Abstract
Dermal resident memory CD4+ T cells (dTrm) provide protection against vector-borne infections. However, the factors that promote their development remain unclear. We tested if an mRNA vaccine, encoding a protective leishmanial antigen, induced dTrm cells. The mRNA vaccine induced robust systemic T-cell responses, but few Trm cells were found in the skin. Since IL-12 promotes Th1 responses, we tested whether IL-12 mRNA combined with the mRNA vaccine could enhance dTrm cell development. This combination significantly expanded Leishmania-specific Th1 cells expressing skin-homing molecules and memory T cell markers in the draining lymph node. Additionally, higher numbers of dTrm cells were maintained in the skin, and mice exhibited functional immunity indicated by a delayed hypersensitivity response and protection upon challenge with Leishmania. These findings highlight IL-12 as a key driver of CD4+ dTrm development, enabling their global seeding across the skin, and underscore the potential of IL-12-enhanced mRNA vaccines to generate durable immunity against cutaneous leishmaniasis and other skin-targeted infections.
Similar content being viewed by others
Introduction
Tissue-resident memory T cells (Trm) are integral components of the immune landscape across various tissues, playing critical roles in maintaining homeostasis, safeguarding against infections, and, at times, contributing to the pathology of autoimmune or allergic conditions1,2,3,4,5,6,7,8,9,10,11,12. Comprising both CD8+ and CD4+ T cells, in addition to NKT cells and innate lymphoid cells (ILCs), these resident populations are established not only within most peripheral tissues but also within secondary lymphoid organs1,13,14. Trm cells are characteristically long-lived within tissues; however, a subset may transition to become ex-Trm cells, departing from the tissue, or alternatively, cycling between the tissues and the bloodstream15,16,17,18. At barrier sites including the skin, gastrointestinal tract, and pulmonary system, Trm cells offer immediate immunological defenses and can be sufficient for pathogen control, but also aid in the recruitment of circulating immune cells to bolster resistance19,20,21,22. Traditional vaccines aim to amplify antibody responses; however, antibody-mediated immunity is ineffective against some pathogens, and in those situations, Trm cells may be essential for protection. Given that most infections initiate at barrier sites, vaccines designed to elicit robust Trm cell responses in barrier tissues hold promise for conferring enhanced protection against a diverse array of pathogens23,24,25,26.
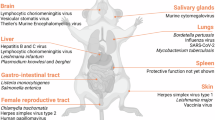
Given their role in localized immune responses in the skin, dermal tissue-resident memory T (dTrm) cells can contribute to protection against vector-borne diseases, certain helminth infections, and skin bacterial, viral, or fungal infections. Notably, these cells must be distributed throughout the skin to ensure an immediate and localized immune response upon pathogen encounter. While dTrm cells may be concentrated in areas of inflamed skin, there is clear evidence that skin-based immunization strategies promote the formation of dTrm cells across the entire skin. For instance, scarification followed by exposure to vaccinia virus generates not only dTrm cells at the scarification site but also in distal non-inflamed skin areas, indicative of a broad protective dermal immunological network27. Although the density of dTrm cells in murine non-inflamed skin (NIS) is significantly lower compared with inflamed skin sites, the dTrm cells in NIS demonstrate a strong protective capacity often comparable to those in inflamed sites27. They also mediate a delayed-type hypersensitivity (DTH) and related responses, which can be used to measure their functionality in the skin28,29,30,31. In human skin, a large population of resident T cells is present32,33, and in ‘dirty mice’, which are exposed to many pathogens, the density of T cells in non-lymphoid tissue is dramatically higher34, suggesting that continual exposure to pathogens results in more T cells seeding the skin. It is these dTrm cells that are an important target for vaccines23,24,25,26, however, a key piece of missing information is how best to expand dTrm cells through a vaccine.
Cutaneous leishmaniasis is associated with a spectrum of clinical outcomes, many of which can be disfiguring and are associated with treatment failure35,36. Macrophages are the primary host cells for these parasites and are responsible for parasite killing. This leishmanicidal function is largely mediated by CD4 + Th1 cells that produce IFN-g that subsequently activates macrophages. In contrast, antibodies are not protective and may even exacerbate disease37,38,39. Thus, unlike many vaccines, the goal of vaccines against many intracellular pathogens, including Leishmania parasites, is to generate protective T-cell immunity rather than antibody responses. Our previous studies suggest that dTrm cells are an important T-cell population to target in a vaccine. We found that Leishmania major infection generates protective CD4+ dermal Trm (dTrm) cells in the lesions and in skin sites distant from lesions or non-inflamed skin29,40,41. These globally seeded dTrm cells are positioned to provide an immediate response to reinfection with Leishmania, which we found could provide protection even in the absence of circulating effector T cells29,40. Conveniently, these dTrm cells also mediate DTH, which provides a non-invasive assessment of their functionality. However, there are currently no approved vaccines for leishmaniasis in humans and none known to induce CD4+ dTrm cells. Given the success of the Sars-CoV-2 mRNA-LNP vaccine42,43, the success of other mRNA-LNP based vaccines44, and their ability to induce T cell responses45,46, we investigated if an mRNA-LNP vaccine, employing a leishmanial antigen that is protective in mice, phosphoenolpyruvate carboxykinase (PEPCK)47, could induce dTrm cells and protective cell-mediated responses.
Our study demonstrates that while a PEPCK mRNA-LNP vaccine induces a robust systemic T-cell response, including the expansion of Th1 and T follicular helper cells (Tfh), it fails to generate Th1-biased dTrm cells that can mediate a DTH response or confer protection against leishmaniasis. However, when combined with IL-12 mRNA-LNP, the vaccine effectively promoted dTrm cell development at the immunization site and, more importantly, in NIS. Notably, IL-12 mRNA-LNP significantly enhanced systemic T-cell expansion and upregulated Trm cell markers. Finally, the presence of dTrm correlated with a DTH response and protection against Leishmania.
Results and discussion
PEPCK mRNA-LNP vaccine induces a systemic response but not protection against Leishmania major
To assess if an mRNA-based vaccine expressing the leishmanial antigen, PEPCK, could induce protective immunity, we immunized mice with a PEPCK mRNA-LNP vaccine. The route of vaccination influences the homing capacity of the T cells that respond, and immunization via the skin is superior to intramuscular immunizations in generating T cells capable of migrating into the skin27,48,49. Furthermore, a previous study demonstrated that footpad injection of PEPCK peptide given with CpG promotes protection against L. major47. Therefore, in our study, mice were immunized subcutaneously in the footpad. To facilitate tracking of PEPCK-specific T cells, T cells from PEPCK-specific TCR transgenic mice50 (Ptg cells) (CD45.2) were adoptively transferred into recipient mice (CD45.1) to create Ptg chimeras. One day after T cell transfer, mice were immunized in the footpad with 2 μg of the PEPCK mRNA-LNP vaccine (referred here as PEPCK mRNA vaccine) (Fig. 1A). At 1-week post-immunization, activated Ptg cells (CD44hi) were found in the popliteal draining lymph node (pdLN) (Fig. 1B). We previously found that CD4+ central memory T (Tcm) cells develop early after infection and contribute to protective immunity in leishmaniasis51, and the PEPCK mRNA vaccine generated Tcm cells (CD62Lhi) (Fig. 1C). As expected, we found that a large number of responding T cells were follicular helper T (Tfh) cells (PD-1hiCXCR5+)52 (Fig. 1C, D). We found comparable results in the spleen (Fig. 1E, F). Importantly, a high frequency and number of responding T cells were Th1 cells (T-bet+, IFN-γ+) (Fig. 1G), a critical T cell subset for protection against Leishmania. None of the responding T cells were Foxp3+ (data not shown). Using a PEPCK-specific tetramer47, we observed similar qualitative responses following immunization with the PEPCK mRNA vaccine (Fig. 1H–N). Additionally, splenocytes from immunized mice, when stimulated with PEPCK peptide, produced IFN-γ (Fig. 1O).
A Experimental schematic showing adoptive transfer of T cells from PEPCK-specific TCR transgenic mice (Ptg) cells (CD45.2+) into congenically distinct CD45.1⁺ hosts on day 0 (d0), followed by subcutaneous immunization with 2 μg PEPCK mRNA-LNP on day 1 (d1). At 1-wk post immunization, flow cytometry analysis of donor Ptg cells was performed in the B popliteal draining lymph node (pdLN) and E spleen. C Representative flow cytometry plots showing donor Ptg cells from the pdLN expressing CD44 vs. CD62L and PD-1hi vs. CXCR5 and D summary plots showing absolute numbers of each T cell subset. F Representative flow cytometry plots of donor Ptg cells from the spleen expressing CD44 vs. CD62L, PD-1hi vs. CXCR5, and T-bet vs. IFN-γ. G Summary plots showing absolute numbers of each T cell subset in the spleen. H Experimental schematic showing subcutaneous immunization with 2 μg PEPCK mRNA-LNP. I–N Same analysis as (B–G) but with endogenous cells stained with PEPCK I-Ab tetramer. O IFN-γ production by splenocytes from naïve or immunized mice stimulated with or without PEPCK peptide for 96 h. P Schematic showing the L. major infection model. WT mice were either naïve (no immunization), immune (recovered from infection), or immunized subcutaneously with 2 μg PEPCK mRNA-LNP 6 weeks prior to infection. Ear thickness was measured to record Q lesion size weekly for 4-weeks post-infection and R delayed-type hypersensitivity responses (DTH) in the first 48- and 72-h post-infection. Both schematic images were created with Biorender.com. Data from at least two independent experiments, n = 3–5 per experiment. Error bars indicate SD; ****P < 0.0001.
Given the substantial systemic CD4+ Th1 response, we predicted that the mRNA vaccine would protect against an infection with Leishmania major. To test this, we infected mice immunized with the PEPCK mRNA vaccine 6 wks earlier with L. major. We infected naïve mice as a control group and an additional group of mice that had resolved a primary infection with L. major (immune mice), which leads to protective immunity (Fig. 1P). As expected, the immune mice exhibited a significant decrease in lesion size compared with the controls (Fig. 1Q). However, there was only a minimal, non-significant reduction in lesion size in the PEPCK mRNA vaccinated group. Furthermore, we found that only the immune mice exhibited a DTH response to challenge infection (Fig. 1R). Since we and others found that dTrm cells were critical for developing a DTH response28,29,30,31, we speculated that while the PEPCK mRNA vaccine induced a systemic Th1 cell response, it may not have induced a robust dTrm response.
PEPCK mRNA-LNP vaccine induces the expression of skin-homing molecules and migration of CD4+ T cells to inflamed and non-inflamed skin
A key factor in the ability of T cells to become dTrm cells is the expression of skin-homing molecules, which include the expression of P and E selectin ligands (PESLs), chemokine receptors, and integrins on the T cell surface53,54,55. PESLs, chemokines, and integrin ligands are highly expressed in inflamed skin (IS), facilitating cell entry. However, T cells can also migrate into non-inflamed (NIS) skin, albeit at a much lower frequency, due to the constitutive low-level expression of P and E selectins, chemokines, and adhesion molecules56,57. The first step in T cell entry into the skin is binding to P- and E-selectins expressed on the endothelium, and therefore, we tested if the lack of a DTH response following PEPCK mRNA vaccination might be due to limited expression of these skin-homing molecules by the responding T cells. Ptg chimeras were immunized, and 1-wk later, PESLs were evaluated in the pdLN and spleen by staining Ptg cells with P and E selectin-Fc molecules and an antibody (1B11) that recognizes a glycoform of CD43 that binds to E selectin ligand58,59,60,61. The PEPCK mRNA vaccine induced a large population of T cells expressing P and E selectin ligands (Fig. 2A–C). Since the mRNA vaccine induced a substantial Tfh cell population, we were interested in whether PESLs were expressed on Tfh or non-Tfh cells. We found that non-Tfh cells preferentially expressed PESLs compared to Tfh cells in both the pdLN and the spleen (Fig. 2D, E). While the expression of PESLs on Ptg cells suggests they have the ability to bind to endothelial cells and enter the skin, successful entry to the tissue is dependent upon other molecules as well. Therefore, we next investigated if Ptg cells were indeed found in the skin after immunization. Ptg chimeras were immunized, and 1-week later we isolated cells from the footpad (IS) and the ear (NIS). Ptg cells were found in both IS and NIS (Fig. 2F–H). As expected, there were significantly more Ptg cells in the IS, although a substantial number were present in the NIS. Consistent with the expression of PESLs, none of the Ptg cells in the skin were Tfh cells (Fig. 2I). These results suggest that the Ptg cells can enter both IS and NIS. Therefore, we next tested if they remained in the skin and became dTrm cells.
A Flow cytometry analysis of P and E selectin ligands assessed by P and E selectin Fc reagents (referred to as PESL-Fc) or CD43/1B11 expression on Ptg cells in the popliteal draining lymph node (pdLN) and B spleen at 1-week post subcutaneous immunization with 2 μg PEPCK mRNA-LNP. C Absolute numbers of PESL-Fc⁺ and CD43/1B11⁺ in each tissue. D Representative plot of PD-1hi vs. CXCR5 expression on donor Ptg cells in the pdLN, histograms and frequencies of CD43/1B11⁺ cells in CXCR5⁺ and CXCR5⁻ subsets. E Same analysis as (D) performed on spleen cells. Representative flow cytometry plots of donor Ptg cells in F inflamed (IS) and G non-inflamed skin (NIS) at 1-week post-immunization. H Frequencies and absolute numbers of donor Ptg cells in inflamed and non-inflamed skin. I Representative PD-1hi vs. CXCR5 expression plots on donor Ptg cells in IS and NIS. Data from two independent experiments, n = 3 per experiment. Error bars indicate SD; ***P = 0.0004; ****P < 0.0001.
PEPCK mRNA-LNP vaccine fails to induce a globally seeded CD4+ dTrm cell population
To determine if the PEPCK mRNA vaccine induced dTrm cells, we first immunized C57BL/6 mice and, 3 wks later, evaluated the specific T cell response to PEPCK using a PEPCK tetramer. In these experiments, we tested two doses of PEPCK mRNA, 2 μg and 5 μg (Fig. 3A). and identified a large number of PEPCK-specific T cells in the IS, with no significant difference between the doses (Fig. 3B, C). However, in the NIS very few PEPCK-specific T cells were detected (Fig. 3B, C). To confirm that dose was not a factor in the development of dTrm cells in NIS, we also tested a higher mRNA vaccine dose (10 μg), which did not substantially increase the frequency or number of Ptg cells in the NIS skin (Supplementary Fig. 1). One issue in evaluating these results is that it is difficult to determine what a functionally significant number of dTrm cells in the NIS might be to mediate DTH and/or protection. However, since immunization with PEPCK peptide administered with CpG (referred here as Peptide vaccine) protects against L. major47, we compared the number and frequency of PEPCK T cells in IS and NIS following these two immunizations. We immunized PEPCK chimeras and, to further enhance the potential development of dTrm cells, mice were boosted with the same dose after 8 days (Fig. 3D). By 4-weeks the frequency and number of Ptg cells following peptide vaccine were significantly higher than in mice immunized with the PEPCK mRNA vaccine (Fig. 3E, F). Notably, there were very few Ptg cells in NIS of PEPCK mRNA immunized mice compared to the peptide vaccine.
A Experimental schematic showing subcutaneous immunization of WT mice with either 2 or 5 μg PEPCK mRNA-LNP. B Representative flow cytometry plots and C total cell numbers of PEPCK I-Ab Tetramer CD4⁺ T cells in inflamed (IS) and non-inflamed skin (NIS) after 3 weeks of either immunization dose. D Schematic showing adoptive transfer of T cells from PEPCK specific TCR transgenic mice (Ptg) cells (CD45.2+) into congenically distinct CD45.1⁺ hosts on day 0 (d0), subcutaneous immunization with either 2 μg PEPCK mRNA-LNP or peptide vaccine on day 1 (d1) and boost on day 8 (d8). E Representative flow cytometry plots comparing donor Ptg cells in IS and NIS after PEPCK mRNA or peptide vaccine and F total donor cell numbers after 4-weeks of either vaccine. Both schematic images were created with Biorender.com. Data from two independent experiments, n = 3–5 per experiment. Error bars indicate SD; ***P ≤ 0.0006.
IL-12 promotes the development of CD4+ dTrm cells in a PEPCK mRNA-LNP vaccine
IL-12 promotes the development of protective Th1-dependent immunity and upregulation of skin-homing molecules62,63,64,65,66, and the inclusion of IL-12 plasmids in vaccines generates strong T cell immunity67. Therefore, we next tested if co-delivery of IL12 mRNA-LNP with PEPCK mRNA-LNP vaccine might enhance the development of dTrm cells. We immunized Ptg chimeras with PEPCK mRNA and IL-12 mRNA. One group of mice was immunized with 2 µg PEPCK mRNA as a control, while the experimental group received 1 µg PEPCK mRNA and 1 µg IL-12 mRNA. In another control group, we immunized mice with 1 µg PEPCK mRNA and 1 µg empty LNP to control for the amount of LNP administered to the mice. We found that the inclusion of IL-12 mRNA significantly increased the systemic T cell response to PEPCK, evident in the spleen (Fig. 4A) and blood (Fig. 4B). Importantly, there was no change in the response induced by 2 µg PEPCK mRNA- LNP and 1 µg PEPCK mRNA administered with 1 µg empty LNP (Fig. 4A). Notably, in addition to this quantitative change, we found that both in the spleen (Fig. 4C) and pdLN (Fig. 4G), a higher frequency of Ptg cells expressed the canonical Trm marker, CXCR6 (Fig. 4D–J). Additionally, other markers that facilitate T cell interactions, Slamf1 and CD54, also found on memory T cells68,69, are upregulated after the inclusion of IL-12 mRNA (Fig. 4D–J). In contrast, there was a dramatic decrease in the frequency of Tfh cells, both in the pdLN and spleen, when the vaccine included IL-12 mRNA (Fig. 4D–J), consistent with previous studies70. However, this effect appears to be transient since by 4wks the Tfh cell population was restored to a similar level induced by PEPCK mRNA alone (Supplementary Fig. 2). Importantly, a study evaluating the antibody response after 42 days of SARS-CoV-2 vaccination showed significantly higher antibody titers when the vaccine was adjuvanted with IL-12p70 mRNA than in a non-adjuvanted vaccine71, suggesting that further investigation may be required to dissect the role of IL-12 mRNA in Tfh cell development and antibody responses.
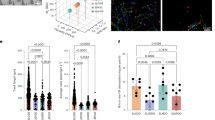
A Systemic (spleen) frequency and total cell number of donor Ptg cells expansion at 1-week post-subcutaneous immunization with either 2 μg PEPCK mRNA-LNP (blue circles), 1 μg PEPCK mRNA-LNP + 1 μg empty-LNP (blue triangles) or 1 μg PEPCK mRNA-LNP + 1 μg IL-12 mRNA-LNP (orange triangles). B Frequency of donor Ptg cells in blood at days 7, 14, 21 and 28 post-immunization with 1 μg PEPCK mRNA-LNP + 1 μg empty-LNP (blue triangles) or 1 μg PEPCK mRNA-LNP + 1 μg IL-12 mRNA-LNP (orange triangles). UMAP projections of high parameter flow cytometry data of Ptg cells in the (C) spleen at 1-week postimmunization, the source of donor Ptg cells overlayed on the projection. D The expression level of each indicated marker is overlayed on the UMAP projection, E histogram, and F frequency of indicated marker by donor Ptg cells from their respective host in the spleen. G–J Same analysis as the spleen but for popliteal draining lymph node (pdLN). K Representative flow cytometry plots comparing donor Ptg cells and total cell numbers in inflamed (IS) and noninflamed skin (NIS) after PEPCK mRNA-LNP or PEPCK + IL-12 mRNA-LNP at 1-week postimmunization. L Same analysis as (K) at 4-weeks post-immunization. 1-week data from four independent experiments, and 4-weeks data from three independent experiments, n = 3–5 per experiment. Error bars indicate SD; **P = 0.007; ***P = 0.0002; ****P < 0.0001.
To determine if these quantitative and qualitative changes in the systemic T cell response led to the generation of more dTrm cells, we assessed the presence of Ptg cells in IS and NIS at 1 and 4-wks post-immunization. We found increased Ptg cells in both skin sites at 1-wk (Fig. 4K). Notably, mice immunized with PEPCK and IL-12 mRNA-LNP had significantly more Ptg cells in the NIS at 4-weeks than mice that received PEPCK mRNA alone (Fig. 4L). The inclusion of IL-12 mRNA-LNP induced significantly higher numbers of Ptg cells in the NIS (Fig. 4K, L) and these cells express Trm canonical markers such as CXCR6 and CD69 (Supplementary Fig. 3).
PEPCK mRNA-LNP and IL-12 mRNA-LNP vaccine promote DTH and protective immunity to L. major
Since a DTH response depends on the presence of dTrm cells that globally seed the NIS28,29, we used the DTH response to measure the functionality of the dTrm cells present in NIS. We challenged Ptg chimera mice with L. major in the ear and compared groups that were either naïve or had been immunized 4-wks earlier in the footpad with PEPCK mRNA alone or in combination with IL-12 mRNA. (Fig. 5A). To assess the DTH response, we measured ear thickness 48 and 72 h post challenge. Only mice that were immunized with PEPCK mRNA plus IL-12 mRNA showed a significant DTH response (Fig. 5B). Importantly, those mice showed decreased lesion size (Fig. 5C), pathology score (Fig. 5D) and parasite burden (Fig. 5E) all indicative of protection. To confirm these results and show that this vaccine combination also enhances protection by endogenous PEPCK-specific CD4 T cells, we also challenged C57BL/6 mice with L. major that were either naïve or had been immunized with PEPCK mRNA or PEPCK mRNA and IL-12 mRNA (Fig. 5F). PEPCK mRNA and IL-12 mRNA immunized mice exhibited a significant DTH response (Fig. 5G), similar to the findings in the Ptg chimeras. As assessed by lesion size (Fig. 5H) and parasite burden (Fig. 5I), only mice immunized with PEPCK mRNA and IL-12 mRNA exhibited significant protection.
A Schematic showing the L. major infection model: adoptive transfer of T cells from PEPCK specific TCR transgenic mice (CD45.2+) into congenically distinct CD45.1⁺ hosts on day 0 (d0), which were either naïve (no immunization) or immunized subcutaneously with 1 μg PEPCK mRNA-LNP + 1 μg empty-LNP (blue triangles) or 1 μg PEPCK mRNA-LNP + 1 μg IL-12 mRNA-LNP (orange triangles) 4-weeks before infection. Ear thickness was measured to assess (B) delayed-type hypersensitivity responses in the first 48- and 72-h post-infection, (C) lesion size and (D) pathology score were recorded weekly for 4-weeks post-infection. Parasite burden was quantified in the (E) infected ear and draining lymph node at 4-weeks post-infection. F Schematic showing the L. major infection model of WT mice that were either naïve (no immunization) or immunized subcutaneously with 1 μg PEPCK mRNA-LNP + 1 μg empty LNP (blue triangles) or 1 μg PEPCK mRNA-LNP + 1 μg IL-12 mRNA-LNP (orange triangles) 4 weeks before infection. Ear thickness was measured to assess (G) delayed-type hypersensitivity responses in the first 48- and 72-h post-infection and (H) lesion size was recorded weekly for 4-weeks post-infection. Parasite burden was quantified in the (I) infected ear and draining lymph node at 4-weeks post-infection. Both schematic images were created with Biorender.com. Data from three independent experiments, n = 5 mice per group. Error bars indicate SD; *P = 0.05; **P 0.002; ****P < 0.0001.
The findings of this study highlight the potential and limitations of mRNA-LNP vaccines. These vaccines elicit strong protective antibody responses and robust Tfh cell populations. However, while the PEPCK mRNA vaccine generated a robust systemic Th1 cell response, it failed to promote the development of dTrm cells or provide protection against L. major. Notably, these results are consistent with prior observations that mRNA vaccines often fail to induce a population of Trm cells, leading to exploring strategies to enhance mRNA-induced Trm cells72,73,74,75,76,77. Our studies found that this limitation was overcome by co-administration of IL-12 mRNA with the PEPCK mRNA vaccine, demonstrating a critical role for IL-12 in CD4+ dTrm cell induction. While there have been conflicting roles reported for IL-12 and T-bet in T cell memory responses78,79, it is clear that IL-12 promotes CD4+ Th1-skewed immunity63,80,81 and CD8+ T cell memory82. Additionally, consistent with previous observations, T-bet is required for vaccine-induced memory T cells and for generating hepatic CD4+ Trm cells83,84. A critical factor in the development of dTrm cells is the ability of T cells to enter the skin, and PESL expression is one critical step in that process. Importantly, IL-12 promotes increased expression of PESLs on T cells, further emphasizing its importance in dTrm cell development65,85. It is important to point out, however, that CD4+ T cells are divided into several subsets with distinct functions, and a limitation of our studies is that we only focused on generating CD4+ dTrm cells that are biased towards a Th1 phenotype. CD8+ dTrm cells expressing IFN-g and IL-17 differ in their developmental pathway86, and the same is likely to hold true for CD4+ dTrm cells. Thus, we anticipate that adjuvants and/or different LNPs must be specifically tailored to generate specific types of CD4+ Trm cells. We have not determined how long the dTrm cells generated by this persist, or whether other adjuvants can similarly enhance dTrm cells development, both of which are additional limitations of this study. Ongoing research continues to refine our understanding of Trm cells7,11,69,86,87,88, promising further insights into dTrm cells in the future. An additional limitation of this study is that it has not assessed the ability of homologous or heterologous boosting at different time points and/or via different routes of administration to promote dTrm cells. Nevertheless, the findings presented here contribute to this growing body of knowledge and underscore the efficacy of incorporating IL-12 to enhance the generation of CD4+ Th1 biased dTrm cells, thus paving the way for developing more effective tissue-targeted vaccine strategies.
Methods
Ethics statement
All animals were used in accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health and the guidelines of the University of Pennsylvania Institutional Animal Use and Care Committee. The Institutional Animal Use and Care Committee approved the protocol.
Anesthesia/Euthanasia of mice
Mice were anesthetized by placing them in a plexiglass chamber with 4% isoflurane, USP (#NDC: 11695-6777-2, covetrus, Dublin, OH, USA) for 4 min, or until fully sedated measured by lack of paw reflex and proceed to any injection. When euthanatized, mice were left in a Crainey Tech chamber with displacement of air with 100% CO2 for at least two minutes after respiration ceased. Then a cervical dislocation was performed to confirm death and proceed to tissue collection.
Mice and T cell transfer
Six-week-old female C57BL/6 and CD45.1 mice were purchased from Charles River and housed in the University of Pennsylvania Animal Care Facilities for 1–2 weeks before use. PEPCK-specific TCR transgenic mice (kindly provided by Dr Jude Uzonna) were bred in the University of Pennsylvania Animal Care Facilities. To create PEPCK chimera, spleen cells from PEPCK-specific TCR transgenic mice were collected, erythrocytes lysed with ACK lysing buffer (Quality Biological, Cat #118-156-101), and CD4+ T cells enriched using a magnetic bead separation kit (Miltenyi Biotec, Cat #130-104-075), 1 × 105 Ptg cells in 100 μL of dPBS were transferred by retroorbital injection into recipient mice.
Parasite culture and intradermal infection
L. major parasites (strain WHO/MHOM/IL/80/Friedlin) were grown in Schneider’s insect medium (GIBCO) supplemented with 20% heat-inactivated fetal bovine serum (FBS), 2 mM glutamine, 100 U/mL penicillin, and 100 mg/mL streptomycin per mL. Infective-stage promastigotes (metacyclics) were isolated from 4 to 5-day-old stationary culture by density gradient separation using Ficoll (Sigma-Aldrich, Cat #F9378). Mice were infected with 1 × 105 L. major metacyclics intradermally in the left ear. Lesion sizes were recorded weekly by measuring ear thickness with a digital caliper (Fisher Scientific). DTH was assessed by measuring ear thickness during the first 3 days of infection and compared with control infected mice that had not been immunized.
mRNA design and synthesis
The phosphoenolpyruvate carboxykinase (PEPCK)47 and IL-12 cytokine (IL-12) amino acid sequences underwent codon optimization and GC enrichment using our proprietary algorithm to improve expression and reduce potential immunogenicity of the in vitro transcribed mRNA. The codon optimized sequences were gene synthetized by Genscript, cloned into our proprietary in vitro transcription template containing an optimized T7 promoter, 3’UTR, 5’UTR and a 100-adenine tail. The PEPCK and IL-12 nucleoside modified mRNA sequences were prepared using the MegaScript transcription kit (ThermoFisher Scientific), co-transcriptionally capped using the 3’OMe CleanCap™ system (TriLink Biotechnologies) and purified using a modified cellulose-based chromatography89, precipitated, eluted in nuclease free water, and quantified using the NanoDrop One system. Length and integrity were determined using the Agilent BioAnalyzer 2100 system. Endotoxin content was measured using the GenScript Toxisensor chromogenic assay, and values were below detection levels (0.1 EU/mL). mRNA was stored at −20 °C until formulation.
mRNA-LNP production and characterization
Purified mRNAs were formulated into lipid nanoparticles using a self-assembly process wherein an ethanolic lipid mixture of an ionizable cationic lipid, phosphatidylcholine, cholesterol, and polyethylene glycol-lipid was rapidly combined with an aqueous solution containing mRNA at acidic pH as previously described90. The ionizable cationic lipid (pKa in the range of 6.0–6.5, proprietary to Acuitas Therapeutics) and LNP composition are described in the patent application WO 2017/004143. The hydrodynamic size, polydispersity index (PDI) and zeta potential of mRNA-LNPs were measured using a Zetasizer Nano ZS90 (Malvern Instruments, Malvern, UK). The mRNA encapsulation efficiency was determined using a modified Quant-iT RiboGreen RNA assay (Invitrogen). Endotoxin levels were determined using the Limulus Amebocyte Lysate (LAL) chromogenic assay, found to be <0.5 endotoxin unit (EU)/mL.
Immunizations
All mice were immunized subcutaneously (s.c.) in their left footpad with the indicated dose of mRNA-LNP in 50 μL of PBS or 50 μL PBS alone as a control. In mice vaccinated with PEPCK mRNA LNP and IL-12 mRNA LNP, particles were mixed so that an equivalent LNP and antigen were given between groups82. Peptide-immunized mice received PEPCK peptide (10 μg), CpG (50 μg), and rmIL-12 (0.5 μg) given in the footpad. Mice that received PEPCK T-cells were immunized 24 h later.
Tissue processing
To prepare a single-cell suspension of the skin samples, the dorsal and ventral layers of the ear were split while the footpad was cut into several pieces in a 24-well plate with 500 μl/well of incomplete RPMI with 250 mg/mL of Liberase (Roche, Cat #05401054001) and 10 mg/mL of DNase I (Sigma-Aldrich, Cat #4536282001) for 90 min (ear) or 120 min (footpad) at 37 °C, 5% CO2. The enzymatic reaction was stopped with 1 mL of RPMI supplemented with 10% FBS. The digested tissues were dissociated using a cell strainer (40 mm) in PBS containing 0.05% BSA and 20 mM EDTA (Invitrogen, Cat #130-104-075). pdLNs and spleen were homogenized using a cell strainer (40 μm Falcon). Red blood cells were lysed when required. Cells were washed for 5 min at 1200 rpm to obtain single-cell suspensions.
ELISA
Splenocytes were incubated for 96 hours with 5 nM PEPCK peptide (Selleckchem) and supernatants were frozen at −20 °C until assayed by ELISA. IFN-γ production was assessed using a Immulon 2HB flat-bottom 96-well plate (ThermoFisher, 3855) coated with 0.5 mg/mL anti-mouse IFN-γ clone AN-18 (eBioscience, 14-7313-85) in 1X dPBS at 4 °C overnight. Standards were prepared by diluting recombinant IFN-γ (Biolegend, 575308) in assay media at a max concentration of 1000 pg/mL with 2-fold serial dilutions. Samples were added at the appropriate dilution in assay media and incubated for 120 min at 37 °C. 100 μL of biotinylated anti-mouse IFN-γ clone R46A2 (eBioscience, 13-7312-85) in 1x dPBS + 5% NCS was added at a concentration of 1 μg/mL and incubated for 60 min at 37 °C. Peroxidase-conjugated Streptadivin (Jackson-Immuno Research, 016-030-084) diluted 1000-fold in 1x dPBS + 5% NCS was added at 100 μL/well. The plate was developed using 100 μL of ABTS peroxidase substrate (SeraCare, 5120-0041) per well. The reaction was read at 405 nm. Between each step, the plate was washed at least 5 times with 1X dPBS containing 0.05% Tween 20 (Sigma®). Only samples with PEPCK antigen stimulation were diluted four times, and this dilution factor was used when calculating final IFN-γ levels.
Flow cytometry staining
For intracellular staining, single-cell suspensions were stimulated in vitro with PMA (50 ng/mL), ionomycin (500 ng/mL; Sigma-Aldrich, St Louis, MO, USA), and brefeldin A (BioLegend, San Diego, CA, USA) for three hours. Cells were washed in FACS buffer, and the pellet was further washed and stained using the Foxp3/Transcription factor Fixation/Permeabilization kit (eBioscience™). Surface staining in FACS buffer. The antibodies used were: CD45.2 (104, eBiosciences), CD69 (H1.2F3, eBiosciences), CD150 (TC15-12F12.2, eBiosciences), CD4 (RM4-5, eBiosciences), CD62L (MEL-14, eBiosciences), CD186/CXCR6 (SA051D1, eBiosciences), PD-1 (29F.1A12, eBiosciences), CD44 (IM7, eBiosciences), CD54 (YN1/1.7.4, eBiosciences), CD43 (1B11, eBiosciences), CXCR5 (L138D7, eBiosciences), IFN-γ (XMG1.2, eBiosciences), T-bet (4B10, eBiosciences), Foxp3 (FJK-16s, eBiosciences), Purified Mouse P-Selectin - IgG Fusion Protein (R&D) and Recombinant Mouse E-Selectin/CD62E Fc Chimera Protein (R&D). Cell acquisition was performed on a BD FACSymphony™ A3 flow cytometer (BD Biosciences, San Jose, CA, USA), and the data were processed using FlowJo software (Tree Star, Ashland, OR, USA). For cell counting from skin tissue, AccuCount fluorescent particles were added before flow cytometry acquisition (Spherotech, Lake Forest, IL, USA).
Assessment of parasite burden
Ear cell suspensions were centrifuged at 3000 rpm for 10 min. The cell pellet was resuspended in 400 μL of completed Schneider’s insect medium and used for parasite titration. LNs were collected, and single-cell suspensions were used for parasite quantitation. The homogenates were serially diluted (1:5) in 96-well plates and incubated at 26 °C. The number of viable parasites was calculated from the highest dilution at which parasites were observed after 7 days of incubation.
UMAP analysis
The FlowJo UMAP plug-in version 4.0.386 was used to generate UMAP projections of flow cytometry data. Prior to UMAP analysis, keywords were used to label features of interest for each sample (for example, target cell population, tissue, immunization) to preserve them during concatenation, and populations of interest were concatenated using FlowJo’s concatenate function. UMAP analysis was then run using all parameters except those used for negative selection.
Statistical analysis
Statistics were performed using GraphPad Prism Version 10.2.2 statistical analysis software. For normally distributed data, comparing two groups along a single variable, a standard Student’s t test was used. A Mann–Whitney Rank Sum Test was used if the data was abnormally distributed. When comparing two groups along more than one variable, an Ordinary One-Way ANOVA with a Dunnett’ s multiple comparisons test was used. P-values less than 0.05 were considered significant.
Data availability
The data supporting the findings of this study are available within the article and the main figures or its supplementary materials. Raw flow cytometry data demonstrated in the figures and used to generate plots are available upon request from the corresponding author (P.S.).
References
Schenkel, J. M. & Masopust, D. Tissue-resident memory T cells. Immunity 41, 886–897 (2014).
Park, C. O. & Kupper, T. S. The emerging role of resident memory T cells in protective immunity and inflammatory disease. Nat. Med. 21, 688–697 (2015).
Mueller, S. N. & Mackay, L. K. Tissue-resident memory T cells: local specialists in immune defence. Nat. Rev. Immunol. 16, 79–89 (2016).
van Gisbergen, K., Zens, K. D. & Munz, C. T-cell memory in tissues. Eur. J. Immunol. 51, 1310–1324 (2021).
Clark, R. A. Resident memory T cells in human health and disease. Sci. Transl. Med. 7, 269rv261 (2015).
Weisberg, S. P., Ural, B. B. & Farber, D. L. Tissue-specific immunity for a changing world. Cell 184, 1517–1529 (2021).
Buggert, M., Price, D. A., Mackay, L. K. & Betts, M. R. Human circulating and tissue-resident memory CD8(+) T cells. Nat. Immunol. 24, 1076–1086 (2023).
Masopust, D. & Soerens, A. G. Tissue-resident T cells and other resident leukocytes. Annu. Rev. Immunol. 37, 521–546 (2019).
Lam, N., Lee, Y. & Farber, D. L. A guide to adaptive immune memory. Nat. Rev. Immunol. 24, 810–829 (2024).
Hondowicz, B. D. et al. Interleukin-2-dependent allergen-specific tissue-resident memory cells drive asthma. Immunity 44, 155–166 (2016).
Christo, S. N., Park, S. L., Mueller, S. N. & Mackay, L. K. The multifaceted role of tissue-resident memory T cells. Annu. Rev. Immunol. 42, 317–345 (2024).
Buquicchio, F. A. et al. Distinct epigenomic landscapes underlie tissue-specific memory T cell differentiation. Immunity 57, 2202–2215 e2206 (2024).
Mackay, L. K. & Kallies, A. Transcriptional regulation of tissue-resident lymphocytes. Trends Immunol. 38, 94–103 (2017).
Beura, L. K. et al. CD4(+) resident memory T cells dominate immunosurveillance and orchestrate local recall responses. J. Exp. Med. 216, 1214–1229 (2019).
Carbone, F. R. & Gebhardt, T. Should I stay or should I go-Reconciling clashing perspectives on CD4(+) tissue-resident memory T cells. Sci. Immunol. 4, eaax5595 (2019).
Klicznik, M. M. et al. Human CD4(+)CD103(+) cutaneous resident memory T cells are found in the circulation of healthy individuals. Sci. Immunol. 4, eaav8995 (2019).
Fonseca, R. et al. Developmental plasticity allows outside-in immune responses by resident memory T cells. Nat. Immunol. 21, 412–421 (2020).
Bromley, S. K., Yan, S., Tomura, M., Kanagawa, O. & Luster, A. D. Recirculating memory T cells are a unique subset of CD4+ T cells with a distinct phenotype and migratory pattern. J. Immunol. 190, 970–976 (2013).
Turner, D. L. & Farber, D. L. Mucosal resident memory CD4 T cells in protection and immunopathology. Front. Immunol. 5, 331 (2014).
Schenkel, J. M., Fraser, K. A., Vezys, V. & Masopust, D. Sensing and alarm function of resident memory CD8(+) T cells. Nat. Immunol. 14, 509–513 (2013).
Ariotti, S. et al. T cell memory. Skin-resident memory CD8⁺ T cells trigger a state of tissue-wide pathogen alert. Science 346, 101–105 (2014).
Teijaro, J. R. et al. Cutting edge: Tissue-retentive lung memory CD4 T cells mediate optimal protection to respiratory virus infection. J. Immunol. 187, 5510–5514 (2011).
Rotrosen, E. & Kupper, T. S. Assessing the generation of tissue resident memory T cells by vaccines. Nat. Rev. Immunol. 23, 655–665 (2023).
Gray, J. I., Westerhof, L. M. & MacLeod, M. K. L. The roles of resident, central and effector memory CD4 T-cells in protective immunity following infection or vaccination. Immunology 154, 574–581 (2018).
Wilk, M. M. & Mills, K. H. G. CD4 T(RM) Cells Following Infection and Immunization: implications for More Effective Vaccine Design. Front. Immunol. 9, 1860 (2018).
Hassert, M. & Harty, J. T. Tissue resident memory T cells- A new benchmark for the induction of vaccine-induced mucosal immunity. Front. Immunol. 13, 1039194 (2022).
Jiang, X. et al. Skin infection generates non-migratory memory CD8+ T(RM) cells providing global skin immunity. Nature 483, 227–231 (2012).
Murata, A. & Hayashi, S. I. CD4(+) resident memory T cells mediate long-term local skin immune memory of contact hypersensitivity in BALB/c Mice. Front. Immunol. 11, 775 (2020).
Glennie, N. D., Volk, S. W. & Scott, P. Skin-resident CD4+ T cells protect against Leishmania major by recruiting and activating inflammatory monocytes. PLoS Pathog. 13, e1006349 (2017).
Shah, P. N. et al. Systemic and skin-limited delayed-type drug hypersensitivity reactions associate with distinct resident and recruited T cell subsets. J. Clin. Invest. 134, e178253 (2024).
Trubiano, J. A. et al. Analysis of skin-resident memory T cells following drug hypersensitivity reactions. J. Invest. Dermatol. 140, 1442–1445 e1444 (2020).
Clark, R. A. et al. The vast majority of CLA+ T cells are resident in normal skin. J. Immunol. 176, 4431–4439 (2006).
Szabo, P. A., Miron, M., Farber, D. L. Location, location, location: tissue resident memory T cells in mice and humans. Sci. Immunol. 4, eaas9673 (2019).
Beura, L. K. et al. Normalizing the environment recapitulates adult human immune traits in laboratory mice. Nature 532, 512–516 (2016).
Jirmanus, L. et al. Epidemiological and clinical changes in American tegumentary leishmaniasis in an area of Leishmania (Viannia) braziliensis transmission over a 20-year period. Am. J. Trop. Med. Hyg. 86, 426–433 (2012).
Scorza, B. M., Carvalho, E. M. & Wilson, M. E. Cutaneous manifestations of human and murine leishmaniasis. Int. J. Mol. Sci. 18, 1296 (2017).
Wells, T. J., Esposito, T., Henderson, I. R. & Labzin, L. I. Mechanisms of antibody-dependent enhancement of infectious disease. Nat. Rev. Immunol. 25, 6–21 (2025).
Buxbaum, L. U. & Scott, P. Interleukin 10- and Fcgamma receptor-deficient mice resolve Leishmania mexicana lesions. Infect. Immun. 73, 2101–2108 (2005).
Scott, P. & Novais, F. O. Cutaneous leishmaniasis: immune responses in protection and pathogenesis. Nat. Rev. Immunol. 16, 581–592 (2016).
Glennie, N. D. et al. Skin-resident memory CD4+ T cells enhance protection against Leishmania major infection. J. Exp. Med 212, 1405–1414 (2015).
Glennie, N. D. & Scott, P. Memory T cells in cutaneous leishmaniasis. Cell. Immunol. 309, 50–54 (2016).
Laczkó, D. et al. A single immunization with nucleoside-modified mRNA vaccines elicits strong cellular and humoral immune responses against SARS-CoV-2 in mice. Immunity 53, 724–732.e727 (2020).
Alameh, M. G., Weissman, D., Pardi, N. Messenger RNA-based vaccines against infectious diseases. Curr. Top. Microbiol. Immunol. 440, 111–145 (2022).
Knudson, C. J. et al. Lipid-nanoparticle-encapsulated mRNA vaccines induce protective memory CD8 T cells against a lethal viral infection. Mol. Ther. 29, 2769–2781 (2021).
Painter, M. M. et al. Rapid induction of antigen-specific CD4(+) T cells is associated with coordinated humoral and cellular immunity to SARS-CoV-2 mRNA vaccination. Immunity 54, 2133–2142 e2133 (2021).
Wherry, E. J. & Barouch, D. H. T cell immunity to COVID-19 vaccines. Science 377, 821–822 (2022).
Mou, Z. et al. Identification of broadly conserved cross-species protective Leishmania antigen and its responding CD4+ T cells. Sci. Transl. Med. 7, 310ra167 (2015).
Louis, L. et al. Intradermal synthetic DNA vaccination generates leishmania-specific T cells in the skin and protection against Leishmania major. Infect. Immun. 87, e00227–19 (2019).
Pan, Y. et al. Epicutaneous immunization with modified vaccinia Ankara viral vectors generates superior T cell immunity against a respiratory viral challenge. NPJ Vaccines 6, 1 (2021).
Gupta, G. et al. The long pentraxin 3 (PTX3) suppresses immunity to cutaneous leishmaniasis by regulating CD4(+) T helper cell response. Cell Rep. 33, 108513 (2020).
Zaph, C., Uzonna, J., Beverley, S. M. & Scott, P. Central memory T cells mediate long-term immunity to Leishmania major in the absence of persistent parasites. Nat. Med. 10, 1104–1110 (2004).
Alameh, M. G. et al. Lipid nanoparticles enhance the efficacy of mRNA and protein subunit vaccines by inducing robust T follicular helper cell and humoral responses. Immunity 54, 2877–2892 e2877 (2021).
Moreau, J. M., Gouirand, V. & Rosenblum, M. D. T-Cell Adhesion in Healthy and Inflamed Skin. JID Innov. 1, 100014 (2021).
Masopust, D. & Schenkel, J. M. The integration of T cell migration, differentiation and function. Nat. Rev. Immunol. 13, 309–320 (2013).
von Andrian, U. H. & Mackay, C. R. T-cell function and migration. Two sides of the same coin. N. Engl. J. Med. 343, 1020–1034 (2000).
Chong, B. F., Murphy, J. E., Kupper, T. S. & Fuhlbrigge, R. C. E-selectin, thymus- and activation-regulated chemokine/CCL17, and intercellular adhesion molecule-1 are constitutively coexpressed in dermal microvessels: a foundation for a cutaneous immunosurveillance system. J. Immunol. 172, 1575–1581 (2004).
Agrewala, J. N. et al. Unique ability of activated CD4+ T cells but not rested effectors to migrate to non-lymphoid sites in the absence of inflammation. J. Biol. Chem. 282, 6106–6115 (2007).
Matsumoto, M. et al. CD43 collaborates with P-selectin glycoprotein ligand-1 to mediate E-selectin-dependent T cell migration into inflamed skin. J. Immunol. 178, 2499–2506 (2007).
Matsumoto, M. et al. CD43 functions as a ligand for E-Selectin on activated T cells. J. Immunol. 175, 8042–8050 (2005).
Alcaide, P. et al. The 130-kDa glycoform of CD43 functions as an E-selectin ligand for activated Th1 cells in vitro and in delayed-type hypersensitivity reactions in vivo. J. Invest. Dermatol. 127, 1964–1972 (2007).
Clark, M. C. & Baum, L. G. T cells modulate glycans on CD43 and CD45 during development and activation, signal regulation, and survival. Ann. N. Y. Acad. Sci. 1253, 58–67 (2012).
Hsieh, C. S. et al. Development of TH1 CD4+ T cells through IL-12 produced by Listeria-induced macrophages. Science 260, 547–549 (1993).
Afonso, L. C. et al. The adjuvant effect of interleukin-12 in a vaccine against Leishmania major. Science 263, 235–237 (1994).
Scott, P. & Trinchieri, G. IL-12 as an adjuvant for cell-mediated immunity. Semin. Immunol. 9, 285–291 (1997).
Ebel, M. E., Awe, O., Kaplan, M. H. & Kansas, G. S. Diverse inflammatory cytokines induce selectin ligand expression on murine CD4 T cells via p38α MAPK. J. Immunol. 194, 5781–5788 (2015).
Stobie, L. et al. The role of antigen and IL-12 in sustaining Th1 memory cells in vivo: IL-12 is required to maintain memory/effector Th1 cells sufficient to mediate protection to an infectious parasite challenge. Proc. Natl Acad. Sci. USA 97, 8427–8432 (2000).
Chattergoon, M. A. et al. Co-immunization with plasmid IL-12 generates a strong T-cell memory response in mice. Vaccine 22, 1744–1750 (2004).
Kohlmeier, J. E., Chan, M. A. & Benedict, S. H. Costimulation of naive human CD4 T cells through intercellular adhesion molecule-1 promotes differentiation to a memory phenotype that is not strictly the result of multiple rounds of cell division. Immunology 118, 549–558 (2006).
Nguyen, Q. P. et al. Transcriptional programming of CD4+ TRM differentiation in viral infection balances effector- and memory-associated gene expression. Sci. Immunol. 8, eabq7486 (2023).
Elsner, R. A. & Shlomchik, M. J. IL-12 blocks Tfh cell differentiation during salmonella infection, thereby contributing to germinal center suppression. Cell Rep. 29, 2796–2809 e2795 (2019).
Brook, B. et al. Adjuvantation of a SARS-CoV-2 mRNA vaccine with controlled tissue-specific expression of an mRNA encoding IL-12p70. Sci. Transl. Med. 16, eadm8451 (2024).
Pieren, D. K. J. et al. Limited induction of polyfunctional lung-resident memory T cells against SARS-CoV-2 by mRNA vaccination compared to infection. Nat. Commun. 14, 1887 (2023).
Nakamae, S. et al. Induction of liver-resident memory T cells and protection at liver-stage malaria by mRNA-containing lipid nanoparticles. Front. Immunol. 14, 1116299 (2023).
Kunzli, M. et al. Route of self-amplifying mRNA vaccination modulates the establishment of pulmonary resident memory CD8 and CD4 T cells. Sci. Immunol. 7, eadd3075 (2022).
Lapuente, D. et al. Protective mucosal immunity against SARS-CoV-2 after heterologous systemic prime-mucosal boost immunization. Nat. Commun. 12, 6871 (2021).
Ganley, M. et al. mRNA vaccine against malaria tailored for liver-resident memory T cells. Nat. Immunol. 24, 1487–1498 (2023).
Tang, J. et al. Respiratory mucosal immunity against SARS-CoV-2 after mRNA vaccination. Sci. Immunol. 7, eadd4853 (2022).
Pearce, E. L. & Shen, H. Generation of CD8 T cell memory is regulated by IL-12. J. Immunol. 179, 2074–2081 (2007).
Marshall, H. D. et al. Differential expression of Ly6C and T-bet distinguish effector and memory Th1 CD4(+) cell properties during viral infection. Immunity 35, 633–646 (2011).
Gurunathan, S. et al. Vaccination with DNA encoding the immunodominant LACK parasite antigen confers protective immunity to mice infected with Leishmania major. J. Exp. Med. 186, 1137–1147 (1997).
Park, A. Y. & Scott, P. Il-12: keeping cell-mediated immunity alive. Scand. J. Immunol. 53, 529–532 (2001).
Aunins, E. A. et al. An IL-12 mRNA-LNP adjuvant enhances mRNA vaccine induced CD8+ T cell responses. Sci. Immunol. 10, eads1328 (2025).
Ivanova, D. L. et al. Vaccine adjuvant-elicited CD8(+) T cell immunity is co-dependent on T-bet and FOXO1. Cell Rep. 42, 112911 (2023).
Depew, C. E. et al. Cutting edge: optimal formation of hepatic tissue-resident memory CD4 T cells requires T-bet regulation of CD18. J. Immunol. 211, 180–185 (2023).
Underhill, G. H. et al. A crucial role for T-bet in selectin ligand expression in T helper 1 (Th1) cells. Blood 106, 3867–3873 (2005).
Park, S. L. et al. Divergent molecular networks program functionally distinct CD8(+) skin-resident memory T cells. Science 382, 1073–1079 (2023).
Scott, M. C. et al. Deep profiling deconstructs features associated with memory CD8(+) T cell tissue residence. Immunity, 58, 162–181.e10 (2025).
Evrard, M. et al. Single-cell protein expression profiling resolves circulating and resident memory T cell diversity across tissues and infection contexts. Immunity 56, 1664–1680 e1669 (2023).
Baiersdorfer, M. et al. A facile method for the removal of dsRNA contaminant from in vitro-transcribed mRNA. Mol. Ther. Nucleic Acids 15, 26–35 (2019).
Muramatsu, H. et al. Lyophilization provides long-term stability for a lipid nanoparticle-formulated, nucleoside-modified mRNA vaccine. Mol. Ther. 30, 1941–1951 (2022).
Acknowledgements
The authors acknowledge and thank the support of the Penn University Laboratory Animal Resources (ULAR); the Penn Institute for RNA Innovation; and the Penn Cytomics and Cell Sorting Shared Resource Laboratory at the University of Pennsylvania. We also thank the NIH Tetramer Core Facility for providing the PEPCK I-Ab Tetramer. This work was performed under the financial support of National Institutes of Health grant RO1 AI 189513 (to P.S.).
Author information
Authors and Affiliations
Contributions
Conceptualization: P.S., C.G.L. Methodology: A.Z.P., C.G.L., E.A.A., A.T.P. Investigation: A.Z.P., C.G.L., P.S. Visualization: A.Z.P. Writing—original draft: A.Z.P., P.S. Writing—review & editing: A.Z.P., C.G.L., M.G.A., L.A.S., A.T.P., E.A.A., Y.K.T., Z.M., J.E.U., D.W., C.A.H., P.S. Supervision, Funding Acquisition and Project administration: P.S.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zabala-Peñafiel, A., Gonzalez-Lombana, C., Alameh, MG. et al. IL-12 mRNA-LNP promotes dermal resident memory CD4+ T cell development. npj Vaccines 10, 154 (2025). https://doi.org/10.1038/s41541-025-01213-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41541-025-01213-x