Abstract
This retrospective cohort study investigates the epidemiology of type 2 diabetes mellitus (T2DM) in adolescents in Kazakhstan from 2014 to 2021, focusing on incidence and all-cause hospital admissions. A cohort of 725 adolescents aged 10–17 years diagnosed with T2DM from 2014 to 2021 and registered in the Unified National Electronic Healthcare System (UNEHS) in Kazakhstan. Baseline demographic characteristics, incidence rates, and associated comorbidities and complications were analyzed. For the analysis of all-cause hospitalization rates, Cox regression modeling was used to assess the risk factors associated with hospitalizations, including demographic parameters and the presence of complications. The incidence of T2DM increased from 1.9 to 5.8 per 100,000 in the 10–13 age group and from 3.5 to 8.2 per 100,000 in the 14–17 age group. Girls had a higher incidence (3.0 to 7.3 per 100,000) compared to boys (2.5 to 6.5 per 100,000). The most common complications included retinopathy (14.62%), neuropathy (12.14%), and diabetic foot (6.62%). After diagnosis, 17.79% of patients were hospitalized due to all causes. Statistically significant risk factors for all-cause hospitalization included rural residence (HR: 1.51, 95% CI: 1.04–2.20), hypertension (HR: 1.99, 95% CI: 1.04–3.79), retinopathy (HR: 2.50, 95% CI: 1.56–4.02), and neuropathy (HR: 2.73, 95% CI: 1.06–2.83).
Similar content being viewed by others
Introduction
Type 2 diabetes mellitus (T2DM) is a metabolic condition associated with hyperglycemia due to diminished response to insulin, or insulin resistance, which represents a significant and growing public health concern globally1. Contrary to the prior tendency of T2DM to be observed predominantly in adults and the elderly, recently, T2DM has been more common among young adults, adolescents, and even children2.
Globally, the incidence and prevalence of pediatric T2DM have been increasing over recent decades. Among youth aged 10–19 years, the prevalence rate of T2DM reached 34 cases per 100,000 population in 2001 in the USA, further increasing up to 46 cases in 2009, which constitutes a 31% increase, and up to 67 cases per 100,000 population in 20171,3,4.
In Europe, the estimated prevalence rates of T2DM among youth are below 0.5 cases per 100,000 population on average, with the estimates in the UK reaching 2.9 cases in 20131. The trends in overweight and obesity, which are key risk factors for T2DM, vary significantly across Europe. A systematic review and meta-analysis covering the period from 1999 to 2016 and focusing on children of age 2–13 years revealed the lower prevalence of overweight and obesity in some regions, such Atlantic and Central Europe (14–21%), and higher estimates in others, such as the Mediterranean region (24–37%)5. While some high-income countries are stabilizing or reducing obesity rates, low- and middle-income countries continue to experience rising trends, emphasizing the need for interventions5.
Pediatric T2DM carries severe clinical implications. Adolescents diagnosed with T2DM often present with a more aggressive phenotype, characterized by rapid progression and early onset of complications such as nephropathy, retinopathy, and cardiovascular disease6. Furthermore, increased morbidity and mortality associated with young-onset T2DM highlights the need for early management to mitigate long-term health outcomes1.
While recent research into diabetes mellitus in Kazakhstan exists7,8,9, the epidemiology of T2DM among adolescents remains underexplored. Comprehensive epidemiological studies are essential to understand the incidence, risk factors, and associated health outcomes. Since 2014, nationwide administrative health data have been aggregated by the Unified National Electronic Health System (UNEHS) in Kazakhstan. Availability of medical records of patients under inpatient and outpatient care on a national scale creates an excellent opportunity to conduct retrospective population-based research into the epidemiology of a wide variety of conditions, including T2DM in adolescents. Using administrative healthcare data, we aim to investigate the incidence of T2DM and the risk of all-cause hospital admissions among adolescents with T2DM diagnosed between 2014 and 2021 in Kazakhstan.
Methods
Study population
This retrospective cohort study included patient records of T2DM adolescents aged 10–17 years at diagnosis who were registered in the UNEHS between January 1st, 2014, and December 31st, 2021. Individual patient records containing socio-demographic and clinical data were extracted from the UNEHS database. The database has been described in greater detail elsewhere10. T2DM was defined using the International Classification of Diseases 10 (ICD-10) as codes E11.x.
Exposures and covariates
Patient records extracted from the UNEHS database contained the following information: age, sex, ethnicity, residence, ICD-10 codes of the diagnoses, anonymized population registry number (RPN), and dates of birth, diagnosis, date of death, date of admission, and date of discharge. Where applicable, the information on the date of death was obtained through linkage with the Population Registry through RPN. Age was divided into 2 categories: 10–13 years and 14–17 years. The following comorbidities were included: arterial hypertension, diabetic retinopathy, diabetic neuropathy, diabetic nephropathy, neoplasms, and diabetic foot.
Outcome assessment
For each year of follow-up between 2014 and 2021, incidence rates per 100,000 population were estimated for T2DM patients by dividing the number of incident cases in a year by Kazakhstan’s total population of ages 10–17 years in that year. The population parameters of Kazakhstan were obtained from the Statistics Committee11. Incidence rates of all-cause hospital admissions were estimated per 1,000 person-years. The follow-up period was defined from the date of T2DM diagnosis to December 31st, 2021, or the date of the earliest hospital admission due to all causes.
Statistical methods
For categorical variables, data were summarized as patient numbers and percentages. The median and interquartile range (IQR) were used to summarize continuous variables. Cox regression modeling was used to produce crude and adjusted hazard ratios (HR) with 95% confidence intervals (CI) corresponding to the associations between risk factors and all-cause hospital admissions.
All statistical analyses were performed using STATA 15 MP2 Version (STATA Corporation, College Station, TX). P values are two-sided and reported as statistically significant at < = 0.05 for all analyses.
Results
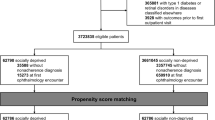
Figure 1 depicts a flowchart of cohort selection. From the inpatient and outpatient registries, records of 353 and 483 of T2DM patients were identified, respectively. After merging the datasets and removing duplicate observations, the final cohort of 725 patients was derived.
Table 1 presents the baseline characteristics of the cohort. From the 725 patients in the cohort, 383 (52.83%) were female, 427 (58.90%) were aged 14–17 years at T2DM diagnosis, 465 (68.89%) were urban residents, and 12 (1.66%) died. The most common complications were retinopathy, affecting 106 (14.62%) patients, neuropathy, affecting 88 (12.14%) patients, and diabetic foot, affecting 48 (6.62%) patients, followed by nephropathy, hypertension, and neoplasms. After the initial T2DM diagnosis, 129 (17.79%) patients were hospitalized at least once due to all causes.
The incidence of T2DM in the cohort showed a noticeable upward trend over the study period. As illustrated in Fig. 2, the incidence rates among adolescents aged 10–13 years old increased from 1.9 per 100,000 population in 2014 to 5.8 per 100,000 population in 2021. Similarly, for adolescents aged 14–17 years, the incidence rates rose from 3.5 per 100,000 population in 2014 to 8.2 per 100,000 population in 2021. The overall trend indicates a significant increase in the incidence of T2DM among both age groups over the years.
Figure 3 illustrates the incidence rates of T2DM stratified by sex and year of diagnosis. The estimates increased from 2.5 to 6.5 cases and from 3.0 to 7.3 cases per 100,000 population between 2014 and 2021 among boys and girls, respectively.
The median follow-up time until all-cause hospital admission was 0.37 years with an IQR of 0.12–0.84 years. The incidence rates of all-cause hospital admissions per 1,000 person-years (PY) in the cohort stratified by age category are depicted in Fig. 4. For adolescents aged 10–13 years, the incidence rates fluctuated from 0.36 per 1,000 PY in 2014 to 0.31 per 1,000 PY in 2021. Among patients aged 14–17 years, the rates varied from 0.14 per 1,000 PY in 2014 to 0.37 per 1,000 PY in 2021. Although there were some fluctuations, a general upward trend is observed in the incidence of all-cause hospital admissions over the study period.
Figure 5 illustrates the incidence rates of all-cause hospital admissions per 1,000 person-years (PY) stratified by sex. Similarly to Fig. 4, there are notable fluctuations in the estimates over the study period. Between 2014 and 2021, the rates ranged from 0.05 to 0.37 and from 0.35 to 0.31 cases per 1,000 PY among male and female patients, respectively.
As presented in Table 2, several risk factors were statistically significantly associated with the risk of all-cause hospital admissions among adolescents with T2DM. Rural residence was associated with a higher risk of all-cause hospitalization compared to urban residence (adjusted HR: 1.51, 95% CI: 1.04–2.20, p = 0.030). The presence of hypertension (adjusted HR: 1.99, 95% CI: 1.04–3.79, p = 0.037), retinopathy (adjusted HR: 2.50, 95% CI: 1.56–4.02, p < 0.001), and neuropathy (adjusted HR: 2.73, 95% CI: 1.06–2.83, p = 0.028) were also significantly associated with higher risks of all-cause hospitalization. In the fully adjusted Cox regression model, 50 cases were censored due to missing data in the parameter of residence (urban/rural). However, inclusion of the parameter of residence into the model substantially improved its explanatory power. It was decided not to use imputation, since the data in this parameter were missing for 50 (6.89%) cases, and only 3 of them had records of hospital admission. In terms of mortality, for all the 12 cases that ended in death over the follow-up period, there were records of hospitalization before death. Since hospital admission was used as the failure event in the model, and death occurred after a documented hospitalization in all these cases, they were not censored.
Discussion
This study provides an analysis of the epidemiology of T2DM in adolescents in Kazakhstan based on data aggregated in the Unified National Electronic Healthcare System (UNEHS) for the period of 2014–2021. The results indicate a noticeable increase in the incidence of T2DM among adolescents, with significant differences observed based on age and sex. Additionally, several factors were identified as statistically significantly associated with the risk of all-cause hospital admissions among adolescents diagnosed with T2DM, namely rural residence and diagnoses of hypertension, retinopathy, and neuropathy.
Our findings show a substantial increase in the incidence of T2DM among adolescents in Kazakhstan from 2014 to 2021. The incidence rates for adolescents aged 10–13 years rose from 1.9 to 5.8 per 100,000 population, while rates for those aged 14–17 years increased from 3.5 to 8.2 per 100,000 population. This trend was consistent for both boys and girls, reflecting a growing public health concern, and aligning with global observations. For instance, the SEARCH for Diabetes in Youth study reported the crude annual incidence rates of 9 cases per 100,000 people in 2002, and 12.5 cases in 20123. A more recent systematic review found that the incidence of T2DM in children and adolescents under 20 years varied dramatically between countries and ranged from 0.1 (Germany) to 90.7 (Iran) cases per 100,000 population12. Additionally, based on the data from the Centers for Disease Control and Prevention, the incidence rates of T2DM among youth have been continuously increasing between 2003 and 201513. Potential contributors outlined in prior research are increased obesity, changes in diets and physical activity, and different diagnostic practices due to improved awareness of T2DM in youth3.
The incidence of all-cause hospital admissions among adolescents with T2DM also exhibited a general upward trend, although with fluctuations. Comparing these findings to diabetes-related hospitalization rates among T2DM adolescents, a study from California reported no change in trends between the ages of 13–19 years14. However, all-cause hospital admissions among youth with T2DM are more likely in general, compared to youth without diabetes mellitus and those with T1DM11. The risks are consistently higher in the year prior to diagnosis of T2DM, 1 year post-diagnosis, and 5 years post-diagnosis15.
The observed increase in hospital admission rates from 2014 to 2018 is followed by a notable decline in 2019, and then a sharp rise through 2021. We interpret these patterns in the context of broader healthcare system dynamics, particularly the impact of the COVID-19 pandemic, which has been studied locally16,17. The drop in 2019 and the subsequent fluctuations likely reflect changes in healthcare utilization during the pandemic period, including reduced access to routine care, decreased monitoring of chronic conditions, and altered health-seeking behavior among patients and families. These disruptions may have temporarily suppressed hospitalization rates, especially among adolescents with T2DM, despite ongoing disease burden.
Adolescents from rural areas had a higher risk of all-cause hospital admissions compared to those from urban areas (adjusted HR: 1.51, 95% CI: 1.04–2.20). This finding is consistent with other studies that have highlighted disparities in healthcare access, socioeconomic status, and health literacy between rural and urban populations18. The presence of hypertension nearly doubled the risk of hospitalization (adjusted HR: 1.99, 95% CI: 1.04–3.79). Hypertension is a common comorbidity in T2DM and contributes to an increased risk of complications and hospitalizations19. Both retinopathy (adjusted HR: 2.50, 95% CI: 1.56–4.02) and neuropathy (adjusted HR: 2.73, 95% CI: 1.06–2.83) were strongly associated with higher hospitalization risks. These complications reflect poor glycemic control and advanced disease stages, underscoring the need for regular screening and early intervention to prevent severe outcomes20.
There are several strengths to this study. Firstly, to our knowledge, this is the first study into the epidemiology of T2DM among adolescents in Kazakhstan and all-cause hospitalizations in this cohort using aggregated data from the nationwide digital healthcare registries, allowing for a more comprehensive look at these topics. Secondly, this retrospective cohort study uses data collected continuously over the period of 8 years, which benefited the analysis of trends over time.
This study has several limitations. The use of secondary data from UNEHS may be influenced by measurement accuracy and documentation practices outside the researchers’ control. The diagnostic coding in the UNEHS database is based on ICD-10 codes assigned by treating clinicians, and we were not able to independently verify the accuracy of the recorded type 2 diabetes (T2D) diagnoses or the completeness of the data. A concern arose that cases of type 1 diabetes may have been misclassified as type 2 diabetes. While such misclassification is a recognized limitation in administrative datasets, it is generally more common in adults, where latent autoimmune diabetes in adults and atypical presentations of type 1 diabetes may be misclassified as T2D21,22. In contrast, type 1 diabetes is more common and more readily recognized in children, making misclassification less likely in pediatric cases. Another limitation is that the data were originally collected for purposes other than the specific research questions of this study. This mismatch in data collection objectives and methodologies may have resulted in certain variables being unavailable or not aligned precisely with the research aims. The use of secondary data also disallows identifying and addressing potential loss to follow-up. Lack of detailed clinical and instrumental data limits the scope of our analysis. Additionally, as an observational study, causality cannot be inferred from the associations observed. Finally, it is acknowledged that there may be residual confounding due to unmeasured or unknown factors.
Despite these limitations, this study provides valuable insights into the epidemiology of T2DM in adolescents in Kazakhstan. It sets the stage for further research to address these limitations and enhance our understanding of this growing public health issue.
Conclusion
In conclusion, this study reveals a concerning rise in the incidence of T2DM among adolescents in Kazakhstan, with rural residents and those with hypertension, retinopathy, and neuropathy being at particularly high risk of all-cause hospital admissions after the diagnosis of T2DM. These findings underscore the need for targeted public health interventions to prevent T2DM and its complications in adolescents, particularly in rural areas where healthcare access may be limited. Improving diabetes management and preventive care will be essential in reducing the burden of this chronic disease and ensuring better health outcomes for Kazakhstan’s youth.
Data availability
All data related to this study are available from the Republican Center for Electronic Health of the Ministry of Health of the Republic of Kazakhstan, but restrictions apply to the availability of these data, which were used under the contract agreement for the current study and are not publicly available. Data are, however, available from the authors upon reasonable request and with permission from the Ministry of Health of the Republic of Kazakhstan. Queries should be directed to– D.G. (d.galiyeva@nu.edu.kz).
References
Magliano, D. J. et al. Young-onset type 2 diabetes mellitus—implications for morbidity and mortality. Nat. Rev. Endocrinol. 16, 321–331. https://doi.org/10.1038/s41574-020-0334-z (2020).
Viner, R., White, B. & Christie, D. Type 2 diabetes in adolescents: a severe phenotype posing major clinical challenges and public health burden. Lancet 389, 2252–2260. https://doi.org/10.1016/S0140-6736(17)31371-5 (2017).
Dabelea, D. et al. Prevalence of type 1 and type 2 diabetes among children and adolescents from 2001 to 2009. JAMA 311, 1778–1786. https://doi.org/10.1001/jama.2014.3201 (2014).
Lawrence, J. M. et al. Trends in prevalence of type 1 and type 2 diabetes in children and adolescents in the US, 2001–2017. JAMA 326, 717–727. https://doi.org/10.1001/jama.2021.11165 (2021).
González-Álvarez, M. A., Lázaro-Alquézar, A. & Simón-Fernández, M. B. Global trends in child obesity: are figures converging? Int. J. Environ. Res. Public. Health. 17, 9252. https://doi.org/10.3390/ijerph17249252 (2020).
Lascar, N. et al. Type 2 diabetes in adolescents and young adults. Lancet Diabetes Endocrinol. 6, 69–80. https://doi.org/10.1016/S2213-8587(17)30186-9 (2018).
Galiyeva, D. et al. Epidemiology of type 1 and type 2 diabetes mellitus in kazakhstan: data from unified National electronic health system 2014–2019. BMC Endocr. Disord. 22, 275. https://doi.org/10.1186/s12902-022-01200-6 (2022).
Galiyeva, D. et al. Epidemiology of type 1 diabetes mellitus in children in Kazakhstan: data from unified National electronic health system 2014–2021. Electron. J. Gen. Med. 20, em543. https://doi.org/10.29333/ejgm/13663 (2023).
Orazumbekova, B. et al. Prevalence of impaired fasting glucose and type 2 diabetes in Kazakhstan: findings from large study. Front. Public. Health. 10, 810153. https://doi.org/10.3389/fpubh.2022.810153 (2022).
Gusmanov, A. et al. Review of the research databases on population-based registries of unified electronic healthcare system of Kazakhstan (UNEHS): possibilities and limitations for epidemiological research and real-world evidence. Int. J. Med. Inf. 170, 104950. https://doi.org/10.1016/j.ijmedinf.2022.104950 (2023).
National Bureau of Statistics of the Republic of Kazakhstan. Demographic yearbook of Kazakhstan. https://stat.gov.kz/en/. Accessed 27 Apr 2024 (Republic of Kazakhstan Strategic Planning and Reform Agency, 2023).
Wu, H. et al. Worldwide estimates of incidence of type 2 diabetes in children and adolescents in 2021. Diabetes Res. Clin. Pract. 185, 109785. https://doi.org/10.1016/j.diabres.2022.109785 (2022).
Buttermore, E., Campanella, V. & Priefer, R. The increasing trend of type 2 diabetes in youth: an overview. Diabetes Metab. Syndr. Clin. Res. Rev. 15, 102253. https://doi.org/10.1016/j.dsx.2021.102253 (2021).
Nip, A. S. Y. & Lodish, M. Trend of diabetes-related hospital admissions during the transition period from adolescence to adulthood in the state of California. Diabetes Care. 44, 2723–2728. https://doi.org/10.2337/dc21-0555 (2021).
Sellers, E. A. C. et al. Hospitalization and comorbidity in children with type 2 diabetes. Pediatr. Diabetes. 23, 660–667. https://doi.org/10.1111/pedi.13369 (2022).
Abilbayeva, A. et al. Clinical and laboratory COVID-19 features in hospitalized patients with concomitant diabetes mellitus type 2: A retrospective study. J. Clin. Med. Kaz. 19, 83–88. https://doi.org/10.23950/jcmk/12719 (2022).
Ashirova, M., Abuova, G. & Kamytbekova, K. COVID-19 and diabetes mellitus: clinical and laboratory features in hospitalized patients. J. Clin. Med. Kaz. 20, 14–17. https://doi.org/10.23950/jcmk/12854 (2023).
Befort, C. A., Nazir, N. & Perri, M. G. Prevalence of obesity among adults from rural and urban areas of the united states: findings from NHANES (2005–2008). J. Rural Health. 28, 392–397. https://doi.org/10.1111/j.1748-0361.2012.00411.x (2012).
Flynn, J. T. et al. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics 140, e20171904. https://doi.org/10.1542/peds.2017-1904 (2017).
Donaghue, K. C. et al. ISPAD clinical practice consensus guidelines 2018: microvascular and macrovascular complications in children and adolescents. Pediatr. Diabetes. 19, 262–274. https://doi.org/10.1111/pedi.12742 (2018).
Manov, A. E. et al. Unmasking type 1 diabetes in adults: insights from two cases revealing misdiagnosis as type 2 diabetes, with emphasis on autoimmunity and continuous glucose monitoring. Cureus 15, e42459. https://doi.org/10.7759/cureus.42459 (2023).
Thomas, N. J. et al. Frequency and phenotype of type 1 diabetes in the first six decades of life: a cross-sectional, genetically stratified survival analysis from UK biobank. Lancet Diabetes Endocrinol. 6, 122–129. https://doi.org/10.1016/S2213-8587(17)30362-5 (2018).
Funding
The study was supported by a grant from the Ministry of Science and Higher Education of the Republic of Kazakhstan from 2024 to 2026 (Funder Project Reference: №AP23490341 Kuralay Atageldiyeva is the PI of the project). The funder has no role in study design, data collection and analysis, decision to publish, or manuscript preparation.
Author information
Authors and Affiliations
Contributions
D.S.: Methodology, Software, Formal Analysis, Data Curation, Writing - Original Draft, Writing - Review & Editing, Visualization. K.M.: Software, Validation, Writing - Review & Editing. D.P.: Conceptualization, Validation, Writing - Review & Editing. K.A.: Conceptualization, Validation, Writing - Review & Editing. A.G.: Conceptualization, Data Curation, Supervision. D.G.: Conceptualization, Writing - Review & Editing, Supervision, Project administration, Funding acquisition.
Corresponding author
Ethics declarations
Ethical standards disclosure
Nazarbayev University Institutional Research Ethics Committee (NU-IREC) approved this project to be exempt from further NU IREC oversight (NU-IREC 505/06122021). The need for informed consent was waived by the NU-IREC as the study involved analysis of anonymized secondary data from the Unified National Electronic Health System (UNEHS). The study was performed according to both international and local ethics guidelines and regulations as well as the Declaration of Helsinki.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Atageldiyeva, K., Syssoyev, D., Mussina, K. et al. All-cause hospital admissions and incidence of type 2 diabetes among adolescents in Kazakhstan. Sci Rep 15, 20746 (2025). https://doi.org/10.1038/s41598-025-07451-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-07451-2