Abstract
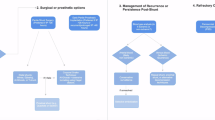
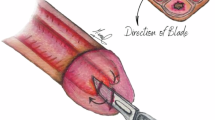
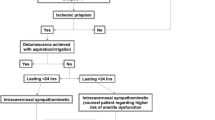
Penoscrotal decompression (PSD) has emerged as a promising surgical intervention for refractory ischaemic priapism, involving proximal corporotomies and the drainage of ischaemic blood. Initial outcomes have shown high success rates in achieving detumescence, low recurrence rates, and relatively good preservation of erectile function. This meta-analysis aims to comprehensively evaluate PSD’s effectiveness across three key metrics: detumescence, prevention of recurrence, and erectile function preservation. A systematic review and meta-analysis, following PRISMA guidelines, identified 9 publications that met the inclusion criteria. They encompassed five case reports, two abstracts, and two observational cohort studies, with data on 62 patients who presented with refractory ischaemic priapism. Notably, around half (46.7%) of the patients had conventional distal shunts prior to PSD. Overall following PSD, detumescence was achieved in 89.3% (CI 95%, 0.78–0.95). Post-PSD recurrence of ischaemic priapism occurred in 12.7% (95% CI, 0.06–0.24). Erectile function was preserved in 54.8% of the patients who had follow-up (95% CI, 0.40–0.68). These findings inform us that PSD proves to be a viable and effective surgical option for refractory ischaemic priapism with a key feature being better sexual function preservation outcomes compared to shunting procedures. Given the paucity of data, further larger scale prospective studies of robust designs are still necessary to better establish PSD’s role within the treatment algorithm for refractory ischaemic priapism.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The original contributions presented in the study are included & referenced in the article. Further inquiries can be directed to the corresponding author.
References
Silberman M, Stormont G, Leslie SW, Hu EW Priapism [Internet]. StatPearls Publishing; 2023. https://www.ncbi.nlm.nih.gov/books/NBK459178
Levey HR, Segal RL, Bivalacqua TJ. Management of priapism: an update for clinicians. Ther Adv Urol. 2014;6:230–44. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4236300/ 10.1177/1756287214542096
Muneer A, Cellek S, Dogan A, Kell PD, Ralph DJ, Minhas S. Investigation of cavernosal smooth muscle dysfunction in low-flow priapism using an in vitro model. Int J Impot Res. 2005;17:10–8. https://doi.org/10.1038/sj.ijir.3901231
Moodley D, Badenhorst A, Choonara Y, Adam A The assessment and aetiology of drug-induced ischaemic priapism. Int J Impot Res. 2024. https://doi.org/10.1038/s41443-024-01006-1
Broderick GA, Kadioglu A, Bivalacqua TJ, Ghanem H, Nehra A, Shamloul R. Priapism: pathogenesis, epidemiology, and management. J Sex Med. 2010;7:476–500. https://doi.org/10.1111/j.1743-6109.2009.01625.x
Biebel MG, Gross MS, Munarriz R. Review of ischemic and non-ischemic priapism. Curr Urol Rep. 2022;23:143–53. https://doi.org/10.1007/s11934-022-01096-8
Arduini GAO, Trovó de Marqui AB. Prevalence and characteristics of priapism in sickle cell disease. Hemoglobin. 2018;42:73–7. https://doi.org/10.1080/03630269.2018.1452760
Shaeer OK, Shaeer KZ, AbdelRahman IF, El-Haddad MS, Selim OM. Priapism as a result of chronic myeloid leukemia: case report, pathology, and review of the literature. J Sex Med. 2015;12:827–34. https://doi.org/10.1111/jsm.12812
Johnson MJ, Hallerstrom M, Alnajjar HM, Johnson TF, Skrodzka M, Chiriaco G, et al. Which patients with ischaemic priapism require further investigation for malignancy? Int J Impot Res. 2020;32:195–200. https://doi.org/10.1038/s41443-019-0141-z
Muneer A, Brown G, Dorkin T, Lucky M, Pearcy R, Shabbir M, et al. BAUS consensus document for the management of male genital emergencies: priapism. BJU Int. 2018;121:835–9. https://doi.org/10.1111/bju.14228
Bivalacqua TJ, Allen BK, Brock GB, Broderick G, Chou R, Kohler T, et al. The diagnosis and management of recurrent ischemic priapism, priapism in sickle cell patients, and non-ischemic priapism: an AUA/SMSNA guideline. J Urol. 2022;208:43–52. https://doi.org/10.1097/JU.0000000000002758
Milenkovic U, Cocci A, Veeratterapillay R, Dimitropoulos K, Boeri L, Capogrosso P, et al. Surgical and minimally invasive treatment of ischaemic and non-ischaemic priapism: a systematic review by the eau sexual and reproductive health guidelines panel. Int J Impot Res. 2022. https://doi.org/10.1038/s41443-022-00654-x
Muneer A, Minhas S, Freeman A, Kumar P, Ralph DJ. Investigating the effects of high-dose phenylephrine in the management of prolonged ischaemic priapism. J Sex Med. 2008;5:2152–9. https://doi.org/10.1111/j.1743-6109.2008.00862.x
Burnett AL, Sharlip ID. Standard operating procedures for priapism. J Sex Med. 2013;10:180–94. https://doi.org/10.1111/j.1743-6109.2012.02707.x
Fuchs JS, Shakir N, McKibben MJ, Mathur S, Teeple S, Scott JM, et al. Penoscrotal decompression—promising new treatment paradigm for refractory ischemic priapism. J Sex Med. 2018;15:797–802. https://doi.org/10.1016/j.jsxm.2018.03.003
Yi Y, Davenport M, Cordon B, Gahan J, Bergeson R, Morey A PD44-07: penoscrotal decompression as a glans-sparing alternative to shunt procedures for surgical relief of refractory ischemic priapism. J Urol. 2019;201(Suppl 4). https://doi.org/10.1097/01.JU.0000557158.16612.b9
Khater U, Ramasamy R, Shah HN. Tamsulosin-induced priapism: report of two cases and review of literature. J Endourol Case Rep. 2020;6:174–6. https://doi.org/10.1089/cren.2020.0054
Baumgarten AS, VanDyke ME, Yi YA, Keith CG, Fuchs JS, Ortiz NM, et al. Favourable multi-institutional experience with penoscrotal decompression for prolonged ischaemic priapism. BJU Int. 2020;126:441–6. https://doi.org/10.1111/bju.15127
Yi Y, Baumgarten A, Keith C, Ortiz N, Davenport M, Cordon B, et al. 357: penoscrotal decompression as a glans-sparing alternative to shunt procedures for surgical relief of refractory ischemic priapism. J Sex Med. 2020;17:S96–S97. (Suppl 1)
Mallory CW, Lopategui DM, Cordon BH. Melanotan tanning injection: a rare cause of priapism. Sex Med. 2021;9:100298 https://doi.org/10.1016/j.esxm.2020.100298
Ottaiano N, Sanekommu G, Koller C, Hellstron W, Morey A, Raheem O V12-12: penoscrotal decompression of refractory ischemic priapism: surgical technique. J Urol. 2022;207(Suppl 5). https://doi.org/10.1097/JU.0000000000002678
Lee WG, Wardak S, Ralph D. Penoscrotal decompression: a new paradigm for managing prolonged ischemic priapism. J Sex Med. 2023;20(Suppl 1):i145–6.
Elkholy M, Zahran A, Yafi F (160) Prospective evaluation of proximal decompression for the management of refractory ischemic priapism. J Sex Med. 2024;21(Suppl 2). https://doi.org/10.1093/jsxm/qdae002.146
Qian L, Reddy A, Izquierdo-Pretel G, Swain S. Successful management of prolonged acute ischemic priapism with penoscrotal decompression: a case report and review of the literature. Cureus. 2023;15:e36757 https://doi.org/10.7759/cureus.36821
Akula KP, Hofer MD. Rapid adoption of penoscrotal decompression for ischemic priapism in private practice. Urol Case Rep. 2024;53:102681 https://doi.org/10.1016/j.eucr.2024.102681
Page MJ, McKenzie JE, Bossuyt PM, Bossuyt PM, Boutron I, Hoffman T, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71 https://doi.org/10.1136/bmj.n71
Covidence—better systematic review management [Internet]. Covidence. 2023. https://www.covidence.org
Wells G, Shea B, O’Connell D Ottawa hospital research institute [Internet]. OHRI.ca. 2019. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp
Wang N. Conducting meta-analyses of proportions in R. J Behav Data Sci. 2023;3:64–126. https://doi.org/10.55965/jbds.60
Reed-Maldonado AB, Kim JS, Lue TF. Avoiding complications: surgery for ischemic priapism. Transl Androl Urol. 2017;6:657–65. https://doi.org/10.21037/tau.2017.06.20
Zacharakis E, Raheem AA, Freeman A, Skolarikos A, Garaffa G, Christopher A, et al. The efficacy of the T-shunt procedure and intracavernous tunneling (snake maneuver) for refractory ischemic priapism. J Urol. 2014;191:164–8. https://doi.org/10.1016/j.juro.2013.07.058
Ortaç M, Çevik G, Akdere H, Bahadir E, Kadioglu A. Anatomic and functional outcome following distal shunt and tunneling for treatment of ischemic priapism: a single-center experience. J Sex Med. 2019;16:1290–6. https://doi.org/10.1016/j.jsxm.2019.05.009
Unal S, Karakus S, Comb WD, Burnett A. Clinical outcomes of the Burnett “snake” maneuver shunt modification for ischemic priapism. J Sex Med. 2024;21:723–8. https://doi.org/10.1093/jsxm/qdae034
Author information
Authors and Affiliations
Contributions
MM: Study Conception & Design, Data Collection & Analysis, Manuscript Writing & Editing. QI: Study Conception & Design, Data Collection, Manuscript Writing. JH: Data Collection, Manuscript Writing & Editing. VB: Supervision, Manuscript Writing & Editing, Approval of Final Version. IP: Supervision, Manuscript Writing & Editing, Approval of Final Version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
Ethical approval was not applicable for this project as there were no patients involved directly. The data retrieved, utilised and synthesized is already available in publicly accessible publications.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mubarak, M., Isa, Q., Hayes, J. et al. The efficacy of penoscrotal decompression for refractory ischaemic priapism: a systematic review and meta-analysis. Int J Impot Res (2025). https://doi.org/10.1038/s41443-025-01044-3
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41443-025-01044-3