Abstract
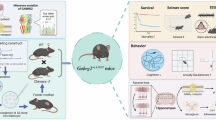
Schizophrenia (SCZ) is a prevalent and disabling mental disorder. Clinically, its complex symptoms, including negative symptoms and cognitive impairment, can be alleviated using electromagnetic techniques such as repetitive transcranial magnetic stimulation (rTMS). To investigate the neural mechanisms of magnetic stimulation and identify selective therapeutic targets, we employed combined magnetic stimulation system treatment (c-MSST). Targeting the left prelimbic cortex (PrL) of mice with c-MSST reversed the SCZ-like behaviors and synaptic abnormalities induced by MK-801 injection and normalized the regional increase in gamma-aminobutyric acid type A receptor subunit epsilon (GABRE) expression. Specific Gabre knockdown in the left PrL ameliorated MK-801-induced SCZ-like behaviors. Importantly, Gabre conditional knock-in mice exhibited SCZ-like behaviors and synaptic plasticity deficits, both of which were reversed by c-MSST. We further demonstrated that the ability of c-MSST to reduce GABRE protein expression may be related to p62/SQSTM1-mediated sequestration of GABARAP family. Our study improves the understanding of the therapeutic mechanisms of magnetic techniques and suggests that Gabre and related molecular circuits are promising targets for SCZ treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
The data discussed in this publication have been deposited in NCBI’s Gene Expression Omnibus and are accessible through GEO Series accession number GSE286434 (https://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE286434).
Code availability
The code required to reanalyze the data reported in this paper can be obtained by contacting the corresponding author.
References
Charlson FJ, Ferrari AJ, Santomauro DF, Diminic S, Stockings E, Scott JG, et al. Global epidemiology and burden of schizophrenia: findings from the global burden of disease study 2016. Schizophrenia Bull. 2018;44:1195–203.
GBD 2019 Mental Disorders Collaborators. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. The Lancet Psychiatry. 2022;9:137–50.
Hilker R, Helenius D, Fagerlund B, Skytthe A, Christensen K, Werge TM, et al. Heritability of schizophrenia and schizophrenia spectrum based on the nationwide danish twin register. Biol Psychiatry. 2018;83:492–8.
Ekin M, Akdal G, Bora E. Antisaccade error rates in first-episode psychosis, ultra-high risk for psychosis and unaffected relatives of schizophrenia: a systematic review and meta-analysis. Schizophr Res. 2024;266:41–9.
Jauhar S, Johnstone M, McKenna PJ. Schizophrenia. Lancet. 2022;399:473–86.
Starzer M, Hansen HG, Hjorthøj C, Albert N, Nordentoft M, Madsen T. 20-year trajectories of positive and negative symptoms after the first psychotic episode in patients with schizophrenia spectrum disorder: results from the OPUS study. World Psychiatry. 2023;22:424–32.
Fusar-Poli P, Papanastasiou E, Stahl D, Rocchetti M, Carpenter W, Shergill S, et al. Treatments of negative symptoms in schizophrenia: meta-analysis of 168 randomized Placebo-Controlled trials. Schizophr Bull. 2015;41:892–9.
Saleh Y, Jarratt-Barnham I, Petitet P, Fernandez-Egea E, Manohar SG, Husain M. Negative symptoms and cognitive impairment are associated with distinct motivational deficits in treatment resistant schizophrenia. Mol Psychiatry. 2023. https://doi.org/10.1038/s41380-023-02232-7.
Üçok A, Ergül C. Persistent negative symptoms after first episode schizophrenia: A 2-year follow-up study. Schizophr Res. 2014;158:241–6.
Tseng P-T, Zeng B-S, Hung C-M, Liang C-S, Stubbs B, Carvalho AF, et al. Assessment of noninvasive brain stimulation interventions for negative symptoms of Schizophrenia: a systematic review and network meta-analysis. JAMA Psychiatry. 2022;79:770–9.
Fitzsimmons SMDD, Oostra E, Postma TS, van der Werf YD, van den Heuvel OA. Repetitive transcranial magnetic stimulation-induced neuroplasticity and the treatment of psychiatric disorders: state of the evidence and future opportunities. Biol Psychiatry. 2023;S0006-3223:01745–6.
Thomson AC, Kenis G, Tielens S, de Graaf TA, Schuhmann T, Rutten BPF, et al. Transcranial magnetic stimulation-induced plasticity mechanisms: TMS-Related gene expression and morphology changes in a human neuron-like cell model. Front Mol Neurosci. 2020;13:528396.
Lefebvre S, Gehrig G, Nadesalingam N, Nuoffer MG, Kyrou A, Wüthrich F, et al. The pathobiology of psychomotor slowing in psychosis: altered cortical excitability and connectivity. Brain. 2024;147:1423–35.
Lefaucheur J-P, Aleman A, Baeken C, Benninger DH, Brunelin J, Di Lazzaro V, et al. Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS): an update (2014–2018). Clinical Neurophysiology. 2020;131:474–528.
Rosen AC, Bhat JV, Cardenas VA, Ehrlich TJ, Horwege AM, Mathalon DH, et al. Targeting location relates to treatment response in active but not sham rTMS stimulation. Brain Stimul. 2021;14:703–9.
Tubbs A, Vazquez EA. Engineering and technological advancements in repetitive transcranial magnetic stimulation (rTMS): a five-year review. Brain Sci. 2024;14:1092.
Lu Q-B, Sun J-F, Yang Q-Y, Cai W-W, Xia M-Q, Wu F-F, et al. Magnetic brain stimulation using iron oxide nanoparticle-mediated selective treatment of the left prelimbic cortex as a novel strategy to rapidly improve depressive-like symptoms in mice. Zool Res. 2020;41:381–94.
Carlén M. What constitutes the prefrontal cortex? Science. 2017;358:478–82.
Smucny J, Dienel SJ, Lewis DA, Carter CS. Mechanisms underlying dorsolateral prefrontal cortex contributions to cognitive dysfunction in schizophrenia. Neuropsychopharmacology. 2022;47:292–308.
Arnsten AFT, Woo E, Yang S, Wang M, Datta D. Unusual molecular regulation of dorsolateral prefrontal cortex layer III synapses increases vulnerability to genetic and environmental insults in Schizophrenia. Biol Psychiatry. 2022;92:480–90.
Zhou Y, Fan L, Qiu C, Jiang T. Prefrontal cortex and the dysconnectivity hypothesis of schizophrenia. Neurosci Bull. 2015;31:207–19.
Yoon JH, Minzenberg MJ, Ursu S, Ryan Walter BS, Wendelken C, Ragland JD, et al. Association of dorsolateral prefrontal cortex dysfunction with disrupted coordinated brain activity in schizophrenia: relationship with impaired cognition, behavioral disorganization, and global function. Am J Psychiatry. 2008;165:1006–14.
Wolkin A, Sanfilipo M, Wolf AP, Angrist B, Brodie JD, Rotrosen J. Negative symptoms and hypofrontality in chronic schizophrenia. Arch Gen Psychiatry. 1992;49:959–65.
Hasan A, Guse B, Cordes J, Wölwer W, Winterer G, Gaebel W, et al. Cognitive effects of high-frequency rTMS in Schizophrenia patients with predominant negative symptoms: results from a multicenter randomized sham-controlled trial. Schizophr Bull. 2016;42:608–18.
Xiu MH, Guan HY, Zhao JM, Wang KQ, Pan YF, Su XR, et al. Cognitive enhancing effect of high-frequency neuronavigated rTMS in chronic schizophrenia patients with predominant negative symptoms: a double-blind controlled 32-Week follow-up study. Schizophr Bull. 2020;46:1219–30.
Guan HY, Zhao JM, Wang KQ, Su XR, Pan YF, Guo JM, et al. High-frequency neuronavigated rTMS effect on clinical symptoms and cognitive dysfunction: a pilot double-blind, randomized controlled study in Veterans with schizophrenia. Transl Psychiatry. 2020;10:79.
Vertes RP. Interactions among the medial prefrontal cortex, hippocampus and midline thalamus in emotional and cognitive processing in the rat. Neuroscience. 2006;142:1–20.
van den Buuse M. Modeling the positive symptoms of schizophrenia in genetically modified mice: pharmacology and methodology aspects. Schizophr Bull. 2010;36:246–70.
Aoyama Y, Mouri A, Toriumi K, Koseki T, Narusawa S, Ikawa N, et al. Clozapine ameliorates epigenetic and behavioral abnormalities induced by phencyclidine through activation of dopamine D1 receptor. Int J Neuropsychopharmacol. 2014;17:723–37.
Kajitani K, Thorne M, Samson M, Robertson GS. Nitric oxide synthase mediates the ability of darbepoetin alpha to improve the cognitive performance of STOP null mice. Neuropsychopharmacology. 2010;35:1718–28.
Potasiewicz A, Holuj M, Litwa E, Gzielo K, Socha L, Popik P, et al. Social dysfunction in the neurodevelopmental model of schizophrenia in male and female rats: Behavioural and biochemical studies. Neuropharmacology. 2020;170:108040.
Yang M, Silverman JL, Crawley JN. Automated Three-Chambered Social Approach Task for Mice. Curr Protoc Neurosci. 2011;56:8–26.
Faure A, Nosjean A, Pittaras E, Duchêne A, Andrieux A, Gory-Fauré S, et al. Dissociated features of social cognition altered in mouse models of schizophrenia: focus on social dominance and acoustic communication. Neuropharmacology. 2019;159:107334.
Guo C, Liu Y, Fang M-S, Li Y, Li W, Mahaman YAR, et al. ω-3PUFAs Improve cognitive impairments through Ser133 phosphorylation of CREB upregulating BDNF/TrkB signal in Schizophrenia. Neurotherapeutics. 2020;17:1271–86.
Kraeuter A-K, Mashavave T, Suvarna A, van den Buuse M, Sarnyai Z. Effects of beta-hydroxybutyrate administration on MK-801-induced schizophrenia-like behaviour in mice. Psychopharmacology (Berl). 2020;237:1397–405.
Wakayama S, Kiyonaka S, Arai I, Kakegawa W, Matsuda S, Ibata K, et al. Chemical labelling for visualizing native AMPA receptors in live neurons. Nat Commun. 2017;8:14850.
Dwyer JM, Maldonado-Avilés JG, Lepack AE, DiLeone RJ, Duman RS. Ribosomal protein S6 kinase 1 signaling in prefrontal cortex controls depressive behavior. Proc Natl Acad Sci USA. 2015;112:6188–93.
Elsworth JD, Morrow BA, Hajszan T, Leranth C, Roth RH. Phencyclidine-induced loss of asymmetric spine synapses in rodent prefrontal cortex is reversed by acute and chronic treatment with olanzapine. Neuropsychopharmacology. 2011;36:2054–61.
Ramsey AJ, Milenkovic M, Oliveira AF, Escobedo-Lozoya Y, Seshadri S, Salahpour A, et al. Impaired NMDA receptor transmission alters striatal synapses and DISC1 protein in an age-dependent manner. Proc Natl Acad Sci USA. 2011;108:5795–5800.
Risher WC, Ustunkaya T, Singh Alvarado J, Eroglu C. Rapid Golgi analysis method for efficient and unbiased classification of dendritic spines. PLoS One. 2014;9:e107591.
Zhong L, Brown J, Kramer A, Kaleka K, Petersen A, Krueger JN, et al. Increased prefrontal cortex neurogranin enhances plasticity and extinction learning. J Neurosci. 2015;35:7503–8.
Corley SM, Tsai S-Y, Wilkins MR, Shannon Weickert C. Transcriptomic analysis shows decreased cortical expression of NR4A1, NR4A2 and RXRB in Schizophrenia and provides evidence for nuclear receptor dysregulation. PLoS One. 2016;11:e0166944.
Maycox PR, Kelly F, Taylor A, Bates S, Reid J, Logendra R, et al. Analysis of gene expression in two large schizophrenia cohorts identifies multiple changes associated with nerve terminal function. Mol Psychiatry. 2009;14:1083–94.
Lu Q, Wu F, Jiao J, Xue L, Song R, Shi Y, et al. Selective activation of ABCA1/ApoA1 signaling in the V1 by magnetoelectric stimulation ameliorates depression via regulation of synaptic plasticity. Iscience. 2022;25:104201.
Chen Y, Gu Y, Wang B, Wei A, Dong N, Jiang Y, et al. Synaptotagmin-11 deficiency mediates schizophrenia-like behaviors in mice via dopamine over-transmission. Nat Commun. 2024;15:10571.
McKinney WT, Moran EC. Animal models of schizophrenia. Am J Psychiatry. 1981;138:478–83.
Fulford D, Holt DJ. Social withdrawal, loneliness, and health in Schizophrenia: psychological and neural mechanisms. Schizophr Bull. 2023;49:1138–49.
McCutcheon RA, Keefe RSE, McGuire PK. Cognitive impairment in schizophrenia: aetiology, pathophysiology, and treatment. Mol Psychiatry. 2023;28:1902–18.
Bauminger H, Zaidan H, Akirav I, Gaisler-Salomon I. Anandamide hydrolysis inhibition reverses the long-term behavioral and gene expression alterations induced by MK-801 in male rats: differential CB1 and CB2 receptor-mediated effects. Schizophr Bull. 2022;48:795–803.
Glantz LA, Lewis DA. Decreased dendritic spine density on prefrontal cortical pyramidal neurons in schizophrenia. Arch Gen Psychiatry. 2000;57:65–73.
Garey LJ, Ong WY, Patel TS, Kanani M, Davis A, Mortimer AM, et al. Reduced dendritic spine density on cerebral cortical pyramidal neurons in schizophrenia. J Neurol Neurosurg Psychiatry. 1998;65:446–53.
Berdenis van Berlekom A, Muflihah CH, Snijders GJLJ, MacGillavry HD, Middeldorp J, Hol EM, et al. Synapse pathology in schizophrenia: a meta-analysis of postsynaptic elements in postmortem brain studies. Schizophr Bull. 2020;46:374–86.
Osimo EF, Beck K, Reis Marques T, Howes OD. Synaptic loss in schizophrenia: a meta-analysis and systematic review of synaptic protein and mRNA measures. Mol Psychiatry. 2019;24:549–61.
Love MI, Huber W, Anders S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 2014;15:550.
Braat S, Kooy RF. The GABAA receptor as a therapeutic target for neurodevelopmental disorders. Neuron. 2015;86:1119–30.
Prévot T, Sibille E. Altered GABA-mediated information processing and cognitive dysfunctions in depression and other brain disorders. Mol Psychiatry. 2021;26:151–67.
Luscher B, Fuchs T, Kilpatrick CL. GABAA receptor trafficking-mediated plasticity of inhibitory synapses. Neuron. 2011;70:385–409.
Berry MD, Gainetdinov RR, Hoener MC, Shahid M. Pharmacology of human trace amine-associated receptors: therapeutic opportunities and challenges. Pharmacol Ther. 2017;180:161–80.
Delhaye S, Bardoni B. Role of phosphodiesterases in the pathophysiology of neurodevelopmental disorders. Mol Psychiatry. 2021;26:4570–82.
Zhu S, Noviello CM, Teng J, Walsh RM, Kim JJ, Hibbs RE. Structure of a human synaptic GABAA receptor. Nature. 2018;559:67–72.
Ferrante M, Migliore M, Ascoli GA. Feed-forward inhibition as a buffer of the neuronal input-output relation. Proc Natl Acad Sci USA. 2009;106:18004–9.
Squadrani L, Wert-Carvajal C, Müller-Komorowska D, Bohmbach K, Henneberger C, Verzelli P, et al. Astrocytes enhance plasticity response during reversal learning. Commun Biol. 2024;7:852.
Coyle JE, Nikolov DB. GABARAP: lessons for synaptogenesis. Neuroscientist. 2003;9:205–16.
Schaaf MBE, Keulers TG, Vooijs MA, Rouschop KMA. LC3/GABARAP family proteins: autophagy-(un)related functions. FASEB J. 2016;30:3961–78.
Ye J, Zou G, Zhu R, Kong C, Miao C, Zhang M, et al. Structural basis of GABARAP-mediated GABAA receptor trafficking and functions on GABAergic synaptic transmission. Nat Commun. 2021;12:297.
Neelands TR, Fisher JL, Bianchi M, Macdonald RL. Spontaneous and gamma-aminobutyric acid (GABA)-activated GABA(A) receptor channels formed by epsilon subunit-containing isoforms. Mol Pharmacol. 1999;55:168–78.
Hui KK, Takashima N, Watanabe A, Chater TE, Matsukawa H, Nekooki-Machida Y, et al. GABARAPs dysfunction by autophagy deficiency in adolescent brain impairs GABAA receptor trafficking and social behavior. Sci Adv. 2019;5:eaau8237.
Sumitomo A, Yukitake H, Hirai K, Horike K, Ueta K, Chung Y, et al. Ulk2 controls cortical excitatory-inhibitory balance via autophagic regulation of p62 and GABAA receptor trafficking in pyramidal neurons. Hum Mol Genet. 2018;27:3165–76.
Brunelin J, Adam O, Mondino M. Recent advances in noninvasive brain stimulation for schizophrenia. Curr Opin Psychiatry. 2022;35:338–44.
Frohlich F, Riddle J. Conducting double-blind placebo-controlled clinical trials of transcranial alternating current stimulation (tACS). Transl Psychiatry. 2021;11:284.
Menardi A, Rossi S, Koch G, Hampel H, Vergallo A, Nitsche MA, et al. Toward noninvasive brain stimulation 2.0 in Alzheimer’s disease. Ageing Res Rev. 2022;75:101555.
Camacho-Conde JA, Del Rosario Gonzalez-Bermudez M, Carretero-Rey M, Khan ZU. Therapeutic potential of brain stimulation techniques in the treatment of mental, psychiatric, and cognitive disorders. CNS Neurosci Ther. 2023;29:8–23.
Xue L, Ye Q, Wu L, Li D, Bao S, Lu Q, et al. Magneto-mechanical effect of magnetic microhydrogel for improvement of magnetic neuro-stimulation. Nano Res. 2023;16:7393–404.
Camacho-Conde JA, Gonzalez-Bermudez MDR, Carretero-Rey M, Khan ZU. Brain stimulation: a therapeutic approach for the treatment of neurological disorders. CNS Neurosci Ther. 2022;28:5–18.
Jannati A, Oberman LM, Rotenberg A, Pascual-Leone A. Assessing the mechanisms of brain plasticity by transcranial magnetic stimulation. Neuropsychopharmacology. 2023;48:191–208.
Basavaraju R, Ithal D, Thanki MV, Ramalingaiah AH, Thirthalli J, Reddy RP, et al. Intermittent theta burst stimulation of cerebellar vermis enhances fronto-cerebellar resting state functional connectivity in schizophrenia with predominant negative symptoms: a randomized controlled trial. Schizophr Res. 2021;238:108–20.
Valiengo LDCL, Goerigk S, Gordon PC, Padberg F, Serpa MH, Koebe S, et al. Efficacy and safety of transcranial direct current stimulation for treating negative symptoms in Schizophrenia: a randomized clinical trial. JAMA Psychiatry. 2020;77:121–9.
Li Z, Yin M, Lyu X-L, Zhang L-L, Du X-D, Hung GC-L. Delayed effect of repetitive transcranial magnetic stimulation (rTMS) on negative symptoms of schizophrenia: Findings from a randomized controlled trial. Psychiatry Res. 2016;240:333–5.
Penzes P, Cahill ME, Jones KA, VanLeeuwen J-E, Woolfrey KM. Dendritic spine pathology in neuropsychiatric disorders. Nat Neurosci. 2011;14:285–93.
Li S, Ma C, Li Y, Chen R, Liu Y, Wan LP, et al. The schizophrenia-associated missense variant rs13107325 regulates dendritic spine density. Transl Psychiatry. 2022;12:361.
Dracheva S, Marras SA, Elhakem SL, Kramer FR, Davis KL, Haroutunian V. N-methyl-D-aspartic acid receptor expression in the dorsolateral prefrontal cortex of elderly patients with schizophrenia. Am J Psychiatry. 2001;158:1400–10.
Luykx JJ, Visscher R, Winter-van Rossum I, Waters P, de Witte LD, Fleischhacker WW, et al. Clinical symptoms and psychosocial functioning in patients with schizophrenia spectrum disorders testing seropositive for anti-NMDAR antibodies: a case-control comparison with patients testing negative. Lancet Psychiatry. 2024;11:828–38.
Janz R, Südhof TC, Hammer RE, Unni V, Siegelbaum SA, Bolshakov VY. Essential roles in synaptic plasticity for synaptogyrin I and synaptophysin I. Neuron. 1999;24:687–700.
Benes FM. The GABA system in schizophrenia: cells, molecules and microcircuitry. Schizophr Res. 2015;167:1–3.
Nutt DJ, Malizia AL. New insights into the role of the GABA(A)-benzodiazepine receptor in psychiatric disorder. Br J Psychiatry. 2001;179:390–6.
Lim L, Mi D, Llorca A, Marín O. Development and functional diversification of cortical interneurons. Neuron. 2018;100:294–313.
Xu M-Y, Wong AHC. GABAergic inhibitory neurons as therapeutic targets for cognitive impairment in schizophrenia. Acta Pharmacol Sin. 2018;39:733–53.
Lu C, Zhu X, Feng Y, Ao W, Li J, Gao Z, et al. Atypical antipsychotics antagonize GABAA receptors in the ventral tegmental area GABA neurons to relieve psychotic behaviors. Mol Psychiatry. 2023. https://doi.org/10.1038/s41380-023-01982-8.
Volk DW, Pierri JN, Fritschy J-M, Auh S, Sampson AR, Lewis DA. Reciprocal alterations in pre- and postsynaptic inhibitory markers at chandelier cell inputs to pyramidal neurons in schizophrenia. Cereb Cortex. 2002;12:1063–70.
Fatemi SH, Folsom TD, Rooney RJ, Thuras PD. Expression of GABAA α2-, β1- and ε-receptors are altered significantly in the lateral cerebellum of subjects with schizophrenia, major depression and bipolar disorder. Transl Psychiatry. 2013;3:e303.
Bristow GC, Bostrom JA, Haroutunian V, Sodhi MS. Sex differences in GABAergic gene expression occur in the anterior cingulate cortex in schizophrenia. Schizophr Res. 2015;167:57–63.
Muir J, Kittler JT. Plasticity of GABAA receptor diffusion dynamics at the axon initial segment. Front Cell Neurosci. 2014;8:151.
Kittler JT, Chen G, Kukhtina V, Vahedi-Faridi A, Gu Z, Tretter V, et al. Regulation of synaptic inhibition by phospho-dependent binding of the AP2 complex to a YECL motif in the GABAA receptor gamma2 subunit. Proc Natl Acad Sci USA. 2008;105:3616–21.
Jacob TC, Moss SJ, Jurd R. GABA(A) receptor trafficking and its role in the dynamic modulation of neuronal inhibition. Nat Rev Neurosci. 2008;9:331–43.
Petrini EM, Ravasenga T, Hausrat TJ, Iurilli G, Olcese U, Racine V, et al. Synaptic recruitment of gephyrin regulates surface GABAA receptor dynamics for the expression of inhibitory LTP. Nat Commun. 2014;5:3921.
Tomoda T, Sumitomo A, Shukla R, Hirota-Tsuyada Y, Miyachi H, Oh H, et al. BDNF controls GABAAR trafficking and related cognitive processes via autophagic regulation of p62. Neuropsychopharmacology. 2022;47:553–63.
Han W, Shepard RD, Lu W. Regulation of GABAARs by transmembrane accessory proteins. Trends Neurosci. 2021;44:152–65.
Kittler JT, Thomas P, Tretter V, Bogdanov YD, Haucke V, Smart TG, et al. Huntingtin-associated protein 1 regulates inhibitory synaptic transmission by modulating gamma-aminobutyric acid type A receptor membrane trafficking. Proc Natl Acad Sci USA. 2004;101:12736–41.
Acknowledgements
We thank Prof. Gavin P. Reynolds and Prof. Yan Kong for conceptual discussions and manuscript editing. This work was supported by the National Natural Science Foundation of China (82371510, 82401761, and 82101572), Social Development Foundation of Jiangsu Province, China (No. BE2023668), and Nanjing Major Science and Technology Project (Life and Health, No. 202305035).
Author information
Authors and Affiliations
Contributions
Conceptualization: XRZ, ZJZ. Experimental design: XRZ, ZJZ, YSH, ZXW. Data analysis: YSH, ZXW, JF, STZ. Investigation: ZXW, YSH, YW, YRL. Visualization: YSH, ZXW, DDX, MYL. Supervision: XRZ, ZJZ. Writing–original draft: YSH, XRZ, ZJZ. Writing–review & editing: all authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
All experimental procedures involving animals were approved by the Institutional Animal Care and Use Committee of Southeast University (approval number: 20210426008) and were conducted in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals. No human participants were involved in this study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hu, Y., Wang, Z., Fang, J. et al. Selective magnetic stimulation downregulates the GABAA receptor ε subunit in the left prelimbic cortex to alleviate schizophrenia-like behaviors in mice. Mol Psychiatry 31, 383–395 (2026). https://doi.org/10.1038/s41380-025-03267-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41380-025-03267-8