Abstract
Cervical white light imaging (CWLI) plays a key role in diagnosing and managing cervical intraepithelial neoplasia (CIN) but is limited by uneven illumination, low contrast, and specular reflections. Cervical image visualization and improvement (CIVI) is designed to improve contrast and uniform brightness while maintaining the histological accuracy of colposcopic images to clearly identify tissue differences. CIVI combines multiple image enhancement techniques, including specular reflection removal, illumination correction, and local contrast enhancement, in a unified framework. This technique was validated on 52 histologically confirmed CWLI images (CIN 1–3). We performed a Local Binary Pattern (LBP) analysis to extract cervical epithelial texture features and quantified blood contrast using the Michelson contrast (MC). A qualitative assessment was conducted by five expert colposcopists using a four-level scale. The mean LBP distance between lesion and normal tissue showed a marked increase from 0.192 to 0.391. The mean MC for blood area and surrounding tissue improved from 0.216 to 0.290. Experts observed an improvement in image quality for all CIN grades, with an average score increase of + 0.71. These initial experimental results demonstrate the potential of the proposed framework to enhance the visualization of CIN, support better treatment decisions, and enable more personalized care.
Similar content being viewed by others
Introduction
Cervical cancer is still a common cancer among women worldwide. However, it is highly preventable with early detection and treatment through regular screening programs1. Current screening methods, such as cytology (Pap smear), high-risk human papillomavirus (hrHPV) testing, and colposcopy, are very important for finding cervical intraepithelial neoplasia (CIN), carcinoma in situ, and early-stage invasive cervical cancer2,3,4. Among these, colposcopy offers an accurate way to diagnose abnormalities, guide biopsy, define treatment protocols, and monitor after treatment.
Colposcopy is a diagnostic procedure using a white lighted source and magnifying instrument to examine the cervix, vagina, and vulva. It allows macroscopic evaluation of cervical morphology, identification of the transformation zone, and finding of visible lesions. During cervical colposcopy, visual inspection with acetic acid (VIA) or Lugol’s iodine (VILI) staining helps to better detect cervical premalignant lesions and guides targeted biopsies. Colposcopy provides real-time visualization of cervical lesions, improving the precision of loop electrosurgical excision procedures, and is also important for evaluating treatment response. Although colposcopy plays a fundamental role in preventing cervical cancer, it has limitations in image quality, which can affect diagnostic accuracy. These limitations, such as uneven illumination, specular reflections, poor tissue contrast, and a loss of structural details–especially in flat, pale, or obscured lesions–can reduce the accuracy of visual inspection during identification, treatment, and follow-up5,6,7,8,9. Several methods and techniques based on traditional computer vision and deep learning have been developed to address these issues. Common algorithms like contrast-limited adaptive histogram equalization (CLAHE) improve local contrast in low-visibility lesions10; Retinex-based illumination correction enhances brightness uniformity11,12; guided filtering supports structure-preserving smoothing12,13; and inpainting techniques are used to reduce specular reflections by filling in missing parts14,15. Each method contributes to improved image quality, but uniform integration of all into clinical practice has yet to be achieved. Recently, AI has the potential to enhance diagnostic precision and lesion classification; however, in clinical practice, the role of the clinician remains crucial in the assessment, sampling, and treatment planning process16,17,18,19,20.
Biopsy-based histopathology remains the gold standard for confirming CIN and assigning a lesion grade. While advancements in AI and image processing have improved lesion detection and preliminary classification, there are still critical clinical demands for improved image quality to assist in identifying lesion characteristics. This is especially important for defining lesion boundaries, color gradations, epithelial texture, and vascular morphology. Similarly, gastrointestinal endoscopy has successfully integrated specialized enhancement technologies, such as Texture and Color Enhancement Imaging (TXI), which significantly improves lesion recognition compared to standard white light21,22,23.
To solve this problem, we propose cervical image visualization and improvement (CIVI), an integrated enhancement pipeline designed specifically for cervical white light imaging (CWLI). Unlike separate processing methods, CIVI combines multiple image enhancement techniques in a unified framework to enhance overall performance and enable more comprehensive image analysis. This framework includes specular reflection removal using HSV-based inpainting, multi-scale Retinex with color restoration (MSRCR) for illumination correction, selective gamma correction for dark base regions, and CLAHE for local contrast enhancement. This pipeline is designed to enhance images in a single step, improving contrast and uniform brightness while maintaining histological accuracy. To evaluate its practical use, CIVI was applied to a dataset of 52 CWLI images from patients with histologically confirmed CIN1–3 lesions. For quantitative evaluation, we used Local Binary Pattern (LBP) analysis to extract texture features of the cervical epithelium and quantified blood-vessel contrast using the Michelson contrast (MC). Additionally, five expert colposcopists performed a qualitative assessment using a four-level standardized image quality scale. Results showed a significant improvement in both technical metrics and expert evaluations, suggesting the potential clinical benefit of CIVI in CIN management. In the future, we will focus on integrating CIVI into real-time colposcopic workflows and performing validation studies on an expanded dataset.
Materials and methods
Colposcopy is instrumental in the diagnosis and treatment of precancerous lesions and carcinoma in situ of the cervix using modalities such as conization and electrocautery. White light colposcopy enables the physician to visualize the cervix to assess color, the condition of the epithelial surface, and to identify visible lesions, facilitating the determination of the location of the squamocolumnar junction and the transition zone, which are critical areas for identifying these lesions. This section presents the CIVI algorithm and the definitions of quantitative evaluation metrics for colposcopy image analysis. All steps in CIVI are designed to closely match the characteristics of CWLI to address the image recognition problem. Compared to conventional approaches, the CIVI framework constitutes an advanced integration of modern enhancement techniques and processing strategies specifically optimized for colposcopic imaging.
CIVI algorithm for cervical image enhancement
The CIVI algorithm aims to enhance white-light colposcopic images. It is specifically optimized for specular reflection removal, correcting non-uniform illumination, detail enhancement, and creating more defined lesion boundaries. The flowchart of CIVI in Fig. 1 illustrates the five main steps of the enhancement process. A detailed description of this method is provided in Supplementary_Code_CIVI, which also includes the MATLAB scripts implementing the algorithm.
Overall flowchart of CIVI.
Step 1: Specular reflection detection and inpainting. The input RGB image is converted to the HSV color space. A preliminary binary mask is generated by thresholding pixels with high brightness (Value channel) relative to the image’s mean and standard deviation, and low saturation. This mask is then combined with the output of Canny edge detection on the Value channel using a logical OR operation. Subsequently, morphological hole filling, median filtering, and dilation are applied to create the final specular mask. The specular regions are inpainted using a region-based interpolation method (roifill)24.
Step 2: Illumination correction via MSRCR. The standard MSRCR color restoration function was modified by replacing the pixel-wise denominator with a channel mean, which stabilized the computation under uneven illumination and preserving natural clinical tissue colors25,26. To maintain chromatic balance, we apply a modified color restoration function, formulated as Eq. (1).
where Ic denotes the pixel intensity of channel c ∈ {R, G, B}, µc is the mean intensity of that channel, and α, β, and gain are empirically determined parameters. The resulting output is decomposed into a base layer and a detail layer. The parameters were determined through a systematic experimental procedure, combining both visual assessment and quantitative analysis. For MSRCR, we refer to the classic Gaussian multiscale configuration, and fine-tuned it to fit the colposcopy images, resulting in σ = [20, 80, 200], α = 100, β = 40, gain = 1.225. The same parameter set was applied uniformly, and chromatic balancing was completed before decomposing the output into base and detail layers.
Step 3a: Base layer adjustment. To enhance visibility and improve visual quality under poor lighting conditions, we apply gamma correction with a fixed exponent of γ = 0.4 to the dark regions of the base layer (Ibase < 0.1) (Eq. (2)). This adjusts the details in underexposed areas while maintaining the image’s overall balance. The base layer after apply gamma correction I’base is expressed as Eq. (2):
Step 3b: Detail layer enhancement. To emphasize diagnostically significant structures, such as blood vessels and lesion boundaries, CLAHE was applied to each channel of the detail layer. The parameters were set to Clip = 0.002 and Tiles = 20 × 20, chosen experimentally in accordance with previous studies that combined MSRCR and CLAHE for image enhancement27. These values were fixed throughout the experiments, as they provided the best balance between brightness, contrast, and naturalness of the enhanced images.
Step 4: Image recombination. The corrected base layer and the enhanced detail layer were recombined via element-wise multiplication. The result was then subjected to guided filtering and intensity clipping to obtain the final image for clinical interpretation.
Image acquisition and algorithm evaluation
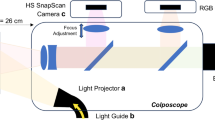
In clinical practice, all colposcopies and guided biopsies were performed using a standard Leisegang colposcope, ensuring ethical standards in biomedical research. To support algorithm development, we also used a custom-designed electronic colposcope developed by Ho Chi Minh City University of Technology, equipped with a CMOS sensor (1920 × 1080 px), a cree white LED light source (Cree XLamp XP-G2, China), non-polarized mode, image acquisition by HDMI, VGA AverMedia Darkcrystal Capture CD311 (Taiwan) video capture card, allowing users to capture video content in the medical field28. During the image processing and evaluation, we focused on the cervical region (usually circle with diameter of 25–30 mm), so the images were cropped to 1440 × 1080 pixels. The device was used for research-related image acquisition only and did not interfere with diagnostic or therapeutic procedures.
Ethics statement
Informed consent was obtained from all subjects participating in this study. The study protocol was approved by the Institutional Evaluation Council of Vietnam National University, Ho Chi Minh City (Ref. No. 1009/DHQG-KHCN). All methods were performed in accordance with the Declaration of Helsinki and relevant institutional guidelines and regulations.
From the validated dataset, a subset of 52 high-quality CWLI images, corresponding to histopathologically confirmed CIN grades 1–3 lesions, was selected for the development and evaluation of the CIVI algorithm (Table 1).
ROI selection for quantitative analysis: (a) CWLI image showing lesion (white squares) and normal mucosa (yellow squares), (b) Reference image after acetic acid application confirming ROI positions.
To evaluate the diagnostic effectiveness of the CIVI enhancement algorithm, we implemented a standardized region of interest (ROI) selection and comparison protocol (Fig. 2). The CWLI images were taken before application of the solution. Then, the acid-stained images were taken after approximately 60 s. These stained images are used by experts to determine the ROI (normal and lesion areas) on the original CWLI images for further analysis. For each image, eight square ROIs (50 × 50 pixels) were manually: four within the CIN-confirmed lesion area and four within adjacent regions of visually normal mucosa. As illustrated in Fig. 2(a), ROI placement was performed on the CWLI image and then cross-validated using the corresponding acetic acid-stained reference image (Fig. 2(b)) to ensure accurate distinction between abnormal and normal tissue. The ROI size corresponds to approximately 2–3 mm² on the cervical surface, which was chosen to balance lesion localization precision with noise suppression. For this study, a total of 52 image sets were used for texture feature analysis (ROI: 50 × 50), and 44 image sets were used for blood/vessel contrast evaluation (ROI: 10 × 10). The performance of CIVI was assessed using two quantitative metrics: (1) texture distance, evaluated via LBP analysis, and (2) blood contrast, measured with the MC.
Texture distance via LBP
We quantified the texture differentiation between lesion and normal regions using the LBP operator, computed over a circular 8-neighbor, radius-1 neighborhood. After converting each ROI to grayscale, a normalized LBP histogram was constructed. The Euclidean distance between the histograms of each lesion–normal ROI pair was then calculated as the LBP-based texture distance (Eq. (3)).
where Hlesion, i and Hnormal, i denote the normalized LBP histograms of the lesion and normal ROIs, respectively. Here, Di represents the LBP-based texture distance for pair i. A larger Di indicates greater distinction between lesion and normal tissues.
Blood contrast via Michelson contrast
For ROI pairs with visible blood vessels or bleeding regions, contrast was computed in grayscale using the Michelson formula (Eq. (4)):
Where Iblood and Ibackground represent the average grayscale intensity values within the blood vessel (or bleeding) regions and their adjacent normal ROIs, respectively.
Stepwise processing in CIVI pipeline: (a) CWLI image, (b) Specular removed, (c) illumination corrected (MSRCR), (d) Gamma on base layer, (e) CLAHE on detail layer, and (f) CIVI image.
Figure 3 shows the workflow of the CIVI algorithm through five main stages. Figure 3(a) shows the original image of cervix captured under white light (CWLI), which typically contains specular reflections and low contrast between tissue regions. In the first step, the algorithm uses a detection-and-filling method to effectively remove high-intensity reflections (Fig. 3(b)). Next, global illumination normalization is applied using MSRCR (Fig. 3(c)), which balances the overall brightness. Then, these two layers (base layer and detail layer) are processed separately: selective gamma correction is applied to the base layer to brighten dark regions without causing over-saturation (Fig. 3(d)), while local CLAHE is applied to the detail layer to enhance local contrast and highlight textural features (Fig. 3(e)). Finally, the two layers are recombined to produce the final image, which has improved sharpness, uniform brightness, and preserved detail (Fig. 3(f)).
Expert image quality scoring
To assess the effectiveness of the CIVI algorithm in observing CIN lesion characteristics on CWLI and CIVI images, an image evaluation test was performed by five colposcopists (three experts and two trainees). Each expert assessed a randomized set of 104 images (52 original CWLI and 52 corresponding CIVI images). The colposcopists scored the lesions using a 4-point visibility scale, while being blinded to the histopathological diagnosis for each case. The evaluation criteria included epithelial surface characteristics, color, vascular patterns, and lesion boundaries. Visibility scores were defined as follows: 1 – Poor (Lesions are hardly detectable even with repeated, careful observation); 2 – Fair (Lesions are difficult to recognize without focused observation); 3 – Good (Lesions can be detected but require careful attention); and 4 – Excellent (Lesions are easily recognized without effort, with clear and detailed visualization).
In addition to CIVI, we established an independent comparison branch by applying the Contrast Limited Adaptive Histogram Equalization (CLAHE) algorithm to the lightness (L) channel of the color images12,21,29. The CLAHE image set, along with the CWLI and CIVI images, was included in the qualitative assessment conducted by colposcopy experts.
Statistical analysis
To evaluate the effect of the CIVI algorithm, we applied several non-parametric statistical tests. The Wilcoxon signed-rank test was used to compare paired measurements (CWLI vs. CIVI) for each image, testing whether CIVI significantly improved LBP distance or Michelson contrast. The Kruskal–Wallis test was applied to compare these quantitative indices among different CIN categories (CIN1, CIN2, CIN3), to evaluate whether the degree of lesion severity influenced the improvement. For the expert visual-quality scores, paired t-tests were used to compare imaging modes (CWLI vs. CIVI; and CWLI vs. CLAHE where applicable) on the subject-level differences. All tests were two-sided; p < 0.01 was considered statistically significant.
Results
Qualitative improvement of lesion visibility
Comparison of image processing methods for cervical image enhancement: (a) CWLI image, (b) CIVI image, (c) CLAHE image, (d) grayscale histogram. Black arrows indicate lesion boundaries, blue stars mark areas of abnormal red epithelium, yellow arrows denote the position of the intrauterine device, and white arrows highlight specular reflections.
A CIN 2 case is presented to compare cervical image enhancement methods. In the original CWLI image (Fig. 4(a)), the lesion occupies most of the cervical surface, surrounding the external os. The irregular, dark-red epithelium and scattered specular reflections present within the lesion obscure boundary definition and surface details. The intrauterine device and cervical os are visible, but blood vessels remain difficult to assess due to glare and low contrast. The CIVI-enhanced image (Fig. 4(b)) shows substantial improvement: lesion boundaries are clearer, surface structures more defined, and specular highlights effectively removed. The epithelial color is more balanced, creating better contrast between abnormal and normal tissue. The CLAHE image (Fig. 4(c)) was obtained by applying the CLAHE algorithm to the lightness (L) channel of a color image. This image shows a strong improvement in contrast, highlighting both bright and dark areas. However, it exhibits significant color shifts, which can result in poor visual quality and make the image appear less natural. The grayscale histogram (Fig. 4(d)) provides a quantitative analysis supporting these visual observations. The CWLI histogram has many sharp fluctuations. The CIVI histogram is much smoother, more spread out, and tends to be shifted to the right, while still retaining the characteristic shape of the original image. The CIVI histogram drops off sharply beyond gray level 240, which corresponds to the successful suppression of specular reflections. The CLAHE histogram (green) exhibits an unnatural redistribution of brightness. This demonstrates that the CIVI algorithm successfully improves local brightness and contrast without destroying the original histological features.
Expert evaluations of 52 CWLI images confirmed consistent improvements in visual quality following CIVI enhancement. On average, post-processing scores increased by 0.71 points compared to the original images, with Δ1 gains of 0.62 ± 0.12 (CIN 1), 0.71 ± 0.09 (CIN 2), and 0.78 ± 0.12 (CIN 3) (p < 0.001). Notably, the degree of improvement correlated with lesion severity, highlighting CIVI’s superior performance in enhancing visualization of high-grade lesions. In contrast, CLAHE processing reduced image quality across all CIN subgroups, as reflected by negative Δ2 values. The small standard error of the mean (SEM) values, particularly for CIVI, indicate strong expert in colposcopy agreement (Table 2). These findings demonstrate CIVI’s potential to outperform conventional enhancement techniques in cervical imaging.
Texture distance improvement via LBP analysis
Representative CWLI images of CIN 1–3 before (a–c) and after CIVI images (d–f).
Figure 5 presents three representative pairs of CIN images from the dataset, corresponding to different grades of CIN 1–3. In the CIN 1 case, a mild specular reflection is present in the original image (Fig. 5(a)), but the enhanced image (Fig. 5(d)) successfully removes this glare. For the CIN 2 case, the original image shows a lesion encircling the external os with scattered specular reflections (Fig. 5(b)), while the CIVI-enhanced image successfully reduces these reflections, restores surface detail, and improves the contrast between lesion and adjacent healthy tissue (Fig. 5(e)). For the CIN 3 case, a severe lesion with an irregular surface occupies most of the cervix. In the original image (Fig. 5(c)), reflections along the raised mucosal areas obscure the blood vessels. In contrast, the enhanced version suppresses these reflections and highlights the lesion borders, blood vessels, and improves the ability to differentiate between normal and lesion areas (Fig. 5(f)). It shows that the algorithm improves visibility by reducing specular reflections and making morphological features, such as abnormal epithelial structures, borders, and blood vessels, more visible.
(a) LBP distance: CWLI vs. CIVI. (b) LBP distance by CIN grade. LBP distance ranges from 0 to 1, where 0 indicates no textural difference between lesion and non-lesion ROIs, and 1 indicates maximal difference.
The LBP distance between the lesion and adjacent normal mucosa was calculated for both the CWLI and CIVI images from 52 cases. The mean LBP distance between lesion and normal ROI increased from 0.192 ± 0.064 (CWLI) to 0.391 ± 0.127 (CIVI). The difference was statistically significant (Wilcoxon signed-rank test, p = 2.8 × 10–7), demonstrating that the algorithm enhanced the visibility of CIN lesion surface features (Fig. 6(a)). To analyze whether the texture enhancement was related to the severity of CIN, the LBP values of CIVI images were compared among CIN grades 1–3 using the Kruskal–Wallis test. No statistically significant difference was found (p = 0.732), showing that the increase in LBP on CIVI images does not correlate with the severity of CIN grades 1–3 (Fig. 6(b)).
Blood contrast enhancement via MC analysis
(a–b) A case with visible blood vessels: (a) CWLI image (MC = 0.17); (b) CIVI image (MC = 0.21); (c–d) A case with cervical bleeding: (c) CWLI image (MC = 0.26), and (d) CIVI image (MC = 0.34).
Figure 7 illustrates the effect of the CIVI algorithm on enhancing blood vessels and bleeding contrast in CWLI images. In a case with visible cervical blood vessels (CIN 3), the CIVI algorithm provided a clearer visualization of fine vascular structures compared to CWLI. It was also highly effective at reducing specular reflection, which highlighted vessel contours more distinctly against the surrounding epithelium (Fig. 7(a–b)). In a case of cervical bleeding, CIVI enhanced the visibility of bleeding regions by reducing background glare, restoring brightness uniformity, and improving the contrast between blood and adjacent tissue (Fig. 7(c–d)). These examples demonstrate the algorithm’s ability to improve diagnostic visualization in both blood vessel and bleeding cases.
Among the 52 cases included in this study, 44 showed clearly visible blood vessels or bleeding areas. In these cases, Michelson contrast was used to quantify the luminance difference between the regions of interest and the background in both CWLI and CIVI images. The mean contrast was higher in CIVI images (0.290 ± 0.116) compared to CWLI images (0.216 ± 0.105), and this difference was highly statistically significant (Wilcoxon signed-rank test, p = 0.00008) (Fig. 8(a)). This confirms that the CIVI algorithm enhances contrast and visibility in specific regions of interest, while preserving overall image quality. To analyze whether the blood contrast was related to the severity of CIN, the MC of CIVI images were compared among CIN grades 1–3 using the Kruskal–Wallis test. No statistically significant difference was found (p = 0.141), showing that the increase in MC on CIVI images does not correlate with the severity of CIN grades 1–3 (Fig. 8(b)).
(a) Michelson contrast: CWLI vs. CIVI, and (b) Michelson contrast by CIN grade. Michelson contrast ranges from 0 to 1, where 0 indicates no contrast between vessels/bleeding regions and background and 1 indicates maximal contrast.
Discussion
Colposcopy combined with biopsy is used in the evaluation and management of patients with cervical lesions, and described as the gold standard for the diagnosis of cervical precancer. In clinical practice, the patients with cervical lesion including CIN2, CIN3, and precancer are at high risk of developing invasive cancer and need active surveillance or immediately treatment7,9. However, the analysis and assessment of precancerous cervical lesions via colposcopy is difficult due to the influence of system factors such as patient movement leading to blurred images, uneven lighting (light fields), and reflections (glare) on the image. Many images obtained have low contrast, multiple combined pathological features, and unclear boundaries between lesion areas, resulting in difficulty interpreting with the naked eye and thus limiting the doctor’s diagnostic ability.
In recent years, numerous image processing and AI integrated algorithms have been introduced to support colposcopy specialists in diagnosis and biopsy. However, most prior efforts concentrate on a single task such as specular reflection removal, or illumination correction using Retinex style enhancement and deep-learning classifiers for lesion recognition12,14,16,17,18. Unlike these approaches that either focus on classification or apply isolated processing steps, CIVI is a unified enhancement framework for unprocessed CWLI that concurrently addresses specular glare, uneven illumination, and low epithelial contrast. The results of the paper are reflected through four main points. Firstly, the proposed method successfully removed specular glare from the cervical surface and incorporated MSRCR for illumination correction, which collectively led to improved visualization of lesion details. Secondly, using the LBP distance to evaluate the contrast between lesional and surrounding tissue, the study confirmed a significantly higher LBP distance in CIVI (0.391 ± 0.127) images compared to the original CWLI images (0.192 ± 0.064). Furthermore, the MC index, which was used to compare the contrast of the vascular area and its background, showed a higher mean MC contrast in CIVI images (0.290 ± 0.116) than in CWLI images (0.216 ± 0.105). This finding demonstrates that CIVI improves the visibility of cervical blood vessels, which is critical for identifying abnormal lesions. Finally, five experts evaluated CIVI images against both the original CWLI and images enhanced with the CLAHE algorithm. The results indicated that the average evaluation score increased by + 0.71 for CIVI compared to CWLI, and decreased by −0.72 for CLAHE compared to CWLI. Improvements were observed to increase from CIN1 to CIN3 cases, as high-grade lesions typically exhibit more prominent pathological features, including extensive lesion areas, distinct vascular patterns, and stronger structural contrast between abnormal and healthy tissue. These characteristics provide greater opportunities for CIVI to enhance visualization, resulting in more pronounced benefits compared to low-grade lesions. Overall, the findings underscore the potential of CIVI to support clinical decision-making, particularly in detecting high-grade lesions where accurate boundary definition and contrast are critical.
To our knowledge, this is the first study to combine specular reflection removal, illumination correction, and contrast optimization into an integrated enhancement framework specifically optimized for CIN imaging. The effectiveness of CIVI was consistent across quantitative metrics (LBP distance and blood/vessel contrast) and subjective expert assessments. At the same time, the CIVI-processed images preserved histological fidelity, enhanced fine details, and balanced illumination in shadowed regions without inducing color distortion, ensuring that the post-processed images remained natural and easy for physicians to read. Although CIVI demonstrated consistent improvements across 52 cases with confirmed histopathology, the study’s reliance on a single-center dataset presents limitations in terms of sample size and diversity. In this pilot clinical study, the CIVI algorithm was performed on a laptop running Windows 10 (64-bit) equipped with an 8th-generation Intel® Core™ i5-8250U CPU, 8 GB RAM, and a 256 GB SSD, using MATLAB (MathWorks, USA). With 1440 × 1080-pixel colposcopy images, the average processing time was ≈ 4.7 s per image, indicating suitability for still-image evaluation rather than real-time video colposcopy. The main computational steps (MSRCR and CLAHE) are highly parallelizable, suggesting substantial speed-ups with GPU support or optimized libraries (e.g., OpenCV). We acknowledge this limitation and consider the present work an initial feasibility assessment toward real-time deployment; future work may also explore the integration of CIVI into real-time video colposcopy platforms, which could facilitate dynamic assessment and enhance its applicability in routine clinical workflows.
Conclusion
This study introduces CIVI, a comprehensive image enhancement algorithm designed to address common visual limitations in white light colposcopy, including glare, uneven illumination, and low contrast in both epithelial structures and vascular patterns. CIVI consistently improved image quality, as reflected in quantitative measurements and expert evaluations, with the most notable gains observed in high-grade cervical intraepithelial neoplasia. In contrast to previous methods that focus primarily on diagnostic classification, CIVI provides a practical and integrated solution for enhancing original CWLI images to support clinical decision-making. These findings suggest that CIVI has the potential to assist visual interpretation during cervical examination. Future research will focus on validating its application within live video colposcopy platforms.
Data availability
The datasets generated and/or analyzed in this study are available from the corresponding author on reasonable request.
Abbreviations
- CIN:
-
Cervical Intraepithelial Neoplasia
- CIVI:
-
Cervical Image Visualization and Improvement
- CLAHE:
-
Contrast-Limited Adaptive Histogram Equalization
- CWLI:
-
Cervical White Light Imaging
- hrHPV:
-
high-risk Human Papilloma Virus
- LBP:
-
Local Binary Pattern
- MC:
-
Michelson Contrast
- MSRCR:
-
Multi-Scale Retinex with Color Restoration
- ROI:
-
Region Of Interest
- SEM:
-
Standard Error of the Mean
- TXI:
-
Texture and Color Enhancement Imaging
- VIA:
-
Visual Inspection with Acetic acid
- VILI:
-
Visual Inspection with Lugol’s Iodine
References
Global strategy to accelerate the elimination of cervical cancer as a public health problem. Geneva: World Health Organization; 2020. Licence: CC BY-NC-SA 3.0 IGO.
Basu, P. et al. Diagnostic accuracy of VIA and HPV detection as primary and sequential screening tests in a cervical cancer screening demonstration project in India. Int. J. Cancer. 137 (4), 859–867 (2015).
Perkins, R. B. et al. 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors. J. Lower Genit. Tract Dis. 24 (2), 102–131 (2020).
Perkins, R. B., Wentzensen, N., Guido, R. S. & Schiffman, M. Cervical cancer screening: a review. Jama 330 (6), 547–558 (2023).
Sellors, J. W. & Sankaranarayanan, R. Colposcopy and Treatment of Cervical Intraepithelial Neoplasia: A Beginner’s Manual (IARC, 2003).
Adelman, M. R. Novel advancements in colposcopy: historical perspectives and a systematic review of future developments. J. Lower Genit. Tract Dis. 18 (3), 246–260 (2014).
Khan, M. J. et al. ASCCP colposcopy standards: role of colposcopy, benefits, potential harms, and terminology for colposcopic practice. J. Lower Genit. Tract Dis. 21 (4), 223–229 (2017).
Smith, S. K. et al. Performance of screening tools for cervical neoplasia among women in low-and middle-income countries: A systematic review and meta-analysis. PLOS Global Public. Health 3(2), e0001598 (2023).
World Health Organization. WHO Guidelines for Screening and Treatment of Precancerous Lesions for Cervical Cancer Prevention (World Health Organization, 2021).
Kim, Y. J. et al. A performance comparison of histogram equalization algorithms for cervical cancer classification model. J. Biomedical Eng. Res. 42 (3), 80–85 (2021).
Fan, J., Liu, J., Xie, S., Zhou, C. & Wu, Y. Cervical lesion image enhancement based on conditional entropy generative adversarial network framework. Methods 203, 523–532 (2022).
Ren, Y., Li, Z. & Xu, C. Cervical precancerous lesion image enhancement based on retinex and histogram equalization. Mathematics 11 (17), 3689 (2023).
Asiedu, M. N. et al. Development of algorithms for automated detection of cervical pre-cancers with a low-cost, point-of-care, pocket colposcope. IEEE Trans. Biomed. Eng. 66 (8), 2306–2318 (2018).
Wang, X. et al. Integration of global and local features for specular reflection inpainting in colposcopic images. J. Healthc. Eng. 2021(1), 5401308 (2021).
Susan, M. J., Subashini, P. & Krishnaveni, M. Comparison of various deep learning inpainting methods in smart colposcopy images. Int. J. Comput. Intell. Stud. 11 (1), 53–72 (2022).
Chen, P., Liu, F., Zhang, J. & Wang, B. Mfem-cin: A lightweight architecture combining Cnn and transformer for the classification of pre-cancerous lesions of the cervix. IEEE Open. J. Eng. Med. Biology. 5, 216–225 (2024).
Darwish, M., Altabel, M. Z. & Abiyev, R. H. Enhancing cervical pre-cancerous classification using advanced vision transformer. Diagnostics 13 (18), 2884 (2023).
Youneszade, N., Marjani, M. & Ray, S. K. A predictive model to detect cervical diseases using convolutional neural network algorithms and digital colposcopy images. IEEE Access. 11, 59882–59898 (2023).
Yan, L. et al. Multi-state colposcopy image fusion for cervical precancerous lesion diagnosis using BF-CNN. Biomed. Signal Process. Control. 68, 102700 (2021).
Allahqoli, L. et al. Diagnosis of cervical cancer and pre-cancerous lesions by artificial intelligence: a systematic review. Diagnostics 12 (11), 2771 (2022).
Sato, T. TXI: texture and color enhancement imaging for endoscopic image enhancement. J. Healthc. Eng. 2021(1), 5518948 (2021).
Koyama, Y. et al. Visibility of early gastric cancers by texture and color enhancement imaging using a high-definition ultrathin transnasal endoscope. Sci. Rep. 13 (1), 1994 (2023).
Ishikawa, T. et al. Efficacy of texture and color enhancement imaging in visualizing gastric mucosal atrophy and gastric neoplasms. Sci. Rep. 11 (1), 6910 (2021).
The MathWorks, Inc. MATLAB and Image Processing Toolbox. Natick, MA, USA. (2016).
Petro, A. B., Sbert, C. & Morel, J. M. Multiscale retinex. Image Process. Line. 4, 71–88 (2014).
Jobson, D. J., Rahman, Z. U. & Woodell, G. A. A multiscale retinex for bridging the gap between color images and the human observation of scenes. IEEE Trans. Image Process. 6 (7), 965–976 (1997).
He, Z. et al. Multi-scale fusion for image enhancement in shield tunneling: A combined MSRCR and CLAHE approach. Meas. Sci. Technol. 35 (5), 056112 (2024).
Khuong, C. P. N. et al. Rapid and efficient characterization of cervical collagen orientation using linearly polarized colposcopic images. J. Innov. Opt. Health Sci. 16(05), 2241001 (2023).
Priyadharsini, C. Retinal image enhancement based on color dominance of image. Sci. Rep. 13, 7172 (2023).
Acknowledgements
This research is funded by Viet Nam National University Ho Chi Minh City (VNU-HCM) under grant number VL2024-20-02. We acknowledge the support of time and facilities from Ho Chi Minh City University of Technology (HCMUT), VNU-HCM for this study.
Author information
Authors and Affiliations
Contributions
T.T.V. and C.P.N.K. implemented the CIVI algorithm and performed image processing. H.P.T. contributed to clinical validation. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Tran, V., Pham, T. & Phan, N. Cervical image visualization and improvement for clinical support in diagnosis and treatment. Sci Rep 15, 41732 (2025). https://doi.org/10.1038/s41598-025-25639-4
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-25639-4