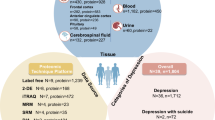
Abstract
The Pearson sample correlation between two biomarkers across a group of individuals can sometimes be much stronger than expected by chance. In the context of psychosis risk, we previously analyzed blood plasma protein data from initial presentations as collected in the North American Prodrome Longitudinal Study 2 (NAPLS2). We found enhanced correlation between proteins SERPINE1 and TIMP1, both promoters of coagulation and inhibitors of remodeling of extracellular matrix (ECM). Participants were unaffected community controls vs. others of clinical high risk. The SERPINE1-TIMP1 correlation was consistently higher in individuals at clinical high risk for psychosis who later converted to a psychotic disorder vs. participants who were nonconverters or unaffected community controls. Here, we extend those findings using data from a larger cohort, the North American Prodrome Longitudinal Study 3 (NAPLS3). Again, the correlation between SERPINE1 and TIMP1 remained higher in psychosis high-risk converters vs. the other groups. In NAPLS3 we added an assay for PLAT (anti-coagulation plasminogen activator strongly inhibited by SERPINE1). Comparing the three NAPLS3 groups we found a decreased correlation between SERPINE1 and PLAT in converters. In summary, the increased correlation of SERPINE1 and TIMP1 in converters is consistent with restricted brain circuit remodeling and increased tendency to coagulation. Rigorous application of permutation testing yielded NAPLS2 vs. NAPLS3 consistency of SERPINE1-TIMP1 correlation patterns with empirical p-value 0.03.
Similar content being viewed by others
Data availability
NAPLS2 and NAPLS3 data are in Supplement 12.
References
Salazar de Pablo G, Radua J, Pereira J, Bonoldi I, Arienti V, Besana F, et al. Probability of transition to psychosis in individuals at clinical high risk: an updated meta-analysis. JAMA Psychiatry. 2021;78:970–8. https://doi.org/10.1001/jamapsychiatry.2021.0830.
Jeffries CD, Perkins DO, Fournier M, Do KQ, Cuenod M, Khadimallah I, et al. Networks of blood proteins in the neuroimmunology of schizophrenia. Transl Psychiatry. 2018;8:112. https://doi.org/10.1038/s41398-018-0158-y.
Momen NC, Plana-Ripoll O, Agerbo E, Benros ME, Borglum AD, Christensen MK, et al. Association between mental disorders and subsequent medical conditions. N Engl J Med. 2020;382:1721–31. https://doi.org/10.1056/NEJMoa1915784.
Cannon TD, Chung Y, He G, Sun D, Jacobson A, van Erp TG, et al. Progressive reduction in cortical thickness as psychosis develops: a multisite longitudinal neuroimaging study of youth at elevated clinical risk. Biol Psychiatry. 2015;77:147–57. https://doi.org/10.1016/j.biopsych.2014.05.023.
Koutsouleris N, Kambeitz-Ilankovic L, Ruhrmann S, Rosen M, Ruef A, Dwyer DB, et al. Prediction models of functional outcomes for individuals in the clinical high-risk state for psychosis or with recent-onset depression: a multimodal, multisite machine learning analysis. JAMA Psychiatry. 2018;75:1156–72. https://doi.org/10.1001/jamapsychiatry.2018.2165.
Lijnen HR. Pleiotropic functions of plasminogen activator inhibitor-1. J Thromb Haemost. 2005;3:35–45. https://doi.org/10.1111/j.1538-7836.2004.00827.x.
Rahman FA, Krause MP. PAI-1, the plasminogen system, and skeletal muscle. Int J Mol Sci. 2020;21:7066. https://doi.org/10.3390/ijms21197066.
Olfson M, Gerhard T, Huang C, Crystal S, Stroup TS. Premature mortality among adults with schizophrenia in the United States. JAMA Psychiatry. 2015;72:1172–81. https://doi.org/10.1001/jamapsychiatry.2015.1737.
Zhu Y, Webster MJ, Mendez Victoriano G, Middleton FA, Massa PT, Weickert CS. Molecular evidence for altered angiogenesis in neuroinflammation-associated schizophrenia and bipolar disorder implicate an abnormal midbrain blood-brain barrier. Schizophrenia bulletin. 2025;51:1146–61. https://doi.org/10.1093/schbul/sbae184.
Addington J, Liu L, Brummitt K, Bearden CE, Cadenhead KS, Cornblatt BA, et al. North American prodrome longitudinal study (NAPLS 3): methods and baseline description. Schizophr Res. 2022;243:262–7. https://doi.org/10.1016/j.schres.2020.04.010.
Addington J, Liu L, Buchy L, Cadenhead KS, Cannon TD, Cornblatt BA, et al. North American prodrome longitudinal study (NAPLS 2): the prodromal symptoms. J Nerv Ment Dis. 2015;203:328–35. https://doi.org/10.1097/nmd.0000000000000290.
Miller TJ, McGlashan TH, Rosen JL, Cadenhead K, Cannon T, Ventura J, et al. Prodromal assessment with the structured interview for prodromal syndromes and the scale of prodromal symptoms: predictive validity, interrater reliability, and training to reliability. Schizophrenia bulletin. 2003;29:703–15. https://doi.org/10.1093/oxfordjournals.schbul.a007040.
First, MB, Spitzer RL, Givvon M, Williams JBW Structured Clinical Interview for DSM-IV TR Axis I Disorders, Non-patient Edition (SCID-I/NP). (Biometrics Research, New York State Psychiatric Institute, 2002).
Juncal-Ruiz M, Riesco-Davila L, de la Foz VO, Ramirez-Bonilla M, Martinez-Garcia O, Irure-Ventura J, et al. The effect of excess weight on circulating inflammatory cytokines in drug-naive first-episode psychosis individuals. J Neuroinflammation. 2018;15:63. https://doi.org/10.1186/s12974-018-1096-6.
Mukaka MM. Statistics corner: a guide to appropriate use of correlation coefficient in medical research. Malawi Med J. 2012;24:69–71.
Szklarczyk D, Gable AL, Lyon D, Junge A, Wyder S, Huerta-Cepas J, et al. STRING v11: protein-protein association networks with increased coverage, supporting functional discovery in genome-wide experimental datasets. Nucleic Acids Res. 2019;47:D607–13. https://doi.org/10.1093/nar/gky1131.
Domenici E, Wille DR, Tozzi F, Prokopenko I, Miller S, McKeown A, et al. Plasma protein biomarkers for depression and schizophrenia by multi analyte profiling of case-control collections. PLoS One. 2010;5:e9166. https://doi.org/10.1371/journal.pone.0009166.
Arpino V, Brock M, Gill SE. The role of TIMPs in regulation of extracellular matrix proteolysis. Matrix Biol. 2015;44-46:247–54. https://doi.org/10.1016/j.matbio.2015.03.005.
Stamenkovic I. Extracellular matrix remodelling: the role of matrix metalloproteinases. J Pathol. 2003;200:448–64. https://doi.org/10.1002/path.1400.
Belaaouaj AA, Li A, Wun TC, Welgus HG, Shapiro SD. Matrix metalloproteinases cleave tissue factor pathway inhibitor. Effects on coagulation. J Biol Chem. 2000;275:27123–8. https://doi.org/10.1074/jbc.M004218200.
Mehra A, Ali C, Parcq J, Vivien D, Docagne F. The plasminogen activation system in neuroinflammation. Biochim Biophys Acta. 2016;1862:395–402. https://doi.org/10.1016/j.bbadis.2015.10.011.
Zhou X, Hu H, Huynh ML, Kotaru C, Balzar S, Trudeau JB, et al. Mechanisms of tissue inhibitor of metalloproteinase 1 augmentation by IL-13 on TGF-beta 1-stimulated primary human fibroblasts. J Allergy Clin Immunol. 2007;119:1388–97. https://doi.org/10.1016/j.jaci.2007.02.011.
Dorrier CE, Jones HE, Pintaric L, Siegenthaler JA, Daneman R. Emerging roles for CNS fibroblasts in health, injury and disease. Nat Rev Neurosci. 2022;23:23–34. https://doi.org/10.1038/s41583-021-00525-w.
Wang T, Lu H, Li D, Huang W. TGF-beta1-Mediated Activation of SERPINE1 is Involved in Hemin-Induced Apoptotic and Inflammatory Injury in HT22 Cells. Neuropsychiatr Dis Treat. 2021;17:423–33. https://doi.org/10.2147/NDT.S293772.
Nardou R, Sawyer E, Song YJ, Wilkinson M, Padovan-Hernandez Y, de Deus JL, et al. Psychedelics reopen the social reward learning critical period. Nature. 2023;618:790–8. https://doi.org/10.1038/s41586-023-06204-3.
Tuck JR, Dunlap LE, Khatib YA, Hatzipantelis CJ, Weiser Novak S, Rahn RM, et al. Molecular design of a therapeutic LSD analogue with reduced hallucinogenic potential. Proc Natl Acad Sci USA 2025;122:e2416106122. https://doi.org/10.1073/pnas.2416106122.
Gumpper RH, Jain MK, Kim K, Sun R, Sun N, Xu Z, et al. The structural diversity of psychedelic drug actions revealed. Nat Commun. 2025;16:2734. https://doi.org/10.1038/s41467-025-57956-7.
Jankowska U, Skupien-Rabian B, Swiderska B, Prus G, Dziedzicka-Wasylewska M, Kedracka-Krok S. Proteome analysis of PC12 cells reveals alterations in translation regulation and actin signaling induced by clozapine. Neurochem Res. 2021;46:2097–2111. https://doi.org/10.1007/s11064-021-03348-4.
Greene LA, Tischler AS. Establishment of a noradrenergic clonal line of rat adrenal pheochromocytoma cells which respond to nerve growth factor. Proc Natl Acad Sci USA 1976;73:2424–8. https://doi.org/10.1073/pnas.73.7.2424.
Pantazopoulos H, Woo TU, Lim MP, Lange N, Berretta S. Extracellular matrix-glial abnormalities in the amygdala and entorhinal cortex of subjects diagnosed with schizophrenia. Arch Gen Psychiatry. 2010;67:155–66. https://doi.org/10.1001/archgenpsychiatry.2009.196.
Berretta S. Extracellular matrix abnormalities in schizophrenia. Neuropharmacology. 2012;62:1584–97. https://doi.org/10.1016/j.neuropharm.2011.08.010.
Pantazopoulos H, Markota M, Jaquet F, Ghosh D, Wallin A, Santos A, et al. Aggrecan and chondroitin-6-sulfate abnormalities in schizophrenia and bipolar disorder: a postmortem study on the amygdala. Transl Psychiatry. 2015;5:e496. https://doi.org/10.1038/tp.2014.128.
Wen TH, Binder DK, Ethell IM, Razak KA. The perineuronal ‘safety’ net? perineuronal net abnormalities in neurological disorders. Front Mol Neurosci. 2018;11:270. https://doi.org/10.3389/fnmol.2018.00270.
Alcaide J, Guirado R, Crespo C, Blasco-Ibanez JM, Varea E, Sanjuan J, et al. Alterations of perineuronal nets in the dorsolateral prefrontal cortex of neuropsychiatric patients. Int J Bipolar Disord. 2019;7:24. https://doi.org/10.1186/s40345-019-0161-0.
Pantazopoulos H, Hossain NM, Chelini G, Durning P, Barbas H, Zikopoulos B, et al. Chondroitin sulphate proteoglycan axonal coats in the human mediodorsal thalamic nucleus. Front Integr Neurosci. 2022;16:934764. https://doi.org/10.3389/fnint.2022.934764.
Hensch TK. Critical period plasticity in local cortical circuits. Nat Rev Neurosci. 2005;6:877–88. https://doi.org/10.1038/nrn1787.
Mataga N, Mizuguchi Y, Hensch TK. Experience-dependent pruning of dendritic spines in visual cortex by tissue plasminogen activator. Neuron. 2004;44:1031–41. https://doi.org/10.1016/j.neuron.2004.11.028.
Pinter P, Alpar A. The role of extracellular matrix in human neurodegenerative diseases. Int J Mol Sci. 2022;23:11085 https://doi.org/10.3390/ijms231911085.
Carulli D, de Winter F, Verhaagen J. Semaphorins in adult nervous system plasticity and disease. Front Synaptic Neurosci. 2021;13:672891. https://doi.org/10.3389/fnsyn.2021.672891.
Pizzorusso T, Medini P, Berardi N, Chierzi S, Fawcett JW, Maffei L. Reactivation of ocular dominance plasticity in the adult visual cortex. Science. 2002;298:1248–51. https://doi.org/10.1126/science.1072699.
Fagiolini M, Hensch TK. Inhibitory threshold for critical-period activation in primary visual cortex. Nature. 2000;404:183–6. https://doi.org/10.1038/35004582.
Hensch TK, Fagiolini M, Mataga N, Stryker MP, Baekkeskov S, Kash SF. Local GABA circuit control of experience-dependent plasticity in developing visual cortex. Science. 1998;282:1504–8. https://doi.org/10.1126/science.282.5393.1504.
Ye Q, Miao QL. Experience-dependent development of perineuronal nets and chondroitin sulfate proteoglycan receptors in mouse visual cortex. Matrix Biol. 2013;32:352–63. https://doi.org/10.1016/j.matbio.2013.04.001.
Lipachev N, Melnikova A, Fedosimova S, Arnst N, Kochneva A, Shaikhutdinov N, et al. Postnatal development of the microstructure of cortical GABAergic synapses and perineuronal nets requires sensory input. Neurosci Res. 2022;182:32–40. https://doi.org/10.1016/j.neures.2022.06.005.
Zheutlin AB, Jeffries CD, Perkins DO, Chung Y, Chekroud AM, Addington J, et al. The role of microRNA expression in cortical development during conversion to psychosis. Neuropsychopharmacology. 2017;42:2188–95. https://doi.org/10.1038/npp.2017.34.
Vita A, De Peri L, Deste G, Sacchetti E. Progressive loss of cortical gray matter in schizophrenia: a meta-analysis and meta-regression of longitudinal MRI studies. Transl Psychiatry. 2012;2:e190. https://doi.org/10.1038/tp.2012.116.
Fawcett JW, Fyhn M, Jendelova P, Kwok JCF, Ruzicka J, Sorg BA. The extracellular matrix and perineuronal nets in memory. Molecular psychiatry. 2022. https://doi.org/10.1038/s41380-022-01634-3.
Nahar L, Delacroix BM, Nam HW. The role of parvalbumin interneurons in neurotransmitter balance and neurological disease. Front Psychiatry. 2021;12:679960. https://doi.org/10.3389/fpsyt.2021.679960.
Roach BJ, Mathalon DH. Event-related EEG time-frequency analysis: an overview of measures and an analysis of early gamma band phase locking in schizophrenia. Schizophrenia bulletin. 2008;34:907–26. https://doi.org/10.1093/schbul/sbn093.
Lensjo KK, Lepperod ME, Dick G, Hafting T, Fyhn M. Removal of perineuronal nets unlocks juvenile plasticity through network mechanisms of decreased inhibition and increased gamma activity. J Neurosci. 2017;37:1269–83. https://doi.org/10.1523/JNEUROSCI.2504-16.2016.
Steullet P, Cabungcal JH, Coyle J, Didriksen M, Gill K, Grace AA, et al. Oxidative stress-driven parvalbumin interneuron impairment as a common mechanism in models of schizophrenia. Molecular psychiatry. 2017;22:936–43. https://doi.org/10.1038/mp.2017.47.
van ‘t Spijker HM, Kwok JCF. A sweet talk: the molecular systems of perineuronal nets in controlling neuronal communication. Front Integr Neurosci. 2017;11:33. https://doi.org/10.3389/fnint.2017.00033.
Bruckner G, Kacza J, Grosche J. Perineuronal nets characterized by vital labelling, confocal and electron microscopy in organotypic slice cultures of rat parietal cortex and hippocampus. J Mol Histol. 2004;35:115–22. https://doi.org/10.1023/b:hijo.0000023374.22298.50.
Pantazopoulos H, Lange N, Hassinger L, Berretta S. Subpopulations of neurons expressing parvalbumin in the human amygdala. J Comp Neurol. 2006;496:706–22. https://doi.org/10.1002/cne.20961.
Lewis DA, Curley AA, Glausier JR, Volk DW. Cortical parvalbumin interneurons and cognitive dysfunction in schizophrenia. Trends Neurosci. 2012;35:57–67. https://doi.org/10.1016/j.tins.2011.10.004.
Hashimoto T, Volk DW, Eggan SM, Mirnics K, Pierri JN, Sun Z, et al. Gene expression deficits in a subclass of GABA neurons in the prefrontal cortex of subjects with schizophrenia. J Neurosci. 2003;23:6315–26.
Nakazawa K, Zsiros V, Jiang Z, Nakao K, Kolata S, Zhang S, et al. GABAergic interneuron origin of schizophrenia pathophysiology. Neuropharmacology. 2012;62:1574–83. https://doi.org/10.1016/j.neuropharm.2011.01.022.
Cowan RL, Wilson CJ, Emson PC, Heizmann CW. Parvalbumin-containing GABAergic interneurons in the rat neostriatum. J Comp Neurol. 1990;302:197–205. https://doi.org/10.1002/cne.903020202.
Ford JM, Krystal JH, Mathalon DH. Neural synchrony in schizophrenia: from networks to new treatments. Schizophrenia bulletin. 2007;33:848–52. https://doi.org/10.1093/schbul/sbm062.
Williams S, Boksa P. Gamma oscillations and schizophrenia. J Psychiatry Neurosci. 2010;35:75–7. https://doi.org/10.1503/jpn.100021.
Bar-Klein G, Cacheaux LP, Kamintsky L, Prager O, Weissberg I, Schoknecht K, et al. Losartan prevents acquired epilepsy via TGF-beta signaling suppression. Ann Neurol. 2014;75:864–75. https://doi.org/10.1002/ana.24147.
Carpenter WT Jr., Kirkpatrick B. The heterogeneity of the long-term course of schizophrenia. Schizophrenia bulletin. 1988;14:645–52. https://doi.org/10.1093/schbul/14.4.645.
Byrne JF, Healy C, Focking M, Heurich M, Susai SR, Mongan D, et al. Plasma complement and coagulation proteins as prognostic factors of negative symptoms: an analysis of the NAPLS 2 and 3 studies. Brain Behav Immun. 2024;119:188–196. https://doi.org/10.1016/j.bbi.2024.03.049.
Lisman JE, Coyle JT, Green RW, Javitt DC, Benes FM, Heckers S, et al. Circuit-based framework for understanding neurotransmitter and risk gene interactions in schizophrenia. Trends Neurosci. 2008;31:234–42. https://doi.org/10.1016/j.tins.2008.02.005.
Shilts J, Severin Y, Galaway F, Muller-Sienerth N, Chong ZS, Pritchard S, et al. A physical wiring diagram for the human immune system. Nature. 2022;608:397–404. https://doi.org/10.1038/s41586-022-05028-x.
Fond G, d’Albis MA, Jamain S, Tamouza R, Arango C, Fleischhacker WW, et al. The promise of biological markers for treatment response in first-episode psychosis: a systematic review. Schizophrenia bulletin. 2015;41:559–73. https://doi.org/10.1093/schbul/sbv002.
Acknowledgements
This work was supported by National Institutes of Health (NIH) grants U01 MH081902 to Dr. Cannon, P50 MH066286 to Dr. Bearden, U01 MH82022 to Dr. Woods, U01 MH066134 to Dr. Addington, U01 MH081944 to Dr. Cadenhead, U01 MH066069 to Dr. Perkins, R01 MH076989 to Dr. Mathalon, U01 MH081928 to Dr. Stone, and U01 MH081988 to Dr. Walker. Many referee comments greatly improved the focus and precision of the manuscript.
Author information
Authors and Affiliations
Contributions
CJ, DP, and JF designed algorithms and statistical checks and helped write the manuscript; CAB discussed the project a various stages; JA, CEB, KC, TC, BC, MK, DM, LS, WS, EW, SW, and DP had executive roles in clinic management and in writing the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declair no competing interest.
Ethics approval and consent to participate
Approval for the NAPLS2 and NAPLS3 projects was obtained by each site by their respective named ethics committees listed below. All methods were performed in accordance with the relevant guidelines and regulations, including obtaining informed consent from all study participants. For IRB details at each site, please see the table in the Supplement 11.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Protein labels are Official Gene Symbols (https://www.ncbi.nlm.nih.gov/gene/) in plaintext while genes themselves are in italics. For example, the gene SERPINE1 encodes the protein serpin family E member 1, that is, SERPINE1. Other notable proteins herein are plasminogen activator, tissue type (PLAT); plasminogen activator, urokinase (PLAU); and TIMP metallopeptidase inhibitor 1 (TIMP1). A complete list of symbols and acronyms is in Supplement.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Jeffries, C.D., Bizon, C.A., Ford, J.R. et al. Correlation networks of blood proteins in the neuroimmunology of schizophrenia—replication and extension. Transl Psychiatry (2026). https://doi.org/10.1038/s41398-026-03934-6
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41398-026-03934-6