Abstract
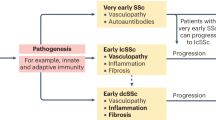
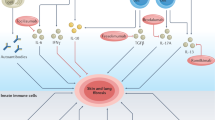
Systemic sclerosis (SSc) is an autoimmune disease in which fibrotic, vascular, autoimmune and fibrotic mechanisms synergize to promote disease progression. SSc is associated with high morbidity and mortality, primarily owing to fibrotic tissue remodelling and subsequent organ failure. Despite progress with the approval of novel therapies, mortality remains high; approximately half of the people diagnosed with SSc will succumb to disease. This statistic highlights the considerable need for novel, effective therapies. Indeed, SSc has become a disease with very active drug development. Numerous drugs with different modes of actions are currently evaluated in or are about to enter clinical trials in SSc. These clinical trials provide hope for effectively slowing or even halting the progression of fibrosis and thereby further improving outcomes for patients with SSc.
Key points
-
Currently available drugs for systemic sclerosis (SSc) might slow down disease progression, but do not halt it, generating a great medical need for novel, more effective therapies.
-
These drug candidates have a broad-spectrum of distinct anti-inflammatory and/or anti-fibrotic modes of action relevant to the pathogenesis of SSc.
-
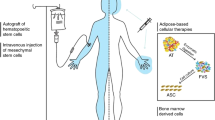
A large number of drug candidates and cellular therapies with different molecular modes of actions are currently under investigation or about to enter clinical trials in SSc.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Distler, J. H. W. et al. Shared and distinct mechanisms of fibrosis. Nat. Rev. Rheumatol. 15, 705–730 (2019).
Tyndall, A. J. et al. Causes and risk factors for death in systemic sclerosis: a study from the EULAR scleroderma trials and research (EUSTAR) database. Ann. Rheum. Dis. 69, 1809–1815 (2010).
Pope, J. E. et al. State-of-the-art evidence in the treatment of systemic sclerosis. Nat. Rev. Rheumatol. 19, 212–226 (2023).
Horn, A. et al. Inhibition of hedgehog signalling prevents experimental fibrosis and induces regression of established fibrosis. Ann. Rheum. Dis. 71, 785–789 (2012).
Lam, A. P. et al. Nuclear beta-catenin is increased in systemic sclerosis pulmonary fibrosis and promotes lung fibroblast migration and proliferation. Am. J. Respir. Cell Mol. Biol. 45, 915–922 (2011).
Horn, A. et al. Hedgehog signaling controls fibroblast activation and tissue fibrosis in systemic sclerosis. Arthritis Rheum. 64, 2724–2733 (2012).
Dees, C. et al. Notch signalling regulates fibroblast activation and collagen release in systemic sclerosis. Ann. Rheum. Dis. 70, 1304–1310 (2011).
He, W. et al. Wnt/beta-catenin signaling promotes renal interstitial fibrosis. J. Am. Soc. Nephrol. 20, 765–776 (2009).
Konigshoff, M. et al. WNT1-inducible signaling protein-1 mediates pulmonary fibrosis in mice and is upregulated in humans with idiopathic pulmonary fibrosis. J. Clin. Invest. 119, 772–787 (2009).
Guan, S. & Zhou, J. Frizzled-7 mediates TGF-β-induced pulmonary fibrosis by transmitting non-canonical Wnt signaling. Exp. Cell Res. 359, 226–234 (2017).
Saito, A. & Nagase, T. Hippo and TGF-β interplay in the lung field. Am. J. Physiol. Lung Cell Mol. Physiol. 309, L756–L767 (2015).
Burgy, O. & Konigshoff, M. The WNT signaling pathways in wound healing and fibrosis. Matrix Biol. 68–69, 67–80 (2018).
Beyer, C. & Distler, J. H. Morphogen pathways in systemic sclerosis. Curr. Rheumatol. Rep. 15, 299 (2013).
Bergmann, C. & Distler, J. H. Canonical Wnt signaling in systemic sclerosis. Lab. Invest. 96, 151–155 (2016).
Beyer, C. et al. Elevated serum levels of sonic hedgehog are associated with fibrotic and vascular manifestations in systemic sclerosis. Ann. Rheum. Dis. 77, 626–628 (2018).
Beyer, C. et al. Elevated serum levels of sonic hedgehog are associated with fibrotic and vascular manifestations in systemic sclerosis. Ann. Rheum. Dis. 77, 626–628 (2017).
Liang, R. et al. The transcription factor GLI2 as a downstream mediator of transforming growth factor-β-induced fibroblast activation in SSc. Ann. Rheum. Dis. 76, 756–764 (2017).
Hu, B. et al. Reemergence of hedgehog mediates epithelial-mesenchymal crosstalk in pulmonary fibrosis. Am. J. Respir. Cell Mol. Biol. 52, 418–428 (2015).
Ding, H. et al. Sonic hedgehog signaling mediates epithelial-mesenchymal communication and promotes renal fibrosis. J. Am. Soc. Nephrol. 23, 801–813 (2012).
El-Agroudy, N. N., El-Naga, R. N., El-Razeq, R. A. & El-Demerdash, E. Forskolin, a hedgehog signalling inhibitor, attenuates carbon tetrachloride-induced liver fibrosis in rats. Br. J. Pharmacol. 173, 3248–3260 (2016).
Dubey, A. K., Dubey, S., Handu, S. S. & Qazi, M. A. Vismodegib: the first drug approved for advanced and metastatic basal cell carcinoma. J. Postgrad. Med. 59, 48–50 (2013).
Maher, T. M. et al. American Thoracic Society International Conference. Am. J. Respir. Crit. Care Med. 209, A1056 (2024).
Song, Y. et al. Pharmacokinetics of fipaxalparant, a small-molecule selective negative allosteric modulator of lysophosphatidic acid receptor 1, and the effect of food in healthy volunteers. Clin. Pharmacol. Drug. Dev. 13, 819–827 (2024).
Tager, A. M. et al. The lysophosphatidic acid receptor LPA1 links pulmonary fibrosis to lung injury by mediating fibroblast recruitment and vascular leak. Nat. Med. 14, 45–54 (2008).
Corte, T. J. et al. Efficacy and safety of admilparant, an LPA(1) antagonist, in pulmonary fibrosis: a phase 2 randomized clinical trial. Am. J. Respir. Crit. Care Med. 211, 230–238 (2025).
Allanore, Y. et al. Lysophosphatidic acid receptor 1 antagonist SAR100842 for patients with diffuse cutaneous systemic sclerosis: a double-blind, randomized, eight-week placebo-controlled study followed by a sixteen-week open-label extension study. Arthritis Rheumatol. 70, 1634–1643 (2018).
Khanna, D. et al. A 24-week, phase IIa, randomized, double-blind, placebo-controlled study of ziritaxestat in early diffuse cutaneous systemic sclerosis. Arthritis Rheumatol. 75, 1434–1444 (2023).
Maher, T. M. et al. Ziritaxestat, a novel autotaxin inhibitor, and lung function in idiopathic pulmonary fibrosis: the ISABELA 1 and 2 randomized clinical trials. JAMA 329, 1567–1578 (2023).
Meng, X. M., Nikolic-Paterson, D. J. & Lan, H. Y. TGF-β: the master regulator of fibrosis. Nat. Rev. Nephrol. 12, 325–338 (2016).
Radaev, S. et al. Ternary complex of transforming growth factor-β1 reveals isoform-specific ligand recognition and receptor recruitment in the superfamily. J. Biol. Chem. 285, 14806–14814 (2010).
Lodyga, M. & Hinz, B. TGF-β1 — a truly transforming growth factor in fibrosis and immunity. Semin. Cell Dev. Biol. 101, 123–139 (2020).
Gyorfi, A. H., Matei, A. E. & Distler, J. H. W. Targeting TGF-β signaling for the treatment of fibrosis. Matrix Biol. 68-69, 8–27 (2018).
Denton, C. P. et al. Recombinant human anti-transforming growth factor β1 antibody therapy in systemic sclerosis: a multicenter, randomized, placebo-controlled phase I/II trial of CAT-192. Arthritis Rheum. 56, 323–333 (2007).
Rice, L. M. et al. Fresolimumab treatment decreases biomarkers and improves clinical symptoms in systemic sclerosis patients. J. Clin. Invest. 125, 2795–2807 (2015).
Mascarenhas, J. et al. A phase Ib trial of AVID200, a TGFβ 1/3 trap, in patients with myelofibrosis. Clin. Cancer Res. 29, 3622–3632 (2023).
Hoeper, M. M. et al. Phase 3 trial of sotatercept for treatment of pulmonary arterial hypertension. N. Engl. J. Med. 388, 1478–1490 (2023).
Han, L. W. et al. A phase 1a study to evaluate safety, tolerability, pharmacokinetics, and pharmacodynamics of RO7303509, an anti-TGFβ3 antibody, in healthy volunteers. Rheumatol. Ther. 11, 755–771 (2024).
Wu, L. et al. Transforming growth factor β3 (TGFβ3) accelerates wound healing without alteration of scar prominence. Histologic and competitive reverse-transcription-polymerase chain reaction studies. Arch. Surg. 132, 753–760 (1997).
Ren, H. L., Zhang, S. H. & Li, P. Y. The multifaceted role of phosphodiesterase 4 in tumor: from tumorigenesis to immunotherapy. Front. Immunol. 16, 1528932 (2025).
Aringer, M. et al. Rationale for phosphodiesterase-4 inhibition as a treatment strategy for interstitial lung diseases associated with rheumatic diseases. RMD Open. 10, e004704 (2024).
McDonough, W. et al. PAN-selective inhibition of cAMP-phosphodiesterase 4 (PDE4) induces gastroparesis in mice. FASEB J. 34, 12533–12548 (2020).
Rogliani, P., Calzetta, L., Cazzola, M. & Matera, M. G. Drug safety evaluation of roflumilast for the treatment of COPD: a meta-analysis. Expert. Opin. Drug Saf. 15, 1133–1146 (2016).
Kolb, M., Crestani, B. & Maher, T. M. Phosphodiesterase 4B inhibition: a potential novel strategy for treating pulmonary fibrosis. Eur. Respir. Rev. 32, 220206 (2023).
Herrmann, F. E., Hesslinger, C., Wollin, L. & Nickolaus, P. BI 1015550 is a PDE4B inhibitor and a clinical drug candidate for the oral treatment of idiopathic pulmonary fibrosis. Front. Pharmacol. 13, 838449 (2022).
Liu, Y. et al. Nerandomilast improves bleomycin-induced systemic sclerosis-associated interstitial lung disease in mice by regulating the TGF-β1 pathway. Inflammation 48, 1760–1774 (2025).
Richeldi, L. et al. Trial of a preferential phosphodiesterase 4B inhibitor for idiopathic pulmonary fibrosis. N. Engl. J. Med. 386, 2178–2187 (2022).
Maher, T. M. et al. Nerandomilast in patients with progressive pulmonary fibrosis. N. Engl. J. Med. 392, 2203–2214 (2025).
Khanna, D. et al. Design of CONQUEST, a novel, randomized, placebo-controlled, phase 2b platform clinical trial to investigate new treatments for patients with early active systemic sclerosis with interstitial lung disease. J. Scleroderma Relat. Disord. 23971983241278079 (2024).
Jager, B. et al. The NLRP3-inflammasome-caspase-1 pathway is upregulated in idiopathic pulmonary fibrosis and acute exacerbations and is inducible by apoptotic A549 cells. Front. Immunol. 12, 642855 (2021).
Gronberg, C. et al. Combined inhibition of IL-1, IL-33 and IL-36 signalling by targeting IL1RAP ameliorates skin and lung fibrosis in preclinical models of systemic sclerosis. Ann. Rheum. Dis. 83, 1156–1168 (2024).
Garlanda, C., Dinarello, C. A. & Mantovani, A. The interleukin-1 family: back to the future. Immunity 39, 1003–1018 (2013).
Kondo, M. et al. Dersimelagon, a novel oral melanocortin 1 receptor agonist, demonstrates disease-modifying effects in preclinical models of systemic sclerosis. Arthritis Res. Ther. 24, 210 (2022).
Wang, W., Guo, D. Y., Lin, Y. J. & Tao, Y. X. Melanocortin regulation of inflammation. Front. Endocrinol. 10, 683 (2019).
Bohm, M. & Stegemann, A. Bleomycin-induced fibrosis in MC1 signalling-deficient C57BL/6J-Mc1r(e/e) mice further supports a modulating role for melanocortins in collagen synthesis of the skin. Exp. Dermatol. 23, 431–433 (2014).
Scholzen, T. E. et al. α-melanocyte stimulating hormone prevents lipopolysaccharide-induced vasculitis by down-regulating endothelial cell adhesion molecule expression. Endocrinology 144, 360–370 (2003).
Vecsernyes, M. et al. The administration of α-melanocyte-stimulating hormone protects the ischemic/reperfused myocardium. Eur. J. Pharmacol. 470, 177–183 (2003).
US National Library of Medicine. Study to evaluate efficacy, safety, and tolerability of MT-7117 in subjects with diffuse cutaneous systemic sclerosis. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT04440592 (2020).
de Valliere, C. et al. pH-sensing G protein-coupled receptor OGR1 (GPR68) expression and activation increases in intestinal inflammation and fibrosis. Int. J. Mol. Sci. 23, 1419 (2022).
Li, J. et al. Ovarian cancer G protein coupled receptor 1 suppresses cell migration of MCF7 breast cancer cells via a Gα12/13-Rho-Rac1 pathway. J. Mol. Signal. 8, 6 (2013).
Zhang, Y. et al. FT011, a new anti-fibrotic drug, attenuates fibrosis and chronic heart failure in experimental diabetic cardiomyopathy. Eur. J. Heart Fail. 14, 549–562 (2012).
Spiera, R. et al. Efficacy and safety of lenabasum, a cannabinoid type 2 receptor agonist, in a phase 3 randomized trial in diffuse cutaneous systemic sclerosis. Arthritis Rheumatol. 75, 1608–1618 (2023).
Roh, J. S. & Sohn, D. H. Damage-associated molecular patterns in inflammatory diseases. Immune Netw. 18, e27 (2018).
Strutz, F. et al. Identification and characterization of a fibroblast marker: FSP1. J. Cell Biol. 130, 393–405 (1995).
Tomcik, M. et al. S100A4 amplifies TGF-β-induced fibroblast activation in systemic sclerosis. Ann. Rheum. Dis. 74, 1748–1755 (2015).
Cerezo, L. A. et al. The metastasis-associated protein S100A4 promotes the inflammatory response of mononuclear cells via the TLR4 signalling pathway in rheumatoid arthritis. Rheumatology 53, 1520–1526 (2014).
Dahlmann, M. et al. RAGE mediates S100A4-induced cell motility via MAPK/ERK and hypoxia signaling and is a prognostic biomarker for human colorectal cancer metastasis. Oncotarget 5, 3220–3233 (2014).
Svec, X. et al. S100A4-neutralizing monoclonal antibody 6B12 counteracts the established experimental skin fibrosis induced by bleomycin. Rheumatology 63, 817–825 (2024).
Denton, C. P. et al. Clinical and pathogenic significance of S100A4 overexpression in systemic sclerosis. Ann. Rheum. Dis. 82, 1205–1217 (2023).
Trinh-Minh, T. et al. Effect of anti-S100A4 monoclonal antibody treatment on experimental skin fibrosis and systemic sclerosis-specific transcriptional signatures in human skin. Arthritis Rheumatol. 76, 783–795 (2024).
Dees, C. et al. TGF-β-induced epigenetic deregulation of SOCS3 facilitates STAT3 signaling to promote fibrosis. J. Clin. Invest. 130, 2347–2363 (2020).
Zehender, A. et al. The tyrosine phosphatase SHP2 controls TGFβ-induced STAT3 signaling to regulate fibroblast activation and fibrosis. Nat. Commun. 9, 3259 (2018).
Chakraborty, D. et al. Activation of STAT3 integrates common profibrotic pathways to promote fibroblast activation and tissue fibrosis. Nat. Commun. 8, 1130 (2017).
Zhang, Y. et al. JAK1-dependent transphosphorylation of JAK2 limits the antifibrotic effects of selective JAK2 inhibitors on long-term treatment. Ann. Rheum. Dis. 76, 1467–1475 (2017).
Zhang, Y. et al. Inhibition of casein kinase II reduces TGFβ induced fibroblast activation and ameliorates experimental fibrosis. Ann. Rheum. Dis. 74, 936–943 (2015).
Dees, C. et al. JAK-2 as a novel mediator of the profibrotic effects of transforming growth factor β in systemic sclerosis. Arthritis Rheum. 64, 3006–3015 (2012).
Avouac, J. et al. Inactivation of the transcription factor STAT-4 prevents inflammation-driven fibrosis in animal models of systemic sclerosis. Arthritis Rheum. 63, 800–809 (2011).
Rueda, B. et al. The STAT4 gene influences the genetic predisposition to systemic sclerosis phenotype. Hum. Mol. Genet. 18, 2071–2077 (2009).
Sofen, H. et al. Efficacy and safety of vixarelimab, a human monoclonal oncostatin M receptor β antibody, in moderate-to-severe prurigo nodularis: a randomised, double-blind, placebo-controlled, phase 2a study. EClinicalMedicine 57, 101826 (2023).
Kwatra, S. G. et al. Phase 3 trial of nemolizumab in patients with prurigo nodularis. N. Engl. J. Med. 389, 1579–1589 (2023).
Misery, L. et al. Basic mechanisms of itch. J. Allergy Clin. Immunol. 152, 11–23 (2023).
Yaseen, B. et al. Interleukin-31 promotes pathogenic mechanisms underlying skin and lung fibrosis in scleroderma. Rheumatology 59, 2625–2636 (2020).
Kuzumi, A. et al. Interleukin-31 promotes fibrosis and T helper 2 polarization in systemic sclerosis. Nat. Commun. 12, 5947 (2021).
Hasegawa, M. et al. Serum levels of interleukin 6 (IL-6), oncostatin M, soluble IL-6 receptor, and soluble gp130 in patients with systemic sclerosis. J. Rheumatol. 25, 308–313 (1998).
de Almeida, A. R. et al. Increased levels of the soluble oncostatin M receptor (sOSMR) and glycoprotein 130 (sgp130) in systemic sclerosis patients and associations with clinical parameters. Immunobiology 225, 151964 (2020).
Denton, C. P. et al. Biological and clinical insights from a randomized phase 2 study of an anti-oncostatin M monoclonal antibody in systemic sclerosis. Rheumatology 62, 234–242 (2022).
Marden, G. et al. The role of the oncostatin M/OSM receptor β axis in activating dermal microvascular endothelial cells in systemic sclerosis. Arthritis Res. Ther. 22, 179 (2020).
Roopenian, D. C. & Akilesh, S. FcRn: the neonatal Fc receptor comes of age. Nat. Rev. Immunol. 7, 715–725 (2007).
Chaudhury, C. et al. The major histocompatibility complex-related Fc receptor for IgG (FcRn) binds albumin and prolongs its lifespan. J. Exp. Med. 197, 315–322 (2003).
Akilesh, S., Christianson, G. J., Roopenian, D. C. & Shaw, A. S. Neonatal FcR expression in bone marrow-derived cells functions to protect serum IgG from catabolism. J. Immunol. 179, 4580–4588 (2007).
Qiao, S. W. et al. Dependence of antibody-mediated presentation of antigen on FcRn. Proc. Natl Acad. Sci. USA 105, 9337–9342 (2008).
Montoyo, H. P. et al. Conditional deletion of the MHC class I-related receptor FcRn reveals the sites of IgG homeostasis in mice. Proc. Natl Acad. Sci. USA 106, 2788–2793 (2009).
Ober, R. J., Martinez, C., Lai, X., Zhou, J. & Ward, E. S. Exocytosis of IgG as mediated by the receptor, FcRn: an analysis at the single-molecule level. Proc. Natl Acad. Sci. USA 101, 11076–11081 (2004).
Prabhat, P. et al. Elucidation of intracellular recycling pathways leading to exocytosis of the Fc receptor, FcRn, by using multifocal plane microscopy. Proc. Natl Acad. Sci. USA 104, 5889–5894 (2007).
Kuo, T. T. et al. Neonatal Fc receptor: from immunity to therapeutics. J. Clin. Immunol. 30, 777–789 (2010).
Ulrichts, P. et al. Neonatal Fc receptor antagonist efgartigimod safely and sustainably reduces IgGs in humans. J. Clin. Invest. 128, 4372–4386 (2018).
Francois, A. et al. B lymphocytes and B-cell activating factor promote collagen and profibrotic markers expression by dermal fibroblasts in systemic sclerosis. Arthritis Res. Ther. 15, R168 (2013).
Matsushita, T. et al. BAFF antagonist attenuates the development of skin fibrosis in tight-skin mice. J. Invest. Dermatol. 127, 2772–2780 (2007).
Francois, A. et al. B cell activating factor is central to bleomycin- and IL-17-mediated experimental pulmonary fibrosis. J. Autoimmun. 56, 1–11 (2015).
Brkic, Z. et al. The interferon type I signature is present in systemic sclerosis before overt fibrosis and might contribute to its pathogenesis through high BAFF gene expression and high collagen synthesis. Ann. Rheum. Dis. 75, 1567–1573 (2016).
Dhillon, S. Telitacicept: first approval. Drugs 81, 1671–1675 (2021).
Arneth, B. M. Impact of B cells to the pathophysiology of multiple sclerosis. J. Neuroinflamm. 16, 128 (2019).
Schett, G., Mackensen, A. & Mougiakakos, D. CAR T-cell therapy in autoimmune diseases. Lancet 402, 2034–2044 (2023).
Muller, F. et al. CD19 CAR T-cell therapy in autoimmune disease — a case series with follow-up. N. Engl. J. Med. 390, 687–700 (2024).
Schett, G. et al. Advancements and challenges in CAR T cell therapy in autoimmune diseases. Nat. Rev. Rheumatol. 20, 531–544 (2024).
Bergmann, C. et al. Treatment of a patient with severe systemic sclerosis (SSc) using CD19-targeted CAR T cells. Ann. Rheum. Dis. 82, 1117–1120 (2023).
Tur, C. et al. CD19-CAR T-cell therapy induces deep tissue depletion of B cells. Ann. Rheum. Dis. 84, 106–114 (2025).
Wang, X. et al. Allogeneic CD19-targeted CAR-T therapy in patients with severe myositis and systemic sclerosis. Cell 187, 4890–4904 e4899 (2024).
Muller, F. et al. BCMA CAR T cells in a patient with relapsing idiopathic inflammatory myositis after initial and repeat therapy with CD19 CAR T cells. Nat. Med. 31, 1793–1797 (2025).
Subklewe, M. et al. Application of blinatumomab, a bispecific anti-CD3/CD19 T-cell engager, in treating severe systemic sclerosis: a case study. Eur. J. Cancer 204, 114071 (2024).
Hagen, M. et al. BCMA-targeted T-cell-engager therapy for autoimmune disease. N. Engl. J. Med. 391, 867–869 (2024).
van de Donk, N. C. J. & Zweegman, S. T-cell-engaging bispecific antibodies in cancer. Lancet 402, 142–158 (2023).
Schiopu, E. et al. Safety and tolerability of an anti-CD19 monoclonal antibody, MEDI-551, in subjects with systemic sclerosis: a phase I, randomized, placebo-controlled, escalating single-dose study. Arthritis Res. Ther. 18, 131 (2016).
Streicher, K. et al. Baseline plasma cell gene signature predicts improvement in systemic sclerosis skin scores following treatment with inebilizumab (MEDI-551) and correlates with disease activity in systemic lupus erythematosus and chronic obstructive pulmonary disease. Arthritis Rheumatol. 70, 2087–2095 (2018).
Fu, N., Xie, F., Sun, Z. & Wang, Q. The OX40/OX40L axis regulates T follicular helper cell differentiation: implications for autoimmune diseases. Front. Immunol. 12, 670637 (2021).
Gourh, P. et al. Association of TNFSF4 (OX40L) polymorphisms with susceptibility to systemic sclerosis. Ann. Rheum. Dis. 69, 550–555 (2010).
Elhai, M. et al. OX40L blockade protects against inflammation-driven fibrosis. Proc. Natl Acad. Sci. USA 113, E3901–E3910 (2016).
Skaug, B. et al. Global skin gene expression analysis of early diffuse cutaneous systemic sclerosis shows a prominent innate and adaptive inflammatory profile. Ann. Rheum. Dis. 79, 379–386 (2020).
Weidinger, S. et al. Safety and efficacy of amlitelimab, a fully human nondepleting, noncytotoxic anti-OX40 ligand monoclonal antibody, in atopic dermatitis: results of a phase IIa randomized placebo-controlled trial. Br. J. Dermatol. 189, 531–539 (2023).
Herro, R. et al. TL1A promotes lung tissue fibrosis and airway remodeling. J. Immunol. 205, 2414–2422 (2020).
Llewellyn, H. et al. Expression of TL1A, inflammatory, and fibrotic pathways in patients with diffuse systemic sclerosis. Arthritis Rheumatol. 75, abstr. 0791 (2023).
Sands, B. E. et al. Phase 2 trial of anti-TL1A monoclonal antibody tulisokibart for ulcerative colitis. N. Engl. J. Med. 391, 1119–1129 (2024).
Stockinger, B. & Omenetti, S. The dichotomous nature of T helper 17 cells. Nat. Rev. Immunol. 17, 535–544 (2017).
Maddur, M. S., Miossec, P., Kaveri, S. V. & Bayry, J. Th17 cells: biology, pathogenesis of autoimmune and inflammatory diseases, and therapeutic strategies. Am. J. Pathol. 181, 8–18 (2012).
Ramani, K. & Biswas, P. S. Interleukin-17: friend or foe in organ fibrosis. Cytokine 120, 282–288 (2019).
Bellando-Randone, S., Della-Torre, E. & Balanescu, A. The role of interleukin-17 in the pathogenesis of systemic sclerosis: pro-fibrotic or anti-fibrotic? J. Scleroderma Relat. Disord. 6, 227–235 (2021).
Ahmed, S., Misra, D. P. & Agarwal, V. Interleukin-17 pathways in systemic sclerosis-associated fibrosis. Rheumatol. Int. 39, 1135–1143 (2019).
Wei, L., Abraham, D. & Ong, V. The Yin and Yang of IL-17 in systemic sclerosis. Front. Immunol. 13, 885609 (2022).
Ono, Y. et al. Interleukin-17A is a potential therapeutic target predicted by proteomics for systemic sclerosis patients at high risk of pulmonary arterial hypertension. Sci. Rep. 14, 29484 (2024).
Dufour, A. M. et al. IL-17A dissociates inflammation from fibrogenesis in systemic sclerosis. J. Invest. Dermatol. 140, 103–112.e8 (2020).
Fukayama, M. et al. Interleukin (IL)-17F and IL-17E are related to fibrosis and vasculopathy in systemic sclerosis. J. Dermatol. 47, 1287–1292 (2020).
Robak, E., Gerlicz-Kowalczuk, Z., Dziankowska-Bartkowiak, B., Wozniacka, A. & Bogaczewicz, J. Serum concentrations of IL-17A, IL-17B, IL-17E and IL-17F in patients with systemic sclerosis. Arch. Med. Sci. 15, 706–712 (2019).
Chizzolini, C., Dufour, A. M. & Brembilla, N. C. Is there a role for IL-17 in the pathogenesis of systemic sclerosis? Immunol. Lett. 195, 61–67 (2018).
Xing, X. et al. IL-17A induces endothelial inflammation in systemic sclerosis via the ERK signaling pathway. PLoS ONE 8, e85032 (2013).
Krueger, J. G. et al. IL-23 past, present, and future: a roadmap to advancing IL-23 science and therapy. Front. Immunol. 15, 1331217 (2024).
Benschop, R. J. et al. Development of tibulizumab, a tetravalent bispecific antibody targeting BAFF and IL-17A for the treatment of autoimmune disease. MAbs 11, 1175–1190 (2019).
Orvain, C., Assassi, S., Avouac, J. & Allanore, Y. Systemic sclerosis pathogenesis: contribution of recent advances in genetics. Curr. Opin. Rheumatol. 32, 505–514 (2020).
Assassi, S. et al. Systemic sclerosis and lupus: points in an interferon-mediated continuum. Arthritis Rheum. 62, 589–598 (2010).
Christmann, R. B. et al. Association of Interferon- and transforming growth factor beta-regulated genes and macrophage activation with systemic sclerosis-related progressive lung fibrosis. Arthritis Rheumatol. 66, 714–725 (2014).
Liu, X. et al. Correlation of interferon-inducible chemokine plasma levels with disease severity in systemic sclerosis. Arthritis Rheum. 65, 226–235 (2013).
Black, C. M. et al. Interferon-α does not improve outcome at one year in patients with diffuse cutaneous scleroderma: results of a randomized, double-blind, placebo-controlled trial. Arthritis Rheum. 42, 299–305 (1999).
Granstein, R. D., Flotte, T. J. & Amento, E. P. Interferons and collagen production. J. Invest. Dermatol. 95, 75S–80S (1990).
Morand, E. F. et al. Trial of anifrolumab in active systemic lupus erythematosus. N. Engl. J. Med. 382, 211–221 (2020).
Goldberg, A. et al. Dose-escalation of human anti-interferon-α receptor monoclonal antibody MEDI-546 in subjects with systemic sclerosis: a phase 1, multicenter, open label study. Arthritis Res. Ther. 16, R57 (2014).
Guo, X. et al. Suppression of T cell activation and collagen accumulation by an anti-IFNAR1 mAb, anifrolumab, in adult patients with systemic sclerosis. J. Invest. Dermatol. 135, 2402–2409 (2015).
Rubio Gomez, M. A. & Ibba, M. Aminoacyl-tRNA synthetases. RNA 26, 910–936 (2020).
Baughman, R. P. et al. Efzofitimod: a novel anti-inflammatory agent for sarcoidosis. Sarcoidosis Vasc. Diffus. Lung Dis. 40, e2023011 (2023).
Cavagna, L. et al. Clinical spectrum time course in anti Jo-1 positive antisynthetase syndrome: results from an international retrospective multicenter study. Medicine 94, e1144 (2015).
Adams, R. A. et al. Serum-circulating His-tRNA synthetase inhibits organ-targeted immune responses. Cell Mol. Immunol. 18, 1463–1475 (2021).
Roy, S. et al. Multifaceted role of neuropilins in the immune system: potential targets for immunotherapy. Front. Immunol. 8, 1228 (2017).
Paz, S. et al. Neuropilin-2, the specific binding partner to ATYR1923, is expressed in sarcoid granulomas and key immune cells. Am. J. Respir. Crit. Care Med. 201, abstr. A3099 (2020).
US National Library of Medicine. Study to evaluate the efficacy, safety, and tolerability of efzofitimod in patients with systemic sclerosis (SSc)-related interstitial lung disease (ILD) (SSc-ILD). ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT05892614 (2023).
Manetti, M. et al. Endothelial-to-mesenchymal transition contributes to endothelial dysfunction and dermal fibrosis in systemic sclerosis. Ann. Rheum. Dis. 76, 924–934 (2017).
Di Benedetto, P. et al. Endothelial-to-mesenchymal transition in systemic sclerosis. Clin. Exp. Immunol. 205, 12–27 (2021).
Abraham, D. J., Krieg, T., Distler, J. & Distler, O. Overview of pathogenesis of systemic sclerosis. Rheumatology 48, iii3–iii7 (2009).
Dees, C. et al. Platelet-derived serotonin links vascular disease and tissue fibrosis. J. Exp. Med. 208, 961–972 (2011).
Beyer, C. et al. Stimulation of soluble guanylate cyclase reduces experimental dermal fibrosis. Ann. Rheum. Dis. 71, 1019–1026 (2012).
Beyer, C. et al. Stimulation of the soluble guanylate cyclase (sGC) inhibits fibrosis by blocking non-canonical TGFβ signalling. Ann. Rheum. Dis. 74, 1408–1416 (2015).
Kaufman, J. et al. Avenciguat: a novel soluble guanylate cyclase activator that affects multiple cell types to inhibit IFN-1 signalling and fibrosis. Rheumatology 64, 4738–4743 (2025).
Matei, A. E. et al. Protein kinases G are essential downstream mediators of the antifibrotic effects of sGC stimulators. Ann. Rheum. Dis. 77, 459 (2018).
Dees, C. et al. Stimulators of soluble guanylate cyclase (sGC) inhibit experimental skin fibrosis of different aetiologies. Ann. Rheum. Dis. 74, 1621–1625 (2015).
Dou, C. et al. P300 acetyltransferase mediates stiffness-induced activation of hepatic stellate cells into tumor-promoting myofibroblasts. Gastroenterology 154, 2209–2221.e14 (2018).
Suzuki, T. et al. Thromboxane-prostanoid receptor signaling drives persistent fibroblast activation in pulmonary fibrosis. Am. J. Respir. Crit. Care Med. 206, 596–607 (2022).
Mulvaney, E. P. et al. NTP42, a novel antagonist of the thromboxane receptor, attenuates experimentally induced pulmonary arterial hypertension. BMC Pulm. Med. 20, 85 (2020).
West, J. D. et al. Antagonism of the thromboxane-prostanoid receptor is cardioprotective against right ventricular pressure overload. Pulm. Circ. 6, 211–223 (2016).
Gibson, F. et al. Epigenetic dysregulation in autoimmune and inflammatory skin diseases. Clin. Rev. Allergy Immunol. 63, 447–471 (2022).
Tsou, P. S., Varga, J. & O’Reilly, S. Advances in epigenetics in systemic sclerosis: molecular mechanisms and therapeutic potential. Nat. Rev. Rheumatol. 17, 596–607 (2021).
Papazoglou, A. et al. Epigenetic regulation of profibrotic macrophages in systemic sclerosis-associated interstitial lung disease. Arthritis Rheumatol. 74, 2003–2014 (2022).
Bergmann, C. & Distler, J. H. Epigenetic factors as drivers of fibrosis in systemic sclerosis. Epigenomics 9, 463–477 (2017).
Malaab, M. et al. Antifibrotic factor KLF4 is repressed by the miR-10/TFAP2A/TBX5 axis in dermal fibroblasts: insights from twins discordant for systemic sclerosis. Ann. Rheum. Dis. 81, 268–277 (2022).
Wang, Z., Chang, C. & Lu, Q. Epigenetics of CD4+ T cells in autoimmune diseases. Curr. Opin. Rheumatol. 29, 361–368 (2017).
Shin, J. Y. et al. Epigenetic activation and memory at a TGFB2 enhancer in systemic sclerosis. Sci. Transl. Med. 11, eaaw0790 (2019).
Ding, W. et al. Genome-wide DNA methylation analysis in systemic sclerosis reveals hypomethylation of IFN-associated genes in CD4+ and CD8+ T cells. J. Invest. Dermatol. 138, 1069–1077 (2018).
Dees, C. et al. The Wnt antagonists DKK1 and SFRP1 are downregulated by promoter hypermethylation in systemic sclerosis. Ann. Rheum. Dis. 73, 1232–1239 (2014).
Noda, S. et al. Simultaneous downregulation of KLF5 and Fli1 is a key feature underlying systemic sclerosis. Nat. Commun. 5, 5797 (2014).
Kramer, M. et al. Inhibition of H3K27 histone trimethylation activates fibroblasts and induces fibrosis. Ann. Rheum. Dis. 72, 614–620 (2013).
Ghosh, A. K. et al. p300 is elevated in systemic sclerosis and its expression is positively regulated by TGF-β: epigenetic feed-forward amplification of fibrosis. J. Invest. Dermatol. 133, 1302–1310 (2013).
Huber, L. C. et al. Trichostatin A prevents the accumulation of extracellular matrix in a mouse model of bleomycin-induced skin fibrosis. Arthritis Rheum. 56, 2755–2764 (2007).
Zehender, A. et al. TGFβ promotes fibrosis by MYST1-dependent epigenetic regulation of autophagy. Nat. Commun. 12, 4404 (2021).
Bergmann, C. et al. The histone demethylase Jumonji domain-containing protein 3 (JMJD3) regulates fibroblast activation in systemic sclerosis. Ann. Rheum. Dis. 77, 150–158 (2018).
O’Reilly, S., Tsou, P. S. & Varga, J. Senescence and tissue fibrosis: opportunities for therapeutic targeting. Trends Mol. Med. 30, 1113–1125 (2024).
Tsou, P. S., Shi, B. & Varga, J. Role of cellular senescence in the pathogenesis of systemic sclerosis. Curr. Opin. Rheumatol. 34, 343–350 (2022).
Zhu, H. et al. Fibroblast subpopulations in systemic sclerosis: functional implications of individual subpopulations and correlations with clinical features. J. Invest. Dermatol. 144, 1251–1261.e13 (2024).
Tabib, T. et al. Myofibroblast transcriptome indicates SFRP2(hi) fibroblast progenitors in systemic sclerosis skin. Nat. Commun. 12, 4384 (2021).
Distler, O. et al. Nintedanib for systemic sclerosis-associated interstitial lung disease. N. Engl. J. Med. 380, 2518–2528 (2019).
Flaherty, K. R. et al. Nintedanib in progressive fibrosing interstitial lung diseases. N. Engl. J. Med. 381, 1718–1727 (2019).
Khanna, D. et al. Safety and efficacy of subcutaneous tocilizumab in adults with systemic sclerosis (faSScinate): a phase 2, randomised, controlled trial. Lancet 387, 2630–2640 (2016).
Khanna, D. et al. Tocilizumab in systemic sclerosis: a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Respir. Med. 8, 963–974 (2020).
Ebata, S. et al. Safety and efficacy of rituximab in systemic sclerosis (DESIRES): a double-blind, investigator-initiated, randomised, placebo-controlled trial. Lancet Rheumatol. 3, e489–e497 (2021).
Maher, T. M. et al. Rituximab versus intravenous cyclophosphamide in patients with connective tissue disease-associated interstitial lung disease in the UK (RECITAL): a double-blind, double-dummy, randomised, controlled, phase 2b trial. Lancet Respir. Med. 11, 45–54 (2023).
Author information
Authors and Affiliations
Contributions
The authors contributed equally to all aspects of the article.
Corresponding author
Ethics declarations
Competing interests
J.H.W.D. has consultancy relationships with Active Biotech, Anamar, ARXX, AstraZeneca, Bayer Pharma, Boehringer Ingelheim, Callidatas, Calluna, Galapagos, GSK, Johnson&Johnson, Kyverna, MSD, Novartis, Prolium, Quell Therapeutics and UCB, has research funding from Anamar, ARXX, BMS, Boehringer Ingelheim, Cantargia, Celgene, CSL Behring, Exo Therapeutics, Galapagos, GSK, Incyte, Inventiva, Kiniksa, Kyverna, Lassen Therapeutics, Mestag, Sanofi-Aventis, SpicaTx, RedX, UCB and ZenasBio, and is CEO of 4D Science and scientific lead of FibroCure. M.K. has received consultancy fees, speaking fees, and research grants from AbbVie, Argenx, Asahi Kasei, AstraZeneca, Boehringer Ingelheim, Chugai, GlaxoSmithKline, Janssen, Kissei, MBL, Mitsubishi Tanabe, Mochida, Novartis and Ono Pharmaceuticals. S.A. reports grants paid to his institution from Boehringer Ingelheim, the Scleroderma Research Foundation, Janssen and aTyr, as well as consultancy fees from AbbVie, AstraZeneca, aTyr, Boehringer Ingelheim, CSL Behring, Merck, Mitsubishi Tanabe, Takeda, and TeneoFour. C.P.D. has consultancy relationships with GlaxoSmithKline, Johnson&Johnson, Bayer, Sanofi, Boehringer Ingelheim, Roche, CSL Behring, Corbus, Acceleron, Horizon, Arxx, Lilly, Novartis, Certa, Mitsubishi, Quell and research grant funding from AbbVie, Arxx, Horizon, GlaxoSmithKline, CSL Behring and Servier.
Peer review
Peer review information
Nature Reviews Rheumatology thanks Dilia Giuggioli, who co-reviewed with Amelia Spinella, Jeska de Vries-Bouwstra and Yoshihide Asano for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Distler, J.H.W., Kuwana, M., Assassi, S. et al. Emerging therapies for the treatment of systemic sclerosis. Nat Rev Rheumatol 21, 612–625 (2025). https://doi.org/10.1038/s41584-025-01294-x
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41584-025-01294-x
This article is cited by
-
Mechanisms of fibrotic tissue remodelling: insights from systemic sclerosis
Nature Reviews Rheumatology (2026)
-
Beyond the skin: unmasking oral telangiectasias in limited cutaneous systemic sclerosis
Clinical Rheumatology (2026)
-
The future of autologous stem cell transplantation in systemic sclerosis
Nature Reviews Rheumatology (2025)