Abstract
More than 1 in 10 babies are compromised by preterm birth, low birthweight, maternal pregnancy complications or perinatal hypoxia-ischemia, leading to death or lifelong disability. Advancements in pregnancy and newborn care to date have been underpinned by mechanistic and physiological insights from fundamental discovery science. However, there are growing challenges to the perinatal research pipeline that threaten the next breakthroughs. Reduced funding, discipline-specific publishing, and high attrition are reducing pipeline research capacity and particularly large animal research; over the last two decades there has been a 12.6% decrease in the number of institutes that conduct large animal perinatal studies. Furthermore, paradoxically, over-prioritisation of translational research has come at the expense of discovery science. The complexity of fetal and newborn physiology, transition at birth, pathophysiology, multi-hit and multi-organ insults, and the progressive nature of development and injury, mean that the fetus and newborn are unique study subjects. The fetus and newborn are not small adults. Consequently, progression to clinical trials must acknowledge all available evidence provided through preclinical and clinical discoveries prior to adopting new interventions. The next critical innovations towards a healthy start to life need a thriving perinatal research pipeline that values and prioritises discovery evidence.
Impact
-
Ensuring a healthy start to life for all infants needs new discoveries. But there are growing challenges to the perinatal research pipeline that threaten the next advances. Poor funding, competitive publishing, and high attrition are reducing discovery research capacity and reducing large animal research. The unique physiology and ongoing organ development in the fetus and neonate means that they are not small adults, and we must support the perinatal research pipeline to accumulate gold-standard evidence that will inform the next successful advances for better newborn health.
Similar content being viewed by others
The importance of fetal and neonatal research
A healthy start to life benefits the individual, their family, and society, supporting a lifetime potential for active contributions to all aspects of community. Many complications can affect fetal and neonatal wellbeing, particularly preterm birth, congenital abnormalities, intrapartum compromise resulting in hypoxic ischemic encephalopathy (HIE), low birthweight, fetal growth restriction (FGR), and infection or sepsis. These can arise from obstetric problems such as hypertension of pregnancy, poor maternal nutrition (under- or over-nutrition) and infection1,2 and are complications that commonly affect newborns around the world.
The World Health Organization (WHO)’s Millennium Development Goals and Every Newborn Action Plan, call for the urgent need to improve newborn survival and outcomes. The single greatest current challenge in perinatal medicine is preterm birth. The WHO and United Nations Children’s Fund (UNICEF) call preterm birth a ‘silent emergency’ with more than 1 in 10 babies born too early at less than 37 weeks’ gestation, affecting more than 13.4 million babies in 2020 and almost 1 million deaths. The rate of preterm birth has not meaningfully changed in the past two decades. The rate of preterm birth is a leading indicator of the health of a nation, due to its association with high mortality and significant risks of brain injury and impaired brain development.3 For survivors of preterm birth, especially following very preterm birth at <32 weeks’ gestation or extremely preterm birth <28 weeks’, the burden of disability, intellectual and psycho-social impairments, risk of metabolic and cardiovascular disease, reduced capacity and financial costs are high.4 “Micropremature” babies born at 22-23 weeks now have improved survival rates but have a particularly high risk of cerebral injury and long-term neurological impairments.5 In the USA, 10.4% of all births are preterm,6 with an annual cost estimated at over $25 billion.7 The USA’s National Institutes of Health (NIH) is the largest funder of biomedical research globally, and in 2024 spent $433 million on research related to preterm birth, low birth weight and health of the newborn, while for comparison, adult cardiovascular research received $2771 million. It is now well established that challenges to the in utero environment with subsequent adverse perinatal outcomes, including low birth weight, significantly increase the risk for adult cardiovascular disease8 - termed the Developmental Origins of Health and Disease Hypothesis.9 Potentially, a significant proportion, >20% of adult cardiovascular disease,10 could be prevented by improving perinatal health. Thus, to achieve meaningful decreases in the causes and consequences of preterm birth and low birth weight, we need to better understand the mechanisms and biomarkers of perinatal compromise. The perinatal research pipeline provides the capability to determine pathogenic mechanisms, and diagnostic and prognostic biomarkers, to inform new treatments and clinical management strategies.
The research pipeline in biomedical and perinatal health
The clinical translation research pipeline describes research progression from discovery science into clinical practice, defined in response to the NIH Roadmap directive for ‘efficient and effective discovery’.11,12 Although there are many variations, classically the pipeline supports progression of knowledge from discovery science, involving cells, animal and/or early human studies, into Phase I human safety and early efficacy trials, through to larger Phase II/III trials in humans to define dosing and evidence of efficacy. Successful therapies may be followed by meta-analyses of clinical studies to support widespread adoption by the medical community13 (Fig. 1). A classic example of the research pipeline is the discovery of surfactant, one of the first therapies targeting improved neonatal respiratory outcomes. The initial discovery of surfactant extraction from animal lungs in the 1950s14 contributed to subsequent findings that a lack of surfactant led to neonatal respiratory demise at autopsy.15 From this point, the importance of endogenous surfactant, and the therapeutic potential for exogenous surfactant, were assessed and refined in large-animal models, ultimately enabling life-saving therapy in neonates (this series of discoveries has been extensively reviewed, for example16). This ‘bedside-to-bench-to-bedside’ paradigm underscores the pivotal role of large-animal models in the research pipeline. Irrespective of whether the research is tackling adult or infant disorders, the length of time for research to progress through the pipeline is often long, with high attrition, and substantial costs and challenges.
Discovery Science Research results characterise pathology, targets, multi-organ outcomes, and treatment and safety efficacy, prior to Translational to Human Trial and Practice. The Translational Pipeline is often not a straight line from bench to bedside, with results at each stage informing forward and backward flow – as represented by the double-ended arrows.
The research pipeline is seldom efficient: 80 to 90% of research studies fail to progress to clinical trial, with an average time lag of 17 years even in successful cases.13,17 This has produced a reactive shift towards human translational or applied research, to satisfy the desire for an urgent human health impact, which circumvents discovery research for expediency18,19 and identification of mechanisms. However, one has to ask the ethical questions; 1) at what point does this type of research fall under the banner of “human experimentation”?, and 2) who becomes accountable for not assessing why a treatment works or fails, as well as unanticipated or off-target consequences? We would suggest that this point is dependent upon whether the science is known or unknown (i.e. an educated guess).
Failure to progress to clinical trial might occur because of insufficient funding, or a lack of funding for essential longitudinal studies comparing the acute and chronic effects of injury and treatment. Arguably these are particularly important in perinatal studies where long-term (lifetime) effects must be characterised. However, the importance of discovery research in perinatal health extends beyond clinical cures, and clinical implementation is not the only measure of success – fundamental studies to advance knowledge on normal and abnormal biological processes, or biomarkers of health and disease, are crucial, and conversely, rushing towards clinical application may be harmful.
Loss of capacity for large animal perinatal research
We present below examples for antenatal corticosteroids for preterm infants, hypothermia for newborns with HIE, and delaying cord clamping for optimised physiological transition, that exemplify successes that have utilised the breadth of outcomes afforded by the research pipeline and large animal research. But a changing landscape of reduced grant success and reprioritising funding towards clinical translation are modifying how funding is allocated.
We analysed the change in the number of research institutes, publications and demographics of perinatal large animal studies conducted two decades apart world-wide. We examined publications in Scopus citing perinatal animal studies using piglets, sheep and primates, using the search terms fetal or neonatal and piglets/sheep/primates from the year 2004 (n = 267 total publications) and compared these to the year 2024 (n = 238 total publications); the search was conducted within the Scopus fields Article title, Abstract, Keywords, limited to English language and Articles. All abstracts were read to ensure the publication described an in vivo large animal study undertaken in a research setting; the research institute of the first and/or last author was allocated as the primary research institute, and where multiple affiliations were used, the place of animal research was confirmed in the publication methods. There was a 12.6% decline in the number of research institutes undertaking perinatal large animal studies between 2004 (n = 111) to 2024 (n = 97). The regions with the highest numbers of individual sites for perinatal large animal studies in 2004 were the USA (n = 39 institutes), Europe (n = 25), the UK (n = 11), Australia and New Zealand (n = 14), Canada (n = 9) and Japan (n = 8), Fig. 2. Between 2004 and 2024, there was a large reduction in the number of institutes undertaking perinatal large animal research across the USA (a fall from n = 39 to 31), the UK (n = 11 to 3), Australia and New Zealand (n = 14 to 7), Canada (n = 9 to 6) and Japan (n = 8 to 0). The only region to show a notable increase in institutions undertaking large animal perinatal research across this period was China (n = 2 sites in 2004, and 18 sites in 2024).
Scopus searches were conducted in the fields Article title, Abstract, Keywords, limited to English language and Articles, using search terms fetal OR neonatal AND piglets/sheep/primates). The total number of research institutes was counted, across regions of interest.
In mid-2025 the NIH announced prioritisation of human-based research, moving away from funding studies that exclusively use animal models. This shift aims to reduce dependence on animal studies, encouraging New Approach Methodologies (NAMs) to validate relevance to human disease, such as human participants, in vitro methods or artificial intelligence.20 Large-scale adoption of NAMs will inevitably lead to a reduction in large animal research facilities. These facilities are expensive to run, and they will not be cost-effective to maintain with falling use or falling numbers of grants to support research. Closures are unlikely to be reversed. A reduction in the number of institutes with perinatal large animal facilities risks high-quality perinatal research across the pipeline.
Funding for fundamental research in perinatal health
The WHO states that every dollar invested in maternal and child health generates a return of $7 in economic benefit, by reducing healthcare costs, increasing productivity and healthier future generations. There are competing pressures globally for limited financial resources, causing uncertainty about the value of discovery research and redistributing available funding.21,22 In high-income countries the success rate for new grant applications is less than 20%,23 and often lower. For example the total number of new grants awarded through the Australian National Health and Medical Research Council scheme almost halved in the decade between 2013 (n = 1226, 22% success rate) to 2023 (n = 686, 14% success rate) despite a modest total funding increase.24 This profile of falling success rates despite a maintained total budget is echoed across high-income countries with publicly accessible data. Even with evidence that national research investment is vital to support an educated, skilled and knowledgeable workforce that improves society,25 research funding is stagnant or falling, while costs are increasing. This is compounded at university/institute level, where short funding cycles, funding gaps and workforce insecurity stifle project continuity, creativity, and discourage the next generation of biomedical researchers.25
Agravat et al. conducted a systematic analysis of major grant funders globally for research funding in newborn health and stillbirth during 2019–2020.26 They found that discovery research—‘basic science, pre-clinical research, technology development’—received 20.9% of new grants in newborn health and stillbirth research, less in both number and dollar value to research covering ‘observational clinical research, epidemiology’.26 The proportion of total funding allocated to discovery science fell from 20.1% in 2011 to 9.9% in 2020.26 During this period there was a considerable shift towards ‘interventional or experimental research’, including larger, more expensive randomised clinical trials (RCTs), from 9.7% of total funding in 2011 to 28.3% in 2020 (equivalent to $19,343,133 USD).26 This shift from discovery science towards RCTs could reflect increased translation of discovery science into clinical application, but this is unlikely given the falling number of new therapies over time. It almost certainly reflects the preference of funding bodies and institutes to support immediate clinical application.
The fetus and newborn are not small adults
We cannot simply extrapolate from adult physiology and pathophysiology when it comes to determining mechanisms of injury in the infant, and establishing appropriate diagnostic and prognostic biomarkers or treatment strategies. The fetus lives and develops in an unique environment that necessitates cardiorespiratory and neural adaptations. These range from cardiorespiratory adaptations to accommodate the placenta as the organ of gas exchange27 to neural function characterised as unarousable unconsciousness (e.g. the fetus does not arouse when exposed to hypoxia) due to higher levels of neuroinhibitors released by the brain and placenta,28 and some neurotransmitters may also function differently, for example GABA is inhibitory in adults but excitatory during most of fetal life.28 The fetus is reliant on the placenta (and mother) for nutrients and gas exchange. Fetal blood flow is shunted past the liquid-filled lung via specialised ducts, making the cardiorespiratory physiology of the fetus very different to adults. Survival at birth requires lung aeration and a complex repurposing and re-organisation of multiple physiological systems, allowing the newborn to be independent from its mother.29
Scaling down treatments that are efficacious in adults often results in treatments that have limited efficacy or are dangerous, given physiological differences, organ immaturity and ongoing critical development. Anti-seizure drugs are a case in point, where therapeutics shown to be effective for treatment of adult seizures are neurotoxic to the developing brain.30 Additionally, we now know that perinatal compromise does not usually come as a ‘single insult hit’. For example, babies born very preterm are often exposed to hypoxia and inflammatory stresses before and after birth, and then spend days to weeks on respiratory support for their immature lungs.31 They also require cardiovascular support for low blood pressure and have complex evolving brain injury that can induce brain haemorrhage, commonly associated with seizures.32,33,34 Each of these individual stressors requires intervention, highlighting the unique nature of perinatal compromise.
In addition to not simply extrapolating from the adult, neither the fetus nor the newborn should be the subject of try-it-and-see approaches rather than evidence-based medicine based on an in-depth understanding of their physiology and pathophysiology. Professor William (Bill) Silverman, an American pioneer of evidence-based neonatal medicine in the area of thermoregulation in the 1950s and 60s, reflected that “The impatient let’s-try-it-and-see approach in the burgeoning field of neonatal medicine has resulted in therapeutic disaster after disaster”.35 He was a strong advocate of evidence-based clinical trials and this is of course now recognised as the appropriate approach. However, we risk development of the evidence base if we do not support and expand use of appropriate preclinical models for perinatal compromise.
Experimental animal models can provide specificity for primary and secondary outcomes, and can characterise perinatal physiology and pathophysiology, together with responses to new treatments prior to clinical application. Relevant preclinical animal models of perinatal compromise include small animal studies in mice and rats with short gestation lengths (~19–22 days), medium size animals including rabbits, guinea pigs and spiny mice (31–65 days), through to large animal studies that most commonly include pigs (113 days), sheep (148 days), and non-human primates including baboons and macaques (165–185 days).36,37,38,39,40,41 Small and large animals each offer advantages and weaknesses for fetal or neonatal studies; Fig. 1. The choice of animal model must be appropriate, and there are excellent reviews comparing animal studies for FGR,38,39,40 preterm birth,36,38 and HIE.37,41 Rodent models allow high throughput studies with a short gestation length and lower animal costs, making them a first choice for assessing pathways to organ injury across a timeline, screening mechanisms and molecular mediators, and long-term functional outcomes; but conversely the brain and lungs of mice and rats are immature at birth compared to the human and integrative physiological studies are not possible. Fetal sheep are the animal model of choice for antenatal studies. The fetus can be studied in real-time in utero, providing detailed integrated physiological insights into how fetal organ systems develop, changes at birth, and responses to challenges.38,42,43,44 Assessment of the complex multi-organ changes that take place during and after birth, or in response to birth asphyxia and development of HIE, have effectively utilised newborn lambs, piglets and non-human primates with their similar size to human infants permitting neonatal intensive care that mimics human care.29,37,41,45,46,47,48,49
Preclinical studies have the advantage of being able to control for separate but cumulative challenges, and assessments of how the timing of an insult or treatment modifies outcome, advancing personalised care. The scientific evidence used to guide clinical application of a novel perinatal intervention must incorporate all available observations (positive and negative), across organs, and with clearly defined physiological consequences.50 Animal studies must be carefully considered with clearly articulated hypothesis and power calculation, and respecting the three pillars of reduce, refine and replace in animal research.51 Here we highlight examples of evidence that has incorporated physiological and multi-organ assessments, of specific relevance to the fetus and neonate.
A brief history of why discovery research matters for perinatal advances
The positive benefits of antenatal corticosteroids to mature the preterm newborn lungs
The seminal 1960s studies of the late Sir Graham “Mont” Liggins revolutionised perinatal medicine with arguably the most important discovery in perinatal science - the introduction of antenatal steroids for preterm survival. Liggins was interested in the mechanisms that initiate labour, convinced that the fetus and not the mother was the driver for parturition.52 Studying pregnant sheep, Liggins showed that preterm lambs exposed to dexamethasone antenatally, either directly or via maternal administration, unexpectedly survived preterm birth and were breathing, with aerated lungs.53 At the time, Liggins noted that the mechanisms by which the steroids aerated the lungs and improved survival were unknown but appeared due to accelerated lung surfactant.53
Liggins and neonatologist Ross Howie translated this finding into clinical trial54 and published the landmark paper reporting the first RCT administering the synthetic glucocorticoid betamethasone to mothers in preterm labour, which improved survival and lung function in preterm newborns. Liggins and Howie administered betamethasone via two 12 mg injections to the mother, 24 h apart. Further clinical trials followed and, while uptake was slow,52 results were strongly supportive that corticosteroids decreased mortality and morbidity associated with respiratory distress syndrome in preterm infants.
In 1994 the NIH released a consensus statement endorsing antenatal corticosteroid therapy for women at risk of premature delivery and this substantially increased the standardised application of antenatal corticosteroids; ~90% of babies born very preterm now receive antenatal corticosteroids.32 To this day, the original dose and treatment regime first used in lambs remains the standard protocol for antenatal betamethasone administration for women in preterm labour.55 Unquestionably, antenatal glucocorticoid exposure has saved the lives of hundreds of thousands of preterm babies by improving lung maturation and respiratory capacity.55 Since the original findings related to lung health, additional preclinical research has shed light on the pronounced effects of antenatal glucocorticoids on other organs including the developing brain.56,57 These findings indicate that exogenous steroids have a range of effects beyond the lungs. Some of these effects are beneficial, such as improving long-term cardiovascular stability,58 while others are potentially adverse, particularly a significant increase in the risk of neurodevelopmental concerns in children born moderately preterm (between 34 and 36 weeks) who were exposed to antenatal corticosteroids.59 This underscores the importance of using these medications judiciously and tailoring their use to specific sub-groups of high-risk infants.60
Umbilical cord clamping: when to clamp?
The debate about ‘when to clamp the cord’ is not new and can be traced back 100’s (Erasmus Darwin) if not 1000’s (Aristotle) of years.27 Until recently, umbilical cord clamping at birth was considered an innocuous act that did not impact infant wellbeing. As a result, cord clamping immediately after birth (ICC) was introduced as standard care in the late 20th century, as part of a package of care for managing labour to reduce post-partum haemorrhage. It wasn’t until the 1960s that delaying umbilical cord clamping (DCC) was shown to increase infant blood volume after birth,61 that perceptions began changing. More recently, studies in preterm lambs have provided the physiological explanation as to why umbilical cord clamping is not an “innocuous act”. To answer the question as to why more than 50% of healthy, well oxygenated infants have a low heart rate at birth,62 research showed that immediate cord clamping caused a 50-60% reduction in cardiac output.63
Separating the infant from the placenta immediately after birth exposes the infant to the simultaneous loss of oxygen and cardiac venous return, putting the infant at risk of ischemia due to low cardiac output, and hypoxia. By characterising the physiology underpinning the adverse effects of ICC in preterm lambs, the solution to this problem became very apparent - to aerate the lungs prior to cord clamping. Studies in preterm lambs demonstrated that aerating the lungs prior to cord clamping avoids the loss in cardiac output by allowing increasing pulmonary blood flow to immediately replace umbilical venous return as the source of left ventricular preload. This allows the lungs to supply oxygen as soon as the cord is clamped.63,64,65,66 This is referred to as ‘physiological based cord clamping’ (PBCC). Subsequent clinical trials have confirmed that the low heart rate (<100 bpm) experienced by infants at birth was an artifact, simply caused by clamping the umbilical cord too early.67,68 Importantly, a recent systematic review and individual participant data network meta-analysis found that deferred cord clamping, including infants receiving PBCC, reduced death before discharge (odds ratio 0.31).69 These findings were replicated in a low-resource setting (Tanzania), whereby delaying umbilical cord clamping until after the infant breathed reduced the risk of death or admission to NICU by 20% for every 10-second delay.70 More recently a large multi-centre RCT showed that PBCC increases intact survival but only in very preterm male infants.71 Importantly, the same study also found that there was a highly significant positive relationship between intact survival and clinical experience with PBCC. These findings highlight the crucial influence of training and procedural familiarity on outcomes, and emphasise the concept of “translational accuracy”, that is, how a lack of experience, incomplete understanding of the physiological rationale, or perceived logistical barriers can undermine the efficacy of a treatment during clinical implementation. Consequently, the overall trial result may underestimate the true physiological benefit of PBCC leading to an assumption that the “science is wrong” or it doesn’t apply to humans. Indeed, any outcome benefit for any medical procedure is closely associated with practise and the frequency at which the procedure is performed, and therefore the experience with translating PBCC into the clinic is unsurprising.
The positive benefits of hypothermia for hypoxic ischemic encephalopathy (HIE)
Perinatal asphyxia, sufficient to cause prolonged and injurious hypoxia-ischemia, is the single most common cause of encephalopathy in term infants. The progression of metabolic disruption and neuropathology caused by perinatal hypoxia-ischemia was characterised in rats, fetal sheep and piglets.72,73,74 The origins of hypothermia as a therapeutic for HIE likely started in the 1700s when Floyer described ‘dipping infants’ after they were born still. In 1949, Miller reported that anoxic neonatal guinea pigs survived longer with a lower body temperature.75 Contemporary studies of therapeutic hypothermia (TH) for neonatal hypoxic-ischemic brain injury began in neonatal rats during the 1980s,76,77 showing that systemic hypothermia reduced brain infarct area (Fig. 3). Laptook et al.78 extended preclinical studies into neonatal piglets to test a modest 2–3 °C decrease in body temperature (equivalent to studies showing neuroprotective efficacy in adult animals) albeit commenced before hypoxia-ischemia. These results applying pre-insult hypothermia therapy in piglets78 were followed by studies showing that TH (to 35 °C) initiated immediately after resuscitation ameliorated the secondary decline in high energy phosphates detectable on magnetic resonance spectroscopy (MRS),79 and TH immediately after resuscitation for short periods (1–3 h) was neuroprotective on immunohistochemistry.80,81 A clear advantage of undertaking these early studies in piglets is that their size permitted clinical correlates for neonatal management, including brain metabolism using MRS, haemodynamic physiology, and brain histopathology.80 Subsequent studies in piglet and fetal sheep models have allowed comprehensive electrophysiological, neuro-imaging and cardiac monitoring, and this advantage has been used to clearly define pathophysiological phases of evolving injury after HI.74,82,83,84,85,86 The similarities between pigs and humans in drug metabolism suggest pigs are well-suited to predicting the pharmacokinetic (PK) profile in humans.87 An example of this is the development of a population-based PK model for melatonin (a possible future adjunct therapy with TH) in newborn piglets to inform the design of a phase I clinical trial of babies with moderate/severe HIE receiving TH (ISRCTN61218504).88
Early discovery science studies progressed from small animal to large animal preclinical studies and then progressed to translation to human trials and standard clinical practice. This set of work demonstrates the effective use of the Translational Pipeline in Perinatal Research to optimise the application of therapeutic hypothermia for human infants with HIE and shows the long duration to progress from bench to bedside.
A series of studies undertaken by the Auckland perinatal group in their term-equivalent fetal sheep model of in utero hypoxia-ischemia defined the key parameters required for neuroprotection with selective head cooling. Studying fetal sheep allowed monitoring of longitudinal, real-time changes in systemic physiology and biochemistry (lactate, pH and glucose), and neurophysiological outcomes (epileptiform events, cortical impedance, EEG, cerebral blood flow and cerebral oxygen delivery).89 Gunn et al. showed that when cooling was delayed by 90 minutes after insult, optimum neuroprotection was achieved with 72 h total duration of moderate TH,89 and that the timing of TH initiation was critical and needed to commence within 6 h of insult to be efficacious,90 and that treatment started after the onset of delayed seizures failed to protect the brain.91 Studies in fetal sheep and piglets have shown that cooling for longer (5 days vs 3 days),92 or deeper than 33.5–35 °C (a decrease of ~3.5 °C),46,93 does not improve brain outcomes and indeed may be detrimental.93
Specifically, many piglet studies have used proton MRS Lactate to N-acetylaspartate (Lac/NAA) peak area ratio which accurately predicts 2-year motor, cognitive and language outcomes in babies with moderate to severe HIE94 and is used as an early surrogate readout in neuroprotection trials.95 The newborn piglet demonstrates similar neurometabolic changes on MRS after HI,82,83 correlating with immunohistochemistry markers of cell death and neuro-inflammation.96 Lac/NAA peak area ratio in the piglet is an important neurological outcome, allowing power calculation for studies and reducing sample sizes. Similarly, acquisition of Lac/NAA peak area ratio in the newborn lamb for neuroprotection studies is feasible,45 although it is a logistic challenge given the need for sedation.
Ultimately, this two-decade body of preclinical work was the foundation for a safety study in asphyxiated human infants showing the benefit of TH,97 leading to multiple subsequent RCTs to show significantly improved survival without disability.98 In 2005, TH was adopted into standard care for infants born ≥36 weeks’ gestation with moderate/severe HIE.99,100,101,102 The preclinical parameters for efficacy were adopted; TH must commence with 6 hours of birth, reducing infant body temperature by 3.5 ± 0.5 °C (33.5–34.5 °C) for 72 h. It is not possible to cost the critical preclinical animal studies that underpinned the development of TH for HIE, but all studies played their part to reveal an optimised protocol for TH.103 In human infants, the application of TH has been assessed in a cost-effectiveness study, determining that cooling was cost-neutral over the first 18 months of life, with significant financial benefits over 18 years; hypothermia saved ~$27,000 USD per disability-free lived year.104 This body of work is now being extended to TH application for infants with mild HIE105 and adjuvant therapies to enhance neuroprotective efficacy.106
Lessons learnt from ignoring large animal results
Fetal growth restriction and the STRIDER trial
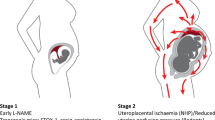
The most common cause of fetal growth restriction (FGR) is placental insufficiency, with the placenta failing to deliver adequate oxygen and nutrients for normal fetal growth.107 Treatments to induce vasodilation of the uteroplacental arteries have been pursued, with sildenafil citrate an appealing candidate given that sildenafil is a selective phosphodiesterase type 5 (PDE-5) inhibitor that promotes vasodilatation through nitric oxide release. A 2005 study by Wareing et al. examined ex vivo small myometrial arteries from pregnant women with and without FGR, and found that sildenafil induced relaxation of FGR myometrial vessels.108 In non-pregnant sheep, sildenafil treatment increased uterine blood flow,109 while in pregnant rats, sildenafil increased fetal weight following hypoxia exposure.110 In the subsequent decade, in vitro and preclinical in vivo studies assessed whether maternal sildenafil improved uteroplacental function and fetal growth (reviewed in ref. 111).
Most clinical and preclinical results supported that sildenafil increased fetal growth secondary to uteroplacental vasodilation. An exception was a 2009 sheep study assessing the acute effects of sildenafil citrate.112 Unexpectedly, maternal sildenafil immediately reduced uterine blood flow in sheep with either a control or FGR fetus, causing fetal hypoxia, hypotension and tachycardia.112 Despite this, the international “Sildenafil therapy in dismal prognosis early onset fetal growth restriction” (STRIDER) international clinical consortium commenced in 2014, with maternal sildenafil given in FGR pregnancies (n = 790 participants), with the primary outcomes of survival, fetal growth and prolongation of pregnancy.113 The UK and Australian arms of STRIDER completed their trials, reporting that sildenafil did not prolong pregnancy or improve pregnancy or fetal growth outcomes.114,115 However, the large Dutch arm of STRIDER (n = 354) was halted early when interim analysis found that neonatal deaths were more common in the sildenafil-treated babies than placebo; of the n = 103 pregnancies treated with sildenafil, 17 babies were diagnosed with the respiratory complication pulmonary hypertension, and 11 died, compared to no deaths from pulmonary hypertension in the placebo group.116,117 A BMJ Letter entitled ‘Comprehensive literature search for animal studies may have saved STRIDER trial’118 noted that the original STRIDER trial protocol paper cited five animal studies supporting the use of sildenafil, with four in small animal models while omitting the negative results in sheep.119 This example underscores the importance of balanced consideration of small and large animal data to inform clinical trials. Symonds and Budge wrote ‘Fetal development differs between small mammals and humans, so safety aspects are better assessed using appropriate, large models of intrauterine growth retardation, such as sheep’.118
Summary
Pregnancy and birth complications are common, affecting more than 1 in 10 infants, or 30,000+ babies across the world, every day. Every research dollar invested towards ensuring a healthy start to life provides benefits the individual and their family, but also for society and national economies. Planning high-quality clinical trials should balance all findings in preclinical models; these studies, especially in large animal models, provide in-depth information on the safety, efficacy, therapeutic window and optimal dose of therapies before clinical translation. Yet the capacity for undertaking large animal studies in the fetus or neonate is declining and there are new challenges in funding and administration that threaten preclinical work. We recommend that clinical trial teams include scientific experts to ensure that, (i) the trial is underpinned by a well-characterised scientific rationale, (ii) that the proposed trial and treatment will accurately test the science in question, and (iii) the outcome measure of benefit is relevant to the treatment. These issues have not been a priority in recent large RCTs in perinatal medicine, and the issue of experience with a treatment has been ignored. We are at a critical juncture in perinatal medicine with an urgency for new interventions to prevent or treat preterm birth, HIE, infection and FGR, but on a backdrop of reduced discovery research funding and closure of large animal facilities. It is important to be moving towards a reduction or replacement of animals in research, but we must not jump to clinical trials in the fetus and newborn too quickly. There remain critical knowledge gaps and interventions in perinatal medicine that require an understanding of the unique physiology and pathophysiology of the fetus and neonate, and often times this can only be provided by preclinical research. Ensuring a healthy start to life for all infants needs new discoveries. The unique physiology and ongoing organ development in the fetus and newborn means that they are not small adults, and the purpose of the perinatal research pipeline is to accumulate gold-standard evidence that informs the next successful advances for better newborn health.
Data availability
All data is available upon reasonable request to the corresponding author, Suzanne Miller.
References
Lassi, Z. S., Majeed, A., Rashid, S., Yakoob, M. Y. & Bhutta, Z. A. The interconnections between maternal and newborn health-evidence and implications for policy. J. Matern. Fetal Neonatal Med. 26, 3–53 (2013).
Oza, S., Lawn, J. E., Hogan, D. R., Mathers, C. & Cousens, S. N. Neonatal cause-of-death estimates for the early and late neonatal periods for 194 countries: 2000-2013. Bull. World Health Organ. 93, 19–28 (2015).
Inder, T. E., Volpe, J. J. & Anderson, P. J. Defining the neurologic consequences of preterm birth. N. Engl. J. Med. 389, 441–453 (2023).
Moster, D., Lie, R. T. & Markestad, T. Long-term medical and social consequences of preterm birth. N. Engl. J. Med. 359, 262–273 (2008).
Hunt, R. W. Cerebral palsy in Australia: optimism and challenges. Med J. Aust. 221, 529–530 (2024).
Maternal Infant Health, Preterm Birth. U.S. Centers for Disease Control and Prevention (CDC), National Center for Health Statistics, https://www.cdc.gov/maternal-infant-health/preterm-birth/index.html (2024).
Waitzman, N. J., Jalali, A. & Grosse, S. D. Preterm birth lifetime costs in the United States in 2016: An Update. Semin Perinatol. 45, 151390 (2021).
Barker, D. J., Osmond, C., Golding, J., Kuh, D. & Wadsworth, M. E. Growth in utero, blood pressure in childhood and adult life, and mortality from cardiovascular disease. BMJ 298, 564–567 (1989).
Oulerich, Z. & Sferruzzi-Perri, A. N. Early-life exposures and long-term health: adverse gestational environments and the programming of offspring renal and vascular disease. Am. J. Physiol. Ren. Physiol. 327, F21–F36 (2024).
Wang, Y. X. et al. Associations of birth weight and later life lifestyle factors with risk of cardiovascular disease in the USA: a prospective cohort study. EClinicalMedicine 51, 101570 (2022).
Kleinman, M. S. & Mold, J. W. Defining the components of the research pipeline. Clin. Transl. Sci. 2, 312–314 (2009).
Zerhouni, E. Medicine. The NIH Roadmap. Science 302, 63–72 (2003).
Seyhan, A. A. Lost in translation: the valley of death across preclinical and clinical divide – identification of problems and overcoming obstacles. Transl. Med. Commun. 4 (2019).
Clements, J. A. Surface tension of lung extracts. Proc. Soc. Exp. Biol. Med 95, 170–172 (1957).
Avery, M. E. & Mead, J. Surface properties in relation to atelectasis and hyaline membrane disease. AMA J. Dis. Child 97, 517–523 (1959).
Hallman, M. & Herting, E. Historical perspective on surfactant therapy: transforming hyaline membrane disease to respiratory distress syndrome. Semin. Fetal Neonatal Med. 28, 101493 (2023).
Morris, Z. S., Wooding, S. & Grant, J. The answer is 17 years, what is the question: understanding time lags in translational research. J. R. Soc. Med. 104, 510–520 (2011).
National Health and Medical Research Council Australia (Australian Government, 2022).
Lorsch, J. R., Tabak, L. A. & Bertagnolli, M. M. Applied research won’t flourish without basic science. Elife 13 (2024).
National Institutes of Health, Vol 18. How does the NIH Initiative to Prioritize Human-Based Research Affect Research Proposing the Use of Laboratory Animals? (Grants & Funding, 2025). https://grants.nih.gov/news-events/nih-extramural-nexus-news/2025/07/how-does-the-nih-initiative-to-prioritize-human-based-research-affect- research-proposing-the-use-of-laboratory-animals.
Spector, J. M., Harrison, R. S. & Fishman, M. C. Fundamental science behind today’s important medicines. Sci. Transl. Med. 10 (2018).
Gitterman, D. P., Hay, W. W. Jr. & Langford, W. S. Making the case for pediatric research: a life-cycle approach and the return on investment. Pediatr. Res. 93, 797–800 (2023).
Lasinsky, A. M. et al. Biomedical research grant resubmission: rates and factors related to success - a scoping review. BMJ Open 14, e089927 (2024).
National Health and Medical Research Council, Australia. https://www.nhmrc.gov.au/funding/data-research/outcomes.
Bennet, L., Campbell, R. E. & Gunn, A. J. Devolution of New Zealand research to a gig economy: time for investment. N.Z. Sci. Rev. 79, 26–32 (2024).
Agravat, P. et al. Research funding for newborn health and stillbirths, 2011-20: a systematic analysis of levels and trends. Lancet Glob. health 11, e1794–e1804 (2023).
Hooper, S. B. et al. The timing of umbilical cord clamping at birth: physiological considerations. Matern Health Neonatol. Perinatol. 2, 4 (2016).
Bennet, L., Walker, D. W. & Horne, R. S. C. Waking up too early—the consequences of preterm birth on sleep development. J. Physiol. 596, 5687–5708 (2018).
Chakkarapani, A. A. et al. Transitional circulation and hemodynamic monitoring in newborn infants. Pediatr. Res 96, 595–603 (2024).
Zhou, K. Q. et al. Treating seizures after hypoxic-ischemic encephalopathy-current controversies and future directions. Int. J. Mol. Sci. 22 (2021).
Humberg, A. et al. Preterm birth and sustained inflammation: consequences for the neonate. Semin. Immunopathol. 42, 451–468 (2020).
Piscopo, B. R. et al. The Interplay between birth weight and intraventricular hemorrhage in very preterm neonates - a retrospective cohort study. Am. J. Obstet. Gynecol. MFM, 101628 (2025).
Polglase, G. R. et al. Respiratory support for premature neonates in the delivery room: effects on cardiovascular function and the development of brain injury. Pediatr. Res. 75, 682–688 (2014).
Volpe, J. J. Brain injury in premature infants: a complex amalgam of destructive and developmental disturbances. Lancet Neurol. 8, 110–124 (2009).
Silverman, W. A. Personal reflections on lessons learned from randomized trials involving newborn infants from 1951 to 1967. Clin. Trials 1, 179–184 (2004).
Gie, A. G. et al. A systematic review of the influence of continuous positive airway pressure on fetal and newborn animal models: suggestions to improve neonatal respiratory care. Neonatology 118, 5–14 (2021).
Inder, T., Neil, J., Yoder, B. & Rees, S. Non-human primate models of neonatal brain injury. Semin. Perinatol. 28, 396–404 (2004).
Morrison, J. L. et al. Improving pregnancy outcomes in humans through studies in sheep. Am. J. Physiol. Regul. Integr. Comp. Physiol. 315, R1123–R1153 (2018).
Swanson, A. M. & David, A. L. Animal models of fetal growth restriction: considerations for translational medicine. Placenta 36, 623–630 (2015).
Valenzuela, I., Kinoshita, M., van der Merwe, J., Marsal, K. & Deprest, J. Prenatal interventions for fetal growth restriction in animal models: a systematic review. Placenta 126, 90–113 (2022).
Yager, J. Y. Animal models of hypoxic-ischemic brain damage in the newborn. Semin. Pediatr. Neurol. 11, 31–46 (2004).
Dudink, I. et al. Fetal Growth restriction adversely impacts trajectory of hippocampal neurodevelopment and function. Brain Pathol. e13330 (2025).
Gunn, A. J. & Bennet, L. Fetal hypoxia insults and patterns of brain injury: insights from animal models. Clin. Perinatol. 36, 579–593 (2009).
Morrison, J. L. et al. Mri characterization of blood flow and oxygen delivery in the fetal sheep whilst exposed to sildenafil citrate. Neonatology 119, 735–744 (2022).
Aridas, J. D. S. et al. Systemic and transdermal melatonin administration prevents neuropathology in response to perinatal asphyxia in newborn lambs. J. Pineal Res 64, e12479 (2018).
Iwata, O. et al. Depth of delayed cooling alters neuroprotection pattern after hypoxia-ischemia. Ann. Neurol. 58, 75–87 (2005).
Aridas, J. D. et al. Melatonin augments the neuroprotective effects of hypothermia in lambs following perinatal asphyxia. J. Pineal Res 71, e12744 (2021).
Papagianis, P. C. et al. Postnatal steroids as lung protective and anti-inflammatory in preterm lambs exposed to antenatal inflammation. Pediatr. Res 95, 931–940 (2024).
Badurdeen, S. et al. Haemodynamic instability and brain injury in neonates exposed to hypoxia(-)ischaemia. Brain Sci. 9 (2019).
Benitz, W. E. & Polin, R. A. Recommitting to rules of evidence and laws of inference. J. Pediatr. 275, 114199 (2024).
Barr, G. Ethical, impactful and better science. The Biologist. https://www.rsb.org.uk/biologist-features/ethical-impactful-and-better-science (2024).
Harding, J. E. & Crowther, C. A. in O&G Magazine Vol. 21 13–2115 (RANZCOG, 2019).
Liggins, G. C. Premature delivery of foetal lambs infused with glucocorticoids. J. Endocrinol. 45, 515–523 (1969).
Liggins, G. C. & Howie, R. N. A controlled trial of antepartum glucocorticoid treatment for prevention of the respiratory distress syndrome in premature infants. Pediatrics 50, 515–525 (1972).
McGoldrick, E., Stewart, F., Parker, R. & Dalziel, S. R. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst. Rev. 12, CD004454 (2020).
Bennet, L., Davidson, J. O., Koome, M. & Gunn, A. J. Glucocorticoids and preterm hypoxic-ischemic brain injury: the good and the bad. J. Pregnancy 2012, 751694 (2012).
Miller, S. L. et al. The effects of maternal betamethasone administration on the intrauterine growth-restricted fetus. Endocrinology 148, 1288–1295 (2007).
Carter, S. W. D. et al. Addressing the long-term risks of administering antenatal steroids. Expert Opin. Pharmacother. 26, 617–629 (2025).
Frier, E. M. et al. Associations of antenatal corticosteroids with neurodevelopment in children aged 27-30 months: a population-based cohort study. BJOG 132, 902–915 (2025).
Miller, S. L. & Wallace, E. M. Effect of antenatal steroids on haemodynamics in the normally grown and growth restricted fetus. Curr. Pediatr. Rev. 9, 67–74 (2013).
Yao, A. C., Moinian, M. & Lind, J. Distribution of blood between infant and placenta after birth. Lancet 2, 871–873 (1969).
Dawson, J. A. et al. Changes in heart rate in the first minutes after birth. Arch. Dis. Child Fetal Neonatal Ed. 95, F177–181 (2010).
Bhatt, S. et al. Delaying cord clamping until ventilation onset improves cardiovascular function at birth in preterm lambs. J. Physiol. 591, 2113–2126 (2013).
Lio, A. et al. Ventilation prior to umbilical cord clamping improves cardiovascular stability and oxygenation in preterm lambs after exposure to intrauterine inflammation. Front. Pediatr. 6, 286 (2018).
Polglase, G. R. et al. Physiologically based cord clamping stabilises cardiac output and reduces cerebrovascular injury in asphyxiated near-term lambs. Arch. Dis. Child Fetal Neonatal Ed. 103, F530–F538 (2018).
Polglase, G. R. et al. Ventilation onset prior to umbilical cord clamping (physiological-based cord clamping) improves systemic and cerebral oxygenation in preterm lambs. PLoS One 10, e0117504 (2015).
Badurdeen, S. et al. Physiologically based cord clamping for infants >/=32+0 weeks gestation: a randomised clinical trial and reference percentiles for heart rate and oxygen saturation for Infants >/=35+0 weeks gestation. PLoS Med. 19, e1004029 (2022).
Blank, D. A. et al. Baby-directed umbilical cord clamping: a feasibility study. Resuscitation 131, 1–7 (2018).
Seidler, A. L. et al. Short, medium, and long deferral of umbilical cord clamping compared with umbilical cord milking and immediate clamping at preterm birth: a systematic review and network meta-analysis with individual participant data. Lancet 402, 2223–2234 (2023).
Ersdal, H. L., Linde, J., Mduma, E., Auestad, B. & Perlman, J. Neonatal outcome following cord clamping after onset of spontaneous respiration. Pediatrics 134, 265–272 (2014).
Knol, R. et al. Physiological versus time based cord clamping in very preterm infants (Abc3): a parallel-group, multicentre, randomised, controlled superiority trial. Lancet Reg. Health Eur. 48, 101146 (2025).
Laptook, A. R., Corbett, R. J., Nguyen, H. T., Peterson, J. & Nunnally, R. L. Alterations in cerebral blood flow and phosphorylated metabolites in piglets during and after partial ischemia. Pediatr. Res 23, 206–211 (1988).
Vannucci, R. C., Christensen, M. A. & Yager, J. Y. Nature, time-course, and extent of cerebral edema in perinatal hypoxic-ischemic brain damage. Pediatr. Neurol. 9, 29–34 (1993).
Williams, C. E., Gunn, A. & Gluckman, P. D. Time course of intracellular edema and epileptiform activity following prenatal cerebral ischemia in sheep. Stroke 22, 516–521 (1991).
Miller, J. A. Factors in neonatal resistance to anoxia. I. Temperature and survival of newborn guinea pigs under anoxia. Science 110, 113–114 (1949).
Ikonomidou, C., Mosinger, J. L. & Olney, J. W. Hypothermia enhances protective effect of mk-801 against hypoxic/ischemic brain damage in infant rats. Brain Res. 487, 184–187 (1989).
Young, R. S., Olenginski, T. P., Yagel, S. K. & Towfighi, J. The effect of graded hypothermia on hypoxic-ischemic brain damage: a neuropathologic study in the neonatal rat. Stroke 14, 929–934 (1983).
Laptook, A. R. et al. Modest hypothermia provides partial neuroprotection for ischemic neonatal brain. Pediatr. Res. 35, 436–442 (1994).
Thoresen, M. et al. Mild hypothermia after severe transient hypoxia-ischemia ameliorates delayed cerebral energy failure in the newborn piglet. Pediatr. Res. 37, 667–670 (1995).
Haaland, K., Loberg, E. M., Steen, P. A. & Thoresen, M. Posthypoxic hypothermia in newborn piglets. Pediatr. Res 41, 505–512 (1997).
Laptook, A. R. et al. Modest hypothermia provides partial neuroprotection when used for immediate resuscitation after brain ischemia. Pediatr. Res. 42, 17–23 (1997).
Lorek, A. et al. Delayed (“Secondary”) cerebral energy failure after acute hypoxia-ischemia in the newborn piglet: continuous 48-hour studies by phosphorus magnetic resonance spectroscopy. Pediatr. Res. 36, 699–706 (1994).
Penrice, J. et al. Proton magnetic resonance spectroscopy of the brain during acute hypoxia-ischemia and delayed cerebral energy failure in the newborn piglet. Pediatr. Res. 41, 795–802 (1997).
Williams, C. E., Gunn, A. J., Mallard, C. & Gluckman, P. D. Outcome after ischemia in the developing sheep brain: an electroencephalographic and histological study. Ann. Neurol. 31, 14–21 (1992).
Jensen, E. C., Bennet, L., Hunter, C. J., Power, G. G. & Gunn, A. J. Post-hypoxic hypoperfusion is associated with suppression of cerebral metabolism and increased tissue oxygenation in near-term fetal sheep. J. Physiol. 572, 131–139 (2006).
Bennet, L., Roelfsema, V., Pathipati, P., Quaedackers, J. S. & Gunn, A. J. Relationship between evolving epileptiform activity and delayed loss of mitochondrial activity after asphyxia measured by near-infrared spectroscopy in preterm fetal sheep. J. Physiol. 572, 141–154 (2006).
Leys, K. et al. Pharmacokinetics during therapeutic hypothermia in neonates: from pathophysiology to translational knowledge and physiologically-based pharmacokinetic (Pbpk) modeling. Expert Opin. Drug Metab. Toxicol. 19, 461–477 (2023).
Pang, R. et al. Melatonin reduces brain injury following inflammation-amplified hypoxia-ischemia in a translational newborn piglet study of neonatal encephalopathy. J. Pineal Res. 76, e12962 (2024).
Gunn, A. J., Gunn, T. R., de Haan, H. H., Williams, C. E. & Gluckman, P. D. Dramatic neuronal rescue with prolonged selective head cooling after ischemia in fetal lambs. J. Clin. Investig. 99, 248–256 (1997).
Gunn, A. J., Gunn, T. R., Gunning, M. I., Williams, C. E. & Gluckman, P. D. Neuroprotection with prolonged head cooling started before postischemic seizures in fetal sheep. Pediatrics 102, 1098–1106 (1998).
Gunn, A. J., Bennet, L., Gunning, M. I., Gluckman, P. D. & Gunn, T. R. Cerebral hypothermia is not neuroprotective when started after postischemic seizures in fetal sheep. Pediatr. Res. 46, 274–280 (1999).
Davidson, J. O. et al. Extending the duration of hypothermia does not further improve white matter protection after ischemia in term-equivalent fetal sheep. Sci. Rep. 6, 25178 (2016).
Alonso-Alconada, D. et al. Brain cell death is reduced with cooling by 3.5 degrees C to 5 degrees C but increased with cooling by 8.5 degrees C in a piglet asphyxia model. Stroke 46, 275–278 (2015).
Mitra, S. et al. Proton magnetic resonance spectroscopy lactate/N-acetylaspartate within 2 weeks of birth accurately predicts 2-year motor, cognitive and language outcomes in neonatal encephalopathy after therapeutic hypothermia. Arch. Dis. Child Fetal Neonatal Ed. 104, F424–F432 (2019).
Azzopardi, D. et al. Prospective qualification of early cerebral biomarkers in a randomised trial of treatment with xenon combined with moderate hypothermia after birth asphyxia. EBioMedicine 47, 484–491 (2019).
Pang, R. et al. Proton magnetic resonance spectroscopy lactate/N-acetylaspartate within 48 H predicts cell death following varied neuroprotective interventions in a piglet model of hypoxia-ischemia with and without inflammation-sensitization. Front. Neurol. 11, 883 (2020).
Gunn, A. J., Gluckman, P. D. & Gunn, T. R. Selective head cooling in newborn infants after perinatal asphyxia: a safety study. Pediatrics 102, 885–892 (1998).
Jacobs, S. E. et al. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst. Rev. 2013, CD003311 (2013).
Gluckman, P. D. et al. Selective head cooling with mild systemic hypothermia after neonatal encephalopathy: multicentre randomised trial. Lancet 365, 663–670 (2005).
Shankaran, S. et al. Whole-body hypothermia for neonates with hypoxic-ischemic encephalopathy. N. Engl. J. Med. 353, 1574–1584 (2005).
Azzopardi, D. V. et al. Moderate hypothermia to treat perinatal asphyxial encephalopathy. N. Engl. J. Med. 361, 1349–1358 (2009).
Edwards, A. D. et al. Neurological outcomes at 18 months of age after moderate hypothermia for perinatal hypoxic ischaemic encephalopathy: synthesis and meta-analysis of trial data. BMJ 340, c363 (2010).
Gunn, A. J. et al. Therapeutic hypothermia translates from ancient history in to practice. Pediatr. Res 81, 202–209 (2017).
Regier, D. A. et al. Cost-effectiveness of therapeutic hypothermia to treat neonatal encephalopathy. Value Health 13, 695–702 (2010).
Garegrat, R. et al. Whole-body hypothermia in mild neonatal encephalopathy: protocol for a multicentre phase iii randomised controlled trial. BMC Pediatr. 24, 460 (2024).
Molloy, E. J. et al. Neuroprotective therapies in the NICU in term infants: present and future. Pediatr. Res. 93, 1819–1827 (2023).
Dall’Asta, A., Melito, C., Morganelli, G., Lees, C. & Ghi, T. Determinants of placental insufficiency in fetal growth restriction. Ultrasound Obstet. Gynecol. 61, 152–157 (2023).
Wareing, M., Myers, J. E., O’Hara, M. & Baker, P. N. Sildenafil citrate (viagra) enhances vasodilatation in fetal growth restriction. J. Clin. Endocrinol. Metab. 90, 2550–2555 (2005).
Zoma, W. D., Baker, R. S. & Clark, K. E. Effects of combined use of sildenafil citrate (viagra) and 17beta-estradiol on ovine coronary and uterine hemodynamics. Am. J. Obstet. Gynecol. 190, 1291–1297 (2004).
Refuerzo, J. S. et al. Sildenafil citrate and fetal outcome in pregnant rats. Fetal Diagn. Ther. 21, 259–263 (2006).
Sibley, C. P. Treating the dysfunctional placenta. J. Endocrinol. 234, R81–R97 (2017).
Miller, S. L., Loose, J. M., Jenkin, G. & Wallace, E. M. The effects of sildenafil citrate (viagra) on uterine blood flow and well being in the intrauterine growth-restricted fetus. Am. J. Obstet. Gynecol. 200, 102 e101–107 (2009).
Pels, A. et al. Strider (sildenafil therapy in dismal prognosis early onset fetal growth restriction): an international consortium of randomised placebo-controlled trials. BMC Preg. Childbirth 17, 440 (2017).
Groom, K. M. et al. Strider Nzaus: a multicentre randomised controlled trial of sildenafil therapy in early-onset fetal growth restriction. BJOG 126, 997–1006 (2019).
Sharp, A. et al. Maternal sildenafil for severe fetal growth restriction (strider): a multicentre, randomised, placebo-controlled, double-blind trial. Lancet Child Adolesc. Health 2, 93–102 (2018).
Hawkes, N. Trial of viagra for fetal growth restriction is halted after baby deaths. BMJ 362, k3247 (2018).
Pels, A. et al. Maternal sildenafil vs placebo in pregnant women with severe early-onset fetal growth restriction: a randomized clinical trial. JAMA Netw. Open 3, e205323 (2020).
Symonds, M. E. & Budge, H. Comprehensive literature search for animal studies may have saved strider trial. BMJ 362, k4007 (2018).
Satterfield, M. C., Bazer, F. W., Spencer, T. E. & Wu, G. Sildenafil citrate treatment enhances amino acid availability in the conceptus and fetal growth in an ovine model of intrauterine growth restriction. J. Nutr. 140, 251–258 (2010).
Funding
B.J.A., S.B.H., G.R.P., and S.L.M. receive funding support from the National Health and Medical Research Council of Australia, and the Victorian Government’s Operational Infrastructure Support Program. L.B. and A.J.G., Health Research Council of New Zealand (grant numbers 17/601, 20/437, 22/559). E.M. is supported by the Health Research Board Ireland, and Research Ireland, and NJR receives funding from the UKRI Medical Research Council (MRC) Developmental Pathway Funding Scheme (DPFS), grant number MR/X030067/1, the Bill and Melinda Gates Foundation (INV-002322) supported by the National Institute for Health and Care Research, and University College London Hospitals Biomedical Research Centre.
Author information
Authors and Affiliations
Contributions
S.L.M. conceptualised the article and all authors—B.J.A., S.B.H., A.J.G., L.B., E.M., N.J.R., G.R.P., and S.L.M. wrote and edited the manuscript for intellectual content. All authors have approved the final version of this manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Allison, B.J., Hooper, S.B., Gunn, A.J. et al. A reduction in large animal research threatens the perinatal translation research pipeline. Pediatr Res (2025). https://doi.org/10.1038/s41390-025-04686-7
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41390-025-04686-7