Abstract
This study examined factors influencing health behaviors for cardiovascular disease prevention among Korean-Chinese migrant workers with metabolic syndrome in South Korea, using an ecological model-based mixed-methods approach. An explanatory sequential design was applied. Data were collected from 204 participants in the Seoul metropolitan area, assessing intrapersonal, interpersonal, institutional, and community-level variables. Participants had a mean age of 51.4 ± 6.3 years; 55.4% were female, and their average length of stay in Korea was 10.8 ± 4.8 years. Hierarchical regression analysis showed that being female (β = 0.25, p < .001), having lower depression levels (β = -0.09, p = .037), higher internal health locus of control (β = 0.26, p < .001), and occupation type (β = -0.11, p = .006) were significant predictors at the intrapersonal level, while social support (β = 0.43, p < .001) was significant at the interpersonal level (Adj. R² = 0.747, p < .001). Content analysis of qualitative data from 12 in-depth interviews identified barriers such as lacks of MetS risk awareness and motivation for lifestyle changes, while highlighting social support and culturally appropriate health education as facilitators. Korean-Chinese workers face multiple challenges in adopting healthy behaviors due to demanding work conditions and limited resources. Interventions to improve mental health, enhance personal motivation, and provide culturally tailored, occupation-specific education and support are essential to promote cardiovascular health in this vulnerable population.
Similar content being viewed by others
Introduction
Among migrant workers engaged in economic activities in South Korea, the incidence rate of Cardiovascular disease (CVD), which is a leading cause of death worldwide, is 77.2%1,2. Migrant workers are classified as a vulnerable group within society3. As of 2024, among the 1.42 million registered foreign workers in Korea, Korean-Chinese workers make up the largest group, accounting for 17.9% (240,000 individuals)4. Most are employed in manual labor sectors such as retail, food service, and accommodation, where unstable working conditions and long hours with insufficient rest (49.6%) are common5. Additionally, low income, poor housing, and limited health awareness heighten health risks6.
Metabolic syndrome (MetS), a key modifiable risk factor for CVD, presents a major public health concern78,. In China, where CVD is the leading cause of death9, a study of 130,018 adults reported MetS prevalence at 31.1%, with high rates of abdominal obesity (40.8%), hypertension (49.4%), and dyslipidemia (41.1%)10—figures exceeding Korea’s 24.9%11. Among Korean-Chinese migrant workers in Korea, rates of obesity (59.8%), hypertension (24.0%), and dyslipidemia (21.2%) are also notable12. These disparities stem from sociocultural factors, such as traditional high-fat diets and increased processed food consumption, which raised MetS risk by 17% over 15 years13. High rates of smoking and alcohol consumption among Chinese adults—33.7% and 43.7%, respectively—are also culturally normalized10, highlighting the need for tailored interventions for Korean-Chinese individuals with MetS.
Preventing CVD at the MetS stage requires both lifestyle modification and pharmacological management, which depend on understanding factors that influence health behaviors14. Key determinants include disease knowledge, health consciousness, and internal health locus of control, whereas depression hinders behavior change15,16. Individuals with lower socioeconomic status are more likely to maintain unhealthy habits17. Korean-Chinese migrant workers often face cultural and healthcare access barriers, which hinder engagement in health-promoting behaviors despite the known benefits of physical activity18,19.
Occupational stress also negatively affects health behaviors among migrant workers in Korea, suggesting the need for targeted stress-reduction strategies20. In China, community-based health programs improved health behaviors, emphasizing the combined role of personal and environmental factors21,22. Notably, 90.8% of Korean-Chinese workers have lived in Korea for over five years5, yet research on disease prevention and health management in this population remains limited due to cultural and institutional challenges2.
This study uses an ecological model23 to examine factors influencing cardiovascular health behaviors among Korean-Chinese migrant workers with MetS in Korea. The model considers multiple levels of influence—namely intrapersonal, interpersonal, institutional, and community. The public policy level, which influences behavior indirectly, was excluded. Quantitative data identify key factors across these levels, including individual characteristics, social support, occupational stress, and access to health resources. Qualitative interviews further explore the contextual and lived experiences underlying these behaviors. The findings will contribute to developing tailored interventions for CVD prevention in migrant worker populations.
Methods
Study design
This research employed a mixed-methods explanatory sequential design24 to objectively and comprehensively understand the factors influencing cardiovascular health behaviors and explore participants’ lifestyle and health behavior experiences.
Setting and participants
The quantitative study included Korean-Chinese workers with MetS engaged in economic activities across three districts in the Seoul metropolitan area. Participants were aged 19 or older, held Chinese nationality, and met at least three of the five MetS diagnostic criteria: elevated blood pressure (≥ 130/85 mmHg or antihypertensive use), fasting glucose (≥ 110 mg/dL or diabetes treatment), triglycerides (≥ 150 mg/dL or lipid-lowering therapy), low high density lipoprotein (HDL) cholesterol (≤ 40 mg/dL for men, ≤ 50 mg/dL for women), and abdominal obesity (waist ≥ 90 cm for men, ≥ 85 cm for women). Eligible participants were full-time workers in Korea, able to communicate in Korean or Chinese, and provided informed consent. Individuals with a history of CVD or clinically diagnosed mental or cognitive disorders were excluded based on self-report during the informed consent process. However, participants with subclinical or undiagnosed depressive symptoms were not excluded. Depression was assessed using the questionnaire and treated as a continuous variable to capture a range of symptom severity.
Sample size was calculated using G*Power 3.1.9.7 for linear regression. Based on a previous study (R² = 0.31)25, a moderate effect size (f² = 0.15), power of 0.90, α = 0.05, and 18 predictors, the minimum required sample was 183. Considering a 10% dropout rate, the final sample size was set at 204. For the qualitative component, 12 participants were purposefully selected from survey respondents based on key characteristics (e.g., MetS knowledge, occupation, gender, age, residence duration, and health behaviors). Interviews were conducted over one month and continued until thematic saturation was reached, consistent with prior guidance that saturation is typically achieved within 6 to 12 interviews in homogeneous samples26.
Data collection
Data were collected from July to August 2024, following approval from the H University Institutional Review Board (Approval No.: --*). The researcher initially visited workplaces such as restaurants, long-term care hospitals, and small businesses to verify health check-up results and recruit eligible participants. Due to limited access through direct visits, snowball sampling was later employed. A total of 204 Korean-Chinese workers with MetS completed structured, self-reported questionnaires through one-on-one interviews. All quantitative data were collected by a single researcher fluent in both Korean and Chinese, ensuring clear communication and consistency. For the qualitative component, the same bilingual researcher conducted one-on-one, in-depth interviews with 12 participants at convenient times and locations. Each session lasted 40–50 min and followed a semi-structured guide. In-depth interviews were conducted in Korean or Chinese according to participant preference. Topics included health behaviors, knowledge of MetS and CVD, perceived barriers and facilitators, environmental influences, and support needs. All interviews were audio-recorded, transcribed, and reviewed to ensure accuracy. All methods were performed in accordance with the relevant guidelines and regulations, and in accordance with the Declaration of Helsinki.
Measurements
This research primarily utilized a self-reported questionnaire. All instruments were obtained via email with permission from their respective developers or translators.
General characteristics of participants
The general characteristics of participants included gender, age, marital status, cohabitation with family, education, economic status, work-related length of stay in Korea, occupation type, body mass index (BMI), working hours, family history of CVD, smoking, alcohol consumption, exercise, and health insurance coverage.
Knowledge of MetS
A self-reported questionnaire assessing individuals’ awareness, knowledge, and health behaviors was used to measure knowledge of MetS27. This instrument includes 20 items covering diagnostic criteria, causes, management methods, and complications of MetS. Participants responded to each item with “True,” “False,” or “Don’t know.” Correct responses were scored as 1 point, while incorrect or “Don’t know” responses were scored as 0, yielding a total score range of 0–20. Higher scores indicated greater knowledge of MetS. The tool’s reliability during development was Kuder-Richardson Formula 20 = 0.75, and in this research, 0.66.
Health consciousness
Health consciousness, referring to an individual’s level of interest and attitude toward their own health, was measured using a tool designed to assess personal engagement with health-related matters28. This scale consists of five items measuring interest in health knowledge, behaviors, and attitudes. Each item is rated on a 5-point Likert scale from 1 (“Not at all”) to 5 (“Very much”), with higher scores indicating greater health consciousness. The tool’s reliability at development was Cronbach’s α = 0.74, and in this research, 0.85.
Internal health locus of control
Internal health locus of control, defined as the belief that one’s health is determined by one’s own actions, was assessed using the Korean version29 of the Multidimensional Health Locus of Control scale30. The scale consists of six items, each rated on a 5-point Likert scale ranging from 1 (“Strongly disagree”) to 5 (“Strongly agree”). Scores range from 6 to 30, with higher scores indicating a stronger internal health locus of control. The tool’s reliability during development was Cronbach’s α = 0.81, and in this research, 0.83.
Depression
Depression was measured using the Patient Health Questionnaire-9 (PHQ-9), a self-reported questionnaire adapted to Korean with validated reliability and validity31. The tool consists of nine items for depression, assessing the frequency of these issues over the past two weeks. Higher total scores on the PHQ-9 indicate greater severity and frequency of depressive symptoms. The reliability of the tool at development was Cronbach’s α = 0.95, and in this research, 0.76.
Social support
Social support was measured using a tool to assess perceived support from family, relatives, friends, and others32. The tool consists of 25 items across four subdomains: emotional support, material support, informational support, and appraisal support. Each item is rated on a 5-point Likert scale from 1 (“Hardly true”) to 5 (“Very true”), with higher scores indicating more excellent social support. The overall reliability of the tool during development was Cronbach’s α = 0.94, and in this research, 0.97.
Occupational stress
Occupational stress was measured using the 24-item Korean Occupational Stress Scale-Short Form, developed by the Korea Occupational Safety and Health Agency33. The tool includes seven subdomains: job demand, job control, interpersonal conflict, job insecurity, institutional system, lack of reward, and workplace culture. Each item is rated on a 4-point scale, with higher scores indicating greater occupational stress. Scores are calculated as weighted domain values, as suggested by the original authors, and averaged across the seven domains. The tool’s reliability during development was Cronbach’s α = 0.93, and in this research, 0.80.
Use of health information and resources
An assessment tool was adapted and developed to measure community-level use of health information and resources, based on reports by the International Organization for Migration and the Migration Research and Training Center34. The tool was tailored to the study population. Content validity was confirmed by 10 experts, including nursing professors, Korean-Chinese community leaders, and workers with MetS; all items achieved a Content Validity Index of ≥ 0.80. The final tool included 10 dichotomous items: two on health education programs, four on access to community health centers/hospitals, and four on healthcare services for migrants. “Yes” responses were scored as 1, and “No” as 0, with higher scores indicating better resource utilization. The tool showed acceptable reliability (Kuder Richardson-20 = 0.61).
Cardiovascular health behaviors
These were measured using a lifestyle assessment tool developed by the Korean National Health Insurance Corporation for CVD prevention, which had been adapted and refined for male drivers in a study35. The tool comprises 18 items across six subdomains: smoking, alcohol consumption, physical activity, dietary habits, stress management, and preventive health care. Each item is rated on a 5-point Likert scale from 1 (“Not at all”) to 5 (“Very much”). For non-smokers, all three smoking-related items were scored as 5 points. The total score ranges from 18 to 90, with higher scores indicating better adherence to preventive health behaviors. The tool’s reliability was Cronbach’s α = 0.93 at development and 0.78 in this research.
Data analysis
Quantitative data were analyzed using SPSS/Win 26.0. Descriptive statistics summarized general characteristics and variables. Group differences in health behaviors were examined using t-tests and ANOVA with Scheffé’s post-hoc test. Pearson’s correlation coefficients assessed associations between variables, and hierarchical regression identified predictors of cardiovascular health behaviors. Qualitative data were transcribed using the CLOVA app and analyzed through inductive content analysis36 with MAXQDA 24 software. Two researchers reviewed the transcripts, conducted open coding, and identified key phrases. Codes were grouped into subcategories and then abstracted into overarching categories and themes. Rigor was ensured through credibility, transferability, dependability, and confirmability37.
Results
Sample characteristics and research variables
Participants had a mean age of 51.4 ± 6.3 years, and 55.4% were female. Most were married (60.3%), lived alone (54.9%), and had a high school education (60.3%). Occupations included restaurant work (23%), self-employment (21.1%), caregiving (19.1%), office work (14.2%), manufacturing (14.2%), and cleaning (8.3%). Average Work-related length of stay was 10.8 ± 4.8 years. Most participants were on hyperlipidemia medication (87.3%), and 51.0% had a body mass index ≥ 25 kg/m². A family history of CVD was reported by 52.0%, smoking by 45.1% (mean duration 7.8 ± 10.4 years), and weekly alcohol use (≥ 2 times) by 53.0%. Aerobic and strength exercise less than twice weekly were reported by 65.7% and 80.9%, respectively (Table 1). The mean scores (± SD) for key research variables were as follows: MetS knowledge (12.70 ± 2.37), health consciousness (20.19 ± 2.85), internal health locus of control (23.01 ± 3.71), and depression (3.44 ± 2.88), with 66.7% of participants classified as having normal levels of depression, 31.4% mild, and 1.9% moderate. Social support scored 88.57 ± 12.56, daily working hours averaged 12.01 ± 1.47, and occupational stress was 44.19 ± 7.86. The average score for the use of health information and resources was 2.15 ± 1.17.
Differences and associations in cardiovascular health behaviors
Women, caregivers, those with < 10 years of residence, and participants with BMI < 25 showed significantly higher cardiovascular health behavior scores. Cardiovascular health behaviors were positively correlated with MetS knowledge (r =.40), health consciousness (r =.62), internal locus of control (r =.67), social support (r =.68), and use of health information and resources (r =.31) (all p <.001). Negative correlations were found with depression (r = –.41, p <.001) and occupational stress (r = –.17, p =.016) (Table 2).
Factors influencing cardiovascular health behaviors
Hierarchical regression revealed that higher social support (β = 0.43, p <.001), internal health locus of control (β = 0.26, p <.001), female gender (β = 0.25, p <.001), caregiver occupation (β = –0.11, p =.006), and lower depression (β = –0.09, p =.037) significantly predicted better cardiovascular health behaviors. The final model accounted for 74.7% of the variance (Adjusted R² = 0.747, F = 55.19, p <.001), with no multicollinearity or autocorrelation issues (Durbin-Watson = 1.705, Variance Inflation Factor = 1.12–2.40) (Table 3).
Qualitative findings
The general characteristics of research participants are presented in Table 4. Through one-on-one in-depth interviews, 122 meaningful statements regarding participants’ lifestyle habits and perceptions of health behaviors were identified. Based on the ecological model, these statements were categorized into domains providing contextual explanations. The meaningful statements were further grouped into 12 subthemes and 6 main themes (Table 5).
Theme 1. Lack of awareness of MetS risks
Participants had low awareness of managing hyperlipidemia and hypertension, often neglecting care or discontinuing medication when asymptomatic. Despite the strong link between chronic diseases like hyperlipidemia, hypertension, and diabetes with CVD, their limited understanding led to risk underestimation and a sense of detachment from these conditions.
Subtheme 1. Overlooking the Importance of Risk Factor Management.
“I stopped taking the medication for hyperlipidemia after a month because I had no symptoms. It didn’t seem serious, and I don’t see much benefit in managing my health. Exercise just makes me tired.” (P1).
“I take blood pressure medication because I feel symptoms like headaches, but I don’t take anything for hyperlipidemia since it has no symptoms and doesn’t feel serious.” (P2).
Subtheme 2. Failure to Recognize the Link to CVD.
“I know that CVD is a condition like stroke, where blood vessels get blocked, but that’s about it. I don’t really know much else. I don’t even know if my current hyperlipidemia affects CVD, or if it’s really that dangerous.” (P1).
“I have diabetes and hyperlipidemia, but I don’t know what connection they have with CVD. I’ve never really paid attention to it, so I’m not sure. It seems like a condition that doesn’t concern me.” (P4).
Theme 2. Lack of motivation for lifestyle changes
Participants recognized the need to limit alcohol and smoking for CVD prevention but struggled with consistency due to their stress-relieving effects. Busy work environments and aging further hindered their ability to seek health information and take proactive action.
Subtheme 1. Difficulty in sustaining commitment to health management.
“I know drinking is bad for CVD, but the stress relief makes me forget my decision to quit. I tell myself, ‘I’m still young, it’ll be fine,’ and keep drinking.” (P2).
“After work, I have a drink with my husband and enjoy late-night snacks. I know I shouldn’t, but I reassure myself that my medication will prevent any harm.” (P3).
“I’ve been smoking for 20 years, so quitting is really hard. I just can’t fully commit to stopping.” (P10).
Subtheme 2. Insufficient access to disease management information.
“My wife and I want to stay healthy as we age, but we don’t know how, so we end up doing nothing. With work and aging, we don’t even take the time to look for information.” (P5).
“I don’t know how to manage my condition, so I just eat more vegetables. I don’t think not exercising is a big issue, so I don’t focus on it.” (P7).
Theme 3. Persistence of unhealthy lifestyle habits due to loneliness and depression
Participants maintained unhealthy lifestyle habits due to loneliness, seeking comfort in greasy foods like Chinese cuisine to cope with homesickness. Living alone and experiencing depression further reduced their motivation for physical activity and health management.
Subtheme 1. Emotional eating and dietary patterns reinforced by loneliness.
“Even after work and on holidays, greasy Chinese food feels right, so I eat it almost daily from a nearby restaurant. Eating helps me cope with loneliness and makes me feel a little better.” (P2).
“I’m saving money to return to China. Staying in Korea during Chinese New Year made me feel very lonely. To cope, I cook Chinese food, especially meat dishes and fried dumplings.” (P11).
Subtheme 2. Neglect of self-management due to depression.
“Living alone for so long makes me feel depressed. I don’t want to stay home, but there’s little to do, so I end up doing nothing. Apart from walking to work, I’m just holding on for my children in China.” (P3).
“I came to Korea with my husband, but after he passed away, I’ve lived alone for years. It’s lonely, and with no one to talk to, my stress built up, leading to depression. I know Living alone feels empty, making me avoid exercise even more.” (P8).
Interpersonal level
Theme 4. Influence of social support on lifestyle habits
Social support motivated participants to engage in healthier behaviors, while its absence led to reduced awareness and neglect of health management.
Subtheme 1. Encouragement from others facilitating exercise participation.
“On holidays, I go biking at Hangang Park. I started because a friend recommended it and sends me health information on WeChat. I also subscribe to health news and read it daily.” (P5).
“My niece, a nurse in China, keeps warning me about cardiovascular disease. So now, I drink only at company dinners and try to walk more and do sit-ups regularly.” (P6).
Subtheme 2. Limited health awareness due to lack of family support.
“Without someone reminding me of my condition, I feel like I’m doing less to take care of my health.” (P1).
“I came to Korea alone to earn money, and without family nagging me, I just take my medication but don’t manage my health otherwise.” (P3).
Theme 5. Challenges in Self-management due to economic activity
Participants struggled with self-care due to long working hours and financial constraints. Irregular eating habits and physical fatigue led to neglect of exercise, while the cost of medical care often resulted in delayed hospital visits and skipped check-ups.
Subtheme 1. Difficulty in maintaining healthy eating habits due to long working hours.
“I work 12-hour shifts six days a week and eat whatever the restaurant provides, mostly salty dishes like kimchi and stews. I used to exercise on my day off, but after long hours of carrying heavy pots and standing all day, my body aches too much. Now, I’d rather rest, watch TV, or meet friends to eat and drink.” (P1).
Subtheme 2. Limited access to medical services due to financial burden.
“Hospitals aren’t far, but every visit costs money, so I only go if absolutely necessary. I’m here to earn for my children in China, so unless the pain is severe, I just go to the pharmacy or endure it.” (P1).
“With my limited income, I prioritize saving over medical care. I avoid clinics due to cost concerns and instead self-medicate with pharmacy drugs.”(P6).
Theme 6. Need for tailored health support for foreign migrant workers
Participants expressed the need for tailored health programs and improved promotion of services for foreign workers. They preferred practical, case-based materials in Chinese and Korean, as well as accessible lectures and free programs to boost motivation for health management.
Subtheme 1. Call for expanded and publicized health support programs for migrants.
“Many Korean-Chinese workers focus on earning money and lack awareness of available health benefits. If diseases were more publicized, we might be more motivated to manage our health.” (P3).
“I received a letter about a free health checkup and found out I have hyperlipidemia. I don’t even know what medical support exists for foreigners or how to use my health insurance. More promotion is needed.” (P5).
Subtheme 2. Demand for culturally tailored health education for Korean-Chinese workers.
“Neither I nor my coworkers have ever received health education. A simple, short booklet in Chinese and Korean with real-life cases would be helpful.” (P2).
“I hope free courses are available where we can learn about our health during our free time.” (P4).
“It would be great to see a video about CVD risks for Korean-Chinese workers, even on platforms like TikTok, buses, or subways.” (P09).
Mixed method integration
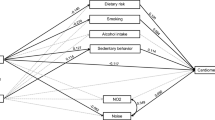
This study, grounded in the Ecological Model, integrated quantitative and qualitative findings to explore factors influencing cardiovascular health behaviors among Korean-Chinese workers with MetS. Six key themes emerged, linking findings across levels. Quantitatively, depression and internal health locus of control (intrapersonal level), and social support (interpersonal level) were significant predictors. These were echoed qualitatively in themes such as: “Persistence of unhealthy habits due to loneliness and depression” and “Lack of motivation for lifestyle changes.” Conversely, MetS knowledge, health consciousness (intrapersonal), occupational stress (institutional), and use of health information and resources (community) were not significant in the quantitative analysis but were elaborated qualitatively through themes: “Lack of MetS risk awareness,” “Challenges in self-management due to work demands,” and “Need for tailored health support for migrant workers” (Fig. 1). Through this integrated analysis, it was found that migrant workers at risk for CVD experience multiple, interacting health determinants at various levels that influence their health behaviors.
Discussion
This study examined factors influencing cardiovascular health behaviors among Korean-Chinese migrant workers with MetS through a mixed-methods approach. The mean cardiovascular health behavior score (50.98 ± 5.60) was similar to previous studies on Korean-Chinese workers12 and Korean male office workers37. However, considering the maximum score of 90, the overall engagement in preventive health behaviors remained insufficient. This aligns with national data showing Korean-Chinese workers engage in fewer health behaviors compared to other migrant groups38. Qualitative data supported these findings, revealing that long working hours, lack of rest, and a busy work environment limited participants’ ability to seek health information or adopt healthy practices. High smoking (45.1%) and alcohol consumption (90.2%) rates, along with low levels of physical activity, underscore the need for systematic interventions.
Hierarchical multiple regression analysis identified gender and occupation as significant factors influencing cardiovascular health behaviors. This result aligns with studies on migrant workers in Korea, where men were found to engage in fewer health promotion behaviors than women39. It also supports findings from a systematic review, which showed that migrant workers in high-income countries, such as caregivers in occupations with better access to health information, were more likely to recognize their health issues and improve health outcomes40. These results suggest that male workers tend to have relatively lower motivation for health behavior practices, while caregivers are more proactive in engaging in behaviors to prevent CVD. In contrast, restaurant and manufacturing workers faced barriers to accessing health information. These results highlight the need for tailored workplace-based interventions and health education programs adapted to different job types.
Internal health locus of control emerged as a key intrapersonal factor positively associated with health behaviors. Participants with a strong belief in their ability to control their health were more likely to engage in healthy behaviors41. Research involving 16,150 Australian adults also linked internal health locus of control to psychological well-being and improved health behaviors42while a systematic review found that belief in health control fosters active health practices43. However, qualitative findings revealed that many participants struggled with unhealthy habits, such as smoking or late-night eating, due to stress and lack of motivation. These behaviors were linked to feelings of helplessness and reduced interest in health. Strengthening internal motivation and self-efficacy through tailored programs could enhance lifestyle modification efforts.
Depression negatively impacted health behaviors as an individual factor in this study, consistent with findings from a study on middle-aged and older workers in China, where depression was shown to hinder health behaviors44. The theme “persistence of unhealthy lifestyle habits due to loneliness and depression” highlighted emotional and social challenges faced by this population. These findings align with previous research demonstrating that psychological distress reduces engagement in health-promoting behaviors20. Therefore, integrating mental health support and social-emotional resources into health programs is essential for improving outcomes.
Social support at the interpersonal level significantly influenced participants’ health behaviors. This aligns with a study on foreign workers in Korea, where support from family, friends, and colleagues played a key role in addressing health issues and fostering healthy lifestyles22. Mixed-methods research similarly highlights the positive impact of social support on CVD prevention behaviors in rural Korean populations45. Qualitative findings highlighted the theme “The Impact of Social Support on Lifestyle Habits,” indicating that encouragement from friends and family promoted healthier behaviors such as exercise and reduced alcohol use. However, limited family support, especially among those living alone (54.9%), often hindered health management. These results underscore the need for systematic programs to enhance social support networks for effective CVD prevention.
Although MetS knowledge was not statistically significant in the regression model, qualitative interviews revealed low awareness of MetS risks. Many participants did not recognize the importance of managing MetS, especially those with lower educational backgrounds. This was reflected in the theme “Lack of awareness of MetS risks,” reinforcing the need for culturally and linguistically tailored educational programs.
At the institutional level, occupational stress was not a significant predictor, possibly due to limitations of the measurement tool, which may not fully capture the stress experienced by self-employed or informally employed migrant workers. Participants reported long work hours, physical fatigue, and limited access to healthcare, which negatively affected their ability to manage health. The theme “Challenges in self-management due to economic activity,"where participants reported working over 12 h daily, leaving little time for healthy meals, exercise, or hospital visits illustrated how employment conditions constrained participants’ time and resources for health. This aligns with research showing that limited rest and economic pressures deprioritize health management46. These findings underscore the importance of developing assessment tools that reflect the realities of diverse labor sectors.
Although community-level variables were not statistically significant in the quantitative analysis, they were prominently highlighted in the qualitative findings. Participants expressed a strong desire for tailored support programs at the community level, particularly emphasizing the need for culturally appropriate materials—such as Korean-Chinese language guides, case-based videos, and regular health education. While most participants were enrolled in the national health insurance system, many lacked knowledge on how to utilize it effectively, reflecting previous findings that show high enrollment but low service utilization among migrant workers.
While this study did not directly measure policy-level factors such as labor conditions or access to health insurance, their potential indirect impact on migrant workers’ health behaviors remains considerable and should be acknowledged. Future research would benefit from incorporating these dimensions to more fully apply the ecological model. Moreover, the findings suggest cross-level interactions that influence health behaviors. For example, limited health literacy at the individual level was often compounded by institutional barriers, such as a lack of culturally sensitive guidance in healthcare settings, leading to reduced service use. These dynamics reflect the ecological model’s emphasis on the interplay between individual and structural factors. A more explicit exploration of such multi-level influences in future research could enhance theoretical integration and guide more effective interventions.
This study has several limitations. First, approximately 21% of participants were self-employed, yet the occupational stress tool used was developed for employees in structured organizational settings. As a result, it may not have adequately captured the unique stressors experienced by self-employed individuals, potentially contributing to discrepancies between quantitative and qualitative findings. This highlights the need for more inclusive measurement tools and practical support tailored to diverse work environments. Second, while snowball sampling was appropriate for reaching a hard-to-reach population, it may have introduced selection bias and limited the generalizability of the results. Third, the use of self-reported data may have introduced response bias, and the qualitative findings may also be limited in generalizability due to voluntary participation and potential researcher interpretation bias.
Nevertheless, a key strength of this study lies in its mixed-methods design grounded in the Ecological Model, which allowed for a multi-level exploration of cardiovascular health behaviors among a relatively underserved population of migrant workers. By integrating quantitative and qualitative data, the study captured not only measurable predictors but also the lived experiences of participants, providing deeper and more practical insights.
Conclusions
This study identified key factors influencing cardiovascular health behaviors in Korean-Chinese workers with MetS. Gender, occupation type, internal health locus of control, depression, and social support were significant predictors, while qualitative findings illuminated contextual barriers, including low awareness, loneliness, economic stress, and limited access to tailored resources. These results emphasize the need for multidimensional interventions addressing individual motivation, psychological well-being, occupational conditions, and community support systems. Culturally sensitive, occupation-specific, and linguistically appropriate programs are essential to improving CVD prevention behaviors and reducing health disparities in this population.
Data availability
The data that support the findings of this study are not openly available due to reasons of sensitivity and are available from the corresponding author upon reasonable request.We used to analyze the data using IBM SPSS version 26.0. https://www.ibm.com/docs/en/spss-statistics/26.0.
References
World Health Organization. Cardiovascular diseases. (2025). https://www.who.int/health-topics/cardiovascular-diseases#tab=tab_1
Korea Occupational Safety & Health Agency. Health vulnerability assessment of migrant workers in hazardous substance exposure workplaces. (2020). https://kosha.or.kr/oshri/publication/researchReportSearch.do?mode=view&articleNo=419767&article.offset=250&articleLimit=5
World Health Organization. Refugee and migrant health. (2025). https://www.who.int/health-topics/refugee-and-migrant-health#tab=tab_1
Korea Ministry of Justice. Status of registered migrant nationals (by region, by nationality). (2024). https://www.moj.go.kr/bbs/immigration/227/585505/artclView.do
Yoon, J. H. Korean-Chinese labor conditions on overseas Koreans and employment visit workers. Korean Labor and Society Institute. (2022). http://www.klsi.org/bbs/board.php?bo_table=B03&id=2595
Chae, D. H., Kim, N. K. & Asami, K. Predictive factors of subjective health among Korean-Chinese and naturalized vietnamese immigrants: focusing on the influence of ethnicity and gender. J. Korean Soc. Multicult Health. 14, 1–16. https://doi.org/10.33502/JKSMH.14.2.001 (2024).
American Heart Association. About MetS. (2023). https://www.heart.org/en/health-topics/metabolic-syndrome/about-metabolic-syndrome
Hayden, M. R. Overview and new insights into the mets: risk factors and emerging variables in developing type 2 diabetes and cerebrocardiovascular disease. Medicina 59, 561. https://doi.org/10.3390/medicina59030561 (2023).
The Writing Committee of the Report on Cardiovascular Health and Diseases in China. Report on cardiovascular health and diseases in china 2022: an updated summary. Biomed. Environ. Sci. 36, 573–603. https://doi.org/10.3967/bes2023.106 (2023).
Yao, F. et al. Prevalence and influencing factors of mets among adults in china from 2015 to 2017. Nutrients 13, 4475. https://doi.org/10.3390/nu13124475 (2021).
Korean Society of CardioMetS. MetS Fact Sheet in Korea 2024. https://www.kscms.org/Fact-sheet/?q=YToxOntzOjEyOiJrZXl3b3JkX3R5 (2024).
Zhang, Y. Z. & Hwang, S. Y. The moderating effect of mental health on the relationship between cardiovascular disease awareness and health behaviors of middle-aged korean chinese workers with cardiovascular risk factors in korea. J. Transcult Nurs. 34, 131–142. https://doi.org/10.1177/10436596221147078 (2023).
Pan, F. et al. Association between ultra-processed food consumption and mets among adults in china—Results from the china health and nutrition survey. Nutrients 15, 752. https://doi.org/10.3390/nu15030752 (2023).
Zheng, X. et al. The effects of a nurse-led lifestyle intervention program on cardiovascular risk, self-efficacy, and health-promoting behaviors among patients with mets: randomized controlled trial. Int. J. Nurs. Stud. 109, 103638. https://doi.org/10.1016/j.ijnurstu.2020.103638 (2020).
Kim, H. J. et al. MetS awareness in the general korean population: results from a nationwide survey. Korean J. Intern. Med. 39, 272–282. https://doi.org/10.3904/kjim.2023.363 (2024).
Remr, J. Validation of the health consciousness scale among the czech population. Healthcare 11, 1628. https://doi.org/10.3390/healthcare11111628 (2023).
Lu, Q. et al. Depressive symptoms, lifestyle behaviors, and risk of cardiovascular disease and mortality in individuals of different socioeconomic status: A prospective cohort research. J. Affect. Disord. 347, 345–351. https://doi.org/10.1016/j.jad.2023.09.025 (2024).
Rosenthal, T., Touyz, R. M. & Oparil, S. Migrating populations and health: risk factors for cardiovascular disease and mets. Curr. Hypertens. Rep. 24, 325–340. https://doi.org/10.1007/s11906-022-01194-5 (2022).
Kim, Y., Lee, H. & Chung, M. L. Living labs for a mobile app-based health program: effectiveness of a 24-week walking intervention for cardiovascular disease risk reduction among female Korean-Chinese migrant workers: a randomized controlled trial. Arch. Public. Health. 80, 181. https://doi.org/10.1186/s13690-022-00941-z (2022).
Jeong, H. & Kim, Y. Structural equation modeling of health promotion behavior on migrant workers: A multi-group analysis based on the period of residence. J. Korean Acad. Nurs. 54, 73–92. https://doi.org/10.4040/jkan.23101 (2024).
Wang, Z., Fang, Y. & Zhang, X. Impact of social capital on health behaviors of middle-aged and older adults in China-An analysis based on CHARLS2020 data. Healthcare 12, 1154. https://doi.org/10.3390/healthcare12111154 (2024).
Jeong, S., Yun, S. B., Park, S. Y. & Mun, S. Understanding cross-data dynamics of individual and social/environmental factors through a public health lens: explainable machine learning approaches. Front. Public. Health. 11, 1257861. https://doi.org/10.3389/fpubh.2023.1257861 (2023).
McLeroy, K. R., Bibeau, D., Steckler, A. & Glanz, K. An ecological perspective on health promotion programs. Health Educ. Behav. 15, 351–377 (1988).
Creswell, J. W. & Plano Clark, V. L. Designing and Conducting Mixed Methods Research 2nd edn (Sage, 2011).
Kim, H. & Song, M. The relationship between cultural adaptation stress and health promotion behaviors of ethnic chinese elderly immigrants in korea. J. Korean Acad. Nurs. 13, 70–80. https://doi.org/10.16952/pns.2016.13.2.70 (2016).
Guest, G., Bunce, A. & Johnson, L. How many interviews are enough? An experiment with data saturation and variability. Field Methods. 18, 59–82. https://doi.org/10.1177/1525822X05279903 (2006).
Oh, Y. G. et al. Knowledge, awareness, and health behaviors related to lifestyle among the risk group of mets in rural areas. J. Korean Acad. Nurs. 37, 790–800. https://doi.org/10.4040/jkan.2007.37.5.790 (2007).
Park, I. H. et al. A survey on the status of environment and elderly health of senior centers in gwangju city. Chonnam Natl. Univ. Res. Inst. Nurs. Sci. (2006).
Wallston, B. D. & Wallston, K. A. Locus of control and health: A review of the literature. Health Educ. Monogr. 6, 107–117 (1978).
Park, B. Y. Factors influencing health-promoting behaviors in middle-aged women. Master’s thesis, Ewha Womans Univ. (2008).
Park, S. J. et al. Reliability and validity of the korean version of the patient health Questionnaire-9 (PHQ-9). J. Korean Soc. Anxiety Disord. 6, 119–124 (2010).
Park, J. W. A research on the development of a social support scale. Master’s thesis, Yonsei Univ. (1985).
Jang, S. J. & Ko, S. B. Korean occupational stress scale (KOSS). Stress Res. 13, 183–197 (2005).
Park, M. J. Issues in immigrant health care policies. Seongnam: Migration Research and Training Center. Report No.: MRTC Issue Brief 2018-08 (2018).
Kim, E. & Hwang, S. Risk of cardiovascular and cerebrovascular diseases, prevention-related knowledge, stage of change, and health behaviors among male drivers in a local region. Korean J. Adult Nurs. 23, 321–331 (2011).
Elo, S. & Kyngäs, H. The qualitative content analysis process. J. Adv. Nurs. 62, 107–115. https://doi.org/10.1111/j.1365-2648.2007.04569.x (2008).
Kim, E. J. & Hwang, S. Y. Awareness and utilization of mobile health and preventive health behavior according to cardiovascular risk factor cluster type in early middle-aged male workers. Korean J. Adult Nurs. 31, 562–572. https://doi.org/10.7475/kjan.2019.31.5.562 (2019).
Kang, S. J. et al. Factors associated with self-rated health among immigrant workers in south korea: analyzing the results of the 2020 survey on immigrants’ living conditions and labor force. Front. Public. Health. 10, 933724. https://doi.org/10.3389/fpubh.2022.933724 (2022).
Nam, Y. The effect of migrant workers’ health beliefs on health behaviors. Korean Soc. Sch. Commun. Health Educ. 21, 91–103. https://doi.org/10.35133/kssche.20200531.07 (2020).
Yang, B. et al. Structural origins of poor health outcomes in documented temporary foreign workers and refugees in high-income countries: A review. Healthcare 11, 1295. https://doi.org/10.3390/healthcare11091295 (2023).
Nowak, P. F., Rogowska, A. M. & Kwaśnicka, A. The mediating role of health behaviors in the relationship between internal locus of control and life satisfaction in public health students. Sci. Rep. 14, 19112. https://doi.org/10.1038/s41598-024-23413-5 (2024).
Slopiecka, A. & Chrapek, M. Relationship between health-related locus of control and health behaviour among university students. Sleep. Med. Disord Int. J. 3, 10–15. https://doi.org/10.15406/smdij.2019.03.00060 (2019).
Dogonchi, M., Mohammadzadeh, F. & Moshki, M. Investigating the relationship between health locus of control and health behaviors: A systematic review. Open. Public. Health J. 15, e187494452208010. https://doi.org/10.2174/18749445-v15-e2208010 (2022).
Zhang, Y. et al. The impact of preventive behaviors on self-rated health, depression symptoms, and daily functioning among middle-aged and elderly chinese: an empirical research. PLoS ONE. 19, e0305672. https://doi.org/10.1371/journal.pone.0305672 (2024).
Park, B., Yang, J. & Kim, Y. Factors influencing cardiovascular disease preventive behaviors among rural residents based on a socio-ecological model in South Korea: A mixed method research. Health Soc. Care Community 6051599 (2023). (2023). https://doi.org/10.1155/2023/6051599
Zhang, F., Xu, W. & Khurshid, A. The interplay of migrant workers’ working hours, income, and well-being in china. Sustainability 15, 11409. https://doi.org/10.3390/su151411409 (2023).
Acknowledgements
Special thanks to all the participants in the study.
Funding
No funding source.
Author information
Authors and Affiliations
Contributions
SYH, YZZ: Study conception and design YZZ: Data collection YZZ, SYH: Data analysis and interpretation YZZ, SYH: Drafting of the article SYH: Critical revision of the article.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was conducted following approval from the Institutional Review Board (IRB) of Hanyang University (Approval Number: HYUIRB-202407-002).
Consent for publication
All participants provided informed consent before participation in the research.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhang, Y.Z., Hwang, S.Y. Factors influencing cardiovascular health behaviors among Korean-Chinese migrant workers with metabolic syndrome using mixed methods. Sci Rep 15, 23165 (2025). https://doi.org/10.1038/s41598-025-05926-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-05926-w