Abstract
Pulmonary lymphoid malignancies comprise various entities, 80% of them are pulmonary marginal zone B-cell lymphomas (PMZL). So far, little is known about point mutations in primary pulmonary lymphomas. We characterized the genetic landscape of primary pulmonary lymphomas using a customized high-throughput sequencing gene panel covering 146 genes. Our cohort consisted of 28 PMZL, 14 primary diffuse large B-cell lymphomas (DLBCL) of the lung, 7 lymphomatoid granulomatoses (LyG), 5 mature small B-cell lymphomas and 16 cases of reactive lymphoid lesions. Mutations were detected in 22/28 evaluable PMZL (median 2 mutation/case); 14/14 DLBCL (median 3 mutations/case) and 4/7 LyG (1 mutation/case). PMZL showed higher prevalence for mutations in chromatin modifier-encoding genes (44% of mutant genes), while mutations in genes related to the NF-κB pathway were less common (24% of observed mutations). There was little overlap between mutations in PMZL and DLBCL. MALT1 rearrangements were more prevalent in PMZL than BCL10 aberrations, and both were absent in DLBCL. LyG were devoid of gene mutations associated with immune escape. The mutational landscape of PMZL differs from that of extranodal MZL of other locations and also from splenic MZL. Their landscape resembles more that of nodal MZL, which also show a predominance of mutations of chromatin modifiers. The different mutational composition of pulmonary DLBCL compared to PMZL suggests that the former probably do not present transformations. DLBCL bear more mutations/case and immune escape gene mutations compared to LyG, suggesting that EBV infection in LyG may substitute for mutations.
Similar content being viewed by others
Introduction
Primary lymphomas of the lung are very rare, accounting for only 0.4% of all lymphomas [1]. Pulmonary marginal zone lymphoma (PMZL), derived from bronchus-mucosa associated lymphatic tissue (BALT/MALT), is the most common type (80% of cases), followed by diffuse large B-cell lymphoma (DLBCL) and lymphomatoid granulomatosis (LyG), an Epstein-Barr virus (EBV)-related disorder [2].
PMZL belongs to the group of extranodal marginal zone lymphomas (EMZL). These EMZL are thought to originate from post-germinal center B-cells, which are located in the external part of secondary follicles, in the so-called marginal zone [2, 3]. PMZL presents mostly in the sixth decade of life without sex predilection. In more than half of the cases, it is an incidental finding and patients do not show any symptoms of lymphoma involvement; however, up to 15% of patients suffer from concurrent autoimmune diseases [4]. Generalized disease involving other organs or the bone marrow is seen in about 25% of PMZL patients [5].
EMZL occur most frequently in the stomach (70%), followed by the lung (14%), ocular adnexa (12%), skin (9%) thyroid (4%), and small intestine (1%) [6, 7]. There is evidence that EMZL are associated with chronic antigenic stimulation, either by autoantigens or by foreign pathogens, leading to the accumulation of MALT in respective organs [8]. The mutational landscape of MZL of different origin is variegated: ocular adnexal [9,10,11,12], gastric [13], thyroid MZL [14, 15], as well as nodal MZL (NMZL) [16, 17] commonly display somatic mutations in genes encoding for compounds of the NF-κB pathway, chromatin modifier-encoding genes and genes related to the NOTCH pathway. Splenic MZL display mainly KLF2 mutations [18]. In ocular adnexal MZL, TNFAIP3 mutations affecting the NF-κB pathway are most prevalent [12]. Cutaneous MZL show recurrent FAS alterations [19].
In contrast, PMZL more commonly display structural and/or numeric chromosomal aberrations. Previous FISH studies revealed frequent t(11;18)(q21;q21) and t(14;18)(q32;q21) involving MALT1, and rarer t(1;14)(p22;q32) and t(3;14)(p14.1;q32) involving BCL10 and FOXP1, respectively, as well as trisomies 3 and 18 [20,21,22]. The mutational landscape of PMZL has not been studied at a larger scale so far. Although mutations—in descending order of frequency—of genes encoding for chromatin modifiers (CREBBP, TET2), members of the NOTCH- (TLBXR1, NOTCH1) and NF-κB signaling pathways (TNFAIP3, CARD11) have been previously detected by two research groups [14, 15], the mutational background of other primary lymphomas of the lung has not been addressed yet.
In this study, we aimed to expand the knowledge on the genetic landscape of PMZL as well as to comparatively analyze other lymphomas involving the lungs. We also investigated reactive lesions such as follicular bronchitis and lymphocytic interstitial pneumonia in order to see whether they can qualify as precursors to PMZL.
Materials and methods
Patients
Our study included 70 formalin-fixed, paraffin-embedded (FFPE) tissue samples of different lymphoproliferative disorders of the lung (Tables 1 and S1). Cases were provided by the departments of pathology of the contributing authors and were collected between 2005 and 2019. All cases were reviewed, and diagnosis was verified by TM and AT. The study was performed according to the safety laws of canton Basel and handling was approved by the ethics committee of Northwestern Switzerland (EKNZ 2014–252).
DNA extraction
Genomic DNA was obtained from the samples containing a tumor cell fraction or, in cases of reactive lymphoproliferations, lymphocyte fraction of more than 60% by conventional microscopy enforced by a CD20 staining, except for LyG cases grade 2, in which the region with the highest content of EBV-positive blasts was taken (Table S1). The extraction was performed according standard procedures with the GeneReadTM DNA-FFPE-Kit (Qiagen, Hilden, Germany), which includes uracil–DNA–glycosylase (UDG) to cleave deaminated cytosines (uracils), reducing C → T or G → A mismatches that lead to common artifacts in FFPE material. Genomic DNA was quantified using a Qubit fluorometer (Invitrogen, Eugene, OR, USA).
Immunohistochemistry, fluorescence in situ hybridization, and immunoglobulin heavy chain-gene (IGH) clonality analysis
Immunohistochemistry and FISH were performed according to routine standard operation procedures and hybridization procedures as described elsewhere [23]. For both BCL10 and MALT1, a break apart probe was used (BCL10–20-OR, Empire Genomics, Williamsville, NY, USA; SPEC MALT1, ZytoVision, Bremerhaven, Germany). Only PMZL and DLBCL cases with available material underwent FISH examination. IGH-BCL2 t(14;18)(q32;q21) and B-cell clonality (monoclonal IGH rearrangement) have been sought for by means of PCR and fragment analysis as described before [24].
Targeted HTS with custom lymphoma panel and data analysis
Targeted HTS was performed with the IonTorrent S5XL instrument; target enrichment for library preparation was done with an amplicon-based (AmpliSeq, IonTorrent, Thermo Fisher Scientific, Carlsbad, California) custom lymphoma panel (Table S2), which has been validated and used in earlier studies [12, 17]. All the samples included in this study had a mean coverage depth of ~1900× (range 1000×–6000×). Information for coverage depth, uniformity, and mapping quality are summarized in Table S3. Sequencing reads were aligned to the reference genome hg19 and the variant caller plug-in v5.10 from the IonTorrent software suite (Thermo Fisher Scientific) with default settings for somatic mutation detection was used to identify variants. Variants were annotated with the Single Sample Annotation Workflow of the Ion Reporter and dbNSFP database v3.2. Filtering was done according to criteria listed in Table S4; in short, variants with Phred-based quality lower or equal than 50, strand bias higher or equal to 0.75 were filtered out. Furthermore, we discarded variants below 5% in all entities except LyG (here the threshold was 1% due to scarcity of tumor cells) as potential artifacts and variants with variant allelic frequencies (VAF) higher than 95% as homozygous SNPs. Finally, variants found in assumingly healthy controls datasets (1000 genomes, ExAC) were excluded. Remaining mutations were manually reviewed, by using the IGV viewer to exclude remaining sequencing artifacts. Ensemble MetaLR score combining multiple functional prediction and conservation algorithms was used for in silico effect prediction of missense somatic point mutations [25]. Table S1 lists all somatic mutations identified in the study.
Statistical analysis
The distribution of entities according to sex was compared by the χ2 test. To assess the significance of mutational burden differences between entities, we applied the Kruskal-Wallis test. To assess the discriminating value of the presence of distinct mutations between PMZL and other lymphomas in this anatomic region, the Fisher’s exact test was used. Correlations were estimated with the Spearman rank correlation test; only strong correlations with ρ > 0.3 were further considered. All statistical calculations including descriptive data analysis were performed with MS Excel, SPSS.25, or R statistical package. Statistical significance threshold of p < 0.05 was assumed in all analyses. Whenever applicable, two-sided test were utilized.
Results
Clinico-pathological parameters
All clinical data are shown in Table 1. There were no significant differences regarding age and sex distribution between the different entities. Representative morphological images of PMZL, pulmonary DLBCL and LyG are shown in Fig. 1.
a Pulmonary marginal zone B-cell lymphoma showing infiltrates of small lymphoid cells with lympho-epithelial lesion (central upper part) (hematoxylin and eosin stain (H&E), 200×); b Mixed angiocentric infiltrates of larger atypical and small reactive lymphoid cells, and plasma cells, characteristic of lymphomatoid granulomatosis (H&E, 200×). c Pulmonary infiltration by sheets of blastoid cells corresponding to diffuse large B-cell lymphoma of the lung (H&E, 200×).
Mutational landscape of PMZL
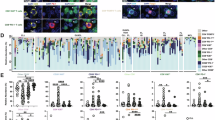
PMZL had a median of 2 mutations per case (0–5) (Fig. 2; Table 2). The most commonly mutated gene was KMT2D (10/28, 36%). Importantly, in PMZL, mutations of other genes encoding for chromatin modifiers (ARID1A, CREBBP, EP300, KMT2C, TET2) were observable in nearly mutually exclusive manner to mutant KMT2D in additional 6 cases, thus altogether 16/28 (57%) displayed a mutant gene in this group of genes. Mutations of TNFAIP3, NOTCH1, KLF2 and SPEN were exclusively seen in PMZL. These mutations as well as mutations of other genes encoding for NF-κB compounds (BCL10, CARD11, MYD88, TNFRSF14) were mutually exclusive. Accordingly, BCL10, MYD88, and TNFRSF14 mutations were also mutually exclusive to MALT1 and BCL10 rearrangements (Supplementary Fig. 1). Finally, NOTCH1 and its antagonists SPEN and KLF2 (and TBL1XR1) were mutually exclusively mutated. The mutation load of PMZL positively correlated with the Ki67 proliferation rate analyzed by immunohistochemistry (Rho = 0.733, p < 0.0001; Supplementary Fig. 2). In comparison to the other studied B-cell lymphomas, mutations of either TNFAIP3, NOTCH1, SPEN, or KLF2 (mutually complementary) were exclusive to PMZL (p = 0.001) and found in 12/28 cases.
Heatmap plot of somatic mutations in the studied entities showing all non-synonymous variants detected by targeted high-throughput sequencing. Each column represents a case grouped according to the assigned subtype. Each row represents a gene ordered top-down in decreasing order of detection frequency in pulmonary marginal zone B-cell lymphomas. When multiple mutations are present in the same gene, the most damaging mutation is displayed. PMZL pulmonary marginal zone lymphoma, LyG lymphomatoid granulomatosis, DLBCL diffuse large B-cell lymphoma, FL follicular lymphoma, FH follicular hyperplasia, NLH nodular lymphoid hyperplasia, LP lymphocytic interstitial pneumonia, MCL mantle cell lymphoma, CLL chronic lymphocytic leukemia.
PMZL and LyG significantly differ from DLBCL of the lung on a genetic basis
DLBCL had a median of 3 mutations per case (1–7) (Fig. 2; Table 2). Mutations of B2M, BRAF, SGK1, GNA13, TP53 were only seen in the DLBCL cohort (p = 0.014), as were e.g. mutations of PIK3R1 and PIM1 (yet not statistically significant). Characteristic mutations of PMZL such as TNFAIP3, NOTCH1, KLF2, and SPEN, were absent from the sub-cohort of DLBCL.
The mutational load of LyG was significantly lower than that of DLBCL (mean 1.1 versus 3.8 mutations/case, p = 0.002). Shared mutations were found in KMT2D, PRDM1, and SOCS1, while no mutations in genes related to immune escape, such as B2M or CD58/CD274, could be detected in LyG (p = 0.014 for B2M). Most mutations in LyG were in genes encoding for epigenetic modifiers (50%). However, one LyG case showed a mutation in TRAF3, which encodes for a CD40-signaling protein that interacts with the latent membrane protein 1 (LMP1) of EBV.
Genetic alterations in other B-cell lymphomas
The other mutations found in CLL, FL, and MCL cases were prototypical mutations for the respective entities such as ATM in CLL, CREBBP in FL, and ATM and CCND1 in MCL.
FISH investigations
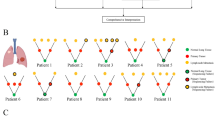
Rearrangements of BCL10 and MALT1 were seen in 1/16 and 4/16 PMZL, respectively (Fig. 3), whereas pulmonary DLBCL did not show rearrangements of these loci. Gains of the MALT1- and BCL10-loci being suggestive for trisomies 18 and 1, respectively, were seen in 4/16 and 5/16 PMZL, and in 1/4 DLBCL and 3/4 DLBCL, respectively. FISH-results are listed in detail in Table S5. The presence of rearrangements in PMZL inversely correlated with the mutational load (Spearman Rho = −0.522, p = 0.038) (Supplementary Fig. 1).
a Break apart probe-based analysis of the BCL10 locus yielding rearranged (split) signals (arrows) (400×); b Break apart analysis of the MALT1 locus yielding rearranged (split) signals (arrows) (400×).
Genetic alterations in reactive lesions
One case of follicular hyperplasia showed the PTEN mutation c.834 C>G (p.Phe278Leu; COSMIC Genomic Mutation ID: COSV64298151). It had a VAF of 17.7%, is absent in population databases and an in silico analysis predict a damaging effect (MetaLR rank score 0.88.) In line with this, immunohistochemistry for PTEN showed loss of protein-expression in the lymphocytes of the lesion, while being retained in the epithelial cells of the lung (Fig. 4), thus suggesting a functional relevance of the mutation. Based on the above-mentioned criteria, this PTEN alteration was considered to represent a relevant somatic mutation and not a germline variant.
a Immunohistochemistry showing preserved PTEN-expression in a case of follicular bronch(iol)it is without detectable mutations (immunohistochemistry, 100×). b Immunohistochemistry showing loss of PTEN-expression confined to the area of follicular hyperplasia/lymphoid compartment, confirming the functional importance of the PTEN-mutation found in the respective case.
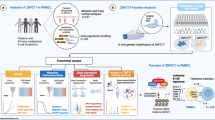
Pathway analysis of PMZL: clusters of chromatin modifiers, NOTCH- and NF-κB pathway
Most commonly, mutations in PMZL affected chromatin modifier-encoding genes subsuming 57% of cases. This cluster was nearly mutually exclusive to the NF-κB-signaling cluster that affected 32% of cases. A further distinct sub-cluster—within the chromatin modifier cluster—was the one related to NOTCH-signaling (21% of all PMZL) (Fig. 5).
Overview of pathways affected by mutations in pulmonary marginal zone lymphomas in comparison to cohorts of nodal marginal zone lymphomas (NMZL) and ocular adnexal marginal zone B-cell lymphomas (OAMZL) analyzed using the same HTS panel. Data of the NMZL and OAMZL cohorts were derived from previous studies of our group [12, 17].
Discussion
In this study on lymphomas of the lung, we could generate several new insights. We show that PMZL have distinct mutational and rearrangement patterns. This knowledge might be of help in diagnostically equivocal cases regarding, for example, other “small B-cell lymphomas” and reactive lymphoid lesions in this anatomic region. Furthermore, we provide genetic evidence, which suggests that PMZL and primary DLBCL of the lungs are genetically distinct.
As in other MZL, the mutational load of PMZL, even in a preselected group of genes relevant for lymphoid neoplasms, is low. The most common mutations in PMZL were found in KMT2D, TNFAIP3, and NOTCH1. TNFAIP3 mutations are known to play an important role in EMZL in general [11]. KMT2D, an epigenetic regulator, was the most common mutant gene in both PMZL and DLBCL. KMT2D mutations are known to be the most frequent mutations in B-cell lymphomas in general and in DLBCL in particular [26]. They are also common in NMZL [16, 17] and gastric MZL [13], while they occur more rarely in other subtypes of EMZL [15]. Other studies of PMZL have also shown both KMT2D mutations and mutations of chromatin modifiers in general, but less frequently than in our cohort [14, 15]. In the six cases of our cohort, in which both mutations of chromatin modifier-encoding genes and genes involved in the NOTCH pathway were present, the VAF of the first group was always higher than of the latter (Supplementary Fig. 3). This indicates that mutations in chromatin modifiers occurred before mutations of genes related to the NOTCH pathway. This finding confirms that mutations of chromatin modifiers are an early event in lymphomagenesis also in EMZL as has been shown for FL [27].
The second most commonly mutant gene, TNFAIP3, inhibits NF-κB activation by exerting dual ubiquitin-editing functions [28]. Furthermore, it augments molecular pathways including tumor necrosis factor receptor (TNFR) TLR/IL1-R and B-cell receptor (BCR) signaling, which are critical in the development of marginal zone B-cells. Similar to our previous study on ocular adnexal MZL and other lymphoproliferations of the orbit [12], also in this study we found that TNFAIP3 was not mutated in lymphoproliferations of the lungs other than PMZL.
Mutations affecting the NOTCH pathway including NOTCH1, SPEN, KLF2, and TBL1XR1 were also common in PMZL, but absent in other lymphoproliferations of the lungs. These genes affect the NOTCH pathway, which is essential for marginal zone B-cell development [29,30,31]. It has been shown that conditional knock out of Notch2 in mice results in the complete absence of marginal zone B-cells [32] leaving other B-cell subsets unaffected. Except for one TBL1XR1 mutant case (TBL1XR1 is suspected of playing a minor role in this pathway), NOTCH-pathway related mutations were absent in our limited pulmonary DLBCL cohort. This observation was made in spite of the fact that in de novo (nodal) DLBCL, NOTCH-mutations are an integral part of two recently defined genetic subsets (BN2 and N1) [33]. Nevertheless, these observations are in line with our remaining data disfavoring a relationship between PMZL and pulmonary DLBCL. Finally, while KLF2 is commonly mutated in splenic MZL [18], no other study on PMZL has described mutations in this gene [14, 15].
Interestingly, the mutational load of PMZL correlated with proliferation rate, in line with respect to lymphoma aggressiveness [34]. The mutational load inversely correlated with rearrangements of the BCL10 or MALT1 loci. In that context, our observed incidence of these rearrangements and their lack in pulmonary DLBCL were similar to previous reports [20, 35]. These translocations appear to be linked through the roles of BCL10 and MALT1 in activating the NF-κB pathway. Indeed, they not only were exclusively detectable in PMZL, thus further strengthening our assumption that pulmonary DLBLC do no not represent transformed PMZL, but were mutually exclusive and – with exception of a CARD11 mutation—mutually exclusive to presence of mutations of other genes encoding for NF-κB pathway compounds.
As to be expected and in line with previous studies of our group [36], LyG had a significantly lower mutational load than DLBCL. According to our knowledge, this is the first comprehensive analysis of the mutational landscape of LyG so far. Looking at primary EBV-positive DLBCL, another recent study could also show that the mutational profiles of EBV-positive and EBV-negative DLBCL significantly differ [37]. Yet in contrast to this study, most mutations in our LyG cases were observable in epigenetic modifiers while no mutations could be detected in MYC, or RHOA or components of the NF-κB pathway. In our previous study analyzing EBV-positive DLBCL-type post-transplant lymphoproliferative disorders (PTLD), mutations of MYC and components of the NF-κB pathway were seen in two cases each. Independent of the actual mutant genes, studies on EBV-positive B-cell lymphomas, including the current one on LyG, uniformly show that such instances display significantly lower mutational load than DLBCL suggesting that EBV infection may “substitute” for mutations. LyG cases furthermore did not show mutations in genes related to immune escape such as B2M or CD58/CD274; amplifications of PDL1 could not be assessed applying our methodology. Interestingly, one iatrogenic immunodeficiency-associated DLBCL case of our pulmonary DLBCL cohort was EBV-positive and did not display mutations in genes related to immune escape as well. These findings are in line with the proposed mechanistic model of EBV-driven lymphomagenesis that preferentially affects immunocompromised patients and/or body niches with decreased immunological control, and do not put tumor (precursor-)cells on pressure to acquire immune escape mutations [38].
Investigating reactive lesions of the lungs, including follicular bronchitis, lymphocytic interstitial pneumonia, and nodular lymphoid hyperplasia, one follicular bronchitis case displayed a known PTEN mutation [12]. In silico prediction and immunohistochemistry confirmed the potentially damaging effect of this mutation leading to PTEN expression loss in the lymphoid compartment. The same mutation was also detected in two other cases of our PMZL cohort. Importantly, within a follow-up period of 12 years this former patient is still alive and without evidence of lymphoma or other tumors. The identical mutation has been observed by us in a case of follicular conjunctivitis [12]. This mutation in both cases is to be considered somatic and not-germline derived due to relatively low VAF and confinement to lymphoid cells based on the immunohistochemical appearance. These two identical observations in extranodal follicular hyperplasias tempt us to speculate whether “clonal lymphopoiesis” exists, and if such PTEN mutant subclones may foster follicular hyperplasias in general, and extranodal follicular hyperplasias in particular. At the very least, these observations in reactive lesions underscore once again the fact that detection of mutations outside a proper clinic-pathologic context is of little diagnostic value.
To conclude, this study consolidates our knowledge on the genetic landscape of PMZL. It confirms the hypothesis that EMZL rely on and cluster around different signaling pathways, some of which are characteristic for their primary site of origin. It brings evidence that PMZL and primary pulmonary DLBCL are probably not related, and confirms the tumorigenic role of EBV in LyG, “substituting” for –especially immune escape- gene mutations.
References
Ferraro P, Trastek VF, Adlakha H, Deschamps C, Allen MS, Pairolero PC. Primary non-Hodgkin’s lymphoma of the lung. Ann Thorac Surg. 2000;69:993–7.
Borie R, Wislez M, Antoine M, Cadranel J. Lymphoproliferative disorders of the lung. Respiration. 2017;94:157–75.
Bertoni F, Rossi D, Zucca E. Recent advances in understanding the biology of marginal zone lymphoma. F1000Res. 2018;7:406.
Borie R, Wislez M, Thabut G, Antoine M, Rabbat A, Couderc L-J, et al. Clinical characteristics and prognostic factors of pulmonary MALT lymphoma. Eur Respir J. 2009;34:1408–16.
Nathwani BN, Anderson JR, Armitage JO, Cavalli F, Diebold J, Drachenberg MR, et al. Marginal zone b-cell lymphoma: a clinical comparison of nodal and mucosa-associated lymphoid tissue types. Non-hodgkin’s lymphoma classification project. J Clin Oncol. 1999;17:2486–92.
Troppan K, Wenzl K, Neumeister P, Deutsch A. Molecular pathogenesis of MALT lymphoma. Gastroenterol Res Pr. 2015;2015:1–10.
Cook JR, PG Isaacson, A Chott, S Nakamura, HK Müller-Hermelink, NL Harris et al. WHO classification of tumours of haematopoietic and lymphoid tissues, 4th ed. Lyon: International Agency for Research on Cancer; 2017.
Schreuder MI, van den Brand M, Hebeda KM, Groenen PJTA, van Krieken JH, Scheijen B. Novel developments in the pathogenesis and diagnosis of extranodal marginal zone lymphoma. J Hematop. 2017;10:91–107.
Cani AK, Soliman M, Hovelson DH, Liu C-J, McDaniel AS, Haller MJ, et al. Comprehensive genomic profiling of orbital and ocular adnexal lymphomas identifies frequent alterations in MYD88 and chromatin modifiers: new routes to targeted therapies. Mod Pathol. 2016;29:685–97.
Jung H, Yoo HY, Ho Lee S, Shin S, Kim SC, Lee S, et al. The mutational landscape of ocular marginal zone lymphoma identifies frequent alterations in TNFAIP3 followed by mutations in TBL1XR1 and CREBBP. Oncotarget. 2017;8:17038–49.
Johansson P, Klein-Hitpass L, Grabellus F, Arnold G, Klapper W, Pförtner R, et al. Recurrent mutations in NF-κB pathway components, KMT2D, and NOTCH1/2 in ocular adnexal MALT-type marginal zone lymphomas. Oncotarget. 2016;7:62627–39.
Vela V, Juskevicius D, Gerlach MM, Meyer P, Graber A, Cathomas G, et al. High throughput sequencing reveals high specificity of TNFAIP3 mutations in ocular adnexal marginal zone B‐cell lymphomas. Hematol Oncol. 2020;107:2718–31.
Hyeon J, Lee B, Shin SH, Yoo HY, Kim SJ, Kim WS, et al. Targeted deep sequencing of gastric marginal zone lymphoma identified alterations of TRAF3 and TNFAIP3 that were mutually exclusive for MALT1 rearrangement. Mod Pathol. 2018;31:1418–28.
Moody S, Thompson JS, Chuang S-S, Liu H, Raderer M, Vassiliou G, et al. Novel GPR34 and CCR6 mutation and distinct genetic profiles in MALT lymphomas of different sites. Haematologica. 2018;103:1329–36.
Cascione L, Rinaldi A, Bruscaggin A, Tarantelli C, Arribas AJ, Kwee I, et al. Novel insights into the genetics and epigenetics of MALT lymphoma unveiled by next generation sequencing analyses. Haematologica. 2019;104:558–61.
Spina V, Khiabanian H, Messina M, Monti S, Cascione L, Bruscaggin A, et al. The genetics of nodal marginal zone lymphoma. Blood. 2016;128:1362–73.
Pillonel V, Juskevicius D, Ng CKY, Bodmer A, Zettl A, Jucker D, et al. High-throughput sequencing of nodal marginal zone lymphomas identifies recurrent BRAF mutations. Leukemia. 2018;32:2412–26.
Clipson A, Wang M, De Leval L, Ashton-Key M, Wotherspoon A, Vassiliou G, et al. KLF2 mutation is the most frequent somatic change in splenic marginal zone lymphoma and identifies a subset with distinct genotype. Leukemia. 2015;29:1177–85.
Maurus K, Appenzeller S, Roth S, Kuper J, Rost S, Meierjohann S, et al. Panel sequencing shows recurrent genetic FAS alterations in primary cutaneous marginal zone lymphoma. J Invest Dermatol. 2018;138:1573–81.
Remstein ED, Dogan A, Einerson RR, Paternoster SF, Fink SR, Law M, et al. The incidence and anatomic site specificity of chromosomal translocations in primary extranodal marginal zone B-cell lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma) in North America. Am J Surg Pathol. 2006;30:1546–53.
Dierlamm J, Baens M, Wlodarska I, Stefanova-Ouzounova M, Hernandez JM, Hossfeld DK, et al. The apoptosis inhibitor gene API2 and a novel 18q gene, MLT, are recurrently rearranged in the t(11;18)(q21;q21) associated with mucosa-associated lymphoid tissue lymphomas. Blood. 1999;93:3601–9.
Willis TG, Jadayel DM, Du M-Q, Peng H, Perry AR, Abdul-Rauf M, et al. Bcl10 Is Involved in t(1;14)(p22;q32) of MALT B cell lymphoma and mutated in multiple tumor types. Cell. 1999;96:35–45.
Tzankov A, Xu-Monette ZY, Gerhard M, Visco C, Dirnhofer S, Gisin N, et al. Rearrangements of MYC gene facilitate risk stratification in diffuse large B-cell lymphoma patients treated with rituximab-CHOP. Mod Pathol. 2014;27:958–71.
Meier VS, Rufle A, Gudat F. Simultaneous evaluation of T- and B-cell clonality, t(11;14) and t(14;18), in a single reaction by a fourcolor multiplex polymerase chain reaction assay and automated high-resolution fragment analysis: A method for the rapid molecular diagnosis of lymphop. Am J Pathol. 2001;159:2031–43.
Liu X, Wu C, Li C, Boerwinkle E. dbNSFP v3.0: a one-stop database of functional predictions and annotations for human nonsynonymous and splice-site SNVs. Hum Mutat. 2016;37:235–41.
Juskevicius D, Jucker D, Klingbiel D, Mamot C, Dirnhofer S, Tzankov A. Mutations of CREBBP and SOCS1 are independent prognostic factors in diffuse large B cell lymphoma: mutational analysis of the SAKK 38/07 prospective clinical trial cohort. J Hematol Oncol. 2017;10:1–10.
Green MR. Chromatin modifying gene mutations in follicular lymphoma. Blood. 2018;131:595–604.
Heyninck K, Beyaert R. A20 inhibits NF-κB activation by dual ubiquitin-editing functions. Trends Biochem Sci. 2005;30:1–4.
Spina V, Rossi D. Molecular pathogenesis of splenic and nodal marginal zone lymphoma. Best Pr Res Clin Haematol. 2017;30:5–12.
Kuroda K, Han H, Tani S, Tanigaki K, Tun T, Furukawa T, et al. Regulation of marginal zone B cell development by MINT, a suppressor of Notch/RBP-J signaling pathway. Immunity. 2003;18:301–12.
Pillai S, Cariappa A. The follicular versus marginal zone B lymphocyte cell fate decision. Nat Rev Immunol. 2009;9:767–77.
Saito T, Chiba S, Ichikawa M, Kunisato A, Asai T, Shimizu K, et al. Notch2 is preferentially expressed in mature B cells and indispensable for marginal zone B lineage development. Immunity. 2003;18:675–85.
Schmitz R, Wright GW, Huang DW, Johnson CA, Phelan JD, Wang JQ, et al. Genetics and pathogenesis of diffuse large B-cell lymphoma. N. Engl J Med. 2018;378:1396–407.
Zhou H, Du X, Zhao T, Ouyang Z, Liu W, Deng M, et al. Distribution and influencing factors of tumor mutational burden in different lymphoma subtypes. J Clin Oncol. 2019;37:e19053–e19053.
Zhu Z, Liu W, Mamlouk O, O’Donnell JE, Sen D, Avezbakiyev B. Primary pulmonary diffuse large B cell non-hodgkin’s lymphoma: a case report and literature review. Am J Case Rep. 2017;18:286–90.
Menter T, Juskevicius D, Alikian M, Steiger J, Dirnhofer S, Tzankov A, et al. Mutational landscape of B-cell post-transplant lymphoproliferative disorders. Br J Haematol. 2017;178:48–56.
Zhou Y, Xu Z, Lin W, Duan Y, Lu C, Liu W, et al. Comprehensive genomic profiling of EBV-positive diffuse large B-cell lymphoma and the expression and clinicopathological correlations of some related genes. Front Oncol. 2019;9:683.
Ok CY, Li L, Young KH. EBV-driven B-cell lymphoproliferative disorders: from biology, classification and differential diagnosis to clinical management. Exp Mol Med. 2015;47:e132–e132.
Acknowledgements
The authors would like to thank Prof. C. Hamilton for critically proofreading the manuscript. The study has been supported by the Stiftung zur Krebsbekaempfung Zuerich (SKB473).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Vela, V., Juskevicius, D., Prince, S.S. et al. Deciphering the genetic landscape of pulmonary lymphomas. Mod Pathol 34, 371–379 (2021). https://doi.org/10.1038/s41379-020-00660-2
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41379-020-00660-2
This article is cited by
-
Clinical characteristics and molecular heterogeneity in Follicular lymphoma with extranodal involvement
Genome Medicine (2025)
-
Two cases demonstrate an association between Tropheryma whipplei and pulmonary marginal zone lymphoma
Infectious Agents and Cancer (2024)
-
Mutational landscape of marginal zone B-cell lymphomas of various origin: organotypic alterations and diagnostic potential for assignment of organ origin
Virchows Archiv (2022)