Abstract
Background
Chronic inflammation and inflammatory-related exposures have been implicated in epithelial ovarian cancer (EOC) prognosis. However, no studies have evaluated whether analgesic medication use impacts survival in Black women with EOC, an understudied population with poor survival.
Methods
Leveraging data from the African American Cancer Epidemiology Study, we examined the association of pre-diagnostic analgesic medication use (aspirin, non-aspirin non-steroidal anti-inflammatory drugs [naNSAIDs], and acetaminophen) with survival among self-identified Black women diagnosed with EOC (N = 541) using multivariable Cox proportional hazards regression. Stratified analyses were conducted by comorbidities and histotype.
Results
Acetaminophen use was associated with a higher risk of mortality overall (HR = 1.40; 95% CI = 1.00–1.97) and for frequent and chronic use (≥30 days per month: HR = 1.62; 95% CI = 1.12–2.34; >5 years: HR = 1.57; 95% CI = 1.03–2.39). These associations were more pronounced among women with high-grade serous carcinoma (HGSC)/carcinosarcoma and those with comorbidities. Among women with comorbidities, naNSAID use was associated with a decreased risk of mortality (HR = 0.71; 95% CI = 0.51–0.99), but no association was observed among women without comorbidities (HR = 0.99; 95% CI = 0.56–1.75). No associations with survival were observed for aspirin.
Conclusion
Chronic use of acetaminophen negatively impacted survival among Black women with EOC, while naNSAID use conferred a survival advantage only among women with comorbidities.
Similar content being viewed by others

Introduction
Some analgesic medications, or pain relievers, represent potential approaches for cancer prevention or improving cancer outcomes due to their anti-inflammatory properties. The two most commonly used non-prescription analgesic medications are acetaminophen and non-steroidal anti-inflammatory drugs (NSAIDs). Acetaminophen has weak anti-inflammatory activity and primarily relieves pain by blocking pain signals in the central nervous system [1, 2], whereas NSAIDs relieve pain by reducing inflammation through the inhibition of cyclooxygenase enzymes and subsequent decreases in prostaglandin production [3]. Aspirin is a type of NSAID that exhibits anti-thrombotic properties in addition to its anti-inflammatory effects, resulting in its use as both an analgesic medication and in the prevention of cardiovascular disease [4]. However, adverse effects can occur with chronic use of these medications, namely gastrointestinal bleeding for NSAIDs and liver damage for acetaminophen [5, 6].
Epithelial ovarian cancer (EOC) is one of the deadliest gynaecologic malignancies in the U.S., with a 5-year survival rate of only 51% [7]. Chronic inflammation has been shown to impact the prognosis of EOC as evidenced by associations of inflammatory-related exposures (e.g. obesity, pro-inflammatory diet, physical inactivity, cigarette smoking) and circulating biomarkers with survival [8,9,10,11,12]. Several studies have investigated the association of analgesic medication use with survival in EOC, but findings have been equivocal for NSAIDs. Most studies [13,14,15,16,17,18] either find no association with mortality for NSAIDs, including aspirin, or a weak inverse association depending on exposure classification and timing of exposure relative to cancer diagnosis. For example, Merritt et al. [18] showed that post-diagnosis rather than pre-diagnosis regular use of aspirin and non-aspirin NSAIDs (naNSAIDs) was associated with better EOC-specific survival in the Nurses’ Health Studies [18]. For acetaminophen, most studies show no association with survival for both pre- and post-diagnostic use [13, 15, 18,19,20].
Prior evidence on the association of analgesic medications and survival in EOC is from populations of predominantly White women. Black women with EOC experience lower survival rates compared to White women [7]. Yet, Black women are often underrepresented in ovarian cancer research, and to date, no studies have examined the role of analgesic medications in outcomes of Black women diagnosed with EOC. The present study investigates the relationship between pre-diagnostic, non-prescription analgesic medication use and survival among Black women with EOC.
Methods
Study population
We utilised data from the African American Cancer Epidemiology Study (AACES) [21], a population-based study of Black or African American women diagnosed with EOC. Study participants were identified through rapid case ascertainment at SEER or state cancer registries, gynaecologic oncology departments and hospitals. Eligible participants self-identified as Black or African American, were aged 20–79 years, were diagnosed with invasive EOC between December 2010 and December 2015, and resided in 11 geographic regions across the U.S.: Alabama, Georgia, Illinois, Louisiana, Michigan [Detroit], New Jersey, North Carolina, Ohio, South Carolina, Tennessee and Texas. A baseline telephone interview was completed to obtain information on demographics, reproductive history, medication use and lifestyle activities (e.g. smoking, physical activity). A shortened questionnaire was available for women who might otherwise have refused. Institutional Review Board approval was obtained at each site, and informed consent was obtained from all participants.
Analgesic medication use
Participants were asked to recall any pain or inflammation medications they had taken regularly (at least once a week or at least 5 days per month) at any point in their lives. To aid in recollection, examples of these medications and their uses were provided. Participants who reported ever using such medications were asked to report the medication name, reason for use, age at first and last use and frequency and duration of use. This process was repeated for each medication used. The medications were then categorised into three groups: aspirin, naNSAIDs and acetaminophen. Combination medications (e.g. Excedrin includes aspirin and acetaminophen) were categorised as both medication types. To determine pre-diagnostic medication use, we categorised women who initiated analgesic medication use within the year before diagnosis or any time after diagnosis as non-users. We also considered women who reported a duration of use less than 6 months as non-users in order to capture the regular users of these medications. Since the short version of the questionnaire did not enquire about analgesic medication use, we only included participants who completed the long version of the questionnaire. Post-diagnostic analgesic medication use was not systematically collected in AACES and was not examined in this analysis.
Statistical analysis
Participant characteristics were summarised using descriptive statistics and compared by analgesic medication use using the Wilcoxon rank sum or chi-square tests. Vital status was determined using data from the National Death Index, cancer registries, the LexisNexis database and patient contact. Follow-up time was calculated as the time from the interview to death or the date of last contact. Multivariable Cox proportional hazard (PH) models were used to estimate hazard ratios (HR) and 95% confidence intervals (CI) for the association of analgesic medication use (ever, frequency [<30 and ≥30 days/month], and duration [≤5 years, >5 years]) with risk of all-cause mortality. The categories for frequency and duration of use were determined by prior literature and data distribution. Several potential confounders were considered in multivariable models, including age (continuous, years), geographic region (North [Illinois, Michigan, New Jersey and Ohio], Southeast [Georgia, North Carolina, South Carolina and Tennessee], and Southwest [Alabama, Texas, Louisiana]), stage (I, II, III and IV), histotype (high-grade serous carcinoma [HGSC]/carcinosarcoma, not HGSC/carcinosarcoma), smoking status (ever, never), physical activity (met vs. did not meet Physical Activity Guidelines for Americans [22]), body mass index ([BMI]; continuous, kg/m2), Charlson comorbidity index [23] ([CCI]; 0, ≥1), education (high school graduate/GED or less, some college or college graduate), income (<$25,000, $25,000 to $74,999, ≥$75,000), insurance (any private insurance, any Medicaid and any Medicare as three separate variables) and debulking status (optimal, suboptimal). Of these, smoking status, physical activity, education and income did not appreciably change the results and were not included in the final models. Additionally, the use of each analgesic medication was included in the models to determine the independent effect of each analgesic medication, adjusting for the use of the others. Adjusted Kaplan-Meier curves were generated using the ggadjustedcurves() function in the survminer R package. The PH assumption was tested by evaluating Schoenfeld residuals and time x covariate interactions individually and collectively across all covariates. Histotype violated the PH assumption (p < 0.05) and was included as a strata term in the models. Stratified analyses were performed by histotype and the CCI (0 vs. ≥1).
Due to missing data on key covariates included in the models (ranging from 0.3% for insurance and 34% for debulking status), we imputed missing data using the multiple imputation by chained equations (‘mice’) R package. A Cox PH model was estimated, including the analgesic medications and all potential confounders described above, as well as the Nelson–Aalen estimate of the cumulative hazard [24]. The fraction of missing information was used to set the number of imputations (n = 39). The imputed and observed distributions of variables with missing data were comparable (Supplementary Table 1). As a sensitivity analysis, the primary analyses were repeated, restricting to participants with complete data.
Results
A total of 541 Black women enrolled in AACES completed the long version of the baseline questionnaire. The median age at diagnosis was 57 years, and most women were diagnosed with late-stage disease (66%) and HGSC/carcinosarcoma (71%; Table 1). The prevalence of medication use was highest for naNSAIDs (22%), followed by aspirin (17%) and acetaminophen (11%). Among analgesic users, most exhibited daily use, as indicated by a frequency of ≥30 days per month (82% for aspirin, 77% for naNSAIDs, 82% for acetaminophen), and used analgesics for >5 years (55% for aspirin, 58% naNSAIDs, 65% acetaminophen). While aspirin and naNSAID users were less likely to report concurrent use of other analgesic medications, more than half of acetaminophen users also used the other types of analgesic medications (Supplementary Fig. 1). Only eight women reported using all three types of analgesic medications. For each analgesic medication, ever users had a higher BMI and CCI compared with never users (Supplementary Table 2). Additionally, ever users of aspirin were older and more likely to be diagnosed with HGSC/carcinosarcoma and have Medicare insurance compared with never users. A higher proportion of naNSAID users were diagnosed with earlier-stage disease, and fewer had HGSC/carcinosarcoma and Medicaid insurance.
During a median follow-up of 4.3 years (range, 0.1–12.2 years), 354 deaths (65%) occurred. For both aspirin and naNSAIDs, an inverse but imprecise association was observed with survival (Table 2, Fig. 1), which persisted when examining frequency and duration of use. A higher risk of mortality was observed with ever use of acetaminophen (HR = 1.40; 95% CI = 1.00–1.97), which was driven by more frequent or daily users (≥30 days per month, HR = 1.62; 95% CI = 1.12–2.34) and a longer duration of use (>5 years, HR = 1.57; 95% CI = 1.03–2.39). Our findings remained consistent in the complete case analysis (Supplementary Table 3).
Adjusted Kaplan-Meier survival curves for the association of ever use of a aspirin, b non-aspirin NSAIDs and c acetaminophen with risk of all-cause mortality. Models were adjusted for the other analgesic medications, age, study site, stage, CCI, BMI, insurance and debulking status, and histotype was included as a strata term due to violations of proportional hazards. NSAID non-steroidal anti-inflammatory drug, CCI Charlson Comorbidity Index, BMI body mass index.
Table 2 and Fig. 2 provide the survival associations by histotype and the CCI. When stratifying by histotype, we observed that the increased risk of mortality for acetaminophen use was present specifically among women with HGSC/carcinosarcoma (HR = 1.66; 95% CI = 1.12–2.44), while an elevated risk of mortality was observed for acetaminophen use among women with non-HGSC/carcinosarcoma, although CIs were wide (HR = 1.29; 95% CI = 0.56–2.99). Likewise, a higher risk of mortality for a higher frequency and a longer duration of acetaminophen use was present among HGSC/carcinosarcoma. However, small sample sizes of non-HGSC/carcinosarcoma resulted in imprecise estimates for acetaminophen duration analyses and precluded the investigation of frequency of use. No appreciable differences in the associations of aspirin and naNSAIDs with survival were observed by histotype.
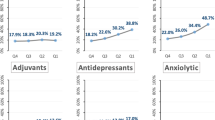
Hazard ratios and 95% confidence intervals for the association of analgesic medication use with risk of all-cause mortality stratified by a histotype (HGSC/carcinosarcoma vs. non-HGSC/carcinosarcoma) and b CCI (CCI of 0 vs. CCI ≥ 1). The histotype models were adjusted for the other analgesic medications, age, study site, stage, CCI, BMI, insurance and debulking status. The CCI models were adjusted for the other analgesic medications, age, study site, stage, BMI, insurance and debulking status, and histotype was included as a strata term due to violations of proportional hazards. HGSC high-grade serous carcinoma, CCI Charlson comorbidity index, BMI body mass index, NSAID non-steroidal anti-inflammatory drug.
Stratifying by the CCI showed that analgesic medication use was not associated with survival among women without comorbidities (CCI = 0). Among women with comorbidities (CCI ≥ 1), we observed an increased risk of mortality for acetaminophen use (HR = 1.46; 95% CI = 0.97–2.19) and a decreased risk of mortality for naNSAID use (HR = 0.71; 95% CI = 0.51–0.99). These associations were pronounced in magnitude for more frequent use (acetaminophen: HR = 1.69; 95% CI = 1.09–2.61 and naNSAIDS: HR = 0.67; 95% CI = 0.46–0.97, respectively) and longer durations of use (acetaminophen: HR = 1.54; 95% CI = 0.94–2.51 and naNSAIDs: HR = 0.61; 95% CI = 0.40–0.93, respectively). No associations were observed for aspirin use and survival by CCI.
Discussion
In a cohort of Black women diagnosed with EOC, we observed a higher risk of mortality for pre-diagnostic acetaminophen use, particularly those reporting daily use and/or 5 years or more of use. These associations occurred primarily among women with HGSC/carcinosarcoma and those with comorbid conditions. We also observed a lower risk of mortality for naNSAID use overall, although estimates were imprecise, and among women with comorbid conditions. However, no associations with survival were observed for aspirin use.
Despite observing worse survival for acetaminophen use in the present study, most existing research suggests that pre-diagnostic acetaminophen use is not associated with ovarian cancer survival [13,14,15, 18, 20]. The conflicting findings between our study and prior literature may be due to inherent differences in the attributes of the study populations. Our cohort is comprised of Black women with EOC residing in the U.S., while prior studies included populations of mostly White women with EOC residing in the U.S. or Australia[13,14,15, 18, 20]. We also found that acetaminophen users in the present study were more likely to report taking acetaminophen at a high frequency and for long durations compared with acetaminophen users in prior literature. Women who used acetaminophen daily or for more than 5 years prior to diagnosis had the highest risk of mortality in our study, suggesting that the association of pre-diagnostic acetaminophen use with survival was largely driven by more frequent or chronic use. These findings may be attributed to the way acetaminophen is processed and its long-term physiologic effects. Acetaminophen is primarily metabolised in the liver by forming conjugates with glucuronide and sulphate, but up to 10% is oxidised to form a reactive toxic intermediate, N-acetyl-p-benzoquinone imine (NAPQI) [25, 26]. Chronic acetaminophen use can lead to an increased production of NAPQI, causing oxidative stress and damage to liver cells, potentially leading to liver dysfunction or failure [25, 26]. These effects may differ by race, as studies have shown that while Black/African populations have a greater clearance of acetaminophen compared to White populations [27], Black/African individuals metabolise acetaminophen by oxidation at a slower rate [28, 29]. However, more work is needed to better understand acetaminophen pharmacokinetics in diverse populations. Additionally, chemotherapy dose adjustments may be applied to prevent further toxicity for patients with liver dysfunction [30], and in ovarian cancer, impaired liver function was associated with chemotherapy dose modifications, treatment discontinuation and worse overall survival [31]. Besides liver impacts, acetaminophen and its metabolites are excreted through the urine, and long-term use can strain the kidneys, resulting in renal impairment or failure [5]. Long-term acetaminophen use has also been linked to hypertension and can induce oxidative stress and inflammation, contributing to endothelial dysfunction and atherosclerosis [5]. Additional work is needed to elucidate the biologic pathways underlying the increased risk of mortality associated with chronic acetaminophen use.
We observed inverse associations between pre-diagnostic aspirin and naNSAID use and survival overall, although CIs were wide and imprecise. These findings are similar to most prior studies considering pre-diagnostic use of aspirin or naNSAIDs [13,14,15,16,17,18]. One study showed that frequent (≥4 days per week) pre-diagnostic NSAID use was associated with better survival in a cohort of Australian women with ovarian cancer [20]. However, comparing findings across studies is challenging due to the lack of standard medication use questionnaires and varying definitions of regular use. For example, Dixon et al. [15] defined regular use as at least once a week, while Merritt et al. [18] defined regular use as ≥2 days per week. Nevertheless, studies consistently show that post-diagnostic NSAID use may be a key factor in ovarian cancer outcomes. In the study of Australian women with ovarian cancer and in the Nurses’ Health Studies [18, 20], post-diagnostic use of naNSAIDs and aspirin was associated with better survival. The present study was unable to reliably assess post-diagnostic use of analgesic medications, but this is likely to be a fruitful avenue for future research.
For both acetaminophen and naNSAIDs, heterogeneity was observed in the survival associations by comorbidities. Among women with comorbidities, we found a higher risk of mortality for acetaminophen use but a lower risk of mortality for naNSAIDs. Conversely, analgesic medication use was not associated with survival among women without comorbidities. These findings may be due to differences in patterns of analgesic medication use by comorbidity status. In our study population, women with comorbidities were more likely to report analgesic medication use as well as a longer duration of use than women without comorbidities. Additionally, women with comorbidities may use certain types of analgesic medications more than others due to potential contraindications [32]. For example, individuals with gastrointestinal diseases are advised to use acetaminophen due to the known risks of gastrointestinal bleeding with continued NSAID use. Drug interactions can also occur between analgesics and medications taken for comorbid conditions, resulting in side effects that could have downstream impacts on morbidity and mortality among women with comorbidities (e.g. concurrent anticoagulant or antidepressant use with NSAIDs increases risk of gastrointestinal bleeding, concurrent use of antidiabetic agents and aspirin increases risk of hypoglycemic effects) [33]. Lastly, our findings may be compounded by the higher prevalence of some comorbidities that are indications for analgesic medications among Black individuals compared to White individuals (e.g. cardiovascular disease) [34].
The histotype stratified analyses did not provide clear evidence to suggest there was heterogeneity in the survival associations by histotype. We observed that the higher risk of mortality for acetaminophen use was present specifically among women with HGSC/carcinosarcoma, with an attenuated association observed among women with non-HGSC/carcinosarcoma, although CIs were wide. The rarity of non-HGSC/carcinosarcoma precluded our ability to investigate frequency of use, limited our power to detect associations for duration of use, and did not allow for stratified analyses within each individual histotype (e.g. endometrioid, clear cell). Thus, these findings should be interpreted with caution and would benefit from further investigation in a larger cohort.
The present study possesses several notable strengths. It is the only study to exclusively focus on analgesic use and ovarian cancer survival among Black women, leveraging data from a well-established population-based study. The AACES features a relatively large cohort of Black women in the U.S. and includes detailed information on analgesic medication use, allowing for effect estimates based on frequency and duration of use, and the ability to adjust for relevant confounders. However, this work also has limitations. The data on analgesic medication use were obtained through self-report, which may be impacted by recall bias, particularly with respect to frequency and duration of use. Moreover, the variety of analgesic medications that could be used over the lifetime and for different indications poses additional recall challenges. Medication use collected from registers or medical records may be more accurate, particularly in the setting of prescription medications, but could suffer from exposure misclassification as over-the-counter medications are not always captured and information on medication compliance is typically unavailable. We were not able to investigate the effect of concurrent analgesic medication use and recency of use due to small stratum sample sizes or to evaluate medication dosing, as study participants did not consistently report this information. While several confounders were considered in our analyses, there is still a possibility of bias due to residual or unmeasured confounding. Although AACES included Black women from 11 sites in the U.S., our findings may not be generalisable to all Black women in the U.S., particularly in the Western region of the country, or other racial and ethnic groups. Additionally, despite having missing data on key covariates, we used multiple imputation and observed consistent findings when restricting analyses to participants with complete data. Lastly, we do not have data on recurrence or cause of death in the entire cohort, precluding examinations of progression-free or cause-specific survival.
In summary, we observed that chronic and frequent acetaminophen use negatively impacted survival among Black women with ovarian cancer, particularly among women with comorbidities, while overall and chronic naNSAID use was associated with better survival only among women with comorbidities. These findings provide valuable insights into potential factors affecting survival among Black women diagnosed with EOC, an understudied population in ovarian cancer research. The evidence base on this topic will be strengthened by investigating the impact of both pre- and post-diagnostic analgesic medication use on survival in larger, more diverse cohorts. Moreover, our lack of understanding of the mechanisms and pathways through which analgesic medications influence survival in cancer patients also warrants further investigation.
Data availability
Data from this study are available from the corresponding author on reasonable request and approval by the study investigators.
References
Ohashi N, Kohno T. Analgesic effect of acetaminophen: a review of known and novel mechanisms of action. Front Pharmacol. 2020;11:580289.
Jóźwiak-Bebenista M, Nowak JZ. Paracetamol: mechanism of action, applications and safety concern. Acta Pol Pharm. 2014;71:11–23.
Vane JR, Botting RM. Anti-inflammatory drugs and their mechanism of action. Inflamm Res. 1998;47:S78–87.
US Preventive Services Task Force. Aspirin use to prevent cardiovascular disease: US Preventive Services Task Force Recommendation Statement. JAMA. 2022;327:1577–84.
McCrae JC, Morrison EE, MacIntyre IM, Dear JW, Webb DJ. Long-term adverse effects of paracetamol—a review. Br J Clin Pharmacol. 2018;84:2218–30.
McEvoy L, Carr DF, Pirmohamed M. Pharmacogenomics of NSAID-induced upper gastrointestinal toxicity. Front Pharmacol. 2021;12:684162.
Siegel RL, Kratzer TB, Giaquinto AN, Sung H, Jemal A. Cancer Statistics, 2025. CA Cancer J Clin. 2025;75:10–45.
Savant SS, Sriramkumar S, O’Hagan HM. The role of inflammation and inflammatory mediators in the development, progression, metastasis, and chemoresistance of epithelial ovarian cancer. Cancers. 2018;10:251.
Brieger KK, Phung MT, Mukherjee B, Bakulski KM, Anton-Culver H, Bandera EV, et al. High prediagnosis inflammation-related risk score associated with decreased ovarian cancer survival. Cancer Epidemiol Biomark Prev. 2022;31:443–52.
Johnson CE, Alberg AJ, Bandera EV, Peres LC, Akonde M, Collin LJ, et al. Association of inflammation-related exposures and ovarian cancer survival in a multi-site cohort study of Black women. Br J Cancer. 2023;129:1119–25.
Minlikeeva AN, Cannioto R, Jensen A, Kjaer SK, Jordan SJ, Diergaarde B, et al. Joint exposure to smoking, excessive weight, and physical inactivity and survival of ovarian cancer patients, evidence from the Ovarian Cancer Association Consortium. Cancer Causes Control. 2019;30:537–47.
Peres LC, Hebert JR, Qin B, Guertin KA, Bandera EV, Shivappa N, et al. Prediagnostic proinflammatory dietary potential is associated with all-cause mortality among African-American women with high-grade serous ovarian carcinoma. J Nutr. 2019;149:1606–16.
Minlikeeva AN, Freudenheim JL, Lo-Ciganic W-H, Eng KH, Friel G, Diergaarde B, et al. Use of common analgesics is not associated with ovarian cancer survival. Cancer Epidemiol Biomark Prev. 2015;24:1291–4.
Nagle CM, Ibiebele TI, DeFazio A, Protani MM, Webb PM. Aspirin, nonaspirin nonsteroidal anti-inflammatory drugs, acetaminophen and ovarian cancer survival. Cancer Epidemiol. 2015;39:196–9.
Dixon SC, Nagle CM, Wentzensen N, Trabert B, Beeghly-Fadiel A, Schildkraut JM, et al. Use of common analgesic medications and ovarian cancer survival: results from a pooled analysis in the Ovarian Cancer Association Consortium. Br J Cancer. 2017;116:1223–8.
Verdoodt F, Kjaer SK, Dehlendorff C, Friis S. Aspirin use and ovarian cancer mortality in a Danish nationwide cohort study. Br J Cancer. 2018;118:611–5.
Majidi A, Na R, Dixon-Suen S, Jordan SJ, Webb PM. Common medications and survival in women with ovarian cancer: a systematic review and meta-analysis. Gynecol Oncol. 2020;157:678–85.
Merritt MA, Rice MS, Barnard ME, Hankinson SE, Matulonis UA, Poole EM, et al. Pre-diagnosis and post-diagnosis use of common analgesics and ovarian cancer prognosis (NHS/NHSII): a cohort study. Lancet Oncol. 2018;19:1107–16.
Peres LC, Camacho F, Abbott SE, Alberg AJ, Bandera EV, Barnholtz-Sloan J, et al. Analgesic medication use and risk of epithelial ovarian cancer in African American women. Br J Cancer. 2016;114:819–25.
Majidi A, Na R, Jordan SJ, DeFazio A, Obermair A, Friedlander M, et al. Common analgesics and ovarian cancer survival: the Ovarian Cancer Prognosis and Lifestyle (OPAL) Study. J Natl Cancer Inst. 2023;115:570–7.
Schildkraut JM, Alberg AJ, Bandera EV, Barnholtz-Sloan J, Bondy M, Cote ML, et al. A multi-center population-based case-control study of ovarian cancer in African-American women: the African American Cancer Epidemiology Study (AACES). BMC Cancer. 2014;14:688.
US Department of Health and Human Services. 2018 Physical Activity Guidelines Advisory Committee Scientific Report. (US Department of Health and Human Services, Washington D.C., U.S., 2018).
Chaudhry S, Jin L, Meltzer D. Use of a self-report-generated Charlson Comorbidity Index for predicting mortality. Med Care. 2005;43:607–15.
White IR, Royston P. Imputing missing covariate values for the Cox model. Stat Med. 2009;28:1982–98.
Yoon E, Babar A, Choudhary M, Kutner M, Pyrsopoulos N. Acetaminophen-Induced Hepatotoxicity: a Comprehensive Update. J Clin Transl Hepatol. 2016;4:131–42.
Mazaleuskaya LL, Sangkuhl K, Thorn CF, FitzGerald GA, Altman RB, Klein TE. PharmGKB summary: pathways of acetaminophen metabolism at the therapeutic versus toxic doses. Pharmacogenet Genom. 2015;25:416–26.
Sommers DK, van Staden DA, Moncrieff J, Schoeman HS. Paracetamol metabolism in African villagers. Hum Toxicol. 1985;4:385–9.
Court MH, Zhu Z, Masse G, Duan SX, James LP, Harmatz JS, et al. Race, gender, and genetic polymorphism contribute to variability in acetaminophen pharmacokinetics, metabolism, and protein-adduct concentrations in healthy African-American and European-American volunteers. J Pharmacol Exp Ther. 2017;362:431–40.
Critchley JA, Nimmo GR, Gregson CA, Woolhouse NM, Prescott LF. Inter-subject and ethnic differences in paracetamol metabolism. Br J Clin Pharmacol. 1986;22:649–57.
Krens SD, Lassche G, Jansman FGA, Desar IME, Lankheet NAG, Burger DM, et al. Dose recommendations for anticancer drugs in patients with renal or hepatic impairment. Lancet Oncol. 2019;20:e200–7.
Schmidt M, Vernooij R, van Nuland M, Smeijsters E, Devriese L, Mohammad NH, et al. Impaired liver function: effect on paclitaxel toxicity, dose modifications and overall survival. BMC Cancer. 2024;24:1553.
Weinstein R, Parikh-Das AM, Salonga R, Schuemie M, Ryan PB, Atillasoy E, et al. A systematic assessment of the epidemiologic literature regarding an association between acetaminophen exposure and cancer. Regul Toxicol Pharmacol. 2021;127:105043.
Fendrick AM, Pan DE, Johnson GE. OTC analgesics and drug interactions: clinical implications. Osteopath Med Prim Care. 2008;2:2.
Tsao CW, Aday AW, Almarzooq ZI, Anderson CAM, Arora P, Avery CL, et al. Heart Disease and Stroke Statistics-2023 Update: a report from the American Heart Association. Circulation. 2023;147:e93–621.
Acknowledgements
The authors would like to acknowledge the AACES interviewers, Christine Bard, LaTonda Briigs, Whitney Franx (North Carolina), Robin Gold (Detroit) and Myneka Macenat (New Jersey). The authors also thank the individuals responsible for facilitating case ascertainment across the 11 sites including Jennifer Burczyk-Brown (Alabama); Rana Bayakly and Vicki Bennett (Georgia); the Louisiana Tumor Registry; Lisa Paddock and Wendy Cedeno (New Jersey); Diana Slone, Yingli Wolinsky, Steven Waggoner, Anne Heugel, Nancy Fusco, Kelly Ferguson, Peter Rose, Deb Strater, Taryn Ferber, Donna White, Lynn Borzi, Eric Jenison, Nairmeen Haller, Debbie Thomas, Vivian von Gruenigen, Michele McCarroll, Joyce Neading, John Geisler, Stephanie Smiddy, David Cohn, Michele Vaughan, Luis Vaccarello, Elayna Freese, James Pavelka, Pam Plummer, William Nahhas, Ellen Cato, John Moroney, Mark Wysong, Tonia Combs, Marci Bowling and Brandon Fletcher (Ohio); Martin Whiteside (Tennessee); and Georgina Armstrong and the Texas Registry, Cancer Epidemiology and Surveillance Branch, Department of State Health Services. The authors would like to thank Rex C. Bentley and Anne M. Mills for the review of the pathology in the AACES.
Funding
This research was supported by R01 CA142081 (Schildkraut) and R01 CA237318 (Schildkraut/Lawson). Additional support was provided by the Metropolitan Detroit Cancer Surveillance System (MDCSS) with federal funds from the National Cancer Institute, National Institute of Health, Department of Health and Human Services, under Contract No. HHSN261201000028C and the Epidemiology Research Core, supported in part by NCI Center Grant (P30CA22453) to the Karmanos Cancer Institute, Wayne State University School of Medicine. Services, results and/or products in support of the research were generated in part by Rutgers Cancer Institute Cancer Prevention and Outcomes Data Support Shared Resource P30CA072720-6852.
Author information
Authors and Affiliations
Contributions
LCP designed the research study and supervised the project. CCL analysed the data and created the tables and figures. CEJ, AJA, EVB, MB, MLC, TAH, KH, AL, JRM, ESP, PDT, JMS and LCP acquired data for this project. CCL, OA and LCP wrote the first draft of the manuscript. All authors reviewed, revised and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
LCP reports research funding from Bristol Myers Squibb, Karyopharm and Janssen unrelated to this work. EVB served on a Pfizer Inc. Advisory Board to enhance minority participation in clinical trials unrelated to this work. No other conflicts of interest are reported by the other authors.
Ethics approval and consent to participate
Institutional Review Board approval was obtained at the parent institution (Duke University, University of Virginia) and each individual study site, and informed consent was obtained for all participants. The study was performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Colin-Leitzinger, C., Aranzabal, O., Johnson, C.E. et al. Use of non-prescription analgesic medications and survival among Black women with ovarian cancer. Br J Cancer 134, 237–244 (2026). https://doi.org/10.1038/s41416-025-03254-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41416-025-03254-4