lymphatic dysfunction. J. Physiol. 594, 4267–4282 (2016).
Nitti, M. D. et al. Obesity-induced lymphatic dysfunction is reversible with weight loss. J. Physiol. 594, 7073–7087 (2016).
Savetsky, I. L. et al. Obesity increases inflammation and impairs lymphatic function in a mouse model of lymphedema. Am. J. Physiol. Heart Circ. Physiol 307, H165–H172 (2014).
Blum, K. S. et al. Chronic high-fat diet impairs collecting lymphatic vessel function in mice. PLoS ONE 9, e94713 (2014).
Lim, H. Y. et al. Hypercholesterolemic mice exhibit lymphatic vessel dysfunction and degeneration. Am. J. Pathol. 175, 1328–1337 (2009).
Zawieja, S. D. et al. Impairments in the intrinsic contractility of mesenteric collecting lymphatics in a rat model of metabolic syndrome. Am. J. Physiol. Heart Circ. Physiol 302, H643–H653 (2012).
Torrisi, J. S. et al. Inhibition of inflammation and iNOS improves lymphatic function in obesity. Sci. Rep. 6, 19817 (2016).
Davis, M. J. et al. Multiple aspects of lymphatic dysfunction in an ApoE−/− mouse model of hypercholesterolemia. Front. Physiol. 13, 1098408 (2022).
Creff, J. et al. Apelin-VEGF-C mRNA delivery as therapeutic for the treatment of secondary lymphedema. EMBO Mol. Med. 16, 386–415 (2024).
Hendrickx, A. A., Damstra, R. J., Krijnen, W. P. & van der Schans, C. P. Improvement of limb volumes after bariatric surgery in nine end-stage primary, secondary, and obesity-induced lymphedema patients: a multiple case report. Lymphat. Res. Biol. 20, 64–70 (2022).
Greene, A. K., Grant, F. D. & Maclellan, R. A. Obesity-induced lymphedema nonreversible following massive weight loss. Plast. Reconstr. Surg. Glob. Open. 3, e426 (2015).
Hosono, K. et al. Deletion of RAMP1 signaling enhances diet-induced obesity and fat absorption via intestinal lacteals in mice. In Vivo 38, 160–173 (2024).
Rehal, S. et al. Regulation of lymphatic function and injury by nitrosative stress in obese mice. Mol. Metab. 42, 101081 (2020).
Castorena-Gonzalez, J. A. Lymphatic valve dysfunction in Western diet-fed mice: new insights into obesity-induced lymphedema. Front. Pharmacol. 13, 823266 (2022).
Kuan, E. L. et al. Collecting lymphatic vessel permeability facilitates adipose tissue inflammation and distribution of antigen to lymph node-homing adipose tissue dendritic cells. J. Immunol. 194, 5200–5210 (2015).
Mikrani, R. et al. Obesity-associated mesenteric lymph leakage impairs the trafficking of lipids, lipophilic drugs and antigens from the intestine to mesenteric lymph nodes. Eur. J. Pharm. Biopharm. 180, 319–331 (2022).
Scallan, J. P., Hill, M. A. & Davis, M. J. Lymphatic vascular integrity is disrupted in type 2 diabetes due to impaired nitric oxide signalling. Cardiovasc. Res. 107, 89–97 (2015).
Vadiveloo, M., Scott, M., Quatromoni, P., Jacques, P. & Parekh, N. Trends in dietary fat and high-fat food intakes from 1991 to 2008 in the Framingham Heart Study participants. Br. J. Nutr. 111, 724–734 (2014).
Adolph, T. E. & Tilg, H. Western diets and chronic diseases. Nat. Med. 30, 2133–2147 (2024).
Hagberg, C. E. & Spalding, K. L. White adipocyte dysfunction and obesity-associated pathologies in humans. Nat. Rev. Mol. Cell. Biol. 25, 270–289 (2024).
Mittendorfer, B., Magkos, F., Fabbrini, E., Mohammed, B. S. & Klein, S. Relationship between body fat mass and free fatty acid kinetics in men and women. Obesity 17, 1872–1877 (2009).
Fedewa, M. V., Hathaway, E. D., Ward-Ritacco, C. L., Williams, T. D. & Dobbs, W. C. The effect of chronic exercise training on leptin: a systematic review and meta-analysis of randomized controlled trials. Sports Med. 48, 1437–1450 (2018).
Becic, T., Studenik, C. & Hoffmann, G. Exercise increases adiponectin and reduces leptin levels in prediabetic and diabetic individuals: systematic review and meta-analysis of randomized controlled trials. Med. Sci. 6, 97 (2018).
Skurk, T., Alberti-Huber, C., Herder, C. & Hauner, H. Relationship between adipocyte size and adipokine expression and secretion. J. Clin. Endocrinol. Metab. 92, 1023–1033 (2007).
Hotamisligil, G. S., Shargill, N. S. & Spiegelman, B. M. Adipose expression of tumor necrosis factor-α: direct role in obesity-linked insulin resistance. Science 259, 87–91 (1993).
Brotman, S. M. et al. Cell-type composition affects adipose gene expression associations with cardiometabolic traits. Diabetes 72, 1707–1718 (2023).
Fain, J. N. Release of inflammatory mediators by human adipose tissue is enhanced in obesity and primarily by the nonfat cells: a review. Mediators Inflamm. 2010, 513948 (2010).
Nanaware, P. P. et al. Role of the afferent lymph as an immunological conduit to analyze tissue antigenic and inflammatory load. Cell Rep. 43, 114311 (2024).
Simons, M., Gordon, E. & Claesson-Welsh, L. Mechanisms and regulation of endothelial VEGF receptor signalling. Nat. Rev. Mol. Cell. Biol. 17, 611–625 (2016).
Dupont, L. et al. ADAMTS2 and ADAMTS14 can substitute for ADAMTS3 in adults for pro-VEGFC activation and lymphatic homeostasis. JCI Insight 7, e151509 (2022).
Stacker, S. A. & Achen, M. G. Emerging roles for VEGF-D in human disease. Biomolecules 8, 1 (2018).
Zafar, M. I. et al. Association between the expression of vascular endothelial growth factors and metabolic syndrome or its components: a systematic review and meta-analysis. Diabetol. Metab. Syndr. 10, 62 (2018).
Kentistou, K. A. et al. Large scale phenotype imputation and in vivo functional validation implicate ADAMTS14 as an adiposity gene. Nat. Commun. 14, 307 (2023).
Karaman, S. et al. Blockade of VEGF-C and VEGF-D modulates adipose tissue inflammation and improves metabolic parameters under high-fat diet. Mol. Metab. 4, 93–105 (2015).
Karaman, S. et al. Transgenic overexpression of VEGF-C induces weight gain and insulin resistance in mice. Sci. Rep. 6, 31566 (2016).
Nitschké, M. et al. Retrograde lymph flow leads to chylothorax in transgenic mice with lymphatic malformations. Am. J. Pathol. 187, 1984–1997 (2017).
Chakraborty, A. et al. Vascular endothelial growth factor-D (VEGF-D) overexpression and lymphatic expansion in murine adipose tissue improves metabolism in obesity. Am. J. Pathol. 189, 924–939 (2019).
Chakraborty, A., Scogin, C. K., Rizwan, K., Morley, T. S. & Rutkowski, J. M. Characterizing lymphangiogenesis and concurrent inflammation in adipose tissue in response to VEGF-D. Front. Physiol. 11, 363 (2020).
Bohlen, H. G., Wang, W., Gashev, A., Gasheva, O. & Zawieja, D. Phasic contractions of rat mesenteric lymphatics increase basal and phasic nitric oxide generation in vivo. Am. J. Physiol. Heart Circ. Physiol 297, H1319–H1328 (2009).
Shirasawa, Y., Ikomi, F. & Ohhashi, T. Physiological roles of endogenous nitric oxide in lymphatic pump activity of rat mesentery in vivo. Am. J. Physiol. Gastrointest. Liver Physiol. 278, G551–G556 (2000).
Scallan, J. P. & Davis, M. J. Genetic removal of basal nitric oxide enhances contractile activity in isolated murine collecting lymphatic vessels. J. Physiol. 591, 2139–2156 (2013).
Elkins, C. et al. Obesity reshapes regulatory T cells in the visceral adipose tissue by disrupting cellular cholesterol homeostasis. Sci. Immunol. 10, eadl4909 (2025).
Gousopoulos, E. et al. Regulatory T cell transfer ameliorates lymphedema and promotes lymphatic vessel function. JCI Insight 1, e89081 (2016).
Nishimura, S. et al. Adipose natural regulatory B cells negatively control adipose tissue inflammation. Cell Metab. 18, 759–766 (2013).
Hos, D. et al. IL-10 indirectly regulates corneal lymphangiogenesis and resolution of inflammation via macrophages. Am. J. Pathol. 186, 159–171 (2016).
Börgeson, E. et al. Lipoxin A4 attenuates adipose inflammation. FASEB J. 26, 4287–4294 (2012).
Cromer, W. E. et al. The effects of inflammatory cytokines on lymphatic endothelial barrier function. Angiogenesis 17, 395–406 (2014).
Chaitanya, G. V. et al. Differential cytokine responses in human and mouse lymphatic endothelial cells to cytokines in vitro. Lymphat. Res. Biol. 8, 155–164 (2010).
Lei, P.-J. et al. Aging-induced changes in lymphatic muscle cell transcriptomes are associated with reduced pumping of peripheral collecting lymphatic vessels in mice. Dev. Cell 60, 1118–1133.e5 (2025).
Chen, Y. et al. The pro-inflammatory cytokine TNF-α inhibits lymphatic pumping via activation of the NF-κB-iNOS signaling pathway. Microcirculation 24, e12364 (2017).
Aldrich, M. B. & Sevick-Muraca, E. M. Cytokines are systemic effectors of lymphatic function in acute inflammation. Cytokine 64, 362–369 (2013).
Oka, M. et al. Inhibition of endogenous TGF-β signaling enhances lymphangiogenesis. Blood 111, 4571–4579 (2008).
Boucher, J. R. M. et al. Apelin, a newly identified adipokine up-regulated by insulin and obesity. Endocrinology 146, 1764–1771 (2005).
Hwangbo, C. et al. Endothelial APLNR regulates tissue fatty acid uptake and is essential for apelin’s glucose-lowering effects. Sci. Transl. Med. 9, eaad4000 (2017).
Sawane, M. et al. Apelin inhibits diet-induced obesity by enhancing lymphatic and blood vessel integrity. Diabetes 62, 1970–1980 (2013).
Cavallo, M. G. et al. Altered glucose homeostasis is associated with increased serum apelin levels in type 2 diabetes mellitus. PLoS ONE 7, e51236 (2012).
Tabata, M. et al. Angiopoietin-like protein 2 promotes chronic adipose tissue inflammation and obesity-related systemic insulin resistance. Cell Metab. 10, 178–188 (2009).
Sasaki, Y. et al. Angiopoietin like protein 2 (ANGPTL2) promotes adipose tissue macrophage and T lymphocyte accumulation and leads to insulin resistance. PLoS ONE 10, e0131176 (2015).
Toyono, T. et al. Angiopoietin-like protein 2 is a potent hemangiogenic and lymphangiogenic factor in corneal inflammation. Invest. Ophthalmol. Vis. Sci. 54, 4278–4285 (2013).
Dietrich, T. et al. Inhibition of inflammatory lymphangiogenesis by integrin α5 blockade. Am. J. Pathol. 171, 361–372 (2007).
Mandard, S. et al. The fasting-induced adipose factor/angiopoietin-like protein 4 is physically associated with lipoproteins and governs plasma lipid levels and adiposity. J. Biol. Chem. 281, 934–944 (2006).
Robciuc, M. R. et al. Serum angiopoietin-like 4 protein levels and expression in adipose tissue are inversely correlated with obesity in monozygotic twins. J. Lipid Res. 52, 1575–1582 (2011).
Janssen, A. W. F. et al. Loss of angiopoietin-like 4 (ANGPTL4) in mice with diet-induced obesity uncouples visceral obesity from glucose intolerance partly via the gut microbiota. Diabetologia 61, 1447–1458 (2018).
Lichtenstein, L. et al. Angptl4 protects against severe proinflammatory effects of saturated fat by inhibiting fatty acid uptake into mesenteric lymph node macrophages. Cell Metab. 12, 580–592 (2010).
Mah, M. S. et al. High-fat feeding drives the intestinal production and assembly of C16:0 ceramides in chylomicrons. Sci. Adv. 10, eadp2254 (2024).
Baek, J. H., Kim, D. H., Lee, J., Kim, S. J. & Chun, K. H. Galectin-1 accelerates high-fat diet-induced obesity by activation of peroxisome proliferator-activated receptor gamma (PPARγ) in mice. Cell Death Dis. 12, 66 (2021).
Fryk, E. et al. Metabolic profiling of galectin-1 and galectin-3: a cross-sectional, multi-omics, association study. Int. J. Obes. 48, 1180–1189 (2024).
Williams, S. P. et al. Genome-wide functional analysis reveals central signaling regulators of lymphatic endothelial cell migration and remodeling. Sci. Signal. 10, eaal2987 (2017).
Sato, A. et al. Novel mechanisms of compromised lymphatic endothelial cell homeostasis in obesity: the role of leptin in lymphatic endothelial cell tube formation and proliferation. PLoS ONE 11, e0158408 (2016).
Yamauchi, T. et al. The fat-derived hormone adiponectin reverses insulin resistance associated with both lipoatrophy and obesity. Nat. Med. 7, 941–946 (2001).
Shimizu, Y. et al. Adiponectin-mediated modulation of lymphatic vessel formation and lymphedema. J. Am. Heart Assoc. 2, e000438 (2013).
Tian, W. et al. Leukotriene B4 antagonism ameliorates experimental lymphedema. Sci. Transl. Med. 9, eaal3920 (2017).
Nandi, P. et al. PGE2 promotes breast cancer-associated lymphangiogenesis by activation of EP4 receptor on lymphatic endothelial cells. BMC Cancer 17, 11 (2017).
Li, P. et al. LTB4 promotes insulin resistance in obese mice by acting on macrophages, hepatocytes and myocytes. Nat. Med. 21, 239–247 (2015).
Spite, M. et al. Deficiency of the leukotriene B4 receptor, BLT-1, protects against systemic insulin resistance in diet-induced obesity. J. Immunol. 187, 1942–1949 (2011).
Lin, C. I. et al. Lysophosphatidic acid upregulates vascular endothelial growth factor-C and tube formation in human endothelial cells through LPA1/3, COX-2, and NF-κB activation- and EGFR transactivation-dependent mechanisms. Cell. Signal. 20, 1804–1814 (2008).
Lin, C. I. et al. Lysophosphatidic acid up-regulates vascular endothelial growth factor-C and lymphatic marker expressions in human endothelial cells. Cell Mol. Life Sci. 65, 2740–2751 (2008).
Mu, H. et al. Lysophosphatidic acid induces lymphangiogenesis and IL-8 production in vitro in human lymphatic endothelial cells. Am. J. Pathol. 180, 2170–2181 (2012).
Hisano, Y. et al. Lysolipid receptor cross-talk regulates lymphatic endothelial junctions in lymph nodes. J. Exp. Med. 216, 1582–1598 (2019).
Blomstrand, R. & Dahlback, O. L. The fatty acid composition of human thoracic duct lymph lipids. J. Clin. Invest. 39, 1185–1191 (1960).
Tsuchiya, K. et al. Chronic blockade of nitric oxide synthesis reduces adiposity and improves insulin resistance in high fat-induced obese mice. Endocrinology 148, 4548–4556 (2007).
Tokarz, V. L., Pereira, R. V. S., Jaldin-Fincati, J. R., Mylvaganam, S. & Klip, A. Junctional integrity and directional mobility of lymphatic endothelial cell monolayers are disrupted by saturated fatty acids. Mol. Biol. Cell 34, ar28 (2023).
Boucher, J., Kleinridders, A. & Kahn, C. R. Insulin receptor signaling in normal and insulin-resistant states. Cold Spring Harb. Perspect. Biol. 6, a009191 (2014).
Jaldin-Fincati, J. R., Pereira, R. V., Bilan, P. J. & Klip, A. Insulin uptake and action in microvascular endothelial cells of lymphatic and blood origin. Am. J. Physiol. Endocrinol. Metab. 315, E204–E217 (2018).
Gonzalez-Nieves, S. et al. Insulin regulates lymphatic endothelial integrity via palmitoylation. J. Lipid Res. 66, 100775 (2025).
Lee, Y., Chakraborty, S., Meininger, C. J. & Muthuchamy, M. Insulin resistance disrupts cell integrity, mitochondrial function, and inflammatory signaling in lymphatic endothelium. Microcirculation 25, e12492 (2018).
Montgomery, M. K., De Nardo, W. & Watt, M. J. Impact of lipotoxicity on tissue “cross talk” and metabolic regulation. Physiology 34, 134–149 (2019).
Turpin, S. M. et al. Obesity-induced CerS6-dependent C16:0 ceramide production promotes weight gain and glucose intolerance. Cell Metab. 20, 678–686 (2014).
Blachnio-Zabielska, A. U., Koutsari, C., Tchkonia, T. & Jensen, M. D. Sphingolipid content of human adipose tissue: relationship to adiponectin and insulin resistance. Obesity 20, 2341–2347 (2012).
Lee, Y., Fluckey, J. D., Chakraborty, S. & Muthuchamy, M. Hyperglycemia- and hyperinsulinemia-induced insulin resistance causes alterations in cellular bioenergetics and activation of inflammatory signaling in lymphatic muscle. FASEB J. 31, 2744–2759 (2017).
Castorena-Gonzalez, J. A., Kim, H. J. & Davis, M. J. Chronic metabolic stress impairs lymphatic contractility via activation of KATP channels in a mouse model of type-2 diabetes. Front. Physiol. 16, 1558763 (2025).
Harvey, N. L. et al. Lymphatic vascular defects promoted by Prox1 haploinsufficiency cause adult-onset obesity. Nat. Genet. 37, 1072–1081 (2005).
Brouillard, P. et al. Primary lymphoedema. Nat. Rev. Dis. Primers 7, 77 (2021).
Greene, A. K., Zurakowski, D. & Goss, J. A. Body mass index and lymphedema morbidity: comparison of obese versus normal-weight patients. Plast. Reconstr. Surg. 146, 402–407 (2020).
Greene, A. K., Grant, F. D. & Slavin, S. A. Lower-extremity lymphedema and elevated body-mass index. N. Engl. J. Med. 366, 2136–2137 (2012).
Chopra, K. et al. Massive localized lymphedema revisited: a quickly rising complication of the obesity epidemic. Ann. Plast. Surg. 74, 126–132 (2015).
Brorson, H., Ohlin, K., Olsson, G. & Karlsson, M. K. Breast cancer-related chronic arm lymphedema is associated with excess adipose and muscle tissue. Lymphat. Res. Biol. 7, 3–10 (2009).
Tavakkolizadeh, A., Wolfe, K. Q. & Kangesu, L. Cutaneous lymphatic malformation with secondary fat hypertrophy. Br. J. Plast. Surg. 54, 367–369 (2001).
Fang, J. et al. Mutations in FOXC2 (MFH-1), a forkhead family transcription factor, are responsible for the hereditary lymphedema-distichiasis syndrome. Am. J. Hum. Genet. 67, 1382–1388 (2000).
Petrova, T. V. et al. Defective valves and abnormal mural cell recruitment underlie lymphatic vascular failure in lymphedema distichiasis. Nat. Med. 10, 974–981 (2004).
Kovacs, P., Lehn-Stefan, A., Stumvoll, M., Bogardus, C. & Baier, L. J. Genetic variation in the human winged helix/forkhead transcription factor gene FOXC2 in Pima Indians. Diabetes 52, 1292–1295 (2003).
Carlsson, E., Groop, L. & Ridderstråle, M. Role of the FOXC2-512C>T polymorphism in type 2 diabetes: possible association with the dysmetabolic syndrome. Int. J. Obes. 29, 268–274 (2005).
Kim, J. K. et al. Adipocyte-specific overexpression of FOXC2 prevents diet-induced increases in intramuscular fatty acyl CoA and insulin resistance. Diabetes 54, 1657–1663 (2005).
Cederberg, A. et al. FOXC2 is a winged helix gene that counteracts obesity, hypertriglyceridemia, and diet-induced insulin resistance. Cell 106, 563–573 (2001).
Koc, M. et al. Lymphedema alters lipolytic, lipogenic, immune and angiogenic properties of adipose tissue: a hypothesis-generating study in breast cancer survivors. Sci. Rep. 11, 8171 (2021).
Zampell, J. C. et al. CD4+ cells regulate fibrosis and lymphangiogenesis in response to lymphatic fluid stasis. PLoS ONE 7, e49940 (2012).
Zou, J. et al. CD4+ T cells memorize obesity and promote weight regain. Cell. Mol. Immunol. 15, 630–639 (2018).
Mauro, C. et al. Obesity-induced metabolic stress leads to biased effector memory CD4+ T cell differentiation via PI3K p110δ-Akt-mediated signals. Cell Metab. 25, 593–609 (2017).
Gasheva, O. Y. et al. Prolonged intake of desloratadine: mesenteric lymphatic vessel dysfunction and development of obesity/metabolic syndrome. Am. J. Physiol. Gastrointest. Liver Physiol 316, G217–G227 (2019).
Rancoule, C. et al. Pro-fibrotic activity of lysophosphatidic acid in adipose tissue: in vivo and in vitro evidence. Biochim. Biophys. Acta 1841, 88–96 (2014).
Rancoule, C. et al. Lysophosphatidic acid impairs glucose homeostasis and inhibits insulin secretion in high-fat diet obese mice. Diabetologia 56, 1394–1402 (2013).
Lin, H. et al. Metabolic signaling of ceramides through the FPR2 receptor inhibits adipocyte thermogenesis. Science 388, eado4188 (2025).
De Nardo, W. et al. Effect of free fatty acids on TGF-β1 mediated fibrogenesis in hepatic stellate cells. Mol. Metab. 104, 102309 (2025).
Bugianesi, E. et al. Insulin resistance in non-diabetic patients with non-alcoholic fatty liver disease: sites and mechanisms. Diabetologia 48, 634–642 (2005).
Aronne, L. J. et al. Continued treatment with tirzepatide for maintenance of weight reduction in adults with obesity: the SURMOUNT-4 randomized clinical trial. JAMA 331, 38–48 (2024).
Antoniak-Pietrynczak, K., Zorena, K., Jaskulak, M., Hansdorfer-Korzon, R. & Koziński, M. Effect of manual lymphatic drainage on the concentrations of selected adipokines, cytokines, C-reactive protein and parameters of carbohydrate and lipid metabolism in patients with abnormal body mass index: focus on markers of obesity and insulin resistance. Int. J. Mol. Sci. 24, 10338 (2023).
Bagby, T. R. et al. Lymphatic trafficking kinetics and near-infrared imaging using star polymer architectures with controlled anionic character. Eur. J. Pharm. Sci. 47, 287–294 (2012).
Hartiala, P. et al. Phase 1 Lymfactin® study: short-term safety of combined adenoviral VEGF-C and lymph node transfer treatment for upper extremity lymphedema. J. Plast. Reconstr. Aesthet. Surg. 73, 1612–1621 (2020).
Szőke, D. et al. Nucleoside-modified VEGFC mRNA induces organ-specific lymphatic growth and reverses experimental lymphedema. Nat. Commun. 12, 3460 (2021).
Breslin, J. W. et al. Vascular endothelial growth factor-C stimulates the lymphatic pump by a VEGF receptor-3-dependent mechanism. Am. J. Physiol. Heart Circ. Physiol 293, H709–H718 (2007).
Kataru, R. P. et al. Lymphatic-specific intracellular modulation of receptor tyrosine kinase signaling improves lymphatic growth and function. Sci. Sig. 14, eabc0836 (2021).
Kang, N. H. et al. Ketoprofen alleviates diet-induced obesity and promotes white fat browning in mice via the activation of COX-2 through mTORC1-p38 signaling pathway. Pflug. Arch. 472, 583–596 (2020).
Hosono, K. et al. Roles of prostaglandin E2-EP3/EP4 receptor signaling in the enhancement of lymphangiogenesis during fibroblast growth factor-2-induced granulation formation. Arterioscler. Thromb. Vasc. Biol. 31, 1049–1058 (2011).
Schmidleithner, L. et al. Enzymatic activity of HPGD in Treg cells suppresses Tconv cells to maintain adipose tissue homeostasis and prevent metabolic dysfunction. Immunity 50, 1232–1248.e14 (2019).
Imamura, M. et al. Celecoxib as a potential treatment for intractable lymphatic malformation. Pediatrics 144, e20190319 (2019).
Tan, G. S. Q. et al. COX2 inhibitor use and type 2 diabetes treatment intensification: a registry-based cohort study. Diabetes Res. Clin. Pract. 207, 111082 (2024).
Lu, C.-H., Hung, Y.-J. & Hsieh, P.-S. Additional effect of metformin and celecoxib against lipid dysregulation and adipose tissue inflammation in high-fat fed rats with insulin resistance and fatty liver. Eur. J. Pharmacol. 789, 60–67 (2016).
Polzer, K. et al. Tumour necrosis factor blockade increases lymphangiogenesis in murine and human arthritic joints. Ann. Rheum. Dis. 67, 1610–1616 (2008).
Bouta, E. M. et al. Brief report: treatment of tumor necrosis factor-transgenic mice with anti-tumor necrosis factor restores lymphatic contractions, repairs lymphatic vessels, and may increase monocyte/macrophage egress. Arthritis Rheumatol. 69, 1187–1193 (2017).
Bernstein, L. E., Berry, J., Kim, S., Canavan, B. & Grinspoon, S. K. Effects of etanercept in patients with the metabolic syndrome. Arch. Intern. Med. 166, 902–908 (2006).
Dominguez, H. et al. Metabolic and vascular effects of tumor necrosis factor-α blockade with etanercept in obese patients with type 2 diabetes. J. Vasc. Res. 42, 517–525 (2005).
Patsalos, O., Dalton, B., Leppanen, J., Ibrahim, M. A. A. & Himmerich, H. Impact of TNF-α inhibitors on body weight and BMI: a systematic review and meta-analysis. Front. Pharmacol. 11, 481 (2020).
Börgeson, E. et al. Lipoxin A4 attenuates obesity-induced adipose inflammation and associated liver and kidney disease. Cell Metab. 22, 125–137 (2015).
Soták, M. et al. Lipoxins reduce obesity-induced adipose tissue inflammation in 3D-cultured human adipocytes and explant cultures. iScience 25, 104602 (2022).
Kim, H. J., Li, M., Nichols, C. G. & Davis, M. J. Large-conductance calcium-activated K+ channels, rather than KATP channels, mediate the inhibitory effects of nitric oxide on mouse lymphatic pumping. Br. J. Pharmacol. 178, 4119–4136 (2021).
Mathias, R. & von der Weid, P.-Y. Involvement of the NO-cGMP-KATP channel pathway in the mesenteric lymphatic pump dysfunction observed in the guinea pig model of TNBS-induced ileitis. Am. J. Physiol. Gastrointest. Liver Physiol. 304, G623–G634 (2012).
Davis, M. J. et al. Kir6.1-dependent K(ATP) channels in lymphatic smooth muscle and vessel dysfunction in mice with Kir6.1 gain-of-function. J. Physiol. 598, 3107–3127 (2020).
Bachmann, S. B. et al. A distinct role of the autonomic nervous system in modulating the function of lymphatic vessels under physiological and tumor-draining conditions. Cell Rep. 27, 3305–3314.e13 (2019).
Shew, T., Wolins, N. E. & Cifarelli, V. VEGFR-3 signaling regulates triglyceride retention and absorption in the intestine. Front. Physiol. 9, 1783 (2018).
Zhang, F. et al. Lacteal junction zippering protects against diet-induced obesity. Science 361, 599–603 (2018).
Suh, S. H. et al. Gut microbiota regulates lacteal integrity by inducing VEGF-C in intestinal villus macrophages. EMBO Rep. 20, e46927 (2019).
Bernier-Latmani, J. et al. DLL4 promotes continuous adult intestinal lacteal regeneration and dietary fat transport. J. Clin. Invest. 125, 4572–4586 (2015).
Nurmi, H. et al. VEGF-C is required for intestinal lymphatic vessel maintenance and lipid absorption. EMBO Mol. Med. 7, 1418–1425 (2015).
Gucciardo, F. et al. Targeting uPARAP modifies lymphatic vessel architecture and attenuates lymphedema. Circulation 151, 1412–1429 (2025).
Kikuchi, Y. et al. A Rho-kinase inhibitor, fasudil, prevents development of diabetes and nephropathy in insulin-resistant diabetic rats. J. Endocrinol. 192, 595–603 (2007).
Patsalos, O., Dalton, B. & Himmerich, H. Effects of IL-6 signaling pathway inhibition on weight and BMI: a systematic review and meta-analysis. Int. J. Mol. Sci. 21, 6290 (2020).
Findeisen, M. et al. Treatment of type 2 diabetes with the designer cytokine IC7Fc. Nature 574, 63–68 (2019).
Klarin, D. et al. Genetics of blood lipids among ~300,000 multi-ethnic participants of the Million Veteran Program. Nat. Genet. 50, 1514–1523 (2018).
Kimura, T. et al. Cilostazol improves lymphatic function by inducing proliferation and stabilization of lymphatic endothelial cells. J. Dermatol. Sci. 74, 150–158 (2014).
D’Alessio, D. et al. Fasting and postprandial concentrations of GLP-1 in intestinal lymph and portal plasma: evidence for selective release of GLP-1 in the lymph system. Am. J. Physiol. Regul. Integr. Comp. Physiol. 293, R2163–R2169 (2007).
Ohlsson, L., Kohan, A. B., Tso, P. & Ahrén, B. GLP-1 released to the mesenteric lymph duct in mice: effects of glucose and fat. Regul. Pept. 189, 40–45 (2014).
Schulz, M. E., Akerstrom, V. L., Dayan, J. H. & Castorena-Gonzalez, J. A. GLP-1R agonism directly improves the pumping capacity of murine collecting lymphatic vessels. Preprint at bioRxiv https://doi.org/10.64898/2025.12.26.696603 (2025).
Crowley, F., Brown, S., Gallagher, E. J. & Dayan, J. H. GLP-1 receptor agonist as an effective treatment for breast cancer-related lymphedema: a case report. Front. Oncol. 14, 1392375 (2024).
Nguyen, J. T. et al. Semaglutide treatment in a patient with extreme obesity and massive lymphedema: a case report. Obes. Facts 17, 641–645 (2024).
Brown, S. et al. Glucagon-like peptide-1 receptor agonists (GLP-1 RAs) may reduce the risk of developing cancer-related lymphedema following axillary lymph node dissection (ALND). Front. Pharmacol. 15, 1457363 (2024).
Aronne, L. J. et al. Tirzepatide as compared with semaglutide for the treatment of obesity. N. Engl. J. Med. 393, 26–36 (2025).
Yoder, S. M., Yang, Q., Kindel, T. L. & Tso, P. Stimulation of incretin secretion by dietary lipid: is it dose dependent? Am. J. Physiol. Gastrointest. Liver Physiol. 297, G299–G305 (2009).
Lim, D. M., Park, K. Y., Hwang, W. M., Kim, J. Y. & Kim, B. J. Difference in protective effects of GIP and GLP-1 on endothelial cells according to cyclic adenosine monophosphate response. Exp. Ther. Med. 13, 2558–2564 (2017).
Vaccaro, A., van de Walle, T., Ramachandran, M., Essand, M. & Dimberg, A. Of mice and lymphoid aggregates: modeling tertiary lymphoid structures in cancer. Front. Immunol. 14, 1275378 (2023).
Moro, K. et al. Innate production of TH2 cytokines by adipose tissue-associated c-Kit+Sca-1+ lymphoid cells. Nature 463, 540–544 (2010).
Okabe, Y. Development and organization of omental milky spots. Immunol. Rev. 324, 68–77 (2024).
Jackson-Jones, L. H. et al. Stromal cells covering omental fat-associated lymphoid clusters trigger formation of neutrophil aggregates to capture peritoneal contaminants. Immunity 52, 700–715.e6 (2020).
Khanal, S., Wieland, A. & Gunderson, A. J. Mechanisms of tertiary lymphoid structure formation: cooperation between inflammation and antigenicity. Front. Immunol. 14, 1267654 (2023).
Cruz-Migoni, S. & Caamaño, J. Fat-associated lymphoid clusters in inflammation and immunity. Front. Immunol. 7, 612 (2016).
Munoz-Erazo, L., Rhodes, J. L., Marion, V. C. & Kemp, R. A. Tertiary lymphoid structures in cancer — considerations for patient prognosis. Cell. Mol. Immunol. 17, 570–575 (2020).
Jackson-Jones, L. H. et al. Fat-associated lymphoid clusters control local IgM secretion during pleural infection and lung inflammation. Nat. Commun. 7, 12651 (2016).
Sato, Y., Silina, K., van den Broek, M., Hirahara, K. & Yanagita, M. The roles of tertiary lymphoid structures in chronic diseases. Nat. Rev. Nephrol. 19, 525–537 (2023).
Lai, Z. et al. Single-cell spatial transcriptomics of tertiary lymphoid organ-like structures in human atherosclerotic plaques. Nat. Cardiovasc. Res. 4, 547–566 (2025).
Mohanta, S. K. et al. Artery tertiary lymphoid organs contribute to innate and adaptive immune responses in advanced mouse atherosclerosis. Circ. Res. 114, 1772–1787 (2014).
Newland, S. A. et al. Type-2 innate lymphoid cells control the development of atherosclerosis in mice. Nat. Commun. 8, 15781 (2017).
Randolph, G. J. et al. Lymphoid aggregates remodel lymphatic collecting vessels that serve mesenteric lymph nodes in Crohn disease. Am. J. Pathol. 186, 3066–3073 (2016).
Czepielewski, R. S. et al. Ileitis-associated tertiary lymphoid organs arise at lymphatic valves and impede mesenteric lymph flow in response to tumor necrosis factor. Immunity 54, 2795–2811.e9 (2021).
da Fonseca, D. M. et al. Microbiota-dependent sequelae of acute infection compromise tissue-specific immunity. Cell 163, 354–366 (2015).
Krishnan, V. et al. Omental macrophages secrete chemokine ligands that promote ovarian cancer colonization of the omentum via CCR1. Commun. Biol. 3, 524 (2020).
Clark, R. et al. Milky spots promote ovarian cancer metastatic colonization of peritoneal adipose in experimental models. Am. J. Pathol. 183, 576–591 (2013).
Randall, T. D. & Mebius, R. E. The development and function of mucosal lymphoid tissues: a balancing act with micro-organisms. Mucosal Immunol. 7, 455–466 (2014).
Rangel-Moreno, J. et al. Omental milky spots develop in the absence of lymphoid tissue-inducer cells and support B and T cell responses to peritoneal antigens. Immunity 30, 731–743 (2009).
Daley, A. D. & Bénézech, C. Fat-associated lymphoid clusters: supporting visceral adipose tissue B cell function in immunity and metabolism. Immunol. Rev. 324, 78–94 (2024).
Betz, M. J. & Enerbäck, S. Targeting thermogenesis in brown fat and muscle to treat obesity and metabolic disease. Nat. Rev. Endocrinol. 14, 77–87 (2018).
Becher, T. et al. Brown adipose tissue is associated with cardiometabolic health. Nat. Med. 27, 58–65 (2021).
Cheong, L. Y. et al. Fibroblastic reticular cells in lymph node potentiate white adipose tissue beiging through neuro-immune crosstalk in male mice. Nat. Commun. 14, 1213 (2023).
Sun, W. et al. snRNA-seq reveals a subpopulation of adipocytes that regulates thermogenesis. Nature 587, 98–102 (2020).
Li, J. et al. Neurotensin is an anti-thermogenic peptide produced by lymphatic endothelial cells. Cell Metab. 33, 1449–1465.e6 (2021).
Vijgen, G. H. et al. Brown adipose tissue in morbidly obese subjects. PLoS ONE 6, e17247 (2011).
Betz, M. J. et al. Isoenergetic feeding of low carbohydrate-high fat diets does not increase brown adipose tissue thermogenic capacity in rats. PLoS ONE 7, e38997 (2012).
Cursiefen, C. et al. VEGF-A stimulates lymphangiogenesis and hemangiogenesis in inflammatory neovascularization via macrophage recruitment. J. Clin. Invest. 113, 1040–1050 (2004).
Shimizu, I. et al. Vascular rarefaction mediates whitening of brown fat in obesity. J. Clin. Invest. 124, 2099–2112 (2014).
Sun, K. et al. Brown adipose tissue derived VEGF-A modulates cold tolerance and energy expenditure. Mol. Metab. 3, 474–483 (2014).
Orava, J. et al. Different metabolic responses of human brown adipose tissue to activation by cold and insulin. Cell Metab. 14, 272–279 (2011).
Park, J. et al. VEGF-A-expressing adipose tissue shows rapid beiging and enhanced survival after transplantation and confers IL-4-independent metabolic improvements. Diabetes 66, 1479–1490 (2017).
Vegiopoulos, A. et al. Cyclooxygenase-2 controls energy homeostasis in mice by de novo recruitment of brown adipocytes. Science 328, 1158–1161 (2010).
Paschos, G. K. et al. Cold-induced browning of inguinal white adipose tissue is independent of adipose tissue cyclooxygenase-2. Cell Rep. 24, 809–814 (2018).
Phan, T. T. et al. Increased adipose tissue lymphatic vessel density inhibits thermogenesis through elevated neurotensin levels. Front. Cell. Dev. Biol. 11, 1100788 (2023).
Redder, E. et al. Specialized mesenteric lymphatic capillaries by-pass the mesenteric lymph node chain to transport peritoneal antigens directly into mediastinal lymph nodes. Preprint at bioRxiv https://doi.org/10.1101/2023.07.11.548304 (2023).
Sarfarazi, A. et al. Therapeutic delivery to the peritoneal lymphatics: current understanding, potential treatment benefits and future prospects. Int. J. Pharm. 567, 118456 (2019).
Ha, C. W. Y. et al. Translocation of viable gut microbiota to mesenteric adipose drives formation of creeping fat in humans. Cell 183, 666–683.e17 (2020).
Erlich, E. C. et al. Distinct roles for B cell-derived LTα3 and LTα1β2 in TNF-mediated ileitis. Nat. Immunol. 26, 1781–1793 (2025).
Author information
Authors and Affiliations
Contributions
W.D.N., A.Y.C. and E.C. researched data for the article. W.D.N. and N.L.T. wrote the article. All authors contributed to the discussion of the content and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
C.J.H.P., N.L.T. and E.C. are inventors of the lymph-directing glyceride prodrug technology (PCT/AU2020/050997) including celecoxib prodrugs for the treatment of metabolic disease (PCT/US 17/753,936), that has been patented and licensed via a commercial agreement with Seaport Therapeutics. The other authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Endocrinology thanks Jorge A. Castorena-Gonzalez, Joseph Rutkowski and Evan Rosen for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
De Nardo, W., Chan, A.Y., Porter, C.J.H. et al. Dysfunctional adipose tissue–lymphatic crosstalk in obesity. Nat Rev Endocrinol (2026). https://doi.org/10.1038/s41574-026-01243-y
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41574-026-01243-y