Abstract
This study aimed to assess the magnitude of hematological toxicity and associated factors in newborns with hyperbilirubinemia. A cross-sectional study was conducted from April to December 2023. A total of 247 newborns were included. The data were collected using questionnaires and a data extraction sheet. Four 4 ml of blood was collected. A Sysmex KX-21 analyzer was used for blood analysis, and a Mindray BS-240 analyzer was used for bilirubin measurement. The data were entered into Epi-data and analyzed by SPSS. The logistic regression was used. The P value was set at 0.05. Before phototherapy, the hematological toxicities, such as anemia, leucopenia, and thrombocytopenia, were 45.7%, 22.2%, and 6.1%, respectively, whereas after phototherapy, anemia and thrombocytopenia, significantly increased, but the leucopenia, significantly decreased. The risk of developing anemia increased, 3.5, 2.7, and 2.1-fold among newborns with bilirubin > 18 mg/dl, with Rh blood group incompatibility, and treated with intensive phototherapy, respectively. Both low birth weight and intensive phototherapy increased the incidence of thrombocytopenia by 2 and 3.4-fold, respectively. Hematological toxicity was found to be a severe public health issue in newborns. Thus, strict follow-up and early detection of toxicity by considering aggravation factors are necessary.
Similar content being viewed by others
Introduction
Hyperbilirubinemia is a complication that occurs when the serum bilirubin concentration exceeds 5 mg per deciliter (mg/dl) within 24 h after birth1. It is characterized by yellowish discoloration of the skin, sclera, conjunctiva, and tongue2. Hyperbilirubinemia can be classified as physiological or pathological3. Physiologically, the bilirubin levels of newborns may increase up to one week after birth4. On the other hand, pathologically, bilirubin levels in newborns may precedes as increased after 1 week of birth5.
Hyperbilirubinemia is a common complication in newborns. Globally, approximately 24 million newborns are at risk for developing hyperbilirubinemia each year6. It affects nearly 60% of term and 80% of preterm newborns7 and frequently results in hospitalization6. More than 75% of affected newborns are born in low- and middle-income countries, with a high prevalence in South Asian regions and sub-Saharan Africa8. In Ethiopia, hyperbilirubinemia is the tenth most common cause of neonatal mortality and morbidity9. The common causes of hyperbilirubinemia in newborns are blood group incompatibility, glucose-6-phosphate dehydrogenase (G6PDH) deficiency, liver disease, treatment side effects, polycythemia, neonatal sepsis, maternal factors, excessive weight loss, and inappropriate feeding10,11.
Moreover, pathological hyperbilirubinemia can result in various complications, such as lethargy, fever, irritability, oculomotor impairments, encephalopathy, neurotoxicity, and hematological toxicity9,12. To minimize these complications, treatment is needed. The main treatment options for pathological hyperbilirubinemia are phototherapy (PT), exchange transfusion13, and pharmacological treatment14. These treatments are not safe and can also cause different side effects, such as hematological toxicity15,16.
In newborns with hyperbilirubinemia, the cause of hematological abnormalities may be related to the initial cause of hyperbilirubinemia, the toxic effect of elevated bilirubin, and the side effects of treatment, especially PT15,17,18. The initial cause of hyperbilirubinemia can result in hematological abnormalities through decreasing the survival and production of blood cells. On the other hand, elevated bilirubin in serum affects hematological parameters by functioning as an antimutagenic agent, inducing antioxidant, immune-modulatory, and inducing antiproliferative and anti-apoptotic factors, degrading hemoglobin (Hb), and damaging DNA19. Phototherapy also induces hematological toxicity by directly damaging the cell membrane of blood cells and increasing blood cell vulnerability to apoptosis20. Besides, PT can affect hematological parameters through directly inducing the expression of cytokines and growth factors as well as the generation of reactive oxygen species (ROS)21,22.
The synergistic effect of the initial cause of hyperbilirubinemia, the toxic effect of hyperbilirubinemia and PT side effects strongly increase the magnitude of hematological toxicity in newborns with hyperbilirubinemia23. In addition, factors such as the age of the newborn, low birth weight, genetic variability, polycythemia, sex, drugs, race, altitude, oxytocin induction, maternal illness, use of breast milk, type of PT used, duration of PT and presence of hemolytic disease affect hematological parameters in newborns with hyperbilirubinemia24.
Hematological toxicities such as anemia, thrombocytopenia and impaired immune function can aggravate morbidity and mortality and negatively affect quality of life in newborns with hyperbilirubinemia25,26. As a result, investigating hematological toxicity and associated factors before and after hyperbilirubinemia treatment is important to benefit from early detection, prevention, and treatment of this toxicity27,28. This may help newborns with hyperbilirubinemia receive timely healthcare. In addition, investigating hematological toxicity may help policy makers develop and implement new guidelines. However, there is limited information regarding hematological toxicity and associated factors before and after PT among newborns with hyperbilirubinemia in Ethiopia and in the study setting. Therefore, the current study was performed to fill this gap by providing information that can ultimately reduce the risk of complications and improve outcomes for affected newborns.
Methods and materials
Study area, design, and period
The cross-sectional study was carried out among newborns with hyperbilirubinemia in Northwest Ethiopia from April 1 to December 30, 2023. The hospital is located approximately 738 km northwest of Addis Ababa, the capital city of Ethiopia, with an elevation of 2133 m above sea level and latitude and longitude of 12° 36′ N and 37′ 28′ E, respectively. The hospital is a teaching hospital in Ethiopia that provides health care services for more than 7 million individuals in a Gondar town and catchment area. It has different units; the neonatal intensive care unit offers critical care services to neonates and has a capacity of approximately 40 beds at any given time29.
Population
All newborns with hyperbilirubinemia who were treated with PT in northwest Ethiopia were considered source populations. Moreover, all newborns with hyperbilirubinemia who were treated with PT in northwest Ethiopia within the study period were considered as study population.
Eligibility criteria
All newborns aged up to 28 days who were confirmed to have hyperbilirubinemia by laboratory tests and who received PT during the study period were included in this study. Newborns who had severe comorbidities, who were critically ill, who took immunosuppressants, who received iron supplements, who had critically ill mothers and whose mothers were not around were excluded from the study.
Variables
Hematological toxicity was considered an outcome variable. On the other hand, sociodemographic characteristics and clinical characteristics of the newborns, such as age, sex, weight, height, gestational age, feeding status, blood group, cause of hyperbilirubinemia, length of hospital stay, total serum bilirubin (TSB) level, place of delivery, duration of PT received, and type of PT, were considered explanatory variables. In addition, the sociodemographic, clinical, and obstetric characteristics of mothers, such as mother’s age, history of sibling, mode of delivery, mother’s residence, mother’s blood group status, birth order, mother’s complications, and maternal iron and folate status, were considered explanatory variables.
Sample size and sampling techniques
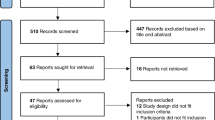
In the present study, the sample size was calculated by following a single population proportion formula using the following formula: Zα/2 = 1.96, margin of error (d) = 5%, and expected magnitude of hematological toxicity = 50%, since no similar previous study regarding hematological toxicity in newborns with hyperbilirubinemia during the study period has been conducted. Subsequently, the sample size was calculated to be 384. However, the estimated study population was less than 10,000 in the study area, and the sample size correction formula was used. After the correction, the final sample size used in the current study was 247. The study participants were selected through the application of a systematic random sampling technique. To obtain actual study participants, the Kth interval was calculated and found to be two. Then, by using the lottery method, the first newborn was selected, and subsequently, in every two intervals, all study participants were selected.
Definitions
Hematological abnormalities were defined based on the hematological reference range of newborns by considering gestational and postnatal ages. Exclusive breastfeeding was defined as the practice in which a newborn solely consumes breast milk and not other liquids or solids30. Exclusive formula feeding was also defined as consuming only formula for the entire preceding time period31. Mixed feeding was defined as the practice in which breastfeeding by the newborn is supplemented with infant formula32.
Data collection and laboratory methods
The demographic and clinical information of the study participants was collected using a structured interview-based questionnaire and a data extraction sheet by two trained nurse professionals. The questionnaires were developed by using American Academy of Pediatrics Clinical Practice Guidelines and by reviewing different studies5,12,33. Four milliliters of venous blood were collected before and after PT for laboratory analysis using a syringe under aseptic conditions by two trained laboratory professionals from each newborn. After collection, 2 ml of blood was transferred to a di-potassium ethylenediaminetetraacetic acid test tube for complete blood count and blood grouping. The remaining blood was transferred to a serum separator tube for bilirubin measurement. The collected samples were then transported to the analysis unit.
Complete blood analysis was performed using the Sysmex KX-21 automated three-differential hematology analyzer by senior medical laboratory technologists. The analyzer used a combination of impedance and optical principles for blood cell counts. In addition, the analyzer uses a spectrophotometric principle to measure the Hb concentration. Total and direct serum bilirubin levels were analyzed using a Mindray BS-240 automated chemistry analyzer by a senior medical laboratory technologist. It operated on the principles of photometry and potentiometry. Blood group of each newborn was determined using commercially prepared reagents and the forward blood grouping technique by the principal investigators. All laboratory analyses were performed in strict accordance with the manufacturer’s instructions and standard laboratory operating procedures. After analysis, all laboratory data were collected by data extraction sheets by two trained laboratory professionals.
Data management and quality control
In the present study, to ensure the consistency of the questionnaires, they were initially prepared in the English language, translated into the local language and then retranslated back to English. Following this process, a pretest was performed on 5% of the total sample, and then, based on feedback, relevant modifications were made. One-day training was given for the data collectors about the data collection process and protocol. The performance of the hematology and clinical chemistry analyzer was assured by running commercially prepared quality control reagents. All laboratory data were collected through strict adherence to standard operational procedures. Furthermore, the investigators closely followed the data collection process and provided timely feedback.
Data analysis and interpretation
The completeness of the collected data was checked manually, and the data were entered into Epi-data software (version 4.6.0). Subsequently, the data were exported to SPSS version 25.0 for analysis. The data were described using descriptive statistics and are presented in tables and figures. The paired chi-square test was used to determine the presence of significant differences in hematological toxicity before and after PT. Additionally, independent chi-square test was used to determine the presence of a significant association between the outcome and the explanatory variable. The strength of the association between hematological toxicity and the explanatory variable was measured using bivariable and multivariable logistic regression models. Multivariable logistic regression analysis was used for explanatory variables with p values less than 0.25 in bivariable logistic regression analysis to control for possible confounders. All logistic regression assumptions were checked and fitted. The crude odds ratio (COR) and adjusted odds ratio (AOR) within the 95% confidence interval (CI) were used to measure the degree of association between the bivariable and multivariable logistic regression analyses, respectively. For all the statistical analyses, a p value < 0.05 was used to determine the level of statistical significance.
Ethical consideration
Ethical approval was obtained from the ethical review committee of the School of Biomedical and Laboratory Science, College of Medicine and Health Sciences, University of Gondar with the letter reference number SBMLS 510/2023. Additionally, a permission letter was obtained from the hospital Chief Clinical Director. After providing an explanation of the possible benefits and risks, informed written consent was obtained from the parents or legal guardians. The collected data were kept confidential. Any abnormal findings obtained were linked to physicians for appropriate patient management.
Consent to participate and ethical approval
All the procedures were performed in accordance with the relevant guidelines and regulations. Ethical approval was obtained from the Ethical Review Committee of the School of Biomedical and Laboratory Sciences, College of Medicine and Health Science, the University of Gondar (Ref number SBMLS 510/2023). The objective and purpose of the study were explained to the medical director, and a permission letter was obtained to collect the data. After providing an explanation of the possible benefits and risks, informed written consent was obtained from the parents or legal guardians. The collected data were kept confidential. Any abnormal findings obtained were linked to physicians for appropriate patient management.
Results
Sociodemographic and clinical characteristics of newborns with hyperbilirubinemia
A total of 247 newborns with hyperbilirubinemia were enrolled in the study, for a 100% response rate. The majority of these, were male (142, 57.5%), aged less than 7 years (64.8%), had a gestational age less than 37 weeks (152, 72.9%), and had a birth weight less than 2.5 kg (141, 57.1%). Before PT treatment, 178 (72.1%) newborns had TSB levels greater than 18 mg/dl, but after treatment, the TSB levels of all newborns were less than 18 mg/dl. About 66% of newborns with hyperbilirubinemia had taken intensive PT. Regarding the cause of hyperbilirubinemia, ABO incompatibility (109/44.1%) was found to be the main cause (Table 1).
Sociodemographic and clinical characteristics of the mothers
The sociodemographic and clinical characteristics of all mothers whose newborns developed hyperbilirubinemia were included in this study. The majority of mothers included were aged less than 25 years (49.0%), followed by those aged between 25 and 35 121 years (39.3%). Seventy-nine (32.0%) mothers who participated in the study had a previous history of hyperbilirubinemia in newborns. Concerning birth order, 179 (72.5%) mothers were multiparous. Of the mothers included, 53 (21.5%) had complications, and 150 (60.7%) had taken iron and folate supplements during pregnancy (Table 2).
Hematological toxicities in newborns with hyperbilirubinemia before and after PT initiation
According current study, median value (IQR) of white blood cell, hemoglobin, platelet and MCV before PT were 14.5 (12.6–16.2), 10.9 (9.1–12.6), and 241 (187–241), whereas median value of white blood cell, hemoglobin, platelet and MCV after PT were 13.5 (11.1–15.1), 11.3 (9.4, 13.2), and 233 (129–284), respectively. Before the initiation of PT, the magnitude hematological toxicity, such as anemia, leucopenia, and thrombocytopenia, were 115/46.6% (95% CI 40.1, 52.6), 52/21.1% (95% CI 16.2, 26.3), and 18/7.3% (95% CI 4.5, 10.5), respectively. After PT, the magnitudes of hematological toxicity, such as anemia and thrombocytopenia, significantly increased (p < 0.05) to 133/53.8% (95% CI 47.8, 60.3) and 78/33.6% (95% CI 25.9, 37.2), respectively. In contrast, after PT treatment, the magnitude of leucopenia significantly decreased (p value < 0.05) to 21/8.5% (95% CI 5.3, 12.1) (Fig. 1).
Among the patients who experienced anemia before PT treatment, 101/87.8% had normocytic normochromic anemia, whereas 10/8% and 4/3.6% had microcytic hypochromic and macrocytic normochromic anemia, respectively. On the other hand, after PT, only normocytic normochromic anemia (125/94%) and microcytic hypochromic anemia (8/6.1%) were observed. Of anemic newborns before PT, 60 (52.2%), 36 (31.3%), and 19 (16.5) were found as mild, moderate and severe, respectively. Similarly, out of anemia newborns after PT, 73 (54.9%), 39 (29.3%), and 21 (15.8%) were found as mild, moderate and severe, respectively). Furthermore, among anemic newborns, 87.7% was preterm, while among thrombocytopenic and leucopenia newborns 63.5% and 82.0%, respectively were preterm newborns (Fig. 2). Regarding WBC toxicity, lymphopenia was the most common toxicity observed before and after treatment [22/8.9% (95% CI 5.7, 12.6) and 16/6.9% (95% CI 4.0, 10.5), respectively] (Supplementary Table S1).
Factors associated with hematological toxicity
In current study, in bivariable analysis variable, age of newborn, birth weight, gestation age, concentration of TSB, mother’s residence, cause of hyperbilirubinemia, and height of neonate were significantly associated with hematological toxicities with p value of less than 0.25 before PT. After adjusting potential confounders, multivariate logistic regression analysis confirmed that, age of newborn, birth weight, concentration of TSB, mother’s residence, cause of hyperbilirubinemia, and height of neonate were found to be significant determinants for hematological toxicities before PT.
Newborns with hyperbilirubinemia before PT who were younger than seven days (AOR 2.5, 95% CI (1.4, 4.6) and whose TSB level was greater than 18 mg/dl (AOR 3.5, 95% CI (1.7– 7.2)) were more likely to develop anemia than were those aged less than seven days and whose TSB level was less than 18 mg/dl, respectively. The occurrence of anemia was about 3 times greater in newborns with Rh blood group incompatibility (AOR 2.7, 95% CI 1.7, 7.2) than in those with other causes of hyperbilirubinemia. Moreover, being a newborn of a rural resident mother increased the risk of developing anemia by 2.6 times (AOR 2.6, 95% CI (1.4, 4.7)) compared with being a newborn of an urban resident’s mother. The odds of thrombocytopenia were two times greater among newborns with birth weights less than 2.5 kg (AOR 2.0, 95% CI (1.0, 3.2)). An increase in the TSB decreased the risk of developing leucopenia by 60% (AOR 0.4, 95% CI (0.2, 0.8)) in contrast to a decrease in the TSB before PT (Table 4).
After PT variables such as type of PT received, duration of PT and birth weight after PT were significantly associated with hematological toxicities with p value of less than 0.25. After adjusting potential confounders, multivariate logistic regression analysis also affirmed that, all variables were found to be significant determinants for hematological toxicities.
Compared with conventional PT treatment, intensive PT treatment increased the risk of developing anemia (AOR 2.1, 95% CI (1.1, 4.2)) and thrombocytopenia (AOR 3.4, 95% CI (1.6, 6.9)) in newborns with hyperbilirubinemia. Newborns who received PT treatment for more than 48 h were approximately twice as likely to have anemia (AOR 1.8, 95% CI (1.1, 3.3)) and thrombocytopenia (AOR 2.1, 95% CI (1.6, 3.8)) than those who received PT treatment for less than 48 h. All factors were assessed for leucopenia after PT treatment, but no statistically significant associations were observed (Table 5).
Discussion
The synergistic effect of the initial cause of hyperbilirubinemia, the toxic effect of bilirubin, and PT can aggravate hematological toxicity and result in morbidity and mortality in newborns with hyperbilirubinemia27. This study aimed to assess hematological toxicity and associated factors among newborns with hyperbilirubinemia before and after the initiation of PT. This study revealed various hematological toxicities.
Before PT, the incidence of anemia among newborns with hyperbilirubinemia was 46.6% (95% CI 40.1, 52.6). This figure shows anemia as a severe public health problem among newborns with hyperbilirubinemia in the study area according to the WHO public health significance classification of anemia34. A possible explanation for the high magnitude of anemia could be an increase in RBC distraction as a result of the initial cause of hyperbilirubinemia, such as blood group incompatibilities, G6PDH deficiency, liver disease, sepsis, and maternal factors10,11. Besides, hemolysis of RBCs by the toxic effect of bilirubin may increase the magnitude of anemia35,36,37. Furthermore, frequent blood sampling to assess different blood parameters in newborns may contribute to increased anemia25. The magnitude of anemia is greater than that reported in studies conducted in different area in Ethiopia38,39,40, Cameroon41, Afghanistan42, and the United States36. This discrepancy could be explained by variations in sample size, study populations, and operational definitions.
On the other hand, after PT treatment, the magnitude of anemia significantly increased. This agrees with studies conducted in Turkey43,44 and Egypt28,45,46,47. The possible reasons could be that PT may induce hemolysis in RBCs, increase oxidative stress in RBCs48,49 and increase the osmotic fragility of RBCs50. Additionally, PT can directly damage DNA in immature RBCs and induce RBC eryptosis in the early stage. This may increase anemia after PT26.
A study revealed that the risk of developing anemia is 2.5 times greater in newborns ≥ 7 days of age than in newborns < 7 days of age. This finding was consistent with previous studies performed in Ethiopia11, Cameroon41, and Japan51. This could be due to physiological changes in the Hgb concentration as the age of the newborn changes52. In addition, newborns with a TSB ≥ 18 mg/dl were 3.5 times more likely to develop anemia than those with a TSB < 18 mg/dl. This was concurrent with studies performed in Egypt28 and Germany53. The possible reason could be the toxic effect of bilirubin, since bilirubin is known to be an inducer of RBC apoptosis, and increasing anemia as the bilirubin level increases is expected53. The occurrence of anemia was 2.7 times greater among newborns who were born with Rh blood group incompatibility. These findings are supported by previous similar studies11,27,54. Since Rh alloimmunization is a well-known cause of severe anemia, this finding is expected55. Furthermore, newborns who underwent intensive PT and who were treated with PT for more than 48 h were approximately two times more likely to develop anemia. The possible reason could be that PT may induce and exacerbate RBC hemolysis48,49.
Thrombocytopenia was identified in 7.3% (95% CI 4.5, 10.5) of the newborns before PT treatment. The occurrence of thrombocytopenia before PT may be related to the aggregation, swelling, and apoptosis of PLTs due to elevated bilirubin56. The finding of the current study is lower than that of studies conducted in Ethiopia57, Iran58,59, India17, and Egypt28. The reason for this disparity may be related to variability in the cutoff point used to define thrombocytopenia since the current study used the hematological reference range of newborns by considering gestational and postnatal ages, which is much different than that used in the above studies. Regarding associated factors, the odds of thrombocytopenia were two times greater among newborns with low birth weight (LBW) than among those with high birth weight. This finding is supported by a study conducted in Egypt60. The possible mechanism could be that LBW newborns often have less mature bone marrow, which might be less efficient for the production of PLTs61.
After PT, thrombocytopenia significantly increased. This finding is similar to those of other studies28,62,63,64. The potential mechanism for the increase in thrombocytopenia following PT could be the effect of white light on PLTs. Photosensitization of PLTs induces the formation of hematoporphyrin, functional impairment, aggregation and the release of essential substances, subsequently shortening the lifespan of PLTs60,65,66. Taking intensive PT and treating with PT for longer than 48 h increased the risk of developing thrombocytopenia 3.4 times and 2.1 times, respectively. These findings are supported by similar studies64,66,67. A potential explanation for this finding is that exposing newborns to double PT for a longer period can compromise the production of PLTs and accelerate deterioration compared with exposing newborns to a single PT68. Additionally, double PT affects DNA, RNA and protein synthesis and shortens the life span of immature PLTs26.
Before PT, leucopenia occurred in 21.1% of newborns (95% CI 16.2 26.3), but after PT, the magnitude of leucopenia significantly decreased to 21/8.5% (95% CI 5.3, 12.1). These findings are supported by studies conducted in Serbia69, Iran21,70, and Egypt47,62. The occurrence of leucopenia before PT may be related to the immunosuppressive effect of hyperbilirubinemia21,62. However, the increase in the WBC count after PT may be attributed to stress from hospitalization and exposure to a new environment18. Besides, decrement WBC count after PT may be related to the generation of ROS, which can in turn activate the immune system and lead to an increase in the production of WBCs71,72,73. Furthermore, alterations in cytokine production following exposure to PT may increase the WBC count74. A lower likelihood of leucopenia was observed among newborns admitted with a TSB greater than 18 mg/dl in the present study. These findings are supported by several studies75,76. The possible reason could ultimately be the stimulation of WBC production by bilirubin76 and the neutralization of ROS by free bilirubin in the serum19.
As a strength, this was a primary study that assessed the magnitude and associated factors of hematological toxicity among newborns with hyperbilirubinemia before and after PT treatment. However, a limitation of this study was the use of data from medical charts for maternal blood groups, which could minimize the accuracy of the data. Besides, we did not perform reticulocyte count due to constraint of reagent during study period, even if it is essential in the anemia diagnostic algorithm for neonates.
Conclusion and recommendation
In the study area, hematological toxicity was found to be a severe public health concern. Various hematological toxicities were observed before and after PT among newborns with hyperbilirubinemia. Among the identified toxicities, anemia, thrombocytopenia and leucopenia were the most prevalent. All of the prevalent toxicities, except leucopenia, were significantly elevated following PT. Additionally, age less than seven days, a TSB level less than 18 mg/dl, Rh blood group incompatibility, and taking intensive PT for a long period were found to be the major causes of most toxicity. Therefore, strict follow-up and early detection of hematological toxicity before and after PT treatment are necessary for better patient management and improved quality of life in newborns. Additionally, physicians should consider hematological complications and their aggravating factors during PT treatment. Furthermore, it is better further study conducted with large sample size which included reticulocyte count.
Data availability
All the data supporting these findings are contained within the manuscript.
Abbreviations
- AOR:
-
Adjusted odds ratio
- Hb:
-
Hemoglobin
- CI:
-
Confidence interval
- COR:
-
Crude odds ratio
- G6PDH:
-
Glucose-6-phosphate dehydrogenase
- LBW:
-
Low birth weight
- MCV:
-
Mean cell volume
- PLT:
-
Platelet
- PT:
-
Phototherapy
- TSB:
-
Total serum bilirubin
- RBCs:
-
Red blood cells
- ROS:
-
Reactive oxygen species
- WBC:
-
White blood cells
- WHO:
-
World Health Organization
References
Schwarzenbach, H.-R.J.P. Jaundice and pathological liver values. Praxis. 102(12), 727–729 (2013).
Leung, T. S., Outlaw, F., MacDonald, L. W. & Meek, J. J. B. Jaundice Eye Color Index (JECI): Quantifying the yellowness of the sclera in jaundiced neonates with digital photography. Biomed. Opt. Express. 10(3), 1250–1256 (2019).
Zhou, S., Wu, X., Ma, A., Zhang, M. & Liu, Y. J. E. Analysis of therapeutic effect of intermittent and continuous phototherapy on neonatal hemolytic jaundice. Exp. Ther. Med. 17(5), 4007–4012 (2019).
Maisels, M. J. J. C. P. Jaundice in a newborn: Answers to questions about a common clinical problem. Contemp. Pediatr. 22(5), 34–41 (2005).
Porter, M. L. & Dennis, M. B. L. J. A. F. P. Hyperbilirubinemia in the term newborn. Am. Fam. Phys. 65(4), 599 (2002).
Bhutani, V. K. et al. Neonatal hyperbilirubinemia and Rhesus disease of the newborn: incidence and impairment estimates for 2010 at regional and global levels. Pediatr. Res. 74(1), 86–100 (2013).
Mitra, S. & Rennie, J. J. B. Neonatal jaundice: Aetiology, diagnosis and treatment. J. Hosp. Med. 78(12), 699–704 (2017).
Mir, S. E., Van Der Geest, B. A. & Been, J. V. Management of neonatal jaundice in low-and lower-middle-income countries. BMJ Paediatr. Open. 3(1), e000408 (2019).
Ayalew, T. et al. Factors associated with neonatal jaundice among neonates admitted at referral hospitals in northeast Ethiopia: A facility-based unmatched case-control study. BMC Pregnancy Childbirth 24(1), 150 (2024).
Belize, M. O. H. Neonatal Clinical Practice Guidelines 2018–2021, 1st edn (2018).
Abiti, H., Dedefo, A. & Lemma, L. Prevalence and associated factors of hyperbilirubinemia among neonates admitted to neonatal intensive care unit of Saint Peter Specialized Hospital, Addis Ababa, Ethiopia. Science. 11(3), 56–63 (2023).
Lin, Q. et al. Risk factors for neonatal hyperbilirubinemia: A systematic review and meta-analysis. Transl. Pediatr. 11(6), 1001 (2022).
Ballot, D. E., Rugamba, G. J. Exchange transfusion for neonatal hyperbilirubinemia in Johannesburg, South Africa, from 2006 to 2011. Int. Sch. Res. Not. 2016 (2016)
Ullah, S., Rahman, K. & Hedayati, M. Hyperbilirubinemia in neonates: Types, causes, clinical examinations, preventive measures and treatments: A narrative review article. Iran. J. Public Health 45(5), 558–568 (2016).
Slominski, A. T., Zmijewski, M. A., Plonka, P. M., Szaflarski, J. P. & Paus, R. J. E. How UV light touches the brain and endocrine system through skin, and why. Endocrinology. 159(5), 1992–2007 (2018).
Jiao, Y., Jin, Y., Meng, H. & Wen, M. An analysis on treatment effect of blue light phototherapy combined with Bifico in treating neonatal hemolytic jaundice. Exp. Ther. Med. 16(2), 1360–1364 (2018).
Khera, S. & Gupta, R. Incidence of thrombocytopenia following phototherapy in hyperbilirubinemic neonates. Med. J. Armed Forces India. 67(4), 329–332 (2011).
Tham, E. H. et al. Phototherapy for neonatal hyperbilirubinemia and childhood eczema, rhinitis and wheeze. Pediatr. Neonatol. 60(1), 28–34 (2019).
Lee, Y. et al. Bilirubin nanoparticles as a nanomedicine for anti-inflammation therapy. Angewandte Chemie (Int. Ed Engl.). 55(26), 7460–7463 (2016).
El-Abdin, M. Y. Z., El-Salam, M. A., Ibrhim, M. Y., Koraa, S. S. & Mahmoud, E. Phototherapy and DNA changes in full term neonates with hyperbilirubinemia. Egypt. J. Med. Hum. Genet. 13(1), 29–35 (2012).
Jahanshahifard, S., Ahmadpour-Kacho, M. & Pasha, Y. Z. Effects of phototherapy on cytokines’ levels and white blood cells in term neonate with hyperbilirubinemia. J. Clin. Neonatol. 1(3), 139 (2012).
Eyada, I., El Saie, A., Ibrahem, G. & Riad, N. Effect of phototherapy on B and T lymphocytes in Egyptian infants suffering from neonatal jaundice. Allergologia et immunopathologia. 45(3), 290–296 (2017).
Wang, J., Guo, G., Li, A., Cai, W.-Q. & Wang, X. Challenges of phototherapy for neonatal hyperbilirubinemia. Exp. Ther. Med. 21(3), 1 (2021).
Vreman, H. J., Wong, R. J., Stevenson, D. K. (eds.) Phototherapy: Current methods and future directions. In Seminars in Perinatology (Elsevier, 2004).
Lokeshwar, M., Singhal, T. & Shah, N. Anemia in the newborn. Indian J. Pediatr. 70, 893–902 (2003).
Faulhaber, F. R., Procianoy, R. S. & Silveira, R. C. Side effects of phototherapy on neonates. Am. J. Perinatol. 36(03), 252–257 (2019).
Mishra, J. P., Mishra, J., Padhi, R. K., Mishra, S. & Manjareeka, M. Hematological profile in neonatal jaundice. J. Basic Clin. Physiol. Pharmacol. 25(2), 225–228 (2014).
Mourad, R. M., Waked, N. M., El Desouky, M. A., El-Khashab, K. M. A. & El-Gayed, A. S. Peripheral Blood count changes in neonates with indirect hyperbilirubinemia after phototherapy. Egypt. J. Hosp. Med. 90(1), 1141–1148 (2023).
Enyew, E. F., Bitew, D. A. & Gelagay, A. A. Incidence, time to recovery and predictors among neonates admitted with respiratory distress to the neonatal intensive care unit at the University of Gondar Comprehensive Specialized Hospital, Northwest Ethiopia, 2021. PLoS One. 17(12), e0278887 (2022).
WHO. Exclusive breastfeeding for optimal growth, development and health of infants 2023. updated 9 August 2023. https://www.who.int/tools/elena/interventions/exclusive-breastfeeding.
Tahir, M. J. et al. Associations of breastfeeding or formula feeding with infant anthropometry and body composition at 6 months. Matern. Child Nutr. 17(2), e13105 (2021).
(ABA) ABA. Mixed feeding: ABA; 2017. https://www.breastfeeding.asn.au/bfinfo/mixed-feeding.
Kemper, A. R., Newman, T. B., Slaughter, J. L., Maisels, M. J., Watchko, J. F., Downs, S. M., et al. Clinical practice guideline revision: Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 150(3) (2022).
Organization, W. H. Haemoglobin Concentrations for the Diagnosis of Anaemia and Assessment of Severity (World Health Organization, 2011).
Kassa, R., Gudeta, H., Assen, Z., Demlew, T. & Teshome, G. Neonatal hyperbilirubinemia: Magnitude and associated etiologic factors among neonates admitted at Tikur Anbessa specialized Hospital, Ethiopia. J. Pregnancy Child Health. 5(04), 1–8 (2018).
Lee, S. et al. Prevalence of anemia and associations between neonatal iron status, hepcidin, and maternal iron status among neonates born to pregnant adolescents. Pediatr. Res. 79(1), 42–48 (2016).
Brites, D., Silva, R. & Brito, A. Effect of bilirubin on erythrocyte shape and haemolysis, under hypotonic, aggregating or non-aggregating conditions, and correlation with cell age. Scand. J. Clin. Lab. Investig. 57(4), 337–349 (1997).
Tilahun, D., Yimer, M. A. & Zamanuel, T. G. High magnitude of neonatal anemia among sick newborns admitted to University of Gondar Comprehensive Specialized Hospital, Northwest Ethiopia. J. Blood Med. 13, 293–302 (2022).
Tigabu Kebede, Z. et al. Hematologic profiles of ethiopian preterm infants with clinical diagnoses of early-onset sepsis, perinatal asphyxia, and respiratory distress syndrome. Glob. Pediatr. Health. 7, 2333794x20960264 (2020).
Alamneh, T. T. et al. Prevalence and associated factors of anemia among newborns at Tibebe Ghion Specialized Hospital, Northwest Ethiopia. Int. J. Gen. Med. 15, 6465–6474 (2022).
Mah, E. M. et al. Determinants of anemia in premature newborns and the immediate outcome at the Mother and Child Center of the Chantal BIYA Foundation, Cameroon. J. Med. Res. 7(5), 146–149 (2021).
Aslamzai, M., Danish, Y., Hakimi, T. & Jawadi, B. Evaluation of the factors associated with anemia in neonates admitted to the neonatal unit of Maiwand Teaching Hospital: A cross-sectional study. Glob. Pediatr. 8, 100164 (2024).
Can, C. & Hamilcıkan, Ş. Effect of neonatal phototherapy on eosinophil levels in nonsevere hyperbilirubinemia. Am. J. Perinatol. 37(9), 929–932 (2020).
Yilmaz, F. H., Buket, K. & Ertan, K. Effects of phototherapy on hematological parameters in newborns with indirect hyperbilirubinemia. Abant. Tıp. Dergisi. 11(3), 283–294 (2022).
El-Sheikh, M. R., Ahmed, A. Y., ElMashad, A. E. R. M., Talaye, I. I. & El-Hawary, E. E. S. Eosinophil count and tumor necrosis factor α in response to phototherapy treatment of neonatal hyperbilirubinemia: A cross sectional study. Ital. J. Pediatr. 48(1), 103 (2022).
Saber, M. A., Abd El Naby, S. A., Helwa, M. A. & Deghedy, R. N. The influence of phototherapy for neonatal hyperbilirubinemia on tumour necrosis factor-α. Menoufia Med. J. 27(1), 44 (2014).
El-Askary, A., Mohamed, S. A., Khalifa, M. M. & El-Tawab, A. A. Effect of neonatal phototherapy on serum levels of interleukin 1, 6, 8, TNFa and white blood cell count. Med. J. Cairo Univ. 86, 3767–3772 (2018).
Ayyappan, S. et al. Antioxidant status in neonatal jaundice before and after phototherapy. J. Pharm. Bioallied Sci. 7(Suppl 1), S16 (2015).
Suzen, S., Gurer-Orhan, H. & Saso, L. Detection of reactive oxygen and nitrogen species by electron paramagnetic resonance (EPR) technique. Molecules. 22(1), 181 (2017).
Roll, E. B., Christensen, T. & Gederaas, O. A. Effects of bilirubin and phototherapy on osmotic fragility and haematoporphyrin-induced photohaemolysis of normal erythrocytes and spherocytes. Acta Paediatr. 94(10), 1443 (2005).
Hirata, M., Kusakawa, I., Ohde, S., Yamanaka, M. & Yoda, H. Risk factors of infant anemia in the perinatal period. Pediatr. Int. 59(4), 447–451 (2017).
Esan, A. Hematological differences in newborn and aging: A review study. Hematol. Transfus. Int. J. 3(3), 178–190 (2016).
Lang, E. et al. Conjugated bilirubin triggers anemia by inducing erythrocyte death. Hepatology (Baltimore, Md). 61(1), 275–284 (2015).
Amar Shah, D. C. S., Shah, D. V., Shah, A. Study of hæmatological parameters among neonates admitted with neonatal jaundice. J. Evol. Med. Dent. Sci. 1(3) (2012).
Sahoo, T., Sahoo, M., Gulla, K. M. & Gupta, M. Rh alloimmunisation: Current updates in antenatal and postnatal Management. Indian J. Pediatr. 87, 1018–1028 (2020).
NaveenKumar, S. K. et al. Unconjugated bilirubin exerts pro-apoptotic effect on platelets via p38-MAPK activation. Sci. Rep. 5(1), 15045 (2015).
Abebe Gebreselassie, H. et al. Incidence and risk factors of thrombocytopenia in neonates admitted with surgical disorders to neonatal intensive care unit of Tikur Anbessa specialized hospital: A one-year observational prospective cohort study from a low-income country. J. Blood Med. 12, 691–697 (2021).
Boskabadi, H., Mafinezhad, S., Bagher, F. & Bozorgnia, Y. Incidence of thrombocytopenia in idiopathic hyperbilirubinemic newborns. Open Access Maced. J. Med. Sci. 2(2), 261–264 (2014).
Sanii, S., Khalessi, N., Khosravi, N. & Zareh, M. F. The prevalence and risk factors for neonatal thrombocytopenia among newborns admitted to intensive care unit of Aliasghar children’s hospital. Iran. J. Blood Cancer. 5(2), 41–45 (2013).
Sonawane, P., Bhaisara, B. & Bhatawdekar, A. Effect of conventional phototherapy on platelet count in full term and preterm neonates with indirect hyperbilirubinemia-A prospective cohort study. J. Med. Sci. Clin. Res. 6(3), 959–966 (2018).
Maurer, H. M. et al. Effects of phototherapy on platelet counts in low-birthweight infants and on platelet production and life span in rabbits. Pediatrics. 57(4), 506–512 (1976).
Abdelhakeem, A., Saad, M., Eldahshan, T. Effect of phototherapy on peripheral blood cell count in full term newborns with neonatal hyperbilirubinemia. Al-azhar assiut Med. J. AAMJ. (2018).
Naqvi, H., Memon, S., Ali Shah, M., Nadeem Chohan, M., Shaikh, N., Shah, F. Frequency of thrombocytopenia in neonates following phototherapy in neonatology unit of tertiary care hospital. (2021).
Sajid, A., Mahmood, T., Riaz, S., Nabi, S. G. Phototherapy in hyperbilirubinemic neonates; Does it affect platelet count? Ann. King Edward Med. Univ. 22(3) (2016).
Sajid, A., Mahmood, T., Riaz, S., Nabi, S. Phototherapy in hyperbilirubinemic neonates; Does it affect platelet count? Ann. King Edward Med. Univ. 22 (2016).
Vafaie, M., Mirzarahimi, M., Sadeghieh-Ahari, S., Enteshari-Moghaddam, A. & Merrikhi, H. Incidence of thrombocytopenia following phototherapy in hyperbilirubinemic neonates in Ardabil City. Int. J. Contemp. Pediatr. 5(6), 2274–2277 (2018).
Sarkar, S. K. et al. A study on effect of phototherapy on platelet count in neonates with unconjugated hyperbilirubinemia: A hospital based prospective observational study. Asian J. Med. Sci. 12(5), 41–46 (2021).
Yılmaz, F. H., Kara, B. & Ertan, K. Effects of phototherapy on hematological parameters in newborns with indirect hyperbilirubinemia. Abant Med. J. 11(3), 283–294 (2022).
Mrkaić, L. et al. Neonatal immune system changes caused by phototherapy. Srpski arhiv za celokupno lekarstvo. 122(Suppl 1), 36–37 (1994).
Zarkesh, M., Dalili, S., Fallah, M. J., Heidarzadeh, A. & Rad, A. H. The effect of neonatal phototherapy on serum level of interlukin-6 and white blood cells′ count. J. Clin. Neonatol. 5(3), 189–192 (2016).
Wang, D., Malo, D. & Hekimi, S. Elevated mitochondrial reactive oxygen species generation affects the immune response via hypoxia-inducible factor-1α in long-lived Mclk1+/− mouse mutants. J. Immunol. 184(2), 582–590 (2010).
Iskander, I., Abdelmonem, S., El Houchi, S., Mandour, I. & Aly, H. Intensive phototherapy and oxidant-antioxidant status in infants with jaundice. Early Hum. Dev. 161, 105465 (2021).
Pham-Huy, L. A., He, H. & Pham-Huy, C. Free radicals, antioxidants in disease and health. Int. J. Biomed. Sci. IJBS. 4(2), 89–96 (2008).
Kurt, A. et al. Use of phototherapy for neonatal hyperbilirubinemia affects cytokine production and lymphocyte subsets. Neonatology. 95(3), 262–266 (2009).
Tsai, W. N. et al. Serum total bilirubin concentrations are inversely associated with total white blood cell counts in an adult population. Ann. Clin. Biochem. 52(Pt 2), 251–258 (2015).
Zhang, L. et al. Serum bilirubin is negatively associated with white blood cell count. Clinics (Sao Paulo, Brazil). 74, e775 (2019).
Acknowledgements
We thank the University of Gondar for financial support.
Funding
The authors declare that the University of Gondar provided financial support for this work. Funder had no other role in this study.
Author information
Authors and Affiliations
Contributions
D.M.B. and B.B.T. and B.W. and E.C. and Z.M. and A.K. contributed to the design and implementation of the study, collected the data, undertook the statistical analysis, performed the data interpretation, and drafted the manuscript. N.C. and M.T. and A.A.A. and A.Y. and E.A. contributed to the data interpretation and drafting. All authors reviewed the main manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Berta, D.M., Woldu, B., Yalew, A. et al. Hematological abnormality and associated factors in newborns with hyperbilirubinemia before and after phototherapy at University of Gondar Comprehensive Specialized Hospital. Sci Rep 14, 18210 (2024). https://doi.org/10.1038/s41598-024-68871-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-68871-0