Abstract
Prenatal exposure to perfluoroalkyl and polyfluoroalkyl substances (PFASs) may cause adverse birth outcomes. Thyroid hormones may play a key role in mediating the effects of PFAS. We enrolled 374 mother-infant pairs from the Ezhou birth cohort study between 2019 and 2020. Eight PFASs and six thyroid hormones were measured in maternal serum during the first trimester of pregnancy. Neonatal growth metrics, including birth weight, length, head circumference, and gestational age, were acquired. Multivariate linear regression was performed to determine the associations between maternal serum PFAS and thyroid hormone levels and birth outcomes and a mediation analysis was also conducted. Except for perfluoroheptanoic acid (41.2%), the other seven PFAS detection rates were more than 85%, and the highest median concentration was observed for PFOSA with levels of 5.21 ng/mL. After controlling for typical confounders, we observed a decrease in birth length (cm) with increasing serum concentrations of perfluorononanoic acid (PFNA) (β = -0.54; 95% CI = -1.0, -0.08) and perfluorohexane sulfonate (PFHxS) (β = -0.64; 95% CI = -0.86, -0.42). Additionally, a decrease in birth head circumference was observed with increasing concentrations of perfluorooctanote (PFOA) (β = -0.73, 95% CI = -1.19, -0.27) and PFHxS (β = -0.30; 95% CI = -0.53, -0.07). Maternal free triiodothyronine (FT3) mediated 36.7% of the negative association between PFNA and birth length, and free thyroxine (FT4) mediated 30.8% of the effect of PFOA on head circumference. When performing stratified analysis by infant sex, the associations might differ between boys and girls. Our study suggested prenatal exposure to some PFASs was negatively associated with birth length and circumference, and FT3 and FT4 may partly mediate the association.
Similar content being viewed by others
Introduction
Perfluoroalkyl and polyfluoroalkyl substances (PFASs) are synthetic fluorine-bearing compounds that have been widely used in consumer products, including surfactants, textiles, fire-fighting foams, lubricants, clothing, and food packaging for decades1. With strong carbon-fluorine bonds, PFASs, especially those with a long carbon chain, such as perfluorohexane sulfonate (PFHxS), perfluorooctane sulfonate (PFOS) and perfluorooctanote (PFOA) can persist in the environment and human body for a long time, with estimated half-lives of 8.5, 5.4 and 3.8 years for PFHxS, PFOS, and PFOA in human serum, respectively2. Serum has been widely used as a reliable matrix for measuring PFAS exposure levels3.
Researchers have reported significant associations between prenatal PFAS concentrations and birth outcomes. Kashino et al. investigated 1985 mother-infant pairs in Japan and reported that prenatal perfluorononanoic acid (PFNA) and perfluorodecanoic acid (PFDA) concentrations were negatively associated with birth weight4. A study from Spain also found marked associations between prenatal exposure to PFOA, PFHxS, and PFNA and birth weight, with reductions in birth weight ranging from 8.6 to 10.3 g per doubling of exposure5. A study from China demonstrated that prenatal exposure to PFOS and perfluoroheptanoic acid (PFHpA) was associated with a higher risk of preterm birth6. However, the mechanisms of the impact of prenatal PFAS exposure on birth outcomes remain unclear.
A growing number of epidemiological studies have demonstrated that PFASs can influence reproductive functions through the regulation of thyroid hormones; however, the results are inconsistent. A study involving pregnant women indicated positive associations between PFAS serum concentrations and thyroid stimulating hormone (TSH) and free thyroxine (FT4) levels7, whereas other studies found either no association8 or a negative association between PFAS concentrations and thyroid hormone levels9. In addition, a fetus is completely reliant on maternal thyroid hormones until 18–20 weeks of gestation, when fetal thyroid hormone production begins10. Hence, maternal thyroid hormones during early pregnancy play a critical role in early birth neural maturation and development. Therefore, we hypothesized that thyroid hormones mediate the effects of PFAS exposure on prenatal development. Furthermore, previous studies have indicated that PFAS have endocrine disruptive potential11, and some PFAS possess estrogenic or anti-androgenic activity12. The sex-dependent associations between prenatal exposure to PFAS and birth outcomes should be further explored.
In this study, we aimed to (1) examine the association between prenatal PFAS exposure and birth outcomes based on a cohort analysis, (2) assess the potential mediating role of maternal thyroid hormones, and (3) evaluate sex-dependent differences in the mediating effects of thyroid hormones.
Materials and methods
Study population and sample collection
Study participants were selected among subjects of the Ezhou birth cohort study, which is an ongoing longitudinal study initiated in January 2019 that aims to evaluate the impact of environmental factors on the health of pregnant women and their children. The details of this study have been previously described13. Women residing in Ezhou City, Hubei Province, China, were recruited in early pregnancy and provided informed consent for their participation in this study. At enrollment, the pregnant women were asked to donate a blood sample for PFAS and thyroid hormone analysis, and a face-to-face questionnaire survey including social demographics, lifestyle habits, and health status was administered by trained interviewers. The women were eligible for enrollment if the following criteria were satisfied: (1) resident of Ezhou City, (2) willing to participate in monthly antenatal examinations and donate serum and urine samples, and (3) planning to deliver in the healthcare center. Between January 2019 and January 2020, 546 pregnant women met the eligibility criteria and agreed to participate in the study. According to the principles for bio-sample usage, we selected urine and serum samples with a volume exceeding 10 mL and 2 mL, respectively, for this study. Maternal PFAS measurements were carried out for 456 (84.1%) of the urine samples in the first trimester of pregnancy (median gestation: 8.4 weeks). After excluding 25 pregnant women who did not complete the questionnaire, 6 pregnant women who had an abortion, and 46 infants who did not participate in the physical examination, a total of 379 mother-infant pairs were included in this study.
PFAS exposure measurement
Maternal blood specimens were collected during the first trimester of pregnancy. The samples were centrifuged at 5000 rpm for 5 min immediately after collection at the hospital. The serum was then separated, stored at -80℃, and shipped on dry ice to the laboratory at Hubei University of Chinese Medicine for analysis. The levels of eight PFASs were analyzed: PFOA, PFOS, PFHxS, PFNA, PFDA, PFOSA, perfluoroheptanesulfonic acid (PFHpS), and PFHpA. The PFAS and internal standard solutions (13C4-PFOS and 13C4-PFOA) were purchased from Sigma-Aldrich (St. Louis, MO, USA) and Cambridge Isotope Laboratories (Andover, MA, USA), respectively. The purity of all standards was ≥ 99%.
The levels of all PFASs were estimated using high-performance liquid chromatography coupled with tandem mass spectrometry (Agilent 6495, Agilent Technologies Co., California, USA) at Hubei University of Chinese Medicine. Sample extract (10 µL) was injected into a C18 column (2.1 × 100 mm, 1.8 μm; Agilent, USA) maintained at 40 ℃. The flow rate was 0.4 mL/min. The solvent phases consisted of (A) distilled water containing 5 mmol/L ammonium acetate and (B) methanol. The gradient elution began with phase A at 5%, increased to 10% at 2 min, and then increased to 25% at 4 min, 50% at 10 min, 75% at 15 min, and 95% at 20 min, and was held for 2 min. The precursor and product ions for each target analyte, as well as applied collision energy and retention time, are summarized in Supplementary Table S1.
Quantification was performed using the internal standard method (Supplementary Table S2). The recoveries ranged from 87 to 112%. The calibration curve ranged from 0.1 ng/mL to 200 ng/mL (R2 > 0.998). Blank and double spike samples with low (0.1 ng/mL) and high (10 ng/mL) concentrations were repeatedly measured at intervals of 20 samples. The recoveries of spike samples ranged from 85.7 to 112.5%, and the relative standard deviation was < 20%. The detection limits (LODs), defined as a signal-to-noise ratio of 3, ranged from 0.006 to 0.200 ng/mL for select PFASs. Concentrations below the LOD were replaced by the value of LOD/√2.
Thyroid hormone measurement
The levels of thyroid hormones, including TSH, free triiodothyronine (FT3), FT4, total thyroxine (TT4), total triiodothyronine (TT3), and thyroglobulin (TG) were also measured in first-trimester blood serum using an automated chemiluminescence immunoassay (Roche, Germany) and various commercial enzymatic assay kits (Shanghai Lianshuo Biotechnology Co., Ltd, China) at Ezhou Maternal and Child Health hospital. The intra-assay coefficient of variation (CV) for all hormones ranged from 4.1% (for TT3) to 8.9% (for TG), and the inter-assay CV ranged from 3.2% (for FT4) to 8.2% (for FT4).
Birth outcomes
Birth outcomes included birth weight (g), length (cm), head circumference (cm), gestational age (weeks) and infant sex, were obtained from the participants’ medical records. Above measurements are normality distribution and show as “Mean ± SD” in Table 1. The gestational age was calculated according to the date of the last menstrual period, as provided by the pregnant women.
Statistical analyses
The baseline characteristics of the study population were described using the frequency (%) or mean ± standard deviation. The concentrations of PFASs and thyroid hormones were expressed as medians and percentiles. The comparison of characteristics between girls and boys was examined using an independent t-test for continuous variables.
PFAS and thyroid hormone concentrations were ln-transformed (Ln) to reduce the influence of extreme values and make interpretations more consistent when the range of compounds varied. The estimated effect was therefore interpreted as the unit change in birth outcomes for each Ln unit increase in prenatal PFAS and thyroid hormone levels.
Multivariate linear regression was performed to estimate β coefficients and 95% confidence intervals (CIs) to explain the relationship between PFAS and thyroid hormone concentrations and birth weight, length, head circumference, and gestational age. Potential covariates were included if they had been previously reported to be relevant to PFAS and developmental outcomes14,15,16. The change-in-effect estimate method was adopted, whereby covariates that altered the main effect estimate by 10% or more were introduced into the models. Ultimately, maternal age at delivery, pre-pregnancy body mass index (BMI), gestational weight gain, living area, maternal education, family income, parity, method of delivery, maternal occupation, second-hand smoke exposure, and the sex of the infant were included (Supplementary Table S3).
We also determined the associations between PFAS and thyroid hormones using multivariable linear regression models. Based on previously reported literature and the change-in-effect estimate method17, we included similar covariates as mentioned above, except for the living area and family income (Supplementary Table S3).
A mediation analysis was conducted to elucidate the potential mediating role of thyroid hormones on the effects of serum PFAS levels on birth outcomes. As described in previous studies, to be classified as a mediator, a factor must satisfy the following criteria: (1) changes in exposure level cause a significant change in the outcome, (2) there is a significant association between the mediator and the outcome, and (3) a change in the level of exposure leads to significant changes in the mediator18. If these three requirements are met, the impact of the mediator can be determined. The total effect (TE) of PFAS concentration on birth outcomes was decomposed into the direct effect (DE; i.e., the effect of PFAS concentration on the neonatal outcome that is not mediated by thyroid hormones) and the natural indirect effect (IE; i.e., the effect that is mediated through thyroid hormones).
The proportion of influence from thyroid hormone mediation was calculated using the ratio of the IE to the TE (i.e., IE/IE + DE). Two-sided p-values of < 0.05 were regarded as statistically significant. All data were estimated using R version 3.5.3 (The R Foundation for Statistical Computing, Vienna, Austria). In addition, considering that some PFASs disrupt estrogenic or anti-androgenic activity, the sex-dependent association between prenatal exposure to PFASs and maternal TSH was explored through a stratified analysis of the results based on birth sex.
Sensitivity analyses
To ensure the robustness of our findings, many sensitive analyses were conducted. Firstly, we adjusted for creatinine as a covariate in the model as proposed by the previous study. Then, we excluded infants with preterm delivery (gestation age < 37 complete weeks, n = 15) and low birth weight (< 2500 g, n = 12) to further evaluate the robustness of our analysis results.
Results
Participant characteristics
The characteristics of the 379 mother-infant pairs in the present study are displayed in Table 1. The average age of the pregnant women was 27.3 ± 3.8 years. Most of the pregnant women were primiparous (67.8%) and lived in households with an annual income of less than USD 10,000 dollars (68.1%). Approximately half of the births (n = 201, 53.0%) were male. The mean gestational age and birth weight, length, and head circumference of infants at delivery were 39.5 ± 1.4 weeks, 3376.2 ± 524.4 g, 50.5 ± 2.8 cm, and 33.4 ± 1.1 cm, respectively. A comparison of the characteristics of 201 boys and 178 girls of birth did not reveal any statistically significant differences (Table 1).
Serum levels of PFASs and thyroid hormones
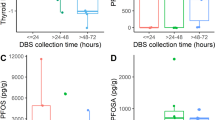
The levels of eight PFASs in the serum of the pregnant women in this study are summarized in Table 2. The PFASs detected at the highest rates were PFOA (100%), PFNA (100%) and PFDA (100%), followed by PFOS (97.7%), PFHpS (97.2%), PFOSA (92.6%), and PFHxS (86.5%), with median concentrations of 1.40 ng/mL, 1.55 ng/mL, 0.87 ng/mL, 3.08 ng/mL, 0.87 ng/mL, 5.21 ng/mL, and 1.12 ng/mL, respectively. Notably, as the detection rate of PFHpA was less than 50%, it was excluded from subsequent analysis.
Table 2 also shows the maternal serum thyroid hormone levels of the pregnant women. All maternal thyroid hormone levels were within the normal range19. Because of the skewed distribution, natural logarithm (Ln) transformations of the thyroid hormone levels were performed to better approximate normal distributions. The median serum levels of TSH, FT3, FT4, TT3, TT4, and TG were 1.62 mlU/L, 4.68 pmol/L, 14.48 pmol/L, 1.28 nmol/L, 133.5 nmol/L and 13.8 nmol/L, respectively.
The associations between serum PFAS and maternal thyroid hormone levels based on multivariate linear regression models are shown in Fig. 1 and Supplementary Table S4. We found that each one Ln unit increment of PFOS and PFNA was associated with 0.36 lg-unit (95% CI: -0.54, -0.18) and 0.33 lg-unit (95% CI: -0.50, -0.15) decrease in TSH levels, respectively. Additionally, the levels of PFNA (β = -0.35; 95% CI: -0.49, -0.21) and PFHpS (β = -0.23, 95% CI: -0.32, -0.14) were negatively associated with the FT3 level, and the level of PFOA (β = -0.31; 95% CI: -0.50, -0.13) was negatively associated with the TSH level. However, the level of PFDA (β = 0.24; 95% CI: 0.10, 0.37) was positively associated with the TT4 level.
Estimated differences and 95% confidence intervals (CIs) for birth outcomes by In-transformed increase in maternal serum PFASs levels. All models were adjusted for maternal age at delivery, level of education, smoking status, occupation, pre-pregnancy body mass index (BMI), gestational weight gain, family income, parity, method of delivery, living area, and the sex of the infant.
Analyses split according to sex revealed that the level of PFNA (β = -0.43, 95% CI: -0.67, -0.19) was negatively associated with the FT3 level in women pregnant with boys. For women pregnant with girls, the levels of PFOS (β = -0.42; 95% CI: -0.70, -0.14) and PFNA (β = -0.48; 95% CI: -0.60, -0.36) were negatively associated with the TSH level, the level of PFHpS was negatively associated with the FT3 (β = -0.48; 95% CI: -0.67, -0.29) and TT4 (β = -0.46; 95% CI: -0.64, -0.31), and the level of PFOA was negatively associated with the FT4 (β = -0.42, 95% CI: -0.64, -0.20) and TG (β = -0.45, 95% CI: -0.72, -0.18) levels, but positively associated with the FT3 (β = 0.18, 95% CI: 0.12, 0.24) level.
Associations between PFASs exposure and birth outcomes
The association between maternal PFAS exposure and infant birth outcomes is shown in Fig. 2 and Supplementary Table S5. For every Ln increase in PFOA, we observed a decrease in the infant’s birth weight of 43.2 g (95% CI: -75.8, -10.6). Additionally, there was negative association between PFNA (β = -0.54 cm, 95% CI:-0.90, -0.18) and PFHxS (β = -0.64 cm, 95% CI: -0.86, -0.42) concentration and birth length. Furthermore, we found that every Ln increase in serum PFOA and PFHpS concentration was associated with a decrease in infant head circumference of 0.73 cm (95% CI: -1.19, -0.27) and 0.30 cm (95% CI: -0.53, -0.07), respectively. Moreover, each Ln increase in PFDA concentration was negatively associated with infant gestational age (β = -0.18 week, 95% CI: -0.26, -0.10).
Estimated differences and 95% confidence intervals (CIs) for birth outcomes by Log-transformed increase in maternal serum thyroid hormone levels. All models were adjusted for maternal age at delivery, level of education, smoking status, occupation, pre-pregnancy body mass index (BMI), gestational weight gain, family income, parity, method of delivery, living area, and the sex of the infant.
Infant sex modified the effect of prenatal PFAS exposure on birth outcome to some extent (Fig. 2). In male infants, we observed significant negative associations between maternal PFNA (β = -0.63 cm; 95% CI: -1.12, -0.14) and PFHxS (β = -0.74 cm; 95% CI: -0.98, -0.50) levels and birth length, as well as PFOA (β = -0.22 weeks; 95% CI: -0.40, -0.04) and PFHpS (β = -0.07 weeks; 95% CI: -0.13, -0.01) levels and gestational age. In females, there were negative associations between the maternal PFOA level and birth weight (β = -53.6 g; 95% CI: -77.8, -29.4), PFHxS level and birth length (β = -0.48 cm; 95% CI: -0.64, -0.32), PFOS (β = -0.64 cm; 95% CI: -0.89, -0.39), PFHpS (β = -0.38 cm; 95% CI: -0.67, -0.09) levels and head circumference, and PFNA concentration and gestational age (β = -0.16 weeks; 95% CI: -0.30, -0.08).
Associations between thyroid hormone levels and birth outcomes
The associations between maternal thyroid hormone levels and birth outcomes are shown in Fig. 3 and Supplementary Table S6. For all infants, a one-unit increase in the Ln maternal serum of TSH was associated with a decrease of 26.2 g (95% CI:-45.6, -6.8) in birth weight. Maternal FT3 (β = -0.38 cm; 95% CI: -0.75, -0.02) and TT3 (β = -0.66 cm; 95% CI: -0.86, -0.47) levels were negatively associated with birth length, FT4 (β = -0.46 cm; 95% CI: -0.62, -0.30) and TG (β = -0.32 cm; 95% CI: -0.61, -0.02) levels were negatively associated with head circumference, and TT4 level was negatively associated with gestational age (β = -0.16 week; 95% CI: -0.27, -0.05).
Estimated differences and 95% confidence intervals (CIs) for thyroid hormones by ln-transformed increase in maternal serum PFASs levels. All models were adjusted for maternal age at delivery, level of education, smoking status, occupation, pre-pregnancy body mass index (BMI), gestational weight gain, family income, parity, method of delivery, living area, and the sex of the infant.
In male infants, the maternal FT3 (β = -0.50 cm; 95% CI: -0.82, -0.18) and TT4 (β = -0.54 cm; 95% CI: -1.06, -0.02) levels were negatively associated with birth length, and TT4 (β = -0.38 week; 95% CI: -0.58, -0.17) levels were negatively associated with gestational age. In female infants, the maternal TSH level was negatively associated with birth weight (β = -18.2 g; 95% CI: -30.8, -5.6), TT3 levels were negatively associated with birth length (β = -0.81 g; 95% CI: -0.94, -0.70), FT4 (β = -0.59 cm; 95% CI: -0.92, -0.26), and TG (β = -0.42 cm; 95% CI: -0.79, -0.05) levels were negatively associated with head circumference, respectively. However, we found a significant positive association between the maternal TSH level and infant gestational age (β = 0.12 weeks; 95% CI: 0.04, 0.20).
Mediating effects of thyroid hormones
Considering that a mediator must be associated with the exposure and the outcome, we conducted mediation analysis to assess the potential role of maternal serum FT3 level as a mediator of the association between prenatal PFNA exposure and birth length, FT4 level as a mediator of the association between PFOA exposure and head circumference, FT4 level as a mediator of the association between PFHpS exposure and head circumference, and TT4 level as a mediator of the association between PFDA exposure and gestational age for all infants. Mediation analysis indicated that 36.7% of the effect of PFNA exposure on birth length was significantly mediated by maternal FT3 level, and 30.8% of the effect of PFOA exposure on head circumference was mediated by maternal FT4 level (Fig. 4). No significant mediation by thyroid hormones was observed in the effect of PFAS exposure on birth weight or gestational age.
Mediation analysis of the estimated effect (95% confidence intervals) of maternal serum PFASs levels and newborn outcomes by maternal serum thyroid hormones for all infants/by sex. The figure presents maternal serum thyroid hormones as a mediator, the estimate of the indirect effect (IE), the estimate of the direct effect (DE), and the proportion of mediation (IE/IE + DE). The mediation model was adjusted for maternal age at delivery, level of education, smoking status, occupation, pre-pregnancy body mass index (BMI), gestational weight gain, family income, parity, method of delivery, living area, and the sex of the infant.
In female infants, the estimated proportion of the negative association between PFHpS exposure and head circumference explained by the maternal TT4 level was 47.4%, and the proportion of the association between PFNA exposure and gestational age mediated by the maternal TSH level was 57.5%. No association was observed in male infants.
Sensitivity analysis
After excluding infants with preterm gestational age or low birth weight, similar results remained for the effects of prenatal PFAS exposure and maternal thyroid hormone levels on birth outcomes (Supplementary Tables S7, S8, and S9).
Discussion
In this cohort study, we systematically examined the prenatal PFAS in maternal serum and their possible impact on birth outcomes and explored the mediation roles of thyroid hormones in the association. Additionally, increased maternal serum concentration of PFNA and PFHxS were associated with decrease birth length, PFOA and PFHpS were negatively associated with head circumference, and PFDA was negatively associated with infant gestational age. Furthermore, maternal thyroid mediated 30 − 36% of the effect of prenatal PFAS exposure on birth outcomes. These associations differed between boys and girls.
Notably, the serum concentrations of PFOA, PFNA, and PFDA, despite their high detection rates (100%), were lower in this study than in previous studies. For example, the median serum concentration of PFOA (1.40 ng/mL) in our study was lower than those reported in studies of Japanese (2.0 ng/mL)20 and Dutch women (1.61 ng/mL)9. Additionally, the concentration of PFOS was lower in our study than in a study of pregnant women at a median gestational age of 12 weeks from the Odense Child Cohort in Denmark (median: 7.72 ng/mL)21 and a study that consisted of 114 participants in Ronneby, Sweden (median 13.0 ng/mL)2. However, the PFNA and PFDA concentrations in our study were slightly higher than those reported in studies from Sweden (0.63 and 0.26 ng/mL, respectively)22 and Japan (0.51 and 0.25 ng/mL, respectively)20. The discrepancies in PFAS distribution between our study and other reports may be due to differences in study design and population demographics.
In our study, a higher prenatal PFOA exposure level was associated with a lower birth weight in females, whereas this association was not significant for males. This is consistent with previous reports, which found that the significant association between prenatal PFOA exposure and birth weight persisted only in female infants after stratification by sex23,24. Our results, showing that prenatal PFNA exposure was associated with decreased body size in infants, are aligned with findings from cohort studies conducted in Colorado, United States25 and Hokkaido, Japan4. After categorizing the data by sex, we determined that this association existed in male infants but not female infants. The gender-specific bioconcentrations of PFNA may be attributed to differences in uptake, metabolism, distribution, elimination, and nutritional needs between males and females, which provides an additional explanation of the gender-specific sensitivity or toxicity of PFNA on body size3. Furthermore, we observed a significant negative association between prenatal exposure to PFHpS and head circumference in female infants. Additionally, exposure to PFDA, which has long carbon chains, was negatively associated with gestational age regardless of the sex of the infant. However, the concentration of PFDA in our study was higher than that reported in a study of Western (Danish, Norwegian, and Australian) populations26. Therefore, the concentration of PFDA in humans requires further investigation.
Associations between prenatal PFAS exposure and maternal thyroid hormone levels were also evaluated. We determined that maternal PFOS and PFNA levels were negatively associated with the TSH level, and PFNA and PFHpS levels were negatively associated with the FT3 level. However, our results differed from those of a Norwegian study27, which reported that women with higher PFOS exposure had increased TSH levels. The reason for this difference might be that the subjects of the study were in the second trimester of pregnancy, leading to a higher serum PFOS concentration (median: 12.73 ng/mL) compared to that in our study. We also found that the maternal PFNA concentration was positively associated with the TT4 level. After categorizing the data by infant sex, a greater number of associations were observed between PFAS concentrations and thyroid hormone levels in pregnant women and birth outcomes of female infants. It is hypothesized that PFAS may increase the hepatic production of thyroxine-binding globulin (TBG)28, and there is an estrogen-induced increase in thyroxine-binding globulin (TBG) production during pregnancy. Estrogen also reduces TBG clearance, thereby increasing its concentration in the body29. This may increase thyroid hormone concentration, whereas androgens have the opposite effect. Consequently, the results show a significant association in girls but not in boys. These results are consistent with previous reports from Norway27 and Korea30, which show that females are more sensitive to EDC.
Similar to the results of animal studies and epidemiologic studies, our results showed that during the first trimester, thyroid dysfunction is associated with suboptimal intrauterine growth and adverse neonatal outcomes. Moreover, in all infants, maternal FT3 demonstrated a mediating effect of 36.7% on the negative association between prenatal PFAS exposure and infant birth length, and maternal FT4 had a mediating effect of 30.8% on the negative association between prenatal PFAS exposure and infant head circumference. Evidence from animal studies has shown that exposure to PFAS can cause histopathologic alterations in the thyroid and reduce circulating thyroid hormone levels in rats, possibly by binding to thyroid hormone receptors and altering their signaling or by affecting thyroid hormone biosynthesis and biotransport31. A study in pregnant mice also observed an effect of PFOS on signaling pathways involved in placental growth, causing follicular shrinkage, loss of TG, and fibrosis of the interfollicular epithelium28. However, when categorizing the data by infant sex, this mediation effect was only observed in females. Thus, additional research is required to determine whether this relationship is sexually dimorphic and to investigate the biological mechanisms of this phenomenon.
The strengths of the present study are that sex-specific associations between maternal PFAS levels and prenatal development were assessed using samples collected in early pregnancy, and mediation by thyroid hormones was explored. Data on maternal TT3, FT3, TT4, FT4, TSH, and TG levels were available, which enabled us to perform a thorough and nuanced examination of the potential effects of PFAS exposure on thyroid hormones. However, the potential limitations of this study should be addressed. First, PFAS-Thyroid hormone associations are cross-sectional, thus limiting the inference of causal relationships. Secondly, we used first-trimester measurements to determine the level of prenatal PFAS exposure and to evaluate its impact on infant outcomes, which led to misclassification. However, because of the long half-lives of these chemical compounds, moderate to high reliability of maternal PFAS measurements during pregnancy, and the reliance of the fetus on placental transfer of maternal thyroid hormones during the first 12 weeks of gestation, relying on a primary estimation may have minimal influence on the results. Third, although at least 23 PFASs can be detected in serum samples, we detected only 8 PFASs related to neonatal development in this study, which may have led to an underestimation of the effect of PFAS exposure on birth outcomes. Finally, all study participants were from one city in China. Therefore, the generalizability of the results to other countries and socioeconomic groups is limited.
Conclusions
Our analysis of maternal PFAS and thyroid hormone levels and infant birth weight, length, head circumference and gestational age revealed the effect of prenatal PFAS exposure on birth outcome. Overall, some maternal PFASs exposure affects birth outcomes, and female infants were more susceptible to prenatal PFAS exposure than male infants. Furthermore, thyroid hormones were shown to mediate the effect of PFAS exposure to some extent.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
Abbreviations
- PFASs:
-
Perfluoroalkyl and polyfluoroalkyl substances
- PFNA:
-
Perfluorononanoic acid
- PFHxS:
-
Perfluorohexane sulfonate
- PFOA:
-
Perfluorooctanote
- PFOS:
-
Perfluorooctane sulfonate
- PFDA:
-
Perfluorodecanoic acid
- PFHpA:
-
Perfluoroheptanoic acid
- PFHpS:
-
Perfluoroheptanesulfonic acid
- FT3:
-
Free triiodothyronine
- FT4:
-
Free thyroxine
- TSH:
-
Thyroid stimulating hormone
- TT4:
-
Total thyroxine
- TT3:
-
Total triiodothyronine
- TG:
-
Thyroglobulin
- CV:
-
Coefficient of variation
- Ln:
-
Ln-transformed
- CIs:
-
Confidence intervals
- BMI:
-
Body mass index
- DE:
-
Direct effect
- IE:
-
Indirect effect
- LODs:
-
Detection limits
- TE:
-
Total effect
References
Evich, M. G. et al. Per- and polyfluoroalkyl substances in the environment. Science 375(6580), eabg9065 (2022).
Li, Y., Andersson, A., Xu, Y., et al. Determinants of serum half-lives for linear and branched perfluoroalkyl substances after long-term high exposure—A study in Ronneby, Sweden. Environ. Int. 163, (2022).
Wang, Y. et al. Prenatal exposure to perfluorocarboxylic acids (PFCAs) and fetal and postnatal growth in the Taiwan maternal and infant cohort study. Environ. Health Perspect. 124(11), 1794–1800 (2016).
Kashino, I., Sasaki, S., Okada, E., et al. Prenatal exposure to 11 perfluoroalkyl substances and fetal growth: A large-scale, prospective birth cohort study. Environ. Int. 136, (2020).
Manzano-Salgado, C. B. et al. Prenatal exposure to perfluoroalkyl substances and birth outcomes in a Spanish birth cohort. Environ. Int. 108, 278–284 (2017).
Liao, Q., Tang, P., Song, Y. Y., et al. Association of single and multiple prefluoroalkyl substances exposure with preterm birth: Results from a Chinese birth cohort study. Chemosphere 307, (2022).
Aimuzi, R. et al. Perfluoroalkyl and polyfluoroalkyl substances and fetal thyroid hormone levels in umbilical cord blood among newborns by prelabor caesarean delivery. Environ. Int. 130, 104929 (2019).
Preston, E. V., Webster, T. F., Oken, E., et al. Maternal plasma per- and polyfluoroalkyl substance concentrations in early pregnancy and maternal and neonatal thyroid function in a prospective birth cohort: Project viva (USA). Environ. Health Perspect. 126(2), (2018).
Derakhshan, A., Kortenkamp, A., Shu, H., et al. Association of per- and polyfluoroalkyl substances with thyroid homeostasis during pregnancy in the SELMA study. Environ. Int. 167, (2022).
Rickard, B. P., Rizvi, I., Fenton, S. E. Per- and poly-fluoroalkyl substances (PFAS) and female reproductive outcomes: PFAS elimination, endocrine-mediated effects, and disease. Toxicology 465, (2022).
Gao, Y. et al. Effect modification by maternal vitamin D status in the association between prenatal exposure to per- and polyfluoroalkyl substances and neurodevelopment in 2-year-old children. Environ. Int. 185, 108563 (2024).
Villeneuve, D. L. et al. Verification of in vivo estrogenic activity for four per- and polyfluoroalkyl substances (PFAS) identified as estrogen receptor agonists via new approach methodologies. Environ. Sci. Technol. 57(9), 3794–3803 (2023).
Wu, W., Ma, Z. L., Yang, F., et al. Urinary phthalate metabolites in pregnant women: occurrences, related factors, and association with maternal hormones. Environ. Sci. Pollut. Res. Int. (2022).
Kashino, I. et al. Prenatal exposure to 11 perfluoroalkyl substances and fetal growth: A large-scale, prospective birth cohort study. Environ. Int. 136, 105355 (2020).
Derakhshan, A. et al. Association of per- and polyfluoroalkyl substances with thyroid homeostasis during pregnancy in the SELMA study. Environ. Int. 167, 107420 (2022).
Wu, W. et al. Urinary phthalate metabolites in pregnant women: Occurrences, related factors, and association with maternal hormones. Environ. Sci. Pollut. Res. Int. 29(22), 33372–33382 (2022).
Zheng, T. et al. Adverse birth outcomes related to concentrations of per- and polyfluoroalkyl substances (PFAS) in maternal blood collected from pregnant women in 1960–1966. Environ. Res. 241, 117010 (2024).
Pan, D. et al. Association between maternal per- and polyfluoroalkyl substance exposure and newborn telomere length: Effect modification by birth seasons. Environ. Int. 161, 107125 (2022).
Zha, J. et al. Establishment of reference range for thyroid hormones in normal pregnant women in China’s coastal area. Clin. Exp. Obstet. Gynecol. 41(2), 135–140 (2014).
Tsai, M.-S., Miyashita, C., Araki, A., et al. Determinants and temporal trends of perfluoroalkyl substances in pregnant women: The Hokkaido study on environment and children’s health. Int. J. Environ. Res. Public Health 15(5), (2018).
Jensen, R. C., Glintborg, D., Timmermann, C. A. G., et al. Higher free thyroxine associated with PFAS exposure in first trimester. The Odense Child Cohort. Environ. Res. 212, (2022).
Norén, E., Lindh, C., Glynn, A., et al. Temporal trends, 2000–2017, of perfluoroalkyl acid (PFAA) concentrations in serum of Swedish adolescents. Environ. Int. 155, (2021).
Tsai, M. S., Miyashita, C., Araki, A., et al. Determinants and temporal trends of perfluoroalkyl substances in pregnant women: The Hokkaido study on environment and children’s health. Int. J. Environ. Res. Public Health 15(5), (2018).
Bach, C. C. et al. Perfluoroalkyl acids in maternal serum and indices of fetal growth: The Aarhus Birth Cohort. Environ. Health Perspect. 124(6), 848–854 (2016).
Kishi, R. et al. The association of prenatal exposure to perfluorinated chemicals with maternal essential and long-chain polyunsaturated fatty acids during pregnancy and the birth weight of their offspring: The Hokkaido Study. Environ. Health Perspect. 123(10), 1038–1045 (2015).
Starling, A. P., Adgate, J. L., Hamman, R. F., et al. Perfluoroalkyl substances during pregnancy and offspring weight and adiposity at birth: Examining mediation by maternal fasting glucose in the healthy start study. Environ. Health Perspect. 125(6), (2017).
Harada, K. H. et al. Odd-numbered perfluorocarboxylates predominate over perfluorooctanoic acid in serum samples from Japan, Korea and Vietnam. Environ. Int. 37(7), 1183–1189 (2011).
Berg, V. et al. Assessing the relationship between perfluoroalkyl substances, thyroid hormones and binding proteins in pregnant women; a longitudinal mixed effects approach. Environ. Int. 77, 63–69 (2015).
Davidsen, N. et al. PFOS-induced thyroid hormone system disrupted rats display organ-specific changes in their transcriptomes. Environ. Pollut. 305, 119340 (2022).
O’Shaughnessy, J. et al. Efficacy of eribulin for metastatic breast cancer based on localization of specific secondary metastases: A post hoc analysis. Sci. Rep. 10(1), 11203 (2020).
Shah-Kulkarni, S. et al. Prenatal exposure to perfluorinated compounds affects thyroid hormone levels in newborn girls. Environ. Int. 94, 607–613 (2016).
Dharpure, R., Pramanik, S. & Pradhan, A. In silico analysis decodes transthyretin (TTR) binding and thyroid disrupting effects of per- and polyfluoroalkyl substances (PFAS). Arch. Toxicol. 97(3), 755–768 (2023).
Acknowledgements
We are grateful to all participants and collaborators for their contribution to the cohort study.
Funding
This work was supported by the Natural Science Foundation of Hubei Province (2023AFB973, 2023CFA004) and Science and Technology Research Project of Hubei Provincial Education Department (D20232003).
Author information
Authors and Affiliations
Contributions
Z.W., W.Y.: conceptualization, writing (original draft), agreement to be accountable for all aspects of the work. M.X., B.L.: interpretation of data, revising the manuscript critically. M.C., J.H.: undertook the statistical analysis. P.W., W.W.: supervision, funding acquisition, final approval of the version to be published.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Hubei University of Chinese Medicine (No. 2018-IEC-010). Written informed consent was obtained from individual or guardian participants.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Wang, Z., Yang, W., Xu, M. et al. Associations between gestational exposure to perfluoroalkyl substances, fetal growth, and the mediation effect of thyroid hormones. Sci Rep 14, 25176 (2024). https://doi.org/10.1038/s41598-024-75210-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-75210-w