Abstract
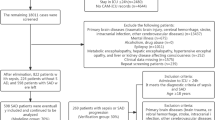
Sepsis-induced hepatic dysfunction contributes significantly to poor clinical outcomes. Although the Fibrosis-4 (FIB-4) index is established for assessing chronic liver fibrosis, its utility as a prognostic marker for acute sepsis mortality—particularly in patients without pre-existing liver disease—remains unclear. We aimed to evaluate the predictive value of FIB-4 in sepsis using two large, multi-center databases.We conducted a multicenter retrospective study using two large critical care databases: MIMIC-IV (n = 13,983) and eICU (n = 9,976). Sepsis was defined based on established clinical criteria. Missing values were handled using multiple imputation to preserve data integrity. The optimal FIB-4 cutoff points were determined via outcome-based stratification (1.25). Patients were categorized into high and low FIB-4 groups accordingly. We applied restricted cubic spline (RCS) modeling to evaluate nonlinear trends, followed by weighted Cox regression to determine independent associations with in-hospital mortality. Kaplan–Meier survival curves assessed time-to-event differences, while subgroup analyses, ROC curves, and sensitivity analyses explored effect consistency and underlying biological pathways. Across 23,959 sepsis patients from the MIMIC-IV and eICU databases, elevated FIB-4 levels were significantly associated with in-hospital mortality (P < 0.001). An FIB-4 index > 1.25 served as an independent risk factor for mortality (adjusted HRs: 1.38–1.55) and outperformed traditional SOFA and APACHE scores in prognostic discrimination. Kaplan–Meier curves showed significantly reduced survival in the high FIB-4 group. Importantly, sensitivity analyses excluding patients with known liver disease, suspected MASLD, or cardiac admissions confirmed the robustness of these findings. The FIB-4 index serves as a robust, independent prognostic marker for in-hospital mortality in sepsis patients, outperforming traditional scores such as SOFA and APACHE II in predictive accuracy. Crucially, its prognostic value persists even after excluding patients with pre-existing liver disease or acute cardiogenic hepatic congestion, suggesting it reflects broader sepsis-induced physiological derangements rather than solely baseline hepatic fibrosis. Given its simplicity and reliance on routinely available laboratory parameters, FIB-4 offers a practical, accessible tool for early risk stratification in the intensive care setting.
Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article and its supplementary information files.
References
Li, A. et al. Epidemiology, management, and outcomes of sepsis in ICUs among countries of differing national wealth across Asia. Am. J. Respir. Crit. Care Med. 206(9), 1107–1116 (2022).
La Via, L. et al. The global burden of sepsis and septic shock. Epidemiologia (Basel) 5(3), 456–478 (2024).
Dong, R. et al. Temporal trends of sepsis-related mortality in China, 2006–2020: a population-based study. Ann Intensive Care. 13(1), 71 (2023).
Dronamraju, S. et al. Comparison of PIRO, APACHE IV, and SOFA scores in predicting outcome in patients with sepsis admitted to intensive care unit: A two-year cross-sectional study at rural teaching hospital. Indian J. Crit. Care Med. 26(10), 1099–1105 (2022).
Xu, X. L. et al. The role of fibrosis index FIB-4 in predicting liver fibrosis stage and clinical prognosis: A diagnostic or screening tool?. J. Formos. Med. Assoc. 121(2), 454–466 (2022).
Mirijello, A. et al. The Fibrosis-4 index predicts all-cause mortality in a cohort of patients at high cardiovascular risk partly through glomerular filtration rate reduction. Nutr. Metab. Cardiovasc. Dis. 35(1), 103768 (2025).
Karagiannakis, D. S. et al. Elevated FIB-4 is associated with higher rates of cardiovascular disease and extrahepatic cancer history in patients with Type 2 Diabetes Mellitus. Biomedicines https://doi.org/10.3390/biomedicines12040823 (2024).
Gaggini, M. et al. FIB-4 index and neutrophil-to-lymphocyte-ratio as death predictor in Coronary Artery Disease patients. Biomedicines https://doi.org/10.3390/biomedicines11010076 (2022).
Bielecka-Dabrowa A, Sakowicz A, Banach M, Slot M. An Elevated FIB-4 Score is associated with the severity of heart failure. European Heart Journal. 2024;45(Supplement_1).
Schleicher, E. M. et al. A higher FIB-4 index is associated with an increased incidence of renal failure in the general population. Hepatol. Commun. 6(12), 3505–3514 (2022).
Albayrak, T. & Yuksel, B. Prognostic value of fibrosis 4 (FIB-4) index in sepsis patients. J. Pers. Med. https://doi.org/10.3390/jpm14050531 (2024).
Johnson, A. E. W. et al. MIMIC-IV, a freely accessible electronic health record dataset. Sci Data. 10(1), 1 (2023).
Zheng, R. et al. Association between triglyceride-glucose index and in-hospital mortality in critically ill patients with sepsis: Analysis of the MIMIC-IV database. Cardiovasc. Diabetol. 22(1), 307 (2023).
Singer, M. et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 315(8), 801–810 (2016).
Hu, W. et al. Identification of indications for albumin administration in septic patients with liver cirrhosis. Crit Care. 27(1), 300 (2023).
Kamada, Y. et al. SWOT analysis of noninvasive tests for diagnosing NAFLD with severe fibrosis: an expert review by the JANIT Forum. J Gastroenterol. 58(2), 79–97 (2023).
Vallet-Pichard, A. et al. FIB-4: An inexpensive and accurate marker of fibrosis in HCV infection. Comparison with liver biopsy and Fibrotest. Hepatology 46(1), 32–36 (2007).
Zhang, Z., Ho, K. M. & Hong, Y. Machine learning for the prediction of volume responsiveness in patients with oliguric acute kidney injury in critical care. Crit Care. 23(1), 112 (2019).
Barichello, T., Generoso, J. S., Singer, M. & Dal-Pizzol, F. Biomarkers for sepsis: more than just fever and leukocytosis-a narrative review. Crit Care. 26(1), 14 (2022).
Schreiner, A. D. et al. Advanced liver fibrosis and the metabolic syndrome in a primary care setting. Diabetes Metab Res Rev. 37(8), e3452 (2021).
Sumida, Y. et al. FIB-4 first in the diagnostic algorithm of Metabolic-Dysfunction-Associated Fatty Liver Disease in the era of the global Metabodemic. Life https://doi.org/10.3390/life11020143 (2021).
Shi, Y. et al. Association between liver fibrosis and the in-hospital mortality in patients with sepsis-induced coagulopathy. BMC Infect Dis. 24(1), 1136 (2024).
Rungta, S., Kumari, S., Deep, A., Verma, K. & Swaroop, S. APRI and FIB-4 performance to assess liver fibrosis against predefined Fibroscan values in chronic hepatitis C virus infection. J Family Med Prim Care. 10(11), 4082–4088 (2021).
Xu, X., Yang, T., An, J., Li, B. & Dou, Z. Liver injury in sepsis: manifestations, mechanisms and emerging therapeutic strategies. Front Immunol. 16, 1575554 (2025).
Chen, J. W. et al. Sepsis-associated liver injury: Mechanisms and potential therapeutic targets. World J Gastroenterol. 30(42), 4518–4522 (2024).
Beyer, D. et al. The liver in sepsis: molecular mechanism of liver failure and their potential for clinical translation. Mol Med. 28(1), 84 (2022).
Wang, T. et al. Relationship between coagulopathy score and survival in critically ill patients with liver cirrhosis and sepsis: A retrospective study. BMC Infect. Dis. 25(1), 418 (2025).
Liu, S. et al. Lactate and lactylation in sepsis: A comprehensive review. J. Inflamm. Res. 17, 4405–4417 (2024).
Anderko, R. R. et al. Sepsis with liver dysfunction and coagulopathy predicts an inflammatory pattern of macrophage activation. Intensive Care Med Exp. 10(1), 6 (2022).
Sun, Z. et al. Potential biomarker for diagnosis and therapy of sepsis: Lactylation. Immun. Inflamm. Dis. 11(10), e1042 (2023).
Funding
This work did not receive any funding.
Author information
Authors and Affiliations
Contributions
**Xiangli Kong** : Methodology, Investigation, Data curation, Software, Writing—original draft. **Bin Jiang** and **Cuiping Xu** : Formal analysis, Software, Data curation. **Xiaohong Zhou** : Data curation, Methodology, Investigation. **Feifei He:** Conceptualization, Validation, Supervision, Writing—review & editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Kong, X., Jiang, B., Xu, C. et al. Prognostic value of the fibrosis-4 index for predicting in-hospital mortality in sepsis patients: evidence from MIMIC-IV and eICU databases. Sci Rep (2026). https://doi.org/10.1038/s41598-026-42522-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-42522-y