Abstract
To evaluate the improvement effect of graded exercise rehabilitation on diaphragm function, exercise function, and respiratory performance in AECOPD patients. 68 AECOPD patients admitted to the Respiratory and Critical Care Department of a tertiary hospital in Zunyi City. Patients were randomly divided into a study group and a control group (each group 34 patients), and then according to the grading criteria, patients in each group were divided into 3 levels, for a total of 6 groups. The control group used conventional rehabilitation, while the study group used graded exercise rehabilitation. Bedside ultrasound was used to monitor the changes in diaphragm function (DE, DTei, DTee, DTF), 6MWT, CAT score, mMRC questionnaire, non-invasive mechanical ventilation time, and hospital stay between two groups of patients before and after rehabilitation. Compared with before the rehabilitation intervention, the study group showed significant improvement in diaphragm movement compared to the control group (P < 0.05). The end-inspiratory, end-expiratory, and diaphragm thickening scores all improved compared to before, and the differences were statistically significant (P < 0.05); The 6MWT and CAT scores of the study group were significantly higher than those of the control group after the intervention, and the difference was statistically significant (P < 0.05); Compared with the control group, the study group had significantly less mechanical ventilation time and hospitalization time, and the difference was statistically significant (both P < 0.05); The total incidence of MV related complications in the study group was lower than that in the control group, and the difference was statistically significant (P < 0.05). There were no actual compression injuries, aspiration, deep vein thrombosis, atelectasis, etc. in either group; The mMRC questionnaire did not show statistical significance (P > 0.05), but there was improvement before the intervention. Graded exercise rehabilitation can effectively improve the overall diaphragm function of patients, and has a positive effect on enhancing exercise quality and endurance; Bedside ultrasound can dynamically and real-time observe the diaphragm movement status of AECOPD patients, objectively and directly evaluate the recovery of respiratory muscle function, and has important clinical value.
Similar content being viewed by others
Introduction
Chronic obstructive pulmonary disease (COPD) is a heterogeneous lesion of the respiratory system that leads to progressive exacerbation of airflow limitation and irreversible lung injury in patients1, and there are currently about 299 million patients with chronic obstructive pulmonary disease (COPD) in the world2, which is the third most common cause of death in the world1, and in recent years, the prevalence rate has increased year by year along with the development of the society and changes in the bad living conditions. Moreover, COPD patients often experience acute exacerbation (AECOPD) under the effect of infection, stress and other factors, which can lead to changes in the geometry of the chest wall and diaphragm, and with the aggravation of obstructive ventilatory dysfunction, it causes a decrease in diaphragm compliance and insufficient contraction, and ultimately triggers diaphragm dysfunction (DD)3, which mainly Diaphragm atrophy, loss of diaphragm strength and fatigue more easily under specific loads lead to inspiratory muscle weakness, which is associated with dyspnea, increased risk of hospitalization due to acute exacerbation and premature death4, and also affects the function of peripheral skeletal muscles, leading to a reduction in their peripheral muscle content, decreased muscular endurance, and reduced mobility, which is closely related to poor prognosis of the patients5. Therefore, early identification, diagnosis of DD, and early rehabilitation nursing interventions are of great significance in reducing the incidence of related complications and patient mortality, and in promoting patients’ pulmonary rehabilitation.
Exercise, as the core of pulmonary rehabilitation (PR), has been shown6 to improve dyspnea symptoms, exercise capacity and quality of life in stable COPD patients, and reasonable, effective, and appropriate exercise workouts are very critical to enhance diaphragm exercise efficacy, which is fundamental to improving their exercise tolerance7,8,9. However, there still seems to be no more ideal early rehabilitation training model for AECOPD patients, and the research information on long-term benefits still needs to be supplemented. Moreover, traditional rehabilitation mostly adopts fixed programs, such as conventional respiratory training and basic limb activities, which lack a hierarchical assessment of the individual’s condition and make it difficult to target improvement of diaphragm function and exercise endurance. In contrast, graded exercise rehabilitation is based on objective data such as respiratory rate and blood gas indexes to stratify the condition, and a stepwise program of passive exercise, active training, and resistance training is designed for patients with different degrees of condition, which can achieve personalized, precise, and dynamic nursing interventions. Based on this, this study implemented graded exercise rehabilitation training for AECOPD patients and used bedside ultrasound to dynamically monitor changes in diaphragm function indexes, and detected the effects of graded exercise rehabilitation on 6MWT, CAT score, and mMRC questionnaire, which provides a new idea for the subsequent clinical rehabilitation treatment of chronic obstructive pulmonary disease and bedside ultrasound diaphragm testing.
Materials and methods
Study design
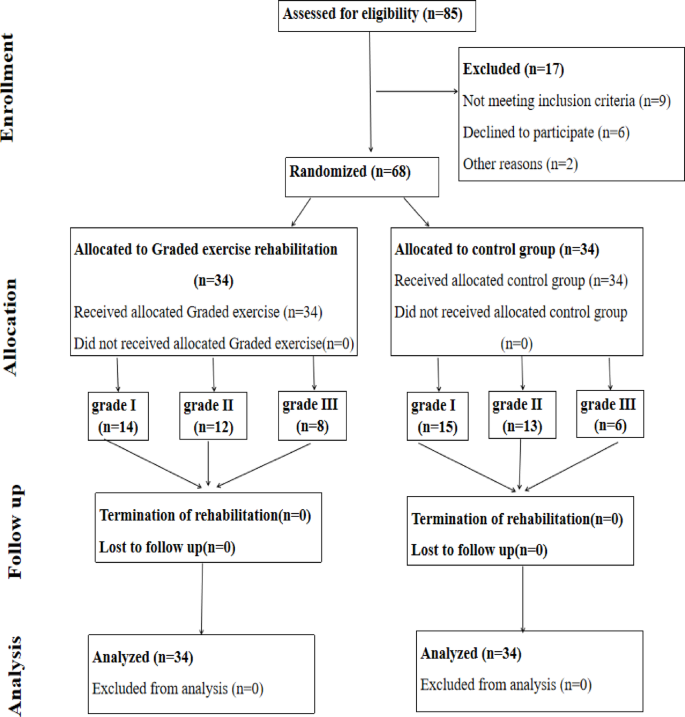
This is a single-center, randomized, prospective randomized controlled trial (RCT) study. This study has been approved by hospital ethics [The Second Affiliated Hospital of Zunyi Medical University, ID:YXLL (KY)-2022-017], conducted by the principles of the Helsinki World Medical Association Declaration, and registered with the Chinese Clinical Trial Registry (registration number: ChiCTR2300072409, date of first registration: 13/06/2023). After a basic assessment, all eligible participants were randomly assigned, drawn from envelopes by an assistant, to a study group, or a control group, with the assignment confidential to the study staff. Data were collected on the first day of the intervention and the day of discharge, see Fig. 1.
Consort diagram of the study.
Participants
68 AECOPD patients admitted to the Respiratory and Critical Care Department of a tertiary hospital in Zunyi City were included as the study subjects, they were assigned into 2 groups: the study group (n = 34) and the control group (n = 34). All participants provided written informed consent forms. The sample size estimation was based on the results of a previous study, and calculations were conducted using G*Power software. With an overall sample size of 54 participants, the total expected sample size was set at 68 participants to allow for a potential dropout rate of 20%.
The participants underwent screening based on the following inclusion criteria:(1) According to the diagnostic criteria for COPD in the Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2024 edition, and if the condition is in an acute exacerbation phase; (2) Meet the requirements of 2022 EXODUSEXpert consensus On Diaphragm Ultra Sonography in the critically ill, Expert consensus on severe diaphragmatic ultrasound detection: any one of the following: diaphragmatic mobility < 2 cm, diaphragmatic thickness < 2.2 mm, and diaphragmatic thickening fraction < 20%;(3) Age between 40 and 80 years old; (4) Clear consciousness, unobstructed language communication, and willingness to cooperate with the researchers in this study. The exclusion criteria were as follows: (1)There are contraindications for exercise: uncontrolled hypertension (> 180/110 mmHg) and hypotension (< 90/60 mmHg); Serious cardiovascular disease; Combined with acute attacks of bronchial asthma, pulmonary embolism, pneumothorax, etc.; There are diseases that affect motor nerves, muscles, bones, and joints; (2) Chest deformity, known diaphragmatic paralysis or chronic neuromuscular disease;
Randomization and blinding
The random allocation sequence was generated by computer in a 1:1 ratio, and an independent investigator graded patients who met the inclusion and exclusion criteria according to the severity of their disease and implemented allocation concealment through sealed opaque envelopes. A single-blind design was used, with random allocation sequence generation and intervention grouping performed by a researcher who was not involved in patient recruitment, and the sonographer and data analysts were unaware of the grouping information.
Intervention
Rehabilitation intervention starts on the second day of patient admission and ends on the day of discharge, with no time interval during the process, twice a day.
Establishing a study group
The research team consists of one nursing manager, one director of the respiratory department, one attending physician of the respiratory department, one B-ultrasound doctor, one rehabilitation doctor, one head nurse, and two respiratory nurses, as well as two nursing master’s students. The nursing manager serves as the team leader and is responsible for coordinating and allocating research work; The director of the respiratory department serves as the deputy team leader, responsible for AECOPD theoretical knowledge training and guidance; Respiratory doctors are responsible for diagnosing grading standards for AECOPD patients and ensuring patient safety during interventions; The B-ultrasound doctor is responsible for bedside diaphragm B-ultrasound testing; Rehabilitation doctors are responsible for providing guidance and training on graded exercise rehabilitation knowledge; The head nurse is responsible for team management, guidance on plans, and quality control work; The responsible nurse is responsible for implementing a graded exercise rehabilitation program under the guidance of a rehabilitation doctor. Nursing master’s students are responsible for collecting baseline data and evaluation indicators.
Method of classification
Due to the rapid and severe progression of AECOPD patients, most of them were unable to complete lung function tests. Therefore, in this study, 68 AECOPD patients who met the inclusion and exclusion criteria were divided into grades I, II, and III according to the grading criteria (see Table 1). Patients in the above three grades were randomly divided into a study group and a control group using a random method.
Intervention methods for the control group
Routine exercise rehabilitation based on symptomatic treatment: ① Turning over: Assist in turning over and changing to a comfortable position, every 2 h; ② Effective cough guidance: Guide the patient to take 5–6 deep breaths first, then keep their mouth open at the end of inhalation, cough continuously several times to bring phlegm to the throat, and then cough vigorously to expel the phlegm; ③ Clamping vibration: The palm is in an empty cup-shaped shape, tapping the lungs from bottom to top and from outside to inside. Each lung lobe is tapped for 1–3 min, lasting for 5–15 min, twice a day; ④ Mechanical sputum removal: Use a vibrating sputum removal device with a frequency of not less than 200 times/min, and the tremor sequence and duration are the same as those of manual lung tightening, 15–20 min, twice a day; ⑤ Pursed lip breathing: The inhalation time and exhalation time should be maintained at a ratio of 1:2 or more, with an expected breathing frequency of 8–10 breaths per minute. Each training session should last for about 5 min, twice a day; ⑥ Abdominal breathing: respiratory rate of 8–10 times/min, each training lasting about 5 min, 2 times/day; ⑦ Upper limb exercise: Dumbbell exercises, place 0.5 kg dumbbells on each hand at shoulder height, use the other hand to straighten and lift and lower the dumbbells, inhale when lifting, exhale when lowering, and repeat this exercise with the other hand. 3 sets/time, 8 pieces/time, 2 times/day; ⑧ Lower limb exercise: Sit in a chair, straighten your knees, keep your legs straight for 5 s, and then relax. Repeat this process, 3 groups/time, 8 groups/time, 2 times/day.
Intervention methods of the study group
Rehabilitation intervention starts on the second day of patient admission and ends on the day of discharge, with no time interval during the process, twice a day. Graded exercise rehabilitation based on symptomatic treatment. This exercise plan has been supported by evidence-based research and two rounds of expert consultation, ensuring its scientific and safe nature. The plan includes pre-exercise safety assessment, exercise intensity, exercise frequency and time, exercise adjustment principles, and suspension standards during exercise. The specific plan is shown in Table 2.
Observation and evaluation indicators
Evaluation time
Both groups of patients were tested and scored within 24 h after enrollment and on the day of discharge.
Evaluation indicators
-
1.
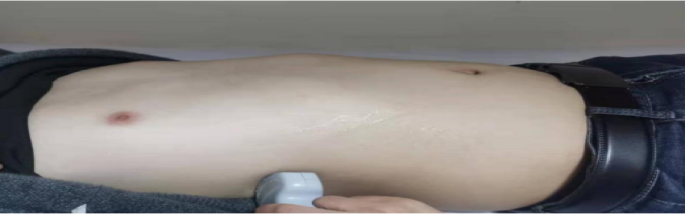
Diaphragm detection: in this study, a portable color Doppler ultrasound system (Mindray UMT-200, Shenzhen Mindray Bio-Medical Electronics Co., Ltd.,Shenzhen, China) was used to detect the right diaphragm area of patients. The low-frequency convex array probe was mainly used to observe diaphragm movement, and the high-frequency linear array probe was used to observe diaphragm thickness. All test values were obtained by the same ultrasound physician using the same measurement method. The detection method is detailed in Fig. 2.
Bedside ultrasonic testing area (right side).
① Diaphragmatic mobility
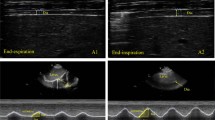
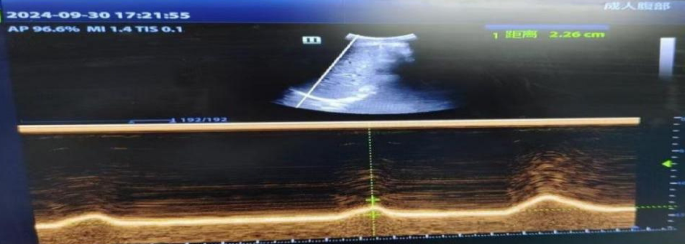
Refers to the difference in displacement distance of the diaphragm at the end of exhalation and inhalation. The patient is in a supine position, with the convex array probe placed at the junction of the midline of the clavicle and the lower edge of the rib arch. The liver is used as the sound window, and the probe is perpendicular to the diaphragm dome. The ultrasound beam is directed toward the head and left and right scans are performed to locate the position of the diaphragm. On the B-mode ultrasound image, select the location with the highest motion amplitude, make the sampling line perpendicular to the diaphragm, convert it to M-ultrasound, and display the trajectory of the diaphragm along the sampling line with respiratory movement. Adjust the scanning speed according to the subject’s respiratory rate, record the difference in distance between the end-expiratory and end-inspiratory phases and the sampling line, measure three times, and take the average. See Fig. 3.
Schematic diagram of diaphragm movement measurement (right side).
② Diaphragm thickness and diaphragm thickening fraction
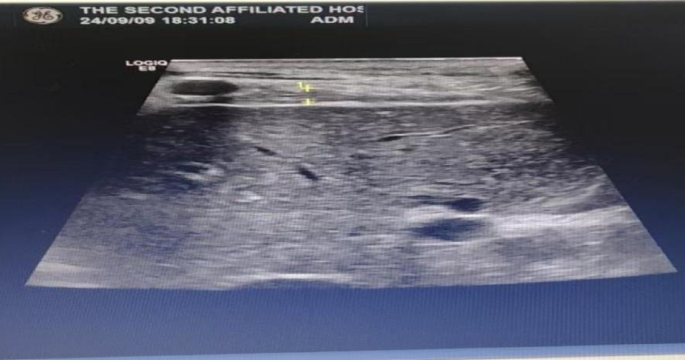
The patient is in a supine position, and a linear array probe with a frequency of 7–13 Hz is placed between the 7th or 8th rib of the right anterior axillary line, which is the area where the diaphragm meets the chest wall. The movement of the diaphragm is scanned, and the distance between the parallel high echo inner sides of the diaphragm on both sides is measured, which is the diaphragm thickness. Measure the end-inspiratory diaphragm thickness (DTei) and end-expiratory diaphragm thickness (DTee) under calm breathing for three respiratory cycles, and calculate the average value. Obtain the diaphragm thickening fraction DTF = (DTei DTee)/DTee × 100% through the formula. See Fig. 4.
Schematic diagram of diaphragm thickness measurement (right side).
-
2.
Sports endurance: using a 6-min walk test (6 MWT) as the testing standard.
-
3.
Quality of life: assessed using the Chronic Obstructive Pulmonary Disease Assessment Test Score Scale (CAT).
-
4.
Respiratory condition: evaluated using the Modified Dyspnea Rating Scale (mMRC).
-
5.
Noninvasive mechanical ventilation duration and length of hospital stay.
-
6.
The overall incidence of complications related to non-invasive mechanical ventilation.
Statistical analysis
Statistical analysis was conducted using SPSS version 29.0 statistical software, and the measurement data followed a normal distribution expressed as mean ± standard deviation. A Paired t-test was used for intra-group comparison before and after, and two independent sample t-tests were used for inter-group comparison.
Results
Comparison of general information between two groups of patients
This study included a total of 68 patients, including 34 in the study group and 34 in the control group. There were no statistically significant differences in general information such as age, gender, body mass index, disease duration, educational level, employment status, occupation, and AECOPD grading between the two groups of patients (all P > 0.05), indicating comparability. See Table 3.
Comparison of changes in diaphragm indicators between two groups of patients
Compared with before training, the study group showed improvement in diaphragm movement compared to the control group, and the difference was statistically significant (P < 0.05); The end-inspiratory, end-expiratory, and diaphragmatic thickening scores have all improved compared to before, and the differences are statistically significant (P < 0.05). See Table 4.
Comparison of 6MWT levels between two groups of patients
There was no statistically significant difference in 6MWT between the two groups of patients before intervention (P > 0.05); After intervention, the 6MWT of the study group was significantly higher than that of the control group, and the difference was statistically significant (P < 0.05). See Table 5.
Comparison of quality of life and respiratory status between two groups of patients before and after treatment
There was a statistically significant difference in CAT scores between the two groups of patients before intervention (P < 0.05); After intervention, the study group showed significant improvement in scores compared to the control group. There was no statistically significant difference in the mMRC questionnaire before and after intervention (all P > 0.05); The scores of the two groups of patients showed significant improvement after intervention compared to before intervention. See Table 6.
Comparison of non-invasive mechanical ventilation time and length of hospital stay between two groups of patients
The non-invasive mechanical ventilation time and hospitalization time of the study group were significantly shorter than those of the control group, and the difference was statistically significant (both P < 0.05). The results are shown in Table 7.
Comparison of total incidence of non-invasive mechanical ventilation-related complications between two groups of patients
The diagnosis of non-invasive mechanical ventilation-related complications in two groups of patients was made by doctors based on patient imaging examinations and clinical manifestations. The total incidence of MV-related complications in the study group was lower than that in the control group, and the difference was statistically significant (P < 0.05). There were no facial compression injuries, aspiration, deep vein thrombosis, atelectasis, etc. in both groups. The results are shown in Table 8.
Discussions
COPD is a common chronic disease of the respiratory system characterized by prolonged and persistent airflow limitation and respiratory symptoms that develop irreversibly. In terms of pathomechanism, patients suffer from emphysema caused by airway narrowing, increased resistance, small airway closure, and pulmonary hyperventilation, which leads to a change in the type of diaphragm fibers, fibrous atrophy, muscle damage, and shortening of the length of the diaphragm. With the aggravation of obstructive ventilation dysfunction, changes in diaphragm structure and contractile function become obvious, resulting in decreased compliance, insufficient contractile force and even dysfunction10, which is the main cause of dyspnea, decreased activity endurance and even death from respiratory failure in patients with AECOPD, and seriously affects the quality of patient’s survival11. At present, the role of pulmonary rehabilitation therapy is now more and more attention, in 1974 by the American College of Chest Physicians (ACCP) Pulmonary Rehabilitation Committee was first proposed, in 1997 the ACCP and the American Association of Cardiovascular Pulmonary Rehabilitation published a guideline for pulmonary rehabilitation, and the 2015 version of the guideline for pulmonary rehabilitation is defined as follows: in a comprehensive assessment of the patient’s basis for the development of comprehensive interventions, which mainly includes exercise training, Patient education and behavioral change, but not limited to, aim to change the physiological and psychological status of patients with chronic respiratory diseases and improve patients’ adherence to long-term healthy behaviors12,13.
In terms of the correlation between intervention design and efficacy, graded exercise rehabilitation is based on the stratification of AECOPD severity (based on objective indicators such as respiratory rate, oxygen demand, and blood gas analysis), and provides individualized programs for patients in different tiers (grade I to III) to gradually improve diaphragmatic dysfunction and exercise intolerance. The intensity was dynamically adjusted by real-time assessment of vital signs and Borg dyspnea score to ensure safety and effectiveness, and at the same time promote the improvement of exercise endurance (6MWT increased by 108.0 m in the study group and by 36.7 m in the control group, p < 0.001), reflecting the enhancement of cardiopulmonary coordination and the reduction of diaphragmatic fatigue. In the study group, the duration of noninvasive mechanical ventilation (7.5 days vs. 9.0 days, P = 0.041), hospitalization (8.25 days vs. 10.75 days, P = 0.034), and the complication rate (6.46% vs. 21.26%, P = 0.046) were significantly optimized, which may be attributed to the fact that exercise can increase the systemic circulation of the internal organs and other blood vessels, promote gastrointestinal peristalsis, and improve the blood circulation to the skin at the facial compression area and gastrointestinal flatus. And blood circulation of the skin at the facial compression site, reducing the risk of facial compression injuries in patients14, and the medical staff constantly reminded the patients to adjust their breathing during the exercise process to avoid excessive gas from entering the patient’s stomach. At the same time, exercise can also improve the respiratory muscle strength, enhance the ability of airway sputum removal, improve oxygenation, promote lung reopening, and reduce the time of non-invasive mechanical ventilation and hospitalization time of patients. And the elevation of DTF (p = 0.042) may also imply that stratified rehabilitation intervention promotes the transformation of diaphragm fibers to oxidative metabolism type (Type I) in the mechanism, and systematic aerobic and resistance training improves peripheral muscle oxygen utilization and reduces assisted respiratory muscle dependence, which reflects the protective effect of targeted training on respiratory muscle recovery and overall prognosis, but it needs to be confirmed by further studies. The strong correlation between diaphragmatic mobility (DE) improvement and 6MWT performance (r = 0.68, P < 0.01) further validated the effectiveness of graded exercise in targeting the core pathological aspects of diaphragmatic dysfunction and decreased activity endurance. In conclusion, graded exercise rehabilitation effectively promotes diaphragm function remodeling and whole-body endurance improvement by adjusting the intervention intensity and dynamically optimizing the parameters according to individual respiratory muscle capacity, which is an important step in the field of evidence-based rehabilitation for AECOPD.
Conclusion
Graded exercise rehabilitation can effectively improve the overall diaphragm function of patients, and has a positive effect on improving exercise quality and endurance; Bedside ultrasound can dynamically and real-time observe the diaphragm movement status of AECOPD patients, objectively and directly evaluate the recovery of respiratory muscle function, and has potential clinical value.
Limitations
① Although this study has achieved some results in exploring the effects of graded exercise rehabilitation on diaphragm function and movement in AECOPD patients, there are still limitations such as small sample size, insufficient sample representativeness, and short intervention time, so in the future, we should expand the sample size to conduct intergroup analysis to verify the differences in rehabilitation between patients with different levels of disease. We should also carry out a multicenter study to include patients from different regions and levels of hospitals to enhance the diversity and representativeness of the samples and further validate the effectiveness of graded exercise rehabilitation; ② Extend the follow-up time, establish a long-term tracking mechanism, and closely observe the patients’ rehabilitation progress, adherence, disease recurrence rate, and long-term impact on the quality of life after discharge from the hospital; Optimize the study design, and adopt a more stringent randomization and stratification Optimize the study design, using a more rigorous randomization and stratification strategy of randomization, set up a comparison of the differences in the effects of different intervention groups, so as to optimize the rehabilitation program and provide more accurate and effective guidance for clinical practice.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request. Data requests should include a brief description of the intended use and any relevant research credentials. All data sharing will comply with applicable ethical guidelines and institutional policies.
References
Kahnert, K., Jörres, R. A., Behr, J. & Welte, T. The diagnosis and treatment of COPD and its comorbidities. Dtsch. Arztebl. Int. 120(25), 434–444. https://doi.org/10.3238/arztebl.m2023.027 (2023).
Chen, S. et al. The global economic burden of chronic obstructive pulmonary disease for 204 countries and territories in 2020–50: A health-augmented macroeconomic modelling stud. Lancet Glob. Health 11(8), e1183–e1193 (2023).
Ruel, M. et al. The diaphragm in emphysema. Chest Surg. Clin. N. Am. 8(2), 381 (1998).
Cao, Y. et al. Diaphragm dysfunction and rehabilitation strategy in patients with chronic obstructive pulmonary disease. Front. Physiol. 13, 872277 (2022).
Schwalm, C. et al. Activation of autophagy in human skeletal muscle is dependent on exercise intensity and AMPK activation. FASEB J. 29(8), 3515–3526 (2015).
Global Initiative for Chronic Obstructive Lung Disease. Global strategy for prevention, diagnosis, and management of chronic obstructive pulmonary disease. 2020.
Chun, E. M., Han, S. J. & Modi, H. N. Analysis of diaphragmatic movement before and after pulmonary rehabilitation using fluoroscopy imaging in patients with COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 10, 193–199 (2015).
Crimi, C. et al. Utility of ultrasound assessment of diaphragmatic function before and after pulmonary rehabilitation in COPD patients. Int. J. Chron. Obstruct. Pulmon. Dis. 13, 3131–3139 (2018).
Neş, S., Gen, A., Kurtaiş, Y. et al. Effects of pulmonary rehabilitation on diaphragm thickness and contractility in patients with chronic obstructive pulmonary disease. Turk. J. Med. Sci. (2021).
Lareau, S. C. et al. Chronic obstructive pulmonary disease (COPD). Am. Respir. Crit. Care Med. 199(1), P1–P2 (2019).
Goligher, E. C. et al. Diaphragmatic myotrauma: A mediator of prolonged ventilation and poor patient outcomes in acute respiratory failure. Lancet Respir. Med. 7(1), 90–98 (2019).
Ries, A. L. et al. Pulmonary rehabilitation joint ACCP/AACVPR evidence-based clinical practice guidelines. J. Chest 131(5 Suppl), 4S-42S. https://doi.org/10.1378/chest.06-2418 (2007).
Rochester, C. L. et al. An official American Thoracic Society European Respiratory Society policy statement enhancing implementation use and delivery of pulmonary rehabilitation. J. Am. J. Respir. Crit. Care Med. 192(11), 1373–1386. https://doi.org/10.1164/rccm.201510-1966ST (2015).
Keirns, B. H. et al. Exercise and intestinal permeability: Another form of exercise-induced hormesis?. Am. J. Physiol. Gastrointest. Liver Physiol. 319(4), G512–G518 (2020).
Acknowledgements
Thanks to all the participants who gave their time and energy to this research.
Funding
1. Funding organizations: 贵州省科学技术厅 Number: 黔科合成果-LC[2024]035 2. Funding organizations: 贵州省护理学会 Number: GZHLKY2022073 3. Funding organizations: 《贵州省老年智慧康养科技创新人才团队建设》 Number: 黔科合平台人-CXTD[2023]028.202411 4. Funding institution name: [The Second Affiliated Hospital of Zunyi Medical University] Funding number: [遵市科合HZ字(2025)123号].
Author information
Authors and Affiliations
Contributions
Hui Zeng: Methodology, Project Administration, Funding Acquisition. Hongmin Ran, Yue Chen: Investigation, Formal Analysis, Writing-Original Draf, Writing-Review & Editing. Lijuan Zhang: provided key technical support (the diaphragm ultrasound examination) Lina Ma, Jimei Luo: Visualization,collected data; Yan Wang, Dandan Fu, Nana Yang, Rong Liu, Luwen Luo, Chuanli Chen: Investigation, calculated the statistical data. All authors participated in the discussion and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Ran, H., Chen, Y., Zhang, L. et al. A randomized controlled trial of graded exercise rehabilitation enhances diaphragm function and exercise tolerance in patients with AECOPD. Sci Rep 15, 28510 (2025). https://doi.org/10.1038/s41598-025-09224-3
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-09224-3