Abstract
Pyroptosis is a type of programmed necrosis triggered by the detection of pathogens or endogenous danger signals in the cytosol. Pyroptotic cells exhibit a swollen, enlarged morphology and ultimately undergo lysis, releasing their cytosolic contents — such as proteins, metabolites, and nucleic acids — into the extracellular space. These molecules can function as danger-associated molecular patterns (DAMPs), triggering inflammation when detected by neighboring cells. Mechanistically, pyroptosis is initiated by members of the gasdermin protein family, which were identified a decade ago as pore-forming executors of cell death. Mammalian gasdermins consist of a cytotoxic N-terminal domain, a flexible linker, and a C-terminal regulatory domain that binds to and inhibits the N-terminus. Proteolytic cleavage within the linker releases the N-terminal domain, enabling it to target various cellular membranes, including nuclear, mitochondrial, and plasma membranes, where it forms large transmembrane pores. Gasdermin pores in the plasma membrane disrupt the electrochemical gradient, leading to water influx and cell swelling. Their formation also activates the membrane protein ninjurin-1 (NINJ1), which oligomerizes to drive complete plasma membrane rupture and the release of large DAMPs. Since their discovery as pore-forming proteins, gasdermins have been linked to pyroptosis not only in host defense but also in various pathological conditions. This review explores the history of pyroptosis, recent insights into gasdermin activation, the cellular consequences of pore formation, and the physiological roles of pyroptosis.
Similar content being viewed by others
Introduction
Cell death is an essential process that is required for the development of multicellular organisms, the maintenance of tissue homeostasis, as well as for immunity and host defense.1 The importance of programmed cell death (PCD) is highlighted by the fact that animals with deficiencies in signaling pathways that regulate the induction of cell death die during embryogenesis, display developmental defects, or have a higher susceptibility to infection.2 Cell death was initially classified into two forms: an actively executed or regulated form of cell death called apoptosis, and passive, unregulated lysis of cells caused by external factors (e.g., cellular damage or toxins) called necrosis.3 Apoptosis is initiated by specific signaling cascades that regulate the activation of apoptotic caspases, a family of cysteine proteases that execute cell death, and is thus classified as a PCD.1,2 Apoptosis preserves plasma membrane integrity and is thus generally considered to be immunologically silent, whereas plasma membrane rupture (PMR) during necrosis releases cytosolic factors that act as so-called ‘danger signals’ or ‘danger-associated molecular patterns (DAMPs)’,4 i.e., molecules that drive inflammation in tissues when detected by neighboring cells.
Research over the past two decades has blurred the distinction between PCD and necrosis, since several additional cell death modalities have been identified that all result in a programmed or regulated form of necrosis.2 The best-studied among these modalities are pyroptosis, necroptosis and ferroptosis. In this review, I focus on pyroptosis, a lytic form of cell death first reported in the late 1990s as part of the immune response to pathogen infection.5 Pyroptosis is primarily linked to the activation of inflammasome complexes, which are innate immune signaling platforms assembled by pattern recognition receptors (PRRs) upon the detection of pathogen-derived or endogenous danger signals.6 However, since the discovery of the gasdermins7 — a family of pore-forming proteins that initiate pyroptosis — it has been recognized that pyroptosis can also be induced by many other signaling pathways independent of inflammasome activation. This has led to a rapid expansion of pyroptosis research revealing important functions of this form of cell death in immunity, development and cancer. Here, I summarize the mechanisms that induce pyroptosis at a cellular level and its role in disease, with a special focus on recent insights into the molecular mechanisms that regulate gasdermin activation and the induction of cell death.
Pyroptosis and the discovery of the gasdermins
First reports of pyroptosis date back to the early 1990s, when it was noted that Bacillus anthracis toxin or Shigella flexneri infections result in macrophage cell death (Fig. 1).8,9 Since DNA fragmentation could readily be detected in S. flexneri-infected cells, it was initially assumed that this type of cell death was apoptosis.9 Later studies found that this form of cell death was also induced by other microbes,10,11,12 and that it involved DNA fragmentation without the typical nuclear condensation observed in apoptotic cells. Furthermore, this form of cell death resulted in permeabilization of the plasma membrane and necrotic morphology, inconsistent with apoptosis induction.13 Clear evidence that this novel form of programmed necrosis was distinct from apoptosis came from findings showing that its induction did not require apoptotic caspases, but rather relied on caspase-1, an inflammatory caspase.14,15 Caspase-1 had been previously identified as the interleukin (IL)-1-converting enzyme (ICE), which cleaved pro-IL-1β/18 to their mature secreted forms.16 Consistent with this, it was also found that the caspase-1-dependent necrosis correlated with the release of mature, bioactive IL-1β/-18.17 To clearly distinguish this novel form of death from accidental necrosis or programmed apoptosis, the term pyroptosis was proposed in 2001, stemming from the Greek pyro (meaning fire or fever) and ptosis (meaning to fall), thus underlining the proinflammatory nature of this form of cell death.5
Timeline listing major discoveries since the first reports related to pyroptosis.
Coining the term pyroptosis coincided with the molecular characterization of the inflammasome — a platform for the activation of caspase-1.18 Inflammasomes are signaling complexes that are assembled by cytosolic PRRs in response to infection, injury, or noxious substances.6 ‘Canonical’ inflammasomes activate caspase-1 and are assembled by the proteins Pyrin, AIM2, CARD8, and multiple members of the NOD-like receptor (NLR) family, which directly or indirectly detect pathogen-derived signals (pathogen-associated molecular patterns, PAMPs) or endogenous danger signals (DAMPs). Conversely, the non-canonical inflammasome pathway, which was first reported in 2011,19 controls the activation of caspase-11 in mice or caspases-4/-5 in humans in response to the bacterial cell wall component lipopolysaccharide (LPS).20,21 Since activation of inflammasomes not only led to caspase-1-dependent production of IL-1β/-18, but also, in most cases, to a caspase-dependent cell death, pyroptosis was redefined as an inflammasome-dependent cell death and an effector mechanism of the inflammasome.22 Nevertheless, how active caspase-1, -11, or -4 induced cell death remained unknown for another decade. But the fact that it required the proteolytic activity of caspases suggested that cleavage of one or several yet unidentified substrate/s must initiate pyroptosis.
Landmark studies published in 2015 finally reported that a single caspase substrate, called gasdermin D (GSDMD), was the long-sought after executioner of pyroptosis.23,24,25 GSDMD is a 53 kDa cytosolic protein and a member of the gasdermin protein family, which features 6 members in humans (GSDMA, -B, -C, -D, -E and -F (also known as pejvakin, PJVK), and 10 in mice (GSDMA1-3, GSDMC1-4, GSDMD, GSDME and PVJK).7 Gasdermins were first identified in the early 2000s and named after the expression pattern of the first family member, GSDMA, in the gastrointestinal tract and the dermis.26 Although links to inflammation and cell death had emerged over time,27,28,29 their function as cell death executioners had not been previously recognized. All three studies that identified GSDMD as the executioner of inflammasome-associated pyroptosis found that GSDMD-deficient cells showed a significant reduction in pyroptosis induction after activation of both canonical and non-canonical inflammasomes.23,24,25 They also demonstrated that caspase-1, -11, or -4 cleave GSDMD after an aspartate residue within a central linker domain (D275 in humans and D276 in mice) to generate a 31-kDa N-terminal GSDMD fragment (GSDMD-NT) and a 22-kDa C-terminal fragment (GSDMD-CT). Furthermore, it was found that expression of the GSDMD-NT induced cytotoxicity with all features of pyroptosis, while the expression of full-length GSDMD (GSDMD-FL) or GSDMD-CT had no impact on cell viability, supporting the conclusion that caspase-mediated cleavage releases the cytotoxic GSDMD-NT from intramolecular autoinhibition by GSDMD-CT.
These findings revealed that the characteristic two-domain structure, comprising an N-terminal cytotoxic domain and a C-terminal inhibitory domain linked by a connector, is not unique to GSDMD but is shared by all gasdermin family members, except for PJVK, which has a truncated C-terminal domain. Moreover, ectopic expression of the N-terminal domain of GSDMA, GSDMB, GSDMC, or GSDME triggers a form of cellular necrosis that resembles pyroptosis induced by GSDMD.30 Consequently, soon after GSDMD was identified as the executor of inflammasome-associated pyroptosis, the gasdermin family was recognized as a novel group of cell death effectors defined by their N-terminal pyroptosis-inducing domain (GSDM-NT).
Additionally, since other gasdermin family members can be activated independently of inflammatory caspases,31 these discoveries indicated that pyroptosis is not solely a consequence of inflammasome activation. This necessitated a reclassification of pyroptosis as a form of mammalian cell death mediated by gasdermin family members.7
Pore formation constitutes the mechanism of gasdermin-induced pyroptosis
Several follow-up studies investigated the mechanism of GSDMD-NT-induced cell death using a combination of biochemistry, cell biology and structural biology (Fig. 2). These studies found that upon cleavage, GSDMD-NT associates with cellular membranes, and that it preferentially targets acidic phospholipids such as phosphoinositides that are found on the inner leaflet of the plasma membrane. The N-terminal domains of other gasdermins, such as those of GSDME, GSDMA and murine GSDMA3, exhibit similar lipid-binding properties, suggesting a common membrane-targeting mechanism for the entire gasdermin family.30,32 Cardiolipin was also found to be a strong binder of GSDM-NT, indicating that gasdermins might also target mitochondrial or bacterial membranes that contain cardiolipin. Consistently, it was recently reported that GSDMD targets and permeabilizes mitochondria in a manner requiring cardiolipin.33 Liposome binding assays further confirmed that GSDMD-NT interacted with membranes, and in addition it was noted that upon binding, the GSDMD-NT permeabilized liposomal membranes.30,32,34,35 Finally, atomic force microscopy or electron microscopy analysis of these liposomes revealed that GSDMD-NT forms pore-like structures in the membranes with an average inner diameter of around 20 nm.30,32,34,35 In summary, these studies thus demonstrated that gasdermin family members, with the exception of PJVK, constitute a novel family of pore-forming cell death executioners.
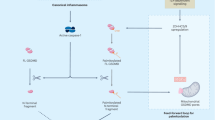
Caspase-1 cleaves GSDMD, separating the GSDMD-NT and GSDMD-CT domains. This cleavage relieves the autoinhibition of GSDMD-NT, enabling it to interact with and insert into the plasma membrane and progressively form pores, or to form pre-pores that insert into the membrane. Once GSDMD pores are formed, ion and water fluxes lead to cell swelling. Mature cytokines, such as IL-1β and IL-18, can be released directly through these pores. An as-yet unidentified signal activates NINJ1, which exists in the plasma membrane as autoinhibited dimers during the swelling phase. This activation causes a conformational change in alpha helix 1 of NINJ1, leading to the formation of flexible, filamentous NINJ1 oligomers. These oligomers can bend to form pore-like structures or release membrane discs via their hydrophilic surface. The resulting NINJ1 pores or lesions facilitate the release of DAMPs, completing the process of pyroptosis.
Today, the mechanism of gasdermin autoinhibition and pore formation has been well characterized at the molecular level, and high-resolution cryo-EM structures of pores formed by GSDMA3, GSDMD and GSDMB have been published.36,37,38 The structures of full-length mGSDMA3 and m/hGSDMD, for example, show that the GSDM-NT consists of a twisted β-sheet that is surrounded by α-helices and a disordered region that is involved in membrane insertion during pore formation.39,40 By contrast, the GSDM-CT consists primarily of tightly packed α-helices.30 In the full-length protein, the GSDM-CT binds and masks membrane-binding elements in GSDM-NT, thus providing the molecular basis for GSDM autoinhibition.30,39,40 The main mechanism that can relieve this autoinhibition and promote GSDM activation is proteolytic cleavage that separates the N- and C-terminal parts, even though other mechanisms are emerging as well, as discussed later. Studies have shown that to process GSDMD, inflammatory caspases first interact with an exosite within the GSDMD-CT,41 which helps to position the interdomain cleavage site of GSDMD close to the catalytic site of the caspases. Interestingly, exosite binding determines substrate specificity but not the tetrapeptide motif (FLTD in human GSDMD), even though Asp275/276 (human/mouse) remains important for cleavage. A similar mechanism applies to the cleavage of pro-IL-18 by caspase-4,42,43 suggesting a generalized mechanism for the cleavage of substrates of inflammatory caspases. Whether GSDMD cleavage can be inhibited by targeting exosite recognition, and which mechanisms apply to the cleavage of other gasdermin family members by other proteases, remains to be determined.
Structural studies on pores formed by recombinant gasdermin N-termini have shown that membrane-inserted GSDM pores feature a coronary ring and a transmembrane β-barrel ring, organized by the large globular subdomain and two side-by-side extended β-hairpins of the GSDM-NT domain.36,37,38 The pore is formed by either 26–28 (GSDMA3), 26–30 (GSDMB) or 31–34 (GSDMD) protomers. This gives rise to pores with an internal diameter of 18 nm, 16 nm or 21.5 nm, respectively. These studies also revealed non-β-barrel pore structures, possibly hinting at the existence of pre-pore structures.36 Comparison of the GSDM-NT in its full-length and pore conformations shows that the protein undergoes major conformational changes during pore formation and assumes the shape of a hand, with the membrane-binding α-helix 1 as a thumb, two β-hairpins as fingers and the rest of the protein forming the palm. Membrane interaction involves two β-hairpins from each protomer that form the β-barrel, and the positively charged helix α1, which is involved in the interaction with negatively charged head groups of phospholipids on the inner leaflet of the plasma membrane. In the autoinhibited, un-cleaved form of the protein, helix α1 and the α1–α2 loops are masked by the GSDM-CT, preventing premature membrane interaction.
Ninjurin-1 is a downstream effector of gasdermin pore formation
Early descriptions of pyroptosis postulated that pyroptosis involved the initial formation of a small pore that drove ion fluxes, followed by oncotic swelling that eventually resulted in plasma membrane rupture (PMR) and passive cell lysis.44 Interestingly, a recent report showed that PMR is actively executed by a small 16-kDa plasma membrane protein known as ninjurin-1 (NINJ1).45 In the absence of NINJ1, cells still induce GSDMD cleavage and pore formation, as measured by the uptake of small DNA-binding dye such as propidium iodide (PI), but fail to release lactate dehydrogenase (LDH), which has often been used as a readout for pyroptosis induction. Furthermore, NINJ1-deficient cells still release IL-1β and IL-18 upon inflammasome activation via GSDMD pores, demonstrating that in the absence of cell lysis, GSDMD pores can serve as direct channels for protein secretion. NINJ1 deficiency does, however, not protect cells from death but efficiently blocks the release of lysis-associated DAMPs like HMGB1 and S100 proteins, suggesting that pyroptosis induction might be less pro-inflammatory in the absence of NINJ1.
The signal that activates NINJ1 is currently unknown, and, although likely, it remains unknown whether all gasdermins can trigger NINJ1 activation. Since NINJ1 activation was observed during almost all forms of necrotic death, ranging from toxin-induced necrosis to ferroptosis and cuproptosis,46,47,48 and even when apoptotic cells undergo secondary necrosis,45 it can be assumed that NINJ1 senses a universal signal that is produced when cells undergo necrosis, possibly linked to changing plasma membrane properties such as tension, fluidity, lipid asymmetry or lipid distribution.
Upon sensing its activation signal, NINJ1 starts to form higher-order oligomers that were recently characterized by super-resolution microscopy and cryo-EM,48,49,50 shedding light on how NINJ1 permeabilizes the membrane. A first study reporting the cryo-EM high-resolution structure of active NINJ1 showed that the protein forms flexible filaments with both a hydrophobic and a hydrophilic face, where NINJ1 protomers are tightly packed in a fence-like array of transmembrane α-helices.48 The structured part of each protomer comprises 4 α-helices, of which α-3 and α-4 are fully extended to pass through the membrane, while α-1 and α-2 form a kinked helix, in which helix α-1 crosses over from one protomer to the next to stabilize the filament. The fact that NINJ1 filaments have a hydrophilic and hydrophobic face suggests that they can cap and stabilize membrane edges, forming large transmembrane lesions (Fig. 2).48 Alternatively, membrane permeabilization could involve the formation of double filaments that associate via their hydrophilic faces, followed by a gradual zipper-like opening once cells swell. Two later studies report a very similar structure with a kinked α1–α2 helix, but a slightly bent α-3 and α-4 helix.49,50 They also find that the NINJ1 filament is slightly bent, with the concave side being hydrophobic and the convex side being hydrophilic. Based on this, the studies propose that NINJ1 forms lesions via a ‘membrane-loss’ model, in which NINJ1 oligomers solubilize membrane patches by encircling them (Fig. 2). Additional studies involving the visualization of NINJ1-induced lesions in cells will be necessary to define whether one or both models apply to NINJ1-driven PMR. Possibly a better understanding of NINJ2, a homolog of NINJ1, could help as well, since NINJ2 was found to also form similar filaments in vitro,49,50 but lacks the ability to permeabilize cells.45,51
Morphological features of pyroptosis
All forms of cell death result in pronounced biochemical, metabolic, and morphological changes at the cellular level. Early studies noted that pyroptotic cells display several striking morphological features that make them distinct from the morphology of apoptotic cells, which are characterized by pyknosis (shrinkage or condensation of a cell with increased nuclear compactness or density), membrane blebbing, and the formation of distinct apoptotic bodies.52 Furthermore, apoptotic cells maintain plasma membrane integrity. By contrast, pyroptosis starts with a loss of plasma membrane integrity due to gasdermin pore formation, resulting in non-specific fluxes of calcium, sodium, and potassium ions, thereby dissipating the electrochemical gradient (Fig. 2).53 Gasdermin pore formation is followed by cell rounding and swelling, culminating usually in the formation of one or several large membrane balloons (Fig. 2). During this process, pyroptotic cells also undergo nuclear rounding and condensation and suffer decay of mitochondria and other organelles, which will eventually lead to metabolic cell death.54 Pyroptotic cells also expose phosphatidylserine (PS) at the plasma membrane, potentially caused by membrane scrambling mediated by TMEM16F, which is activated by calcium fluxes.55 Finally, these events culminate in NINJ1-dependent loss of plasma membrane integrity, causing the cells to lose their swollen morphology.45 At this stage, large lesions are formed by NINJ1, either by the formation of NINJ1 pores or by the release of membrane discs.48,49,50 Mass spectrometry studies have shown that cells release cytosolic and organellar proteins in an NINJ1-dependent manner, which can act as potential danger signals.45,46 A recent work also found that NINJ1 lesions are needed to allow filamentous actin from necrotic cells to engage CLEC9A signaling in dendritic cells.56 Experimentally, the easiest readout for NINJ1-induced cell lysis is to measure the release of LDH from cells or the uptake of large dyes. It is worth noting that in the absence of NINJ1, pyroptosis will proceed to the stage of cell swelling, and the cell will be dead and will take up PI or other dyes via GSDM pores. Thus, DNA-binding dyes are not well-suited for assessing NINJ1 lesion formation. After their demise, pyroptotic cells have also been reported to release extracellular vesicles (EVs) that can deliver signals to distant cells.57,58,59 EVs might be generated by membrane repair mechanisms, such as ESCRT, that remove GSDMD pores from membranes60 or by other processes.
All the above changes are initiated by the formation of gasdermin pores, and can be recapitulated in cells with inducible expression of GSDM-NT, and are thus independent of the upstream caspases that cleave and activate gasdermins. However, in the context of inflammasome activation, for example, inflammatory caspases cleave not only GSDMD but also pro-IL-1β and -18.6 Interestingly, the mature form — but not the precursors — is released from pyroptotic cells independently of cell lysis as shown by the use of osmoprotectants that prevent lysis or genetically by deleting NINJ1.37,45,61 This indicates that GSDM pore formation might be associated with the limited release of cytosolic proteins even before full permeabilization, yet, thus far, this pore-specific secretome has not been described or functionally characterized. Two recent studies reported that in addition to proteins, oxylipins and metabolites can also be released from pyroptotic cells, and that these can drive tissue repair.62,63 Furthermore, under certain conditions, inflammasome activation can induce IL-1β release without pyroptotic cell death,64 a phenomenon called hyperactivation. This suggests that GSDM pore formation may facilitate unconventional protein secretion independent of cell death.65
Many studies on pyroptosis primarily use mouse or human macrophages, but this form of cell death may exhibit distinct characteristics in other cell types, such as neutrophils66 or intestinal epithelial67 cells. Although pyroptotic cells have a morphology that clearly differentiates them from apoptotic cells, distinguishing pyroptosis from other necrotic processes, e.g., necroptosis or ferroptosis, based on morphology alone is challenging. Features like membrane integrity loss, cell rounding and swelling, and eventual PMR are common among necrotic cell death forms.2 Therefore, definitively identifying pyroptosis requires integrating morphological analysis with biochemical characterization and genetic knockouts. This involves studying cells or animals lacking key components of upstream pathways and gasdermins, alongside detecting active proteases and gasdermin cleavage. While inhibitors could be useful in specific contexts, no selective gasdermin inhibitors are currently available.
Gasdermin activation and the induction of pyroptotic cell death
Expression of a full-length wild-type gasdermin cannot by itself drive pyroptosis, and requires an activation event, as summarized below:
Activation by proteolytic cleavage
The best-studied mechanism of gasdermins is based on proteolytic cleavage and the separation of the pore-forming GSDM-NT from the regulatory GSDM-CT (Fig. 3a). Over the last decade, a number of proteases have been reported to cleave gasdermin family members and thereby initiate pore formation and cell death. Among all these proteases, caspases have emerged as the key regulators of gasdermin activation, as exemplified by the inflammatory caspases (e.g., caspase-1, -11, and -4) that in mammals cleave GSDMD.23,24,25 Interestingly though, caspase-1 can still induce pyroptosis in animals that do not feature GSDMD, such as birds, reptiles and amphibians, as it has been reported to target GSDMA under these conditions due to the presence of a caspase-1 cleavage site within its linker.68 A second group of caspases that target gasdermins are the apoptotic caspases, which is paradoxical as these are normally thought of as executioners of apoptosis, a non-necrotic immunologically silent form of death. For example, it has been shown that in mouse macrophages — but not human macrophages — caspase-8 cleaves GSDMD at the same residues as inflammatory caspases, and thus re-routing extrinsic apoptosis into pyroptosis, which contributes to host defense against Yersinia.69,70,71 Caspase-8 has also been shown to cleave GSDMC, at either D365 or D240.72,73 Recently a signaling axis involving ZBP1, caspase-8 and GSDMC was shown to cause pyroptosis that led to impaired mucosal repair after DSS-induced colitis in mice.74 Besides the initiator caspase-8, executioner caspase-3/-7 were shown to process GSDME and thereby induce pyroptosis.75,76 Here, the expression levels of GSDME and its potential subcellular targeting play a decisive role in determining whether a cell undergoes pyroptosis. In macrophages, for example, GSDME has been suggested to target mitochondria, promoting cytochrome c release to augment apoptosis.77 In cancer cell lines, the expression levels of GSDME play a role in deciding whether cells die by apoptosis or pyroptosis upon treatment with chemotherapeutic drugs, and consequently many cancer cell lines have downregulated GSDME expression.76 GSDME activation during apoptosis may contribute to the loss of membrane integrity in late apoptotic cells, a process known as secondary necrosis. However, it might not be the only determining factor, as NINJ1 has also been shown to permeabilize the membrane of apoptotic cells.45 Granzymes, a family of death-inducing proteases produced by NK cells and cytotoxic T-cells can also cleave gasdermins. For example, GrzA can process GSDMB,78 while GrzB processes GSDME,79 respectively. Thus, attack by these cells can also convert apoptosis into an inflammatory cell death if the target cell expresses the respective gasdermins. In neutrophils, GSDMD was also found to be cleaved by elastase80 and Cathepsin G81 resulting in neutrophil death. A curious case is the activation of GSDMA: to date, no mammalian enzyme has been shown to cleave GSDMA. However, SpeB, a protease from S. pyogenes, has been found to cleave and activate GSDMA during infection, thereby inducing pyroptosis and host defense.82,83
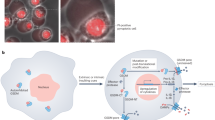
Three distinct mechanisms have so far been proposed to result in the activation of mammalian gasdermins. a Activation by proteolysis. Proteolytic cleavage within or close to the interdomain linker separates the regulatory C-terminus from the pore-forming N-terminal domain, allowing the formation of transmembrane pores by the GSDM-NT. Proteases and the respective cleavage sites are listed. b Activating mutations. Mutations in mouse GSDMA3 and exon skipping of human GSDME have been shown to result in a loss of autoinhibition, allowing the uncleaved protein to form membrane pores. c Activation by PTM. Palmitoylation of GSDMD and PARylation of GSDME have been proposed to relieve autoinhibition, thereby allowing the full-length protein to form pores. The small molecule DMB can also induce cleavage-independent GSDMD activation by binding Cys191. Gasdermin pore structures were modeled based on structures (PDB: 6VFE, and EMDB: EMD-44034) using ChimeraX1.8.
Activation by gain-of-function mutations
The earliest reports of gasdermin-induced inflammation or cell death involve mutations that disrupt intramolecular autoinhibition, allowing the full-length protein to form pores (Fig. 3b). Notably, several mutations in mouse GSDMA3 interfere with autoinhibition interfaces I and II, leading to the protein’s autoactivation and causing alopecia in mice.84,85 Additionally, several gain-of-function variants of GSDME (DFNA5) have been linked to autosomal dominant hearing loss in humans.28 This mutated, autoactive form of GSDME arises from exon 8 skipping, which results in a truncated GSDM-CT domain and subsequent loss of autoinhibition. It is believed that the high expression of GSDME in cochlear hair cells makes them particularly vulnerable to pyroptosis triggered by mutated GSDME alleles.30 Mutations in DFNB59 have also been associated with hearing loss;86 however, since DFNB59 has not been shown to form pores, the underlying mechanism remains unclear.
Activation by post-translational modification (PTMs)
An emerging theme is the activation of gasdermins by PTMs (Fig. 3c). So far, only three studies report cleavage-independent activation in mammals, while other examples exist for gasdermins in fungi and lower animals. For example, Du et al. recently reported that even the uncleavable GSDMD D275A mutant induced a low level of pyroptosis and IL-1β release after inflammasome activation.87 Further experiments linked this to ROS-dependent palmitoylation of GSDMD at C191, which is known as a PTM that promotes GSDM membrane association. However, in their study, the authors place ROS production and GSDMD palmitoylation downstream of inflammasome activation and initial GSDMD pore formation, indicating that it mainly acts as an amplification mechanism. Notably, a host of studies, however, have used D275A/D276A GSDMD as controls,23,24 going as far as generating a GSDMD-D276A knock-in mouse,88 and not found any cleavage-independent activation, indicating that in most cases cleavage is the main driver of activation. GSDMD was also reported to be activated independently of cleavage by 6,7-dichloro-2-methylsulfonyl-3-N-tert-butylaminoquinoxaline (DMB), a GLP-1 receptor agonist, which covalently modifies C191, thereby overcoming autoinhibition.89 Another study reported that UVC irradiation triggered DNA damage that drove activation of nuclear PARP1 and the formation of poly(ADP-ribose) polymers.90 Once released to the cytosol, these polymers lead to PARP5-dependent PARylation of GSDME, which induces a structural change, allowing the induction of cleavage-independent pyroptosis. Altogether the studies suggest that additional mechanisms of activation might exist and could thus expand the number of conditions or diseases in which gasdermins play a decisive role as inducers of pyroptosis.
Further insight into potential activation mechanisms comes from studies that have investigated gasdermins in lower animals and other kingdoms of life. Over the past few years, these studies have revealed that gasdermins can be found in bacteria,91 fungi,92,93 cnidaria94 and corals,95 where they have been shown to induce cell death through membrane pore formation in immunological settings such as phage defense or allorecognition. Interestingly, while processing is the primary activation mechanism of such gasdermins,91,93 other cleavage-independent mechanisms also exist.94
Role of pyroptosis in disease
Since the discovery of the pore-forming function of gasdermins, it has become evident that pyroptosis is not solely an inflammasome/GSDMD-driven form of cell death but can also occur downstream of other gasdermins in various contexts. Since then, a growing number of studies have explored the physiological roles of gasdermins, as recently reviewed in several articles.96,97 Given the extensive literature on this topic, I will focus on the most well-established roles of pyroptosis in (auto)inflammatory and infectious diseases, while referring readers to excellent reviews that discuss the involvement of gasdermins and pyroptosis in cancer.96,97,98
Role in infectious diseases
Pyroptosis is well recognized as an anti-microbial form of cell death that can restrict the growth of intracellular pathogens by killing their replicative niche. This mechanism is evident in the context of viral infections, but whether pyroptosis can kill intracellular bacteria or parasites is less well understood. A few studies have noted that gasdermins can kill intracellular bacteria,32,99 and thus different mechanisms have been proposed by which pyroptosis restricts bacterial replication. The antimicrobial role of pyroptosis is best understood in the intestine, where it has been shown that during infections with Salmonella typhimurium, cell death driven by the activation of the NLRC4 inflammasome or caspase-4 promotes the expulsion of dying cells from the intestinal epithelium,100,101,102 thereby restricting bacterial numbers within intestinal epithelial cells (IECs). It is less clear whether pyroptosis restricts bacteria in dying macrophages, but one study found that pyroptotic cell corpses can trap bacteria,103 which are then cleared by neutrophils that ingest the dead cells.
The anti-microbial functions of pyroptosis are mainly based on studies that explored the role of GSDMD in infectious diseases, since many of the pathogens examined are known to activate inflammasomes. These studies have reported that animals lacking inflammasome receptors, inflammatory caspases, or Gsdmd are highly susceptible to infections with bacteria such as S. typhimurium,102 Burkholderia pseudomallei,104 Francisella novicida105 and Citrobacter rodentium23 and Leishmania parasites.106,107 During viral infections, pyroptosis can either restrict the pathogen or cause pathology. For instance, NLRP9b and GSDMD have been shown to restrict rotavirus infections in the intestine,108 while NLRP3 and GSDMD-driven pyroptosis contribute to immunopathology during Norovirus infections.109 Additionally, H7N9 virus infection triggers a lethal cytokine storm through GSDME-mediated pyroptosis of lung alveolar epithelial cells,110 and GSDME-dependent pyroptosis causes severe disease during enterovirus 71 infection.111 Pyroptosis can also favor the pathogen during Candida albicans infections, where it promotes pathogen escape from infected macrophages.112 GSDMD is not only activated by inflammasomes but has also been reported to be cleaved by caspase-8 in Yersinia-infected cells. Consistently, Gsdmd-deficient animals have higher CFU during Yersinia infections.113 Nevertheless, some reports find that Gsdmd-deficient animals have no phenotype or only show a moderate increase in pathogen burden when compared to animals lacking inflammasome receptors or inflammatory caspases. This has, for example, been reported for Legionella pneumophila and F. novicida, where Gsdmd deficiency provided only a mild increase in CFU counts.114,115 A possible explanation for this discrepancy could be that in the absence of GSDMD, active caspase-1 induces a rapid lytic backup pathway that relies on active apoptotic caspases and can compensate, to some degree, for Gsdmd deficiency.116,117 It is also important to note that Gsdmd deficiency abrogates both pyroptosis as well as the release of IL-1β and IL-18, and thus does not allow a definitive conclusion on which inflammasome effector mechanisms drive host defense. Comparatively little is known regarding the role of other gasdermins in host defense. GSDMA has been shown to induce pyroptosis in S. pyogenes-infected keratinocytes, and mice deficient in Gsdma1 or Gsdma1–3 have been found to display larger lesions and uncontrolled bacterial dissemination to systemic sites.82,83
GSDME activation can also mediate anti-microbial immunity. Infections with VSV-1 or HSV-1 activate intrinsic apoptosis, which in keratinocytes results in GSDME-dependent pyroptosis that releases IL-1α and restricts infection.118 Similarly, induction of extrinsic apoptosis, induced by Yersinia infections, results in GSDME activation in neutrophils and the initiation of a host defence.113 While gasdermin activation is also detrimental in models of septic shock, Gsdmd deficiency, for example, was found to be protective in LPS-induced lethality models23 and in polymicrobial sepsis caused by cecal ligation and puncture (CLP).119 Gasdermin-dependent PS exposure has also been shown to trigger blood clotting and tissue thrombosis upon LPS injection in mice,120 and GSDMD-dependent pyroptosis in endothelial cells causes the disruption of the blood–brain barrier during LPS challenge or Klebsiella pneumoniae infections.121 These data suggest that inhibiting inflammasomes or GSDMD in sepsis could be beneficial for patients.
Autoinflammatory genetic diseases
Aberrant activation of inflammasomes causes or contributes to multiple hereditary autoinflammatory diseases. Gain-of-function mutations in NLRP3 for example cause a spectrum of diseases, such as familial cold urticaria (FCAS), Muckle–Wells syndrome (MWS), and neonatal-onset multisystem inflammatory disease (NOMID, also referred to as chronic infantile neurological cutaneous and joint syndrome, CINCA), that are commonly referred to as cryopyrin-associated periodic syndromes (CAPS) or NLRP3-associated autoinflammatory diseases (NLRP3-AID).122 The role of GSDMD has been experimentally addressed in a mouse model of NOMID, and shown to prevent the development of symptoms, suggesting that GSDMD pores are a main driver of disease.123 Yet, since most NLRP3-AID patients are highly responsive to IL-1β-targeted therapies, it indicates that not pyroptosis per se, but the associated cytokine release drives disease. Another disease caused by mutations in inflammasome receptors, is Familial Mediterranean Fever (FMF), which is the most prevalent monogenic autoinflammatory disease worldwide and caused by mutations in MEFV (encoding the protein Pyrin). GSDMD deficiency has also been shown to abrogate auto-inflammation in the context of an animal model of FMF (expressing MefvV726A).124
Therapeutic targeting of pyroptosis
Given the role of gasdermins and pyroptosis in human disease, the development of drugs that inhibit pyroptosis could open new avenues for anti-inflammatory therapies. Anti-IL-1 therapies are currently used with success to reduce inflammation in patients affected by inflammasomopathies.125 However, these therapies have shown limited impact on patients with NOMID, suggesting that IL-1 may not be the primary driver of disease in this context. This highlights the potential benefit of targeting upstream processes. In this regard, the ongoing development of inhibitors that directly target NLRP3, such as MCC950,126 could prove valuable.
Inhibition of GSDMD or other gasdermins represents an alternative approach that could reduce both inflammasome-associated cell death and cytokine release. Several potential inhibitors have been reported over the years, including Dimethyl fumarate (DMF),127 necrosulfonamide,128 and disulfiram129 (Fig. 4). The mechanism of these drugs is likely linked to the crucial role of palmitoylation at Cys191/192 in the membrane association of cleaved GSDMD-NT.87,130 For example, DMF induces succination of Cys192,127 among other residues, while necrosulfonamide and disulfiram also target Cys192,128,129 reducing its palmitoylation.87 Interestingly, DMF also blocks GSDME,127 as it succinates Cys45, suggesting a similar mechanism.
Treatment with Dimethyl fumarate (DMF), Necrosulfonamide (NSA) and Disulfirma have been shown to block GSDMD pore formation by targeting C191/C192 in human and mouse GSDMD, respectively. Anti-GSDMD antibodies can also block GSDMD pore formation but require entry into the cell through already existing GSDMD pores. Antagonizing NINJ1 oligomerization with antibodies can prevent the lysis step following GSDMD pore formation.
While these drugs may not be specific to GSDMD alone, animal models of LPS-induced lethality, Mediterranean fever, and experimental autoimmune encephalitis have shown that they can block inflammasome- or pyroptosis-induced inflammation in vivo.127,129 Another alternative could be the use of antibodies that target GSDMD (Fig. 4). Recent studies have demonstrated that administration of antagonistic GSDMD nanobodies can prevent pyroptosis and cytokine release in cell culture,131 and shown that this involves an entry of these nanobodies through GSDMD pore, which then prevent further GSDMD pore formation. However, whether this approach would be effective in vivo remains to be tested.
An alternative approach to preventing inflammation associated with pyroptosis could involve inhibiting cell lysis and DAMP release driven by NINJ1 (Fig. 4). Two recent studies have reported a role for NINJ1 in models of liver damage in mice, caused by LPS plus D-galactosamine, concanavalin A, Jo2 anti-Fas agonist antibody, or ischemia-reperfusion injury.132,133 One of these studies also demonstrated that anti-NINJ1 neutralizing antibodies, which prevent NINJ1 oligomerization, significantly reduced circulating DAMPs, including IL-18, HMGB1, mitochondrial DNA, and markers of liver inflammation.133 However, further characterization of NINJ1 in vivo is needed to fully assess its physiological significance. Interestingly, no role for NINJ1 was found in a model of LPS-induced septic shock, which has been shown to be GSDMD-dependent.23 Thus, additional experiments are required to validate NINJ1 as a potential target for therapeutic interventions.
Perspectives
Since the discovery of pyroptosis, significant progress has been made in understanding the molecular mechanisms that induce this form of cell death, as well as its role in health and disease. The groundbreaking identification of gasdermins as the executioners of pyroptosis has transformed the field, providing insight into how cells undergo pyroptosis and enabling genetic studies to explore the importance of gasdermins and pyroptosis in various diseases. These studies have demonstrated that pyroptotic cell death is a physiologically significant process essential for host defense against a wide range of pathogens. However, it has also become clear that when pyroptosis occurs uncontrollably, as seen in inflammasomopathies, it can be highly detrimental to the host, underscoring the need for strategies to regulate pyroptosis induction.
To address this, further research is needed to explore how cells control gasdermin activation, particularly through PTMs and other mechanisms that govern gasdermin–membrane interactions and pore formation. Understanding these processes could uncover innovative strategies to block pyroptosis. Additionally, research should focus on developing inhibitors or antagonistic antibodies. These have shown promise, as anti-GSDMD nanobodies can reduce pyroptosis in cells, and anti-NINJ1 antibodies can alleviate inflammation in liver injury models. It is crucial to further validate these approaches in disease models where gasdermins are confirmed to be involved. Given the multifaceted roles that gasdermins play in inflammation and cell death, the quest to develop new ways to modulate their activity will undoubtedly remain a dynamic area of research in the years ahead.
References
Green, D. R. Means to an End: Apoptosis and Other Cell Death Mechanisms (Cold Spring Harbor Laboratory Press, Cold Spring Harbor, NY, 2011).
Galluzzi, L. et al. Molecular mechanisms of cell death: recommendations of the Nomenclature Committee on Cell Death 2018. Cell Death Differ. 25, 486 (2018).
Majno, G. & Joris, I. Apoptosis, oncosis, and necrosis. An overview of cell death. Am. J. Pathol. 146, 3–15 (1995).
Gallucci, S. & Matzinger, P. Danger signals: SOS to the immune system. Curr. Opin. Immunol. 13, 114–119 (2001).
Cookson, B. T. & Brennan, M. A. Pro-inflammatory programmed cell death. Trends Microbiol. 9, 113–114 (2001).
Broz, P. & Dixit, V. M. Inflammasomes: mechanism of assembly, regulation and signalling. Nat. Rev. Immunol. 16, 407–420 (2016).
Broz, P., Pelegrín, P. & Shao, F. The gasdermins, a protein family executing cell death and inflammation. Nat. Rev. Immunol. 20, 143–157 (2020).
Friedlander, A. M. Macrophages are sensitive to anthrax lethal toxin through an acid-dependent process. J. Biol. Chem. 261, 7123–7126 (1986).
Zychlinsky, A., Prevost, M. C. & Sansonetti, P. J. Shigella flexneri induces apoptosis in infected macrophages. Nature 358, 167–169 (1992).
Hersh, D. et al. The Salmonella invasin SipB induces macrophage apoptosis by binding to caspase-1. Proc. Natl. Acad. Sci. USA 96, 2396–2401 (1999).
Monack, D. M., Raupach, B., Hromockyj, A. E. & Falkow, S. Salmonella typhimurium invasion induces apoptosis in infected macrophages. Proc. Natl. Acad. Sci. USA 93, 9833–9838 (1996).
Brennan, M. A. & Cookson, B. T. Salmonella induces macrophage death by caspase-1-dependent necrosis. Mol. Microbiol. 38, 31–40 (2000).
Fernandez-Prada, C. M., Hoover, D. L., Tall, B. D. & Venkatesan, M. M. Human monocyte-derived macrophages infected with virulent Shigella flexneri in vitro undergo a rapid cytolytic event similar to oncosis but not apoptosis. Infect. Immun. 65, 1486–1496 (1997).
Chen, Y., Smith, M. R., Thirumalai, K. & Zychlinsky, A. A bacterial invasin induces macrophage apoptosis by binding directly to ICE. EMBO J. 15, 3853–3860 (1996).
Hilbi, H., Chen, Y., Thirumalai, K. & Zychlinsky, A. The interleukin 1beta-converting enzyme, caspase 1, is activated during Shigella flexneri-induced apoptosis in human monocyte-derived macrophages. Infect. Immun. 65, 5165–5170 (1997).
Thornberry, N. A. et al. A novel heterodimeric cysteine protease is required for interleukin-1 beta processing in monocytes. Nature 356, 768–774 (1992).
Zychlinsky, A., Fitting, C., Cavaillon, J. M. & Sansonetti, P. J. Interleukin 1 is released by murine macrophages during apoptosis induced by Shigella flexneri. J. Clin. Invest. 94, 1328–1332 (1994).
Martinon, F., Burns, K. & Tschopp, J. The inflammasome: a molecular platform triggering activation of inflammatory caspases and processing of proIL-beta. Mol. Cell 10, 417–426 (2002).
Kayagaki, N. et al. Non-canonical inflammasome activation targets caspase-11. Nature 479, 117–121 (2011).
Kayagaki, N. et al. Noncanonical inflammasome activation by intracellular LPS independent of TLR4. Science 341, 1246–1249 (2013).
Hagar, J. A., Powell, D. A., Aachoui, Y., Ernst, R. K. & Miao, E. A. Cytoplasmic LPS activates caspase-11: implications in TLR4-independent endotoxic shock. Science 341, 1250–1253 (2013).
Lamkanfi, M. Emerging inflammasome effector mechanisms. Nat. Rev. Immunol. 11, 213–220 (2011).
Kayagaki, N. et al. Caspase-11 cleaves gasdermin D for non-canonical inflammasome signalling. Nature 526, 666–671 (2015).
Shi, J. et al. Cleavage of GSDMD by inflammatory caspases determines pyroptotic cell death. Nature 526, 660–665 (2015).
He, W. T. et al. Gasdermin D is an executor of pyroptosis and required for interleukin-1beta secretion. Cell Res. 25, 1285–1298 (2015).
Saeki, N., Kuwahara, Y., Sasaki, H., Satoh, H. & Shiroishi, T. Gasdermin (Gsdm) localizing to mouse Chromosome 11 is predominantly expressed in upper gastrointestinal tract but significantly suppressed in human gastric cancer cells. Mamm. Genome 11, 718–724 (2000).
Tanaka, S., Mizushina, Y., Kato, Y., Tamura, M. & Shiroishi, T. Functional conservation of Gsdma cluster genes specifically duplicated in the mouse genome. G3 3, 1843–1850 (2013).
Op de Beeck, K. et al. The DFNA5 gene, responsible for hearing loss and involved in cancer, encodes a novel apoptosis-inducing protein. Eur. J. Hum. Genet. 19, 965–973 (2011).
Van Rossom, S. et al. The splicing mutant of the human tumor suppressor protein DFNA5 induces programmed cell death when expressed in the yeast Saccharomyces cerevisiae. Front. Oncol. 2, 77 (2012).
Ding, J. et al. Pore-forming activity and structural autoinhibition of the gasdermin family. Nature 535, 111–116 (2016).
Chen, K. W. & Broz, P. Gasdermins as evolutionarily conserved executors of inflammation and cell death. Nat. Cell Biol. 26, 1394–1406 (2024).
Liu, X. et al. Inflammasome-activated gasdermin D causes pyroptosis by forming membrane pores. Nature 535, 153–158 (2016).
Miao, R. et al. Gasdermin D permeabilization of mitochondrial inner and outer membranes accelerates and enhances pyroptosis. Immunity 56, 2523–2541.e8 (2023).
Aglietti, R. A. et al. GsdmD p30 elicited by caspase-11 during pyroptosis forms pores in membranes. Proc. Natl. Acad. Sci. USA 113, 7858–7863 (2016).
Sborgi, L. et al. GSDMD membrane pore formation constitutes the mechanism of pyroptotic cell death. EMBO J. 35, 1766–1778 (2016).
Ruan, J., Xia, S., Liu, X., Lieberman, J. & Wu, H. Cryo-EM structure of the gasdermin A3 membrane pore. Nature 557, 62–67 (2018).
Xia, S. et al. Gasdermin D pore structure reveals preferential release of mature interleukin-1. Nature 593, 607–611 (2021).
Wang, C. et al. Structural basis for GSDMB pore formation and its targeting by IpaH7.8. Nature 616, 590–597 (2023).
Kuang, S. et al. Structure insight of GSDMD reveals the basis of GSDMD autoinhibition in cell pyroptosis. Proc. Natl. Acad. Sci. USA 114, 10642–10647 (2017).
Liu, Z. et al. Structures of the gasdermin D C-terminal domains reveal mechanisms of autoinhibition. Structure 26, 778–784.e3 (2018).
Wang, K. et al. Structural mechanism for GSDMD targeting by autoprocessed caspases in pyroptosis. Cell 180, 941–955.e20 (2020).
Shi, X. et al. Recognition and maturation of IL-18 by caspase-4 noncanonical inflammasome. Nature 624, 442–450 (2023).
Devant, P. et al. Structural insights into cytokine cleavage by inflammatory caspase-4. Nature 624, 451–459 (2023).
Fink, S. L. & Cookson, B. T. Caspase-1-dependent pore formation during pyroptosis leads to osmotic lysis of infected host macrophages. Cell. Microbiol. 8, 1812–1825 (2006).
Kayagaki, N. et al. NINJ1 mediates plasma membrane rupture during lytic cell death. Nature 591, 131–136 (2021).
Ramos, S., Hartenian, E., Santos, J. C., Walch, P. & Broz, P. NINJ1 induces plasma membrane rupture and release of damage-associated molecular pattern molecules during ferroptosis. EMBO J. 43, 1164–1186 (2024).
Dondelinger, Y. et al. NINJ1 is activated by cell swelling to regulate plasma membrane permeabilization during regulated necrosis. Cell Death Dis. 14, 755 (2023).
Degen, M. et al. Structural basis of NINJ1-mediated plasma membrane rupture in cell death. Nature 618, 1065–1071 (2023).
David, L. et al. NINJ1 mediates plasma membrane rupture by cutting and releasing membrane disks. Cell 187, 2224–2235.e16 (2024).
Sahoo, B., Mou, Z., Liu, W., Dubyak, G. & Dai, X. How NINJ1 mediates plasma membrane rupture and why NINJ2 cannot. Cell 188, 292–302.e11 (2025).
Hartenian, E. et al. Ninjurin-1 mediated plasma membrane rupture is a two-step process requiring cell swelling. bioRxiv https://doi.org/10.1101/2024.10.29.620849 (2024).
Vitale, I. et al. Apoptotic cell death in disease-Current understanding of the NCCD 2023. Cell Death Differ. 30, 1097–1154 (2023).
Chen, X. et al. Pyroptosis is driven by non-selective gasdermin-D pore and its morphology is different from MLKL channel-mediated necroptosis. Cell Res. 26, 1007–1020 (2016).
de Vasconcelos, N. M., Van Opdenbosch, N., Van Gorp, H., Parthoens, E. & Lamkanfi, M. Single-cell analysis of pyroptosis dynamics reveals conserved GSDMD-mediated subcellular events that precede plasma membrane rupture. Cell Death Differ. 26, 146–161 (2019).
Ousingsawat, J., Wanitchakool, P., Schreiber, R. & Kunzelmann, K. Contribution of TMEM16F to pyroptotic cell death. Cell Death Dis. 9, 300 (2018).
Holley, C. L. et al. Pyroptotic cell corpses are crowned with F-actin-rich filopodia that engage CLEC9A signaling in incoming dendritic cells. Nat. Immunol. 26, 42–52 (2025).
Budden, C. F. et al. Inflammasome‐induced extracellular vesicles harbour distinct RNA signatures and alter bystander macrophage responses. J. Extracell. Vesicle 10, e12127 (2021).
Cypryk, W., Ohman, T., Eskelinen, E.-L., Matikainen, S. & Nyman, T. A. Quantitative proteomics of extracellular vesicles released from human monocyte-derived macrophages upon β-glucan stimulation. J. Proteome Res. 13, 2468–2477 (2014).
Qin, X. et al. Caspase-1-mediated extracellular vesicles derived from pyroptotic alveolar macrophages promote inflammation in acute lung injury. Int. J. Biol. Sci. 18, 1521–1538 (2022).
Rühl, S. et al. ESCRT-dependent membrane repair negatively regulates pyroptosis downstream of GSDMD activation. Science 362, 956–960 (2018).
Heilig, R. et al. The Gasdermin-D pore acts as a conduit for IL-1β secretion in mice. Eur. J. Immunol. 48, 584–592 (2018).
Mehrotra, P. et al. Oxylipins and metabolites from pyroptotic cells act as promoters of tissue repair. Nature 631, 207–215 (2024).
Chi, Z. et al. Gasdermin D-mediated metabolic crosstalk promotes tissue repair. Nature 634, 1168–1177 (2024).
Zanoni, I., Tan, Y., Di Gioia, M., Springstead, J. R. & Kagan, J. C. By capturing inflammatory lipids released from dying cells, the receptor CD14 induces inflammasome-dependent phagocyte hyperactivation. Immunity 47, 697–709.e3 (2017).
Broz, P. Unconventional protein secretion by gasdermin pores. Semin. Immunol. 69, 101811 (2023).
Chen, K. W. et al. The neutrophil NLRC4 inflammasome selectively promotes IL-1beta maturation without pyroptosis during acute Salmonella challenge. Cell Rep. 8, 570–582 (2014).
Churchill, M. J., Mitchell, P. S. & Rauch, I. Epithelial pyroptosis in host defense. J. Mol. Biol. 434, 167278 (2022).
Billman, Z. P. et al. Caspase-1 activates gasdermin A in non-mammals. Elife 12, RP92362 (2024).
Orning, P. et al. Pathogen blockade of TAK1 triggers caspase-8-dependent cleavage of gasdermin D and cell death. Science 362, 1064–1069 (2018).
Sarhan, J. et al. Caspase-8 induces cleavage of gasdermin D to elicit pyroptosis during Yersinia infection. Proc. Natl. Acad. Sci. USA 115, E10888–E10897 (2018).
Chen, K. W. et al. Extrinsic and intrinsic apoptosis activate pannexin-1 to drive NLRP3 inflammasome assembly. EMBO J. 8, e101638 (2019).
Zhang, J.-Y. et al. The metabolite α-KG induces GSDMC-dependent pyroptosis through death receptor 6-activated caspase-8. Cell Res. 31, 980–997 (2021).
Hou, J. et al. PD-L1-mediated gasdermin C expression switches apoptosis to pyroptosis in cancer cells and facilitates tumour necrosis. Nat. Cell Biol. 22, 1264–1275 (2020).
Jena, K. K. et al. Type III interferons induce pyroptosis in gut epithelial cells and impair mucosal repair. Cell 187, 7533–7550.e23 (2024).
Rogers, C. et al. Cleavage of DFNA5 by caspase-3 during apoptosis mediates progression to secondary necrotic/pyroptotic cell death. Nat. Commun. 8, 14128 (2017).
Wang, Y. et al. Chemotherapy drugs induce pyroptosis through caspase-3 cleavage of a gasdermin. Nature 547, 99–103 (2017).
Rogers, C. et al. Gasdermin pores permeabilize mitochondria to augment caspase-3 activation during apoptosis and inflammasome activation. Nat. Commun. 10, 1689 (2019).
Zhou, Z. et al. Granzyme A from cytotoxic lymphocytes cleaves GSDMB to trigger pyroptosis in target cells. Science 368, eaaz7548 (2020).
Zhang, Z. et al. Gasdermin E suppresses tumour growth by activating anti-tumour immunity. Nature 579, 415–420 (2020).
Sollberger, G. et al. Gasdermin D plays a vital role in the generation of neutrophil extracellular traps. Sci. Immunol. 3, eaar6689 (2018).
Burgener, S. S. et al. Cathepsin G inhibition by Serpinb1 and Serpinb6 prevents programmed necrosis in neutrophils and monocytes and reduces GSDMD-driven inflammation. Cell Rep. 27, 3646–3656.e5 (2019).
LaRock, D. L. et al. Group A Streptococcus induces GSDMA-dependent pyroptosis in keratinocytes. Nature 605, 527–531 (2022).
Deng, W. et al. Streptococcal pyrogenic exotoxin B cleaves GSDMA and triggers pyroptosis. Nature 602, 496–502 (2022).
Tanaka, S. et al. A new Gsdma3 mutation affecting anagen phase of first hair cycle. Biochem. Biophys. Res. Commun. 359, 902–907 (2007).
Zhou, Y. et al. Gsdma3 mutation causes bulge stem cell depletion and alopecia mediated by skin inflammation. Am. J. Pathol. 180, 763–774 (2012).
Collin, R. W. J. et al. Involvement of DFNB59 mutations in autosomal recessive nonsyndromic hearing impairment. Hum. Mutat. 28, 718–723 (2007).
Du, G. et al. ROS-dependent S-palmitoylation activates cleaved and intact gasdermin D. Nature 630, 437–446 (2024).
Lee, B. L. et al. Caspase-11 auto-proteolysis is crucial for noncanonical inflammasome activation. J. Exp. Med. 215, 2279–2288 (2018).
Fontana, P. et al. Small-molecule GSDMD agonism in tumors stimulates antitumor immunity without toxicity. Cell 187, 6165–6181.e22 (2024).
Zhou, B. et al. Full-length GSDME mediates pyroptosis independent from cleavage. Nat. Cell Biol. 26, 1545–1557 (2024).
Johnson, A. G. et al. Bacterial gasdermins reveal an ancient mechanism of cell death. Science 375, 221–225 (2022).
Daskalov, A., Mitchell, P. S., Sandstrom, A., Vance, R. E. & Glass, N. L. Molecular characterization of a fungal gasdermin-like protein. Proc. Natl. Acad. Sci. USA 117, 18600–18607 (2020).
Clavé, C. et al. Fungal gasdermin-like proteins are controlled by proteolytic cleavage. Proc. Natl. Acad. Sci. USA 119, e2109418119 (2022).
Li, Y. et al. Cleavage-independent activation of ancient eukaryotic gasdermins and structural mechanisms. Science 384, adm9190 (2024).
Jiang, S., Zhou, Z., Sun, Y., Zhang, T. & Sun, L. Coral gasdermin triggers pyroptosis. Sci. Immunol. 5, eabd2591 (2020).
Liu, X., Xia, S., Zhang, Z., Wu, H. & Lieberman, J. Channelling inflammation: gasdermins in physiology and disease. Nat. Rev. Drug Discov. 20, 384–405 (2021).
Zhu, C. et al. The gasdermin family: emerging therapeutic targets in diseases. Signal Transduct. Target. Ther. 9, 87 (2024).
Yang, X. & Tang, Z. Role of gasdermin family proteins in cancers (Review). Int. J. Oncol. 63, 100 (2023).
Hansen, J. M. et al. Pathogenic ubiquitination of GSDMB inhibits NK cell bactericidal functions. Cell 184, 3178–3191.e18 (2021).
Sellin, M. E. et al. Epithelium-intrinsic NAIP/NLRC4 inflammasome drives infected enterocyte expulsion to restrict Salmonella replication in the intestinal mucosa. Cell Host Microbe 16, 237–248 (2014).
Knodler, L. A. et al. Noncanonical inflammasome activation of caspase-4/caspase-11 mediates epithelial defenses against enteric bacterial pathogens. Cell Host Microbe 16, 249–256 (2014).
Fattinger, S. A. et al. Gasdermin D is the only Gasdermin that provides protection against acute Salmonella gut infection in mice. Proc. Natl. Acad. Sci. USA 120, e2315503120 (2023).
Jorgensen, I., Zhang, Y., Krantz, B. A. & Miao, E. A. Pyroptosis triggers pore-induced intracellular traps (PITs) that capture bacteria and lead to their clearance by efferocytosis. J. Exp. Med. 213, 2113–2128 (2016).
Wang, J., Deobald, K. & Re, F. Gasdermin D protects from melioidosis through pyroptosis and direct killing of bacteria. J. Immunol. 202, 3468–3473 (2019).
Zhu, Q., Zheng, M., Balakrishnan, A., Karki, R. & Kanneganti, T.-D. Gasdermin D promotes AIM2 inflammasome activation and is required for host protection against Francisella novicida. J. Immunol.201, 3662–3668 (2018).
de Sá, K. et al. Gasdermin-D activation promotes NLRP3 activation and host resistance to Leishmania infection. Nat. Commun. 14, 1049 (2023).
Goris, M. et al. NLRP1-dependent activation of Gasdermin D in neutrophils controls cutaneous leishmaniasis. PLoS Pathog. 20, e1012527 (2024).
Zhu, S. et al. Nlrp9b inflammasome restricts rotavirus infection in intestinal epithelial cells. Nature 546, 667–670 (2017).
Dubois, H. et al. Nlrp3 inflammasome activation and Gasdermin D-driven pyroptosis are immunopathogenic upon gastrointestinal norovirus infection. PLoS Pathog. 15, e1007709 (2019).
Wan, X. et al. H7N9 virus infection triggers lethal cytokine storm by activating gasdermin E-mediated pyroptosis of lung alveolar epithelial cells. Natl. Sci. Rev. 9, nwab137 (2022).
Dong, S. et al. Gasdermin E is required for induction of pyroptosis and severe disease during enterovirus 71 infection. J. Biol. Chem. 298, 101850 (2022).
Ding, X. et al. Inflammasome-mediated GSDMD activation facilitates escape of Candida albicans from macrophages. Nat. Commun. 12, 6699 (2021).
Chen, K. W. et al. RIPK1 activates distinct gasdermins in macrophages and neutrophils upon pathogen blockade of innate immune signaling. Proc. Natl. Acad. Sci. USA 118, e2101189118 (2021).
Schneider, K. S. et al. The inflammasome drives GSDMD-independent secondary pyroptosis and IL-1 release in the absence of caspase-1 protease activity. Cell Rep. 21, 3846–3859 (2017).
Gonçalves, A. V. et al. Gasdermin-D and Caspase-7 are the key Caspase-1/8 substrates downstream of the NAIP5/NLRC4 inflammasome required for restriction of Legionella pneumophila. PLoS Pathog. 15, e1007886 (2019).
Heilig, R. et al. Caspase-1 cleaves Bid to release mitochondrial SMAC and drive secondary necrosis in the absence of GSDMD. Life Sci. Alliance 3, e202000735 (2020).
Tsuchiya, K. et al. Caspase-1 initiates apoptosis in the absence of gasdermin D. Nat. Commun. 10, 2091 (2019).
Orzalli, M. H. et al. Virus-mediated inactivation of anti-apoptotic Bcl-2 family members promotes Gasdermin-E-dependent pyroptosis in barrier epithelial cells. Immunity 54, 1447–1462.e5 (2021).
Chen, H. et al. RIPK3 collaborates with GSDMD to drive tissue injury in lethal polymicrobial sepsis. Cell Death Differ. 27, 2568–2585 (2020).
Yang, X. et al. Bacterial endotoxin activates the coagulation cascade through gasdermin D-dependent phosphatidylserine exposure. Immunity 51, 983–996.e6 (2019).
Wei, C. et al. Brain endothelial GSDMD activation mediates inflammatory BBB breakdown. Nature 629, 893–900 (2024).
Harapas, C. R., Steiner, A., Davidson, S. & Masters, S. L. An update on autoinflammatory diseases: inflammasomopathies. Curr. Rheumatol. Rep. 20, 40 (2018).
Xiao, J. et al. Gasdermin D mediates the pathogenesis of neonatal-onset multisystem inflammatory disease in mice. PLoS Biol. 16, e3000047 (2018).
Kanneganti, A. et al. GSDMD is critical for autoinflammatory pathology in a mouse model of Familial Mediterranean Fever. J. Exp. Med. 215, 1519–1529 (2018).
Goldbach-Mansky, R. & Kastner, D. L. Autoinflammation: the prominent role of IL-1 in monogenic autoinflammatory diseases and implications for common illnesses. J. Allergy Clin. Immunol. 124, 1141–1149 (2009). quiz 1150–1151.
Coll, R. C. et al. A small-molecule inhibitor of the NLRP3 inflammasome for the treatment of inflammatory diseases. Nat. Med. 21, 248–255 (2015).
Humphries, F. et al. Succination inactivates gasdermin D and blocks pyroptosis. Science 369, 1633–1637 (2020).
Rathkey, J. K. et al. Chemical disruption of the pyroptotic pore-forming protein gasdermin D inhibits inflammatory cell death and sepsis. Sci. Immunol. 3, eaat2738 (2018).
Hu, J. J. et al. FDA-approved disulfiram inhibits pyroptosis by blocking gasdermin D pore formation. Nat. Immunol. 21, 736–745 (2020).
Balasubramanian, A. et al. Palmitoylation of gasdermin D directs its membrane translocation and pore formation in pyroptosis. bioRxiv https://doi.org/10.1101/2023.02.21.529402 (2023).
Schiffelers, L. D. J. et al. Antagonistic nanobodies implicate mechanism of GSDMD pore formation and potential therapeutic application. Nat. Commun. 15, 8266 (2024).
Kim, M. W. et al. Deficiency of Ninjurin1 attenuates LPS/D-galactosamine-induced acute liver failure by reducing TNF-α-induced apoptosis in hepatocytes. J. Cell Mol. Med. 26, 5122–5134 (2022).
Kayagaki, N. et al. Inhibiting membrane rupture with NINJ1 antibodies limits tissue injury. Nature 618, 1072–1077 (2023).
Acknowledgements
This work is supported by Swiss National Science Foundation project funding (310030_219286) to P.B.
Funding
Open access funding provided by University of Lausanne.
Author information
Authors and Affiliations
Contributions
The article was conceived and written by P.B.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Broz, P. Pyroptosis: molecular mechanisms and roles in disease. Cell Res 35, 334–344 (2025). https://doi.org/10.1038/s41422-025-01107-6
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41422-025-01107-6
This article is cited by
-
Assessing the cytotoxicity and apoptosis-inducing ability of solar irradiated Salmonella Typhimurium in the RAW264.7 cell line in vitro
Scientific Reports (2026)
-
Damage-induced pyroptosis drives endogenous thymic regeneration by activating the purinergic receptor P2Y2
Cell Death & Disease (2026)
-
Autophagy regulation of pyroptosis and ferroptosis: a new strategy for colorectal cancer treatment
Apoptosis (2026)
-
Potential of potentiometric biosensors for the study of ion influx and efflux via gasdermin pores in plasma membrane in pyroptosis: a hypothesis
Human Cell (2026)
-
Pseudomonas aeruginosa induces tumor pyroptosis and immune activation to enhance checkpoint blockade in colorectal cancer
Cancer Immunology, Immunotherapy (2026)