Abstract
Chimeric antigen receptor macrophages (CAR-M) are emerging as a next-generation cellular modality for therapies ranging from viral infection to solid tumors, leveraging innate phagocytic and antigen-presenting functions. Here, we compared CAR constructs incorporating intracellular signaling domains (ICDs) derived from CD3ζ, Fc gamma receptor IIa (CD32a), complement receptor 3 (CR3), and Toll-like receptor 4 (TLR4) in THP-1-derived monocytes and macrophages. Using an anti-viral SARS-CoV-2 model as a screening platform, we subsequently validated key findings in an anti-tumor mesothelin (MSLN) model. Results indicated that CARCD32a exhibited superior phagocytic capacity compared with CARCD3ζ in both monocytes and macrophages. While combining CR3 (CD11b and CD18) and CD32a domains did not enhance phagocytosis, it significantly increased the expression of pro-inflammatory cytokines (IL-1β, IL-6 and TNF-α). The incorporation of TLR4 signaling domain reduced surface CAR expression and phagocytic capacity but markedly increased inflammatory cytokine induction, suggesting that TLR4-driven cytokine production can be enhanced despite diminished phagocytosis in this setting. Furthermore, following phagocytosis, CAR-monocytes induced antigen-specific CD8+ T cell activation via antigen presentation. Collectively, these findings highlight CD32a-based and combinatorial ICD designs as a framework for functionally tuned CAR-M platform for solid tumor immunotherapy and anti-viral applications.
Similar content being viewed by others
Introduction
The landscape of chimeric antigen receptor (CAR)-based cell therapies is rapidly expanding, encompassing diverse immune cell platforms such as T cells, natural killer (NK) cells, and macrophages1,2. These engineering strategies are being extensively developed to target a wide spectrum of pathologies, ranging from viral infections3 and autoimmune diseases4,5,6 to various malignancies7,8,9. Among these, CAR-T cell therapy has achieved remarkable clinical success, particularly in the treatment of hematological malignancies, establishing a paradigm for engineered cell therapies10,11. Building on this breakthrough, CAR-macrophage (CAR-M) therapy has emerged as a promising next-generation modality12, attracting significant research interest for both anti-viral13 and anti-tumor applications14,15. As professional phagocytes of the innate immune system, macrophages offer unique effector functions distinct from lymphoid cells16,17,18. Crucially, they also function as professional antigen-presenting cells (APCs) that bridge innate and adaptive immunity by processing engulfed targets and priming T-cell responses19,20. Leveraging these inherent phagocytic capabilities, CAR-Ms have shown promise in preclinical studies for clearing viral pathogens and eliminating diseased cells21,22, and their therapeutic scope is actively expanding, with ongoing preclinical23 and clinical24,25 investigations evaluating their efficacy against solid tumors.
While CAR-M therapy holds significant potential, its development remains less mature than CAR-T cell therapy14,20,26. A key distinction is that macrophages rely on intracellular signaling domains (ICDs) that differ from those of T cells for robust phagocytosis, cytokine secretion, and T-cell activation1,27. CAR-T cells conventionally utilize CD3ζ-based ICDs for activation, but macrophages appear to require specialized signaling motifs to more effectively engage their phagocytic and pro-inflammatory capabilities17,28,29. Phagocytosis plays a critical role in clearing pathogenic cells or particles, while the secretion of pro-inflammatory cytokines such as TNF-α, IL-1β, and IL-6 can amplify immune responses by promoting the recruitment and activation of other immune cells28,29. Recent studies have begun to explore the incorporation of Fcγ receptor IIa (FcγRIIa, CD32a) and toll-like receptors (TLRs) into CAR constructs to enhance macrophage function14,30.
However, a systematic, head-to-head comparison of macrophage-relevant ICDs, including FcγR and complement receptor (CR), remains limited16. To address these knowledge gaps, this study aimed to optimize CAR constructs for monocytes by incorporating ICDs from professional phagocytic receptors and immunomodulatory receptors into novel CAR constructs. Specifically, we investigated the functional impact of CD32a, as well as CD11b and CD18, key components of CR316. CD32a mediates phagocytosis through the formation of a “phagocytic cup”, a process that depends on Syk-related signaling via its immunoreceptor tyrosine-based activation motif (ITAM). CR3, on the other hand, typically mediates phagocytosis through a “sinking” mechanism, and can engage Syk-associated signaling through cooperation with other receptors/adaptors, contributing to cytoskeletal remodeling and particle internalization16,31. TLRs contribute to phagocytosis-associated activity by recognizing pathogen-associated molecular patterns (PAMPs) and damage-associated molecular patterns (DAMPs), thereby activating intracellular signaling pathways that enhance phagocytosis and promote pro-inflammatory cytokine secretion32,33.
We employed a two-step strategy to identify ICD combinations that optimally support key CAR-M functions. First, we used an antiviral CAR targeting the SARS-CoV-2 spike protein as a controlled screening platform to quantify phagocytosis, cytokine induction, and antigen presentation–mediated activation of primary CD8 + T cells. We then applied the most informative ICD combinations to a clinically relevant anti-tumor CAR targeting mesothelin (MSLN) to evaluate translatability across disease contexts. Using this approach, we found that CD32a-based CARs mediated stronger phagocytosis than conventional CD3ζ-based constructs, while combinatorial inclusion of CD11b/CD18 or TLR4 preferentially enhanced inflammatory cytokine induction. Together, these findings establish ICD selection as a key design lever to tune CAR-Ms toward either maximal phagocytic clearance or immunomodulatory programs relevant to remodeling the solid-tumor microenvironment.
Results
CD32a-based CAR exhibits superior phagocytic activity
In many first- and second-generation CAR-M designs, CD3ζ-derived ITAM signaling modules, commonly used in CAR-T cells, have been adopted to drive phagocytic activity14,20. However, CD3ζ is a T-cell signaling module and is not natively coupled to the professional phagocytic machinery of macrophages16,34. To determine the optimal intracellular signaling domain (ICD) for CAR-M, we utilized the SARS-CoV-2 antigen system35 as a proof-of-concept model for comprehensive functional screening. Using this model, we initially compared the phagocytic activities of constructs incorporating CD3ζ, CD32a, CD11b, and CD1816 (Fig. 1a). Lentiviral vectors encoding these CAR constructs were transduced into THP-1 cells. Flow cytometric analysis revealed high expression levels for CARCD32a and CARCD11b (~ 95%) and slightly lower expression for CARCD3ζ (79.1%) (Fig. 1b).
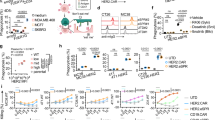
Phagocytic capability of scavenger receptor-based CARCD32a, CARCD11b, CARCD18, and CARCD3ζ. (a) Schematic representation of the CAR constructs containing the ICDs of CD3ζ, CD32a, CD11b, and CD18 for CAR-M. (b) Flow cytometric analysis was performed to assess the transduction efficiency of ACE2 CAR-m containing various ICDs. Biotinylated recombinant wild-type SARS-CoV-2 RBD and PE‒conjugated streptavidin were used for detection, and data were processed using FlowJo. (c, d) Phagocytosis of antigen-coated fluorescent beads by CAR-m. CAR-m cells were co-incubated with protein-conjugated (c) 1 μm or (d) 6 μm red fluorescent beads at an E/T ratio of 1:10 for 2 h. Bead-positive CAR-m cells were analyzed by flow cytometry. (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001) (e, f) Kinetic phagocytic activity of (e) M0 and (f) M1 macrophages containing ACE2 CAR. Phagocytosis kinetics were measured over time using pHrodo-protein-conjugated red fluorescent beads at an E/T ratio of 1:3 on a BioTek Cytation 5 (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by two-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001). UTD, untransduced.
Phagocytic activity was assessed by co-culturing CAR-expressing monocytes (CAR-m) with fluorescent beads conjugated to the D614G spike protein at an effector-to-target (E: T) ratio of 1:10. After 2 h of co-culture, phagocytic activity of each CAR-m was assessed by flow cytometry. Interestingly, CAR-mCD32a and CAR-mCD11b, which contain fewer ITAMs than CD3ζ, exhibited the highest levels of phagocytosis (Fig. 1c and d). For 1 μm beads, CAR-mCD32a and CAR-mCD11b showed phagocytic rates of 22.2 ± 1.7% and 20.4 ± 1.6% (mean ± s.d.), respectively, which were significantly higher than that of CAR-mCD3ζ at 15.8 ± 1.1% (mean ± s.d.; p = 0.0006 and p = 0.006, respectively; one-way ANOVA) (Fig. 1c). For 6 μm beads, the phagocytic rates were 80.7 ± 0.6% and 85.1 ± 1.0% (mean ± s.d.) for CAR-mCD32a and CAR-mCD11b, respectively, higher than that of CAR-mCD3ζ monocytes at 68.1 ± 1.1% (mean ± s.d.; both p < 0.0001; one-way ANOVA) (Fig. 1d).
To further assess phagocytic activity, we analyzed the kinetic phagocytic activity of the M0 and M1 CAR macrophages (CAR-M0 and CAR-M1). After differentiation, CAR-macrophages were incubated with pHrodo and D614G spike protein-loaded fluorescent beads at an E: T ratio of 1:3. Using a live cell analysis system, we monitored phagocytosis over time. The results showed that all CAR-M0s showed significantly higher CAR-dependent phagocytosis compared with non-transduced control (p < 0.0001, two-way ANOVA). CAR-M0CD32a showed the most robust and rapid phagocytic activity in a time-dependent manner without saturation for a total duration of 2 h (mean ± s.d., 34,229.7 ± 660.5 μm²). This was 1.85-fold higher than CAR-M0CD3ζ (mean ± s.d., 18,458.9 ± 1,633.7 μm²) (Fig. 1e). Consistent with the M0 results, CAR-M1CD32a showed the fastest and most robust phagocytic activity in a time-dependent manner (51,841.2 ± 3,867.0 μm² at 2 h), 1.89-fold more potent than CAR-M1CD3ζ (mean ± s.d., 27,447.5 ± 2,534.0 μm² at 2 h) (Fig. 1f). Under all conditions tested, CARCD32a consistently showed superior phagocytic activity, highlighting its potential as an optimal signaling domain for CAR macrophage designs, whereas CARCD11b showed the slowest and weakest phagocytic activity (Fig. 1e and f).
These findings demonstrate that CD32a, despite containing fewer ITAMs than CD3ζ36,37, consistently outperformed CD3ζ in promoting phagocytosis. This suggests that the identity and coupling properties of the signaling domain, rather than simply the number of ITAMs, are key determinants in driving efficient phagocytosis in macrophages.
CAR-mediated phagocytosis stimulated inflammatory cytokine expression
Monocytes and macrophages secrete diverse cytokines following phagocytosis, influenced by their polarization state38,39. To assess the impact of CAR-mediated phagocytosis on cytokine production, we analyzed the gene expression of inflammatory cytokines using quantitative PCR (qPCR).
In CAR monocytes co-cultured with D614G spike pseudovirus, CAR-mCD3ζ showed significantly elevated IL1B (1.5-fold), and TNF (3.3-fold) expression compared with the control (UTD) (p < 0.05). CAR-mCD32a showed a significant increase in TNF (3.2-fold) expression compared with UTD (p < 0.05), while other cytokines showed no elevation (Fig. 2a).
Prototype CARs induce pro-inflammatory cytokines without driving pro-inflammatory polarization. (a–b) qRT-PCR analysis of immune-related cytokine genes (IL1B, IL6, and TNF). Gene expression levels were determined (a) in D614G spike pseudovirus-cocultured CAR-m at an E/T ratio of 1:500 for 24 h, (b) in D614G spike+ HEK293F-co-cultured CAR-M0 at an E/T ratio of 1:2 for 24 h (n = 3 biologically independent samples per group). (c) Quantification of secreted immune-related cytokines (IL-1β, IL-6, and TNF-α) by ELISA. Cytokine secretion was measured from supernatants of CAR-M0 co-cultured with D614G spike+ HEK293T cells at an E/T ratio of 2:1 for 24 h (n = 3 biologically independent samples per group). (d) CD86 and CD206 expression on CAR-M0 was analyzed by flow cytometry after 24 h co-culture with D614G spike+ HEK293T cells at an E/T ratio of 2:1 (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001)
We next examined cytokine profiles in CAR-M0 following co-culture with D614G spike+ HEK293F cells. CAR-M0 exhibited a general increase in inflammatory cytokine gene expression across all CAR constructs, except IL1B (Fig. 2b). Notably, CAR-M0CD32a significantly upregulated IL6 and TNF compared with the UTD control (p < 0.0001). Similarly, CAR-M0CD3ζ, CAR-M0CD11b, and CAR-M0CD18 showed elevated levels of IL6 and TNF (p < 0.05) expression (Fig. 2b).
To further characterize the functional phenotype of CAR-Ms, we assessed cytokine secretion profiles and macrophage polarization following co-culture with target cells. Quantitative analysis revealed a significant upregulation of pro-inflammatory cytokines, including IL-1β, IL-6, and TNF-α in all CAR-M groups compared with the UTD control (p < 0.0001) (Fig. 2c). Subsequently, to determine whether CAR-mediated phagocytosis induces a specific polarization towards a pro-inflammatory or anti-inflammatory phenotype, we evaluated the surface expression of CD86 and CD206. However, flow cytometric analysis showed no significant increase in the expression of either CD86 or CD206 compared with the UTD control (Fig. 2d).
Collectively, these data indicate that prototype CAR constructs are sufficient to trigger target-specific phagocytosis and inflammatory cytokine induction/secretion, but are not sufficient on their own to drive a sustained activation-state shift, at least as assessed by CD86 and CD206.
Effects of CR3 domains combined with CD32a on phagocytic activity
Given that CAR-Ms incorporating CD32a as the primary ICD demonstrated enhanced phagocytosis and pro-inflammatory cytokine induction, we sought to amplify these capabilities by leveraging generation-specific ICD combinations used in CAR-T cells. Specifically, we replaced canonical CAR-T co-stimulatory modules with CR3-derived signaling components (CD11b or CD18), which engage phagocytosis via a pathway distinct from FcγR-mediated phagocytosis31. Based on this strategy, we designed dual-ICD CAR constructs CD32a+CD11b or CD32a+CD18 (Fig. 3a).
Evaluation of CR3-derived immunomodulatory CAR expression and phagocytic activity in monocytes and macrophages. (a) Schematic illustration of the CAR constructs containing the ICDs of CD32a+CD11b and CD32a+CD18 for CAR-M. (b) Flow cytometric analysis was performed to determine the transduction efficiency of ACE2 CAR-m containing various ICDs. Biotinylated recombinant wild-type SARS-CoV-2 RBD and PE-conjugated streptavidin were used for detection, and data were processed using FlowJo. (c, d) Phagocytosis of antigen-coated fluorescent beads by CAR-m cells. After co-incubation with protein-conjugated (c) 1 μm or (d) 6 μm red fluorescent beads at an E/T ratio of 1:10 for 2 h, bead-positive CAR-m cells were analyzed by flow cytometry. (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001). (e, f) Kinetic phagocytic activity of (e) M0 and (f) M1 macrophages containing ACE2-CAR. Phagocytosis kinetics were measured over time using pHrodo-protein-conjugated red fluorescent beads at an E/T ratio of 1:3 on a BioTek Cytation 5 (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by two-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001)
The dual-ICD CAR constructs were transduced into THP-1 cells, and CAR expression was assessed by flow cytometry, showing over 95% expression (Fig. 3b). Phagocytic capacity was assessed by co-culturing CAR-m cells with fluorescent beads conjugated to the D614G spike antigen. CAR-mCD32a showed the highest phagocytosis with 1 μm beads (mean ± s.d., 36.8 ± 2.1%), but differences were not statistically significant (Fig. 3c). In contrast, CAR-mCD32a+CD11b exhibited a significant increase in phagocytosis (mean ± s.d., 87.6 ± 0.1%) compared with UTD with 6 μm beads (Fig. 3d).
Kinetic phagocytic activity was also assessed. Among CAR-M0 cells, CAR-M0CD32a showed the highest activity throughout the 2-h observation window (mean ± s.d., 22,704.4 ± 384.6 μm²) (Fig. 3e). However, incorporating CD11b or CD18 ICD into CARCD32a did not enhance phagocytosis in CAR-M0 (Fig. 3e). Conversely, in CAR-M1 cells, CAR-M1CD32a+CD11b led to the highest phagocytic activity (mean ± s.d., 59,641.1 ± 3,552.1 μm²), but showed only marginal, non-significant improvement over CAR-M1CD32a (mean ± s.d., 53,719.2 ± 1,815.7 μm²) (Fig. 3f). We postulate that the already elevated basal signaling or saturated downstream adaptors in M1 macrophages may limit the additive benefit of the CD11b-derived ICD.
These results suggest that combining complement receptor ICDs with the FcγR ICD does not universally enhance phagocytic activity in macrophages, indicating that these pathways may not act synergistically.
Effects of TLR4 domains combined with CD32a on phagocytic activity
Given that adding CR3-derived ICDs did not enhance phagocytosis, we investigated whether a TLR4-derived immunomodulatory module could tune phagocytosis and inflammatory signaling. Using this approach, we designed CAR constructs with CD32a+TLR4, CD32a+TLR4 + CD11b, and CD32a+TLR4 + CD18 (Fig. 4a), which were then introduced into the THP-1 cell line.
Evaluation of TLR4-derived immunomodulatory CAR expression and phagocytic activity in monocytes and macrophages. (a) Schematic illustration of the CAR constructs containing the ICDs of CD32a+TLR4, CD32a+TLR4 + CD11b, and CD32a+TLR4 + CD18 for CAR-M. (b) Flow cytometric analysis was performed to determine the transduction efficiency of ACE2 CAR-m containing diverse ICD domains. Biotinylated recombinant wild-type SARS-CoV-2 RBD and PE-conjugated streptavidin were used for detection, and data were processed using FlowJo. (c, d) Phagocytosis of antigen-coated fluorescent beads by CAR-m cells. After co-incubation with protein-conjugated (c) 1 μm or (d) 6 μm red fluorescent beads at an E/T ratio of 1:10 for 2 h, bead-positive CAR-Ms were analyzed by flow cytometry. (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001) (e, f) Kinetic phagocytic activity of (e) M0 and (f) M1 macrophages containing ACE2-CAR. Phagocytosis kinetics were measured over time using pHrodo-protein-conjugated red fluorescent beads at an E/T ratio of 1:3 on a BioTek Cytation 5 (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by two-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001)
Flow cytometry confirmed expression of the TLR4-containing CAR constructs, albeit at reduced levels (< 80%) (Fig. 4b). TLR4-containing constructs exhibited reduced phagocytic activity with 1 μm beads compared with CAR-mCD32a (p < 0.0001) but were comparable to CAR-mCD32a with 6 μm beads (mean ± s.d., 84.07 ± 1.02%) (Fig. 4c and d). In particular, CAR-mCD32a+TLR4, CAR-mCD32a+TLR4+CD11b, and CAR-mCD32a+TLR4+CD18 achieved phagocytosis rates of 83.7 ± 1.5%, 79.0 ± 1.8%, and 77.5 ± 1.1% (mean ± s.d.), respectively (Fig. 4d). Kinetic analysis revealed that TLR4-containing CARs had lower phagocytic activity compared with CAR-MCD32a in both M0-like and M1-like macrophages (p < 0.05). Furthermore, additional incorporation of CD11b or CD18 into the CD32a+TLR4 construct resulted in further reduction in phagocytic activity relative to CAR-MCD32a alone (Fig. 4e and f).
Overall, CD32a signaling alone was sufficient for robust phagocytosis. The addition of ICDs from CR3 components or TLR4 did not enhance phagocytic capacity, emphasizing the need for ICD compatibility in optimizing CAR-mediated phagocytosis.
Effects of Immunomodulatory domains on cytokine production and activation markers
To investigate whether the immunomodulatory domains enhance pro-inflammatory responses, a critical function of CAR-Ms, we analyzed the gene expression of key inflammatory cytokines via qPCR during CAR-induced phagocytosis.
First, we assessed inflammatory cytokines (IL1B, IL6, and TNF) in CAR monocytes after co-culture with D614G spike pseudovirus. CAR-mCD32a+CD11b exhibited significantly elevated IL1B (1.3-fold) and TNF (3.7-fold) compared with both the control (UTD) and CAR-mCD32a (p < 0.001). Similarly, CAR-mCD32a+CD18 showed a significant increase in TNF expression (2.8-fold) compared with the control and CAR-mCD32a. In contrast, CAR constructs incorporating TLR4 did not significantly increase cytokine transcripts in monocytes under these conditions (Fig. 5a). This observation aligns with the relatively low phagocytic capacity observed for TLR4-containing CARs against smaller-sized beads (Fig. 4c), suggesting a potential correlation between phagocytic activity and cytokine production.
Immunomodulatory ICDs enhance inflammatory cytokine induction and activation markers. (a–b) qRT-PCR analysis of immune-related cytokine genes (IL1B, IL6, and TNF). Gene expression levels were measured (a) in D614G spike pseudovirus-cocultured CAR-m at an E/T ratio of 1:500 for 24 h, (b) in D614G spike+ HEK293F-cocultured CAR-M0 at an E/T ratio of 1:2 for 24 h (n = 3 biologically independent samples per group). (c) Quantification of secreted immune-related cytokines (IL-1β, IL-6, and TNF-α) by ELISA. Cytokine secretion was measured from supernatants of CAR-M0 co-cultured with D614G spike+ HEK293T cells at an E/T ratio of 2:1 for 24 h (n = 3 biologically independent samples per group). (d) CD86 and CD206 expression on CAR-M0 was analyzed by flow cytometry after 24 h co-culture with D614G spike+ HEK293T cells at an E/T ratio of 2:1 (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001)
Next, we differentiated the CAR-expressing monocytes into M0-like macrophages and observed the cytokine profiles in CAR-M cells co-cultured with D614G spike+ HEK293F cells. Differentiation into M0 macrophages led to an overall increase in the expression of inflammatory cytokine genes across all CAR constructs except for IL1B. Notably, only TLR4-containing CARs showed significant increases in IL6 and TNF expression levels compared with both the UTD control and CAR-MCD32a (p < 0.05). CAR-MCD32a+CD11b showed significantly elevated IL6 expression levels compared with both the UTD control and CAR-MCD32a, while CAR-MCD32a+CD18 exhibited significantly elevated IL6 expression levels compared with the UTD control (Fig. 5b).
Finally, we evaluated the cytokine secretion profiles and macrophage polarization status of the optimized CAR-M constructs following co-culture with target cells. Quantitative analysis revealed that the secretion of pro-inflammatory cytokines, including IL-1β, IL-6, and TNF-α, was significantly elevated in all CAR-M groups compared with the UTD control. Notably, the inclusion of specific immunomodulatory domains differentially enhanced cytokine production compared with the CD32a-only CAR. For IL-1β, constructs incorporating CAR-MCD32a+CD11b, CAR-MCD32a+CD18 and CAR-MCD32a+TLR4 exhibited significantly higher secretion levels than CAR-MCD32a. For IL-6, CAR-MCD32a+TLR4 and CAR-MCD32a+TLR4+CD18 constructs showed a significant increase compared with CAR-MCD32a. Similarly, TNF-α secretion was significantly augmented in the CAR-MCD32a+CD11b and CAR-MCD32a+CD18 groups compared with CAR-MCD32a (Fig. 5c). Subsequently, to assess the polarization phenotype, we analyzed the surface expression of CD86 and CD206 by flow cytometry after co-culture. While we observed no significant difference in CD206 expression between CAR-M variants and the UTD control, CD86 expression was significantly upregulated in all CD32a-based CAR constructs containing CR3-based (CD11b, CD18) or TLR4-based immunomodulatory domains compared with the CD32a-only construct (Fig. 5d).
Collectively, these findings indicate that ICD selection is best understood as function-specific tuning with explicit trade-offs, rather than a single “optimal” configuration. CD11b/CD18-containing CARs maintained high surface expression and robust phagocytosis comparable to CD32a alone (Fig. 3), whereas TLR4-containing CARs preferentially enhanced inflammatory cytokine induction and increased CD86 expression (Fig. 5) but exhibited trade-offs in core effector properties, including reduced CAR surface expression and/or phagocytosis (Fig. 4).
CAR monocytes effectively stimulate T cell activation
Monocytes and macrophages serve as antigen-presenting cells (APCs) capable of stimulating T cells19,40. This process includes antigen spreading, where T cells target antigens independent of the CAR specificity via MHC-mediated presentation41,42. Antigen spreading is a key mechanism that contributes to the enhanced anti-tumor efficacy of CAR monocytes and macrophages43,44. Based on prior experimental results demonstrating significant efficacy in terms of phagocytosis and immunomodulation, we evaluated the antigen-presenting and T-cell-stimulating abilities of our engineered CAR constructs. We co-cultured antigen-loaded CAR-m cells with PBMCs from HLA-A*02:01-positive healthy donors previously vaccinated against COVID-19, and assessed activation of CD8+ T cells within the PBMCs.
Antigen-loaded CAR-mCD32a cells significantly increased the frequency of CD69+CD8+ T cells producing IFN-γ and IL-2 compared with the control (p < 0.05) (Fig. 6a). Furthermore, co-culture with spike protein-loaded CAR-mCD32a+CD11b and CAR-mCD32a+CD18 significantly increased the frequencies of CD69+, CD69+IFN-γ+, and CD69+TNF-α+ CD8+ T cells (p < 0.05) (Fig. 6b). Similarly, CAR-mCD32a+TLR4 cells significantly enhanced the frequencies of CD69+IFN-γ+ and CD69+TNF-α+ CD8+ T cells (p < 0.05) (Fig. 6b).
SARS-CoV-2 spike protein-specific CD8+ T-cell response by ACE2 CAR monocytes. (a) PBMCs from HLA-A*02:01-positive healthy donors previously vaccinated (n = 3 biologically independent samples per group) were co-cultured for 24 h with CAR-m loaded with (spike) or without (ctrl) antigen. The spike protein-specific CD8+ T-cell response was evaluated by assessing the expression of CD69 and cytokines (IFN-γ, TNF-α, and IL-2). Representative flow cytometry plots (left panel) and a corresponding bar graph (right panel) are shown. (b) PBMCs (n = 3 biologically independent samples per group) were co-cultured for 24 h with various CAR-m containing the cytosolic domains of CD32a, CD32a+CD11b, CD32a+CD18, and CD32a+TLR4 in the absence or presence of antigen. Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by unpaired two-tailed Student’s t-test and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001)
These findings demonstrate that CD32a-based CAR-m cells possess potent T-cell stimulation capabilities. They effectively present antigens and activate antigen-specific memory CD8+ T cells, highlighting their potential to bridge innate and adaptive immunity in both foundational and combination CAR constructs.
The construction of MSLN-targeting CD32a-based dual-ICD CAR constructs
Our preceding results from the SARS-CoV-2 model confirmed that the combinatorial, CD32a-based dual-ICD constructs (CD32a+CD11b, CD32a+CD18, and CD32a+TLR4) showed robust phagocytic capacity, immunomodulatory activity, and the ability to stimulate T cells. To verify the generalizability of these CD32a-based dual-ICD CARs for solid tumor targeting, we next incorporated these selected ICD combinations into a CAR targeting mesothelin (MSLN), a well-established tumor-associated antigen (TAA) that is highly overexpressed in various solid tumors45,46,47,48. To validate our findings with a clinically relevant target, we constructed a series of anti-MSLN CARs utilizing the well-characterized SS1 scFv49,50 as the antigen-recognition domain. These constructs were transduced into THP-1 cells via lentiviral delivery to generate SS1 CAR-mCD32a and the combinatorial variants (SS1 CAR-mCD32a+CD11b, SS1 CAR-mCD32a+CD18, and SS1 CAR-mCD32a+TLR4) (Fig. 7a).
Generation and functional characterization of anti-MSLN CAR constructs with modified ICDs in THP-1 cells. (a) Schematic representation of the CAR constructs containing the ICDs of CD32a+CD11b, CD32a+CD18, and CD32a+TLR4 for CAR-M. (b) Flow cytometric analysis was performed to assess the transduction efficiency of SS1 CAR-m containing various ICDs. Biotinylated recombinant MSLN protein and PE‒conjugated streptavidin were used for detection, and data were processed using FlowJo. (c) Phagocytosis of antigen-coated fluorescent beads by CAR-m cells. CAR-m cells were co-incubated with protein-conjugated 6 μm red fluorescent beads at an E/T ratio of 1:10 for 2 h. Bead-positive CAR-m cells were analyzed by flow cytometry (n = 3 biologically independent samples per group). Data are analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001) (d) Phagocytosis of target cells by CAR-M0s. CAR-M0s were co-incubated with MSLN− K562 and MSLN+ K562 at an E/T ratio of 2:1 for 2 h. The population double-positive for target cells and CAR-Ms was analyzed by flow cytometry (n = 3 biologically independent samples per group). Data were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001) (e) Antigen-dependent ERK activation in CAR-m following MSLN-coated bead engagement. Western blot analysis demonstrates the activation of the ITAM downstream MAPK cascade. CAR-m cells were treated with MSLN-coated beads (+) for 30 min or untreated (-) as a control.
CAR expression was assessed by flow cytometry. Surface expression exceeded 70% for SS1 CAR-mCD32a, SS1 CAR-mCD32a+CD11b, and SS1 CAR-mCD32a+CD18. Consistent with our previous data, the SS1 CAR-mCD32a+TLR4 construct exhibited lower surface expression (48.3%) compared with the other constructs (Fig. 7b). To determine whether this lower expression level was due to impaired surface stability (e.g., defective trafficking or rapid degradation) or simply lower total protein expression, we assessed whether the construct retained antigen engagement–dependent internalization. We compared the internalization kinetics of all SS1 CAR-m constructs following engagement with the MSLN antigen. Our results demonstrated that all SS1 CAR constructs underwent time-dependent internalization (Supplementary Figure S1). These results suggest that the low surface expression of SS1 CAR-mCD32a+TLR4 is more consistent with reduced overall expression levels than with a defect in antigen-dependent internalization or trafficking. The construct retained antigen-dependent internalization kinetics comparable to the higher-expressing constructs.
SS1 CAR-M mediates target-specific phagocytosis via ITAM signaling
To evaluate the phagocytic capacity of our CAR constructs, we performed phagocytosis assays using both antigen-coated beads and target cells. We conducted a bead-based assay by co-culturing CAR-m cells with 6 μm MSLN-coated beads (Fig. 7c). Minimal non-specific phagocytosis was observed against the BSA-coated control beads. In contrast, all SS1 CAR constructs demonstrated significantly higher phagocytic capacity against MSLN-coated beads compared with the UTD control. Notably, SS1 CAR-mCD32a+CD18 exhibited the highest activity among the combinatorial constructs (mean ± s.d., 45.0 ± 0.35%) (Fig. 7c). We further validated this function using a cell-based assay with MSLN+ K562 cells and MSLN− K562 cells. None of the SS1 CAR-M variants exhibited non-specific phagocytosis against MSLN− K562 cells compared with the UTD control. However, against MSLN+ K562 cells, all SS1 CAR-M showed significantly enhanced phagocytosis. The SS1 CAR-MCD32a demonstrated the highest efficacy (mean ± s.d., 19.9 ± 0.25%) (Fig. 7d). Collectively, these data confirm that all our engineered CD32a-based SS1 CARs mediate efficient, and target-specific phagocytosis.
We next sought to confirm that this phagocytic activity was mediated by the downstream signaling of the CD32a ITAM. We analyzed the phosphorylation of ERK (pERK), a downstream readout of the ITAM signaling cascade51, via Western blot (Fig. 7e and Supplementary Figure S2). The UTD cells showed no pERK induction, regardless of MSLN-bead stimulation. In contrast, both the SS1 CAR-mCD32a and all dual-ICD CAR-m constructs exhibited robust, antigen-dependent ERK phosphorylation only upon engagement with MSLN-coated beads. These results support that CD32a-based CAR engagement activates ITAM-coupled signaling in an antigen-dependent manner (Fig. 7e).
Combinatorial CD32a-based SS1 CAR-Ms increase CD86 expression and pro-inflammatory cytokine secretion
Effective CAR-M therapy in solid tumors is expected to overcome the immunosuppressive tumor microenvironment (TME)52,53. To achieve this, CAR-Ms ideally should be multifunctional, capable of not only executing target cell phagocytosis but also polarizing into a pro-inflammatory phenotype and secreting pro-inflammatory cytokines54,55. This immune upregulation is crucial for promoting a broader anti-tumor immune response by inducing the infiltration and activation of other immune cells, such as T cells2,53.
To determine whether target engagement induces a pro-inflammatory activation-state shift, we differentiated SS1 CAR-m into M0-like macrophages and assessed CD86 and CD206 expression by flow cytometry (Fig. 8a). While the SS1 CAR-MCD32a showed no difference in CD86 expression compared with the UTD control, all dual-ICD CAR-M constructs (CD11b, CD18, and TLR4) induced a significant upregulation of CD86. Notably, the SS1 CAR-MCD32a+TLR4 induced the largest increase in CD86 MFI (2.89-fold vs. UTD). Conversely, no significant change in CD206 expression was observed in any group (Fig. 8a).
Enhanced pro-inflammatory phenotype of combinatorial anti-MSLN CAR-M constructs. (a) CD86 and CD206 expression on CAR-M0 was analyzed by flow cytometry after a 24 h co-culture with MSLN+ K562 cells at an E/T ratio of 2:1. (n = 3 biologically independent samples per group). (b) qRT-PCR analysis of immune-related cytokine genes (IL1B, IL6, and TNF). Gene expression levels were measured in CAR-M0 co-cultured with MSLN+ K562 cells at an E/T ratio of 2:1 for 24 h (n = 3 biologically independent samples per group). (c) Quantification of secreted immune-related cytokines (IL-1β, IL-6, and TNF-α) by ELISA. Cytokine secretion was measured from supernatants of CAR-M0 co-cultured with MSLN+ K562 cells at an E/T ratio of 2:1 for 24 h (n = 3 biologically independent samples per group). Data of (a), (b), and (c) were analyzed using GraphPad Prism 8.0.2. Statistical significance was determined by one-way ANOVA with multiple comparisons and is presented as the mean ± s.d. (ns, not significant; *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001).
Next, to determine whether target cell engagement induces increased pro-inflammatory cytokine mRNA expression and subsequent protein secretion, we performed qPCR and ELISA on the SS1 CAR-M0 co-cultures with target cells. Consistent with the CD86 upregulation, qPCR analysis revealed that all SS1 CAR-M constructs showed significantly increased mRNA levels of IL1B and TNF compared with UTD control following target engagement (p < 0.0001). For IL6, a significant increase compared with UTD was observed only in the SS1 CAR-MCD32a and SS1 CAR-MCD32a+TLR4 (p < 0.01) (Fig. 8b). To confirm that these transcriptional changes led to functional protein secretion, we quantified cytokine levels in the supernatant by ELISA. In alignment with the qPCR data, all SS1 CAR-M groups induced significantly higher secretion of IL-1β, IL-6, and TNF-α compared with UTD (p < 0.0001). Critically, the SS1 CAR-MCD32a+TLR4 induced significantly more IL-6 and TNF-α secretion than the SS1 CAR-MCD32a (p < 0.0001) (Fig. 8c).
Taken together, these data indicate that our combinatorial SS1 CAR-M designs (CD32a+CD11b, CD32a+CD18, and CD32a+TLR4) enhance CD86 upregulation and inflammatory cytokine induction upon MSLN engagement. Among the constructs tested, the CD32a+TLR4 produced the strongest immunomodulatory readouts, supporting this design as a promising strategy for CAR-M programming within the contexts evaluated here.
Discussion
Our study provides valuable insights into the optimization of CAR constructs for macrophage-based therapies, moving beyond the conventional reliance on T-cell-derived signaling domains14,20,56. Our findings show that CD32a, despite possessing a single ITAM, consistently outperforms the tri-ITAM CD3ζ, underscoring the importance of optimal signal calibration over sheer ITAM quantity. This aligns with the macrophages’ intrinsic reliance on single-ITAM receptors and mirrors CAR-T studies in which reducing the number of ITAMs has been shown to reduce exhaustion and enhance functional potency57. Although macrophage activation programs differ from T-cell exhaustion, this comparison supports the broader principle that signal strength and quality shape functional outcomes. Thus, CD32a may provide a more functionally calibrated signal in macrophages, as it supports robust phagocytosis with a distinct inflammatory output profile compared with CD3ζ (Figs. 1 and 2). We hypothesize that this superior efficacy is driven by CD32a’s ability to more effectively couple with macrophage-specific cytoskeletal machinery (e.g., via Syk recruitment).
Notably, while the first-generation/prototype CAR constructs were sufficient to trigger target-dependent acute cytokine induction and secretion (Fig. 2a–c), they did not produce a clear shift in activation-state markers such as CD86/CD206 (Fig. 2d), suggesting that phagocytosis-associated activation alone is insufficient to imprint a sustained pro-inflammatory state. This gap motivated our dual-ICD strategy to actively program macrophage immunomodulatory phenotypes. Perhaps the most significant implication for next-generation design stems from our combinatorial ICD constructs. While combining CD32a with CR3 or TLR4 signaling domains did not show superior phagocytosis compared with CD32a alone (Figs. 3 and 4, and 7), it significantly altered the immunological profile of the CAR-Ms. These combinatorial constructs markedly enhanced both the expression and secretion of pro-inflammatory cytokines and drove the cells toward a pro-inflammatory activation signature (Figs. 5 and 8), extending beyond the acute inflammatory outputs observed with single-domain constructs to imprint a clearer activation-state shift (Figs. 2 and 5, and 8). This finding is critical, as it suggests CAR-M can be ‘tuned’ for specific therapeutic roles: some optimized for maximal phagocytic clearance, and others (like the CD32a+TLR4) designed as potent TME modulators. Together, these data suggest that incorporating immunomodulatory ICDs (e.g., TLR4) is an attractive strategy to outperform CD3ζ-based signaling for macrophage programming within the ICDs tested here.
Furthermore, this study advances the CAR-M field by positioning these cells as a critical bridge between innate and adaptive immunity. We demonstrated that following phagocytosis, our CD32a-based CAR-m effectively processes and presents antigens, leading to the robust activation of primary CD8+ T cells. This dual functionality is a significant advantage for treating infectious diseases or solid tumors, offering a mechanism to overcome antigen heterogeneity (Fig. 6).
Our study first established the functional efficacy of our CAR constructs in an anti-viral context using the ACE2/SARS-CoV-2 model. While this served as a well-controlled platform to identify the best-performing ICDs based on our functional screening metrics, we squarely acknowledge its limitations in fully recapitulating the complexity of solid tumor biology. Building upon these findings, we sought to demonstrate the platform’s versatility by extending its application to solid tumor immunotherapy. To this end, we pivoted to a clinically relevant solid tumor model targeting mesothelin (MSLN). Consistently, these CD32a-based MSLN-targeting CARs recapitulated the key findings observed in the viral system, demonstrating superior phagocytosis, inflammatory activation (CD86 upregulation and inflammatory cytokine induction), and enhanced pro-inflammatory cytokine secretion compared with UTD controls. Critically, the SS1 CARCD32a+TLR4 again exhibited the most potent immunomodulatory readouts (e.g., cytokine/activation-marker induction), with accompanying trade-offs in core effector properties relative to CD11b/CD18 combinations (Figs. 7 and 8).
Despite these promising findings, several limitations should be acknowledged. Firstly, this study was conducted in vitro using a THP-1-based system. To translate these findings toward clinical application, validation in primary human monocyte-derived macrophages obtained from healthy donors or cancer patients is a prerequisite. This step is crucial to confirm that the enhanced signaling kinetics of CD32a and TLR4 are conserved in non-transformed cells with heterogeneous genetic backgrounds. Moreover, while our in vitro results are robust, they cannot fully account for the intricate complexities of the TME, such as hypoxia and immunosuppressive cellular interactions. Additionally, the mechanisms underlying the consistently low surface expression of TLR4-containing CARs observed in our study (Figs. 4b and 7b) require further elucidation. We speculate that this phenotype may stem from tonic signaling-induced internalization, where constitutive activation of the potent TLR4 domain triggers receptor endocytosis as a negative feedback mechanism58. Alternatively, protein instability or folding issues within the endoplasmic reticulum (ER)59 due to the complex structural composition of the chimeric ICD could contribute to reduced surface display. Furthermore, while we hypothesize that the superior efficacy of CD32a is driven by its ability to couple with macrophage-specific cytoskeletal machinery, verifying whether this domain induces distinct “actin remodeling” dynamics compared to CD3ζ remains a critical objective for future mechanistic studies.
Therefore, future translational studies must focus on assessing the in vivo efficacy, persistence, and safety profile, specifically the management of systemic cytokine release, using humanized mouse models or immunocompetent syngeneic tumor models. Additionally, establishing robust Good Manufacturing Practice (GMP)-compliant protocols for generating CAR-Ms, potentially via efficient lentiviral transduction or lipid nanoparticle (LNP)-mediated mRNA delivery to primary monocytes, will be a pivotal milestone for successful clinical implementation.
In conclusion, this study demonstrates that CD32a-based constructs, particularly when combined with immunomodulatory signals like TLR4, can effectively bridge innate and adaptive immunity. By validating this platform against a clinically relevant target like MSLN, we lay the groundwork for next-generation CAR macrophage therapies optimized for solid tumor treatment and infectious diseases.
Materials and methods
Cell culture
The THP-1, K562, and Lenti-X 293 T cells were purchased from the ATCC (USA) and Takara Bio (Japan) respectively. The THP-1 cells were cultured in RPMI 1640 (Welgene, Republic of Korea) with 10% fetal bovine serum (FBS, Gibco, USA), 1× Penicillin-Streptomycin (Gibco, USA) and 50 µM 2-mercaptoethanol (Gibco). The Lenti-X 293 T cells were cultured in DMEM (Biowest, France) supplemented with 10% FBS (Gibco) and 1× Penicillin-Streptomycin (Gibco). The K562 cells were cultured in RPMI 1640 (Welgene) with 10% fetal bovine serum (FBS, Gibco, USA), 1× Penicillin-Streptomycin (Gibco, USA). All cells were grown at 37 °C and 5% CO2 under humidified conditions. For THP-1 derived macrophages, THP-1 cells were differentiated into M0-like type macrophages by 24 h incubation with 150 nM phorbol 12-myristate 13-acetate (PMA, biogems) followed by 24 h incubation in fresh RPMI medium. Polarization of macrophages to M1-like type was obtained by incubation with 20 ng/mL of IFN-γ (PeproTech, USA) and 10 pg/mL of LPS (Invivogen)60.
Preparation of Recombinant antigen proteins
The recombinant receptor binding domain (RBD) and spike (D614G mutant) of SARS-CoV-2 and MSLN genes were cloned into the pcDNA3.4 vector using Gibson assembly cloning (NEB, Ipswich, MA, USA) and SARS-CoV-2 antigens were produced in Expi293 cells (Thermo Fisher Scientific, Waltham, MA, USA)61. The His-tagged RBD, D614G spike and MSLN were purified using Ni-NTA agarose resin (Thermo Fisher Scientific) affinity chromatography. The eluted samples were subjected to buffer exchange and were analyzed for purity by SDS-PAGE gel analysis. For additional experiments, the recombinant RBD, D614G spike and MSLN were biotinylated using the EZ-Link™ Sulfo-NHS-Biotinylation Kit (Thermo Fisher Scientific, Waltham, MA, USA).
Construction of lentiviral vectors
All lentiviral vectors were cloned into the pCDH-EF1A-CAR using Gibson Assembly cloning (NEB, Ipswich, MA, USA). The angiotensin-converting enzyme 2 (ACE) CAR consisted of the extracellular domain (ECD) of human ACE2 (a.a. 18–615) linked to the CD32a (Ig-like domain 2 ~ transmembrane domain, a.a. 122–240). The ACE2 CAR was designed with the following ICDs: (1) CD3ζ (a.a. 52–164), (2) CD32a (a.a. 241–317), (3) CD11b (a.a 1129‒1152), (4) CD18 (a.a. 724‒769), and (5) Toll-like receptor 4 (TLR4) (a.a. 653–839). The optimized CARs were constructed using various combinations of the following ICDs; CD32a, CD11b, CD18, and TLR4 inserted into ACE2 CAR.
Lentivirus production
Three million Lenti-X 293 T cells were seeded in a 100-mm culture dish. After a few days, the medium was replaced with pre-warmed fresh DMEM. Then, 10 µg CAR-encoding transfer plasmid, 10 µg psPAX2, and 5 µg pLP/VSVG were transfected into Lenti-X 293 T cells using Lipofectamine 3000 (Thermo Fisher Scientific, Waltham, MA, USA). Supernatant harvested 24 and 48 h post-transfection was concentrated by ultracentrifugation for 120 min at 112,700 ×g at 4 °C in polypropylene tubes. The lentivirus was resuspended in PBS at a volume 100 times concentrated and was stored at − 80 °C before use.
Generation of CAR monocytes
Two hundred fifty thousand THP-1 cells were transduced with lentivirus using complete culture media containing 8 µg/mL of polybrene for 48 h. Transduction efficiency was analyzed by binding to wild type SARS-CoV-2 RBD or MSLN with flow cytometry.
Preparation of D614G Spike pseudovirus
The Pseudovirus expressing the SARS-CoV-2 S protein was produced as described previously62. HIV-1 NL4-3 ΔEnv Vpr Luciferase Reporter Vector from Dr. Nathaniel Landau63,64 and the GP-pCAGGS plasmid containing the SARS-CoV-2 S protein were obtained through the NIH AIDS Reagent Program, Division of AIDS, NIAID, NIH. These plasmids were co-transfected into 293T cells. At 24 and 48 h post-transfection, supernatants containing SARS-CoV-2 pseudovirus were collected and filtered through a 0.45 μm cellulose acetate syringe filter. The filtered supernatants were then concentrated by ultracentrifugation in Beckman thin-wall polypropylene centrifuge tubes (Beckman Coulter, High Wycombe, UK) using a Beckman SW32Ti swinging-bucket rotor at 112,700 ×g for 2 h at 4 °C. Pseudovirus yield was titrated using Lentivirus Titer Kit (#TR30038, OriGene, Rockville, MD, USA).
Flow cytometry-based CAR expression level analysis
Fifty thousand CAR monocytes were resuspended in a round bottom 96-well plate and centrifugated at 300 ×g for 3 min. The cell pellets were washed with PBSF (1% FBS in PBS). Biotinylated recombinant wild type SARS-CoV-2 RBD or MSLN was treated to a concentration of 200 nM and incubated at 4 °C. After 1 h, those cells were washed with PBSF and then stained with Streptavidin, R-Phycoerythrin Conjugate (SAPE) (1:200 dilution, Invitrogen, USA) at 4 °C for 15 min in the dark. After incubation, those cells were washed with PBSF and analyzed by flow cytometer (BD FACS Canto TM II (BD Biosciences). The flow cytometry data were analyzed using FlowJo.
Flow cytometry-based bead phagocytosis assay
The recombinant protein of wild-type SARS-CoV-2 RBD, MSLN and bovine serum albumin (BSA) was covalently coupled to red fluorescent 1 μm beads (Thermo Fisher Scientific, Waltham, MA, USA) and red fluorescent 6 μm beads (CD Bioparticles, USA) via a two-step carbodiimide reaction. The red fluorescent beads were activated with activation buffer (0.1 M NaH2PO4, pH 6.2), Sulfo-NHS, and EDC and incubated for 30 min at RT in the dark. The beads were washed three times with coupling buffer (50 mM MES, pH 5.2) and then incubated with protein in coupling buffer for 2 h at RT in the dark. The beads were subsequently washed and blocked with PBS-TBN (0.1% BSA in PBS), or PBSA (5% BSA in PBS) overnight at 4 °C in the dark and then washed and resuspended in 100 µL PBS.
Fifty thousand CAR monocytes were resuspended per well in a round-bottom 96-well plate. The antigen-coated beads were added to obtain a 10:1 bead-to-cell ratio, and the plate was incubated at 37 °C and 5% CO2 under humidified conditions. After 2 h, the cells were washed with fresh PBSF and analyzed with flow cytometer (BD FACS Canto TM II (BD Biosciences). The flow cytometry data were analyzed using FlowJo.
Kinetics of phagocytosis
The recombinant protein D614G SARS-CoV-2 spike and BSA was covalently coupled to red fluorescent beads by using the methods described above. Beads were spun down and resuspended in 0.1 M sodium bicarbonate buffer (pH 8.5) and labeled with 10 µM pHrodo Green STP Ester (Thermo Fisher Scientific, Waltham, MA, USA) for 30 min at RT in the dark. Beads were spun down to remove free dye and resuspended in PBS for use in experiments. The 1 × 104 monocytes were transferred to black wall clear flat bottom 96-well plate. For differentiation to M0-like macrophages, the monocytes were incubated with 150 nM PMA for 24 h followed by 24 h incubation in fresh RPMI medium. To differentiate to M1, the M0 cells were incubated with IFN-γ (20 ng/mL) and LPS (10 pg/mL) for 48 h60. After differentiation, the cells were washed with fresh medium. The pHrodo-labeled, antigen-coated fluorescent beads were added to obtain a 3:1 bead to cell ratio and the plate was incubated in BioTek Cytation 5 (Agilent, USA). The pHrodo fluorescence (green) and bead fluorescence (red) were measured kinetically. The results were analyzed based on the area of phagocytic events per image (µm2) (green/red colocalization).
Real-time quantitative reverse transcription PCR
Total RNA extraction was performed using a QIAzol (QIAGEN, The Netherlands) per the manufacturer’s protocol. cDNA was prepared using amfiRivert cDNA Synthesis Platinum Master Mix (GenDEPOT, USA). The gene expression was measured in triplicates using KAPA SYBR® FAST qPCR Master Mix (2×) Kit (Kapa Biosystems, USA) on a Bio-Rad PCR machine (CFX Connect Real-Time PCR Detection System). The primer sequences used in the qRT-PCR assay are listed in the Supplementary Table S1.
Study subjects and collection of PBMCs
We enrolled study participants who were vaccinated with COVID-19 and who developed memory T cells specific against to SARS-CoV-2 spike protein, confirmed with flow cytometry using PBMCs from HLA-A*02:01-positive healthy donors previously vaccinated against COVID-1962,65,66. Blood samples were collected and peripheral blood mononuclear cells (PBMCs) were purified using a Ficoll–Histopaque gradient (1.077 g/mL; GE Healthcare Life Sciences, Piscataway, NJ, USA). They were stored in liquid nitrogen until analysis in freezing medium comprising 50% FBS, 10% dimethyl sulfoxide (DMSO), and 40% RPMI 1640 (all reagents from Thermo Fisher Scientific). The Institutional Review Board of Seoul National University Hospital approved the study (No. H-2201-120-1295), and all participants provided written informed consent in accordance with the Declaration of Helsinki.
Antigenic stimulation by CAR monocytes
To evaluate the antigen-presenting and antigen-stimulating ability of CAR monocytes, stored PBMCs (1 × 106 cells/mL) were co-cultured with CAR monocytes with or without antigen (1:20 PBMC to CAR monocytes ratio) for 24 h in the presence of 10 µg/mL of anti-human CD28/CD49d antibodies (BD Biosciences, San Jose, CA, USA) for co-stimulation. Cells were treated with BD Golgistop™ (monensin, BD Biosciences) and BD Golgiplug™ (brefeldin A, BD Biosciences) for the final 4 h of the antigen stimulation.
Flow cytometry-based evaluation of T-cell response
After antigenic stimulation, surface antigens were stained with BUV496–anti-human CD8 (clone, RPA-T8), Brilliant Violet™ 605 (BV605)–anti-human CD69 (clone, FN50) Abs. After fixation and permeabilization with a Cytofix/Cytoperm kit (BD Biosciences), cells were incubated with BV711–anti-human interleukin (IL)-2 (clone, MQ1-17H12;), phycoerythrin (PE)-cychrom 7 (Cy7)–anti-human interferon (IFN)-γ (clone, B27), and allophycocyanin (APC)–anti-human tumor necrosis factor (TNF)-α (clone, Mab11) Abs (all from BD Biosciences except BioLegend’s anti-human TNF-α Ab, San Diego, CA, USA) in Perm/Wash buffer containing Brilliant Stain Buffer (BD Biosciences). Stained cells were acquired using a BD LSRFortessa™ flow cytometer (BD Biosciences) and analyzed using FlowJo 10.8.1 software (Tree Star, Ashland, OR, USA). The frequencies of SARS-CoV-2-specific cytokine-producing cells (IFN-γ, TNF-α, and IL-2) among CD69+ CD8+ T cells were evaluated.
Flow cytometry-based cell phagocytosis assay
Target cells were washed with DPBS twice and resuspended in fresh DPBS. The washed target cells were labeled with 4 µM pHrodo Red STP Ester (Thermo Fisher Scientific, Waltham, MA, USA) for 30 min at RT in the dark. The labeled cells were washed twice with DPBS and resuspended with complete media for phagocytosis assay.
CAR-M0s were seeded in a 24-well plate. After overnight incubation, the pHrodo-target cells were added to obtain an E/T ratio of 2:1, and the plate was incubated at 37 °C and 5% CO2 under humidified conditions. After 2 h, the cells were washed with DPBS. The CAR-M0 were detached with trypsin-EDTA and washed with PBSF (1% FBS in PBS). To detect macrophages, the detached cells were labeled with APC anti-human CD14 antibody (Biolegend, clone M5E2, USA) at 4 °C for 15 min in the dark. After washing with PBSF, the cells were analyzed by flow cytometer (BD FACS Canto TM II (BD Biosciences). The flow cytometry data were analyzed using FlowJo.
Western blot analysis
Cells were lysed using RIPA buffer (Thermo Fisher Scientific, Waltham, MA, USA) containing a protease inhibitor cocktail (Sigma-Aldrich, USA) and phosSTOP (Roche, Switzerland). Protein concentrations from lysates were quantified by BCA assay. Equal amounts of protein from each sample were separated by SDS-PAGE and transferred onto polyvinylidene difluoride (PVDF) membranes. The membranes were blocked with 5% skim milk in 0.05% Tween 20/TBS (TBST, tween 20 0.05% in TBS) overnight at 4 °C. After washing, membranes were incubated with anti-phospho-ERK 1/2 antibody (1:1000; Cat.4376 S, Cell Signaling Technology, USA) for 2 h at RT. The membranes were subsequently stripped and re-probed with anti-ERK 1/2 antibody (1:1000; Cat.9102 S, Cell Signaling Technology, USA) or anti-GAPDH antibody (1:1000; Cat.2118 S, Cell Signaling Technology, USA). After washing, membranes were incubated with HRP-conjugated goat anti-rabbit IgG (1:3,000; Cat.6721, Abcam, UK) and visualized using Dyne ECL Pico Plus (Dyne Bio, Republic of Korea) with a ChemiDoc imaging system (Bio-Rad Laboratories, Hercules, CA, USA).
Flow cytometry-based CD86 and CD206 expression analysis
CAR-M0s were seeded in a 24-well plate. After overnight incubation, the target cells were added to obtain an E/T ratio of 2:1, and the plate was incubated at 37 °C and 5% CO2 under humidified conditions. After 24 h, the cells were washed with DPBS. The CAR-M0 were detached with trypsin-EDTA and washed with PBSF (1% FBS in PBS). To detect CD86 and CD206, the detached cells were labeled with APC anti-human CD14 antibody (Biolegend, clone M5E2, USA), PE anti-human CD86 antibody (Biolegend, clone BU63, USA) and FITC anti-human CD206 antibody (Biolegend, clone 15 − 2, USA) at 4 °C for 15 min in the dark. After washing with PBSF, the cells were analyzed by flow cytometer (BD FACS Canto TM II (BD Biosciences). The flow cytometry data were analyzed using FlowJo(Tree Star).
Detection of pro-inflammatory cytokines
To evaluate cytokine secretion, CAR-M0 were co-cultured with target cells at an E/T ratio of 2:1. After 24 h of incubation, the culture supernatants were collected. The concentrations of IL-1β, IL-6, and TNF-α were quantified using respective ELISA MAX Deluxe Sets (Biolegend, USA; Cat. 437004, 430504, and 430104, respectively) according to the manufacturer’s instructions.
Statistical analysis
Data are presented as mean ± standard deviation (s.d.) from at least three independent experiments. Statistical significance was determined using unpaired two-tailed Student’s t-test, one-way ANOVA or two-way ANOVA with Tukey’s post hoc test for multiple comparisons. A p-value of less than 0.05 was considered statistically significant. All statistical analyses were performed using GraphPad Prism 8.0.2 (GraphPad Software, La Jolla, CA, USA).
Data availability
All data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Pan, K. et al. CAR race to cancer immunotherapy: from CAR T, CAR NK to CAR macrophage therapy. J. Exp. Clin. Cancer Res. 41, 119 (2022).
Hou, Y. et al. Beyond CAR-T cells: exploring CAR-NK, CAR-M, and CAR-γδ T strategies in solid tumor immunotherapy. Front. Immunol. 16, 1675807 (2025).
Chen, Y. et al. Developing CAR-immune cell therapy against SARS-CoV-2: current status, challenges and prospects. Biochem. Pharmacol. 222, 116066 (2024).
Wu, D. et al. CAR T-cell therapy in autoimmune diseases: a promising frontier on the horizon. Front. Immunol. 16, 1613878 (2025).
Gao, J. et al. Efficacy and safety of allogeneic CD19 CAR NK-cell therapy in systemic lupus erythematosus: a case series in China. Lancet 406, 2968–2979 (2025).
Cao, Q. et al. Targeting inflammation with chimeric antigen receptor macrophages using a signal switch. Nat. Biomed. Eng. 9, 1502–1516 (2025).
Li, J., Liu, C., Zhang, P., Shen, L. & Qi, C. Optimizing CAR T cell therapy for solid tumours: a clinical perspective. Nat. Rev. Clin. Oncol. 22, 953–968 (2025).
Li, T. et al. CAR-NK cells for cancer immunotherapy: recent advances and future directions. Front. Immunol. 15, 1361194 (2024).
Alrehaili, M., Couto, P. S., Khalife, R. & Rafiq, Q. A. CAR-macrophages in solid tumors: promise, progress, and prospects. Npj Precis Onc. 9, 382 (2025).
Khan, A. N., Asija, S., Pendhari, J. & Purwar, R. CAR-T cell therapy in hematological malignancies: where are we now and where are we heading for? Eur. J. Haematol. 112, 6–18 (2024).
Zhang, X., Zhu, L., Zhang, H., Chen, S. & Xiao, Y. CAR-T cell therapy in hematological malignancies: current opportunities and challenges. Front. Immunol. 13, 927153 (2022).
Shi, Y. et al. Exploring the potential of CAR-macrophage therapy. Life Sci. 361, 123300 (2025).
Fu, W. et al. CAR macrophages for SARS-CoV-2 immunotherapy. Front Immunol 12, (2021).
Lei, A. et al. A second-generation M1-polarized CAR macrophage with antitumor efficacy. Nat. Immunol. 25, 102–116 (2024).
Zhang, H. et al. Silencing of SIRPα enhances the antitumor efficacy of CAR-M in solid tumors. Cell. Mol. Immunol. 21, 1335–1349 (2024).
Freeman, S. A. & Grinstein, S. Phagocytosis: receptors, signal integration, and the cytoskeleton. Immunol. Rev. 262, 193–215 (2014).
Chen, S. et al. Macrophages in immunoregulation and therapeutics. Sig Transduct. Target. Ther. 8, 207 (2023).
Mantovani, A., Allavena, P., Marchesi, F. & Garlanda, C. Macrophages as tools and targets in cancer therapy. Nat. Rev. Drug Discov. 21, 799–820 (2022).
Muntjewerff, E. M. & Meesters, L. D. & van den Bogaart, G. Antigen Cross-Presentation by macrophages. Front Immunol 11, (2020).
Klichinsky, M. et al. Human chimeric antigen receptor macrophages for cancer immunotherapy. Nat. Biotechnol. 38, 947–953 (2020).
Gao, Z. et al. Targeting cardiac fibrosis with chimeric antigen receptor macrophages. Cell. Discov. 10, 86 (2024).
Wang, J. et al. CAR-Macrophage therapy alleviates myocardial Ischemia-Reperfusion injury. Circul. Res. 135, 1161–1174 (2024).
Pierini, S. et al. Chimeric antigen receptor macrophages (CAR-M) sensitize HER2 + solid tumors to PD1 Blockade in pre-clinical models. Nat. Commun. 16, 706 (2025).
Reiss, K. A. et al. CAR-macrophage therapy for HER2-overexpressing advanced solid tumors: a phase 1 trial. Nat. Med. 31, 1171–1182 (2025).
Huang, T., Bei, C., Hu, Z. & Li, Y. CAR-macrophage: breaking new ground in cellular immunotherapy. Front. Cell. Dev. Biol. 12, 1464218 (2024).
Liu, M. et al. CAR-Macrophages and CAR-T cells synergistically kill tumor cells in vitro. Cells 11, 3692 (2022).
Hadiloo, K., Taremi, S., Heidari, M. & Esmaeilzadeh, A. The CAR macrophage cells, a novel generation of chimeric antigen-based approach against solid tumors. Biomark. Res. 11, 103 (2023).
Kloosterman, D. J. & Akkari, L. Macrophages at the interface of the co-evolving cancer ecosystem. Cell 186, 1627–1651 (2023).
Duan, Z. & Luo, Y. Targeting macrophages in cancer immunotherapy. Signal. Transduct. Target. Ther. 6, 127 (2021).
Duan, Z., Li, Z., Wang, Z., Chen, C. & Luo, Y. Chimeric antigen receptor macrophages activated through TLR4 or IFN-γ receptors suppress breast cancer growth by targeting VEGFR2. Cancer Immunol. Immunother. 72, 3243–3257 (2023).
Walbaum, S. et al. Complement receptor 3 mediates both sinking phagocytosis and phagocytic cup formation via distinct mechanisms. J. Biol. Chem. 296, 100256 (2021).
McInturff, J. E., Modlin, R. L. & Kim, J. The role of Toll-like receptors in the pathogenesis and treatment of dermatological disease. J. Invest. Dermatology. 125, 1–8 (2005).
Sharma, V., Sharma, P. & Singh, T. G. Mechanistic insights on TLR-4 mediated inflammatory pathway in neurodegenerative diseases. Pharmacol. Rep. 76, 679–692 (2024).
Clevers, H., Alarcon, B., Wileman, T. & Terhorst, C. The T cell receptor/CD3 complex: a dynamic protein ensemble. Annu. Rev. Immunol. 6, 629–662 (1988).
Lan, J. et al. Structure of the SARS-CoV-2 Spike receptor-binding domain bound to the ACE2 receptor. Nature 581, 215–220 (2020).
Bettini, M. L. et al. Cutting edge: CD3 ITAM diversity is required for optimal TCR signaling and thymocyte development. J. Immunol. 199, 1555–1560 (2017).
Anania, J. C., Chenoweth, A. M., Wines, B. D. & Hogarth, P. M. The human FcγRII (CD32) family of leukocyte FcR in health and disease. Front Immunol 10, (2019).
Hickman, E. et al. Expanded characterization of in vitro polarized M0, M1, and M2 human monocyte-derived macrophages: bioenergetic and secreted mediator profiles. PLOS ONE. 18, e0279037 (2023).
Suleimanov, S. K. et al. Radical-Generating Activity, Phagocytosis, and mechanical properties of four phenotypes of human macrophages. Int. J. Mol. Sci. 25, 1860 (2024).
Affandi, A. J. et al. CD169 defines activated CD14 + Monocytes with enhanced CD8 + T cell activation capacity. Front Immunol 12, (2021).
Brossart, P. The role of antigen spreading in the efficacy of immunotherapies. Clin. Cancer Res. 26, 4442–4447 (2020).
Gulley, J. L. et al. Role of antigen spread and distinctive characteristics of immunotherapy in cancer treatment. JNCI: J. Natl. Cancer Inst. 109, djw261 (2017).
Liang, Y., Xu, Q. & Gao, Q. Advancing CAR-based immunotherapies in solid tumors: CAR- macrophages and neutrophils. Front. Immunol. 14, 1291619 (2023).
Lu, J. et al. CAR macrophages: a promising novel immunotherapy for solid tumors and beyond. Biomark. Res. 12, 86 (2024).
Saha, S. et al. High expression of mesothelin in plasma and tissue is associated with poor prognosis and promotes invasion and metastasis in gastric cancer. Adv. Cancer Biology - Metastasis. 7, 100098 (2023).
Lv, J. & Li, P. Mesothelin as a biomarker for targeted therapy. Biomark. Res. 7, 18 (2019).
Faust, J. R., Hamill, D., Kolb, E. A., Gopalakrishnapillai, A. & Barwe, S. P. Mesothelin: an immunotherapeutic target beyond solid tumors. Cancers 14, 1550 (2022).
Chung, J. Y. et al. Rapid CAR Screening and circRNA-driven CAR-NK Cells for Persistent Shed-resistant Immunotherapy. 08.19.671003 Preprint at (2025). https://doi.org/10.1101/2025.08.19.671003 (2025).
Chowdhury, P. S., Viner, J. L., Beers, R. & Pastan, I. Isolation of a high-affinity stable single-chain Fv specific for mesothelin from DNA-immunized mice by phage display and construction of a recombinant immunotoxin with anti-tumor activity. Proceedings of the National Academy of Sciences 95, 669–674 (1998).
Chowdhury, P. S. & Pastan, I. Improving antibody affinity by mimicking somatic hypermutation in vitro. Nat. Biotechnol. 17, 568–572 (1999).
Lucas, M., Zhang, X., Prasanna, V. & Mosser, D. M. ERK activation following macrophage FcγR ligation leads to chromatin modifications at the IL-10 Locus1. J. Immunol. 175, 469–477 (2005).
Li, J., Chen, P. & Ma, W. The next frontier in immunotherapy: potential and challenges of CAR-macrophages. Experimental Hematol. Oncol. 13, 76 (2024).
Morva, A., Arroyo, A. B., Andreeva, L. & Tapia-Abellán, A. Luengo-Gil, G. Unleashing the power of CAR-M therapy in solid tumors: a comprehensive review. Front. Immunol. 16, 1615760 (2025).
Huo, Y. et al. M1 polarization enhances the antitumor activity of chimeric antigen receptor macrophages in solid tumors. J. Transl Med. 21, 225 (2023).
Zhang, W. et al. Macrophage polarization in the tumor microenvironment: emerging roles and therapeutic potentials. Biomed. Pharmacother. 177, 116930 (2024).
Sterner, R. C. & Sterner, R. M. CAR-T cell therapy: current limitations and potential strategies. Blood Cancer J. 11, 69 (2021).
Feucht, J. et al. Calibration of CAR activation potential directs alternative T cell fates and therapeutic potency. Nat. Med. 25, 82–88 (2019).
Ciesielska, A., Matyjek, M. & Kwiatkowska, K. TLR4 and CD14 trafficking and its influence on LPS-induced pro-inflammatory signaling. Cell. Mol. Life Sci. 78, 1233–1261 (2021).
Wang, P. et al. Chimeric antigen receptor with novel intracellular modules improves antitumor performance of T cells. Signal. Transduct. Target. Ther. 10, 20 (2025).
Genin, M., Clement, F., Fattaccioli, A., Raes, M. & Michiels, C. M1 and M2 macrophages derived from THP-1 cells differentially modulate the response of cancer cells to Etoposide. BMC Cancer. 15, 577 (2015).
Lee, H. N. et al. Novel FRET-based immunological synapse biosensor for the prediction of chimeric antigen Receptor-T cell function. Small Methods. 9, 2401016 (2025).
Kang, C. K. et al. Broad humoral and cellular immunity elicited by one-dose mRNA vaccination 18 months after SARS-CoV-2 infection. BMC Med. 20, 181 (2022).
He, J. et al. Human immunodeficiency virus type 1 viral protein R (Vpr) arrests cells in the G2 phase of the cell cycle by inhibiting p34cdc2 activity. J. Virol. 69, 6705–6711 (1995).
Connor, R. I., Chen, B. K., Choe, S. & Landau, N. R. Vpr is required for efficient replication of human immunodeficiency virus type-1 in mononuclear phagocytes. Virology 206, 935–944 (1995).
Kang, C. K. et al. Longitudinal analysis of human memory T-Cell response according to the severity of illness up to 8 months after severe acute respiratory syndrome coronavirus 2 infection. J. Infect. Dis. 224, 39–48 (2021).
Kang, C. K. et al. Distinct immune response at 1 year Post-COVID-19 according to disease severity. Front. Immunol. 13, 830433 (2022).
Acknowledgements
English grammar was reviewed and revised by ChatGPT, a language model developed by OpenAI in San Francisco, CA, USA.
Funding
This work was supported in part by the Creative-Pioneering Researchers Program through Seoul National University (to C.-H. L. and H.-R. Kim) and the Bio & Medical Technology Development Program of the National Research Foundation (NRF) & funded by the Korean government (MSIT) (RS-2021-NR056559 to H.-R. Kim, RS-2024-00440679 to C.-H.L.).
Author information
Authors and Affiliations
Contributions
C.-H.L. and J.S.H. conceived and designed the project. J.S.H., S.J.L., and Y.J.K. performed the experiments. C.-H.L., H.R.K., and J.S.H. analyzed the data. C.-H.L., H.R.K., J.S.H., C.K.K., W.B.P., and H.M.S. wrote the manuscript. All authors have reviewed the manuscript and approved its submission.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Hong, J., Lee, S., Kim, Y. et al. Optimization of THP-1-CAR monocytes utilizing CD32a signaling phagocytosis for antigen-specific T cell activation. Sci Rep 16, 8175 (2026). https://doi.org/10.1038/s41598-026-39406-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-39406-6