Abstract
Schizophrenia (SCZ) is a severe neurodevelopmental mental disorder characterised by a complex and multifactorial disease aetiology. Patients can suffer from both positive symptoms (e.g. hallucinations) and negative symptoms (e.g. social withdrawal) as well as cognitive impairments. The former are currently discussed to be caused by a hyperdopaminergic state in the striatum, whereas for the latter a hypodopaminergic state in the prefrontal cortex (PFC) is hypothesised. However, the underlying mechanism of hypodopaminergic signalling in the PFC, especially via the mesocortical pathway, is currently not known to any great detail. By analysing the transcriptome of iPSC-derived dopaminergic neurons from SCZ patients, we found that genes involved in dopaminergic differentiation as well as in dopamine synthesis and transport were downregulated. Furthermore, the expression of the D2 subtype of the dopamine receptor (DRD2) was also decreased, suggesting a hypodopaminergic phenotype and disinhibition of neuronal activity. Calcium imaging of a purely SCZ co-culture of human dopaminergic and glutamatergic telencephalic neurons revealed increased activity of both types of neurons, which was selectively reduced by a DRD2 agonist. Further quantification of synapse marker densities indicated a loss of glutamatergic synapses both on NGN2 and ALN neurons, whereas dopaminergic synapses were unaffected. Using mixed co-cultures comprising glutamatergic/dopaminergic neurons from healthy controls and SCZ patients, calcium imaging identified SCZ-ALN neurons as a major driver of increased activity in SCZ. Thus, the proposed model may be useful for the study of hypodopaminergic phenotypes of schizophrenia.
Similar content being viewed by others
Introduction
Schizophrenia spectrum (SCZ) is a complex neurodevelopmental disorder affecting 1% of the population. It is characterized by cognitive, social, and motor impairments. The disorder manifests in various symptoms: positive (e.g. hallucinations and delusions), negative (e.g. amotivation, anhedonia and social withdrawal), and cognitive (deficits in attention, memory and planning) [1]. The complexity of the disease is reflected by high heterogeneity in both its aetiology and symptomatology and both genetic as well as environmental factors play a role in its pathogenesis. Common hypotheses claim that excess dopamine (DA) transmission is a key disease mechanism as suggested from antipsychotic effects of antagonists of the DA receptor D2 (DRD2) [2].
Aberrations of two major dopaminergic pathways, the mesolimbic and the mesocortical pathways, have been implicated in SCZ both of which originate in the ventral tegmental area (VTA) of the midbrain. In the case of the former, dopaminergic neurons project to the nucleus accumbens of the ventral striatum, whereas in the latter they project to the prefrontal cortex [3]. The role of the dopaminergic system was highlighted by initial findings demonstrating that psychostimulant drugs, such as amphetamine, can induce psychotic symptoms in healthy individuals similar to those seen in patients with SCZ, a process mediated by elevated DA levels [4, 5]. Supporting this, early studies in mice and SCZ patients showed that reducing DA levels alleviated these symptoms [6, 7]. Whilst, early hypotheses proposed an excess of DA transmission in patients with SCZ, they were later reformulated to stating an imbalance between excess DA in subcortical regions, responsible for positive symptoms, and reduced DA in the prefrontal cortical (PFC) areas contributing to negative and cognitive symptoms [8, 9]. At the neurochemical level, recent PET studies of SCZ patients support the hypothesis of a cortical hypodopaminergic state correlating with poor cognitive performance [10, 11]. Consistently, post-mortem studies of patients with SCZ have revealed a reduction in dopaminergic input to the PFC [12]. In the microcircuit of the PFC, the integration of excitatory and inhibitory signals is tightly controlled by several neurodevelopmental processes responsible for accurate synapse formation [13]. Multiple lines of evidence propose a disturbance in the excitation and inhibition (E-I) balance in the PFC as one biological consequence in SCZ patients. However, to what extent the hypodopaminergic phenotype contributes to the deficit in the E-I microcircuit, and vice versa, remains elusive.
In the PFC, dopaminergic neurons show highest innervation density in layers II/III and V by forming synaptic connections with dendritic spines of pyramidal neurons and inhibitory interneurons [14], thereby modulating higher cognitive processes, such as working memory, planning and attention [15]. Both DA receptor types, the stimulating DRD1 and the inhibitory DRD2, have been identified in the human cortex [16] and are expressed by cortical neurons [17]. Generally, cortical neurons expressing DRD1 and DRD2 are segregated and project to distinct subcortical regions [18, 19]. Research on DRD1 receptor density in the PFC of SCZ patients yielded inconsistent results. While studies on drug-naïve patients have reported elevated DRD1 density in the PFC [20, 21], those involving chronically treated patients have found a reduction in DRD1 expression [22]. Nevertheless, alterations in DRD1 binding potential are thought to contribute to impairments in cognition, such as working memory deficits [20, 23]. Post-mortem and in vivo imaging studies mainly focused on DRD2 binding capacity in the striatum and demonstrated increased DRD2 expression [24, 25]. Thus, there is little evidence on putative aberrant DRD2 density in the cortex of SCZ patients and their interplay with DRD1 receptors. Projections of glutamatergic pyramidal neurons from the PFC into the VTA allow for reciprocal connection and the formation of a neuronal circuitry [26]. As the roles of glutamatergic and dopaminergic neurons of the mesocortical pathway are poorly understood, analysing this interaction may provide further mechanistic insight into schizophrenia disease mechanisms.
Here, we established a defined induced pluripotent stem cell (iPSC)-based co-culture system comprising dopaminergic neurons, generated by lentiviral overexpression of the transcription factors ASCL1/LMX1B/NURR1 (ALN) and telencephalic glutamatergic neurons, generated by lentiviral overexpression of NGN2 [27,28,29]. Transcriptome analysis of ALN neurons revealed downregulation of mRNAs associated with dopaminergic differentiation and DA metabolism, as well as downregulation of the DRD2 receptor, in parallel with reduced expression of genes assigned to gene ontology (GO) terms such as “synapse” and “neuron projection”. Calcium imaging indicated increased spontaneous neuronal activity of both ALN and NGN2 neurons which was rescued by a selective DRD2 agonist. Quantification of synapse marker densities indicated a loss of glutamatergic synapses both on NGN2 and ALN neurons.
Materials and methods
iPSC lines
The methods were performed in accordance with relevant guidelines and regulations and approved by the Ethics Committee of the University Hospital and Faculty of Medicine Tuebingen. We confirm that participants provided a written informed consent to take part in the study. All eight iPSC lines (four healthy controls, four from individuals with schizophrenia) used in this study were previously described and fully characterized [30, 31]. Additional information for all iPSC lines is summarized in Supplementary Table 1. iPSC were cultured on Matrigel (Corning, Inc., Corning, NY)-coated 6-well plates in mTeSRTM Plus medium (STEMCELL Technologies, Vancouver, Canada) at 37 °C in humified 5% CO2 atmosphere. Medium change was performed daily, and cells were enzymatically passaged using Accutase (Sigma-Aldrich, St. Louis, MO).
Lentiviral vectors
For the differentiation of dopaminergic neurons, the lentiviral vector TetO-ASCL1-LMX1B-NURR1 (ALN) (Addgene, Watertown, MA) was further modified: The coding sequence for the puromycin resistance gene (Puro) was cloned immediately downstream of the NURR1 open reading frame, linked by a 2 A peptide encoding sequence allowing for bicistronic expression. of Thus, successfully transduced recombinant cells were selected. pEF1α-Synaptophysin-mRuby (Addgene, Watertown, MA) was cloned into a lentiviral backbone via Gateway integration according to manufacturer’s instructions (Thermo Fisher Scientific, Waltham, MA).
To produce third generation lentiviruses for pLV-TetO-ALN-Puro, pLV-EF1α-Synaptophysin-mRuby, pLV-FUdeltaGW-rtTA (Addgene, Watertown, MA) and pLV-TetO-hNGN2-eGFP-Puro (Addgene, Watertown, MA), the cell line HEK293-FT weas used. HEK293-FT is a rapidly proliferating, highly transfectable cell line, making it particularly suitable for high-titer lentivirus production [32]. The cell line is derived from the HEK293 parental line, a stable, immortalized cell line originally established from primary human embryonic kidney tissue. The cells are transformed with the E1A adenovirus gene, enabling them to produce high levels of viral particles [33]. For this purpose, HEK293-FT cells were transfected with the respective plasmid using a Lentiviral Packaging Plasmid Mix (Cellecta, Mountain View, CA) mixed with Lipofectamine 2000 (Thermo Fisher Scientific, Waltham, MA). Lenti-X p24 Rapid Titer Kit (Takara Bio USA, Inc., San Jose, CA) was used to determine lentiviral titers which usually were in the range of 5 × 1010 to 5 × 1011 particles per ml. Plasmids and lentiviral vectors are listed in Supplementary Table 2.
Neural progenitor cell generation and maintenance
Neural progenitor cells (NPCs) were generated following the embryoid body (EB) protocol according to the manufacturer’s instructions using the STEMdiffTM SMADi Neural Induction Kit (STEMCELL Technologies, Vancouver, Canada). In brief, iPSC were enzymatically detached and 2 × 106 cells were seeded into each well of an AggreWell™800 24-well plate pretreated with Anti-Adherence Rinsing Solution (STEMCELL Technologies, Vancouver, Canada). After 4 days of incubation with a daily 50% medium exchange, EBs were collected and filtered through a 37 µm reversible strainer (STEMCELL Technologies, Vancouver, Canada). EBs were then replated onto poly-l-ornithine/Laminin-coated 6-well plates. Plates were treated with 20% poly-l-ornithine (PLO, Sigma-Aldrich, St. Louis, MO) diluted in DPBS for 2 h at RT, washed with DPBS and DMEM/F12, and incubated with 10 µg/ml in DMEM/F12 diluted Laminin (Sigma-Aldrich, St. Louis, MO) overnight at 37 °C. After seven days of incubation in STEMdiff™ Neural Induction Medium, neural rosettes were selected after exposure to STEMdiffTM Neural Rosette Selection Reagent (STEMCELL Technologies, Vancouver, Canada) for 1.5 h at 37 °C. Neural rosettes were transferred to PLO/Laminin-coated 6-well plates and further grown in STEMdiffTM Neural Progenitor medium (STEMCELL Technologies, Vancouver, Canada).
Differentiation of NGN2-EGFP neurons
Differentiation of NPCs into NGN2-EGFP neurons was performed according to a published protocol [34]. One day before lentiviral transduction, NPCs were seeded on PLO/Laminin-coated 12-well plates in Neural Progenitor medium at a density of 5.26×104/cm2. On the following day, NPCs were co-transduced with pLV-FUdeltaGW-rtTA and pLV-TetO-hNGN2-EGFP-Puro. After 24 h, medium was changed to Neural Progenitor medium containing 1 µg/ml of Doxycycline (Sigma-Aldrich, St. Louis, MO). The following day selection of transduced cells was initiated by addition of 1 µg/ml of the antibiotic Puromycin (Thermo Fisher Scientific, Waltham, MA).
Differentiation of ALN neurons
The induction of ALN neurons was performed according to a published protocol starting from iPSC [35]. In brief, iPSC were enzymatically detached, centrifuged and counted. Cells were diluted in mTeSRTM Plus medium with 10 µM ROCK inhibitor (STEMCELL Technologies, Vancouver, Canada) to obtain a final cell titre of 7.89 × 104 iPSC/cm2. After addition of the lentiviral vectors pLV-FUdeltaGW-rtTA and pLV-TetO-ALN-Puro, the cell suspension was plated in Matrigel-coated 12-well plates. After overnight incubation, medium was replaced by Induction medium, consisting of DMEM/F12 (Thermo Fisher Scientific, Waltham, MA) supplemented with 1x Penicillin/Streptomycin (Thermo Fisher Scientific, Waltham, MA), 1x GlutaMAXTM (Thermo Fisher Scientific, Waltham, MA), 1x Sodium Pyruvat (Thermo Fisher Scientific, Waltham, MA), 1x B-27TM (Thermo Fisher Scientific, Waltham, MA), 1x N-2 (Thermo Fisher Scientific, Waltham, MA) and 1 µg/ml of Doxycycline. The following day, medium was replaced by Induction medium supplemented with 1 µg/ml of Doxycycline and 1 µg/ml of Puromycin and repeated for three days. On day 6 and 7 of differentiation, 2 µM of Ara-C (Sigma-Aldrich, St. Louis, MO) was added to the Induction medium to eliminate non-differentiating iPSC. Daily medium changes with Induction medium supplemented with 1 µg/ml of Doxycycline were continued until day 10 of differentiation.
Transduction of pLV-EF1α-Synaptophysin-mRuby
For overexpression of Synaptophysin (SYP)-mRuby for labelling of synaptic boutons, pLV-EF1α-Synaptophysin-mRuby was added to lentiviral suspension comprising pLV-FUdeltaGW-rtTA and pLV-TetO-ALN-Puro for differentiation of ALN neurons from iPSC, or pLV-FUdeltaGW-rtTA and pLV-TetO-hNGN2-EGFP-Puro for differentiation of NGN2 neurons from NPCs. The differentiation was subsequently performed as described in the section above.
Co-culture of ALN and NGN2-EGFP-induced neurons
Pre-differentiated ALN neurons at day 10 of differentiation and NGN2-GFP neurons at day 3 of differentiation were detached using Accutase and seeded either as mono- orco-cultures at a ratio of 50:50 on PLO/Laminin-coated plates. The total seeding density was 1.56×105 neurons/cm2. Neurons were incubated in Neuron medium, consisting of BrainPhys (STEMCELL Technologies, Vancouver, Canada) supplemented with 1x Penicillin/Streptomycin, 1x GlutaMAXTM, 1x Sodium Pyruvat, 1x B-27TM, 1x N-2, 20 ng/µl BDNF and 20 ng/µl GDNF (Thermo Fisher Scientific, Waltham, MA) 200 nM L-Ascorbic Acid (Sigma-Aldrich, St. Louis, MO), 500 µg/ml dibutyryl cAMP (Sigma-Aldrich, St. Louis, MO), 1 µg/ml Laminin and 1 µg/ml of Doxycycline. After neuronal attachment, 3.125×104/cm2 primary murine astrocytes were added to mono- as well as co-cultures. Astrocytes were included in all experiments except for transcriptome analysis. With a 50% medium exchange every other day, neurons were further incubated in Neuron medium without Doxycycline until day 24 of differentiation. Doxycycline was subsequently added to the medium until 28 days of differentiation for ALN neurons and 21 days of differentiation for NGN2 neurons.
In most experiments, the iPSC lines were individually differentiated into ALN-induced or NGN2-induced neurons and then mixed for co-cultures of ALN and NGN2 neurons from the same individual, respectively. For permutating healthy controls and neurons from diseased individuals in all combinations, the three control (CTR) lines (CTR1, CTR2, CTR3) were pooled, and all four SCZ lines were likewise pooled. These pooled samples were then combined to generate a mixed co-culture comprising the four possible combinations: CTR ALN + CTR NGN2, SCZ ALN + CTR NGN2, CTR ALN + SCZ NGN2 and SCZ ALN + SCZ NGN2. Detailed overview of the four permutations is summarized in Supplementary Table 7.
Preparation of murine astrocytes
One day old newborn pups from the wildtype RjOrl mouse strain (Janvier-Labs) were used for the isolation of murine astrocytes, which was performed according to a published protocol [36]. Briefly, newborn pups were decapitated, and the scalp was gently removed. Along the midline, that separates the hemispheres, the skull was cut open and carefully pulled apart. Next, the brain was removed with a small spoon and placed immediately into ice-cold DPBS supplemented with 15 mM HEPES buffer (Thermo Fisher Scientific, Waltham, MA) + 1x Penicillin-Streptomycin. Using sharp and sterile scissors, the olfactory bulbs and the cerebellum were then separated from the cortex, followed by stripping away the meninges using fine forceps. Subsequently, the hemispheres were separated, and the hippocampi were removed when possible. These steps were performed under a stereomicroscope. The cortices were chopped into smaller pieces and kept on ice in a falcon tube with DPBS + 15 mM HEPES buffer + 1x Penicillin-Streptomycin. After the preparation of all cortices, the DPBS solution was discarded, and 5 ml of 0.025% trypsin/EDTA (Thermo Fisher Scientific, Waltham, MA) were added, which was then gently mixed. The cortices were then incubated in a 37 °C water bath for 20 minutes, followed by replacing the trypsin/EDTA solution by astrocyte medium consisting of DMEM, high glucose, GlutaMAX™ Supplement (Thermo Fisher Scientific, Waltham, MA) supplemented with 10% FBS (Thermo Fisher Scientific, Waltham, MA), 1x Penicillin/Streptomycin, 1x GlutaMAXTM, 1x Sodium Pyruvate. After gentle trituration, cortical fragments were further cultivated in T75 flasks containing astrocyte medium and incubated at 37 °C with 8% CO₂, with complete medium changes every other day. After one week, the astrocytes were passaged enzymatically with trypsin/EDTA 0.025% to remove neurons, microglia, and oligodendrocytes. For co-cultivation with neurons, astrocytes up to passage P2 were used.
Immunocytochemistry
ALN neurons differentiated on 96-well half area µclear plates (Greiner, Frickenhausen, Germany) for 28 days, and NGN2 neurons differentiated for 21 days were washed once with DPBS, fixed with 4% PFA in PBS for 15 min at RT and washed 3x with DPBS. Following fixation, cells were permeabilized and blocked using a blocking solution consisting of 0.1% Triton-X100 (Carl Roth, Karlsruhe, Germany) in DPBS and 1% blocking reagent BMB (Roche, Rotkreuz, Switzerland) for 30 min at RT. After overnight incubation at 4 ˚C with primary antibodies diluted in blocking solution (see Supplementary Table 3 for details), cells were washed 3 x with DPBS and subsequently exposed to following fluorescently labeled secondary antibodies: Cy3 anti-mouse (1:500; 115-165-146) and Cy5 anti-rabbit (1:500; 111-175-144, both from Dianova, Eching, Germany), Alexa FluorTM 488 goat anti-chicken (1:400; A-11039) and Alexa FluorTM 405 goat anti-chicken (1:150; A48260, both from Thermo Fisher Scientific, Waltham, MA). Nuclei were stained using Hoechst Dye 33258 (1:1000 in PBS; 861405, Sigma-Aldrich, St. Louis, MO). Secondary antibody solution was added for 2 h at RT. Subsequently, cells were washed and stored in DPBS at 4˚C.
Image acquisition and processing
Z-stacks were taken using Cell Observer SD spinning disk confocal laser scan microscope (Zeiss, Oberkochen, Germany) with either a 20x or 63x plan-apochromatic oil immersion objective. For each condition, two wells per cell line were imaged for each replicate. In each well, five areas of comparable MAP2/βIII-tubulin fibre density were chosen for subsequent image analysis.
For the quantification of tyrosine hydroxylase (TH)-positive cells as a measure for dopaminergic neuron differentiation, ALN neurons cultured individually were fixed after four weeks of differentiation and stained for the dopaminergic marker TH and Hoechst to stain DNA. Accordingly, NGN2 neurons in monocultures were stained for the neuron-specific nuclear marker NeuN and Hoechst after three weeks of differentiation. Z-stacks of the three CTR lines (CTR1, CTR2, CTR3) and the four SCZ lines (SCZ1, SCZ2, SCZ4, SCZ5) were acquired. In total, three independent differentiations per donor were analysed. Z-stacks were further processed in Zen (blue edition, 3.5) by creating orthogonal projections, which were then exported. Further processing of orthogonal projections was performed in Fiji (ImageJ). Images acquired from ALN monocultures were split into the TH and Hoechst channels, while images acquired from NGN2 monocultures were split into the channels NeuN and Hoechst. Next, a threshold was set, which allowed for the analysis of particles for each individual channel. The Fiji processing tool ‘Image Calculator’ was then applied to determine particles double-positive for TH and Hoechst as a surrogate for ALN-derived dopaminergic neurons, and particles double-positive for NeuN and Hoechst as a surrogate for NGN2-derived glutamatergic neurons. For each image, the number of double-positive cells was divided by the total number of Hoechst-positive cells and ratios obtained from one well were averaged.
A second approach for the quantification of the dopaminergic differentiation efficiency was based on measurements of the cell surface area, in order to exclude the co-cultured murine astrocytes stained by the nuclear marker Hoechst. For the quantification of TH-positive cells as a measure for dopaminergic neuron differentiation, images of the three CTR lines (CTR1, CTR2, CTR3) and the four SCZ lines (SCZ1, SCZ2, SCZ4, SCZ5) were acquired for each replicate. For the calculation of differentiation efficiencies, the IMARIS Bitplane 10.0.0 software (Oxford Instruments, Abigdon, UK) was used. To this end, volumes of the βIII-tubulin surface (µm3) and the TH surface (µm3) were determined, and the TH surface volume was divided by the respective βIII-tubulin surface volume to calculate differentiation efficiency.
Quantification of synaptic marker expression was performed with the help of the IMARIS Bitplane 10.0.0 software, as described previously [37]. For synapse analysis in co-cultures, EGFP-labelling of NGN2 neurons allowed to distinguish ALN neurons from NGN2 neurons.
Calcium imaging
Calcium imaging of ALN-NGN2 co-cultures was conducted when ALN neurons reached day 28 of differentiation, while at this time point NGN2 neurons had been differentiated for 21 days. Accordingly, recordings from ALN and NGN2 monocultures were performed at day 28 and day 21 of differentiation, respectively. Neurons were stained with 2 µM Cal-520® AM in DMEM/F12 (for ALN monocultures) or with 2 µM CalbryteTM 590 AM (for ALN/NGN2 co-cultures; both from AAT Bioquest, Pleasanton, CA) for 30 min at 37 ˚C. After washing once with DMEM/F12, neurons were incubated for 10–15 min at 37 °C in Neuron medium to allow for recovery. Immediately prior to calcium signal recording, snapshots of the CalbryteTM 590 AM and EGFP signals were taken to assign recorded calcium signals to co-cultured ALN and NGN2-EGFP neurons. 3 min videos of spontaneous single-cell calcium activity were retrieved from two microscopic areas of similar cell density using the 20x objective of the Cell Observer SD.
The recorded videos were further processed with the help of the image processing software Fiji. A minimum of five neurons per neuronal subtype from each video were analysed. Active neuronal somatas were circled with the freehand selection tool for subsequent measurement using the ROI Manager tool. The Origin 2015G Peak Analyzer software (OriginLab Corporation, USA) was employed for processing. Four peak parameters were analysed: area under the curve (AUC), full width at half maximum (FWHM), amplitude (ΔF/F0), and peak frequency (number of peaks per second, Hz). These parameters were averaged across all peaks of a single neuron, and the data from multiple cells within a single well were further averaged and normalised to the CTR group.
Pramipexole dihydrochloride or Sulpiride (both from MedChemExpress, Monmouth Junction, NJ) were dissolved in DMSO to obtain a concentration of 10 mM and 50 mM, respectively. Pramipexole dihydrochloride, Sulpiride or DMSO only as a solvent control were added to Neuron medium to a final concentration of 10 µM and applied to mixed co-cultures for 24 h. Subsequent calcium imaging was performed as described above.
Transcriptome analysis
Whole transcriptome sequencing and bioinformatical evaluation of ALN neurons after 3 weeks of differentiation, cultured in the absence of murine astrocytes, was performed by CeGaT GmbH (Tübingen, Germany). Cell pellets of three independent differentiations were pooled for each line. Differential expression analysis between CTR and SCZ groups was performed with DESeq2 (version 1.24.0) presented in Love et al. 2014 [38] followed by Benjamini-Hochberg correction. A significance level of 5% (cut-off of padj<0.05) was used to assess statistically significant differences in gene expression. GO enrichment analysis was performed using the online PantherDB classification system (https://pantherdb.org/) with the following statistical enrichment tests for cellular components. Hierarchical clustering of transcriptome data with log2 fold changes was performed using the MeV software (Multiple Experiment Viewer, USA).
Statistics
Statistical analysis was performed using GraphPad Prism 9.4.1 (GraphPad Software, Inc, USA). Outliers were removed and data checked for Gaussian distribution. For non-pairwise comparisons between two groups, normally distributed data was analyzed using unpaired t-tests and non-normally distributed data was analyzed using unpaired Mann-Whitney U tests. Group comparisons were analyzed by ordinary one-way Anova tests and Kruskal-Wallis tests with Dunn’s post-hoc for normally and non-normally distributed data, respectively. For group comparisons including more than two groups, ordinary two-way Anova with Tukey’s multiple comparison test was performed. Data was obtained from a minimum of three independent neuronal differentiations per line. Data points represent mean values from multiple recordings/images taken within one well ± SEM. For transcriptome data, each data point represents a cell line including three independent differentiations. P-values were assigned as follows: * = p ≤ 0.05, ** = p ≤ 0.01, *** = p ≤ 0.001, **** = p ≤ 0.0001. For calcium imaging and quantitative immunofluorescence, for each bar chart depicting pooled results from all cell lines and biological replicates, all data points and the mean effect of the respective single cell lines are shown in supplemental figures to demonstrate that pooled results are not biased by differences in the amounts of data points included between the across cell lines.
Results
Transcriptome analysis of ALN neurons
For the characterization of dopaminergic neurons, ALN-transduced neurons were stained for neuronal and cell type specific markers after four weeks of differentiation (DIV28; Fig. 1A, B). MAP2-positive ALN neurons showed robust expression of FOXA2, an important transcription factor for dopaminergic neuron development and maintenance [39] (Fig. 1A). Most neurons co-expressed MAP2 and TH, indicating efficient conversion into dopaminegric neurons (Fig. 1B, Supplementary Figure 1A). Precise analysis of the ratio of TH and Hoechst double-positive cells, as well as TH-positive cells over βIII-tubulin-positive cells indicated differentiation efficiencies between 60–80% (Supplementary Figure 1B, C), irrespective of whether the cells had originated from healthy donors (CTR) or from patients suffering from schizophrenia (SCZ).
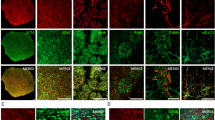
MAP2- or βIII-tubulin-positive ALN neurons differentiated for 28 days express the dopaminergic markers FOXA2 or TH (A, B). Hoechst staining visualizes nuclei (Scale bars 20 µm). (C) Volcano plot of significantly deregulated genes (cut-off levels for y-axis=1.3 (-log10(pvalue) ≤ 0.05); for x-axis = <3 and >3) depicted by brown lines, blue dots indicate downregulated, red dots indicate upregulated genes) identified by RNA sequencing of ALN neurons differentiated for 21 days. RNA sequencing was done for following cell lines: CTR1, CTR2, CTR3, SCZ1, SCZ2, SCZ4, SCZ5 (CTR, n = 3; SCZ, n = 4). (D) Hierarchical cluster analysis of the top 5% of upregulated and downregulated DEGs revealed segregation of CTR and SCZ samples. (E) GO enrichment analysis (PantherDB) identified deregulated gene sets in the category cellular components CC. Top 17 downregulated pathways (blue) and top 12 upregulated pathways (red) are depicted. (F) Expression of selected dopaminergic marker genes. Normalised read counts are represented as mean ± SEM. DRD1: CTR = 97.39 ± 27.28; SCZ = 429.88 ± 186.13; DRD2: CTR = 62550.66 ± 13727.71; SCZ = 11815.34 ± 3547.33; DRD3: CTR = 8.69 ± 7.69; SCZ = 1.00 ± 0; DRD4: CTR = 2338.62 ± 577.00; SCZ = 4146.43 ± 1217.14; DRD5: CTR = 3.64 ± 1.32; SCZ = 24.76 ± 11.13. (Changes in expression levels were statistically not significant (CTR n = 3, SCZ n = 4; Each n was retrieved from a pool composed of three independent replicates; TH=tyrosine hydroxylase, DDC = L-amino acid decarboxylase, DBH=dopamine beta-hydroxylase, COMT=catechol-O-methyltransferase, DAT=dopamine transporter, VMAT1/2=vesicular monoamine transporter 1/2).
After 3 weeks of differentiation, the transcriptome of ALN-transduced neurons was analyzed to identify deregulated genes in SCZ neurons compared to healthy controls. In total, we identified 1559 differentially expressed genes (DEGs) with 723 genes being downregulated and 836 being upregulated (Fig. 1C, DEGs are listed in Supplementary Table 4). Hierarchical clustering of the top 5% of upregulated and downregulated DEGs revealed two separated clusters, representing the three CTR lines and the four SCZ lines, respectively (Fig. 1D). A GO enrichment analysis was performed using the online classification system PantherDB to identify deregulated gene sets in the category “cellular components” (CC; cut-off q-val <0.05). The most prominent downregulated gene sets in CC were assigned to the following subcategories “cellular anatomical entity”, “synapse”, “cellular component” and “neuron projection” (Fig. 1E). In contrast, gene sets associated with “plasma membrane bounded cell projection”, “apical part of cell”, “cilium”, “cell periphery” and “projection” appeared to be upregulated. Interestingly, more gene sets became downregulated than upregulated (for detailed information see Supplementary Table 5 and Supplementary Table 6).
Closer inspection of the normalised read counts of genes downregulated in SCZ neurons in comparison to CTR neurons revealed the genes affected to be involved in dopaminergic differentiation or in DA transmission (Fig. 1F). In comparison to healthy control samples, RNA sequencing of SCZ ALN neurons identified drastic downregulation of gene transcripts for FOXA2, NURR1, TH, DDC and DBH, all of which are involved in dopaminergic differentiation and synthesis of DA. Moreover, genes important for the re-uptake of DA from the synaptic cleft or the cytosol, such as the DA transporter (DAT) and the vesicular monoamine transporters 1 and 2 (VMAT1, VMAT2) were significantly downregulated in SCZ ALN neurons. In contrast, COMT, a gene involved in DA degradation, was found to be upregulated. Analysis of DA receptor expression suggested that DRD2 prevail over a minor DRD4 expression, while DRD1, DRD3, and DRD5 were hardly detectable. The comparison between SCZ and CTR samples revealed reduced DRD2 expression in SCZ ALN neurons ( < 20% of control), while low level expression of DRD 1 (4.4-fold of control), DRD 4 (1.7-fold of control), and DRD5 (6.8-fold of control; for normalised read counts see legend Fig. 1) became upregulated. It is of note that stem cell marker genes including POU5F1, LIN28A, NANOG and SOX2 as well as neural progenitor marker genes including PAX6 and the progenitor surface marker FGFR1 were upregulated while no differences were found for NES and FZD9 expression (Supplementary Figure 2).
In conclusion, ALN neurons derived from patients with SCZ showed an upregulation of stem cell and neural progenitor marker genes, whereas transcription factors essential for dopaminergic development and differentiation were downregulated, suggesting aberrations in early development. Furthermore, reduced expression of genes important for DA synthesis and signalling implies a hypodopaminergic phenotype further exacerbated by increased COMT expression. The preponderance of DRD2 suggests an inhibitory action of DA with reduced inhibition in SCZ ALN neurons.
Increased spontaneous activity of ALN and NGN2 neurons in co-culture
The suspected hypodopaminergic phenotype together with the decreased expression of the inhibitory DA autoreceptor DRD2 may contribute to a disinhibition of the activity of dopaminergic neurons. We therefore examined neuronal activity levels in ALN and NGN2 neurons by calcium imaging. Precise analysis of the ratio of NeuN and Hoechst double-positive cells, as well as TH-positive cells indicated differentiation efficiencies of NGN2 neurons between 55–70% (Supplementary Figure 3). Calcium signals retrieved from separately cultivated ALN and NGN2 neurons, respectively, did not show any differences between CTR and SCZ samples (Supplementary Figure 4 and 5). To further examine the interaction between dopaminergic and glutamatergic neurons, we established a co-culture model comprising ALN and NGN2 neurons stained with the red calcium dye CalbryteTM 590 AM. CalbryteTM 590 AM /EGFP double-positive cells were considered as NGN2 neurons while CalbryteTM 590 AM-positive/EGFP-negative cells were assigned to the group of ALN neurons (Fig. 2A). In contrast to the separately cultivated ALN and NGN2 neurons, in co-culture both ALN and NGN2 neurons exhibited significantly increased peak frequencies when derived from SCZ patients (Fig. 2B, F, J, Supplementary Figure 6D, H). Calcium signals of SCZ ALN neurons showed decreased FWHM, whereas AUC and ΔF/F0 were not affected (Fig. 2C–E, Supplementary Figure 6A–C). FWHM, AUC and ΔF/F0 remained unaltered in NGN2 neurons (Fig. 2G–I, Supplementary Figure 6E–G). In conclusion, the increased peak frequency observed for ALN and NGN2 neurons implies an overall increased activity in our SCZ co-culture system. Since this was only observed in co-culture (for calcium analysis in ALN and NGN2 monocultures see Supplementary Figures 4 and 5), the interaction between these two cell types might account for the enhanced activity observed. The increased neuronal activity of ALN neurons supports the hypothesis of a hypodopaminergic phenotype suggested by the transcriptome data.
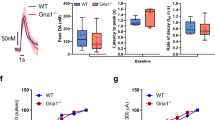
(A) Neurons in ALN-NGN2 co-cultures stained with the red fluorescent calcium indicator Calbryte 590 AM. NGN2 neurons express EGFP, allowing the discrimination of ALN from NGN2 neurons in co-cultures (arrowhead: NGN2 neuron; open arrowhead: ALN neuron). Scale bar: 50 µm. (B) Representative calcium traces recorded for 3 min from spontaneously active CTR ALN and SCZ ALN neurons, as well as from CTR NGN2 and SCZ NGN2 neurons. (C–J) Mean peak parameters ± SEM are indicated: area under the curve (AUC), full width at half maximum (FWHM), amplitude (ΔF/F0) and peak frequency (Hz) of ALN neurons and NGN2 neurons. Two tailed Mann Whitney-U tests (**=p ≤ 0.01, ***=p ≤ 0.001, ns=not significant). Values are normalised to CTR, while values for peak frequency are represented as absolute values. Parameters of multiple cells within one well were averaged and normalised to the CTR group for each replicate. Following cell lines were included in the calcium imaging experiment: CTR1, CTR2, CTR3, SCZ1, SCZ2, SCZ4, SCZ5. (C) AUC of ALN neurons (CTR n = 26, SCZ n = 37, p = 0.0927). (D) FWHM of ALN neurons (CTR n = 26, SCZ n = 37, p = 0.0008). (E) ΔF/F0 of ALN neurons (CTR n = 26, SCZ n = 37, p = 0.6128). (F) Peak frequency of ALN neurons (CTR n = 26, SCZ n = 37, p = 0.0002). (G) AUC of NGN2 neurons (CTR n = 26, SCZ n = 37, p = 0.2132). (H) FWHM of NGN2 neurons (CTR n = 26, SCZ n = 37, p = 0.062). (I) ΔF/F0 of NGN2 neurons (CTR n = 26, SCZ n = 37, p = 0.9613). (J) Peak frequency of NGN2 neurons (CTR n = 26, SCZ n = 37, p = 0.0037).
To further corroborate these findings, we examined calcium peak frequencies in the presence of Pramipexole, a selective DRD2 agonist, or Sulpiride, a selective DRD2 inhibitor. We found that application of Pramipexole completely rescued elevated peak frequencies of SCZ ALN and SCZ NGN2 lines to the base levels observed for untreated healthy control lines (Fig. 3). In contrast, Sulpiride did not alter the frequency of calcium transients in SCZ ALN neurons, whereas the frequency of SCZ NGN2 neurons showed a slight increase, which was not statistically significant. Both drugs were ineffective when applied to healthy control lines. Other parameters such as AUC, FWHM or amplitude were not affected (Supplementary Figure 7). Given the observed effects on both ALN and NGN2 SCZ neurons, we assume that Pramipexole exerts a direct effect on both neuronal cell types expressing DRD2, or alternatively, an indirect effect involving reciprocal interactions between SCZ neurons. The selective impact on SCZ neurons implies specific, DRD2-dependent regulation of neuronal activity not observed with healthy control neurons. Therefore, the hypodopaminergic phenotype of SCZ ALN neurons may increase the activity both of ALN and NGN2 neurons.
A, B Peak frequency analysis of calcium traces retrieved from spontaneously active ALN and NGN2 neurons after 24 h treatment with DMSO (solvent control), 10 µM of Pramipexole dihydrochloride (DRD2 agonist) or 10 µM of Sulpiride (DRD2 antagonist). Two-way ANOVA with Tukey’s multiple comparison test (*=p ≤ 0.05). Values are normalised to CTR DMSO. Following cell lines were included in the calcium imaging experiment: CTR1, CTR2, CTR3, SCZ1, SCZ2, SCZ4, SCZ5. A Peak frequency of ALN neurons (CTR DMSO n = 10, CTR Pramipexole n = 10, CTR Sulpiride n = 10, SCZ DMSO n = 10, SCZ Pramipexole n = 10, SCZ Sulpiride n = 9, CTR: DMS0 vs. Pramipexole p = 0.8369, DMS0 vs. Sulpiride p = 0.3033, Pramipexole vs. Sulpiride p = 0.108, SCZ: DMS0 vs. Pramipexole p = 0.0229, DMS0 vs. Sulpiride p = 0.8101, Pramipexole vs. Sulpiride p = 0.1128). B Peak frequency of NGN2 neurons (CTR DMSO n = 10, CTR Pramipexole n = 10, CTR Sulpiride n = 10, SCZ DMSO n = 10, SCZ Pramipexole n = 10, SCZ Sulpiride n = 9, CTR: DMS0 vs. Pramipexole p = 0.7611, DMS0 vs. Sulpiride p = 0.242, Pramipexole vs. Sulpiride p = 0.6273, SCZ: DMS0 vs. Pramipexole p = 0.0384, DMS0 vs. Sulpiride p = 0.3477, Pramipexole vs. Sulpiride p = 0.0009).
Reduced glutamatergic synapse densities on ALN and NGN2 neurons
An alternative explanation for the increased activity patterns of SCZ neurons, and one independent of DA signalling, may rely on increased numbers of glutamatergic synapses. We therefore asked whether deficiencies in the formation or stabilization of synapses occur as a consequence of the interaction between ALN and NGN2 neurons. In a first set of experiments, we stained ALN-NGN2 co-cultures for the presynaptic marker synapsin 1 (SYN1) and for the postsynaptic density protein 95 (PSD95, Fig. 4A). The density of presynaptic terminals was quantified on MAP2-positive neurons. To this end, spot densities of pre- and postsynaptic markers (SYN1 + PSD95) in close apposition on MAP2-positive neurons were assigned to a morphological synapse. On both ALN and NGN2 neurons, we observed significantly decreased SYN1-positive presynaptic densities, as well as reduced densities of morphological synapses in SCZ co-cultures (Fig. 4B–E, Supplementary Figure 8A, B, E, F). When ALN neurons were cultured separately, both the pre- and postsynaptic markers SYN1 and PSD95 were found to be co-localized (Supplementary Figure 9A). However, in contrast to synaptic phenotypes observed in SCZ co-cultures, monocultures did not show deregulated pre- or postsynaptic marker densities (Supplementary Figure 9B–FE, Supplementary Figure 10).
Representative images of ALN-NGN2 co-cultures stained for the presynaptic marker SYN1 (A–E) or vGLUT1 (F–J) and the postsynaptic marker PSD95 on MAP2-positive dendrites and somata (Scale bars 20 µm). EGFP-expression allows for discrimination of ALN neurons (MAP2-positive/EGFP-negative somata; open arrow heads in A, A”, F, F”) from NGN2 neurons MAP2-positive/EGFP-positive somata A, A’, F, F’). Apposition of SYN1 and PSD95 spots (A”’-A””) or vGLUT1 and PSD95 spots (F”’-F””) is considered as a morphological synapse (indicated by arrow heads). (B–E) Quantification of presynaptic (SYN1) and synaptic cluster densities (SYN1 + PSD95) on ALN or NGN2 neurons. Two tailed Mann Whitney-U tests (**=p ≤ 0.01, ***=p ≤ 0.001, ****=p ≤ 0.0001). Values are normalised to CTR. Synapse densities from individual images within a single well were averaged and normalised to CTR within individual differentiations. Following cell lines were included in the synapse quantification experiment: CTR1, CTR2, CTR3, SCZ1, SCZ2, SCZ4, SCZ5. (B) Presynaptic density (SYN1) on ALN neurons (CTR n = 24, SCZ n = 28, p = 0.0002). (C) Synaptic density (SYN1 + PSD95) on ALN neurons (CTR n = 24, SCZ n = 28, p < 0.0001). (D) Presynaptic density (SYN1) on NGN2 neurons (CTR n = 24, SCZ n = 28, p = 0.0048). (E) Synaptic density (SYN1 + PSD95) on NGN2 neurons (CTR n = 24, SCZ n = 28, p = 0.0048). (G–J) Quantification of presynaptic (vGlUT1) and synaptic cluster densities (vGluT1 + PSD95) on ALN or NGN2 neurons. Two tailed Mann Whitney-U tests (*=p ≤ 0.05, ns=not significant). Values are normalised to CTR. (G) Excitatory presynaptic density (vGLUT1) on ALN neurons (CTR n = 24, SCZ n = 32, p = 0.1033). (H) Excitatory synaptic density (vGLUT1 + PSD95) on ALN neurons (CTR n = 24, SCZ n = 32, p = 0.1025). (I) Excitatory presynaptic density (vGLUT1) on NGN2 neurons (CTR n = 24, SCZ n = 32, p = 0.0131). (J) Excitatory synaptic density (vGLUT1 + PSD95) on NGN2 neurons (CTR n = 24, SCZ n = 32, p = 0.0533).
Since SYN1 staining does not allow to differentiate between dopaminergic and glutamatergic terminals, vesicular glutamate transporter 1 (vGLUT1) staining was applied to identify the involvement of aberrant synaptic connectivity in SCZ. vGLUT1 mRNA is expressed in cortical areas and is not found in the VTA [40, 41]. As described for the SYN1 analysis, vGLUT1-positive, excitatory presynaptic marker densities and vGLUT1 + PSD95 excitatory synapse densities in apposition were analyzed on MAP2-positive neurons (Fig. 4F). Presynaptic marker densities and synapse densities were slightly reduced on SCZ ALN neurons compared to CTR ALN neurons,but did not reach levels of significance (Fig. 4G, H, Supplementary Figure 8C, D). On NGN2 neurons, excitatory synapse density as well as presynaptic vGLUT1 cluster density were decreased in SCZ (Fig. 4I, J, Supplementary Figure 8G, H). In conclusion, glutamatergic synapses on glutamatergic neurons appeared to be reduced while for ALN neurons the effects were not clear.
In a control experiment we unexpectedly observed vGLUT1/PSD95-positive synapses on ALN neurons grown in isolation (Supplementary Figure 11). Thus, the analyses shown above may be biased by potential expression of vGLUT1-positive synapses by ALN neurons which does not allow for a clear-cut discrimination from glutamatergic synapses originating from NGN2 neurons. Since typical dopaminergic synaptic marker expression in ALN neurons was too faint to enable quantification of synapse densities, we pursued another strategy for an unambiguous assignment of synaptic terminal to ALN neurons. Prior to the assembly of co-cultures, either NGN2 or ALN neurons were transduced with pLV-EF1α-SYP-mRuby expressing a Synaptophysin-mRuby fusion protein to efficiently label presynaptic terminals of the respective phenotype (Fig. 5A). Staining for vGLUT1 and analysis of co-localizing SYP-mRuby spots revealed mutually exclusive expression patterns (Fig. 5B) suggesting discrimination of vGLUT1-positive NGN2 neuron terminals from SYP-mRuby-positive ALN neuron terminals in the co-culture model. Quantification of presynaptic terminals derived from ALN neurons expressing SYP-mRuby did not reveal any differences in presynapse formation neither on ALN neurons nor on NGN2 neurons between CTR and SCZ cultures (Fig. 5C, D). In contrast, presynaptic terminals derived from SYP-mRuby transduced NGN2 neurons were significantly reduced on NGN2 and ALN neurons (Fig. 5E, F). Results for each line separately are depicted in Supplementary Figure 12. In conclusion, our results suggest that presynaptic terminals of NGN2 glutamatergic neurons are reduced in SCZ while a loss of terminals derived from dopaminergic terminals was not observed. Therefore, the increased activity of SCZ ALN or NGN2 neurons cannot be explained by more glutamatergic input based on the number of contacting glutamatergic terminals.
Representative images of ALN-NGN2 co-culture depicting SYP-mRuby transduced ALN neurons (A) and SYP-mRuby transduced ALN neurons co-stained with vGLUT1 (B; Scale bars 20 µm). EGFP-expression in NGN2-transduced neurons allows for discrimination between ALN and NGN2 neurons (open arrow heads indicate ALN neurons). C–F Transduction of ALN (C, D) or NGN2 (E, F) neurons and quantification of SYP-mRuby-positive presynaptic boutons on ALN and NGN2 neurons in co-culture. Two tailed Mann Whitney-U test (*=p ≤ 0.05, ns=not significant). Values are normalised to CTR. C SYP-mRuby-positive presynaptic density on ALN neurons (CTR n = 34, SCZ n = 50, p = 0.4220). (D) SYP-mRuby-positive presynaptic density on NGN2 neurons (CTR n = 31, SCZ n = 48, p = 0.4780). E SYP-mRuby-positive presynaptic density on ALN neurons (CTR n = 24, SCZ n = 35, p = 0.0016). F SYP-mRuby-positive presynaptic density on NGN2 neurons (CTR n = 25, SCZ n = 38, p = 0.0065). Following cell lines were included in the SYP-mRuby quantification experiment: CTR1, CTR2, CTR4, SCZ1, SCZ2, SCZ4, SCZ5.
Increased activity in SCZ is mainly driven by SCZ ALN neurons
To further strengthen our hypothesis that the hypodopaminergic phenotype of SCZ ALN neurons is the major driver of increased activity in SCZ neurons, we combined control and SCZ neurons, both of glutamatergic and dopaminergic phenotypes in all four possible permutations: CTR ALN + CTR NGN2, SCZ ALN + CTR NGN2, CTR ALN + SCZ NGN2, SCZ ALN + SCZ NGN2. To this end, the three CTR lines (CTR1, CTR2, CTR3) and the four SCZ lines (SCZ1, SCZ2, SCZ4, SCZ5) were pooled to give rise to two populations of CTR and SCZ samples, which were subsequently differentiated into either ALN or NGN2 phenotypes before the four combinations were set up.
In line with the observations shown in Fig. 2F, J, a comparison of the two combinations CTR ALN + CTR NGN2 and SCZ ALN + SCZ NGN2 indicated increased peak frequency for both ALN and NGN2 neurons in the SCZ condition (Fig. 6A, B). Likewise, the co-culture combination SCZ ALN + CTR NGN2 showed an equally increased activity of ALN neurons compared to the CTR ALN + CTR NGN2 combination, which however was not observed for the CTR ALN + SCZ NGN2 combination. This suggests, that SCZ ALN neurons are sufficient for the elevated activity (Fig. 6A). In the case of NGN2 neurons, we observed a gradual increase with significant differences only found in the combination of SCZ ALN and SCZ NGN2 neurons (Fig. 6B). Therefore, ALN neurons are necessary for increased activity of NGN2 neurons but are not sufficient per se. Additional NGN2-specific factors are required. Other parameters such as AUC, FWHM, and ΔF/F0 remained unchanged throughout all combinations (Supplementary Figure 13).
Equal numbers of CTR cells (n = 3) and SCZ cells (n = 4) derived from all individuals were added into two pools CTR and SCZ to be differentiated into ALN and NGN2 neurons, separately. For co-culture all four samples were combined to give yield to four combinations: CTR ALN + CTR NGN2, SCZ ALN + CTR NGN2, CTR ALN + SCZ NGN2 and SCZ ALN + SCZ NGN2. A, B Peak frequency analysis of calcium traces of spontaneously active ALN and NGN2 neurons. Kruskal-Wallis test with Dunn’s post-hoc test (*=p ≤ 0.05, **=p ≤ 0.01, ns=not significant). Following cell lines were included in the calcium imaging experiment: CTR1, CTR2, CTR3, SCZ1, SCZ2, SCZ4, SCZ5. A Peak frequency of ALN neurons (for each combination n = 16, CTR ALN + CTR NGN2 vs. SCZ ALN + CTR NGN2 p = 0.0337, CTR ALN + CTR NGN2 vs. CTR ALN + SCZ NGN2 p > 0.9999, CTR ALN + CTR NGN2 vs. SCZ ALN + SCZ NGN2 p = 0.01). B Peak frequency of NGN2 neurons (for each combination n = 16, CTR ALN + CTR NGN2 vs. SCZ ALN + CTR NGN2 p = 0.58, CTR ALN + CTR NGN2 vs. CTR ALN + SCZ NGN2 p = 0.2985, CTR ALN + CTR NGN2 vs. SCZ ALN + SCZ NGN2 p = 0.0019). C, D Quantification of excitatory synapse density (vGLUT1 + PSD95) on ALN neurons and NGN2 neurons in mixed co-cultures. Kruskal-Wallis test with Dunn’s post-hoc test (*=p ≤ 0.05, **=p ≤ 0.01, ***=p ≤ 0.001). Values were normalised to CTR ALN + CTR NGN2. Following cell lines were included in the synapse quantification experiment: CTR1, CTR2, CTR3, SCZ1, SCZ2, SCZ4, SCZ5. (C) Excitatory synapse density on ALN neurons (for each combination n = 14, CTR ALN + CTR NGN2 vs. SCZ ALN + CTR NGN2 p = 0.002, CTR ALN + CTR NGN2 vs. CTR ALN + SCZ NGN2 p = 0.0026, CTR ALN + CTR NGN2 vs. SCZ ALN + SCZ NGN2 p = 0.0008). (D) Excitatory synapse density on NGN2 neurons (for each combination n = 14, CTR ALN + CTR NGN2 vs. SCZ ALN + CTR NGN2 p = 0.0093, CTR ALN + CTR NGN2 vs. CTR ALN + SCZ NGN2 p = 0.0044, CTR ALN + CTR NGN2 vs. SCZ ALN + SCZ NGN2 p = 0.0103).
We also quantified morphological synapse densities (vGlUT1 + PSD95 in apposition) in all permutations. As shown in Fig. 4H, J, the comparison of the combination CTR ALN + CTR NGN2 to SCZ ALN + SCZ NGN2 showed a decrease in glutamatergic synapse density. Synapse densities of both intermediate combinations SCZ ALN + CTR NGN2 and CTR ALN + SCZ NGN2 were equally reduced both on ALN and NGN2 neurons suggesting that impaired synapse formation or stabilization in SCZ is a more general SCZ phenomenon not specific for the cell types under study (Fig. 6C, D).
Discussion
Here, we present a disease model that is potentially useful for the representation of prefrontal hypodopaminergic phenotypes in SCZ. Transcriptome analysis of dopaminergic SCZ neurons implies decreased DA signalling due to reduced expression of 1) genes required for dopaminergic neuron differentiation, 2) genes involved in DA synthesis and transport, 3) upregulation of DA degrading COMT, and 4) downregulation of the major inhibitory DRD2 autoreceptor. Remarkably, we observed strongly enhanced activity of dopaminergic and interestingly glutamatergic neurons in a co-culture model of both cell types. This effect appeared to be mitigated by a selective DRD2 agonist, though this was specifically noted in SCZ neurons. Mixed co-cultures (CTR vs SCZ) of DA and glutamatergic neurons further strengthen our hypothesis that the hypodopaminergic phenotype of SCZ neurons may explain both the reduced autoinhibition of DA neurons and the reduced inhibition of co-cultured glutamatergic neurons.
A major finding of the transcriptome analysis is the implied hypodopaminergic phenotype of dopaminergic neurons based on the downregulation of many genes involved in dopaminergic neuron development as well as in the synthesis or transport of DA. In the course of dopaminergic development, transcription factors such as FOXA2 and LMX1B are involved in the regulation of cell proliferation and early specification of dopaminergic midbrain neurons [42]. In the post-mitotic phase, the expression of NURR1 is crucial for proper development into mature dopaminergic neurons, and it is additionally required for the expression of genes involved in DA synthesis [43]. The downregulation of transcription factors such as FOXA2, LMX1B, and NURR1 that are essential for dopaminergic differentiation may therefore hint at an impaired differentiation capacity as an early SCZ disease mechanism. In this context, it is of note that decreased mRNA expression of NURR1 was identified in the PFC of SCZ patients’ post-mortem brains [44]. Likewise, Nurr1 deficient mice lack dopaminergic neurons [45]. Impaired development may also impact the functionality of the more mature nervous system. It is therefore conceivable that the expression of genes involved in the synthesis or transport of DA such as DAT become compromised. However, with respect to patients with SCZ this hypothesis is under dispute. A recent meta-analysis of post-mortem studies claimed that DAT expression is not altered in the PFC [46], while a PET imaging study reported increased DAT levels that were restricted to brain region BA 10, without alterations in other cortical regions [47].
Interestingly, transcriptome analysis revealed DRD2 as the most abundant DA receptor expressed in ALN neurons. DRD2 serves as an autoreceptor for feedback inhibition which decreases excitability, as well as the release of DA upon stimulation [48]. This effect was confirmed in our study by application of the selective DRD2 agonist Pramipexole which selectively rescued the hyperactive state of SCZ co-cultures to baseline levels, while CTR co-cultures did not respond. It is presently unclear why CTR cells do not respond to Pramipexole although DRD2 was considerably expressed. The observation is important since it demonstrates specificity of Pramipexole for SCZ samples. Eventually, CTR cells are resistant due to some kind of homeostasis after long-term Pramipexole application associated with altered intracellular signalling. We also found that elevated activity of SCZ NGN2 neurons was rescued by Pramipexole which let us assign their elevated activity to the functional expression of DRD2 receptors. This hypothesis is further strengthened by transcriptome analysis of NGN2-derived neurons indicating DRD2 expression in agreement with previous reports [49,50,51]. DRD2 was the dominant DA receptor expressed by NGN2 neurons exceeding each DRD1, DRD3, and DRD4 expression by a factor of approximately 10 (GEO accession number: GSE282524) [49]. While this confirms a potential direct effect of Pramipexole on NGN2 neurons, we cannot exclude an alternative possibility that Pramipexole exerts an indirect effect on SCZ NGN2 neurons by acting on ALN neurons, leading to reciprocal interactions between the two neuronal populations.
On the other hand, the mixed co-culture models in Fig. 6 suggested a putative intrinsic effect of SCZ NGN2 neurons in addition to reduced dopaminergic signalling through ALN neurons. An intrinsic effect of NGN2 neurons may be explained by reduced DRD2 expression in SCZ which was 20% of the CTR situation [49]. Alternatively, deregulated glutamate receptor expression in SCZ may account for increased activity of NGN2 neurons in SCZ. GRIA1 expression was increased in SCZ NGN2 neurons by 60%. Consequently, increased responsiveness to glutamate may account for increased activity similar to the situation found in epilepsy [52], which is frequently observed in SCZ patients [53]. It is noteworthy, that a shift from GRIN2A to GRIN2B expression was observed as found in patients with SCZ [54]. NGN2 neurons also expressed AMPA receptors (GRIA1, GRIA2, GRIA3, GRIA4) and metabotropic glutamate receptors (GRM1, GRM2, GRM3, GRM4, GRM5, GRM7, GRM8).
The use of iPSC-derived neurons for disease modelling benefits from patients-derived cell lines to represent the genomic repertoire of the patient. Many papers report the characterization of just one neuronal phenotype or of an undefined mixture of different cell types, both of which do not reflect the complex connectivity of the intact brain [55,56,57,58]. Our results clearly demonstrate the limitations of studying just one cell type in isolation. SCZ phenotypes in terms of synaptic or functional aberrations did not become apparent in dopaminergic or glutamatergic neurons grown in isolation. The observed disease-associated phenotypes were unique for the co-culture system indicating that mutual interactions of glutamatergic and dopaminergic neurons fundamentally change their phenotypes. While the interaction between glutamatergic and dopaminergic neurons has not been described so far in a SCZ co-culture model, other reports showed interactions between glutamatergic and GABAergic neurons [37, 59, 60]. It is of note that network oscillations were improved in the co-culture model [61] showing the advantages of more complex culture models.
Another critical consideration whether dopaminergic, iPSC-derived neurons represent populations of the SNc or of the VTA. Several studies have shown that GIRK2 is strongly expressed in dopaminergic neurons of the SNc, while Calbindin is predominantly expressed in dopaminergic neurons of the VTA [62, 63]. However, these markers are not mutually exclusive, and only different expression levels allow for the distinction between these two dopaminergic neuron populations [62, 64]. In the original ALN-induced dopaminergic differentiation protocol, Powell et al. demonstrated that ALN-induced neurons were predominantly comparable to SN neurons but also showed enrichments for VTA neurons [35]. In line with these observations, our ALN-induced neurons revealed the expression of both genes KCNJ6 (which encodes GIRK2) and CALB1 (which encodes Calbindin) as identified by transcriptome analysis. Therefore, ALN neurons cannot be precisely assigned to a brain subregion.
A surprising observation was the formation of aberrant vGLUT1/PSD95-positive morphological synapses formed by ALN neurons grown in isolation. We did not find glutamatergic synapses of ALN neurons in our co-culture model presumably due to the interaction between glutamatergic and dopaminergic neurons. This observation may be eventually explained by a less mature state of dopaminergic neurons grown in isolated cultures while interaction with glutamatergic neurons may promote the maturation of ALN neurons. Notably, we observed a reduction in excitatory synapse formation in our co-culture model, which is consistent with its classification as a synaptic disorder. In general, patients with SCZ display a reduction of grey matter volumes, especially in the PFC, which is assumed to be due to an excess loss of synapses [65]. This theory is further supported by several post-mortem and in vivo SCZ patient studies, which demonstrated reduced levels of pre- and postsynaptic density markers, such as for example the synaptic vesicle proteins Synaptophysin (SYP) and SV2A [66,67,68] suggesting aberrant synapse formation in the PFC. Similar observations have been reported in studies of iPSC-derived forebrain neurons, predominantly glutamatergic neurons, which demonstrated reduced neurite branching and impaired synapse formation in neuronal cultures derived from SCZ patients compared to CTR [58, 69, 70]. Both in vivo and in vitro studies of SCZ patients indicate an excessive synapse elimination during a critical phase of brain development, coinciding with the onset of SCZ symptoms in adolescence and young adulthood [71]. This mechanism is partially thought to be driven by various risk genes associated with excitatory and inhibitory synaptic signalling such as for example the glutamate receptor subunit GRIN2A and the metabotropic GABA receptor GABBR2 [72].
In summary, in this study, we present a new, iPSC-based model that offers the opportunity to study dopaminergic-glutamatergic neuron-neuron interactions in SCZ in more detail. It may support the study of hypodopaminergic phenotypes of the prefrontal cortex, which is suspected to account for the cognitive deficits and the negative symptoms of SCZ and which are hardly addressed by currently available therapeutic approaches.
Data availability
The data discussed in this publication have been deposited in NCBI’s Gene Expression Omnibus (GEO) [73] and are accessible through GEO Series accession number GSE275064 (https://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE275064).
Additional data supporting the findings of this study are available from the corresponding author upon request.
References
Kesby JP, Eyles DW, McGrath JJ, Scott JG. Dopamine, psychosis and schizophrenia: the widening gap between basic and clinical neuroscience. Transl Psychiatry. 2018;8:30.
Haddad PM, Correll CU. The acute efficacy of antipsychotics in schizophrenia: a review of recent meta-analyses. Ther Adv Psychopharmacol. 2018;8:303–18.
Geibl FF, Henrich MT, Oertel WH. Mesencephalic and extramesencephalic dopaminergic systems in Parkinson’s disease. J Neural Transm (Vienna). 2019;126:377–96.
Angrist B, Sathananthan G, Wilk S, Gershon S. Amphetamine psychosis: behavioral and biochemical aspects. J Psychiatr Res. 1974;11:13–23.
Lieberman JA, Kane JM, Alvir J. Provocative tests with psychostimulant drugs in schizophrenia. Psychopharmacology (Berl). 1987;91:415–33.
Carlsson A, Lindqvist M, Magnusson T. 3,4-Dihydroxyphenylalanine and 5-hydroxytryptophan as reserpine antagonists. Nature. 1957;180:1200.
Campden-Main BC, Wegielski Z. The control of deviant behavior in chronically disturbed psychotic patients by the oral administration of reserpine. Ann N Y Acad Sci. 1955;61:117–22.
Toda M, Abi-Dargham A. Dopamine hypothesis of schizophrenia: making sense of it all. Curr Psychiatry Rep. 2007;9:329–36.
Brisch R, Saniotis A, Wolf R, Bielau H, Bernstein HG, Steiner J, et al. The role of dopamine in schizophrenia from a neurobiological and evolutionary perspective: old fashioned, but still in vogue. Front Psychiatry. 2014;5:47.
Rao N, Northoff G, Tagore A, Rusjan P, Kenk M, Wilson A, et al. Impaired prefrontal cortical dopamine release in schizophrenia during a cognitive task: a [11C]FLB 457 positron emission tomography study. Schizophr Bull. 2019;45:670–9.
Townsend L, Pillinger T, Selvaggi P, Veronese M, Turkheimer F, Howes O. Brain glucose metabolism in schizophrenia: a systematic review and meta-analysis of (18)FDG-PET studies in schizophrenia. Psychol Med. 2023;53:4880–97.
Akil M, Pierri JN, Whitehead RE, Edgar CL, Mohila C, Sampson AR, et al. Lamina-specific alterations in the dopamine innervation of the prefrontal cortex in schizophrenic subjects. Am J Psychiatry. 1999;156:1580–9.
Sohal VS, Rubenstein JLR. Excitation-inhibition balance as a framework for investigating mechanisms in neuropsychiatric disorders. Mol Psychiatry. 2019;24:1248–57.
Cousineau J, Plateau V, Baufreton J, Le Bon-Jego M. Dopaminergic modulation of primary motor cortex: From cellular and synaptic mechanisms underlying motor learning to cognitive symptoms in Parkinson’s disease. Neurobiol Dis. 2022;167:105674.
Bahmani Z, Clark K, Merrikhi Y, Mueller A, Pettine W, Isabel Vanegas M, et al. Prefrontal Contributions to Attention and Working Memory. Curr Top Behav Neurosci. 2019;41:129–53.
Hurd YL, Suzuki M, Sedvall GC. D1 and D2 dopamine receptor mRNA expression in whole hemisphere sections of the human brain. J Chem Neuroanat. 2001;22:127–37.
Reynolds LM, Flores C. Mesocorticolimbic dopamine pathways across adolescence: diversity in development. Front Neural Circuits. 2021;15:735625.
Green SM, Nathani S, Zimmerman J, Fireman D, Urs NM. Retrograde labeling illuminates distinct topographical organization of D1 and D2 receptor-positive pyramidal neurons in the prefrontal cortex of mice. eNeuro. 2020;7:ENEURO.0194-20.2020.
Wei X, Ma T, Cheng Y, Huang CCY, Wang X, Lu J, et al. Dopamine D1 or D2 receptor-expressing neurons in the central nervous system. Addict Biol. 2018;23:569–84.
Abi-Dargham A, Mawlawi O, Lombardo I, Gil R, Martinez D, Huang Y, et al. Prefrontal dopamine D1 receptors and working memory in schizophrenia. J Neurosci. 2002;22:3708–19.
Karlsson P, Farde L, Halldin C, Sedvall G. PET study of D(1) dopamine receptor binding in neuroleptic-naive patients with schizophrenia. Am J Psychiatry. 2002;159:761–7.
Hirvonen J, van Erp TG, Huttunen J, Aalto S, Nagren K, Huttunen M, et al. Brain dopamine d1 receptors in twins discordant for schizophrenia. Am J Psychiatry. 2006;163:1747–53.
Goldman-Rakic PS, Castner SA, Svensson TH, Siever LJ, Williams GV. Targeting the dopamine D1 receptor in schizophrenia: insights for cognitive dysfunction. Psychopharmacology (Berl). 2004;174:3–16.
Abi-Dargham A, Rodenhiser J, Printz D, Zea-Ponce Y, Gil R, Kegeles LS, et al. Increased baseline occupancy of D2 receptors by dopamine in schizophrenia. Proc Natl Acad Sci USA. 2000;97:8104–9.
Silvestri S, Seeman MV, Negrete JC, Houle S, Shammi CM, Remington GJ, et al. Increased dopamine D2 receptor binding after long-term treatment with antipsychotics in humans: a clinical PET study. Psychopharmacology (Berl). 2000;152:174–80.
Sesack SR, Carr DB. Selective prefrontal cortex inputs to dopamine cells: implications for schizophrenia. Physiol Behav. 2002;77:513–7.
Zhang Y, Pak C, Han Y, Ahlenius H, Zhang Z, Chanda S, et al. Rapid single-step induction of functional neurons from human pluripotent stem cells. Neuron. 2013;78:785–98.
Das D, Sonthalia S, Stein OBG, Wahbeh MH, Feuer K, Goff L, et al. Insights for disease modeling from single-cell transcriptomics of iPSC-derived Ngn2-induced neurons and astrocytes across differentiation time and co-culture. BMC Biol. 2024;22:75.
Mattar P, Langevin LM, Markham K, Klenin N, Shivji S, Zinyk D, et al. Basic helix-loop-helix transcription factors cooperate to specify a cortical projection neuron identity. Mol Cell Biol. 2008;28:1456–69.
Keller AL, Binner A, Breitmeyer R, Vogel S, Anderle N, Rothbauer U, et al. Generation and characterization of the human induced pluripotent stem cell line NMIi010-A from peripheral blood mononuclear cells of a healthy 49-year old male individual. Stem Cell Res. 2021;54:102427.
Stock R, Vogel S, Mau-Holzmann UA, Kriebel M, Wust R, Fallgatter AJ, et al. Generation and characterization of human induced pluripotent stem cells lines from four patients diagnosed with schizophrenia and one healthy control. Stem Cell Res. 2020;48:101961.
Naldini L, Blomer U, Gage FH, Trono D, Verma IM. Efficient transfer, integration, and sustained long-term expression of the transgene in adult rat brains injected with a lentiviral vector. Proc Natl Acad Sci USA. 1996;93:11382–8.
Graham FL, Smiley J, Russell WC, Nairn R. Characteristics of a human cell line transformed by DNA from human adenovirus type 5. J Gen Virol. 1977;36:59–74.
Ho SM, Hartley BJ, Tcw J, Beaumont M, Stafford K, Slesinger PA, et al. Rapid Ngn2-induction of excitatory neurons from hiPSC-derived neural progenitor cells. Methods. 2016;101:113–24.
Powell SK, O’Shea C, Townsley K, Prytkova I, Dobrindt K, Elahi R, et al. Induction of dopaminergic neurons for neuronal subtype-specific modeling of psychiatric disease risk. Mol Psychiatry. 2023;28:1970–82.
Schildge S, Bohrer C, Beck K, Schachtrup C Isolation and culture of mouse cortical astrocytes. J Vis Exp. 2013.
Heider J, Stahl A, Sperlich D, Hartmann SM, Vogel S, Breitmeyer R, et al. Defined co-cultures of glutamatergic and GABAergic neurons with a mutation in DISC1 reveal aberrant phenotypes in GABAergic neurons. BMC Neurosci. 2024;25:12.
Love MI, Huber W, Anders S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 2014;15:550.
Domanskyi A, Alter H, Vogt MA, Gass P, Vinnikov IA. Transcription factors Foxa1 and Foxa2 are required for adult dopamine neurons maintenance. Front Cell Neurosci. 2014;8:275.
Fremeau RT Jr., Troyer MD, Pahner I, Nygaard GO, Tran CH, Reimer RJ, et al. The expression of vesicular glutamate transporters defines two classes of excitatory synapse. Neuron. 2001;31:247–60.
Yamaguchi T, Sheen W, Morales M. Glutamatergic neurons are present in the rat ventral tegmental area. Eur J Neurosci. 2007;25:106–18.
Tian L, Al-Nusaif M, Chen X, Li S, Le W. Roles of transcription factors in the development and reprogramming of the dopaminergic neurons. Int J Mol Sci. 2022;23:845.
Perlmann T, Wallen-Mackenzie A. Nurr1, an orphan nuclear receptor with essential functions in developing dopamine cells. Cell Tissue Res. 2004;318:45–52.
Xing G, Zhang L, Russell S, Post R. Reduction of dopamine-related transcription factors Nurr1 and NGFI-B in the prefrontal cortex in schizophrenia and bipolar disorders. Schizophr Res. 2006;84:36–56.
Kadkhodaei B, Ito T, Joodmardi E, Mattsson B, Rouillard C, Carta M, et al. Nurr1 is required for maintenance of maturing and adult midbrain dopamine neurons. J Neurosci. 2009;29:15923–32.
Fusar-Poli P, Meyer-Lindenberg A. Striatal presynaptic dopamine in schizophrenia, Part I: meta-analysis of dopamine active transporter (DAT) density. Schizophr Bull. 2013;39:22–32.
Sekiguchi H, Pavey G, Dean B. Altered levels of dopamine transporter in the frontal pole and dorsal striatum in schizophrenia. NPJ Schizophr. 2019;5:20.
Ford CP. The role of D2-autoreceptors in regulating dopamine neuron activity and transmission. Neuroscience. 2014;282:13–22.
Heider J, Gonzalez EP, Hartmann SM, Kannaiyan N, Vogel S, Wust R, et al. Aberrant neuronal connectivity and network activity of neurons derived from patients with idiopathic schizophrenia. Neurobiol Dis. 2024;201:106678.
Tian R, Gachechiladze MA, Ludwig CH, Laurie MT, Hong JY, Nathaniel D, et al. CRISPR Interference-Based Platform for Multimodal Genetic Screens in Human iPSC-Derived Neurons. Neuron. 2019;104:239–55 e12.
Sagar R, Azoidis I, Zivko C, Xydia A, Oh ES, Rosenberg PB, et al. Excitatory neurons derived from human-induced pluripotent stem cells show transcriptomic differences in Alzheimer’s patients from controls. Cells. 2023;12:1990.
Pfisterer U, Petukhov V, Demharter S, Meichsner J, Thompson JJ, Batiuk MY, et al. Identification of epilepsy-associated neuronal subtypes and gene expression underlying epileptogenesis. Nat Commun. 2020;11:5038.
Adachi N, Ito M. Epilepsy in patients with schizophrenia: Pathophysiology and basic treatments. Epilepsy Behav. 2022;127:108520.
Harrison PJ, Bannerman DM. GRIN2A (NR2A): a gene contributing to glutamatergic involvement in schizophrenia. Mol Psychiatry. 2023;28:3568–72.
Pak C, Danko T, Mirabella VR, Wang J, Liu Y, Vangipuram M, et al. Cross-platform validation of neurotransmitter release impairments in schizophrenia patient-derived NRXN1-mutant neurons. Proc Natl Acad Sci USA. 2021;118:e2025598118.
Wen Z, Nguyen HN, Guo Z, Lalli MA, Wang X, Su Y, et al. Synaptic dysregulation in a human iPS cell model of mental disorders. Nature. 2014;515:414–8.
Page SC, Sripathy SR, Farinelli F, Ye Z, Wang Y, Hiler DJ, et al. Electrophysiological measures from human iPSC-derived neurons are associated with schizophrenia clinical status and predict individual cognitive performance. Proc Natl Acad Sci USA. 2022;119:e2109395119.
Brennand KJ, Simone A, Jou J, Gelboin-Burkhart C, Tran N, Sangar S, et al. Modelling schizophrenia using human induced pluripotent stem cells. Nature. 2011;473:221–5.
Wang S, Rhijn JV, Akkouh I, Kogo N, Maas N, Bleeck A, et al. Loss-of-function variants in the schizophrenia risk gene SETD1A alter neuronal network activity in human neurons through the cAMP/PKA pathway. Cell Rep. 2022;39:110790.
Wang S, Hesen R, Mossink B, Nadif Kasri N, Schubert D. Generation of glutamatergic/GABAergic neuronal co-cultures derived from human induced pluripotent stem cells for characterizing E/I balance in vitro. STAR Protoc. 2023;4:101967.
Parodi G, Brofiga M, Pastore VP, Chiappalone M, Martinoia S. Deepening the role of excitation/inhibition balance in human iPSCs-derived neuronal networks coupled to MEAs during long-term development. J Neural Eng. 2023;20:056011.
Reyes S, Fu Y, Double K, Thompson L, Kirik D, Paxinos G, et al. GIRK2 expression in dopamine neurons of the substantia nigra and ventral tegmental area. J Comp Neurol. 2012;520:2591–607.
Chung CY, Seo H, Sonntag KC, Brooks A, Lin L, Isacson O. Cell type-specific gene expression of midbrain dopaminergic neurons reveals molecules involved in their vulnerability and protection. Hum Mol Genet. 2005;14:1709–25.
Carmichael K, Sullivan B, Lopez E, Sun L, Cai H. Diverse midbrain dopaminergic neuron subtypes and implications for complex clinical symptoms of Parkinson’s disease. Ageing Neurodegener Dis. 2021;1:10.20517.
Howes OD, Shatalina E. Integrating the neurodevelopmental and dopamine hypotheses of schizophrenia and the role of cortical excitation-inhibition balance. Biol Psychiatry. 2022;92:501–13.
Berdenis van Berlekom A, Muflihah CH, Snijders G, MacGillavry HD, Middeldorp J, Hol EM, et al. Synapse pathology in schizophrenia: a meta-analysis of postsynaptic elements in postmortem brain studies. Schizophr Bull. 2020;46:374–86.
Osimo EF, Beck K, Reis Marques T, Howes OD. Synaptic loss in schizophrenia: a meta-analysis and systematic review of synaptic protein and mRNA measures. Mol Psychiatry. 2019;24:549–61.
Lynch BA, Lambeng N, Nocka K, Kensel-Hammes P, Bajjalieh SM, Matagne A, et al. The synaptic vesicle protein SV2A is the binding site for the antiepileptic drug levetiracetam. Proc Natl Acad Sci USA. 2004;101:9861–6.
Breitmeyer R, Vogel S, Heider J, Hartmann SM, Wust R, Keller AL, et al. Regulation of synaptic connectivity in schizophrenia spectrum by mutual neuron-microglia interaction. Commun Biol. 2023;6:472.
Grunwald LM, Stock R, Haag K, Buckenmaier S, Eberle MC, Wildgruber D, et al. Comparative characterization of human induced pluripotent stem cells (hiPSC) derived from patients with schizophrenia and autism. Transl Psychiatry. 2019;9:179.
Habela CW, Song H, Ming GL. Modeling synaptogenesis in schizophrenia and autism using human iPSC derived neurons. Mol Cell Neurosci. 2016;73:52–62.
Trubetskoy V, Pardinas AF, Qi T, Panagiotaropoulou G, Awasthi S, Bigdeli TB, et al. Mapping genomic loci implicates genes and synaptic biology in schizophrenia. Nature. 2022;604:502–8.
Edgar R, Domrachev M, Lash AE. Gene Expression Omnibus: NCBI gene expression and hybridization array data repository. Nucleic Acids Res. 2002;30:207–10.
Acknowledgements
SMH and PPG were funded by the German Federal Ministry of Education and Research (grant no. 01EK2101A). JH, SV, RW, AJF, and HV were funded by the State of Baden-Wuerttemberg (grant no. AZ 35-4223.10/8) and German Center for Mental Health (DZPG), partner site Tübingen (grant no. 01EE2306B). LSW was funded by the German Research Foundation (DFG) (grant no. DFG VO 941/10-1). The pLV-FUdeltaGW-rtTA plasmid was a gift from Konrad Hochedlinger, the plasmid pLV-TetO-hNGN2-eGFP-Puro was a gift from Kristen Brennand, the pLV-TetO-ALN was a gift from John Gearhart and the pEF-Synaptophysin-mRuby plasmid was a gift from Edwin Chapman. We thank Aaron Stahl for performing hierarchical clustering analysis on our transcriptome data using the MeV software. We thank Frank Weise for critical comments.
Author information
Authors and Affiliations
Contributions
S.-M.H., J.H., L.-S.W., and H.V. designed the experiments. S.-M.H., J.H., S.V., L.-S.W., P. P.G. conducted experiments, collected and analyzed data. S.-M.H., J.H., S.V., and P.P.G. performed statistical analysis. S.-M.H., R.W., and H.V. wrote the manuscript. S.V. provided patient cell lines. S.-M.H., J.H., R.W., and A.J.F. reviewed data interpretation and manuscript. A.J.F. and H.V. were involved in project administration and funding.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hartmann, SM., Pizarro Garcia, P., Heider, J. et al. A co-culture model of dopaminergic and glutamatergic neurons derived from patients with idiopathic schizophrenia reveals a hypodopaminergic phenotype. Mol Psychiatry 31, 2376–2389 (2026). https://doi.org/10.1038/s41380-025-03384-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41380-025-03384-4