Abstract
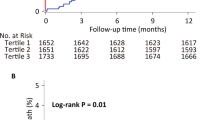
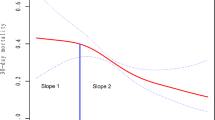
Restrictive red blood cell transfusion strategies (hemoglobin trigger 7.0–8.0 g/dL) are well established, yet existing evidence addresses primarily when to initiate transfusion. The optimal achieved post-transfusion hemoglobin level in critically ill patients with severe anemia (pre-transfusion hemoglobin ≤ 8.0 g/dL) remains unknown. We analyzed 3,710 intensive care unit admissions in the Medical Information Mart for Intensive Care IV (MIMIC-IV; 3,339 training, 371 test) and externally validated findings in 4,719 admissions from the eICU Collaborative Research Database. Eligible subjects received red blood cells within 48 h of ICU admission, had a pre-transfusion hemoglobin ≤ 8.0 g/dL, and had no additional transfusions between 48 h and seven days. Using a double machine learning causal forest, we estimated treatment effects for post-transfusion hemoglobin targets from 8.0 to 14.0 g/dL relative to 8.0 g/dL, identified the target with the lowest predicted in-hospital mortality, evaluated subgroups, and modeled predictors of targets below 10.0 g/dL. Dose–response curves were U-shaped in all datasets. The estimated optimal hemoglobin was 11.0 g/dL in the training set, 10.9 g/dL in the test set, and 11.0 g/dL in external validation. Estimated optimal levels near 11.0 g/dL were consistent across chronic kidney disease, end-stage kidney disease, myocardial infarction, congestive heart failure, hypertension, and diabetes. Lower baseline hemoglobin and lower estimated glomerular filtration rate were associated with lower individualized optimal levels. Indicators of inflammation or hemodynamic instability, including hypotension, fever, leukocytosis, hyperlactatemia, acidosis, and vasopressor requirements, were associated with estimated optimal achieved post-transfusion hemoglobin levels below 10.0 g/dL. Among ICU subjects transfused under a restrictive trigger (hemoglobin ≤ 8.0 g/dL), an achieved post-transfusion hemoglobin around 11.0 g/dL was associated with the lowest predicted in-hospital mortality.
Similar content being viewed by others
Acknowledgements
Not applicable.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical Approval and Consent to participate
This study was a secondary analysis of de-identified, publicly available data and was exempt from review by the Institutional Review Board of Korea University Guro Hospital (No. K2025-1397-001). As all data are anonymized and freely accessible, individual informed consent was not required
Consent for publication
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kang, M.W., Yun, S., Song, S.M. et al. Impact of post-transfusion hemoglobin levels on survival in critically Ill patients: a machine learning–based causal inference analysis. Sci Rep (2026). https://doi.org/10.1038/s41598-026-50363-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-50363-y