Abstract
A metamaterial integrated applicator operating at 2.45 GHz has been developed for focused heating in clinical hyperthermia applications, effectively heating tumors while minimizing surface hot spots. This innovative applicator combines a double spiral antenna (DSA) for energy delivery, a spiral frequency selective surface (SFSS) for focused energy distribution, and an artificial magnetic conductor (AMC) as a reflector to enhance penetration and uniformity. To ensure durability and environmental protection, the entire structure, including the DSA, SFSS, and AMC, is encased in a Teflon layer. The applicator’s performance is evaluated using heterogeneous phantoms, the Gustav Voxel model, and head tissue-simulating liquid, replicating real-world conditions. Its thermal efficiency is further analyzed with a water bolus that includes a 1 mm polyvinyl chloride (PVC) layer to safeguard superficial tissues and enable uniform heat distribution. The applicator achieves a therapeutic temperature of 44 °C in tumors with just 3 W of input power, demonstrating exceptional efficiency. Impedance matching and resonance at 2.45 GHz ensure effective energy delivery to target tissues. Specific absorption rate (SAR) measurements at 0.1 W input confirm consistent energy distribution across varying depths. The strong alignment between simulation and experimental results validates the applicator’s design, making it a reliable and precise tool for hyperthermia therapy.
Similar content being viewed by others
Introduction
In 21st century, cancer incidences are on the rise, not only in developed nations but also in developing regions. This surge has inflicted devastating physical, mental, and socioeconomic impacts on individuals worldwide. Despite escalating research efforts, the available treatment modalities fail to consistently deliver promising outcomes for cancer patients, often accompanied by debilitating side effects. Addressing this urgent need for effective and minimally invasive treatment options, microwave hyperthermia emerges as a beacon of hope in the realm of cancer therapy. Microwave hyperthermia holds significant promise in targeting tumors while minimizing adverse effects on the body. In this proposal, the adoption of hyperthermia as an adjuvant cancer treatment modality is advocated. Hyperthermia is a therapeutic technique employed to elevate body or localized tissue temperatures to approximately 41–45 °C for a specified duration, aimed at sensitizing cells for supplementary therapies1. Microwave hyperthermia has a number of benefits, such as quick heat transfer, volumetric, and targeted heating, precise control, and environmentally friendly heating. It is commonly utilized in conjunction with chemotherapy and radiotherapy for cancer treatment. Temperature elevation induces subtle yet extensive alterations in the physiology of the tissue, including increased metabolic activity, vascular permeability, and blood flow. The intensified blood flow at the tumor site enhances therapeutic chemical drug concentration. Furthermore, increased vascular permeability within the tumor facilitates a higher drug penetration rate into the target zone. Elevated temperature can also amplify reactive oxygen species production, such as superoxide and hydrogen peroxide, resulting in increased oxidative stress. Hyperthermia sensitizes nuclear proteins, leading to their aggregation. In the presence of oxygen, the ability of cancer cells to multiply decreases, resulting in a reduction in their proliferation capacity. This reduction enhances the effectiveness of radiation and chemotherapy treatments. However, the application of hyperthermia in clinical settings is still fraught with challenges, particularly in terms of heat delivery and treatment planning. As a result, to deliver a uniform field distribution in the near field with sufficient penetration depth (PD) and temperature based on the tumor type and location, effective hyperthermia applicators must be designed. Numerous applicators have been developed thus far for the ISM band (434, 915, and 2450 MHz)2,3,4 and investigated for hyperthermia treatment. These applicators are categorized into non-planar applicators5,6,7 and planar applicators8,9,10,11. The frequency plays an essential part in developing a hyperthermia applicator; microwave applicators work on a lower frequency that penetrates deeper radiation in the tissue (high PD) and, for a higher frequency, vice versa12,13,14. The frequency of the applicator is selected based on tumor dimensions and its type and regions. For deep cancer tissue treatment, many non-planar (horn, waveguide) applicators have been developed at 915 MHz and 434 MHz. For these applicators, the electric field reported tangential at the cancer tissue interface and enhanced the power coupling. These applicators are highly focused but have drawbacks like large sizes, high weight, and not having the flexibility to treat different types of cancer tissues (due to the fixed size of aperture) and also lead to excessive heating of normal tissues15,16,17. Therefore, the planar applicators have been investigated to overcome these shortcomings. These applicators are small in dimensions, flexible, and have less weight than the non-planar applicator and provide comfort to the patient7,12,18,19,20,21,22. However, the large aperture size at 434 MHz and 915 MHz frequencies4,10,23 provides a minimum effective field size (EFS) almost equal to the wavelength and limited PD. Going for these applicators for hyperthermia treatment also creates a hot spot for the normal tissue. To overcome this disadvantage, a cavity-backed miniaturized patch antenna has been developed at 434 MHz, giving the EFS/aperture size of the antenna greater than 1, but the effective PD of this applicator is up to 1.26 cm24.
Further, to improve the PD and align the bidirectional pattern into a directional one, a design utilizing metamaterial based structures has been developed. Many AMC structures have been designed by changing the reactance of the conducting part and placing it behind the antenna to enhance its characteristics. AMC structures are employed to suppress the backfield, increase the gain and directivity, and improve the antenna’s bandwidth25,26,27,28,29. Based on these characteristics, an AMC is successfully utilized for hyperthermia treatment. A slot microstrip patch antenna with AMC resonating at 2.45 GHz has been designed for superficial tumor treatment. The AMC is placed behind the antenna, which converges the backfield and enhances the phantom’s heating depth30. These applicators are easy to design and easy to install for clinical use. However, the PD value was less than 2.9 cm for compact structures with low input power. To further enhance the PD and focusing capability, lens applicators have been investigated31,32,33. An FSS structure is placed in front of an object or source to make a lens structure. The FSS structures have a planar metallic array of elements on a dielectric substrate that shows transmission, absorbance, and reflection at a required frequency34. This integrated structure enhances the bandwidth and PD up to a few centimeters but creates the hot spot for the uppermost layer of tissues30,33.
To protect the top layer of tissue from hot spots or burning, research must explore uniform, focused heating and compact applicators that are easy to handle and require low input power. Therefore, employ compact applicators and minimize input power requirements to increase power deposition while ensuring uniform heating. Recognizing the strengths and weaknesses of previously documented applicators used in hyperthermia treatment, this research aims to create a compact, focused metamaterial integrated applicator with improved PD and EFS utilizing AMC and FSS structure. The use of these metamaterial structures can potentially overcome the limitations associated with conventional hyperthermia treatments, such as uneven heat distribution and damage to surrounding healthy tissues or protection from hot spots. By addressing the challenges associated with the design and use of metamaterial applicators, this research aims to bring us one step closer to a more effective and safer application of hyperthermia in cancer treatment. The design, optimization, and analysis were done in a finite integration technique-based computer simulation technology microwave studio (CST MWS)35.
Metamaterial integrated applicator for effective hyperthermia
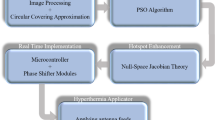
In this paper, a metamaterial integrated applicator is designed. The applicator includes optimized DSA, SFSS, and AMC structure covered by the Teflon layer (PTFE) to protect the applicator from environmental effects and converge more focused energy inside the phantom and easy to integrate with the phantom. This section presents the design and analysis of a metamaterial integrated applicator for effective hyperthermia treatment. An analysis of optimized DSA with SFSS encapsulated with a Teflon layer was done, and the same was done for DSA with SFSS and AMC structure in the presence of water bolus for hyperthermia treatment. Additionally, the impact of the metamaterial based applicator on different tissues within the Gustav voxel model is investigated. The study evaluates the specific absorption rate (SAR) both with and without tumors, as well as the effect of tumor placement at various locations within the phantom and the Gustav voxel model. The hyperthermia treatment planning system is explained with the help of a schematic diagram, as shown in Fig. 1, which illustrates how the designed applicator treats the tumor or raises the temperature of the tumor. Further, the detailed design and analysis of the metamaterial integrated applicator are discussed in the following subsection.
A schematic diagram of the hyperthermia treatment planning system.
Design and analysis of a metamaterial integrated applicator
To make a metamaterial integrated applicator, a DSA with SFSS and AMC structure encapsulated with Teflon layer (PTFE) [dielectric constant (εr) 2.1, tangent loss (tan δ) 0.0002, and thickness 5 mm] to protect the applicator from environmental effects and converge more focused energy inside the phantom as compared to the applicator without PTFE encased. The DSA structure is optimized for proper impedance, as shown in Fig. 2a. The design and analysis of the optimized DSA and SFSS structure are shown in Fig. 2a, designed to operate at 2.45 GHz and discussed in Ref36. The SFSS is placed above the DSA at an optimized distance of 1.5 mm to focus the maximum energy inside the phantom, as given in Fig. 2b. The electric field distribution of the spiral lens applicator shows that some fields are radiated in the back direction. An AMC structure is placed at an optimized distance (2.7 mm) from DSA, as demonstrated in Fig. 2b, to converge these back radiation in the forward direction. The design and analysis of the AMC structure are discussed in Ref37, the AMC structure is shown in Fig. 1. To protect the upper layer of the phantom, a 10 mm water bolus (having a relative dielectric constant (εr) of water is 78, the density of water is 998 kg/m3), is placed on the metamaterial integrated applicator, which covers with 1 mm of polyvinyl chloride (PVC) [dielectric constant (εr) 3.1, and thickness 1 mm]. This arrangement makes this applicator for practical applications and provides a uniform field distribution in the phantom. The different configurations of the applicator are shown in Fig. 3. These configurations consist of optimized DSA with SFSS, and optimized DSA with SFSS and AMC structure are encapsulated with and without Teflon layer (5 mm) with water bolus in the presence of tumor embedded in phantom, and metamaterial integrated applicator with head, arm, leg tissue of the Gustav voxel model. The tumor is placed 10 mm distance from the skin surface, as shown in Fig. 3b.
(a) Prototype of DSA, SFSS, and AMC structure, and (b) side view of metamaterial integrated applicator structure.
(a) Different Configuration with tumor embedded in phantom, (b) metamaterial integrated applicator with and without tumor embedded in phantom and Gustav voxel model, and (c) applicator without PTFE encased.
Results and discussion
The performance evaluation of the metamaterial integrated applicator is conducted based on various factors, including S-parameters, SAR within a heterogeneous phantom, and the Gustav voxel model, PD, and EFS in the phantom. The temperature distribution within the heterogeneous phantom is also analyzed to estimate the temperature enhancement required for effective hyperthermia treatment, starting from an initial temperature of 37 °C. This section presents the analysis of the results obtained from the designed applicator for hyperthermia treatment.
Analysis of metamaterial integrated applicator with Phantom and Gustav voxel model
The applicator is designed for 2.45 GHz, as depicted in Fig. 2. The S-parameter analysis was conducted for various configurations, namely with DSA (optimized DSA), DSA with SFSS, and metamaterial integrated applicator with a tumor embedded phantom (skin (1 mm), fat (5 mm), and muscle (50 mm))16 covered with PTFE layer, with Gustav voxel model for different tissues (like arm, head, leg), and as well as applicator without PTFE encased, as illustrated in Fig. 3. Initially, the DSA is placed with tumor embedded phantom covered with PTFE layer, in the presence of water bolus, as shown in Fig. 3a, the DSA covers the frequency band from 2.50 to 2.91 GHz based on a − 10 dB reflection coefficient and the bandwidth of the antenna is 410 MHz as depicted in Fig. 4. In the case of a DSA with SFSS applicator, the tumor placed in the phantom covered with a layer, in the presence of water bolus, as depicted in Fig. 3a, the applicator covers the frequency band from 2.30 to 2.90 GHz based on a − 10 dB reflection coefficient and enhances the bandwidth of the antenna (600 MHz) as depicted in Fig. 4.
Reflection coefficient versus frequency plots for different configurations.
Although there is a shifting in the frequency to the left side of the resonance frequency due to the effective permittivity of the DSA, it is increased in the presence of the SFSS structure. Also, the total electric length of the current is increased due to the loading effect of the SFSS structure. However, it still covers the required frequency band of 2.40 GHz to 2.48 GHz, as indicated in Fig. 4. Further, an AMC structure is placed with DSA and SFSS and studied the S-parameter with tumor and without tumor embedded in phantom. The designed metamaterial integrated applicator covers the desired frequency band from 2.40 to 2.48 GHz. Nevertheless, the applicator still operates within the desired ISM band for hyperthermia applications, making it suitable for tumor treatment. The metamaterial integrated applicator is also tested with various tissues of the Gustav voxel model, as shown in Fig. 3b. The applicator operates at the desired frequency of 2.45 GHz, though frequency shifts occur due to variations in tissue dielectric properties. However, it continues to effectively cover the target frequency band. The applicator, without the PTFE casing, also evaluated in the presence of a heterogeneous phantom with an embedded tumor, as shown in Fig. 3c. In comparison to the metamaterial integrated applicator, a frequency shift toward higher values was observed, as depicted in Fig. 4. However, the applicator remains within the required frequency band of 2.42 to 2.48 GHz. Based on this analysis, the applicator demonstrates effective impedance matching across different configurations, making it suitable for hyperthermia treatment of various tissue types. The hyperthermia parameters for the metamaterial integrated applicator are calculated in the following section for hyperthermia applications.
Hyperthermia characteristics parameter
The performance of the metamaterial integrated applicator is evaluated in the presence of heterogeneous phantom and the Gustav voxel model with tumor embedded in phantom for hyperthermia application as demonstrated in Fig. 3. For hyperthermia applications, the SAR distribution is taken into consideration for the study. Further, SAR in terms of PD and EFS is investigated for an applicator in close proximity to the phantom. By utilizing an input power of 1 W to DSA, the maximum SAR value of 1.97 W/kg is achieved within the heterogeneous phantom for a single antenna when a tumor is placed at 10 mm depth from the skin. The maximum SAR value for DSA with SFSS applicator is 4.29 W/kg, as depicted in Fig. 5. The SFFS structure enhances the SAR value twice as much as the single antenna or DSA. The maximum SAR value is 5.59 W/ kg for a metamaterial integrated applicator, as given in Fig. 5 along the z-axis. In the case of the applicator without a PTFE casing, the maximum SAR value is 4.6 W/kg, which is lower than that of the metamaterial integrated applicator. This suggests that the PTFE casing enhances the electric field focusing within the phantom. Additionally, SAR analysis is conducted using the Gustav voxel model for different tissues, including the head, arm, and leg, as presented in Fig. 5. The maximum SAR value obtained in these cases is 5 W/kg, which is considered a favorable outcome. From this SAR analysis, it is evident that the metamaterial integrated applicator significantly enhances SAR values compared to the DSA with SFSS and the applicator without PTFE casing. These findings indicate that the applicator is suitable for tumor treatment across different tissue types and can be effectively utilized for hyperthermia treatment in various human body parts, demonstrating its versatility. The SAR is also calculated at different depths of tumors; the values are given in Table 1. As the depth increases, the SAR value decreases gradually but provides a good SAR value at a depth of 20 mm, i.e., 4.49 W/ kg.
SAR distribution for different configurations along the depth.
The PD and EFS are also considered to evaluate the effectiveness of the applicator. The calculated PD and EFS values indicate that the metamaterial integrated applicator exhibits superior performance in terms of field focusing. Specifically, the PD for the metamaterial integrated applicator is 29 mm, whereas for the applicator without a PTFE casing, it is slightly lower. Additionally, the EFS for the metamaterial integrated applicator is 24 × 24 mm2, demonstrating enhanced field concentration, while the applicator without PTFE encasing has a broader EFS of 30 × 30 mm2. These results, as shown in Fig. 6a, b, confirm that the metamaterial-integrated applicator effectively enhances electric field focusing compared to the applicator without PTFE casing. The PD of the applicator is compared with different configurations, and the absorbance of the EM field is drawn in Fig. 6. Interestingly, a significant enhancement in PD (from 27 to 29 mm) and EFS is observed when the applicator is compared with different configurations.
(a) Normalized SAR for different configurations along the z-axis, and (b) along the x/y-axis at z = 10 mm from the skin surface.
Furthermore, the PD and EFS are calculated by embedding the tumor at different depths within the phantom, and the values are given in Table 1. Table 1 analyses that the applicator will treat the tumor at various depths. The applicator enhanced the field in the intended direction and improved the focus of microwave energy toward the tumor. The SAR is also analyzed for the placement of SFSS structures at different distances, and the effect on PD and EFS is studied. As given in Table 2, the metamaterial integrated applicator can treat tumors of different sizes/ areas by placing the SFSS at different distances. The SAR value is 5 W/kg for all the configurations of SFSS. The SAR analysis concludes that the designed metamaterial integrated applicator is compatible with deeply placed tumors for hyperthermia treatment.
Thermal distribution in Phantom
The thermal distribution of a metamaterial integrated applicator within a tumor embedded phantom is investigated for both steady state and transient state scenarios by utilizing the Multiphysics simulator, using Pennes’ bioheat equation38. Figure 7 illustrates the thermal distribution along the depth and in a transverse plane, revealing uniform heat generation within the tumor for different configurations. When 3 W of input power was applied to the applicator, the maximum temperature at the center of the tumor was 44 °C (as depicted in Fig. 8). It is worth noting that using the metamaterial integrated applicator, the tumor temperature is enhanced at the same input power as compared to the DSA, DSA with SFSS (42 °C), and applicator without PTFE encased. In the case of the Gustav voxel model, the maximum temperature (44 °C) was reached in the head tissue, as shown in Fig. 7, compared to the arm and leg tissues. Figure 8 concludes that the water bolus protects the skin layer from overheating and maintains a low temperature. The metamaterial integrated applicator heats the tumor in a focused manner and does not affect the normal tissues.
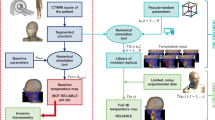
The temperature distribution analysis also considered the transient state, as depicted in Fig. 9. The results indicated that the focused applicator reached a steady state temperature after 5 min while maintaining a constant temperature within the tumor. With an input power of 3 W, the maximum temperature of 44 °C is achieved in the transient state. Consequently, based on the aforementioned analysis, it can be concluded that the designed applicator can effectively treat tumors of various shapes with different input power. Figure 10 illustrates the complete flowchart depicting the designed applicator’s impact on clinical treatment, highlighting its usability and effectiveness.
Temperature distribution inside tumor embedded phantom along depth for different configurations.
Temperature distribution for different configurations along the x/y-axis at z = 10 mm from the skin surface.
Transient temperature distribution for different configurations.
Designed applicator impact on clinical treatment with usability and effectiveness.
Methods
Metamaterial integrated applicator prototype and its experimental validation
The development of prototypes for hyperthermia treatment and validates the simulation results with measurement results for different configurations. The experimental setup for S-parameter, SAR, and temperature measurement is also discussed. The SAR is measured for different points along the depth and the transverse plane. These prototypes are tested in the presence of a head-simulating liquid, which is equivalent to a human phantom. The following section provides a detailed discussion of the fabrication process and the experimental validation of the prototypes.
Metamaterial integrated applicator prototype
A metamaterial integrated applicator is fabricated on an FR4 substrate (having a dielectric constant (εr) of 4.4, tangent loss (tan δ) of 0.018, and thickness (t) of 1.6 mm, and all the copper thickness is chosen as 35 µm), which consists of an optimized DSA, SFSS, and AMC structure encapsulated with PTFE material having a thickness of 5 mm, as discussed in the design section. The optimized metamaterial integrated applicator is shown in Fig. 11, consisting of three structures: DSA, SFSS, and AMC structure. The DSA, SFSS, and AMC structure is placed inside the cavity, as shown in Fig. 11. The cavity protects the applicator from environmental effects and is easy to use in clinical settings. The AMC and SFSS structures are placed at the top and bottom of the DSA with cavity structure. The top and side views are given in Fig. 11. The dimensions of the applicator are 100 × 100 × 35.1 mm³, and its weight is 55 g. This makes the applicator compact and lightweight, facilitating easy handling, precise positioning, and enhanced patient comfort, ensuring its practical suitability for clinical hyperthermia treatment.
Fabricated prototype of metamaterial integrated applicator.
Experimental validation of metamaterial integrated applicator
The fabricated metamaterial integrated applicator is measured with the help of VNA (E5063A), as shown in Fig. 12a. The S-parameter is measured in the presence of head-simulating liquid (HBBL600-10000V6), which has the same electrical and thermal properties as a mimicked phantom. This liquid possesses specific electrical and thermal properties: a dielectric constant (εr) of 40.9, conductivity (σ) of 1.82 S/m, a heat capacity of 3.574 kJ/(kg K), and a density (ρ) of 1.042 g/cm³. The metamaterial integrated applicator is in close agreement with the simulated one, as shown in Fig. 12b. There is a slight shift in the S-parameters of fabricated prototypes due to testing with head simulating liquid and errors in the fabrication process, but it covers the desired frequency band.
(a) Experimental setup for S-parameter measurement of a metamaterial integrated applicator with head simulating liquid, and (b) reflection coefficient versus frequency plots for different configurations.
Experimental setup for SAR measurement
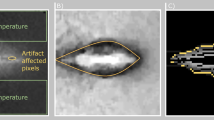
This section will detail the experimental setup for various applicator configurations using a head tissue simulating liquid (HBBL600-10000V6) to measure SAR. The measurement procedures and detailed analysis of the SAR results will be thoroughly discussed. The SAR distribution within head tissue simulating liquid (HBBL600-10000V6) is computed when 0.1 W of power is applied to the applicator. The experimental setup for measuring SAR is depicted in Fig. 13. SAR calculations are conducted at various depths within the human mimicked liquid using a SAR probe kit, determining the maximum SAR value with an input power of 0.1 W as illustrated in Fig. 14. The SAR is measured in a head tissue simulating liquid, which serves as a realistic phantom substitute. The liquid is filled up to a height of 50 mm in a box, with the applicators placed at the back of the box for experimental setup as depicted in Fig. 14. The 0.1 W of power is supplied to the applicator using an RF signal generator (9 kHz–3 GHz). The maximum input power is set to 0.1 W (20 dBm), which is the highest power level the RF signal generator can produce. The SAR is measured using the exposure acquisition system (EASY6 system), where an EX3DV4–SN7817 probe is directly connected to the data acquisition electronics (DAE). This system connects via an optical fiber cable to the remote unit (RU) and then to the computer.
Firstly, DSA is placed, and the maximum SAR value is measured by inserting the probe into the liquid. The maximum SAR value is 1.156 at 10 mm depth inside the head, simulating liquid within the liquid when 0.1 W (20 dBm) of power is applied to the DSA; the value is given in Table 3. After that, DSA with SFSS and AMC is placed, and the SAR value is measured at different depths, as presented in Table 3. Table 3 shows that the metamaterial integrated applicator gives the maximum SAR value at 20 mm. This means that the applicator focuses the EM field inside the tissue (phantom) without affecting the top layer of tissue or normal tissue.
Layout of the experimental setup for SAR measurements.
Experimental setup for measurement of SAR in head tissue simulating liquid.
The SAR is also measured for DSA and metamaterial integrated applicator at different depths with varying input power from 5 dBm to 20 dBm, and calculated values are given in Table 4, and drawn in Fig. 15, which shows that the metamaterial integrated applicator focuses the EM field inside the tissue compared to the DSA. The maximum SAR value is measured to be 2.87 W/kg at a depth of 20 mm within the liquid when 0.1 W of power is applied to the applicator. This result indicates promising SAR levels at low power, as extrapolating for 1 W would yield a maximum SAR of 19 W/kg. Further measurements are taken at a different depth, yielding a SAR value that closely aligns with the simulated SAR. Consequently, the metamaterial integrated applicator demonstrates its suitability as a promising candidate for clinical procedures, particularly for treating cancer or tumor at depth.
Measured SAR value along with depth plot at different input power for various configurations.
Experimental setup for RF power measurement
This section will discuss the experimental setup of the metamaterial integrated applicator to measure RF power for different configurations. The setup for RF power measurement is shown in Fig. 16 for DSA and metamaterial integrated applicator. The RF power is measured using a power sensor, the power is given by an RF signal generator to the DSA, and the DSA is radiated EM radiation, which is received by a microwave horn antenna connected with an RF power sensor to the RF power meter. The received RF power is measured at input power that varies from 20 to 5 dBm; values are given in Table 5. The RF power is measured at a far field when the applicator is placed 15 cm from the horn antenna, as shown in Fig. 16. The bar graph shows that the metamaterial integrated applicator increases the DSA gain by its double value as given in Fig. 17. From this analysis, we can conclude that the AMC and SFSS structure enhance the characteristics of the DSA well. Consequently, these applicators could be a good option for treating tumor cells using hyperthermia.
Experimental setup for RF power measurement for (a) DSA (antenna), and (b) for metamaterial integrated applicator.
Measured received RF power for different configurations with varying input power.
The received signal power (Pr) is calculated using the RF link budget equation (Pr = Pt + Gt + Gr − Total Losses)39, where Pt is the transmitted power, Gt is the transmitting antenna gain, Gr is the receiving antenna gain, and total losses include transmitter losses (such as cable and connector losses), free space path loss (FSPL) due to signal attenuation over distance, and receiver losses. The values for transmitted power, received power, and total losses for DSA, DSA with AMC, DSA with FSS, and the metamaterial integrated applicator are provided in Table 6.
Experimental setup for temperature measurement
This section outlines the experimental setup for a metamaterial integrated applicator designed to measure temperature in a head tissue-simulating liquid. The procedures for temperature measurement and a detailed analysis of the results are thoroughly discussed. The experimental setup consisted of a high-precision fiber optic temperature sensor system, selected for its high sensitivity, minimal interference with electromagnetic fields, and capability to provide real-time temperature readings. The sensor was placed at a depth of 20 mm within the tissue-simulating liquid to replicate the in-depth heating effect of the applicator is illustrated in Fig. 18, and temperature readings were recorded at regular intervals to analyze the heating pattern over time. The setup was maintained in a thermally controlled environment to minimize external influences on temperature rise. Multiple measurements were conducted at the same depth to confirm consistency and reduce experimental uncertainties. Temperature measurements were recorded at varying input power levels (2 W, 3 W, 4 W, and 5 W) to analyze the heating characteristics under different conditions. The temperature variations over time for each input power level are plotted to observe the heating trend, as shown in Fig. 19. The results indicate that the maximum temperature of 44 °C is reached after 50 min of heating at an input power of 3 W, whereas the same temperature is achieved in just 32 min at 5 W input power. This analysis confirms that the temperature increases with higher input power, while lower power levels require a longer duration to reach the same temperature. These experimental findings demonstrate the effectiveness of the proposed applicator in achieving controlled heating, highlighting its potential suitability for clinical applications in cancer treatment.
Experimental setup for temperature measurement in head tissue simulating liquid.
Measured temperature plot at 20 mm depth in head simulating liquid with different input power.
Key findings
New Cancer Treatment Technology—A special device using advanced materials helps heat tumors more accurately.
Deep and Precise Targeting—It can reach tumors up to 29 mm deep and focus heat on a small 24 × 24 mm2 area, reducing harm to healthy tissues.
Low Power, High Effectiveness—The device heats tumors to 44 °C using only 3 W of power, making it safer and more efficient.
Better for Patients—The technology can be adapted for different body areas, improving treatment accuracy, patient safety, and ease of use in hospitals.
Comparison of the characteristics of the metamaterial integrated applicator with previous studies in the literature
Table 7 compares the characteristics of the proposed metamaterial integrated applicator, including size, frequency, SAR, PD, EFS, and temperature, with existing applicators. The proposed applicator demonstrates improved PD, EFS, and a 44 °C temperature while operating at a very low input power of 3 W. Additionally, it provides focused heating for tumors, making it highly effective for hyperthermia treatment.
Conclusion
The metamaterial integrated applicator, incorporating an optimized DSA, SFSS, and an AMC structure, is encased in a Teflon layer for enhanced practicality. SAR measurements in a head tissue-simulating liquid revealed that the SAR value is doubled when using the metamaterial integrated applicator compared to a standalone DSA. Notably, the metamaterial applicator achieves maximum SAR at a depth of 20 mm, whereas the DSA produces maximum SAR at the surface of the phantom. This applicator effectively heats tumors to 44 °C with a low input power of 3 W, preventing surface hot spots or burns on the phantom. To enable efficient hyperthermia treatment, the adjustable placement of the SFSS allows for precise targeting of tumors of various sizes. This applicator, resonating at 2.45 GHz, is a promising candidate for hyperthermia applications, offering the versatility to treat tumors at different depths and sizes. For real-world conditions, in the future, our approach involves designing a single integrated device that incorporates robotic arms to position the applicator, along with an RF generator and a temperature and SAR measurement system. This integrated setup will enhance ease of use and improve practicality for clinical applications, ensuring precise and efficient hyperthermia treatment.
Data availability
The data supporting the findings of this study are available from the corresponding author upon request.
References
Habash, R. W. Y., Bansal, R., Krewski, D. & Alhafid, H. T. Thermal therapy, part 2: hyperthermia techniques. Crit. Rev. Biomed. Eng. 34 (6), 491–542. https://doi.org/10.1615/CritRevBiomedEng.v34.i6.30 (2006).
Korkmaz, E., Isik, O. & Nassor, M. A. A compact microstrip spiral antenna embedded in water bolus for hyperthermia applications, Int. J. Antennas Propag. 2013. https://doi.org/10.1155/2013/954986 (2013).
Correia, D. et al. Body conformal antennas for superficial hyperthermia: the impact of bending contact flexible microstrip applicators on their electromagnetic behavior. IEEE Trans. Biomed. Eng. 56 (12), 2917–2926. https://doi.org/10.1109/TBME.2009.2029081 (2009).
Petra Kok, H. et al. SAR deposition by curved CFMA-434 applicators for superficial hyperthermia: measurements and simulations. Int. J. Hyperth. 26 (2), 171–184. https://doi.org/10.3109/02656730903397321 (2010).
Guy, A. W. Electromagnetic fields and relative heating patterns due to a rectangular aperture source in direct contact with bilayered biological tissue. IEEE Trans. Microw. Theory Tech. 16 (2), 214–223. https://doi.org/10.1109/TMTT.1968.1127485 (1968).
Lehmann, J. F., Guy, A. W., Stonebridge, J. B. & Lateur, B. J. Evaluation of a therapeutic direct-contact 915-MHz microwave applicator for effective deep-tissue heating in humans. IEEE Trans. Microw. Theory Tech. 26 (8), 556–563. https://doi.org/10.1109/TMTT.1978.1129438 (1978).
Uzunoglu, N. K., Angelikas, E. A. & Cosmidis, P. A. A 432-MHz local hyperthermia system using an indirectly cooled, water-loaded waveguide applicator. IEEE Trans. Microw. Theory Tech. 35 (2), 106–111. https://doi.org/10.1109/TMTT.1987.1133611 (1987).
Tanabe, E. et al. Microstrip spiral antenna for local hyperthermia. In MTT-S International Microwave Symposium Digest, MTT005 133–134. https://doi.org/10.1109/MWSYM.1984.1131715 (1984).
Koo, Y. S., Kazemi, R., Liu, Q., Phillips, J. C. & Fathy, A. E. Development of a high SAR conformal antenna for hyperthermia tumors treatment. IEEE Trans. Antennas Propag. 62 (11), 5830–5840. https://doi.org/10.1109/TAP.2014.2357419 (2014).
Curto, S., McEvoy, P., Bao, X. & Ammann, M. J. Compact patch antenna for electromagnetic interaction with human tissue at 434 MHz. IEEE Trans. Antennas Propag. 57 (9), 2564–2571. https://doi.org/10.1109/TAP.2009.2027040 (2009).
Curto, S., See, T. S. P., McEvoy, P., Ammann, M. J. & Chen, Z. N. In-silico hyperthermia performance of a near-field patch antenna at various positions on a human body model. IET Microwaves Antennas Propag. 5 (12), 1408–1415. https://doi.org/10.1049/iet-map.2010.0611 (2011).
Rajendran, T. & Arunachalam, K. Microwave intracavitary applicator using 434 mhz conformal patch antennas for hyperthermia treatment of gynaecological cancers. IET Microwaves Antennas Propag. 15 (9), 1117–1126. https://doi.org/10.1049/mia2.12122 (2021).
Du, Y. X., Xi, X. L. & Qin, L. The design of four-arm spiral antenna for microwave hyperthermia. In 2010 4th Int. Conf. Bioinform. Biomed. Eng. iCBBE 2010 10–12. https://doi.org/10.1109/ICBBE.2010.5515123 (2010).
Lyu, C., Li, W., Li, S., Mao, Y. & Yang, B. Design of ultra-wideband phased array applicator for breast cancer hyperthermia therapy. Sensors 23 (3), 1051. https://doi.org/10.3390/s23031051 (2023).
Gupta, R. C. & Singh, S. P. Analysis of the SAR distributions in three-layered bio-media in direct contact with a water-loaded modified box-horn applicator. IEEE Trans. Microw. Theory Tech. 53 (9), 2665–2671. https://doi.org/10.1109/TMTT.2005.854209 (2005).
Singh, S. & Singh, S. P. Water-loaded metal diagonal Horn applicator for hyperthermia. IET Microwaves Antennas Propag. 9, 814–821. https://doi.org/10.1049/iet-map.2014.0699 (2015).
Thumm, M. K. & Kasparek, W. file:///C:/Users/sharm/Downloads/s11042-021-11827-7.pdf. IEEE Trans. Plasma Sci. 30 (3), 755–786. https://doi.org/10.1109/TPS.2002.801653 (2002).
Singh, S., Singh, D. & Singh, S. P. Compact conformal slot antenna for hyperthermia applications. In 2019 Int. Conf. Signal Process. Commun. ICSC 2019, vol. 1, 130–132. https://doi.org/10.1109/ICSC45622.2019.8938390 (2019).
Mahmoud, K. R. & Montaser, A. M. Design of multiresonance flexible antenna array applicator for breast cancer hyperthermia treatment. IEEE Access. 10, 93338–93352. https://doi.org/10.1109/ACCESS.2022.3203431 (2022).
Elsaadi, M., Aid, Y., Abbas, M., Embarek, A. & Salih, K. Hyperthermia for breast cancer treatment using slotted circular patch antenna. Circuits Syst. 10 (03), 37–44. https://doi.org/10.4236/cs.2019.103003 (2019).
Kotchapradit, S., Thongsopa, C. & Thosdeekoraphat, T. Analysis and design of microwave dielectric heating with curved plate applicator for deep hyperthermia in breast cancer treatment. Radioengineering 28, 703–713. https://doi.org/10.13164/re.2019.0703 (2019).
Mukai, Y. & Suh, M. Development of a conformal woven fabric antenna for wearable breast hyperthermia. Fash Text. 8 (1), 1–12. https://doi.org/10.1186/s40691-020-00231-8 (2021).
Gelvich, E. A. & Mazokhin, V. N. Contact flexible microstrip applicators (CFMA) in a range from microwaves up to short waves. IEEE Trans. Biomed. Eng. 49 (9), 1015–1023. https://doi.org/10.1109/TBME.2002.802053 (2002).
Rattina, M. & Ramu, S. Miniaturized 434 mhz cavity encapsulated patch antenna for superficial hyperthermia treatment. IEEE J. Electromagn. RF Microwaves Med. Biol. 1, 1–8. https://doi.org/10.1109/JERM.2023.3307220 (2023).
Liu, H., Wang, J. & Luo, X. Flexible and compact AMC based antenna for WBAN applications. In 2017 IEEE Antennas Propag. Soc. Int. Symp. Proc., vol. 2017, 587–588. https://doi.org/10.1109/APUSNCURSINRSM.2017.8072336 (2017).
Sanusi, O. M. et al. Development of a 2.45 ghz antenna for flexible compact radiation dosimeter tags. IEEE Trans. Antennas Propag. 67 (8), 5063–5072. https://doi.org/10.1109/TAP.2019.2911647 (2019).
Joshi, A. & Singhal, R. Gain enhancement in probe-fed hexagonal ultra wideband antenna using AMC reflector. J. Electromagn. Waves Appl. 33 (9), 1185–1196. https://doi.org/10.1080/09205071.2019.1605939 (2019).
Foroozesh, A. & Shafai, L. Investigation into the application of artificial magnetic conductors to bandwidth broadening, gain enhancement and beam shaping of low profile and conventional monopole antennas. IEEE Trans. Antennas Propag. 59 (1), 4–20. https://doi.org/10.1109/TAP.2010.2090458 (2011).
Agarwal, K., Nasimuddin & Alphones, A. Unidirectional wideband circularly polarised aperture antennas backed with artificial magnetic conductor reflectors. IET Microwaves Antennas Propag. 7 (5), 338–346. https://doi.org/10.1049/iet-map.2012.0580 (2013).
Singh, S., Sahu, B. & Singh, S. P. Conformal microstrip slot antenna with an AMC reflector for hyperthermia. J. Electromagn. Waves Appl. 30 (12), 1603–1619. https://doi.org/10.1080/09205071.2016.1207568 (2016).
Jaffar, N. A., Buniyamin, N. & Lias, K. An overview of available metamaterial-based antenna for non-invasive hyperthermia cancer treatment. Indones J. Electr. Eng. Comput. Sci. 14 (2), 697–705. https://doi.org/10.11591/ijeecs.v14.i2.pp697-705 (2019).
Gong, Y. & Wang, G. Superficial tumor hyperthermia with flat left-handed metamaterial lens. Prog Electromagn. Res. 98, 389–405. https://doi.org/10.2528/PIER09091401 (2009).
Tao, Y. & Wang, G. Influence of source offset on breast tumor hyperthermia with Γ-shaped LHM lens applicator. In 2010 Int. Conf. Microw. Millim. Wave Technol. ICMMT 2010 1859–1861. https://doi.org/10.1109/ICMMT.2010.5524876 (2010).
Liu, H., Lei, S., Shi, X. & Li, L. Study of antenna superstrates using metamaterials for directivity enhancement based on Fabry–Perot resonant cavity. Int. J. Antennas Propag. 741, 2013. https://doi.org/10.1155/2013/209741 (2013).
Sharma, N., Singh, H. S., Khanna, R., Kaur, A. & Agarwal, M. Development of metasurface based hyperthermia lens applicator for heating of cancerous tissues. Biomed. Eng. Lett. https://doi.org/10.1007/s13534-023-00300-z (2023).
Sharma, N., Kaur, A. & Khanna, R. Design and development of a double spiral antenna with an artificial magnetic conductor structure for hyperthermia treatment. Int. J. RF Microwave Comput. Aided Eng. 1, 1–17. https://doi.org/10.1002/mmce.23470 (2022).
Pennes, H. H. Analysis of tissue and arterial blood temperatures in the resting human forearm. J. Appl. Physiol. 85 (1), 5–34. https://doi.org/10.1152/jappl.1998.85.1.5 (1998).
Griffin, J. D., Durgin, G. D., Haldi, A. & Kippelen, B. RF Tag antenna performance on various materials using radio link budgets. IEEE Antennas Wirel. Propag. Lett. 5 (1), 247–250. https://doi.org/10.1109/LAWP.2006.874072 (2006).
Pyrexar Medical International Product Site. https://www.pyrexar.com/ (Accessed 05 March 2025).
ALBA ON 4000D|Precision Hyperthermia. https://www.albahyperthermia.com/project/alba-on-4000d-precision-hyperthermia/ (Accessed 05 March 2025).
Gelvich, E. A. & Mazokhin, V. N. Contact flexible microstrip applicators (CFMA) in a range from microwaves up to short waves. 49, 1015–1023 (2002).
Rajebi, S., Ghobadi, C., Nourinia, J. & Mostafapour, E. SAR enhancement of slot microstrip antenna by using silicon layer in hyperthermia applications. Wirel. Pers. Commun. 111, 1761–1774. https://doi.org/10.1007/s11277-019-06955-1 (2020).
Sharma, N., Singh, H. S., Khanna, R., Kaur, A. & Agarwal, M. Development of a metamaterial-based compact applicator for hyperthermia. Microw. Opt. Technol. Lett. 65 (2), 525–533. https://doi.org/10.1002/mop.33531 (2023).
Gang Wang, H. W. & Gong, Y. Schemes of microwave hyperthermia by using flat left-handed material lenses. Microw. Opt. 48 (12), 2611–2615. https://doi.org/10.1002/mop (2006).
Choi, W. C., Lim, S. & Yoon, Y. J. Evaluation of transmit-array lens antenna for deep-seated hyperthermia tumor treatment. IEEE Antennas Wirel. Propag. Lett. 19 (5), 866–870. https://doi.org/10.1109/LAWP.2020.2982676 (2020).
Abd Rahman, A., Kamardin, K., Yamada, Y. & Takahashi, M. Design method of a focusing dielectric lens antenna and temperature increment measurement at the focusing spot. Heliyon 10, e28061 (2024). https://doi.org/10.1016/j.heliyon.2024.e28061.
Choudhary, R. & Arunachalam, K. Dielectric loaded antenna with conformal waterbolus and improved SAR for hyperthermia treatment of localized superficial cancer. IEEE Access. https://doi.org/10.1109/ACCESS.2025.3558614 (2025).
Firuzalizadeh, M. et al. Joint optimization of antenna system matching and specific absorption rate focusing in microwave hyperthermia cancer treatment. Cancers 17, 1–16. https://doi.org/10.3390/cancers17030386 (2025).
Acknowledgements
The authors would like to take this opportunity to thank the Ministry of Electronics and Information Technology (MeiTY) [File No. 1(2)/2022/-ME&HI] for providing financial support to carry out this research. Also, authors would like to thank the TIET-VT Center of Excellence in Emerging Materials (CEEMS), TIET for facilitating the laboratory to carry out the research.
Author information
Authors and Affiliations
Contributions
Nitika Sharma: Conceptualization, Formal analysis, Investigation, Writing—original draft, review & editing. Rajesh Khanna: Funding acquisition, Project administration, Supervision, Writing—review & editing.Hari Shankar Singh: Funding acquisition, Project administration, Supervision, Writing—review & editing. Mayank Kumar Rai: Supervision, Writing—review & editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Sharma, N., Khanna, R., Singh, H.S. et al. Experimental analysis of metamaterial integrated applicator for hyperthermia cancer treatment. Sci Rep 15, 18771 (2025). https://doi.org/10.1038/s41598-025-01599-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-01599-7