Abstract
Background
Diet plays a crucial role in metabolic syndrome (MetS) which might develop into diabetes mellitus and cardiovascular disease.
Objective
We aimed to evaluate the effects of low-carbohydrate diet (LCD) interventions on MetS and its components.
Methods
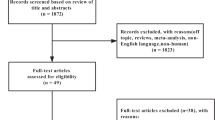
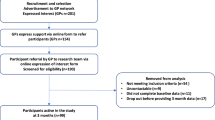
Four electronic databases including PubMed, Embase, Cochrane Central Register of Controlled Trials, and Medline were selected from database inception until March 2024. Randomized clinical trials in adults with MetS evaluated LCD interventions (50–130 g of carbohydrates/day or 10–40% of total dietary energy at 2000 kcal/day) and a control intervention for at least 12 weeks. Four reviewers independently extracted data and assessed risk of bias using Cochrane tool. Meta-analyses used a random-effects model to calculate mean differences (MD) and 95% confidence intervals (CI) and analyzed heterogeneity, sensitivity, and publication bias.
Results
A total of 41 articles satisfied the study’s inclusion criteria. Thirty articles were incorporated in the meta-analysis, of which 25 were high-quality studies and 5 were of moderate quality. In total, 3806 adults were assessed. Pooled analysis of mean differences (MD) indicated that compared to the control dietary intervention, the LCD intervention reduced BMI (MD −0.43 kg/m2, 95% CI −0.75, −0.11), waist circumference (MD −0.77 cm, 95% CI −1.43, −0.12), systolic blood pressure (MD −1.19 mmHg, 95% CI −2.36, −0.02), diastolic blood pressure (MD −1.49 mmHg, 95% CI −2.36, −0.02), HbA1c (MD −0.62%, 95% CI −0.91, −0.32) and triglycerides (MD −0.24 mmol/L, 95% CI −0.42, −0.05), and increased high-density lipoprotein cholesterol (MD 0.06 mmol/l, 95% CI 0.03, 0.09). The subgroup analysis results indicated that the source of high heterogeneity might come from the dosage of intervention.
Conclusion
In summary, LCD interventions improved MetS-related biomarkers in adults with MetS. Moreover, further research is needed to determine the optimal intervention period of LCD on MetS.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Data are available from the corresponding authors upon reasonable request.
References
Grundy SM. Metabolic syndrome pandemic. Arterioscler Thrombosis Vasc Biol. 2008;28:629–36. https://doi.org/10.1161/atvbaha.107.151092.
Saklayen MG. The global epidemic of the metabolic syndrome. Curr Hypertens Rep. 2018;20:12. https://doi.org/10.1007/s11906-018-0812-z.
O’Neill S, O’Driscoll L. Metabolic syndrome: a closer look at the growing epidemic and its associated pathologies. Obes Rev. 2015;16:1–12. https://doi.org/10.1111/obr.12229.
Grundy SM, Brewer HB Jr, Cleeman JI, Smith SC Jr, Lenfant C. Definition of metabolic syndrome: report of the National Heart, Lung, and Blood Institute/American Heart Association conference on scientific issues related to definition. Arterioscler Thrombosis Vasc Biol. 2004;24:e13–8. https://doi.org/10.1161/01.Atv.0000111245.75752.C6.
Isomaa B, Almgren P, Tuomi T, Forsén B, Lahti K, Nissén M, et al. Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diab Care. 2001;24:683–9. https://doi.org/10.2337/diacare.24.4.683.
Lakka HM, Laaksonen DE, Lakka TA, Niskanen LK, Kumpusalo E, Tuomilehto J, et al. The metabolic syndrome and total and cardiovascular disease mortality in middle-aged men. JAMA. 2002;288:2709–16. https://doi.org/10.1001/jama.288.21.2709.
Nupponen M, Pahkala K, Juonala M, Magnussen CG, Niinikoski H, Rönnemaa T, et al. Metabolic syndrome from adolescence to early adulthood: effect of infancy-onset dietary counseling of low saturated fat: the Special Turku Coronary Risk Factor Intervention Project (STRIP). Circulation. 2015;131:605–13. https://doi.org/10.1161/circulationaha.114.010532.
Amirfaiz S, Shahril MR. Objectively measured physical activity, sedentary behavior, and metabolic syndrome in adults: systematic review of observational evidence. Metab Syndr Relat Disord. 2019;17:1–21. https://doi.org/10.1089/met.2018.0032.
Yusuf S, Hawken S, Ounpuu S, Bautista L, Franzosi MG, Commerford P, et al. Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study. Lancet. 2005;366:1640–9. https://doi.org/10.1016/s0140-6736(05)67663-5.
Aude YW, Mego P, Mehta JL. Metabolic syndrome: dietary interventions. Curr Opin Cardiol. 2004;19:473–9. https://doi.org/10.1097/01.hco.0000134610.68815.05.
Pasupulati AK, Reddy GB. Nutrition & metabolic syndrome. Rev Endocr Metab Disord. 2013;14:217. https://doi.org/10.1007/s11154-013-9267-3.
Castro-Barquero S, Ruiz-León AM, Sierra-Pérez M, Estruch R, Casas R. Dietary strategies for metabolic syndrome: a comprehensive review. Nutrients. 2020;12:2983 https://doi.org/10.3390/nu12102983.
Dyson P. Low carbohydrate diets and type 2 diabetes: what is the latest evidence?. Diab Ther. 2015;6:411–24. https://doi.org/10.1007/s13300-015-0136-9.
Ebrahimpour-Koujan S, Shayanfar M, Benisi-Kohansal S, Mohammad-Shirazi M, Sharifi G, Esmaillzadeh A. Adherence to low carbohydrate diet in relation to glioma: a case-control study. Clin Nutr. 2019;38:2690–5. https://doi.org/10.1016/j.clnu.2018.11.023.
Papadaki A, Nolen-Doerr E, Mantzoros CS. The effect of the Mediterranean diet on metabolic health: a systematic review and meta-analysis of controlled trials in adults. Nutrients. 2020;12:3342. https://doi.org/10.3390/nu12113342.
Schwingshackl L, Bogensberger B, Hoffmann G. Diet quality as assessed by the healthy eating index, alternate healthy eating index, dietary approaches to stop hypertension score, and health outcomes: an updated systematic review and meta-analysis of cohort studies. J Acad Nutr Dietetics. 2018;118:74–100.e11. https://doi.org/10.1016/j.jand.2017.08.024.
Liu YS, Wu QJ, Xia Y, Zhang JY, Jiang YT, Chang Q, et al. Carbohydrate intake and risk of metabolic syndrome: a dose-response meta-analysis of observational studies. Nutr Metab Cardiovasc Dis. 2019;29:1288–98. https://doi.org/10.1016/j.numecd.2019.09.003.
Institute of Medicine. Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids. Washington, USA: National Academies Press. 2005.
Joshi S, Shi R, Patel J. Risks of the ketogenic diet in CKD - the con part. Clin Kidney J. 2024;17:sfad274. https://doi.org/10.1093/ckj/sfad274.
O’Neill B, Raggi P. The ketogenic diet: pros and cons. Atherosclerosis. 2020;292:119–26. https://doi.org/10.1016/j.atherosclerosis.2019.11.021.
Barber TM, Hanson P, Kabisch S, Pfeiffer AFH, Weickert MO. The low-carbohydrate diet: short-term metabolic efficacy versus longer-term limitations. Nutrients. 2021;13:1187. https://doi.org/10.3390/nu13041187.
Hashimoto Y, Fukuda T, Oyabu C, Tanaka M, Asano M, Yamazaki M, et al. Impact of low-carbohydrate diet on body composition: meta-analysis of randomized controlled studies. Obes Rev. 2016;17:499–509. https://doi.org/10.1111/obr.12405.
Krejčí H, Vyjídák J, Kohutiar M. Low-carbohydrate diet in diabetes mellitus treatment. Vnitrni Lek. 2018;64:742–52.
Willems AEM, Sura-de JongM, van Beek AP, Nederhof E, van Dijk G. Effects of macronutrient intake in obesity: a meta-analysis of low-carbohydrate and low-fat diets on markers of the metabolic syndrome. Nutr Rev. 2021;79:429–44. https://doi.org/10.1093/nutrit/nuaa044.
Macedo RCO, Santos HO, Tinsley GM, Reischak-Oliveira A. Low-carbohydrate diets: effects on metabolism and exercise - a comprehensive literature review. Clin Nutr ESPEN. 2020;40:17–26. https://doi.org/10.1016/j.clnesp.2020.07.022.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. https://doi.org/10.1136/bmj.n71.
Cumpston M, Li T, Page MJ, Chandler J, Welch VA, Higgins JP, et al. Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev. 2019;10:Ed000142 https://doi.org/10.1002/14651858.Ed000142.
Higgins JPT, Li T, Deeks JJ. Cochrane Handbook for Systematic Reviews of Interventions (2nd ed.). Wiley-Blackwell. Chapter 6: Choosing effect measures and computing estimates of effect. Chichester, UK: Wiley. 2019, pp 143–76.
Higgins JPT, Savović J, Page MJ, Elbers RG, Sterne JAC. Cochrane Handbook for Systematic Reviews of Interventions (2nd ed.). Wiley-Blackwell. Chapter 8: Assessing risk of bias in a randomized trial. Chichester, UK: Wiley. 2019, pp 205–28.
Kanters S. Fixed- and random-effects models. Methods Mol Biol. 2022;2345:41–65. https://doi.org/10.1007/978-1-0716-1566-9_3.
Schünemann HJ, Oxman AD, Vist GE, Higgins JPT, Deeks JJ, Glasziou P et al. Cochrane Handbook for Systematic Reviews of Interventions. Wiley-Blackwell. Chapter 12: Interpreting results and drawing conclusions. Chichester, UK: Wiley. 2008, pp 359–87.
Diabetes UK. (2017). Position statement: Low carb diets for people with diabetes. Diabetes UK. https://www.diabetes.org.uk/professionals/position-statements-reports/food-nutrition-lifestyle/low-carb-diets-for-people-with-diabetes.
Brehm BJ, Seeley RJ, Daniels SR, D’Alessio DA. A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J Clin Endocrinol Metab. 2003;88:1617–23. https://doi.org/10.1210/jc.2002-021480.
Dorans KS, Bazzano LA, Qi L, He H, Chen J, Appel LJ, et al. Effects of a low-carbohydrate dietary intervention on hemoglobin A1c. JAMA Netw Open. 2022;5:e2238645. https://doi.org/10.1001/jamanetworkopen.2022.38645.
Ebbeling CB, Knapp A, Johnson A, Wong JMW, Greco KF, Ma C, et al. Effects of a low-carbohydrate diet on insulin-resistant dyslipoproteinemia—a randomized controlled feeding trial. Am J Clin Nutr. 2022;115:154–162. https://doi.org/10.1093/ajcn/nqab287.
Foraker RE, Pennell M, Sprangers P, Vitolins MZ, DeGraffinreid C, Paskett ED. Effect of a low-fat or low-carbohydrate weight-loss diet on markers of cardiovascular risk among premenopausal women: a randomized trial. J Women’s Health. 2014;23:675–80. https://doi.org/10.1089/jwh.2013.4638.
Volek JS, Ballard KD, Silvestre R, Judelson DA, Quann EE, Forsythe CE, et al. Effects of dietary carbohydrate restriction versus low-fat diet on flow-mediated dilation. Metabolism. 2009;58:1769–77. https://doi.org/10.1016/j.metabol.2009.06.005.
Weber P, Thomsen MN, Skytte MJ, Samkani A, Carl MH, Astrup A, et al. Effects of carbohydrate restriction on body weight and glycemic control in individuals with type 2 diabetes: a randomized controlled trial of efficacy in real-life settings. Nutrients. 2022;14:5244. https://doi.org/10.3390/nu14245244.
Hu T, Yao L, Reynolds K, Whelton PK, Niu T, Li S, et al. The effects of a low-carbohydrate diet vs. a low-fat diet on novel cardiovascular risk factors: a randomized controlled trial. Nutrients. 2015;7:7978–94. https://doi.org/10.3390/nu7095377.
Brinkworth GD, Noakes M, Keogh JB, Luscombe ND, Wittert GA, Clifton PM. Long-term effects of a high-protein, low-carbohydrate diet on weight control and cardiovascular risk markers in obese hyperinsulinemic subjects. Int J Obes. 2004;28:661–70. https://doi.org/10.1038/sj.ijo.0802617.
Keogh JB, Brinkworth GD, Clifton PM. Effects of weight loss on a low-carbohydrate diet on flow-mediated dilatation, adhesion molecules and adiponectin. Br J Nutr. 2007;98:852–9. https://doi.org/10.1017/s0007114507747815.
Liu X, Zhang G, Ye X, Li H, Chen X, Tang L, et al. Effects of a low-carbohydrate diet on weight loss and cardiometabolic profile in Chinese women: a randomised controlled feeding trial. Br J Nutr. 2013;110:1444–53. https://doi.org/10.1017/s0007114513000640.
Watson N, Dyer K, Buckley J, Brinkworth G, Coates A, Parfitt G, et al. Effects of low-fat diets differing in protein and carbohydrate content on cardiometabolic risk factors during weight loss and weight maintenance in obese adults with type 2 diabetes. Nutrients. 2016;8:289. https://doi.org/10.3390/nu8050289.
Wycherley TP, Thompson CH, Buckley JD, Luscombe-Marsh ND, Noakes M, Wittert GA, et al. Long-term effects of weight loss with a very-low carbohydrate, low saturated fat diet on flow mediated dilatation in patients with type 2 diabetes: a randomised controlled trial. Atherosclerosis. 2016;252:28–31. https://doi.org/10.1016/j.atherosclerosis.2016.07.908.
Dening J, Mohebbi M, Abbott G, George ES, Ball K, Islam SMS. A web-based low carbohydrate diet intervention significantly improves glycaemic control in adults with type 2 diabetes: results of the T2Diet Study randomised controlled trial. Nutr Diab. 2023;13:12. https://doi.org/10.1038/s41387-023-00240-8.
Lean ME, Han TS, Prvan T, Richmond PR, Avenell A. Weight loss with high and low carbohydrate 1200 kcal diets in free living women. Eur J Clin Nutr. 1997;51:243–8. https://doi.org/10.1038/sj.ejcn.1600391.
Daly ME, Paisey R, Paisey R, Millward BA, Eccles C, Williams K, et al. Short-term effects of severe dietary carbohydrate-restriction advice in Type 2 diabetes-a randomized controlled trial. Diabet Med. 2006;23:15–20. https://doi.org/10.1111/j.1464-5491.2005.01760.x.
Morris E, Aveyard P, Dyson P, Noreik M, Bailey C, Fox R, et al. A food-based, low-energy, low-carbohydrate diet for people with type 2 diabetes in primary care: a randomized controlled feasibility trial. Diab Obes Metab. 2020;22:512–20. https://doi.org/10.1111/dom.13915.
Rolland C, Hession M, Murray S, Wise A, Broom I. Randomized clinical trial of standard dietary treatment versus a low-carbohydrate/high-protein diet or the LighterLife Programme in the management of obesity*. J Diab. 2009;1:207–17. https://doi.org/10.1111/j.1753-0407.2009.00033.x.
Hockaday TD, Hockaday JM, Mann JI, Turner RC. Prospective comparison of modified fat-high-carbohydrate with standard low-carbohydrate dietary advice in the treatment of diabetes: one year follow-up study. Br J Nutr. 1978;39:357–62. https://doi.org/10.1079/bjn19780045.
Barengolts E, Chen C-Y, Huang W-S, Chen H-C, Chang C-H, Lee L-T, et al. Effect of a 90 g/day low-carbohydrate diet on glycaemic control, small, dense low-density lipoprotein and carotid intima-media thickness in type 2 diabetic patients: an 18-month randomised controlled trial. Plos One. 2020;15:e0240158. https://doi.org/10.1371/journal.pone.0240158.
Han Y, Cheng B, Guo Y, Wang Q, Yang N, Lin P. A low-carbohydrate diet realizes medication withdrawal: a possible opportunity for effective glycemic control. Front Endocrinol. 2021;12:779636. https://doi.org/10.3389/fendo.2021.779636.
Wang L-L, Wang Q, Hong Y, Ojo O, Jiang Q, Hou Y-Y, et al. The effect of low-carbohydrate diet on glycemic control in patients with type 2 diabetes mellitus. Nutrients. 2018;10:661. https://doi.org/10.3390/nu10060661.
Chen CY, Huang WS, Ho MH, Chang CH, Lee LT, Chen HS, et al. The potential prolonged effect at one-year follow-up after 18-month randomized controlled trial of a 90 g/day low-carbohydrate diet in patients with type 2 diabetes. Nutr Diab. 2022;12:17 https://doi.org/10.1038/s41387-022-00193-4.
Yamada Y, Uchida J, Izumi H, Tsukamoto Y, Inoue G, Watanabe Y, et al. A non-calorie-restricted low-carbohydrate diet is effective as an alternative therapy for patients with type 2 diabetes. Intern Med. 2014;53:13–19. https://doi.org/10.2169/internalmedicine.53.0861.
Atkin SL, Sato J, Kanazawa A, Hatae C, Makita S, Komiya K, et al. One year follow-up after a randomized controlled trial of a 130 g/day low-carbohydrate diet in patients with type 2 diabetes mellitus and poor glycemic control. Plos One. 2017;12:e0188892. https://doi.org/10.1371/journal.pone.0188892.
Sato J, Kanazawa A, Makita S, Hatae C, Komiya K, Shimizu T, et al. A randomized controlled trial of 130 g/day low-carbohydrate diet in type 2 diabetes with poor glycemic control. Clin Nutr. 2017;36:992–1000. https://doi.org/10.1016/j.clnu.2016.07.003.
Izaola O, Primo D, Gomez Hoyos E, Lopez Gomez JJ, Ortola A, de Luis D. Association of rs670 variant of APOA1 gene with lipid profile and insulin resistance after 9 months of a high protein/low carbohydrate vs a standard hypocaloric diet. Clin Nutr. 2020;39:988–93. https://doi.org/10.1016/j.clnu.2019.04.030.
de Luis DA, Aller R, Izaola O, Romero E. Effects of a high-protein/low-carbohydrate versus a standard hypocaloric diet on adipocytokine levels and cardiovascular risk factors during 9 months, role of rs6923761 gene variant of glucagon-like peptide 1 receptor. J Endocrinological Investig. 2015;38:1183–9. https://doi.org/10.1007/s40618-015-0304-9.
de Luis DA, Aller R, Izaola O, Gonzalez Sagrado M, Bellioo D, Conde R. Effects of a low-fat versus a low-carbohydrate diet on adipocytokines in obese adults. Horm Res Paediatrics. 2007;67:296–300. https://doi.org/10.1159/000099329.
Jenkins DJA, Wong JMW, Kendall CWC, Esfahani A, Ng VWY, Leong TCK, et al. Effect of a 6-month vegan low-carbohydrate (‘Eco-Atkins’) diet on cardiovascular risk factors and body weight in hyperlipidaemic adults: a randomised controlled trial. BMJ Open. 2014;4:e003505. https://doi.org/10.1136/bmjopen-2013-003505.
Oliveira BF, Chang CR, Oetsch K, Falkenhain K, Crampton K, Stork M, et al. Impact of a low-carbohydrate compared with low-fat breakfast on blood glucose control in type 2 diabetes: a randomized trial. Am J Clin Nutr. 2023;118:209–17. https://doi.org/10.1016/j.ajcnut.2023.04.032.
Frisch S, Zittermann A, Berthold HK, Götting C, Kuhn J, Kleesiek K, et al. A randomized controlled trial on the efficacy of carbohydrate-reduced or fat-reduced diets in patients attending a telemedically guided weight loss program. Cardiovasc Diabetol. 2009;8:36. https://doi.org/10.1186/1475-2840-8-36.
Haufe S, Engeli S, Kast P, Böhnke J, Utz W, Haas V, et al. Randomized comparison of reduced fat and reduced carbohydrate hypocaloric diets on intrahepatic fat in overweight and obese human subjects. Hepatology. 2011;53:1504–14. https://doi.org/10.1002/hep.24242.
Jonasson L, Guldbrand H, Lundberg AK, Nystrom FH. Advice to follow a low-carbohydrate diet has a favourable impact on low-grade inflammation in type 2 diabetes compared with advice to follow a low-fat diet. Ann Med. 2014;46:182–7. https://doi.org/10.3109/07853890.2014.894286.
Goldenberg JZ, Day A, Brinkworth GD, Sato J, Yamada S, Jönsson T, et al. Efficacy and safety of low and very low carbohydrate diets for type 2 diabetes remission: systematic review and meta-analysis of published and unpublished randomized trial data. BMJ. 2021;372:m4743. https://doi.org/10.1136/bmj.m4743.
Al-Sarraj T, Saadi H, Calle MC, Volek JS, Fernandez ML. Carbohydrate restriction, as a first-line dietary intervention, effectively reduces biomarkers of metabolic syndrome in Emirati adults. J Nutr. 2009;139:1667–76. https://doi.org/10.3945/jn.109.109603.
Al-Sarraj T, Saadi H, Volek JS, Fernandez ML. Carbohydrate restriction favorably alters lipoprotein metabolism in Emirati subjects classified with the metabolic syndrome. Nutr Metab Cardiovasc Dis. 2010;20:720–6. https://doi.org/10.1016/j.numecd.2009.06.004.
Hansen CD, Gram-Kampmann E-M, Hansen JK, Hugger MB, Madsen BS, Jensen JM, et al. Effect of calorie-unrestricted low-carbohydrate, high-fat diet versus high-carbohydrate, low-fat diet on type 2 diabetes and nonalcoholic fatty liver disease. Ann Intern Med. 2023;176:10–21. https://doi.org/10.7326/m22-1787.
Wrzosek M, Woźniak J, Włodarek D. The effect of high-fat versus high-carb diet on body composition in strength-trained males. Food Sci Nutr. 2021;9:2541–8. https://doi.org/10.1002/fsn3.2204.
Currenti W, Losavio F, Quiete S, Alanazi AM, Messina G, Polito R, et al. Comparative evaluation of a low-carbohydrate diet and a mediterranean diet in overweight/obese patients with type 2 diabetes mellitus: a 16-week intervention study. Nutrients. 2023;16:95. https://doi.org/10.3390/nu16010095.
Klemsdal TO, Holme I, Nerland H, Pedersen TR, Tonstad S. Effects of a low glycemic load diet versus a low-fat diet in subjects with and without the metabolic syndrome. Nutr Metab Cardiovasc Dis. 2010;20:195–201. https://doi.org/10.1016/j.numecd.2009.03.010.
Larsen RN, Mann NJ, Maclean E, Shaw JE. The effect of high-protein, low-carbohydrate diets in the treatment of type 2 diabetes: a 12 month randomised controlled trial. Diabetologia. 2011;54:731–40. https://doi.org/10.1007/s00125-010-2027-y.
Guldbrand H, Dizdar B, Bunjaku B, Lindström T, Bachrach-Lindström M, Fredrikson M, et al. In type 2 diabetes, randomisation to advice to follow a low-carbohydrate diet transiently improves glycaemic control compared with advice to follow a low-fat diet producing a similar weight loss. Diabetologia. 2012;55:2118–27. https://doi.org/10.1007/s00125-012-2567-4.
Apekey TA, Maynard MJ, Kittana M, Kunutsor SK. Comparison of the effectiveness of low carbohydrate versus low fat diets, in type 2 diabetes: systematic review and meta-analysis of randomized controlled trials. Nutrients. 2022;14:4391. https://doi.org/10.3390/nu14204391.
Jooste BR, Kolivas D, Brukner P, Moschonis G. Effectiveness of technology-enabled, low carbohydrate dietary interventions, in the prevention or treatment of type 2 diabetes mellitus in adults: a systematic literature review of randomised controlled and non-randomised trials. Nutrients. 2023;15:4362. https://doi.org/10.3390/nu15204362.
Li S, Ding L, Xiao X. Comparing the efficacy and safety of low-carbohydrate diets with low-fat diets for type 2 diabetes mellitus patients: a systematic review and meta-analysis of randomized clinical trials. Int J Endocrinol. 2021;2021:8521756. https://doi.org/10.1155/2021/8521756.
Lei L, Huang J, Zhang L, Hong Y, Hui S, Yang J. Effects of low-carbohydrate diets versus low-fat diets on metabolic risk factors in overweight and obese adults: a meta-analysis of randomized controlled trials. Front Nutr. 2022;9:935234. https://doi.org/10.3389/fnut.2022.935234.
Alexandraki I, Palacio C, Mooradian AD. Relative merits of low-carbohydrate versus low-fat diet in managing obesity. South Med J. 2015;108:401–16. https://doi.org/10.14423/smj.0000000000000308.
Foley PJ. Effect of low carbohydrate diets on insulin resistance and the metabolic syndrome. Curr Opin Endocrinol Diab Obes. 2021;28:463–8. https://doi.org/10.1097/med.0000000000000659.
Meng Y, Bai H, Wang S, Li Z, Wang Q, Chen L. Efficacy of low carbohydrate diet for type 2 diabetes mellitus management: a systematic review and meta-analysis of randomized controlled trials. Diab Res Clin Pract. 2017;131:124–31. https://doi.org/10.1016/j.diabres.2017.07.006.
Salehi-Abargouei A, Maghsoudi Z, Shirani F, Azadbakht L. Effects of Dietary Approaches to Stop Hypertension (DASH)-style diet on fatal or nonfatal cardiovascular diseases-incidence: a systematic review and meta-analysis on observational prospective studies. Nutrition. 2013;29:611–8. https://doi.org/10.1016/j.nut.2012.12.018.
Author information
Authors and Affiliations
Contributions
JXZ and QZ designed and finalized the topic of this meta-analysis. JXZ, QZ, XG, SJC, ZCY and DL helped write the manuscript. QZ, XR, RTW, and LJZ screened the articles, XG intervened to resolve disputes. QZ, XR, RTW, and LJZ completed the study quality scores. XCP meta-analyzed the data. All authors contributed to the article and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zheng, Q., Gao, X., Ruan, X. et al. Are low carbohydrate diet interventions beneficial for metabolic syndrome and its components? A systematic review and meta-analysis of randomized controlled trials. Int J Obes 49, 1252–1263 (2025). https://doi.org/10.1038/s41366-025-01822-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-025-01822-5