Abstract
Candidiasis is one of the most dangerous human diseases caused by fungi, resulting in high morbidity and mortality worldwide. Epidemiology is crucial for understanding the spread and risk factors of these infections. However, there is a lack of epidemiological data concerning the prevalence of candidiasis in Panama. Here, we collected and analyzed data from the Ministry of Health and reexamined recent literature to investigate the epidemiology of candidiasis in Panama from 2010 to 2020. Additionally, a dashboard was created to facilitate the visualization and management of the obtained data. Overall, the average prevalence rate of candidiasis in Panama was 198 cases per 100,000 inhabitants, with a higher incidence in women than in men. The most affected provinces are Veraguas, Los Santos, and the Guna Yala Comarca, while Panama and Colon recorded few cases. The age groups most affected ranged from 0 to 4 and 20 to 24 years old. The highest mortality rates were observed among children under one year of age and individuals over 65 years old. These findings highlight the importance of conducting larger national studies to create prevention and treatment strategies that are specific to local conditions.
Similar content being viewed by others
Introduction
Systemic mycoses are responsible for approximately 1.5 million human deaths each year1. Candidiasis has been classified by the World Health Organization (WHO) as a public health priority due to its high incidence, significant impact on mortality, and the growing challenges associated with antifungal resistance2. Candida species are opportunistic pathogens capable of establishing a commensal colonization in the human body3. There are over 200 species of Candida, with around 20 known to cause infections in humans4. Of these, C. albicans is the primary causative agent of candidiasis in adult and pediatric patients5.
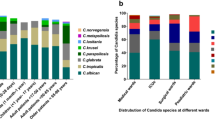
Although C. albicans represents the majority of cases worldwide, other species such as C. parapsilosis, C. glabrata, and C. tropicalis have been pathogenic to humans for several decades6. The emerging number of Candida species resistant to multiple drugs, notably C. auris, is considered a serious problem for the Centers for Disease Control and Prevention7. Suspected isolates of C. auris were detected in Panama, but specialized analysis revealed that most of these isolates were C. duobushaemulonii, a multidrug-resistant species8. This highlights the importance of laboratory surveillance and accurate diagnosis to prevent delays in implementing control measures and providing the necessary treatment9. Candida species are responsible for a wide variety of diseases, ranging from superficial ones such as cutaneous candidiasis (affecting the skin) or mucocutaneous candidiasis (infection of the mucous membranes, skin, and nails), to systemic or invasive candidiasis (generalized infection of deep organs and the bloodstream) and disseminated candidiasis syndrome10,11.
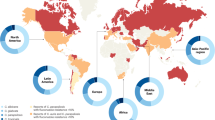
The global prevalence of candidiasis varies depending on the type of infection1. The reported rate of invasive candidiasis is ~ 700,000 cases annually, while the rate of oral candidiasis is around 2 million cases among patients with HIV. Additionally, recurrent vulvovaginal candidiasis affects 134 million women each year, with nearly 500 million women experiencing it at some point in their lives12. Candida infections have a significant economic impact on public health in the United States. Hospitalizations related to these infections generated a total cost of $1.4 billion from 2005 to 2014 is cost was calculated by insurer costs and out-of-pocket costs (such as deductibles, co-payments, and co-insurance), Medicare supplemental insurance, and Medicaid13. Outpatient care for noninvasive candidiasis in the United States accounted for 3.6 million visits and $2.1 billion, with vaginal ($368 million) and oral ($335 million) candidiasis standing out.
The cost of treating patients with candidiasis in Panama is not available, but reports indicate that drug prices are, on average, 27.8% higher than in other Central American countries, such as Colombia and the Dominican Republic14. This cost disparity impacts on the accessibility and adherence to treatment for infections. The high costs in Panama may be attributed to price discrimination, as regulatory measures are relatively weak. The presence of both state and private sector markets, the arbitrary pricing decisions made by manufacturers, and the intense competition among them often adversely affect patients15.
In Panama, candidiasis is a disease that is often overlooked and inadequately reported. Consequently, it has been challenging to fully understand the impact that this condition has on the healthcare system. Recently, the estimated prevalence of candidiasis in Panama was found to be 3,285 cases per 100,000 women of childbearing age16. However, few studies are compiling epidemiological data on this infection in the country. In Panama, the main entities that make up the healthcare system are the Caja de Seguro Social (CSS) and the Ministry of Health (MINSA), which is the main public healthcare network at the primary, secondary, and tertiary levels17. However, there is also a private healthcare sector that is experiencing significant growth. There are more than 900 facilities and resources, but they are concentrated in Panama City, San Miguelito, West Panama, and Chiriquí. Despite advances in recent years, such as the implementation of MINSA-CAPSI or new diagnostic technologies, the system suffers from regional inequalities, limitations in specialized health personnel, and a large gap in modernization, especially in rural areas or indigenous regions.
The goal of this study is to evaluate the prevalence of candidiasis over 11 years across different ages, sexes, and geographical locations in Panama. Additionally, we have developed a tool designed to facilitate the visualization, manipulation, and analysis of data online to increase interaction with research on fungemia, providing support to the healthcare system. This study will provide important information regarding the prevalence, distribution, and risk factors associated with candidiasis. The findings will assist the Panamanian healthcare system in developing strategies for the surveillance and control of fungal infections in the region.
Materials and methods
This retrospective, data-based study was conducted in Panama from 2010 to 2020. The raw data were obtained from the Epidemiology Database within the Health Statistics Information System (SIES), managed by the Department of Health Records and Statistics, under the Ministry of Health (MINSA) (https://www.minsa.gob.pa/informacion-salud/epidemiologia) of Panama. Due to the retrospective nature of the study, the need to obtain informed consent was waived by the Bioethical Committee. All methods were carried out in accordance with relevant guidelines and regulations. Cases were classified and coded according to the Tenth Revision of the International Classification of Diseases (ICD-10)18. The ICD-10 coding corresponds to a classification used by entities responsible for studying the morbidity and mortality of specific cases of different diseases and other health conditions, using an alphanumeric system that facilitates the use, storage, and dissemination of the results obtained (Fig. 1). The National Institute of Statistics and Census (INEC) (https://www.inec.gob.pa/) provided inhabitants data, including age, sex, locality, and year, which were used to calculate age-adjusted morbidity and mortality rates. The data does not include clinical information related to the reported deaths. Therefore, it could be understood that they are due to the primary causes of candidiasis.
The inclusion criteria covered cases of candidiasis reported in the SIES and MINSA databases from 2010 to 2020, including all age groups, specified health regions, and diagnosed types. The data did not specify the institutions or provinces with access to diagnosis of invasive fungal infection (IFI).
Flowchart illustrating the inclusion criteria for candidiasis in Panama. In the identified categories of candidiasis, the letters and numbers correspond to the (ICD-10).
The province of Panama consists of Panama Norte, Panama Metro, Panama Este, Panama Oeste, and San Miguelito, due to the lack of disaggregated estimates from INEC for these subregions, reflecting the urban continuity and socioeconomic homogeneity of these areas. This optimization of resource allocation facilitates effective public health planning.
Data analysis
Generalized Linear Models (GLMs) with a Poisson distribution were employed to analyze prevalence counts, which was essential due to the dataset’s non-homogeneity and non-normality (p < 0.001). The R software (version 4.3.1), along with the MASS package and the glm function, was used for data processing and statistical analyses. The response variable was the overall prevalence of candidiasis, while the predictor variables included age group, health region, and years. Differences in prevalence between genders were assessed using a Chi-Square Goodness-of-Fit test.
The results were visualized through interactive maps and dynamic graphical representations developed in R, using the Tidyverse, ggplot2, and leaflet packages. Additionally, an interactive R Shiny application was developed for real-time exploration of epidemiological morbidity data in Panama19. This application, available on shinyapps.io (GitHub Repository), allows for the analysis of morbidity trends by region, year, cause, age, gender, prevalence, and number of cases, providing an analytical framework for epidemiological studies. The application is based on a modular architecture that separates the user interface (UI) from the server (Fig. 1), ensuring efficient and scalable implementation20. Packages such as dplyr and purrr were used for data manipulation, shinydashboard for structured organization of elements, and shinyjs to enhance interactivity. Additionally, a reactive programming model was implemented using reactive() and observeEvent(), allowing for the dynamic updating of graphs and tables in response to changes in data or user selections.
To enhance performance in processing large datasets, strategies such as lazy loading and caching were implemented21. A crucial aspect of the analysis involved creating a data transformation algorithm to convert unstructured data into a tidy format, optimizing its manipulation and analysis22.This approach led to restructuring the original dataset from 131 rows and 39 columns to a tidy format with 24,200 rows and 7 columns, enabling the use of advanced analytical techniques and the generation of dynamic visualizations within the application.
Confidentiality and anonymity of patient data were maintained following national and international ethical research guidelines. Likewise, all methods were performed following the National guidelines and regulations. The study’s limitations include the potential for underreporting, exclusion of certain institutional data, and biases that could impact the representativeness of the results. To ensure replicability and scalability, all files, functions, and data used are available on GitHub (https://github.com/dannymu/proyecto-inec-app2), allowing for local execution and integration with other projects. This implementation enhances its applicability in public health research, offering a robust platform for exploring epidemiological trends and facilitating evidence-based decision-making.
Results
A total of 85,912 cases of candidiasis were recorded in Panama during the period covered by this study. This data includes cases from outpatient consultations at primary care centers. Considering the cases that met the inclusion criteria of the study, the data were classified according to the clinical types of candidiasis (Table 1).
The average prevalence rate of candidiasis in Panama was 198 cases per 100,000 inhabitants (Table 2). When examining this data disaggregated by sex, it is observed that the mean annual prevalence in men was 60 cases per 100,000 inhabitants. In contrast, the prevalence rate in women was substantially higher (χ² = 193.27, df = 1, p < 0.00001), reaching 337 cases per 100,000 inhabitants.
Spatial distribution of the National overall prevalence of candidiasis in Panama from 2010 to 2020
Significant variability (p < 0.00001) in the prevalence of candidiasis was observed across provinces in Panama. The provinces with the highest prevalence rates, exceeding 500 cases per 100,000 inhabitants, were Los Santos (517 cases) and The Guna Yala Comarca (509 cases), making them the regions with the highest burden of candidiasis (Fig. 2). Other provinces also exhibited high prevalence rates, ranging from 400 to 500 cases per 100,000 inhabitants, including Veraguas (n = 444) and Darien (n = 424) (Fig. 2). In contrast, Bocas del Toro showed a moderate prevalence of 336 cases per 100,000 inhabitants (Fig. 2). At the other end of the spectrum, the provinces with the lowest prevalence rates, ranging between 100 and 300 cases per 100,000 inhabitants, were Chiriqui (n = 242), Herrera (n = 279), Cocle (n = 250), Colon (n = 141), Panama (129 cases), and the Ngäbe Bugle Comarca, which had the lowest prevalence at 128 cases per 100,000 inhabitants (Fig. 2).
Average prevalence of candidiasis by province (2010–2020). Provinces are represented using a color gradient with green indicating the lowest prevalence and red indicating the highest prevalence. The Embera comarca is displayed in gray as there were no reported cases. The pie chart illustrates the distribution of candidiasis cases by type.
Average annual prevalence of candidiasis for each region, separated by sex
Overall, the prevalence of candidiasis varies significantly between sexes (p < 0.0001) in the studied regions, with a higher prevalence observed in females (Fig. 3). Depending on the province, the differences in prevalence between men and women can range from 2 to 10 times. For men, the average annual prevalence of candidiasis was notably higher in the provinces of Darien (214 cases per 100,000 inhabitants) and the Guna Yala Comarca (356 cases per 100,000 inhabitants). In other provinces and comarcas, the value remained below 100 cases per 100,000 inhabitants. During the period 2010–2020, the prevalence of candidiasis among women showed significant variability across different geographical regions (p < 0.0001). Provinces like Los Santos (937 cases per 100,000 inhabitants), Veraguas (802 cases per 100,000 inhabitants), Darien (634 cases per 100,000 inhabitants), and the Guna Yala Comarca (661 cases per 100,000 inhabitants) had prevalences three times higher than provinces such as Panama (219 cases per 100,000 inhabitants), Colon (236 cases per 100,000 inhabitants), and the Ngäbe Bugle Comarca (221 cases per 100,000 inhabitants). Provinces such as Chiriqui (413 cases per 100,000 inhabitants), Cocle (427 cases per 100,000 inhabitants), Herrera (476 cases per 100,000 inhabitants), and Bocas del Toro (556 cases per 100,000 inhabitants) had intermediate values between these two groups (Fig. 3). The variability in candidiasis prevalence during the study period was more pronounced among females. In comparison to the average annual prevalence, the standard deviation fluctuated between 50 and 250 cases. In contrast, males exhibited less variability in prevalence rates, with a standard deviation ranging from 10 to 75 cases (Fig. 3).
Average annual prevalence of candidiasis for each of the study regions in Panama during 2010–2020. The perpendicular lines represent the annual variability.
Prevalence of candidiasis in Panama among different age groups from 2010 to 2020
Although the overall prevalence of candidiasis is higher in females, this difference is not evident at younger ages. In fact, there are no statistically significant differences in prevalence between genders in the group under 4 years of age (p > 0.056). The average annual prevalence in males within this age group (395 cases per 100,000 inhabitants) is much higher than that observed in the other groups, all of which have values of less than 100 cases per 100,000 inhabitants. For women, the groups with the highest average annual prevalence were girls under 4 years of age (480 cases per 100,000 inhabitants) and those aged 15 to 49 years, with an average annual prevalence ranging from 360 to 600 cases per 100,000 inhabitants. The annual variability of prevalence, as shown above, is greater in females (Fig. 4).
Average annual prevalence of candidiasis in Panama for each of the age groups during 2010–2020. The vertical lines represent annual variability.
Fluctuation of the National average prevalence of candidiasis in Panama for each age group from 2010 to 2020
Distinct patterns were observed between men and women when analyzing the annual prevalence of candidiasis by age group from 2010 to 2020. For men, the prevalence remained relatively constant for all age groups above 5 years. However, in children under 5 years, there was a decreasing trend, with cases ranging between 600 and 200 per 100,000 inhabitants (Fig. 5 A). On the other hand, females exhibited varying patterns of prevalence. The group of girls under 5 years experienced a decrease, from 700 cases per 100,000 in 2010 to 230 cases in 2020. Meanwhile, women aged 6 to 64 years had slight fluctuations, with an increase in the period from 2018 to 2019, followed by a decrease. In women over 65 years the prevalence remained relatively constant (Fig. 5B). When averaging the data without distinguishing between sexes, there was a clear decrease in prevalence in the under-5 age group, similar trends among those aged 6 to 64 years, and minimal variation in those over 65 years (Fig. 5 C).
Fluctuation of the national average prevalence of candidiasis in Panama for each of the age groups during 2010–2020. (A) Males, (B) Females, (C) Both sexes.
Mortality due to candidiasis in Panama from 2010 to 2020
During the study period in Panama, mortality from candidiasis totaled 70 cases (Table 3). Vital statistics were obtained from the Comptroller General of the Republic, which was taken from the database of the National Institute of Statistics and Census. Institutional data was provided by the Ministry of Health (MINSA) through the Planning Directorate and its Department of Health Records and Statistics. The province of Panama leads with the highest mortality rate, with a total of 69% of cases, most of which occurred between 2017 and 2019. The other provinces presented the following results: Veraguas with 9%, followed by Colon, Chiriqui, Cocle, and Herrera, all with 4% each, the Ngäbe-Bugle Comarca with 3%, and finally Bocas del Toro and Los Santos, which reported 1%. The Guna Yala Comarca and Darien had no reports of death from candidiasis during the study period. The types of candidiasis reported include sepsis, unspecified, pulmonary, meningitis, Candidiasis in other locations, urogenital, stomatitis, and endocarditis (Table 3).
Discussion
The prevalence of candidiasis cases in Panama (198 cases per 100,000 inhabitants) is lower compared to neighboring countries. The higher prevalence of vulvovaginal candidiasis in women shown in this study is minimal compared to Mexican women, where at least 2.5 million women experience four or more episodes of CVR per year25. Although many of the conditions that occur in Panama are comparable to those in Mexico, such as CVR in women of childbearing age, many of the cases recorded correspond to hospital health levels, fields that would include secondary and tertiary health sectors, which would give rise to incomparable numbers. This is because this study includes cases treated in primary care centers, indicating a marked underestimation of cases. Globally, it is estimated that 70–75% of women will experience vulvovaginitis at least once in their lifetime, and 5–9% will have recurrent cases. In Ecuador, it has been reported that pregnant women have a prevalence of 81% of C. albicans, and it is indicated that the increase in this infection is caused by diabetes, contraceptive use, and hormonal changes33. Additionally, 57% of cases were classified as unspecified candidiasis, which can be contrasted with the 25% prevalence in Africa, where the lack of advanced diagnostic tools (e.g., MALDI-Tof, PCR, or serological tests) hinders correct species identification31. In countries such as Vietnam and Peru, microscopy and culture are available in multiple health centers, ensuring a minimum basis for identification34,35. However, advanced testing remains limited and concentrated in the capital area of the country, leading to underreporting and delays in treatment.
Candidal stomatitis showed a prevalence of 40%, similar to a report in the Greek elderly population (39.6%), where the most associated factor was wearing dentures, accompanied by nighttime use and poor hygiene36. Additionally, the presence of systemic diseases such as diabetes was also noted. The prevalence of candidiasis in certain clinical cases, such as sepsis, pulmonary, urogenital, endocarditis, or skin and nails, was considerably low, with only 1–4 cases reported. Sepsis had a prevalence of 1, which remains low compared to other countries. Invasive candidiasis is the leading cause of fungal sepsis in the ICU, accounting for between 10% and 15% of fungal infections and 5% of all cases of severe sepsis or septic shock37. It tends to occur more frequently in critically ill hospitalized patients, highlighting the vulnerability of this population. Candida meningitis is one of the least common forms, with a prevalence of 0.09/100,000 inhabitants38. The low prevalence of this form of candidiasis may be due to multiple factors; however, it is mainly associated with the inhalation of spores in patients with severely weakened immune systems, which could explain its low incidence. We cannot discard the possibility that this lower prevalence of meningitis could be associated with more marked seasonal changes, e.g., the warmer seasons. This suggests a relationship between warm weather and a decrease in the disease, with countries with warmer climates, such as Panama, having fewer cases of this type. Candida endocarditis accounts for 1% to 2% of global endocarditis cases; however, its association with mortality is significant, as it is seen in 30% to 80% of deaths, and has increased considerably in recent years39. Candidiasis of the skin and nails has a usual prevalence of less than 5.5%, being overshadowed by cases caused by dermatophytes40. Urogenital cases, particularly candiduria, have an approximate frequency of 4.6%, which is consistent with our data41. Pulmonary cases are considered rare and isolated, and are associated with other conditions, mainly tuberculosis or the use of mechanical ventilators42.
Our findings may be influenced by factors such as smaller total inhabitants and limited access to healthcare services in certain regions. More developed countries, like the United States and Canada, also have a higher number of cases per capita due to accessible and efficient diagnosis23,24. In contrast, developing country, such as Irak, have demonstrated a lower number of cases, highlighting the challenges in diagnosing this infection30.
We report a significantly higher prevalence of candidiasis in females, a trend consistently documented in previous studies, especially for vulvovaginal type43,44. Intrinsic conditions in the female body, such as anatomical, metabolic and sociocultural factors, play a crucial role in this difference, as discussed by Vieira-Baptista & Bornstein45. When measuring the prevalence of Candida infections in men, it is important to consider the possibility of asymptomatic pathologies, particularly balanitis. This contributes to the underdiagnosis and underreporting of candidiasis cases in this group, leading to a low prevalence of male candidiasis in the national territory, as seen in this study.
In the case of neonates, the prevalence reported may be associated with multiple risk factors, such as age under 28 days, hospitalization in the intensive care unit, the use of mechanical ventilators, parenteral nutrition, and antibiotics treatment46. It is worth highlighting that in Latin America the rate of candidiasis acquisition presents an HIV-like pattern, as it is transferred from mother to child47. In addition to this spectrum of possible sources of infection, diaper rash can further increase the rates as they are widely used on infants under 5 years of age48.
In pregnant women aged 20 to 24 years, the high incidence of candidiasis reported could be associated with factors such as free unions, the use of intimate soaps, vaginal douching, and, ultimately, the marital status of women49,50. Divorce and widowhood tend to occur more frequently at older ages, which is reflected in the data showing a decrease in the prevalence of candidiasis with increasing age.
The provinces with the highest reported prevalence of candidiasis (Los Santos and Veraguas), are rural areas that are challenging to access. Other studies have also noted the high prevalence of candidiasis in rural areas50,51. This can be attributed to factors such as limited access to healthcare and the impact of population density on prevalence rates. Areas with fewer inhabitants tend to have higher prevalence values due to a smaller denominator. National prevalence rates are also influenced by spatial distribution, with rates increasing in regions farther from the capital city.
In the Ngäbe Bugle Comarca, the low prevalence of candidiasis is likely due to underdiagnosis and underreporting of cases. The Pan-American organization has identified several barriers that indigenous people face, including geographical, socio-cultural, and economic factors, which limit their access to quality medical care52. A notable trend in Panama’s epidemiological data is the significant decrease in candidiasis cases in 2020. This could be attributed to a decreased impact due to the SARS-CoV-2 pandemic53. This suggests that the lack of accurate reporting may have led to the underreporting of actual cases, resulting in a miscount.
The high prevalence of candidiasis in rural areas of Panama can be better understood through an approach that links epidemiological evidence with structural and health determinants. A study conducted at the Morro Solar Health Center in Peru found a significant prevalence of C. albicans (31.27%) in women of childbearing age and revealed that coming from rural areas was statistically significantly associated with higher infection rates (p < 0.05)54. Additionally, among the associated epidemiological factors were the use of antibiotics (17.7%) and, more notably, the non-use of condoms (23.89%), both of which were statistically significant (p < 0.05). This demonstrates how behavioral and exposure factors increase the risk of candidiasis in rural settings.
On the other hand, the PENCYT 2025–2029 Sectoral Notebook indicates that Panama’s public health system faces profound inequalities, such as marked fragmentation, greater concentration of medical personnel and hospital beds in urban areas, and serious challenges of access and coverage in rural and indigenous regions55. Although the analysis provided above does not directly break down candidiasis, the structural determinants described contribute to delayed diagnosis and an overrepresentation of cases in vulnerable rural areas. The high prevalence of candidiasis may be related to multiple factors. Comorbid conditions such as HIV, diabetes, drug-induced immunosuppression, or antibiotic use increase the likelihood of Candida infection and overgrowth56. Also, socioeconomic factors present another way of looking at the situation, as economic inequality leads to unequal access to clinical care and treatment, disparities in sanitation, malnutrition, forced displacement, and other factors that compromise the population’s exposure to environments where fungal proliferation is favorable or that can weaken the immune system in some way.
Panama reported 70 deaths from candidiasis over an eleven-year period. This percentage is relatively low compared to Italy, Spain, Brazil, and Greece, which recorded a monthly mortality rate of approximately 27% due to septic shock57. Mortality in Panama was particularly pronounced among children under one year old. A similar phenomenon was observed in a retrospective study in Taiwan, reporting a hospital mortality rate in neonates of 42%, which is extremely alarming58. The over-65 age group also experiences a significant mortality rate, as many patients in this group may be immunocompromised and have comorbidities, devices, or medications that increase the likelihood of developing septic shock59. More than 85,000 cases of fungal diseases were estimated in Panama in 2022, with recurrent candidiasis being the most common, along with oral and esophageal candidiasis in people with HIV16. It should be noted that candidemia is associated with cancer, diabetes, immunosuppression, or other forms of critical clinical instability, while mucocutaneous cases are related to HIV patients. Vulvovaginal candidiasis does not require predisposing factors to occur. However, the study focused on the prevalence and incidence parameters of cases, excluding mortality cases from in-depth detail. Therefore, the 70 reported cases require a review of clinical parameters and more information from the centers reporting them.
To improve the diagnosis of candidiasis and other fungal infections in Panama, it is essential to implement specific changes in the current health system, inspired by the model developed by Global Action Fund for Fungal Infections (GAFFI) in Guatemala27. This involves strengthening the diagnostic infrastructure by creating specialized reference laboratories and expanding the capacity of regional laboratories to process tests for serious fungal infections. Similarly, it is essential to provide ongoing training to healthcare personnel, including physicians, laboratory technicians, and public health personnel, in the early identification and proper management of these infections.
Various non-culture-based techniques have emerged as appropriate clinical practices for treatment, including antigen detection, PCR-based testing, and next-generation sequencing technologies60. The combination of these techniques increases diagnostic accuracy, leading to better fungal treatment before the patient’s death. Likewise, microfluidic technologies and artificial intelligence systems show the potential to transform diagnosis to faster and less invasive methods. These have already been observed in more robust health systems, which may indicate a correlation between their application and accurate identification of fungal infections61,62. However, unequal access to these techniques, high costs, and a lack of specialized personnel limit their implementation, leading to a lack of timely diagnosis and being a key factor in the underreporting of deaths from fungal infections63.
The utilization of an interactive tool like the dashboard developed in R Shiny signifies a major advancement in the management of epidemiological data in Panama. It also enhances data visualization, allowing for the observation of patterns through geographical or temporal distribution, thereby facilitating a deeper understanding of the available data. This tool has been proven effective in monitoring various diseases such as bluetongue disease, West Nile virus, brucellosis, and malaria60. Additionally, it has played a crucial role in controlling pandemic-level diseases like SARS-CoV-265.
Conclusions
This retrospective study identified patterns of prevalence and mortality associated with candidiasis infections in Panama between 2010 and 2020. Differences between genders, age groups, and regions were highlighted. It is critically important to strengthen epidemiological surveillance, especially in regions like Veraguas and Los Santos which showed a higher number of candidiasis cases and areas like Panama which had higher mortality rates. These findings not only provide a deeper understanding of the behavior of candidiasis in Panama, also serve as a basis for the development of more effective prevention, diagnosis, and treatment strategies, thus contributing to public health decision-making and the strengthening of health policies in the country.
In addition to this, the tool developed for interaction with the data could serve as a key pillar in strengthening the health system in Panama, particularly concerning this disease. Furthermore, it could be adapted or replicated for the epidemiology of other diseases affecting the country.
Data availability
The data used in this study comes from official sources. Data on candidiasis was obtained from the Ministry of Health [(MINSA, [https://www.minsa.gob.pa](https:/www.minsa.gob.pa)), contact email: [consultadincavv@minsa.gob.pa](mailto: consultadincavv@minsa.gob.pa)], while census data was provided by the National Institute of Statistics and Census [(INEC, [https://www.inec.gob.pa](https:/www.inec.gob.pa)), contact email: [cie\_inec@contraloria.gob.pa](mailto: cie_inec@contraloria.gob.pa)]. To access these data, it is recommended to contact the corresponding institutions directly or visit their official platforms mentioned above.
References
Bongomin, F., Gago, S., Oladele, R. O. & Denning, D. W. Global and multi-national prevalence of fungal diseases—estimate precision. Journal of Fungi 3, Preprint at https://doi.org/10.3390/jof3040057 (2017).
World Health Organization. WHO Fungal Priority Pathogens List to Guide Research, Development and Public Health Action. (2022). https://www.who.int/publications-detail/9789240060241
Hube, B. From commensal to pathogen: stage- and tissue-specific gene expression of Candida albicans. Curr. Opin. Microbiol. 7, 336–341 (2004).
Samanta, I. Springer India,. Cutaneous, subcutaneous and systemic mycology. In Veterinary Mycology 11–153 https://doi.org/10.1007/978-81-322-2280-4_4 (2015).
Mantilla-Florez, Y. F., Tuta-Quintero, E., Brito-Rodriguez, A. J. & Clavijo-Moreno, L. C. Candidiasis and Candida albicans. Bol. Malariol. Salud Ambient. 61, 391–400 (2021).
Bilal, H. et al. Distribution and antifungal susceptibility pattern of Candida species from Mainland china: A systematic analysis. Virulence 13 (1), 1573–1589. https://doi.org/10.1080/21505594.2022.2123325 (2022).
Talapko, J. et al. Candida albicans-The virulence factors and clinical manifestations of infection. J. Fungi (Basel). 7 (2), 79. https://doi.org/10.3390/jof7020079 (2021). PMID: 33499276; PMCID: PMC7912069.
Araúz, A. B. et al. Isolation of Candida auris from 9 patients in Central America: Importance of accurate diagnosis and susceptibility testing. Mycoses. 61(1):44–47. (2018). https://doi.org/10.1111/myc.12709. Epub 2017 Oct 16. PMID: 28945325.
Villanueva Reyes, J. A. R. Candidiasis mucocutánea: Una revisión. Revista Mexicana De Micología. 25, 91–104 (2007).
Cornely, O. A. et al. Global guideline for the diagnosis and management of candidiasis: an initiative of the ECMM in cooperation with ISHAM and ASM. The Lancet Infectious Diseases. 25, e280–e293 Preprint at (2025). https://doi.org/10.1016/S1473-3099(24)00749-7
McKloud, E. et al. Recurrent vulvovaginal candidiasis: a dynamic interkingdom biofilm disease of Candida and Lactobacillus. mSystems 6, (2021).
Benedict, K., Jackson, B. R., Chiller, T. & Beer, K. D. Estimation of direct healthcare costs of fungal diseases in the united States. Clin. Infect. Dis. 68, 1791–1797 (2018).
Ministerio de Salud. Estudio de Precios de Medicamentos En El Sector Privado En Panamá https://www.minsa.gob.pa (2018).
Gómez Pérez, J. A. Panamá, Mercado de medicamentos: Intervención estatal y política de precios. D´Economía 2, 13–29 (2022).
Rodríguez-Vargas, C., Alastruey-Izquierdo, A. & Denning, D. W. & Belén Araúz, A. Estimated burden of fungal infections in Panama. Journal Med. Mycology 34, 101466 (2024).
Ministerio de Salud de Panamá. Listado De Instalaciones Por región De Salud MINSA-CSS (Año 2020) (Dirección de Planificación de la Salud – Departamento de Registros y Estadísticas de Salud. Panamá, 2021).
World Health Organization. International Statistical Classification of Diseases and Related Health Problems. (2016).
Tahir ul Qamar, M., Noor, F., Guo, Y. X., Zhu, X. T. & Chen, L. L. Deep-HPI-pred: an R-Shiny applet for network-based classification and prediction of Host-Pathogen protein-protein interactions. Comput. Struct. Biotechnol. J. 23, 316–329 (2023).
Zhao, Z. et al. Online application for the diagnosis of atherosclerosis by six genes. PLoS One 19, e0301912 (2024).
Malladi, S. et al. ASF Shiny app: an interactive web application for exploring premovement active surveillance scenarios for early African swine fever detection. iSoftwareX 30, 102105 (2025).
Murillo-Gonzalez, D. & Anino, Y. Automating the Transformation of Tidy Data on Morbidity Causes from INEC with R. in Proceedings – 2024 9th International Engineering, Sciences and Technology Conference, IESTEC 404–409 (Institute of Electrical and Electronics Engineers Inc., 2024). https://doi.org/10.1109/IESTEC62784.2024.10820295 (2024).
Dufresne, S. F., Cole, D. C., Denning, D. W. & Sheppard, D. C. Serious fungal infections in Canada. Eur. J. Clin. Microbiol. Infect. Dis. 36, 987–992 (2017).
Rayens, E. & Norris, K. A. Prevalence and healthcare burden of fungal infections in the united States, 2018. Open Forum Infect. Dis 9, ofab593 (2022).
Corzo-León, D. E., Armstrong-James, D. & Denning, D. W. Burden of serious fungal infections in Mexico. Mycoses 58, 34–44 (2015).
Agudelo Higuita, N. I., Bustillo, V., Denning, D. W. & D. & Burden of serious fungal infections in Honduras. Mycoses 65, 429–439 (2022).
Medina, N. et al. Burden of serious fungal infections in Guatemala. Eur. J. Clin. Microbiol. Infect. Dis. 36, 965–969 (2017).
Darce Bello, M., Gonzalez, A., Barnabé, C. & Larrouy, G. First characterization of Candida albicans by random amplified polymorphic DNA method in Nicaragua and comparison of the diagnosis methods for vaginal candidiasis in Nicaraguan women. Mem Inst. Oswaldo Cruz Rio De Janeiro 97, 985–9 (2002).
Rodriguez-Tudela, J. L. et al. Burden of serious fungal infections in Spain. Clin. Microbiol. Infect. 21, 1–7 (2014).
Mohammad, K. A. et al. Fungal disease incidence and prevalence in Iraq – Preliminary estimates. Journal Med. Mycology 34, 101516 (2024).
Okoye, C. A., Nweze, E. & Ibe, C. Invasive candidiasis in Africa, What is the current picture? Pathogens and Disease 80 1–17. https://doi.org/10.1093/femspd/ftac012 Preprint at (2022).
Riera, F. O., Caeiro, J. P. & Denning, D. W. Burden of serious fungal infections in Argentina. Journal Fungi 4, 51 (2018).
Chila Santana Louis Alfonso. Anzules Guerra Jazmín Beatriz; Milian Hernández Eduardo Josué; Izaguirre Bordelois Marioneya. Perfil clínico microbiológico de La candidiasis vulvovaginal En mujeres Embarazadas. Higia De Salud Revista Científica Biomédica Del. ITSUP 6, https://revistas.itsup.edu.ec/index.php/Higia/article/view/651/1296 (2022).
Hieu, V. N. et al. Mycology laboratory diagnostic capacity for invasive fungal diseases in public hospitals in Vietnam. Med Mycol 62, myae082 (2024).
Maquera-Afaray, J. et al. Fungi under fire: diagnostic capacities and antifungal availability in Peruvian healthcare facilities. Microbiol Spectr 13, e0202024 (2025).
Kossioni, A. E. The prevalence of denture stomatitis and its predisposing conditions in an older Greek population. Gerodontology 28, 85–90 (2011).
Delaloye, J. & Calandra, T. Invasive candidiasis as a cause of sepsis in the critically ill patient. Virulence. 5, 154–162 Preprint at https://doi.org/10.4161/viru.26187 (2014).
Okike, I. O. et al. Trends in bacterial, mycobacterial, and fungal meningitis in England and Wales 2004-11: an observational study. Lancet Infect. Dis. 14, 301–307 (2014).
Arnold, C. J. et al. Candida infective endocarditis: an observational cohort study with a focus on therapy. Antimicrob. Agents Chemother. 59, 2365–2373 (2015).
Leung, A. K. C. et al. Onychomycosis: an updated review. Recent. Pat. Inflamm. Allergy Drug Discov. 14, 32–45 (2019).
Konje, E. T. et al. Five-year cross-sectional study to determine the burden of Candida spp. Infections of the urinary tract system among patients attending tertiary hospital in Northwestern Tanzania. BMJ Open 13, e074833 (2023).
Meena, D. S. & Kumar, D. Candida pneumonia: an innocent bystander or a silent killer? Med. Principles Pract. 31, 98–102 (2022).
Corsello, S. et al. An epidemiological survey of vulvovaginal candidiasis in Italy. Eur. J. Obstet. Gynecol. Reproductive Biology. 110, 66–72 (2002).
Yano, J. et al. Current patient perspectives of vulvovaginal candidiasis: incidence, symptoms, management and post-treatment outcomes. BMC Womens Health 19, 48 (2019).
Vieira-Baptista, P., Bornstein, J. & Candidiasis, Bacterial Vaginosis, trichomoniasis and other vaginal conditions affecting the vulva. In Vulvar Disease: Breaking the Myths (ed. Springer) 167–205 (Springer International Publishing, 2019). https://doi.org/10.1007/978-3-319-61621-6_24.
Santolaya, M. E. et al. Recommendations for the management of candidemia in neonates in Latin America. Rev. Iberoam Micol. 30, 158–170 (2013).
Castillo-Martínez, N. A., Mouriño-Pérez, R. R. & Cornejo-Bravo, J. M. Gaitán-Cepeda, L. A. Factores relacionados a candidiasis oral En niños y adolescentes Con VIH, caracterización de especies y susceptibilidad antifúngica. Revista Chil. De Infectología. 35, 377–385 (2018).
Lopez Granja, J. Dermatitis Del pañal. Revisión. Belize J. Med. 4, 8–11 (2015).
Bermúdez, M. L. Gabriela;, Caba Canaza Denis Aldo;, Enríquez Salazar Helen Cintia;, Palma mancilla Reinaldo Junior; & Nava Carpio Fernando. Factores asociados a candidiasis vaginal En mujeres En edad fértil En El servicio de ginecología Del Centro de Salud San Jorge Del municipio de Zudáñez En El bimestre Octubre- Noviembre Del 2012. Archivos Bolivianos De Medicina 18, 7–16 (2012).
Fule, S. R., Das, D. & Fule, R. P. Detection of phospholipase activity of Candida albicans and Non albicans isolated from women of reproductive age with vulvovaginal candidiasis in rural area. Indian J. Med. Microbiol. 33, 92–95 (2014).
Ramesh Swaminathan, K., Devi, M., Thomas, M., Gerald, B., Prakesh, S. C. & S. & Prevalence of vulvovaginal candidiasis in the women of the reproductive age, in rural India. Int. J. Clin. Obstet. Gynecol. 1, 37–39 (2017).
Organización Panamericana de la Salud. Clasificación Estadística Internacional de Enfermedades y Problemas Relacionados Con La Salud. vol. 1 (OPS, Oficina Sanitaria Panamericana, Oficina Regional de la Organización Mundial de la Salud, Washington, D.C. (2008).
Al-Hatmi, A. M. S., Mohsin, J., Al-Huraizi, A. & Khamis, F. COVID-19 associated invasive candidiasis. J. Infect. 82, 45–46 (2020). https://doi.org/10.1016/j.jinf.2020.08.005 Preprint at.
Sayago Alabrin, B. A. W., Diaz, O., Ubillus, B. R. A., Fernández, J. E. & Guerrero, R. M. Rodríguez Neyra, Bach. M. R. Candida albicans y Su relación Con factores epidemiológicos En mujeres En edad fértil Atendidas En El Centro Salud Morro Solar – Jaén 2019. Ciencia Latina Revista Científica Multidisciplinar. 7, 4786–4802 (2023).
Secretaría, N. & de Ciencia, T. e I. (SENACYT). Plan Estratégico Nacional de Ciencia, Tecnología e Innovación En Salud 2025–2029. (2025).
Rivas-Pinedo, P., Motta, J. C. & Gutierrez, J. M. O. Invasive Candidiasis in Contexts of Armed Conflict, High Violence, and Forced Displacement in Latin America and the Caribbean (2005–2025). Journal of Fungi 11 Preprint at https://doi.org/10.3390/jof11080583 (2025).
Bassetti, M. et al. A multicenter multinational study of abdominal candidiasis: epidemiology, outcomes and predictors of mortality. Intensive Care Med. 41, 1601–1610 (2015).
Hsu, J. F. et al. Comparison of the incidence, clinical features and outcomes of invasive candidiasis in children and neonates. BMC Infect. Dis 18, 1–11 (2018).
Dekkers, B. G. J. et al. Invasive candidiasis in the elderly: considerations for drug therapy. Drugs Aging. 35, 781–789 (2018).
Fang, W. et al. Diagnosis of invasive fungal infections: challenges and recent developments. Journal of Biomedical Science. 30 Preprint at https://doi.org/10.1186/s12929-023-00926-2 (2023).
Yadav, C. P. & Sharma, A. National Institute of malaria Research-Malaria dashboard (NIMR-MDB): A digital platform for analysis and visualization of epidemiological data. The Lancet Reg. Health 5, 100030 (2022).
Fernandez-Lozano, C. & Cedron, F. Shiny dashboard for monitoring the COVID-19 pandemic in Spain. Proc. West. Mark. Ed. Assoc. Conf. 51, 23 (2020).
Chin, C. D. et al. Microfluidics-based diagnostics of infectious diseases in the developing world. Nat. Med. 17, 1015–1019 (2011).
Menzin, J. et al. Mortality, length of hospitalization, and costs associated with invasive fungal infections in high-risk patients. Am. J. Health-System Pharm. 66, 1711–1717 (2009).
Acknowledgements
This work was funded by the National Secretariat of Science and Technology of Panama (SENACYT) through the National Research System received by L.A.R.-C. I.C.A. and L.A.R.-C. also received support from the Universidad de Panamá (CUFI-2023-CNET-EG-015). We also thank MINSA and INEC for providing the fundamental databases for this study.
Author information
Authors and Affiliations
Contributions
I.C.A. was responsible for developing the study, drafting the manuscript, and contributing to statistical analyses. D.M. and Y.A., performed the statistical analyses and contributed to interpreting the results. L.A.R.-C. conceived the main concept and contributed to the revision and proofreading of the paper, providing guidance on the structure and approach of the study. All authors reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Arana, I.C., Añino, Y., Murillo, D. et al. Nationwide epidemiology of candidiasis in Panama, 2010–2020. Sci Rep 15, 43223 (2025). https://doi.org/10.1038/s41598-025-27218-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-27218-z