Abstract
Background
Patients undergoing bariatric surgery have complex bio-psycho-social needs which require integrated care. This study aimed to evaluate changes of integrated care needs from pre- to one-year post-surgery and to identify baseline variables associated with integrated care needs at follow-up.
Methods
A retrospective cohort study analyzed routinely collected data from a questionnaire-based psychosocial screening conducted prior to evaluation for bariatric surgery and annual follow-up. Integrated care needs were assessed using the INTERMED self-assessment questionnaire (IM-SA), which assesses care needs of four domains (biological, psychological, social, healthcare-related) and identifies patients with case complexity (total score ≥19). Multiple regression analysis examined associations between baseline variables and integrated care needs at follow-up.
Results
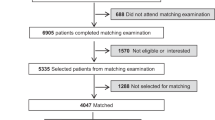
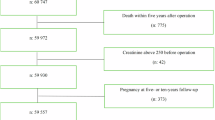
Out of 225 patients who were screened and underwent bariatric surgery between June 2020 and June 2022, 117 provided both pre- and one-year postsurgical data (52%) and thus were included in the study. At one-year post-surgery, integrated care needs were reduced (p < 0.001) and the proportion of patients with case complexity decreased (10.3% vs. 24.8%, p < 0.001). IM-SA scores were reduced in all domains – except the social domain. Sick leave (β = 0.172, p = 0.030) and symptoms of anxiety at baseline (β = 0.235, p = 0.018) were associated with integrated care needs at follow-up.
Conclusions
Bio-psycho-social care needs should be evaluated in pre- and post-bariatric surgery care through a structured assessment, social workers included in the multidisciplinary team, and patients offered psychosocial support prior and after surgery. Rethinking the role and training of social workers is essential, along with developing innovative social interventions extending beyond traditional support.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The data that support the findings of this study are not publicly available due to legal restrictions. For requests regarding data access, contact the corresponding author.
References
Goodwin N. Understanding integrated care. Int J Integr Care. 2016;16:6.
Tortajada S, Giménez-Campos MS, Villar-López J, Faubel-Cava R, Donat-Castelló L, Valdivieso-Martínez B, et al. Case management for patients with complex multimorbidity: development and validation of a coordinated intervention between primary and hospital care. Int J Integr Care. 2017;17:4.
Wild B, Hünnemeyer K, Sauer H, Teufel M. Psychotherapeutische interventionen nach adipositaschirurgie. Psychotherapeut. 2017;62:222–9.
Dawes AJ, Maggard-Gibbons M, Maher AR, Booth MJ, Miake-Lye I, Beroes JM, et al. Mental health conditions among patients seeking and undergoing bariatric surgery: a meta-analysis. JAMA. 2016;315:150–63.
Rotenberg KJ, Bharathi C, Davies H, Finch T. Obesity and the social withdrawal syndrome. Eat Behav. 2017;26:167–70.
Bramming M, Jørgensen MB, Christensen AI, Lau CJ, Egan KK, Tolstrup JS. BMI and labor market participation: a cohort study of transitions between work, unemployment, and sickness absence. Obes. 2019;27:1703–10.
Sharples AJ, Mahawar K. Systematic review and meta-analysis of randomised controlled trials comparing long-term outcomes of Roux-En-Y gastric bypass and sleeve gastrectomy. Obes Surg. 2020;30:664–72.
King WC, Hinerman AS, White GE. A 7-Year study of the durability of improvements in pain, physical function, and work productivity after Roux-en-Y Gastric bypass and sleeve gastrectomy. JAMA Netw Open. 2022;5:e2231593.
Morgan DJR, Ho KM, Platell C. Incidence and determinants of mental health service use after bariatric surgery. JAMA Psychiatry. 2020;77:60–7.
King WC, Chen JY, Courcoulas AP, Dakin GF, Engel SG, Flum DR, et al. Alcohol and other substance use after bariatric surgery: prospective evidence from a U.S. multicenter cohort study. Surg Obes Relat Dis. 2017;13:1392–402.
Sharples AJ, Cheruvu CV. Systematic review and meta-analysis of occupational outcomes after bariatric surgery. Obes Surg. 2017;27:774–81.
Bramming M, Becker U, Jørgensen MB, Neermark S, Bisgaard T, Tolstrup JS. Bariatric surgery and risk of unemployment and sickness absence. Obes Surg. 2022;32:720–8.
Stiefel FC, Huyse FJ, Söllner W, Slaets JP, Lyons JS, Latour CH, et al. Operationalizing integrated care on a clinical level: the INTERMED project. Med Clin North Am. 2006;90:713–58.
Corminboeuf Y, Wild B, Zdrojewski C, Schellberg D, Favre L, Suter M, et al. BMI Course Over 10 Years After bariatric surgery and biopsychosocial complexity assessed with the INTERMED: a retrospective study. Obes Surg. 2021;31:3996–4004.
Boehlen FH, Joos A, Bergmann F, Stiefel F, Eichenlaub J, Ferrari S. et al. Evaluation of the German Version of the “INTERMED-Self-Assessment”-Questionnaire (IM-SA) to Assess Case Complexity. Psychother Psychosom Med Psychol. 2016;66:180–6.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ. 2007;335:806–8.
van Reedt Dortland AKB, Peters LL, Boenink AD, Smit JH, Slaets JPJ, Hoogendoorn AW, et al. Assessment of biopsychosocial complexity and health care needs: measurement properties of the INTERMED self-assessment version. Psychosom Med. 2017;79:485–92.
Hawker GA, Mian S, Kendzerska T, French M. Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP). Arthritis Care Res. 2011;63:S240–52.
Kroenke K, Spitzer RL. The PHQ-9: A new depression diagnostic and severity measure. Psychiatr Ann. 2002;32:509–15.
Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166:1092–7.
Wild B, Eckl A, Herzog W, Niehoff D, Lechner S, Maatouk I, et al. Assessing generalized anxiety disorder in elderly people using the GAD-7 and GAD-2 scales: results of a validation study. Am J Geriatr Psychiatry. 2014;22:1029–38.
Fairburn CG, Beglin SJ. Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord. 1994;16:363–70.
Musella M, Apers J, Rheinwalt K, Ribeiro R, Manno E, Greco F, et al. Efficacy of Bariatric Surgery in Type 2 Diabetes Mellitus Remission: the Role of Mini Gastric Bypass/One Anastomosis Gastric Bypass and Sleeve Gastrectomy at 1 Year of Follow-up. A European survey. Obes Surg. 2016;26:933–40.
Fisher DP, Liu L, Arterburn D, Coleman KJ, Courcoulas A, Haneuse S, et al. Remission and relapse of hypertension after bariatric surgery: a retrospective study on long-term outcomes. Ann Surg Open. 2022;3:e158.
Tolvanen L, Svensson Å, Hemmingsson E, Christenson A, Lagerros YT. Perceived and preferred social support in patients experiencing weight regain after bariatric surgery-a qualitative study. Obes Surg. 2021;31:1256–64.
Livhits M, Mercado C, Yermilov I, Parikh JA, Dutson E, Mehran A, et al. Is social support associated with greater weight loss after bariatric surgery?: A systematic review. Obes Rev. 2011;12:142–8.
Andersen JR, Hernæs UJ, Hufthammer KO, Våge V. Employment status and sick-leave following obesity surgery: a five-year prospective cohort study. PeerJ. 2015;3:e1285.
Giel KE, Thiel A, Teufel M, Mayer J, Zipfel S. Weight bias in work settings - a qualitative review. Obes Facts. 2010;3:33–40.
Zullig LL, Whitson HE, Hastings SN, Beadles C, Kravchenko J, Akushevich I, et al. A systematic review of conceptual frameworks of medical complexity and new model development. J Gen Intern Med. 2016;31:329–37.
Sporinova B, Manns B, Tonelli M, Hemmelgarn B, MacMaster F, Mitchell N, et al. Association of mental health disorders with health care utilization and costs among adults with chronic disease. JAMA Netw Open. 2019;2:e199910.
Horenstein A, Heimberg RG. Anxiety disorders and healthcare utilization: A systematic review. Clin Psychol Rev. 2020;81:101894.
Snyder-Mackler N, Burger JR, Gaydosh L, Belsky DW, Noppert GA, Campos FA, et al. Social determinants of health and survival in humans and other animals. Science. 2020;368:eaax9553.
Author information
Authors and Affiliations
Contributions
BW, CP, UZ, and HCF contributed to the study conception and design. Data collection was performed by UZ. Data analysis was performed by CP and supervised by BW. CP drafted the initial manuscript. All authors critically reviewed, revised, and approved the final manuscript as submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Paul, C., Friederich, HC., Zech, U. et al. Pre-post changes of integrated care needs in patients undergoing bariatric surgery. Int J Obes 49, 1511–1515 (2025). https://doi.org/10.1038/s41366-025-01797-3
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-025-01797-3