Abstract
Background
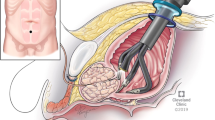
Robot-Assisted Simple Prostatectomy (RASP) is recommended for the treatment of large prostate glands. The introduction of the Single-Port (SP) platform in 2018 has enabled transvesical approach to SP-RASP with promising outcomes. Our aim was to describe the functional and urinary continence outcomes of SP-RASP.
Methods
Clinical and surgical data from all consecutive patients who underwent transvesical SP-RASP between February 2020 and March 2024 were collected in a prospectively maintained institutional dataset and retrospectively analyzed. All procedures were performed using the da Vinci SP platform without any conversions to open surgery. Postoperative outcomes were gathered and analyzed, with a particular focus on the incidence of urinary incontinence (UI) and the time to continence recovery.
Results
Overall, 89 patients underwent SP-RASP, with a median prostate size of 110 grams (90–171.5) and a median PSA level of 5.5 mg/dl (2.77–10.93). All patients were on at least one prostate medication prior to surgery. Preoperative evaluations showed a median International Prostate Symptoms Score (IPSS) of 23 (20-27), Quality of Life (QoL) of 4 (3-5), and Post-voiding Residual (PVR) of 153 ml (60–400). The median operative time was 180 min (164–200), with a median estimated blood loss of 100 ml (30–180). Postoperatively, no patients required continuous bladder irrigation. The median postoperative opioid intake was 6.5 morphine equivalents (0–10), with over 78% not requiring narcotics after discharge. Overall, 77.5% were same day discharged. No Clavien-Dindo > 2 complications were recorded. The median follow-up time was 18 (7-35) months. At the last postoperative urological evaluation, the median IPSS was 5 (3-7), QoL was 1 (0-2), and PVR was 10 ml (0-25). Only 4 patients (4.5%) experienced UI postoperatively, and all were continent within 3 months.
Conclusions
The UI incidence rate and functional outcomes of SP-RASP are very encouraging, likely due to precise adenoma and urethra dissection and bladder neck reconstruction. This approach also allows for same-day discharge.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data associated with the paper are not publicly available, but they are available from the corresponding author on reasonable request.
References
Berry SJ, Coffey DS, Walsh PC, Ewing LL. The development of human benign prostatic hyperplasia with age. J Urol. 1984;132:474–9.
Panel G, Lerner LB, Barry MJ, Anurag, Das K, Gandhi MC, et al. Management of lower urinary tract symptoms attributed to benign prostatic hyperplasia (BPH): AUA guideline amendment 2023. J Urol. 2024;211:11–19.
Lee MS, Assmus MA, Ganesh M, Han J, Helon J, Mai Q, et al. An outcomes comparison between holmium laser enucleation of the prostate, open simple prostatectomy, and robotic simple prostatectomy for large gland Benign prostatic hypertrophy. Urology. 2023;173:180–6.
Autorino R, Zargar H, Mariano MB, Sanchez-Salas R, Sotelo RJ, Chlosta PL, et al. Perioperative outcomes of robotic and laparoscopic simple prostatectomy: A european-American multi-institutional analysis. Eur Urol. 2015;68:86–94.
Franco A, Ditonno F, Manfredi C, Johnson AD, Mamgain A, Feldman-Schultz O, et al. Robot-assisted surgery in the field of urology: The most pioneering Approaches 2015–2023. Res Rep Urol. 2023;15:453–70.
Kaouk J, Sawczyn G, Wilson C, Aminsharifi A, Fareed K, Garisto J, et al. Single-port percutaneous transvesical simple prostatectomy using the SP robotic system: initial clinical experience. Urology. 2020;141:173–7.
Cannoletta D, Pellegrino A, Pettenuzzo G, Pacini M, Sauer RC, Torres-Anguiano JR, et al. Single-port transvesical vesico-vaginal fistula repair: an initial experience. Int Braz J Urol. 2024;50:502–3.
Talamini S, Lai A, Palmer C, van de Walle G, Zuberek M, Crivellaro S. Surgical treatment of benign prostatic hyperplasia: Thulium enucleation versus single-port transvesical robotic simple prostatectomy. BJUI Compass. 2023;4:549–55.
Abou Zeinab M, Ramos R, Ferguson EL, Okhawere KE, Iarajuli T, Wilder S, et al. Single port versus multiport robot-assisted simple prostatectomy: a multi-institutional study from the single-port advanced research consortium (SPARC). Urology. 2023;176:94–101.
Ganesan V, Steinberg RL, Garbens A, Trivedi H, Sorokin I, Roehrborn CA, et al. Single-port robotic-assisted simple prostatectomy is associated with decreased post-operative narcotic use in a propensity score matched analysis. J Robot Surg. 2022;16:295–300.
Franco A, Ditonno F, Manfredi C, Pellegrino AA, Licari LC, Bologna E, et al. Single port robot-assisted radical and simple prostatectomy: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2024.
Franco A, Ditonno F, Manfredi C, Licari LC, Bologna E, Cherullo EE, et al. Robot-assisted single-port transvesical enucleation of the prostate: step-by-step technique and early single-centre experience. BJU Int. 2024;133:778–82.
Assel M, Sjoberg D, Elders A, Wang X, Huo D, Botchway A, et al. Guidelines for reporting of statistics for clinical research in urology. BJU Int. 2019;123:401–10.
Castellani D, Enikeev D, Gokce MI, Petov V, Gadzhiev N, Mahajan A, et al. Influence of prostate volume on the incidence of complications and urinary incontinence following thulium fiber laser enucleation of the prostate: results from multicenter, real-world experience of 2732 patients. Eur Urol Open Sci. 2024;63:38–43.
Capogrosso P, Ventimiglia E, Fallara G, Schifano N, Costa A, Candela L, et al. Holmium laser enucleation of the prostate is associated with complications and sequelae even in the hands of an experienced surgeon following completion of the learning curve. Eur Urol Focus. 2023;9:813–21.
Hashim H, Herrmann T, Malde S, Netsch C, De Nunzio C, Rieken M, et al. Non-neurogenic male lower urinary tract symptoms (LUTS). EAU Guidelines;2024.
Ditonno F, Franco A, Manfredi C, Veccia A, De Nunzio C, De Sio M, et al. Single-port robot-assisted simple prostatectomy: techniques and outcomes. World J Urol. 2024;42:98.
Hout M, Gurayah A, Arbelaez MCS, Blachman-Braun R, Shah K, Herrmann TRW, et al. Incidence and risk factors for postoperative urinary incontinence after various prostate enucleation procedures: systemic review and meta-analysis of PubMed literature from 2000 to 2021. World J Urol. 2022;40:2731–45.
Abou Zeinab M, Beksac AT, Corse T, Talamini S, Morgantini L, Kaviani A, et al. The multi-institutional experience in single-port robotic transvesical simple prostatectomy for Benign prostatic hyperplasia management. J Urol. 2022;208:369–78.
Kaouk J, Ferguson E, Ramos-Carpinteyro R, Chavali J, Geskin A, Cummings KC, et al. Transvesical percutaneous access allows for epidural anesthesia without mechanical ventilation in single-port robotic radical and simple prostatectomy. Urology. 2023;175:209–15.
Lee H, So S, Cho MC, Cho SY, Paick JS, Oh SJ. Clinical outcomes of holmium laser enucleation of the prostate: A large prospective registry-based patient cohort study under regular follow-up protocol. Investig Clin Urol. 2024;65:361–7.
Abou Zeinab M, Kaviani A, Ferguson E, Beksac AT, Schwen Z, Gill B, et al. Single-port transvesical versus open simple prostatectomy: a perioperative comparative study. Prostate Cancer Prostatic Dis. 2023;26:538–42.
Steinberg RL, Passoni N, Garbens A, Johnson BA, Gahan JC. Initial experience with extraperitoneal robotic-assisted simple prostatectomy using the da Vinci SP surgical system. J Robot Surg. 2020;14:601–7.
Author information
Authors and Affiliations
Contributions
M.P., L.L., S.C. have given a substantial contribution to the design of the study; M.P., G.A., A. Ma., R.B. contributed in the first draft of the manuscript; M.P., S.C., L.M., L.L., R.C., G.B., H.H. have given their contribution in data collecting and data analysis; G.P., H.H., M.P., A.Z., S.C., J.T., A.M., revised the manuscript critically. All Authors have participated to drafting the manuscript. All Authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
Dr. Simone Crivellaro is a consultant for Intuitive, other authors have nothing to disclose.
Ethics approval and consent to participate
Institutional review board approval (protocol n° 2017-0152 from Office of Vice Chancellor for Research, University of Illinois at Chicago) was obtained previously to data collecting and analysis. This study was conducted in accordance with ethical principles given by the Helsinki Declaration about clinical studies on human participants, and written informed consent was obtained from all subjects.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41391_2024_923_MOESM1_ESM.docx (download DOCX )
Supplementary Table. Complications rate and Urinary Incontinence rate according to previous prostate biopsy and incidental PCa finding.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pacini, M., Lambertini, L., Avesani, G. et al. Single-port transvesical simple prostatectomy for the surgical treatment of benign prostatic hyperplasia: functional and continence outcomes. Prostate Cancer Prostatic Dis 28, 451–456 (2025). https://doi.org/10.1038/s41391-024-00923-y
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41391-024-00923-y
This article is cited by
-
Short term results after minimally invasive treatments for benign prostatic enlargement: the first randomized trial comparing transperineal laser ablation and water vapor ablation
Prostate Cancer and Prostatic Diseases (2025)
-
Benign Prostatic Hyperplasia and Sexual Dysfunction: Review of the Impact of New Medical and Surgical Therapies on Sexual Health
Current Urology Reports (2025)
-
Transvesical robot-assisted radical prostatectomy for recalcitrant bladder neck contracture after holmium laser enucleation of prostate: initial experience and clinical outcomes
World Journal of Urology (2025)