Abstract
Hepatocellular carcinoma (HCC) is a leading cause of cancer-related mortality worldwide. Curative-intent treatments offer the best long-term outcomes for selected patients. However, recurrence rates after resection approach 70% at 5 years, and access to transplantation remains limited by donor scarcity and stringent eligibility criteria. Emerging data reveal that recurrence is a reflection of underlying tumour biology, immune evasion and microenvironmental permissiveness. Advances in immunogenomic profiling, liquid biopsy and functional imaging are reshaping the concept of surgical eligibility, enabling biological risk stratification beyond conventional staging. At the same time, innovations in perioperative immunotherapy, graft preservation using machine perfusion and integrated multidisciplinary care are expanding the boundaries of curative treatment. These developments herald a shift from static criteria to dynamic, biology-driven paradigms that personalize surgical and transplant strategies. In this Review, we examine the evolving landscape of surgical treatment for HCC. We highlight the limitations of current selection frameworks, discuss how biological insights can inform resection and transplant decision-making and explore the role of perioperative and neoadjuvant therapies in reducing the recurrence of disease. Finally, we outline a future precision oncology model that integrates tumour genomics, immune phenotype and regenerative biology to improve outcomes in patients undergoing curative-intent treatment for HCC.
Key points
-
Curative-intent surgery for hepatocellular carcinoma — liver resection, ablation and liver transplantation — offers the best chance of long-term survival; however, recurrence remains common after resection or ablation, and access to transplantation is limited.
-
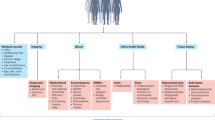
Traditional anatomical criteria for surgical selection are increasingly being replaced by biology-informed frameworks, incorporating tumour markers, immune profiling and functional imaging to assess risk and optimize outcomes.
-
Biological resectability, defined by tumour behaviour, regenerative capacity and microenvironmental permissiveness, is emerging as a more accurate predictor of surgical success than tumour size or number alone.
-
Machine perfusion technologies and expanded listing criteria are widening transplant access for select patients beyond conventional thresholds, including those with multifocal disease or portal vein tumour thrombosis.
-
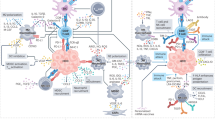
Recurrence after curative surgery reflects complex tumour–immune–liver interactions, including micrometastatic persistence, immune escape and regenerative signalling, offering targets for perioperative intervention.
-
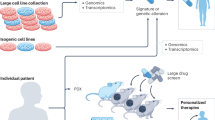
Perioperative immunotherapy and liquid biopsy technologies represent promising strategies to reduce recurrence and personalize care, but require further evaluation in prospective trials and integrated multidisciplinary frameworks.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Sung, H. et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 71, 209–249 (2021).
McGlynn, K. A., Petrick, J. L. & El-Serag, H. B. Epidemiology of hepatocellular carcinoma. Hepatology 73, 4–13 (2021).
Vitale, A. et al. Epidemiological trends and trajectories of MAFLD-associated hepatocellular carcinoma 2002–2033: the ITA.LI.CA database. Gut 72, 141–152 (2023).
Le, M. H. et al. Forecasted 2040 global prevalence of nonalcoholic fatty liver disease using hierarchical Bayesian approach. Clin. Mol. Hepatol. 28, 841–850 (2022).
Rumgay, H. et al. Global burden of primary liver cancer in 2020 and predictions to 2040. J. Hepatol. 77, 1598–1606 (2022).
Singal, A. G., Kanwal, F. & Llovet, J. M. Global trends in hepatocellular carcinoma epidemiology: implications for screening, prevention and therapy. Nat. Rev. Clin. Oncol. 20, 864–884 (2023).
Norén, S., Bengtsson, B., Hagström, H., Ljunggren, G. & Wahlin, S. Hepatocellular carcinoma in Stockholm, Sweden 2003–2018: a population-based cohort study. Scand. J. Gastroenterol. 57, 1080–1088 (2022).
Cullen, K. et al. Cost of hepatocellular carcinoma to the national health service in England: a registry-based analysis. BMJ Open Gastroenterol. 10, e000998 (2023).
Fulgenzi, C. A. M. et al. Immunotherapy vs best supportive care for patients with hepatocellular cancer with Child–Pugh B dysfunction. JAMA Oncol. 10, 1253–1258 (2024).
Vogel, A., Meyer, T., Sapisochin, G., Salem, R. & Saborowski, A. Hepatocellular carcinoma. Lancet 400, 1345–1362 (2022).
Allaire, M. et al. New frontiers in liver resection for hepatocellular carcinoma. JHEP Rep. 2, 100134 (2020).
Portolani, N. et al. Early and late recurrence after liver resection for hepatocellular carcinoma: prognostic and therapeutic implications. Ann. Surg. 243, 229–235 (2006).
Sapisochin, G. & Bruix, J. Liver transplantation for hepatocellular carcinoma: outcomes and novel surgical approaches. Nat. Rev. Gastroenterol. Hepatol. 14, 203–217 (2017).
Nguyen, P. H. D. et al. Trajectory of immune evasion and cancer progression in hepatocellular carcinoma. Nat. Commun. 13, 1441 (2022).
Sia, D. et al. Identification of an immune-specific class of hepatocellular carcinoma, based on molecular features. Gastroenterology 153, 812–826 (2017).
Donne, R. & Lujambio, A. The liver cancer immune microenvironment: therapeutic implications for hepatocellular carcinoma. Hepatology 77, 1773–1796 (2023).
Chen, K., Shuen, T. W. H. & Chow, P. K. H. The association between tumour heterogeneity and immune evasion mechanisms in hepatocellular carcinoma and its clinical implications. Br. J. Cancer 131, 420–429 (2024).
Safri, F., Nguyen, R., Zerehpooshnesfchi, S., George, J. & Qiao, L. Heterogeneity of hepatocellular carcinoma: from mechanisms to clinical implications. Cancer Gene Ther. 31, 1105–1112 (2024).
Reig, M. et al. BCLC strategy for prognosis prediction and treatment recommendation: the 2022 update. J. Hepatol. 76, 681–693 (2022).
Hasegawa, K. et al. Clinical practice guidelines for hepatocellular carcinoma: the Japan Society of Hepatology 2021 version (5th JSH-HCC Guidelines). Hepatol. Res. 53, 383–390 (2023).
Korean Liver Cancer Association, National Cancer Center. 2022 KLCA-NCC Korea practice guidelines for the management of hepatocellular carcinoma. Clin. Mol. Hepatol. 28, 583–705 (2022).
Singal, A. G. et al. AASLD practice guidance on prevention, diagnosis, and treatment of hepatocellular carcinoma. Hepatology 78, 1922–1965 (2023).
Sangro, B. et al. EASL clinical practice guidelines on the management of hepatocellular carcinoma. J. Hepatol. 82, 315–374 (2025).
Benson, A. B. et al. Hepatobiliary cancers, version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J. Natl Compr. Canc. Netw. 19, 541–565 (2021).
Suddle, A. et al. British Society of Gastroenterology guidelines for the management of hepatocellular carcinoma in adults. Gut 73, 1235–1268 (2024).
Reig, M. et al. BCLC strategy for prognosis prediction and treatment recommendations: the 2025 update. J. Hepatol. https://doi.org/10.1016/j.jhep.2025.10.020 (2025).
Lau, G. et al. APASL clinical practice guidelines on systemic therapy for hepatocellular carcinoma — 2024. Hepatol. Int. 18, 1661–1683 (2024).
Mazzaferro, V. et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N. Engl. J. Med. 334, 693–699 (1996).
Di Sandro, S. et al. Surgical and oncological outcomes of hepatic resection for BCLC-B hepatocellular carcinoma: a retrospective multicenter analysis among 474 consecutive cases. Updates Surg. 71, 285–293 (2019).
Hyun, M. H. et al. Hepatic resection compared to chemoembolization in intermediate- to advanced-stage hepatocellular carcinoma: a meta-analysis of high-quality studies. Hepatology 68, 977–993 (2018).
Tsilimigras, D. I. et al. Prognosis after resection of Barcelona Clinic Liver Cancer (BCLC) stage 0, A, and B hepatocellular carcinoma: a comprehensive assessment of the current BCLC classification. Ann. Surg. Oncol. 26, 3693–3700 (2019).
Torzilli, G. et al. A snapshot of the effective indications and results of surgery for hepatocellular carcinoma in tertiary referral centers: is it adherent to the EASL/AASLD recommendations?: an observational study of the HCC East-West study group. Ann. Surg. 257, 929–937 (2013).
Finn, R. S. et al. Atezolizumab plus bevacizumab in unresectable hepatocellular carcinoma. N. Engl. J. Med. 382, 1894–1905 (2020).
Llovet, J. M. et al. Sorafenib in advanced hepatocellular carcinoma. N. Engl. J. Med. 359, 378–390 (2008).
Abou-Alfa Ghassan, K. et al. Tremelimumab plus durvalumab in unresectable hepatocellular carcinoma. NEJM Evid. 1, EVIDoa2100070 (2022).
Kudo, M. et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: a randomised phase 3 non-inferiority trial. Lancet 391, 1163–1173 (2018).
Bruix, J. et al. Adjuvant sorafenib for hepatocellular carcinoma after resection or ablation (STORM): a phase 3, randomised, double-blind, placebo-controlled trial. Lancet Oncol. 16, 1344–1354 (2015).
Qin, S. et al. Atezolizumab plus bevacizumab versus active surveillance in patients with resected or ablated high-risk hepatocellular carcinoma (IMbrave050): a randomised, open-label, multicentre, phase 3 trial. Lancet 402, 1835–1847 (2023).
Yopp, A. et al. LBA39 updated efficacy and safety data from IMbrave050: phase III study of adjuvant atezolizumab (atezo) + bevacizumab (bev) vs active surveillance in patients (pts) with resected or ablated high-risk hepatocellular carcinoma (HCC). Ann. Oncol. 35, S1230 (2024).
Berardi, G. et al. Transarterial radioembolization can downstage intermediate and advanced hepatocellular carcinoma to liver transplantation. Transplantation 109, e54–e63 (2025).
Chapman, W. C. et al. Outcomes of neoadjuvant transarterial chemoembolization to downstage hepatocellular carcinoma before liver transplantation. Ann. Surg. 248, 617–625 (2008).
Pracht, M. et al. Lobar hepatocellular carcinoma with ipsilateral portal vein tumor thrombosis treated with yttrium-90 glass microsphere radioembolization: preliminary results. Int. J. Hepatol. 2013, 827649 (2013).
Prince, D. S. et al. Selective internal radiation therapy for hepatocellular carcinoma: a 15-year multicenter Australian cohort study. J. Gastroenterol. Hepatol. 37, 2173–2181 (2022).
Tabrizian, P. et al. Ten-year outcomes of liver transplant and downstaging for hepatocellular carcinoma. JAMA Surg. 157, 779–788 (2022).
Yin, C. et al. Bridging and downstaging with TACE in early and intermediate stage hepatocellular carcinoma: predictors of receiving a liver transplant. Ann. Gastroenterol. Surg. 7, 295–305 (2023).
Mazzaferro, V. et al. Liver transplantation in hepatocellular carcinoma after tumour downstaging (XXL): a randomised, controlled, phase 2b/3 trial. Lancet Oncol. 21, 947–956 (2020).
Squires, M. H. III et al. Transplant versus resection for the management of hepatocellular carcinoma meeting Milan criteria in the MELD exception era at a single institution in a UNOS region with short wait times. J. Surg. Oncol. 109, 533–541 (2014).
Koniaris, L. G. et al. Is surgical resection superior to transplantation in the treatment of hepatocellular carcinoma? Ann. Surg. 254, 527–537 (2011).
Lim, K. C. et al. Cost-effectiveness analysis of liver resection versus transplantation for early hepatocellular carcinoma within the Milan criteria. Hepatology 61, 227–237 (2015).
Adam, R. et al. Resection or transplantation for early hepatocellular carcinoma in a cirrhotic liver: does size define the best oncological strategy? Ann. Surg. 256, 883–891 (2012).
Cherqui, D. et al. Liver resection for transplantable hepatocellular carcinoma: long-term survival and role of secondary liver transplantation. Ann. Surg. 250, 738–746 (2009).
Ferrer-Fabrega, J. & Bruix, J. Resection vs. transplantation for hepatocellular carcinoma: a never ending challenge. Hepatobiliary Surg. Nutr. 12, 443–446 (2023).
Tsilimigras, D. I. et al. Defining the chance of cure after resection for hepatocellular carcinoma within and beyond the Barcelona Clinic Liver Cancer guidelines: a multi-institutional analysis of 1,010 patients. Surgery 166, 967–974 (2019).
Dixon, M., Cruz, J., Sarwani, N. & Gusani, N. The future liver remnant : definition, evaluation, and management. Am. Surg. 87, 276–286 (2021).
Farges, O. et al. Portal vein embolization before right hepatectomy: prospective clinical trial. Ann. Surg. 237, 208–217 (2003).
Imamura, H. et al. Preoperative portal vein embolization: an audit of 84 patients. Hepatology 29, 1099–1105 (1999).
She, W. H. & Chok, K. Strategies to increase the resectability of hepatocellular carcinoma. World J. Hepatol. 7, 2147–2154 (2015).
Child, C. G. & Turcotte, J. G. Surgery and portal hypertension. Major Probl. Clin. Surg. 1, 1–85 (1964).
Abbas, N. et al. Guidance document: risk assessment of patients with cirrhosis prior to elective non-hepatic surgery. Frontline Gastroenterol. 14, 359 (2023).
Berardi, G. et al. Development of a nomogram to predict outcome after liver resection for hepatocellular carcinoma in Child–Pugh B cirrhosis. J. Hepatol. 72, 75–84 (2020).
Johnson, P. J. et al. Assessment of liver function in patients with hepatocellular carcinoma: a new evidence-based approach — the ALBI grade. J. Clin. Oncol. 33, 550–558 (2015).
de Franchis, R. et al. Renewing consensus in portal hypertension. J. Hepatol. 76, 959–974 (2022).
Maithel, S. K. et al. Importance of low preoperative platelet count in selecting patients for resection of hepatocellular carcinoma: a multi-institutional analysis. J. Am. Coll. Surg. 212, 638–648 (2011).
Azoulay, D. et al. Liver resection for hepatocellular carcinoma in patients with clinically significant portal hypertension. JHEP Rep. 3, 100190 (2021).
Kobayashi, Y. et al. Expanded Makuuchi’s criteria using estimated indocyanine green clearance rate of future liver remnant as a safety limit for maximum extent of liver resection. HPB 21, 990–997 (2019).
de Graaf, W., van den Esschert, J. W., van Lienden, K. P. & van Gulik, T. M. Induction of tumor growth after preoperative portal vein embolization: is it a real problem? Ann. Surg. Oncol. 16, 423–430 (2009).
Del Basso, C. et al. Current strategies to induce liver remnant hypertrophy before major liver resection. World J. Hepatol. 13, 1629–1641 (2021).
Wong, P. et al. Augmenting the future liver remnant prior to major hepatectomy: a review of options on the menu. Ann. Surg. Oncol. 32, 5694–5709 (2025).
Obmann, V. C. et al. T1 reduction rate with Gd-EOB-DTPA determines liver function on both 1.5 T and 3 T MRI. Sci. Rep. 12, 4716 (2022).
Tsujita, Y. et al. Prediction of post-hepatectomy liver failure using gadoxetic acid-enhanced magnetic resonance imaging for hepatocellular carcinoma with portal vein invasion. Eur. J. Radiol. 130, 109189 (2020).
Baleato-González, S. et al. Current and advanced applications of gadoxetic acid-enhanced MRI in hepatobiliary disorders. Radiographics 43, e220087 (2023).
Lauscher, J. C. et al. Prediction of post-hepatectomy liver failure by preoperative gadoxetate disodium-enhanced magnetic resonance imaging. HPB 26, 782–788 (2024).
Luo, N. et al. A functional liver imaging score for preoperative prediction of liver failure after hepatocellular carcinoma resection. Eur. Radiol. 32, 5623–5632 (2022).
Nevola, R. et al. Predictors of early and late hepatocellular carcinoma recurrence. World J. Gastroenterol. 29, 1243–1260 (2023).
Ryu, T. et al. Double- and triple-positive tumor markers predict early recurrence and poor survival in patients with hepatocellular carcinoma within the Milan criteria and Child–Pugh class A. J. Gastrointest. Surg. 21, 957–966 (2017).
Mahmud, N., John, B., Taddei, T. H. & Goldberg, D. S. Pre-transplant alpha-fetoprotein is associated with post-transplant hepatocellular carcinoma recurrence mortality. Clin. Transpl. 33, e13634 (2019).
Norman, J. S. et al. AFP-L3 and DCP strongly predict early hepatocellular carcinoma recurrence after liver transplantation. J. Hepatol. 79, 1469–1477 (2023).
Calderaro, J. et al. Histological subtypes of hepatocellular carcinoma are related to gene mutations and molecular tumour classification. J. Hepatol. 67, 727–738 (2017).
Calderaro, J., Ziol, M., Paradis, V. & Zucman-Rossi, J. Molecular and histological correlations in liver cancer. J. Hepatol. 71, 616–630 (2019).
Ziol, M. et al. Macrotrabecular-massive hepatocellular carcinoma: a distinctive histological subtype with clinical relevance. Hepatology 68, 103–112 (2018).
Montironi, C. et al. Inflamed and non-inflamed classes of HCC: a revised immunogenomic classification. Gut 72, 129–140 (2023).
Salié, H. et al. Spatial single-cell profiling and neighbourhood analysis reveal the determinants of immune architecture connected to checkpoint inhibitor therapy outcome in hepatocellular carcinoma. Gut 74, 451–466 (2025).
Sangro, B. et al. Association of inflammatory biomarkers with clinical outcomes in nivolumab-treated patients with advanced hepatocellular carcinoma. J. Hepatol. 73, 1460–1469 (2020).
Feng, Z. et al. CT radiomics to predict macrotrabecular-massive subtype and immune status in hepatocellular carcinoma. Radiology 307, e221291 (2023).
Gillies, R. J., Kinahan, P. E. & Hricak, H. Radiomics: images are more than pictures, they are data. Radiology 278, 563–577 (2016).
Gong, X. Q. et al. Radiomics models based on multisequence MRI for predicting PD-1/PD-L1 expression in hepatocellular carcinoma. Sci. Rep. 13, 7710 (2023).
Han, Z. et al. Delta-radiomics models based on multi-phase contrast-enhanced magnetic resonance imaging can preoperatively predict glypican-3-positive hepatocellular carcinoma. Front. Physiol. 14, 1138239 (2023).
Greten, T. F. et al. Biomarkers for immunotherapy of hepatocellular carcinoma. Nat. Rev. Clin. Oncol. 20, 780–798 (2023).
Ogle, L. F. et al. Imagestream detection and characterisation of circulating tumour cells — a liquid biopsy for hepatocellular carcinoma? J. Hepatol. 65, 305–313 (2016).
Qi, L. N. et al. Circulating tumor cells undergoing EMT provide a metric for diagnosis and prognosis of patients with hepatocellular carcinoma. Cancer Res. 78, 4731–4744 (2018).
Wehrle, C. J. et al. Tumor mutational burden from circulating tumor DNA predicts recurrence of hepatocellular carcinoma after resection: an emerging biomarker for surveillance. Ann. Surg. 280, 504–513 (2024).
Siejka-Zielińska, P. et al. Cell-free DNA TAPS provides multimodal information for early cancer detection. Sci. Adv. 7, eabh0534 (2021).
Lim, C. et al. 18F-FDG PET/CT predicts microvascular invasion and early recurrence after liver resection for hepatocellular carcinoma: a prospective observational study. HPB 21, 739–747 (2019).
Zheng, W. J. et al. (18)F-FDG PET/CT predicts the prognosis of patients with hepatocellular carcinoma undergoing liver transplantation. Liver Cancer 5, 1–21 (2025).
Chok, K. S. et al. Surgical outcomes in hepatocellular carcinoma patients with portal vein tumor thrombosis. World J. Surg. 38, 490–496 (2014).
Kokudo, T. et al. Survival benefit of liver resection for hepatocellular carcinoma associated with portal vein invasion. J. Hepatol. 65, 938–943 (2016).
Kokudo, T. et al. Liver resection for hepatocellular carcinoma associated with hepatic vein invasion: a Japanese nationwide survey. Hepatology 66, 510–517 (2017).
Yamamoto, Y. et al. Post-hepatectomy survival in advanced hepatocellular carcinoma with portal vein tumor thrombosis. World J. Gastroenterol. 21, 246–253 (2015).
Wee, I. J. Y. et al. Extending surgical resection for hepatocellular carcinoma beyond Barcelona Clinic for Liver Cancer (BCLC) stage A: a novel application of the modified BCLC staging system. J. Hepatocell. Carcinoma 9, 839–851 (2022).
Kadi, D. et al. Imaging prognostication and tumor biology in hepatocellular carcinoma. J. Liver Cancer 23, 284–299 (2023).
Chen, J. et al. A multimodal atlas of hepatocellular carcinoma reveals convergent evolutionary paths and ‘bad apple’ effect on clinical trajectory. J. Hepatol. 81, 667–678 (2024).
Hamaoka, M. et al. Hepatectomy after down-staging of hepatocellular carcinoma with portal vein tumor thrombus using chemoradiotherapy: a retrospective cohort study. Int. J. Surg. 44, 223–228 (2017).
Peng, Z. et al. Adjuvant transarterial chemoembolization with sorafenib for portal vein tumor thrombus: a randomized clinical trial. JAMA Surg. 159, 616–624 (2024).
Ding, X. et al. Transarterial chemoembolization plus lenvatinib versus transarterial chemoembolization plus sorafenib as first-line treatment for hepatocellular carcinoma with portal vein tumor thrombus: a prospective randomized study. Cancer 127, 3782–3793 (2021).
Cucchetti, A. et al. Selective internal radiation therapy (SIRT) as conversion therapy for unresectable primary liver malignancies. Liver Cancer 5, 303–311 (2016).
de la Torre-Alaez, M. et al. Nivolumab after selective internal radiation therapy for the treatment of hepatocellular carcinoma: a phase 2, single-arm study. J. Immunother. Cancer 10, e005457 (2022).
Reeves, H. L., Reicher, J., Priona, G., Manas, D. M. & Littler, P. Selective internal radiation therapy (SIRT) for hepatocellular carcinoma (HCC): informing clinical practice for multidisciplinary teams in England. Frontline Gastroenterol. 14, 45–51 (2023).
Regnault, H. et al. Selective internal radiation therapy for unresectable HCC: the SIRT downstaging study. Hepatol. Commun. 8, e0475 (2024).
Koh, J. H. et al. Liver resection versus liver transplantation for hepatocellular carcinoma within Milan criteria: a meta-analysis of 18,421 patients. Hepatobiliary Surg. Nutr. 11, 78–93 (2022).
Li, C. et al. Liver resection versus transplantation for multiple hepatocellular carcinoma: a propensity score analysis. Oncotarget 8, 81492–81500 (2017).
Sung, P. S. et al. Long-term outcome of liver resection versus transplantation for hepatocellular carcinoma in a region where living donation is a main source. Ann. Transpl. 22, 276–284 (2017).
Roayaie, S. et al. The role of hepatic resection in the treatment of hepatocellular cancer. Hepatology 62, 440–451 (2015).
Chapman, W. C. et al. Surgical treatment of hepatocellular carcinoma in North America: can hepatic resection still be justified? J. Am. Coll. Surg. 220, 628–637 (2015).
Yao, F. Y. et al. Liver transplantation for hepatocellular carcinoma: expansion of the tumor size limits does not adversely impact survival. Hepatology 33, 1394–1403 (2001).
Mazzaferro, V. et al. Predicting survival after liver transplantation in patients with hepatocellular carcinoma beyond the Milan criteria: a retrospective, exploratory analysis. Lancet Oncol. 10, 35–43 (2009).
Kaido, T. et al. Usefulness of the Kyoto criteria as expanded selection criteria for liver transplantation for hepatocellular carcinoma. Surgery 154, 1053–1060 (2013).
Sapisochin, G. et al. The extended Toronto criteria for liver transplantation in patients with hepatocellular carcinoma: a prospective validation study. Hepatology 64, 2077–2088 (2016).
Duvoux, C. et al. Liver transplantation for hepatocellular carcinoma: a model including alpha-fetoprotein improves the performance of Milan criteria. Gastroenterology 143, 986–994.e3 (2012).
Mazzaferro, V. et al. Metroticket 2.0 model for analysis of competing risks of death after liver transplantation for hepatocellular carcinoma. Gastroenterology 154, 128–139 (2018).
Wehrle, C. J. et al. Risk assessment in liver transplantation for hepatocellular carcinoma: long-term follow-up of a two-centre experience. Int. J. Surg. 110, 2818–2831 (2024).
Halazun, K. J. et al. Dynamic α-fetoprotein response and outcomes after liver transplant for hepatocellular carcinoma. JAMA Surg. 156, 559–567 (2021).
Xu, E. et al. Downstaging of hepatocellular carcinoma before liver transplantation: results from a national multicenter prospective cohort study. Hepatology 82, 612–625 (2025).
Tabrizian, P. et al. Intention-to-treat outcomes of patients with hepatocellular carcinoma receiving immunotherapy before liver transplant: the multicenter VITALITY study. J. Hepatol. 82, 512–522 (2025).
Jiang, N. et al. Circulating tumor DNA is a potential prognostic risk factor of recurrence in patients with hepatocellular carcinoma treated by liver transplantation. J. Clin. Oncol. 40, e16196 (2022).
Gonçalves, E., Gonçalves-Reis, M., Pereira-Leal, J. B. & Cardoso, J. DNA methylation fingerprint of hepatocellular carcinoma from tissue and liquid biopsies. Sci. Rep. 12, 11512 (2022).
Ahn, J. C., Qureshi, T. A., Singal, A. G., Li, D. & Yang, J. D. Deep learning in hepatocellular carcinoma: current status and future perspectives. World J. Hepatol. 13, 2039–2051 (2021).
Calderaro, J., Seraphin, T. P., Luedde, T. & Simon, T. G. Artificial intelligence for the prevention and clinical management of hepatocellular carcinoma. J. Hepatol. 76, 1348–1361 (2022).
Cao, S. et al. Deep learning for hepatocellular carcinoma recurrence before and after liver transplantation: a multicenter cohort study. Sci. Rep. 15, 7730 (2025).
Kwong, A. et al. Machine learning to predict waitlist dropout among liver transplant candidates with hepatocellular carcinoma. Cancer Med. 11, 1535–1541 (2022).
Altaf, A. et al. Artificial intelligence-based model for the recurrence of hepatocellular carcinoma after liver transplantation. Surgery 176, 1500–1506 (2024).
Soin, A. et al. Are patients with hepatocellular carcinoma and portal vein tumour thrombosis candidates for liver transplantation? J. Hepatol. 78, 1124–1129 (2023).
Lee, K.-W. et al. Macrovascular invasion is not an absolute contraindication for living donor liver transplantation. Liver Transplant. 23, 19–27 (2017).
Jeong, Y. et al. Liver transplantation after transarterial chemoembolization and radiotherapy for hepatocellular carcinoma with vascular invasion. J. Gastrointest. Surg. 21, 275–283 (2017).
Liu, J., Qian, J., Yang, Z., Zhou, L. & Zheng, S. Patients with hepatocellular carcinoma and portal vein tumour thrombosis after successful downstaging may be candidates for liver transplantation: a meta-analysis. J. Hepatol. 80, e219–e221 (2024).
Schurink, I. J. et al. Salvage of declined extended-criteria DCD livers using in situ normothermic regional perfusion. Ann. Surg. 276, e223–e230 (2022).
Gaurav, R. et al. Liver transplantation outcomes from controlled circulatory death donors: SCS vs in situ NRP vs ex situ NMP. Ann. Surg. 275, 1156–1164 (2022).
De Carlis, R., Paolo, M. & Taner, B. Donation after circulatory death: novel strategies to improve the liver transplant outcome. J. Hepatol. 78, 1169–1180 (2023).
Oniscu, G. C. et al. Improved organ utilization and better transplant outcomes with in situ normothermic regional perfusion in controlled donation after circulatory death. Transplantation 107, 438–448 (2023).
Rigo, F. et al. Impact of hypothermic oxygenated machine perfusion on hepatocellular carcinoma recurrence after liver transplantation. J. Pers. Med. 13, 703 (2023).
Brubaker, A. L. et al. US liver transplant outcomes after normothermic regional perfusion vs standard super rapid recovery. JAMA Surg. 159, 677–685 (2024).
Mehta, N., Dodge, J. L., Hirose, R., Roberts, J. P. & Yao, F. Y. Increasing liver transplantation wait-list dropout for hepatocellular carcinoma with widening geographical disparities: implications for organ allocation. Liver Transpl. 24, 1346–1356 (2018).
Sokolich, J. et al. HCC liver transplantation wait list dropout rates before and after the mandated 6-month wait time. Am. Surg. 86, 1592–1595 (2020).
Wallace, D. et al. National time trends in mortality and graft survival following liver transplantation from circulatory death or brainstem death donors. Br. J. Surg. 109, 79–88 (2021).
Bernards, S. et al. The impact of median model for end-stage liver disease at transplant minus 3 national policy on waitlist outcomes in patients with and without hepatocellular carcinoma. Liver Transpl. 28, 376–385 (2022).
Mueller, M. et al. Hypothermic oxygenated liver perfusion (HOPE) prevents tumor recurrence in liver transplantation from donation after circulatory death. Ann. Surg. 272, 759–765 (2020).
Mergental, H. et al. Transplantation of discarded livers following viability testing with normothermic machine perfusion. Nat. Commun. 11, 2939 (2020).
Sousa Da Silva, R. X., Weber, A., Dutkowski, P. & Clavien, P. A. Machine perfusion in liver transplantation. Hepatology 76, 1531–1549 (2022).
Schlegel, A. et al. Machine perfusion of the liver and bioengineering. J. Hepatol. 78, 1181–1198 (2023).
Eshmuminov, D. et al. An integrated perfusion machine preserves injured human livers for 1 week. Nat. Biotechnol. 38, 189–198 (2020).
Cillo, U., Nalesso, F., Bertacco, A., Indraccolo, S. & Gringeri, E. Normothermic perfusion of a human tumoral liver for 17 days with concomitant extracorporeal blood purification therapy: case description. J. Hepatol. 81, e96–e98 (2024).
Sugawara, Y., Tamura, S. & Makuuchi, M. Living donor liver transplantation for hepatocellular carcinoma: Tokyo University Series. Dig. Dis. 25, 310–312 (2007).
Lee, S. G. et al. Expanded indication criteria of living donor liver transplantation for hepatocellular carcinoma at one large-volume center. Liver Transpl. 14, 935–945 (2008).
Goldaracena, N. et al. Live donor liver transplantation for patients with hepatocellular carcinoma offers increased survival vs. deceased donation. J. Hepatol. 70, 666–673 (2019).
Shah, S. A. et al. Recurrence after liver resection for hepatocellular carcinoma: risk factors, treatment, and outcomes. Surgery 141, 330–339 (2007).
Tabrizian, P., Jibara, G., Shrager, B., Schwartz, M. & Roayaie, S. Recurrence of hepatocellular cancer after resection: patterns, treatments, and prognosis. Ann. Surg. 261, 947–955 (2015).
Lima, H. A. et al. Application of hazard functions to investigate recurrence after curative-intent resection for hepatocellular carcinoma. HPB 25, 260–268 (2023).
Abou-Alfa, G. K. et al. Tremelimumab plus durvalumab in unresectable hepatocellular carcinoma. NEJM Evid. 1, EVIDoa2100070 (2022).
Zimmerman, M. A. et al. Recurrence of hepatocellular carcinoma following liver transplantation: a review of preoperative and postoperative prognostic indicators. Arch. Surg. 143, 182–188 (2008).
Toso, C., Mentha, G. & Majno, P. Liver transplantation for hepatocellular carcinoma: five steps to prevent recurrence. Am. J. Transpl. 11, 2031–2035 (2011).
Shi, F. et al. PD-1 and PD-L1 upregulation promotes CD8+ T-cell apoptosis and postoperative recurrence in hepatocellular carcinoma patients. Int. J. Cancer 128, 887–896 (2011).
Qiu, Z.-Q. et al. The clinical relevance of epithelial–mesenchymal transition and its correlations with tumorigenic immune infiltrates in hepatocellular carcinoma. Immunology 166, 185–196 (2022).
Lee, H. A. et al. Change in the recurrence pattern and predictors over time after complete cure of hepatocellular carcinoma. Gut Liver 15, 420–429 (2021).
Jung, S. M. et al. Characteristics of early recurrence after curative liver resection for solitary hepatocellular carcinoma. J. Gastrointest. Surg. 23, 304–311 (2019).
Xing, H. et al. Defining and predicting early recurrence after liver resection of hepatocellular carcinoma: a multi-institutional study. HPB 22, 677–689 (2020).
Shah, S. A. et al. Factors associated with early recurrence after resection for hepatocellular carcinoma and outcomes. J. Am. Coll. Surg. 202, 275–283 (2006).
Zhu, Y. et al. Factors influencing early recurrence of hepatocellular carcinoma after curative resection. J. Int. Med. Res. 48, 300060520945552 (2020).
Hoare, M., Das, T. & Alexander, G. Ageing, telomeres, senescence, and liver injury. J. Hepatol. 53, 950–961 (2010).
Bernsmeier, C., van der Merwe, S. & Périanin, A. Innate immune cells in cirrhosis. J. Hepatol. 73, 186–201 (2020).
Rosato, V. et al. Factors affecting long-term changes of liver stiffness in direct-acting anti-hepatitis C virus therapy: a multicentre prospective study. J. Viral Hepat. 29, 26–34 (2022).
Marasco, G. et al. Role of liver and spleen stiffness in predicting the recurrence of hepatocellular carcinoma after resection. J. Hepatol. 70, 440–448 (2019).
Ding, X. et al. Genomic and epigenomic features of primary and recurrent hepatocellular carcinomas. Gastroenterology 157, 1630–1645.e6 (2019).
Anbarasu, C. R., Williams-Perez, S., Camp, E. R. & Erstad, D. J. Surgical implications for nonalcoholic steatohepatitis-related hepatocellular carcinoma. Cancers 16, 2773 (2024).
Pfister, D. et al. NASH limits anti-tumour surveillance in immunotherapy-treated HCC. Nature 592, 450–456 (2021).
Leslie, J. et al. CXCR2 inhibition enables NASH-HCC immunotherapy. Gut 71, 2093–2106 (2022).
Ma, C. et al. Gut microbiome-mediated bile acid metabolism regulates liver cancer via NKT cells. Science 360, eaan5931 (2018).
Lapidot, Y. et al. Alterations in the gut microbiome in the progression of cirrhosis to hepatocellular carcinoma. mSystems 5, e00153-20 (2020).
Sun, J. et al. Butyrate as a promising therapeutic target in cancer: from pathogenesis to clinic (review). Int. J. Oncol. 64, 44 (2024).
Zheng, J. et al. Neutrophil to lymphocyte ratio and platelet to lymphocyte ratio as prognostic predictors for hepatocellular carcinoma patients with various treatments: a meta-analysis and systematic review. Cell. Physiol. Biochem. 44, 967–981 (2017).
Zanetto, A. et al. Influence of hepatocellular carcinoma on platelet aggregation in cirrhosis. Cancers 13, 1150 (2021).
Boccatonda, A. et al. Platelet, antiplatelet therapy and metabolic dysfunction-associated steatotic liver disease: a narrative review. Life 14, 473 (2024).
Malehmir, M. et al. Platelet GPIbα is a mediator and potential interventional target for NASH and subsequent liver cancer. Nat. Med. 25, 641–655 (2019).
Yang, F., Hua, Q., Zhu, X. & Xu, P. Surgical stress induced tumor immune suppressive environment. Carcinogenesis 45, 185–198 (2024).
Onuma, A. E., Zhang, H., Gil, L., Huang, H. & Tsung, A. Surgical stress promotes tumor progression: a focus on the impact of the immune response. J. Clin. Med. 9, 4096 (2020).
Krall, J. A. et al. The systemic response to surgery triggers the outgrowth of distant immune-controlled tumors in mouse models of dormancy. Sci. Transl Med. 10, eaan3464 (2018).
Shi, J. H. & Line, P. D. Hallmarks of postoperative liver regeneration: an updated insight on the regulatory mechanisms. J. Gastroenterol. Hepatol. 35, 960–966 (2020).
Dehlke, K. et al. Predicting liver regeneration following major resection. Sci. Rep. 12, 13396 (2022).
Chen, H. et al. One shoot, two birds: alleviating inflammation caused by ischemia/reperfusion injury to reduce the recurrence of hepatocellular carcinoma. Front. Immunol. 13, 879552 (2022).
Chen, Z. et al. Analysis of preoperative circulating tumor cells for recurrence in patients with hepatocellular carcinoma after liver transplantation. Ann. Transl. Med. 8, 1067 (2020).
Carissimi, F. et al. Finding the seed of recurrence: hepatocellular carcinoma circulating tumor cells and their potential to drive the surgical treatment. World J. Gastrointest. Surg. 13, 967–978 (2021).
Xu, W. et al. Isolation of circulating tumor cells in patients with hepatocellular carcinoma using a novel cell separation strategy. Clin. Cancer Res. 17, 3783–3793 (2011).
Li, C. X. et al. CXCL10/CXCR3 signaling mobilized-regulatory T cells promote liver tumor recurrence after transplantation. J. Hepatol. 65, 944–952 (2016).
Wei, X. et al. Prediction of tumor recurrence by distinct immunoprofiles in liver transplant patients based on mass cytometry. Am. J. Cancer Res. 12, 4160–4176 (2022).
Zhang, G., Duan, B. & Li, G. mTORi-based immunosuppression reduces HCC recurrence at the expense of increased adverse side effects: a systematic review and meta-analysis. Clin. Transpl. 36, e14823 (2022).
Wang, R. et al. Rapamycin inhibits the secretory phenotype of senescent cells by a Nrf2-independent mechanism. Aging Cell 16, 564–574 (2017).
Geissler, E. K. et al. Sirolimus use in liver transplant recipients with hepatocellular carcinoma: a randomized, multicenter, open-label phase 3 trial. Transplantation 100, 116–125 (2016).
Rimassa, L. et al. Five-year overall survival update from the HIMALAYA study of tremelimumab plus durvalumab in unresectable HCC. J. Hepatol. 83, 899–908 (2025).
Sangro, B. et al. Durvalumab with or without bevacizumab with transarterial chemoembolisation in hepatocellular carcinoma (EMERALD-1): a multiregional, randomised, double-blind, placebo-controlled, phase 3 study. Lancet 405, 216–232 (2025).
Rizvi, N. A. et al. Cancer immunology. Mutational landscape determines sensitivity to PD-1 blockade in non-small cell lung cancer. Science 348, 124–128 (2015).
Llovet, J. M. et al. Immunotherapies for hepatocellular carcinoma. Nat. Rev. Clin. Oncol. 19, 151–172 (2022).
Steffin, D. et al. Interleukin-15-armoured GPC3 CAR T cells for patients with solid cancers. Nature 637, 940–946 (2025).
Fu, Q. et al. RUNX-3-expressing CAR T cells targeting glypican-3 in patients with heavily pretreated advanced hepatocellular carcinoma: a phase I trial. EClinicalMedicine 63, 102175 (2023).
Yarchoan, M. et al. Personalized neoantigen vaccine and pembrolizumab in advanced hepatocellular carcinoma: a phase 1/2 trial. Nat. Med. 30, 1044–1053 (2024).
Yarchoan, M., Johnson, B. A., Lutz, E. R., Laheru, D. A. & Jaffee, E. M. Targeting neoantigens to augment antitumour immunity. Nat. Rev. Cancer 17, 209–222 (2017).
Sethna, Z. et al. RNA neoantigen vaccines prime long-lived CD8+ T cells in pancreatic cancer. Nature 639, 1042–1051 (2025).
Dudek, M. et al. Auto-aggressive CXCR6+ CD8 T cells cause liver immune pathology in NASH. Nature 592, 444–449 (2021).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/study/NCT03847428 (2025).
Jimenez Exposito, M. J. et al. CA209-9DX: phase III, randomized, double-blind study of adjuvant nivolumab vs placebo for patients with hepatocellular carcinoma (HCC) at high risk of recurrence after curative resection or ablation. Ann. Oncol. 29, ix65 (2018).
Kaseb, A. O. et al. Perioperative nivolumab monotherapy versus nivolumab plus ipilimumab in resectable hepatocellular carcinoma: a randomised, open-label, phase 2 trial. Lancet Gastroenterol. Hepatol. 7, 208–218 (2022).
Marron, T. U. et al. Neoadjuvant cemiplimab for resectable hepatocellular carcinoma: a single-arm, open-label, phase 2 trial. Lancet Gastroenterol. Hepatol. 7, 219–229 (2022).
Nakazawa, M. et al. Impact of neoadjuvant immunotherapy on recurrence-free survival in patients with high-risk localized HCC. Cancer Res. Commun. 4, 2123–2132 (2024).
D’Alessio, A. et al. Preliminary results from a phase Ib study of neoadjuvant ipilimumab plus nivolumab prior to liver resection for hepatocellular carcinoma: the PRIME-HCC trial. J. Clin. Oncol. 40, 4093 (2022).
Pinato, D. J. et al. PRIME-HCC: phase Ib study of neoadjuvant ipilimumab and nivolumab prior to liver resection for hepatocellular carcinoma. BMC Cancer 21, 301 (2021).
Nordness, M. F. et al. Fatal hepatic necrosis after nivolumab as a bridge to liver transplant for HCC: are checkpoint inhibitors safe for the pretransplant patient? Am. J. Transpl. 20, 879–883 (2020).
Tai, D. et al. Radioembolisation with Y90-resin microspheres followed by nivolumab for advanced hepatocellular carcinoma (CA 209-678): a single arm, single centre, phase 2 trial. lancet. Gastroenterol. Hepatol. 6, 1025–1035 (2021).
Kudo, M. et al. Transarterial chemoembolisation combined with lenvatinib plus pembrolizumab versus dual placebo for unresectable, non-metastatic hepatocellular carcinoma (LEAP-012): a multicentre, randomised, double-blind, phase 3 study. Lancet 405, 203–215 (2025).
Highfill, S. L. et al. Disruption of CXCR2-mediated MDSC tumor trafficking enhances anti-PD1 efficacy. Sci. Transl Med. 6, 237ra67 (2014).
Thangaraj, J. L., Coffey, M., Lopez, E. & Kaufman, D. S. Disruption of TGF-β signaling pathway is required to mediate effective killing of hepatocellular carcinoma by human iPSC-derived NK cells. Cell Stem Cell 31, 1327–43.e5 (2024).
Huang, Y. et al. The hepatic senescence-associated secretory phenotype promotes hepatocarcinogenesis through Bcl3-dependent activation of macrophages. Cell Biosci. 11, 173 (2021).
Qian, G. X. et al. Computed tomography-based radiomics to predict early recurrence of hepatocellular carcinoma post-hepatectomy in patients background on cirrhosis. World J. Gastroenterol. 30, 2128–2142 (2024).
Liu, Q. et al. Radio-immunomics in hepatocellular carcinoma: unraveling the tumor immune microenvironment. Meta-Radiol. 2, 100098 (2024).
Chiang, C. L. et al. Complete response to locoregional therapy plus immunotherapy for hepatocellular carcinoma. JAMA Oncol. 10, 1548–1553 (2024).
Nault, J.-C., Calderaro, J. & Ronot, M. Integration of new technologies in the multidisciplinary approach to primary liver tumours: the next-generation tumour board. J. Hepatol. 81, 756–762 (2024).
Dhanasekaran, R., Suzuki, H., Lemaitre, L., Kubota, N. & Hoshida, Y. Molecular and immune landscape of hepatocellular carcinoma to guide therapeutic decision-making. Hepatology 81, 1038–1057 (2025).
Schlegel, A. et al. A multicenter randomized-controlled trial of hypothermic oxygenated perfusion (HOPE) for human liver grafts before transplantation. J. Hepatol. 78, 783–793 (2023).
De Luna, W. et al. Transarterial chemoinfusion for hepatocellular carcinoma as downstaging therapy and a bridge toward liver transplantation. Am. J. Transpl. 9, 1158–1168 (2009).
Renner, P. et al. Hepatocellular carcinoma progression during bridging before liver transplantation. BJS Open 5, zrab005 (2021).
Mehta, N. et al. Wait time of less than 6 and greater than 18 months predicts hepatocellular carcinoma recurrence after liver transplantation: proposing a wait time ‘sweet spot’. Transplantation 101, 2071–2078 (2017).
Chen, C. P. Role of external beam radiotherapy in hepatocellular carcinoma. Clin. Liver Dis. 24, 701–717 (2020).
Llovet, J. M. et al. Locoregional therapies in the era of molecular and immune treatments for hepatocellular carcinoma. Nat. Rev. Gastroenterol. Hepatol. 18, 293–313 (2021).
Salem, R. et al. Radioembolization for hepatocellular carcinoma using yttrium-90 microspheres: a comprehensive report of long-term outcomes. Gastroenterology 138, 52–64 (2010).
Salem, R. et al. Y90 radioembolization significantly prolongs time to progression compared with chemoembolization in patients with hepatocellular carcinoma. Gastroenterology 151, 1155–1163.e2 (2016).
Brown, A. M. et al. TACE versus TARE for patients with hepatocellular carcinoma: overall and individual patient level meta-analysis. Cancer. Medicine 12, 2590–2599 (2023).
Lewandowski, R. J. et al. A comparative analysis of transarterial downstaging for hepatocellular carcinoma: chemoembolization versus radioembolization. Am. J. Transpl. 9, 1920–1928 (2009).
Dhondt, E. et al. 90Y radioembolization versus drug-eluting bead chemoembolization for unresectable hepatocellular carcinoma: results from the TRACE phase II randomized controlled trial. Radiology 303, 699–710 (2022).
Baumgartner, R. et al. Comparing the accuracy of prediction models to detect clinically relevant post-hepatectomy liver failure early after major hepatectomy. Br. J. Surg. 111, znad433 (2024).
Olthof, P. B. et al. Postoperative liver failure risk score: identifying patients with resectable perihilar cholangiocarcinoma who can benefit from portal vein embolization. J. Am. Coll. Surg. 225, 387–394 (2017).
Reissfelder, C. et al. Postoperative course and clinical significance of biochemical blood tests following hepatic resection. Br. J. Surg. 98, 836–844 (2011).
Wang, X., Cao, J. & Li, J. Anatomic liver resection based on portal territory with margin priority for hepatocellular carcinoma. JAMA Surg. 159, 710–711 (2024).
Sun, Z. et al. Anatomic versus non-anatomic resection of hepatocellular carcinoma with microvascular invasion: a systematic review and meta-analysis. Asian J. Surg. 44, 1143–1150 (2021).
Li, S. Q. et al. Anatomical versus non-anatomical liver resection for hepatocellular carcinoma exceeding Milan criteria. Br. J. Surg. 104, 118–127 (2017).
Marubashi, S. et al. Anatomical versus non-anatomical resection for hepatocellular carcinoma. Br. J. Surg. 102, 776–784 (2015).
Zhong, X. P. et al. Anatomical versus non-anatomical resection for hepatocellular carcinoma with microscope vascular invasion: a propensity score matching analysis. J. Cancer 10, 3950–3957 (2019).
Zhao, H. et al. Anatomical versus non-anatomical resection for solitary hepatocellular carcinoma without macroscopic vascular invasion: a propensity score matching analysis. J. Gastroenterol. Hepatol. 32, 870–878 (2017).
Kirimker, E. O. et al. Comparison of anatomic and non-anatomic liver resection for hepatocellular carcinoma: a retrospective cohort study. Medicina 58, 1305 (2022).
Xu, H. et al. Laparoscopically anatomical versus non-anatomical liver resection for large hepatocellular carcinoma. HPB 22, 136–143 (2020).
Zhong, J. H. et al. Repeat hepatic resection versus radiofrequency ablation for recurrent hepatocellular carcinoma: retrospective multicentre study. Br. J. Surg. 109, 71–78 (2021).
Sato, N. & Marubashi, S. What is the optimal surgical treatment for hepatocellular carcinoma beyond the debate between anatomical versus non-anatomical resection? Surg. Today 52, 871–880 (2022).
Fischer, C. et al. Chemotherapy after portal vein embolization to protect against tumor growth during liver hypertrophy before hepatectomy. JAMA Surg. 148, 1103–1108 (2013).
Spelt, L., Sparrelid, E., Isaksson, B., Andersson, R. G. & Sturesson, C. Tumour growth after portal vein embolization with pre-procedural chemotherapy for colorectal liver metastases. HPB 17, 529–535 (2015).
Heil, J. et al. Preoperative portal vein or portal and hepatic vein embolization: DRAGON collaborative group analysis. Br. J. Surg. 108, 834–842 (2021).
Ogata, S. et al. Sequential arterial and portal vein embolizations before right hepatectomy in patients with cirrhosis and hepatocellular carcinoma. Br. J. Surg. 93, 1091–1098 (2006).
Zhang, C. W. et al. Simultaneous transcatheter arterial chemoembolization and portal vein embolization for patients with large hepatocellular carcinoma before major hepatectomy. World J. Gastroenterol. 26, 4489–4500 (2020).
Schlegel, A. et al. ALPPS: from human to mice highlighting accelerated and novel mechanisms of liver regeneration. Ann. Surg. 260, 839–846 (2014).
Sparrelid, E. & van Gulik, T. M. Tumor progression in two-stage liver resections — Is the shorter inter-stage period in associated liver partition and portal vein ligation for staged hepatectomy (ALPPS) of benefit to the patient? Hepatobiliary Surg. Nutr. 8, 316–317 (2019).
Wanis, K. N. et al. Variation in complications and mortality following ALPPS at early-adopting centers. HPB 23, 46–55 (2021).
James, S. et al. DRAGON 2 — protocol — an international multicentre randomized controlled trial comparing combined portal and hepatic vein embolization (PVE/HVE) with PVE alone. HPB 25, S289 (2023).
Acknowledgements
A.K.M. is supported by a clinical research training fellowship from the Medical Research Council (MR/Z50502X/1). The views expressed in this manuscript are solely those of the authors and do not reflect those of the Medical Research Council or affiliated institutions.
Author information
Authors and Affiliations
Contributions
A.K.M. and D.A.M. researched data for the article. All authors contributed substantially to discussion of the content. A.K.M., D.A.M. and S.A.W. wrote the article. All authors reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Gastroenterology & Hepatology thanks Phillipe Abreu, Arno Kornberg and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Malik, A.K., Geh, D., Jeffry Evans, T.R. et al. Improving surgical treatments for hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol 23, 208–226 (2026). https://doi.org/10.1038/s41575-025-01143-y
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41575-025-01143-y