Abstract
Background
Prostate cancer remains the most frequently diagnosed cancer among men. High-Intensity Focused Ultrasound (HIFU) has emerged as a thermal ablative technique for partial-gland-ablation (PGA), aiming to minimize collateral damage while maximizing tumor control. Monitoring after HIFU PGA relies on serial PSA testing, multiparametric-MRI, and biopsies. The diagnostic accuracy of MRI for clinically-significant cancer(csPCa) recurrence is challenging.
Objective
This systematic review and meta-analysis aim to evaluate the accuracy of MRI in detecting early recurrence of localized prostate cancer following HIFU PGA.
Methods
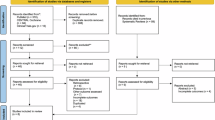
Adhering to PRISMA guidelines, a comprehensive literature search was conducted until May 8th 2024 using MEDLINE and Scopus. The inclusion criteria encompassed randomized controlled trials and cohort studies involving men diagnosed with localized prostate cancer who had as primary treatment HIFU PGA. The primary outcome measures included the sensitivity, specificity, positive-predictive value (PPV), and negative-predictive value (NPV) of MRI for csPCa(ISUP ≥ 2) based on biopsy results. We pooled data from studies with sufficient csPCa and csPCa-free patients (≥5) post HIFU for statistical analysis.
Results
Fifteen studies meet the inclusion criteria, encompassing 1093 patients and 12 studies were eligible for meta-analysis. MRI sensitivity in detecting clinically-significant prostate cancer (csPCa) recurrence post HIFU PGA varied widely (0–89%), with a pooled sensitivity of 0.52 (95% CI:0.36–0.68). Specificity ranged from 44% to 100%, with a pooled specificity of 0.81 (95% CI:0.68–0.91). The pooled NPV was 0.82 (95% CI:0.72–0.90), and the pooled PPV was 0.50 (95% CI:0.35–0.65). Three studies reported in-field diagnostic performance with sensitivities ranging from 0.42 to 0.80 and specificities from 0.45 to 0.97.
Conclusion
MRI accuracy for clinically-significant recurrence after partial gland ablation with HIFU for localized prostate cancer shows low diagnostic performance in the treated lobe with pooled sensitivity of 0.52 (95% CI:0.36–0.68) and specificity of 0.81 (95% CI:0.68–0.91). Limits of this review include the low number of studies reporting about site of recurrence in or out of the treated lobe.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71:209–49.
Valerio M, Cerantola Y, Eggener SE, Lepor H, Polascik TJ, Villers A, et al. New and Established Technology in Focal Ablation of the Prostate: A Systematic Review. Eur Urol 2017;71:17–34.
Ploussard G, Fiard G, Barret E, Brureau L, Créhange G, Dariane C, et al. French AFU Cancer Committee Guidelines - Update 2022-2024: prostate cancer - Diagnosis and management of localised disease. Prog Urol. 2022;32:1275–372.
Cornford P, van den Bergh RCN, Briers E, Van den Broeck T, Brunckhorst O, Darraugh J, et al. EAU-EANM-ESTRO-ESUR-ISUP-SIOG Guidelines on Prostate Cancer-2024 Update. Part I: Screening, Diagnosis, and Local Treatment with Curative Intent. Eur Urol. 2024;86:148–63.
Huber PM, Afzal N, Arya M, Boxler S, Dudderidge T, Emberton M, et al. Prostate Specific Antigen Criteria to Diagnose Failure of Cancer Control following Focal Therapy of Nonmetastatic Prostate Cancer Using High Intensity Focused Ultrasound. J Urol. 2020;203:734–42.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A. Rayyan-a web and mobile app for systematic reviews. Syst Rev. 2016;5:210.
Whiting PF, Rutjes AWS, Westwood ME, Mallett S, Deeks JJ, Reitsma JB, et al. QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med. 2011;155:529–36.
Freeman MF, Tukey JW. Transformations Related to the Angular and the Square Root. Ann Math Stat. 1950;21:607–11.
Deeks JJ, Altman DG, Bradburn MJ. Statistical Methods for Examining Heterogeneity and Combining Results from Several Studies in Meta‐Analysis. 2024; Available from: https://onlinelibrary.wiley.com/doi/10.1002/9780470693926.ch15.
Wang N. Conducting Meta-analyses of Proportions in R. J Behav Data Sci. 2023;3:64–126.
Tay KJ, Schulman AA, Sze C, Tsivian E, Polascik TJ. New advances in focal therapy for early stage prostate cancer. Expert Rev Anticancer Ther. 2017;17:737–43.
Dickinson L, Ahmed HU, Hindley RG, McCartan N, Freeman A, Allen C, et al. Prostate-specific antigen vs. magnetic resonance imaging parameters for assessing oncological outcomes after high intensity-focused ultrasound focal therapy for localized prostate cancer. Urol Oncol. 2017;35:30.e9–30.e15.
von Hardenberg J, Westhoff N, Baumunk D, Hausmann D, Martini T, Marx A, et al. Prostate cancer treatment by the latest focal HIFU device with MRI/TRUS-fusion control biopsies: A prospective evaluation. Urol Oncol. 2018;36:401.e1–401.e9.
Lotte R, Lafourcade A, Mozer P, Conort P, Barret E, Comperat E, et al. Multiparametric MRI for Suspected Recurrent Prostate Cancer after HIFU:Is DCE still needed? Eur Radiol. 2018;28:3760–9.
Rosenhammer B, Niessen C, Rotzinger L, Reiss J, Schnabel MJ, Burger M, et al. Oncological Outcome and Value of Postoperative Magnetic Resonance Imaging after Focal High-Intensity Focused Ultrasound Therapy for Prostate Cancer. Urol Int. 2019;103:270–8.
Bass R, Fleshner N, Finelli A, Barkin J, Zhang L. Klotz L. Oncologic and Functional Outcomes of Partial Gland Ablation with High Intensity Focused Ultrasound for Localized Prostate Cancer. J Urol. 2019;201:113–9.
Mortezavi A, Krauter J, Gu A, Sonderer J, Bruhin J, Reeve KA, et al. Extensive Histological Sampling following Focal Therapy of Clinically Significant Prostate Cancer with High Intensity Focused Ultrasound. J Urol. 2019;202:717–24.
Shoji S, Hiraiwa S, Uemura K, Nitta M, Hasegawa M, Kawamura Y, et al. Focal therapy with high-intensity focused ultrasound for the localized prostate cancer for Asian based on the localization with MRI-TRUS fusion image-guided transperineal biopsy and 12-cores transperineal systematic biopsy: prospective analysis of oncological and functional outcomes. Int J Clin Oncol. 2020;25:1844–53.
Bacchetta F, Martins M, Regusci S, Jichlinski P, Meuwly JY, Lucca I, et al. The utility of intraoperative contrast-enhanced ultrasound in detecting residual disease after focal HIFU for localized prostate cancer. Urol Oncol. 2020;38:846.e1–846.e7.
Rompré-Brodeur A, Marcq G, Tholomier C, Fugaru I, Loutochin O, Anidjar M, et al. Role of Systematic Control Biopsies following Partial Gland Ablation with High-Intensity Focused Ultrasound for Clinically Significant Prostate Cancer. J Urol. 2021;206:1177–83.
Yee CH, Chiu PKF, Teoh JYC, Ng CF, Chan CK, Hou SM. High-Intensity Focused Ultrasound (HIFU) Focal Therapy for Localized Prostate Cancer with MRI-US Fusion Platform. Adv Urol. 2021;2021:7157973.
Ahn H, Hwang SI, Lee HJ, Kim SY, Cho JY, Lee H, et al. Diagnostic performance of MRI for prediction of recurrent prostate cancer after high-intensity focused ultrasound: a systematic review and meta-analysis. Prostate Int. 2023;11:59–68.
Khandwala YS, Morisetty S, Ghanouni P, Fan RE, Soerensen SJC, Rusu M, et al. Evaluation of post-ablation mpMRI as a predictor of residual prostate cancer after focal high intensity focused ultrasound (HIFU) ablation. Urol Oncol. 2022;40:489.e9–489.e17.
Pausch AM, Elsner C, Rupp NJ, Eberli D, Hötker AM. MRI-based monitoring of prostate cancer after HIFU: Inter-reader agreement and diagnostic performance of the PI-FAB score. Eur J Radiol. 2024;175:111463.
Dellabella M, Branchi A, Di Rosa M, Pucci M, Gasparri L, Claudini R, et al. Oncological and functional outcome after partial prostate HIFU ablation with Focal-One®: a prospective single-center study. Prostate Cancer Prostatic Dis. 2021;24:1189–97.
Giganti F, Dickinson L, Orczyk C, Haider A, Freeman A, Emberton M, et al. Prostate Imaging after Focal Ablation (PI-FAB): A Proposal for a Scoring System for Multiparametric MRI of the Prostate After Focal Therapy. Eur Urol Oncol. 2023;6:629–34.
Light A, Mayor N, Cullen E, Kirkham A, Padhani AR, Arya M, et al. The Transatlantic Recommendations for Prostate Gland Evaluation with Magnetic Resonance Imaging After Focal Therapy (TARGET): A Systematic Review and International Consensus Recommendations. Eur Urol. 2024;85:466–82.
Barentsz JO, Weinreb JC, Verma S, Thoeny HC, Tempany CM, Shtern F, et al. Synopsis of the PI-RADS v2 Guidelines for Multiparametric Prostate Magnetic Resonance Imaging and Recommendations for Use. Eur Urol. 2016;69:41–9.
Panebianco V, Villeirs G, Weinreb JC, Turkbey BI, Margolis DJ, Richenberg J, et al. Prostate Magnetic Resonance Imaging for Local Recurrence Reporting (PI-RR): International Consensus -based Guidelines on Multiparametric Magnetic Resonance Imaging for Prostate Cancer Recurrence after Radiation Therapy and Radical Prostatectomy. Eur Urol Oncol 2021;4:868–76.
Author information
Authors and Affiliations
Contributions
DS and JO were responsible for conceptualization, data collection and writing. JL provided statistical analysis and methodological guidance. PP, EB, XL, RRP, GP, and AV contributed through senior editorial review. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41391_2024_885_MOESM1_ESM.docx (download DOCX )
Supplementary Table 1: Leave-one-out Sensitivity analyses of the pooled performance of MRI alone to diagnose early recurrence of csPCa
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Séguier, D., Puech, P., Barret, E. et al. MRI accuracy for recurrence after partial gland ablation with HIFU for localized prostate cancer. A systematic review and meta-analysis. Prostate Cancer Prostatic Dis 28, 592–600 (2025). https://doi.org/10.1038/s41391-024-00885-1
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41391-024-00885-1
This article is cited by
-
Focal radiation therapies for localized prostate cancer: a systematic review of clinical evidence and outcomes
Prostate Cancer and Prostatic Diseases (2025)