Abstract
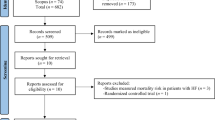
This study aimed to quantify the associations between adherence to three dietary patterns—the Dietary Approaches to Stop Hypertension (DASH), Mediterranean diet (MED), and Alternative Healthy Eating Index (AHEI)—and the risk of heart failure (HF) through a dose–response meta-analysis. Prospective cohort studies evaluating the associations between these dietary patterns and HF incidence were systematically identified from the PubMed, EMBASE, Web of Science, Cochrane Library, Scopus, and ClinicalTrials.gov databases. Random-effects models were used to pool effect estimates. Generalized least squares regression and restricted cubic spline models were applied to explore potential dose–response relationships between dietary adherence and HF risk. Eleven independent cohorts (n = 450,451; ≥18,877 HF events) were included in the final analysis. Combined across patterns, the highest adherence group had a 25% lower risk of HF than the lowest adherence group did (hazard ratio [HR] 0.75; 95% confidence interval [CI]: 0.67–0.84; P < 0.001). Subgroup analyses revealed significant inverse associations for the DASH (HR 0.81; 95% CI: 0.67–0.98; P = 0.034), MED (HR 0.74; 95% CI: 0.64–0.87; P < 0.001), and AHEI (HR 0.75; 95% CI: 0.63–0.89; P < 0.001) patterns, with no significant differences across patterns (P = 0.860). Dose–response analyses revealed linear associations between adherence to each dietary pattern and HF risk. High adherence to DASH, MED, and AHEI is associated with lower HF risk, with similar effects among the different dietary patterns and linear dose–response relationships. PROSPERO registration: CRD420251024001

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
Data generated or analyzed during this study are provided in full within this manuscript and its supplementary materials. Data are available upon reasonable request from the corresponding authors.
References
Savarese G, Becher PM, Lund LH, Seferovic P, Rosano GMC, Coats AJS. Global burden of heart failure: a comprehensive and updated review of epidemiology. Cardiovasc Res. 2023;118:3272–87. https://doi.org/10.1093/cvr/cvac013.
Beghini A, Sammartino AM, Papp Z, von Haehling S, Biegus J, Ponikowski P, et al. 2024 update in heart failure. ESC Heart Fail. 2025;12:8–42. https://doi.org/10.1002/ehf2.14857.
Boorsma EM, Ter Maaten JM, Damman K, Dinh W, Gustafsson F, Goldsmith S, et al. Congestion in heart failure: a contemporary look at physiology, diagnosis and treatment. Nat Rev Cardiol. 2020;17:641–55. https://doi.org/10.1038/s41569-020-0379-7.
Yan T, Zhu S, Yin X, Xie C, Xue J, Zhu M, et al. Burden, Trends, and Inequalities of Heart Failure Globally, 1990 to 2019: A Secondary Analysis Based on the Global Burden of Disease 2019 Study. J Am Heart Assoc. 2023;12:e027852 https://doi.org/10.1161/jaha.122.027852.
Khan MS, Shahid I, Bennis A, Rakisheva A, Metra M, Butler J. Global epidemiology of heart failure. Nat Rev Cardiol. 2024;21:717–34. https://doi.org/10.1038/s41569-024-01046-6.
Arayici ME, Kilic ME, Yilmaz MB. High and Low Adherence to Mediterranean and DASH Diet Patterns and the Risk of Heart Failure: A Meta-Analysis of Observational Studies. Life. 2025;15:63 https://doi.org/10.3390/life15010063.
Kraus WE, Powell KE, Haskell WL, Janz KF, Campbell WW, Jakicic JM, et al. Physical Activity, All-Cause and Cardiovascular Mortality, and Cardiovascular Disease. Med Sci Sports Exerc. 2019;51:1270–81. https://doi.org/10.1249/mss.0000000000001939.
Tessier AJ, Wang F, Korat AA, Eliassen AH, Chavarro J, Grodstein F, et al. Optimal dietary patterns for healthy aging. Nat Med. 2025;31:1644–52. https://doi.org/10.1038/s41591-025-03570-5.
Ibsen DB, Levitan EB, Åkesson A, Gigante B, Wolk A. The DASH diet is associated with a lower risk of heart failure: a cohort study. Eur J Prev Cardiol. 2022;29:1114–23. https://doi.org/10.1093/eurjpc/zwac003.
Goyal P, Balkan L, Ringel JB, Hummel SL, Sterling MR, Kim S, et al. The Dietary Approaches to Stop Hypertension (DASH) Diet Pattern and Incident Heart Failure. J Card Fail. 2021;27:512–21. https://doi.org/10.1016/j.cardfail.2021.01.011.
Abrignani V, Salvo A, Pacinella G, Tuttolomondo A. The Mediterranean Diet, Its Microbiome Connections, and Cardiovascular Health: A Narrative Review. Int J Mol Sci. 2024;25:4942 https://doi.org/10.3390/ijms25094942.
Veronese N, Ragusa FS, Maggi S, Witard OC, Smith L, Dominguez LJ, et al. Effect of the Mediterranean diet on incidence of heart failure in European countries: a systematic review and meta-analysis of cohort studies. Eur J Clin Nutr. 2025;79:195–9. https://doi.org/10.1038/s41430-024-01519-4.
Belin RJ, Greenland P, Allison M, Martin L, Shikany JM, Larson J, et al. Diet quality and the risk of cardiovascular disease: the Women’s Health Initiative (WHI). Am J Clin Nutr. 2011;94:49–57. https://doi.org/10.3945/ajcn.110.011221.
Agha G, Loucks EB, Tinker LF, Waring ME, Michaud DS, Foraker RE, et al. Healthy lifestyle and decreasing risk of heart failure in women: the Women’s Health Initiative observational study. J Am Coll Cardiol. 2014;64:1777–85. https://doi.org/10.1016/j.jacc.2014.07.981.
Ergas IJ, Cheng RK, Roh JM, Kushi LH, Kresovich JK, Iribarren C, et al. Diet quality and cardiovascular disease risk among breast cancer survivors in the Pathways Study. JNCI Cancer Spectr. 2024;8:pkae013 https://doi.org/10.1093/jncics/pkae013.
Shang X, Liu J, Zhu Z, Zhang X, Huang Y, Liu S, et al. Healthy dietary patterns and the risk of individual chronic diseases in community-dwelling adults. Nat Commun. 2023;14:6704. https://doi.org/10.1038/s41467-023-42523-9.
Del Gobbo LC, Kalantarian S, Imamura F, Lemaitre R, Siscovick DS, Psaty BM, et al. Contribution of Major Lifestyle Risk Factors for Incident Heart Failure in Older Adults: The Cardiovascular Health Study. JACC Heart Fail. 2015;3:520–8. https://doi.org/10.1016/j.jchf.2015.02.009.
Wirth J, di Giuseppe R, Boeing H, Weikert C. A Mediterranean-style diet, its components and the risk of heart failure: a prospective population-based study in a non-Mediterranean country. Eur J Clin Nutr. 2016;70:1015–21. https://doi.org/10.1038/ejcn.2016.140.
Lu L, Jing W, Qian W, Fan L, Cheng J. Association between dietary patterns and cardiovascular diseases: A review. Curr Probl Cardiol. 2024;49:102412 https://doi.org/10.1016/j.cpcardiol.2024.102412.
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. Jama. 2000;283:2008–12. https://doi.org/10.1001/jama.283.15.2008.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Bmj. 2021;372:n71 https://doi.org/10.1136/bmj.n71.
Nettleton JA, Steffen LM, Mayer-Davis EJ, Jenny NS, Jiang R, Herrington DM, et al. Dietary patterns are associated with biochemical markers of inflammation and endothelial activation in the Multi-Ethnic Study of Atherosclerosis (MESA). Am J Clin Nutr. 2006;83:1369–79. https://doi.org/10.1093/ajcn/83.6.1369.
Wagenknecht LE, Mayer EJ, Rewers M, Haffner S, Selby J, Borok GM, et al. The insulin resistance atherosclerosis study (IRAS) objectives, design, and recruitment results. Ann Epidemiol. 1995;5:464–72. https://doi.org/10.1016/1047-2797(95)00062-3.
Mayer-Davis EJ, Vitolins MZ, Carmichael SL, Hemphill S, Tsaroucha G, Rushing J, et al. Validity and reproducibility of a food frequency interview in a Multi-Cultural Epidemiology Study. Ann Epidemiol. 1999;9:314–24. https://doi.org/10.1016/s1047-2797(98)00070-2.
Orsini N, Li R, Wolk A, Khudyakov P, Spiegelman D. Meta-Analysis for Linear and Nonlinear Dose-Response Relations: Examples, an Evaluation of Approximations, and Software. Am J Epidemiol. 2011;175:66–73. https://doi.org/10.1093/aje/kwr265.
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. Bmj. 2008;336:924–6. https://doi.org/10.1136/bmj.39489.470347.AD.
Lim GH, Neelakantan N, Lee YQ, Park SH, Kor ZH, van Dam RM, et al. Dietary Patterns and Cardiovascular Diseases in Asia: A Systematic Review and Meta-Analysis. Adv Nutr. 2024;15:100249 https://doi.org/10.1016/j.advnut.2024.100249.
Gu X, Wang DD, Fung TT, Mozaffarian D, Djoussé L, Rosner B, et al. Dietary quality and risk of heart failure in men. Am J Clin Nutr. 2022;116:378–85. https://doi.org/10.1093/ajcn/nqac119.
Tektonidis TG, Åkesson A, Gigante B, Wolk A, Larsson SC. Adherence to a Mediterranean diet is associated with reduced risk of heart failure in men. Eur J Heart Fail. 2016;18:253–9. https://doi.org/10.1002/ejhf.481.
Strengers JG, den Ruijter HM, Boer JMA, Asselbergs FW, Verschuren WMM, van der Schouw YT, et al. The association of the Mediterranean diet with heart failure risk in a Dutch population. Nutr Metab Cardiovasc Dis. 2021;31:60–66. https://doi.org/10.1016/j.numecd.2020.08.003.
Campos CL, Wood A, Burke GL, Bahrami H, Bertoni AG. Dietary Approaches to Stop Hypertension Diet Concordance and Incident Heart Failure: The Multi-Ethnic Study of Atherosclerosis. Am J Prev Med. 2019;56:819–26. https://doi.org/10.1016/j.amepre.2018.11.022.
Levitan EB, Wolk A, Mittleman MA. Relation of consistency with the dietary approaches to stop hypertension diet and incidence of heart failure in men aged 45 to 79 years. Am J Cardiol. 2009;104:1416–20. https://doi.org/10.1016/j.amjcard.2009.06.061.
Gardner CD, Vadiveloo MK, Petersen KS, Anderson CAM, Springfield S, Van Horn L, et al. Popular Dietary Patterns: Alignment With American Heart Association 2021 Dietary Guidance: A Scientific Statement From the American Heart Association. Circulation. 2023;147:1715–30. https://doi.org/10.1161/cir.0000000000001146.
Filippou CD, Tsioufis CP, Thomopoulos CG, Mihas CC, Dimitriadis KS, Sotiropoulou LI, et al. Dietary Approaches to Stop Hypertension (DASH) Diet and Blood Pressure Reduction in Adults with and without Hypertension: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Adv Nutr. 2020;11:1150–60. https://doi.org/10.1093/advances/nmaa041.
Couch SC, Saelens BE, Khoury PR, Dart KB, Hinn K, Mitsnefes MM, et al. Dietary Approaches to Stop Hypertension Dietary Intervention Improves Blood Pressure and Vascular Health in Youth With Elevated Blood Pressure. Hypertension. 2021;77:241–51. https://doi.org/10.1161/hypertensionaha.120.16156.
Ataran A, Pompian A, Hajirezaei H, Lodhi R, Javaheri A. Fueling the Heart: What Are the Optimal Dietary Strategies in Heart Failure?. Nutrients. 2024;16:3157 https://doi.org/10.3390/nu16183157.
Campbell TM, Campbell EK, Attia J, Ventura K, Mathews T, Chhabra KH. et al.The acute effects of a DASH diet and whole food, plant-based diet on insulin requirements and related cardiometabolic markers in individuals with insulin-treated type 2 diabetes.Diabetes Res Clin Pract. 2023;202:110814 https://doi.org/10.1016/j.diabres.2023.110814.
Ishikawa Y, Laing EM, Anderson AK, Zhang D, Kindler JM, Trivedi-Kapoor R, et al. Adherence to the Dietary Approaches to Stop Hypertension (DASH) diet is associated with low levels of insulin resistance among heart failure patients. Nutr Metab Cardiovasc Dis. 2022;32:1841–50. https://doi.org/10.1016/j.numecd.2022.04.018.
Drüeke TB. Salt and health: time to revisit the recommendations. Kidney Int. 2016;89:259–60. https://doi.org/10.1016/j.kint.2015.12.009.
He FJ, Campbell NRC, Woodward M, MacGregor GA. Salt reduction to prevent hypertension: the reasons of the controversy. Eur Heart J. 2021;42:2501–5. https://doi.org/10.1093/eurheartj/ehab274.
Guasch-Ferré M, Willett WC. The Mediterranean diet and health: a comprehensive overview. J Intern Med. 2021;290:549–66. https://doi.org/10.1111/joim.13333.
Panagiotakos DB, Notara V, Kouvari M, Pitsavos C. The Mediterranean and other Dietary Patterns in Secondary Cardiovascular Disease Prevention: A Review. Curr Vasc Pharmacol. 2016;14:442–51. https://doi.org/10.2174/1570161114999160719104731.
Parker WR, Annabathula RV, Skipina TM, Soliman EZ. Associations of empirical dietary inflammatory index with heart failure in adults from the United States. Eur J Clin Nutr. 2023;77:112–5. https://doi.org/10.1038/s41430-022-01198-z.
Jiménez-Torres J, Jiménez-Juan C, Villa-Martínez A, Gutiérrez-García M, Moreno-Gaviño L, Aparicio-Santos R, et al. The Influence of Adherence to a Mediterranean Diet on Decompensation in Patients with Chronic Heart Failure. Nutrients. 2024;16:3278 https://doi.org/10.3390/nu16193278.
Bayerle P, Beyer S, Tegtbur U, Kück M, Adel J, Kwast S, et al. Exercise Capacity, Iron Status, Body Composition, and Mediterranean Diet in Patients with Chronic Heart Failure. Nutrients. 2022;15:36 https://doi.org/10.3390/nu15010036.
Sanches Machado d’Almeida K, Ronchi Spillere S, Zuchinali P, Corrêa Souza G. Mediterranean Diet and Other Dietary Patterns in Primary Prevention of Heart Failure and Changes in Cardiac Function Markers: A Systematic Review. Nutrients. 2018;10:58 https://doi.org/10.3390/nu10010058.
Zhang Y, Chadaideh KS, Li Y, Li Y, Gu X, Liu Y, et al. Butter and Plant-Based Oils Intake and Mortality. JAMA Intern Med. 2025;185:549–60. https://doi.org/10.1001/jamainternmed.2025.0205.
Das S, Alagappan VK, Bagchi D, Sharma HS, Maulik N, Das DK. Coordinated induction of iNOS-VEGF-KDR-eNOS after resveratrol consumption: a potential mechanism for resveratrol preconditioning of the heart. Vascul Pharmacol. 2005;42:281–9. https://doi.org/10.1016/j.vph.2005.02.013.
Petrovski G, Gurusamy N, Das DK. Resveratrol in cardiovascular health and disease. Ann N Y Acad Sci. 2011;1215:22–33. https://doi.org/10.1111/j.1749-6632.2010.05843.x.
Dehghan M, Mente A, Teo KK, Gao P, Sleight P, Dagenais G, et al. Relationship between healthy diet and risk of cardiovascular disease among patients on drug therapies for secondary prevention: a prospective cohort study of 31 546 high-risk individuals from 40 countries. Circulation. 2012;126:2705–12. https://doi.org/10.1161/circulationaha.112.103234.
McIntosh, N, Billingsley, H, Hummel, SL, and Mills, WL, Medically tailored meals in heart failure: a systematic review of the literature, 2013–2023. J Card Fail, 2024. https://doi.org/10.1016/j.cardfail.2024.10.446.
Burgeiro A, Fuhrmann A, Cherian S, Espinoza D, Jarak I, Carvalho RA, et al. Glucose uptake and lipid metabolism are impaired in epicardial adipose tissue from heart failure patients with or without diabetes. Am J Physiol Endocrinol Metab. 2016;310:E550–64. https://doi.org/10.1152/ajpendo.00384.2015.
Huedo-Medina TB, Garcia M, Bihuniak JD, Kenny A, Kerstetter J. Methodologic quality of meta-analyses and systematic reviews on the Mediterranean diet and cardiovascular disease outcomes: a review. Am J Clin Nutr. 2016;103:841–50. https://doi.org/10.3945/ajcn.115.112771.
Haro C, García-Carpintero S, Rangel-Zúñiga OA, Alcalá-Díaz JF, Landa BB, Clemente JC, et al., Consumption of Two Healthy Dietary Patterns Restored Microbiota Dysbiosis in Obese Patients with Metabolic Dysfunction. Mol Nutr Food Res, 2017. 61. https://doi.org/10.1002/mnfr.201700300.
Haro C, Montes-Borrego M, Rangel-Zúñiga OA, Alcalá-Díaz JF, Gómez-Delgado F, Pérez-Martínez P, et al. Two Healthy Diets Modulate Gut Microbial Community Improving Insulin Sensitivity in a Human Obese Population. J Clin Endocrinol Metab. 2016;101:233–42. https://doi.org/10.1210/jc.2015-3351.
Marques-Vidal P, Tsampasian V, Cassidy A, Biondi-Zoccai G, Chrysohoou C, Koskinas K, et al., Diet and nutrition in cardiovascular disease prevention: a scientific statement of the European Association of Preventive Cardiology and the Association of Cardiovascular Nursing & Allied Professions of the European Society of Cardiology. Eur J Prev Cardiol, 2025. https://doi.org/10.1093/eurjpc/zwaf310.
Levitan EB, Wolk A, Mittleman MA. Consistency with the DASH diet and incidence of heart failure. Arch Intern Med. 2009;169:851–7. https://doi.org/10.1001/archinternmed.2009.56.
Tektonidis TG, Åkesson A, Gigante B, Wolk A, Larsson SC. A Mediterranean diet and risk of myocardial infarction, heart failure and stroke: A population-based cohort study. Atherosclerosis. 2015;243:93–8. https://doi.org/10.1016/j.atherosclerosis.2015.08.039.
Acknowledgements
The graphical abstract in this article was created using BioRender.com, and we gratefully acknowledge BioRender for providing the illustration platform. We also extend our sincere appreciation to the researchers and participants of all original studies included in this meta-analysis, whose dedication and contributions laid the foundation for this work.
Funding
This study was supported by the National Mentorship Program (No. Qngg2022049), Suzhou Science and Technology Development Plan (No. SKYD2023205), Jiangsu Province Traditional Chinese Medicine Science and Technology Development Plan General Projects (No. MS2023106), and Project of Jiangsu Province Society of Traditional Chinese Medicine (No. XYLD2024036).
Author information
Authors and Affiliations
Contributions
Fang Yan: Conceptualization, Data curation, Formal analysis, Investigation, Writing – original draft. Moqing Yin: Conceptualization, Data curation, Validation, Writing – review and editing. Longzhi Li: Data curation, Software. Lihua Fan: Project administration, Supervision, Writing – review and editing. Yunhu Chen: Conceptualization, Methodology, Resources, Supervision, Writing – review and editing. Lijuan Zhao: Conceptualization, Methodology, Writing – review and editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical approval
This study is a secondary analysis of existing published data; therefore, ethical approval and participant consent were not required.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yan, F., Fan, L., Yin, M. et al. Dose‒response relationships of DASH, Mediterranean, and AHEI dietary patterns with heart failure incidence: a systematic review and meta-analysis of cohort studies. Eur J Clin Nutr 80, 248–262 (2026). https://doi.org/10.1038/s41430-025-01697-9
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41430-025-01697-9