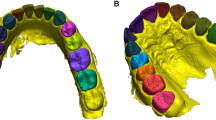
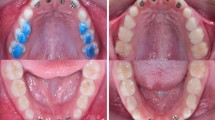
Abstract
The objective of this study was to compare the aging changes of the dental arches in patients treated without extractions and untreated normal occlusion subjects after a four-decade follow-up. This retrospective study evaluated two groups: The Treated Group (Group T) comprised 16 patients (6 male; 10 female) presenting with Class I or Class II malocclusions treated orthodontically without extractions. Dental models were evaluated 3 stages: T1 (pretreatment, 13.20 years), T2 (posttreatment, 15.07 years) and T3 (long-term posttreatment, 50.32 years). The Untreated Group (Group UT) consisted of 22 untreated normal occlusion individuals. The dental casts were evaluated at the ages of 13.32 (T1), 17.82 (T2) and 60.95 years (T3). The dental casts were digitized and the irregularity index, intercanine, interpremolar and intermolar widths, overjet and overbite, arch length and perimeter were measured. Intergroup comparisons were performed with independent t tests (P < 0.05). From T1 to T2, the treated group showed maxillary and mandibular crowding and overjet decrease and a maxillary interpremolar and intermolar width increase compared to the untreated group. From T2 to T3, a greater maxillary and mandibular crowding increase and a greater arch length decrease were observed in the treated group compared to the normal occlusion subjects. Overbite increased in the treated group and decreased in the untreated group. The maturational changes of treated patients were different from untreated normal occlusion subjects. Relapse might have contributed for the greater changes observed in incisor crowding and arch length observed in orthodontically treated patients. The aging changes of untreated normal occlusions and nonextraction treated patients, after a four-decade follow-up, proved to be different, indicating that relapse of orthodontic treatment played a role in aging changes of treated patients.
Similar content being viewed by others
Introduction
Relapse is a topic widely studied in orthodontic literature. Results 40 year after treatment show that anterior crowding increases and arch dimensions decreases in the posttreatment phase in both cases treated with or without extractions1. Besides, there is no significant difference in the changes of anterior alignment and transverse arch dimensions in patients treated with and without premolar extraction, except for a higher percentage of mandibular anterior tooth alignment changes in nonextraction cases1.
The increase of mandibular anterior crowding with aging was also already reported in the literature, even in normal occlusion untreated cases2,3,4,5. Many years after treatment, the changes that occur due to the aging of the occlusion often cannot be distinguished from what is considered a relapse of the orthodontic treatment itself. In this sense, some authors claim that these long-term changes in treated and untreated patients are similar in origin, however, different in their extent6.
Recently, Freitas et al7. compared the aging changes of the dental arches in patients treated with four premolar extraction and untreated subjects after a 4-decade follow-up period. The findings showed that the long-term changes of treated patients were different from untreated subjects. The patients treated with four premolar extraction showed relapse of crowding and a decrease in arch form. They concluded relapse might have contributed to greater changes in incisor crowding and arch widths observed in the patients treated with extraction7. However, there is no known study that compared patients treated nonextraction and untreated subjects after a really long period of time.
This study aimed to compare the aging changes of the dental arches in patients treated without extractions and untreated normal occlusion subjects after a four-decade follow-up.
Materials and methods
Material
This research was approved by the Human Ethics Committee of the Bauru Dental School, University of São Paulo, Bauru, Brazil (n. 16121719.7.0000.5417) and all patients signed informed consent to participate. All research was performed in accordance with the Declaration of Helsinki.
Sample size calculation was based on an alpha significance level of 5% and a beta of 20% to achieve a power of the 80% to detect a minimum difference of 1 mm, with a standard deviation of 1.05 for the mandibular irregularity index2. The sample size calculation showed the need for 18 individuals in each group.
Two samples were included in the study.
Group T (Orthodontically Treated)comprised the retrospective records of individuals treated by graduate students at Bauru Dental School, University of São Paulo, Bauru, Brazil, selected according to the following inclusion criteria: Class I or Class II malocclusion at the beginning of orthodontic treatment; dental spacing up to 3 mm; treatment protocol without extractions; complete orthodontic treatment with fixed appliances; all permanent teeth erupted up to the first molars, at the initial stage; absence of tooth agenesis and other anomalies; no tooth loss; no retention when the follow-up records were taken7. Dental casts at pretreatment (T1), posttreatment (T2) and long-term posttreatment follow-up of at least 25 years after the end of orthodontic treatment (T3) should be available when the study was conducted. The sample comprised 16 subjects (6 male; 10 female), with a mean pretreatment age of 13.20 years (SD = 0.82). The mean posttreatment age was 15.07 years (SD = 1.16) and the mean treatment time was 1.86 years (SD = 0.82). The mean age at the long-term posttreatment follow-up evaluation was 50.32 years (SD = 6.05). The mean time of long-term posttreatment follow-up was 35.25 years (SD = 6.11). Six subjects presented Class I and 10 had Class II malocclusions. At the end of the active orthodontic treatment, all patients used as retention a removable Hawley plate in the maxillary arch and a 3 × 3 fixed retainer bonded to the mandibular arch. The Hawley plate was used for a mean of 1.53 years (SD = 0.48) and the 3 × 3 fixed retainer was used for a mean period of 2.26 years (SD = 1.17).
Group UT (Untreated normal occlusion) consisted of 22 subjects (12 males, 10 females) evaluated at three time points (T1, T2 and T3), with mean age of 13.32 (SD = 1.00), 17.82 (SD = 1.35) and 60.95 years (SD = 1.47), respectively2,7. The mean period between the first and second evaluations (T2-T1) was 4.50 years (SD = 0.89) and the mean time of follow-up was 43.12 years (SD = 1.51). The initial normal occlusion sample group was obtained from 1967 to 1974 at Bauru, SP, Brazil and comprised 82 white subjects (39 men, 43 women)2,7. Dental casts were obtained at 13 years of age (T1) and 17 years of age (T2). At T1, all subjects had a clinically acceptable occlusion in the complete permanent dentition, dental and skeletal Class I relationships, no crossbite, normal overjet and overbite, and a maximum 2 mm of incisors’ crowding with no previous orthodontic treatment. From April 2015 to May 2016, the sample was recalled, and new dental casts were obtained (T3)2,7. Thirty-eight subjects were contacted and 27 were enrolled. Five of them were excluded due to the following exclusion criteria: orthodontic treatment performed before the follow-up evaluation, complete tooth loss, and no dental casts at any of the three time points2,7.
Methods
From each subject, the dental models from three stages were used: initial (T1), posttreatment (T2) and long-term follow-up (T3) for the treated patients and at similar stages for the untreated individuals7. The dental models were digitized using an R700 3-dimensional scanner (3Shape, Copenhagen, Denmark) and measured using the OrthoAnalyzer 3-dimensional software (3Shape, Copenhagen, Denmark) by a single examiner (KMSF).
For both maxillary and mandibular arches, the Little irregularity index was measured to evaluate anterior crowding8,9. The intercanine, interpremolar and intermolar widths, arch perimeter and arch length were also measured to evaluate arch form, besides overjet and overbite7.
The differences between the T1 and T2 (T2-T1) were calculated to evaluate the amount of changes in this period, indicating the treatment/observation changes in the treated and untreated groups respectively, and from T2 and T3 (T3-T2) to evaluate the long-term follow-up changes in both groups.
Error study
Within a month interval from the first measurement, the dental casts of 15 subjects (45 pairs of dental models) were randomly selected and re-measured by the same examiner (KMSF). The intraexaminer reliability was assessed using intraclass correlation coefficients10and the Bland-Altman method11.
Statistical analysis
The Shapiro-Wilk test was used to test normal distribution of the data.
Intergroup comparability of sex distribution and ages and periods of evaluation was performed by Chi-square and independent t tests, respectively.
Intergroup comparisons at T1 and the T2-T1 and T3-T2 changes were evaluated using independent t tests.
All tests were performed using the Statistica software (Statistica for Windows, version 12.0, Copyright StatSoft, Inc., Tulsa, Oklahoma, USA, 2005), at P < 0.05.
Results
The intraclass correlation coefficients (ICCs) varied from 0.89 to 0.97, indicating excellent intra-rater agreement12. The variable with the widest limit of agreement was the mandibular arch length (-1.02 and 1.11).
The groups were comparable regarding sex distribution (Table 1) and initial age (Table 1). The untreated group was older at T2 and T3 and had a greater follow-up period than the treated group (Table 1).
Since groups were not comparable regarding the long-term follow-up time (T2 to T3), the untreated group changes (T3-T2) were annualized to the respective treated group follow-up time13,14,15. This way, all individuals of the untreated group had the follow-up changes of each variable divided by their follow-up time (of each subject), and then multiplied by the mean long-term posttreatment time (T3-T2) of the treated group, that was 35.25 years (Table 1).
The initial stage (T1) comparison between the two groups demonstrated that the treated group presented greater maxillary and mandibular anterior crowding and also a greater overjet than the untreated group (Table 2). Maxillary intermolar width was greater in the untreated than in the treated group (Table 2).
The T2-T1 changes indicated that the treated group showed a greater reduction of maxillary and mandibular anterior crowding, a greater increase in maxillary interpremolar and intermolar widths and a greater decrease of the overjet than the untreated group (Table 3). The long-term follow-up changes (T3-T2) demonstrated that the treated group showed a greater increase in maxillary and mandibular anterior crowding than the untreated group (Table 3 and Fig. 1). Maxillary and mandibular arch length showed greater decrease in the treated group. The overbite increased in the treated group and decreased in the untreated group (Table 3).
Box plots with mean differences, standard deviations, maximum and minimum values showing the long-term follow up changes (T3-T2) for the maxillary and mandibular Little indexes and overbite for the treated and untreated groups.
Discussion
Sample selection and compatibility
Initial age was similar between the groups, but the treated patients were younger than untreated subjects in the second and third evaluations (Table 1), and the time of long-term follow-up of the groups presented a difference of 7.87 years (35.25 in the treated group x 43.12 in the untreated group). This could be considered a limitation in this study; however, the changes between the second and third evaluations were annualized in the untreated group to overcome this limitation and allow reliable results and conclusions13,14,15. And since no previous comparison between patients treated nonextraction and untreated subjects with a follow-up greater than 30 years is known, the study brings new information to the orthodontic literature. Besides, we speculate that changes in the occlusion from the fifth to sixth decade of life, that is the difference of the T3 age of the groups, is few and could not impair the findings of this study. One can say that the non-homogeneity of the sample malocclusion type may have a significant impact on the results if the only variables evaluated were solely the orthodontic treatment results. However, we believe that the age factor did not influenced the results of the present study, since our aim was to compare the changes that occurred over time between treated and untreated samples. Although the ages recorded at time points T2 and T3 demonstrated statistical significance, clinically, this distinction is negligible, as the physiological changes occurring within the assessed age groups are similar2,4,6,16.
Incisors irregularity
At T1, the treated group presented greater maxillary and mandibular anterior crowding than the untreated group (Table 2), as expected, since the untreated group presented normal occlusions and the untreated group was about to be treated orthodontically. The anterior crowding was corrected with treatment in the treated group and showed a slight increase in the untreated group (Table 3).
The anterior crowding changes of the orthodontic treatment (T3-T2) in the treated group was greater than the increase of this crowding due to the aging of the occlusion in the untreated normal occlusion subjects (Table 3). These results are similar to a previous study with the same untreated sample, but compared to a patients treated with four premolar extraction7. These outcomes resemble a previous study that evaluated short-term relapse and physiological changes in anterior crowding in subjects from 15 to 20 years of age17. All these findings show that the incisor crowding observed after orthodontic treatment is not only the result of physiological maturational and aging process but also the consequence of the incisor crowding changes in treated patients.
In the study comparing extraction treated patients, the mandibular anterior crowding changes was numerically greater than the maxillary7, and this was also found by other previous studies18,19,20. However, in the present study, the maxillary and mandibular crowding changes of the nonextraction treated group was similar (2.57 mm and 2.61 mm, respectively), and was numerically smaller than the changes observed in the extraction treated group in the previous study (3.11 mm for the maxillary arch crowding changes and 4.28 mm for the mandibular crowding changes)7. This is probably because the initial crowding was also smaller in our nonextraction treated group (Figs. 2 and 3) than in the extraction treated group of the other study7. This greater crowding was expected since the extraction of four premolars were planned and performed in this group mainly to correct this malocclusion feature7.
Some patients of the nonextraction treated group illustrating different degrees of maxillary incisor changes (T1, initial, T2, final, and T3, long-term posttreatment follow-up).
Some patients of the nonextraction treated group illustrating different degrees of mandibular incisor changes (T1, initial, T2, final, and T3, long-term posttreatment follow-up).
The untreated subjects of the sample presented tooth loss and were also included in the study (a table with the missing and rehabilitated teeth of the untreated sample can be found in our previous study)7. In the treated group, patients presented no tooth loss from T1 to T3. This could have influenced the results, since the tooth loss present could dissolves some of the anterior crowding throughout life, because the teeth migrate to the extracted tooth space4.
Late mandibular growth
The role of late mandibular growth cannot be overlooked when evaluating the increase in mandibular anterior crowding over time. Additionally, it can be inferred that complex growth changes likely contribute to the progression of late mandibular arch crowding21. Pubertal changes occur from ages 10 to 14 in females and 11 to 15 in males22. According to Ochoa et al23., males exhibits a longer and more pronounced growth period than the females, resulting in a straighter facial profile due to increased chin prominence, whereas the female profile remained more convex. The complexity of this phenomenon, combined with sexual dimorphism, may complicate clarifying the underlying relationship21. In addition, growth does not stop immediately after puberty. While post-adolescent changes are smaller than those during adolescence, they accumulate over time, contributing to the facial features associated with aging. From late adolescence to late adulthood, there is an average increase of 2 mm in maxillary length, 3 mm in mandibular length, and 3.5 mm in lower anterior facial height24. This age range coincides mainly with the mean age at T2 of Group 1 (Table 1). Thus, it can be hypothesized that late growth may have contributed to increased crowding in the treated group. Although the late growth of the mandible involves a forward rotation of the lower jaw, no definitive relationship with increased crowding was established6. However, this suggests that while late mandibular growth occurs, its impact on dental crowding might be mitigated or obscured by other factors such as the use of fixed retainers. Nevertheless, during this period of late growth, the patients in Group 1 were wearing fixed 3 × 3 retainers, which likely contributed to maintaining the alignment of the mandibular incisors and mitigating the effects of mandibular growth.
Arch form
Arch form was similar between the groups at T1, except for the maxillary intermolar width that was greater in the untreated subjects (Table 2). This difference was probably due to a constricted maxillary arch caused by malocclusion in the treated group.
With the nonextraction treatment, the maxillary interpremolar and intermolar widths increased in the treated group and presented a slight decrease in this period in the untreated group (Table 3). In the extraction group of our previous study, the intercanine distance showed an increase with treatment, probably due to the moderate to severe initial crowding7, which was not observed in the present study. One can speculate that maintaining intercanine and intermolar distances during orthodontic treatment would minimize the increase in posttreatment crowding. However, studies show that the changes that occur in the intercanine distance are similar in patients treated with and without extraction, and are unrelated to the stability of orthodontic treatment1,25,26. Furthermore, considerations regarding treatment stability must incorporate the aspect of muscular balance. It is essential to educate patients that dental crowding may represent a natural consequence of aging and should not necessarily be interpreted as a failure of orthodontic intervention27.
The maxillary and mandibular arch length showed a decrease in the long-term follow-up in both groups, but with a greater reduction in the treated group than in the untreated group (Table 3). The crowding in the treated group was probably corrected with buccal inclination and protrusion of the incisors, since no extraction and no interproximal stripping were performed, relapsing over the follow-up years. Some studies in treated and untreated patients demonstrated reduction in the arch length over the years due to posterior teeth mesial shift2,28,29,30,31,32.
Anterior relationships
The treated group presented greater overjet than the untreated group at the first evaluation (T1) (Table 2). This was expected since the malocclusion of the treated group was treated orthodontically. Ten patients of the treated group had Class II malocclusions with increased overjet33 while the normal occlusion group presented normal overjet, as expected. Due to the overjet correction in the treated group, this variable decreased more with treatment in this group than the change from T1 to T2 in the long-term follow-up period of the untreated group (Table 3).
Overbite was similar in both groups in the first evaluation (T1) and the changes from T1 to T2 was also similar in the treated and untreated groups, showing a slight decrease (Table 3). In the long-term follow-up, the overbite increased in the treated group and decreased in the untreated group (Table 3 and Fig. 1). This small change was also found in the extraction group of our previous study7and is not considered a relapse that could deteriorate the occlusion in the treated group33. Maturational changes with aging showed a decrease in overbite with time2,7.
Conclusions
-
Long-term posttreatment changes of the nonextraction treated group showed a greater increase of maxillary and mandibular anterior crowding compared to the untreated group.
-
Maxillary and mandibular arch length decreased more in the treated group than in the untreated group. Overbite increased in the treated group and decreased in the untreated normal occlusion subjects.
-
The maturational changes of treated patients were different from untreated normal occlusion subjects.
Data availability
Most of the generated and analyzed data is included in this published article. Detailed datasets of the current study are available from the corresponding author on reasonable request.
References
Cotrin, P. et al. Anterior tooth alignment and arch dimensions changes: 37-year follow-up in patients treated with and without premolar extraction. Am. J. Orthod. Dentofac. Orthop. 158, e5–e15. https://doi.org/10.1016/j.ajodo.2020.07.013 (2020).
Massaro, C. et al. Maturational changes of the normal occlusion: a 40-year follow-up. Am. J. Orthod. Dentofac. Orthop. 154, 188–200. https://doi.org/10.1016/j.ajodo.2017.10.028 (2018).
Thilander, B. Orthodontic relapse versus natural development. Am. J. Orthod. Dentofac. Orthop. 117, 562–563 (2000).
Miranda, F. et al. Aging of the normal occlusion. Eur. J. Orthod. 41, 196–203. https://doi.org/10.1093/ejo/cjy044 (2019).
Thilander, B. Dentoalveolar development in subjects with normal occlusion. A longitudinal study between the ages of 5 and 31 years. Eur. J. Orthod. 31, 109–120. https://doi.org/10.1093/ejo/cjn124 (2009).
Sinclair, P. M. & Little, R. M. Maturation of untreated normal occlusions. Am. J. Orthod. 83, 114–123 (1983).
Freitas, K. M. S. et al. Occlusal changes in orthodontically treated subjects 40 years after treatment and comparison with untreated control subjects. Am. J. Orthod. Dentofac. Orthop. 160, 671–685. https://doi.org/10.1016/j.ajodo.2020.05.027 (2021).
Canuto, L. F., de Freitas, M. R., Janson, G., de Freitas, K. M. & Martins, P. P. Influence of rapid palatal expansion on maxillary incisor alignment stability. Am J Orthod Dentofacial Orthop 137:164 e1-6; discussion 164-5. doi: (2010). https://doi.org/10.1016/j.ajodo.2009.06.017
Little, R. M. The irregularity index: a quantitative score of mandibular anterior alignment. Am. J. Orthod. 68, 554–563 (1975).
Shrout, P. E. & Fleiss, J. L. Intraclass correlations: uses in assessing rater reliability. Psychol. Bull. 86, 420–428 (1979).
Bland, J. M. & Altman, D. G. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1, 307–310 (1986).
Fleiss, J. L. The Design and Analysis of Clinical Experiments (Wiley, 1986).
Angelieri, F., de Almeida, R. R., Janson, G., Castanha Henriques, J. F. & Pinzan, A. Comparison of the effects produced by headgear and pendulum appliances followed by fixed orthodontic treatment. Eur. J. Orthod. 30, 572–579. https://doi.org/10.1093/ejo/cjn060 (2008).
McNamara, J. A. Jr., Howe, R. P. & Dischinger, T. G. A comparison of the Herbst and Frankel appliances in the treatment of class II malocclusion. Am. J. Orthod. Dentofac. Orthop. 98, 134–144. https://doi.org/10.1016/0889-5406(90)70007-Y (1990).
Mills, C. M. & McCulloch, K. J. Posttreatment changes after successful correction of class II malocclusions with the twin block appliance. Am. J. Orthod. Dentofac. Orthop. 118, 24–33. https://doi.org/10.1067/mod.2000.104902 (2000).
Tibana, R. H., Palagi, L. M. & Miguel, J. A. Changes in dental arch measurements of young adults with normal occlusion–a longitudinal study. Angle Orthod 74:618 – 23. d2004). https://doi.org/10.1043/0003-3219(2004)074%3C0618:CIDAMO%3E2.0.CO;2
Freitas, K. M. et al. Posttreatment and physiologic occlusal changes comparison. Angle Orthod. 83, 239–245. https://doi.org/10.2319/030512-181.1 (2013).
Kahl-Nieke, B., Fischbach, H. & Schwarze, C. W. Post-retention crowding and incisor irregularity: a long-term follow-up evaluation of stability and relapse. Br. J. Orthod. 22, 249–257 (1995).
Erdinc, A. E., Nanda, R. S. & Isiksal, E. Relapse of anterior crowding in patients treated with extraction and nonextraction of premolars. Am. J. Orthod. Dentofac. Orthop. 129, 775–784. https://doi.org/10.1016/j.ajodo.2006.02.022 (2006).
Freitas, K. M. S., Guirro, W. J. G., de Freitas, D. S., de Freitas, M. R. & Janson, G. Relapse of anterior crowding 3 and 33 years postretention. Am. J. Orthod. Dentofac. Orthop. 152, 798–810. https://doi.org/10.1016/j.ajodo.2017.05.022 (2017).
Richardson, M. E. The etiology of late lower arch crowding alternative to mesially directed forces: a review. Am. J. Orthod. Dentofac. Orthop. 105, 592–597 (1994).
Buschang, P. H., Julien, K., Sachdeva, R. & Demirjian, A. Childhood and pubertal growth changes of the human symphysis. Angle Orthod 62:203 – 10. doi: (1992). https://doi.org/10.1043/0003-3219(1992)062%3C0203:CAPGCO%3E2.0.CO;2
Ochoa, B. K. & Nanda, R. S. Comparison of maxillary and mandibular growth. Am. J. Orthod. Dentofac. Orthop. 125, 148–159. https://doi.org/10.1016/j.ajodo.2003.03.008 (2004).
Pecora, N. G., Baccetti, T., McNamara & JAJr. The aging craniofacial complex: a longitudinal cephalometric study from late adolescence to late adulthood. Am. J. Orthod. Dentofac. Orthop. 134, 496–505. https://doi.org/10.1016/j.ajodo.2006.11.022 (2008).
Bishara, S. E., Chadha, J. M. & Potter, R. B. Stability of intercanine width, overbite, and overjet correction. Am. J. Orthod. 63, 588–595. https://doi.org/10.1016/0002-9416(73)90183-8 (1973).
Burke, S. P. et al. A meta-analysis of mandibular intercanine width in treatment and postretention. Angle Orthod. 68, 53–60 (1998).
Rajbhoj, A. A., Parchake, P., Begnoni, G., Willems, G. & Cadenas de Llano-Perula, M. Dental changes in humans with untreated normal occlusion throughout lifetime: a systematic scoping review. Am. J. Orthod. Dentofac. Orthop. 160, 340–362e3. https://doi.org/10.1016/j.ajodo.2021.02.014 (2021).
Tsiopas, N., Nilner, M., Bondemark, L. & Bjerklin, K. A 40 years follow-up of dental arch dimensions and incisor irregularity in adults. Eur. J. Orthod. 35, 230–235. https://doi.org/10.1093/ejo/cjr121 (2013).
Carter, G. A. & McNamara, J. A. Jr. Longitudinal dental arch changes in adults. Am. J. Orthod. Dentofac. Orthop. 114, 88–99 (1998).
Quaglio, C. L., de Freitas, K. M., de Freitas, M. R., Janson, G. & Henriques, J. F. Stability and relapse of maxillary anterior crowding treatment in class I and class II division 1 malocclusions. Am. J. Orthod. Dentofac. Orthop. 139, 768–774 (2011). http://doi.org/10.1016/j.ajodo.2009.10.044. S0889-5406(11)00254-X [pii].
Little, R. M., Wallen, T. R. & Riedel, R. A. Stability and relapse of mandibular anterior alignment - first premolar extraction cases treated by traditional edgewise orthodontics. Am. J. Orthod. 80, 349–365 (1981).
de la Cruz, A., Sampson, P., Little, R. M., Artun, J. & Shapiro, P. A. Long-term changes in arch form after orthodontic treatment and retention. Am. J. Orthod. Dentofac. Orthop. 107, 518–530 (1995).
Francisconi, M. F. et al. Overjet, overbite, and anterior crowding relapses in extraction and nonextraction patients, and their correlations. Am. J. Orthod. Dentofac. Orthop. 146, 67–72. https://doi.org/10.1016/j.ajodo.2014.04.012 (2014).
Funding
No funding was obtained for this research.
Author information
Authors and Affiliations
Contributions
KMSF and DG made Conceptualization. KMSF, CM, FM, CMGT and PC made Methodology, Formal analysis, Investigation, Data curation. KMSF and MRF wrote the original draft. DG Project administration and supervision. All authors reviewed the manuscript and approved its final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study was approved bu the Research Ethics Committee of Bauru Dental School, University of São Paulo, Bauru, Brazil (n. 16121719.7.0000.5417).
Consent to participate
All patients signed informed consent to participate in this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Freitas, K.M.S., Massaro, C., Miranda, F. et al. Comparison of aging of nonextraction treated and normal untreated occlusions: 40-year follow up. Sci Rep 14, 25458 (2024). https://doi.org/10.1038/s41598-024-76976-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-76976-9
Keywords
This article is cited by
-
A randomized controlled trial comparing retainers in bimaxillary proclination cases
Clinical Oral Investigations (2025)