Abstract
Background
The evaluation and management of lower urinary symptoms (LUTS) experienced in the immediate post-operative period after benign prostatic obstruction surgery (BPO), remain unclear. Aim of our study is to systematically report the evidence on management of post-operative transient urinary symptoms after BPO surgery.
Methods
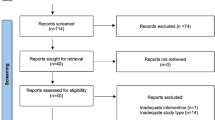
A systematic review of the literature was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-analyses checklist (PRISMA). PubMed, Embase, Scopus and Cochrane databases were searched up to March 2025. Studies evaluating pharmacotherapy, phytotherapy and/or physical treatment for post-operative transient LUTS in men aged were evaluated. Only randomized clinical trials (RCTs) were included.
Results
Overall, nine RCTs were included. Among the surgical techniques investigated, most data were available for transurethral resection of the prostate. The methods used to assess post-operative LUTS, as well as the timing of evaluation, varied considerably across studies. The most commonly submitted questionnaire was the International Prostate Symptom Score, and the most frequently performed diagnostic tool was uroflowmetry. Anticholinergic drugs seems to have the greatest efficacy in improving post-operative LUTS, even if the level of evidence is low. In contrast, alpha-blockers did not appear to offer significant additional benefits in this setting of patients. Phytocomplexes (Graminex G63, Curcumin complexes) were effective in improving patients’ quality of life (QoL) after BPO surgery. Pelvic floor muscle exercises (PFME) also demonstrated a reduction in symptom-related bother.
Conclusion
Current strategies for evaluating and managing transient postoperative LUTS are heterogeneous, and available evidence remains limited. Anticholinergic agents and phytotherapeutic compounds are among the most commonly prescribed treatments, though their efficacy is suboptimal. High-quality randomized trials are needed to provide robust clinical recommendations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Data and material are available upon request
References
Egan KB. The Epidemiology of Benign Prostatic Hyperplasia Associated with Lower Urinary Tract Symptoms. Urologic Clin North Am. 2016;43:289–97.
Gravas S, Manuel-Palacios J, Chavan C, Roehrborn CG, Oelke M, Averbeck MA, et al. Modeling study of the effect of placebo and medical therapy on storage and voiding symptoms, nocturia, and quality of life in men with prostate enlargement at risk for progression. Prostate Cancer Prostatic Dis Springe Nat. 2024;27:469–77.
Feiertag JH, Clark JY. National Trends in Surgical Management for Benign Prostatic Hyperplasia From 2013 to 2019 in the United States. Urol Pr. 2024;11:303–11.
Del Giudice F, Oh JK, Basran S, Nicaise E, Song PH, Kim W, et al. Recent trends in the diagnostic and surgical management of benign prostatic hyperplasia in the U.S. from 2004 to 2017: Annual Changes in the Selection of Treatment Options and Medical Costs. Applied Sciences (Switzerland). MDPI; 2022;12. https://doi.org/10.3390/app12178697.
Daniels JP, Patel DN, Galvan GC, Friedrich NA, Das S, Akhavein A, et al. Investigating trends in interest for benign prostatic hyperplasia surgery options using Google Trends. Prostate Cancer Prostatic Dis Springe Nat. 2024;27:150–2.
Nguyen DD, Li T, Ferreira R, Baker Berjaoui M, Nguyen ALV, Chughtai B, et al. Ablative minimally invasive surgical therapies for benign prostatic hyperplasia: A review of Aquablation, Rezum, and transperineal laser prostate ablation. Prostate Cancer Prostatic Dis. Springer Nature; 2024. p. 22–8.
Singla N, Singla AK Evaluation and Management of Lower Urinary Tract Symptoms After Outlet Surgery for Benign Prostatic Hyperplasia. Curr Bladder Dysfunct Rep. Current Medicine Group LLC 1; 2016. p. 242–7.
Kim SJ, Al Hussein Alawamlh O, Chughtai B, Lee RK Lower Urinary Tract Symptoms Following Transurethral Resection of Prostate. Curr Urol Rep. Current Medicine Group LLC 1; 2018. https://doi.org/10.1007/s11934-018-0838-4.
Rassweiler J, Teber D, Kuntz R, Hofmann R. Complications of transurethral resection of the prostate (TURP)-incidence, management, and prevention. Eur Urol. 2006. 969–80.
Campbell J, Reid J, Ordon M, Welk B. The utilization of Benign prostatic hyperplasia and bladder-related medications after a transurethral prostatectomy. Urol Elsevier Inc. 2019;130:126–31.
Puri K, Smaling A, Lloyd SN. How is follow-up after transurethral prostatectomy best performed? BJU Int [Internet] BJU Int. 1999;84:795–8. cited 2025 Jul 13].
Cindolo L, Marchioni M, Emiliani E, De Francesco P, Primiceri G, Castellan P, et al. Bladder neck contracture after surgery for benign prostatic obstruction. Minerva Urol Nephrol. 2017;69. https://doi.org/10.23736/S0393-2249.16.02777-6.
Tsai CH, Fan YH, Lin ATL, Huang WJ. Risk factors for pharmacotherapy for storage symptoms after transurethral resection of the prostate in patients with benign prostatic hyperplasia. LUTS: Low Urinary Trac Symptoms John Wiley Sons Inc. 2022;14:329–33.
Chughtai B, Simma-Chiang V, Kaplan SA Evaluation and management of post-transurethral resection of the prostate lower urinary tract symptoms. Curr Urol Rep. Current Medicine Group LLC 1; 2014. https://doi.org/10.1007/s11934-014-0434-1.
Hashim H, Herrmann T, Malde, Netsch C, De Nunzio C, Rieken M, et al. EAU guidelines on non-neurogenic male lower urinary tract symptoms (LUTS). 2025. https://uroweb.org/guidelines/management-of-non-neurogenic-male-luts.
Rieken M, de Nunzio C, Cornu JN, Ramasamy R, Misrai V, Malde S, et al. Medical treatment incidence and persistence after surgical relief of lower urinary tract symptoms suggestive of Benign Prostatic Obstruction: A Critical Analysis of the Literature. Eur Urol Focus. Elsevier B.V.; 2024. 421–31.
Tehranchi A, Rezaei Y, Shojaee R. Tolterodine to relieve urinary symptoms following transurethral resection of the prostate: a double-blind placebo-controlled randomized clinical trial. Korean J Urol Ⓒ Korean Urological Assoc [Internet]. 2014;55:260–4.
Shin YS, Zhang LT, You JH, Choi IS, Zhao C, Park JK. Efficacy and safety of tamsulosin hydrochloride 0.2 mg and combination of tamsulosin hydrochloride 0.2 mg plus solifenacin succinate 5 mg after transurethral resection of the prostate: A prospective, randomized controlled trial. Clin Inter Aging Dove Med Press Ltd. 2016;11:1301–7.
Sipal T, Akdere H. The relation between the storage symptoms before and after transurethral resection of the prostate, analysis of the risk factors and the prevention of the symptoms with solifenacin. Int Braz J Urol Braz Soc Urol. 2020;46:575–84.
Seli N CEI, Schm Id Li F, Orst FB, Hner SR, Gra Ber P. Oxybutynin in the treatment of early detrusor instability after transurethral resection of the prostate. Br J Urol. 1997;79:915–9.
Porru D, Campus G, Caria A, Madeddu G, Cucchi A, Rovereto B, et al. Impact of early pelvic floor rehabilitation after transurethral resection of the prostate. Neurourol Urodyn. 2001;20:53–9.
Hou CP, Chen TY, Chang CC, Lin YH, Chang PL, Chen CL, et al. Use of the SF-36 quality of life scale to assess the effect of pelvic floor muscle exercise on aging males who received transurethral prostate surgery. Clin Inter Aging. 2013;8:667–73.
Lee CL, Kuo HC. Treating overactive bladder symptoms after transurethral prostatic surgery for benign prostatic hyperplasia - Which medication to choose?. Tzu Chi Med J Wolters Kluwer Medknow Publ. 2023;35:312–6.
AB Di Pasquale, Cassani A, Masciovecchio S, Zasa G, Ranieri G, Romano G, et al. Postoperative treatment with phytotheraphy Graminex G63 (CERNILEN-Flogo®) after greenlight laser XPS (180W) photovaporization of the prostate (PVP), can affect patient’s quality of life? 2020. https://doi.org/10.26355/eurrev_202009_22858.
Cindolo L, Lombardo R, De Stefanis P, Varvello F, Oriti R. Efficacy of qurmin on post-operative lower urinary tract symptoms after photoselective vaporization of the prostate: a multicentre case-control study. J Urol Nephrol. 2021;8:5.
Wroclawski ML, Castellani D, Heldwein FL, Teles SB, Cha JD, Zhao H, et al. Shedding light on polypragmasy of pain after transurethral prostate surgery procedures: a systematic review and meta-analysis. World J Urol [Internet] World J Urol. 2021;39:3711–20.
Lombardo R, Russo GI, Romagnoli M, Tema G, Nacchia A, Franco A, et al. Yoga, benign prostatic hyperplasia and lower urinary tract symptoms: a new path for clinical trials. Prostate Cancer Prostatic Dis. 2024;27:432–4.
Hegazy M, Sheir KZ, Gaballah MA, Elshal AM. A randomized controlled trial evaluating low-intensity shockwave therapy for treatment of persistent storage symptoms following transurethral surgery for benign prostatic obstruction. Prostate Cancer Prostatic Dis Springe Nat. 2024;27:305–11.
Heiman J, Snead WM, DiBianco JM Persistent Lower Urinary Tract Symptoms After BPH Surgery. Curr Urol Rep. Springer; 2024. p. 125–31.
Orihuela E, Pow-Sang M, Motamedi M, Cowan DF, Warren MM. Mechanism of healing of the human prostatic urethra following thermal injury. Urology. 1996;48:600–8.
Wang X, Zhuo J, Luo G, Zhu Y, Yu D, Zhao R, et al. Androgen deprivation accelerates the prostatic urethra wound healing after thulium laser resection of the prostate by promoting re-epithelialization and regulating the macrophage polarization. Prostate. 2017;77:708–17.
Ninan N, Thomas S, Grohens Y. Wound healing in urology. Adv Drug Deliv Rev. 2015;82–83:93–105.
Huet R, Mathieu R, Rohou T, Peyronnet B, Manunta A, Verhoest G, et al. MRI assessment of tissue effects after 180-W XPS greenlight laser vaporization of the prostate. Lasers Surg Med. 2017;49:577–81.
de Nunzio C, Franco G, Rocchegiani A, Iori F, Leonardo C, Laurenti C. The evolution of detrusor overactivity after watchful waiting, medical therapy and surgery in patients with bladder outlet obstruction. J Urol. 2003;169:535–9.
Antunes AA, Iscaife A, Reis ST, Albertini A, Nunes MA, Lucon AM, et al. Can We Predict Which Patients will Experience Resolution of Detrusor Overactivity after Transurethral Resection of the Prostate?. J Urol. 2015;193:2028–32.
Castellani D, Rubilotta E, Fabiani A, Maggi M, Wroclawski ML, Teoh JY-C, et al. Correlation between transurethral interventions and their influence on type and duration of postoperative urinary incontinence: results from a systematic review and meta-analysis of comparative studies. J Endourol. 2022;36:1331–47.
Panel G, Lerner LB, Barry MJ, Anurag, Das K, Gandhi MC, et al. Management of lower urinary tract symptoms attributed to Benign prostatic hyperplasia: AUA Guideline 2023 Amendment Panel Staff and Consultants. 2023.
Yamaguchi O. Latest treatment for lower urinary tract dysfunction: Therapeutic agents and mechanism of action. Int J Urol. 2013;20:28–39.
Seki N, Masaoka H, Song Y, Dejima T, Sato Y, Maeda S. Efficacy and safety of Vibegron for the treatment of residual overactive bladder symptoms after laser vaporization of the prostate: a single-center prospective randomized controlled trial (VAPOR TRIAL). LUTS: Lower Urinary Tract Symptoms. John Wiley and Sons Inc; 2024;16. https://doi.org/10.1111/luts.12529.
De Nunzio C, Salonia A, Gacci M, Ficarra V Inflammation is a target of medical treatment for lower urinary tract symptoms associated with benign prostatic hyperplasia. World J Urol. Springer Science and Business Media Deutschland GmbH; 2020. 2771–9.
De Nunzio C, Kramer G, Marberger M, Montironi R, Nelson W, Schröder F, et al. The controversial relationship between benign prostatic hyperplasia and prostate cancer: the role of inflammation. Eur Urol. 2011;60:106–17.
Gravas S, De Nunzio C, Campos Pinheiro L, Ponce de León J, Skriapas K, Milad Z, et al. Development and validation of a clinical nomogram to predict prostatic inflammation in men with lower urinary tract symptoms. Prostate Cancer Prostatic Dis. Springer Nature; 2024; https://doi.org/10.1038/s41391-024-00857-5.
Sun X, Jin X, Leng K, Zhao Y, Zhang H. 180-W GreenLight laser photoselective vaporization with multiple triamcinolone acetonide injections for the treatment of bladder neck contractures. Lasers Med Sci Springe Sci Bus Media Dtschl GmbH. 2022;37:3115–21.
Zhang L, Liu S, Wu K, Mu X, Yang L. Management of highly recurrent bladder neck contractures via transurethral resection combined with intra- and post-operative triamcinolone acetonide injections. World J Urol Springe Sci Bus Media Dtschl GmbH. 2021;39:527–32.
Cosentino V, Fratter A, Cosentino M, Cosentino M. Anti-inflammatory effects exerted by Killox®, an innovative formulation of food supplement with curcumin, in urology. Eur Rev Med Pharmacol Sci. 2016;20:1390–8.
Cacciamani GE, Sholklapper T, Dell’Oglio P, Rocco B, Annino F, Antonelli A, et al. The Intraoperative Complications Assessment and Reporting with Universal Standards (ICARUS) Global Surgical Collaboration Project: Development of Criteria for Reporting Adverse Events During Surgical Procedures and Evaluating Their Impact on the Postoper. Eur Urol Focus [Internet] Elsevier B V. 2022;8:1847–58.
Au RC, Jenjitranant P, Cool DW, Izawa J, Inman B, Ward A, et al. Artificial intelligence may enhance the role of magnetic resonance imaging in prostate cancer focal therapy [Internet]. Prostate Cancer Prostatic Dis. Nature;2025 [cited 2025 Dec 4]. 1–4.
Lombardo R, Cicione A, Santoro G, De Nunzio C. ChatGPT in prostate cancer: myth or reality? [Internet]. Prostate Cancer Prostatic Dis. Nature;2023 [cited 2025 Dec 4]. 9–10.
Cocci A, Pezzoli M, Lo Re M, Russo GI, Asmundo MG, Fode M, et al. Quality of information and appropriateness of ChatGPT outputs for urology patients. Prostate Cancer Prostatic Dis [Internet] Nat. 2023;27:103–8.
Collin H, Keogh K, Basto M, Loeb S, Roberts MJ. ChatGPT can help guide and empower patients after prostate cancer diagnosis. Prostate Cancer Prostatic Dis [Internet] Nat. 2024;28:513–5.
Puerto Nino AK, Garcia Perez V, Secco S, De Nunzio C, Lombardo R, Tikkinen KAO, et al. Can ChatGPT provide high-quality patient information on male lower urinary tract symptoms suggestive of benign prostate enlargement?. Prostate Cancer Prostatic Dis [Internet] Nat. 2024;28:167–72.
Zhao Y, Zhang L, Zhang S, Li J, Shi K, Yao D, et al. Machine learning-based MRI imaging for prostate cancer diagnosis: systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2026;29:159–66.
Fong KY, Gauhar V, Herrmann TRW, Nedbal C, Enikeev D, Teoh JYC, et al. Machine learning models to predict postoperative incontinence after endoscopic enucleation of the prostate for benign prostatic hyperplasia: an EAU-Endourology study. Prostate Cancer Prostatic Dis. 2026;29:175–80.
Xie XR, Hou Y, Shan S, Zhi R, Wu CJ, Xia YF, et al. AI-aided diagnostic performance for prostate MRI: systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2025. https://doi.org/10.1038/s41391-025-01053-9.
Tun HM, Naing L, Malik OA, Rahman HA. Artificial intelligence (AI)-based tools in the diagnosis and management of prostate cancer: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2025. https://doi.org/10.1038/s41391-025-01060-w.
Author information
Authors and Affiliations
Contributions
CDeN: substantial contributions to the conception and design of the work; drafting the work, final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. GG: substantial contributions to the conception and design of the work; substantial contributions to the acquisition, analysis, and interpretation of data for the work, drafting the work, final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. RL: substantial contributions to the conception and design of the work; substantial contributions to the acquisition, analysis, and interpretation of data for the work; drafting the work, final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. AC: substantial contributions to the acquisition, analysis, and interpretation of data for the work; revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. JNC: substantial contributions to the acquisition, analysis, and interpretation of data for the work; revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. AF: substantial contributions to the acquisition, analysis, and interpretation of data for the work; revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. FF: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. SM: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. CM: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. CN: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. MR: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. SG: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. MG: revising the work critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gallo, G., Lombardo, R., Cicione, A. et al. Evaluation and management of transient lower urinary tract symptoms (LUTS) after surgery for Benign prostatic obstruction (BPO): a systematic review. Prostate Cancer Prostatic Dis (2026). https://doi.org/10.1038/s41391-026-01082-y
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41391-026-01082-y