Abstract
Acute kidney injury (AKI) is a common condition globally associated with substantial morbidity, mortality and costs to health-care systems. The epidemiology and outcomes of AKI differ within and between countries, and depend on multiple factors. Social determinants of health (SDoHs) are the circumstances in which people are born, grow, work, live and age, including the broader set of forces and systems that influence the conditions of everyday life. Despite advances in medical care, many inequities, including those associated with socioeconomic status, race, ethnicity, gender and environment, persist and are increasingly recognized to influence health outcomes. Superimposed on these inequities are differences in access to health care and health resources, including public health prevention, access to screening, early diagnosis and treatment (including kidney replacement therapy), and quality of care, which vary within and between high- and low-resource settings. Over the past few years, these disparities have intensified as societies have emerged from a global pandemic and are challenged with accelerating climate change and escalating levels of global conflict. However, the role of SDoHs remains poorly defined for people with or at risk of AKI. Targeted policies addressing SDoHs are essential to reduce AKI burden globally. Here, we examine the effects of SDoHs on the incidence, recognition, management, follow-up and outcomes of adult and paediatric populations at risk of or with AKI.
Key points
-
Social determinants of health influence acute kidney injury (AKI) incidence, management and outcomes substantially. Consequently, factors such as economic deprivation, education gaps and health-care access barriers drive AKI disparities globally.
-
Environmental exposures, climate change and conflict exacerbate AKI risks, especially in low-resource settings, where increased risks are typically also accompanied by limitations in health-care provision.
-
Paediatric and adolescent populations face unique AKI vulnerabilities owing to systemic inequities, with gaps in research exacerbating the ability to implement adequate interventions and improve patient outcomes.
-
Addressing social determinants of health aligns with Sustainable Development Goals and is essential for reducing AKI incidence globally, achieving equitable AKI care and reducing its long-term health implications, which include adverse effects at individual and societal levels.
-
Interdisciplinary strategies, education and policy reforms that are tailored to local needs and resources, as well as being integrated into current efforts to address non-communicable diseases, are needed to reduce AKI burden worldwide.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Susantitaphong, P. et al. World incidence of AKI: a meta-analysis. Clin. J. Am. Soc. Nephrol. 8, 1482–1493 (2013).
Hoste, E. A. J. et al. Global epidemiology and outcomes of acute kidney injury. Nat. Rev. Nephrol. 14, 607–625 (2018).
Mena, J. et al. Incidence, recognition, and follow-up of laboratory evidence of acute kidney injury in primary care practices: analysis of 93,259 creatinine results. Am. J. Med. 138, 79–86 (2025).
Holmes, J. et al. Community acquired acute kidney injury: findings from a large population cohort. QJM 110, 741–746 (2017).
Hsu, C. N. et al. Incidence, outcomes, and risk factors of community-acquired and hospital-acquired acute kidney injury: a retrospective cohort study. Medicine 95, e3674 (2016).
Macedo, E. et al. Recognition and management of community-acquired acute kidney injury in low-resource settings in the ISN 0by25 trial: a multi-country feasibility study. PLoS Med. 18, e1003408 (2021).
Pande, C. K. et al. Neurodevelopmental outcomes in infants with cardiac surgery associated acute kidney injury. Ann. Thorac. Surg. 114, 2347–2354 (2022).
McNicholas, B., Akcan Arikan, A. & Ostermann, M. Quality of life after acute kidney injury. Curr. Opin. Crit. Care 29, 566–579 (2023).
Grant, C. H. et al. Health inequalities and outcomes following acute kidney injury: a systematic review & meta-analyses of observational studies. BMC Nephrol. 26, 494 (2025).
Ghazi, L. et al. Association of neighborhood social determinants of health with acute kidney injury during hospitalization. Clin. J. Am. Soc. Nephrol. 19, 1371–1381 (2024).
World Health Organization. Social determinants of health. who.int https://www.who.int/news-room/fact-sheets/detail/social-determinants-of-health (2025).
Hacker, K., Auerbach, J., Ikeda, R., Philip, C. & Houry, D. Social determinants of health — an approach taken at CDC. J. Public. Health Manag. Pract. 28, 589–594 (2022).
Centers for Disease Control & Prevention. Why is addressing social determinants of health important? cdc.gov https://www.cdc.gov/about/priorities/why-is-addressing-sdoh-important.html (2024).
Meena, J., Mathew, G., Kumar, J. & Chanchlani, R. Incidence of acute kidney injury in hospitalized children: a meta-analysis. Pediatrics 151, e2022058823 (2023).
Wainstein, M. et al. Association of country income level with the characteristics and outcomes of critically ill patients hospitalized with acute kidney injury and COVID-19. Kidney Int. Rep. 8, 1514–1530 (2023).
Mehta, R. L. et al. International Society of Nephrology’s 0by25 initiative for acute kidney injury (zero preventable deaths by 2025): a human rights case for nephrology. Lancet 385, 2616–2643 (2015).
Bello, A. K. et al. Assessment of global kidney health care status. JAMA 317, 1864–1881 (2017).
Crews, D. C., Bello, A. K. & Saadi, G. Burden, access, and disparities in kidney disease. Kidney Dis. 5, 126–133 (2019).
Cerda, J. et al. Acute kidney injury recognition in low- and middle-income countries. Kidney Int. Rep. 2, 530–543 (2017).
Grams, M. E. et al. Explaining the racial difference in AKI incidence. J. Am. Soc. Nephrol. 25, 1834–1841 (2014).
Vart, P., Gansevoort, R. T., Crews, D. C., Reijneveld, S. A. & Bultmann, U. Mediators of the association between low socioeconomic status and chronic kidney disease in the United States. Am. J. Epidemiol. 181, 385–396 (2015).
Ashruf, O. S. et al. Sociodemographic disparities in 1-year outcomes of children with community-acquired acute kidney injury. JAMA Netw. Open. 7, e2440988 (2024).
Shiao, C.-C. et al. Association between regional economic status and renal recovery of dialysis-requiring acute kidney injury among critically ill patients. Sci. Rep. 10, 14573 (2020).
Holmes, J. et al. Acute kidney injury, age, and socioeconomic deprivation: evaluation of a national data set. Kidney Int. Rep. 4, 824–832 (2019).
Hounkpatin, H. O. et al. The association of socioeconomic status with incidence and outcomes of acute kidney injury. Clin. Kidney J. 13, 245–252 (2020).
Peracha, J. et al. Centre variation in mortality following post-hospitalization acute kidney injury: analysis of a large national cohort. Nephrol. Dial. Transpl. 37, 2201–2213 (2022).
Sawhney, S. et al. Care processes and outcomes of deprivation across the clinical course of kidney disease: findings from a high-income country with universal healthcare. Nephrol. Dial. Transplant. 38, 1170–1182 (2022).
Sawhney, S. et al. Individual and neighborhood-level social and deprivation factors impact kidney health in the GLOMMS-CORE study. Kidney Int. 106, 928–942 (2024).
Starr, M. C., Fisher, K., Thompson, K., Thurber-Smith, K. & Hingorani, S. A pilot investigation of food insecurity among children seen in an outpatient pediatric nephrology clinic. Prev. Med. Rep. 10, 113–116 (2018).
Starr, M. C. et al. Association of food insecurity and short-term kidney outcomes in neonates. Am. J. Perinatol. 43, 425–429 (2025).
Xiang, X., Zhu, X. & Zhang, L. Association of malnutrition with risk of acute kidney injury: a systematic review and meta-analysis. Int. J. Clin. Pract. 2023, 9910718 (2023).
Arques, S. Human serum albumin in cardiovascular diseases. Eur. J. Intern. Med. 52, 8–12 (2018).
Yu, M. Y. et al. Hypoalbuminemia at admission predicts the development of acute kidney injury in hospitalized patients: a retrospective cohort study. PLoS ONE 12, e0180750 (2017).
Borrelli, S. et al. Sodium intake and chronic kidney disease. Int. J. Mol. Sci. 21, 4744 (2020).
Fernald, L. C., Gertler, P. J. & Hou, X. Cash component of conditional cash transfer program is associated with higher body mass index and blood pressure in adults. J. Nutr. 138, 2250–2257 (2008).
Vervaet, B. A., D’Haese, P. C. & Verhulst, A. Environmental toxin-induced acute kidney injury. Clin. Kidney J. 10, 747–758 (2017).
Wesseling, C. et al. Resolving the enigma of the Mesoamerican nephropathy: a research workshop summary. Am. J. Kidney Dis. 63, 396–404 (2014).
Xue, B. et al. Indoor solid fuel use and renal function among middle-aged and older adults: a national study in rural China. Env. Res. 206, 112588 (2022).
Artazcoz, L., Borrell, C., Cortes, I., Escriba-Aguir, V. & Cascant, L. Occupational epidemiology and work related inequalities in health: a gender perspective for two complementary approaches to work and health research. J. Epidemiol. Community Health 61, ii39–ii45 (2007).
Luyckx, V. A. & Naicker, S. Acute kidney injury associated with the use of traditional medicines. Nat. Clin. Pract. Nephrol. 4, 664–671 (2008).
Hajat, S. et al. Ambient heat and acute kidney injury: case-crossover analysis of 1 354 675 automated e-alert episodes linked to high-resolution climate data. Lancet Planet. Health 8, e156–e162 (2024).
Qu, Y. et al. Associations between ambient extreme heat exposure and emergency department visits related to kidney disease. Am. J. Kidney Dis. 81, 507–516.e1 (2023).
Rao, I. R. et al. Chronic kidney disease of unknown aetiology: a comprehensive review of a global public health problem. Trop. Med. Int. Health 28, 588–600 (2023).
Mora, C. et al. Over half of known human pathogenic diseases can be aggravated by climate change. Nat. Clim. Chang. 12, 869–875 (2022).
Goldfarb, D. S. & Patel, A. A. Climate change and its implications for kidney health. Curr. Opin. Urol. 34, 377–383 (2024).
Williams, A. E. & Diamantidis, C. J. Social determinants of health in acute kidney injury: looking beyond the hospital room. Clin. J. Am. Soc. Nephrol. 19, 1359–1361 (2024).
Guthrie, G. D. & Bell, S. Deprivation and kidney disease — a predictor of poor outcomes. Clin. Kidney J. 13, 128–132 (2020).
Kwong, Y. D. & Kao, P. F. Acute kidney injury provider and survivor education: current and emerging tools. Adv. Kidney Dis. Health 32, 144–153 (2025).
Mottes, T. et al. Pediatric AKI in the real world: changing outcomes through education and advocacy — a report from the 26th Acute Disease Quality Initiative (ADQI) consensus conference. Pediatr. Nephrol. 39, 1005–1014 (2024).
Norton, J. M. et al. Social determinants of racial disparities in CKD. J. Am. Soc. Nephrol. 27, 2576–2595 (2016).
Crews, D. C. et al. Low income, community poverty and risk of end stage renal disease. BMC Nephrol. 15, 192 (2014).
Hassan, M. O. & Balogun, R. A. The effects of race on acute kidney injury. J. Clin. Med. 11, 5822 (2022).
Muiru, A. N. et al. Black and white adults with CKD hospitalized with acute kidney injury: findings from the Chronic Renal Insufficiency Cohort (CRIC) Study. Am. J. Kidney Dis. 80, 610–618.e1 (2022).
Norris, K. & Nissenson, A. Racial disparities in chronic kidney disease: tragedy, opportunity, or both? Clin. J. Am. Soc. Nephrol. 3, 314–316 (2008).
Johansen, K. L. et al. US renal data system 2023 annual data report: epidemiology of kidney disease in the United States. Am. J. Kidney Dis. 83, A8–A13 (2024).
Inker, L. A. et al. New creatinine- and cystatin C-based equations to estimate GFR without race. N. Engl. J. Med. 385, 1737–1749 (2021).
Delgado, C. et al. A unifying approach for GFR estimation: recommendations of the NKF-ASN task force on reassessing the inclusion of race in diagnosing kidney disease. Am. J. Kidney Dis. 79, 268–288.e1 (2022).
Pandey, M. et al. Impacts of English language proficiency on healthcare access, use, and outcomes among immigrants: a qualitative study. BMC Health Serv. Res. 21, 741 (2021).
Elmer, E. M., van Tilburg, T. G. & Fokkema, T. Age and gender identity in the relationship between minority stress and loneliness: a global sample of sexual and gender minority adults. J. Sex. Res. 62, 1080–1099 (2024).
Heidari, S., Babor, T. F., De Castro, P., Tort, S. & Curno, M. Sex and gender equity in research: rationale for the SAGER guidelines and recommended use. Res. Integr. Peer Rev. 1, 2 (2016).
Lumlertgul, N. et al. Sex and gender considerations in randomized controlled trials in critical care nephrology: a meta-epidemiologic study. BMC Med. 23, 386 (2025).
Curtis, L. M. Sex and gender differences in AKI. Kidney360 5, 160–167 (2024).
Dahiya, A., Pannu, N. & Soranno, D. E. Sex as a biological variable in acute kidney injury. Curr. Opin. Crit. Care 29, 529–533 (2023).
Starr, M. C. et al. Advances in pediatric acute kidney injury pathobiology: a report from the 26th Acute Disease Quality Initiative (ADQI) conference. Pediatr. Nephrol. 39, 941–953 (2023).
Neugarten, J. & Golestaneh, L. Female sex reduces the risk of hospital-associated acute kidney injury: a meta-analysis. BMC Nephrol. 19, 314 (2018).
Mehta, R. H. et al. Association of gender and lowest hematocrit on cardiopulmonary bypass with acute kidney injury and operative mortality in patients undergoing cardiac surgery. Ann. Thorac. Surg. 96, 133–140 (2013).
Thakar, C. V. et al. ARF after open-heart surgery: influence of gender and race. Am. J. Kidney Dis. 41, 742–751 (2003).
Moore, R. D., Smith, C. R., Lipsky, J. J., Mellits, E. D. & Lietman, P. S. Risk factors for nephrotoxicity in patients treated with aminoglycosides. Ann. Intern. Med. 100, 352–357 (1984).
Soranno, D. E. et al. The role of sex and gender in acute kidney injury-consensus statements from the 33rd acute disease quality initiative. Kidney Int. 107, 606–616 (2025).
Katz-Greenberg, G. & Shah, S. Sex and gender differences in kidney transplantation. Semin. Nephrol. 42, 219–229 (2022).
Daher, M. et al. Gender disparities in difficulty accessing healthcare and cost-related medication non-adherence: the CDC behavioral risk factor surveillance system (BRFSS) survey. Prev. Med. 153, 106779 (2021).
Eckenrode, H. E., Gutierrez, O. M., Osis, G., Agarwal, A. & Curtis, L. M. Kidney disease prevalence in transgender individuals. Clin. J. Am. Soc. Nephrol. 17, 280–282 (2022).
Coleman, E. et al. Standards of care for the health of transgender and gender diverse people, version 8. Int. J. Transgend. Health 23, S1–S259 (2022).
Collister, D., Saad, N., Christie, E. & Ahmed, S. Providing care for transgender persons with kidney disease: a narrative review. Can. J. Kidney Health Dis. 8, 2054358120985379 (2021).
Tienforti, D. et al. Effects of gender affirming hormone therapy with testosterone on renal function of assigned female at birth transgender people: a meta-analysis. Front. Endocrinol. 16, 1537838 (2025).
Remillard, B. D., Buteau, J. H. & Cléophat, P. Kidney care in Haiti — the role of partnerships. Nat. Rev. Nephrol. 11, 183–188 (2015).
GBD Chronic Kidney Disease Collaboration Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 395, 709–733 (2020).
Sever, M. S., Vanholder, R. & Lameire, N. Acute kidney injury in active wars and other man-made disasters. Semin. Nephrol. 40, 341–353 (2020).
Barbara, P. G. & Gaetano, M. The disasters of war. On kidney patients in the Ukrainian-Russian war. J. Nephrol. 35, 375–376 (2022).
Gorbatkin, C., Finkelstein, F. O. & Kazancioglu, R. T. Peritoneal dialysis during active war. Semin. Nephrol. 40, 375–385 (2020).
Sever, L. & Balat, A. Renal crisis in children during armed conflict. Semin. Nephrol. 40, 408–420 (2020).
Karam, S. et al. Capacity for the management of kidney failure in the International Society of Nephrology Middle East region: report from the 2023 ISN Global Kidney Health Atlas (ISN-GKHA). Kidney Int. Suppl. 13, 57–70 (2024).
Kahramanlar, D. et al. Acute kidney injury in pediatric burn patients. Pediatr. Nephrol. 39, 2515–2524 (2024).
Parkes, P. et al. Telemedicine interventions in six conflict-affected countries in the WHO Eastern Mediterranean region: a systematic review. Confl. Health 16, 64 (2022).
Ossai, N. -o, Hour, B. T. & Szerlip, H. M. Border-Crossers’ nephropathy: the risk of coming to America. Ren. Fail. 35, 483–486 (2013).
Vanholder, R. et al. Inequities in kidney health and kidney care. Nat. Rev. Nephrol. 19, 694–708 (2023).
Anandh, U., Meena, P., Karam, S. & Luyckx, V. Social, political and legal determinants of kidney health: Perspectives from lower- and middle-income countries with a focus on India. Front. Nephrol. 2, 1024667 (2022).
Singh, P. et al. From resolution to reality: advancing point-of-care diagnostics for kidney disease in low-resource settings. Nat. Rev. Nephrol. 22, 1–2 (2026).
Evans, R. D. R. et al. Management of acute kidney disease as part of routine clinical care in low-resource settings: the International Society of Nephrology Kidney Care Network Project. PLoS ONE 20, e0315802 (2025).
Htay, H. et al. Global access of patients with kidney disease to health technologies and medications: findings from the Global Kidney Health Atlas project. Kidney Int. Suppl. 8, 64–73 (2018).
Jones, E. et al. Survey on available treatment for acute kidney injury in the Southern African Development Community and Nigeria: are we ready for zero deaths by 2025 in sub-Saharan Africa? BMJ Open 9, e029001 (2019).
Lunyera, J., Kilonzo, K., Lewington, A., Yeates, K. & Finkelstein, F. O. Acute kidney injury in low-resource settings: barriers to diagnosis, awareness, and treatment and strategies to overcome these barriers. Am. J. Kidney Dis. 67, 834–840 (2016).
Evans, R., Rudd, P., Hemmila, U., Dobbie, H. & Dreyer, G. Deficiencies in education and experience in the management of acute kidney injury among Malawian healthcare workers. Malawi Med. J. 27, 101–103 (2015).
Gardiner, F. W. et al. Poor access to kidney disease management services in susceptible patient populations in rural Australia is associated with increased aeromedical retrievals for acute renal care. Intern. Med. J. 50, 951–959 (2020).
Francis, A. et al. Barriers to accessing essential medicines for kidney disease in low- and lower middle-income countries. Kidney Int. 102, 969–973 (2022).
Baelani, I. et al. Identifying resource needs for sepsis care and guideline implementation in the Democratic Republic of the Congo: a cluster survey of 66 hospitals in four eastern provinces. Middle East. J. Anaesthesiol. 21, 559–575 (2012).
Olowu, W. A. et al. Outcomes of acute kidney injury in children and adults in sub-Saharan Africa: a systematic review. Lancet Glob. Health 4, e242–e250 (2016).
Okpechi, I. G. et al. Progress of nations in the organisation of, and structures for, kidney care delivery between 2019 and 2023: cross sectional survey in 148 countries. BMJ 387, e079937 (2024).
Nkunu, V. et al. Landscape of kidney replacement therapy provision in low- and lower-middle income countries: a multinational study from the ISN-GKHA. PLoS Glob. Public. Health 4, e0003979 (2024).
Lumlertgul, N. et al. In-house production of dialysis solutions to overcome challenges during the coronavirus disease 2019 pandemic. Kidney Int. Rep. 6, 200–206 (2021).
The Division of Nephrology, Columbia University Vagelos College of Physicians Working Group. Disaster response to the COVID-19 pandemic for patients with kidney disease in New York city. J. Am. Soc. Nephrol. 31, 1371–1379 (2020).
Cullis, B., McCulloch, M. & Finkelstein, F. O. Development of PD in lower-income countries: a rational solution for the management of AKI and ESKD. Kidney Int. 105, 953–959 (2024).
Luyckx, V. A., Miljeteig, I., Ejigu, A. M. & Moosa, M. R. Ethical challenges in the provision of dialysis in resource-constrained environments. Semin. Nephrol. 37, 273–286 (2017).
Teerawattananon, Y. et al. The access to dialysis in low- and middle-income countries commission: lessons for universal health coverage. Nat. Med. 31, 19–21 (2025).
Reid, E. et al. Out-of-pocket costs near end of life in low- and middle-income countries: a systematic review. PLoS Glob. Public. Health 2, e0000005 (2022).
Sengthavisouk, N. et al. Epidemiology and short-term outcomes of acute kidney injury among patients in the intensive care unit in Laos: a nationwide multicenter, prospective, and observational study. BMC Med. 18, 180 (2020).
Kusirisin, P., Peerapornratana, S., Sutawong, J., Teerawattananon, Y. & Srisawat, N. Lesson learnt from implementing a CRRT reimbursement program in a resource-limited setting. J. Crit. Care 88, 155089 (2025).
McCulloch, M. et al. Challenges of access to kidney care for children in low-resource settings. Nat. Rev. Nephrol. 17, 33–45 (2021).
Moist, L. M. et al. Travel time to dialysis as a predictor of health-related quality of life, adherence, and mortality: the Dialysis Outcomes and Practice Patterns Study (DOPPS). Am. J. Kidney Dis. 51, 641–650 (2008).
Razon, N. et al. Transportation insecurity and outcomes in hemodialysis patients: a retrospective cohort study. Clin. J. Am. Soc. Nephrol. 20, 1111–1118 (2025).
Côté, J. M., Beaubien-Souligny, W., Hamel, L. & Bouchard, J. Primary care providers barriers, comfort and awareness in follow-up care of acute kidney injury patients: a comprehensive survey on current practices. Can. J. Kidney Health Dis. 11, 20543581241304517 (2024).
Okpechi, I. G. et al. A global assessment of kidney care workforce. Nephrol. Dial. Transpl. 39, ii43–ii48 (2024).
Silver, S. A. et al. Association of an acute kidney injury follow-up clinic with patient outcomes and care processes: a cohort study. Am. J. Kidney Dis. 81, 554–563.e1 (2023).
Blakeman, T., Harding, S. & O’Donoghue, D. Acute kidney injury in the community: why primary care has an important role. Br. J. Gen. Pract. 63, 173–174 (2013).
Abdelhamid, Y. M. et al. Medical care of acute kidney injury in limited resource settings: a call to action. Kidney Int. 107, 959–962 (2025).
Tu, Y. et al. Inequality in infrastructure access and its association with health disparities. Nat. Hum. Behav. 9, 1669–1682 (2025).
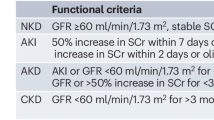
Lameire, N. H. et al. Harmonizing acute and chronic kidney disease definition and classification: report of a kidney disease: improving global outcomes (KDIGO) consensus conference. Kidney Int. 100, 516–526 (2021).
Gaspar, A., Iturricha-Cáceres, M. F., Macedo, E., Mehta, R. L. & Claure-Del Granado, R. The use of a medical application improves the diagnosis of acute kidney injury: a pre-post study. Front. Med. 9, 817387 (2022).
Singh, G. et al. Post-Discharge mortality and rehospitalization among participants in a comprehensive acute kidney injury rehabilitation program. Kidney360 2, 1424–1433 (2021).
Esezobor, C. I. et al. Paediatric nephrology in Africa. Curr. Pediatr. Rep. 9, 134–141 (2021).
Che, R., Quadri, M. M. & Zhang, A. The epidemiology and management of pediatric AKI in Asia. Semin. Nephrol. 40, 516–532 (2020).
Raina, R., Chakraborty, R., Tibrewal, A., Sethi, S. K. & Bunchman, T. Advances in pediatric acute kidney injury. Pediatr. Res. 91, 44–55 (2022).
Banerjee, S., Kamath, N., Antwi, S. & Bonilla-Felix, M. Paediatric nephrology in under-resourced areas. Pediatr. Nephrol. 37, 959–972 (2022).
Dessalegn, N. et al. Acute kidney injury magnitude, mortality, and associated factors among neonates in sub-Saharan Africa: a systematic review and meta-analysis. Pediatr. Nephrol. 40, 3067–3076 (2025).
Jetton, J. G. et al. Incidence and outcomes of neonatal acute kidney injury (AWAKEN): a multicentre, multinational, observational cohort study. Lancet Child. Adolesc. Health 1, 184–194 (2017).
Davidson, B., Okpechi, I., McCulloch, M. & Wearne, N. Adolescent nephrology: an emerging frontier for kidney care in sub-Saharan Africa. Nephrology 22, 933–939 (2017).
Ranchin, B. et al. Technical requirements and devices available for long-term hemodialysis in children-mind the gap! Pediatr. Nephrol. 39, 2579–2591 (2024).
Smoyer, W. E. et al. “Saving Young Lives” with acute kidney injury: the challenge of acute dialysis in low-resource settings. Kidney Int. 89, 254–256 (2016).
McCulloch, M. I. et al. Lessons learned from regional training of paediatric nephrology fellows in Africa. Pediatr. Nephrol. 38, 3757–3768 (2023).
Morton, S., Pencheon, D. & Squires, N. Sustainable Development Goals (SDGs), and their implementation: a national global framework for health, development and equity needs a systems approach at every level. Br. Med. Bull. 124, 81–90 (2017).
Karam, S., Wong, M. M. Y. & Jha, V. Sustainable development goals: challenges and the role of the international society of nephrology in improving global kidney health. Kidney360 4, 1494–1502 (2023).
Luyckx, V. A. et al. Sustainable development goals relevant to kidney health: an update on progress. Nat. Rev. Nephrol. 17, 15–32 (2021).
Agency for toxic substances and disease registry. Social Vulnerability Index | Place and Health - Geospatial Research, Analysis, and Services Program (GRASP). cdc.gov https://www.atsdr.cdc.gov/place-health/php/svi/index.html (2024).
Ganjkhanloo, F. et al. Evolving patterns of COVID-19 mortality in US counties: a longitudinal study of healthcare, socioeconomic, and vaccination associations. PLoS Glob. Public. Health 4, e0003590 (2024).
The World Bank. Poverty & Inequality Platform. worldbank.org https://pip.worldbank.org/home (2022).
Haddad, C. N. et al. The World Bank’s New Inequality Indicator: The Number of Countries with High Inequality (World Bank Group, 2024).
Zhang, Y. et al. Social isolation, loneliness, and the risk of incident acute kidney injury in middle-aged and older adults: a prospective cohort study. J. Psychosom. Res. 177, 111587 (2024).
Chen, Y. C. et al. The roles of social support and health literacy in self-management among patients with chronic kidney disease. J. Nurs. Scholarsh. 50, 265–275 (2018).
Wang, C., Lang, J., Xuan, L., Li, X. & Zhang, L. The effect of health literacy and self-management efficacy on the health-related quality of life of hypertensive patients in a western rural area of China: a cross-sectional study. Int. J. Equity Health 16, 58 (2017).
Riski, M., Puspitasari, I. M., Rahayu, C. & Alfian, S. D. Factors associated with self-care behavior in patients with chronic kidney disease: a systematic review. BMC Nephrol. 26, 210 (2025).
May, H. P. et al. Posthospital multidisciplinary care for AKI survivors: a feasibility pilot. Kidney Med. 5, 100734 (2023).
Krissberg, J., Fishbein, J. & Verghese, P. Screening of social determinants of health in pediatric nephrology clinic: a pilot program. Pediatr. Nephrol. 40, 1121–1122 (2025).
Mokiao, R. & Hingorani, S. Food insecurity and kidney disease: symptoms of structural racism. Clin. J. Am. Soc. Nephrol. 16, 1903–1905 (2021).
Silver, S. A. et al. Ambulatory care after acute kidney injury: an opportunity to improve patient outcomes. Can. J. Kidney Health Dis. 2, 36 (2015).
Silver, S. A. et al. Strategies to enhance rehabilitation after acute kidney injury in the developing world. Kidney Int. Rep. 2, 579–593 (2017).
Lean, K., Nawaz, R. F., Jawad, S. & Vincent, C. Reducing urinary tract infections in care homes by improving hydration. BMJ Open Qual. 8, e000563 (2019).
Macedo, E. et al. Recognition and management of acute kidney injury in children: the ISN 0by25 Global Snapshot study. PLoS ONE 13, e0196586 (2018).
Kirwan, C. J. et al. A nurse-led intervention improves detection and management of AKI in Malawi. J. Ren. Care 42, 196–204 (2016).
Levy, H. & Janke, A. Health literacy and access to care. J. Health Commun. 21 (Suppl. 1), 43–50 (2016).
Liu, K. D. et al. AKI!Now initiative: recommendations for awareness, recognition, and management of AKI. Clin. J. Am. Soc. Nephrol. 15, 1838–1847 (2020).
Lombardi, R. et al. Raising awareness of acute kidney injury: a Latin American experience. Kidney Int. Rep. 3, 1416–1423 (2018).
Cerdá, J. & Freshly, B. L. AKI!Now: from recognition to recovery. Clin. J. Am. Soc. Nephrol. 12, 15–17 (2020).
International Society of Nephrology. Education Resources. theisn.org https://www.theisn.org/in-action/education/ (2025).
UK Kidney Association. Acute Kidney Injury: The Essentials. ukkidney.org https://education.ukkidney.org/course/aki-1 (2025).
Li, J. et al. Health poverty reduction policies and effectiveness evaluation in China since 2015: a narrative review. Inquiry 62, 469580251337232 (2025).
Jang, S. M. et al. NSAID-avoidance education in community pharmacies for patients at high risk for acute kidney injury, upstate New York, 2011. Prev. Chronic Dis. 11, E220 (2014).
Borges do Nascimento, I. J. et al. Transforming women’s health, empowerment, and gender equality with digital health: evidence-based policy and practice. Lancet Digit. Health 7, 100858 (2025).
Praveen, D. et al. SMARTHealth India: development and field evaluation of a mobile clinical decision support system for cardiovascular diseases in Rural India. JMIR Mhealth Uhealth 2, e54 (2014).
Barraclough, K. A., Blashki, G. A., Holt, S. G. & Agar, J. W. M. Climate change and kidney disease-threats and opportunities. Kidney Int. 92, 526–530 (2017).
Meena, P. & Jha, V. Environmental change, changing biodiversity, and infections-lessons for kidney health community. Kidney Int. Rep. 8, 1714–1729 (2023).
Agar, J. W. Green dialysis: the environmental challenges ahead. Semin. Dial. 28, 186–192 (2015).
Luyckx, V. A., Tonelli, M. & Stanifer, J. W. The global burden of kidney disease and the sustainable development goals. Bull. World Health Organ. 96, 414–422D (2018).
Author information
Authors and Affiliations
Consortia
Contributions
All authors researched data for the article, made substantial contributions to discussions of the content and wrote, reviewed or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
S.B. has received consultancy fees from AstraZeneca, GSK, Novo Nordisk and Stada UK unrelated to this work. M.O. received research funding from Baxter and BioMérieux (paid to their institution). The other authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Nephrology thanks Anthony Batte and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
Centre for Community-Driven Response: https://www.cc-dr.org/
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bell, S., Claure-Del Granado, R., Lumlertgul, N. et al. The impact of social determinants of health on acute kidney injury. Nat Rev Nephrol (2026). https://doi.org/10.1038/s41581-026-01063-3
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41581-026-01063-3