Abstract
Study design
This is an animal study.
Objectives
Metformin is a safe drug for controlling blood sugar in diabetes. It has been shown that metformin improves locomotor recovery after spinal cord injury (SCI). Neuropathic pain is also a disturbing component of SCI. It is indicated that metformin has neuroprotective and anti-inflammatory effects, which attenuate neuropathic pain and hyperalgesia in injured nerves. Thus, we evaluated metformin’s therapeutic effects on SCI neuroinflammation and its sensory and locomotor complications. Meanwhile, results were compared to minocycline, an anti-neuroinflammation therapy in SCI.
Setting
Experimental Medicine Research Center, Tehran University of Medical Sciences, Iran
Methods
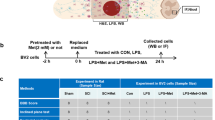
In an animal model of SCI, 48 male rats were subjected to T9 vertebra laminectomy. Animals were divided into a SHAM-operated group and five treatment groups. The treatments included normal saline as a vehicle control group, minocycline 90 mg/kg and metformin at the doses of 10, 50 and 100 mg/kg. Locomotor scaling, behavioral tests for neuropathic pain and weight changes were evaluated and compared through a 28-days period. At the end of the study, tissue samples were taken to assess neuroinflammatory changes.
Results
Metformin 50 mg/kg improved the locomotors ability (p < 0.001) and decreased sensitivity to mechanical and thermal allodynia (p < 0.01). These results were compatible with minocycline effect on SCI (p > 0.05). While metformin led to weight loss, both metformin and minocycline significantly decreased neuroinflammation in the assessment of cord tissue histopathology, and levels of TNF-α and interleukin-1β (p < 0.001).
Conclusions
Metformin could be considered as an alternative therapeutic agent for SCI, as it potentially attenuates neuroinflammation, sensory and locomotor complications of cord injury.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Anwar MA, Al Shehabi TS, Eid AH. Inflammogenesis of secondary spinal cord injury. Front Cell Neurosci. 2016;10:98.
Faden AI, Wu J, Stoica BA, Loane DJ. Progressive inflammation‐mediated neurodegeneration after traumatic brain or spinal cord injury. Br J Pharmacol. 2016;173:681–91.
Nees TA, Finnerup NB, Blesch A, Weidner N. Neuropathic pain after spinal cord injury: the impact of sensorimotor activity. Pain. 2017;158:371–6.
Tateda S, Kanno H, Ozawa H, Sekiguchi A, Yahata K, Yamaya S, et al. Rapamycin suppresses microglial activation and reduces the development of neuropathic pain after spinal cord injury. J Orthop Res. 2017;35:93–103.
Marchand F, Tsantoulas C, Singh D, Grist J, Clark AK, Bradbury EJ, et al. Effects of Etanercept and Minocycline in a rat model of spinal cord injury. Eur J Pain. 2009;13:673–81.
Howell JJ, Hellberg K, Turner M, Talbott G, Kolar MJ, Ross DS, et al. Metformin inhibits hepatic mTORC1 signaling via dose-dependent mechanisms involving AMPK and the TSC complex. Cell Metab. 2017;25:463–71.
Zhang D, Xuan J, Zheng B-b, Zhou Y-l, Lin Y, Wu Y-s, et al. Metformin improves functional recovery after spinal cord injury via autophagy flux stimulation. Mol Neurobiol. 2017;54:3327–41.
Wang C, Liu C, Gao K, Zhao H, Zhou Z, Shen Z, et al. Metformin preconditioning provide neuroprotection through enhancement of autophagy and suppression of inflammation and apoptosis after spinal cord injury. Biochem Biophys Res Commun. 2016;477:534–40.
Pan Y, Sun X, Jiang L, Hu L, Kong H, Han Y, et al. Metformin reduces morphine tolerance by inhibiting microglial-mediated neuroinflammation. J Neuroinflamm. 2016;13:294.
Łabuzek K, Gabryel B, Okopień B. Metformin as a key to alternative activation of microglia? Post Hig Med Dosw (Online). 2014;68:247–57.
Oliveira WH, Nunes AK, Franca ME, Santos LA, Los DB, Rocha SW, et al. Effects of metformin on inflammation and short-term memory in streptozotocin-induced diabetic mice. Brain Res. 2016;1644:149–60.
Inyang K,Szabo-Pardi T,Price T, Treatment of Chronic pain: long term effects of Metformin on chronic neuropathic pain and microglial activation. J Pain. 2016;17:S53
Lee SM, Yune TY, Kim SJ, Park DW, Lee YK, Kim YC, et al. Minocycline reduces cell death and improves functional recovery after traumatic spinal cord injury in the rat. J Neurotrauma. 2003;20:1017–27.
Basso DM, Beattie MS, Bresnahan JC. A sensitive and reliable locomotor rating scale for open field testing in rats. J Neurotrauma. 1995;12:1–21.
Qiao F, Atkinson C, Kindy MS, Shunmugavel A, Morgan BP, Song H, et al. The alternative and terminal pathways of complement mediate post-traumatic spinal cord inflammation and injury. Am J Pathol. 2010;177:3061–70.
Gonzalez R, Glaser J, Liu MT, Lane TE, Keirstead HS. Reducing inflammation decreases secondary degeneration and functional deficit after spinal cord injury. Exp Neurol. 2003;184:456–63.
Kanno H, Ozawa H, Sekiguchi A, Yamaya S, Tateda S, Yahata K, et al. The role of mTOR signaling pathway in spinal cord injury. Cell Cycle. 2012;11:3175–9.
Lee-Kubli CA, Ingves M, Henry KW, Shiao R, Collyer E, Tuszynski MH, et al. Analysis of the behavioral, cellular and molecular characteristics of pain in severe rodent spinal cord injury. Exp Neurol. 2016;278:91–104.
Shinozaki M, Iwanami A, Fujiyoshi K, Tashiro S, Kitamura K, Shibata S, et al. Combined treatment with chondroitinase ABC and treadmill rehabilitation for chronic severe spinal cord injury in adult rats. Neurosci Res. 2016;113:37–47.
Rooney GE, Endo T, Ameenuddin S, Chen B, Vaishya S, Gross L, et al. Importance of the vasculature in cyst formation after spinal cord injury. J Neurosurg: Spine. 2009;11:432–7.
Yuan Y-M, He C. The glial scar in spinal cord injury and repair. Neurosci Bull. 2013;29:421–35.
Gwak YS, Hulsebosch CE, Leem JW. Neuronal-Glial interactions maintain chronic neuropathic pain after spinal cord injury. Neural Plast. 2017; 2017:2480689. https://www.hindawi.com/journals/np/2017/2480689/
Festoff BW, Ameenuddin S, Arnold PM, Wong A, Santacruz KS, Citron BA. Minocycline neuroprotects, reduces microgliosis, and inhibits caspase protease expression early after spinal cord injury. J Neurochem. 2006;97:1314–26.
Yune TY, Lee JY, Jung GY, Kim SJ, Jiang MH, Kim YC, et al. Minocycline alleviates death of oligodendrocytes by inhibiting pro-nerve growth factor production in microglia after spinal cord injury. J Neurosci. 2007;27:7751–61.
Bradesi S. Role of spinal cord glia in the central processing of peripheral pain perception. Neurogastroenterol & Motil. 2010;22:499–511.
Hyun B, Shin S, Lee A, Lee S, Song Y, Ha NJ, et al. Metformin Down-regulates TNF-alpha Secretion via Suppression of Scavenger Receptors in Macrophages. Immune Netw. 2013;13:123–32.
Song GJ, Suk K. Pharmacological modulation of functional phenotypes of microglia in neurodegenerative diseases. Front Aging Neurosci. 2017;9:139.
Gong K, Zou X, Fuchs PN, Lin Q. Minocycline inhibits neurogenic inflammation by blocking the effects of tumor necrosis factor‐α. Clin Exp Pharmacol Physiol. 2015;42:940–9.
Shultz RB, Zhong Y. Minocycline targets multiple secondary injury mechanisms in traumatic spinal cord injury. Neural Regen Res. 2017;12:702.
Gensel JC, Zhang B. Macrophage activation and its role in repair and pathology after spinal cord injury. Brain Res. 2015;1619:1–11.
Kuno R, Wang J, Kawanokuchi J, Takeuchi H, Mizuno T, Suzumura A. Autocrine activation of microglia by tumor necrosis factor-alpha. J Neuroimmunol. 2005;162:89–96.
Pugazhenthi S, Zhang Y, Bouchard R, Mahaffey G. Induction of an inflammatory loop by interleukin-1β and tumor necrosis factor-α involves NF-kB and STAT-1 in differentiated human neuroprogenitor cells. PLoS ONE. 2013;8:e69585.
Engelmann C, Weih F, Haenold R. Role of nuclear factor kappa B in central nervous system regeneration. Neural Regen Res. 2014;9:707.
Bracchi-Ricard V, Lambertsen KL, Ricard J, Nathanson L, Karmally S, Johnstone J, et al. Inhibition of astroglial NF-kappaB enhances oligodendrogenesis following spinal cord injury. J Neuroinflamm. 2013;10:869.
Schulze-Osthoff K, Ferrari D, Riehemann K, Wesselborg S. Regulation of NF-kappa B activation by MAP kinase cascades. Immunobiology. 1997;198:35–49.
Ahmad A, Biersack B, Li Y, Kong D, Bao B, Schobert R, et al. Targeted regulation of PI3K/Akt/mTOR/NF-κB signaling by indole compounds and their derivatives: mechanistic details and biological implications for cancer therapy. Anticancer Agents Med Chem. 2013;13:1002–13.
Song Z-p, Xiong B-r, Guan X-h, Cao F, Manyande A, Zhou Y-q, et al. Minocycline attenuates bone cancer pain in rats by inhibiting NF-κB in spinal astrocytes. Acta Pharmacol Sin. 2016;37:753–62.
Zhang H, Wang Y. Identification of molecular pathway changes after spinal cord injury by microarray analysis. J Orthop Surg. 2016;11:101.
Wu J, Stoica BA, Faden AI. Cell cycle activation and spinal cord injury. Neurotherapeutics. 2011;8:221–8.
Thibault-Halman G, Casha S, Singer S, Christie S. Acute management of nutritional demands after spinal cord injury. J Neurotrauma. 2011;28:1497–507.
Powell D, Affuso O, Chen Y. Weight change after spinal cord injury. J Spinal Cord Med. 2017;40:130–7.
Malin SK, Kashyap SR. Effects of metformin on weight loss: potential mechanisms. Curr Opin Endocrinol Diabetes Obes. 2014;21:323–9.
de Araújo AA, Pereira AdSBF, de Medeiros CACX, de Castro Brito GA, de Carvalho Leitão RF, de Souza Araújo L, et al. Effects of metformin on inflammation, oxidative stress, and bone loss in a rat model of periodontitis. PLoS ONE. 2017;12:e0183506.
Riddle M, Combining sulfonylureas and other oral agents. Am J Med. 2000;108:15s–22.
Acknowledgements
This study was financially supported by Experimental Medicine Research Center, Tehran University of Medical Sciences, Tehran, Iran (Grant No 95-01-30-31469) and by a grant (96002757) from the Iran National Science Foundation (INSF). We gratefully acknowledge the dedicated efforts of the investigators including Dr. Mohsen Afarideh and the coordinators who participated in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Afshari, K., Dehdashtian, A., Haddadi, NS. et al. Anti-inflammatory effects of Metformin improve the neuropathic pain and locomotor activity in spinal cord injured rats: introduction of an alternative therapy. Spinal Cord 56, 1032–1041 (2018). https://doi.org/10.1038/s41393-018-0168-x
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41393-018-0168-x
This article is cited by
-
Sex differences in the orofacial antinociceptive effect of metformin and the role of transient receptor potential channels
Naunyn-Schmiedeberg's Archives of Pharmacology (2025)
-
Metformin’s therapeutic potential in spinal cord injury: a systematic review and meta-analysis on locomotor recovery, neuropathic pain alleviation, and modulation of secondary injury mechanisms
Acta Neurochirurgica (2025)
-
Metformin and fibromyalgia pathophysiology: current insights and promising future therapeutic strategies
Molecular Biology Reports (2025)
-
Pharmacological mechanism and research progress of traditional Chinese medicine in the treatment of burns and scalds
Discover Medicine (2025)
-
Protective Effects of Glatiramer Acetate Against Paclitaxel-Induced Peripheral Neuropathy in Rats: A Role for Inflammatory Cytokines and Oxidative Stress
Neurochemical Research (2024)