Abstract
Nasopharyngeal carcinomas (NPC) are malignancies that have seen growing burdens with human papilloma virus (HPV) infection. This investigation aims to characterize social determinant factor of health (SDoH) differences across HPV-differentiated NPC across the USA. NPC-patients with confirmed-HPV status between 2010 and 2018 from the Surveillance-Epidemiology-End Results (SEER) database were analyzed by cox-proportional and logistic regressions of age, sex, race-ethnicity, census-level rurality-urbanicity, and census-level Yost-Socioeconomic Status (SES)-Index measures to assess mortality, staging, and delayed-treatment differences. Among 820-HPV( −) and 402-HPV(+) NPCs, both NPC-cohorts displayed reduced overall mortality risk with younger age (HR 0.56, 95% CI 0.38–0.81; HR 0.57, 0.45–0.73) and higher risk with male sex (HR 1.71, 95% CI 1.11–2.64; HR 1.42, 95% CI 1.07–1.87). For HPV(–) only, Hispanic (HR 0.51, 95% CI 0.32–0.82) and Asian ethnicities (HR 0.44, 95% CI 0.33–0.58) reduced overall mortality risk, while low Yost-SES-Index increased it (HR 1.44, 1.14–1.87). For HPV( −) only, delayed treatment occurred with lower Yost-SES-Index (OR 1.97, 95% CI 1.16–3.42). Using the Yost-SES-Index and other individual/census-level SDoH, multilevel SDoH-analyses of HPV-differentiated NPC-patients display vast prognostic and treatment differences based on HPV-status. These present specific targets to prospectively and strategically address drivers of disparity with limited public health resources.
Similar content being viewed by others
Introduction
Nasopharyngeal carcinomas (NPC) are rare head and neck malignancies which arise from nasopharynx epithelial mucosa1. NPC accounted for less than 1% (129,000 cases) of cancers globally in 2018; over 70% of NPC incidence is reported from East and Southeast Asia alone1,2,3. In the United States, NPC accounts for 2% of head and neck cancer burden, with an incidence rate of less than 1 per 100,000 person-years4,5. The striking geographic disparity suggests an etiology featuring a mix of genetics, Epstein Barr Virus (EBV) infection, dietary habits, lifestyle, and exposures to environmental risk factors6,7. Historically, NPC’s poor prognosis has largely been attributed to lack of awareness of symptoms and risk, although detection of early-stage NPC and appropriate targeted therapy has been shown to mitigate this outlook6,7,8. As a result, effective population screening using plasma EBV DNA has emerged a useful tool in reducing population NPC burden4,9.
An underappreciated viral risk factor for NPC may be human papillomavirus (HPV), which has otherwise been extensively studied in oropharyngeal carcinoma (OPC)10,11,12. Among prior investigations of HPV association with NPC, several single-site studies within the USA and United Kingdom detected significant prevalence of unique NPC-subtypes comprised of EBV-negative, HPV-positive (HPV(+)) infection status while observing prognostic differences among HPV(+) and HPV-negative (HPV(−)) NPC-subtype groups13,14,15. In addition, larger studies across national-spanning patient cohorts have observed associations between history of HPV infection and higher incidence of NPC, alongside poorer prognostic outcomes of increased tumor burden independent of EBV-infection status, age, race-ethnicity, and smoking behaviors16,17,18. Additionally, growing epidemiologic trends have showcased robust independent associations between HPV-status and primary sites outside of traditional OPC sites19.
Given these clinical associations of HPV with NPC and other head and neck cancers, social determinants of health (SDoH), such as age, race-ethnicity, sex, insurance, and income level, have also been implicated in several HPV-related investigations of OPC, as well as in non-HPV-focused NPC studies observing Asian and black race-ethnicity5,8,20,21,22,23,24. However, SDoH-focused investigations into NPC on HPV-status with more recent samplings of national populations (2010 and after) have yet to be performed. This is in spite of prior evidence on the propensity for HPV-infection to independently influence squamous cell cancer sites outside of OPC sites. Moreover, multivariable models accounting for a wider variety of SDoH to allow enhanced real-world generalizability, namely comprising both individual and community-level factors, have yet to be considered.
To address these shortcomings, our retrospective cohort study aims to utilize comprehensive multivariable models for examining differences in SDoH-contribution of mortality, preliminary staging, and treatment delay across HPV(+) and HPV(−) NPCs. In doing so, this study incorporates the Yost Index, a composite metric comprising seven differentially weighted census-level socioeconomic status factors, alongside numerous individual-level SDoH-variables to predict specific, adjusted relationships between certain SDoH-factors and HPV-differentiated NPC outcomes.
Methods
This retrospective cohort study follows the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. Due to this study utilizing retrospective, deidentified public databases, the Northwestern University Institutional Review Board deems this research as non-human research and therefore this study is exempted from the approval process per their institutional policy.
Databases
The National Cancer Institute-Surveillance, Epidemiology, and End Results Program (SEER) database contains national datasets of patient variables, pathological characteristics, treatment modalities, and prognostic outcomes. This study utilizes the specially authorized incidence database for head and neck tumors with linked census tract-level socioeconomic status (SES) and rurality-urbanicity, spanning patients from 2010 to 2018 and 18 registries across the USA.
The Yost Index is a census tract-level, composite SES measure provided within the specialized SEER dataset aforementioned. It is comprised of seven census-level measures for each of the 72,158 USA-Census tracts: median household income, percent below 150% of poverty line, median house value, median rent, percent working class, percent unemployed, and education index level18. To maintain chronological consistency of these measures based on the date of tumor diagnosis, these socioeconomic status was based on averaged measures of the seven factors across various sets of American Community Survey (ACS)/USA Census 5-year estimates of which the year of diagnosis overlaps within the ACS estimate (i.e. a tumor diagnosed in 2012 will have their Yost Index score and quintile calculated from the averaged measures of the 2008–2012, 2009–2013, 2010–2014, 2011–2015, and 2012–2016 ACS 5-year estimates).
Population definitions
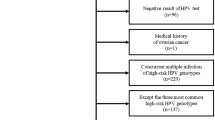
All cases of nasopharyngeal carcinomas were selected from International Classification of Disease for Oncology version 3.8 (ICD‐O-3) tumor site codes [C11.0–11.9] between 2010 and 2018. Disease or histological classifications of squamous cell carcinoma were determined by ICD-O-3 codes recategorized by SEER-determined labels. Inclusion criteria were adult patients (20 + years) with confirmed HPV(+) or HPV(−) status, which was determined by IHC for p16 expression per SEER-documentation.
Characteristics and outcome variable definitions
The individual-level sociodemographic/SDoH variables consisted of age (< 65 and 65+ years as the categories), biological sex, race-ethnicity (Non-Hispanic White, Black, Hispanic, Asian and Native Pacific Islander, Native American, and Unknown) on a per-patient basis. The census-level SDoH variables consisted of census-level Yost-Index-SES score and a composite urbanicity-rurality comprised of the two available SEER-variables. For the former, patients were split into two equivalently sized cohorts of “Lower SES,” which encompassed quintiles of “Lowest,” “Lower” and “Middle” SES, which comprised quintiles of “Higher” and “Highest” SES. For the latter, rurality status was determined when the patient either had a RUCA designation of “Non-Urban” or a URIC designation of “Mostly Rural” or “All Rural.”
Outcome variables consisted of the following: cancer/disease-specific and all-cause-related mortality was determined by SEER-categorized variables, alongside time points for three-year and five-year mortality. Advanced staging for malignant tumors was based on SEER-designated variables labeled as “Stage IV,” “distant [expansion],” or “distal [expansion]” and recoded under SEER’s most recent tumor staging data: American Joint Committee on Cancer, 6th Edition (AJCC-6) classifications. Delay in treatment after diagnosis was based on months after preliminary diagnosis with designated timepoints of 1-month and 3-month delays.
For the specific specialized dataset utilized, all sociodemographic factors available and permitted were utilized in multivariable models as independent and dependent variable components.
Statistical analysis
All multivariable models consisted of the following covariates: younger age (being younger than 65 years old upon diagnosis, reference level being 65 and older), male sex (reference being female sex), being of black race-ethnicity (reference not being of black race-ethnicity), being of Hispanic race-ethnicity (reference not being of Hispanic race-ethnicity), being of Asian or Pacific Islander race-ethnicity (reference not being of Asian or Pacific Islander race-ethnicity), Yost Index/”Lower Socioeconomic Status” (being in the lowest, lower, or middle SES quintiles, reference being in the higher, highest SES quintiles), and increased rurality (being of “rural” RUCA-designation or “all rural” and “mostly rural” URIC-designations; reference being “urban” RUCA-designation or “all urban” and “mostly urban” URIC-designations); stratifying variate of HPV(+) or HPV(−) status. Covariates were selected based on inclusion in previous studies demonstrating granular disparities amongst socioeconomics and demographics in head and neck cancers based on HPV status and nasopharyngeal cancer outcomes5,10,22,25,26,27.
Multivariable cox-proportional hazard models were used to evaluate factors contributing to quicker time-to-mortal event secondary to all causes. Multivariable logistic regression models were also used to delineate covariate effects on aspects of mortality not well-represented within cox-proportional models of overall mortality/survival, which principally focuses on the whole timespan of mortal events with time as a continuous covariate while censoring significant events that obscure covariate effects at specific timepoints28. Multivariable logistic regression models were also used to assess odds of having a late-presenting stage (based on SEER-recoded combined staging, reference level being diagnosed with Stage I-III) and 1 or 3-month-or-more delay-in-treatment after diagnosis (reference level being treatment receipt in less than 1 months or 3 months, respectively) based on prior literature standards for time cutoffs29,30. These regressions were performed as separate, multivariable models within HPV(+)and HPV(−) groups based on traditionally noted demographic differences among HPV-statused populations31,32. Two-sided p-values were calculated and p < 0.05 was considered statistically significant. All statistical analyses were performed using R version 4.2.1.
Results
Patient demographics
Among the 1222 patients with NPC that were identified, 820 (57.7%) were HPV(−) and 402 (28.3%) were HPV(+). The highest represented sociodemographic characteristics were 45–64 years of age (n = 669, 54.7%), males (n = 881 , 72.1%), and white race (n = 521, 42.6%). The highest represented census-level characteristics were Low-Middle Socioeconomic Status by Yost-Index Score (n = 582, 50.2%), “All Urban” rural-urbanicity (n = 888, 75.3%). The highest represented clinical characteristics include NPC-staging of I, II, or III per AJCC-6 overall TNM-classifications (n = 653, 54.6%). These characteristics stratified by HPV status are further described in Table 1.
Mortality
Mortality was assessed using four outcomes: time to overall mortality, and whether or not a cancer-specific mortality, 3-year all-cause mortality, or 5-year all-cause mortality would occur across HPV status cohorts.
Predictors of time to overall mortality
In both HPV(+) and HPV(−) NPCs, younger age less than 65 years old showed decreased overall mortality risk (respectively, HR 0.56, 95%CI 0.38–0.81, p = 0.003; HR 0.57, 0.45–0.73, p < 0.001), while being male showed increased overall mortality risk (respectively, HR 1.71, 95%CI 1.11–2.64, p = 0.001; HR 1.42, 95%CI 1.07–1.87, p = 0.012).
Within only HPV(−) NPCs, being of Hispanic (HR 0.51, 95%CI 0.32–0.82, p = 0.002) and Asian or Pacific Islander race-ethnicity (0.44, 0.33–0.58, p < 0.001) showed associations of decreased overall mortality risk while low Yost-Index (i.e. poor socioeconomic status) showed associations of increased risk of quicker time-to-mortal event (1.44, 1.14–1.87, p = 0.003). These are tabulated in Table 2.
Effectors of cancer/disease-specific mortality
With HPV(−) status, younger age less than 65 years old (OR 3.24, 95%CI 1.68–6.37, p < 0.001) and Hispanic race (6.11, 1.14–114, p = 0.032) uniquely demonstrated increased odds of cancer-specific mortality. Also unique to HPV(−) status NPCs, male sex (0.30, 0.11–0.73, p = 0.006) demonstrated decreased odds of cancer-specific mortality. These results are tabulated in Table 3.
Effectors of 3-year all-cause mortality
In both HPV(+) and HPV(−) cancers, younger age showed decreased odds of 3-year all-cause mortality (respectively OR 0.43, 95%CI 0.23–0.80, p = 0.007; 0.41, 0.28–0.61, p < 0.001). Unique to HPV(+), Male sex demonstrated increased odds of 3-year all-cause mortality (1.81, 1.01–3.31, p = 0.049). Unique to HPV(−), being of Asian or Pacific Islander race-ethnicity (0.36, 0.24–0.55, p < 0.001) and Hispanic race-ethnicity (0.40, 0.20–0.78, p = 0.007) showed decreased odds. Also only found within HPV(−) cohorts, low Yost-Index demonstrated increased odds of 3-year all-cause mortality (1.72, 1.17–2.53, p = 0.006). These results are tabulated in Table 4.
Effectors of 5-year all-cause mortality
Amongst both HPV(+) and HPV(−) NPCs, younger age (respectively OR 0.30, 95%CI 0.11–0.71, p = 0.005; 0.38, 0.23–0.62, p < 0.001) and being of Asian or Pacific Islander race-ethnicity (respectively 0.37, 0.17–0.78, p = 0.009; 0.37, 0.23–0.60, p < 0.001) showed decreased odds of 5-year all-cause mortality. Unique to HPV(−), being of Hispanic race-ethnicity demonstrated decreased odds (0.38, 0.18–0.81, p = 0.012) while low Yost-Index had demonstrated increased odds of 5-year all-cause mortality (1.71, 1.11–2.66, p = 0.016). These results are tabulated in Table 5.
Effectors of advanced preliminary staging
HPV(−) NPCs uniquely showed younger age (OR 1.48, 95%CI 1.07–2.05, p = 0.018) and Black race (1.87, 1.14–3.09, p = 0.013) demonstrated increased odds of advanced preliminary staging. These are tabulated in Table 6.
Effectors of delay of treatment from diagnosis
Delay-in-treatment from diagnosis was assessed as primary treatment occurring at or after 1 month and 3 months since diagnosis of NPC. For patients diagnosed with HPV(−) NPCs, low Yost-Index uniquely showed increased odds of having a 1-month delay of treatment initiation (1.61, 1.15–2.25, p = 0.005) that markedly increased with having a 3-month delay of treatment (1.97, 1.16–3.42, p = 0.012). For patients diagnosed with HPV(+) NPCs, younger age was associated with decreased odds of having a 1-month delay of treatment (0.47, 0.27–0.84, p = 0.012). These results are tabulated in Table 7.
Discussion
To our knowledge, this is the first study to show differences in detrimental contributions of a multitude of individual- and community-level SDoH-factors for nasopharyngeal carcinoma stratified by HPV status in outcomes of mortality, advanced preliminary staging, and delay of treatment.
NPC prognosis, like in other head and neck cancers, has been shown to be associated with several predictors of mortality such as age above 65, advanced tumor staging, White race, and lack of insurance8,33,34,35,36. While HPV(+) is a protective factor in non-NPC head and neck cancer, the prognostic role of HPV in NPC remains unclear10,20. In an analysis of 517 patients from the SEER database, Wotman et al. found that cause-specific survival was not associated with HPV status, although intergroup ethnicity differences manifested significant differences25. Interestingly, they found that 34.8% of patients in their study cohort were positive for HPV(−) associated NPC where East Asians and individuals over the age of 25 were more likely to be HPV(−)25. Tham et al. conducted a meta-analysis of HPV significance in NPC with pooled hazard ratios demonstrating no association with overall survival, although subgroup analysis and consideration of the different study designs included make it difficult to draw any definitive conclusions37. Nevertheless, evidence from USA population studies uncovering the clinical phenomenon of HPV(+) as opposed to EBV(+) NPC as well as the endemic burden of HPV provide impetus to better understand prognostic significance38,39.
We found several meaningful implications of HPV status differentiation in cancer/disease-specific mortality, 3-year all-cause mortality, and 5-year all-cause mortality. Patients with HPV(−) NPC cancer-specific mortality were more likely to be Hispanic or less than 65 years old, and they were more likely to be Male. In a retrospective study of the National Cancer Data Base (NCDB), Verma et al. found an association between age as a continuous variable with HPV(+) NPC40. Furthermore, younger age fails to be uniquely predicted across HPV status for both 3- and 5-year all-cause mortality, but Hispanic race presents as negatively predicted by HPV(−) status, potentially indicating that Hispanic race is differentially associated with either cancer-specific or all-cause mortality. To our knowledge, there have been no substantive associations between Hispanic race and HPV status in NPC prognosis, warranting further exploration. 3-year all-cause mortality analysis demonstrates that HPV(−) is a factor associated negatively with Asian race as opposed to White race, contradicting other studies finding an association with HPV(+) and White patients25,37,41,42. However, these studies may be limited by specific subsets of endemic populations, as Kang et al. found p16 expression in more than half of South Korean patients with NPC43. Nevertheless, 5-year all-cause mortality analysis fails to uniquely demonstrate HPV(−) as negatively associated with Asian/Pacific Islander race-ethnicity.
Of the notable differences in effects, slower time to overall mortality per cox-proportional models was observed with NPC patients of Hispanic or Asian-Pacific Islander race-ethnicity across both HPV(+) and HPV(−) groups. However, these observed associations were only present within HPV(−) observed occurrences of 3-year mortality and only became present across both HPV-cohorts for observed occurrences of 5-year mortality. Furthermore, when looking at disease-specific mortality, among patients that did suffer mortal events regardless of when it occurred, Hispanic NPC-HPV(−) patients displayed uniquely higher odds in comparison to other NPC patients of other races/ethnicities.
For both 3- and 5- year all-cause but not cancer-specific mortality, HPV(−) was positively associated with low Yost index, suggesting that patients with HPV(−) NPC are more likely to experience higher risks of earlier mortality with lower composite SES. Given that HPV(−) demographics (e.g. male, older) have traditionally shown riskier individual behaviors, these unique aspects of earlier all-cause mortality but not cancer-specific mortality remain consistent with these prior observed relationships. Consistent with these interpretations, earlier 3-year timepoints among HPV(−) showcase significant but lower magnitude detrimental associations with Yost-Index and other sociodemographic factors compared to the effect sizes observed with later 5-year timepoints. Such increases from 3-year to 5-years showcase an expected outcome of the above outlined relationship, where riskier individual behaviors over longer periods of time would experience increased mortality risks.
Additionally, for patients with a delay of treatment, HPV(−) was also uniquely positively associated with low Yost-Index. The Yost Index has previously been utilized in a variety of cancer studies ranging from intracranial tumor metastases to head and neck cancers such as NPC where there is a consistent association between socioeconomic status and disease prognosis5,44,45. Furthermore, these studies have displayedimportant impacts of socioeconomic disadvantage with treatment modality, clinical course, and preliminary tumor staging upon diagnosis5,44,45,46,47. The results of the present study support these trends and suggest that HPV(−) NPC possesses unique detrimental associations with socioeconomic disadvantage underlying lack of access to care, inequality of resources, or higher risk behaviors and environmental exposures in the USA cancer population48,49,50,51. Furthermore, HPV(−) NPC showed uniquely positive associations ofyounger age and Black race with advanced tumor staging upon preliminary diagnosis, corresponding with the literature on social factors like minority race and HPV(+) status on favorable head and neck cancer clinical presentations10,11,20,34. As more data accumulates on how HPV status may mediate the association between socioeconomics and demographic risk, mortality, treatment modality, and clinical course, it is necessary to design screening, intervention, and future research inclusive of quality of life and psychological considerations as well52,53.
This study has several limitations. First, while this analysis demonstrates unique prediction of patient exposure characteristics given HPV status, it does not necessarily indicate translation of exposure into either HPV(−) or HPV(+) NPC. In addition, the majority of studies on HPV in NPC are retrospective database studies of varying designs, sample sizes, and patient populations. Therefore, it will be important to substantiate our results and those of the literature alongside longitudinal prospective analyses or larger retrospective analyses employing more specific patient selection and exposure definition criteria. Another limitation of this study is the use of HPV status based on SEER p16 status data, which may not be entirely concordant but was necessitated due to it being the only designated variable available for determining HPV-status. In addition, our HPV-stratified approach of sociodemographic analyses may inherently present biases from which excluded mechanisms associated with changes in HPV-status are not properly ascertained. It should be denoted that the present study’s approach should restrict the findings of significant associations solely within the selected HPV-cohorts themselves, rather than cross-comparing to assess differential effects comparisons. It is also important to note that use of the Yost index approximates patient disadvantage with their census tracts, a useful and validated methodology in population-based health services research. Boscoe et al. further substantiated the utility of the Yost index by comparing it with other similarly designed socioeconomic indices, demonstrating high face validity with a cautionary note for inherent uncertainties accounting for up to ± 8 percentiles54,55. Future research should look into proprietary datasets that would allow the linkage of heterogenous, community-level SDoH-variables that go beyond the categories represented in our current models. Finally, this study examines HPV status in isolation of EBV status, although this interplay is necessary to explore further in extrapolation to the larger United States population.
Using multivariable models assessing individual-level and census-level measures of social determinant factors, this national investigation of nasopharyngeal carcinomas displayed disparities in outcomes of mortality, advanced preliminary staging, and delay of treatment differentiated by confirmed HPV status. It was found that the role of HPV status of race and ethnicity in mortality highlights a differential effect in Hispanic patients for cancer-specific vs all-cause mortality while complicating our understanding of Asian race and mortality across HPV status in NPC. Furthermore, HPV(−) status was positively associated with low community-level socioeconomic status, as measured by the Yost index, in all-cause mortality and treatment delay and positively associated with younger age and Black race in advanced preliminary staging. Altogether, our findings demonstrate that HPV-status is an important effector in understanding the impact of social determinants on the NPC population, promoting more directable means of recognizing and establishing health strategies and risk mitigation for providers and policymakers alike in tackling SDoH-disparities of HPV-differentiated nasopharyngeal carcinoma.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Chen, Y.-P. et al. Nasopharyngeal carcinoma. Lancet 394, 64–80 (2019). https://doi.org/10.1016/S0140-6736(19)30956-0
Bray, F. et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 68, 394–424. https://doi.org/10.3322/caac.21492 (2018).
Chan, A. T., Teo, P. M. & Johnson, P. J. Nasopharyngeal carcinoma. Ann. Oncol. 13, 1007–1015. https://doi.org/10.1093/annonc/mdf179 (2002).
Sinha, S. & Gajra, A. in StatPearls (StatPearls Publishing Copyright © 2023, StatPearls Publishing LLC., 2023).
London, A. O. et al. Impact of race, ethnicity, and socioeconomic status on nasopharyngeal carcinoma disease-specific and conditional survival. J. Neurol. Surg. B Skull Base 83, 451–460. https://doi.org/10.1055/s-0041-1741111 (2022).
Lee, H. M., Okuda, K. S., González, F. E. & Patel, V. Current perspectives on nasopharyngeal carcinoma. Adv. Exp. Med. Biol. 1164, 11–34. https://doi.org/10.1007/978-3-030-22254-3_2 (2019).
Chang, E. T., Ye, W., Zeng, Y. X. & Adami, H. O. The evolving epidemiology of nasopharyngeal carcinoma. Cancer Epidemiol. Biomark. Prev. 30, 1035–1047. https://doi.org/10.1158/1055-9965.Epi-20-1702 (2021).
Osazuwa-Peters, N. et al. Predictors of stage at presentation and outcomes of head and neck cancers in a university hospital setting. Head Neck 38(Suppl 1), E1826-1832. https://doi.org/10.1002/hed.24327 (2016).
Shah, A. B. & Nagalli, S. in StatPearls (StatPearls Publishing Copyright © 2023, StatPearls Publishing LLC., 2023).
Wu, Q. et al. HPV positive status is a favorable prognostic factor in non-nasopharyngeal head and neck squamous cell carcinoma patients: A retrospective study from the surveillance, epidemiology, and end results database. Front. Oncol. 11, 688615. https://doi.org/10.3389/fonc.2021.688615 (2021).
Timbang, M. R. et al. HPV-related oropharyngeal cancer: a review on burden of the disease and opportunities for prevention and early detection. Hum. Vaccin. Immunother. 15, 1920–1928. https://doi.org/10.1080/21645515.2019.1600985 (2019).
Tanaka, T. I. & Alawi, F. Human papillomavirus and oropharyngeal cancer. Dental Clin. N. Am. 62, 111–120 (2018). https://doi.org/10.1016/j.cden.2017.08.008
Robinson, M. et al. Oncogenic human papillomavirus-associated nasopharyngeal carcinoma: An observational study of correlation with ethnicity, histological subtype and outcome in a UK population. Infect. Agents Cancer 8, 30. https://doi.org/10.1186/1750-9378-8-30 (2013).
Walline, H. M. et al. High-risk human papillomavirus detection in oropharyngeal, nasopharyngeal, and oral cavity cancers: Comparison of multiple methods. JAMA Otolaryngol. Head Neck Surg. 139, 1320–1327. https://doi.org/10.1001/jamaoto.2013.5460 (2013).
Shimizu, Y. et al. Clinical impact of p16 positivity in nasopharyngeal carcinoma. Laryngoscope Investig. Otolaryngol. 7, 994–1001 (2022). https://doi.org/10.1002/lio2.832
Jacinto, J. K. M. et al. Clinical behavior and outcome of HPV-positive nasopharyngeal carcinoma. Int. J. Radiat. Oncol. Biol. Phys. 111, e384–e385 (2021). https://doi.org/10.1016/j.ijrobp.2021.07.1125
Hung, S.-H., Yang, T.-H., Cheng, Y.-F., Chen, C.-S. & Lin, H.-C. Association of nasopharynx cancer with human papillomavirus infections. Cancers 15, 4082 (2023).
Huang, S. H. et al. Clinical presentation and outcome of human papillomavirus-positive nasopharyngeal carcinoma in a North American cohort. Cancer 128, 2908–2921. https://doi.org/10.1002/cncr.34266 (2022).
Amanian, A., Ishii, M., Fakhry, C. & London, N. R. Jr. Epidemiologic trends in human papillomavirus-associated sinonasal squamous cell carcinoma. JAMA Otolaryngol. Head Neck Surg. https://doi.org/10.1001/jamaoto.2024.1311 (2024).
Pike, L. R. G. et al. Outcomes of HPV-associated squamous cell carcinoma of the head and neck: Impact of race and socioeconomic status. J. Natl. Compr. Cancer Netw. 18, 177–184. https://doi.org/10.6004/jnccn.2019.7356 (2020).
Stein, E. et al. Systematic review and meta-analysis of racial survival disparities among oropharyngeal cancer cases by HPV status. Head Neck 42, 2985–3001. https://doi.org/10.1002/hed.26328 (2020).
Mazul, A. L. et al. Gender and race interact to influence survival disparities in head and neck cancer. Oral Oncol. 112, 105093. https://doi.org/10.1016/j.oraloncology.2020.105093 (2021).
Habib, A. M. et al. Impact of race and insurance status on primary treatment for HPV-associated oropharyngeal squamous cell carcinoma. Otolaryngol. Head Neck Surg. 166, 1062–1069. https://doi.org/10.1177/01945998211029839 (2022).
Chang, T. S. et al. The combined effect of individual and neighborhood socioeconomic status on nasopharyngeal cancer survival. PLoS ONE 8, e73889. https://doi.org/10.1371/journal.pone.0073889 (2013).
Wotman, M. et al. HPV status in patients with nasopharyngeal carcinoma in the United States: A SEER database study. Am. J. Otolaryngol. 40, 705–710. https://doi.org/10.1016/j.amjoto.2019.06.007 (2019).
Zhou, L. et al. The racial disparity of nasopharyngeal carcinoma based on the database analysis. Am. J. Otolaryngol. 40, 102288. https://doi.org/10.1016/j.amjoto.2019.102288 (2019).
Settle, K. et al. Racial survival disparity in head and neck cancer results from low prevalence of human papillomavirus infection in black oropharyngeal cancer patients. Cancer Prev. Res. (Phila.) 2, 776–781. https://doi.org/10.1158/1940-6207.Capr-09-0149 (2009).
Annesi, I., Moreau, T. & Lellouch, J. Efficiency of the logistic regression and Cox proportional hazards models in longitudinal studies. Stat. Med. 8, 1515–1521. https://doi.org/10.1002/sim.4780081211 (1989).
Goel, A. N. et al. Survival impact of treatment delays in surgically managed oropharyngeal cancer and the role of human papillomavirus status. Head Neck. 41(6), 1756–1769. https://doi.org/10.1002/hed.25643 (2019).
Morse, E. et al. treatment delays in primarily resected oropharyngeal squamous cell carcinoma: national benchmarks and survival associations. Otolaryngol. Head Neck Surg. 159(6), 987–997. https://doi.org/10.1177/0194599818779052 (2018).
Liederbach, E. et al. The national landscape of human papillomavirus-associated oropharynx squamous cell carcinoma. Int. J. Cancer. 140(3), 504–512. https://doi.org/10.1002/ijc.30442 (2017).
Young, D. et al. Increase in head and neck cancer in younger patients due to human papillomavirus (HPV). Oral Oncol. 51(8), 727–730. https://doi.org/10.1016/j.oraloncology.2015.03.015 (2015).
Goshtasbi, K. et al. A comprehensive analysis of treatment management and survival outcomes in nasopharyngeal carcinoma. Otolaryngol. Head Neck Surg. 165, 93–103. https://doi.org/10.1177/0194599820973241 (2021).
Chow, L. Q. M. Head and neck cancer. N. Engl. J. Med. 382, 60–72. https://doi.org/10.1056/NEJMra1715715 (2020).
Sun, L. M., Li, C. I., Huang, E. Y. & Vaughan, T. L. Survival differences by race in nasopharyngeal carcinoma. Am. J. Epidemiol. 165, 271–278. https://doi.org/10.1093/aje/kwk008 (2007).
Wang, Y., Zhang, Y. & Ma, S. Racial differences in nasopharyngeal carcinoma in the United States. Cancer Epidemiol. 37, 793–802. https://doi.org/10.1016/j.canep.2013.08.008 (2013).
Tham, T., Teegala, S., Bardash, Y., Herman, S. W. & Costantino, P. Is human papillomavirus and p16 expression associated with survival outcomes in nasopharyngeal cancer? A systematic review and meta-analysis. Am. J. Otolaryngol. 39, 764–770. https://doi.org/10.1016/j.amjoto.2018.07.005 (2018).
Maxwell, J. H. et al. HPV-positive/p16-positive/EBV-negative nasopharyngeal carcinoma in white North Americans. Head Neck 32, 562–567. https://doi.org/10.1002/hed.21216 (2010).
Ngan, H. L., Wang, L., Lo, K. W. & Lui, V. W. Y. Genomic landscapes of EBV-associated nasopharyngeal carcinoma vs. HPV-associated head and neck cancer. Cancers (Basel) (2018). https://doi.org/10.3390/cancers10070210
Verma, V., Simone, C. B. 2nd. & Lin, C. Human papillomavirus and nasopharyngeal cancer. Head Neck 40, 696–706. https://doi.org/10.1002/hed.24978 (2018).
Thavaraj, S. in Seminars in Diagnostic Pathology. 104–111 (Elsevier).
Lin, Z. et al. Human papillomavirus 16 detected in nasopharyngeal carcinomas in white Americans but not in endemic Southern Chinese patients. Head Neck 36, 709–714 (2014).
Kang, H. et al. Clinical implications of human papilloma virus and other biologic markers in nasopharyngeal cancer. Oral Oncol. 55, e7–e10 (2016). https://doi.org/10.1016/j.oraloncology.2016.02.002
Li, Y. et al. Socioeconomic factors are associated with the prognosis of Thyroid Cancer. J. Cancer 12, 2507–2512. https://doi.org/10.7150/jca.52329 (2021).
Rodrigues, A., Li, G., Bhambhvani, H. & Hayden-Gephart, M. Socioeconomic disparities in brain metastasis survival and treatment: A population-based study. World Neurosurg. 158, e636–e644. https://doi.org/10.1016/j.wneu.2021.11.036 (2022).
Reitzel, L. R. et al. Neighborhood deprivation and clinical outcomes among head and neck cancer patients. Health Place 18, 861–868. https://doi.org/10.1016/j.healthplace.2012.03.005 (2012).
Ellis, L. et al. Racial and ethnic disparities in cancer survival: The contribution of tumor, sociodemographic, institutional, and neighborhood characteristics. J. Clin. Oncol. 36, 25–33. https://doi.org/10.1200/jco.2017.74.2049 (2018).
Naghavi, A. O. et al. Having Medicaid insurance negatively impacts outcomes in patients with head and neck malignancies. Cancer 122, 3529–3537. https://doi.org/10.1002/cncr.30212 (2016).
Liu, L., Deapen, D. & Bernstein, L. Socioeconomic status and cancers of the female breast and reproductive organs: A comparison across racial/ethnic populations in Los Angeles County, California (United States). Cancer Causes Control 9, 369–380. https://doi.org/10.1023/a:1008811432436 (1998).
Yost, K., Perkins, C., Cohen, R., Morris, C. & Wright, W. Socioeconomic status and breast cancer incidence in California for different race/ethnic groups. Cancer Causes Control 12, 703–711. https://doi.org/10.1023/a:1011240019516 (2001).
Rajeshuni, N., Zubair, T., Ludwig, C. A., Moshfeghi, D. M. & Mruthyunjaya, P. Evaluation of racial, ethnic, and socioeconomic associations with treatment and survival in uveal melanoma, 2004–2014. JAMA Ophthalmol. 138, 876–884. https://doi.org/10.1001/jamaophthalmol.2020.2254 (2020).
Henry, M. et al. Psychosocial outcomes of human papillomavirus (HPV)- and non-HPV-related head and neck cancers: A longitudinal study. Psychooncology 31, 185–197. https://doi.org/10.1002/pon.5803 (2022).
Janmunee, N., Peerawong, T., Phenwan, T., Supanichwatana, S. & Kongkamol, C. Factors influencing job retention and quality of life amongst nasopharyngeal carcinoma patients. Asian Pac. J. Cancer Prev. 22, 1401–1406 (2021). https://doi.org/10.31557/apjcp.2021.22.5.1401
Boscoe, F. P., Liu, B., Lafantasie, J., Niu, L. & Lee, F. F. Estimating uncertainty in a socioeconomic index derived from the American community survey. SSM Popul. Health 18, 101078. https://doi.org/10.1016/j.ssmph.2022.101078 (2022).
Boscoe, F. P., Liu, B. & Lee, F. A comparison of two neighborhood-level socioeconomic indexes in the United States. Spat. Spatiotemporal Epidemiol. 37, 100412. https://doi.org/10.1016/j.sste.2021.100412 (2021).
Author information
Authors and Affiliations
Contributions
D.F-Z., S.A., D.C., A.S., N.O-P., J.R. designed the study; D.F-Z., S.A. contributed to data acquisition; all authors assisted with data interpretation and critical revision; D.F-Z., S.A. drafted the manuscript; D.F-Z. and S.A. designed and generated data visualization; D.F-Z. conducted the statistical analysis; D.C., A.S., N.O-P., J.R. oversaw the work.
Corresponding author
Ethics declarations
Competing interests
Mr. Fei-Zhang has advised Atila Biosystems and Nightingale Open Science outside the submitted work. Dr. Chelius has received a coordinator stipend from the American Academy of Otolaryngology outside the submitted work. Dr. Smith owns stock in Abbott outside the submitted work. Dr. Osazuwa-Peters is a scientific advisor to Navigating Cancer. He also reported receiving grants from the National Institute of Health/National Institute of Dental and Craniofacial Research (R01 DE032216) outside of the submitted work. No other disclosures, competing financial interests, or conflicts of interest were reported by the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Fei-Zhang, D., Asthana, S., Smith, S. et al. Individual and community-level social determinant impact on HPV-differentiated nasopharyngeal carcinoma disparities in the USA. Sci Rep 15, 26778 (2025). https://doi.org/10.1038/s41598-025-10522-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-10522-z