Abstract
Objectives
The objective of this study is to identify the populations at greatest risk for COVID-19 complications during pregnancy and determine their adverse maternal and neonatal outcomes in a time period prior to vaccine availability.
Study design
Cohort study using delivery hospitalization discharge data linked to vital records for all births in California during the baseline pre-COVID-19 period and for all births during the COVID-19 Study period.
Results
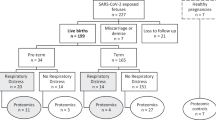
Among 344,894 deliveries, a total of 7181 (2.08%) hospitalized patients tested positive for COVID-19 during pregnancy. Of these, 571 (0.17%) patients were hospitalized with severe respiratory illness. Rate of severe maternal morbidity (242/571, 42%) and maternal death (10/571, 1.8%) were markedly elevated in those hospitalized patients with COVID-19 related respiratory disease compared to both uninfected parturients and infected parturients with less severe disease. Higher rates of COVID-19 related respiratory conditions were associated with Hispanic ethnicity, Native American race, state-funded insurance, and lower education levels.
Conclusion
In pregnancies complicated by COVID-19, the excess risks of maternal mortality, SMM, and adverse neonatal outcomes were restricted to the patients with COVID-19 related respiratory conditions. Significant disparities were noted for respiratory conditions, mortality and SMM related to race-ethnicity and socioeconomic status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Metz TD, Clifton RG, Hughes BL, Sandoval GJ, Grobman WA, Saade GR, et al. Disease severity and perinatal outcomes of pregnant patients with coronavirus disease 2019 (COVID-19). Obstet Gynecol. 2021;137:571–80. https://doi.org/10.1097/AOG.0000000000004339.
Metz TD, Collier C, Hollier LM. Maternal mortality from coronavirus disease 2019 (COVID-19) in the United States. Obstet Gynecol. 2020;136:313–6. https://doi.org/10.1097/AOG.0000000000004024.
Zambrano LD, Ellington S, Strid P, Galang RR, Oduyebo T, Tong VT, et al. Update: characteristics of symptomatic women of reproductive age with laboratory-confirmed SARS-CoV-2 infection by pregnancy status—United States, January 22–October 3, 2020. Morb Mortal Wkly Rep. 2020;69:1641–7. https://doi.org/10.15585/mmwr.mm6944e3.
Yan J, Guo J, Fan C, Juan J, Yu X, Li J, et al. Coronavirus disease 2019 in pregnant women: a report based on 116 cases. Am J Obstet Gynecol. 2020;223:111.e1–111.e14. https://doi.org/10.1016/j.ajog.2020.04.014.
Blitz MJ, Rochelson B, Minkoff H, Meirowitz NB, Prasannan L, London V, et al. Maternal mortality among women with coronavirus disease 2019 admitted to the intensive care unit. Am J Obstet Gynecol. 2020. https://doi.org/10.1016/j.ajog.2020.06.020.
Knight M, Bunch K, Vousden N, Morris E, Simpson N, Gale C, et al. Characteristics and outcomes of pregnant women admitted to hospital with confirmed SARS-CoV-2 infection in UK: national population-based cohort study. BMJ. 2020;369:m2107 https://doi.org/10.1136/bmj.m2107.
Ellington S, Strid P, Tong VT, Woodworth K, Galang RR, Zambrano LD, et al. Characteristics of women of reproductive age with laboratory-confirmed SARS-CoV-2 infection by pregnancy status—United States, January 22–June 7, 2020. Morb Mortal Wkly Rep. 2020;69:769–75. https://doi.org/10.15585/mmwr.mm6925a1.
Kim CNH, Hutcheon J, van Schalkwyk J, Marquette GP, Brown H, Money D, et al. Maternal outcome of pregnant women admitted to intensive care units for COVID-19. Am J Obstet Gynecol. 2020. https://doi.org/10.1016/j.ajog.2020.08.002.
Lokken EM, Taylor GG, Huebner EM, Vanderhoeven J, Hendrickson S, Coler B, et al. Higher severe acute respiratory syndrome coronavirus 2 infection rate in pregnant patients. Am J Obstet Gynecol. 2021;225:75.e1–75.e16. https://doi.org/10.1016/j.ajog.2021.02.011.
Hudak ML, Flannery DD, Barnette K, Getzlaff T, Gautam S, Dhudasia MB, et al. Maternal and newborn hospital outcomes of perinatal SARS-CoV-2 infection: a national registry. Pediatrics. 2023;151:e2022059595. https://doi.org/10.1542/peds.2022-059595.
Mullins E, Perry A, Banerjee J, Townson J, Grozeva D, Milton R, et al. Pregnancy and neonatal outcomes of COVID-19: the PAN-COVID study. Eur J Obstet Gynecol Reprod Biol. 2022;276:161–7. https://doi.org/10.1016/j.ejogrb.2022.07.010.
Villar J, Ariff S, Gunier RB, Thiruvengadam R, Rauch S, Kholin A, et al. Maternal and neonatal morbidity and mortality among pregnant women with and without COVID-19 infection: the INTERCOVID multinational cohort study. JAMA Pediatr. 2021;175:817–26. https://doi.org/10.1001/jamapediatrics.2021.1050.
Centers for Disease Control and Prevention. COVID data tracker: data on COVID-19 during pregnancy: birth and infant outcomes. 2021. https://covid.cdc.gov/covid-data-tracker/#pregnant-birth-infant.
Galang RR, Newton SM, Woodworth KR, Griffin I, Oduyebo T, Santharam V, et al. Risk factors for illness severity among pregnant women with confirmed SARS-CoV-2 infection—Surveillance for Emerging Threats to Mothers and Babies Network, 22 state, local, and territorial health departments, 29 March 2020–5 March 2021. Clin Infect Dis. 2021;73:S17–S23. https://doi.org/10.1093/cid/ciab432.
Metz TD, Clifton RG, Hughes BL, Sandoval GJ, Grobman WA, Saade GR, et al. Association of SARS-CoV-2 infection with serious maternal morbidity and mortality from obstetric complications. JAMA. 2022;327:748–59. https://doi.org/10.1001/jama.2022.1190.
Beate D. Probabilistic record linkages for generating a comprehensive epidemiological research file on maternal and infant health. 2002. http://www.health-info-solutions.com/Probabilistic%20Record%20Linkages%20may%202002.pdf
COVID-19 Treatment Guidelines Panel. Coronavirus disease 2019 (COVID-19) treatment guidelines. National Institutes of Health. 2021. https://www.covid19treatmentguidelines.nih.gov/.
Centers for Disease Control and Prevention. Severe maternal morbidity indicators and corresponding ICD codes during delivery hospitalizations. 2021. https://www.cdc.gov/reproductivehealth/maternalinfanthealth/smm/severe-morbidity-ICD.htm.
The Joint Commission. Measure PC-06.1 (NQF 716). 2018. https://manual.jointcommission.org/releases/TJC2018B/MIF0393.html.
Zhao K Proper estimation of relative risk using PROC GENMOD in population studies. In: Proceedings of the SAS Global Forum 2013 Conference. Cary, NC: SAS Institute Inc.
Leonard SA, Kennedy CJ, Carmichael SL, Main EK. An expanded obstetric comorbidity scoring system for predicting severe maternal morbidity. Obstet Gynecol. 2020;136:440–9.
Ko JY, DeSisto CL, Simeone RM, Ellington S, Galang RR, Oduyebo T, et al. Adverse pregnancy outcomes, maternal complications, and severe illness among US delivery hospitalizations with and without a coronavirus disease 2019 (COVID-19) diagnosis. Clin Infect Dis. 2021;73:S24–S31. https://doi.org/10.1093/cid/ciab344.
Jering KS, Claggett BL, Cunningham JW, Rosenthal N, Vardeny O, Greene MF, et al. Clinical characteristics and outcomes of hospitalized women giving birth with and without COVID-19. JAMA Intern Med. 2021;181:714–7. https://doi.org/10.1001/jamainternmed.2020.9241.
Macias Gil R, Marcelin JR, Zuniga-Blanco B, Marquez C, Mathew T, Piggott DA. COVID-19 pandemic: disparate health impact on the Hispanic/Latinx population in the United States. J Infect Dis. 2020;222:1592–5. https://doi.org/10.1093/infdis/jiaa474.
Velasco-Huerta F, Ramirez EG, Payén SS, Alvarez A, Ottosen MJ, Hernandez DC. Social determinants of health and Latinx families, risk for COVID-19 infection. Fam Community Health. 2021;44:99–101. https://doi.org/10.1097/FCH.0000000000000289.
Main EK, Chang SC, Carpenter AM, Wise PH, Stevenson DK, Shaw GM. Singleton preterm birth rates for racial and ethnic groups during the coronavirus disease 2019 pandemic in California. Am J Obstet Gynecol. 2021;224:239–41.
Centers for Disease Control and Prevention. COVID-19 vaccination among pregnant people aged 18–49 years by race/ethnicity and date reported—Vaccine Safety Datalink, United States. 2025. https://www.cdc.gov.
Razzaghi H, Meghani M, Pingali C, Crane BE, Naleway AL, Weintraub E, et al. COVID-19 vaccination coverage among pregnant women during pregnancy—eight integrated health care organizations, United States, December 14, 2020–May 8, 2021. Morb Mortal Wkly Rep. 2021;70:895–9. https://doi.org/10.15585/mmwr.mm7024e2.
Brillo E, Tosto V, Gerli S, Laganà AS, Vitale SG, Zullo F, et al. COVID-19 vaccination in pregnancy and postpartum. J Matern Fetal Neonatal Med. 2021:1–21. https://doi.org/10.1080/14767058.2021.1937991.
Adhikari EH, SoRelle JA, McIntire DD, Spong CY. Increasing severity of COVID-19 in pregnancy with Delta (B.1.617.2) variant surge. Am J Obstet Gynecol. 2021. https://doi.org/10.1016/j.ajog.2021.09.008.
Yao R, Martin CB, Haase VS. Initial clinical characteristics of gravid severe acute respiratory syndrome coronavirus 2-positive patients and the risk of progression to severe coronavirus disease 2019. Am J Obstet Gynecol MFM. 2021;3:100365. https://doi.org/10.1016/j.ajogmf.2021.100365.
Author information
Authors and Affiliations
Contributions
CM conceptualized and led the study, contributed to study design, interpreted results, and drafted the manuscript. S-CC contributed to study design, performed statistical analyses, and critically revised the manuscript. CS assisted with data acquisition and manuscript drafting. NA contributed to interpretation of findings and manuscript review. JG provided methodological guidance and editorial input. DS contributed to study conceptualization and critical manuscript review. EM oversaw the project, advised on study design and data interpretation, and reviewed the manuscript for final approval. All authors reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
All methods were performed in accordance with relevant guidelines and regulations. Ethics approval was obtained from Stanford University Institutional Review Board and the California Committee for the Protection of Human Subjects (CPHS) for the use of linked administrative and vital records data. This study used de-identified data. Informed consent from individual participants was not required or applicable. No identifiable images or personal identifiers are included in this publication.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Martin, C.B., Chang, SC., Sakowski, C. et al. Impact of COVID-19 respiratory conditions on pregnancy outcomes in California. J Perinatol (2026). https://doi.org/10.1038/s41372-025-02550-4
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-025-02550-4