Abstract
The incidence of multiple pronuclei (≥ 3PN) zygotes and blastomere multinucleation was found to be elevated in the presence of increased estradiol (E2) levels and a greater number of retrieved oocytes. This implies a potential link between the incidence of multinucleation at the two-cell stage (MN2) and a higher proportion of ≥ 3PN zygotes. We aimed to investigate the effect of high proportion of ≥ 3PN zygotes on MN2 incidence during conventional in vitro fertilization (C-IVF) by using time-lapse monitoring. This study included 1195 patients from January 2020 to December 2022. The patients were categorized into three groups: Group 1 comprised patients with no ≥ 3PN zygotes (n = 422), Group 2 included those with 0–25% ≥3PN zygotes (n = 617), and Group 3 consisted of patients with more than 25% ≥3PN zygotes (n = 156). The MN2 rate, types of MN2 and clinical outcomes were compared among the three groups. Our data indicated that the MN2 rate was significantly lower in groups 1 and 2 compared to group 3 (18.33 versus 25.62%; p < 0.001 and 19.45 versus 25.62%; p < 0.001). The MN2 embryos exhibited similar rates of high-quality embryos (42.27 versus 43.50 versus 40.67%; p = 0.401) and available embryos (84.96 versus 84.04 versus 83.21%; p = 0.460) rates among the three groups. There were no significant differences in the proportion of MN2 with different types among the three groups (p > 0.05). The embryos displaying binucleated at the two-cell stage in one blastomere (2BI1) and true multinucleated at the two-cell stage in one blastomere (2MULTI1) showed significantly higher blastocyst formation rates compared to embryos exhibiting true multinucleated at the two-cell stage in both blastomeres (2MULTI2) (59.50 versus 45.40%; p < 0.001 and 59.40 versus 45.40%; p < 0.001). In conclusion, the occurrence of MN2 events might be associated with high proportion of ≥ 3PN zygotes incidence. The types of MN2 had significant reference value when selecting embryos for transfer during the cleavage stage.
Similar content being viewed by others
Introduction
The phenomenon of blastomere multinucleation at the two-cell stage (MN2) is a common nuclear abnormality observed in early human embryos1. The reported incidence of MN2 demonstrates a significant variation, ranging between 15% and 40%2,3. A blastomere exhibiting multiple nuclei has been observed to undergo independent dissolution of nuclear membranes, resulting in asynchronous nuclear events pivotal for cell division. Studies have reported that the incidence of MN2 exerts a considerable detrimental influence on embryo development, blastocyst formation, and successful implantation4.
The incidence of multiple pronuclei (≥ 3PN) is identified as one of the most prevalent chromosomal abnormalities impacting human gestation5. Prior research suggests a higher proportion of ≥ 3PN zygotes negatively influences embryo development and clinical outcomes in both conventional in vitro fertilization (C-IVF) and intracytoplasmic sperm injection (ICSI) cycles6,7.
Chen et al. demonstrated that the propensity toward ≥ 3PN was related to ovarian stimulation, as indicated by elevated peak estradiol (E2) levels and substantial oocyte yields8. Furthermore, several studies have indicated that cycles with multinucleation exhibited increased E2 levels and a higher count of retrieved oocytes9,10. In our previous study, we selected two patients who had a single normal zygote and more than four ≥ 3PN zygotes in the initial C-IVF cycle. We then observed the incidence of MN2 in the single normal embryo utilizing time-lapse monitoring (TLM)11. These findings implied a potential association between the incidence of MN2 and a higher proportion of ≥ 3PN zygotes. Consequently, our study aimed to investigate the impact of a high proportion of ≥ 3PN zygotes on the incidence of MN2.
Materials and methods
This study encompassed 1195 C-IVF patients who underwent TLM from January 2020 to December 2022. Only elective single blastocyst embryo transfers (eSBETs) were included in this study. The TLM patients were categorized into three groups: Group 1 comprised patients with no ≥ 3PN zygotes (n = 422), Group 2 included those with 0–25% ≥3PN zygotes (n = 617), and Group 3 consisted of patients with more than 25% ≥3PN zygotes (n = 156). All female patients were not beyond 38 years old to eliminate possible age-related cycle characteristics. Additionally, all cycles were the first attempt at down-regulated ovarian stimulation. Patients with severe endometriosis, those using a gestational carrier, those undergoing in-vitro maturation, those with the presence of uninterrupted hydrosalpinx or intrauterine adhesions, those with polycystic ovary syndrome, and those with fertilization failure were excluded from this study.
The ovarian stimulation protocol employed in this study has been previously delineated12. Briefly, stimulation protocols were executed utilizing a combination of Gonadotropin-Releasing Hormone (GnRH) agonist/GnRH antagonist and recombinant Follicle-Stimulating Hormone (FSH). The ovarian response was continually monitored via serial ultrasound examinations and hormone measurements. Upon the detection of three follicles exceeding 18 mm, patients were administered 10,000 units of Human Chorionic Gonadotropin (hCG). Oocyte retrieval was subsequently executed 36 h later through transvaginal ultrasonography-guided aspiration.
Post-retrieval, the oocyte-cumulus complexes were cultured in the medium (IVF; Vitrolife). C-IVF was performed 39 to 40 h after hCG administration while incubated in fertilization medium (IVF; Vitrolife). Five hours post-IVF fertilization, zygotes were transferred to a cleavage medium (G-1; Vitrolife). Embryos designated for blastocyst culture were moved to a blastocyst medium (G-2; Vitrolife) on day 3 and remained until day 6. All media were overlaid with paraffin oil and incubated in a humidified atmosphere at 37 °C for a preceding duration of 24 h.
After 64 to 68 h of culture, the cleavage-stage embryos were scored according to homogeneous degree of blastomeres, the number of blastomeres and embryo fragmentation. The high-quality cleavage-stage embryos were graded I and II. The available cleavage-stage embryos were graded I, II, and III. The blastocyst-stage embryos were scored according to the stage of development from 1 to 6, the grade of the inner cell mass and the trophectoderm13. The high-quality blastocyst was graded ≥ 3BB.
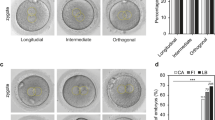
For culture with the EmbryoScope (Vitrolife, Sweden), dedicated 16-well plates were prepared with 25 µl microdrops of culture medium (Vitrolife, Sweden) overlaid by 1.4 ml of mineral oil (Vitrolife) at 37 °C, in 6% CO2, 5% O2, and 89% N2. Retrospective analysis of each embryo’s images was conducted using the EmbryoViewer external image analysis software (Unisense FertiliTech, Sweden). Images were acquired every 20 min in seven different focal planes during culture. The specific parameters were recorded according to relevant references14. The embryos exhibiting abnormal cleavage (division of one cell into three cells) or direct cleavage (duration of the 2-cell stage ≦ 5 h) were omitted due to their recognized detrimental effect on implantation15. The nucleus status of the blastomeres was evaluated as non-multinuclear at the two-cell stage (2MONO) when each blastomere contained at most one nucleus. Blastomeres with two nuclei were defined as 2BI. Blastomeres with more than two nuclei and were defined as 2MULTI.
The embryo transfer catheter (Cook Ireland Ltd., Limerick, Ireland) was used for transfer. Prior to the transfer, any vaginal and cervical secretions were gently removed from the vagina/cervix with small pledgets of cotton wool, moistened with warm normal saline. Any mucus present in the cervical canal was also removed. Following the transfer, the catheter was examined for any retained embryos or presence of blood. Post-transfer, all patients received luteal support via Duphaston (progesterone injection). Clinical pregnancy was confirmed by the detection of an intrauterine gestational sac and fetal heartbeat via transvaginal ultrasound four weeks post-embryo transfer.
The comparison of continuous variable outcomes between groups was conducted using the Student’s t-test for normally distributed data and the non-parametric Mann-Whitney U-test for skewed data. Categorical variable outcomes, expressed as numbers and percentages, were compared between groups using the chi-square test or Fisher’s exact test. The statistical analyses were performed utilizing SPSS version 21 (IBM Corp., USA). A p-value of less than 0.05 was considered to indicate statistical significance. When p < 0.05 among the three groups, a pairwise comparison was performed between the two groups. For this study among the three groups, the adjusted α level was 0.016667. If the p value of the pairwise comparison was less than 0.016667, the difference between the two groups was statistically significant.
Results
The study flow chart was presented in Fig. 1. The demographic and baseline characteristics of the study population were detailed in Table 1. No significant differences were noted in the female age, body mass index (BMI), duration of infertility, basal FSH level, basal E2 level, total gonadotropin (Gn) dose, Gn stimulation duration, number of retrieved oocytes, and endometrial thickness (p > 0.05).
Study Flow Chart. eSBET: elective single blastocyst-stage embryo transfer; MN2: multinucleation at the two-cell stage; 2MONO: non-multinucleated at the two-cells stage; 2BI1: binucleated at the two-cell stage in one blastomere; 2BI2: binucleated at the two-cell stage in both blastomere; 2MULTI1: true multinucleated at the two-cell stage in one blastomere; 2BI1/2MULTI1: binucleated in one blastomere and true multinucleated in the other blastomere at the two-cell stage; 2MULTI2: true multinucleated at the two-cell stage in both blastomeres; Group 1: the patients with no ≥ 3PN zygotes; Group 2: the patients with 0–25% ≥3PN zygotes; Group 3: the patients with more than 25% ≥3PN zygotes. The comparison of clinical outcomes included clinical pregnancy, ectopic pregnancy, ongoing pregnancy, and live birth rates.
We observed no significant differences in the clinical pregnancy (70.14 versus 72.12 versus 66.67%; p = 0.180), ectopic pregnancy (0.68 versus 0.45 versus 0.96%; p = 0.524) and ongoing pregnancy (64.93 versus 66.77 versus 61.54%; p = 0.218) rates among the three groups. Our data revealed a significant difference in birth rates among the three groups (62.32 versus 65.32 versus 56.41%; p = 0.047), though no significant differences emerged upon further pairwise comparisons (62.32 versus 65.32%; p = 0.323 and 62.32 versus 56.41%; p = 0.196 and 65.32 versus 56.41%; p = 0.039) (Table 2). There were no significant differences observed in the rates of high-quality embryos (47.76 versus 49.17 versus 46.37%; p = 0.213), available embryos (85.78 versus 84.64 versus 84.03%; p = 0.382), blastocyst formation (58.35 versus 59.30 versus 57.45%; p = 0.362), direct cleavage (DC) (26.29 versus 25.09 versus 23.52%; p = 0.069) and reverse cleavage (RC) (5.90 versus 6.00 versus 6.41%; p = 0.617) rates among the three groups. The results indicated that the MN2 rate was significantly lower in groups 1 and 2 compared to group 3 (18.33 versus 25.62%; p < 0.001 and 19.45 versus 25.62%; p < 0.001) (Table 3). The MN2 embryos exhibited similar rates of high-quality embryos (42.27 versus 43.50 versus 40.67%; p = 0.401) and available embryos (84.96 versus 84.04 versus 83.21%; p = 0.460) rates among the three groups (Table 4). The blastomeres’ nucleus status at the two-cell stage was shown in Fig. 2. There were no significant differences in the proportion of MN2 with different types among the three groups (p > 0.05) (Table 4). The type of MN2 mainly displayed in three forms, namely binucleated at the two-cell stage in one blastomere (2BI1), true multinucleated at the two-cell stage in one blastomere (2MULTI1) and true multinucleated at the two-cell stage in both blastomeres (2MULTI2). There were no significant differences in the blastocyst formation rates for embryos with different type of MN2 among the three groups (p > 0.05) (Table 4).
The embryos displaying 2BI1 and 2MULTI1 showed significantly higher blastocyst formation rates compared to 2MULTI2 embryos (59.50 versus 45.40%; p < 0.001 and 59.40 versus 45.40%; p < 0.001) (Fig. 3). Transfer characteristics as well as the distribution of nucleus status at the two-cell stage were shown in Table 5. Elective single blastocyst embryo transfer was mostly from embryos exhibiting non-multinucleated at the two-cells stage (2MONO) (Table 5). There were no significant differences in the clinical pregnancy rates for all transfers with different type of MN2 among the three groups (p > 0.05) (Table 6). The blastocysts displaying 2MULTI2 were correlated with a significantly reduced implantation potential compared to 2MONO and 2BI1 embryos after blastocyst transfer (54.70 versus 74.10%; p = 0.002 and 54.70 versus 74.10%; p = 0.002) (Fig. 4).
Discussion
In this research, we focused on patients who used TLM and concluded that the occurrence of MN2 events might be associated with high proportion of ≥ 3PN zygotes incidence. And the types of MN2 had significant reference value when selecting embryos for transfer during the cleavage stage. In our center, we primarily conducted TLM on the embryos of the following groups of individuals. One group consisted of patients with a higher number of oocytes retrieved, while the other group included patients with a history of unsuccessful cycles. The iDAScore could be used in a time-lapse system (EmbryoScope+) equipped with the adequate software (Vitrolife Technology Hub) which was confirmed to be associated with decreased miscarriage rates and increased live birth rates16. Therefore, we selected patients with a high number of eggs because they typically undergo blastocyst culture for all day 3 embryos. The reason for selecting multi-cycle patients to use TLS was to identify the underlying causes of infertility in the context of embryonic development. It could capture the temporal parameters of various cleavage events and could also observe the information on normal cleavage and abnormal cleavage patterns, which might be closely associated with the embryo development and clinical outcomes17. In addition, the preimplantation genetic testing (PGT) cycles were always performed using TLM. The accuracy of the results was not affected by the study design and enrolled population.
It was well known that the etiology of ≥ 3PN incidence was complicated which were primarily attributed to oocyte-derived meiotic failure and polyspermic fertilization. Sachs et al. clearly illustrated that the occurrence of ≥ 3PN was associated with a heightened response to gonadotropin stimulation, characterized by elevated peak E2 level on the day of hCG administration and a high number of retrieved oocytes8. Physiologically, patients with a robust response to the drug frequently yielded a higher proportion of immature or overripe oocytes. Immature oocytes were unable to undergo proper cortical and zona reactions, leading to an elevated rate of polyspermy. After aging of overripe egg, only part or no cortical granules might be released. It resulted in incomplete or unsuccessful cortical reaction, thereby increasing the likelihood of polyspermy occurrence.
Multinucleation was a nuclear abnormality resulting from an error in the cytokinesis process18. Jackson et al. found multinucleation present in cycles that exhibited a heightened response to treatment, characterized by elevated E2 levels and a high number of retrieved oocytes9. Figueira et al. demonstrated that most of the patients experiencing MN2 incidence exhibited a greater quantity of follicles and retrieved oocytes10. These observations suggested that multinucleated embryos might result from ovulation induction regimens in which the ovaries were more sensitive to gonadotrophin therapy, leading to increased oocyte production. Some oocytes generated in these exuberant cycles seemed to be abnormal, potentially resulting in chromosomal abnormalities, cytokinesis errors, and multinucleation9,19.
To sum up, elevated peak serum E2 level and a higher number of retrieved oocytes might be associated with the incidence of ≥ 3PN zygotes and MN2 embryos. The way a single embryo was affected might indicate how the entire cohort was affected, even if the remaining embryos did not exhibit similar characteristics. It also suggested that a high proportion of ≥ 3PN zygotes could increase the likelihood of MN2 embryos occurrence originating from surplus 2PN zygotes. Subsequently, our findings revealed a positive correlation between the MN2 rate and the incidence of ≥ 3PN embryos.
Figueira et al. showed that a high proportion of ≥ 3PN zygotes might reflect a globally dysfunctional oocyte cohort and make negative influence on the embryo potential development20. A retrospective analysis of cleavage-stage embryos also indicated that the appearance of MN2 was associated with impaired cleavage and increased fragmentation8. Nevertheless, we observed comparable good-quality and available embryo rates in groups with high proportion of ≥ 3PN zygotes compared with groups with low or absent ≥ 3PN zygotes in this investigation. Conflicting conclusions might be due to the capacity for self-correction during initial cleavage divisions. Balakier et al. demonstrated a significant decrease in the blastomere multinucleation rate during the transition from the 2- to 4-cell stage4. The potential for self-correction was also proposed in earlier FISH studies, which revealed that some MN2 embryos might restore normal ploidy during preimplantation development21.
We further investigated the nucleus status at the two-cell stage for all transfers and our findings showed that elective single blastocyst embryo transfer was predominantly from those embryos with one nucleus in each blastomere. Our findings indicated that MN2 mainly displayed in three forms: binucleation in one blastomere, multinucleation in one blastomere and multinucleation in both blastomeres which was consistent with previous report22. In this study, embryos exhibiting some types of MN2 showed a comparable blastocyst formation rate to that of normal embryos. Embryos exhibiting binucleated in one blastomere and multinucleated in both blastomeres showed enhanced development leading to the formation of high-quality blastocysts in comparison to other types of MN2 embryos. Similar to our research, Talbot et al. also indicated that embryos displaying binucleated in one blastomere were correlated with enhanced development resulting in the formation of high-quality blastocysts22.
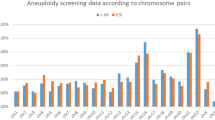
The relationship between multinucleation and aneuploidy remains unclear. Studies utilizing preimplantation genetic screening have indicated similar aneuploidy rates between embryos with multinucleation and those without multinucleation23. Hence, it has been proposed that the presence of MN2 should not be considered as a reliable indicator of aneuploidy or for embryo selection. It has been suggested that most MN2 embryos have the capacity for self-correction during early cleavage divisions and can develop into euploid blastocysts resulting in healthy babies4. It was also illustrated that blastocysts derived from MN2 embryos exhibited comparable implantation potential to those from normal embryos24. Our study also demonstrated that blastocysts displaying binucleated at the two-cell stage in one or two blastomeres exhibited comparable implantation potential to that of normal embryos. Therefore, these findings suggest that culture of MN2 embryos to the blastocyst stage for transfer might be an alternative option.
It is difficult to predict the potential for embryo development into a blastocyst and the potential for successful implantation in the cleavage-stage embryo transfers. It is worth noting that there are differences in the implantation rates of blastocysts from different types of MN2. Based on our data, if we need to transfer the MN2 embryos at the cleavage-stage, we strongly recommend the embryos exhibiting binucleated at the two-cell stage in one blastomere as these embryos demonstrate a higher likelihood of developing into blastocysts. Meanwhiles, the blastocysts displaying binucleated at the two-cell stage in one blastomere exhibited ideal implantation potential compared to that from normal embryos. Our results emphasized the importance of differentiating the subgroups of multinucleated embryos at the two-cell stage. The types of MN2 had significant reference value when selecting embryos for transfer during the cleavage stage.
Data availability
Data available on request corresponding author due to privacy and ethical restrictions.
References
Aguilar, J. et al. Study of nucleation status in the second cell cycle of human embryo and its impact on implantation rate. Fertil. Steril. 106, 291–299 (2016).
Yilmaz, A. et al. Chromosomal complement and clinical relevance of multinucleated embryos in PGD and PGS cycles. Reprod. Biomed. Online. 28, 380–387 (2014).
Sun, L. et al. Chromosomal polymorphisms are independently associated with multinucleated embryo formation. J. Assist. Reprod. Genet. 35, 149–156 (2018).
Balakier, H. et al. Impact of multinucleated blastomeres on embryo developmental competence, morphokinetics, and aneuploidy. Fertil. Steril. 106, 608–614 (2016).
Chen, S. et al. Tripronuclear zygotes in IVF Laboratory Quality Control: experimental evaluation and potential applications. Int. J. Gen. Med. 28, 949–954 (2022).
Figueira, R. C. et al. Prognostic value of triploid zygotes on intracytoplasmic sperm injection outcomes. J. Assist. Reprod. Genet. 28, 879–883 (2011).
Li, M. Z. et al. Effects of triploidy incidence on clinical outcomes for IVF-ET cycles in different ovarian stimulation protocols. Gynecol. Endocrinol. 31, 769–773 (2015).
Chen, W. N. et al. Effects of three pro-nuclei (3PN) incidence on laboratory and clinical outcomes after early rescue intracytoplasmic sperm injection (rescue-ICSI): an analysis of a 5-year period. Gynecol. Endocrinol. 37, 137–140 (2021).
Jackson, K. V. et al. Multinucleation in normally fertilized embryos is associated with an accelerated ovulation induction response and lower implantation and pregnancy rates in in vitro fertilization-embryo transfer cycles. Fertil. Steril. 70, 60–66 (1998).
Figueira, R. C. et al. Blastomere multinucleation: contributing factors and effects on embryo development and clinical outcome. Hum. Fertil. (Camb). 13, 143–150 (2010).
Li, M. Z. et al. High three pro-nuclei (3PN) zygotes proportion associated with normal embryo multinucleation at the two-cell stage: two cases report. Gynecol. Endocrinol. 36, 1042–1044 (2020).
Dong, X. H. et al. Live birth rate following a failed first in vitro fertilization cycle with no embryos for transfer. Sci. Rep. 13, 8343 (2023).
Garbhini, P. G. et al. Day-3 vs. Day-5 fresh embryo transfer. JBRA Assist. Reprod. 27, 163–168 (2023).
Zhang, X. D. et al. Comparison of embryo implantation potential between time-lapse incubators and standard incubators: a randomized controlled study. Reprod. Biomed. Online. 45, 858–866 (2022).
Rubio, I. et al. Limited implantation success of direct-cleaved human zygotes: a time-lapse study. Fertil. Steril. 98, 1458–1463 (2012).
Ueno, S. et al. Correlation between an annotation-free embryo scoring system based on deep learning and live birth/neonatal outcomes after single vitrified-warmed blastocyst transfer: a single-centre, large-cohort retrospective study. J. Assist. Reprod. Genet. 39, 2089–2099 (2022).
Ma, B. X. et al. Neonatal outcomes of embryos cultured in a time-lapse incubation system: an analysis of more than 15,000 fresh transfer cycles. Reprod. Sci. 29, 1524–1530 (2022).
Ono, Y. et al. Shape of the first mitotic spindles impacts multinucleation in human embryos. Nat. Commun. 15, 5381 (2024).
Haaf, T. et al. A high oocyte yield for intracytoplasmic sperm injection treatment is associated with an increased chromosome error rate. Fertil. Steril. 91, 733–738 (2009).
Barberet, J. et al. Can novel early non-invasive biomarkers of embryo quality be identified with time-lapse imaging to predict live birth? Hum. Reprod. 34, 1439–1449 (2019).
Hashimoto, S. et al. Multinucleation per se is not always sufficient as a marker of abnormality to decide against transferring human embryos. Fertil. Steril. 106, 133–139 (2016).
Talbot, A. L. et al. Binucleated embryos at the two-cell stage show higher blastocyst formation rates and higher pregnancy and live birth rates compared to non-multinucleated embryos. Hum. Reprod. Open hoac049 (2022).
Desai, N. et al. Analysis of embryo morphokinetics, multinucleation and cleavage anomalies using continuous time-lapse monitoring in blastocyst transfer cycles. Reprod. Biol. Endocrinol. 12, 54 (2014).
Akiyoshi, E. et al. Developmental capacity and implantation potential of the embryos with multinucleated blastomeres. J. Reprod. Dev. 61, 595–600 (2015).
Funding
This project was supported by Shaanxi Technology Committee Industrial Public Relation Project (Project Number: 2023-YBSF-034) and Young Physicians Program of Chinese Medical Association (No. 17020470716).
Author information
Authors and Affiliations
Contributions
M.L. and J.S. designed the research; M.L. and X.X. performed the research. X.X. analyzed the data; All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study. This study was approved by the Ethics Review Board of the Northwest Women’ s and Children’ s Hospital, Xi’an, China (2022007).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Li, M., Xue, X. & Shi, J. High proportion of zygotes with multiple pronuclei increase the embryo multinucleation rate during conventional IVF. Sci Rep 14, 26497 (2024). https://doi.org/10.1038/s41598-024-78342-1
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-78342-1