Abstract
There is currently no consensus on the optimal treatment for femoral neck fractures in middle-aged and young adults. This research seeks to evaluate and compare the clinical efficacy of three different approaches: three cannulated screws (CS), a dynamic hip system combined with cannulated screws (DHS), and a new femoral neck system (FNS) in the management of these fractures. Seventy-eight middle-aged and young patients admitted for femoral neck fractures were divided into three groups based on the surgical procedure: CS, DHS, and FNS groups. The surgical time, incision length, intraoperative blood loss, number of fluoroscopies, Harris Hip Score and postoperative complications among the groups were compared. All patients were followed for 16 to 24 months, with an average follow-up duration of 18.42 ± 2.25 months. The operation times, intraoperative blood losses, the median and interquartile range for incision length, all showing significant differences. The median number of intraoperative X-ray fluoroscopies was 28 (8) for the CS group, 16 (6) for the DHS group, and 11 (7) for the FNS group, with significant differences between the CS group and both the DHS and FNS groups. The complication rates showed significant differences between the CS group and the other two groups. At the 3- and 6-month follow-ups, there were no statistically significant differences in Harris Hip scores among the three groups. However, at the final follow-up, the scores were 80.39 ± 6.81 (CS), 87.13 ± 3.43 (DHS), and 87.95 ± 3.58 (FNS), with the CS group showing significantly lower scores compared to the DHS and FNS groups, indicating a better overall outcome for the latter two. Treating young and middle-aged patients with femoral neck fractures using CCS, DHS, or FNS resulted in satisfactory clinical outcomes. In comparison to CCS, DHS and FNS reduced intraoperative fluoroscopy use, shortened surgery times, and minimized complications such as femoral neck shortening, nonunion, and femoral head necrosis. Furthermore, the FNS group had a smaller incision length and a shorter operation time than the DHS group.
Similar content being viewed by others
Introduction
Accounting for 3.6% of all fractures and 48% to 54% of hip fractures, femoral neck fractures are more common among the elderly. However, due to the rapid growth in the economy and transportation sectors, the incidence among middle-aged and young adults is on the rise, attributed to an increase in high-energy injuries. These fractures are often highly displaced and have vertical fracture lines, making them predominantly unstable. They pose a major challenge in orthopedic trauma care, with fracture reduction and internal fixation being the treatment of choice. Despite this, the rate of postoperative complications remains notably high1,2,3. It has been reported that the medial circumflex femoral artery and its supportive branches, which serve as essential blood supplies to the femoral head following femoral neck fractures, are prone to injury from high-energy trauma and during surgical intervention4, such damage can lead to severe postoperative complications, including fracture nonunion and avascular necrosis of the femoral head5. There is significant debate surrounding the surgical treatment of femoral neck fractures in young and middle-aged adults. Controversies include the optimal timing of surgery, methods of fracture reduction, selection of internal fixation devices, and techniques for fracture fixation. Regardless of the method employed, the objective of surgical treatment is to achieve anatomical reduction and secure fixation of the fracture, promoting swift postoperative recovery6,7. The commonly used internal fixation methods currently include cannulated compression screws (CCS), dynamic hip screws (DHS), compression plates, and the new compression locking plate system. However, each method has issues such as loosening of the internal fixation device, screw backout, and weak anti-rotation stability. Therefore, there is still debate about which internal fixation method is the best8,9. Numerous prior studies have systematically compared the biomechanical performance and clinical outcomes of CCS and dynamic hip screws DHS. While CCS is favored for its simplicity, minimal invasiveness, and cost-effectiveness, approximately one-third of patients experience complications such as screw back-out, rotational instability, and femoral neck shortening10,11,12,13. In contrast, DHS + CS offers improved resistance to these failure modes, albeit at the expense of a larger surgical incision and more extensive soft tissue dissection14,15. To integrate the benefits of minimally invasive surgery and angular stability, the femoral neck system (FNS) was introduced in 2018. Multiple finite element and biomechanical studies have demonstrated that FNS provides rotational and axial stability comparable to DHS and nearly twice the load-to-failure compared to CCS16,17,18,19. Recent retrospective case-control and prospective cohort studies have further suggested that FNS may reduce femoral neck shortening and early implant failure in the treatment of Pauwels type III fractures20,21,22,23. This study aims to comprehensively evaluate and compare the clinical efficacy, radiological outcomes, and complication rates associated with CCS, DHS, and the FNS in the treatment of femoral neck fractures among young and middle-aged individuals.
Method
Human ethics and consent to participate declarations
The research protocol was approved by The Jiujiang University Affiliated Hospital Ethics Committee, and The First Affiliated Hospital of Jinan University Ethics Committee. The clinical procedures adhered to the principles of the declaration of Helsinki. Written informed consent had been provided by the subjects (or their representatives) involved in this study.
A retrospective study was conducted on patients aged 20–65 who were admitted for femoral neck fractures between December 2017 and January 2021. Inclusion criteria included: (1) young and middle-aged patients (20–65 years), (2) unilateral, fresh, closed femoral neck fractures (classified by Garden and Pauwels), and (3) treatment using CS, DHS, or FNS. Exclusion criteria were: (1) pathological fractures, (2) patients with multiple traumas, (3) failure of closed reduction, and (4) other specific medical histories such as substance abuse or alcoholism. The 78 patients were categorized into CS, DHS, and FNS groups based on their surgical treatment, and comparisons were made regarding gender, age, fracture type, and cause of injury (Table 1).
Surgical technique
Patients underwent spinal epidural or general anesthesia, and all surgeries were performed by the same team of doctors. Patients were placed supine on an orthopedic traction bed, and after confirming adequate fracture reduction with a C-arm X-ray, the standard sterilization procedure was followed.
CS group
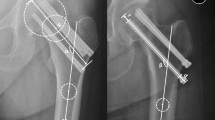
Under fluoroscopy, the first Kirschner wire (K-wire) was manually inserted, closely aligned with the femoral calcar on the anteroposterior view and centered along the femoral neck axis on the lateral view. The second K-wire was then inserted parallel to the first, positioned centrally in the femoral neck on the anteroposterior view and anteriorly on the lateral view. The third K-wire was inserted centrally on the anteroposterior view and posteriorly on the lateral view. A hollow drill was used along the K-wires to create screw paths, the depth was measured, and screws were inserted to ensure the threads crossed the fracture line. Finally, the skin was sutured. A representative case of CS group was showed in Figs. 1, 2.
Comparison of Surgery-related criteria among three groups. (A). operative time; (B). intra-op bleeding; (C). incision length; (D). intra-op fluoroscopy; (E). Harris hip score.
A 59-year-old male patient with a right femoral neck fracture is classified in the CS group. (a) Preoperative CT indicates a Garden type II right femoral neck fracture. (b,c) On the second day post-operation, anteroposterior and lateral X-rays show satisfactory fracture reduction. (d) Nineteen months post-operation, anteroposterior X-rays show fracture healing with femoral neck shortening and slight screw back-out (red arrow). (e) CT confirms the fracture healing. Due to partial pain symptoms caused by screw irritation, screws were removed, and the follow-up image is shown in (f).
DHS group
An incision was made on the proximal lateral femur, starting from the tip of the greater trochanter and extending distally for 8 cm. Skin, subcutaneous tissue, and deep fascia were incised, exposing the lateral side of the femur. At 3.5 cm below the greater trochanter, a 135° guide was used to position and insert the guide pin parallelly. A K-wire was inserted at the greater trochanter to prevent rotation. After confirming the position with C-arm fluoroscopy, the depth was measured, drilling and tapping were done, and a DHS main nail of appropriate length was inserted, followed by the placement of the side plate. The main nail cap was tightened, and screws were inserted through the plate holes after drilling and measuring the depth. A hollow screw was added above the main nail to prevent rotation. Fluoroscopy was used to confirm satisfactory fracture reduction and fixation, and the skin was sutured.A representative case of DHS group was showed in Fig. 3.
A 50-year-old female patient with a left femoral neck fracture is classified in the DHS group. (a) Preoperative CT indicates a Pauwels type III left femoral neck fracture. (b,c) On the second day post-operation, anteroposterior and lateral X-rays show satisfactory fracture reduction. (d) Thirteen months post-operation, anteroposterior X-rays show fracture healing with good internal fixation positioning. (e) CT confirms the fracture healing.
FNS group
A rotation-prevention pin was inserted parallel to the femoral neck axis. Under fluoroscopic guidance, a 4 cm skin incision was made, cutting through the skin to the subcutaneous tissue, fascia lata, and separating the lateral femoral muscle to expose the femur. Using a 130° guide, a second K-wire was inserted. Fluoroscopy confirmed the K-wire was centrally placed in the femoral neck, reaching the subchondral bone. The depth was measured, drilling was done, and the FNS plate and dynamic rod were inserted. Rotation-prevention and locking screws were then placed, followed by the removal of the rotation-prevention K-wire, and the incision was closed in layers.A representative case of FNS group was showed in Fig. 4.
A 55-year-old male patient with a right femoral neck fracture is classified in the FNS group. (a) Preoperative CT indicates a Pauwels type III right femoral neck fracture. (b,c) Postoperative anteroposterior and lateral X-rays show satisfactory fracture reduction. (d) Eighteen months post-operation, anteroposterior X-rays show fracture healing with femoral neck shortening and slight screw back-out (red arrow). CT confirms the fracture healing.
Postoperatively, antibiotics were administered for 24 h to prevent infection. After ruling out bleeding disorders, low molecular weight Heparin sodium was given for anticoagulation 12h post-surgery. Venous pumps were used to prevent thrombosis from the second postoperative day. Isometric muscle exercises and passive hip and knee joint movements were initiated on the second day. Patients were encouraged to gradually sit up beside the bed within the first week. Weight-bearing was avoided for the first three months, with decisions based on radiographic evaluations to determine the timing of weight-bearing and crutch discontinuation.
Assessment criteria
General patient information was recorded, and perioperative data were collected, including operative time, incision length, intraoperative blood loss, and number of intraoperative fluoroscopy scans. Imaging evaluations were performed using the Garden alignment index to assess the quality of fracture reduction (Grade 1: angulation < 160° in anteroposterior view and 180° in lateral view. Grade 2: angulation 155°−160° in anteroposterior view and 180° in lateral view. Grade 3: angulation 150°−155° in anteroposterior view or > 180° in lateral view. (If the lateral view angle is greater than 180°, it is at least Grade 3). Grade 4: angulation < 150° in anteroposterior view and > 180° in lateral view.). The Healing status of the femoral neck fracture and the occurrence of femoral Head necrosis were observed, and femoral neck shortening was measured. Clinical outcomes were evaluated using the Harris Hip Score system, and the rate of excellent and good outcomes was calculated, with scores of 90–100 considered excellent, 80–89 considered good, 70–79 considered fair, and < 70 considered poor.
Statistical analysis
Statistical analysis was performed using SPSS version 23.0 (IBM Corporation, Armonk, NY, USA). For continuous variables, the Shapiro-Wilk test was initially employed to assess normality. Among these variables, age, Harris Hip Scores at various time points, operative time, and intraoperative blood loss were normally distributed and presented as mean ± standard deviation (x ± s). Group comparisons were conducted using one-way analysis of variance (ANOVA). In contrast, intraoperative fluoroscopy scans and incision length did not follow a normal distribution and were described using the median (interquartile range). Group comparisons were made using the non-parametric Kruskal-Wallis H test. Categorical variables, such as gender, cause of injury, rate of excellent and good outcomes, and complications, were expressed as percentages (%) and analyzed using the chi-square (χ2) test. When theoretical frequencies were less than 1, Fisher’s exact test was applied. A significance level of P ≤ 0.05 was considered statistically significant, denoted as *, ** for P ≤ 0.01, and *** for P ≤ 0.001, while “ns” indicated non-significance (P > 0.05).
Result
Patients were followed up for 16 to 24 months postoperatively, with an average follow-up time of 18.42 ± 2.25 months. General data of the three groups of patients are presented in Table 1. The surgical durations for the three groups were 82.19 ± 10.20 min (CS), 61.09 ± 5.91 min (DHS), and 54.89 ± 4.84 min (FNS), with statistically significant differences observed among the groups (Fig. 1A). Intraoperative blood loss was recorded as 39.39 ± 6.33 ml (CS), 102.65 ± 12.09 ml (DHS), and 85.58 ± 14.93 ml (FNS), with statistically significant differences noted among the groups (Fig. 1B). Incision lengths and fluoroscopy counts were expressed as medians with interquartile ranges, with incision lengths of 3 (1) for the CS group, 8 (2) for the DHS group, and 5 (1) for the FNS group, showing statistically significant differences among the groups (Fig. 1C). Intraoperative X-ray fluoroscopy counts were reported as 28 (8) for CS, 16 (6) for DHS, and 11 (7) for FNS, with statistically significant differences observed between the CS group and both the DHS and FNS groups (Fig. 1D). At the 3-month and 6-month follow-ups, there were no statistically significant differences in Harris scores among the three groups. However, at the final follow-up, the scores were 80.39 ± 6.81 (CS), 87.13 ± 3.43 (DHS), and 87.95 ± 3.58 (FNS), with statistically significant differences observed between the CS group and both the DHS and FNS groups (Fig. 1E). The excellent rate of hip joint function at Fthe final follow-up was 55.56% for CS, 73.91% for DHS, and 73.68% for FNS. The excellent rate of CS was significantly different from that of both the DHS and FNS groups (Table 2). The rates of nonunion were 16.7% for CS, 8.7% for DHS, and 5.2% for FNS, with statistically significant differences observed between the CS group and both the DHS and FNS groups. The rates of femoral Head necrosis were 13.9% for CS, 8.7% for DHS, and 10.5% for FNS, with no statistically significant differences observed. The rates of femoral neck shortening were 38.9% for CS, 13.1% for DHS, and 26.3% for FNS, with statistically significant differences observed. The rates of screw cutout were 11.1% for CS, 4.3% for DHS, and 0% for FNS, with statistically significant differences noted in Table 2.
Discussion
While there is considerable literature on internal fixation treatment for mid-young femoral neck fractures, previous biomechanical experiments have demonstrated the mechanical characteristics of CCS, DHS, and FNS in stabilizing fractures24. To the best of my knowledge, there are few studies that compile the clinical efficacy of CCS, DHS, and FNS internal fixations together, which holds significant importance. Following the emergence of FNS, research on it has gradually increased. By employing a nail-in-nail combination, the stability against rotation and overall biomechanical performance have been enhanced. Unlike the rotational insertion of dynamic hip screws, the FNS rod is inserted via impact, thereby avoiding rotational torque-induced secondary rotation displacement of the femoral head. Stofel conducted a comparative study on the biomechanical performance of FNS, dynamic hip screws (DHS), and CS fixation in the treatment of Pauwels III femoral neck fractures. The results revealed that the mechanical stability of FNS was similar to DHS, with its load-bearing capacity being twice that of hollow screws and its rotational stability being 1.5 times that of hollow screws. Both FNS and DHS effectively controlled the collapse of the femoral neck fracture site, thus promoting fracture healing. For significantly displaced or unstable femoral neck fractures, both FNS and DHS internal fixations could provide robust mechanical stability to resist shear forces at the fracture site16. Schopper evaluated the biomechanical performance of FNS and the Hansson Pin system in treating Pauwels II fractures. The study demonstrated that FNS exhibited greater resistance to varus deformity compared to the Hansson Pin system. Additionally, FNS did not require highly specific implant positioning, as acceptable internal fixation positions could still provide robust resistance against shear and rotational forces25. The clinical outcomes in our study were consistent with previous findings, in which the use of cannulated screws required the placement of three screws in a parallel, inverted triangular configuration. Achieving this optimal spatial distribution often necessitated multiple adjustments to the guide wire trajectory, resulting in increased intraoperative fluoroscopy time and, consequently, higher radiation exposure for both patients and surgical staff. In our study, the median number of intraoperative fluoroscopies in the FNS group was 28 times for the CS group, 16 times for the DHS group, and as low as 11 times for the FNS group, showing a statistically significant difference. Despite the relatively short duration of FNS appearance and clinical application, it shares many similarities with the implantation method of DHS. One of the authors of this study had experience with dynamic hip screw surgeries, resulting in a short learning curve for FNS, thus not increasing the surgical duration. Regarding the surgical duration, our results confirmed the superiority of FNS. The average surgical duration was 82.19 ± 10.20 Min for the CS group, 61.09 ± 5.91 Min for the DHS group, and 54.89 ± 4.84 min for the FNS group. Although statistically significant differences existed, these disparities seemed to lack clinical relevance.
During the Healing process following internal fixation of femoral neck fractures, some patients experience femoral neck shortening. A study by Zlowodski reported that among femoral neck fracture patients treated with CCS, 34% exhibited no shortening or mild shortening, 36% had moderate shortening, and 30% experienced severe shortening26. Guy Romeo Kenmegne identified patients with femoral neck shortening if the difference between the relative contralateral sides was over 10mm. Among the FNS group, this criterion was met in 3 cases (5.35%), while in a comparative study of FNS and CS treatments for femoral neck fractures, 12 cases (20.68%) exhibited severe femoral neck shortening, with a higher prevalence observed in the CCS group compared to the FNS group27. Konrad Schuetze’s clinical study on the treatment of femoral neck fractures with FNS and DHS showed that the average shortening for DHS and FNS was (4.8 ± 2.1, 5.3 ± 1.9) respectively, with rates of shortening of 5 millimeters or more at (27.7%, 27.4%), but the difference was not statistically significant28. The overall incidence of femoral neck shortening in our cohort was 26.92%. Among them, the CS group had the highest rate at 38.9%, followed by the DHS group (13.1%) and the FNS group (26.3%). The differences among the three groups were significant, which aligns closely with findings in the literature. Combining biomechanical experiment results with our clinical research, it underscores the significant role of angular stability devices in resisting femoral neck shortening during the femoral neck healing process. However, whether femoral neck shortening leads to compromised hip joint function remains a matter of debate. Thomas Haider’s research suggests that femoral neck shortening following internal fixation of femoral neck fractures is relatively common in non-elderly patients. Nevertheless, despite this occurrence, the overall functional outcomes in the study population remain highly favorable, with a median Harris Hip Score of 96 points29. According to certain authors, even a 5 mm shortening may result in limping, and as the degree of shortening progresses, hip joint function deteriorates. Increasingly, research suggests that femoral neck shortening is associated with dysfunction in hip joint functionality30,31,32. Although Harris hip scores did not differ significantly among groups at 3 and 6 months postoperatively, statistically significant differences became evident at the 12-month follow-up. This delayed divergence appears to be associated with femoral neck shortening, particularly in the CCS group. Notably, screw backout secondary to femoral neck shortening during fracture healing may lead to irritation of surrounding muscles and fascia. This was clinically evident in several patients who required CCS removal due to soft tissue discomfort. In contrast, both DHS and FNS allow controlled sliding within designated channels, reducing the risk of soft tissue irritation and representing an additional advantage of these fixation systems.
Previous studies have shown that the nonunion rate for femoral neck fractures treated with three cannulated screws is as high as 19%, whereas traditional angular stable fixation devices, such as the DHS, have a nonunion rate of only 8%33,34,35. Recent studies have reported that the nonunion rate for femoral neck fractures treated with FNS ranges from 3.6% to 10%19,36. In our study, the CS group experienced 6 cases of nonunion, the DHS group had 2 cases, and the FNS group had 1 case, with a statistically significant difference in postoperative fracture nonunion among the three groups. The overall nonunion rate was 11.53%, which aligns with rates reported in other studies. Factors contributing to nonunion include fracture type, quality of reduction, choice of internal fixation, and timing of postoperative weight-bearing, some of which can be addressed through intervention37. Research has shown that the proper choice of internal fixation for different fracture types can markedly improve healing capabilities. Although CS has a long history of use in femoral neck fractures, it is becoming more challenged by fractures that involve high shear forces38. Furthermore, evidence suggests that the quality of fracture reduction is crucial for successful postoperative healing. Hence, surgical reduction should be meticulously performed following the Garden alignment index39. In cases where reduction is inadequate, open reduction should be promptly performed to achieve anatomical alignment and subsequent internal fixation. Anatomical reduction is essential for both restoring femoral Head blood supply and reestablishing the biomechanical properties of the femoral neck. Additionally, the timing of postoperative weight-bearing is a controllable factor. Studies have shown that following femoral neck fracture surgery, internal fixation supports only 25% of the stress, while the fracture itself bears the remaining 75%40. Even with non-weight-bearing use of crutches, the muscles required for maintaining body balance exert additional stress on the fracture site, thus increasing the risk of nonunion. For most patients, a healing period of at least three months is reasonable. Examining the causes of nonunion in our study, it was found that in the FNS and DHS groups, most cases were due to inadequate fracture reduction (one patient had an unsatisfactory Garden index) and premature weight-bearing. While strong mechanical stability enhances the biological environment for fracture Healing, it may also lead to premature weight-bearing by patients. In the CS group, the selection of high shear angle fixation in an inverted triangle pattern plays a crucial role. There were 12 cases of Pauwels type III fractures in the CS group, with three resulting in nonunion. Although the sample size is small, this is considered an important factor by the authors. Another major complication associated with femoral neck fractures is avascular necrosis of the femoral Head, with reported incidence rates ranging from 10% to 30%41,42. The overall incidence of avascular necrosis (AVN) of the femoral Head in our cohort was 11.39%. This included five cases in the CCS group, two cases in the DHS group, and two cases in the FNS group. Despite the differences in these numbers, the variation is not statistically significant. According to the literature, the risk of developing AVN can continue up to five years or longer after surgery43,44. Therefore, it is necessary to conduct a longer follow-up for this group of cases, with a particular focus on the occurrence of avascular necrosis of the femoral head in the future.
Despite our findings, this study has several limitations. It represents the experience of patients from a single institution, which may not be generalizable to other centers. Given our relatively small sample size, we plan to collect more cases in the future. Additionally, the follow-up period was not long enough, and we aim to report longer follow-up data to identify potential complications.
Conclusion
This study assessed the clinical efficacy of three internal fixation methods for closed reduction of subcapital femoral neck fractures in young and middle-aged patients. Results show that compared to CCS, DHS and FNS reduce intraoperative fluoroscopy, shorten surgery duration, and mitigate complications including femoral neck shortening, nonunion, and avascular necrosis. Notably, FNS exhibits a shorter incision length and operative time compared to DHS. FNS represents a promising new choice for young and middle-aged patients with femoral neck fractures.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Thorngren, K. G. et al. Epidemiology of femoral neck fractures. Injury 33 (Suppl 3), C1–7 (2002).
Florschutz, A. V. et al. Femoral neck fractures: current management. J. Orthop. Trauma. 29 (3), 121–129 (2015).
Ly, T. V. & Swiontkowski, M. F. Treatment of femoral neck fractures in young adults. J. Bone Joint Surg. Am. 90 (10), 2254–2266 (2008).
Gill, T. J. et al. Intraoperative assessment of femoral head vascularity after femoral neck fracture. J. Orthop. Trauma. 12 (7), 474–478 (1998).
KregorPJ The effect of femoral neck fractures on femoral head blood flow. Orthopedics 19 (12), 1031–1036 (1996). quiz 1037-8.
Medda, S., Snoap, T. & Carroll, E. A. Treatment of young femoral neck fractures. J. Orthop. Trauma. 33 (Suppl 1), S1–S6 (2019).
Hakim, G. & Volpin, G. Surgical treatment of femoral neck fractures in young adults. Isr. Med. Assoc. J. 17 (6), 380–382 (2015).
Chan, D. S. Femoral neck fractures in young patients: state of the Art. J. Orthop. Trauma. 33 (Suppl 1), S7–S11 (2019).
Estrada, Lance S., et al. "Fixation failure in femoral neck fractures." Clinical Orthopaedics and Related Research (1976-2007) 399 (2002): 110-118.
Bout, C. A., Cannegieter, D. M. & Juttmann, J. W. Percutaneous cannulated screw fixation of femoral neck fractures: the three point principle. Injury 28 (2), 135–139 (1997).
Baitner A C, Maurer S G, Hickey D G, et al. Vertical shear fractures of the femoral neck a biomechanical study[J]. Clinical Orthopaedics and Related Research®, 1999, 367: 300-305.
Ramadanov, N. et al. Factors that influence the complications and outcomes of femoral neck fractures treated by cannulated screw fixation. Sci. Rep. 10 (1), 758 (2020).
Jiang, X. et al. Biomechanical evaluation of different internal fixation methods based on finite element analysis for Pauwels type III femoral neck fracture. Injury 53 (10), 3115–3123 (2022).
Zhang, Y. L. et al. Osteonecrosis of the femoral head, nonunion and potential risk factors in Pauwels grade-3 femoral neck fractures: a retrospective cohort study. Med. (Baltim). 95 (24), e3706 (2016).
Razik, F. et al. Time to internal fixation of femoral neck fractures in patients under Sixty years—does this matter in the development of osteonecrosis of femoral head? Int. Orthop. 36 (10), 2127–2132 (2012).
Stoffel, K. et al. Biomechanical evaluation of the femoral neck system in unstable Pauwels III femoral neck fractures: a comparison with the dynamic hip screw and cannulated screws. J. Orthop. Trauma. 31 (3), 131–137 (2017).
Wang, K. et al. Fracture morphology and Biomechanical characteristics of Pauwels III femoral neck fractures in young adults. Injury 52 (11), 3227–3238 (2021).
Zeng, W., Liu, Y. & Hou, X. Biomechanical evaluation of internal fixation implants for femoral neck fractures: a comparative finite element analysis. Comput. Methods Programs Biomed. 196, 105714 (2020).
Teng, Y., Zhang, Y. & Guo, C. Finite element analysis of femoral neck system in the treatment of Pauwels type III femoral neck fracture. Med. (Baltim). 101 (28), e29450 (2022).
Fan, Z. et al. How to choose the suitable FNS specification in young patients with femoral neck fracture: A finite element analysis. Injury 52 (8), 2116–2125 (2021).
He, C. et al. Comparison of the clinical efficacy of a femoral neck system versus cannulated screws in the treatment of femoral neck fracture in young adults. BMC Musculoskelet. Disord. 22 (1), 994 (2021).
Wang, G. et al. Minimally invasive open reduction combined with proximal femoral Hollow locking plate in the treatment of Pauwels type III femoral neck fracture. J. Int. Med. Res. 47 (7), 3050–3060 (2019).
Zhou, Y. et al. Femoral neck system vs. cannulated screws on treating femoral neck fracture: a meta-analysis and system review. Front. Surg. 10, 1224559 (2023).
Sun X, Han Z, Cao D, et al. Finite Element Analysis of Six Internal Fixations in the Treatment of Pauwels Type III Femoral Neck Fracture[J]. Orthopaedic Surgery, 2024, 16(7): 1695-1709.
Schopper, C. et al. Higher stability and more predictive fixation with the femoral neck system versus Hansson pins in femoral neck fractures Pauwels II. J. Orthop. Translat. 24, 88–95 (2020).
Zlowodzki, M. et al. Femoral neck shortening after fracture fixation with multiple cancellous screws: incidence and effect on function. J. Trauma. 64 (1), 163–169 (2008).
Kenmegne, G. R. et al. Femoral neck fractures in non-geriatric patients: femoral neck system versus cannulated cancellous screw. BMC Musculoskelet. Disord. 24 (1), 70 (2023).
Schuetze, K. et al. Is new always better: comparison of the femoral neck system and the dynamic hip screw in the treatment of femoral neck fractures. Arch. Orthop. Trauma. Surg. 143 (6), 3155–3161 (2023).
Haider, T. et al. Femoral shortening does not impair functional outcome after internal fixation of femoral neck fractures in non-geriatric patients. Arch. Orthop. Trauma. Surg. 138 (11), 1511–1517 (2018).
Felton, J. et al. Femoral neck shortening after hip fracture fixation is associated with inferior hip function: results from the FAITH trial. J. Orthop. Trauma. 33 (10), 487–496 (2019).
Zlowodzki, M. et al. The effect of shortening and varus collapse of the femoral neck on function after fixation of intracapsular fracture of the hip: a multi-centre cohort study. J. Bone Joint Surg. Br. 90 (11), 1487–1494 (2008).
Stockton, D. J. et al. Incidence, magnitude, and predictors of shortening in young femoral neck fractures. J. Orthop. Trauma. 29 (9), e293–e298 (2015).
Samsami, S. et al. Comparison of three fixation methods for femoral neck fracture in young adults: experimental and numerical investigations. J. Med. Biol. Eng. 35 (5), 566–579 (2015).
Xu, X. et al. Comparison of femoral neck system to multiple cancellous screws and dynamic hip screws in the treatment of femoral neck fractures. Injury 54 (Suppl 2), S28–S35 (2023).
Cai, L. et al. Comparison of young femoral neck fractures treated by femoral neck system, multiple cancellous screws and dynamic hip screws: a retrospectively comparison study. BMC Musculoskelet. Disord. 25 (1), 188 (2024).
Hu, H. et al. Clinical outcome of femoral neck system versus cannulated compression screws for fixation of femoral neck fracture in younger patients. J. Orthop. Surg. Res. 16 (1), 370 (2021).
Raaymakers, E. L. & Marti, R. K. Nonunion of the femoral neck: possibilities and limitations of the various treatment modalities. Indian J. Orthop. 42 (1), 13–21 (2008).
Zhang, R. Y. et al. Biomechanical research of three parallel cannulated compression screws in oblique triangle configuration for fixation of femoral neck unstable fractures. Orthop. Surg. 16 (4), 953–964 (2024).
Cong, B., Han, Z. & Zhang, H. Exploring the displacement characteristics of garden III femoral neck fractures and the reliability, validity, and value of the anteroposterior garden index in assessing displacement severity. J. Orthop. Surg. Res. 18 (1), 797 (2023).
Wang, G. et al. A quantitative Biomechanical study of positive buttress techniques for femoral neck fractures: a finite element analysis. Chin. Med. J. (Engl). 132 (21), 2588–2593 (2019).
Bachiller F G C, Caballer A P, Portal L F. Avascular necrosis of the femoral head after femoral neck fracture[J]. Clinical Orthopaedics and Related Research®, 2002, 399: 87-109.
Min, B. W. & Kim, S. J. Avascular necrosis of the femoral head after osteosynthesis of femoral neck fracture. Orthopedics 34 (5), 349 (2011).
LUCIE R S, FULLER S, BURDICK D C, et al. Early prediction of avascular necrosis of the femoral head following femoral neck fractures[J]. Clinical Orthopaedics and Related Research (1976-2007), 1981, 161: 207-214.
Ehlinger, M. et al. Early prediction of femoral head avascular necrosis following neck fracture. Orthop. Traumatol. Surg. Res. 97 (1), 79–88 (2011).
Funding
This work was supported by Science and Technology Projects in Guangzhou (No. 2024A04J4323), Science and Technology Program of Health Commission of Jiangxi Province (No. 202311519), Science and Technology Research Project of Education Department of Jiangxi Province (GJJ190926), Key Research and Development Plan of Jiujiang (S2022ZDYFN337), Dongguan Science and Technology of Social Development Program (No. 20231800939902), Guangdong Basic and Applied Basic Research Foundation (No. 2022A1515140171) and Medical Joint Fund of Jinan University (No. YXJC2022011).
Author information
Authors and Affiliations
Contributions
Haiwu Wan, Liang Chen, Guoliang Chen and Kai Sun designed and supervised the experiments. Guoliang Chen and Kai Sun acquired fundings. Kai Sun, Gang Xu and Jianjun Liu acquired analyzed the data. Kai Sun and Gang Xu wrote the draft of the manuscript.Haiwu Wan revised the manuscript. All authors read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Human ethics and consent to participate declarations
The research protocol was approved by the Jiujiang University Affiliated Hospital Ethics Committee, and The First Affiliated Hospital of Jinan University Ethics Committee. The clinical procedures adhered to the principles of the declaration of Helsinki. Written informed consent had been provided by the subjects (or their representatives) involved in this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Sun, K., Xu, G., Liu, J. et al. FNS as a more satisfactory surgical option for young and middle-aged patients with femoral neck fractures. Sci Rep 15, 35998 (2025). https://doi.org/10.1038/s41598-025-19883-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-19883-x