Abstract
Introduction Anaphylaxis, although rare, can occur in dental settings. While local anaesthetics (LAs) are widely used in dentistry, true allergic reactions to LAs are uncommon. Most adverse reactions associated with their use are non-allergic in nature, often resulting from factors such as vasovagal syncope, toxicity, or procedural trauma. The overlap in clinical presentation makes distinguishing true allergic reactions from other causes particularly challenging.
Aims To determine the prevalence of true LA allergies and characterise the nature of adverse drug reactions (ADRs) following LA administration.
Design Retrospective, observational study.
Materials and methods Data from 37 patients referred with suspected LA allergies (December 2021 to June 2024) were analysed. Skin prick testing, intradermal testing, and drug provocation tests were performed to assess ADRs and identify potential allergens, including co-administered medications.
Results None of the patients tested positive for immunoglobulin E (IgE)-mediated LA allergies. Four patients had allergies to co-administered agents, while other reactions were non-allergic, including vasovagal syncope and procedural trauma.
Discussion True IgE-mediated LA allergies are rare. Non-allergic reactions, such as vasovagal syncope and toxicity, are more common and often misinterpreted as allergies.
Conclusion Accurate diagnosis is essential to distinguish between true allergies and non-allergic reactions, especially in dental settings. Enhanced training can help reduce misdiagnosis and unnecessary interventions.
Key points
-
This article highlights the difficulty that dentists face in identifying anaphylaxis.
-
Emphasises that if a patient does have a true anaphylactic reaction, it was unlikely to have been cause by local anaesthetic.
-
Dentists should exercise caution in labelling a patient as being allergic to local anaesthetics as it is extremely rare and such a label can delay vital treatments.
Similar content being viewed by others
Introduction
Anaphylaxis is a severe and potentially life-threatening medical emergency that can occur in dental practice. Although a variety of commonly used medications, antiseptics, or materials in dentistry can trigger allergic reactions, there is still an ongoing debate about the contribution of local anaesthetics (LAs) to this burden.
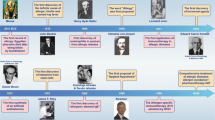
LAs have been employed for anaesthesia since the initial introduction of cocaine in the late 19th century. They can be administered through various routes, including topical application, infiltration, nerve blocks, epidural, or spinal techniques. Since their development, LA agents have been extensively used across multiple medical specialties, including dentistry, minor surgery, dermatology, orthopaedics, obstetrics and others.
LAs can be broadly classified into two groups: amides (such as lidocaine, articaine, and mepivacaine) and esters (including benzocaine, procaine, and cocaine).2 Allergies are more common with the ester group, as they are metabolised into para-aminobenzoic acid, which can cause delayed type IV hypersensitivity reactions,2,3 leading to contact allergies affecting the skin or mucosa. However, most LAs used in dentistry are from the amide group,2 where true allergic reactions are rare. When allergies to amide LAs do occur, they are more likely to be related to excipients or preservatives in the formulation rather than the anaesthetic itself.4
While LAs are generally safe, complications can occur and are clinically important to distinguish. A rare but potentially life-threatening event is LA systemic toxicity (LAST), caused by high plasma concentrations due to overdose or inadvertent intravascular injection. LAST typically presents with central nervous system symptoms such as tinnitus, perioral numbness, confusion, and seizures, and may progress to cardiovascular collapse. The estimated incidence is approximately one in 10,000 regional anaesthetic procedures.1 More frequently, patients experience non-allergic adverse effects such as vasovagal syncope, characterised by hypotension and bradycardia;5 sympathetic stimulation, presenting with palpitations, tremor, and flushing, often triggered by pain, procedural stress, endogenous catecholamine release, or exogenous adrenaline;6 and psychomotor agitation, associated with anxiety or heightened emotional arousal.7 Although these reactions are benign and self-limiting, they can mimic allergic responses and contribute to diagnostic confusion.5,6,7 True immunoglobulin E (IgE)-mediated hypersensitivity, by contrast, is exceedingly rare, accounting for less than 1% of reported LA adverse reactions.3
Although adverse reactions to LAs are relatively common, the majority are non-allergic in nature.6 A recently published paper, with data from a National Pharmacovigilance Registry, documented that LAs were implicated in 20% of all cases of drug-induced anaphylaxis.8 However, other sources have claimed that the rate of adverse-effects from LAs is roughly 0.1–1%, and of these, only 1% are due to true allergy.3,4 Furthermore, a Danish study of 162 patients with suspected amide-type LA allergy failed to demonstrate an IgE-mediated reaction in a single person,9 calling into question whether true allergy to the amide LAs even exist. This ambiguity in the cause-effect relationship combined with studies indicating a lack of confidence among dentists in diagnosing anaphylaxis10 can lead to mislabelling of patients as LA allergic. Carrying the label of LA allergy can cause anxiety and delayed treatment.
Aims
The aim of this study was to review patients referred to the Department of Immunology at St. James' Hospital, Dublin, Ireland, with suspected LA allergy, to determine the true prevalence of LA allergy and to describe the main characteristics of adverse drug reactions (ADRs) following LA application. Additionally, the study aimed to identify whether an alternate explanation for each patient's reaction was evident.
Methods
This retrospective, observational study included all patients referred to the Department of Immunology at St. James's Hospital, Dublin, Ireland, for evaluation of suspected LA allergy between December 2021 and June 2024.
All patients were admitted to the immunology day ward, where a clinical history was recorded and written informed consent was obtained before testing. Reactions were categorised based on clinical presentation: IgE-mediated immediate hypersensitivity, T cell-mediated delayed hypersensitivity, vasovagal syncope, sympathetic stimulation, systemic toxicity, or procedural trauma. Definitions were applied as follows:
-
Immediate hypersensitivity – onset within one hour of exposure, including urticaria, angioedema, respiratory or cardiovascular symptoms
-
Delayed hypersensitivity – onset more than one hour after exposure, typically presenting as allergic contact dermatitis or localised swelling
-
Sympathetic stimulation – tachycardia, hypertension, or palpitations
-
Vasovagal syncope – bradycardia, hypotension, pallor, and syncope
-
Systemic toxicity – numbness, tingling, or convulsions
-
Procedural trauma – localised swelling or pain directly attributable to the injection site.
Patients discontinued antihistamines and corticosteroids one week before testing. Skin testing was performed using both the suspected LA agent and a standardised panel consisting of the agents listed in Table 1.
Skin prick testing (SPT) was performed using undiluted solutions of each LA, with histamine (10 mg/mL) as the positive control and 0.9% sodium chloride as the negative control. A test was considered positive if a wheal ≥3 mm larger than the negative control developed within 15 minutes (Fig. 1).
Post-skin prick testing. Positive control (P) demonstrates a wheal >3 mm. The rest of tested agents are negative (Li = lignocaine, B = bupivacaine, Le = levobupivacaine, M = mepivacaine, La = latex, Chl = chlorhexidine)
If SPT was negative, intradermal testing was conducted using a 1/10 dilution of the LA. A result was considered positive if the wheal size increased by ≥3 mm from the initial bleb after 20 minutes (Fig. 2). Testing was conducted in accordance with guidelines from the British Society for Allergy and Clinical Immunology and the European Academy of Allergy and Clinical Immunology.
Post-intradermal testing. None of the tested agents demonstrate a positive result
Patients with negative skin testing underwent subcutaneous drug provocation testing (DPT) using a 1 mL therapeutic dose of the index LA injected into the lateral upper arm. Vital signs were monitored for one hour post-administration. DPT was considered negative if no objective symptoms were observed during the observation period.
Skin testing was also performed for co-administered agents when relevant. These included polyethylene glycol (PEG), polysorbate 80, chlorhexidine, latex, and corticosteroids.
Results
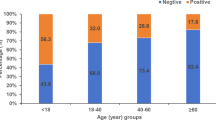
The included patient characteristics are summarised in Table 2. The total number of patients included in the study was 37. The mean age was 50.5 years (range 19–85 years). The female-to-male ratio was 3.1:1. The number of patients with a history of atopy was 11 (29.7%). The number of patients who reported other drug adverse reactions was 20 (54%), summarised in Table 3. The number of patients who had been referred following a reaction during a dental procedure was 24 (64.8%), in-hospital procedure was 11 (29.7%) and general practice was two (5.4%). The type of reaction and number of patients in each group are summarised in Table 4. The time between administration of the LA agent and onset of symptoms is summarised in Table 5. Most patients (31 out of 37) experienced symptoms within the first hour following LA administration. The LA agents that were implicated at the time of referral are summarised in Table 6. Whether or not the included patients required treatment at the time of the ADR and the type of treatment administered are summarised in Table 7. Results of SPT are summarised in Table 8: no patient (0%) involved in the study had a positive SPT or intradermal testing to any LA. A total of 36 patients (97.2%) had a negative DPT. One patient (2.7%) declined the challenge.
We identified four patients (10.8%) who were found to have positive SPT to a medication or antiseptic that was co-administered at the same time as the LA. Additionally, one patient (2.7%) had a history consistent with anaphylaxis secondary to ibuprofen administration post-procedure but this was not formally tested for.
Discussion
This study reinforces the rarity of true IgE-mediated hypersensitivity to LAs. Among the 37 patients referred to our tertiary allergy service with suspected LA allergy between December 2021 and June 2024, none were found to have a confirmed IgE-mediated reaction on formal testing. A significant proportion of patients (25/37; 67.6%) experienced symptoms consistent with non-IgE-mediated mechanisms, including vasovagal syncope, sympathetic stimulation (such as palpitations and tachycardia), systemic toxic effects, psychomotor response (e.g., perioral tingling, dizziness), and procedural trauma. These presentations often lacked objective allergic features and were self-limited in nature. Nevertheless, they frequently resulted in emergency intervention and all received specialist referral, particularly when the cardiovascular or neurologic symptoms were interpreted as early anaphylaxis.
Even among the seven patients (18.9%) whose symptoms initially suggested IgE-mediated hypersensitivity, alternative diagnoses were established following detailed workup. Four patients (10.8%) had positive skin testing to substances co-administered with the LA, specifically, PEG, polysorbate 80, and chlorhexidine. Two patients (5.4%) were diagnosed with chronic spontaneous urticaria, and one additional case was highly suggestive of anaphylaxis related to ibuprofen administered post-procedure, though formal testing was not performed. These findings underscore the importance of testing all agents administered during the reaction episode, not just the LA, as failure to do so risks misattributing causality.11 Diagnosis was excluded using a combination of detailed clinical history, negative skin testing, and negative DPT in 36 of 37 patients (97.3%), with one patient declining challenge.
A notable feature of our cohort was the high proportion of referrals originating from dental practice (64.8%; 24/37). This likely reflects the increased use of LAs in dental procedures, where they are a mainstay in both routine and surgical care. In addition, LA use in dentistry is more complex than in many other settings. Injections are frequently delivered into highly vascular oral tissues, and adrenaline-containing formulations are often used to prolong anaesthesia and control bleeding. These factors increase the risk of rapid systemic absorption or inadvertent intravascular administration, leading to acute symptoms such as palpitations, flushing, tremor, or dizziness.1 Although these effects are pharmacological and typically self-limiting, they may be mistaken for early signs of anaphylaxis in the moment, especially in time-pressured clinical environments. This misinterpretation can result in emergency management, labelling of allergy, unnecessary avoidance, and referral for specialist assessment, even in the absence of objective allergic features.
None of the patients referred in this cohort had serum tryptase measured at the time of their reaction, despite several being treated for suspected anaphylaxis. Although serum tryptase is not diagnostic on its own and a normal level does not exclude anaphylaxis, a post-event elevation can support the diagnosis when interpreted alongside clinical features and timing.12 Its absence represents a missed opportunity to strengthen diagnostic certainty, particularly when patients undergo escalation of care such as adrenaline administration. Wider awareness and accessibility of tryptase testing in dental and general practice settings may help reduce misclassification in future cases.
A total of 17 patients (45.9%) in our study recovered from their adverse reaction without receiving any treatment, suggesting that a substantial proportion of suspected allergic reactions are in fact transient, non-allergic events that resolve spontaneously. These cases reinforce the need for careful consideration of acute management, particularly when there are no objective signs of systemic involvement. Conversely, adrenaline was administered in five patients (13.5%), sometimes in repeated doses, despite the lack of confirmatory evidence of anaphylaxis. While adrenaline is the mainstay of anaphylaxis treatment, the absence of clinical improvement following appropriate dosing should prompt reconsideration of the working diagnosis.13 Vasovagal syncope, anxiety, and sympathomimetic side effects from adrenaline itself may explain persistent symptoms in such cases. Escalating treatment without reassessment risks reinforcing misdiagnosis, potentially leading to long-term avoidance of safe and effective medications.14
Demographically, our patient cohort had a female predominance (3.1:1) and a mean age of 50.5 years (range 19–85). A total of 11 patients (29.7%) reported a history of atopy, and 20 patients (54.0%) reported previous adverse reactions to other drug classes, including antibiotics, non-steroidal anti-inflammatory drugs, opioids, general anaesthetics, and radiocontrast agents. However, these historical features were not associated with an increased likelihood of confirmed LA allergy in our analysis. In fact, the tendency to accumulate multiple suspected drug allergies may reflect heightened symptom vigilance or past misinterpretations, reinforcing the value of formal allergy assessment before applying long-term diagnostic labels.15
These findings have important implications for daily clinical practice, particularly in dentistry and minor surgical specialties where LAs are frequently used. Dentists and general practitioners should be aware that most acute reactions to LAs are not true allergies, and in the absence of clear signs such as urticaria, angioedema, bronchospasm, or hypotension, the likelihood of anaphylaxis is low.16 Improved understanding of the pharmacological effects of adrenaline and the expected physiological responses following local injection can help clinicians better assess these events in real time. Strengthening this clinical awareness is key to avoiding misdiagnosis, inappropriate treatment, and unnecessary avoidance.17
In the event of acute symptoms following LA administration in a private or outpatient setting, clinicians should assess the clinical context thoroughly before assuming an allergic cause. Key features that support an allergic diagnosis include sudden-onset skin involvement, respiratory compromise, or cardiovascular instability. If anaphylaxis is strongly suspected, intramuscular adrenaline should be administered promptly, and emergency services contacted. However, in milder or ambiguous cases, supportive care, patient reassurance, and careful monitoring may be more appropriate.18 Clinicians should also document the reaction in detail and consider timely referral for allergy testing where uncertainty persists.19,20
To reduce unnecessary referrals, dental professionals should be trained to distinguish between pharmacological side effects and true allergic reactions. Taking a detailed history at the time of the event, including timing, symptoms, drugs administered, and response to treatment, can help stratify risk. Recording the specific LA product, along with any co-administered substances (e.g., chlorhexidine, topical anaesthetics), is essential. When in doubt, non-urgent referral to an allergy clinic is preferred over avoidance without evaluation, as structured testing is the only reliable way to confirm or exclude LA allergy.11
Access to allergy services remains limited in many regions. This systemic limitation contributes to delays in definitive diagnosis and extended uncertainty for both patients and clinicians. Expanding clinician education, particularly in dentistry and primary care, may help reduce unnecessary referrals and unwarranted LA avoidance, while improving patient safety and resource use.
Our findings are reinforced by recent international literature confirming the rarity of true IgE-mediated LA allergy. A national Danish study by Kvisselgaard et al. (2017) evaluated 162 patients referred for suspected LA allergy over a 10-year period and found no confirmed cases of IgE-mediated hypersensitivity.9 Similarly, the UK-based DALES study (Thomas et al., 2021), a prospective multicentre review of over 5,000 elective surgery patients, reported that 86% of recorded drug allergy labels, including many related to anaesthetics, were incorrect.11 From France, Hascoët et al. (2022) retrospectively reviewed LA-related reactions in dental procedures and identified only nine confirmed cases of anaphylaxis among tens of thousands of procedures, estimating an incidence below 0.01%.21 These large-scale, geographically diverse studies align closely with our own findings and emphasise the importance of structured diagnostic evaluation in reducing misdiagnosis, unnecessary avoidance, and unwarranted referral.
Our study has several limitations. It was retrospective and conducted at a single tertiary allergy centre, which may limit generalisability to broader clinical contexts. The relatively small sample size (n = 37) reduces statistical power and increases sensitivity to selection bias. As a specialist centre, our patient population is likely enriched for complex or ambiguous presentations, potentially skewing referral patterns and diagnostic yield. Tryptase testing was not performed at the time of reaction in any patient, limiting our ability to corroborate or refute mast cell activation in cases managed as anaphylaxis. Additionally, while many alternative diagnoses were identified with high clinical confidence, objective confirmation (e.g., via challenge testing for co-administered drugs) was not always feasible. Regional differences in LA formulations, administration practices, and access to dental anaesthesia protocols may also affect generalisability.
Conclusion
In conclusion, this study supports the growing evidence that true IgE-mediated allergy to LAs is exceptionally rare. Most adverse reactions labelled as LA allergy are due to non-allergic mechanisms, alternative agents, or benign, transient responses. The predominance of dental referrals may reflect the particular procedural and pharmacologic characteristics of that setting. Improving clinician education, diagnostic confidence, and access to allergy services will be essential in preventing misdiagnosis, reducing unnecessary avoidance of effective medications, and ensuring optimal patient outcomes.
Data availability
Due to GDPR restrictions, the supporting data for this study are not publicly available.
References
El-Boghdadly K, Pawa A, Chin K J. Local anesthetic systemic toxicity: current perspectives. Local Reg Anesth 2018; 11: 35–44.
Henderson S. Allergy to local anaesthetic agents used in dentistry – what are the signs, symptoms, alternative diagnoses and management options? Dent Update 2011; 38: 410–412.
Kvisselgaard A D, Krøigaard M, Mosbech H F, Garvey L H. No cases of perioperative allergy to local anaesthetics in the Danish Anaesthesia Allergy Centre. Acta Anaesthesiol Scand 2017; 61: 149–155.
Harboe T, Guttormsen A B, Aarebrot S, Dybendal T, Irgens A, Florvaag E. Suspected allergy to local anaesthetics: follow-up in 135 cases. Acta Anaesthesiol Scand 2010; 54: 536–542.
Hutse I, Coppens M, Herbelet S, Seyssens L, Marks L. Syncope in dental practices: a systematic review on aetiology and management. J Evid Based Dent Pract 2021; 21: 101581.
Jiang S, Tang M. Allergy to local anesthetics is a rarity: review of diagnostics and strategies for clinical management. Clin Rev Allergy Immunol 2023; 64: 193–205.
Klein S M, Benveniste H. Anxiety, vocalization, and agitation following peripheral nerve block with ropivacaine. Reg Anesth Pain Med 1999; 24: 175–178.
Butranova O, Zyryanov S, Gorbacheva A, Asetskaya I, Polivanov V. Drug-induced anaphylaxis: national database analysis. Pharmaceuticals 2024; 17: 90.
Kvisselgaard A D, Mosbech H F, Fransson S, Garvey L H. Risk of immediate-type allergy to local anesthetics is overestimated-results from 5 years of provocation testing in a Danish allergy clinic. J Allergy Clin Immunol Pract 2018; 6: 1217–1223.
Cherrez-Ojeda I, Gallardo-Bastidas J C, Borrero G R et al. Knowledge and attitudes toward anaphylaxis to local anesthetics in dental practice. BDJ Open 2024; 10: 28.
Thomas C, Clark S, Fallaha D et al. DALES, Drug Allergy Labels in Elective Surgical patients: a prospective, multicentre cross-sectional study of prevalence, nature and anaesthetists' approach to management. Br J Anaesth 2021; 127: 897–904.
Harper N J N, Dixon T, Dugué P et al. Suspected anaphylactic reactions associated with anaesthesia. Anaesthesia 2009; 64: 199–211.
Resuscitation Council UK. Emergency Treatment of Anaphylaxis: Guidelines for Healthcare Providers. 2021. Available at https://www.resus.org.uk/sites/default/files/2021-05/Emergency%20Treatment%20of%20Anaphylaxis%20May%202021_0.pdf (accessed 9 November 2025).
Jefferson A A, Khan D A, Shaker M S. The penicillin allergy label: expensive to maintain, inexpensive to remove. J Allergy Clin Immunol Pract 2018; 6: 1028–1029.
Chiang V, Kan A K C, Saha C, Au E Y L, Li P H. Identifying the most at-risk age-group and longitudinal trends of drug allergy labeling amongst 7.3 million individuals in Hong Kong. BMC Med 2024; 22: 30.
Shaker M S, Wallace D V, Golden D B K et al. Anaphylaxis – a 2020 practice parameter update, systematic review, and Grading of Recommendations, Assessment, Development and Evaluation (GRADE) analysis. J Allergy Clin Immunol 2020; 145: 1082–1123.
Lin Y-Y, Chang H-A, Kao Y-H et al. Investigation of the underuse of adrenaline (epinephrine) and prognosis among patients with anaphylaxis at emergency department admission. Front Med 2023; 10: 1163817.
Muraro A, Worm M, Alviani C et al. EAACI guidelines: anaphylaxis (2021 update). Allergy 2022; 77: 357–377. DOI: 10.1111/all.15032.
Berkun Y, Ben-Zvi A, Levy Y, Galili D, Shalit M. Evaluation of adverse reactions to local anesthetics: experience with 236 patients. Ann Allergy Asthma Immunol 2003; 91: 342–345.
Garvey L H, Melchiors B B, Ebo D G, Mertes P-M, Krøigaard M. Medical algorithms: Diagnosis and investigation of perioperative immediate hypersensitivity reactions. Allergy 2020; 75: 2139–2142.
Hascoët E, Mahé J, Meillard H, Théophile H, Cloitre A, Lesclous P. Anaphylactic reactions to local anesthetics in dental practice: a nationwide French retrospective study. Clin Oral Investig 2022; 26: 1667–1676.
Funding
University of Dublin, Trinity College Open Access funding provided by the IReL Consortium.
Author information
Authors and Affiliations
Contributions
DM: reviewed all the drug allergy testing data and collated the local anaesthetic allergy testing data; submitted the research ethics committee proposal and obtained approval from the committee; analysed the data and created the tables; wrote the first draft of the manuscript. NC: reviewed manuscript for factual correctness from an immunology perspective and provided advice on the publishing process. DP: reviewed the manuscript for factual correctness from a dentistry/maxillofacial surgery perspective. SA: had the initial idea to perform the study; performed the drug allergy testing on the immunology day ward; reviewed manuscript and provided detailed edits; wrote the discussion section in its entirety.
Corresponding author
Ethics declarations
The authors declare no conflicts of interest. Ethical approval was not required for this study, as it was classified as a clinical audit by the Research and Innovation Office at St. James's Hospital and therefore exempt from the formal ethical approval process. Consent was not required for retrospective data collection.
Rights and permissions
Open Access. This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0.© The Author(s) 2025.
About this article
Cite this article
Mannion, D., Conlon, N., Pierse, D. et al. Are we numb to the facts? Our experience of local anaesthetic allergy testing in a tertiary hospital immunology department. Br Dent J (2025). https://doi.org/10.1038/s41415-025-8921-y
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41415-025-8921-y