Abstract
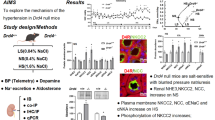
The distal nephron of the kidney has a central role in sodium and fluid homeostasis, and disruption of this homeostasis due to mutations of with-no-lysine kinase 1 (WNK1), WNK4, Kelch-like 3 (KLHL3), or Cullin 3 (CUL3) causes pseudohypoaldosteronism type II (PHAII), an inherited hypertensive disease. WNK1 and WNK4 activate the NaCl cotransporter (NCC) at the distal convoluted tubule through oxidative stress-responsive gene 1 (OSR1)/Ste20-related proline–alanine-rich kinase (SPAK), constituting the WNK–OSR1/SPAK–NCC phosphorylation cascade. The level of WNK protein is regulated through degradation by the CUL3–KLHL3 E3 ligase complex. In the normal state, the activity of WNK signaling in the kidney is physiologically regulated by sodium intake to maintain sodium homeostasis in the body. In patients with PHAII, however, because of the defective degradation of WNK kinases, NCC is constitutively active and not properly suppressed by a high salt diet, leading to abnormally increased salt reabsorption and salt-sensitive hypertension. Importantly, recent studies have demonstrated that potassium intake, insulin, and TNFα are also physiological regulators of WNK signaling, suggesting that they contribute to the salt-sensitive hypertension associated with a low potassium diet, metabolic syndrome, and chronic kidney disease, respectively. Moreover, emerging evidence suggests that WNK signaling also has some unique roles in metabolic, cardiovascular, and immunological organs. Here, we review the recent literature and discuss the molecular mechanisms of the WNK signaling pathway and its potential as a therapeutic target.
Similar content being viewed by others
Introduction
The kidneys have a crucial role in body fluid homeostasis and regulation of blood pressure. Their function is mediated by sodium reabsorption through several ion transporters present throughout the nephron. Although sodium transporters in the proximal nephron account for most sodium reabsorption, fine-tuning of sodium homeostasis in response to variable sodium intake is mediated by transporters in the distal nephron [1]. For instance, high salt intake is usually offset by decreased sodium reabsorption in the distal nephron, and aberrantly activated sodium reabsorption in persons on a high salt diet leads to hypervolemia and high blood pressure. Among sodium transporters in the distal nephron, the importance of thiazide-sensitive NaCl cotransporter (NCC) in the distal convoluted tubule (DCT) is illustrated by two monogenic diseases. One of these conditions, Gitelman syndrome, is an inherited salt-losing disease caused by a loss-of-function NCC mutation [2]. The other is pseudohypoaldosteronism type II (PHAII), in which inappropriately activated NCC results in salt-sensitive hypertension, hyperkalemia, and metabolic acidosis despite a normal glomerular filtration rate [3, 4]. Interestingly, however, gain-of-function mutations in NCC have not been found in PHAII patients. Instead, developments in genetics have led to the elucidation of the cause of this disease. In 2001, linkage analysis of a family of PHAII patients revealed that mutations in with-no-lysine kinase 1 (WNK1) and WNK4 genes cause PHAII [5]. Later, in 2012, the whole exome sequence method was used to identify two additional genes responsible for PHAII, Kelch-like 3 (KLHL3), and Cullin 3 (CUL3) [6, 7]. In this review, we describe (1) how these four gene products interact with each other to regulate blood pressure and electrolyte homeostasis, (2) the physiological regulatory mechanisms of WNK signaling and their roles in disease conditions, and (3) the newly discovered functions of WNK signaling in metabolic organs, such as adipose tissue and skeletal muscle.
Discovery of the WNK–OSR1/SPAK–NCC phosphorylation cascade
WNK kinase is a unique serine–threonine kinase in which the lysine (K) residue in the catalytic domain, that is found in the majority of kinases is not conserved [8]. In mammals, there are four WNK kinase family members (WNK1–4) [9]. WNK1 also has a kidney-specific isoform (KS-WNK1) that lacks a kinase domain (Fig. 1) [10,11,12].
Structures of the with-no-lysine kinase (WNK) signaling pathway components. a The conserved C-terminal (CCT) domain of oxidative stress-responsive gene 1 (OSR1)/Ste20-related proline–alanine–rich kinase (SPAK) interacts with the motif (RFxV/I) to bind WNK kinases and Na/Cl cotransporter (NCC). Upon this interaction, WNK kinases phosphorylate OSR1/SPAK at one threonine residue in the kinase domain and one serine residue in the S-motif. OSR1/SPAK phosphorylates NCC at three residues (T53, T58, and S71) in the N-terminal cytoplasmic domain. WNK kinases have a conserved Cl− binding pocket in the kinase domain. The PHAII-causing mutation D561A is located within the acidic motif of WNK4. b Interaction between WNK kinases, Kelch-like 3 (KLHL3), and Cullin 3 (CUL3). KLHL3 and CUL3 comprise the E3 ubiquitin ligase complex. The PHAII-causing mutation R528H is located within the Kelch repeat in KLHL3, which interacts with the acidic motif in WNK kinases. The BTB domain of KLHL3 binds to the N-terminus of CUL3. Exon 9-deleted mutant CUL3 has low affinity for the COP9 signalosome (CSN), leading to aberrant neddylation. CUL3 interacts with the ubiquitin-conjugated E2 enzyme via RING-box protein 1 (RBX1), catalyzing ubiquitin transfer to WNK kinases
Most WNK4 mutations identified in PHAII patients are in a motif named the “acidic motif” and gain-of-function mutations [5, 13, 14]. This acidic domain is located downstream of the N-terminal kinase domain and is well conserved within all WNK kinases. PHAII model mice that carry one of these WNK4 mutations (Wnk4D561A/+) exhibit increased WNK4 protein abundance and phosphorylated NCC levels (resulting in increased NCC activity), and they recapitulate the PHAII phenotype (salt-sensitive hypertension, hyperkalemia, and metabolic acidosis) [15, 16]. In contrast, WNK4-deficient mice show decreased NCC phosphorylation and manifested hypotension and a Gitelman-like phenotype [17, 18]. These observations indicate that WNK4 positively regulates NCC function.
WNK1 also positively regulates NCC function. PHAII-causing WNK1 mutations are large deletions in intron 1 that have been shown to increase WNK1 transcription in leukocytes of patients with PHAII, indicating that activation of WNK1 signaling causes PHAII [5]. In fact, a PHAII-causing WNK1 deletion mutant mouse model (WNK1+/FHHt) exhibits increased renal transcription of full-length (L-) WNK1 in the DCT and increased phosphorylation of NCC, suggesting that L-WNK1 is also a positive regulator of NCC [19]. On the other hand, the physiological functions of KS-WNK1 remain controversial; early investigations reported that KS-WNK1 is expressed predominantly in the DCT and antagonizes L-WNK1 [20, 21], but recent evidence suggests it has a positive effect on WNK signaling [22, 23].
Although WNK kinases (WNK1 and WNK4) positively regulate NCC, NCC is not a direct substrate of WNK kinases. However, two studies reported that two serine–threonine kinases, oxidative stress-responsive gene 1 (OSR1) and Ste20-related proline–alanine-rich kinase (SPAK), are direct substrates of WNK1 and WNK4 [24, 25]. Moreover, it has also been demonstrated that the C-terminal domains of OSR1 and SPAK interact with the RFx[V/I] motif in both WNK kinases and solute carrier family 12 (SLC12) transporters, including NCC (Fig. 1) [26, 27]. WNK kinases phosphorylate SPAK and OSR1 at the conserved threonine residue in the kinase domain (T233 in SPAK and T185 in OSR1) and increase their kinase activity [25, 28]. Accordingly, activated OSR1/SPAK phosphorylates NCC at three conserved residues in the N-terminus (T53, T58, and S71) [15, 24, 29]. The transporter activity of NCC is increased by phosphorylation [30]. Moreover, it has also been reported that phosphorylated NCC is protected from ubiquitination and subsequent endocytosis and/or degradation, leading to preferential localization at the apical plasma membrane [15, 31]. These molecular mechanisms indicate that WNK–OSR1/SPAK–NCC signaling in the DCT regulate sodium reabsorption (Fig. 2). Consistent with this supposition, Wnk4D561A/+ mice manifest increased phosphorylation of OSR1/SPAK kinases [15]. When these mice were crossed with SPAK and OSR1 knock-in mice in which WNK phosphorylation residues of SPAK (T243) and OSR1 (T185) were mutated to alanine and no longer phosphorylated, the increased phosphorylation of NCC was abolished, and the PHAII phenotype was reversed, providing further evidence that WNK kinases activate NCC through OSR1/SPAK [32, 33].
The with-no-lysine kinase (WNK)–oxidative stress-responsive gene 1 (OSR1)/STE20-related proline/alanine-rich kinase (SPAK)–sodium chloride cotransporter (NCC) phosphorylation cascade in distal convoluted tubule epithelial cells. WNK kinases phosphorylate and activate OSR1/SPAK, and activated OSR1/SPAK phosphorylates and activates NCC. Phosphorylated NCC is also preferentially expressed at the apical membrane and protected from ubiquitination and degradation, leading to increased reabsorption of sodium and chloride
Regulation of WNK kinases by the KLHL3–CUL3 E3 ligase complex
In 2012, mutations in KLHL3 and CUL3 were additionally identified in families with PHAII by whole exome sequencing [6, 7]. KLHL3 and CUL3 comprise the E3 ubiquitin ligase complex in which KLHL3 functions as an adapter to capture substrates and CUL3 catalyzes ubiquitin transfer from E2 to these substrates (Fig. 1b) [34]. Then, ubiquitinated substrates are normally subject to proteasomal degradation. Therefore, subsequent studies were focused on identifying substrates of the KLHL3–CUL3 E3 ligase complex and determining whether this complex is involved in WNK signaling.
Soon after the identification of mutations in KLHL3 and CUL3, in vitro studies revealed that both WNK1 and WNK4 are substrates of KLHL3 and therefore are degraded by the KLHL3–CUL3 E3 ligase complex [16, 35,36,37]. KLHL3 is composed of three domains, the kelch repeat, BTB and BACK domains, and PHAII-causing mutations are found in all three domains (Fig. 1b) [6, 7, 34]. These PHAII-causing mutations result in the defective degradation and increased protein expression of WNK1 and WNK4 because mutations in kelch repeats impair the capture of WNK kinases, and mutated BTB and BACK domains are unable to interact with CUL3 [16, 35,36,37,38]. These findings are supported by experiments showing that mice carrying a PHAII-associated kelch repeat mutation (KLHL3R528H/+) exhibited overexpression of the WNK1 and WNK4 proteins, leading to increased phosphorylation of OSR1/SPAK and NCC [39]. Moreover, the observation that KLHL3-deficient mice (KLHL3−/−) showed increased protein abundance of WNK kinases also supports the idea that PHAII-causing mutations in KLHL3 are loss-of-function mutations [40]. In addition, it has been demonstrated that KLHL3 dimer formation is required for the degradation of WNK kinases. Interestingly, in contrast to autosomal dominant inheritance of the KLHL3 R528H mutation, KLHL3+/− mice do not manifest the PHAII phenotype [40], suggesting that KLHL3 is redundant in the normal state and that KLHL3 R528H impairs the function of WT KLHL3 when they are heterodimerized (i.e., dominant-negative effect).
All CUL3 mutations reported to date are heterozygous and result in the production of a mutant CUL3 that lacks exon 9 (CUL3Δex9), leading to defective degradation of WNK kinases [6]. CUL3Δex9 is not a simple loss-of-function mutation, but is considered to have a dominant-negative effect because mice with heterozygous CUL3 ablation or decreased CUL3 transcription do not manifest the PHAII phenotype [41, 42]. Although consensus has not been reached regarding the pathogenic roles of CUL3Δex9, several in vitro and in vivo studies have suggested that CUL3Δex9 enhances the ubiquitination and degradation of KLHL3, leading to impaired degradation of WNK kinases [43, 44]. Yoshida et al. reported that KLHL3 protein expression is indeed decreased in the kidneys from CUL3Δex9/+ mice. CUL3 utilizes various adapter proteins, in addition to KLHL3, to target a broad range of substrates [45], but interestingly, CUL3Δex9 seemed to degrade KLHL3 specifically, while other adapter proteins, including KLHL2, were not affected [44]. It is surprising because KLHL2/3 share >80% of their amino acid sequences, but this selective effect of CUL3Δex9 might explain why patients with mutated CUL3 manifest a selective PHAII phenotype, which is inconsistent with the ubiquitous expression and multiple essential functions of CUL3. It is not well understood how Δex9 confers this novel function to CUL3, but aberrant neddylation may have a role [46]. It is known that the ubiquitin-like molecule NEDD8 is attached to the C-terminal lysine residue (Lys721) of CUL3 (Fig. 1) [47]. The attachment (neddylation) and subsequent detachment (deneddylation) cycle of NEDD8 influences the catalytic activity of CUL3. Schumacher et al. demonstrated that CUL3Δex9 was unable to interact with the deneddylation complex COP9 signalosome (CSN), resulting in hyperneddylation. Aberrant neddylation of CUL3Δex9 may be involved in the enhanced ubiquitination and degradation of KLHL3 because inactivation or ablation of CSN also causes hyperneddylation of CUL3 and accelerated KLHL3 protein degradation in vitro and in vivo [48, 49]. It should be noted, however, that some groups did not observe decreased KLHL3 protein expression in their PHAII model mice with CUL3 mutations [42, 50]. Moreover, several studies have reported other properties of CUL3Δex9, such as autoubiquitination and self-degradation and the inability to degrade WNK4 independent of KLHL3 degradation [42, 46, 48]. Therefore, further research is still needed to elucidate the function of CUL3Δex9.
Identification of the molecular interactions between WNK kinases and the KLHL3–CUL3 E3 ligase complex has provided new insights into the pathogenic role of WNK4 mutations. As explained above, most PHAII-causing mutations of WNK4 are located within the acidic domain. Wakabayashi et al. revealed that KLHL3 interacts with WNK4 through this acidic domain and that WNK4 with a mutated acidic domain is unable to bind KLHL3 [16]. Consistently, WNK4D561A/+ mice had increased WNK4 protein abundance. Moreover, WNK4 transgenic mice with multiple copies of WT WNK4 genes manifested increased phosphorylation of OSR1/SPAK and NCC proportional to their WNK4 protein expression levels [16]. Altogether, these observations indicate that the activity of WNK–OSR1/SPAK–NCC signaling is primarily determined by the protein abundance of WNK kinases, which is negatively regulated by the KLHL3–CUL3 E3 ligase complex (Fig. 3).
Aberrant activation of the with-no-lysine kinase (WNK)–oxidative stress-responsive gene 1 (OSR1)/STE20-related proline/alanine-rich kinase (SPAK)–sodium chloride cotransporter (NCC) phosphorylation cascade causes salt-sensitive hypertension in PHAII. All PHAII-causing mutations of WNK4, Kelch-like 3 (KLHL3), and Cullin 3 (CUL3) result in defective degradation of WNK kinases. On the other hand, mutation of WNK1 causes increased transcription and protein expression. Accordingly, accumulated WNK kinase protein activates the OSR1/SPAK–NCC phosphorylation cascade and increases sodium reabsorption. The activated WNK signaling pathway is not properly suppressed by a high salt diet, leading to salt-sensitive hypertension. Enhanced sodium reabsorption at the distal convoluted tubule (DCT) decreases sodium delivery to the downstream cortical collecting ducts (CCDs). Given that sodium reabsorption through the epithelial sodium channels (ENaCs) in the CCDs are electrically coupled with potassium excretion through the renal outer membrane potassium channel (ROMK), decreased sodium delivery results in potassium retention and hyperkalemia in PHAII patients
Interestingly, there are genotype–phenotype correlations in terms of disease severity in PHAII cases [6]. Patients with CUL3 mutations have the most severe phenotype followed by those with KLHL3 mutations, and patients with WNK4 or WNK1 mutations are the least severely affected. Most patients with mutated CUL3 develop hypertension before the age of 18 years, and the average age of diagnosis is 9 years. In contrast, patients with WNK1 mutations are typically diagnosed in their thirties. The molecular mechanisms characterizing PHAII may provide reasonable explanations for these differences. Mutations in CUL3 or KLHL3 result in accumulation of both WNK1 and WNK4 proteins, which may lead to a more severe phenotype than those with mutations in either WNK1 or WNK4. Moreover, recent studies suggest that, in addition to renal salt retention, CUL3Δex9 increases arterial stiffness by accumulating RhoA, which may explain the earlier onset of the hypertension observed in patients with CUL3 mutations [50, 51]. It should also be noted that WNK4 is essential for NCC activation. Consistent with this requirement, when crossed with WNK4−/− mice, KLHL3R528H/+ and WT mice exhibited comparable levels of NCC phosphorylation despite the increased protein expression of WNK1 in the KLHL3R528H/+ mice [52].
Physiological regulators of the WNK phosphorylation cascade
The discovery of the WNK–OSR1/SPAK–NCC phosphorylation cascade has implications not only for rare inherited diseases but also for NaCl homeostasis and blood pressure regulation under normal physiological conditions. The WNK phosphorylation cascade is also involved in salt-sensitive hypertension associated with common (patho-)physiological conditions. Clinical studies have characterized a population with increased salt sensitivity and revealed that phenotypes, such as metabolic syndrome, diabetes mellitus, low potassium intake, chronic kidney disease (CKD), older age, and African–American ethnicity, are often associated with salt-sensitive hypertension [53, 54]. Investigation of the WNK phosphorylation cascade associated with these conditions has revealed novel regulators of this pathway (Fig. 4). In this section, we describe the physiological regulation of WNK signaling.
(Patho-)physiological regulation of the with-no-lysine kinase (WNK)–oxidative stress-responsive gene 1 (OSR1)/STE20-related proline/alanine-rich kinase (SPAK)–sodium chloride cotransporter (NCC) phosphorylation cascade. Sodium intake regulates the WNK signaling pathway by modulating angiotensin II/aldosterone. The WNK signaling pathway is involved in salt-sensitive hypertension associated with low potassium intake, chronic kidney disease, and metabolic syndrome. Corresponding regulators are low intracellular chloride concentration (due to hyperpolarized membrane potential), TNFα, and insulin
Sodium chloride intake and the renin–angiotensin–aldosterone (RAA) system
Because of its important role in NaCl homeostasis, it is reasonable to suggest that the WNK phosphorylation cascade is primarily regulated by salt intake. To support this supposition, studies have shown that sodium restriction activates and sodium loading inactivates the WNK phosphorylation cascade [55]. In the case of inadequate suppression of the WNK phosphorylation cascade by high salt intake, kidneys fail to excrete sodium properly, which is an essential mechanism for the increased salt sensitivity observed in PHAII [55]. Aldosterone and angiotensin II (Ang II) are regarded as underlying effectors of this regulation [17, 56,57,58]. Actually, the angiotensin II type 1 receptor antagonist and mineralocorticoid receptor blocker downregulate WNK signaling in the murine kidney [55,56,57]. The effect of aldosterone on NCC is also supported by animal [59] and human studies [60], the latter of which showing that mineralocorticoid treatment increases the abundance of total and phosphorylated NCC in urinary exosomes. It should be noted, however, that aldosterone may also have an indirect effect on WNK signaling by modulating potassium [61, 62]. On the other hand, Ang II is reported to phosphorylate KLHL3 at S433 in the KLHL repeat through protein kinase C [63]. Mutation at S433 is also reported in PHAII kindred with autosomal dominant inheritance. Similar to the effect of the mutation, phosphorylated KLHL3 is not able to capture and degrade WNK kinases, leading to an increased abundance of WNK kinases. This could be one of the mechanisms underlying the RAA system regulation of WNK signaling.
Dietary potassium intake
According to epidemiological evidence, low daily potassium intake is related to high blood pressure and increased risk of cardiovascular disease and death [64,65,66]. Recently, growing evidence suggests that NCC functions as a regulator of renal potassium excretion [18, 67,68,69,70,71,72]. The DCT does not directly process potassium, but sodium reabsorption through NCC influences sodium delivery to the downstream connecting tubule (CNT) and cortical collecting ducts (CCDs), where sodium reabsorption through epithelial sodium channel (ENaC) is electrically coupled to potassium excretion through ROMK (Fig. 3). Patients with PHAII manifest hyperkalemia and metabolic acidosis because activation of NCC decreases sodium delivery into the CNT and CCDs and suppresses sodium reabsorption and the excretion of potassium and hydrogen ions [15]. In line with these disease outcomes, many studies have demonstrated that a low potassium diet activates the WNK–OSR1/SPAK–NCC phosphorylation cascade, which also decreases potassium excretion and thus maintains potassium homeostasis. Importantly, mice fed a low potassium and high sodium diet exhibit increased NCC activity and salt-sensitive hypertension [67, 71].
The mechanism by which potassium regulates the WNK phosphorylation cascade has been rigorously investigated in the last few years. In 2014, Piala et al. demonstrated that WNK1 has a chloride-sensing motif in its kinase domain [73]. This motif is conserved among all WNK isoforms (Fig. 1), and chloride binding to this motif decreases the catalytic activity of WNK kinases [68]. Based on in vitro experiments, Terker et al. proposed that an extracellular low potassium concentration enhances the basolateral potassium exit by inwardly rectifying potassium channel intake (Kir4.1/5.1 heterotetramer) and hyperpolarizing DCT cells [67]. In response to hyperpolarization, DCT cells lose chloride through the basolateral ClC–K2 chloride channel, and consequently, a low intracellular chloride concentration activates WNK kinases. This mechanism has been validated in vivo by using Kir4.1- or Kir5.1-knockout mice, which show abolished NCC activation in response to a low potassium diet [74, 75]. Nomura et al. also demonstrated that a low potassium diet did not activate the WNK phosphorylation cascade in barttin hypomorphic mice (Bsndneo/neo) [76]. This finding suggests that ClC–K2 has an essential role in low potassium-induced NCC activation because barttin is a β-subunit of ClC–K, and Bsndneo/neo mice have low expression of barttin and ClC–K. Recently, Chen et al. provided clear in vivo evidence that chloride sensing by WNK4 is indispensable for the NCC activation induced by a low potassium diet [77]. They created knock-in mice carrying a chloride-insensitive WNK4 mutation (L319F/L321F) and demonstrated that these mice maintained on a normal diet exhibit activated OSR1/SPAK–NCC signaling and hyperkalemia, metabolic acidosis, and high blood pressure resembling the PHAII phenotype. On the other hand, OSR1/SPAK–NCC signaling was not further activated in response to a low potassium diet. In contrast to all known PHAII-causing mutations of WNK1, WNK4, KLHL3, and CUL3, which result in an increased protein abundance of WNK kinases, WNK4 protein expression was not increased in these mice, providing in vivo evidence that the activity of WNK kinase is regulated not solely by protein abundance but also by chloride sensing.
In contrast to the effect of a low potassium diet, potassium loading inactivates NCC. However, it should be noted that acute and chronic loading of potassium has different effects and that accompanying anions, such as Cl−, HCO3−, citrate, and gluconate, confound these effects [78]. It is generally accepted that dietary intake of KCl decreases NCC phosphorylation, but the involvement of WNK signaling in high potassium-induced NCC dephosphorylation is less clear. In fact, most studies did not detect parallel decreases in WNK4 and SPAK [71, 72, 79, 80]. On the other hand, protein phosphatases, such as PP1 [81] and calcineurin (CaN) [80], have been suggested to dephosphorylate NCC. Shoda et al. demonstrated that oral gavage of potassium rapidly dephosphorylates NCC independent of OSR1/SPAK and that the CaN inhibitor tacrolimus prevents this dephosphorylation, indicating the involvement of CaN in high potassium-induced NCC dephosphorylation.
Insulin
Clinical evidence suggests that salt sensitivity is increased in patients who are obese and have metabolic syndrome [82], which prompted research groups to investigate the underlying mechanism. Metabolic syndrome is characterized by insulin resistance, which results in hyperinsulinemia. It has been demonstrated that insulin stimulates WNK4–OSR1/SPAK–NCC signaling and increases salt sensitivity [18, 83,84,85]. Consistently, WNK signaling is activated and not suppressed by a high salt diet in a db/db mouse model of hyperinsulinemic metabolic syndrome [86, 87]. Nishida et al. also clarified that inactivation of WNK signaling or inhibition of phosphatidylinositol 3-kinase (PI-3K) or Akt attenuates increased NCC phosphorylation in db/db mice, indicating that insulin stimulates WNK4–OSR1/SPAK–NCC signaling through the PI-3K/Akt pathway. In fact, in addition to protein kinase C, KLHL3 is also phosphorylated by Akt at S433, leading to defective degradation of WNK kinases [88]. These observations suggest that WNK signaling is a promising therapeutic target for blood pressure control in metabolic syndrome. Because it is known that long-term use of thiazide diuretics is complicated by glucose intolerance and dyslipidemia [89], other strategies, such as inhibition of WNK or SPAK kinases, may be of clinical value [90,91,92]. Interestingly, recent reports have demonstrated that antidiabetic drugs, such as metformin [93] and SGLT2 inhibitors [87], exert blood pressure-lowering effects by modulating NCC and WNK signaling, respectively.
TNFα
Hypertension is the most common comorbidity associated with CKD and one of the most important modifiable risk factors of CKD progression and cardiovascular disease [94]. However, it is often difficult to achieve appropriate blood pressure control in patients with CKD. A major reason for refractory hypertension in CKD patients is increased salt sensitivity. Importantly, recent evidence suggests that, in addition to reduced glomerular filtration, inappropriate sodium handling in renal tubules contributes to salt sensitivity in CKD [95,96,97].
On the other hand, emerging evidence suggests that the immune system has an important role in hypertension [98, 99]. Many studies support the idea that both innate and adaptive immunity and secreted cytokines contribute to vascular dysfunction and renal salt retention, leading to hypertension. For example, the idea that TNFα, an inflammatory cytokine, is involved in hypertension is supported by the observation that depletion or inhibition of TNFα prevents mice from developing hypertension in response to Ang II infusion [100, 101]. Moreover, a clinical report demonstrated that a TNFα antagonist had an antihypertensive effect in patients with rheumatoid arthritis [102]. Consistent with these findings, it has also been reported that TNFα activated the WNK1–SPAK–NCC phosphorylation cascade and contributed to salt-sensitive hypertension in several CKD mouse models [103]. Renal TNFα increases WNK1 protein expression by suppressing NEDD4–2, which is another E3 ligase that degrades WNK1 [104]. Accordingly, the WNK1–SPAK–NCC signaling pathway is activated in the CKD kidney with increased intrarenal TNFα, leading to salt-sensitive hypertension. These results suggest that the WNK phosphorylation cascade is regulated by the immune system and involved in salt-sensitive hypertension in CKD.
WNK signaling in other organs
In addition to blood pressure control, WNK signaling has some distinct roles in various organs. In adipocytes in organs, for example, WNK4 functions as an adipogenic factor, and deletion of WNK4 protects against diet-induced obesity [105]. The Gamba group reported that mice carrying an inactivating mutation of SPAK (SPAKT243A/T243A) exhibited improved glucose tolerance and were resistant to diet-induced obesity through a pleiotropic effect on metabolic organs, such as muscle and brown and white adipose tissue [106]. These observations suggest that drugs targeting WNK–SPAK signaling may have an advantage over NCC inhibition because thiazide diuretics often cause impaired glucose tolerance and dyslipidemia, as explained above [89].
Mandai et al. reported that, in skeletal muscle, WNK1 enhanced muscle cell hypertrophy by suppressing forkhead box protein O4 [107]. Consistent with this finding, WNK1 protein expression is known to increase with exercise and decrease with renal failure, suggesting that WNK1 may be a novel therapeutic target to prevent sarcopenia.
WNK signaling has also been proposed as an immune system regulator. In T cells, both chemokine receptor and T-cell receptor signaling increases WNK1 kinase activity [108]. WNK1 negatively regulates integrin-mediated adhesion, and WNK1-deficient T cells exhibit impaired homing capacity to lymphoid organs, such as lymph nodes and the spleen. Recently, Perry et al. reported that WNK1–SPAK/OSR1–NKCC1 signaling also has an important role in the process of apoptotic cell clearance (efferocytosis) [109]. Efferocytosis is characterized by anti-inflammation, but defective WNK signaling in phagocytes during cell corpse incorporation results in increased inflammatory and oxidative stress-related gene expression.
Several studies have also reported other functions of WNK signaling, such as angiogenesis [110, 111] and cancer progression [112]. Altogether, accumulating evidence suggests that WNK signaling is important not only for blood pressure control but also for various (patho-)physiological processes. Further understanding of this pathway will provide unique opportunities to manipulate these processes.
Summary and future directions
Identification of causative genes in PHAII helped elucidate the WNK–SPAK–NCC phosphorylation cascade and WNK degradation pathway through the CUL3–KLHL3 E3 ligase complex. In PHAII, the WNK signaling pathway is constitutively active because of the accumulation of WNK kinases and improperly suppressed high salt intake, leading to salt-sensitive hypertension. Interestingly, it has been found that the WNK signaling pathway also has effects in the salt-sensitive hypertension associated with more common conditions, such as a low potassium diet, metabolic syndrome, and CKD. In summary, the WNK signaling pathway is actively regulated by various factors, including membrane polarity, hormones, and inflammation. Moreover, recent findings have suggested that this pathway is involved in multiple cellular processes in addition to electrolyte and fluid homeostasis. Thus, with these unique properties, the WNK signaling pathway is a promising drug target. To date, several compounds have been found that modulate this pathway [90,91,92], but none of them is ready for clinical use because of their off-target effects. Further research is necessary to develop a more specific way to modulate the WNK signaling pathway.
References
Palmer LG, Schnermann J. Integrated control of Na transport along the nephron. Clin J Am Soc Nephrol. 2015;10:676–87. https://doi.org/10.2215/CJN.12391213.
Simon DB, Nelson-Williams C, Johnson Bia M, Ellison D, Karet FE, Morey Molina A, et al. Gitelman’s variant of Barter’s syndrome, inherited hypokalaemic alkalosis, is caused by mutations in the thiazide-sensitive Na–Cl cotransporter. Nat Genet. 1996;12:24–30. https://doi.org/10.1038/ng0196-24.
Gordon RD. Syndrome of hypertension and hyperkalemia with normal glomerular filtration rate. Hypertension. 1986;8:93–102. https://doi.org/10.1161/01.HYP.8.2.93.
Mayan H, Attar-Herzberg D, Shaharabany M, Holtzman EJ, Farfel Z. Increased urinary Na-Cl cotransporter protein in familial hyperkalaemia and hypertension. Nephrol Dial Transpl. 2007;23:492–6. https://doi.org/10.1093/ndt/gfm641.
Wilson FH, Disse-Nicodème S, Choate KA, Ishikawa K, Nelson-Williams C, Desitter I, et al. Human hypertension caused by mutations in WNK kinases. Science. 2001;293:1107–12. https://doi.org/10.1126/science.1062844.
Boyden LM, Choi M, Choate KA, Nelson-Williams CJ, Farhi A, Toka HR, et al. Mutations in kelch-like 3 and cullin 3 cause hypertension and electrolyte abnormalities. Nature. 2012;482:98–102. https://doi.org/10.1038/nature10814.
Louis-Dit-Picard H, Barc J, Trujillano D, Miserey-Lenkei S, Bouatia-Naji N, Pylypenko O, et al. KLHL3 mutations cause familial hyperkalemic hypertension by impairing ion transport in the distal nephron. Nat Genet. 2012;44:456–60. https://doi.org/10.1038/ng.2218.
Xu B, English JM, Wilsbacher JL, Stippec S, Goldsmith EJ, Cobb MH. WNK1, a novel mammalian serine/threonine protein kinase lacking the catalytic lysine in subdomain II. J Biol Chem. 2000;275:16795–801. https://doi.org/10.1074/jbc.275.22.16795.
Veríssimo F, Jordan P. WNK kinases, a novel protein kinase subfamily in multi-cellular organisms. Oncogene. 2001;20:5562–9. https://doi.org/10.1038/sj.onc.1204726.
Delaloy C, Lu J, Houot A-M, Disse-Nicodeme S, Gasc J-M, Corvol P, et al. Multiple promoters in the WNK1 gene: one controls expression of a kidney-specific kinase-defective isoform. Mol Cell Biol. 2003;23:9208–21. https://doi.org/10.1128/MCB.23.24.9208-9221.2003.
O’Reilly M. WNK1, a gene within a novel blood pressure control pathway, tissue-specifically generates radically different isoforms with and without a kinase domain. J Am Soc Nephrol. 2003;14:2447–56. https://doi.org/10.1097/01.ASN.0000089830.97681.3B.
Vidal-Petiot E, Cheval L, Faugeroux J, Malard T, Doucet A, Jeunemaitre X. et al. A new methodology for quantification of alternatively spliced exons reveals a highly tissue-specific expression pattern of WNK1 isoforms. PLoS One. 2012;7:e37751. https://doi.org/10.1371/journal.pone.0037751.
Gong H, Tang Z, Yang Y, Sun L, Zhang W, Wang W, et al. A patient with pseudohypoaldosteronism type II caused by a novel mutation in WNK4 gene. Endocrine. 2008;33:230–4. https://doi.org/10.1007/s12020-008-9084-8.
Golbang AP, Murthy M, Hamad A, Liu C-H, Cope G, Van’t Hoff W, et al. A new kindred with pseudohypoaldosteronism type II and a novel mutation (564D>H) in the acidic motif of the WNK4 gene. Hypertension. 2005;46:295–300. https://doi.org/10.1161/01.HYP.0000174326.96918.d6.
Yang S-S, Morimoto T, Rai T, Chiga M, Sohara E, Ohno M, et al. Molecular pathogenesis of pseudohypoaldosteronism type II: generation and analysis of a Wnk4D561A/+ knockin mouse model. Cell Metab. 2007;5:331–44. https://doi.org/10.1016/j.cmet.2007.03.009.
Wakabayashi M, Mori T, Isobe K, Sohara E, Susa K, Araki Y, et al. Impaired KLHL3-mediated ubiquitination of WNK4 causes human hypertension. Cell Rep. 2013;3:858–68. https://doi.org/10.1016/j.celrep.2013.02.024.
Castañeda-Bueno M, Cervantes-Pérez LG, Vázquez N, Uribe N, Kantesaria S, Morla L, et al. Activation of the renal Na+:Cl- cotransporter by angiotensin II is a WNK4-dependent process. Proc Natl Acad Sci USA. 2012;109:7929–34. https://doi.org/10.1073/pnas.1200947109.
Takahashi D, Mori T, Nomura N, Khan MZH, Araki Y, Zeniya M, et al. WNK4 is the major WNK positively regulating NCC in the mouse kidney. Biosci Rep. 2014;34. https://doi.org/10.1042/BSR20140047.
Vidal-Petiot E, Elvira-Matelot E, Mutig K, Soukaseum C, Baudrie V, Wu S, et al. WNK1-related familial hyperkalemic hypertension results from an increased expression of L-WNK1 specifically in the distal nephron. Proc Natl Acad Sci USA. 2013;110:14366–71. https://doi.org/10.1073/pnas.1304230110.
Liu Z, Xie J, Wu T, Truong T, Auchus RJ, Huang C-L. Downregulation of NCC and NKCC2 cotransporters by kidney-specific WNK1 revealed by gene disruption and transgenic mouse models. Hum Mol Genet. 2011;20:855–66. https://doi.org/10.1093/hmg/ddq525.
Hadchouel J, Soukaseum C, Busst C, Zhou X-o, Baudrie V, Zurrer T, et al. Decreased ENaC expression compensates the increased NCC activity following inactivation of the kidney-specific isoform of WNK1 and prevents hypertension. Proc Natl Acad Sci USA. 2010;107:18109–14. https://doi.org/10.1073/pnas.1006128107.
Boyd-Shiwarski CR, Shiwarski DJ, Roy A, Namboodiri HN, Nkashama LJ, Xie J, et al. Potassium-regulated distal tubule WNK bodies are kidney-specific WNK1 dependent. Mol Biol Cell. 2018;29:499–509. https://doi.org/10.1091/mbc.E17-08-0529.
Argaiz ER, Chavez-Canales M, Ostrosky-Frid M, Rodríguez-Gama A, Vázquez N, Gonzalez-Rodriguez X, et al. Kidney-specific WNK1 isoform (KS-WNK1) is a potent activator of WNK4 and NCC. Am J Physiol Ren Physiol. 2018;315:F734–45. https://doi.org/10.1152/ajprenal.00145.2018.
Moriguchi T, Urushiyama S, Hisamoto N, Iemura S, Uchida S, Natsume T, et al. WNK1 regulates phosphorylation of cation-chloride-coupled cotransporters via the STE20-related kinases, SPAK and OSR1. J Biol Chem. 2005;280:42685–93. https://doi.org/10.1074/jbc.M510042200.
Vitari AC, Deak M, Morrice NA, Alessi DR. The WNK1 and WNK4 protein kinases that are mutated in Gordon’s hypertension syndrome phosphorylate and activate SPAK and OSR1 protein kinases. Biochem J. 2005;391:17–24. https://doi.org/10.1042/BJ20051180.
Piechotta K, Lu J, Delpire E. Cation chloride cotransporters interact with the stress-related kinases Ste20-related proline-alanine-rich kinase (SPAK) and oxidative stress response 1 (OSR1). J Biol Chem. 2002;277:50812–9. https://doi.org/10.1074/jbc.M208108200.
Vitari AC, Thastrup J, Rafiqi FH, Deak M, Morrice NA, Karlsson HKR, et al. Functional interactions of the SPAK/OSR1 kinases with their upstream activator WNK1 and downstream substrate NKCC1. Biochem J. 2006;397:223–31. https://doi.org/10.1042/BJ20060220.
Zagórska A, Pozo-Guisado E, Boudeau J, Vitari AC, Rafiqi FH, Thastrup J, et al. Regulation of activity and localization of the WNK1 protein kinase by hyperosmotic stress. J Cell Biol. 2007;176:89–100. https://doi.org/10.1083/jcb.200605093.
Yang S-S, Lo Y-F, Wu C-C, Lin S-W, Yeh C-J, Chu P, et al. SPAK-knockout mice manifest Gitelman syndrome and impaired vasoconstriction. J Am Soc Nephrol. 2010;21:1868–77. https://doi.org/10.1681/ASN.2009121295.
Pacheco-Alvarez D, Cristóbal PS, Meade P, Moreno E, Vazquez N, Muñoz E, et al. The Na+:Cl- cotransporter is activated and phosphorylated at the amino-terminal domain upon intracellular chloride depletion. J Biol Chem. 2006;281:28755–63. https://doi.org/10.1074/jbc.M603773200.
Hossain Khan MZ, Sohara E, Ohta A, Chiga M, Inoue Y, Isobe K, et al. Phosphorylation of Na-Cl cotransporter by OSR1 and SPAK kinases regulates its ubiquitination. Biochem Biophys Res Commun. 2012;425:456–61. https://doi.org/10.1016/j.bbrc.2012.07.124.
Rafiqi FH, Zuber AM, Glover M, Richardson C, Fleming S, Jovanović S, et al. Role of the WNK-activated SPAK kinase in regulating blood pressure. EMBO Mol Med. 2010;2:63–75. https://doi.org/10.1002/emmm.200900058.
Chiga M, Rafiqi FH, Alessi DR, Sohara E, Ohta A, Rai T, et al. Phenotypes of pseudohypoaldosteronism type II caused by the WNK4 D561A missense mutation are dependent on the WNK-OSR1/SPAK kinase cascade. J Cell Sci. 2011;124:1391–5. https://doi.org/10.1242/jcs.084111.
Lai F, Orelli BJ, Till BG, Godley LA, Fernald AA, Pamintuan L, et al. Molecular characterization of KLHL3, a human homologue of the Drosophila kelch gene. Genomics. 2000;66:65–75. https://doi.org/10.1006/geno.2000.6181.
Ohta A, Schumacher F-R, Mehellou Y, Johnson C, Knebel A, Macartney TJ, et al. The CUL3-KLHL3 E3 ligase complex mutated in Gordon’s hypertension syndrome interacts with and ubiquitylates WNK isoforms: disease-causing mutations in KLHL3 and WNK4 disrupt interaction. Biochem J. 2013;451:111–22. https://doi.org/10.1042/BJ20121903.
Shibata S, Zhang J, Puthumana J, Stone KL, Lifton RP. Kelch-like 3 and Cullin 3 regulate electrolyte homeostasis via ubiquitination and degradation of WNK4. Proc Natl Acad Sci USA. 2013;110:7838–43. https://doi.org/10.1073/pnas.1304592110.
Wu G, Peng J-B. Disease-causing mutations in KLHL3 impair its effect on WNK4 degradation. FEBS Lett. 2013;587:1717–22. https://doi.org/10.1016/j.febslet.2013.04.032.
Mori Y, Wakabayashi M, Mori T, Araki Y, Sohara E, Rai T, et al. Decrease of WNK4 ubiquitination by disease-causing mutations of KLHL3 through different molecular mechanisms. Biochem Biophys Res Commun. 2013;439:30–4. https://doi.org/10.1016/j.bbrc.2013.08.035.
Susa K, Sohara E, Rai T, Zeniya M, Mori Y, Mori T, et al. Impaired degradation of WNK1 and WNK4 kinases causes PHAII in mutant KLHL3 knock-in mice. Hum Mol Genet. 2014;23:5052–60. https://doi.org/10.1093/hmg/ddu217.
Sasaki E, Susa K, Mori T, Isobe K, Araki Y, Inoue Y, et al. KLHL3 knockout mice reveal the physiological role of KLHL3 and the pathophysiology of pseudohypoaldosteronism type II caused by mutant KLHL3. Mol Cell Biol. 2017;37. https://doi.org/10.1128/MCB.00508-16.
Araki Y, Rai T, Sohara E, Mori T, Inoue Y, Isobe K, et al. Generation and analysis of knock-in mice carrying pseudohypoaldosteronism type II-causing mutations in the cullin 3 gene. Biol Open. 2015;4:1509–17. https://doi.org/10.1242/bio.013276.
Ferdaus MZ, Miller LN, Agbor LN, Saritas T, Singer JD, Sigmund CD, et al. Mutant Cullin 3 causes familial hyperkalemic hypertension via dominant effects. JCI Insight. 2017;2. https://doi.org/10.1172/jci.insight.96700.
McCormick JA, Yang C-L, Zhang C, Davidge B, Blankenstein KI, Terker AS, et al. Hyperkalemic hypertension–associated cullin 3 promotes WNK signaling by degrading KLHL3. J Clin Invest. 2014;124:4723–36. https://doi.org/10.1172/JCI76126.
Yoshida S, Araki Y, Mori T, Sasaki E, Kasagi Y, Isobe K, et al. Decreased KLHL3 expression is involved in the pathogenesis of pseudohypoaldosteronism type II caused by cullin 3 mutation in vivo. Clin Exp Nephrol. 2018;22:1251–7. https://doi.org/10.1007/s10157-018-1593-z.
Genschik P, Sumara I, Lechner E. The emerging family of CULLIN3-RING ubiquitin ligases (CRL3s): cellular functions and disease implications. EMBO J. 2013;32:2307–20. https://doi.org/10.1038/emboj.2013.173.
Schumacher F, Siew K, Zhang J, Johnson C, Wood N, Cleary SE, et al. Characterisation of the Cullin‐3 mutation that causes a severe form of familial hypertension and hyperkalaemia. EMBO Mol Med. 2015;7:1285–306. https://doi.org/10.15252/emmm.201505444.
Pintard L, Kurz T, Glaser S, Willis JH, Peter M, Bowerman B. Neddylation and deneddylation of CUL-3 is required to target MEI-1/Katanin for degradation at the meiosis-to-mitosis transition in C. elegans. Curr Biol. 2003;13:911–21. https://doi.org/10.1016/s0960-9822(03)00336-1.
Cornelius RJ, Zhang C, Erspamer KJ, Agbor LN, Sigmund CD, Singer JD, et al. Dual gain and loss of cullin 3 function mediates familial hyperkalemic hypertension. Am J Physiol Physiol. 2018;315:F1006–18. https://doi.org/10.1152/ajprenal.00602.2017.
Cornelius RJ, Si J, Cuevas CA, Nelson JW, Gratreak BDK, Pardi R, et al. Renal COP9 signalosome deficiency alters CUL3-KLHL3-WNK signaling pathway. J Am Soc Nephro. 2018. https://doi.org/10.1681/ASN.2018030333.
Abdel Khalek W, Rafael C, Loisel-Ferreira I, Kouranti I, Clauser E, Hadchouel J, et al. Severe arterial hypertension from cullin 3 mutations is caused by both renal and vascular effects. J Am Soc Nephrol. 2019;30:811–23. https://doi.org/10.1681/ASN.2017121307.
Agbor LN, Ibeawuchi S-RC, Hu C, Wu J, Davis DR, Keen HL, et al. Cullin-3 mutation causes arterial stiffness and hypertension through a vascular smooth muscle mechanism. JCI Insight. 2016;1. https://doi.org/10.1172/jci.insight.91015.
Susa K, Sohara E, Takahashi D, Okado T, Rai T, Uchida S. WNK4 is indispensable for the pathogenesis of pseudohypoaldosteronism type II caused by mutant KLHL3. Biochem Biophys Res Commun. 2017;491:727–32. https://doi.org/10.1016/j.bbrc.2017.07.121.
Kotchen TA, Cowley AW, Frohlich ED. Salt in Health and Disease—a delicate balance. N Engl J Med. 2013;368:1229–37. https://doi.org/10.1056/NEJMra1212606.
Hall JE. Renal dysfunction, rather than nonrenal vascular dysfunction, mediates salt-induced hypertension. Circulation. 2016;133:894–906. https://doi.org/10.1161/CIRCULATIONAHA.115.018526.
Chiga M, Rai T, Yang S-S, Ohta A, Takizawa T, Sasaki S, et al. Dietary salt regulates the phosphorylation of OSR1/SPAK kinases and the sodium chloride cotransporter through aldosterone. Kidney Int. 2008;74:1403–9. https://doi.org/10.1038/ki.2008.451.
San-Cristobal P, Pacheco-Alvarez D, Richardson C, Ring AM, Vazquez N, Rafiqi FH, et al. Angiotensin II signaling increases activity of the renal Na-Cl cotransporter through a WNK4-SPAK-dependent pathway. Proc Natl Acad Sci USA. 2009;106:4384–9. https://doi.org/10.1073/pnas.0813238106.
Talati G, Ohta A, Rai T, Sohara E, Naito S, Vandewalle A, et al. Effect of angiotensin II on the WNK-OSR1/SPAK-NCC phosphorylation cascade in cultured mpkDCT cells and in vivo mouse kidney. Biochem Biophys Res Commun. 2010;393:844–8. https://doi.org/10.1016/j.bbrc.2010.02.096.
van der Lubbe N, Lim CH, Fenton RA, Meima ME, Jan Danser AH, Zietse R, et al. Angiotensin II induces phosphorylation of the thiazide-sensitive sodium chloride cotransporter independent of aldosterone. Kidney Int. 2011;79:66–76. https://doi.org/10.1038/ki.2010.290.
Cheng L, Poulsen SB, Wu Q, Esteva-Font C, Olesen ETB, Peng L, et al. Rapid aldosterone-mediated signaling in the DCT increases activity of the thiazide-sensitive NaCl cotransporter. J Am Soc Nephrol. 2019;30:1454–70. https://doi.org/10.1681/ASN.2018101025.
Wolley MJ, Wu A, Xu S, Gordon RD, Fenton RA, Stowasser M. In primary aldosteronism, mineralocorticoids influence exosomal sodium-chloride cotransporter abundance. J Am Soc Nephrol. 2017;28:56–63. https://doi.org/10.1681/ASN.2015111221.
Czogalla J, Vohra T, Penton D, Kirschmann M, Craigie E, Loffing J. The mineralocorticoid receptor (MR) regulates ENaC but not NCC in mice with random MR deletion. Pflügers Arch—Eur J Physiol. 2016;468:849–58. https://doi.org/10.1007/s00424-016-1798-5.
Terker AS, Yarbrough B, Ferdaus MZ, Lazelle RA, Erspamer KJ, Meermeier NP, et al. Direct and indirect mineralocorticoid effects determine distal salt transport. J Am Soc Nephrol. 2016;27:2436–45. https://doi.org/10.1681/ASN.2015070815.
Shibata S, Arroyo JP, Castaneda-Bueno M, Puthumana J, Zhang J, Uchida S, et al. Angiotensin II signaling via protein kinase C phosphorylates Kelch-like 3, preventing WNK4 degradation. Proc Natl Acad Sci USA. 2014;111:15556–61. https://doi.org/10.1073/pnas.1418342111.
Mente A, O’Donnell MJ, Rangarajan S, McQueen MJ, Poirier P, Wielgosz A, et al. PURE investigators. Association of urinary sodium and potassium excretion with blood pressure. N Engl J Med. 2014;371:601–11. https://doi.org/10.1056/NEJMoa1311989.
Mente A, O’Donnell M, Rangarajan S, McQueen M, Dagenais G, Wielgosz A, et al. Urinary sodium excretion, blood pressure, cardiovascular disease, and mortality: a community-level prospective epidemiological cohort study. Lancet. 2018;392:496–506. https://doi.org/10.1016/S0140-6736(18)31376-X.
O’Donnell M, Mente A, Rangarajan S, McQueen MJ, Wang X, Liu L, et al. Urinary sodium and potassium excretion, mortality, and cardiovascular events. N Engl J Med. 2014;371:612–23. https://doi.org/10.1056/NEJMoa1311889.
Terker AS, Zhang C, McCormick JA, Lazelle RA, Zhang C, Meermeier NP, et al. Potassium modulates electrolyte balance and blood pressure through effects on distal cell voltage and chloride. Cell Metab. 2015;21:39–50. https://doi.org/10.1016/j.cmet.2014.12.006.
Terker AS, Zhang C, Erspamer KJ, Gamba G, Yang C-L, Ellison DH. Unique chloride-sensing properties of WNK4 permit the distal nephron to modulate potassium homeostasis. Kidney Int. 2016;89:127–34. https://doi.org/10.1038/ki.2015.289.
Wade JB, Liu J, Coleman R, Grimm PR, Delpire E, Welling PA. SPAK-mediated NCC regulation in response to low-K+ diet. Am J Physiol Ren Physiol. 2015;308:F923–31. https://doi.org/10.1152/ajprenal.00388.2014.
Ferdaus MZ, Barber KW, López-Cayuqueo KI, Terker AS, Argaiz ER, Gassaway BM, et al. SPAK and OSR1 play essential roles in potassium homeostasis through actions on the distal convoluted tubule. J Physiol. 2016;594:4945–66. https://doi.org/10.1113/JP272311.
Vitzthum H, Seniuk A, Schulte LH, Müller ML, Hetz H, Ehmke H. Functional coupling of renal K + and Na + handling causes high blood pressure in Na + replete mice. J Physiol. 2014;592:1139–57. https://doi.org/10.1113/jphysiol.2013.266924.
Castañeda-Bueno M, Cervantes-Perez LG, Rojas-Vega L, Arroyo-Garza I, Vázquez N, Moreno E, et al. Modulation of NCC activity by low and high K + intake: insights into the signaling pathways involved. Am J Physiol Physiol. 2014;306:F1507–19. https://doi.org/10.1152/ajprenal.00255.2013.
Piala AT, Moon TM, Akella R, He H, Cobb MH, Goldsmith EJ. Chloride Sensing by WNK1 involves inhibition of autophosphorylation. Sci Signal. 2014;7:ra41. https://doi.org/10.1126/scisignal.2005050.
Wang M-X, Cuevas CA, Su X-T, Wu P, Gao Z-X, Lin D-H, et al. Potassium intake modulates the thiazide-sensitive sodium-chloride cotransporter (NCC) activity via the Kir4.1 potassium channel. Kidney Int. 2018;93:893–902. https://doi.org/10.1016/j.kint.2017.10.023.
Wu P, Gao Z-X, Zhang D-D, Su X-T, Wang W-H, Lin D-H. Deletion of Kir5.1 impairs renal ability to excrete potassium during increased dietary potassium intake. J Am Soc Nephrol. 2019;30:1425–38. https://doi.org/10.1681/ASN.2019010025.
Nomura N, Shoda W, Wang Y, Mandai S, Furusho T, Takahashi D, et al. Role of ClC-K and barttin in low potassium-induced sodium chloride cotransporter activation and hypertension in mouse kidney. Biosci Rep. 2018;38. https://doi.org/10.1042/BSR20171243.
Chen J-C, Lo Y-F, Lin Y-W, Lin S-H, Huang C-L, Cheng C-J. WNK4 kinase is a physiological intracellular chloride sensor. Proc Natl Acad Sci USA. 2019;116:4502–7. https://doi.org/10.1073/pnas.1817220116.
Nomura N, Shoda W, Uchida S. Clinical importance of potassium intake and molecular mechanism of potassium regulation. Clin Exp Nephrol. 2019;23:1175–80. https://doi.org/10.1007/s10157-019-01766-x.
Rengarajan S, Lee DH, Oh YT, Delpire E, Youn JH, McDonough AA. Increasing plasma [K +] by intravenous potassium infusion reduces NCC phosphorylation and drives kaliuresis and natriuresis. Am J Physiol Physiol. 2014;306:F1059–68. https://doi.org/10.1152/ajprenal.00015.2014.
Shoda W, Nomura N, Ando F, Mori Y, Mori T, Sohara E, et al. Calcineurin inhibitors block sodium-chloride cotransporter dephosphorylation in response to high potassium intake. Kidney Int. 2017;91:402–11. https://doi.org/10.1016/j.kint.2016.09.001.
Penton D, Moser S, Wengi A, Czogalla J, Rosenbaek LL, Rigendinger F, et al. Protein phosphatase 1 inhibitor–1 mediates the cAMP-dependent stimulation of the renal NaCl cotransporter. J Am Soc Nephrol. 2019;30:737–50. https://doi.org/10.1681/ASN.2018050540.
Chen J, Gu D, Huang J, Rao DC, Jaquish CE, Hixson JE GenSalt Collaborative Research Group, et al. Metabolic syndrome and salt sensitivity of blood pressure in non-diabetic people in China: a dietary intervention study. Lancet. 2009;373:829–35. https://doi.org/10.1016/S0140-6736(09)60144-6.
Chávez-Canales M, Arroyo JP, Ko B, Vázquez N, Bautista R, Castañeda-Bueno M. et al. Insulin increases the functional activity of the renal NaCl cotransporter. J Hypertens. 2013;31:303–11. https://doi.org/10.1097/HJH.0b013e32835bbb83.
Komers R, Rogers S, Oyama TT, Xu B, Yang C-L, McCormick J, et al. Enhanced phosphorylation of Na(+)-Cl- co-transporter in experimental metabolic syndrome: role of insulin. Clin Sci. 2012;123:635–47. https://doi.org/10.1042/CS20120003.
Sohara E, Rai T, Yang S-S, Ohta A, Naito S, Chiga M. et al. Acute insulin stimulation induces phosphorylation of the Na-Cl cotransporter in cultured distal mpkDCT cells and mouse kidney. PLoS One. 2011;6:e24277. https://doi.org/10.1371/journal.pone.0024277.
Nishida H, Sohara E, Nomura N, Chiga M, Alessi DR, Rai T, et al. Phosphatidylinositol 3-kinase/Akt signaling pathway activates the WNK-OSR1/SPAK-NCC phosphorylation cascade in hyperinsulinemic db/db mice. Hypertension. 2012;60:981–90. https://doi.org/10.1161/HYPERTENSIONAHA.112.201509.
Ishizawa K, Wang Q, Li J, Xu N, Nemoto Y, Morimoto C, et al. Inhibition of sodium glucose cotransporter 2 attenuates the dysregulation of Kelch-Like 3 and NaCl cotransporter in obese diabetic mice. J Am Soc Nephrol. 2019;30:782–94. https://doi.org/10.1681/ASN.2018070703.
Yoshizaki Y, Mori Y, Tsuzaki Y, Mori T, Nomura N, Wakabayashi M, et al. Impaired degradation of WNK by Akt and PKA phosphorylation of KLHL3. Biochem Biophys Res Commun. 2015;467:229–34. https://doi.org/10.1016/j.bbrc.2015.09.184.
Punzi HA, Punzi CF. Metabolic issues in the antihypertensive and lipid-lowering heart attack trial study. Curr Hypertens Rep. 2004;6:106–10. https://doi.org/10.1007/s11906-004-0084-7.
Mori T, Kikuchi E, Watanabe Y, Fujii S, Ishigami-Yuasa M, Kagechika H, et al. Chemical library screening for WNK signalling inhibitors using fluorescence correlation spectroscopy. Biochem J. 2013;455:339–45. https://doi.org/10.1042/BJ20130597.
Kikuchi E, Mori T, Zeniya M, Isobe K, Ishigami-Yuasa M, Fujii S, et al. Discovery of novel SPAK inhibitors that block WNK kinase signaling to cation chloride transporters. J Am Soc Nephrol. 2015;26:1525–36. https://doi.org/10.1681/ASN.2014060560.
Yamada K, Park H-M, Rigel DF, DiPetrillo K, Whalen EJ, Anisowicz A, et al. Small-molecule WNK inhibition regulates cardiovascular and renal function. Nat Chem Biol. 2016;12:896–8. https://doi.org/10.1038/nchembio.2168.
Hashimoto H, Nomura N, Shoda W, Isobe K, Kikuchi H, Yamamoto K, et al. Metformin increases urinary sodium excretion by reducing phosphorylation of the sodium-chloride cotransporter. Metabolism. 2018;85:23–31. https://doi.org/10.1016/j.metabol.2018.02.009.
Townsend RR, Taler SJ. Management of hypertension in chronic kidney disease. Nat Rev Nephrol. 2015;11:555–63. https://doi.org/10.1038/nrneph.2015.114.
Kamat NV, Thabet SR, Xiao L, Saleh MA, Kirabo A, Madhur MS, et al. Renal transporter activation during angiotensin-II hypertension is blunted in interferon-γ-/- and interleukin-17A-/- mice. Hypertension. 2015;65:569–76. https://doi.org/10.1161/HYPERTENSIONAHA.114.04975.
Gonzalez-Villalobos RA, Janjoulia T, Fletcher NK, Giani JF, Nguyen MTX, Riquier-Brison AD, et al. The absence of intrarenal ACE protects against hypertension. J Clin Invest. 2013;123:2011–23. https://doi.org/10.1172/JCI65460.
Kobayashi R, Wakui H, Azushima K, Uneda K, Haku S, Ohki K, et al. An angiotensin II type 1 receptor binding molecule has a critical role in hypertension in a chronic kidney disease model. Kidney Int. 2017;91:1115–25. https://doi.org/10.1016/j.kint.2016.10.035.
Rucker AJ, Rudemiller NP, Crowley SD. Salt, hypertension, and immunity. Annu Rev Physiol. 2018;80:283–307. https://doi.org/10.1146/annurev-physiol-021317-121134.
Norlander AE, Madhur MS, Harrison DG. The immunology of hypertension. J Exp Med. 2018;215:21–33. https://doi.org/10.1084/jem.20171773.
Guzik TJ, Hoch NE, Brown KA, McCann LA, Rahman A, Dikalov S, et al. Role of the T cell in the genesis of angiotensin II–induced hypertension and vascular dysfunction. J Exp Med. 2007;204:2449–60. https://doi.org/10.1084/jem.20070657.
Zhang J, Patel MB, Griffiths R, Mao A, Song Y, Karlovich NS, et al. Tumor necrosis factor-α produced in the kidney contributes to angiotensin II-dependent hypertension. Hypertension. 2014;64:1275–81. https://doi.org/10.1161/HYPERTENSIONAHA.114.03863.
Yoshida S, Takeuchi T, Kotani T, Yamamoto N, Hata K, Nagai K, et al. Infliximab, a TNF-α inhibitor, reduces 24-h ambulatory blood pressure in rheumatoid arthritis patients. J Hum Hypertens. 2014;28:165–9. https://doi.org/10.1038/jhh.2013.80.
Furusho T, Sohara E, Mandai S, Kikuchi H, Takahashi N, Fujimaru T, et al. Renal TNFα activates the WNK phosphorylation cascade and contributes to salt-sensitive hypertension in chronic kidney disease. Kidney Int. 2020;97:713–27. https://doi.org/10.1016/j.kint.2019.11.021.
Roy A, Al-Qusairi L, Donnelly BF, Ronzaud C, Marciszyn AL, Gong F, et al. Alternatively spliced proline-rich cassettes link WNK1 to aldosterone action. J Clin Invest. 2015;125:3433–48. https://doi.org/10.1172/JCI75245.
Takahashi D, Mori T, Sohara E, Tanaka M, Chiga M, Inoue Y, et al. WNK4 is an adipogenic factor and its deletion reduces diet-induced obesity in mice. EBioMedicine. 2017;18:118–27. https://doi.org/10.1016/j.ebiom.2017.03.011.
Torre-Villalvazo I, Cervantes-Pérez LG, Noriega LG, Jiménez JV, Uribe N, Chávez-Canales M, et al. Inactivation of SPAK kinase reduces body weight gain in mice fed a high-fat diet by improving energy expenditure and insulin sensitivity. Am J Physiol Metab. 2018;314:E53–65. https://doi.org/10.1152/ajpendo.00108.2017.
Mandai S, Mori T, Nomura N, Furusho T, Arai Y, Kikuchi H, et al. WNK1 regulates skeletal muscle cell hypertrophy by modulating the nuclear localization and transcriptional activity of FOXO4. Sci Rep. 2018;8. https://doi.org/10.1038/s41598-018-27414-0.
Köchl R, Thelen F, Vanes L, Brazão TF, Fountain K, Xie J, et al. WNK1 kinase balances T cell adhesion versus migration in vivo. Nat Immunol. 2016;17:1075–83. https://doi.org/10.1038/ni.3495.
Perry JSA, Morioka S, Medina CB, Iker Etchegaray J, Barron B, Raymond MH, et al. Interpreting an apoptotic corpse as anti-inflammatory involves a chloride sensing pathway. Nat Cell Biol. 2019;21:1532–43. https://doi.org/10.1038/s41556-019-0431-1.
Dbouk HA, Weil LM, Perera GKS, Dellinger MT, Pearson G, Brekken RA, et al. Actions of the protein kinase WNK1 on endothelial cells are differentially mediated by its substrate kinases OSR1 and SPAK. Proc Natl Acad Sci USA. 2014;111:15999–6004. https://doi.org/10.1073/pnas.1419057111.
Xie J, Yoon J, Yang S-S, Lin S-H, Huang C-L. WNK1 protein kinase regulates embryonic cardiovascular development through the OSR1 signaling cascade. J Biol Chem. 2013;288:8566–74. https://doi.org/10.1074/jbc.M113.451575.
Gallolu Kankanamalage S, Karra AS, Cobb MH. WNK pathways in cancer signaling networks. Cell Commun Signal. 2018;16:72. https://doi.org/10.1186/s12964-018-0287-1.
Acknowledgements
This work was supported in part by Grants-in-Aid for Scientific Research (KAKENHI) from the Japan Society for the Promotion of Science (JSPS) [Grant Numbers: 25221306–00, 19H01049, 18K19534, 16H05314, and 19H03672], a Health Labor Science Research Grant from the Ministry of Health, Labor, and Welfare, AMED under Grant Number JP18ek0109304, and grants from the Yukiko Ishibashi Foundation and the Salt Science Research Foundation (1925).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Furusho, T., Uchida, S. & Sohara, E. The WNK signaling pathway and salt-sensitive hypertension. Hypertens Res 43, 733–743 (2020). https://doi.org/10.1038/s41440-020-0437-x
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-020-0437-x
Keywords
This article is cited by
-
The genetics of hypertension
Nature Reviews Nephrology (2026)
-
Role of dietary potassium and salt substitution in the prevention and management of hypertension
Hypertension Research (2025)
-
CYLD alleviates NLRP3 inflammasome-mediated pyroptosis in osteoporosis by deubiquitinating WNK1
Journal of Orthopaedic Surgery and Research (2024)
-
Integrative single-cell characterization of a frugivorous and an insectivorous bat kidney and pancreas
Nature Communications (2024)
-
Pathophysiological role of Na–Cl cotransporter in kidneys, blood pressure, and metabolism
Human Cell (2024)