Abstract
Sonogenetics combines genetic tools and low-intensity ultrasound to non-invasively modulate specific neuronal populations and circuits, exhibiting potential for treating brain diseases. This study examines sonogenetics’ potential in a mouse depression model, targeting excitatory medial prefrontal cortex (mPFC) neurons projecting to the dorsal raphe nucleus (DRN). Projecting neurons were induced to express a mechanosensitive ion channel (MscL-G22S), and alterations in patterns of neuronal activation and despair-like behaviors upon sonication were evaluated. Sonogenetics selectively activated targeted excitatory mPFC neurons projecting to the DRN, enhancing real-time DRN neuronal activity and serotonin release, with no observed tissue damage or astrocytic/microglial activation. Tail suspension and forced swim tests revealed that sonogenetically activating this pathway rapidly reversed despair-like behaviors in stressed mice, whereas effects observed upon mPFC sonication were abrogated by functionally silencing downstream DRN neurons, and this effect is fully recapitulated by selective inhibition of DRN serotonergic neurons alone. Collectively, this study constitutes the first demonstration of the potential for a circuit-targeted sonogenetic therapeutic approach for relieving despair behaviors.
Similar content being viewed by others
Introduction
Major depressive disorder (MDD) is a common but debilitating mental disorder, affecting an estimated 3.8% of the population worldwide [1] and becoming the second-leading contributor to chronic disease burden in the past few decades [2]. MDD is typically characterized by a loss of interest in previously-rewarding activities and persistent despair, a major contributing factor to suicide [1]. It was reported in 2023 that more than 700,000 deaths result from suicide every year and that the highest mortality of unnatural causes was depression (30%) [3, 4]. The primary method of medically countering MDD’s devastating effects is the use of different classes of antidepressants; these include selective serotonin reuptake inhibitors (SSRIs), serotonin and norepinephrine reuptake inhibitors (SNRIs), monoamine oxidase inhibitors (MAOIs), and tricyclic antidepressants (TCAs). These drugs are understood to relieve depressive symptoms by increasing the availability of neurotransmitters, particularly serotonin (a.k.a., 5-HT), norepinephrine, and dopamine, in the central nervous system (CNS) [5]. Systematic reviews have shown that the response rates of all these antidepressants are around 50%, and several weeks are required for the effective onset of therapeutic effects [6, 7].
Simultaneously, several non-pharmacological modalities for more direct neuromodulation have also been under development, with some showing promise as alternative treatments for depression, particularly for patients unresponsive to antidepressant drugs. Some methods have obtained approval from the United States Food and Drug Administration (FDA), including electroconvulsive therapy (ECT), vagus nerve stimulation (VNS) (only for adults), and transcranial magnetic stimulation (TMS) [8]. While these approaches offer possible symptomatic relief to patients who cannot be helped pharmacologically, they each have important limitations, such as the risk of cognitive impairment or even long-lasting memory loss [8], surgical invasiveness [9], and long initiation time or even no response [10]. An important factor contributing to the generation of such side-effects is the inability to accurately target the neuromodulation to specific neuronal populations [11, 12]. This insight has led to newer neuromodulation techniques being specifically targeted at specific cell types or circuits that are abnormally altered in pathological states. An optogenetic approach that selectively activated excitatory neurons in the medial prefrontal cortex (mPFC - a central hub for processing cognitive and emotional information [13]), which project to the dorsal raphe nucleus (DRN, the major source of serotonin in the brain [14]) was shown to rapidly reverse despair-like states in rodents [15]. This study also implicated the neuronal pathway from the mPFC to the DRN as a potential intervention target for alleviating depression-related behaviors [15]. However, owing to the opacity of brain tissue, optogenetics requires optical fibers to be invasively implanted into the targeted brain regions to deliver light locally for the entire duration of the treatment, which hampers its clinical translation [16]. A neuromodulation method capable of combining the advantages of improved targeting - predictable and controllable antidepressant effects with rapid action and minimal side-effects - with greater non-invasiveness and fine spatiotemporal resolution could significantly accelerate the development of next-generation treatments.
Sonogenetics - a method analogous to optogenetics - uses low-intensity ultrasound to non-invasively manipulate specific neuronal populations and circuits by genetically inducing them to overexpress ultrasound-sensitive ion channels [17,18,19,20,21,22,23,24]. This recently-developed strategy is capable of manipulating neuronal activities and neurotransmitter release in specific neuronal populations and neural circuits [17,18,19,20,21,22,23,24]. Specifically, sonogenetics can affect mesoscale circuits, even in deeper brain regions, such as the ventral tegmental area (VTA)-nucleus accumbens (NAc) dopaminergic projection pathway [24]. This approach requires only the initial invasive delivery of genetic agents to the brain, while all subsequent ultrasound treatments are external. Moreover, by using ultrasound and microbubbles to open the BBB for AAV delivery, even this initial step could be rendered non-invasive, potentially paving the way for a fully non-invasive protocol. This offers a potential method of disease management with the added merits of non-invasiveness, selectivity, deep penetration, and fine spatiotemporal resolution [25]. However, this research is still in its early stages, and the feasibility and effectiveness of this approach, particularly with regard to depression-related circuitry, has not yet been comprehensively demonstrated in vivo. Putting together these facts, we hypothesized that a sonogenetic neuromodulation approach could be an effective candidate for non-invasively modulating depression-related circuitry, activating excitatory neurons from the mPFC to the DRN and alleviating despair-like behaviors.
In this study, we employed MscL-G22S—a gain-of-function mutant of the bacterial mechanosensitive channel of large conductance (MscL)—as a sonogenetic actuator to target the excitatory mPFC-to-DRN circuit. Unlike the wild-type MscL channel, which requires high-intensity membrane tension for activation, the MscL-G22S mutant possesses a lower mechanical threshold, enabling its precise gating with low-intensity ultrasound [24]. This sonogenetic approach was applied to a mouse model of depression induced via chronic restraint stress (CRS), and symptoms were monitored at the level of cellular signaling and behavioral tests. We found that sonogenetic modulation of the excitatory neuron in mPFC and increased DRN neuronal activity and serotonin release in real-time. Importantly, sonogenetic modulation of this circuit rapidly relieved despair-like behaviors in stressed mice, as reflected by spending less time immobile and more time struggling in tail suspension and forced swim tests, which are widely-employed measurements of despair-like behavioral states in rodents [26]. Furthermore, the functional silencing of downstream DRN neurons abrogated the anti-despair effects of sonogenetic modulation applied in the upstream mPFC, indicating that the specific and effective sonogenetic activation of this circuit was the major contributor to the observed effects. In addition, there was no sign of tissue damage or abnormal activation of microglia and astrocytes. Taken together, this study is the first attempt to ameliorate despair-like behaviors by sonogenetic modulation of specific neuronal circuits in rodents, laying the groundwork for the future development of new therapeutic methods for depression.
Materials and methods
Mice
All experiments were conducted on 8–12-week-old male C57BL/6 J mice. Mice were housed in the Centralized Animal Facilities (CAF) at the Hong Kong Polytechnic University. All animal experiments were approved by the Animal Subjects Ethics Sub-Committee (ASESC) of the Hong Kong Polytechnic University and were performed in compliance with the guidelines of the Department of Health-Animals (Control of Experiments) of the Hong Kong S.A.R. government.
Viral vectors
All viruses were obtained from BrainVTA, Wuhan, P.R.C., and were as prepared as follows: AAV2/9-CaMKIIα-DIO-MSCL-G22S-F2A-EGFP (titre: 5.34 × 1012 vg/ml), AAV2/9-CaMKIIα-DIO-EGFP (titre: 5.15 × 1012 vg/ml), AAV2/9-CaMKIIα-DIO-MSCL-G22S-F2A-mCherry (titre: 5.08 × 1012 vg/ml), AAV2/9-CaMKIIα-DIO-mCherry (titre: 5.40 × 1012 vg/ml), AAV2/retro-hSyn-Cre (titre: 5.45 × 1012 vg/ml), AAV2/9-hSyn-GCaMP6s (titre: 5.22 × 1012 vg/ml), AAV2/9-hSyn-5HT2.1 (titre: 2.93 × 1012 vg/ml), AAV2/9-hSyn-hM4D(Gi)-mCherry (titre: 5.25 × 1012 vg/ml), and AAV2/9-hSyn-mCherry (titre: 5.31 × 1012 vg/ml). Viruses were diluted to 1 × 1012 vg/ml, aliquoted, and stored at −80 °C until use.
Stereotaxic surgery
Mice were anesthetized with a ketamine/xylazine (100 mg/kg for ketamine and 10 mg/kg for xylazine) cocktail and then placed into a stereotaxic apparatus (RWD Life Science Co., Ltd., Shenzhen, China). The scalp was removed by a sterile surgical blade to expose bregma and lambda. After cleaning and leveling the skull, virus solution was injected, optical fibers implanted, or ultrasound collimators installed (as described in the sub-sections to follow). After all stereotaxic surgery, mice were immediately put on a heating pad until they awoke. Fiber photometry recording or behavioral tests were conducted on mice at least 7 days after surgery.
Virus injection
After cleaning and leveling the skull on the stereotaxic apparatus, a tiny hole in the skull was made with a micro drill (RWD Life Science Co., Ltd., Shenzhen, China) above the targeted brain area. To target excitatory neuron in the mPFC which project to DRN, monosynaptic retrograde transport virus encoding Cre recombinase under the control of the hSyn promoter (AAV2/retro-hSyn-Cre) was injected into the DRN (0.5 µL; AP, −4.4 mm; ML, 0 mm; DV, −3.4 mm) and Cre-dependent virus encoding MscL-G22S under the control of the CaMKIIα promoter (AAV2/9-CaMKIIα-DIO-MSCL-G22S-F2A-EGFP or AAV2/9-CaMKIIα-DIO-MSCL-G22S-F2A-mCherry) or the respective control (AAV2/9-CaMKIIα-DIO-EGFP or AAV2/9-CaMKIIα-DIO-mCherry) was injected into the mPFC (1 µL; AP, 1.8 mm from bregma; ML, ± 0.35 mm; DV, −2.0 mm) by a glass pipette at the rate of 0.1 µL/min. The glass pipette was left in place for an extra 5 min for infusion before withdrawing. For detecting calcium activity or serotonin release in the DRN, 0.5 µL AAV2/9-hSyn-GCaMP6s (a genetically-encoded calcium sensor with green fluorescence [27]) or AAV2/9-hSyn-5HT2.1 (a genetically-encoded GPCR-activation-based 5-HT sensor with green fluorescence [28]) was then infused into the DRN. For general neuronal chemogenetic inhibition, 0.5 µL AAV2/9-hSyn-hM4D(Gi)-mCherry or its control virus AAV2/9-hSyn-mCherry were infused into the DRN. For chemogenetic inhibition of serotonin neurons, a 1:1 mixture of AAV-Sert-Cre and either AAV2/9-CAG-DIO-hM4D(Gi)-mCherry or its control virus AAV2/9-CAG-DIO-mCherry was infused into the DRN, with a total injection volume of 0.5 μL. Mice were given at least 3 weeks for recovery post-surgery.
Optical fiber implantation
The head of the mice was fixed on the stereotaxic apparatus. A portion of the scalp was excised and a small hole in the skull was made with the micro driller above the DRN. Then, a black fiber optic cannula (model, FOC-B-1.25-200-0.37-3.5; Inper Co., Ltd., Zhejiang, China) was implanted into the DRN (AP, −4.4 mm from bregma; ML, 0 mm; DV, −3.35 mm) and fixed with dental cement.
Ultrasonic collimator installation
After being fixed on the stereotaxic apparatus, a portion of the scalp was excised above the mPFC. A customized wearable ultrasonic collimator was put onto the intact skull aligned with the targeted brain area and fixed with dental cement.
Ultrasound system and stimulation
The function generator’s output (AFG251, Tektronix Inc., Beaverton, USA) was connected to the input of the power amplifier (A075, Electronics & Innovation Ltd., Rochester, USA) via a BNC wiring, and the output of the amplifier was connected to customized wearable transducers. Then, the customized wearable transducer was installed into the collimator coupled with ultrasound gel. The two-dimensional acoustic field distribution was measured with a hydrophone. The parameters of ultrasound stimulation in this study were shown as follows: central frequency, 0.8 MHz; intensity, 0.15 or 0.3 MPa; pulse width, 500 µs; pulse repetition frequency, 1 kHz; stimulation duration, 300 ms; stimulation interval, 3 s. All behavioral tests were performed on awake mice.
Fiber photometry recording
Mice were anesthetized with 1 ~ 2% isoflurane. Eye ointment was applied to prevent corneal drying. A fiber-optic patch cord was used to connect the implanted fiber and the recording system (Thinker Tech Nanjing Biotech Co., Ltd., Nanjing, China). The excitation wavelength for GCaMP6s and 5-HT2.1 was 480 nm. Data was collected at 100 Hz and analyzed using a customized MATLAB script. The fluorescence change (ΔF/F) was calculated as (F-F0)/F0, where F0 is the baseline fluorescence signal.
Chemogenetic inhibition
Mice heterologously overexpressing hM4D(Gi)-mCherry or mCherry were subjected to a process of habituation, in which intraperitoneal (i.p.) injection with 100 µL saline was conducted daily for 1 week. Then, clozapine-N-oxide (CNO, Tocris, MO) was given (i.p., 1 mg/kg) 30 min or 3 days before the behavioral assessment.
Chronic restraint stress (CRS)
Mice were individually placed into a well-ventilated 50 ml conical tube for ~3 h per day for 14 consecutive days, and control mice stayed in their home cages. After each day of CRS, restrained mice were removed from the tube and immediately returned to their home cages [29].
Tail suspension test (TST)
Mice were suspended 25 cm above the horizontal floor for 6 min by fixing their tail with adhesive tape. An observer blinded to animal treatment groups videotaped and analyzed the animal behaviors offline. “Immobility time” was defined as the time when the body and all four limbs were still [30]. “Struggling time” was defined as the time when strong movements of body jerks and jumps were observed [30].
Forced swim test (FST)
Mice were individually placed into a Plexiglas cylinder (12 cm diameter, 25 cm height) containing water (24 ± 1 °C) to a depth of 10 cm and allowed to swim freely for 6 min. After each test, the cylinder was cleaned and refilled with fresh water. An observer blinded to animal treatments videotaped and analyzed the behaviors offline. “Immobility time” was defined as when the mouse was floating without any movement except for those necessary to keep the nose above water during the last 4 min [31]. “Struggling time” was defined as the time during which quick forelimb movements were observed such that the front paws broke the surface of the water during the last 4 min [31].
Open field test (OFT)
Mice were individually placed in the central area of a cubic plastic chamber (50 cm × 50 cm × 50 cm) and allowed to move freely for 6 min. Animal behaviors were videotaped and the speed of mice in the 6-min test session was measured with ToxTrac software by an observer blinded to animal treatment groups.
In vitro electrophysiological recordings
Mice were anesthetized with a ketamine/xylazine cocktail and transcardially perfused with ice-cold cutting NMDG-HEPES artificial cerebrospinal fluid (ACSF) containing in mM: 92 NMDG, 2.5 KCl, 1.2 NaH2PO4, 30 NaHCO3, 20 HEPES, 25 glucose, 2 thiourea, 5 Na-ascorbate, 3 Na-pyruvate, 0.5 CaCl2, and 10 MgSO4 (pH titrated to 7.3–7.4). Following experiments, the brain was quickly removed and cut into 300 µm-thick coronal sections in ice-cold cutting ACSF with a vibrating microtome (VT1200S; Leica Biosystems GmbH, Wetzlar, Germany). Sections containing the DRN were transferred to the holding HEPES ACSF (in mM): 92 NaCl, 2.5 KCl, 1.2 NaH2PO4, 30 NaHCO3, 20 HEPES, 25 glucose, 2 thiourea, 5 Na-ascorbate, 3 Na-pyruvate, 2 CaCl2, and 2 MgSO4, incubated at 32 °C for 10 min, and subsequently maintained at room temperature for 60 min before recording. During recording sessions, sections were transferred to a recording chamber with oxygenated recording ACSF (in mM): 124 NaCl, 2.5 KCl, 1.25 NaH2PO4, 24 NaHCO3, 12.5 glucose, 5 HEPES, 2 CaCl2, and 2 MgSO4 was continuously perfused. Neurons overexpressing hM4D(Gi)-mCherry were observed with an upright fluorescent microscope (Olympus, Japan). Borosilicate glass-made patch pipettes were used to record, which were pulled with a micropipette puller (P-97, Sutter Instrument Co., USA) to a resistance of 3 to 5 MO and filled with KCl pipette solution (in mM): 138 KCl, 10 NaCl, 1 MgCl2 and 10 HEPES with D-mannitol compensated for OSM 290. To confirm the hM4D(Gi)-mediated inhibitory effect on neurons in the DRN, action potentials were recorded by the current clamp configuration. After recording firing spikes for 3–5 min, 5 µM CNO (Tocris, MO) was bath-applied for 2 min followed by washout.
Immunofluorescence staining
Mice were anesthetized with a ketamine/xylazine cocktail. After anesthesia, mice were perfused with PBS (Cat. no., 70011044; Thermo Fisher Scientific Inc., Waltham, USA) followed by a 4% paraformaldehyde (PFA) solution (Cat. no., sc-281692; Santa Cruz Biotechnology Inc., California, USA), and brain was extracted and post-fixed with 4% PFA solution overnight at 4 °C. Coronal sections with a thickness of 40 µm were obtained from the fixed brain by a vibrating microtome (VT1200S; Leica Biosystems GmbH, Wetzlar, Germany). Slices were blocked with blocking solution (10% normal goat serum + 1% BSA + 0.3% Triton in 1× PBS) for 90 min at room temperature and incubated with prepared primary antibody solution against c-Fos (1:500; Cat. no., 2250; CST, Massachusetts, USA), Iba-1 (1:1000; Cat. no., 17198; CST, Massachusetts, USA), GFAP (1:1000; Cat. no., 12389; CST, Massachusetts, USA) or Tph2 (1:200; Cat. no., 51124, CST) overnight in a 4 °C refrigerator. The slices were then washed with 1× PBS (5 min each, 3 times). After washing, slices were incubated with anti-rabbit Alexa Fluor 488 or 633 secondary antibodies (1:1000; Thermo Fisher Scientific Inc., Waltham, USA) for 90 min at room temperature. The sections were then washed in PBS and mounted on glass by a mounting medium with DAPI (Cat. no., ab104139; Abcam, Cambridge, UK). The stained sections were visualized by Nikon Eclipse Ti2-E Fluorescence Imaging System or a confocal microscope (TCS SP8 MP; Leica Microsystems GmbH, Wetzlar, Germany) and analyzed by an observer blinded to the treatment groups with ImageJ.
Hematoxylin and eosin staining
Mice were anesthetized with a ketamine/xylazine cocktail. After anesthesia, mice were perfused with PBS followed by a 4% PFA solution. The brain tissue was extracted and post-fixed with 4% PFA solution for 24 h in a 4 °C refrigerator and then washed with PBS. Following experiments, brain tissues were dehydrated with successively higher concentrations of alcohol (70%, 80%, 90%, 95%, 100%), hyalinized with xylene, and embedded with paraffin. Coronal brain sections of 5 µm thickness were obtained from paraffin-embedded blocks with a microtome (Leica RM2235) and stained using a hematoxylin and eosin stain kit (Solarbio G1121). After staining, sections were re-dehydrated with the gradient alcohol, re-hyalinized with xylene, and mounted in resinene for microscopic observation.
Data analysis
The sample size per group was determined based on previous studies and in accordance with ethical principles that promote the 3Rs. No formal statistical methods were used to estimate sample size. Mice were randomly assigned to each conditioning group. No data points were excluded from the analyses. Throughout the experimental procedures and outcome evaluation, the investigator was blinded to group assignments. All figure legends include detailed descriptions of the statistical tests applied, justification for their use, and measures of variability within each group (mean ± SEM).
GraphPad Prism 7.0 was used to analyze data and generate figures. Schematic illustrations were prepared with CorelDRAW X8. Data were analyzed using two-tailed unpaired t-tests when 2 experimental groups were involved or two-way analyses of variance (ANOVA) with post-hoc Tukey testing when >2 groups were compared. Bar charts represent mean ± SEM. P values < 0.05 were considered statistically significant. * P < 0.05, ** P < 0.01, *** P < 0.001, **** P < 0.0001, n.s., not significant. All statistically significant relationships are shown on graphs.
Results
Wearable ultrasound system and characteristics
For this study, a wearable transducer was first customized. The transducer had a central frequency of 0.8 MHz and was fabricated using PZT-5H/Epoxy 1–3 composite material. Tungsten powder was mixed into the epoxy to fabricate the matching layer of the transducer. Its physical dimensions included an outer diameter of 7.8 mm, and the aluminum housing featured three protrusions designed to secure the transducer within the collimator (Fig. 1A and B). The collimator had a 5 mm aperture size (Fig. 1C). To drive the transducer, an electrical signal was generated with a function generator and amplified by a radio frequency (RF) amplifier, similar to our previous studies [32]. The transducer output intensity and the acoustic distribution profile were measured with a hydrophone scanning system, controlled by a 3D translational motor system (Fig. 1D). The lateral acoustic beam profile at 0.3 MPa output intensity, measured 2 mm away from the collimator surface, is shown in Fig. 1E. The collimator was installed on the mouse head so as to align the ultrasound beam with the mPFC right underneath, while the DRN was left uncovered by the collimator (Fig. 1F and G). Then, the customized wearable transducer was installed into the collimator, with ultrasound coupling gel filled in the intermediate space (Fig. 1H). The parameters of ultrasound stimulation in this study were: central frequency, 0.8 MHz; pulse width, 500 µs; pulse repetition frequency, 1 kHz; stimulation duration, 300 ms; stimulation interval, 3 s; pressure, 0–0.3 MPa (Fig. 1I).
A Schematic diagram of the ultrasonic transducer and collimator. “①” indicates the wearable customized ultrasonic transducer. “②” indicates the ultrasonic collimator. B Photograph for scale of the ultrasonic transducer and collimator. C Bottom view of the ultrasonic collimator (aperture size = 5 mm). D Schematic diagram of the transducer scanning platform. RF, radio frequency; ADC, analog-to-digital converter. E Distribution of the acoustic field of the transducer in the XY plane (0.3 MPa). F Photograph illustrating the location above the mPFC and DRN. G Photograph showing the ultrasonic collimator’s alignment with the mPFC without affecting the DRN. H Photograph illustrating the customized wearable transducer with collimator affixed to the head of a mouse, above the mPFC. I Illustration of the ultrasound temporal profile used in this study.
Sonogenetic modulation of DRN-projecting excitatory neurons in the mPFC enhances neuronal activity along this circuit
Previous studies, including our own, have shown that low-intensity ultrasound stimulation of neurons in the striatum or primary visual cortex with heterologously overexpressed MscL-G22S was sufficient to specifically trigger their activation and alter locomotion activity or induce vision in mice [23, 24]. We continued to use MscL-G22S (referred to as ‘MscL’) as a validated sonogenetic tool in the present study, to examine whether sonogenetics could specifically modulate the circuit from excitatory neurons in the mPFC to the DRN, considered strongly correlated with depression [15]. First, monosynaptic retrograde transport virus encoding Cre recombinase under the control of the hSyn promoter (AAV2/Retro-hSyn-Cre, which permits efficient retrograde access to projection neurons [33]) was delivered into the DRN and Cre-dependent virus encoding MscL under the control of the CaMKIIα promoter (AAV-CaMKIIα-DIO-MscL-mCherry, which induces overexpression in specific neuronal populations via Cre-activated “DIO” switch [34]) into the mPFC. An empty vector without MscL was used as a control (Ctrl), and an appropriate fluorescent reporter was chosen to avoid overlap with the genetic sensor (Fig. 2A and E). This combination allowed selective overexpression of the MscL channel in DRN-projecting excitatory neurons in the mPFC. The DRN was also made to express GCaMP6s, a genetically-encoded calcium sensor [27], or 5-HT2.1, a genetically-encoded serotonin sensor [28].
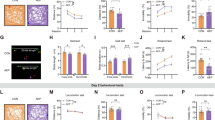
A Schematic illustration of viral transduction and fiber photometry recording of calcium activity in the DRN during sonication of the mPFC. B Left: representative image showing MscL-expressing neurons (red) and DAPI (blue) in the mPFC (scale bar = 200 µm); Right: representative image showing the axon terminals from MscL-expressing neurons of the mPFC (red), Ca2+ sensor GCaMP6s (green), and DAPI (blue) in the DRN (scale bar = 200 µm). C Left: representative traces of GCaMP6s fluorescence changes in MscL (red) and Ctrl (blue) groups upon multiple 0.3 MPa ultrasound stimuli; Right: averaged GCaMP6s fluorescence signals shown in left panel. D Averaged peak change of GCaMP6s fluorescence (Peak ∆F/F) in response to 0, 0.15, 0.3 MPa ultrasound stimulation. n = 3 mice per group. E Schematic illustration of viral transduction and fiber photometry recording of 5-HT release in the DRN during sonication of the mPFC. F Left: Representative image showing MscL-expressing neurons (red) and DAPI (blue) in the mPFC (scale bar = 200 µm); Right: representative image showing the axon terminals from MscL-expressing neurons of the mPFC (red), 5-HT2.1 (green), and DAPI (blue) in the DRN (scale bar = 200 µm). G Left: representative traces of 5-HT2.1 fluorescence change in the MscL (red) and Ctrl (blue) groups upon multiple 0.3 MPa ultrasound stimuli; Right: averaged 5-HT2.1 fluorescence signal from the left panel. H Averaged peak change of 5-HT2.1 fluorescence (Peak ∆F/F) in response to 0, 0.15, 0.3 MPa ultrasound stimulation. n = 3 mice per group. I Representative images of c-Fos levels in the mPFC and DRN at low magnification and high magnification. White arrows indicate c-Fos signals in MscL-expressing mPFC neurons, or c-Fos positive DRN neurons surrounded by axon terminals of projecting mPFC MscL-expressing neurons. J Counts of c-Fos positive cells imaged in the mPFC. n = 6 mice per group. K Counts of c-Fos positive cells imaged in the DRN. n = 6 mice per group.
To confirm the sonogenetic modulation of this circuit specifically, an ultrasound transducer was assembled above the mPFC, and calcium activity (GCaMP6s) or 5-HT release (5-HT2.1, a genetically-encoded GPCR-activation-based 5-HT sensor with green fluorescence) in the DRN were monitored in real-time through an implanted optical fiber during sonication of the mPFC. Fluorescence imaging showed the presence of MscL-expressing neurons in the mPFC, with the axon terminals in the DRN co-expressing the calcium sensor (Fig. 2B). Before ultrasound stimulation, MscL and Ctrl groups exhibited comparable levels of GCaMP6s baseline fluorescence (Fig. 2C and D). Ultrasound stimuli of 0.3 MPa repeatedly induced synchronous and reversible elevation of GCaMP6s fluorescence intensity in the MscL group with sub-second latency, while the Ctrl group showed no obvious responses (Fig. 2C). The peak fluorescence change in the MscL group was significantly higher than the Ctrl at 0.3 MPa stimulation (Peak ΔF/F, Ctrl vs. MscL: 0.070 ± 0.013% vs. 0.240 ± 0.016%, p = 2.90 × 10−5, Fig. 2D), indicating specific activation of the selected neurons and neural pathways. To further test the possible neural type in expressing GCaMP6s under hSyn promoter, brain sections containing DRN were processed for immunofluorescence using a primary antibody against Tryptophan Hydroxylase 2 (Tph2), a specific marker for serotonin neurons. Quantitative analysis revealed a high degree of colocalization, with the majority of GCaMP6s-expressing neurons also positive for Tph2 (90.75 ± 2.63%, SI Appendix, Fig. S1). This confirms successful targeting of the serotonergic population in the DRN.
Following the lead of previous studies demonstrating that the activation of DRN neurons increases the release of 5-HT in the CNS [28, 35], we also recorded 5-HT sensor fluorescence changes during sonogenetic stimulation (Fig. 2E). Fluorescent imaging showed the presence of MscL-expressing neurons in the mPFC, with the axon terminals in the DRN co-expressed with the 5-HT sensor (Fig. 2F). Pre-ultrasound, both groups showed comparable levels of 5-HT sensor fluorescence (Fig. 2G and H) but ultrasound stimuli (0.3 MPa) could induce repeatable, synchronous and reversible increases in fluorescence intensity in the MscL group with sub-second latency, but not in the Ctrl group (Fig. 2G). The peak 5-HT sensor fluorescence change in the MscL group was significantly higher than the Ctrl with 0.3 MPa ultrasound stimulation (Peak ΔF/F, Ctrl vs. MscL: 0.088 ± 0.023% vs. 0.404 ± 0.038%, p = 7 × 10−6, Fig. 2H). Thus, we found that 0.3 MPa ultrasound stimuli delivered to the DRN-projecting excitatory neurons in the mPFC induced sub-second, repeatable and reversible activity in the downstream DRN neurons in real-time.
To further verify sonogenetic activation of neurons in the mPFC and DRN, we examined relative levels of c-Fos expression. c-Fos is a well-established molecular marker of activated neurons, thought to interact with other genes and mediate long-term changes in neural functioning [36]. After sonogenetic modulation at 0.3 MPa for 20 min, we found that the number of c-Fos positive neurons in the mPFC in the MscL+US group was significantly higher than in Ctrl or -US groups (c-Fos positive cells for Ctrl-US = 17 ± 3.54, MscL-US = 21 ± 4.13, Ctrl+US = 32 ± 5.83, MscL+US = 119 ± 6.67, Fig. 2I and J). Similarly, c-Fos levels in the DRN were significantly elevated in the MscL+US group compared to all others (c-Fos positive cells for Ctrl-US = 11 ± 1.84, MscL-US = 14 ± 2.47, Ctrl+US = 22 ± 3.16, MscL+US = 76 ± 3.14, Fig. 2I and K), likely because of the excitatory projections from the mPFC to this brain region and enhance the neural activity in DRN. To assess the broader projection targets of sonogenetically modulated mPFC neurons, we measured neural activity (via c-Fos) in several downstream regions: the nucleus accumbens (NAc), hippocampus (HIP), basolateral amygdala (BLA), ventral tegmental area (VTA), and central amygdala (CeA). This analysis revealed a specific engagement of the CeA. Animals expressing MscL showed a significantly higher density of c-Fos⁺ cells in the CeA compared to controls, whereas no significant changes were observed in the NAc, HIP, BLA, or VTA (SI Appendix, Fig. S2A-G).
To identify the phenotype of activated DRN neurons, we performed dual immunofluorescence for c-Fos and the serotonergic marker Tph2. Quantification showed that 29.91 ± 3.34% of all c-Fos⁺ neurons in the DRN were Tph2-positive (SI Appendix, Fig. S2H). Moreover, the proportion of activated (c-Fos⁺) serotonergic neurons was significantly higher in the MscL group than in the control group.
In addition, to control for potential auditory confounds, we compared c-Fos levels in the auditory cortex between Ctrl and MscL groups following ultrasound stimulation. No significant difference was found (SI Appendix, Fig. S3), indicating that auditory effects are unlikely to be a contributing factor to the observed mPFC-DRN circuit regulation. Collectively, these data demonstrate that sonogenetic activation of DRN-projecting mPFC excitatory neurons selectively enhances neuronal activity within this specific pathway.
Sonogenetic modulation of DRN-projecting excitatory neurons in the mPFC rapidly alleviates despair-like behaviors in stressed mice
Having observed that 0.3 MPa ultrasound stimulation of DRN-projecting, MscL-expressing excitatory mPFC neurons enhanced neuronal activity and serotonin release in the DRN, we next wanted to investigate whether this sonogenetic approach could correspondingly affect changes in despair-like behaviors in awake mice. A chronic restraint stress (CRS) mouse model of depression was used, which has been demonstrated to induce alterations similar to depressive patients at molecular and behavioral levels [37]. After being subjected to CRS for 14 days, mice robustly exhibited despair-like behaviors, reflected by spending more time immobile and less time struggling in the tail suspension test (TST) and forced swim test (FST) (SI Appendix, Fig. S4).
Following model establishment, we observed the effects of sonogenetically modulating DRN-projecting excitatory mPFC neurons on despair-like behaviors in stressed mice (Fig. 3A). The ultrasound stimulation protocol involved a 15 min pre-stimulation session targeting the mPFC, followed by a 6 min session administered during the behavioral tests (TST and FST). The cumulative ultrasound exposure time was therefore 21 min. MscL-expressing neurons in the mPFC and their axon terminals in the DRN were observed (Fig. 3B), indicating successful selective overexpression. MscL+US mice spent significantly less time immobile (immobile duration for Ctrl-US = 127 ± 14.33 s, MscL-US = 131 ± 12.86 s, Ctrl+US = 122 ± 12.97 s, MscL+US = 59 ± 6.72 s, Fig. 3D) and more time struggling (struggle duration for Ctrl-US = 55 ± 6.88 s, MscL-US = 62 ± 6.80 s, Ctrl+US = 65 ± 6.03 s, MscL+US = 101 ± 7.39 s, Fig. 3E) in the TST (Fig. 3C) than the MscL-US group and both Ctrl groups. Similarly, mice in the MscL+US group also exhibited reduced immobility time (immobile duration for Ctrl-US = 143 ± 10.97 s, MscL-US = 132 ± 9.31 s, Ctrl+US = 138 ± 8.40 s, MscL+US = 75 ± 7.61 s, Fig. 3G) and more struggling time (struggle duration for Ctrl-US = 51 ± 6.74 s, MscL-US = 59 ± 6.44 s, Ctrl+US = 57 ± 5.48 s, MscL+US = 93 ± 6.94 s, Fig. 3H) in the FST (Fig. 3F). However, sonogenetic modulation of the broader excitatory mPFC neuron population had no obvious changes in despair-like behaviors (SI Appendix, Fig. S5), highlighting the importance of specific activation of the mPFC-DRN pathway.
A Schematic illustration of viral transduction and ultrasound stimulation protocols. CRS was administered ~3 h/day for 14 days. 0.3 MPa ultrasound stimulation was applied starting 15 min before behavioral tests until the end of 6 min test sessions in awake mice. B MscL-expressing neurons (red) in the mPFC (left; scale bar = 200 µm) and their axon terminals in the DRN (right; scale bar = 200 µm). C Illustration of immobility and struggling behaviors of mice in the TST. D Mean TST immobility time displayed by mice in each group. E Mean TST struggling times displayed by mice in each group. F Illustration of immobility and struggling behaviors of mice in the FST. G Mean FST immobility time displayed by mice in each group. H Mean FST struggling time displayed by mice in each group. I Schematic illustration of OFT box setup (50 × 50 × 50 cm). J Representative locomotion traces of mice from each group. K Mean calculated velocity of mice in each group.
The open field test (OFT) revealed no significant differences in locomotor activity among the four groups (Fig. 3I-K), which rules out motor performance as a confounding factor in the despair-like behaviors observed in the TST and FST. Furthermore, the absence of a significant increase in center area duration—as corroborated by the representative movement traces—indicates that the antidepressant-like effect is not mediated by a reduction in anxiety-like behavior. Taken together, these results indicate that sonogenetic modulation of DRN-projecting excitatory neurons in the mPFC enhanced neuronal activity along this circuit, thereby alleviating despair-like behaviors.
DRN neurons are necessary to alleviate despair-like behaviors through sonogenetic neuromodulation of the mPFC-DRN circuit
We observed that sonogenetic modulation of DRN-projecting excitatory neurons in the mPFC increased neuronal activity along the circuit and reversed despair-like behaviors. To further ascertain the role of DRN neurons in mediating this effect, the circuit was blocked downstream of the site of stimulation by chemogenetically inhibiting the activity of DRN neurons. Briefly, DRN-projecting mPFC excitatory neurons were transduced with MscL and the activity of DRN neurons was controlled via a chemogenetic approach. AAVs encoding engineered Gi-coupled hM4D receptor under the hSyn promoter (AAV-hSyn-hM4D-mCherry) were delivered into the DRN (Fig. 4A) and clozapine-N-oxide (CNO) was injected intraperitoneally to activate the hM4D receptor, thereby engaging the Gi signaling pathway and inhibiting DRN neuronal activity [38]. The presence of MscL-expressing mPFC neurons and their axon terminals surrounding hM4D-overexpressing DRN neurons were observed via fluorescent microscopy (Fig. 4B). To validate the efficacy of hM4D(Gi)-mediated neuronal inhibition, we performed patch-clamp recordings on acute brain slices. The recordings showed that application of CNO induced a significant reduction in baseline neuronal activity compared to the pre-CNO baseline. This suppression was reversible upon washout, with activity returning to baseline levels, thereby confirming the successful and reversible function of the chemogenetic tool (Fig. 4C and D).
A Schematic illustration of the viral transduction scheme. B Representative images in the mPFC (left, MscL-expressing neurons = green, scale bar = 200 µm) and the DRN (right, hM4D-expressing DRN neurons = red; axon terminals from MscL-expressing DRN-projecting mPFC neurons = green, scale bar = 200 µm). C DIC, fluorescent, and merged images of recorded hM4D-expressing DRN neurons (scale bar = 10 µm) in ex vivo patch clamp experiments. D Representative traces showing the inhibitory effects of CNO on hM4D-expressing DRN neurons. E Mean TST immobility time of different groups. F Mean TST struggling time of different groups. G Mean FST immobility time of different groups. H Mean FST struggling time of different groups. I Mean OFT velocities of different groups. For panels E-I, n = 6 mice per group.
Following this, despair-like behaviors during sonogenetic modulation of the mPFC-to-DRN pathway were examined in stressed mice. In behavioral tests in vivo, no significant differences were found in baseline despair-like behaviors between mCherry and hM4D (with CNO) without ultrasound stimulation (mCherry-US and hM4D-US) (Fig. 4E-H). However, upon ultrasound stimulation following 30 min of CNO administration, hM4D mice exhibited significantly more immobility time in the TST (hM4D+US (30 min post CNO) vs. mCherry+US (30 min post CNO): 131 ± 8.11 s vs. 60.33 ± 6.91 s, p = 0.00011, Fig. 4E) and less struggling time (hM4D+US (30 min post CNO) vs. mCherry+US (30 min post CNO): 55.83 ± 7.01 s vs. 98.67 ± 7.58 s, p = 0.0099 Fig. 4F). Similarly, in the FST, the hM4D+US (30 min post CNO) group spent significantly more time immobile (hM4D+US (30 min post CNO) vs. mCherry+US (30 min post CNO): 125.3 ± 8.40 s vs. 64.17 ± 7.11 s, p = 0.0003, Fig. 4G) and less time struggling (hM4D+US (30 min post CNO) vs. mCherry+US (30 min post CNO): 58.17 ± 5.59 s vs. 106.70 ± 5.70 s, p = 0.0002, Fig. 4H). These results indicate that artificially silencing the neuronal activity of DRN neurons blocked the anti-despair effects of sonogenetic neuromodulation along the mPFC-DRN circuit. Furthermore, when neurons were allowed 3 days to metabolize the CNO and then stimulated with ultrasound, hM4D and mCherry groups showed comparable immobility and struggling times in both tests, indicating that the observed changes in the hM4D group were not due to damage from the chemogenetic treatment (Fig. 4E-H). This point was emphasized by post-experiment OFTs, which showed no significant differences in the general locomotion ability among these groups (Fig. 4I).
Next, to test whether serotonin neurons are required for the behavioral effects of sonogenetic mPFC-DRN circuit modulation, we used a combined viral approach. A 1:1:1 mixture of three viral vectors—AAV2/retro-hSyn-Cre, AAV-Sert-Cre and either AAV-DIO-hM4D-mCherry or AAV-DIO-mCherry—was injected into the dorsal raphe nucleus (DRN) to achieve Cre-dependent expression of the inhibitory designer receptor hM4D or the control fluorophore mCherry specifically in serotonin neurons. While the AAV-CaMKIIα-DIO-MscL-EGFP viral vector was injected in the mPFC region (SI Appendix, Fig. S6A). At baseline, without ultrasound stimulation, no significant difference in despair‑like behavior was observed between Sert‑Cre & DIO-mCherry mice and Sert‑Cre & DIO-hM4D mice treated with CNO. However, upon ultrasound stimulation following 30 min of CNO administration, Sert‑Cre & DIO-hM4D mice showed obviously more immobility time in the TST time and less struggling time in the TST test compared to the Sert‑Cre & DIO-mCherry mice (SI Appendix, Fig. S6 B, C). Taken together, these data show that inhibiting serotonin neurons abrogated the anti-despair effects of sonogenetically modulating the mPFC-DRN circuit.
This finding indicates that the observed effects of the MscL-mediated sonogenetic stimulation in the present study were effectuated through the specific activation of the mPFC-DRN circuit, and underlines the ability of this approach to stimulate the targeted neuronal population, activate specific mesoscale neuronal circuits, and elicit changes in behavior patterns, which may be beneficial in the disease context.
Sonogenetic modulation is safe at the cellular and tissue levels
To assess the safety of sonogenetic modulation at the cellular level, we performed immunostaining for microglia and astrocyte markers following 20 min of ultrasound stimulation (central frequency, 0.8 MHz; intensity, 0.15 or 0.3 MPa; pulse width, 500 µs; pulse repetition frequency, 1 kHz; stimulation duration, 300 ms; stimulation interval, 3 s). Specifically, we stained for ionized calcium-binding adapter molecule 1 (Iba1), a biomarker for microglia [39], and glial fibrillary acidic protein (GFAP), a biomarker for astrocytes [40]. The abnormal activation of these cell types has been identified as an early indicator of adverse inflammatory responses [41]. As shown in Fig. 5 A-C and SI Appendix, Fig. S7, there was no significant difference in the number or morphology of astrocytes and microglia among the groups MscL+US, Ctrl+US, MscL-US, and Ctrl-US groups, indicating there are no severe inflammatory responses after sonogenetic modulation. Brain sections containing the mPFC were procured and stained with H&E to examine the safety of our sonogenetic approach at a tissue level. Neuronal axons were found to be clear without signs of loss or damage after sonogenetic modulation (Fig. 5D). No abnormal alterations in the morphology of neurons were observed, nor any detectable tissue damage after sonogenetic neuromodulation. In addition, to evaluate the effects of higher sonication intensity, we applied ultrasound at NUS, 0.3 MPa and 0.5 MPa targeted to the mPFC. We assessed neuroinflammation using Iba1 immunostaining, analyzing both the relative number and morphology of microglia in the mPFC, DRN, and the cortical region directly above the mPFC. Even at the higher sonication intensity, no significant inflammatory response was observed (SI Appendix, Fig. S8), indicating that the 0.3 MPa exposure is safe. Taken together, these results suggest that the outlined sonogenetic modulation approach was capable of activating the targeted neuronal populations without inducing obvious microglial/astrocytic activation or tissue damage.
A Representative images of GFAP (upper panel, red) and Iba1 (lower panel, green) in the mPFC (scale bar = 100 µm). B Mean counts of GFAP-positive cells per slice in the mPFC. n = 4 mice per group. C Mean counts of Iba1-positive cells per slice in the mPFC. n = 4 mice per group. D H&E staining imaged in the mPFC with low magnification (scale bar = 100 µm) and high magnification (scale bar = 20 µm). n = 1 mouse per group.
Discussion
The present study attempts, for the first time, to utilize sonogenetic modulation as a novel therapeutic modality in the context of depression. We found that non-invasive ultrasound stimulation of DRN-projecting excitatory mPFC neurons, heterologously made to express MscL-G22S, enhanced real-time neuronal activity and serotonin release in the DRN. We observed calcium and serotonin responses in the DRN closely synchronous with ultrasound stimuli (sub-second responses), and these responses were repeatable and reversible. Crucially, we also demonstrated that sonogenetic modulation of DRN-projecting excitatory neurons in the mPFC specifically enhanced the activity of this neuronal circuit and alleviated despair-like behaviors in stressed mice, without any sign of tissue damage or abnormal activation of microglia or astrocytes. Functionally silencing downstream DRN neurons and serotonin neurons abrogated the effects during sonogenetic stimulation of the mPFC, suggesting that sonogenetic activation of this circuit was the major mechanism underlying the observed behavioral effects. Taken together, we lay the groundwork for a new strategy to ameliorate despair states and, potentially, other brain diseases.
In the present study, our low-intensity sonogenetic stimulation method activated a targeted mesoscale circuit from the mPFC to the DRN and rapidly rescued despair-like behaviors, without obvious activation of other brain areas or glial cells. The top-down control of serotonin systems by the prefrontal cortex is a typical pathway strongly associated with depression [42]. However, due to the complicated profile of endogenous expression of mechanosensitive ion channels, even when using sonogenetic neuromodulation and focusing on the same circuit as previously reported, it remains a challenge to straightforwardly replicate the results observed in optogenetic stimulation studies or other similar research. Several studies suggest that ultrasound stimulation alone (consecutive stimulation over weeks) without genetic modification has a positive effect on depressive behaviors in rodents and humans (refer to the recent review for details [43]). However, given the mixed and ambiguous spatial profile of endogenous ultrasound-responsive ion channels in the brain, it is challenging to achieve specific, targeted bioeffects or interpret clear mechanisms underlying behaviors through such an approach [43, 44]. In sonogenetic neuromodulation, exogenous overexpression of mechanosensitive ion channels into targeted neuronal populations can help sensitize them to ultrasound stimulation at even lower intensities than ultrasound alone, thereby achieving relative specificity [45]. Both ultrasound stimulation alone and sonogenetic modulation have their advantages and disadvantages.
The present proof-of-concept study demonstrated that a single round of sonogenetic modulation of DRN-projecting excitatory mPFC neurons rapidly reversed despair-like states in mice, providing a foundation for further research. In this real-time condition, we controlled, to the greatest possible extent, ultrasound parameters to minimize off-target effects. The promising acute effects reported here naturally lead to questions about chronic application. For this sonogenetic strategy to have clinical relevance, its long-term safety and efficacy must be unequivocally established. Future investigations will need to determine the stability of neuronal MscL expression over months and assess whether repeated ultrasound delivery elicits any subtle tissue alterations or glial reactivity. Furthermore, it will be crucial to monitor for behavioral adaptations, such as tolerance to the antidepressant effect. Successfully navigating these translational milestones is essential for advancing this neuromodulation approach toward potential use in treating enduring neuropsychiatric conditions. This study demonstrates that activating the mPFC-DRN pathway rapidly alleviates despair-like behaviors, coinciding with increased serotonin release in the mPFC. While this supports a role for serotonin in the observed effect, the ongoing debate reminds us that depression’s neurobiology extends beyond a single neurotransmitter [61]. Our findings suggest a more nuanced circuit-based mechanism: top-down cortical control over the DRN can regulate depressive-like states, potentially by modulating downstream serotonergic and possibly non-serotonergic systems.
Over a decade ago, it was reported that deep brain stimulation (DBS) of the mPFC improved depression-related behaviors, and this improvement was entirely abrogated when serotonin was depleted in a rat model of depression [46]. However, the antidepressant-like effects of DBS varied as a function of stimulation parameters and targets [47]. DBS has been developed for many years and has shown treatment efficacy in treatment-resistant depression (TRD), but the inconsistent findings reported by clinical studies hinder its advance in clinical practices [8, 48]. The inter-individual response heterogeneity, at least in part, contributes to this controversial observation [11]. Recently, a closed-loop deep brain stimulation (CLS) study in one patient with treatment-resistant depression involved implanting focal electrical stimulation electrodes and intracranial electrophysiology recording systems to identify personalized symptom-specific biomarkers and treatment sites [11]. This was followed by the implantation of a NeuroPace responsive neurostimulation system to continuously sense neural activity and deliver electrical stimulation triggered by pre-specified patterns of neuronal activities, resulting in rapid and sustained depression amelioration [11]. A clinical trial investigating CLS in a broader population of depression is ongoing (ClinicalTrials.gov, NCT04004169). Sonogenetic modulation could further be utilized with other techniques, such as functional magnetic resonance imaging (fMRI), to identify personalized, symptom-specific brain areas and provide tailored treatments. It is also suitable for development into a CLS technique, where adjustable ultrasound is output based on monitoring patients’ clinical conditions.
In this study, we demonstrated that sonogenetic neuromodulation of DRN-projecting excitatory neurons in the mPFC rapidly induced neuronal activity and serotonin release, leading to an acute reversal of despair-like states in mice. There is substantial evidence supporting the role of the medial prefrontal cortex (mPFC) in the etiology and treatment of depression in both rodents [49] and humans [50]. The mPFC projects to various downstream brain regions, producing diverse and sometimes opposing effects. For instance, optogenetic activation of DRN-projecting excitatory neurons has been shown to reverse despair-like states in rodents, while activation of lateral habenula (LHb)-projecting excitatory neurons induces despair-like effects [15]. This underscores the importance of selectivity in targeting specific neuronal pathways. In addition, previous studies have highlighted that subregions of the mPFC differentially modulate dorsal serotonergic activities [51]. The infralimbic (IL) and prelimbic (PrL) cortices, parts of the mPFC in rodents, are analogous to the ventral anterior cingulate cortex (vACC) and dorsolateral prefrontal cortex (PFC) in humans, respectively [52,53,54]. It was reported that an acute pharmacological increase in glutamatergic neurotransmission selectively in the infralimbic (IL, part of the mPFC) rather than the prelimbic (PrL, part of the mPFC) cortex triggered immediate antidepressant-like responses in rats [55]. This was associated with the activation of IL-raphe pathways, resulting in a rapid increase in serotonergic activity [55]. Interestingly, some studies have reported significant antidepressant-like responses following deep brain stimulation (DBS) of the PrL but not the IL [47]. Other studies indicated that electrical stimulation of both the IL and PrL induced serotonin release in the DRN, possibly due to varying stimulation parameters [51]. Furthermore, optogenetic activation of Drd1-expressing excitatory neurons in the mPFC produced rapid antidepressant responses, whereas Drd2-expressing neurons did not [56]. These findings highlight the distinct functions of mPFC subregions and the varying outcomes depending on the methods used to stimulate them. Hence, the effects of sonogenetic neuromodulation in different mPFC subregions and their underlying mechanisms warrants further investigation. Furthermore, the present study focused on a chronic restraint stress mouse model of depression and primarily assessed despair-like behaviors, which, while useful experimental indicators, do not perfectly generalize to other forms of stress or capture the full range of human symptoms, such as sadness and anhedonia [57].
Our findings establish the efficacy of a specific sonogenetic protocol in activating the mPFC-DRN pathway to produce a rapid antidepressant effect. The differing timescales observed—where brief stimulation sufficed for neurotransmitter release, yet prolonged stimulation was needed to induce c-Fos—suggest a compelling clinical duality. This implies that treatment protocols could be tailored for either immediate intervention or sustained benefit, akin to the acute versus chronic dosing regimens of conventional pharmacotherapies.
While this study establishes that sonogenetic activation of the mPFC-DRN circuit with a defined parameter set (0.3 MPa) is sufficient to induce rapid antidepressant-like effects, several translational challenges remain. A critical next step is the systematic optimization of acoustic parameters (e.g., intensity, pulse regimens) to establish a dose-response relationship that maximizes efficacy while minimizing potential side effects. Furthermore, the long-term safety and efficacy of chronic ultrasound stimulation require thorough evaluation. Finally, the current necessity of invasive viral delivery for MscL expression represents a significant translational hurdle that must be addressed by future developments in non-invasive gene delivery or engineered viral vectors. To further realize full noninvasiveness and pave the way for clinical translation, developing safe ways to deliver sonogenetic tools (e.g., ultrasound-sensitive channels like MscL-G22S) is needed, instead of transcranial injections. Early evidence is present for minimally invasive approaches such as tail-vein [58] or intranasal [59] administration, and ultrasound-facilitated gene delivery via transiently opening the blood-brain barrier [60]. However, these will still require significant work before they can replace local administration, and should be the subject of study in the near future.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Organization, W.H. Depression. 2022; https://www.who.int/news-room/fact-sheets/detail/depression.
Global Burden of Disease Study, C. Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;386:743–800.
Bachmann S. Epidemiology of Suicide and the Psychiatric Perspective. Int. J. Env. Res. Public. Health. 2018;15:1425.
Organization, W.H. Suicide prevention. 2023. https://www.who.int/health-topics/suicide#tab=tab_1.
Clinic,M Antidepressants: Selecting one that’s right for you. [cited 2023 February]. https://www.mayoclinic.org/diseases-conditions/depression/in-depth/antidepressants/art-20046273.
Otte C, Gold SM, Penninx BW, Pariante CM, Etkin A, Fava M, et al. Major depressive disorder. Nat. Rev. Dis. Primers. 2016;2:16065.
Cipriani A, Furukawa TA, Salanti G, Chaimani A, Atkinson LZ, Ogawa Y, et al. Comparative efficacy and acceptability of 21 antidepressant drugs for the acute treatment of adults with major depressive disorder: a systematic review and network meta-analysis. Lancet. 2018;391:1357–66.
Zugliani MM, Fidry M, Steffen RE, Lan K, Brietzke E, Milev R, et al. Clinical effectiveness of non-TMS neurostimulation in depression: Clinical trials from 2010 to 2020. Prog. Neuropsychopharmacol. Biol. Psychiatry. 2021;110:110287.
Ben-Menachem E. Vagus nerve stimulation, side effects, and long-term safety. J. Clin. Neurophysiol. 2001;18:415–8.
Chail A, Saini RK, Bhat PS, Srivastava K, Chauhan V. Transcranial magnetic stimulation: a review of its evolution and current applications. Ind. Psychiatry J. 2018;27:172–80.
Scangos KW, Khambhati AN, Daly PM, Makhoul GS, Sugrue LP, Zamanian H, et al. Closed-loop neuromodulation in an individual with treatment-resistant depression. Nat. Med. 2021;27:1696–1700.
Biselli T, Lange SS, Sablottny L, Steffen J, Walther A. Optogenetic and chemogenetic insights into the neurocircuitry of depression-like behaviour: a systematic review. Eur. J. Neurosci. 2021;53:9–38.
Riga D, Matos MR, Glas A, Smit AB, Spijker S, Van den Oever MC. Optogenetic dissection of medial prefrontal cortex circuitry. Front. Syst. Neurosci. 2014;8:230.
Ishimura K, Takeuchi Y, Fujiwara K, Tominaga M, Yoshioka H, Sawada T. Quantitative analysis of the distribution of serotonin-immunoreactive cell bodies in the mouse brain. Neurosci. Lett. 1988;91:265–70.
Warden MR, Selimbeyoglu A, Mirzabekov JJ, Lo M, Thompson KR, Kim SY, et al. A prefrontal cortex-brainstem neuronal projection that controls response to behavioural challenge. Nature. 2012;492:428–32.
Shin Y, Yoo M, Kim HS, Nam SK, Kim HI, Lee SK, et al. Characterization of fiber-optic light delivery and light-induced temperature changes in a rodent brain for precise optogenetic neuromodulation. Biomed. Opt. Express. 2016;7:4450–71.
Ibsen S, Tong A, Schutt C, Esener S, Chalasani SH. Sonogenetics is a non-invasive approach to activating neurons in Caenorhabditis elegans. Nat. Commun. 2015;6:8264.
Duque M, Lee-Kubli CA, Tufail Y, Magaram U, Patel J, Chakraborty A, et al. Sonogenetic control of mammalian cells using exogenous transient receptor potential A1 channels. Nat. Commun. 2022;13:600.
Huang YS, Fan CH, Hsu N, Chiu NH, Wu CY, Chang CY, et al. Sonogenetic modulation of cellular activities using an engineered auditory-sensing protein. Nano Lett. 2020;20:1089–1100.
Fan CH, Wei KC, Chiu NH, Liao EC, Wang HC, Wu RY, et al. Sonogenetic-Based neuromodulation for the amelioration of parkinson’s disease. Nano Lett. 2021;21:5967–76.
Ye J, Tang S, Meng L, Li X, Wen X, Chen S, et al. Ultrasonic control of neural activity through activation of the mechanosensitive channel MscL. Nano Lett. 2018;18:4148–55.
Qiu Z, Kala S, Guo J, Xian Q, Zhu J, Zhu T, et al. Targeted neurostimulation in mouse brains with non-invasive ultrasound. Cell Rep. 2020;32:108033.
Cadoni S, Demene C, Alcala I, Provansal M, Nguyen D, Nelidova D, et al. Ectopic expression of a mechanosensitive channel confers spatiotemporal resolution to ultrasound stimulations of neurons for visual restoration. Nat. Nanotechnol. 2023;18:667–76.
Xian Q, Qiu Z, Murugappan S, Kala S, Wong KF, Li D, et al. Modulation of deep neural circuits with sonogenetics. Proc. Natl Acad. Sci. USA. 2023;120:e2220575120.
Wang S, Meng W, Ren Z, Li B, Zhu T, Chen H, et al. Ultrasonic neuromodulation and sonogenetics: a new era for neural modulation. Front. Physiol. 2020;11:787.
Castagne V, Moser P, Roux S, Porsolt RD. Rodent models of depression: forced swim and tail suspension behavioral despair tests in rats and mice. Curr. Protoc. Neurosci. 2011;Chapter 8:Unit 8 10A.
Fosque BF, Sun Y, Dana H, Yang CT, Ohyama T, Tadross MR, et al. Neural circuits. labeling of active neural circuits in vivo with designed calcium integrators. Science. 2015;347:755–60.
Wan J, Peng W, Li X, Qian T, Song K, Zeng J, et al. A genetically encoded sensor for measuring serotonin dynamics. Nat. Neurosci. 2021;24:746–52.
Lei T, Dong D, Song M, Sun Y, Liu X, Zhao H. Rislenemdaz treatment in the lateral habenula improves despair-like behavior in mice. Neuropsychopharmacology. 2020;45:1717–24.
Can, A, DT Dao, CE Terrillion, SC Piantadosi, S Bhat, and TD Gould, The tail suspension test. J Vis Exp, 2012: e3769.
Yankelevitch-Yahav, R, M Franko, A Huly, and R Doron, The forced swim test as a model of depressive-like behavior. J Vis Exp, 2015;52587.
Xian Q, Qiu Z, Kala S, Guo J, Zhu J, Wong KF, et al. Protocol for the sonogenetic stimulation of mouse brain by non-invasive ultrasound. STAR. Protoc. 2021;2:100393.
Tervo DG, Hwang BY, Viswanathan S, Gaj T, Lavzin M, Ritola KD, et al. A Designer AAV variant permits efficient retrograde access to projection neurons. Neuron. 2016;92:372–82.
Sjulson L, Cassataro D, DasGupta S, Miesenbock G. Cell-Specific targeting of genetically encoded tools for neuroscience. Annu. Rev. Genet. 2016;50:571–94.
Miyazaki KW, Miyazaki K, Tanaka KF, Yamanaka A, Takahashi A, Tabuchi S, et al. Optogenetic activation of dorsal raphe serotonin neurons enhances patience for future rewards. Curr. Biol. 2014;24:2033–40.
Kovacs KJ. Measurement of immediate-early gene activation- c-fos and beyond. J. Neuroendocrinol. 2008;20:665–72.
Seewoo BJ, Hennessy LA, Feindel KW, Etherington SJ, Croarkin PE, Rodger J. Validation of chronic restraint stress model in young adult rats for the study of depression using longitudinal multimodal MR imaging. eNeuro. 2020;7:ENEURO.0113–20.2020.
Stachniak TJ, Ghosh A, Sternson SM. Chemogenetic synaptic silencing of neural circuits localizes a hypothalamus->midbrain pathway for feeding behavior. Neuron. 2014;82:797–808.
Jurga AM, Paleczna M, Kuter KZ. Overview of general and discriminating markers of differential microglia phenotypes. Front. Cell Neurosci. 2020;14:198.
Zhang S, Wu M, Peng C, Zhao G, Gu R. GFAP expression in injured astrocytes in rats. Exp. Ther. Med. 2017;14:1905–8.
Norden DM, Trojanowski PJ, Villanueva E, Navarro E, Godbout JP. Sequential activation of microglia and astrocyte cytokine expression precedes increased Iba-1 or GFAP immunoreactivity following systemic immune challenge. Glia. 2016;64:300–16.
Challis C, Berton O. Top-Down control of serotonin systems by the prefrontal cortex: a path toward restored socioemotional function in depression. ACS Chem. Neurosci. 2015;6:1040–54.
Tan G, Chen H, Leuthardt EC. Ultrasound Applications in the Treatment of Major Depressive Disorder: A Systematic Review of Techniques and Therapeutic Potentials in Clinical Trials and Animal Model Studies. Neuromodulation: Technology at the Neural Interface, 2025.
Blackmore DG, Razansky D, Gotz J. Ultrasound as a versatile tool for short- and long-term improvement and monitoring of brain function. Neuron. 2023;111:1174–90.
Liu T, Choi MH, Zhu J, Zhu T, Yang J, Li N, et al. Sonogenetics: Recent advances and future directions. Brain Stimul. 2022;15:1308–17.
Hamani C, Diwan M, Macedo CE, Brandao ML, Shumake J, Gonzalez-Lima F, et al. Antidepressant-like effects of medial prefrontal cortex deep brain stimulation in rats. Biol. Psychiatry. 2010;67:117–24.
Hamani C, Diwan M, Isabella S, Lozano AM, Nobrega JN. Effects of different stimulation parameters on the antidepressant-like response of medial prefrontal cortex deep brain stimulation in rats. J. Psychiatr. Res. 2010;44:683–7.
Holtzheimer PE, Husain MM, Lisanby SH, Taylor SF, Whitworth LA, McClintock S, et al. Subcallosal cingulate deep brain stimulation for treatment-resistant depression: a multisite, randomised, sham-controlled trial. Lancet Psychiatry. 2017;4:839–49.
Hare BD, Duman RS. Prefrontal cortex circuits in depression and anxiety: contribution of discrete neuronal populations and target regions. Mol. Psychiatry. 2020;25:2742–58.
Maier SF. Behavioral control blunts reactions to contemporaneous and future adverse events: medial prefrontal cortex plasticity and a corticostriatal network. Neurobiol. Stress. 2015;1:12–22.
Lopez-Terrones E, Paz V, Campa L, Conde-Berriozabal S, Masana M, Artigas F, et al. Differential modulation of dorsal raphe serotonergic activity in rat brain by the infralimbic and prelimbic cortices. Int. J. Mol. Sci. 2023;24:4891.
Groenewegen HJ, Uylings HB. The prefrontal cortex and the integration of sensory, limbic and autonomic information. Prog. Brain Res. 2000;126:3–28.
Quirk GJ, Beer JS. Prefrontal involvement in the regulation of emotion: convergence of rat and human studies. Curr. Opin. Neurobiol. 2006;16:723–7.
Alexander L, Clarke HF, Roberts AC. A focus on the functions of area 25. Brain Sci. 2019;9:129.
Gasull-Camos J, Tarres-Gatius M, Artigas F, Castane A. Glial GLT-1 blockade in infralimbic cortex as a new strategy to evoke rapid antidepressant-like effects in rats. Transl. Psychiatry. 2017;7:e1038.
Hare BD, Shinohara R, Liu RJ, Pothula S, DiLeone RJ, Duman RS. Optogenetic stimulation of medial prefrontal cortex Drd1 neurons produces rapid and long-lasting antidepressant effects. Nat. Commun. 2019;10:223.
Planchez B, Surget A, Belzung C. Animal models of major depression: drawbacks and challenges. J. Neural Transm. 2019;126:1383–408.
Chan KY, Jang MJ, Yoo BB, Greenbaum A, Ravi N, Wu WL, et al. Engineered AAVs for efficient noninvasive gene delivery to the central and peripheral nervous systems. Nat. Neurosci. 2017;20:1172–9.
Ye D, Yuan J, Yang Y, Yue Y, Hu Z, Fadera S, et al. Incisionless targeted adeno-associated viral vector delivery to the brain by focused ultrasound-mediated intranasal administration. EBioMedicine. 2022;84:104277.
Wu CY, Fan CH, Chiu NH, Ho YJ, Lin YC, Yeh CK. Targeted delivery of engineered auditory sensing protein for ultrasound neuromodulation in the brain. Theranostics. 2020;10:3546–61.
Acknowledgements
The authors would like to thank the facility and technical support from the University Research Facility in Life Sciences (ULS) and University Research Facility in Behavioral and Systems Neuroscience (UBSN) of The Hong Kong Polytechnic University.
Funding
This work was financially supported by the Hong Kong Research Grants Council Collaborative Research Fund (C5053-22 GF), General Research Fund (15126524, 15224323 and 15104520), National Key Research and Development Program of Ministry of Science and Technology of China (2023YFC2410900), and internal funding from the Hong Kong Polytechnic University (G-SACD), Research Center for Non-invasive Brain Computer Interface (1-CE0M), and Research Institute of Smart Ageing (1-CDJM).
Author information
Authors and Affiliations
Contributions
T.L. and Q.X. contributed equally to this work. T.L., Q.X., and L.S. contributed to the conceptualization; T.L., Q.X., D.L., M.S., Y.W., X.H., J.J., Y.J., X.H., J.Z. performed research; L.S. contributed new reagents/analytic tools; T.L., Q.X., D.L., M.S., Y.W., K.F.W., J.G., Z.Q., and L.S. analyzed data; and T.L., Q.X., and L.S. wrote the paper. L.S. contributed to the funding acquisition.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Lei, T., Xian, Q., Li, D. et al. Rapid rescue of despair behaviors by sonogenetic neuromodulation of the mPFC-DRN pathway. Mol Psychiatry (2026). https://doi.org/10.1038/s41380-026-03616-1
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41380-026-03616-1