Abstract
While previous research has focused on individual risk factors, few studies have utilized an intersectionality-informed framework to examine how multiple social factors collectively impact depression risk, particularly in the context of childhood adversities. This study investigates the association between adverse childhood experiences (ACEs) and depression while considering the intersecting roles of sex, socioeconomic status (SES), and ethnicity in identifying high-risk population subgroups. Data were drawn from the Canadian Longitudinal Study on Aging (CLSA), a nationally representative prospective cohort comprising over 50,000 adults aged 45 and older. We included 20,559 participants from the Comprehensive cohort who completed both baseline and first follow-up assessments. Depression was measured using a validated scale (CES-D-10). Key variables included ACE exposure, sex, SES, ethnicity, and other sociodemographic covariates. Latent class analysis was conducted to explore latent ACEs groups. Multilevel analysis of individual heterogeneity and discriminatory accuracy (MAIHDA) was employed to investigate whether ACE patterns and intersectional social groups predicted differential risks of depression. Three distinct patterns of ACEs were identified. The high ACE group was associated with an elevated risk of depression, especially among females, individuals with low SES, and non-White groups. This risk was compounded among those with multiple marginalized identities, such as females with low SES and exposure to high ACE, highlighting the cumulative nature of depression vulnerability. In contrast, male sex and high SES were protective, particularly in the absence of ACE exposure. Integrating ACEs with an intersectional framework reveals the complex etiology of depression and underscores the need for targeted, equity-oriented prevention strategies considering cumulative disadvantage.
Similar content being viewed by others
Introduction
Depression represents a significant public health concern, affecting around 322 million people and being responsible for 7.5% of all years lived with disability globally [1]. As the global older population continues to rise, late-life depression poses an escalating challenge [2]. The global senior population is projected to more than double over the next 30 years, reaching approximately 1.5 billion people worldwide by 2050 [3]. Among those older than 55, nearly 14% struggle with depression, with 2% grappling with its severe form (i.e., major depression) [4]. In older adults, depression manifests with typical core symptoms, yet it often leads to a more burdensome disease course [5, 6], diminished life satisfaction [7], heightened healthcare utilization, and compromised functional abilities [8, 9].
Adverse childhood experiences (ACEs) are well-established risk factors for depression [10,11,12,13,14]. Existing literature underscores the multifaceted nature of ACEs, with distinct impacts stemming from various forms of childhood adversity [15, 16]. Emotional abuse, for instance, is link to both internalizing and externalizing behavioral problems, while physical abuse specifically correlates with externalizing problems [16]. Furthermore, ACEs frequently co-occur across different contexts and developmental stages, creating a phenomenon known as polyvictimization [17]. Polyvictimization studies have revealed the intricate interrelationships among diverse types of victimization, uncovering shared risks and synergistic effects on health outcomes [18]. To date, studies indicate several crucial trends: 1) distinct patterns of ACEs exhibit varying relationships with mental disorders [19, 20]; 2) polyvictimized individuals face a higher risk of severe victimizations and show disproportionate signs of psychological distress [21]; 3) the consequences of polyvictimization tend to be enduring; and 4) while systematic assessment of ACEs is recommended in psychiatric specialties and considered good clinical practice, with several validated tools available to capture multiple exposure types [22], translating this into routine care remains challenging. Barriers such as time constraints, variations in clinician training, and the complexity of integrating multifactorial adversity histories into treatment planning may limit consistent implementation, particularly in non-specialist settings where many older adults seek help [23]. Moreover, evidence on the most effective ways to assess and address specific patterns of ACEs, such as polyvictimization, in late-life populations, and how they interact with other social determinants, is lacking [24]. Studies have suggested that the combined impact of ACEs and other psychosocial stressors reinforces the negative sequelae of ACEs in the general population [25]. Likewise, in research contexts, ACEs are frequently treated as a cumulative score, which may obscure the unique or interactive effects of specific adversity patterns [26]. Prior research has shown that the psychological and biological effects of ACEs can persist for decades, influencing stress response systems, emotional regulation, and vulnerability to psychiatric disorders well into older adulthood. Despite consistent evidence showing the associations between various ACEs and depression as well as the established dose-response relationships linking cumulative ACEs to depression risk [27], research specifically examining how different ACE patterns, including polyvictimization, relate to late-life depression, and how these relationships are shaped by intersecting social positions, remains limited.
Several studies have shown that key social determinants, such as ethnicity, sex, and socioeconomic status (SES), are associated with both depression as well as ACEs [28,29,30,31]. Importantly, interactions of these characteristics increase the likelihood of depression (e.g., females with low SES) [32, 33]. Sex differences in depression rates, symptoms, risk factors, and progression are well-documented [34, 35]. Females report higher rates of depression than males [36, 37]. Furthermore, sex differences also contribute to varying depression rates via SES [38]. To enhance mental health care and achieve sex equity, it is crucial to integrate sex-based analyses into depression exploration [39]. The World Health Organization (WHO) defines social determinants of health as the conditions in which people are born, grow, live, work, and age, as well as the systems in place to address illnesses [40]. The WHO’s definition emphasizes the cumulative impact of social, economic, environmental, and interpersonal factors on health. However, research exploring the relationships between health inequality and depression often focuses on a single factor, e.g., comparing low vs. high socioeconomic status. This is unfortunate since health inequality often stems from complex interactions among social inequality, power dynamics, and contextual factors within social hierarchies. These complex intersections naturally characterize one’s experiences in the real world [41]. To understand how these social factors influence the risk of depression, it is vital to assess various forms of inequality simultaneously.
To gain a deeper understanding of depression within diverse social contexts, adopting an intersectionality framework is highly recommended [42]. It was created to capture how multiple and overlapping forms of social stratification collectively shape individuals’ lived experiences. What sets this framework apart is its ability to transcend the simplistic analysis of socioeconomic and demographic factors. Instead, it delves into the intricate interplay of multiple social, economic, and demographic dimensions that define specific social strata. This approach offers transformative potential for advancing the prevention and treatment of late-life depression, which remains an understudied issue in Canada [43]. In clinical practice, however, many clinicians may struggle to effectively integrate multiple risk factors, such as childhood adversity, sex, and socioeconomic status, into their decision-making processes. By adopting an intersectional lens, this study expands conventional sociodemographic classifications to comprehensively examine how combinations of childhood adversity, sex, socioeconomic status, and ethnicity interact to shape the risk of late-life depression. Unlike traditional cumulative scoring methods, multilevel analysis of individual heterogeneity and discriminatory accuracy (MAIHDA) captures multidimensional vulnerability patterns by considering both individual heterogeneity and the discriminatory accuracy of intersecting social positions, aiming to identify the most vulnerable subgroups and the distinct pathways through which cumulative disadvantage influences mental health outcomes.
Overall, the current study aims to examine the interactions between distinct profiles of ACEs and the intersection of various social, economic, and demographic factors in relation to depression. This study was primarily exploratory in nature, as no preregistration or predefined hypotheses were established prior to the analysis of the data. Nevertheless, based on prior literature and theoretical frameworks of cumulative disadvantage, it is reasonable to postulate that individuals from certain disadvantaged social strata are more likely to report experiencing depression, particularly if they have been exposed to ACEs [44, 45]. To empirically test this hypothesis, we operationalized social disadvantage using multidimensional indicators (sex, ethnicity, and socioeconomic status) and examined their interactions with ACE profiles in the current study.
Methods
Data resources and study cohort
The data used were from the Canadian Longitudinal Study on Aging (CLSA), a large, national, longitudinal study of more than 50,000 Canadians who are being followed for at least 20 years [46]. Recruitment involved random selection from within 25–50 km of the 11 data collection sites in 7 Canadian provinces. The CLSA consists of a comprehensive cohort and a tracking cohort. The CLSA includes 30,097 participants who completed standardized in-home interviews and underwent comprehensive physical and clinical assessments at designated data collection sites. Participants were randomly selected from seven Canadian provinces, with baseline data collected between 2011 and 2015. Follow-up assessments were conducted every three years. The present study cohort includes 1) adults aged 45 years or older, 2) those who completed two data collections at baseline (2015) and the 3-year follow-up (Follow-up 1, 2018), and 3) those who had complete data on ACEs, depressive symptoms, and core sociodemographic covariates (sex, ethnicity, and SES indicators). Finally, 20,559 eligible participants were included in the current study.
Ethical review of the CLSA protocol was conducted by the research ethics board at each research site, with coordination from the McMaster Research Ethics Board. This study received Ethics Approval from the Institutional Research Ethics Board at the Douglas Research Centre and conforms to the provisions of the Declaration of Helsinki. All CLSA participants provided written consent before participating in the study.
Measures
Depression
Depressive symptoms were measured using the Center for Epidemiologic Studies Short Depression Scale (CES-D10) [47]. It includes three items on depressed affect, five items on somatic symptoms, and two items on positive affect. Depression was defined using two complementary approaches: a) clinical depression was identified based on self-reported physician diagnosis and receipt of depression treatment [47]; or b) the Depression Scale (CES-D-10), with a cut-off score of 10 used to distinguish individuals with elevated symptom levels. While the clinical diagnosis captures formal recognition and treatment of depression, the CES-D-10 offers a standardized measure of current symptom severity, allowing the detection of subclinical or undiagnosed cases [48]. Physician-diagnosed clinical depression was based on the response to the questions “Has a doctor ever told you that you suffer from clinical depression?” and “At what age, or in what year, were you first told you were clinically depressed?”.
Adverse childhood experiences (ACEs)
ACEs covered a wide range of adverse events that occurred prior to age 18, such as childhood maltreatment, including physical, sexual, and emotional abuse, neglect, and witnessing intimate partner violence in the household, and other adverse events, including parental death or serious illness, parental divorce or separation, and mental or psychiatric illness of a family member. ACEs were measured using items derived from the Childhood Experiences of Violence Questionnaire [49, 50], and the National Longitudinal Study of Adolescent to Adult Health Wave III questionnaire [51]. These 14 items were used as indicators to identify latent clusters of polyvictimization. The CLSA participants were asked whether they had experienced 1) the death or serious illness of a parent or primary caretaker; 2) the divorce or separation of parents; or 3) lived with a family member with mental or psychiatric illness, prior to the age of 18 years. Frequency and severity of events related to physical abuse, emotional abuse, sexual abuse, neglect, and exposure to intimate partner violence, prior to the age of 16 years, were assessed on an ordinal scale with five response options (“never”, “1–2 times”, “3–5 times”, “6–10 times”, “more than 10 times”). The internal consistency of the adapted ACE measure was acceptable (Cronbach’s α = 0.710). A confirmatory factor analysis further supported its construct validity, showing acceptable model fit (CFI = 0.951, RMSEA = 0.063).
Intersectionality of social groups
Self-reported measures included sex assigned at birth, educational level (less than secondary, secondary school, some post-secondary graduation, post-secondary graduation), household income (less than $40,000, $40,000–$79,999, $80,000–$99,999, $100,000–$149,999, $150,000 and more), current employment status (yes, no), and race/ethnicity (White, non-White). These variables were used to construct intersectional groups defined by every possible combination. SES was conceptualized as a multidimensional construct encompassing education, income, and employment status, consistent with established frameworks in social epidemiology [52]. Specifically, a composite SES index was first derived using standardized indicators to capture cumulative socioeconomic advantage. To enhance interpretability and enable stratified analyses of gradient effects, the continuous SES distribution was partitioned into three levels (low, middle, and high) using sample-based quantile thresholds.
Statistical analysis
To unfold the relationship between ACE patterns and depression, latent class analysis (LCA) was first used to uncover latent patterns of ACEs. LCA has been commonly used to identify distinct classes that have homogeneity within each class but clear differences between classes [53]. The number of classes in the LCA model was incrementally increased until the model was no longer well identified. Model fit was evaluated using multiple criteria, including the Akaike Information Criterion (AIC), Bayesian Information Criterion (BIC), adjusted BIC, Lo-Mendell-Rubin likelihood ratio test, absence of boundary parameter estimates, local independence, parsimony, and interpretability [53]. Missing data were handled in the LCA models using a Full Information Maximum Likelihood (FIML) function, under the missing at random (MAR) assumption [54], using Mplus version 8.1 [55]. To examine potential interactions between latent ACE patterns and intersectionality in relation to depression, MAIHDA was conducted using the R package ‘ggeffects’. MAIHDA was chosen to detect both within- and between-group variations in the associations between ACEs and depression across various intersectional strata. It provides distinct methodological and theoretical advantages over traditional intersectionality approaches and has increasingly been regarded as the emerging gold standard for the investigation of health disparities [56]. A two-level random-intercept regression model was employed to examine depression outcomes, with individuals (Level 1) nested within intersectional strata (Level 2) defined by selected social determinants. Consistent with previous MAIHDA analyses, Bayesian Markov Chain Monte Carlo (MCMC) estimation with diffuse (non-informative) priors was used, facilitated by the ‘MCMCglmm’ packagein R (version 4.2.2). A comprehensive assessment of missing data patterns was conducted. For variables identified as missing at random, multiple imputation using chained equations was performed to address missingness. All statistical analyses incorporated sampling weights provided by the CLSA to account for the complex survey design and to improve the generalizability of findings to the national population.
Results
The study included a total of 20,559 participants in the analysis (10,721 males and 9838 females). Of them, 15,662 were classified into the ‘low-adversity’ class, 3807 into the ‘moderate-adversity’ class, and 1090 into the ‘high-adversity’ class. Most participants were aged between 55 and 74 years (65.1%), White (94.8%), and were currently employed (70.0%). The majority were married or in a common-law relationship (70.2%) and had less than a secondary school education (45.0%). In the present study, 1801 participants (8.8%) were classified into the low SES group, 14,645 (71.2%) into the middle SES group, and 4113 (20.0%) into the high SES group. Overall, participants in the ‘high-adversity’ class were generally younger, less educated, and more likely to belong to the low-SES group, compared with those in the low- and moderate-adversity classes (see Table S1).
Three distinct subgroups of ACE were identified, as shown in Fig. 1. The three-class solution was chosen based on statistical fit indices and interpretability, with the highest entropy value (0.88) and adequate subgroup size.; The smallest class comprised 5.6% (N = 1151) of the study sample. The optimal model also displayed favorable fit indices. Details can be found in Table 1. The largest group, labeled the “Low-Adversity” class (75.5%, N = 15,522), was characterized by uniformly low probabilities across nearly all ACE indicators (except exposures to getting spanked), with slightly elevated experience of having parental mental illness and parental separation/divorce. The “Moderate-Adversity” class (5.6%) was characterized by moderate probabilities of exposure to family-related stressors, including parental mental illness and verbal abuse, particularly experiences of being yelled at or witnessing verbal conflict, while the likelihood of physical and sexual abuse remained low. The “High-adversity” class (18.9%, N = 3886) demonstrated consistently high probabilities across nearly all ACE items, reflecting a highly vulnerable subgroup with extensive, multidimensional traumatic exposures.
This figure displays the item-response probability profiles for three distinct latent classes of adverse childhood experiences identified within the study cohort.
The identified ACEs groups were then integrated with the MAIHDA model to explore how these distinct profiles were associated with depression outcomes. Table 2 presents the MAIHDA models of the relationships among ACEs, sociodemographic factors, and the risk of depression. The final model demonstrated an improved fit compared to the null model, as evidenced by lower AIC and BIC values. The decrease in the Variance Partition Coefficient (VPC) from 14.2% in the null model to 10.3% in the final model suggests that the included covariates accounted for approximately 27% of the initial between-strata variance. In the final MAIHDA model, the high ACE group was more likely to have depression (OR = 1.98, 95%CI:1.79–2.20) compared to the low ACE group. Similarly, females had 45% greater odds of having depression than males (OR = 1.45, 95%CI:1.32–1.59). SES demonstrated the most pronounced gradient, with low-SES individuals exhibiting 4.74-fold higher odds (95%CI:3.95- 5.69) compared to high-SES counterparts. No statistical significance was found between non-White and White individuals (OR = 1.19, 95%CI:0.98–1.45). Variance partitioning revealed that SES accounted for the largest proportion of explainable between-strata variance, as indicated by the proportional change in variance (PCV = 87.3%), which reflects the reduction in variance attributable to the inclusion of covariates. It was substantially greater than the contributions of sex (17.5%) and ethnicity (0.5%).
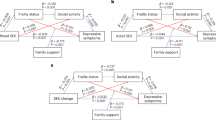
Figure 2 illustrates the predicted incidence of developing depression across 36 intersectional social strata, derived from combinations of ACE, sex, ethnicity, and SES. Overall, a general trend was observed in which greater accumulation of social disadvantage was associated with a higher likelihood of depression, although this pattern was not strictly monotonic across all combinations. Individuals with the lower predicted incidence of depression were characterized by low levels of ACE exposure, being male, and having high SES. In particular, the group at the lowest predicted risk for depression consisted of White males with high SES and low exposure to ACEs, who had a predicted probability of 3.1% (95%CI: 2.4–3.9%), while non-White males with similar profiles showed a probability of 3.9% (95%CI: 1.8–8.4%). In contrast, the highest predicted probabilities of depression were observed in distinct groups. These high-risk groups, most of whom were females, consistently exhibit risk-enhancing profiles marked by high ACE exposure and low SES. Specifically, these high-risk populations included White females with high ACE exposure and low SES (32.6%; 95 CI: 26.9–38.9%), non-White females with high ACE exposure and low SES (31.8%; 95 CI: 16.1–53.1%), and White males with similarly high ACE exposure and low SES (32.8%; 95 CI: 26.5–39.7%). Details can be found in Table S2. These groups represent individuals with multiple intersecting vulnerabilities, including early life adversity, economic disadvantage, and female sex. As such, they were identified as the most susceptible populations in terms of predicted depression risk, and the intersection of these factors significantly elevated their vulnerability to depression. Importantly, the elevated depression risk observed across these groups also indicates that ACEs and SES may play a more substantial role in shaping depression outcomes than sex or ethnicity alone. Additionally, the analyses of sex-stratified ACE patterns revealed distinct disparities across socioeconomic and ethnic groups (Fig. 3). Females exhibited higher predicted probabilities of depression compared to males within equivalent social strata. For instance, the predicted probability of depression for White females with low SES and low ACE exposure was 0.19 (95% CI: 0.17–0.22), compared to 0.15 (95% CI: 0.12–0.18) for males in the same group. Similarly, non-White females with medium SES and medium ACE exposure had a predicted probability of 0.20 (95% CI: 0.10–0.35), compared to 0.12 (95% CI: 0.06–0.23) for males in the same category.
It illustrates the predicted incidence of developing depression across 36 intersectional social strata, derived from combinations of ACE, sex, ethnicity, and SES.
A presents predicted depression probabilities for males with low levels of ACE across various social strata defined by ethnicity and SES; B presents predicted depression probabilities for females with low levels of ACE across various social strata defined by ethnicity and SES; C presents predicted depression probabilities formales with medium levels of ACE across various social strata defi ned by ethnicity and SES; D presents predicted depression probabilities for females with medium levels of ACE across various social strata defined by ethnicity and SES; E presents predicted depression probabilities for males with high levels of ACE across various social strata defined by ethnicity and SES; F presents predicted depression probabilities for females with high levels of ACE across various social strata defined by ethnicity and SES.
Discussions
This is the first study to adopt an intersectionality framework in exploring the complex interactions between ACEs and multiple socioeconomic and demographic factors in predicting depression risk among middle- and old-aged Canadian populations. The findings highlight the heterogeneity of ACE profiles in the national cohort of individuals aged 45 and older, emphasizing the importance of person-centered approaches to identify distinct risk constellations. Such differentiation is clinically relevant, as it supports tailored screening and intervention strategies based on individuals’ combined exposure to early adversity and current social positioning. By leveraging the intersectional framework, this study extends beyond conventional analyses that typically examine single dimensions, such as socioeconomic or demographic factors, in isolation. Instead, it thoroughly examines multiple forms of disparities based on various social determinants and exposures to ACEs. This approach has both theoretical and practical value for understanding depression, as it allows for a more comprehensive understanding of how ACE exposure, sex, ethnicity, and SES interact to shape the risk of depression. Our findings indicate that the lowest predicted risk for depression was associated with low ACE exposure, male sex, and high SES, regardless of ethnicity. In contrast, individuals with high ACE exposure, low SES, and female sex had the highest predicted depression incidence, suggesting the cumulative effect of early adversity, sex-based risk, and social disadvantage. This pattern highlights that females with both high ACE exposure and socioeconomic disadvantage represent a subgroup for whom standard risk screening may underestimate vulnerability. For clinicians, these findings suggest the need for stratified assessment protocols that integrate life-course adversity with present-day social stressors, as well as trauma-informed and socially responsive care approaches. The convergence of these intersecting vulnerabilities also highlights the need for targeted and dedicated intervention programs. Moreover, the modest but consistent effect sizes observed across strata indicate that even small additive risks may translate into substantial population-level burden, given the high prevalence of ACEs. Hence, identifying and prioritizing such high-risk intersections could improve early detection, inform referral pathways, and guide targeted preventive interventions in primary and community care settings.
Consistent with previous research, the current study highlights SES as the predominant structural determinant of depression risk, with ACEs and female sex acting as significant, yet independent, risk factors [57,58,59]. Notably, the observed 45% higher odds of depression among females were lower than commonly reported estimates. This attenuation may reflect the characteristics of the sample, comprising community-dwelling mid- to older-aged adults, where the sex gap in depression typically narrows [60]. Moreover, the use of a symptom-based measure (CES-D) and adjustment for socioeconomic covariates may have further reduced the apparent sex difference [61]. Individuals from lower SES backgrounds often face chronic stressors such as financial instability, limited access to education and healthcare, and exposure to unsafe living conditions, all of which can contribute to the elevated risk of depression [62]. In addition to SES, adverse experiences during childhood, such as neglect, abuse, and household dysfunction, have emerged as robust independent predictors of depression with far-reaching and enduring consequences across the lifespan [63]. These early-life stressors disrupt both emotional regulation and neurobiological development, impairing cognitive and social functioning [64]. These disruptions could then increase the likelihood of depression in adulthood via maladaptive coping, insecure attachment, and poor stress-response systems, all of which contribute to emotional vulnerability in later years [65]. Conversely, high SES often provides individuals with better coping resources, such as access to health services and care, opportunities for healthy lifestyle choices, and supportive social networks [66]. High SES and the absence of early childhood adversity could also reduce the depression risk by buffering the negative effects of other risk factors [67, 68].
In line with the literature, we found that females are disproportionately affected by depression in disadvantaged populations. Studies have suggested that males may experience fewer societal expectations around emotional labor, reduced exposure to interpersonal trauma, and greater social autonomy during childhood and adolescence, all of which interact with biological factors to reduce depression vulnerability [69]. Conversely, the elevated risk of depression among females exemplifies how structural disadvantages compound individual vulnerabilities. These findings underscore the importance of considering both sex and developmental stage when designing mental health policies in countries like Canada [70]. Sexed norms may limit access to coping resources. Females may be more likely to be exposed to greater psychosocial stress, and this increases their susceptibility to early-life adversities such as emotional neglect or abuse [71]. Therefore, while male sex may buffer against depression through both biological and psychosocial pathways, the depression risk associated with female sex cannot be simply determined by sex alone. Instead, it reflects an intersection of individual-level vulnerability and societal/structural disadvantage.
Although the current study did not find a distinct difference between White and other ethnic groups in terms of depression risk, race and ethnicity still play important roles in shaping one’s risk of depression, as they could influence other factors, such as experience of childhood adversity, opportunities and barriers to SES, cultural norms, access to care, historical discrimination, and others, provide considerable influence on depression indirectly [72].
Methodologically, the current study represents a novel contribution by integrating the intersectional framework into ACE research. Unlike traditional latent class or cumulative ACE approaches, MAIHDA simultaneously estimates multiple effects across several social identities (e.g., sex, SES, ethnicity), allowing for a rigorous quantification of between-stratum variation in depression risk. This analytic strategy captures both the unique and combined effects of psychosocial disadvantages, offering deeper insights into how various inequalities shape mental health outcomes in later life. By integrating intersectionality theory with advanced multilevel modeling, this study advances the methodological toolkit available for population mental health research.
Taken together, our study offers a comprehensive examination of the cumulative role of various social determinants and childhood adversity by identifying depression risk across social strata among older populations. These social strata reflect the existence of population groups in real-world settings. The deleterious effects of ACEs on depressive symptomatology may be exacerbated in the disadvantaged socioeconomic context, whereas the interplay between low ACE and male sex may be attenuated under conditions of structural adversity. Recognizing and addressing these interlocking axes of inequality is essential for designing interventions that meaningfully address the structural roots of mental health disparities.
Strengths and limitations
This study utilized data from a large, nationally representative Canadian cohort of older adults, which included extensive demographic, psychosocial, and clinical data, providing valuable insights at the population level. Additionally, by employing an intersectionality framework, it resonated with real-world situations that multiple social determinants, as well as ACEs, collectively shaped the depression risk. Finally, the study’s longitudinal design enables the examination of temporal associations and strengthens the capacity to infer potential causal relationships. However, some limitations should be acknowledged. First, the use of retrospective self-reported ACEs and depressive symptoms may be subject to recall and/or reporting biases. Given the long interval between childhood adversity and adult assessment, participants’ recollections of early-life experiences may be influenced by memory decay, their current mood state, or exposure to treatment. For instance, individuals with a history of depression or psychotherapy may have greater awareness and insight into past adversities, potentially leading to differential recall and inflation of observed associations. Second, it should be noted that certain forms of maltreatment were assessed only up to age 16, rather than 18. This discrepancy stems from the original design of the CEVQ. Consequently, some late-adolescent adversities may not have been captured, potentially leading to a modest underestimation of ACE exposure. Nonetheless, as most severe adversities typically occur earlier in childhood, this limitation is unlikely to substantially alter the observed associations [73, 74]. Additionally, information on adult trauma or revictimization was unavailable, which may lead to unmeasured/residual confounding and potential overestimation of the effects attributed solely to childhood adversity. Third, the generalizability of this study is limited by volunteer bias, socioeconomic skew, and the exclusion of institutionalized individuals and Indigenous communities living on reserves. Additionally, the ethnic and immigration composition of the sample may not accurately reflect the diversity of the Canadian population. While the findings offer valuable insights, they may not be applicable to other countries with distinct population compositions, cultural, and socioeconomic contexts. Differences in socioeconomic status and ethnic composition across regions may shape how these factors intersect and influence depression risk in ways that differ from those observed in the study population. Fourth, certain intersectional strata had relatively small sample sizes, which reduced statistical power to detect specific interactions. Finally, the CLSA did not collect information on the age of depression onset or diagnosis, preventing the establishment of precise temporal sequencing between ACE exposure and the development of depression.
Conclusions
Overall, the intersectionality of the selected social determinants (sex, SES, and race/ethnicity) and ACEs was associated with depression risk among individuals aged 45 and over. Those from marginalized groups, including females with lower SES and those exposed to ACEs, were more likely to experience depression. It is essential and critical to adopt an intersectional and equity-oriented perspective in both research and practice. Targeted interventions should be developed to identify and address the vulnerability origin(s) of “structural intersectionality”, particularly for those with early life traumatic experiences. Our findings advocate for personalized approaches to tackle mental health problems (i.e., depression) to recognize the complexity of childhood adversity and social determinants. Future research could extend these findings by examining the impact of ACEs on additional mental health outcomes beyond depression, exploring potential mediating mechanisms such as emotion regulation, and evaluating dedicated intervention strategies tailored to high-risk intersectional subgroups identified in this study.
Data availability
Data are available from the Canadian Longitudinal Study on Aging (www.clsa-elcv.ca) for researchers who meet the criteria for access to de-identified CLSA data. And the code in the article will be made available upon reasonable request.
References
World Health Organization. Depression and other common mental disorders: global health estimates. 2017;24.
Strauss R, Kurdyak P, Glazier RH. Mood disorders in late life: a population-based analysis of prevalence, risk factors, and consequences in community-dwelling older adults in ontario: troubles de l’humeur en age avance : une analyse dans la population de la prevalence, des facteurs de risque et des consequences chez des adultes ages vivant en milieu communautaire en Ontario. Can. J. Psychiatry. 2020;65:630–40. https://doi.org/10.1177/0706743720927812.
Navaneetham, K, & Arunachalam, D. 2023 Global population aging, 1950–2050. In Handbook of Aging, Health and Public Policy: Perspectives from Asia: Springer. Singapore, pp. 1–18.
Beekman AT, Copeland JR, Prince MJ. Review of community prevalence of depression in later life. Br. J. Psychiatry. 1999;174:307–11. https://doi.org/10.1192/bjp.174.4.307.
Kok RM, Reynolds CF 3rd. Management of depression in older adults: a review. JAMA. 2017;317:2114–22. https://doi.org/10.1001/jama.2017.5706.
Veltman E, Kok A, Lamers F, Stek M, van der Mast R, Rhebergen D. Stability and transition of depression subtypes in late life. J. Affect. Disord. 2020;265:445–52. https://doi.org/10.1016/j.jad.2020.01.049.
Koivumaa-Honkanen H, Kaprio J, Honkanen R, Viinamaki H, Koskenvuo M. Life satisfaction and depression in a 15-year follow-up of healthy adults. Soc. Psychiatry Psychiatr. Epidemiol. 2004;39:994–9. https://doi.org/10.1007/s00127-004-0833-6.
Beekman AT, Penninx BW, Deeg DJ, de Beurs E, Geerling SW, van Tilburg W. The impact of depression on the well-being, disability and use of services in older adults: a longitudinal perspective. Acta Psychiatr. Scand. 2002;105:20–27. https://doi.org/10.1034/j.1600-0447.2002.10078.x.
Taylor WD. Clinical practice. depression in the elderly. N. Engl. J. Med. 2014;371:1228–36. https://doi.org/10.1056/NEJMcp1402180.
Li M, D’Arcy C, Meng X. Maltreatment in childhood substantially increases the risk of adult depression and anxiety in prospective cohort studies: systematic review, meta-analysis, and proportional attributable fractions. Psychol. Med. 2016;46:717–30. https://doi.org/10.1017/S0033291715002743.
Li M, O’Donnell KJ, Caron J, Meaney MJ, Kobor M, D’Arcy C, et al. To what extent do social support and coping strategies mediate the relation between childhood maltreatment and major depressive disorder: a longitudinal community-based cohort. Dev. Psychopathol. 2022;36:1–12. https://doi.org/10.1017/S0954579422000918.
Su Y, D’Arcy C, Meng X. Social support and positive coping skills as mediators buffering the impact of childhood maltreatment on psychological distress and positive mental health in adulthood: analysis of a national population-based sample. Am. J. Epidemiol. 2020;189:394–402. https://doi.org/10.1093/aje/kwz275.
Su Y, D’Arcy C, Meng X. Intergenerational effect of maternal childhood maltreatment on next generation’s vulnerability to psychopathology: a systematic review with meta-analysis. Trauma. Violence Abuse. 2022;23:152–62. https://doi.org/10.1177/1524838020933870.
Su Y, Li M, D’Arcy C, Caron J, O’Donnell K, Meng X. To what extent do social support and mastery mediate the association between childhood maltreatment and depression? a sequential causal mediation analysis. Epidemiol. Psychiatr. Sci. 2022;31:e77 https://doi.org/10.1017/S2045796022000609.
Gilbert R, Widom CS, Browne K, Fergusson D, Webb E, Janson S. Burden and consequences of child maltreatment in high-income countries. Lancet. 2009;373:68–81. https://doi.org/10.1016/S0140-6736(08)61706-7.
Yoon D, Yoon S, Pei F, Ploss A. The roles of child maltreatment types and peer relationships on behavior problems in early adolescence. Child. Abuse Negl. 2021;112:104921 https://doi.org/10.1016/j.chiabu.2020.104921.
Finkelhor D, Ormrod RK, Turner HA. Poly-victimization: a neglected component in child victimization. Child. Abuse Negl. 2007;31:7–26. https://doi.org/10.1016/j.chiabu.2006.06.008.
Narayan AJ, Merrick JS, Lane AS, Larson MD. A multisystem, dimensional interplay of assets versus adversities: revised benevolent childhood experiences (BCEs) in the context of childhood maltreatment, threat, and deprivation. Dev. Psychopathol. 2023;35:2444–63. https://doi.org/10.1017/S0954579423000536.
Afifi TO, Taillieu T, Salmon S, Davila IG, Stewart-Tufescu A, Fortier J, et al. Adverse childhood experiences (ACEs), peer victimization, and substance use among adolescents. Child. Abuse Negl. 2020;106:104504 https://doi.org/10.1016/j.chiabu.2020.104504.
Salmon S, Chartier M, Roos LE, Afifi TO. Typologies of child maltreatment and peer victimization and the associations with adolescent substance use: a latent class analysis. Child. Abuse Negl. 2023;140:106177 https://doi.org/10.1016/j.chiabu.2023.106177.
Finkelhor, D, Turner, H, Hamby, S, & Ormrod, R (2011). Polyvictimization: children’s exposure to multiple types of violence, crime, and abuse. Available from: https://www.ojp.gov/pdffiles1/ojjdp/235504.pdf.
Anda RF, Butchart A, Felitti VJ, Brown DW. Building a framework for global surveillance of the public health implications of adverse childhood experiences. Am. J. Prev. Med. 2010;39:93–8. https://doi.org/10.1016/j.amepre.2010.03.015.
Finkelhor D. Screening for adverse childhood experiences (ACEs): cautions and suggestions. Child. Abuse Negl. 2018;85:174–9. https://doi.org/10.1016/j.chiabu.2017.07.016.
Chang X, Jiang X, Mkandarwire T, Shen M. Associations between adverse childhood experiences and health outcomes in adults aged 18–59 years. PLoS one. 2019;14:e0211850 https://doi.org/10.1371/journal.pone.0211850.
McLaughlin, KA Future directions in childhood adversity and youth psychopathology. In Future work in clinical child and adolescent psychology. Routledge. New York, NY, 2018 pp. 345-66
Matsumoto M, Piersiak HA, Letterie MC, Humphreys KL. Population-Based estimates of associations between child maltreatment types: a meta-analysis. Trauma. Violence Abuse. 2023;24:487–96. https://doi.org/10.1177/15248380211030502.
England-Mason G, Casey R, Ferro M, MacMillan HL, Tonmyr L, Gonzalez A. Child maltreatment and adult multimorbidity: results from the Canadian community health survey. Can. J. Public. Health. 2018;109:561–72. https://doi.org/10.17269/s41997-018-0069-y.
Bailey RK, Mokonogho J, Kumar A. Racial and ethnic differences in depression: current perspectives. Neuropsychiatr. Dis. Treat. 2019;15:603–9. https://doi.org/10.2147/NDT.S128584.
Hyde JS, Mezulis AH. Gender differences in depression: biological, affective, cognitive, and sociocultural factors. Harv. Rev. Psychiatry. 2020;28:4–13. https://doi.org/10.1097/HRP.0000000000000230.
Lemstra M, Neudorf C, D’Arcy C, Kunst A, Warren LM, Bennett NR. A systematic review of depressed mood and anxiety by SES in youth aged 10-15 years. Can. J. Public. Health. 2008;99:125–9. https://doi.org/10.1007/BF03405459.
Meinzer MC, Pettit JW, Viswesvaran C. The co-occurrence of attention-deficit/hyperactivity disorder and unipolar depression in children and adolescents: a meta-analytic review. Clin. Psychol. Rev. 2014;34:595–607. https://doi.org/10.1016/j.cpr.2014.10.002.
Balloo K, Hosein A, Byrom N, Essau CA. Differences in mental health inequalities based on university attendance: Intersectional multilevel analyses of individual heterogeneity and discriminatory accuracy. SSM Popul. Health. 2022;19:101149 https://doi.org/10.1016/j.ssmph.2022.101149.
Kern MR, Duinhof EL, Walsh SD, Cosma A, Moreno-Maldonado C, Molcho M, et al. Intersectionality and adolescent mental well-being: a cross-nationally comparative analysis of the interplay between immigration background, socioeconomic status and gender. J. Adolesc. Health. 2020;66:S12–S20. https://doi.org/10.1016/j.jadohealth.2020.02.013.
Bangasser DA, Valentino RJ. Sex differences in stress-related psychiatric disorders: neurobiological perspectives. Front. Neuroendocrinol. 2014;35:303–19. https://doi.org/10.1016/j.yfrne.2014.03.008.
Tozzi L, Garczarek L, Janowitz D, Stein DJ, Wittfeld K, Dobrowolny H, et al. Interactive impact of childhood maltreatment, depression, and age on cortical brain structure: mega-analytic findings from a large multi-site cohort. Psychol. Med. 2020;50:1020–31. https://doi.org/10.1017/S003329171900093X.
Grant BF, Dawson DA, Stinson FS, Chou SP, Dufour MC, Pickering RP. The 12-month prevalence and trends in DSM-IV alcohol abuse and dependence: United States, 1991-1992 and 2001-2002. Drug. Alcohol. Depend. 2004;74:223–34. https://doi.org/10.1016/j.drugalcdep.2004.02.004.
Kendler KS, Kessler RC, Walters EE, MacLean C, Neale MC, Heath AC, et al. Stressful life events, genetic liability, and onset of an episode of major depression in women. Am. J. Psychiatry. 1995;152:833–42. https://doi.org/10.1176/ajp.152.6.833.
Smith DT, Mouzon DM, Elliott M. Reviewing the assumptions about men’s mental health: an exploration of the gender binary. Am. J. Mens. Health. 2018;12:78–89.
Wenham C, Smith J, Morgan R, Gender and COVID-19 Working Group. COVID-19: the gendered impacts of the outbreak. Lancet. 2020;395:846–8. https://doi.org/10.1016/S0140-6736(20)30526-2.
Marmot M, Friel S, Bell R, Houweling TAJ, Taylor S, on behalf of the Commission on Social Determinants of Health. Closing the gap in a generation: health equity through action on the social determinants of health. Lancet. 2008;372:1661–9. https://doi.org/10.1016/S0140-6736(08)61690-6.
Collins, PH. Black feminist thought: Knowledge, consciousness, and the politics of empowerment. Routledge, New York, 1990.
McCall I. The complexity of intersectionality. Signs. 2005;30:1771–1800.
Hankivsky O, Christoffersen A. Intersectionality and the determinants of health: a Canadian perspective. Crit. Public. Health. 2008;18:271–83.
McLaughlin KA, Costello EJ, Leblanc W, Sampson NA, Kessler RC. Socioeconomic status and adolescent mental disorders. Am. J. Public. Health. 2012;102:1742–50. https://doi.org/10.2105/AJPH.2011.300477.
Mersky JP, Topitzes J, Reynolds AJ. Impacts of adverse childhood experiences on health, mental health, and substance use in early adulthood: a cohort study of an urban, minority sample in the US. Child. Abuse Negl. 2013;37:917–25. https://doi.org/10.1016/j.chiabu.2013.07.011.
Raina P, Wolfson C, Kirkland S, Griffith LE, Balion C, Cossette B, et al. Cohort profile: The Canadian longitudinal study on aging (CLSA). Int. J. Epidemiol. 2019;48:1752–1753j. https://doi.org/10.1093/ije/dyz173.
Andresen EM, Malmgren JA, Carter WB, Patrick DL. Screening for depression in well older adults: evaluation of a short form of the CES-D (center for epidemiologic studies depression scale). Am. J. Prev. Med. 1994;10:77–84.
Zhang W, O’Brien N, Forrest JI, Salters KA, Patterson TL, Montaner JS, et al. Validating a shortened depression scale (10 item CES-D) among HIV-positive people in British Columbia, Canada. PLoS One. 2012;7:e40793 https://doi.org/10.1371/journal.pone.0040793.
Tanaka M, Wekerle C, Leung E, Waechter R, Gonzalez A, Jamieson E, et al. Preliminary evaluation of the childhood experiences of violence questionnaire short form. J. Interpers. Violence. 2012;27:396–407. https://doi.org/10.1177/0886260511416462.
Walsh CA, MacMillan HL, Trocmé N, Jamieson E, Boyle MH. Measurement of victimization in adolescence: development and validation of the childhood experiences of violence questionnaire. Child. Abuse Negl. 2008;32:1037–57. https://doi.org/10.1016/j.chiabu.2008.05.003.
Harris, KM, & Udry, JR National Longitudinal Study of adolescent to adult health (add health), 1994-2008 [public use]. Ann Arbor, MI: Carolina Population Center, University of North Carolina-Chapel Hill [distributor], Inter-university Consortium for Political and Social Research [distributor], 2022:08–06.
Barker LC, Hussain-Shamsy N, Rajendra KL, Bronskill SE, Brown HK, Kurdyak P, et al. The use of key social determinants of health variables in psychiatric research using routinely collected health data: a systematic analysis. Soc. Psychiatry Psychiatr. Epidemiol. 2023;58:183–91. https://doi.org/10.1007/s00127-022-02368-x.
Geiser C Latent class analysis. In: Data Analysis With Mplus. The Guilford Press, New York, NY, 2012. pp. 232–70. .
Enders CK. Applied missing data analysis. New York, NY. Guilford Press. 2010.
Muthén LK, Muthén. B Mplus user’s guide Retrieved from Los Angeles, Muthén & Muthén, California. 2017.
Merlo J. Multilevel analysis of individual heterogeneity and discriminatory accuracy (MAIHDA) within an intersectional framework. Soc. Sci. Med. 2018;203:74–80. https://doi.org/10.1016/j.socscimed.2017.12.026.
Gilman SE, Kawachi I, Fitzmaurice GM, Buka SL. Socioeconomic status in childhood and the lifetime risk of major depression. Int. J. Epidemiol. 2002;31:359–67.
Haahr-Pedersen I, Perera C, Hyland P, Vallières F, Murphy D, Hansen M, et al. Females have more complex patterns of childhood adversity: implications for mental, social, and emotional outcomes in adulthood. Eur. J. Psychotraumatol. 2020;11:1708618.
Su Y, Li M, Caron J, Li D, Meng X. Differential effects of lifetime stressors on major depressive disorder severity: a longitudinal community-based cohort study. Eur. Psychiatry. 2024;67:e66.
Salk RH, Hyde JS, Abramson LY. Gender differences in depression in representative national samples: meta-analyses of diagnoses and symptoms. Psychological Bull. 2017;143:783.
Sonnenberg CM, Beekman AT, Deeg DJ, van Tilburg W. Sex differences in late-life depression. Acta Psychiatr Scand. 2000;101:286–92.
Schreier H, Chen E. Socioeconomic status and the health of youth: a multilevel, multidomain approach to conceptualizing pathways. Pediatrics. 2013;139:606.
Su Y, Li M, D’Arcy C, Caron J, Meng X. Childhood maltreatment and major depressive disorder in well-being: a network analysis of a longitudinal community-based cohort. Psychol. Med. 2023;53:7180–8.
Smith KE, Pollak SD. Early life stress and development: potential mechanisms for adverse outcomes. J. Neurodev. Disord. 2020;12:1–15.
Hammen, C, Bistricky, SL, & Ingram, RE Vulnerability to psychopathology: Risk across the lifespan. The Guilford Press, New York, NY, 2001;226-57.
Taylor SE, Stanton AL. Coping resources, coping processes, and mental health. Annu. Rev. Clin. Psychol. 2007;3:377–401.
Dinwiddie GY, Gaskin DJ, Chan KS, Norrington J, McCleary RJ. Residential segregation, geographic proximity and type of services used: evidence for racial/ethnic disparities in mental health. Soc. Sci. Med. 2013;80:67–75.
Kirkbride JB, Anglin DM, Colman I, Dykxhoorn J, Jones PB, Patalay P, et al. The social determinants of mental health and disorder: evidence, prevention and recommendations. World Psychiatry. 2024;23:58–90.
Tabler J, Schmitz RM, Nagata JM, Geist CJ. Self-perceived gender expression, discrimination, and mental health disparities in adulthood. SSM - Ment. Health. 2021;1:100020.
Li S, Zhang X, Cai Y, Zheng L, Pang H, Lou L. Sex difference in incidence of major depressive disorder: an analysis from the Global Burden of Disease Study 2019. Ann. Gen. Psychiatry. 2023;22:53. https://doi.org/10.1186/s12991-023-00486-7.
Mengelkoch S, Slavich GM. Sex differences in stress susceptibility as a key mechanism underlying depression risk. Curr. Psychiatry Rep. 2024;26:157–65.
Vines AI, Ward JB, Cordoba E, Black KZ. Perceived racial/ethnic discrimination and mental health: a review and future directions for social epidemiology. Curr. Epidemiol. Rep. 2017;4:156–65.
Dunn EC, Nishimi K, Gomez SH, Powers A, Bradley B. Developmental timing of trauma exposure and emotion dysregulation in adulthood: are there sensitive periods when trauma is most harmful?. J. Affect. Disord. 2018;227:869–77. https://doi.org/10.1016/j.jad.2017.10.045.
Hardt J, Rutter M. Validity of adult retrospective reports of adverse childhood experiences: review of the evidence. J. Child. Psychol. Psyc. 2004;45:260–73. https://doi.org/10.1111/j.1469-7610.2004.00218.x.
Acknowledgements
This research was made possible using the data/biospecimens collected by the Canadian Longitudinal Study on Aging (CLSA). Funding for the Canadian Longitudinal Study on Aging (CLSA) is provided by the Government of Canada through the Canadian Institutes of Health Research (CIHR) under grant reference: LSA 94473 and the Canada Foundation for Innovation, as well as the following provinces, Newfoundland, Nova Scotia, Quebec, Ontario, Manitoba, Alberta, and British Columbia. This research has been conducted using the CLSA dataset Baseline Comprehensive Dataset (Version 7.0), and Follow-up 1 Comprehensive Dataset version 5.0, under Application Number 23CA014. The CLSA is led by Drs. Parminder Raina, Christina Wolfson and Susan Kirkland. Funding for support of the CLSA COVID-19 questionnaire-based study is provided by the Juravinski Research Institute, Faculty of Health Sciences, McMaster University, the Provost Fund from McMaster University, the McMaster Institute for Research on Aging, the Public Health Agency of Canada/CIHR grant reference CMO 174125 and the government of Nova Scotia. The time and commitment of the participants to the CLSA study platform is gratefully acknowledged, without whom this research would not be possible.
Funding
This study was funded by a Catalyst Grant: Analysis of CLSA Data, from the Canadian Institutes of Health Research, grant number 192900.
Author information
Authors and Affiliations
Contributions
XFM and YYS had full access to all of the data in the study and took responsibility for the integrity of the data and the accuracy of the data analysis. Conceptualization: XFM. Acquisition, analysis, and interpretation of data: All authors. Drafting of the manuscript: XFM, YYS. Critical revision of the manuscript for important intellectual content: All authors. Statistical analysis: XFM, YYS. Administrative, technical, or material support: MJ, CA. Study supervision: XFM.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Disclaimer
The opinions expressed in this manuscript are the author’s own and do not reflect the views of the Canadian Longitudinal Study on Aging.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Su, Y., Li, M., Fleury, MJ. et al. Understanding depression through an intersectional framework: the joint impact of childhood adversities and social determinants using Canadian longitudinal study on aging (CLSA) data. Transl Psychiatry 16, 227 (2026). https://doi.org/10.1038/s41398-026-03973-z
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41398-026-03973-z