Abstract
Objective To evaluate the joint orthodontic, paediatric and restorative (JOPR) clinic at Leeds Dental Institute, which manages complex dental cases requiring multidisciplinary care.
Design Retrospective service evaluation.
Setting Multidisciplinary clinic at Leeds Dental Institute.
Materials and methods Data were collected from all new patient consultations at the JOPR clinic between March 2023 and April 2024. Referral sources, case types, patient demographics, treatment pathways, and outcomes were analysed, along with timeframes along the patient journey.
Results Hypodontia was the most common reason for referral, followed by ectopic/impacted teeth, trauma, and developmental abnormalities. Most referrals originated internally, particularly from orthodontics. Treatment planning typically involved orthodontic-led space management, followed by restorative or paediatric input. A significant proportion of patients were referred to primary care for treatment delivery. The average triage time was 13 days, and average time from referral to clinic attendance was 69 days. Treatment duration varied significantly due to case complexity and interdepartmental coordination.
Conclusion The JOPR clinic facilitates efficient interdisciplinary planning and care for patients with complex dental needs. This model improves coordination, reduces duplication, and supports targeted treatment delivery. Findings may inform the development of similar services and align with national care improvement initiatives.
Key points
-
This paper offers a valuable understanding of how a collaborative approach across specialties can improve the management of complex dental cases, providing a model for other institutions to follow.
-
The article describes effective referral and triage processes, which can help other clinics optimise their patient management systems and ensure timely, appropriate care.
-
The paper identifies areas for enhancing clinic efficiency, suggesting strategies that can benefit other multidisciplinary clinics seeking to improve service delivery.
Similar content being viewed by others
Introduction
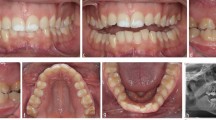
The joint orthodontic, paediatric and restorative (JOPR) clinic at the Leeds Dental Institute (LDI) aims to integrate the expertise of orthodontic, restorative and paediatric dental specialities in managing cases that require interdisciplinary care. Hypodontia represents the highest proportion of the cases, along with tooth size discrepancies (e.g., microdontia); ectopic or impacted teeth causing complex problems, such as resorption; tooth development defects, such as amelogenesis imperfecta and dentinogenesis imperfecta; as well as complex dental trauma.
Treatment approaches typically involve a combination of orthodontic space management and restorative intervention through direct/indirect restoration or tooth replacement. Particularly complex cases may also involve pre-prosthetic bone augmentation procedures, with or without adjunctive orthognathic surgery. Aesthetic concerns are addressed in this multidisciplinary clinic, such as closing spaces and correcting tooth size or shape discrepancies through composite bonding. Restorative and paediatric dentists also play a crucial role in the endodontic management of non-vital or infected teeth affected by trauma or developmental abnormalities. In cases of ectopic or impacted teeth, the management approach is tailored according to the tooth's position and the patient's age. Where surgical exposure is required, this may be completed by either the paediatric dentistry or oral surgery team, depending on the patient age, medical history and complexity of surgical care needed.
An overview of the joint orthodontic, paediatric and restorative clinic
The JOPR clinic is a tertiary clinic operating as one multidisciplinary unit, with each specialty contributing to formulating and executing comprehensive treatment plans. The decision as to what the best options for management may be is dictated by the severity of the condition and stage of dental development of the patient, as well as the patient and parent/guardian preferences.
The restorative team is also involved in the planning of these cases and generally focuses on restoration of tooth form or appearance, and the prosthetic replacement of missing teeth through removable or fixed prostheses, including implant-based replacement.
The paediatric dentistry team provides age-appropriate restorative treatment items for patients aged 15 and under. They also have access to inhalation sedation and general anaesthetic services when patient cooperation would otherwise preclude their treatment.
The orthodontic team are responsible for redistributing space, aligning teeth and improving interocclusal relationships to facilitate any further restorative treatment that may be required.
Effective communication and coordination among these specialities are essential for achieving optimal functional and aesthetic outcomes, as treatment often spans from many months to several years and requires long-term follow-up. The clinic also serves as a valuable training environment for resident dentists, such as dental core and specialty trainees, enabling them to gain experience in developing treatment plans and the multidisciplinary management of patients, by working closely with consultants from all three specialities. There are two consultants from each specialty, who alternate attendance at the clinic. This small team helps with consistency of approach and long-term planning.
Patient journey
Patients referred from primary care are first assessed by the relevant specialty team to determine whether a multidisciplinary approach is required. Following this initial assessment, a clinic referral pro forma is completed and the referrals, are triaged to assess their suitability for review on the joint clinic. The pre-JOPR specialty assessment serves a valuable role in ensuring that only appropriate cases requiring multidisciplinary input are forwarded to the joint clinic. Additionally, up-to-date clinical records, including radiographs, study models, and photographs, are often taken during this visit. These assist in treatment planning at the multidisciplinary team stage and provide essential diagnostic information for the involved teams, thus avoiding repetition and enhancing treatment planning efficiency. A multidisciplinary pre-clinic meeting is attended by all team members before every JOPR clinic. Each case is presented along with their records to identify potential treatment strategies, identify challenges and ensure all specialties are prepared to address them to ensure efficient use of clinic time.
During the clinic, patients are evaluated by a team of resident clinicians under the supervision of consultants. Based on this assessment, a provisional treatment plan is developed. Patients then undergo treatment within the relevant specialty clinic(s).
The clinic also promotes young people and parents in shared decision-making for hypodontia. This may influence the approach taken initially. As a result, patients may undergo interim reviews on the JOPR clinic. These reviews serve to address new treatment considerations/challenges, evaluate progress, or assess overall treatment outcomes. Figure 1 illustrates the clinic's workflow.1
Joint orthodontic, paediatric and restorative patient clinic workflow
Methodology
A retrospective service evaluation was carried out to analyse data from all new patient consultations at the JOPR clinic between March 2023 and April 2024. This timeframe was chosen following implementation of a prospective database of patients who had been referred to this clinic from March 2023. A total of 110 patient records were examined to capture referral sources, case types, provider involvement, and patient demographics. Data were recorded on an Excel spreadsheet.
The principle aims for this service evaluation were:
-
To understand referral sources and case diversity on the JOPR clinic
-
To assess timeframes along the JOPR patient's journey
-
To measure post-JOPR clinic consultation patient outcomes.
Results
Referral patterns and patient demographics
The majority of referrals to the JOPR clinic were received internally from other departments within the LDI (Fig. 2). The orthodontic department referred the largest number of patients to the JOPR clinic (n = 64), while the paediatric and restorative departments referred significantly lower numbers: 24 and eight, respectively. Only six out of 110 referrals came directly from primary care orthodontic services, all of which were made by clinicians working in both LDI and primary care who regularly assess patients on JOPR. This is because all referrals to LDI must first be triaged and assessed within individual specialties before proceeding to a JOPR assessment. JOPR has also received 21 referrals from sources such as other secondary care units seeking opinion or advice on case management. This highlights that the multidisciplinary nature of the clinic not only facilitates complex case management within the LDI but may also offer valuable insights and guidance to specialists from outside institutions.
Joint orthodontic, paediatric and restorative patient referral sources
The referrals included 21 urgent cases, 74 routine cases, and 15 cases where the referral urgency was not specified. Urgent cases typically involved issues that required prompt attention to prevent further deterioration, such as advanced root resorption, active tooth wear, significant malalignment of teeth of critical importance, or recent complicated dental trauma.
The age of patients seen on the JOPR clinic ranged from 8–19 years. The median and mean ages of JOPR patients were 15 and 16 years, respectively. This highlights the clinic's ability to cater to a wide spectrum of dental developmental phases, from childhood to late adolescence, and its flexibility in addressing various dental issues, from managing early intervention cases to more complex, delayed treatments.
Frequently seen conditions and initial management
Hypodontia accounted for the largest proportion of cases seen at the JOPR clinic, with 54 out of 110 patients referred for management of this condition. Other frequently seen cases included ectopic or impacted teeth (23 patients), trauma-related cases (15 patients), and microdontia (12 patients). Nine patients were referred for other developmental abnormalities, such as molar-incisor hypomineralisation or regional odontodysplasia (Fig. 3).
Joint orthodontic, paediatric and restorative patient case types
Initial treatment plans are usually formulated after the first consultation, with patients then subsequently referred to a chosen speciality for initiation or continuation of the treatment plan. A total of 59 patients were directed to the orthodontic department, nine to paediatric and 14 to restorative. A significant proportion of the patients (n = 21) were referred to primary care general dental practice or joint primary orthodontic/general dental care for treatment delivery following assessment and formulation of a treatment plan on JOPR. This suggests that a substantial number of JOPR patients can be successfully treated in primary care, following the development of their treatment plans within a specialist tertiary care setting. Seven of the patients were managed through joint interdisciplinary care, receiving multiple treatments simultaneously across different departments, for example, undergoing removable orthodontic appliance treatment while also receiving restorative work (Fig. 4).
Referrals to specialities from joint orthodontic, paediatric and restorative
The initial consultation on the JOPR clinic is typically where the decision is made regarding who will carry out any subsequent restorative work. For the majority of the assessed cohort, treatment plans were scheduled to be carried out by the LDI restorative department (32 cases), while the LDI paediatric dentistry team managed 15 cases. This distribution was due to cases seen on JOPR typically involving greater restorative complexity or requiring treatment to be postponed until orthodontic treatment was completed, by which time patients are often over 16 and no longer eligible for paediatric dental care. Here, 22 cases were referred to their general dental practitioners (GDPs) for restorative care, while in 31 cases, no decision was made at the time of the first JOPR appointment. In these instances, patients were informed that the decision would be deferred until the completion of orthodontic treatment, and that future treatment might involve financial considerations should restorative treatment be discharged to a primary care setting. Interestingly, one patient required joint restorative care, with treatments provided by both the GDP and the LDI restorative department, emphasising the need for effective coordination between primary and secondary care providers to manage JOPR patient care efficiently (Fig. 5).
Restorative treatment provider
For the patients managed within the restorative department for treatment, the majority (12 patients) were planned to be managed by a specialty trainee, while four patients were referred for treatment by a consultant. Two patients were referred for treatment with a dental therapist, and for 14 patients, the decision regarding their clinician had not yet been made at the time of the JOPR clinic.
Timeframes along the patient journey
-
Triage time – the mean triage time was ~13 days, with urgent cases triaged in an average of eight days and routine cases in 11 days. The longest triage time recorded was 43 days – this constitutes a significant outlier and was a result of a missed referral correspondence. This was addressed via incident reporting pathways
-
Time from referral to clinic – the mean time from referral to clinic appointment was 69 days. Urgent cases waited an average of 53 days, while routine cases waited 72 days. The longest time recorded for routine cases was 237 days – this outlier has been a result of patient repeatedly postponing appointments
-
Time from triage to clinic attendance – the average time from triage to clinic attendance was 57 days, with urgent cases averaging 47.4 days and routine cases 60.9 days
-
Time from initial consultation to treatment completion – for a small number of patients (n = 7) who did complete all their overall treatment at the time of writing this article, the average time from JOPR consultation to treatment completion was 297 days, with a shortest time of 94 days and longest of 524 days, highlighting a large variability in patients' overall treatment journey timeframes.
Restorative treatment duration
For the patients who have completed their restorative treatment within the LDI, either in the restorative (n = 8) or paediatric dentistry departments (n = 5), by the time of writing of this article, the duration varied significantly, with an average treatment time of 179 days (range 7–366 days) from initial planning to completion. One of the patients referred for treatment within the paediatric dentistry department was discharged early due to not being brought for appointments.
Discussion
The data collected in this project provide a valuable insight into the efficiency and effectiveness of the JOPR clinic's interdisciplinary approach. The majority of referrals were internal, emphasising the need for strong interdisciplinary communication between departments in the LDI. The relatively small number of referrals from primary care (n = 6) reflects one of the clinic's referral criteria, which specify that cases must first be assessed within LDI by a one of the specialty teams. This helps to ensure that only appropriate cases requiring multidisciplinary input are seen in the clinic, avoiding unnecessary appointments.
Our findings indicate that hypodontia remains the most prevalent condition managed by the joint clinic. This supports the clinic's focus on providing long-term care for patients with missing teeth, involving both orthodontic and restorative interventions, ensuring that patients receive comprehensive care tailored to their individual needs.
Data from this service evaluation demonstrate a significant variability in the duration of restorative treatment for patients seen at the JOPR clinic. The average restorative treatment duration was 162 days (approximately 5.4 months), with treatment times ranging from 7–393 days. This wide range reflects not only the complexity of many cases but also the impact of long waiting lists and the need for interdisciplinary coordination, where multiple specialists must be involved to ensure optimal outcomes. When compared to similar evaluations, the variability and overall treatment duration at the LDI JOPR clinic align with findings from other multidisciplinary hypodontia clinics.2
Stevenson et al. (2017) reported a total treatment duration of 38 months (3.2 years) for patients requiring combined orthodontic and restorative care, with an orthodontic phase lasting an average of 21 months and a shorter restorative phase, averaging two months but extending up to six months in some cases.2 A key difference observed between the two clinics is the proportion of patients referred for restorative care within a general dental practice setting – 10% in the Dundee study compared to 20% at LDI. This variation may reflect efforts to manage long restorative waiting lists by appropriately directing cases that do not meet the criteria for specialist-level care, such as single-unit resin-bonded bridges, to primary care. Alternatively, it could suggest an increasing capability within general dental practice to manage multidisciplinary cases since the publication of Stevenson's study in 2013. Other contributing factors may include geographical and political differences, such as the number and experience of local GDPs or variations in dental remuneration systems between Scotland and England.
The difference in times between urgent and routine cases regarding referral to triage and triage to consultation was minimal, averaging around 2.5 days. This highlights the efficiency of the triage processes at the JOPR clinic, as both urgent and non-urgent cases are seen within an acceptable timeframe. However, the average times for the patient journey were affected by outliers, including patients who frequently cancelled appointments or referrals that were lost in the system. This suggests a need for closer monitoring and timely intervention for referrals with significantly longer-than-average waiting times. In younger patients, consideration of the Was Not Brought pathway may be warranted to ensure appropriate follow-up and care.3
Conclusion and limitations
The JOPR clinic plays a critical role in the management of complex dental cases, particularly hypodontia, through a collaborative approach involving orthodontic, restorative, and paediatric dentistry specialities. This service evaluation highlights the clinic's strengths in providing comprehensive care but also identifies areas for potential improvement and may be valuable to the wider readership if considering a referral to, or the setting up of, a similar service. The findings of this evaluation may contribute to the ongoing aims of the Getting It Right First Time programme, by highlighting how effective interdisciplinary collaboration can improve care pathways, reduce unnecessary appointments, and ensure efficient resource use. Evaluations like this provide data that can help improve and standardise multidisciplinary team services, ensuring more consistent and equitable specialist dental care.
The variability in restorative treatment durations highlights the need for further evaluation of clinic processes to enhance efficiency and reduce patient waiting times. As data collection began in March 2023, most patients are still undergoing treatment, making it impossible to draw conclusions about the overall treatment duration for the majority of the cohort studied. The values obtained for restorative treatment duration are based on a relatively small number of patients who have completed their treatment, specifically, only eight out of 31 restorative patients and five out of 32 paediatric dentistry patients had finished their treatment by the time of writing this article. Future evaluations should extend data collection to include the missing treatment completion dates to gain a better understanding of the long-term timeline of the JOPR patient journey.
Data availability
The data that support the findings of this study are not publicly available due to institutional data governance policies but are available from the corresponding author on reasonable request.
References
Barber S, Jones A, Patel V A, Ashley M P. Involving young people and parents in decision-making for hypodontia. Br Dent J 2023; 235: 529–534.
Stevenson B, Patel D, Ricketts D, Cord A. The orthodontic-restorative interface in patients with hypodontia: the patient's journey. Dent Update 2013; 40: 354–360.
British Dental Association. Was not brought safeguarding resources. Available at https://www.bda.org/advice/patient-care-and-safety/safeguarding-was-not-brought (accessed 1 January 2025).
Author information
Authors and Affiliations
Contributions
SS led the data collection, analysis, presentation, and drafting of the manuscript. NJP, HPB, KO'D, CL, SM, KD and HKD contributed to critical review, revisions, and co-authorship of the final manuscript.
Corresponding author
Ethics declarations
The authors declare no conflicts of interest related to this study. As this project was a retrospective service evaluation involving anonymised patient data and did not alter patient care, formal ethics approval and individual patient consent were not required.
Rights and permissions
Open Access. This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0.© The Author(s) 2025.
About this article
Cite this article
Stasiak, S., Patel, N., Beddis, H. et al. Evaluation of the joint orthodontic-paediatric-restorative clinic at Leeds Dental Institute: a review of referral sources, case management, and outcomes. Br Dent J (2025). https://doi.org/10.1038/s41415-025-8874-1
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41415-025-8874-1