Abstract
This study aimed to investigate the prevalence of daytime sleepiness and to identify its influencing factors among nursing students. A total of 1658 nursing students from 8 schools in 5 regions of China were selected. SPSS26.0 software was used for univariate and binary Logistic analysis to identify the influencing factors of sleepiness between nursing days. 299 (18.03%) Nursing students had daytime sleepiness and Internet addiction (OR = 4.401, 95% CI 3.166 to 6.117), Drinking (OR = 1.603, 95% CI 1.093 to 2.350), Clinical practice (OR = 1.991, 95% CI 1.521 to 2.607), and Psychosomatic illness (OR = 2.970, 95% CI 1.360 to 6.486) had statistical significance (all P < 0.05). The incidence of excessive daytime sleepiness is relatively high. Internet addiction, Drinking, Clinical practice, and Psychosomatic illness are the factors that affect excessive daytime sleepiness. Therefore, early identification of high-risk groups of excessive daytime sleepiness by clinical nursing educators and clinical nursing managers can provide a reference for nursing educators to take targeted preventive measures.
Similar content being viewed by others
Introduction
Excessive daytime sleepiness (EDS) refers to uncontrollable sleepiness during the day, which is temporary sleepiness or sleep that is difficult to maintain or cannot be contained while staying awake and can occur at any time and in any setting1,2. Studies have reported that the incidence of EDS in the general population is about 12–16%2, while the incidence of EDS in college students is about 24–39%3,4, and the incidence of EDS in medical students is 24–54%1,2,3,4,5. EDS can lead to inattention, decreased academic performance, negative emotions (anxiety, depression), and reduced life satisfaction 6,7,8,9. In addition, some studies have found that the occurrence of EDS has a particular relationship with drug abuse, criminal behaviour, and self-injury suicide9,10,11. Nurses are an indispensable force in medical and health care, playing a key role in protecting lives, preventing diseases, treating diseases and promoting health. Nursing students are the future nursing professionals, and the professional level of nursing students directly affects the patient’s medical experience and treatment effect.
Some studies have found that nursing students’ lifestyle factors, behaviors, daily commitments and sleep habits can lead to daytime sleepiness, seriously affecting their academic and professional performance12. The occurrence of daytime sleepiness will affect the cognitive function of nursing students and affect the nursing work of patients13,14,15. Therefore, it is essential to identify the factors that influence EDS in nursing students as early as possible and reduce its occurrence. This study aimed to (1) determine the prevalence of EDS among nursing students, (2) examine the association between internet addiction and EDS, and (3) explore coping strategies for affected students.
Methods
Design
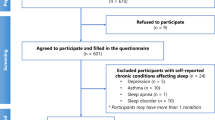
A multicenter cross-sectional study was conducted among nursing students from eight universities across Shandong, Jiangxi, Shanghai, Guangdong and Liaoning provinces between August and September 2024. The electronic questionnaire was distributed through nursing teachers. The first page of the questionnaire contained a detailed informed consent statement explaining the study purpose, procedures, confidentiality measures, and participants’ rights. Explicit consent was obtained digitally before participants could access the survey questions; those who declined consent were automatically directed to a termination page. The study was approved by the hospital’s research ethics committee [Peking University Shenzhen Hospital Ethics Committee Approval No. 2022–094], and all procedures adhered to the principles of the Declaration of Helsinki. From the initial 1710 responses collected, 52 were excluded due to incomplete responses or inconsistent answer patterns, resulting in 1658 valid responses.
Measures
General information questionnaire
Gender, Age, Educational level, Clinical practice, Family situation, Monthly household income, Father’s educational level, Mother’s educational level, Recent hospitalization etc.
Internet addiction
The Internet Addiction Scale was compiled by Yeong (1999) of the University of Pittsburgh16. It has been widely used to measure Internet addiction17. The scale consists of 20 items, each with five choices (almost none–always), assigned a score of 1–5. It includes four dimensions: network damage, compulsive symptoms, network relationship addiction, and the influence of destructive emotions. The subjects’ Internet use was determined according to the scale’s total score. The higher the score, the more serious the degree of addiction to the internet. The score of 20–49 was everyday Internet use, and the score of 50–100 was internet addiction. Previous studies have shown that this scale has good reliability and validity in college students18,19. In this study, the Cronbach’s α for the sample was 0.949.
Epworth sleepiness scale (ESS)
The Epworth Sleepiness Scale translated and revised by Peng Lili et al. was adopted to evaluate the daytime sleepiness of college students20. The scale consisted of 8 items and was scored with 4 points, 0 indicating “never dozing off” and 3 indicating “often dozing off”. The total score ranged from 0 to 24 points. The higher the score, the more serious the degree of daytime sleepiness. A total score of ≥ 11 indicates excessive daytime sleepiness. Previous studies have shown that this scale has good reliability and validity in college students15. In this study, the Cronbach’s α coefficient of this scale was 0.877.
Statistical analysis
Data analysis was conducted using SPSS 26.0 statistical software. Counting data were presented as the number of cases and percentage, and inter-group comparisons were performed using the Chi-square test. Measurement data were expressed as Mean ± standard deviation or [M(Q1, Q3)], and inter-group comparisons were carried out using the t-test or non-parametric test of two independent samples. A binary logistics regression model was employed to assess the impact of different factors on EDS, with variable screening conducted using a stepwise backward method. A significance level of P ≤ 0.05 was considered statistically significant.
Results
General information of nursing students
This study investigated 1658 nursing students, including 367 male and 1291 female students. 299 (18.03%) nursing students had EDS, and 1359 (81.97%) did not. There were statistically significant differences between non-Excessive Daytime Sleepiness and Excessive Daytime Sleepiness nursing students in terms of Educational level, Clinical practice, Drinking, Psychosomatic illness, and Internet addiction (P < 0.05), as shown in Table 1.
Multifactor analysis of EDS in nursing students
In univariate analysis, statistically significant indicators such as Education level, Drinking, and Physical and mental illness, and Internet addiction were taken as independent variables. EDS of nursing students was taken as the dependent variable and binary Logistic regression analysis was conducted. The results showed that Clinical practice, Internet addiction, Drinking, and Physical and mental illness were the influencing factors for sleepiness between nursing days (P < 0.05), as shown in Table 2.
Discussion
Incidence of ESD
The results of this study found that the incidence of EDS among nursing students was 18.03% (299/1658), which was similar to the results of Demirde’s survey on nursing students (17.9%)21. It is higher than the EDS survey results of Chinese scholar Wang Zhan on college students in a university in Jiangsu (15.7%)22. Nursing is a major that has strong theory and practice. Compared with college students in other majors, nursing students need to take examinations of clinical practice, skill operation and theoretical knowledge, which leads to a heavier learning burden and decreased sleep quality, leading to EDS. Lack of sleep will reduce learning efficiency, cognitive impairment, and adverse effects on individuals’ physical and mental health23,24. Therefore, early identification of EDS and timely support and help to nursing students are of great significance in preventing EDS and reducing adverse events caused by EDS.
Internet addiction and drinking
Internet addiction is an influential factor of EDS in nursing students. Research shows that Internet addiction is a positive correlation factor for insomnia, and the higher the degree of Internet addiction, the higher the risk of insomnia25. Foreign studies have shown that among adolescents with Internet addiction, 26.7–69.4% of them have sleep disorders of varying degrees26,27. About 75% of students have experienced dizziness, fatigue, neurasthenia, depression, anxiety and other symptoms caused by Internet addiction, leading to the occurrence of EDS28. Therefore, for nursing students with Internet addiction, it is essential to guide them to rebuild a healthy lifestyle and sleep habits, including limiting Internet use time, establishing a regular sleep schedule, avoiding the use of electronic devices before going to bed, and actively coping with the adverse effects of Internet addiction. Alcohol consumption is a risk factor for daytime sleepiness among nursing students, and the results of this study are consistent with those of previous studies1,29,30. Alcohol use disrupts the balance of the central nervous system and endocrine system and affects the quality of sleep31. In addition, alcohol can disrupt the body’s sleep rhythm system, causing the body clock to be confused, making you feel sleepy and sleepy during the day. Therefore, schools and families should pay more attention to nursing students who drink alcohol, provide personalized measures for alcohol abstinence, reduce the number of nursing students who drink alcohol, improve their sleep quality and improve the occurrence of EDS.
Clinical practice and psychosomatic illness
This study showed that clinical practice was a risk factor for EDS in nursing students.
Research has found that due to factors such as long-term and frequent night shifts, highly tense and high-workload working environments, nurses’ sleep disorders are exacerbated32. After shift work, they are unable to quickly return to a normal sleep–wake cycle, which in turn leads to daytime sleepiness. Clinical internship is a crucial stage for the combination of medical theory and practice, and it is also an inevitable process for student nurses to gradually transform into professional nurses33. Nursing interns often need to study clinical knowledge for a long time and at a high intensity. They also have to follow clinical instructors on night shifts and endure the clinical practice pressure such as night shifts and high-intensity working environments. All these factors can bring psychological pressure to nursing interns, which in turn affects their sleep quality34. In addition, nursing students are faced with three shifts in clinical practice. When their circadian rhythm changes are out of sync with the natural circadian rhythm, it will lead to circadian rhythm disturbance, which will have an impact on individual sleep quality and EDS to a certain extent35. Studies have shown that the incidence of depression and anxiety among nursing students is 54.7% and 28.9%36. Anxiety and depression are common physical and mental diseases among nursing students. Among depressed students, the incidence of EDS is as high as 50.4%37. EDS is closely associated with anxiety and depression among nursing students. As a common symptom of both sleep disorders and depressive conditions, EDS contributes to reduced positive affect, motivation, and concentration. It further promotes negative cognitive patterns—such as rumination and pessimism—which are core features of depression38,39. Additionally, EDS can exacerbate nighttime sleep difficulties, including increased insomnia, and heighten the likelihood of daytime napping, thereby further disrupting the sleep–wake cycle. The underlying psychological mechanism linking EDS to depressive symptoms involves reduced physiological arousal, wherein depressive states lower overall alertness levels, resulting in increased daytime sleepiness38,39,40. According to the study of foreign scholar BOZ41, EDS during rehabilitation is more likely to occur, and EDS may be a residual symptom after recovery from depression. Therefore, nursing educators should not ignore nursing students suffering from physical and mental diseases, especially those with depression, increase communication, provide good sleep conditions, pay attention to the sleeping conditions of nursing students, reduce the occurrence of EDS, and guide students to seek help from psychiatric professionals when necessary.
Conclusion
This study investigated the incidence of daytime sleepiness and its influencing factors in 1658 nursing students. The study found that the incidence of EDS was higher among nursing students, and the main influencing factors included Internet addiction, drinking, psychosomatic diseases and clinical practice. These factors affect students’ learning and quality of life and may also negatively affect their future career performance as nursing students. The findings underscore the importance of integrating sleep health and psychological support into nursing education; consequently, we suggest that schools and relevant departments take effective measures—such as providing sleep health education, psychological counselling, and optimized curriculum arrangements—to improve students’ sleep status and overall health.
Strengths and limitations
Although our study conducted an extensive sample survey and provided essential insights into EDS among nursing students, some limitations cannot be ignored. First, the study’s cross-sectional design cannot determine causality, and future studies can use a longitudinal design to explore further the dynamic relationship between various factors and daytime sleepiness. Second, the data mainly rely on self-reports; there may be recall bias and social expectation bias; future research can be combined with objective measurement methods (such as sleep monitoring equipment) to improve the accuracy of the data. In addition, the sample did not cover all regions of China, which may limit the universality of the results. Future studies should expand the sample scope to include more institutions and areas to improve the study’s external validity. Finally, other potential influencing factors (such as eating habits, exercise frequency, caffeine intake and screen time before bed. etc.) were not fully considered in the study, and more variables can be included in future studies to analyze the influencing factors of nursing students’ EDS comprehensively.
Data availability
The data sets analyzed in this study are available from the authors of this study upon reasonable request.
References
Shen, Y. et al. Excessive daytime sleepiness in medical students of Hunan Province: Prevalence, correlates, and its relationship with suicidal behaviors. J. Affect. Disord. 255, 90–95 (2019).
el Hangouche, A. J. et al. Relationship between poor quality sleep, excessive daytime sleepiness and low academic performance in medical students. Adv. Med. Educ. Pract. 9, 631–638 (2018).
Chung, K. F. & Cheung, M. M. Sleep-wake patterns and sleep disturbance among Hong Kong Chinese adolescents. Sleep 31(2), 185–194 (2008).
Rodrigues, R. N. D. et al. Daytime sleepiness and academic performance in medical students. Arq. Neuropsiquiatr. 60, 6–11 (2002).
Dutra da Silva, R. C. et al. Prevalence and factors associated with excessive and severe daytime sleepiness among healthcare university students in the Brazilian Midwest. J. Sleep Res. 31(3), e13524 (2022).
Rhie, S., Lee, S. & Chae, K. Y. Sleep patterns and school performance of Korean adolescents assessed using a Korean version of the pediatric daytime sleepiness scale. Korean J. Pediatr. 54(1), 29–35 (2011).
Owens, J. Insufficient sleep in adolescents and young adults: An update on causes and consequences. Pediatrics 134(3), e921-932 (2014).
Raine, A. & Venables, P. H. Adolescent daytime sleepiness as a risk factor for adult crime. J. Child Psychol. Psychiatry 58(6), 728–735 (2017).
Hansen, S. L., Capener, D. & Daly, C. Adolescent sleepiness: Causes and consequences. Pediatr. Ann. 46(9), e340–e344 (2017).
Jiahao, H., Yingying, Z. & Shaoqian, L. Relationship among daytime sleepiness, bedtime procrastination and sleep quality in college students. Chin. Mental Health J. 37(12), 1065–1070 (2023).
Liu, X. et al. Daytime sleepiness predicts future suicidal behavior: A longitudinal study of adolescents. Sleep 42(2), zsy225 (2019).
Blome, M. J. et al. Sleep quality and daytime sleepiness in prelicensure baccalaureate nursing students. J. Nurs. Educ. 60(4), 196–202 (2021).
Demir, G. Daytime sleepiness and related factors in nursing students. Nurse Educ. Today 59, 21–25 (2017).
Alhamed, A. A. The link among academic stress, sleep disturbances, depressive symptoms, academic performance, and the moderating role of resourcefulness in health professions students during COVID-19 pandemic. J. Prof. Nurs. 46, 83–91 (2023).
Huang, C. F. et al. Determinants of daytime sleepiness in first-year nursing students: A questionnaire survey. Nurse Educ. Today 34(6), 1048–1053 (2014).
Young, K. et al. Cyber disorders: The mental health concern for the new millennium. Cyberpsychol. Behav. 2(5), 475–479 (1999).
Lee, J. Y. et al. Relationship between problematic Internet use and post-traumatic stress disorder symptoms among students following the Sewol ferry disaster in South Korea. Psychiatry Investig. 14(6), 871–875 (2017).
Song, Y. et al. Incidence and risk factors of depressive symptoms in Chinese College Students. Neuropsychiatr. Dis. Treat. 16, 2449–2457 (2020).
Wang, W. et al. Associations among screen time, sleep duration and depressive symptoms among Chinese adolescents. J. Affect. Disord. 284, 69–74 (2021).
Li-Li, P. E. N. G. et al. Reliability and validity of the simplified Chinese version of Epworth sleepiness scale. Chin. J. Otorhinolaryngol. Head Neck Surg. 46(1), 44–49 (2011).
Demir, G., Arslan, S. & Kocoglu-Tanyer, D. Daytime sleepiness in University Students and Internet addiction as the determinant. J. Addict. Nurs. 31(3), 153–160 (2020).
Zhan, W. et al. Cross-sectional study on current status of sleep quality and associated factors among college students in Jiangsu. Chin. J. Sch. Health 35(07), 1025–1027 (2014).
Biddle, D. J. et al. Insomnia symptoms and short sleep duration predict trajectory of mental health symptoms. Sleep Med. 54, 53–61 (2019).
Liu, R. T. et al. Sleep and suicide: A systematic review and meta-analysis of longitudinal studies. Clin. Psychol. Rev. 81, 101895 (2020).
Wenping, J. et al. Association of depressive symptoms, Internet addiction and insomnia among medical students in Anhui Province. Chin. J. Sch. Health 44(08), 1174–1177 (2023).
Zhang, M. W. B. et al. Internet addiction and sleep quality among Vietnamese youths. Asian J. Psychiatr. 28, 15–20 (2017).
Wolniczak, I. et al. Association between Facebook dependence and poor sleep quality: A study in a sample of undergraduate students in Peru. PLoS ONE 8(3), e59087 (2013).
Juan, R. Internet addiction and sleep quality among adolescents: Mediating effects of depression and moderating effects of social support. 2023. Anhui Medical University.
Mei, S. et al. Excessive daytime sleepiness and related factors in medical students. Chin. Ment. Health J. 37(06), 458–463 (2023).
Joo, S. et al. Prevalence and correlates of excessive daytime sleepiness in high school students in Korea. Psychiatry Clin. Neurosci. 59(4), 433–440 (2005).
Ziyin, H. et al. Sleep quality and its influencing factors in senior high school students. Chin. J. Sch. Health 43(01), 108–111 (2022).
Arbour, M. et al. Factors that contribute to excessive sleepiness in midwives practicing in the United States. J. Midwifery Womens Health. 64(2), 179–185 (2019).
Xiaodan, W. et al. A multilevel model analysis of intervention effect of sleep quality of nursing interns. J. Nurs. (China) 23(07), 73–76 (2016).
Min, Z. et al. Research progress of sleep quality in medical trainees. Occup. Health. 34(21), 3023–3025 (2018).
Golombek, D. A. et al. The times they’re a-changing: Effects of circadian desynchronization on physiology and disease. J. Physiol. Paris 107(4), 310–322 (2013).
Juan, G. et al. A typical correlation analysis of anxiety, depression and professional adaptability in 799 undergraduate nursing students. J. Nurs. (China). 27(02), 70–73 (2020).
Hein, M. et al. Prevalence and risk factors of excessive daytime sleepiness in major depression: A study with 703 individuals referred for polysomnography. J. Affect. Disord. 243, 23–32 (2019).
Ma, Y. B. et al. Mediating and moderating effects of experiential avoidance between excessive daytime sleepiness and anxiety symptoms. J. Affect. Disord. 391, 120065 (2025).
Biscarini, F. et al. Co-occurrence of anxiety and depressive symptoms, suicidal thoughts, and hopelessness in patients with narcolepsy type 1. Sleep Med. 124, 141–145 (2024).
Varallo, G. et al. Navigating narcolepsy: Exploring coping strategies and their association with quality of life in patients with narcolepsy type 1. Sci. Rep. 14(1), 11837 (2024).
Boz, S. et al. Risk of excessive daytime sleepiness associated to major depression in adolescents. Psychiatr. Q. 92(4), 1473–1488 (2021).
Funding
The study is funded by General Program for Clinical Research at Peking University Shenzhen Hospital (LCYJ2021015), Shenzhen Science and Technology Project (JCYJ20240813115912017), Shenzhen Key Medical Discipline Construction Fund (No. SZXK056), Sanming Project of Medicine in Shenzhen (No. SZSM202111013).
Author information
Authors and Affiliations
Contributions
Lingyu Hou 12345, Guangli Qin 2345, Chengyuan He123, Xuan Zhang124, Shuyuan Ouyang 125, Linlin Lu12345. 1. Conceptualization; 2. Methodology; 3. Data curation; 4. Writing—Original Draft; 5. Writing—Review and Editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
Patients/participants provided written informed consent to participate in the study. We confirm that all the experiment is in accordance with the relevant guidelines and regulations such as the declaration of Helsinki.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Hou, L., Qin, G., He, C. et al. Excessive daytime sleepiness and associated factors among nursing students in China: a large-scale, multicenter, cross-sectional study. Sci Rep 15, 40431 (2025). https://doi.org/10.1038/s41598-025-22434-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-22434-z