Abstract
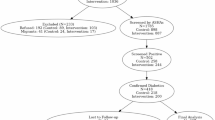
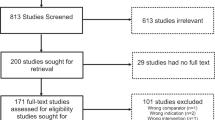
This study evaluated the effectiveness and implementation of a telecare-enhanced hybrid consultation model for diabetes management in public general outpatient clinics. In a single-blind, non-inferiority randomized controlled trial involving 786 adults with type 2 diabetes across seven clinics, participants were assigned to either a hybrid care group, receiving alternating telecare and in-person consultations, or a control group, receiving in-person care only, over 84 weeks. The intervention group (IG) showed comparable HbA1c levels to the control group (CG). Blood pressure readings were consistently lower in the IG, and medication adherence remained stable, unlike the CG, which experienced a midline decline. All clinics sustained the telecare model post-trial. Implementation was facilitated by strong leadership and a reliable digital infrastructure, though challenges such as digital literacy and staff workload remained. The model proved effective, comparable cost, and feasible within a public healthcare setting.
Similar content being viewed by others
Data availability
All proposals for data use will need the approval of the study team before any data are released. Usage rights for the raw data are retained by the study team. De-identified individual participant data will be available upon reasonable request to researchers. Requests should be directed to the corresponding author via email, accompanied by a detailed research proposal. Access will be granted following the approval of the proposal and the signing of a data access agreement. Only data from participants who have consented to share their data will be provided. Data sharing will be authorized following proposal approval and the execution of a signed data access agreement, strictly for scientific use.
References
Protection, C.f.H. Non-communicable diseases watch. (The Government of the Hong Kong Special Administrative Region, 2018).
Organization, W.H. Diabetes: key facts. (2020).
Long, A. N. & Dagogo-Jack, S. Comorbidities of diabetes and hypertension: mechanisms and approach to target organ protection. J. Clin. Hypertens. 13, 244–251 (2011).
McGhee, S. M., Thomas, G. N., Schooling, C. M., Chau, J. & Wong, L. C. Economic burden of diabetes related to excess body weight in Hong Kong. Hong. Kong Med. J. 20, 5–7 (2014).
Lian, J. et al. Long-term cost-effectiveness of a Patient Empowerment Programme for type 2 diabetes mellitus in primary care. Diab. Obes. Metab. 21, 73–83 (2019).
Lee CP, L.S., Leung MKW, Hui EMT, Li PKT. A family medicine specialist led diabetes mellitus clinic in a general out-patient clinic. Hong Kong Practitioner 39, 38-42 (2017).
Wan, E. Y. F. et al. Five-year effectiveness of the multidisciplinary risk assessment and management programme-diabetes mellitus (RAMP-DM) on diabetes-related complications and health service uses-a population-based and propensity-matched cohort study. Diab. Care 41, 49–59 (2018).
Sood, A., Watts, S. A., Johnson, J. K., Hirth, S. & Aron, D. C. Telemedicine consultation for patients with diabetes mellitus: a cluster randomised controlled trial. J. Telemed. Telecare 24, 385–391 (2018).
Freeman, K. A., Duke, D. C. & Harris, M. A. Behavioral health care for adolescents with poorly controlled diabetes via Skype: does working alliance remain intact? J. Diab. Sci. Technol. 7, 727–735 (2013).
Mello Delphino Machado, T., Ferreira Santana, R. & Serra Hercules, A.B. Telecare central: nursing intervention perspective. Cogitare Enfermagem 25(2020).
Shea, S. et al. A randomized trial comparing telemedicine case management with usual care in older, ethnically diverse, medically underserved patients with diabetes mellitus: 5 year results of the IDEATel study. J. Am. Med. Inform. Assoc. 16, 446–456 (2009).
Zhai, Y. -k, Zhu, W. -j, Cai, Y. -l, Sun, D. -x & Zhao, J. Clinical- and cost-effectiveness of telemedicine in type 2 diabetes mellitus: a systematic review and meta-analysis. Medicine 93, e312 (2014).
Lee, J. Y. et al. Using telemedicine to support care for people with type 2 diabetes mellitus: a qualitative analysis of patients’ perspectives. BMJ Open 9, e026575 (2019).
Scott, S. N., Fontana, F. Y., Züger, T., Laimer, M. & Stettler, C. Use and perception of telemedicine in people with type 1 diabetes during the COVID-19 pandemic-Results of a global survey. Endocrinol. Diab. Metab. 4, e00180 (2021).
Mignerat, M., Lapointe, L. & Vedel, I. Using telecare for diabetic patients: a mixed systematic review. Health Policy Technol. 3, 90–112 (2014).
Greenhalgh, T. et al. Real-world implementation of video outpatient consultations at macro, meso, and micro levels: mixed-method study. J. Med Internet Res 20, e150 (2018).
Seifert, A., Cotten, S. R. & Xie, B. A double burden of exclusion? digital and social exclusion of older adults in times of COVID-19. J. Gerontology: Ser. B 76, e99–e103 (2020).
Wong, A. K. C. et al. Exploring Desired Features of mobile health applications for patients with diabetes to enhance engagement and self-management: a qualitative study. JMIR Diab. 10, e69176 (2025).
Lam, E. T., Lam, C. L., Fong, D. Y. & Huang, W. W. Is the SF-12 version 2 Health Survey a valid and equivalent substitute for the SF-36 version 2 Health Survey for the Chinese? J. Eval. Clin. Pr. 19, 200–208 (2013).
Berliner, J. L., Brodke, D. J., Chan, V., SooHoo, N. F. & Bozic, K. J. Can preoperative patient-reported outcome measures be used to predict meaningful improvement in function after TKA? Clin. Orthop. Relat. Res 475, 149–157 (2017).
Fowe, I. E. Evaluating organizational readiness for change in the implementation of telehealth and mobile health interventions for chronic disease management. AMIA Jt Summits Transl. Sci. Proc. 2021, 210–219 (2021).
Schwamm, L. H. et al. Recommendations for the implementation of telehealth in cardiovascular and stroke care: a policy statement from the American Heart Association. Circulation 135, e24–e44 (2017).
Glasgow, R. E., Vogt, T. M. & Boles, S. M. Evaluating the public health impact of health promotion interventions: the RE-AIM framework. Am. J. Public Health 89, 1322–1327 (1999).
Van Deursen, A. J. & Van Dijk, J. A. The digital divide shifts to differences in usage. N. media Soc. 16, 507–526 (2014).
HA Annual Plan 2024-2025. (Hospital Authority, 2024).
Curran, G. M., Bauer, M., Mittman, B., Pyne, J. M. & Stetler, C. Effectiveness-implementation hybrid designs: combining elements of clinical effectiveness and implementation research to enhance public health impact. Med. Care 50, 217–226 (2012).
Wong, A. K. C. et al. Outcomes of a risk assessment and management program using telecare consultation among patients with diabetes mellitus in general out-patient clinic: a hybrid effectiveness-implementation study protocol. Ann. Med 55, 2262088 (2023).
Authority, H. Hospital Authority Statistical Report 2018-19: New Territories West Cluster. (2019).
Munch, L. et al. Shared care management of patients with type 2 diabetes across the primary and secondary healthcare sectors: study protocol for a randomised controlled trial. Trials 17, 277 (2016).
Cheng, L. et al. Effectiveness of a patient-centred, empowerment-based intervention programme among patients with poorly controlled type 2 diabetes: a randomised controlled trial. Int. J. Nurs. Stud. 79, 43–51 (2018).
Munch, L. et al. Management of people with Type 2 diabetes shared between a specialized outpatient clinic and primary health care is noninferior to management in a specialized outpatient clinic: a randomized, noninferiority trial. Diabet. Med. 36, 854–861 (2019).
Durlak, J. A. & DuPre, E. P. Implementation matters: a review of research on the influence of implementation on program outcomes and the factors affecting implementation. Am. J. Community Psychol. 41, 327–350 (2008).
group, R.-A.w. Checklist for inclusion of RE-AIM issues by RE-AIM dimension. (2012).
Derr, R., Garrett, E., Stacy, G. A. & Saudek, C. D. Is HbA(1c) affected by glycemic instability? Diab. Care 26, 2728–2733 (2003).
Prevention., C.f.D.C.a. About adult BMI. (2017).
Zhou, Y., Liao, L., Sun, M. & He, G. Self-care practices of Chinese individuals with diabetes. Exp. Ther. Med 5, 1137–1142 (2013).
Yin, X., Savage, C., Toobert, D., Wei, P. & Whitmer, K. Adaptation and testing of instruments to measure diabetes self-management in people with type 2 diabetes in mainland China. J. Transcult. Nurs. 19, 234–242 (2008).
Heerman, W. J. et al. Food insecurity is associated with diabetes self-care behaviours and glycaemic control. Diabet. Med. 33, 844–850 (2016).
Kripalani, S., Risser, J., Gatti, M. E. & Jacobson, T. A. Development and evaluation of the Adherence to Refills and Medications Scale (ARMS) among low-literacy patients with chronic disease. Value Health 12, 118–123 (2009).
Montazeri, A. et al. The 12-item medical outcomes study short form health survey version 2.0 (SF-12v2): a population-based validation study from Tehran, Iran. Health Qual. Life Outcomes 9, 12 (2011).
Wen, K. Y. et al. Developing and validating a model to predict the success of an IHCS implementation: the Readiness for Implementation Model. J. Am. Med. Inf. Assoc. 17, 707–713 (2010).
Wu, S. F. et al. Self-efficacy, outcome expectations and self-care behaviour in people with type 2 diabetes in Taiwan. J. Clin. Nurs. 16, 250–257 (2007).
Glasgow, R. E. et al. RE-AIM planning and evaluation framework: adapting to new science and practice with a 20-year review. Front Public Health 7, 64 (2019).
Braun, V. & Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 3, 77–101 (2006).
Cane, J., O’Connor, D. & Michie, S. Validation of the theoretical domains framework for use in behaviour change and implementation research. Implement. Sci. 7, 37 (2012).
Gale, N. K., Heath, G., Cameron, E., Rashid, S. & Redwood, S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med. Res. Methodol. 13, 1–8 (2013).
Ma, Z. & Wu, M. The Psychometric Properties of the Chinese eHealth Literacy Scale (C-eHEALS) in a Chinese Rural Population: Cross-Sectional Validation Study. J. Med Internet Res 21, e15720 (2019).
Acknowledgements
This study was funded by the Health and Medical Research Fund, Health Bureau, Hong Kong (Ref: 18191221). We extend our heartfelt thanks to the Hong Kong Hospital Authority and the seven GOPCs within the New Territories West Cluster for their organization and support, which provided the foundation for the design and implementation of our eRAMP services. We are deeply grateful to the multidisciplinary team, including doctors, nurses, optometrists, dietitians, podiatrists, physiotherapists, and patient care assistants, whose continuous cooperation, support, and collaboration were essential for the successful implementation and validation of our hybrid model. We sincerely thank all of the patients who participated in this study; their trust, acceptance, participation, and feedback were crucial to achieving our research objectives. Additionally, we express our appreciation to the HA Go technical team for their essential technical support and continuous optimization of our telecare model.
Author information
Authors and Affiliations
Contributions
A.W. and F.W. developed the conception and design of the initial study. A.W. was responsible for obtaining funding. A.W., S.C., and L.L. performed the statistical analyses, interpreted the data, and drafted the manuscript. J.L., D.T., M.C., M.W., B.W., V.H., C.T., W.H., and S.C. provided a critical review of the manuscript and intellectual input on the study design, methodology, and evaluation. All authors contributed to, reviewed, and approved the manuscript. All authors were responsible for the decision to submit for publication.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Wong, A.K.C., Chen, SC., Wong, F.K.Y. et al. Evaluating eRAMP telecare for diabetes in outpatient clinics: a hybrid effectiveness-implementation study. npj Digit. Med. (2026). https://doi.org/10.1038/s41746-026-02424-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41746-026-02424-9