Abstract
Most patients with alcohol-associated liver disease (ALD) engage in heavy drinking defined as 4 or more drinks per day (56 g) or 8 (112 g) or more drinks per week for women and 5 or more drinks per day (70 g) or 15 (210 g) or more drinks per week for men. Although abstinence from alcohol after diagnosis of ALD improves life expectancy and reduces the risk of decompensation of liver disease, few studies have evaluated whether treatment of alcohol use disorders will reduce progression of liver disease and improve liver-related outcomes. In November 2021, the National Institute of Alcohol Abuse and Alcoholism commissioned a task force that included hepatologists, addiction medicine specialists, statisticians, clinical trialists and members of regulatory agencies to develop recommendations for the design and conduct of clinical trials to evaluate the effect of alcohol use, particularly treatment to reduce or eliminate alcohol use in patients with ALD. The task force conducted extensive reviews of relevant literature on alcohol use disorders and ALD. Findings were presented at one in-person meeting and discussed over the next 16 months to develop the final recommendations. As few clinical trials directly address this topic, the 28 recommendations approved by all members of the task force represent a consensus of expert opinions.
Similar content being viewed by others
Introduction
Alcohol-associated liver disease (ALD) is the main cause of liver-related morbidity and mortality worldwide. Globally, 47% of liver-related deaths in 2016 were estimated to be attributable to alcohol1. In the USA, a report from the National Institute on Alcohol Abuse and Alcoholism (NIAAA) showed that 52% of cirrhosis-related deaths in 2019 were attributable to alcohol2. Most patients with ALD engage in heavy drinking defined by the NIAAA and the Centers for Disease Control and Prevention (CDC) as 4 or more drinks (56 g) on any given day or 8 drinks (112 g) or more per week for women and 5 or more drinks (70 g) on any given day or 15 drinks (210 g) or more per week for men over an extended period3. The WHO defines low-risk drinking as <40 g per day for men and <20 g per day for women equivalent to <280 g per week for men and <140 g per week for women4. The WHO drinking levels and the NIAAA/CDC definition of heavy drinking were created in 2000 and 2005, respectively. The reference to men and women was based on sex at birth — preferred gender was not accounted for in these definitions. Approximately 75–80% of patients with ALD also meet criteria for alcohol use disorder (AUD)5,6,7. Continued consumption of alcohol ≥280 g per week after a diagnosis of advanced liver disease increased all-cause mortality (HR 1.98; 95% CI (1.21–3.24)) and the risk of decompensated liver disease (HR 1.62; 95% CI (1.02–2.56))8. Conversely, abstinence is associated with improved life expectancy and in some cases recompensation5,9,10. Although these findings are widely acknowledged, and might be incorporated into clinical care, relatively few studies have incorporated active treatment of AUD or other interventions to reduce or eliminate heavy alcohol consumption in this population as a strategy to prevent or reduce progression of ALD.
Studies designed to address heavy drinking and AUD in patients with ALD should incorporate methods, measures and outcomes from both research arenas to achieve the highest quality studies11,12. Likewise, ALD clinical trials should integrate AUD research methods, because alcohol use strongly influences biomedical, psychosocial and quality-of-life outcomes for patients with ALD. In this Consensus Statement, an international multidisciplinary group of experts, commissioned by the NIAAA, developed consensus statements and recommendations on how to define and combine best investigative and clinical practices for both AUD and ALD in single clinical trials in which the intervention targets reduction or elimination of alcohol use in patients with ALD or in which the intervention directly targets liver function in ALD without an intended direct effect on alcohol use. Evidence from observational studies suggests that reducing alcohol use should improve both liver-related and alcohol-related outcomes in patients with ALD, but this hypothesis requires empirical confirmation and clinical trials are urgently needed9,10.
Methods
In November 2021, the NIAAA commissioned a task force to develop guidance for studying treatment of AUD in patients with ALD. Members of the task force were selected by the organizing committee (L.E.N., M.C.M. and S.R.) appointed by the NIAAA, based on having expertise in design and conduct of clinical trials for the treatment of AUD or ALD or experience in randomized clinical trial (RCT) methodology. Selection of members and subsequent recommendations were not intended to represent the views of any professional societies, specific geographical representation, drug regulatory agencies, the NIAAA or other funding organizations. The task force included hepatologists, addiction medicine specialists, statisticians, clinical trialists and members of regulatory agencies. The task force was organized, met virtually on four occasions during the winter and spring of 2022 before an in-person meeting in July 2022 at which individual task force members presented a review of the published literature in their area of expertise along with recommendations for how to incorporate these findings into the design of trials to treat AUD in patients with ALD emphasizing how to evaluate the effect of treatment on the progression of liver disease. Following the meeting, the task force divided into subgroups to develop specific recommendations and guidelines (AUD: K.W. (Chair) with B.C., S.D., N.D., A.F.D., D.E.F., A.C.F., M.N.G., L.L., R.L., M.R.L., M.E.M., A.J.S., N.L.S. and K.W.; ALD: B.P.L. (Chair) with M.N.G., A.J.S., M.R.T., S.D., A.L., M.R.L., T.G.C., N.A.T., N.L.S., R.B., A.K.S., E.C.V., P.S.K. and F.A.A.; RCT methodology: J.M. (Chair) with A.C.F., R.B., S.D., K.S.D., L.E.N., M.C.M. and S.R. (organizers) met with all subgroups). Each of the subgroups met virtually on two or more occasions during 2022 to prepare consensus recommendations, which were then endorsed by all members of the subgroups. The proposed recommendations were integrated by the subgroup chairs (B.P.L., K.W. and J.M.) for review by the entire task force at virtual meetings in March and June of 2023. Preliminary recommendations were submitted in written form to each member to provide edits and suggestions that were incorporated into the final recommendations that were sent to each member of the task force for approval. Each member of the task force contributed suggested changes to the concepts, the recommendations and the specific wording of the text that were circulated to all members of the task force for review and approval, seeking universal consensus. This iterative process was guided by the National Institutes of Health consensus development programme as revised by the Institute of Medicine (now National Academy of Medicine USA)13. However, the process did not employ the Delphi method or other formal methods for anonymous voting. The final recommendations including clarifications and edits during the review process are reported in this manuscript (Table 1).
Definitions
Heavy drinking and alcohol use disorder
-
Recommendation numbers 1–2
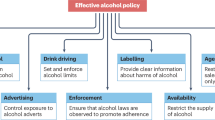
Alcohol use should be quantified based on the number of standard drinks, frequency and duration of drinking. Given that the quantity of ethanol in a standard drink varies by country, standard drinks should be converted to grams of ethanol in research studies to provide global uniformity and comparability. Quantification of alcohol use, including past use and changes over time, is important because alcohol exposure is the central factor in the aetiology and diagnosis of ALD14, as well as treatment responses and clinical outcomes. For those trials in which interventions primarily target liver function, accurate measurement of alcohol use is essential to account for a major driver of liver-related outcomes: alcohol use. The WHO defines four sex-specific levels of drinking, based on average grams of alcohol consumed per day, that correspond to low (1–40 g per day male individuals; 1–20 g per day female individuals), medium (41–60 g per day male individuals; 21–40 g per day female individuals), high (61–100 g per day male individuals; 41–60 g per day female individuals) or very high risk (>100 g per day male individuals; >60 g per day for female individuals)4. NIAAA-defined and CDC-defined heavy drinking levels correspond approximately to the WHO levels of drinking above low risk (Fig. 1). Reducing drinking by at least one or two WHO risk drinking levels is associated with considerable improvement in how patients feel and function, including reductions in risk of ALD15 and improvements in liver tests16. Recommendations for quantifying alcohol consumption are outlined in Table 2.
The level of alcohol consumption in gram per week is shown for male (blue) and female (pink) individuals according to the multisociety Delphi consensus statement by Rinella et al. (2023)26 for metabolic dysfunction-associated steatotic liver disease (MASLD), MASLD and increased alcohol intake (MetALD) and alcohol-related liver disease (ALD) in comparison to the National Institute on Alcohol Abuse and Alcoholism (NIAAA) heavy drinking levels and WHO risk levels of drinking.
Importantly, not all patients who engage in heavy drinking have AUD, which requires substantiation through application of diagnostic criteria from either the Diagnostic and Statistical Manual of Mental Health Disorders 5th (DSM-5) edition17 or the International Classification of Diseases 11th (ICD-11) edition18. The DSM-5 criteria for AUD are based on physiological, psychological and behavioural criteria19, which can be further categorized into four domains. The severity of AUD is defined by the number of criteria met: 2–3 for mild, 4–5 for moderate and 6 or more for severe. The ICD-11 diagnosis of alcohol dependence requires the presence of two or more of three possible symptoms representing impaired control over alcohol use, alcohol use interfering with other aspects of life and physiological features including tolerance or withdrawal and is consistent with the DSM-5 diagnosis of AUD20,21. Both DSM-5 and ICD-11 include disease course specifiers to characterize whether the disorder is active, whether some criteria are no longer present (partial remission) and whether the individual is in early or stable remission. Correct categorization of a study population in clinical trial design is essential to interpret study outcomes. For example, a meta-analysis published in 2021 found the magnitude and variability of the placebo effect in RCTs depend on the severity of AUD and course specifiers of the study population22.
Steatotic liver disease
-
Recommendations 3–4
Hepatic steatosis is influenced by obesity, cardiometabolic factors and alcohol consumption23,24,25. A multisociety Delphi consensus statement proposed in 2023, now endorsed by more than 80 professional societies, changed the nomenclature of ‘non-alcoholic fatty liver disease’ to ‘metabolic dysfunction-associated steatotic liver disease (MASLD)’ both to emphasize metabolic dysfunction as a primary driver of hepatic steatosis and to reduce stigma26. Heretofore, non-alcoholic fatty liver disease had been defined as a ‘diagnosis of exclusion’ in patients with steatotic liver disease (SLD) who did not consume ‘significant amounts of alcohol’ defined as >21 standard drinks per week (294 g) for men and >14 standard drinks per week (196 g) for women27,28. However, the risk of advanced liver disease increases with alcohol consumption above 1 drink per day for women and 2 drinks per day for men29.
The diagnosis of MASLD requires hepatic steatosis and the presence of at least one cardiometabolic risk factor (CMRF) such as BMI ≥ 25, increased waist circumference, diabetes, hypertension, elevated triglyceride levels or low levels of HDL and non-heavy amounts of alcohol consumption. The multisociety Delphi consensus statement noted that alcohol is a primary driver of steatosis along with CMRF. A new category of steatotic liver disease called MetALD was defined as female individuals with MASLD who drink 140–350 g of ethanol per week and male individuals with MASLD who drink 210–420 g ethanol per week26 (Fig. 1). On the basis of the expert opinion using the Delphi method, the threshold for alcohol consumption defining MetALD is the same as the WHO medium risk level of drinking for females and the NIAAA level of heavy drinking for male individuals26. The relative contribution to SLD of metabolic risk factors versus alcohol intake might vary from individual to individual. More research on this newly defined entity, MetALD, is needed.
Alcohol-associated liver disease
-
Recommendations 3–4
Previous studies have shown that insulin resistance, low LDL cholesterol level, active drinking and genetic risk factors were most predictive of advanced fibrosis and inflammation in a cohort of 79 female individuals drinking >24 g per day and 246 male individuals drinking >36 g per day with biopsy-proven ALD25. The multisociety Delphi consensus statement defined ALD with or without CMRF as alcohol consumption exceeding 420 g per week for men and 350 g per week for women. The analysis of the National Health and Nutrition Examination Survey (NHANES) data from 2017 to 2020 (N = 7,367) found that fewer than 0.1% of participants were classified as ALD without any reported CMRF, whereas 0.7% of participants were classified as ALD with CMRF, 2.2% were classified as MetALD and 31% were classified as MASLD defined as <140 g of ethanol per week for female participants and <210 g ethanol per week for male participants in the previous 12 months30. A number of participants with advanced fibrosis, defined as a liver stiffness measurement (LSM) ≥11.7 kPa, but without steatosis reported high alcohol consumption suggesting a need for careful evaluation of remote as well as recent alcohol consumption30. Considering the high prevalence of CMRF in patients with ALD, for the purposes of clinical trials, populations with ALD should include both patients with and without these known CMRFs, which should be stratified in trials.
We propose that clinical trials that focus primarily on the effect of alcohol use on the progression of SLD use a threshold of more than 140 g per week in women and 210 g per week in men, consistent with the NIAAA or CDC definition of heavy drinking and in alignment with the recently proposed multisociety Delphi consensus nomenclature for defining MetALD and ALD26 (Fig. 1).
Subpopulations of ALD
-
Recommendation numbers 5–6
ALD represents a broad spectrum of disease severity, which for clinical trial design must be classified into distinct subpopulations that can be linked to indications for regulatory approval of drugs. Classification must be objective, reproducible and specific with respect to factors that influence disease progression and outcomes, as signs and symptoms of liver disease are nonspecific. Although liver biopsy has historically been considered a gold standard for diagnosis, it is invasive and costly and typically not necessary for classification into appropriate subpopulations31. Vibration-controlled transient elastography correlates well with stage of fibrosis in patients with ALD32,33,34. Liver stiffness decreases in some actively drinking patients after as little as 1 week of abstinence, but usually not to a degree sufficient to alter the category of fibrosis, particularly in those with stages F3–F4 (ref. 35). For the purposes of clinical trial design, we recommend utilizing the term ‘advanced chronic liver disease (ACLD)’ for the following reasons: cirrhosis is defined histologically; to align with Baveno Consensus36,37; patients with stage 3–4 fibrosis based on non-invasive methods such as vibration-controlled transient elastography or magnetic resonance elastography are at high risk of developing liver-related complications; and cut-offs for non-invasive tests to assess liver fibrosis in ALD have mostly been studied to identify advanced (stage ≥3 of 4) fibrosis rather than cirrhosis (stage 4 fibrosis)32,33,34,38,39.
Thus, we propose the following subpopulations for clinical trials among patients who regularly drink heavy amounts of alcohol as defined earlier. ‘Early-stage ALD without advanced fibrosis’ is defined as a subpopulation with steatosis and with minimal-to-moderate (stage 0–2 of 4) fibrosis based on liver histology or non-invasive tests38. This subpopulation is at lowest risk of liver-related events, but might progress to more advanced stages (stage ≥3 fibrosis) of ALD33. Patients are typically asymptomatic and lack signs of portal hypertension. Although Baveno VI recommended an LSM < 10 kPa cut-off to select patients without stage ≥3 fibrosis and cirrhosis, a large study from 10 European centres found using the receiver operating characteristic curve that LSM < 8 kPa was a more optimal cut-off in patients with ALD37,39.
‘Compensated ACLD (cACLD)’ is defined as a subpopulation with liver histology or non-invasive testing showing advanced (stage ≥3 of 4) fibrosis. Baveno VI and VII suggested a cut-off of LSM >15 kPa to identify asymptomatic patients with cACLD36,37. However, in ALD, LSM >12 kPa is a better cut-off to select patients with cACLD as defined33,39, but as non-invasive tests can overestimate the degree of fibrosis36, a combination of non-invasive tests might be necessary in patients with LSM >12 kPa for inclusion in clinical trials33,38. Patients in this subpopulation are often asymptomatic and diagnosed with non-invasive tests (Box 1). They might have mild portal hypertension without liver decompensation (for example, non-bleeding varices or hepatic venous pressure gradient ≥5 mmHg without ascites).
‘Decompensated ALD’ is defined, according to Baveno VII, by the presence of any form of liver decompensation: ascites; hepatic encephalopathy; variceal bleeding occurring in patients with ALD36. As decompensated ALD can recompensate by reducing alcohol use, we recommend that clinical trials for decompensated ALD should standardize the time frame of the most recent liver decompensation (for example, within 1 year of study enrolment) necessary for study inclusion36.
‘Alcohol-associated hepatitis (AH)’ is a severe, sub-acute clinical manifestation of ALD with recent onset of jaundice, liver-related complications and high short-term mortality40. Most patients with AH have concomitant underlying ACLD. Only patients who meet criteria for ‘definite’ (biopsy-confirmed) or ‘probable’ (compatible clinical history and laboratory results, and in whom confounding factors can be excluded), as previously published40, should be considered for studies for AH.
Stigma
-
Recommendation number 7
Stigma refers to negative beliefs about individuals or groups based on characteristics that might set them apart from others. Stigma is commonly experienced by individuals who have AUD, including those with ALD41,42. Diseases related to alcohol use are among the most stigmatized diseases43. International data suggest that ‘persistent barriers related to stigma’ are some of the main contributors to the low prevalence of treatment44. Barriers related to stigma exist at the level of the patient, the clinician, the health-care system or organization and society45. Stigma operates under the conditions of a label (for example, ‘alcoholic’) and an associated stereotype (for example, ‘irresponsible’) to produce a negative response (that is, systematic discrimination)43,46. Stigma manifests itself in many forms including public, self and structural. Public stigma occurs when the lay public holds negative attitudes and beliefs towards specific groups. Although difficult to measure, public stigma can contribute to the slow development of new treatments for alcohol use and ALD. Self-stigma occurs when these negative attitudes and beliefs are held about oneself47. Structural stigma refers to the systematic and institutional barriers that prevent individuals with ALD from accessing the resources and services they need to manage their condition (for example, ineligibility for liver transplantation because of active AUD). When conducting clinical trials in AUD and ALD, we recommend measuring stigma and discussing ways to reduce stigma with all team members (for example, an unbiased approach, using person-first language, recognizing that both AUD and ALD are treatable conditions, ensuring equal access to health care)42,48,49. When possible, patient representatives and other stakeholders should participate in the design of clinical trials. The NIAAA Core Resource on Alcohol includes a section with suggestions for overcoming barriers related to stigma50.
Minimum data set
Demographics
-
Recommendation numbers 8–9
Selecting a study population for which treatment is expected to have clinically meaningful benefits is critical for the success of a clinical trial51. Demographic data including age, biological sex, gender identity, race, family history of AUD and ALD and ethnicity should be included52. Differences between male and female individuals exist across rates of alcohol consumption, diagnosis and treatment response53. Racial and ethnic subgroups have different prevalence rates and might have differences in physiological effects of alcohol54. Additional variables include weight, height, body mass index, waist–hip ratio and metabolic comorbidities including levels of systolic blood pressure, diastolic blood pressure, waist circumference, total cholesterol, LDL cholesterol, HDL cholesterol, triglycerides and HbA1c levels.
Previous diagnosis of liver disease (including the method of diagnosis) and liver-related complications including AH, history of substance use disorder, alcohol use by spouse or partner, smoking and/or tobacco history, presence and stage of kidney disease, history of pancreatitis, history of sleep apnoea and WHO risk drinking levels and sociodemographic variables including employment status (occupation), income level, foreign birth, health-care insurance status and type, highest educational attainment, preferred language and marital status are of interest in some clinical trials.
Liver disease clinical parameters and biochemical tests
-
Recommendation number 10
Biomarkers that can be used for identifying stage of disease, safety and response considerations for therapeutic interventions and trial end points in terms of liver function trajectory in response to treatment (Box 1) will be crucial components for any clinical trial. Ideal biomarkers would be non-invasive, accurate and reproducible, specific to the stage of disease and reflect dynamic changes in disease status and be associated with clinically important outcomes. The ideal biomarkers can include a combination of static and dynamic models of liver function, especially at the more severe end of the spectrum of AUD or ALD. Major advances in imaging-based assessment of liver steatosis and liver stiffness might be of value when available. Imaging techniques, including ultrasonography, CT and MRI, can be useful for detecting steatosis, staging fibrosis, detecting signs of portal hypertension and for hepatocellular carcinoma screening and diagnosis55.
Alcohol use history
Measurements of alcohol use are typically obtained by interviewing a patient along with collateral reports (for example, interviews with family or friends, assessment of previous medical records, criminal record, etc., when indicated) to develop an in-depth assessment of recent and lifetime use (such as heaviest period of drinking), as well as periods of abstinence or reduced drinking56,57,58,59. Table 2 provides a summary of the measures that should be used to assess alcohol use and the advantages and disadvantages of each measure. At a minimum for all trials in patients with ALD, participants should be asked to report their alcohol use through validated measures (such as Alcohol Use Disorders Identification Test-concise (AUDIT-C)) as well as problems related to alcohol use through validated measures such as the full Alcohol Use Disorders Identification Test (AUDIT) questionnaire. For trials in which alcohol use is the intervention target, more granular detail about alcohol consumption patterns should be obtained using Timeline Follow-back, daily diary or ecological momentary assessments (Table 2).
Biological markers (Table 3 notes measures commonly collected in AUD clinical trials) are often used in research and/or clinical practice to supplement self-report alcohol use data60. The performance of a biomarker depends on sensitivity and specificity of the measure and alcohol consumption (that is, amount consumed, duration of consumption, peak alcohol level achieved and time between last use and testing). Although the direct measurement of ethanol in blood or breath, or its metabolites ethyl glucuronide and ethyl sulfate in urine, is simple, only relatively recent alcohol use will be identified, owing to the rapid rate of metabolism of ethanol (on average, 0.0179 ± 0.0030 g ethanol per decilitre per hour in women and 0.0159 ± 0.0028 g ethanol per decilitre per hour in men)61,62. Measuring phosphatidylethanol (PEth) concentration requires whole blood and is costly but has higher sensitivity and specificity for detecting past alcohol exposure up to 4 weeks63,64 than other biomarkers such as carbohydrate-deficient transferrin, γ-glutamyl transpeptidase and mean corpuscular volume. Carbohydrate-deficient transferrin has lower specificity in advanced liver disease65, whereas agreement between laboratories for PEth values is excellent and can be used to validate self-reported consumption64. We recommend using PEth to corroborate self-reported alcohol consumption, particularly if doubt about veracity exists.
As noted, heavy alcohol use is not synonymous with AUD, and validated measures of AUD are also important for assessing how alcohol use is affecting the quality of life of a patient, particularly for trials targeting alcohol use directly.
Individual susceptibility and genetics
-
Recommendation number 11
Patients with heavy alcohol consumption have variable individual susceptibility to develop severe forms of ALD66. These predisposing factors include environmental, genetic and epigenetic determinants that might affect anticipated event rates in clinical trials as they could represent different phenotypes of disease. Whether excessive drinking continues after the identification of ALD as well as the quantity of alcohol consumed are key risk factors that influence progression of ALD31. Female sex, ethnicity, obesity, cigarette smoking and coexistence of other causes of liver injury have been shown to negatively influence the disease development and outcomes67. Several genetic loci have been associated with the risk of developing severe ALD. Although risk loci in PNPLA3, TM6SF2, MBOAT7 and HNRNPUL1 increase the risk of ALD progression, risk variants in HSD17B13, MARC1 and FAF2 confer protection towards progressive ACLD68. Many people of Hispanic ethnicity are predisposed to develop AH, possibly owing to mutations in PNPLA3 that influence disease development and severity69. Epigenetic factors that modulate gene expression in the absence of changes in DNA sequence might also influence susceptibility70. MicroRNA-regulated gene expression and changes in methylation and histone acetylation are implicated in both progression of ACLD and the development of AH70. Given the influence of genetic factors that modify risk of fibrosis, inflammation and steatosis in patients with ALD25, future clinical trials in patients with early-stage ALD and cACLD should consider stratifying patients or use other methods to balance the study populations according to known genetic risk factors.
Trial components
Inclusion and exclusion criteria
-
Recommendation number 12
Inclusion and exclusion criteria for clinical trials are listed in Box 2. Participants or their representatives should have adequate cognitive function to provide written informed consent. Trials should include men and women above age 18 years. Providing all assessment, recruitment and treatment materials in the language (languages) that are represented in the population is desirable.
Early-stage ALD or cACLD
As patients with ongoing heavy alcohol use have substantial competing risk of non-liver-related mortality, presence of extrahepatic diseases (such as cancer, cardiovascular, pulmonary or kidney conditions) must be considered during clinical trial design71,72. Threshold criteria to exclude patients who are more likely to experience outcomes related to extrahepatic disease rather than liver disease should depend on the goals of the clinical trial. For example, trials in early-stage ALD or cACLD, which have lower liver-related event rates, might need to exclude patients with mild–moderate extrahepatic diseases, whereas only severe extrahepatic disease might need to be excluded in trials enrolling decompensated ACLD or severe AH. The goal for trials in early-stage ALD is to prevent progression to ACLD, whereas the goal for cACLD is to reduce the risk of decompensation and death. Excluding too many patients with extrahepatic diseases could make the study less feasible and affect generalizability of the findings owing to the high prevalence of medical comorbidities in ALD. Calculation of the sample size could be affected if patients with extrahepatic comorbidities are not excluded.
Patients with early-stage ALD and cACLD have a minimal risk of decompensation (<25% at 3 years in ACLD) if they are abstinent or consume low amounts of alcohol8. In clinical trials assessing interventions for AUD in patients with early-stage ALD or cACLD, the target population should include patients with continuing alcohol use or those who are at high risk of resuming alcohol use. Development of tools to objectively predict future alcohol use could improve clinical trial design. Feasibility limits prospective studies in patients with AUD focusing on long-term end points (for example, incidence of cirrhosis at 10 years). Thus, any strategy aiming to reduce liver-related risks should focus on patients with cACLD as defined earlier. Finally, metabolic dysfunction-associated liver disease progresses less rapidly than ALD and acts as a cofactor in the progression of fibrosis73. Hence, patients with metabolic risk factors should not be excluded from trials dedicated to alcohol, but metabolic risk factors should be recorded in the data set and methods should be used to balance the study populations at inclusion24,74.
Decompensated ALD and AH
In the clinical course of decompensated ALD, the broad usage of the term ‘acute-on-chronic liver failure’ is problematic because many factors (gastrointestinal bleeding, AH, infection, etc.) can precipitate decompensation and liver failure, and each has a specific prognosis75,76,77,78. In clinical trials of AH, recent onset of jaundice is considered fundamental to clinically diagnose AH40, but there is no consensus regarding the maximal duration of jaundice to make a diagnosis of AH. Indeed, the published criterion requiring jaundice onset within the past 8 weeks is arbitrary40. Between 18% and 32% of patients with severe AH develop infection after the onset of jaundice77,78,79,80. Because the outcome is similar to non-infected patients, they might be included in trials after infection is controlled with appropriate antibiotics. All patients presenting with AH and many who present with new onset decompensation of ACLD have a history of recent alcohol consumption. It follows that these patients are at risk of alcohol-withdrawal syndrome81. Eligibility for entry into clinical trials should be delayed until the risk of withdrawal has passed or alcohol-withdrawal syndrome has been successfully managed.
End points
-
Recommendation number 13
ALD-related end points
Outcomes or events (end points) in clinical trials need to be defined to determine whether the treatment has been beneficial. However, as regulatory agencies have not defined specific end points for clinical trials for ALD, the clinical research community will need to define acceptable end points by consensus but currently there is a lack of consensus (Supplementary Table 1). End points should be clinically meaningful in the context of the stage of clinical development and the overall intended goal of the trial (reduction in consumption of alcohol versus improvement in liver-related outcomes independently of changes in alcohol use). In phase II studies, in which the objective is to demonstrate evidence of a clinical effect, the study size might limit the ability to demonstrate statistically significant differences in relatively uncommon clinical events, for example, mortality. In this case, surrogate end points (Table 4) can be used to demonstrate a clinical effect that can then be formally tested in a phase III study.
In early-stage ALD, clinical outcomes, such as hepatic decompensation or death, are rare and prognosis is generally good in patients who achieve alcohol abstinence8. Thus, the most appropriate clinical outcome might be the percentage of participants who achieve abstinence and duration of abstinence. In early-stage ALD, progression of fibrosis to ACLD, monitored by non-invasive testing, might not be a clinical outcome, but this disease landmark is an important indicator of future risk of complications82.
In cACLD, the most important clinical outcome is to prevent hepatic decompensation, defined by jaundice, ascites, encephalopathy, variceal haemorrhage or progression of portal hypertension as defined by Baveno criteria36. Prevention of decompensation has a major influence on quality of life and health-care expenditure83,84. Decompensation events are, therefore, an appropriate trial end point in both phase II and phase III trials. Patient-related outcomes, including reduction in WHO risk levels4 and quality of life, are reasonable secondary end points.
In decompensated ACLD, the primary purpose of treatment is to reduce mortality, but there are multiple threats to life in this setting. Any solo intervention targeting a given threat might not improve mortality while still providing clinical benefit. Both liver-related mortality and all-cause mortality are important end points. Thus, there is room for innovative trial designs that use hierarchical end points such as the ‘win ratio’85 used in heart failure trials or the Desirability of Outcome Ranking and Response (DOOR) approach used in sepsis trials86. These complex outcomes could be used as alternatives to mortality or hospital admission rates in both phase II and III trials to avoid losing promising therapeutic candidates during development. In phase II studies, improvement in scoring systems such as model for end-stage liver disease (MELD) score could be acceptable. In phase III studies, these scoring systems could be used to stratify patients. However, in phase III studies, irrespective of the specific end point, there is no consensus on the crucial time point at which to measure outcome rates (Supplementary Table 1). Thus, we recommend using a minimum of 6 months.
In non-severe AH, the best prognostic indicator is recovery of liver function, best assessed as improvement in traditional MELD score71. In severe AH, the consensus primary end point is mortality at 90–180 days. Although this end point is appropriate for phase III trials, surrogate outcomes could be used in phase II studies31. Both the Lille score and improvement in MELD score are good prognostic indicators and can be used to demonstrate therapeutic improvement when treatment is compared against standard of care40,79,87. The Lille score predicted 6-month survival in patients treated with anakinra, zinc and pentoxyfiline as well as those treated with methylprednisolone in the DASH trial79. Mortality beyond 180 days is also important and can be influenced substantially by drinking ≥30 g per day, 6 months after a diagnosis of severe AH (hazard ratio for mortality 3.90; 95% CI 2.61–5.82)87.
In decompensated ALD and AH, patients might receive liver transplantation during the study follow-up. Given that liver transplantation is intended for medically refractory ALD, we recommend that transplant-free survival rather than overall survival be used as the primary end point. In clinical trials assessing MELD improvement, the MELD score before transplantation can be imputed and subtracted from baseline MELD among patients who receive transplant before the study end point time. Because the application of early transplantation for AH (that is, without mandated period of abstinence) varies by country and centre, heterogeneity in transplant practice might introduce confounding results in clinical trials, particularly if a substantial proportion of individuals will be eligible for early transplantation88,89,90,91. For example, a therapy that decreases early mortality could paradoxically increase the number of patients surviving long enough to be eligible for transplantation. In this instance, overall survival, rather than transplant-free survival, would be a more appropriate primary outcome. Transplant-related data should be analysed by centre (for example, early transplant policies and/or criteria and median MELD at transplant) and by individual (time from diagnosis to transplant and trajectory of MELD score before transplant) to determine whether overall or transplant-free survival better reflects an improvement in outcome.
AUD-related end points
The most common end points in clinical trials for AUD are derived from calendar-based methods for assessing daily alcohol consumption (for example, the Timeline Follow-Back methodology92), quantity–frequency questionnaires (for example, the Daily Drinking Questionnaire93) that capture frequency and intensity of drinking over a period of time or that define alcohol risk levels based on the AUDIT94 and AUDIT-C (Table 2). Craving was shown to correlate with mood obtained from ecological momentary assessments in patients with ALD95. Biological markers (Table 3) are often used in clinical trials to supplement self-report alcohol use data60. Understanding which outcomes related to drinking (for example, abstinent and heavy drinking days, reduction in WHO risk score, AUD symptom severity, AUDIT scores and biomarker level) are most closely associated with optimal ALD outcomes is critical to optimizing care for patients with ALD.
Treatment considerations
The type and duration of treatment must be clear. Treatments that are aimed solely at improving liver function or treating complications of liver disease should be evaluated separately from treatments aimed at reducing alcohol consumption or managing AUD.
Pharmacotherapy
-
Recommendation number 14
Drugs studied under an Investigational New Drug application require existing preclinical toxicology and in vitro drug interaction testing, but data on the effects of severe organ dysfunction and interactions with alcohol may be incomplete. Any drug trial that involves subjects with ALD, irrespective of the drug target, should account for potential alterations in pharmacodynamics and pharmacokinetics owing to both alcohol consumption and ACLD96,97,98. Any pharmacotherapy study for patients with AUD and ALD should also consider potential drug–alcohol interactions that may limit efficacy or introduce safety concerns. The protocol should include a robust safety component for both adverse events (AEs) and suspected unexpected severe adverse reactions.
Behavioural or cognitive therapies
-
Recommendation numbers 15–17
Many behavioural treatments for AUD can be delivered in residential (for example, inpatient), intensive outpatient and outpatient settings, but relatively few randomized clinical trials have been conducted with patients with comorbid AUD and ALD99. A recent systematic review of 10 studies conducted with patients with ALD who engaged in heavy drinking (AUDIT score >16 or at least 80% of the sample met criteria for an AUD using valid assessment tools) concluded that behavioural therapies can reduce drinking or promote abstinence among individuals with ALD100. Results indicated that motivation enhancement therapy and motivational interviewing, which can be delivered in four treatment sessions or fewer, showed benefit over minimal intervention. Mobile health treatments are gaining in popularity, have demonstrated effectiveness for AUD and may be feasible for those with AUD and ALD101,102.
All trials for ALD should acknowledge explicitly the benefits of reduced drinking and the potential need for AUD treatment. Brief motivational interviewing for reducing heavy drinking should be offered with few exceptions99. Questions about alcohol use should be open-ended using a non-judgmental and collaborative style. In clinical practice, asking open-ended questions using a non-judgmental stance can be therapeutic for patients and can be considered a minimum intervention103,104,105,106. If patients are interested in further treatment and/or meet diagnostic criteria for AUD, a plan for management of AUD may be incorporated into clinical protocols and motivation enhancement therapy that can be delivered in as few as four sessions is recommended for first-line treatment107.
For clinical trials studying ALD, testing distinct AUD treatment (treatments) including pharmacological, behavioural or cognitive should be pre-specified in the protocol with stratified results if more than one treatment modality for AUD is pre-specified. Evidence-based therapies for heavy alcohol use and AUD that leverage motivational, behavioural and cognitive strategies to support abstinence and reduced alcohol use should be considered. Effect sizes for many of these therapies are moderate to large when compared with no treatment or minimal treatment108. Combining behavioural therapies with medications for AUD may increase overall treatment effects including reduction in alcohol use and AUD symptoms109. Specific therapies with demonstrated efficacy for AUD through randomized controlled trials include brief interventions, motivational enhancement therapy, cognitive behavioural therapy, mindfulness-based treatments, behavioural couples therapy, community reinforcement approach, contingency management and 12-step facilitation110. When manualized, theory-based therapies are compared in head-to-head trials, no single approach demonstrates superiority. However, brief interventions and motivational enhancement approaches are generally best for those with at-risk drinking or mild AUD, whereas more intensive approaches are best for those with moderate-to-severe AUD111. Harm reduction therapy approaches also lead to reduction in alcohol use and AUD symptoms in randomized controlled trials112,113. Supporting patients in their treatment goals is most important for maintaining a collaboration as those patients who initially express an interest in drinking reductions tend to transition to abstinence goals.
Time frame for AUD interventions
-
Recommendation numbers 14–17
Behavioural treatment approaches can be initiated once at-risk drinking or AUD is detected and when a subject is medically stable enough to engage in treatment. Although there is no optimal start time for behavioural treatment, early intervention is better for prevention of and escalation of use or symptoms. In patients with hepatic encephalopathy, alcohol-withdrawal syndrome or those who are seriously ill requiring intensive medical care, treatment might need to be delayed until the medical complications have stabilized. Duration of therapy depends on protocol and type of therapy but generally more severe AUD needs more intensive treatment with continuing care for long-term recovery. Relapses may require repeated therapy or adaptive interventions that increase or decrease intensity based on treatment response.
Statistical considerations
-
Recommendation number 18
For all trials, we recommend that investigators obtain accurate and complete data from all participants. Before conducting any inferential analyses, the distribution of trial outcomes and any covariates should be examined for non-normality and outliers. Non-normal data, such as zero inflation, if many people are not drinking and the tendency for skewed or bimodal distributions are common in AUD and ALD clinical trials, and appropriate transformations or non-parametric approaches should be applied. Outliers can be retained or recoded to the next highest or lowest value in the data set. Linear mixed models (for normally distributed outcomes) and generalized linear mixed models (for count or binary outcomes) are robust methods for examining change in outcomes over time56. Missing data are common in AUD and ALD clinical trials. Regulatory agencies currently recommend worst-case imputation for missing outcome data (for example, imputing death if mortality is the missing outcome; imputing heavy drinking if no heavy drinking days is the missing outcome); however, this approach is highly biased, and sensitivity analyses using modern missing data methods (for example, maximum likelihood or multiple imputations) are recommended as alternatives to single imputation methods114.
Innovative trial and statistical designs
-
Recommendation 19
Some features of ALD and AUD make studies challenging when considering clinical trial design, implementation and analysis. Heterogeneity in disease severity, complex intervention delivery, measurement of both short-term and long-term outcomes and differences in treatment timing based on disease severity can all complicate clinical trial designs.
Adaptive trial designs might address some issues in AUD and ALD research. Adaptive design is an umbrella term for designs that allow pre-planned changes based on accumulating data115,116,117. That is, some aspects (aspect) about the trial might change for future patients based on data from previous patients. Examples include group sequential designs, sample size re-estimation, outcome adaptive randomization and enrichment designs. Specifically in AUD and ALD research, group sequential designs include predetermined interim analyses that allow the trial to stop early for efficacy, futility or safety, and enrichment designs might start with broad eligibility criteria, but modify eligibility criteria to enrich the sample for the group whereby the intervention seems most promising. Adaptive designs tend to favour interventions with immediate benefit, so other designs, such as the sequential, multiple assignment, randomized trial (SMART)118 designs (described in Box 3), or more standard designs might be more appropriate if interventions could have a more delayed or long-term benefit. In planning phase III trials for marketing, the sponsor should submit its statistical analysis plan to regulatory authorities.
Trial safety and regulatory considerations
-
Recommendation number 20
In general, the design and conduct of early-phase (phase IIa or proof-of-concept studies) clinical trials for drug development in ALD should exclude people with AH and decompensated ACLD. Individuals with such decompensation at baseline will likely have clinical events that would otherwise be components of clinical efficacy end points40,119. However, if investigators want to expand enrolment criteria to also include individuals with severe AH or decompensated ACLD, then current advice from regulatory agencies would be to conduct hepatic impairment studies before embarking on a phase II or phase III clinical study120. If an investigational product (IP) is primarily excreted unchanged in the urine, then renal impairment studies might be advisable. Hepatic and renal impairment studies should be conducted during phase II development or at least before large-scale phase III trials. Details for early-phase populations who meet criteria for AUD or heavy drinking (NIAAA or CDC) and ALD and clinical end points for early-stage and late-stage drug development can be discussed with regulators.
Adverse events
-
Recommendation numbers 21–22
AEs are of special concern in individuals with conditions that are associated with a high complication rate — the investigator must distinguish between events that are most likely caused by the underlying condition (for example, ALD), and those that are related to the IP. We recommend standardized reporting that includes seriousness, expectedness and relatedness and recommend careful attention to AE reporting during site initiation visits. A commonly misunderstood term is ‘possibly related’. The timing of an AE in relationship to an IP is important, but not the sole determinant in assigning causality. In patients with ACLD and/or AH, the clinical condition can worsen owing to infection or other complications. Assigning causality categorically as possibly related without direct evidence can be misleading. In therapeutic trials, possibly related should be reserved for cases for which no other cause including events commonly related to the underlying disease is likely. For example, a patient might have a variceal haemorrhage during an infusion; although the temporal relationship is obvious, the event could be related to underlying cirrhosis.
Common liver-related AEs
Three broad categories of liver-related AEs might occur in trials of ALD: worsening liver injury and function; development of or worsening of a portal hypertension-related hepatic decompensation event or complication thereof; and cascade of liver failure leading to multiorgan dysfunction75,121,122.
The degree of elevation of aminotransferase levels in the ALD spectrum is modest and generally below 250 IU/l (refs. 40,123). In any of the phenotypes of ALD, a substantial worsening of either (aspartate aminotransferase) AST or alanine transaminase (ALT, also known as alanine aminotransferase) should raise concern for an additional cause of liver injury such as drug-induced liver injury (DILI), ischaemic liver injury or sepsis. An increase in the alkaline phosphatase level might also reflect DILI or biliary tract disease such as choledocholithiasis or acalculous cholecystitis. Worsening bilirubin and INR (international normalized ratio) are reflected in the MELD score and can indicate worsening AH or acute on chronic liver injury. Underlying sepsis and acute kidney injury (AKI) can worsen hyperbilirubinaemia124,125,126. Generally, a 5-point127 increase in MELD above baseline is considered to reflect worsening AH. Patients with severe AH could have rapid increase in MELD related to the development acute kidney injury (AKI-HRS) independent of changes in bilirubin or INR. For stable patients with ACLD, an increase in MELD from values <12 to >15 might reflect progression of the disease or superimposed injury from alcohol or other causes. Given the multiple factors influencing liver enzymes (AST, ALT and alkaline phosphatase) and liver function (INR and bilirubin), frequent laboratory monitoring is required.
In patients with cACLD, liver decompensation events (ascites, hepatic encephalopathy or variceal haemorrhage) are used to assess efficacy of therapy as the incidence of these events is expected to be lower than that in control arms. Liver decompensation might be further complicated by spontaneous bacterial peritonitis and hepatorenal syndrome in individuals with infections. In decompensated ACLD, further worsening of the severity of the event (for example, development of refractory ascites or development of a complication such as spontaneous bacterial peritonitis) is often noted as part of the natural course of the disease and the benefits of therapy can be measured in terms of a reduced incidence in the treatment arm.
Liver decompensation can be present at the time of diagnosis of AH or can develop during hospitalization40,128. In the absence of a clear imbalance between study arms and a biological explanation (such as sepsis) in those receiving immunosuppressive therapy for AH, it might be challenging to attribute decompensatory events, or the lack thereof to study intervention. Because there is no reliable diagnostic test for DILI, expert opinion is needed to evaluate available data to distinguish DILI from worsening of underlying ALD. The cascade of progressive liver decompensation leading to multiorgan dysfunction is well recognized75,122,129. Worsening multiorgan dysfunction often leads to need for intensive care, renal replacement therapy, pressor and ventilatory support. Such interventions indicate a marked deterioration of clinical status and should be reported. They are particularly relevant for ACLD and AH trials and could be considered as ‘events of special interest’.
Common alcohol-related AEs
AUD is a complex illness with multiple organ effects. The study team needs to monitor alcohol use and be ready to manage alcohol-withdrawal syndrome81. Relatedness of AEs (that is, possibly, probably and definitely related) to study medication and study interventions is needed for both pharmacotherapy and behavioural treatment trials. In practice, separating alcohol-related AEs from liver-related AEs can be difficult. Safety monitoring can alert investigators to complications from alcohol use and the evaluation should include physical examinations including weight and body composition given the frequency and rate of muscle loss or sarcopenia in these individuals130. Monitoring for pregnancy in people of childbearing age must be in place and advice regarding avoidance of pregnancy must be pre-specified before initiating any clinical intervention. Follow-up monitoring can be tailored to the study but needs to account for frequent AEs in patients with AUD. Immunological complications can include a chronic pro-inflammatory response with bone marrow suppression (granulocytopenia and thrombocytopenia)131,132 that makes patients with AUD vulnerable to infections133. Folate deficiency was reported in 23% of men drinking an average of 160 g per day (ref. 134). Other micronutrient deficiencies and zinc and their complications are also common135. The relative risk of atrial fibrillation is increased (1.36; 95% CI (127–146)) in individuals drinking ≥48 g per day136, and the relative risk of hypertension is also increased 2.64 (95% CI 2.14–3.26) in Asian individuals and 1.81 (95% CI 1.14–2.86) in non-Asian individuals drinking ≥100 g per day (ref. 137). Alcohol-related cardiomyopathy was reported to account for 6.3% of all cardiomyopathies in 2015, but the issue of whether alcohol causes cardiomyopathy is a subject of controversy138,139,140,141. Gastrointestinal complications separate from liver damage can include gastritis, pancreatitis, gastrointestinal bleeding (of many aetiologies) and gastrointestinal cancers142,143. Finally, central nervous system complications include risk of head trauma and bleeding, brain atrophy and cognitive impairments including Wernicke–Korsakoff syndrome, neuropathies, mood, anxiety and sleep disturbances144.
Assessment of hepatotoxicity and nephrotoxicity
Alcohol use is a potential risk factor and pre-existing liver disease is associated with worse outcomes in patients with idiosyncratic DILI145,146. The diagnosis of DILI or drug-induced kidney injury can be particularly challenging in the presence of severe AH or decompensated ALD when baseline elevations in liver tests and serum creatinine are present. The MELD score147 stratifies severity of AH and ACLD, but is also a predictor of mortality in patients with DILI148,149,150.
In trials that exclude participants with ACLD, unexplained elevation in the levels of AST or ALT ≥3 times baseline or ≥3 times higher than in the control group; or AST >500 U/l; or stage ≥ 1 AKI (increase in the serum creatinine level >0.3 mg/dl (22.88 μmol) within 48 h) is an indication to hold the drug even in the absence of an increase in bilirubin or INR until further adjudication151. The degree of renal dysfunction (stages of AKI) is defined: stage 1, increase in serum creatinine by greater than 0.3 mg/dl within 48 h or to 1.5 times baseline or urine volume <0.5 ml/kg/h for 6 h; stage 2 (2.0–2.9 times serum creatinine increase from baseline or urine output <0.5 ml/kg/h for ≥12 h); and stage 3 (serum creatinine ≥3 times baseline or urine output <0.3 ml/kg/h for ≥24 h or anuria for >12 h)152.
Given unanticipated changes and potential decompensation events, clinical trials should incorporate pre-specified safety parameters to guide site investigators including, but not limited to, enhanced laboratory testing, imaging modalities, dose-reduction and drug-discontinuation parameters. These pre-specified guidelines are important components to the development of individual stopping rules. Large-scale trials should include an independent, blinded hepatic safety adjudication committee that meets frequently to adjudicate AEs of special interest and potential signals of DILI and report their findings to an unblinded data monitoring committee and the sponsor (sponsors) of the trial153.
Stopping rules and data safety monitoring board
-
Recommendation numbers 23–25
Two types of stopping rules should be incorporated into the study protocol: trial stopping rules (for the entire cohort based on unexpected harm or clear demonstration of benefit) and individual stopping rules (because of serious AEs in the individual). Inclusion of study stopping rules could enhance study safety and efficacy by allowing early termination for either positive (primary end point reached) or negative (likely futility or excessive harm) outcomes. Adaptive study designs that use interim analyses to drop inferior treatment arms or stop a trial early might benefit both study sponsors (reduced study time and costs) and participants (reduced harm including eliminating an inferior therapeutic agent or placebo if treatment is effective). However, interim analyses have statistical implications that must be considered at the start of the trial.
Oversight by a Data Safety Monitoring Board (DSMB) whose members are knowledgeable about the natural history of ALD is essential. In trials involving ALD and/or AUD, trial stopping rules based on excessive harm indicated by a statistically significant imbalance between study arms in the following: death, liver transplantation or palliative care measured over a finite period of time (for example, 1–12 months) depending on the acuity of the condition (acute versus chronic), duration of study drug administration and potential for delayed consequences of drug exposure; evidence of serious organ damage (hepatotoxicity, nephrotoxicity, cardiopulmonary and haematological toxicity); mechanism-based adverse effects (for example, infections in the case of immunomodulatory drugs); and excessive suicidality and neurocognitive events. Participant heterogeneity and potential concurrent alcohol use can influence study outcomes and therefore necessitate robust consideration of confounders in any stopping decision. This aspect is particularly relevant in stopping rules for futility in which early termination of the study based on interim results might limit identification of benefits with longer-term follow-up or within specific subgroups of individuals with ALD and AUD. Hence, although serial measures of alcohol and/or illicit drug use are integral to the assessment of treatment of AUD in therapeutic studies for ALD, these data should be closed to the study personnel but made available to the DSMB. Any decision to halt a study based on stopping rules should include review by this committee.
In most clinical studies, one grade 5 serious AEs (SAEs), two grade 4 SAEs or three grade 3 SAEs mandate pausing a study until the DSMB adjudicates the event (events) and determines causality154,155. However, the high mortality of decompensated ACLD or AH that makes survival a good study end point can also hinder trial execution. Stopping for any death would likely lead to frequent enrolment delays, treatment interruptions and hindrance of DSMB causality assessments. Thus, the sponsor might need to rely on site investigator assessments to avoid repeated pauses awaiting DSMB adjudication. For example, the clinical trial could be paused for DSMB assessment only if the site investigator concludes that the death is not related to decompensated ACLD with ACLF, or severe AH. To facilitate accurate death attribution, site investigators and the DSMB should be well versed in disease course, the mechanism of action of the study drug and results of hepatic and renal impairment studies before embarking on a phase II or III clinical study. Alternatively, a sponsor could choose to use a suspected unexpected severe adverse reaction to reframe the typical trial stopping rules as listed previously.
In most instances, a trial will benefit from the creation of a separate hepatic safety adjudication committee that conducts adjudication in a blinded manner and reports to the unblinded DSMB. By contrast, the DSMB is unblinded to data and might find that an event occurred in the placebo arm and not the treatment arm. The hepatic safety committee should adjudicate AEs of special interest and potential signals of DILI. For these situations, independent hepatologists with expertise in DILI adjudication are necessary.
Individual stopping rules
-
Recommendation number 26
Individual stopping rules should be in place to hold and/or discontinue investigational drug treatment in patients with evidence of infections refractory to treatment, an increase in levels of AST >500 or ALT >400 without alternative explanation, development of liver failure characterized by rising bilirubin levels, worsening coagulopathy or the development of AKI (greater than stage 2 with increase in the serum creatinine level 2.0–2.9 times baseline) with hepatorenal physiology (HRS-AKI) during further evaluation and adjudication. In 2021, an expert consensus panel (IQ-DILI) recommended that an investigational drug should be held and the possibility of DILI should be investigated in participants with an increase in MELD >5 over baseline if baseline MELD is ≤12 and an increase >3 if baseline MELD is >12 (ref. 153). These recommendations were made for patients with ACLD owing to hepatitis C virus infection, hepatitis B virus infection and MASLD, but not specifically alcohol153. In patients with decompensated ACLD or severe AH, challenges arise in discerning causality and how to apply individual stopping rules. Individual stopping rules should consider that HRS-AKI develops as a consequence of infection, overuse of diuretics, iodinated contrast dye, exposure to known nephrotoxic drugs and as part of the natural history of advanced liver disease. For these reasons, the expertise of an independent blinded safety assessment committee is critical to review data and adjudicate causality.
Challenges and future directions
Recruitment and retention
-
Recommendation number 27
Recruitment and retention present some of the most notable challenges in the success of clinical trials. By some estimates, over half of all clinical trials failed to meet their recruitment targets within the allocated time, whereas others fell short of retention goals156,157,158,159,160,161,162. This issue has been of particular concern for ALD clinical trials, in which low recruitment and retention rates have been problematic, resulting in prolonged study timelines, biased study samples, questionable conclusions and, ultimately, a failed investigation157,163,164.
ALD investigators are also confronted with challenges unique to the ALD population. Especially among those with advanced ALD, advanced illness with acute symptoms, feeling too ill to participate in or lacking motivation to participate in clinical studies and being physically and emotionally vulnerable are patient-related factors that contribute to poor recruitment and retention rates. Recognized logistical barriers to recruitment in populations with alcohol and substance use disorders include a lack of one or more of the following: transportation, medical insurance, social support and a stable living environment165.
An analysis, published in 2024 of recruitment and retention by the Alcoholic Hepatitis Network (AlcHepNet) using an observational cohort that enrolled 465 patients with AH, 168 individuals with heavy drinking without liver disease and 119 healthy volunteers and a randomized clinical trial that enrolled 147 patients with severe AH, provides strategies to improve patient recruitment and retention in populations with ALD by reducing modifiable barriers while providing objective criteria to measure site performance in clinical trials, as detailed166 (Table 5).
Future studies
-
Recommendation number 28
Integrated care in the clinical setting is an interdisciplinary process that relies heavily on the performance of key coordinated care tasks within teams; the relationships in these teams are built on a foundation of good communication, mutual respect, shared goals and shared knowledge167,168,169. Integrated care, sometimes referred to as coordinated care, is beneficial and necessary at the intersection of both medical and mental health disorders that are often comorbid with ALD (for example, obesity) and AUD (for example, substance use disorder, depression, anxiety disorders and post-traumatic stress disorder), respectively.
Potential limitations
Many of the recommendations in this manuscript are based on a consensus of expert opinions drawn both from interpretation of the literature and from personal experience. In some instances, the empirical evidence to support these recommendations is incomplete. For example, definitions of heavy drinking (NIAAA/CDC) and WHO risk categories of drinking were developed between 2000 and 2005 for men and women without attention to the possibility of gender identification or sex reassignment, both of which often involve hormonal treatment that could affect metabolism of ethanol and/or patterns of consumption. Future studies will need to clarify gender and sex at birth to provide a more complete view of how these parameters may affect outcomes. These recommendations are based on literature and experiences that are limited in the diversity of patient demographics, practice settings (most often academic medical centres), pharmacotherapy options for reducing alcohol consumption in patients with ACLD, input from patient representatives and other stakeholders and geographic distribution of the experts who participated in the task force. The members of the task force were mostly from North America with a few from Europe and the UK; there were no members from Asia, South America, Australia or Africa. The task force did not use the Delphi method or other formal processes for anonymous voting on the recommendations. The process was based on the NIH consensus development programme as revised by the Institute of Medicine (now National Academy of Medicine USA)13. Ongoing discussion among experts in ALD and AUD, patient representatives and members of the pharmaceutical industry as well as regulatory agencies such as FDA and European Medicines Agency will enhance the development of new and more effective treatments for alcohol-associated liver disease.
Conclusions
Observational studies show that heavy drinking after a diagnosis of ALD increases all-cause mortality8 and that abstinence improves survival and liver-related outcomes5,9,10. Despite this evidence, few clinical trials have been conducted to confirm these observations. The 28 recommendations approved by the task force organized by the NIAAA represent a consensus of expert opinions to guide the design of clinical trials to study the effects of alcohol use and AUD on clinical outcomes in patients with ALD. We recommend integrating research experts from hepatology and addiction medicine to ensure multidisciplinary representation on the research team. Inclusion of addiction medicine experts to ALD research teams enables accurate selection of key measures for alcohol use and AUD symptoms and for accurate reporting of key alcohol and AUD-related outcomes. Careful measurement of alcohol consumption before and during clinical trials in all patients with steatotic liver disease is necessary given the deleterious and potentially confounding effects of alcohol on liver-related outcomes5,9,10. The recommendations also include assessing cardiometabolic risk factors for SLD and tailoring inclusion and exclusion criteria according to the stage of liver disease. During the trial, careful monitoring and adjudication of AEs by a separate hepatic safety committee with well-defined individual and study stopping rules are strongly encouraged. Finally, addressing stigma and developing other strategies are necessary to improve recruitment and retention to ensure validity and generalizability of the findings.
References
Rehm, J. & Shield, K. D. Global Burden of Alcohol Use Disorders and Alcohol Liver Disease. MDPI https://www.mdpi.com/2227-9059/7/4/99 (2019).
Chen, C. M. & Yoon, Y.-H. Surveillance Report #118 Liver Cirrhosis Mortality in the United States: National, State, and Regional Trends, 2000–2019. NIH https://www.niaaa.nih.gov/publications/surveillance-reports/surveillance118#:~:Text=Cirrhosis%20Mortality%20Trends,12.2%20deaths%20per%20100%2C000%20population (2022).
National Institute on Alcohol Abuse and Alcoholism. a. What is Heavy Drinking? NIH https://www.niaaa.nih.gov/health-professionals-communities/core-resource-on-alcohol/basics-defining-how-much-alcohol-too-much#pub-toc4 (2023).
World Health Organization. International Guide for Monitoring Alcohol Consumption and Related Harm (World Health Organization, 2000).
DiMartini, A., Weinrieb, R., Lane, T., Day, N. & Fung, J. Defining the alcoholic liver transplant population: implications for future research. Liver Transpl. 7, 428–431 (2001).
Dawson, D. A., Li, T. K. & Grant, B. F. A prospective study of risk drinking: at risk for what? Drug Alcohol Depend. 95, 62–72 (2008).
Singal, A. K., Leggio, L. & DiMartini, A. Alcohol use disorder in alcohol-associated liver disease: two sides of the same coin. Liver Transpl. 30, 200–212 (2023).
Louvet, A. et al. Low alcohol consumption influences outcomes in individuals with alcohol-related compensated cirrhosis in a French multicenter cohort. J. Hepatol. 78, 501–512 (2023).
Hofer, B. S. et al. Alcohol abstinence improves prognosis across all stages of portal hypertension in alcohol-related cirrhosis. Clin. Gastroenterol. Hepatol. 21, 2308–2317.e7 (2023).
Lackner, C. et al. Histological parameters and alcohol abstinence determine long-term prognosis in patients with alcoholic liver disease. J. Hepatol. 66, 610–618 (2017).
Mellinger, J., Winder, G. S. & Fernandez, A. C. Measuring the alcohol in alcohol-associated liver disease: choices and challenges for clinical research. Hepatology 73, 1207–1212 (2021).
Singal, A. K. et al. Research methodologies to address clinical unmet needs and challenges in alcohol-associated liver disease. Hepatology 75, 1026–1037 (2022).
Institute of Medicine (US) Committee to Improve the National Institutes of Health Consensus Development Program. Consensus Development at the NIH: Improving the Program 1st edn (National Academies Press, 1990).
Bellentani, S. et al. Drinking habits as cofactors of risk for alcohol induced liver damage. the Dionysos Study Group. Gut 41, 845–850 (1997).
Knox, J. et al. Reduction in nonabstinent WHO drinking risk levels and change in risk for liver disease and positive AUDIT-C scores: prospective 3-year follow-up results in the U.S. general population. Alcohol Clin. Exp. Res. 42, 2256–2265 (2018).
Witkiewitz, K. et al. Drinking risk level reductions associated with improvements in physical health and quality of life among individuals with alcohol use disorder. Alcohol Clin. Exp. Res. 42, 2453–2465 (2018).
American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders 5th edn (American Psychiatric Publishing, 2013).
World Health Organization. International Classification of Diseases 11th edn (World Health Organization, 2019).
Hasin, D. S. et al. DSM-5 criteria for substance use disorders: recommendations and rationale. Am. J. Psychiatry 170, 834–851 (2013).
Lundin, A. et al. Towards ICD-11 for alcohol dependence: diagnostic agreement with ICD-10, DSM-5, DSM-IV, DSM-III-R and DSM-III diagnoses in a Swedish general population of women. Drug Alcohol Depend. 227, 108925 (2021).
Slade, T. et al. DSM-5 and ICD-11 alcohol use disorder criteria in young adult regular drinkers: lifetime prevalence and age of onset. Drug Alcohol Depend. 229, 109184 (2021).
Scherrer, B. et al. Baseline severity and the prediction of placebo response in clinical trials for alcohol dependence: a meta-regression analysis to develop an enrichment strategy. Alcohol Clin. Exp. Res. 45, 1722–1734 (2021).
Aberg, F. et al. Combined effects of alcohol and metabolic disorders in patients with chronic liver disease. Clin. Gastroenterol. Hepatol. 18, 995–997.e2 (2020).
Aberg, F., Byrne, C. D., Pirola, C. J., Mannisto, V. & Sookoian, S. Alcohol consumption and metabolic syndrome: clinical and epidemiological impact on liver disease. J. Hepatol. 78, 191–206 (2023).
Israelsen, M. et al. Metabolic and genetic risk factors are the strongest predictors of severity of alcohol-related liver fibrosis. Clin. Gastroenterol. Hepatol. 20, 1784–1794.e9 (2022).
Rinella, M. E. et al. A multi-society Delphi consensus statement on new fatty liver disease nomenclature. Hepatology 78, 1966–1986 (2023).
Chalasani, N. et al. The diagnosis and management of non-alcoholic fatty liver disease: practice guideline by the American Association for the Study of Liver Diseases, American College of Gastroenterology, and the American Gastroenterological Association. Hepatology 55, 2005–2023 (2012).
Chalasani, N. et al. The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology 67, 328–357 (2018).
Rehm, J. et al. Alcohol as a risk factor for liver cirrhosis: a systematic review and meta-analysis. Drug Alcohol Rev. 29, 437–445 (2010).
Lee, B. P., Dodge, J. L. & Terrault, N. A. National prevalence estimates for steatotic liver disease and sub-classifications using consensus nomenclature. Hepatology 79, 666–673 (2023).
Crabb, D. W., Im, G. Y., Szabo, G., Mellinger, J. L. & Lucey, M. R. Diagnosis and treatment of alcohol-associated liver diseases: 2019 practice guidance from the American Association for the Study of Liver Diseases. Hepatology 71, 306–333 (2020).
Thiele, M. et al. Transient and 2-dimensional shear-wave elastography provide comparable assessment of alcoholic liver fibrosis and cirrhosis. Gastroenterology 150, 123–133 (2016).
Nguyen-Khac, E. et al. Non-invasive diagnosis of liver fibrosis in patients with alcohol-related liver disease by transient elastography: an individual patient data meta-analysis. Lancet Gastroenterol. Hepatol. 3, 614–625 (2018).
Pavlov, C. S. et al. Transient elastography for diagnosis of stages of hepatic fibrosis and cirrhosis in people with alcoholic liver disease. Cochrane Database Syst. Rev. 1, CD010542 (2015).
Trabut, J. B. et al. Rapid decline of liver stiffness following alcohol withdrawal in heavy drinkers. Alcohol Clin. Exp. Res. 36, 1407–1411 (2012).
de Franchis, R. et al. Baveno VII — renewing consensus in portal hypertension. J. Hepatol. 76, 959–974 (2022).
de Franchis, R. & Baveno, V. I. F. Expanding consensus in portal hypertension: report of the Baveno VI Consensus Workshop: stratifying risk and individualizing care for portal hypertension. J. Hepatol. 63, 743–752 (2015).
Thiele, M. et al. Accuracy of the enhanced liver fibrosis test vs fibrotest, elastography, and indirect markers in detection of advanced fibrosis in patients with alcoholic liver disease. Gastroenterology 154, 1369–1379 (2018).
Papatheodoridi, M. et al. Refining the Baveno VI elastography criteria for the definition of compensated advanced chronic liver disease. J. Hepatol. 74, 1109–1116 (2021).
Crabb, D. W. et al. Standard definitions and common data elements for clinical trials in patients with alcoholic hepatitis: recommendation from the NIAAA alcoholic hepatitis consortia. Gastroenterology 150, 785–790 (2016).
Kilian, C. et al. Stigmatization of people with alcohol use disorders: an updated systematic review of population studies. Alcohol Clin. Exp. Res. 45, 899–911 (2021).
Schomerus, G. et al. The stigma of alcohol-related liver disease and its impact on healthcare. J. Hepatol. 77, 516–524 (2022).
Ashford, R. D., Brown, A. M. & Curtis, B. Substance use, recovery, and linguistics: the impact of word choice on explicit and implicit bias. Drug Alcohol Depend. 189, 131–138 (2018).
Grant, B. F. et al. Epidemiology of DSM-5 alcohol use disorder: results from the National Epidemiologic Survey on alcohol and related conditions III. JAMA Psychiatry 72, 757–766 (2015).
DiMartini, A. F., Leggio, L. & Singal, A. K. Barriers to the management of alcohol use disorder and alcohol-associated liver disease: strategies to implement integrated care models. Lancet Gastroenterol. Hepatol. 7, 186–195 (2022).
Link, B. G. & Phelan, J. C. Conceptualizing stigma. Annu. Rev. Sociol. 27, 363–385 (2001).
Stangl, A. L. et al. The Health Stigma and Discrimination Framework: a global, crosscutting framework to inform research, intervention development, and policy on health-related stigmas. BMC Med. 17, 31 (2019).
Smith, L. R., Earnshaw, V. A., Copenhaver, M. M. & Cunningham, C. O. Substance use stigma: reliability and validity of a theory-based scale for substance-using populations. Drug Alcohol Depend. 162, 34–43 (2016).
American Association for the Study of Liver Disease, European Association for the Study of the Liver, Latin American Association for the Study of the Liver & Asian Pacific Association for the Study of the Liver. Ending stigmatizing language in alcohol and liver disease: a liver societies’ statement†. Hepatology 78, 1682–1683 (2023).
National Institute on Alcohol Abuse and Alcoholism. Stigma: Overcoming a Pervasive Barrier to Optimum Care. NIH https://www.niaaa.nih.gov/health-professionals-communities/core-resource-on-alcohol/basics-defining-how-much-alcohol-too-much#pub-toc4 (2023).
Zhao, L., Tian, L., Cai, T., Claggett, B. & Wei, L. J. Effectively selecting a target population for a future comparative study. J. Am. Stat. Assoc. 108, 527–539 (2013).
Karriker-Jaffe, K. J., Chartier, K. G., Bares, C. B., Kendler, K. S. & Greenfield, T. K. Intersection of familial risk and environmental social control on high-risk drinking and alcohol dependence in a US national sample of adults. Addict. Behav. 113, 106668 (2021).
Kezer, C. A., Simonetto, D. A. & Shah, V. H. Sex differences in alcohol consumption and alcohol-associated liver disease. Mayo Clin. Proc. 96, 1006–1016 (2021).
Vaeth, P. A., Wang-Schweig, M. & Caetano, R. Drinking, alcohol use disorder, and treatment access and utilization among U.S. racial/ethnic groups. Alcohol Clin. Exp. Res. 41, 6–19 (2017).
Moreno, C., Mueller, S. & Szabo, G. Non-invasive diagnosis and biomarkers in alcohol-related liver disease. J. Hepatol. 70, 273–283 (2019).
Witkiewitz, K., Finney, J. W., Harris, A. H., Kivlahan, D. R. & Kranzler, H. R. Recommendations for the design and analysis of treatment trials for alcohol use disorders. Alcohol Clin. Exp. Res. 39, 1557–1570 (2015).
Koenig, L. B., Jacob, T. & Haber, J. R. Validity of the lifetime drinking history: a comparison of retrospective and prospective quantity–frequency measures. J. Stud. Alcohol Drugs 70, 296–303 (2009).
Longnecker, M. P. et al. The reliability of self-reported alcohol consumption in the remote past. Epidemiology 3, 535–539 (1992).
Jayasekara, H. et al. Alcohol consumption for different periods in life, intake pattern over time and all-cause mortality. J. Public Health 37, 625–633 (2015).
Litten, R. Z. & Fertig, J. Self-report and biochemical measures of alcohol consumption. Addiction 98, iii–iv (2003).
Litten, R. Z., Bradley, A. M. & Moss, H. B. Alcohol biomarkers in applied settings: recent advances and future research opportunities. Alcohol Clin. Exp. Res. 34, 955–967 (2010).
Dettling, A. et al. Ethanol elimination rates in men and women in consideration of the calculated liver weight. Alcohol 41, 415–420 (2007).
Ulwelling, W. & Smith, K. The PEth blood test in the security environment: what it is; why it is important; and interpretative guidelines. J. Forensic Sci. 63, 1634–1640 (2018).
Helander, A. & Hansson, T. The alcohol biomarker phosphatidylethanol (PEth) — test performance and experiences from routine analysis and external quality assessment. Scand. J. Clin. Lab. Invest. 83, 424–431 (2023).
DiMartini, A. et al. Carbohydrate deficient transferrin in abstaining patients with end-stage liver disease. Alcohol Clin. Exp. Res. 25, 1729–1733 (2001).
Morgan, M., Sharma, M. & Atkinson, S. Genetic and environmental susceptibility to alcoholic hepatitis. Clin. Liver Dis. 25, 517–535 (2021).
Liangpunsakul, S., Haber, P. & McCaughan, G. W. Alcoholic liver disease in Asia, Europe, and North America. Gastroenterology 150, 1786–1797 (2016).
Schnabl, B. et al. Liver specific, systemic and genetic contributors to alcohol-related liver disease progression. J. Gastroenterol. 60, 36–44 (2022).
Liangpunsakul, S. et al. Interaction between the patatin-like phospholipase domain-containing protein 3 genotype and coffee drinking and the risk for acute alcoholic hepatitis. Hepatol. Commun. 2, 29–34 (2017).
Ajoolabady, A., Aslkhodapasandhokmabad, H., Zhou, Y. & Ren, J. Epigenetic modification in alcohol-related liver diseases. Med. Res. Rev. 42, 1463–1491 (2022).
Degre, D. et al. Long-term outcomes in patients with decompensated alcohol-related liver disease, steatohepatitis and Maddrey’s discriminant function < 32. J. Hepatol. 72, 636–642 (2020).
Moon, A. M., Yang, J. Y., Barritt, A. S. T., Bataller, R. & Peery, A. F. Rising mortality from alcohol-associated liver disease in the United States in the 21st century. Am. J. Gastroenterol. 115, 79–87 (2020).
Israelsen, M. et al. Validation of the new nomenclature of steatotic liver disease in patients with a history of excessive alcohol intake: an analysis of data from a prospective cohort study. Lancet Gastroenterol. Hepatol. 9, 218–228 (2024).
Dam-Larsen, S. et al. Long term prognosis of fatty liver: risk of chronic liver disease and death. Gut 53, 750–755 (2004).
Moreau, R. et al. Acute-on-chronic liver failure is a distinct syndrome that develops in patients with acute decompensation of cirrhosis. Gastroenterology 144, 1426–1437.e1–9 (2013).
Bajaj, J. S. et al. Second infections independently increase mortality in hospitalized patients with cirrhosis: the North American Consortium for the Study of End-Stage Liver Disease (NACSELD) experience. Hepatology 56, 2328–2335 (2012).
Vergis, N. et al. In patients with severe alcoholic hepatitis, prednisolone increases susceptibility to infection and infection-related mortality, and is associated with high circulating levels of bacterial DNA. Gastroenterology 152, 1068–1077.e4 (2017).
Louvet, A. et al. Infection in patients with severe alcoholic hepatitis treated with steroids: early response to therapy is the key factor. Gastroenterology 137, 541–548 (2009).
Szabo, G. et al. IL-1 receptor antagonist plus pentoxifylline and zinc for severe alcohol-associated hepatitis. Hepatology 76, 1058–1068 (2022).
Gawrieh, S. et al. Randomized-controlled trial of anakinra plus zinc vs. prednisone for severe alcohol-associated hepatitis. J. Hepatol. 80, 684–693 (2024).
Carlson, R. W. et al. Alcohol withdrawal syndrome. Crit. Care Clin. 28, 549–585 (2012).
Rasmussen, D. N. et al. Prognostic performance of 7 biomarkers compared to liver biopsy in early alcohol-related liver disease. J. Hepatol. 75, 1017–1025 (2021).
Labenz, C. et al. Health-related quality of life in patients with compensated and decompensated liver cirrhosis. Eur. J. Intern. Med. 70, 54–59 (2019).
Mellinger, J. L. et al. The high burden of alcoholic cirrhosis in privately insured persons in the United States. Hepatology 68, 872–882 (2018).
Pocock, S., Ariti, C., Collier, T. & Wang, D. The win ratio: a new approach to the analysis of composite endpoints in clinical trials based on clinical priorities. Eur. Heart J. 33, 176–182 (2012).
Perez, F. et al. Desirability of outcome ranking for the management of antimicrobial therapy (DOOR MAT) reveals improvements in the treatment of bloodstream infections caused by Escherichia coli and Klebsiella pneumoniae in patients from the Veterans Health Administration. Clin. Infect. Dis. 73, 1231–1238 (2021).
Louvet, A. et al. Main drivers of outcome differ between short term and long term in severe alcoholic hepatitis: a prospective study. Hepatology 66, 1464–1473 (2017).
Lee, B. P., Vittinghoff, E., Dodge, J. L., Cullaro, G. & Terrault, N. A. National trends and long-term outcomes of liver transplant for alcohol-associated liver disease in the United States. JAMA Intern. Med. 179, 340–348 (2019).
Asrani, S. K. et al. Meeting report: the Dallas Consensus Conference on liver transplantation for alcohol associated hepatitis. Liver Transpl. 26, 127–140 (2020).
European Association for the Study of the Liver. EASL clinical practice guidelines: management of alcohol-related liver disease. J. Hepatol. 69, 154–181 (2018).
Arab, J. P. et al. Alcohol-related liver disease: clinical practice guidelines by the Latin American Association for the Study of the Liver (ALEH). Ann. Hepatol. 18, 518–535 (2019).
Sobell, L. C. & Sobell, M. B. Measuring Alcohol Consumption: Psychosocial and Biochemical Methods 41–72 (Humana Press/Springer Nature, 1992).
Collins, R. L., Parks, G. A. & Marlatt, G. A. Social determinants of alcohol consumption: the effects of social interaction and model status on the self-administration of alcohol. J. Consult. Clin. Psychol. 53, 189–200 (1985).
Saunders, J. B., Aasland, O. G., Babor, T. F., de la Fuente, J. R. & Grant, M. Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption — II. Addiction https://doi.org/10.1111/j.1360-0443.1993.tb02093.x (1993).
Wu, T. et al. Smartphone sensor data estimate alcohol craving in a cohort of patients with alcohol-associated liver disease and alcohol use disorder. Hepatol. Commun. 7, e0329 (2023).
Pelkonen, O. & Sotaniemi, E. Drug metabolism in alcoholics. Pharmacol. Ther. 16, 261–268 (1982).
Moore, A., Whiteman, E. & Ward, K. Risks of combined alcohol/medication use in older adults. Am. J. Geriatr. Pharmacother. 5, 64–74 (2007).
Pena, M., Horga, J. & Zapater, P. Variations of pharmacokinetics of drugs in patients with cirrhosis. Expert Rev. Clin. Pharmacol. 9, 441–458 (2016).
Ting, P. S., Wheatley, J. & Chen, P. H. Behavioral treatment for patients with alcohol-related liver disease: a primer for hepatologists. Clin. Liver Dis. 15, 31–35 (2020).
Hemrage, S., Brobbin, E., Deluca, P. & Drummond, C. Efficacy of psychosocial interventions to reduce alcohol use in comorbid alcohol use disorder and alcohol-related liver disease: a systematic review of randomized controlled trials. Alcohol Alcohol. 58, 478–484 (2023).
DeMartini, K. S. et al. Text messaging to reduce alcohol relapse in prelisting liver transplant candidates: a pilot feasibility study. Alcohol Clin. Exp. Res. 42, 761–769 (2018).
Suffoletto, B. & Scaglione, S. Using digital interventions to support individuals with alcohol use disorder and advanced liver disease: a bridge over troubled waters. Alcohol Clin. Exp. Res. 42, 1160–1165 (2018).
Magill, M. et al. A meta-analysis of motivational interviewing process: technical, relational, and conditional process models of change. J. Consult. Clin. Psychol. 86, 140–157 (2018).
Magill, M. et al. Do what you say and say what you are going to do: a preliminary meta-analysis of client change and sustain talk subtypes in motivational interviewing. Psychother. Res. 29, 860–869 (2018).
McCrady, B. S., Owens, M. D., Borders, A. Z. & Brovko, J. M. Psychosocial approaches to alcohol use disorders since 1940: a review. J. Stud. Alcohol Drugs Suppl. 75, 68–78 (2014).
Miller, W. R. & Rose, G. S. Toward a theory of motivational interviewing. Am. Psychol. 64, 527–537 (2009).
Dieperink, E. et al. Efficacy of motivational enhancement therapy on alcohol use disorders in patients with chronic hepatitis C: a randomized controlled trial. Addiction 109, 1869–1877 (2014).
Magill, M. & Ray, L. A. Cognitive-behavioral treatment with adult alcohol and illicit drug users: a meta-analysis of randomized controlled trials. J. Stud. Alcohol Drugs 70, 516–527 (2009).
Ray, L. A. et al. Combined pharmacotherapy and cognitive behavioral therapy for adults with alcohol or substance use disorders: a systematic review and meta-analysis. JAMA Netw. Open 3, e208279 (2020).
Witkiewitz, K., Pfund, R. A. & Tucker, J. A. Mechanisms of behavior change in substance use disorder with and without formal treatment. Annu. Rev. Clin. Psychol. 18, 497–525 (2022).
Witkiewitz, K., Litten, R. Z. & Leggio, L. Advances in the science and treatment of alcohol use disorder. Sci. Adv. 5, eaax4043 (2019).
Mann, K., Aubin, H.-J. H.-J. & Witkiewitz, K. Reduced drinking in alcohol dependence treatment, what is the evidence? Eur. Addict. Res. 23, 219–230 (2017).
Marlatt, G. A. & Witkiewitz, K. Harm reduction approaches to alcohol use: health promotion, prevention, and treatment. Addict. Behav. 27, 867–886 (2002).
Hallgren, K. A. & Witkiewitz, K. Missing data in alcohol clinical trials: a comparison of methods. Alcohol Clin. Exp. Res. 37, 2152–2160 (2013).
Bhatt, D. L. & Mehta, C. Adaptive designs for clinical trials. N. Engl. J. Med. 375, 65–74 (2016).
Chow, S. C. Adaptive clinical trial design. Annu. Rev. Med. 65, 405–415 (2014).
Thorlund, K., Haggstrom, J., Park, J. J. & Mills, E. J. Key design considerations for adaptive clinical trials: a primer for clinicians. Br. Med. J. 360, k698 (2018).
Murphy, S. A. An experimental design for the development of adaptive treatment strategies. Stat. Med. 24, 1455–1481 (2005).
Sola, E. et al. Endpoints and design of clinical trials in patients with decompensated cirrhosis: position paper of the LiverHope Consortium. J. Hepatol. 74, 200–219 (2021).
FDA. Guidance for Industry Pharmacokinetics in Patients with Impaired Hepatic Function: Study Design, Data Analysis, and Impact on Dosing and Labeling. FDA https://www.fda.gov/media/71311/download (2003).
Sarin, S. K. et al. Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific association for the study of the liver (APASL): an update. Hepatol. Int. 13, 353–390 (2019).
O’Leary, J. G. et al. NACSELD Acute-on-Chronic Liver Failure (NACSELD-ACLF) score predicts 30-day survival in hospitalized patients with cirrhosis. Hepatology 67, 2367–2374 (2018).
Singal, A. K. & Mathurin, P. Diagnosis and treatment of alcohol-associated liver disease: a review. JAMA 326, 165–176 (2021).
Szabo, G., Romics, L. Jr & Frendl, G. Liver in sepsis and systemic inflammatory response syndrome. Clin. Liver Dis. 6, 1045–1066 (2002).
Mookerjee, R. P. et al. The role of liver biopsy in the diagnosis and prognosis of patients with acute deterioration of alcoholic cirrhosis. J. Hepatol. 55, 1103–1111 (2011).
Adebayo, D. & Wong, F. Pathophysiology of hepatorenal syndrome — acute kidney injury. Clin. Gastroenterol. Hepatol. 21, S1–S10 (2023).
Thursz, M., Kamath, P. S., Mathurin, P., Szabo, G. & Shah, V. H. Alcohol-related liver disease: areas of consensus, unmet needs and opportunities for further study. J. Hepatol. 70, 521–530 (2019).
Bataller, R., Arab, J. P. & Shah, V. H. Alcohol-associated hepatitis. N. Engl. J. Med. 387, 2436–2448 (2022).
Sarin, S. K. et al. Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific Association for the Study of the Liver (APASL). Hepatol. Int. 3, 269–282 (2009).
Welch, N. et al. Continued muscle loss increases mortality in cirrhosis: impact of aetiology of liver disease. Liver Int. 40, 1178–1188 (2020).
Shi, X., DeLucia, A. L., Bao, J. & Zhang, P. Alcohol abuse and disorder of granulopoiesis. Pharmacol. Ther. 198, 206–219 (2019).
Silczuk, A. & Habrat, B. Alcohol-induced thrombocytopenia: current review. Alcohol 86, 9–16 (2020).
Simou, E., Britton, J. & Leonardi-Bee, J. Alcohol and the risk of pneumonia: a systematic review and meta-analysis. BMJ Open. 8, e022344 (2018).
Sanvisens, A. et al. Folate deficiency in patients seeking treatment of alcohol use disorder. Drug Alcohol Depend. 180, 417–422 (2017).
McClain, C. J., Rios, C. D., Condon, S. & Marsano, L. S. Malnutrition and alcohol-associated hepatitis. Clin. Liver Dis. 25, 557–570 (2021).
Larsson, S. C., Drca, N. & Wolk, A. Alcohol consumption and risk of atrial fibrillation: a prospective study and dose–response meta-analysis. J. Am. Coll. Cardiol. 64, 281–289 (2014).
Taylor, B. et al. Alcohol and hypertension: gender differences in dose–response relationships determined through systematic review and meta-analysis. Addiction 104, 1981–1990 (2009).
Manthey, J., Probst, C., Rylett, M. & Rehm, J. National, regional and global mortality due to alcoholic cardiomyopathy in 2015. Heart 104, 1663–1669 (2018).
Andersson, C., Schou, M., Gustafsson, F. & Torp-Pedersen, C. Alcohol intake in patients with cardiomyopathy and heart failure: consensus and controversy. Circ. Heart Fail. 15, e009459 (2022).
Kaul, R. et al. Alcohol and atrial fibrillation: a pathophysiologic perspective. Cardiol. Rev. 31, 177–184 (2023).
Puddey, I. B., Mori, T. A., Barden, A. E. & Beilin, L. J. Alcohol and hypertension — new insights and lingering controversies. Curr. Hypertens. Rep. 21, 79 (2019).
Lankisch, P. G., Apte, M. & Banks, P. A. Acute pancreatitis. Lancet 386, 85–96 (2015).
Vanella, G., Archibugi, L., Stigliano, S. & Capurso, G. Alcohol and gastrointestinal cancers. Curr. Opin. Gastroenterol. 35, 107–113 (2019).
Hammoud, N. & Jimenez-Shahed, J. Chronic neurologic effects of alcohol. Clin. Liver Dis. 23, 141–155 (2019).
Chalasani, N. et al. Causes, clinical features, and outcomes from a prospective study of drug-induced liver injury in the United States. Gastroenterology 135, 1924–1934 (2008).
European Association for the Study of the Liver. EASL clinical practice guidelines: drug-induced liver injury. J. Hepatol. 70, 1222–1261 (2019).
Kamath, P. S. et al. A model to predict survival in patients with end-stage liver disease. Hepatology 33, 464–470 (2001).
Jeong, R. et al. Model for end-stage liver disease score as a predictor of short-term outcome in patients with drug-induced liver injury. Scand. J. Gastroenterol. 50, 439–446 (2015).
Schmidt, L. E. & Larsen, F. MELD score as a predictor of liver failure and death in patients with acetaminophen-induced liver injury. Hepatology 45, 789–796 (2007).
Reuben, A., Koch, D. G., Lee, W. & the Acute Liver Failure Study Group. Drug-induced acute liver failure: results of a U.S. multicenter, prospective study. Hepatology 52, 2065–2076 (2010).
FDA. Guidance for Industry Drug-Induced Liver Injury: Premarketing Clinical Evaluation. FDA https://www.fda.gov/media/116737/download (2009).
Nadim, M. K. & Garcia-Tsao, G. Acute kidney injury in patients with cirrhosis. N. Engl. J. Med. 388, 733–745 (2023).
Treem, W. R. et al. Consensus guidelines: best practices for detection, assessment and management of suspected acute drug-induced liver injury during clinical trials in adults with chronic viral hepatitis and adults with cirrhosis secondary to hepatitis B, C and nonalcoholic steatohepatitis. Drug Saf. 44, 133–165 (2021).
Coates, S., Taubel, J. & Lorch, U. Practical risk management in early phase clinical trials. Eur. J. Clin. Pharmacol. 75, 483–496 (2019).
Food and Drug Administration. Guidance for industry and investigators safety reporting requirements for INDs and BA/BE studies. FDA https://www.fda.gov/regulatory-information/search-fda-guidance-documents/safety-reporting-requirements-inds-and-babe-studies (2012).
Walters, S. J. et al. Recruitment and retention of participants in randomised controlled trials: a review of trials funded and published by the United Kingdom health technology assessment programme. BMJ Open 7, e015276 (2017).
Fogel, D. B. Factors associated with clinical trials that fail and opportunities for improving the likelihood of success: a review. Contemp. Clin. Trials Commun. 11, 156–164 (2018).
Wong, C. H., Siah, K. W. & Lo, A. W. Estimation of clinical trial success rates and related parameters. Biostatistics 20, 273–286 (2019).
Briel, M. et al. Exploring reasons for recruitment failure in clinical trials: a qualitative study with clinical trial stakeholders in Switzerland, Germany, and Canada. Trials 22, 844 (2021).
Kasenda, B. et al. Prediction of RECRUITment in randomized clinical trials (RECRUIT-IT) — rationale and design for an international collaborative study. Trials 21, 731 (2020).
Jacques, R. M. et al. Recruitment, consent and retention of participants in randomised controlled trials: a review of trials published in the National Institute for Health Research (NIHR) Journals Library (1997–2020). BMJ Open 12, e059230 (2022).
Natale, P. et al. Transparency, trust and minimizing burden to increase recruitment and retention in trials: a systematic review. J. Clin. Epidemiol. 134, 35–51 (2021).
Bentley, C. et al. Conducting clinical trials — costs, impacts, and the value of clinical trials networks: a scoping review. Clin. Trials 16, 183–193 (2019).
Gul, R. B. & Ali, P. A. Clinical trials: the challenge of recruitment and retention of participants. J. Clin. Nurs. 19, 227–233 (2010).
Comerford, M. et al. Challenges in patient enrollment and retention in clinical studies for alcoholic hepatitis: experience of the TREAT consortium. Alcohol Clin. Exp. Res. 41, 2000–2006 (2017).
Dasarathy, S. et al. Development and evaluation of objective trial performance metrics for multisite clinical studies: experience from the AlcHep Network. Contemp. Clin. Trials 138, 107437 (2024).
Mellinger, J. L. & Winder, G. S. Alcohol use disorders in alcoholic liver disease. Clin. Liver Dis. 23, 55–69 (2019).
Winder, G. S., Clifton, E. G., Perumalswami, P. & Mellinger, J. L. The art of interprofessional psychosocial communication: optimizing patient interfaces with psychiatric specialists in liver transplantation. Transpl. Rev. 36, 100728 (2022).
Winder, G. S., Fernandez, A. C. & Mellinger, J. L. Integrated care of alcohol-related liver disease. J. Clin. Exp. Hepatol. 12, 1069–1082 (2022).
Kintz, P. Consensus of the society of hair testing on hair testing for chronic excessive alcohol consumption 2011. Forensic Sci. Int. 218, 2 (2012).
Berger, L. et al. Ethyl glucuronide in hair and fingernails as a long-term alcohol biomarker. Addiction 109, 425–431 (2014).
Lees, R. et al. Comparison of ethyl glucuronide in hair with self-reported alcohol consumption. Alcohol Alcohol. 47, 267–272 (2012).
Vaa, B., Asrani, S., Dunn, W., Kamath, P. & Shah, V. Influence of serum sodium on MELD-based survival prediction in alcoholic hepatitis. Mayo Clin. Proc. 86, 37–42 (2011).
Dunn, W. et al. MELD accurately predicts mortality in patients with alcoholic hepatitis. Hepatology 41, 353–358 (2005).
Sullivan, J. T., Sykora, K., Schneiderman, J., Naranjo, C. A. & Sellers, E. M. Assessment of alcohol withdrawal: the revised Clinical Institute Withdrawal Assessment for Alcohol Scale (CIWA-Ar). Br. J. Addict. 84, 1353–1357 (1989).
Acknowledgements
The authors disclose support for their work from the following funding sources: NIAAA internal funds for FY2022 Logistical Support of NIH-Hosted Meetings to Division of Metabolism and Health Effects. B.P.L. is supported by K23 AA029752 and R01 AA030960. K.W. is supported by R01AA022328. J.M. is supported by K23 026333 and R01 030748, R01 030969 and R01 030470. R.B. is supported by U01 AA026264. K.S.D. is supported by P50 AA012870. P.S.K. is supported by AA26974. L.L. is supported by the NIDA/NIAAA IRPs. B.C. is supported by the NIDA IRP. T.G.C. is supported by K23 AA031310. S.D. is supported by P50 AA024333; R01 AA021890; 3U01AA026976 — 03S1 and U01 AA 026976. M.E.M. is supported by U01 AA020890; R01 DA042094; P50 AA02611; P01 AA029544 and R01 AA030368. L.E.N. is supported by U01 AA026264, U01 AA026938 and P50 AA024333. M.C.M. is supported by U01 AA026975 and R01 AA030956. The authors thank P. Stein and C. Winchell from the FDA, Maryland, USA, for their participation in the in-person meeting in July 2022. The views expressed in this paper are those of the authors and do not necessarily represent the opinions of the FDA, the US Department of Health and Human Services or the US government.
Author information
Authors and Affiliations
Contributions
All authors researched data for the article, wrote the article and reviewed and/or edited the manuscript before submission. M.C.M., B.P.L., K.W., J.M., R.B., S.D., N.D., A.F.D., D.E.F., A.C.F., P.S.K., K.M.K., L.L., A.L., A.J.S., N.L.S., N.A.T., M.R.T., E.C.V., S.R. and L.E.N. contributed substantially to discussion of the content.
Corresponding authors
Ethics declarations
Competing interests
R.B. is a consultant for GlaxoSmithKline and Novo Nordisk. B.P.L. is a consultant for GlaxoSmithKline, Novo Nordisk and HepaTX. J.M. is a consultant for GlaxoSmithKline. I.D. is on the Board of Amygdala Neuroscience. A.J.S. has ownership interests in Durect, Tiziana, Exhalenz, Inversago, Galmed and Genfit and is a consultant to Intercept, Gilead, Merck, Boehringer Ingelhiem, Eli Lilly, Novo Nordisk, 89BIO, Pfizer, Regeneron, Avant Sante, Hemoshear, Takeda, GlaxoSmithKline, Amgen, Genentech, Histoindex, Path AI, Bristol Myers Squibb, Malinckrodt, Salix, Ocelot, Astra Zeneca, Madrigal, Hanmi, LG and Fortress Bio. A.L. is a consultant for GlaxoSmithKline. M.R.T. is a consultant for GlaxoSmithKline, Resolution Therapeutics, HepaTx, Galecto, Durect, Intercept and Prodigy. M.R.L. receives research support from TARGET PharmaSolutions, AbbVie to University of Wisconsin. E.C.V. receives research support from Salix. N.A.T. receives research support from GSK; Genentech-Roche; Helio Health; Durect Corp; Gilead Sciences; Eiger Pharmaceuticals; Madrigal to her institution. N.L.S. is an employee of Durect Corporation. K.W. is a member of the Alcohol Clinical Trials Initiative (ACTIVE) Workgroup. In the past 36 months, its activities were supported by Alkermes, Dicerna, Ethypharm, Lundbeck, Mitsubishi and Otsuka. M.C.M. is a consultant for GlaxoSmithKline, Prodigy, HepaTX and a Board member of Amygdala Neuroscience; research support to his institution from Durect. The other authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Gastroenterology & Hepatology thanks Helena Cortez-Pinto, who co-reviewed with Juliana Serrazina; Juan Pablo Arab; and Alexander Krag for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR): https://www.psychiatry.org/psychiatrists/practice/dsm
ICD-11: https://icd.who.int/en
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lee, B.P., Witkiewitz, K., Mellinger, J. et al. Designing clinical trials to address alcohol use and alcohol-associated liver disease: an expert panel Consensus Statement. Nat Rev Gastroenterol Hepatol 21, 626–645 (2024). https://doi.org/10.1038/s41575-024-00936-x
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41575-024-00936-x
This article is cited by
-
Incorporating genetic variations in alcohol-associated liver disease trials for East Asian populations
Nature Reviews Gastroenterology & Hepatology (2025)
-
Reply to ‘Incorporating genetic variations in alcohol-associated liver disease trials for East Asian populations’
Nature Reviews Gastroenterology & Hepatology (2025)
-
Pharmacological and Nonpharmacological Interventions to Address Sleep Disturbance in Substance use Disorders
Current Sleep Medicine Reports (2025)
-
Clinical trial design, biomarkers and end points in metabolic and alcohol-related liver disease
Nature Reviews Gastroenterology & Hepatology (2025)
-
Shaping new paths in clinical trial design to address alcohol use disorders and alcohol-associated liver disease
Nature Reviews Gastroenterology & Hepatology (2024)