Abstract
We recently reported that a 4% high-salt diet + saline for drinking (HS + saline) leads to a catabolic state, reduced heart rate, and suppression of cardiovascular energy expenditure in mice. We suggested that HS + saline reduces heart rate via the suppression of the sympathetic nervous system to compensate for the high salt intake-induced catabolic state. To test this hypothesis, we directly measured renal sympathetic nerve activity (RSNA) in conscious Sprague-Dawley (SD) rats using a radiotelemetry system. We confirmed that HS + saline induced a catabolic state. HS + saline decreased heart rate, while also reducing RSNA in SD rats. In contrast, Dahl salt-sensitive (DSS) rats exhibited no change in heart rate and increased RSNA during high salt intake. Renal denervation significantly decreased heart rate and attenuated the catabolic state independent of blood pressure in DSS rats fed HS + saline, suggesting that salt-sensitive animals were unable to decrease cardiovascular energy consumption due to abnormal renal sympathetic nerve activation during high salt intake. These findings support the hypothesis that RSNA mediates heart rate during high salt intake in SD rats. However, the insensitivity of heart rate and enhanced RSNA observed in DSS rats may be additional critical diagnostic factors for salt-sensitive hypertension. Renal denervation may benefit salt-sensitive hypertension by reducing its effects on catabolism and cardiovascular energy expenditure.
Similar content being viewed by others
Introduction
Sodium is the main extracellular ion, and the steady-state concept of Na+ homeostasis states that sodium regulation is responsible for extracellular volume and water content [1, 2]. Sodium and anions are osmolytes that draw in and retain water in the body. Salt is excreted into the urine, and the resulting increase in urinary osmolytes (Na+ and Cl−) generates an osmotic driving force for water excretion. In addition, eating large amounts of salt increases thirst. According to the current understanding, intake of a high amount of salt increases water intake and urine volume to maintain the sodium and water balance [3,4,5]. These conclusions were largely drawn from studies of extreme levels of salt intake. We examined ultralong-term sodium and water balance in healthy humans in response to normal-range salt intake of various concentrations (6, 9, and 12 g/day) under metabolic ward conditions [3]. The results of the study revealed that a 6 g increase in daily salt intake did not affect urine volume and significantly decreased drinking in healthy subjects [3]. It was also shown that urea-driven body water conservation via a hepato-renal-muscular axis facilitated water balance during high salt intake [3, 6]. On the basis of our findings, we suggested some alternative explanations regarding water balance in response to salt intake. During high salt intake (i) a urea-driven water reabsorption/urine Na+ concentration mechanism acts in the kidney to excrete the salt load with minimal water loss and (ii) the urea-producing enzyme arginase drives the production of urea, which consumes ATP and amino acids and induces a catabolic state, in the liver. The increased catabolism is compensated by either increased food intake or by energy and nitrogen transfer from skeletal muscle. In the latter case, (iii) nitrogen and energy transfer from skeletal muscle to the liver via the alanine-glucose-shuttle results in a predisposition to body weight loss due to muscle wasting [3, 6]. Urea-driven renal free water reabsorption counterbalances Na+ and Cl− excretion-driven osmotic diuresis [3, 6]. Therefore, a high-salt (HS) diet does not increase urine volume in humans [3]. In addition, the energy-intensive nature of hepatic urea production leads to a catabolic state, leading to a predisposition to an increase in endogenous metabolic water production. This endogenous water production may explain the reduced fluid intake that we observed in humans [3]. These findings suggest that the natriuretic-ureotelic regulation of body fluid homeostasis could be an additional critical feature of high salt intake, which leads to energy deficits and induces a catabolic state [3, 6].
In our mouse model, a salt-driven catabolic state not only led to changes in energy metabolism in the liver and muscle but also altered cardiovascular function [6]. High salt-fed mice exhibited reduced cardiovascular energy expenditure via a decrease in heart rate, implying that energy was saved for water conservation [6]. Since higher heart rates and a catabolic state are major risk factors for cardiovascular diseases [7,8,9,10], slower heart rate and reduced cardiovascular energy expenditure may be important responses to high salt intake for preventing cardiovascular events. We decided to investigate these responses further. Since the sympathetic nervous system is a master regulator of cardiovascular function [11], we measured renal sympathetic nerve activity (RSNA) directly in conscious rats using a radiotelemetry system. We used the Sprague-Dawley (SD) strain, which is a healthy strain that is widely used for investigating physiological responses, as a general control rat model in the present study. In a separate experiment, we also used Dahl salt-sensitive (DSS) rats as a salt-sensitive hypertension model and identified significant differences in RSNA responses.
Methods
Animal study
The Animal Research Committee of Kagawa University and Osaka General City Hospital approved all experimental protocols and procedures (Nos. 15037 and 18627). Male SD (Slc:SD) and DSS (DIS/EiS) rats (Japan SLC Inc., Shizuoka, Japan) were used, and the animals were housed under controlled temperature (24 ± 2 °C) and humidity (55 ± 5%) on a 12-h light/dark cycle. A 0.2% NaCl normal salt (NS) diet and a 4% NaCl high-salt (HS) diet were used (Oriental Yeast Co, Tokyo, Japan; Supplementary Table 1) and provided ad libitum.
Experimental protocol 1: 6-week-old male SD rats in the HS and NS groups were provided free access to water with or without 0.9% NaCl to drink for 6 weeks (n = 6 or 7 per group). Daily food intake and body weight were measured, urine samples were collected before sacrifice, and the rats were sacrificed 6 weeks following treatment.
Experimental protocol 2: A radiotelemetry system was implanted into SD, DSS, and renal-denervated DSS rats (250–300 g body weight), and arterial blood pressure, heart rate, and RSNA were measured in conscious rats. Sham operation or renal denervation (RDX) and radiotelemetry insertion were performed in one surgical procedure. The rats were fed NS, HS, and HS + saline diets in this order for 4 days beginning 10–14 days following surgery.
Experimental protocol 3: 4-week-old male DSS rats were divided into three groups: (i) the sham operation + NS group, (ii) the sham operation + HS + saline group, and (iii) the RDX + HS + saline group (n = 6 per group). Sham operation or RDX was performed in these rats. Beginning 2 weeks postsurgery, the rats were fed the respective diets. Daily food intake and body weight were measured, urine samples were collected before sacrifice, and the rats were sacrificed 6 weeks following treatment. Systolic blood pressure was also measured by the tail-cuff method once per week during the experiment.
Blood pressure measurement
A tail-cuff plethysmograph (BP-98A; Softron Co, Tokyo, Japan) was used in experimental protocol 3, and a radiotelemetry system (Data Sciences International (DSI), St Paul, MN, USA) was used in experimental protocol 2, as described previously [12]. A radiofrequency transmitter (PA-C40; DSI) and a receiver (RPC-1; DSI) were used to measure blood pressure and heart rate in renal-denervated rats. Data were collected and analyzed using Dataquest ART version 4.3 (DSI).
Urine collection and urinary sodium measurement
Twenty-four-hour urine volume and fluid intake were measured in experiments 1 and 3. All rats underwent a 12-h acclimatization period in metabolic cages prior to urine collection. Urinary sodium excretion (UNaV) was measured by using an automated analyzer (7020-Automatic Analyzer; Hitachi High-Technologies, Japan) as described previously [13].
Renal noradrenaline content measurement
Renal noradrenaline content was measured as described previously [14]. Briefly, 100 mg of renal cortex tissue was collected and homogenized in 500 µL of 0.2 M perchloric acid and then centrifuged (0 °C, 20,000 × g, 15 min). Following centrifugation, the supernatant was filtered using a regenerated cellulose membrane (Minisart RC4, Sartorius, Japan) and subjected to high-performance liquid chromatography for the measurement of noradrenaline content.
Renal denervation
Bilateral RDX was performed as described previously [13, 15]. Briefly, all detectable renal nerves around the renal arteries and veins were cut, after which the vessels were painted with a solution of 10% phenol in ethanol. In the present study, the efficiency of RDX was confirmed by measuring renal noradrenaline content 4 weeks postsurgery in experimental protocol 2 (163 ± 19 tissue vs. 7.6 ± 4.3 ng/g tissue, n = 3 or 6 per group, P < 0.01) and 8 weeks postsurgery in experimental protocol 3 (74 ± 40 tissue vs. 8.1 ± 5.7 ng/g tissue, n = 12 per group, P < 0.01).
Renal sympathetic nerve activity measurement
A radiofrequency transmitter (F50-W-F2; DSI) with nerve recording electrodes, a radiofrequency transmitter for blood pressure and heart rate (PA-C40; DSI), a receiver (RPC-3; DSI), an analog adaptor for RSNA (DL11; DSI), a digital-to-analog converter (R11CPA; DSI), and an analogue-to-digital converter (PowerLab 8/30; AD Instruments, Australia) were used to measure RSNA. Twenty-four-hour continuous signals of RSNA and blood pressure were sampled at 1 kHz and 400 Hz, respectively. The original RSNA signal was high-pass filtered at 50 Hz, amplified, full-wave rectified, and integrated. RSNA, blood pressure, and heart rate data were recorded and analyzed continuously for 24 h in conscious rats. The radiotelemetry system used for RSNA measurement was implanted as described previously [16, 17]. Briefly, an incision was made in the abdominal skin and peritoneum, and the transmitter was placed in the abdomen and secured to the abdominal wall with sutures. Subsequently, a dorsal incision was made, the accessory nerve recording electrodes were tunneled subcutaneously from the abdominal incision to the dorsal incision, and then the abdominal skin was closed. The left renal artery was carefully exposed via the retroperitoneal approach without damaging arteries, veins, lymph vessels, or nerves, and renal sympathetic nerves were detected with a high-power dissecting microscope; an ~2–3 mm piece of the renal sympathetic nerve was carefully separated from the surrounding tissue. The electrodes were anchored to the left renal artery using 7/0 silk sutures, gently applied to the sympathetic nerve and embedded in a two-component silicone gel (604; Wacker-Chemie, Munich, Germany). Following hardening, the retroperitoneal and dorsal incisions were closed.
Statistical analysis
All values are expressed as the mean ± SD. A p value < 0.05 was considered statistically significant. We used SPSS software (IBM, Armonk, NY, USA) for statistical analysis. Daily average food intake, body weight before and after the treatment, fluid intake, urine volume, UNaV, and water balance gap were analyzed by two-tailed unpaired Student’s t test or one-way analysis of variance followed by Tukey’s multiple comparison test. The frequency distributions of blood pressure, heart rate, and RSNA were analyzed by Pearson’s chi-square test.
Results
We first examined the effects of a HS diet + saline for drinking (HS + saline) on body energy balance in SD rats. HS + saline significantly reduced body weight gain under similar food intake conditions (Fig. 1a, b), although a HS diet with tap water for drinking (HS + tap) did not alter these parameters (Fig. 1c, d). Compared with NS + tap, HS + tap induced a 14-fold increase in UNaV (2.9 ± 0.4 vs. 39 ± 3.9 mmol/day/kg, P < 0.01). On the other hand, compared with NS + tap, HS + saline induced a 26-fold increase in UNaV (2.4 ± 0.1 vs. 63 ± 7.2 mmol/day/kg, P < 0.01). These results show that a HS diet combined with saline to drink induces a catabolic state in mice [6] and rats. Both HS + saline and HS + tap significantly increased fluid intake and urine volume and did not alter the water balance gap (fluid intake–urine volume), suggesting that water intake and output are not associated with the HS + saline-induced catabolic state (Supplementary Fig. 1A and B).
Effects of high salt intake on food intake and body weight gain in Sprague-Dawley rats. a Daily food intake (average) of Sprague-Dawley (SD) rats fed a 0.2% NaCl diet with tap water to drink (NS + tap) or a 4% NaCl diet with saline to drink (HS + saline) (n = 6 per group). b Body weight of the same NS + tap- and HS + saline-fed SD rats before and 6 weeks after the administration of the special diets. c Daily food intake (average) of SD rats fed NS + tap or a 4% NaCl diet with tap water to drink (HS + tap) (n = 6 or 7 per group). d Body weight of the same NS + tap- and HS + tap-fed SD rats before and 6 weeks after the administration of the special diets. All values are expressed as the mean ± SD
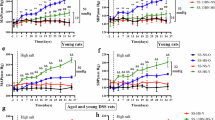
We next tested the hypothesis that HS + saline reduces heart rate and sympathetic nerve activity and therefore reduces cardiovascular energy consumption to compensate for the catabolic state. Blood pressure, heart rate, and RSNA were recorded in conscious rats using a radiotelemetry system, and their frequency distributions were analyzed to show a visual representation of the distribution of each variable. HS + tap marginally but significantly increased blood pressure during the active period (dark phase) but did not affect heart rate or RSNA in SD rats in the active or inactive period (light phase) (Fig. 2a–d). HS + saline significantly increased blood pressure and reduced heart rate and RSNA during the active period (Fig. 2a–d). Furthermore, the changes in RSNA were associated with 75% of the variability in heart rate (Fig. 2e). These data indicate that HS + saline reduces heart rate, while also suppressing RSNA to reduce cardiovascular energy expenditure in SD rats.
Effects of high salt intake on blood pressure, heart rate and renal sympathetic nerve activity in conscious Sprague-Dawley rats. a Renal sympathetic nerve activity (RSNA), heart rate, and mean arterial pressure over a 12-day period in conscious Sprague-Dawley (SD) rats (n = 3) fed a 0.2% NaCl diet with tap water to drink (NS + tap), a 4% NaCl diet with tap water to drink (HS + tap) or a 4% NaCl diet with saline to drink (HS + saline). b Mean arterial pressure distribution in the same SD rats during each salt intake phase. The data from the dark phase (active period) and the light phase (inactive period) were analyzed separately. c Heart rate distribution in the same SD rats during each salt intake phase. d RSNA distribution in the same SD rats during each salt intake phase. e The relationship between heart rate (bpm) and RSNA (µV s) for all hourly average data (n = 288) in the same SD rats presented in a. All values are expressed as the mean ± SD
A previous study reported that HS diet-fed DSS rats exhibited increased renal noradrenaline content, suggesting renal sympathetic nerve activation in salt-sensitive hypertension [18]. Therefore, we next examined the effects of high salt intake on blood pressure, heart rate, and RSNA in conscious DSS rats. Treatment with either HS + tap or HS + saline significantly increased blood pressure and RSNA in DSS rats during the active and inactive periods, whereas high salt intake did not change heart rate (Fig. 3a–d). The variability in heart rate (55%) was associated with changes in RSNA in DSS rats (Fig. 3e). Based on these observations, we hypothesized that DSS rats may not be able to reduce their heart rates during high salt intake due to renal sympathetic nervous activation. We next performed denervation studies.
Effects of high salt intake on blood pressure, heart rate and renal sympathetic nerve activity in conscious Dahl salt-sensitive rats. a Renal sympathetic nerve activity (RSNA), heart rate, and mean arterial pressure over a 12-day period in conscious Dahl salt-sensitive (DSS) rats (n = 3) fed a 0.2% NaCl diet with tap water to drink (NS + tap), a 4% NaCl diet with tap water to drink (HS + tap), or a 4% NaCl diet with saline to drink (HS + saline). b Mean arterial pressure distribution in the same DSS rats during each salt intake phase. The data from the dark phase (active period) and the light phase (inactive period) were analyzed separately. c Heart rate distribution in the same DSS rats during each salt intake phase. d RSNA distribution in the same DSS rats during each salt intake phase. e The relationship between heart rate (bpm) and RSNA (µV s) for all hourly average data (n = 288) in the same DSS rats presented in a. All values are expressed as the mean ± SD
In renal-denervated DSS rats, HS + tap, and HS + saline significantly increased blood pressure, as was the case in nondenervated DSS rats (Fig. 4a, b). We found that high salt intake significantly reduced heart rate in renal-denervated DSS rats (Fig. 4a, c), suggesting that the renal sympathetic nervous system is a key mediator of heart rate, which may explain the insensitivity of heart rate changes to high salt intake in DSS rats. These findings also suggest that RDX can improve a catabolic state via a reduction in cardiovascular energy expenditure in high salt-fed DSS rats. Therefore, the effects of RDX on energy balance in HS + saline-treated DSS rats were examined.
Effects of high salt intake on blood pressure and heart rate in conscious renal-denervated Dahl salt-sensitive rats. a Heart rate and mean arterial pressure over a 12-day period in conscious renal-denervated Dahl salt-sensitive (DSS) rats (n = 3) fed a 0.2% NaCl diet with tap water to drink (NS + tap), a 4% NaCl diet with tap water to drink (HS + tap) or a 4% NaCl diet with saline to drink (HS + saline). b Mean arterial pressure distribution in the same DSS rats during each salt intake phase. The data from the dark phase (active period) and the light phase (inactive period) were analyzed separately. c Heart rate distribution in the same DSS rats during each salt intake phase. All values are expressed as the mean ± SD
HS + saline markedly increased blood pressure, UNaV, fluid intake, and urine volume in DSS rats, whereas RDX did not significantly alter the increases in these parameters (Fig. 5a, b and Supplementary Fig. 1C). In addition, compared with NS diet-fed DSS rats in the sham group, HS diet-fed DSS rats exhibited significantly reduced body weight gain, although there were no significant differences in food intake among all groups (Fig. 5c, d). Of note, RDX significantly increased body weight gain in HS diet-fed DSS rats (Fig. 5d). These findings suggest that RDX attenuates a catabolic state in HS + saline-treated DSS rats.
Effects of renal denervation on blood pressure, food intake and body weight gain in high salt-fed Dahl salt-sensitive rats. a Systolic blood pressure (SBP) over a 6-week period in sham-operated Dahl salt-sensitive (DSS) rats fed a 0.2% NaCl diet with tap water to drink (sham + NS + tap) or a 4% NaCl diet with saline to drink (sham + HS + saline) and renal-denervated DSS rats fed a 4% NaCl diet with saline to drink (RDX + HS + saline) (n = 6 per group). b Urinary sodium excretion (UNaV) in the same DSS rats (n = 6 per group). c Daily food intake (average) of the same DSS rats. d Body weight over a 42-day period of the same DSS rats. All values are expressed as the mean ± SD. *P < 0.05; **P < 0.01, vs. sham + NS + tap, †P < 0.05, vs. sham + HS + saline
Discussion
An important finding of our study is that HS + saline reduced RSNA in addition to reducing heart rate in conscious SD rats. In our earlier mouse study, we showed that the same HS model induced a reduction in heart rate in conscious C57BL/6 J mice [6]. In contrast, we did not observe similar cardiovascular or renal sympathetic nerve responses to high salt intake in conscious DSS rats. Alternatively, the DSS rats exhibited increased RSNA during high salt intake, suggesting that salt-sensitive animals are not able to reduce their heart rates due to increased renal sympathetic nervous activation. Renal-denervated DSS rats exhibited a reduction in heart rate during high salt intake. These results suggest that high salt intake reduces heart rate via the suppression of RSNA in healthy subjects (Supplementary Fig. 2A). The insensitivity of the heart to changes in heart rate following high salt intake due to renal sympathetic nervous activation may be an additional critical diagnostic factor for salt-sensitive hypertension (Supplementary Fig. 2B). One of the limitations of this study is that we could not clarify why DSS rats exhibited significantly increased RSNA but not heart rate during high salt intake.
The sympathetic nervous system is one of the master mediators of cardiovascular function and regulates various unconscious cardiovascular actions, including vascular tone and heartbeat, to maintain hemodynamic homeostasis [19]. The renal sympathetic nervous system has both efferent and afferent nerve activity; therefore, it can exert an influence on the sympathetic nerve regulation of the central sympathetic nervous system, including baroreflex [20], and other organs [21, 22]. Foss et al. [21] reported that renal afferent sympathetic nerve denervation suppressed the bradykinin-induced increase in heart rate in rats, suggesting that the renal sympathetic nervous system has afferent nerve activity and that it influences heartbeat. In fact, RDX did not significantly alter UNaV in high salt-fed DSS rats, suggesting that RDX-induced decreases in heart rate were not mediated by the efferent renal nervous system, which regulates sodium reabsorption in the kidney [23, 24]. Therefore, RDX may decrease heart rate via the deletion of abnormally activated renal afferent nerves in high salt-fed DSS rats. However, we did not measure sodium intake and UNaV for several days before and after RDX. Thus, we may not have been able to precisely evaluate the effects of RDX on UNaV. In addition, the RDX approach used in the present study interrupted both efferent and afferent renal sympathetic nervous systems. The roles of renal efferent and/or afferent nerve activity in the regulation of heartbeat remain to be fully elucidated. Previous studies have also found that renal efferent nerve activity regulates kidney-driven humoral factors such as renin, which ultimately produces angiotensin II in the circulatory system [23, 25]. This process could influence heart rate. Thus, we cannot rule out the possibility that RDX alters certain renal humoral factors via the deletion of renal efferent sympathetic nerve activity, thereby reducing heart rate independent of renal afferent sympathetic nerve activity.
Heartbeat is an essential life activity, and heart rate is strongly associated with the average life span of the majority of animals [7]. Previous studies have also reported that heart rate is negatively associated with longevity in healthy humans and patients with cardiovascular diseases and that a high heart rate is a risk factor for cardiovascular events, suggesting that changes in heart rate are associated with the protection of the cardiovascular system [7, 8]. Therefore, a reduction in heart rate on a HS diet could provide an important cardiovascular protective factor, and RDX may prevent cardiovascular events by decreasing heart rate in salt-sensitive hypertension. In contrast, the cardiovascular system, in particular, the pumping heart, is an important site of basal metabolism and energy consumption in the body, which can contribute to energy metabolism in the body [7]. A previous study reported that an elevated heart rate leads to an increase in oxygen consumption, indicating enhanced energy expenditure, in mice [14]. Therefore, changes in heart rate during high salt intake are important from the perspective of both cardiovascular function and energy metabolism. In the present study, we showed that renal-denervated DSS rats exhibited an attenuated catabolic state on a HS diet, suggesting that RDX can improve total body energy balance, at least partly via a reduction in heart rate and cardiovascular energy expenditure. This improved body energy state also contributes to cardiovascular protection, as a catabolic state, including muscle wasting and cachexia, is an exacerbating factor for chronic heart failure [9, 10]. In addition, RDX can also alter energy metabolism in other organs, including the kidney, liver, and muscle, which may possibly contribute to the attenuation of the salt-driven catabolic state [13, 26,27,28].
In our previous long-term salt and water balance study in humans, we found that dietary salt was excreted into the urine by a renal concentrating mechanism, which was associated with a reduction in water intake and increases in glucocorticoid and catabolic hormone levels [3]. These findings suggest that the renal Na+ concentration process during high salt intake induces a catabolic state and increases endogenous metabolic water production in humans [3]. However, there are major differences regarding salt-driven catabolism between humans and rodents [3, 6]. Rodents have a stronger renal concentration ability than humans, which enables the kidneys to concentrate dietary salt into the urine easily without inducing catabolism [6]. In addition, mice and rats exhibit markedly increased water intake on a HS diet, indicating that a HS diet alone cannot mimic the salt and water metabolism observed in humans [3]. HS + tap treatment does not induce a catabolic state in mice [6] or rats. Therefore, feeding a HS diet with saline to drink, an extremely HS diet and/or a HS diet without free access to water is required to observe high salt-induced catabolism in rodents [6]. Moreover, drinking saline could affect behavior such as locomotor activity in rodents, which may alter energy expenditure and induce a catabolic state in the HS + saline model. The effects of drinking saline on behavior should be addressed in future studies. This HS + saline model is one of the limitations of animal studies involving rodents; thus, a novel animal model requiring lower salt levels may be required to mimic the salt and water metabolism observed in humans.
In a previous study, we found that HS + saline significantly increased daily food intake in mice [6]. Interestingly, we observed that a 12 g/day HS diet led our human subjects to complain about being hungry all the time [3]. We concluded that high salt intake increases appetite to compensate for the salt-driven catabolic state [3, 6]. However, HS + saline, irrespective of RDX, did not increase food intake in the SD or DSS rats. Further investigations are required to explain the difference in high salt-stimulated appetite between humans, mice, and rats, although there may be differences between Mus musculus and Rattus norvegicus in that regard.
Renal sympathetic nervous system activation increases blood pressure, and thus RDX is an attractive therapeutic tool for the treatment of hypertensive patients [29, 30]. In the present study, we found that high salt intake enhanced RSNA and increased blood pressure in DSS rats. However, the effects of RDX on blood pressure in salt-sensitive hypertension were not apparent, as has been reported in other studies [31,32,33]. These findings suggest that abnormal renal sympathetic nervous activation is not a dominant cause of salt-sensitive hypertension and that RDX reduces heart rate and attenuates a catabolic state in high salt-fed DSS rats independent of blood pressure-related effects. One limitation of this study is that we measured the long-term effect of RDX on blood pressure only using the tail-cuff method.
The effects of RDX on blood pressure in resistant hypertensive patients in clinical trials are controversial [34,35,36]. However, improvements in the equipment used, improved nerve ablation techniques, adherence to antihypertensive drugs, and improvements in clinical study settings have led to significant decreases in the blood pressure of patients with resistant hypertension [29, 30]. There is growing evidence for the beneficial effects of RDX on resistant hypertension in clinical studies, and the renal sympathetic nerve ablation technique may become a novel treatment for hypertension in the future. On the other hand, clinical studies have shown the beneficial effects of RDX beyond its blood pressure-lowering properties. Pokushalov et al. [37] reported that compared with pulmonary vein isolation (PVI) therapy alone, combination therapy with PVI with RDX significantly decreased blood pressure, and the recurrence of arterial fibrillation (AF) in patients with refractory symptomatic AF and resistant hypertension. Feyz et al. [38] reported that combination therapy with PVI and RDX significantly reduced total AF time 1 year following surgery. Ambulatory blood pressure monitoring in this study revealed that RDX did not alter blood pressure, a finding indicating that RDX improved AF independent of blood pressure. In addition, RDX led to blood pressure-independent improvements in apnea/hypoxia indices, emotional reactions, and sleep disorders in patients with sleep apnea syndrome [39, 40]. In terms of cardiovascular markers, a previous meta-analysis revealed that RDX improved left ventricular mass index, central augmentation index, and carotid–femoral pulse wave velocity independent of blood pressure [41]. In animal studies, Watanabe et al. [42] and Jiang et al. [43] reported the blood pressure-independent cardioprotective effects of RDX in DSS and spontaneously hypertensive rats. These basic and clinical findings suggest that RDX can also decrease the risk of cardiovascular disease through methods other than reducing blood pressure. In the present study, the RDX-induced changes in cardiovascular energy expenditure and body energy state may have partially accounted for the blood pressure-independent beneficial effects of RDX on the cardiovascular system. In fact, the SPYRAL HTN-OFF MED trial recently revealed that catheter-based RDX reduces heart rate in hypertensive patients not receiving antihypertensive medications [44]. This observation suggests that RDX may also decrease heartbeat in humans [44]. Salt intake was not manipulated and presumably remained constant in that study. The reevaluation of the beneficial effects of RDX on heart rate and cardiovascular energy metabolism, in addition to blood pressure, in clinical studies is required. In addition, salt intake and salt sensitivity should be considered in future trials.
In summary, we found that the renal sympathetic nervous system is one of the major regulators of cardiac beat during high salt intake (Supplementary Fig. 2) and that RDX can attenuate the salt-driven catabolic state at least partly via a reduction in cardiovascular energy expenditure in salt-sensitive hypertension. We need to evaluate the blood pressure-independent beneficial effects of RDX on cardiovascular energy metabolism.
References
Bonventre JV, Leaf A. Sodium homeostasis: steady states without a set point. Kidney Int. 1982;21:880–3.
Hollenberg NK. Set point for sodium homeostasis: surfeit, deficit, and their implications. Kidney Int. 1980;17:423–9.
Rakova N, Kitada K, Lerchl K, Dahlmann A, Birukov A, Daub S, et al. Increased salt consumption induces body water conservation and decreases fluid intake. J Clin Investig. 2017;127:1932–43.
Lerchl K, Rakova N, Dahlmann A, Rauh M, Goller U, Basner M, et al. Agreement between 24-hour salt ingestion and sodium excretion in a controlled environment. Hypertension. 2015;66:850–7.
Rakova N, Juttner K, Dahlmann A, Schroder A, Linz P, Kopp C, et al. Long-term space flight simulation reveals infradian rhythmicity in human Na(+) balance. Cell Metab. 2013;17:125–31.
Kitada K, Daub S, Zhang Y, Klein JD, Nakano D, Pedchenko T, et al. High salt intake reprioritizes osmolyte and energy metabolism for body fluid conservation. J Clin Investig. 2017;127:1944–59.
Boudoulas KD, Borer JS, Boudoulas H. Heart rate, life expectancy and the cardiovascular system: therapeutic considerations. Cardiology. 2015;132:199–212.
Palatini P. Role of elevated heart rate in the development of cardiovascular disease in hypertension. Hypertension. 2011;58:745–50.
Araujo JP, Lourenco P, Rocha-Goncalves F, Ferreira A, Bettencourt P. Nutritional markers and prognosis in cardiac cachexia. Int J Cardiol. 2011;146:359–63.
Loncar G, Fulster S, von Haehling S, Popovic V. Metabolism and the heart: an overview of muscle, fat, and bone metabolism in heart failure. Int J Cardiol. 2013;162:77–85.
de Lucia C, Piedepalumbo M, Paolisso G, Koch WJ. Sympathetic nervous system in age-related cardiovascular dysfunction: pathophysiology and therapeutic perspective. Int J Biochem Cell Biol. 2019;108:29–33.
Sufiun A, Rafiq K, Fujisawa Y, Rahman A, Mori H, Nakano D, et al. Effect of dipeptidyl peptidase-4 inhibition on circadian blood pressure during the development of salt-dependent hypertension in rats. Hypertens Res. 2015;38:237–43.
Rafiq K, Fujisawa Y, Sherajee SJ, Rahman A, Sufiun A, Kobori H, et al. Role of the renal sympathetic nerve in renal glucose metabolism during the development of type 2 diabetes in rats. Diabetologia. 2015;58:2885–98.
Lei B, Nakano D, Fujisawa Y, Liu Y, Hitomi H, Kobori H, et al. N-type calcium channel inhibition with cilnidipine elicits glomerular podocyte protection independent of sympathetic nerve inhibition. J Pharm Sci. 2012;119:359–67.
Luippold G, Beilharz M, Muhlbauer B. Chronic renal denervation prevents glomerular hyperfiltration in diabetic rats. Nephrol Dial Transpl. 2004;19:342–7.
Salman IM, Sarma Kandukuri D, Harrison JL, Hildreth CM, Phillips JK. Direct conscious telemetry recordings demonstrate increased renal sympathetic nerve activity in rats with chronic kidney disease. Front Physiol. 2015;6:218.
Stocker SD, Muntzel MS. Recording sympathetic nerve activity chronically in rats: surgery techniques, assessment of nerve activity, and quantification. Am J Physiol Heart Circ Physiol. 2013;305:H1407–16.
Nagasu H, Satoh M, Fujimoto S, Tomita N, Sasaki T, Kashihara N. Azelnidipine attenuates glomerular damage in Dahl salt-sensitive rats by suppressing sympathetic nerve activity. Hypertens Res. 2012;35:348–55.
Cohn JN. Sympathetic nervous system activity and the heart. Am J Hypertens. 1989;2:353S–6S.
Thames MD, Miller BD, Abboud FM. Baroreflex regulation of renal nerve activity during volume expansion. Am J Physiol. 1982;243:H810–14.
Foss JD, Wainford RD, Engeland WC, Fink GD, Osborn JW. A novel method of selective ablation of afferent renal nerves by periaxonal application of capsaicin. Am J Physiol Regul Integr Comp Physiol. 2015;308:R112–22.
Schlaich MP, Esler MD, Fink GD, Osborn JW, Euler DE. Targeting the sympathetic nervous system: critical issues in patient selection, efficacy, and safety of renal denervation. Hypertension. 2014;63:426–32.
Prosnitz EH, DiBona GF. Effect of decreased renal sympathetic nerve activity on renal tubular sodium reabsorption. Am J Physiol. 1978;235:F557–63.
DiBona GF. Neural regulation of renal tubular sodium reabsorption and renin secretion. Fed Proc. 1985;44:2816–22.
DiBona GF, Kopp UC. Neural control of renal function. Physiol Rev. 1997;77:75–197.
Rafiq K, Noma T, Fujisawa Y, Ishihara Y, Arai Y, Nabi AH, et al. Renal sympathetic denervation suppresses de novo podocyte injury and albuminuria in rats with aortic regurgitation. Circulation. 2012;125:1402–13.
Chen W, Chang Y, He L, Jian X, Li L, Gao L, et al. Effect of renal sympathetic denervation on hepatic glucose metabolism and blood pressure in a rat model of insulin resistance. J Hypertens. 2016;34:2465–74.
Tsioufis C, Dimitriadis K, Kasiakogias A, Kalos T, Liatakis I, Koutra E, et al. Effects of multielectrode renal denervation on elevated sympathetic nerve activity and insulin resistance in metabolic syndrome. J Hypertens. 2017;35:1100–8.
Kandzari DE, Bohm M, Mahfoud F, Townsend RR, Weber MA, Pocock S, et al. Effect of renal denervation on blood pressure in the presence of antihypertensive drugs: 6-month efficacy and safety results from the SPYRAL HTN-ON MED proof-of-concept randomised trial. Lancet. 2018;391:2346–55.
Azizi M, Schmieder RE, Mahfoud F, Weber MA, Daemen J, Davies J, et al. Endovascular ultrasound renal denervation to treat hypertension (RADIANCE-HTN SOLO): a multicentre, international, single-blind, randomised, sham-controlled trial. Lancet. 2018;391:2335–45.
Foss JD, Fiege J, Shimizu Y, Collister JP, Mayerhofer T, Wood L, et al. Role of afferent and efferent renal nerves in the development of AngII-salt hypertension in rats. Physiol Rep. 2018;6:e13602.
Nagasu H, Satoh M, Kuwabara A, Yorimitsu D, Sakuta T, Tomita N, et al. Renal denervation reduces glomerular injury by suppressing NAD(P)H oxidase activity in Dahl salt-sensitive rats. Nephrol Dial Transpl. 2010;25:2889–98.
Tudorancea I, Lohmeier TE, Alexander BT, Pieptu D, Serban DN, Iliescu R. Reduced renal mass, salt-sensitive hypertension is resistant to renal denervation. Front Physiol. 2018;9:455.
Symplicity HTNI, Esler MD, Krum H, Sobotka PA, Schlaich MP, Schmieder RE, et al. Renal sympathetic denervation in patients with treatment-resistant hypertension (The Symplicity HTN-2 Trial): a randomised controlled trial. Lancet. 2010;376:1903–9.
Bhatt DL, Kandzari DE, O’Neill WW, D’Agostino R, Flack JM, Katzen BT, et al. A controlled trial of renal denervation for resistant hypertension. N Engl J Med. 2014;370:1393–401.
Kario K, Ogawa H, Okumura K, Okura T, Saito S, Ueno T, et al. SYMPLICITY HTN-Japan—first randomized controlled trial of catheter-based renal denervation in asian patients. Circ J. 2015;79:1222–9.
Pokushalov E, Romanov A, Corbucci G, Artyomenko S, Baranova V, Turov A, et al. A randomized comparison of pulmonary vein isolation with versus without concomitant renal artery denervation in patients with refractory symptomatic atrial fibrillation and resistant hypertension. J Am Coll Cardiol. 2012;60:1163–70.
Feyz L, Theuns DA, Bhagwandien R, Strachinaru M, Kardys I, Van Mieghem NM. et al. Atrial fibrillation reduction by renal sympathetic denervation: 12 months’ results of the AFFORD study. Clin Res Cardiol. 2018;10:018-1391
Warchol-Celinska E, Prejbisz A, Kadziela J, Florczak E, Januszewicz M, Michalowska I, et al. Renal denervation in resistant hypertension and obstructive sleep apnea: randomized proof-of-concept Phase II trial. Hypertension. 2018;72:381–90.
Krawczyk-Ozog A, Tokarek T, Moczala K, Siudak Z, Dziewierz A, Mielecki W, et al. Long-term quality of life and clinical outcomes in patients with resistant hypertension treated with renal denervation. Postepy Kardiol Interwencyjnej. 2016;12:329–33.
Kordalis A, Tsiachris D, Pietri P, Tsioufis C, Stefanadis C. Regression of organ damage following renal denervation in resistant hypertension: a meta-analysis. J Hypertens. 2018;36:1614–21.
Watanabe H, Iwanaga Y, Miyaji Y, Yamamoto H, Miyazaki S. Renal denervation mitigates cardiac remodeling and renal damage in Dahl rats: a comparison with beta-receptor blockade. Hypertens Res. 2016;39:217–26.
Jiang W, Tan L, Guo Y, Li X, Tang X, Yang K. Effect of renal denervation procedure on left ventricular hypertrophy of hypertensive rats and its mechanisms. Acta Cir Bras. 2012;27:815–20.
Bohm M, Mahfoud F, Townsend RR, Kandzari DE, Pocock S, Ukena C, et al. Ambulatory heart rate reduction after catheter-based renal denervation in hypertensive patients not receiving anti-hypertensive medications: data from SPYRAL HTN-OFF MED, a randomized, sham-controlled, proof-of-concept trial. Eur Heart J. 2019;40:743–51.
Acknowledgements
This study was partially supported by the Japan Society for the Promotion of Science Grants-in-Aid for Scientific Research (KAKENHI: 18H03191) and the Salt Sciences Foundation (18C5) to AN. We are deeply grateful to Mr. Masao Masui and Ms. Sachiko Okegawa (Osaka General City Hospital) for animal maintenance at Osaka General City Hospital.
Author information
Authors and Affiliations
Contributions
NM, KK, YF, DY, LL, YZ, and TM performed the animal experiments. KK, TM, YK, TY, JT, and AN provided essential material and contributed to the design of the experiments. SK measured, analyzed, and interpreted the tissue noradrenaline content data. NM and YF performed animal surgery and radiotelemetry measurements. NM, KK, and YF analyzed the radiotelemetry data. NM, KK, DN, DY, JT, and AN designed and planned the experiments and analyzed and interpreted the data. NM, KK, DN, FL, JT, and AN wrote the paper. YK, TY, FL, JT, and AN supervised the research project.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Morisawa, N., Kitada, K., Fujisawa, Y. et al. Renal sympathetic nerve activity regulates cardiovascular energy expenditure in rats fed high salt. Hypertens Res 43, 482–491 (2020). https://doi.org/10.1038/s41440-019-0389-1
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-019-0389-1
Keywords
This article is cited by
-
Effects of renal denervation on the kidney: albuminuria, proteinuria, and renal function
Hypertension Research (2024)
-
Comparison of the effects of renal denervation at early or advanced stages of hypertension on cardiac, renal, and adipose tissue pathology in Dahl salt-sensitive rats
Hypertension Research (2024)
-
Do tissue sodium levels support renal denervation?
Hypertension Research (2024)
-
Dietary salt intake predicts future development of metabolic syndrome in the general population
Hypertension Research (2023)
-
Contributions of renal water loss and skin water conservation to blood pressure elevation in spontaneously hypertensive rats
Hypertension Research (2023)