Abstract
Purpose
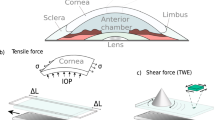
The eyeball and, in particular, the cornea deform in vitro by the application of a distending force like other visco-elastic tissue. If the force is large enough, the cornea strains beyond the elastic range, and a permanent deformation occurs. Such permanent strain is referred to as ‘plastic’ strain. The phenomenon, however, has never been observed or produced on living tissue. This report seeks to demonstrate that the central radius of a patient’s cornea can be altered in a controlled manner designed to correct refractive errors.
Methods
To plastically deform the living cornea, we applied a vacuum to the cornea of eight rabbits and five human eyes with a novel device. This device consists of a chamber of 11 mm in diameter. The chamber is radially divided into four interconnected sub-chambers.
Results
Here we show that a strain can be achieved in vivo with a force produced by the application of the specially designed chamber where air is evacuated. An anatomical modification of the cornea of humans and rabbits was achieved. The deformation of the cornea was plastic, and therefore permanent.
Conclusions
The method described here–Pneumatic Keratology– can be used to alter the cornea by non-invasive means. A vacuum chamber with radial openings alters the collagen fibers in the stroma and flattens the cornea. A flatter cornea corrects or reduces myopia.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Boyce BL, Jones RE, Nguyen TD, Grazier JM . Stress-controlled viscoelastic tensile response of bovine cornea. J Biomech 2007; 40: 2367–2376.
Elsheikh A, Anderson K . Comparative study of corneal strip extensiometry and inflation tests. J R Soc Interface 2005; 2: 177–185.
Nguyen TD, Jones RE, Boyce BL . A nonlinear anisotropic viscoelastic model for the tensile behavior of the corneal stroma. J Biomech Eng 2008; 130: 041020.
Hatami-Marbini H, Rahimi A . Effects of bathing solution on tensile properties of the cornea. Exp Eye Res 2014; 120: 103–108.
Hoeltzel DA, Alman P, Buzard K, Choe K . Strip extensiometry for comparison of the mechanical response of bovine, rabbit, and human corneas. J Biomech Eng 1992; 114: 202–215.
Boschetti F, Triaca V, Spinelli L, Pandolfi A . Mechanical characterization of porcine corneas. J Biomech Eng 2012; 134: 031003.
Boyce BL, Grazier JM, Jones RE, Nguyen TD . Full-field deformation of bovine cornea under constrained inflation conditions. Biomaterials 2008; 29: 3896–3904.
Elsheikh A, Wang D, Pye D . Determination of the modulus of elasticity of the human cornea. J Refract Surg 2007; 23: 808–818.
Elsheikh A, Wang D, Rama P, Campanelli M . Experimental assessment of human corneal hysteresis. Curr Eye Res 2008; 33: 205–213.
Hennighausen H, Feldma ST, Bille JF, McCulloch AD . Anterior-posterior strain variation in normally hydrated and swollen rabbit cornea. Invest Ophthalmol Vis Sci 1998; 39: 253–262.
Shin TJ, Vito RP, Johnson LW, McCarey BE . The distribution of strain in the human cornea. J Biomech 1997; 30: 497–503.
Jue B, Maurice DM . The mechanical properties of the rabbit and human cornea. J Biomech 1986; 19: 847–853.
Rowsey JJ, Balyeat HD, Monlux R, Holladay J, Waring GO, Lynn MJ . Prospective evaluation of radial keratotomy. Ophthalmology 1988; 95: 322–334.
Angel LK, Rob RM, Berson FG . Visual prognosis in patients with ruptures in Descement´s membrane due to forceps injury. Arch Ophthalmol 1981; 99: 2137.
Hamed Sayed AA, Solouma NH, El-Berry AA, Kadah YM . Finite element models for computer simulation of intrastromal photorefractive keratectomy. J Mech Med Biol 2011; 11: 1255–1270.
Slettedal JK, Ringvold A . Correlation between corneal and ambient temperature with particular focus on polar conditions. Acta Ophthalmol 2015; 93 (5): 422–426.
Fabiani C, Li Voti R, Rusciano D, Mutolo MG, Pescosolido N . Relationship between corneal temperature and intraocular pressure in healthy individuals: a clinical thermographic analysis. J Ophthalmol 2016; 2016: 3076031.
Greene PR, McMahon TA . Scleral creep vs. temperature and pressure in vitro. Exp Eye Res 1979; 29: 527–537.
Ku DN, Greene PR . Scleral creep in vitro resulting from cyclic preasure pulses: applications to myopia. Am J Optom Physiol Opt 1981; 58: 528–535.
Lombardo G, Serrao S, Rosati M, Lombardo M . Analysis of the viscoelastic properties of the human cornea using scheimpflug imaging in inflation experiment of eye globes. PLoS One 2014; 9: e112169.
Uchio E, Ohno S, Kudoh J, Aoki K, Kisielewicz LT . Simulation model of an eyeball based on finite element analysis on a supercomputer. Br J Ophthalmol 1999; 83: 1106–1111.
Ward B, Thompson FB The Myopias: Pathogenesis and Pathophysiology In Myopia Surgery. Macmillan Publishing: New York, NY, USA, 1990; 1–30.
Medina A . The progression of corrected myopia. Graefes Arch Clin Exp Ophthalmol 2015; 253: 1273–1277.
Fyodorov SN, Durnev VV . Operation of dosage dissection of corneal circular ligament in cases of myopia of mild degree. Ann Ophthalmol 1979; 11: 1885–1890.
Trokel ST, Srinivasan R, Braren B . Excimer laser treatment on the cornea. Am J Ophthalmol 1983; 96: 710.
Gartry D, Muir MK, Marshall J . Excimer laser treatment of corneal surface pathology: a laboratory and clinical study. Br J Ohthalmol 1991; 75: 258–265.
Pallikaris IG, Papatzanaki ME, Siganos DS, Tsilimbaris MK . A corneal flap technique for laser in situ keratomileusis. Human studies. Arch Ophthalmol 1991; 109: 1699–1702.
AlSamman AH . Anterior chamber foldable phakic intra ocular lens safety and efficacy. J Clin Res Ophthalmol 2016; 3 (1): 011–017.
Curtin BJ . Physiolpathologic aspects of scleral stress-strain. Trans Am Ophthalmol Soc 1969; 67: 417–461.
Gloster J, Perkins ES, Pommier ML . Extensibility of strips of sclera and cornea. Br J Ophthalmol 1957; 41: 103–110.
Woo SL, Kobayashi AS, Schlegel WA, Lawrence C . Non linear material properties of intact cornea and sclera. Exp Eye Res 1972; 14: 29–39.
Greene PR . Stress amplification and plastic flow for spheroidal shells: Applications to myopia. Rheol Acta 1987; 26: 479–484.
Acknowledgements
We are especially grateful to the Hospital Provincial, Valencia, Hospital de la Cruz Roja, Barcelona, Hospital Provincial, Castellon, Spain and the Centro de Microcirugia Ocular y Laser, Santo Domingo, Dominican Republic. The expert assistance of doctors Enrique Fariza, Cesar Villa, Victor Menezo, Jorge Lopez, Donald Sanders, David Brown, Del Valle, Rafael Feliz, Carlos Jimenez and Jordi Desola propelled this work. Further appreciation to Mary Goon for her writing assistance. This work was done at nonprofit institutions with no proprietary rights or interest. The author expects that other parties will use the results here to further develop and bring this technology to the market.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Eye website
Rights and permissions
About this article
Cite this article
Medina, A. Plastic modification of the cornea by pneumatic force corrects myopia: Pneumatic keratology. Eye 31, 1621–1627 (2017). https://doi.org/10.1038/eye.2017.123
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/eye.2017.123