Abstract
This study aimed to investigate the relationship between peripheral blood transferrin receptor protein (TfR) and tumor cell ferroptosis, as well as bladder cancer invasion and metastasis, and further reveal the mechanism of action of TfR in bladder cancer progression. Fifteen patients with bladder cancer, treated at the Department of Urology in our hospital from February 2022 to August 2023, were recruited as research subjects. The patients were aged between 44 and 68 years, with an average age of 52.57 ± 4.38 years. General patient data were analyzed, and the level of peripheral blood TfR was detected at baseline (T0), 3 months (T1), 6 months (T2), and 9 months (T3) post-treatment using a repeated measures design. The levels of GPX4, Ferroportin, and transferrin receptor in the peripheral blood were measured by enzyme-linked immunosorbent assay (ELISA) at T0, T1, T2, and T3. Tumor size and invasiveness were assessed using MRI imaging at the same time points. Protein expressions of MMP-2, MMP-9, and N-Cadherin were analyzed by Western blot at T0, T1, T2, and T3. Pearson correlation analysis was utilized to examine the relationship between TfR, GPX4, Ferroportin, transferrin receptor levels, and tumor invasion and metastasis. As treatment progressed, TfR levels at T3 and T2 were significantly lower than those at T1 and T0 (P < 0.05). Similarly, markers of tumor cell ferroptosis (GPX4, Ferroportin, and transferrin receptor) also showed significant decreases (P < 0.05). Tumor volume at T3 was smaller compared to T0, T1, and T2 (P < 0.05). The protein expressions of MMP-2, MMP-9, and N-Cadherin at T3 and T2 were significantly lower than those at T0 and T1 (P < 0.05). Increased peripheral blood TfR levels and reduced tumor cell ferroptosis were associated with higher cancer cell invasion and metastasis. A reduction in peripheral blood TfR levels is associated with the effectiveness of bladder cancer treatment. This reduction may decrease the invasiveness and migration ability of cancer cells by affecting the iron metabolism pathway. These findings may provide a basis for the development of new targeted therapeutic strategies to improve outcomes for patients with bladder cancer.
Similar content being viewed by others
Introduction
According to the Global Cancer Statistics 2022 released by the World Health Organization (WHO) and the International Agency for Research on Cancer (IARC), bladder cancer remains a significant global health challenge. In 2022, there were approximately 613,791 new cases of bladder cancer worldwide, accounting for 3.1% of all malignancies16. In China, bladder cancer is the 11th most common cancer overall, with an estimated 92,900 new cases in 2024 (73,200 in males and 19,700 in females). Notably, bladder cancer ranks 8th among all male malignancies in China, and its incidence has shown a persistent upward trend over the past decade1,2. Iron is an essential trace element for cell growth, playing a crucial role in DNA synthesis, cell division, and various metabolic pathways3,4,5. However, the abnormal regulation of iron metabolism is common in many types of cancer, including bladder cancer. This dysregulation may enhance the metastatic potential of tumor cells by promoting oxidative stress and affecting cell death pathways. Transferrin receptor (TfR) in peripheral blood is one of the key proteins regulating iron metabolism6,7,8. Located on the cell membrane, TfR mediates the intracellular uptake of the iron-transferrin complex, ensuring that tumor cells obtain sufficient iron to support their rapid proliferation needs.
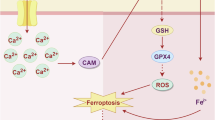
Studies have shown that the expression level of TfR is significantly elevated in many cancers, correlating with the malignancy, poor prognosis, and high recurrence rates of tumors9,10. In recent years, iron-dependent cell death (ferroptosis) has gained considerable attention as a novel programmed cell death mode11,12. Unlike traditional apoptosis, ferroptosis is induced by the accumulation of iron ions within cells and a surge in lipid peroxidation. In this process, GPX4 (glutathione peroxidase 4) and Ferroportin play crucial regulatory roles. GPX4 prevents lipid peroxidation, while Ferroportin controls intracellular iron levels by regulating iron ion flow inside and outside the cell. Ferroptosis, a novel form of cell death regulation associated with reactive oxygen species (ROS), is closely linked to iron accumulation and lipid peroxidation. Its biochemical mechanism differs from necrosis and apoptosis, exhibiting unique morphological features: cell volume shrinkage, increased mitochondrial membrane density with outer membrane rupture and reduced cristae, while nuclear morphology remains normal13. Diverse pathways can induce ferroptosis, including inhibition of cysteine uptake, inactivation of glutathione peroxidase 4 (GPX4), or chemical/mutational intervention on the cystine/glutamate antiporter. Ultimately, accumulated ROS exist as lipid peroxides. Notably, ROS accumulation correlates with iron chelators’ inhibitory effects on tumor cell apoptosis. Increased ROS accumulation can promote tumor cell death, while the addition of the iron chelator deferoxamine inhibits both ROS accumulation and tumor cell apoptosis. Other studies have confirmed ferroptosis’s ability to suppress tumor cell progression14. The molecular mechanism of ferroptosis primarily focuses on the generation and elimination of lipid peroxidation. Iron and polyunsaturated fatty acids serve as substrates for lipid peroxidation, driving ferroptosis, while GPX4 exerts inhibitory effects by utilizing reduced glutathione (GSH) as its substrate. Previous studies have explored the relationship between intracellular iron ion concentration and bladder tumor proliferation. Research shows that when transferrin binds iron, decreased free iron concentration in tumor cells promotes bladder cancer cell proliferation. Conversely, using gallium (Ga) to interfere with iron-transferrin binding increases intracellular free iron content, thereby inhibiting bladder tumor cell proliferation15.
Bladder cancer is a common tumor of the urinary system, presenting significant challenges in its treatment and management16,17,18. The prognosis of patients with bladder cancer is closely related to tumor invasion and metastasis19,20. Tumor invasion is not only associated with the degradation of the extracellular matrix but also with functional changes in cell adhesion molecules such as N-Cadherin and alterations in cell-to-cell interactions. Abnormal regulation of iron metabolism may play a critical role in these processes. Guo et al.21 pointed out that iron death is a new form of cell death with tumor suppressive effect, and iron death plays an important role in the pathogenesis, progression and incidence of ovarian cancer, so iron death is likely to become a key target for ovarian cancer treatment. Guan et al.22 pointed out that iron death was involved in the occurrence and development of gastric cancer. Xie et al.23 pointed out that ovarian cancer and breast cancer are closely related to iron death.
The purpose of this study is to explore the relationship between TfR in peripheral blood and ferroptosis, as well as the invasion and metastasis of bladder cancer cells. By evaluating the expression changes and functional status of TfR, GPX4, Ferroportin, and other related proteins, we aim to reveal the mechanism of action of these proteins in bladder cancer progression in the development of bladder cancer and assess their feasibility as potential therapeutic targets.
Materials and methods
General information
Fifteen patients with bladder cancer, treated in the urology department of our hospital from February 2022 to August 2023, were recruited for this study. The participants were aged between 44 and 68 years, with an average age of 52.57 ± 4.38 years. Of these, nine were male and six were female, all diagnosed by tissue biopsy and classified into stages 0-III. Informed consent was obtained from all patients before their inclusion in the study.
Admission criteria
-
Age range: 18–70 years.
-
Gender: Male or female.
-
Diagnosed with bladder cancer confirmed by pathological examination.
-
No other major diseases.
-
Adequate provision of clinical data and blood samples.
-
Signed informed consent form.
Exclusion criteria
-
Pregnant or lactating women.
-
Patients with hypertension, coronary heart disease, diabetes and other underlying diseases or suffering from other malignant tumors.
-
Patients with active infections.
-
Patients with incomplete clinical data.
-
Refusal to sign the informed consent form.
Treatment regimen
During the 9-month observation period (T0–T3), all patients received standardized combination therapy consisting of the GC chemotherapy regimen and immune checkpoint inhibitors, in accordance with the National Comprehensive Cancer Network (NCCN) guidelines for muscle-invasive bladder cancer. The GC regimen comprised gemcitabine (1000 mg/m2 administered via intravenous infusion on Days 1 and 8 of each cycle) and cisplatin (70 mg/m2 via intravenous infusion on Day 2). Each treatment cycle spanned 21 days, with a total of 3 cycles completed over 9 weeks. Cisplatin administration was preceded by a prehydration protocol of ≥ 1500 mL normal saline, and antiemetic prophylaxis (5-HT3 receptor antagonist plus dexamethasone) was routinely provided.
Concurrent immunotherapy was initiated based on baseline PD-L1 expression status assessed using the Ventana SP142 assay. Patients received one of three PD-1 inhibitors: toripalimab (240 mg), tislelizumab (200 mg), or pembrolizumab (200 mg), all administered intravenously every 3 weeks for 3 cycles. Supportive care measures included post-cisplatin renal protection (2000 mL/day hydration for 3 days), weekly complete blood count monitoring, and granulocyte colony-stimulating factor (G-CSF) administration for neutropenia (absolute neutrophil count < 1.5 × 109/L).
Dose modifications followed predefined criteria: gemcitabine was reduced by 25% for Grade 3 thrombocytopenia or neutropenia (CTCAE v5.0), cisplatin was withheld if creatinine clearance dropped below 60 mL/min (Cockcroft-Gault formula), and immunotherapy was permanently discontinued for Grade 3 immune-related adverse events. Treatment adherence data indicated that 13 of 15 patients completed all planned cycles, while 2 patients required cisplatin dose reductions due to Grade 2 nephrotoxicity. No treatment-related mortality occurred.
Post-treatment follow-up included serial CT urography at baseline, after 3 cycles, and every 3 months thereafter. Laboratory assessments (serum creatinine, electrolytes) were performed weekly during chemotherapy, and tumor response was evaluated using RECIST v1.1 criteria at T0, T3, T6, and T9 months. This protocol aimed to objectively assess the synergistic effects of combined chemoimmunotherapy on progression-free survival and recurrence risk reduction.
Medical ethics issues
The study was approved by the ethics committee of The First Hospital of Hebei Medical University (NO. 2022–10 A-03), and all patients signed informed consent prior to participation. The research team designed the study with the patient’s condition and prognosis in mind and decided to observe in cases where radical cystectomy was not appropriate to avoid unnecessary surgical risk to the patient.
Methods
ELISA detection of peripheral blood
Peripheral blood samples were collected at baseline (T0), 3 months (T1), 6 months (T2), and 9 months (T3) after treatment, with each sample volume ranging from 5 to 10 mL. The samples were centrifuged (3000 rpm, 10 min), and the plasma was transferred to sterile tubes and stored at − 80 °C until analysis. A specialized ELISA kit (The ELISA kit S0111B-96 produced by Junyan Biotechnology (Shanxi) Co., LTD has a detection range of 0.5-32ng/ml, and the r2 can reach 0.99 after 4-pl fitting of the relevant standard curve) was used for testing. The procedure included adding standards and samples to a 96-well plate, followed by detection antibody incubation for 1–2 h. After washing to remove unbound antibodies, a substrate solution was added and incubated for 20–30 min for color development. The reaction was terminated with a stop solution, and absorbance was read at 450 nm using an enzyme-labeled instrument. Protein concentrations were determined via software analysis. Each sample was repeated 3 times to ensure the reliability of the results.
MRI analysis of tumor volume
MRI imaging technology was employed to analyze tumor volume changes in bladder cancer patients at T0, T1, T2 and T3 time points, respectively. Patients were instructed to fast for 6 h prior to scanning to optimize image quality. MRI scans were conducted using 1.5–3 Tesla equipment, capturing transverse, sagittal, and coronal images of the bladder area. Techniques like Fast Spin Echo (FSE) and Volume Cross Acceleration (VIBE) were utilized to enhance tissue contrast. Conventional MR plain scan: The automatic echo parameters of T1WI were set as slice thickness and slice interval of 4 mm and 4 mm, tube voltage of 120 KV, TR/TE of 450 ms/8.5 ms, and matrix of 256 × 256. The T2WI scan was performed using the fastSE sequence, with TR/TE of 4800 ms/120 ms. The DMI-MRI sequence adopted single-shot echo planar imaging, with slice thickness and slice interval of 4 mm and 1.0 mm, voltage of 120 KV, TR/TE of 4000 ms/0.1 ms, and matrix of 512 × 512. Subsequently, GD-DTPA was injected for enhanced scanning, with TR/TE of 3.5 ms/1.5 ms and matrix of 256 × 256. The images were post-processed using MRI-specific software, and the three-dimensional dimensions of the tumor were measured to calculate the volume. After the examination, two experienced physicians analyzed the imaging data using a double-blind method. All radiologists evaluating the MRI images were blinded to the treatment group of the patients to reduce assessment bias.
Western blot analysis
Total proteins were extracted from blood samples using RIPA lysis buffer (Biotech) and Thermo Scientific Halt Protease Inhibitor Cocktail (Thermo Fisher Scientific). Protein extracts were separated by SDS-PAGE and electrophoresed. The immune complex was incubated with enzyme-labeled secondary antibodies and detected using a Western Blot detection kit (Biotech) and the Tanon-5200 system (Tanon, Shanghai, P.R. China). GAPDH was used as the standard for loading control to ensure the accuracy of the results. The quantification of protein imprinting band strength was performed using ImageJ software to ensure data repeatability.
Statistical analysis
The sample size was calculated using Cohen’s d method to ensure sufficient statistical power at α = 0.05, β = 0.80. All the data collected in this study were analyzed using SPSS 22.0 software (SPSS, Inc., Chicago, IL, USA). Statistical images were produced using Prism 9.0 software program (GraphPad software Inc., San Diego, CA, USA). The statistical significance of differences was assessed by a two-tailed Student’s t test or bidirectional ANOVA, and Bonferroni adjustments were used for all multiple comparisons. Pearson correlation coefficients were used to analyze the correlation between TfR, GPX4, Ferroportin levels, and tumor invasion and metastasis. Differences were considered statistically significant at P < 0.05.
Results
Comparison of general data of patients
The general data of the patients in this study revealed that the average age was 52.57 ± 4.38 years, with a mean BMI of 23.16 ± 2.51 kg/m2. Tumor staging among the patients varied: 3 cases were at stage 0, 5 cases at stage I, 4 cases at stage II, and 3 cases at stage III. Additionally, comorbid conditions included 2 cases of hypertension, 1 case of diabetes, 4 cases of smoking, and 3 cases of drinking. Detailed statistics are provided in Table 1.
Detection of TfR in peripheral blood
The levels of transferrin receptor (TfR) in peripheral blood of rats were repeatedly determined by ELISA. The results showed that with the progress of treatment, TfR levels decreased significantly, and compared with T1 and T0, T3 decreased by 29.26%, 32.88%, and T2 decreased by 16.24% and 20.53%, respectively (P < 0.05). (Table 2)
Detection of Iron death markers
The levels of iron death markers, including GPX4, Ferroportin, and Transferrin Receptor, were measured in the patients’ peripheral blood using ELISA. Treatment progress corresponded with a significant reduction in these markers at T3 and T2 relative to T1 and T0 (P < 0.05). These results are graphically represented in Fig. 1 and summarized in Table 3.
Detection of Iron death markers by ELISA. This figure illustrates the levels of iron death markers, specifically GPX4, Ferroportin, and Transferrin Receptor, measured in the peripheral blood of patients at four different time points (T0, T1, T2, T3) during treatment. The ELISA results show a significant reduction in these markers at T3 and T2 compared to T1 and T0 (P < 0.05), indicating a correlation between treatment progress and the decrease in iron death markers. *P < 0.05. **P < 0.01.
Tumor volume detection
Tumor volume and invasiveness were assessed using MRI at various time points (T0, T1, T2, T3). The data indicated that the tumor volume significantly decreased by T3 compared to T0, T1, and T2 (P < 0.05), as detailed in Table 4.
Western blot analysis
The protein expressions of MMP-2, MMP-9, and N-Cadherin were examined via Western blotting at different stages (T0, T1, T2, T3). The results indicated that the expression levels of these proteins were significantly lower at T3 and T2 compared to T0 and T1 (P < 0.05). Detailed results are provided in Fig. 2; Table 5.
Western blot analysis of MMP-2, MMP-9, and N-Cadherin This figure demonstrates the protein expression levels of MMP-2, MMP-9, and N-Cadherin at four different stages of treatment (T0, T1, T2, T3) as determined by Western blot analysis. The results reveal a significant decrease in the expression levels of these proteins at T3 and T2 compared to T0 and T1 (P < 0.05). *P < 0.05. **P < 0.01.
Pearson correlation analysis
Pearson correlation analysis was performed to explore the relationship between the levels of TfR, GPX4, Ferroportin, and Transferrin Receptor in peripheral blood and the invasion and metastasis markers of bladder cancer. The results showed that these peripheral blood proteins were positively correlated with MMP-2, MMP-9, and N-Cadherin (P < 0.05), indicating that higher levels of TfR and lower levels of iron death in tumor cells are associated with increased cancer cell invasion and metastasis (Table 6).
Discussion
Transferrin receptor (TfR) is a cell surface receptor responsible for the uptake of iron ions. As a fundamental nutrient, iron not only supports cellular life activities but also participates in DNA synthesis, an indispensable part of cell growth and division24,25. Under normal circumstances, intracellular iron levels are strictly regulated. However, in cancer states, this regulation is often disrupted. The expression of TfR increases in many types of cancer to meet the high iron demand of tumor cells. Nevertheless, excessive iron accumulation can promote the formation of reactive oxygen species (ROS), which can damage cell structures, including lipids, proteins, and DNA, leading to cell dysfunction and even death. Ferroptosis, a specific type of cell death driven by iron excess, is distinct from autophagy and apoptosis and is particularly dependent on the accumulation of lipid peroxidation26,27. In cancer treatment, inducing ferroptosis shows potential therapeutic value, as many cancer cells are particularly sensitive to this form of cell death28,29. By regulating the activity of TfR and related iron metabolism pathways, it may be possible to affect the survival state of tumor cells and thereby influence the development and metastasis of cancer. This study investigated the relationship between peripheral blood transferrin receptor protein (TfR) and the invasion and metastasis of bladder cancer, as well as ferroptosis of tumor cells.
The observed decrease in TfR levels with treatment time in this study is consistent with previous research, indicating that TfR levels can serve as potential biomarkers for evaluating treatment effects and tumor burden. In addition, studies have shown the role of voltage-gated ion channels in tumor cells, particularly in terms of iron uptake such as: Not only does iron compete with calcium to enter these cells, but iron uptake (similar to calcium uptake) is inhibited by Nimodipine, a specific L-type VGCC blocker, and enhanced in a dose-dependent manner by FPL 64,176, an L-VGCC activator30,31,32,33. As treatment progresses, especially in the late stages, a reduction in tumor burden is usually accompanied by a reduced iron demand, which is reflected in the downregulation of TfR levels. This change not only indicates decreased iron bioavailability but may also point to a slowdown in tumor cell proliferation rates34,35. Iron ions play a crucial role in tumor therapy, supporting basic metabolic activities and participating in key biochemical processes such as electron transfer and redox reactions. To maintain their proliferation needs, tumor cells often increase iron intake by upregulating TfR expression. Therefore, a decrease in TfR expression after effective treatment can usually be interpreted as a reduction in tumor cell proliferation ability due to treatment, thus affecting their iron demand. Excessive iron can increase cellular oxidative stress by promoting free radical formation and cause iron-dependent cell death through lipid peroxidation, differing from traditional ferroptosis. Promoting the transformation of tumor cells to ferroptosis by regulating iron metabolism pathways has become a new therapeutic strategy in cancer treatment. According to the study of Shi et al.36, the maximum diameter of superficial bladder cancer is 0.5–3.0 cm, and the average diameter is 1.6 cm. Transurethral plasma resection of bladder tumor combined with gemcitabine bladder infusion chemotherapy can reduce the level of tumor markers in patients and prevent the occurrence of adverse reactions. The study of Mu et al.37 pointed out that laparoscopic radical bladder cancer surgery can effectively clear the symptoms of bladder cancer patients and reduce the level of serum ferritin (SF) at the same time. However, surgery is a traumatic operation, and chemotherapy is associated with obvious side effects. In this study, effective treatment measures can effectively reduce tumor diameter, which is of great significance. By regulating iron metabolism pathway, tumor cells are promoted to iron death, especially for those tumor cells with strong resistance to traditional treatment methods. This treatment mode shows unique advantages, opening up new research directions and treatment ideas for the field of tumor treatment.
GPX4 (glutathione peroxidase 4) is an antioxidant enzyme that reduces lipid peroxides to their corresponding alcohols, thereby preventing lipid peroxidation chain reactions catalyzed by iron ions, which is one of the core pathways of ferroptosis38. Therefore, the downregulation of GPX4 can lead to the accumulation of lipid peroxides in tumor cells, increasing cell fragility and making them more prone to programmed cell death through ferroptosis. Ferroportin, the main export protein for cellular iron ions, plays a decisive role in maintaining intracellular iron ion balance. In cancer states, downregulation of Ferroportin expression can lead to iron ion accumulation in tumor cells, increasing the concentration of free iron39. Free iron, a strong oxidant, can catalyze the production of highly reactive hydroxyl radicals, further promoting lipid peroxidation and exacerbating ferroptosis. This change in the intracellular environment, caused by the expression changes of GPX4 and Ferroportin, not only increases the probability of ferroptosis but also significantly impacts tumor cell growth and survival. In fact, ferroptosis, as a non-apoptotic cell death mode, shows potential in targeted therapy for drug-resistant tumor cells.
MMP-2 and MMP-9 are enzymes that degrade the extracellular matrix (ECM), providing a pathway for tumor cells to physically cross the basement membrane and invade adjacent tissues40. Their expression and activity are usually increased in many cancers and are directly related to tumor invasion and metastasis. The activity of MMPs is regulated by tissue inhibitors (TIMPs), and an imbalance between MMPs and TIMPs leads to excessive ECM degradation, promoting tumor spread. Therefore, the decrease in MMP-2 and MMP-9 activities observed during treatment may reflect that effective treatment strategies can restore this balance and limit tumor cell invasion paths. N-Cadherin is a cell surface adhesion molecule involved in maintaining intercellular connections. In tumor biology, increased N-Cadherin expression is often associated with phenotypic transformation and enhanced migration ability of tumor cells, known as epithelial-mesenchymal transition (EMT)41. EMT enables tumor cells to acquire more mesenchymal characteristics, including enhanced migration and invasion42. Thus, the decrease in N-Cadherin expression due to treatment may indicate that tumor cells have lost part of their migration ability, potentially related to restored or strengthened intercellular adhesion, hindering collective migration and intercellular synergy.
Pearson correlation analysis revealed a positive correlation between TfR, GPX4, Ferroportin, and transferrin receptors in peripheral blood with proteins related to bladder cancer invasion and migration (MMP-2, MMP-9, and N-Cadherin). The increase in TfR correlates with increased expression of MMP-2 and MMP-9, key enzymes for ECM degradation, facilitating tumor cell invasion of adjacent tissues. Additionally, the upregulation of N-Cadherin as a cell adhesion molecule usually indicates enhanced tumor cell migration ability, further emphasizing the relationship between iron metabolism and tumor invasion. The antioxidant effect of GPX4 and the role of Ferroportin in regulating iron ion export directly affect intracellular iron balance and oxidative stress. In this study, changes in these two proteins positively correlated with changes in tumor invasion-related proteins, suggesting that the ferroptosis pathway may be related to the enhanced invasion ability of bladder cancer cells. This association reflects the complex interaction between iron metabolism and the migration and invasion abilities of tumor cells. These results suggest that changes in TfR, GPX4, Ferroportin, and transferrin receptor in peripheral blood not only reflect the increased iron demand by tumor cells but also reveal the potential relationship between these iron metabolism-related proteins and the invasion and migration abilities of bladder cancer. Iron is a potential regulator of the activity of MMP-2 and MMP-9. Iron produces reactive oxygen species (ROS) through Fenton reaction, activates signaling pathways such as MAPK and NF-κB, and then up-regulates the expression of MMP-2 and MMP-9, promoting tumor invasion. Under hypoxia conditions, HIF-1α can simultaneously up-regulate the expression of TfR, MMP-2 and MMP-9, forming a synergistic metastasis promoting effect43. Tfr-mediated iron uptake may activate the PI3K/AKT pathway, promote downstream mTOR signaling, and indirectly enhance transcription and secretion of MMP-2 and MMP-9. Iron overload may be activated by STAT3 phosphorylation to induce MMP-9 expression (especially in liver cancer and breast cancer)44,45.
Transferrin receptor (TFRC) regulates iron metabolism through autophagy in colorectal cancer. The study found that knockdown of ANXA10 inhibits autophagy-mediated TFRC degradation, leading to intracellular iron accumulation and triggering ferroptosis. This mechanism is specific to colorectal cancer. Ferroptosis induction is more dependent on the lipid peroxidation pathway46. For example, metal polyphenol nanocomposites synergistically generate reactive oxygen species (ROS) through sonodynamic therapy (SDT) and chemodynamic therapy (CDT), and deplete glutathione (GSH) to inhibit glutathione peroxidase 4 (GPX4). However, the expression of ferroptosis suppressor protein 1 (FSP1) in breast cancer may provide an additional resistance mechanism46. The regulation of iron metabolism is more involved in ferritinophagy and iron storage proteins such as ferritin heavy chain 1 (FTH1)47. For example, cytoglobin regulates ferroptosis by binding to transferrin receptor (TFR) and promoting ferritin degradation. This pathway may be replaced by other proteins in liver cancer. Resistance is closely related to the antioxidant pathway mediated by FSP1. FSP1 protects cell membranes from lipid peroxidation by reducing coenzyme Q10, thus resisting ferroptosis. The regulation of ferroptosis in colorectal cancer is more dependent on GPX4, while other cancers may resist ferroptosis through different mechanisms such as FSP1, ferritinophagy, or external ROS induction, suggesting that cancer type-specific regulatory networks need to be targeted differentially47. Among them, colorectal cancer needs to target GPX4, TFRC, and intestinal metabolites, while breast cancer, liver cancer, etc. need to be combined with nanotechnology or ferritinophagy interventions. These differences suggest that ferroptosis therapies need to be designed with specific protocols according to cancer types. At the same time, challenges brought about by drug resistance (such as B7H3-mediated cholesterol metabolism) and microenvironmental heterogeneity (such as hypoxia) need to be addressed48,49,50. Future research should further analyze the intersections and uniqueness of iron metabolism networks in different cancers, develop multimodal combination therapies, and explore more precise biomarkers to guide precision treatment.
There is a limitation of small sample size in this study, which may limit the universality of the results and lead to the bias of the research conclusions. Future studies should consider larger cohorts to validate the findings of this study. In addition, the integration of genetic biomarkers in cancer prognosis has significantly advanced through recent studies, exemplified by research on IGFBPs and MAPK signaling pathways in glioma. The 2023 bioinformatic study on IGFBPs demonstrated their critical diagnostic and prognostic value, where elevated IGFBP2 expression correlates with higher-grade gliomas and mesenchymal subtypes51. Similarly, the MAPK signaling pathway-based classification identified distinct glioma subtypes with machine-learning models predicting patient survival risks and highlighting key hub proteins like MAPK1/ERK2 as therapeutic targets52.
In summary, the results of this study show that the decrease in TfR levels in peripheral blood is associated with the effectiveness of bladder cancer treatment and may reduce the invasion and migration abilities of cancer cells by affecting iron metabolism. These findings may provide a basis for the development of new targeted therapeutic strategies to improve outcomes for patients with bladder cancer.
Data availability
The data and materials used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- ECM:
-
Extracellular matrix
- ELISA:
-
Enzyme-linked immunosorbent assay
- EMT:
-
Epithelial–mesenchymal transition
- FSE:
-
Fast spin echo
- GPX4:
-
Glutathione peroxidase 4
- ROS:
-
Reactive oxygen species
- TfR:
-
Transferrin receptor protein
- TIMPs:
-
Tissue inhibitors
- VIBE:
-
Volume cross acceleration
References
Portugal-Gaspar, F. et al. Giant cell carcinoma of the urinary bladder: clinicopathologic analysis and oncological outcomes. Virch. Arch. 485 (3), 535–546 (2024).
Seok, J., Kwak, Y., Kim, S., Kim, E. M. & Kim, A. Advances in liquid biopsy for diagnosis of bladder cancer. Int. Neurourol. J. 28 (2), 83–95 (2024).
Huang, Q. T., Hu, Q. Q., Wen, Z. F. & Li, Y. L. Iron oxide nanoparticles inhibit tumor growth by ferroptosis in diffuse large B-cell lymphoma. Am. J. Cancer Res. 13 (2), 498–508 (2023).
Song, C., Li, D., Zhang, J. & Zhao, X. Berberine hydrochloride alleviates Imatinib mesylate-induced cardiotoxicity through the Inhibition of Nrf2-dependent ferroptosis. Food Funct. 14 (2), 1087–1098 (2023).
Feng, Q. et al. Quercetin ameliorates diabetic kidney injury by inhibiting ferroptosis via activating Nrf2/HO-1 signaling pathway. Am. J. Chin. Med. 51 (4), 997–1018 (2023).
Yu, L. et al. Dysregulation of iron homeostasis by TfR-1 renders EZH2 wild type diffuse large B-cell lymphoma resistance to EZH2 Inhibition. Acta Pharmacol. Sin. 44 (10), 2113–2124 (2023).
Liu, S. et al. The gut microbiota metabolite glycochenodeoxycholate activates TFR-ACSL4-mediated ferroptosis to promote the development of environmental toxin-linked MAFLD. Free Radic. Biol. Med. 193 (Pt 1), 213–226 (2022).
Zhou, B. et al. Puerarin protects against sepsis-induced myocardial injury through AMPK-mediated ferroptosis signaling. Aging. 14 (8), 3617–3632 (2022).
Shen, H. & Zhai, L. Hepcidin regulates neuronal ferroptosis: A mechanism for postoperative cognitive dysfunction. J. Biochem. Mol. Toxicol. 36 (11), e23190 (2022).
Aschner, M. et al. Ferroptosis as a mechanism of non-ferrous metal toxicity. Arch. Toxicol. 96 (9), 2391–2417 (2022).
Shi, J. et al. Amelioration of white matter injury through mitigating ferroptosis following Hepcidin treatment after spinal cord injury. Mol. Neurobiol. 60 (6), 3365–3378 (2023).
Huang, S. et al. Hepatic TGFβr1 deficiency attenuates Lipopolysaccharide/D-Galactosamine-Induced acute liver failure through inhibiting GSK3β-Nrf2-Mediated hepatocyte apoptosis and ferroptosis. Cell. Mol. Gastroenterol. Hepatol. 13 (6), 1649–1672 (2022).
Lei, G., Zhuang, L. & Gan, B. The roles of ferroptosis in cancer: tumor suppression, tumor microenvironment, and therapeutic interventions. Cancer Cell. 42 (4), 513–534 (2024).
Liu, H. Expression and potential immune involvement of Cuproptosis in kidney renal clear cell carcinoma. Cancer Genet. 274–275, 21–25 (2023).
Chen, Z. et al. Integrating single-cell transcriptomics to reveal the ferroptosis regulators in the tumor microenvironment that contribute to bladder urothelial carcinoma progression and immunotherapy. Front. Immunol. 15, 1427124 (2024).
Shi, P. et al. Neutrophil-like cell membrane-coated SiRNA of LncRNA AABR07017145.1 therapy for cardiac hypertrophy via inhibiting ferroptosis of CMECs. Mol. Ther. Nucleic Acids. 27, 16–36 (2022).
Guan, S. et al. Preventive effects of lactoferrin on acute alcohol-induced liver injury via iron chelation and regulation of iron metabolism. J. Dairy Sci. 107 (8), 5316–5329 (2024).
Wang, W. et al. Knockdown of CXCL5 inhibits the invasion, metastasis and stemness of bladder cancer lung metastatic cells by downregulating CD44. Anti-cancer Drugs. 33 (1), e103–e112 (2022).
Hiromatsu, M., Toshida, K. & Itoh, S. Transferrin receptor is associated with sensitivity to ferroptosis inducers in hepatocellular carcinoma. Ann. Surg. Oncol. 30 (13), 8675–8689 (2023).
Harryman, W. L. & Marr, K. D. Cohesive cancer invasion of the biophysical barrier of smooth muscle. 40(1), 205–219 (2021).
Guo, K. et al. Ferroptosis: mechanism, immunotherapy and role in ovarian cancer. Front. Immunol. 15, 1410018 (2024).
Guan, X. et al. Blocking ubiquitin-specific protease 7 induces ferroptosis in gastric cancer via targeting Stearoyl-CoA desaturase. Adv. Sci. (Weinheim Baden-Wurttemberg Germany). 11 (18), e2307899 (2024).
Xie, X. et al. Targeting GPX4-mediated ferroptosis protection sensitizes BRCA1-deficient cancer cells to PARP inhibitors. Redox Biol. 76, 103350 (2024).
Li, H. et al. Quercetin inhibits neuronal pyroptosis and ferroptosis by modulating microglial M1/M2 polarization in atherosclerosis. J. Agric. Food Chem. 72 (21), 12156–12170 (2024).
Shi, X. et al. Ferroptosis is involved in passive Heymann nephritis in rats. Heliyon 9 (10), e21050 (2023).
Yang, X. et al. Polydopamine nanoparticles targeting ferroptosis mitigate intervertebral disc degeneration via reactive oxygen species depletion, Iron ions chelation, and GPX4 ubiquitination suppression. Adv. Sci. (Weinheim Baden-Wurttemberg Germany). 10 (13), e2207216 (2023).
He, Y. et al. SP2509 functions as a novel ferroptosis inhibitor by reducing intracellular iron level in vascular smooth muscle cells. Free Radic. Biol. Med. 219, 49–63 (2024).
Hao, H., Chen, H., Xie, L. & Liu, H. YKL-40 promotes invasion and metastasis of bladder cancer by regulating epithelial mesenchymal transition. Ann. Med. 53 (1), 1170–1178 (2021).
Chen, W. et al. ARHGAP6 inhibits bladder cancer cell viability, migration, and invasion via β-catenin signaling and enhances mitomycin C sensitivity. Hum. Cell. 36 (2), 786–797 (2023).
Liu, H., Weng, J., Huang, C. L. & Jackson, A. P. Voltage-gated sodium channels in cancers. Biomark. Res. 12 (1), 70 (2024).
Liu, H., Weng, J., Huang, C. L. & Jackson, A. P. Is the voltage-gated sodium channel β3 subunit (SCN3B) a biomarker for glioma? Funct. Integr. Genom. 24 (5), 162 (2024).
Liu, H., Dilger, J. P. & Lin, J. A pan-cancer-bioinformatic-based literature review of TRPM7 in cancers. Pharmacol. Ther. 240, 108302 (2022).
Gaasch, J. A., Geldenhuys, W. J., Lockman, P. R., Allen, D. D. & Van der Schyf, C. J. Voltage-gated calcium channels provide an alternate route for iron uptake in neuronal cell cultures. Neurochem Res. 32 (10), 1686–1693 (2007).
Ye, Y. et al. Quercetin alleviates deoxynivalenol-induced intestinal damage by suppressing inflammation and ferroptosis in mice. J. Agric. Food Chem. 71 (28), 10761–10772 (2023).
Kang, L., Piao, M., Liu, N., Gu, W. & Feng, C. Sevoflurane exposure induces neuronal cell ferroptosis initiated by increase of intracellular hydrogen peroxide in the developing brain via ER stress ATF3 activation. Mol. Neurobiol. 61 (4), 2313–2335 (2024).
Yang, S. & Liuhu, H. Clinical efficacy of transurethral plasma electroresection of bladder tumor combined with gemcitabine intravesical perfusion chemotherapy for superficial bladder cancer. Chin. J. Surg. Oncol. 16 (05), 475–479 (2024).
Jianjun, M. et al. Clinical efficacy of laparoscopic radical cystectomy and its influence on the levels of serum SF, SIL – 2R and TSGF in patients. Progr. Mod. Biomed. 17 (24), 4695–4698 (2017).
Xue, Q. et al. Copper-dependent autophagic degradation of GPX4 drives ferroptosis. 19(7), 1982–1996 (2023).
Xie, J. et al. Nox4-and Tf/TfR-mediated peroxidation and iron overload exacerbate neuronal ferroptosis after intracerebral hemorrhage: involvement of EAAT3 dysfunction. Free Radic. Biol. Med. 199, 67–80 (2023).
Chakrabarti, S. & Patel, K. D. Matrix metalloproteinase-2 (MMP-2) and MMP-9 in pulmonary pathology. Exp. Lung Res. 31 (6), 599–621 (2005).
Cao, Z. Q., Wang, Z. & Leng, P. Aberrant N-cadherin expression in cancer. Biomed. Pharmacother. Biomedecine Pharmacotherapie. 118, 109320 (2019).
Alnuaimi, A. R. et al. Emerging role of Caldesmon in cancer: A potential biomarker for colorectal cancer and other cancers. World J. Gastrointest. Oncol. 14 (9), 1637–1653 (2022).
Longhe, S., Jianguo, X., Chunhua, Q., Min, T. & Minglan, Q. Resveratrol inhibits the proliferation and migration of gastric cancer SGC – 7901 cells through the Pi3K/AKT pathway. Progr. Mod. Biomed. 16 (17), 3237–3240 (2016).
Liping, W. CLDN6 promotes the migration and invasion of liver cancer cells by activating the Src/STAT3 signaling pathway. Master’s thesis. (2022).
Zhihui, Z. Research on BMP9 inhibiting breast cancer by regulating the interaction between breast cancer cells and preadipocytes. Master’s Thesis. (2015).
Estêvão, D. et al. Iron metabolism in colorectal cancer: a balancing act. Cell. Oncol. (Dordr). 46 (6), 1545–1558 (2023).
Jin, H. et al. B7H3 increases ferroptosis resistance by inhibiting cholesterol metabolism in colorectal cancer. Cancer Sci. 114 (11), 4225–4236 (2023).
Wu, Y. C. et al. Targeting of FSP1 regulates iron homeostasis in drug-tolerant persister head and neck cancer cells via lipid-metabolism-driven ferroptosis. Aging (Albany NY). 16 (1), 627–647 (2024).
Huang, N. et al. Iron metabolism protein transferrin receptor 1 involves in cervical cancer progression by affecting gene expression and alternative splicing in HeLa cells. Genes Genom. 44 (6), 637–650 (2022).
Fan, C. et al. Cytoglobin augments ferroptosis through autophagic degradation of ferritin in colorectal cancer cells. Mol. Cell. Biochem. (2024).
Liu, H. & Tang, T. A bioinformatic study of IGFBPs in glioma regarding their diagnostic, prognostic, and therapeutic prediction value. Am. J. Transl. Res. 15 (3), 2140–2155 (2023).
Liu, H. & Tang, T. MAPK signaling pathway-based glioma subtypes, machine-learning risk model, and key hub proteins identification. Sci. Rep. 13 (1), 19055 (2023).
Funding
This study was supported by Medical Science Research Project of Hebei Province (No. 20240451).
Author information
Authors and Affiliations
Contributions
A.Z. and S.Z. contributed to the conception and design of the study; L.Z. and Z.X. performed the experiments; L.R., J.G. and H.C. collected and analyzed data; L.Z. and Z.X. wrote the manuscript; A.Z. and S.Z. revised the manuscript. All authors reviewed and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
This study protocol was in accordance with the Declaration of Helsinki of the World Medical Association. This study was approved by the Ethical Research Committee of the The First Hospital of Hebei Medical University. Prior to participation in the study, patients and their guardians provided informed consent, demonstrating their willingness to be included in the research.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhao, L., Xu, Z., Ren, L. et al. Investigating the relationship between peripheral blood transferrin receptor protein and tumor cell ferroptosis, invasion, and metastasis in bladder cancer. Sci Rep 15, 32197 (2025). https://doi.org/10.1038/s41598-025-12187-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-12187-0
Keywords
This article is cited by
-
The promising arsenal of ferroptosis inducers in bladder cancer
Journal of Molecular Medicine (2026)