Abstract
Objective
International Classification of Diseases (ICD) codes in electronic health records (EHRs) are increasingly used for health services research, in spite of unknown diagnostic accuracy. The accuracy of ICD codes to identify bronchopulmonary dysplasia (BPD) is unknown.
Study design
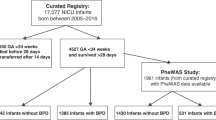
Retrospective cohort study in a single-center NICU (n = 166) to evaluate sensitivity and specificity of ICD-10 codes for the diagnosis of BPD. Analysis of large insurance claims database (n = 7887) to determine date of assignment of the code.
Results
The sensitivity of any BPD-related ICD codes ranged from 0.82 to 0.95, while the specificity ranged from 0.25 to 0.36. In a large national insurance database, the most common date of ICD-9 or ICD-10 code assignment was the day of birth, which is inconsistent with the clinical definition.
Conclusions
ICD codes registered for BPD are unlikely to accurately reflect the current clinical definition and should be interpreted with caution.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Ducharme R, Benchimol EI, Deeks SL, Hawken S, Fergusson DA, Wilson K. Validation of diagnostic codes for intussusception and quantification of childhood intussusception incidence in Ontario, Canada: a population-based study. J Pediatr. 2013. https://doi.org/10.1016/j.jpeds.2013.05.034.
Myers RP, Leung Y, Shahee AAM, Li B. Validation of ICD-9-CM/ICD-10 coding algorithms for the identification of patients with acetaminophen overdose and hepatotoxicity using administrative data. BMC Health Serv Res. 2007;7:159.
Fleet JL, Dixon SN, Shariff SZ, Quinn RR, Nash DM, Harel Z, et al. Detecting chronic kidney disease in population-based administrative databases using an algorithm of hospital encounter and physician claim codes. BMC Nephrol. 2013. https://doi.org/10.1186/1471-2369-14-81.
Thygesen SK, Christiansen CF, Christensen S, Lash TL, Sørensen HT. The predictive value of ICD-10 diagnostic coding used to assess Charlson comorbidity index conditions in the population-based Danish National Registry of Patients. BMC Med Res Methodol. 2011. https://doi.org/10.1186/1471-2288-11-83.
National Center for Health Statistics. Public health transition to ICD-10-CM/PCS. Classification of dieseases, functioning, and disability. National Center for Health Statistics. 2015. https://www.cdc.gov/nchs/icd/icd10cm_pcs.htm.
Beam AL, Fried I, Palmer N, Agniel D, Brat G, Fox K, et al. Estimates of healthcare spending for preterm and low-birthweight infants in a commercially insured population: 2008-2016. J Perinatol. 2020;40:1091–9. https://doi.org/10.1038/s41372-020-0635-z.
Fried I, Beam AL, Kohane IS, Palmer NP. Utilization, cost, and outcome of branded vs compounded 17-alpha hydroxyprogesterone caproate in prevention of preterm birth. JAMA Intern Med. 2017. https://doi.org/10.1001/jamainternmed.2017.5017.
Grosse SD, Waitzman NJ, Yang N, Abe K, Barfield WD. Employer-sponsored plan expenditures for infants orn preterm. Pediatrics. 2017. https://doi.org/10.1542/peds.2017-1078.
Juhl SM, Hansen ML, Fonnest G, Gormsen M, Lambæk ID, Greisen G. Poor validity of the routine diagnosis of necrotising enterocolitis in preterm infants at discharge. Acta Paediatr. 2017. https://doi.org/10.1111/apa.13541.
Agniel D, Kohane IS, Weber GM. Biases in electronic health record data due to processes within the healthcare system: retrospective observational study. BMJ. 2018. https://doi.org/10.1136/bmj.k1479.
Pallatto E, Hunt P, Reber K, Evans J, Padula M. Topics in neonatal informatics: standardizing diagnoses in neonatology: bronchopulmonary dysplasia and beyond. Neoreviews. 2012;13:e577–82.
Beam AL, Kohane IS. Big data and machine learning in health care. JAMA. 2018;319:1317 https://doi.org/10.1001/jama.2017.18391.
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook A, Walsh M, et al. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics. 2010;126:443–56. https://doi.org/10.1542/peds.2009-2959.
Lapcharoensap W, Lee HC, Nyberg A, Dukhovny D. Health care and societal costs of bronchopulmonary dysplasia. Neoreviews. 2018. https://doi.org/10.1542/neo.19-4-e211.
Lefkowitz W, Rosenberg SH. Bronchopulmonary dysplasia: pathway from disease to long-term outcome. J Perinatol. 2008. https://doi.org/10.1038/jp.2008.110.
Parad RB, Davis JM, Lo J, Thomas M, Marlow N, Calvert S, et al. Prediction of respiratory outcome in extremely low gestational age infants. Neonatology. 2015. https://doi.org/10.1159/000369878.
Northway WH, Rosan RC, Porter DY. Pulmonary disease following respirator therapy of hyaline-membrane disease. Bronchopulmonary dysplasia. N Engl J Med. 1967. https://doi.org/10.1056/NEJM196702162760701.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat N, Keszler M, et al. The diagnosis of bronchopulmonary dysplasia in very preterm infants. an evidence-based approach. Am J Respir Crit Care Med. 2019;200:751–9. https://doi.org/10.1164/rccm.201812-2348OC.
Beam KS, Aliaga S, Ahlfeld SK, Cohen-Wolkowiez M, Smith PB, Laughon MM. A systematic review of randomized controlled trials for the prevention of bronchopulmonary dysplasia in infants. J Perinatol. 2014;34:705–10.
Higgins RD, Jobe AH, Koso-Thomas M, Bancalari E, Viscardi R, Hartert T, et al. Bronchopulmonary dysplasia: executive summary of a workshop. J Pediatr. 2018. https://doi.org/10.1016/j.jpeds.2018.01.043.
Member Map and Member List. Vermont Oxford Network, 1 January 2019. https://public.vtoxford.org/member-map/.
R Core Team. R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2020.
Ehrenkranz RA. Validation of the National Institutes of Health Consensus definition of bronchopulmonary dysplasia. Pediatrics. 2005;116:1353–60. https://doi.org/10.1542/peds.2005-0249.
Quan H, Li B, Duncan Saunders L, Parson G, Nillson C, Alibhai A, et al. Assessing validity of ICD-9-CM and ICD-10 administrative data in recording clinical conditions in a unique dually coded database. Health Serv Res. 2008. https://doi.org/10.1111/j.1475-6773.2007.00822.x.
Reeves SL, Madden B, Wu M, Miller L, Anders D, Caggana M, et al. Performance of ICD-10-CM diagnosis codes for identifying children with Sickle Cell Anemia. Health Serv Res. 2020. https://doi.org/10.1111/1475-6773.13257.
Landry JS, Croitoru D, Menzies D. Validation of ICD-9 diagnostic codes for bronchopulmonary dysplasia in Quebec’s provincial health care databases. Chronic Dis Inj Can. 2012;33:47–52.
O’Malley KJ, Cook KF, Price MD, Wildes KR, Hurdle JF, Ashton CM. Measuring diagnoses: ICD code accuracy. Health Serv Res. 2005. https://doi.org/10.1111/j.1475-6773.2005.00444.x.
Acknowledgements
The authors wish to thank Dr. Kathe Fox and Dr. John Zupancic for their helpful comments on a draft of this manuscript.
Funding
KSB was supported by AHRQ grant number T32HS000063 as part of the Harvard-wide Pediatric Health Services Research Fellowship Program. AB was supported by a grant from the NIH NHLBI (award #: 7K01HL141771–02).
Author information
Authors and Affiliations
Contributions
KSB conceived of the project, analyzed the single-institution data, performed chart review, and contributed to the drafting of the manuscript. ML analyzed the insurance data and contributed to the drafting of the manuscript. KH created the single-institution cohort and collected the respiratory data. AB conceived of the project, provided input on the statistical analysis, and helped draft the manuscript. RBP conceived of the project and contributed the drafting of the manuscript
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Beam, K.S., Lee, M., Hirst, K. et al. Specificity of International Classification of Diseases codes for bronchopulmonary dysplasia: an investigation using electronic health record data and a large insurance database. J Perinatol 41, 764–771 (2021). https://doi.org/10.1038/s41372-021-00965-3
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-021-00965-3
This article is cited by
-
International classification of diseases codes have low positive predictive value for neonatal morbidities
Journal of Perinatology (2025)
-
Artificial intelligence in the neonatal intensive care unit: the time is now
Journal of Perinatology (2024)
-
The validity of hospital diagnostic and procedure codes reflecting morbidity in preterm neonates born <32 weeks gestation
Journal of Perinatology (2023)
-
Definitions of necrotizing enterocolitis: What are we defining and is machine learning the answer?
Pediatric Research (2022)