Abstract
Adolescents with asthma are at heightened risk of somatic and mental health challenges, particularly during large-scale stressors such as the COVID-19 pandemic. This study explored the self-reported prevalence of asthma, co-occurring somatic complaints, psychological distress, and perceived pandemic impact in a multinational sample of 4802 upper secondary school students (aged 15–19) from Sweden, the United States, Serbia, Morocco, and Vietnam. Participants completed a web-based survey between November 2020 and June 2021. Approximately 9% reported having a physician-diagnosed asthma condition, with prevalence varying across countries. An additional 3.2% of the total sample reported uncertainty about whether they had asthma, with this uncertainty most frequently observed in Vietnam and Morocco. Adolescents with asthma reported slightly higher psychological distress than their peers without asthma, particularly among females, yet paradoxically reported a lower perceived impact of the pandemic on daily life. Physical activity levels were comparable between groups. Asthma was found to be associated with several co-occurring somatic complaints, with one gender-specific pattern observed in relation to thyroid disease. The observed variability in asthma prevalence and diagnostic uncertainty underscores the influence of national healthcare systems, health literacy, and communication practices. These findings highlight the need for gender-sensitive and context-aware approaches in adolescent health care, especially during global public health disruptions.
Similar content being viewed by others
Introduction
Asthma exists in people of all ages, and according to Global Initiative for Asthma1, it estimated to affect 300 million individuals worldwide2. It is the most common chronic condition in children (9.5%)3,4. During adolescence, there is a change in sex-specific risk and prevalence. While, in those under 13, asthma is more prevalent in males, the prevalence of asthma becomes higher in females during adolescence5. This change is suggested to be based on hormonal transformation and sex-specific environmental exposures6. It is estimated that 50% of adolescents and young adults with asthma-related symptoms are not receiving a medical diagnosis of asthma, mainly in low- and middle-income countries1.
Because asthma is a heterogeneous chronic respiratory disease, with the outbreak of COVID-19, it became important to establish whether people with asthma would be at increased risk of contracting or being seriously affected by another respiratory disease, SARS-CoV-2. While no increased risk of contracting COVID-19 or being seriously effected was shown1, nevertheless, people with asthma who required oral corticosteroids for their symptoms had an increased risk of death from COVID-191,7.
A review of the past 20 years of research on asthma concluded in a comparison to the substantial body of research in children and adults that only a few studies have focused on adolescents, and the evidence level in this regard is therefore low8. Stress-related psychiatric disorders, such as depression and anxiety, are more common among adults with asthma9,10. Conversely, a higher prevalence of anxiety is often observed in adolescents with asthma, and this has been shown to affect their night-sleep negatively11. Disturbed night-sleep in children with asthma is related to night-time symptoms, such as nocturnal cough12. Disturbed night-sleep with shorter sleep duration has been reported in adolescents with asthma13. Interestingly, an increased prevalence of asthma is coupled with neuropsychiatric disorders, such as autism spectrum disorder and, most commonly, attention deficit/hyperactivity disorder (ADHD)14,15. Having any psychiatric disorder may result in increased asthma exacerbation and more emergency-room visits8.
According to a national survey in the US, 5% of children and adolescents with asthma have one or more coexisting health conditions, which is a greater prevalence than among children without asthma16. Adolescents with asthma have a greater risk of migraines as compared with those without asthma17. Several somatic diseases, which can each be coupled to systemic inflammation, such as chronic rhinitis, atopic dermatitis, urticaria, anaphylaxis, chronic sinusitis, irritable bowel syndrome, thyroid diseases, and allergies, are overrepresented among adolescents with asthma as compared to those without asthma18.
Importantly, to understand the impact of the high prevalence of co-existing conditions on children’s and adolescents’ quality of life, it should be considered that every additional chronic condition that occurs with asthma is associated with a greater likelihood of the need for medical attention, care and missed school days16. If the symptoms of asthma cannot be controlled despite relevant treatment, then there is a possibility that comorbidities are not being assessed and correctly treated, which leads to problems in asthma treatment1. In the present study, we collected self-reported data from adolescents from five countries during the first year of the COVID-19 pandemic. Respondents with and without self-reported diagnoses of asthma described their somatic and mental health and rated the overall impact of the pandemic on their lives. The present study utilized data from the multinational MeSHe survey to investigate health profiles and pandemic-related perceptions among adolescents with and without asthma. Specifically, the study aimed to assess: (1) the prevalence of allergic and non-allergic somatic comorbidities among adolescents with asthma; (2) their levels of psychological distress across multiple domains; and (3) how they perceived the overall impact of the COVID-19 pandemic on their daily lives. By identifying patterns across five diverse countries, this study contributes to a deeper understanding of how adolescents with chronic conditions navigate physical and psychological challenges, especially in the context of global disruptions like the COVID-19 pandemic.
Methods
Procedure
The current analysis is based on data from the Mental and Somatic Health without borders (MeSHe) epidemiological study (https://meshe.se/), a cross-sectional, multinational survey investigating adolescent health and well-being. The MeSHe study employed a stratified sampling method targeting upper-secondary school students aged 15–19 years across Sweden, Vietnam, Serbia, Morocco, and the US. Data collection occurred between September 2020 and February 2021 using paper-based and/or online survey methods, depending on country-specific logistics. Overall, 5114 adolescents participated, yielding a response rate of approximately 85% based on school attendance figures provided by participating institutions. A full description of the study protocol and procedures is available in Kerekes et al.19. The MeSHe survey, which was available in paper-and-pen and/or electronic versions, was translated into the participating countries’ languages and consisted of several validated questionnaires capturing adolescents’ self-rated mental and physical health; aggressive, antisocial, and self-harm behaviours; intensity and frequency of leisure time physical activity; mood; and personality. During this data collection, the MeSHe survey was completed along with a COVID-19-related questionnaire.
Participants
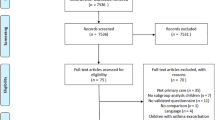
The comprehensive MeSHe survey was completed by 5114 adolescents who were 15–19 years old (mean age 16.69, SD = 1.02). Table 1 summarizes the national and gender distribution of our study population. Asthma diagnosis was assessed through a self-report item asking whether the respondent had ever received a physician’s diagnosis of asthma. No additional questions about asthma symptoms or medication use were included in the survey. Although this self-report method aligns with international epidemiological approaches, we acknowledge the limitation of not being able to validate diagnoses with symptom data or clinical records. A total of 225 participants (4.4%) were excluded from the analysis due to missing or uncertain responses to the asthma question. Specifically, 64 did not respond and 161 selected “don’t know.” These individuals were excluded to ensure the validity of the comparison between clearly defined groups with and without asthma. There were also 82 respondents reporting a non-binary gender or not responding to the question concerning their gender identity. Excluding all the previously listed categories, the final study population in the present study consisted of 4807 adolescents.
Questionnaires
In the present study, the following instruments were utilized.
MeSHe health survey
The MeSHe health survey includes questions about the self-reported existence of somatic diseases and complaints. The survey has previously been used in adolescent populations20,21 and has shown good test-retest reliability20.
Brief Symptom Inventory (BSI)
The BSI measures an adolescent’s perceived mental distress and assesses it via 53 items in nine primary domains (somatization, obsession-compulsion, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation, and psychoticism) and a global index, the General Severity Index (GSI), which measures overall psychological distress levels. The BSI domains and its GSI have shown good reliability in multinational adolescent study samples, except for the hostility domain22; therefore, in the present study, we report scores for eight of the primary domains and the GSI.
The impact of the COVID-19 pandemic
In the COVID-19-related questionnaire, that was part of the MeSHe survey, there was one item that asked the respondent to rate, with a number between 0 (slight or no effect at all) and 10 (affected me immensely), the overall impact of the COVID-19 pandemic on their everyday life.
Godwin–Shephard leisure-time physical activity questionnaire (LTEQ)
The LTEQ is a 3 + 1-item scale for assessing the frequency and intensity of leisure-time physical exercise during a typical seven-day period23. The first three items measure how often the respondent engages in leisure-time physical activities of various intensities (mild, moderate, and strenuous). Based on the reported frequency of the workouts, the intensity of leisure-time exercise can be calculated mathematically (total leisure-time physical activity = 3 x mild + 5 x moderate + 9 x strenuous activities)23. The fourth item of the LTEQ is an independent question that measures the frequency of the various types of exercise that lasted longer than 15 min during the respondent’s leisure time. In the present study, we used the total leisure-time physical activity scores.
Statistical analysis
The Statistical Package for the Social Sciences (SPSS) Version 28.0 was used for analyses. Descriptive statistics: frequencies (%), mean (M) and standard deviation (SD) were calculated. To compare asthma prevalence in adolescents between different country and the prevalence of somatic complaints/diagnoses between adolescents with and without asthma, Pearson’s Chi-square with risk estimate (odds Ratio) and Fisher’s exact tests were used, as well as Cramer’s V to report the effect size (small [0.10–0.29], medium [0.30–0.49] or large [≥ 0.500] with one degrees of freedom). Because the data on the scales were not normally distributed (p < 0.001 based on the Kolmogorov-Smirnov test), to compare the impact of COVID-19 and the level of psychological distress in adolescents with and without asthma, the Mann–Witney U-test was used, and η2 to report effect size (η2 = Z2/(N-1)) where η2 = 0.01 indicates a small effect; η2 = 0.06 indicates a medium effect; η2 = 0.14 indicates a large effect. To explore whether the relationship between asthma and comorbid somatic conditions varied by gender, interaction terms (condition × gender) were included in the logistic regression models. Only participants identifying as male or female were included in these analyses. Internal consistency of the psychometric scales used in the study was evaluated using Cronbach’s alpha. Across the instruments used, Cronbach’s alpha ranged from 0.73 to 0.97, indicating acceptable to excellent reliability. These values apply to the eight domains and the global index (GSI) of the Brief Symptom Inventory (BSI).
Results
The prevalence of asthma in a multinational sample of adolescents
Approximately 9% (n = 448) of the respondents, a similar proportion of both genders, reported having received a doctor-diagnosed asthma diagnosis. There were 3.2% (n = 161) who did not know whether they had asthma or not. The distribution of the asthma cases and those with indefinite responses is provided according to nationality in Table 2.
The differences in the prevalence of asthma and in the proportion of adolescents who did not know if they have asthma or not was significant, with a small effect size (Cramer’s V = 0.153, p < 0.001) between countries. In the US and Sweden, considerably more and, in Vietnam and Morocco, considerably fewer adolescents reported asthma, while in Vietnam and Morocco, considerably more and, in Serbia, considerably fewer adolescents reported that they were unsure whether they had asthma than was statistically expected.
The prevalence of somatic complaints in adolescents with and without asthma
Table 3 summarizes the prevalence of defined somatic diseases and gastrointestinal complaints in the study population. The prevalence of each somatic disease, except cancer, diabetes, epilepsy, and skin diseases, and the two assessed gastrointestinal complaints (constipation and diarrhoea) were significantly more frequently reported in adolescents with asthma as compared to those reporting no asthma. The odds of an adolescent who had asthma also reporting the existence of other allergies was increased 10-fold as compared to an adolescent who had no asthma. The co-occurrence of allergies with asthma showed a moderately strong difference in effect as compared to the prevalence of allergies in adolescents without asthma (Cramer’s V = 0.36). There was a high odds ratio for with asthma coexisting with tuberculosis; however, the effect size of this association was negligible due to the low prevalence of tuberculosis in our study population. The odds of an adolescent with asthma also suffering from other inflammatory/autoimmune diseases, such as celiac disease, thyroid diseases, or rheumatologic disease, were 2–3-fold higher than those of an adolescent without asthma, and the odds of asthma were increased by 70% in cases of migraine, however, each of these had a negligible effect size (data not shown).
In the initial logistic regression models testing the association between asthma and various somatic conditions, gender was included as a covariate. Across these models, gender alone did not significantly predict asthma status. However, a significant interaction was found between gender and thyroid disease (p = 0.017), indicating a differential association by gender. To further explore this, we conducted stratified analyses by gender. As shown in Table 4, adolescent men with asthma had notably higher odds of reporting certain co-occurring somatic conditions and gastrointestinal complaints compared to adolescent women with asthma. These differences were especially pronounced for cancer, diabetes, thyroid disease, tuberculosis, and constipation, where odds ratios in adolescent men were several times greater than those observed in their female counterparts.
The level of psychological distress in adolescents with and without asthma
Adolescents with asthma reported a significantly higher distress level in each domain of the BSI and on the GSI as compared to adolescents without asthma, but with a negligible effect size, except for somatization, for which the effect size was small (Table 5).
When analyzing psychological distress levels in adolescent men and adolescent women with and without asthma, it appeared that the above-described differences were enlarged in adolescent women, while the difference in the level of phobic anxiety in adolescent men with and without asthma did not differ significantly (Table 6). Adolescent women with asthma reported a significantly but with negligible effect size increased levels of psychological distress in all domains and on the GSI than adolescent men with asthma (Table 6).
Leisure-time physical activity
The total score on the LTEQ was somewhat but not significantly (p = 0.21) lower in adolescents with asthma (M = 49.27; SD = 42.13, Md = 39) than in those without asthma (M = 52.10; SD = 43.77, Md = 43). There were no significant differences if the analysis was performed within the groups of adolescent men (p = 0.57) or adolescent women (p = 0.22).
The COVID-19 pandemic’s impact on adolescents with and without asthma
Adolescents reported the COVID-19 pandemic’s impact on their everyday lives on a scale between 0 and 10. The mean score for the study population was 4.46 (SD = 2.93). Adolescents with asthma reported a significantly (p = 0.026) lower impact (M = 4.16, SD = 2.90) on the part of the pandemic on their lives than adolescent without asthma (M = 4.47, SD = 2.92). There was no significant difference in the self-rated impact of the COVID-19 pandemic on adolescent women and adolescent men with asthma (p = 0.95); however, adolescent women with asthma reported a significantly (p = 0.009) lower impact (M = 4.19, SD = 2.90) on the part of the pandemic on their everyday lives than their same sex counterparts without asthma (M = 4.64, SD = 2.88). There was no significant difference between adolescent men with and without asthma concerning the impact of the COVID-19 pandemic on their everyday lives.
Discussion
The MeSHe project made it possible to assess the prevalence of somatic and mental health complaints and the impact of the COVID-19 pandemic in a multinational sample of adolescents with and without asthma. The prevalence of asthma, based on self-reports, was about 9%, with a similar prevalence having been reported in men and women, 15–19-year-old upper secondary school students at the end of 2020. The International Study of Asthma and Allergies in Children (ISAAC)24 indicated a comparably higher prevalence (13.0% and 14.6%) of asthma for 13–14-years-old men and women, respectively, in 2013. The prevalence of physician-diagnosed asthma in men aged 16 to 18 years old has been reported to be 11.4%25. The findings of this study reveal the highest prevalence in the adolescent multinational population was measured in Sweden and the US, and the lowest was measured in Vietnam. Wide variability in the prevalence of asthma has been previously identified not only between countries but also between regions in same country and even between different centres in the same city24. The reason for these variations is likely the complex combined effect of bio-psycho-social factors. It has been previously suggested that the prevalence of asthma in developing countries is increasing2. However, even in this context, there is no consensus in the research field26. In our multinational sample, the highest prevalence was indeed found in the two most developed countries (the US and Sweden, with both having prevalence rates around 16%). However, it is important to recognize that, in these countries, there was also the lowest rate of uncertainty about having asthma. The highest rate of those who did not know whether they have asthma or not was reported from Morocco, followed by Vietnam. This observation—of adolescents reporting uncertainty about whether they have received an asthma diagnosis—may reflect broader challenges related to health literacy, diagnostic communication, and access to health care. In contexts where healthcare systems are under-resourced or where disease awareness is lower, young people may be less likely to receive timely, clear information about chronic conditions like asthma. A recent study of Swedish adolescents with ADHD highlighted a related issue: adolescents who experienced greater uncertainty about their health status also reported increased somatic complaints and anxiety regarding undiagnosed conditions27. While our study does not focus on adolescents with ADHD, the parallel finding of diagnostic uncertainty among adolescents in countries like Vietnam and Morocco may suggest a shared vulnerability in health-related understanding. This underscores the need to support adolescents’ health literacy and ensure that diagnoses are clearly communicated across diverse healthcare settings.
Because the MeSHe survey did not measure socioeconomic status or family-related biological factors, we can only speculate regarding the reason for this significantly higher prevalence of asthma in developed countries. Our hypothesis is that the high quality of healthcare ensures widespread knowledge in such societies about the symptoms of asthma and enables the early identification of the disease.
Adolescents with asthma had significantly higher odds of having several somatic diseases and/or gastrointestinal complains. However, the difference in odds ratios was accompanied by a small or negligible effect size, except for the odds ratio for co-existing allergies. Allergies are the most common comorbidity, which aligns with the clinical phenotype of allergic asthma, which is triggered by allergens and classified as type 2 inflammation1. A similar result was found in a study from Italy involving children and adolescents, in which the clinical significance of type 2 inflammation in asthma pathology and its implications for the treatment of asthma were highlighted28. A better comprehension of the underlying mechanisms of asthma may contribute to our understanding of the disease and its association with various comorbidities, such as allergies.
In our study, adolescents with asthma reported a significantly higher prevalence of celiac disease and rheumatoid arthritis as compared to those without asthma. Our results corroborate a previous study29 that similarly demonstrated a higher likelihood of adolescents with celiac diseases also having asthma. Also, individuals with asthma have a significantly elevated risk of developing rheumatoid arthritis in comparison to those without asthma30. While these findings are aligned with our expectations, it is important to note that, in our study, although these differences were statistically significant, none of them reached the threshold for a small effect size. Therefore, they should be referred to with caution.
As As discussed above, both adolescent males and females with asthma demonstrated increased odds of reporting various co-occurring somatic conditions and gastrointestinal complaints. However, most of these associations were characterized by small effect sizes. Among adolescent males with asthma, the associations with thyroid disease, tuberculosis, and constipation reached statistical significance and showed small but meaningful effect sizes when compared to males without asthma. These results align with previous findings indicating that adolescent males with asthma commonly present with comorbidities such as chronic rhinitis, atopic dermatitis, urticaria, anaphylaxis, irritable bowel syndrome, and thyroid disorders18. Notably, that study did not report a higher prevalence of rheumatism, consistent with our own observations. Our analyses also revealed a significant interaction between gender and thyroid disease, suggesting that the relationship between asthma and thyroid disease differed by gender. Specifically, adolescent females with thyroid disease were more likely than their male counterparts to report asthma, which aligns with existing knowledge about gender differences in autoimmune and endocrine conditions. No other gender-by-condition interactions reached statistical significance. These findings underscore the importance of interpreting statistically significant results in the context of effect sizes and sample distribution and highlight the complexity of asthma-related comorbidities. They also point to the value of incorporating gender-sensitive perspectives in adolescent health research and care planning.
Adolescents with asthma exhibited a statistically significantly, albeit negligibly, higher level of psychological distress during the COVID-19 pandemic as compared to their counterparts without asthma. This discrepancy was particularly noticeable among adolescent women, who reported significantly higher levels of psychological distress than their men peers with asthma. It is noteworthy that adolescent women, in general, tend to exhibit significantly higher levels of psychological distress19,22,31. Thus, it is premature to conclude that the COVID-19 pandemic placed any elevated psychological burden on adolescents with asthma. Surprisingly, these individuals, mainly adolescent women, reported a significantly lower impact on the part of COVID-19 as compared to their peers without asthma. This may be attributed to their limited exposure to severe COVID-19 cases given their age and asthma. In a Swedish asthma population under the age of 18, only 0.02% (eight out of 46,123 patients) required hospitalization due to COVID-1932. Similarly, in the US, among 5656 children aged 5 to 18, there were no COVID-19-related hospitalizations33. During the pandemic years, as stated by GINA1, the consistent use of asthma medication remained crucial. Notably, during these years, there was a significant reduction in asthma exacerbation33. Concurrently, visits to pediatric emergency departments due to asthma showed a significant decline34. Maintaining optimal asthma control minimizes the risk of exacerbation, subsequently reducing the likelihood of hospitalization and lowering COVID-19 exposure35. The benefits of adhering to inhaled corticoid steroid treatment clearly outweigh the potential risks of severe COVID-19. As a result, recommendations endorse the utilization of inhaled corticoid steroid in individuals with asthma35,36.
Based on our findings, another potential protective factor working against the adverse psychological impact of the COVID-19 pandemic on adolescents with asthma is their level of leisure-time physical activity, which is comparable to that of their peers without asthma. In contrast, a few years ago, research suggested that adolescents with asthma exhibited lower levels of physical activity as compared to those without asthma37. The current findings could reflect the positive outcomes of enhanced asthma care, in which structured education emphasizes the significance of engaging in physical activity1. Regular physical activity offers important health benefits and can positively impact asthma control and lung function1. Moreover, evidence indicates that physical activity is associated with reduced psychological distress38. This dual benefit highlights the potential role of physical activity in mitigating both the physical and psychological challenges posed by asthma, particularly in the context of the COVID-19 pandemic. In addition to individual-level factors, the broader national context may have influenced how adolescents with asthma perceived the pandemic’s impact. Our study included participants from five countries with varying public health strategies. For instance, Sweden did not impose formal lockdowns, while Vietnam and Serbia implemented stricter restrictions. These policy differences may have shaped adolescents’ day-to-day experiences during the pandemic. Although both groups—those with and without asthma—were drawn from the same upper secondary high-school populations within each country, and were thus similarly exposed to national conditions, the overall comparison must still be interpreted with caution. It is plausible that the milder reported COVID-19 impact among adolescents with asthma reflects both effective asthma management and contextual factors such as reduced social disruption in certain countries. Taken together, these findings suggest that both effective asthma self-management and national-level public health strategies may have played a role in buffering the perceived impact of the COVID-19 pandemic among adolescents with asthma, offering new insights into resilience factors in youth with chronic conditions.
Strengths and limitations
This study offers several strengths that enhance its contribution to the understanding of adolescent health during the COVID-19 pandemic. First, its multinational scope—encompassing upper-secondary students from five culturally and geographically diverse countries—enables a broad perspective on adolescent well-being across contexts. The sample size is substantial, and the inclusion of both adolescents with and without asthma allowed for comparative analyses across key physical and psychological domains. Second, the study collected data during the first year of the pandemic, providing timely insight into how adolescents perceived and responded to an unprecedented global health crisis. Third, the dataset uniquely enabled a comprehensive examination of coexisting somatic conditions, psychological distress, and physical activity levels among adolescents with asthma, contributing to the limited literature on chronic illness in youth during times of societal stress.
Despite these strengths, several limitations must be acknowledged. One notable limitation is the study’s reliance on self-reported data, including asthma diagnosis and psychological symptoms. While self-report methods are common and practical in large-scale adolescent research, they may introduce recall bias or inaccuracies in diagnostic reporting. The relatively high proportion of adolescents who indicated uncertainty about whether they had asthma further underscores this point, highlighting that the findings are not based on clinically verified diagnoses. In addition, the study did not include measures of asthma severity or control, which would have allowed for more nuanced interpretation of health outcomes within the asthma subgroup.
The cross-sectional design is another limitation, as it precludes any causal conclusions. All associations observed—between asthma status, comorbidities, psychological distress, and the perceived impact of the pandemic—are correlational and should be interpreted accordingly.
Moreover, while we reported asthma prevalence at the country level, we refrained from conducting stratified country-specific analyses due to the non-representative nature of national subsamples. As such, findings are best understood in relation to the overall multinational sample and should not be generalized to specific national populations.
Lastly, national context is an important consideration. The five participating countries implemented markedly different public health strategies during the pandemic. For example, Sweden did not enforce formal lockdowns, while Vietnam and Serbia applied stricter containment measures. These differences may have influenced how adolescents perceived the pandemic’s impact. Although both groups—those with and without asthma—were drawn from the same school populations within each country, and thus likely experienced similar contextual exposures, we acknowledge that country-level policy environments could have affected self-reported outcomes. We now address this more explicitly in the Discussion, urging caution in interpreting the results without considering the broader societal context.
Conclusion
This multinational study offers important insights into the somatic and mental health of adolescents with asthma during the COVID-19 pandemic. Adolescents with asthma reported slightly higher levels of psychological distress than their peers without asthma, particularly among females. However, the overall impact of the pandemic on daily life was perceived as lower in the asthma group. Physical activity levels were comparable between groups, suggesting potential resilience factors among adolescents managing chronic illness.
The results also highlight significant variability in self-reported asthma prevalence and diagnostic certainty across countries, pointing to differences in health literacy, diagnostic practices, and healthcare access. Notably, the higher proportion of adolescents in Vietnam and Morocco who were unsure about their asthma diagnosis underlines the importance of clear health communication and supports the need for improved adolescent health literacy.
While the findings must be interpreted in light of the study’s cross-sectional design and non-representative national samples, they underscore the complexity of asthma’s psychosocial context in adolescence. They also emphasize the value of cross-national perspectives in understanding how public health infrastructure and cultural factors may shape young people’s experiences of chronic illness, particularly during global disruptions such as the COVID-19 pandemic.
Data availability
Data will be made available on reasonable request to the project leader, Professor Nóra Kerekes (nora.kerekes@hv.se).
References
GINA. Global Initiative for Asthma; Global Strategy for Asthma Management and Prevention. https://ginasthma.org/ (2021).
GINA. Pocket Guid för Asthma Managhment and Prevention (2021).
Barrio Cortes, J. et al. Enfermedades crónicas en población pediátrica: comorbilidades y uso de servicios en atención primaria. An. de. Pediatría 93, 183–193, https://doi.org/10.1016/j.anpedi.2019.12.019 (2020).
CDC CfDCP. Vital signs: asthma prevalence, disease characteristics, and self-management education: United States, 2001–2009. MMWR. Morbidity Mortal. Wkly. Report. 60, 547–552 (2011).
Chowdhury, N. U., Guntur, V. P., Newcomb, D. C. & Wechsler, M. E. Sex and gender in asthma. Eur. Respir. Rev. 30, 210067, https://doi.org/10.1183/16000617.0067-2021 (2021).
Almqvist, C., Worm, M. & Leynaert, B. Impact of gender on asthma in childhood and adolescence: a GA2LEN review. Allergy 63, 47–57, https://doi.org/10.1111/j.1398-9995.2007.01524.x (2007).
Tashiro, H. & Shore, S. A. Obesity and severe asthma. Allergol. Int. 68, 135–142, https://doi.org/10.1016/j.alit.2018.10.004 (2019).
Landeo-Gutierrez, J. & Celedón, J. C. Chronic stress and asthma in adolescents. Ann. Allergy Asthma Immunol. 125, 393–398, https://doi.org/10.1016/j.anai.2020.07.001 (2020).
Akula, M., Kulikova, A., Khan, D. A. & Brown, E. S. The relationship between asthma and depression in a community-based sample. J. Asthma 55, 1271–1277, https://doi.org/10.1080/02770903.2017.1418885 (2018).
Ye, G., Baldwin, D. S. & Hou, R. Anxiety in asthma: a systematic review and meta-analysis. Psychol. Med. 51, 11–20, https://doi.org/10.1017/S0033291720005097 (2021).
Fidler, A. et al. Anxiety among adolescents with asthma: relationships with asthma control and sleep quality. Clin. Pract. Pediatric Psychol. 7, 151–156, https://doi.org/10.1037/cpp000026710.1037/cpp0000267.supp (2019). (Supplemental).
Banasiak, N. C. Understanding the relationship between asthma and sleep in the pediatric population. J. Pediatric Healthc. 30, 546–550, https://doi.org/10.1016/j.pedhc.2015.11.012 (2016).
Estanislau, N. R. D. A. et al. Association between asthma and sleep hours in Brazilian adolescents: ERICA. J. de. Pediatr. 97, 396–401, https://doi.org/10.1016/j.jped.2020.07.007 (2021).
Cortese, S. et al. Association between attention deficit hyperactivity disorder and asthma: a systematic review and meta-analysis and a Swedish population-based study. Lancet Psychiatry 5, 717–726, https://doi.org/10.1016/S2215-0366(18)30224-4 (2018).
Kaas, T. H. et al. Association between childhood asthma and attention deficit hyperactivity or autism spectrum disorders: a systematic review with meta‐analysis. Clin. Exp. Allergy 51, 228–252, https://doi.org/10.1111/cea.13750 (2021).
Patel, M. R., Leo, H. L., Baptist, A. P., Cao, Y. & Brown, R. W. Asthma outcomes in children and adolescents with multiple morbidities: findings from the National Health Interview Survey. J. Allergy Clin. Immunol. 135, 1444–1449, https://doi.org/10.1016/j.jaci.2014.11.008 (2015).
Graif, Y., Shohat, T., Machluf, Y., Farkash, R. & Chaiter, Y. Association between asthma and migraine: a cross-sectional study of over 110 000 adolescents. Clin. Respir. J. 12, 2491–2496, https://doi.org/10.1111/crj.12939 (2018).
Cohen, S. et al. Co-morbidities and cognitive status in a cohort of teenagers with asthma. Pediatric Pulmonol. 51, 901–907, https://doi.org/10.1002/ppul.23443 (2016).
Kerekes, N. et al. Changes in Adolescents’ psychosocial functioning and well-being as a consequence of long-term COVID-19 restrictions. Int. J. Environ. Res. Public. Health 18, 20210819, https://doi.org/10.3390/ijerph18168755 (2021).
Zouini, B., Sfendla, A., Senhaji, M., Råstam, M. & Kerekes, N. Somatic health and its association with negative psychosocial factors in a sample of Moroccan adolescents. SAGE Open. Med. 7, 72050312119852527 (2019).
Kerekes, N., Zouini, B., Tingberg, S. & Erlandsson, S. Psychological distress, somatic complaints, and their relation to negative psychosocial factors in a sample of swedish high school students. Front. Public. Health 9, 669958, https://doi.org/10.3389/fpubh.2021.669958 (2021).
Nguyen, H. T. M. et al. The COVID-19 pandemic and Adolescents’ psychological distress: a multinational cross-sectional study. Int. J. Environ. Res. Public. Health 19, 8261, https://doi.org/10.3390/ijerph19148261 (2022).
Godin, G. The godin-shephard leisure-time physical activity questionnaire. Health Fit. J. Can. 4, 18–22 (2011).
Mallol, J. et al. The International Study of Asthma and Allergies in Childhood (ISAAC) phase three: a global synthesis. Allergol. Immunopathol. 41, 73–85, https://doi.org/10.1016/j.aller.2012.03.001 (2013).
Alruwaili, M. F. & Elwan, A. Prevalence of asthma among male 16 to 18-year-old adolescents in the Northern Borders Region of Saudi Arabia. Electron. Physician 10, 6920–6926, https://doi.org/10.19082/6920 (2018).
Asher, M. I., García-Marcos, L., Pearce, N. E. & Strachan, D. P. Trends in worldwide asthma prevalence. Eur. Respir. J. 56, 2002094, https://doi.org/10.1183/13993003.02094-2020 (2020).
Lundqvist, S., Röjås, S., Bador, K., Råstam, M. & Kerekes, N. Somatic comorbidities and health related uncertainty among Swedish adolescents with ADHD. Front. Psychiatry 16, 1534280, https://doi.org/10.3389/fpsyt.2025.1534280 (2025).
Licari, A. et al. Asthma in children and adolescents: the ControL’Asma project. Acta Biomed. 91, e2020002, https://doi.org/10.23750/abm.v91i11-S.10295 (2020).
Assa, A., Frenkel-Nir, Y., Tzur, D., Katz, L. H. & Shamir, R. Large population study shows that adolescents with celiac disease have an increased risk of multiple autoimmune and nonautoimmune comorbidities. Acta Paediatr. 106, 967–972, https://doi.org/10.1111/apa.13808 (2017).
Charoenngam, N. et al. Patients with asthma have a higher risk of rheumatoid arthritis: a systematic review and meta-analysis. Semin. Arthritis Rheum. 50, 968–976, https://doi.org/10.1016/j.semarthrit.2020.07.015 (2020).
Zouini, B., Sfendla, A., Hedman Ahlström, B., Senhaji, M. & Kerekes, N. Mental health profile and its relation with parental alcohol use problems and/or the experience of abuse in a sample of Moroccan high school students: an explorative study. Ann. Gen. Psychiatry 18, 1–8 (2019).
Karlsson Sundbaum, J. et al. Severe COVID-19 among patients with asthma and COPD: a report from the Swedish National Airway Register. Ther. Adv. Respir. Dis. 15, 17534666211049738, https://doi.org/10.1177/17534666211049738 (2021).
Hurst, J. H., Zhao, C., Fitzpatrick, N. S., Goldstein, B. A. & Lang, J. E. Reduced pediatric urgent asthma utilization and exacerbations during the COVID-19 pandemic. Pediatr. Pulmonol. 56, 3166–3173, https://doi.org/10.1002/ppul.25578 (2021).
Levene, R., Fein, D. M., Silver, E. J., Joels, J. R. & Khine, H. The ongoing impact of COVID-19 on asthma and pediatric emergency health-seeking behavior in the Bronx, an epicenter. Am. J. Emerg. Med. 43, 109–114, https://doi.org/10.1016/j.ajem.2021.01.072 (2021).
Hasan, S. S., Capstick, T., Zaidi, S. T. R., Kow, C. S. & Merchant, H. A. Use of corticosteroids in asthma and COPD patients with or without COVID-19. Respir. Med. 170, 106045, https://doi.org/10.1016/j.rmed.2020.106045 (2020).
Bloom, C. I. et al. Risk of adverse outcomes in patients with underlying respiratory conditions admitted to hospital with COVID-19: a national, multicentre prospective cohort study using the ISARIC WHO Clinical Characterisation Protocol UK. Lancet Respir. Med. 9, 699–711, https://doi.org/10.1016/s2213-2600(21)00013-8 (2021).
Groth, S. W., Rhee, H. & Kitzman, H. Relationships among obesity, physical activity and sedentary behavior in young adolescents with and without lifetime asthma. J. Asthma 53, 19–24, https://doi.org/10.3109/02770903.2015.1063646 (2016).
Okuyama, J. et al. Mental health and physical activity among children and adolescents during the COVID-19 pandemic. Tohoku J. Exp. Med. 253, 203–215, https://doi.org/10.1620/tjem.253.203 (2021).
World Medical Association of Helsinki. World Medical Association declaration of Helsinki: ethical principles for medical research involving human subjects; Seoul 2008. Guildford: Canary Publications; (2008), p. 8.
Acknowledgements
We would like to express our gratitude to all the young people who took the time to respond to the online questionnaire. We thank Professor Britt Hedman Ahlström (Sweden); Dr. Btissame Zouini, Dr. Anis Sfendla, and Professor Meftaha Senhaji (Morocco); Professor Zsuzsa Szombathyne Meszaros (US); Dr. Dejan Stevanovic (Serbia); and Professor Hang Thi Minh Nguyen (Vietnam) for coordinating data collection in the participating countries.
Funding
Open access funding provided by University West.
Author information
Authors and Affiliations
Contributions
Conceptualization, M.E. and N.K.; methodology, M.E, K.B., and N.K.; formal analysis, M.E. and K.B; writing—original draft preparation, M.E. and N.K.; writing—review and editing, M.E, K.B.,C.J and N.K.; visualization, M.E. and K.B.; supervision, N.K.; project administration, N.K.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The ethical principles of the Helsinki Declaration39 were followed in the MeSHe study. In each participating country, the national, regional, or institutional ethic board has reviewed and approved the study. In Sweden, this was The National Ethical Board, Dnrs: 689–17 and 2020-03351. In the USA, this was The Institutional Review Board for the Protection of Human Subjects, SUNY Upstate Medical University, 1651637-32020-E. In Morocco, this was The Regional Directorate of the Ministry of National Education in Tetouan authorization number 85. In Vietnam, this was the Review Board of the Center for Assisting and Consulting Psychology, University of Social Sciences and Humanities, Hanoi, RPSY-101. In Serbia, this was the ethics committee of the Clinic for Neurology and Psychiatry for Children and Youth Belgrade, No. 21-85/2. All data collection was based on voluntary and anonymous participation, which means that no tracking or follow-up of individuals is possible.
Content for publications
All authors have read and agreed to the published version of the manuscript.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Emilsson, M., Bador, K., Johansson, C. et al. Somatic and mental health of and the COVID-19 pandemic’s impact on adolescents diagnosed with asthma. npj Prim. Care Respir. Med. 35, 37 (2025). https://doi.org/10.1038/s41533-025-00444-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41533-025-00444-8